STUDY. fungoides (FMF) is an uncommon
|
|
|
- Richard Manning
- 5 years ago
- Views:
Transcription
1 STUDY Folliculotropic Mycosis Fungoides Single-Center Study and Systematic Review Julia S. Lehman, MD; Robert H. Cook-Norris, MD; Brent R. Weed, MD; Roger H. Weenig, MD; Lawrence E. Gibson, MD; Amy L. Weaver, MS; Mark R. Pittelkow, MD Objectives: To clarify clinicopathologic features and reconcile discrepancies in previous studies of folliculotropic mycosis fungoides (FMF). Design: A single-center retrospective clinicopathologic study and a systematic review of FMF. Setting: Tertiary referral center in the midwestern United States. Patients: Patients with clinical and histopathologic evidence of FMF seen at the tertiary referral center during a year period. Main Outcome Measures: Clinicopathologic features of FMF. Results: Fifty patients (32 male [64%] and 18 female [36%]) met study criteria for the clinicopathologic review. Pruritic patches, plaques, and folliculocentric lesions (milia, cysts, and alopecia) on the head, neck, and trunk were common clinical findings. The mean time to diagnosis of FMF was 5.0 years. Diagnostic latency did not affect risk of death. One-year and 5-year overall survival rates were 96% and 62%, respectively. Frequent microscopic features were follicular mucinosis (74%) and epidermotropism (54%). Systematic review of 186 additional patients confirmed male predominance (ratio of men to women, 3.2:1.0), prevalent pruritus (73%), frequent follicular mucinosis (69%) and epidermotropism (37%) microscopically, and common head, neck, and trunk involvement. Combined data demonstrated that 6% of patients with FMF had concurrent non mycosis fungoides hematologic malignant neoplasms and that the 5-year overall survival rate was 62% to 64%. Conclusion: Folliculotropic mycosis fungoides has distinct clinical and microscopic features and is associated with a poor 5-year overall survival rate. Arch Dermatol. 2010;146(6): Author Affiliations: Department of Dermatology (Drs Lehman, Cook-Norris, Weed, Weenig, Gibson, and Pittelkow) and Division of Biostatistics (Ms Weaver), Mayo Clinic, Rochester, Minnesota. Dr Weenig is now with Associated Skin Care Specialists, PA, Fridley, Minnesota. FOLLICULOTROPIC MYCOSIS fungoides (FMF) is an uncommon subtype of mycosis fungoides that seems to have a more aggressive natural history than other forms of mycosis fungoides as demonstrated in the results of stage-for-stage comparisons. 1,2 The clinical presentation of FMF often differs from the patches and plaques of classic mycosis fungoides and may be associated with decreased clinical suspicion for mycosis fungoides. Moreover, histopathologic findings regarding FMF are varied and may be subtle. These factors may account for a prolonged time to diagnosis. For editorial comment see page 662 The characteristics of FMF have been published in previous clinical and histopathologic studies and case series. 1-8 The objectives of the present study were to corroborate or challenge previous observations of FMF, to reconcile inconsistencies in findings, and to expand existing knowledge regarding clinical, histopathologic, and therapeutic observations and CME available online at biologic behavior. To achieve these goals, we reviewed the clinical and histopathologic features of FMF in patients who were seen at Mayo Clinic, Rochester, Minnesota, during years. We also conducted a systematic review and compared our results with those published in the medical literature. METHODS This study was approved by the Mayo Clinic Institutional Review Board. We searched the medical index at Mayo Clinic (Rochester, Minnesota) for patients who received a diagnosis of 607
2 16 Patients excluded with initial screen because of false-positive diagnosis (eg, follicular adenoma of thyroid) 38 Patients excluded with medical record and biopsy specimen review because inclusion criteria were not met Figure 1. Study flow diagram. 104 Patients identified with electronic medical database search 50 Patients included FMF between January 1, 1995, and July 31, We searched for the terms follicular, folliculotropic, pilotropic, adnexotropic, and syringotropic, as well as variations of them. We also searched the Mayo Clinic dermatopathology database for these terms. Our search was conducted in accord with Minnesota statute ; we included only patients who had not denied access to their medical records for research purposes. Clinical inclusion criteria were the following: medical record with clinical descriptions from our institution; persistent cutaneous lesions compatible with FMF; and papules, patches, plaques, nodules, pustules, or erythroderma. Histopathologic inclusion criteria were cutaneous biopsy specimens available for review, histopathologic findings consistent with mycosis fungoides, atypical lymphoid infiltrate surrounding or involving perifollicular epithelium, CD4 predominance of lymphocytic infiltrate (when immunohistochemistry had been performed), epidermotropism (supportive criterion), and follicular mucinosis (supportive criterion). Two patients with typical clinical findings of FMF (alopecic plaques) were included, despite the absence of folliculotropism but the presence of atypical lymphocytes manifesting syringotropism microscopically in 1 patient and the absence of a hair follicle in biopsy specimens available but the presence of papillary dermal and epidermotropic atypical lymphocytes in the other patient. All available histopathology slides for patients who received a clinical or histopathologic diagnosis of FMF (or a synonym) were reviewed by a board-certified dermatopathologist (R.H.W.) or by an experienced dermatopathology fellow (B.R.W.). Several slides were reviewed by both observers to ensure consistency. The following data were noted: character of inflammatory infiltrate, features of immunohistochemical staining when available, presence or absence of large-cell transformations or dermal tumors, and evidence of folliculotropism, syringotropism, epidermotropism, or follicular mucinosis. Histopathologic findings for multiple biopsy specimens were combined on a per-patient basis to facilitate analysis. We reviewed the electronic medical record of each patient who had microscopically confirmed FMF. The recorded clinical features included the following when available: sex, age at symptom onset, physical findings, clinical course, time between symptom onset and diagnosis of mycosis fungoides, time between symptom onset and diagnosis of FMF, other clinical characteristics (such as associated symptoms, presence of draining material, and presence of hematologic or oncologic comorbidities), and results of relevant radiologic imaging and molecular-based studies (ie, results of flow cytometric immunotyping and T-cell receptor [TCR] gene rearrangement analysis of the involved skin or peripheral blood). Standard descriptive statistics were used to summarize the data. For survival analysis, duration of follow-up was calculated from the date of the mycosis fungoides diagnosis to the date of the last follow-up or death. Overall survival was estimated using the Kaplan-Meier method. Adverse clinical outcomes were defined as the development of nodules, erythroderma, microscopically confirmed extracutaneous involvement, or death from disease. Time to the first adverse clinical outcome was calculated from the date of onset of skin lesions; for patients without an adverse clinical outcome, the interval was censored at the date of the last clinical follow-up. Separate univariate Cox proportional hazards regression models were fit to evaluate the association between patient characteristics and time to death or time to first adverse clinical outcome. The hazard ratio (HR) that was estimated from the Cox proportional hazards regression model and the corresponding 95% confidence interval (CI) were used to summarize the associations. All calculated P values were 2-sided, and P.05 was considered statistically significant. Analyses were performed using commercially available statistical software (SAS, version 9.1; SAS Institute, Inc, Cary, North Carolina). For our systematic review, the clinical, histopathologic, molecular, and prognostic data from our study were compared with those from previous retrospective clinical and histopathologic studies and case series of FMF, 1-8 which we identified using PubMed searches and bibliographic cross-referencing. Search terms included folliculotropic mycosis fungoides, pilotropic mycosis fungoides, follicular mycosis fungoides, and adnexotropic mycosis fungoides. Studies describing 3 or more patients with FMF were included. Whenever possible, data were combined by weighted mean. RESULTS CLINICAL FEATURES Fifty patients met study inclusion criteria (Figure 1). Characteristics of 50 study patients (32 male and 18 female) are summarized in the first column of etable 1 ( The mean interval between onset of symptoms and diagnosis of mycosis fungoides was 3.9 years. The mean age at diagnosis of mycosis fungoides (57.7 years) was similar to the mean age at diagnosis of FMF (58.8 years). For 31 patients, folliculotropic lesions were recognized at or before the time of microscopic diagnosis of mycosis fungoides. The mean age at diagnosis of mycosis fungoides was significantly older for women than for men (63.1 years vs 54.6 years; P=.04, 2-sample t test). Five patients (4 male and 1 female) were younger than 40 years at the time of diagnosis of mycosis fungoides. Of 41 patients whose medical record included staging data at the time of diagnosis, most patients (30 [73%]) had skin involvement only, without erythroderma. Four patients (10%) had generalized erythroderma. Six patients (15%) had clinical lymphadenopathy but negative microscopic findings from a lymph node biopsy, and only 1 patient (2%) had microscopically confirmed nodal involvement. One patient was found to have visceral involvement at the time of staging. Clinical features at the time of initial presentation are listed in Table 1, and representative clinical images are shown in Figure 2. Of 47 patients whose symptoms were recorded, 44 (94%) had symptoms that were associated with their skin disease, including pruritus (35 patients [74%]) and pain (13 patients [28%]). Mucinorrhea (ie, 608
3 Table 1. Clinical Characteristics of Patients With Folliculotropic Mycosis Fungoides in the Present Study and in Previous Retrospective Studies and Case Series a Variable Present Study (n=50) van Doorn et al, 1 (n=51) Gerami et al, (n=43) Source, No./Total No. (%) Gerami and Guitart, (n=34) Cerroni et al, 6 (n=28) Hodak et al, Vergier et al, Flaig et al, Pereyo et al, (n=3) Combined Data, % Anatomical Area Head and neck 29 (58) 45 (88) 37 (86) 20/25 (80) b 14 (50) 2 (22) NA NA 3 (100) 72 Trunk 30 (60) NA 41 (95) NA 23 (82) 8 (89) NA NA 3 (100) 79 Extremities 38 (76) NA NA NA 9 (32) 6 (67) NA NA 3 (100) 62 Genitalia and buttocks 10 (20) NA NA NA NA 1 (11) NA NA NA 19 Morphologic Features of Lesions Patches, plaques, or 49 (98) 44 (86) 32 (74) 4/27 (15) c 26 (93) 7 (78) 7 (78) NA 2 (67) 78 papules Nodules 9 (18) 14 (27) 26 (60) NA 0 1 (11) NA NA 1 (33) 27 Erythroderma 4 (8) 3 (6) 3 (7) NA 2 (7) 0 NA NA NA 7 Alopecia 19 (38) NA 28 (65) NA NA 7 (78) 3 (33) NA NA 51 Folliculocentric lesions 25 (50) 4 (8) NA NA NA 9 (100) 9 (100) NA 3 (100) 41 such as milia, cysts, and acneiform lesions Mucinorrhea d 6/47 (13) 3 (6) A few cases NA NA NA NA NA NA 9 Pruritus 35/47 (74) Most patients 30 (70) NA NA NA NA NA 3 (100) 73 Comorbid Malignant Neoplasms Hematologic 3 (6) NA 2 (5) NA NA NA NA NA NA 5.5 Solid organ 5 (10) NA NA NA NA 2 (22) NA NA NA 11.8 Abbreviation: NA, data were unavailable or were unavailable in a format amenable to direct comparison. a Whether some of the patients in the study by Gerami et al 2 also were reported in the study by Gerami and Guitart 3 is unknown. Whether some of the patients in the study by Cerroni et al 6 also were reported in the study by Flaig et al 8 is unknown. b Limited anatomic distribution of disease data available for 25 patients. c Limited disease morphologic data available for 27 patients. d When mucinorrhea was not addressed, it was assumed to be absent. A B C D E F Figure 2. Clinical findings in folliculotropic mycosis fungoides. A, Alopecic patch. B, Folliculocentric umbilicated papules with overlying excoriation. C and D, Diffuse perifollicular inflammatory papules coalescing into plaques. E, Cystlike nodules. F, Nodules with associated alopecia. 609
4 A SYSTEMIC INVOLVEMENT DATA Twelve patients (24%) with localized FMF had distant lymph node involvement, which was detected radiographically (9 patients [18%]), histologically (6 patients [12%]), or in both ways. Peripheral smear results for 37 patients indicated that 11 patients (30% of those tested) had unequivocal evidence of circulating convoluted lymphocytes (Sézary cells); 2 of these patients also had generalized erythroderma. Four of 37 patients who had peripheral smears had equivocal evidence of Sézary cells, and 1 of these patients had generalized erythroderma. One of 13 patients who underwent bone marrow biopsy had disease involvement of the marrow. HISTOPATHOLOGIC CHARACTERISTICS B Figure 3. Microscopic findings in folliculotropic mycosis fungoides. Atypical T lymphocytes surround and involve the pilosebaceous unit (hematoxylin-eosin, original magnification 100). A, Infundibulocystic change. B, Epidermotropism and follicular mucinosis. fluid expression from follicular ostia) was present in 6 patients (13%), of whom 5 had histopathologic evidence of follicular mucinosis. At presentation, 4 patients had erythroderma. During the follow-up period, 1 patient demonstrated the development of erythroderma and the presence of Sézary cells, which were identified on peripheral smear. Among 50 patients in the study, the most common dermatologic diagnoses attributed to the eruptions (diagnoses later determined to be FMF) included the following: dermatitis(25 patients[50%]), follicular mucinosis(11 patients [22%]), dermatophyte infection (8 patients [16%]), psoriasis (6 patients [12%]), and folliculitis (4 patients [8%]). Several patients had more than 1 previous dermatologic diagnosis. One patient had a forehead nodule diagnosed previously as unspecified peripheral T-cell lymphoma. Seven patients (14%) had a concomitant malignant neoplasm, and 1 of these 7 patients had both breast cancer and a B-cell lymphoproliferative disorder (Table 1). Hematologic comorbidities included chronic lymphocytic leukemia (2 patients [4%]) and unspecified B-cell lymphoproliferative disorder (1 patient [2%]). Oncologic comorbidities included breast cancer (2 patients [4%]) and bladder cancer, lung adenocarcinoma, and prostate cancer (1 patient each [2%]). One patient had monoclonal gammopathy of undetermined significance. Histopathologic features are summarized in etable 2, and representative photomicrographs are shown in Figure 3. Prominent syringotropism of atypical lymphocytes without folliculotropism was noted in 1 biopsy specimen, and prominent syringotropism was present in another biopsy specimen in which no hair follicle could be found in numerous sections. Both patients had clinical evidence of follicular involvement (associated alopecia) and were included in the analysis. Immunohistochemical data were available for biopsy specimens from 42 patients (84%), with staining of neoplastic lymphoid cells in all specimens indicating a CD3 CD4 CD8 immunophenotype. The presence of tissue eosinophilia had low sensitivity (19%) but much higher specificity (70%) for predicting pruritus. MOLECULAR DATA Flow cytometric immunotyping was performed on peripheral blood of 31 patients (62%), resulting in the identification of an unequivocal circulating clone in the specimens from 7 patients (23% of those tested). For 3 patients, the circulating clone was attributed to a lymphoproliferative malignant neoplasm other than mycosis fungoides. To detect TCR gene rearrangement clones, polymerase chain reaction or flow cytometry studies were performed on the peripheral blood of 17 patients (34%). A clonal population of T cells was identified in the peripheral blood of 8 patients (47% of those tested), one of whom had another lymphoproliferative malignant neoplasm. Polymerase chain reaction or flow cytometry studies were performed on the lesional skin of 21 patients, revealing a clone in the specimens from 15 patients (71%). Of 9 patients whose peripheral blood and lesional skin were tested for TCR gene rearrangement, 6 had a clone detected in both tissues. Of 4 patients in whom the peripheral blood clone was compared with that of the skin, 2 had identical clones. Of patients who had both skin and peripheral blood specimens tested for TCR gene rearrangement clones, all were found to have positive clones in lesional skin tissue. OVERALL FOLLOW-UP AND SURVIVAL General follow-up data were available for 47 patients (94%), and treatment data were available for 43 patients (86%). Among 15 patients known to be deceased, the 610
5 Table 2. Treatment and Prognostic Data from the Present Study and From Previous Retrospective Studies and Case Series a Variable Present Study (n=50) van Doorn et al, 1 (n=51) Gerami et al, (n=43) Source Gerami and Guitart, (n=34) Cerroni et al, 6 (n=28) Most Common Initial Treatment Before Diagnosis of Mycosis Fungoides, No. (%) Topical corticosteroids 22 (44) NA NA NA NA NA NA NA NA 44 Oral antibiotics 11 (22) NA NA NA NA NA NA NA NA 22 Systemic corticosteroids 9 (18) NA NA NA NA NA NA NA NA 18 Initial Mycosis Fungoides Directed Treatment, No./Total No. (%) PUVA with or without 21/47 (45) 22 (43) 20 (47) NA NA 5 (56) 1 (11) NA 0 43 other therapies Total-body electron beam 2/47 (4) b 18 (35) 1 (2) NA NA 1 (11) 4 (44) NA 2 (67) 17 irradiation or other radiation therapy Other b 27/47 (57) 11 (22) 16 (37) NA NA 3 (33) 8 (89) NA 1 (33) 41 Clinical Status at Last Follow-up, No./Total No. (%) Alive Without disease 1/47 (2) 5 (10) NA NA 2 (7) 3/7 (43) 4 (44) NA 0 10 With disease 31/47 (66) 20 (39) NA NA 17 (61) 4/7 (57) 4 (44) NA 3 (100) 54 Dead Of FMF 3/47 (6) 20 (39) NA NA 7 (25) 0 c 1 (11) NA 0 21 Of unknown or other cause 12/47 (26) 6 (12) NA NA 2 (7) 0 c 0 NA 0 14 Overall Survival Rate, y, % d NA NA NA NA NA NA NA NA NA d NA NA NA NA NA NA NA NA NA d NA NA NA NA NA NA NA 10 NC NA NA NA NA NA NA NA 15 NC NA NA NA e NA NA NA NA NA Hodak et al, Vergier et al, Flaig et al, Pereyo et al, (n=3) Combined Data, % Abbreviations: FMF, folliculotropic mycosis fungoides; NA, data were unavailable or were unavailable in a format amenable to direct comparison; NC, not calculated because fewer than 10 patients still at risk; PUVA, psoralen UV-A. a Whether some of the patients in the study by Gerami et al 2 also were reported in the study by Gerami and Guitart 3 is unknown. Whether some of the patients in the study by Cerroni et al 6 also were reported in the study by Flaig et al 8 is unknown. b Includes topical corticosteroids, nitrogen mustard, narrow-band UV-B phototherapy, extracorporeal photopheresis, topical or oral retinoids, and no therapy. c Treatment response reported in 7 patients. d No follow-up data were available for 3 patients. e After a mean follow-up period of 125 months, 7 patients had died of complications of mycosis fungoides. After a mean follow-up period of 61 months, 19 patients were alive. Two patients died of unrelated causes at 48 months and at 59 months. mean follow-up period from mycosis fungoides diagnosis to death was 3.3 years (range, years). Among 32 patients alive at last follow-up, the median duration from diagnosis of mycosis fungoides to last follow-up was 2.9 years (range, 4 days to 14.7 years). The overall survival rates at 1, 2, and 5 years after diagnosis were 96%, 90%, and 62%, respectively (Table 2 and Figure 4). The cause-specific survival rate was not calculated because only 3 patients died of mycosis fungoides. The interval between onset of skin lesions and diagnosis did not affect risk of death (HR per 1-year increase in time to diagnosis, 1.02; P=.77). TREATMENT AND FOLLOW-UP Initial treatment data are given in Table 2. The mean number of individual treatments per patient was 4.2 (range, 1-10; median, 4.0). Fifteen patients (30% of all 50 patients) were hospitalized for management of their cutaneous disease at some point in the follow-up period. At the time of their last clinical assessment, 21 of 43 patients (49%) for whom treatment follow-up data were available had improved partially or completely. Five of 43 patients (12%) had complete or near-complete resolution of skin lesions at least once in the follow-up period; 1 patient had disease remission throughout the follow-up period. These 5 patients were treated using topical corticosteroids with L-lysine hydrochloride, psoralen UV-A photochemotherapy as monotherapy, or psoralen UV-A photochemotherapy with local radiotherapy, topical corticosteroids, or both. Of 43 patients, 7 (16%) had stable disease, and 15 (35%) had progressive disease. PROGNOSTIC ASSOCIATIONS Among 50 patients identified for the study, 15 (30%) had an adverse clinical outcome. The median time from onset of skin lesions to adverse clinical outcome was 3.4 years (range, years; mean, 5.1 years). Development of an adverse outcome was not associated with male sex (HR, 1.02; 95% CI, ; P=.97) or with older age at onset (HR per 10-year increase in age, 0.89; ; P=.58). Adverse clinical outcomes did not seem to be associated with histopathologic findings of follicular mucinosis (HR, 0.55; 95% CI, ; P=.28), neutrophilic inflammation (0.29; ; P=.10), eosinophilic inflammation (0.39; ; P=.08), or granulomatous inflammation (0.17; ; P=.09). No association was noted between adverse clinical out- 611
6 Overall Survival, % Time After MF Diagnosis, y Figure 4. Kaplan-Meier curve demonstrating overall survival of 47 patients with folliculotropic mycosis fungoides (MF) in years after diagnosis. The numbers of patients still at risk were 37, 29, and 14 for years 1, 2, and 5, respectively. comes and the presence of Sézary cells on peripheral smear (2.17; ; P=.22). SYSTEMATIC REVIEW We identified 8 previously published studies 1-8 that each reported the clinical features of FMF in 3 or more patients; FMF has been described in 236 patients overall, including our study. Authors of 2 of the histopathologic studies 3,8 also published clinical analyses 2,6 that were included in our systematic review; therefore, the same patient data may have been referenced twice in the systematic review analysis. Patient characteristics and diagnostic data are summarized in etable 1, clinical data in Table 1, histopathologic data in etable 2, and therapeutic and prognostic data in Table 2. COMMENT Also termed pilotropic or follicular mycosis fungoides, FMF is a mycosis fungoides variant characterized by hair follicle epithelium infiltration by neoplastic lymphoid cells. 9 It is more common in men than in women. 1-8 Compared with that in men, the mean age at disease onset in women was significantly older, coinciding with postmenopausal years. Estrogen could serve as a protective factor (or testosterone as a predisposing factor) in patients otherwise prone to FMF. Mycosis fungoides has numerous clinical manifestations, 1,2,4,10,11 and the folliculotropic variant is no exception. Although head and neck involvement is frequent in FMF, these areas generally are spared in classic mycosis fungoides. 1,2 The clinical index of suspicion for mycosis fungoides may be reduced, leading to a delay in diagnosis. 1,4 Several patients with FMF in our series had comorbid hematologic malignant neoplasms. Although composite cutaneous lymphomas have been documented in patients with mycosis fungoides and B-cell chronic lymphocytic leukemia, 12 we observed no neoplastic B cells in cutaneous biopsy specimens from our cohort. The implications of having circulating Sézary cells without erythroderma (observed among 9 patients in our study) are undetermined. 13 One group uses the term mycosis fungoides with leukemic involvement to describe mycosis fungoides with circulating Sézary cells in patients not otherwise meeting diagnostic criteria for Sézary syndrome. 13 In our study, 1 patient had FMF that progressed to Sézary syndrome. Just as the clinical features of FMF are varied, so are the histopathologic findings (etable 2). Distinguishing between the clinical entity of follicular mucinosis (alopecia mucinosa) and FMF can be challenging histologically. 6,14-17 Some authors have proposed that mycosis fungoides, follicular mucinosis, and FMF represent conditions along a continuous spectrum. 18 Accurate diagnosis is important because follicular mucinosis unassociated with mycosis fungoides, especially in young patients, tends to have a persistent but benign disease course, 15 in contrast to FMF. 1,2 In our opinion, development of intrafollicular mucin deposits is a nonspecific secondary phenomenon that may occur when neoplastic or nonneoplastic lymphoid cells infiltrate the follicular epithelium. Clinical variables and close observation over time may be required to establish the diagnosis with certainty. Presence of a prominent eosinophilic infiltrate identified in our patients and in others 1,3,6,8 was reasonably specific for associated pruritus. Although clonal T-cell populations were detected in the biopsy specimens of most patients in our study and in others, detection of a T-cell clone is not specific for cutaneous malignant neoplasms. However, in the appropriate clinical context, the presence of a clone with TCR gene rearrangement may serve as an independent predictor of disease progression. 20,21 Blood T-cell clones also are nonspecific and should not be interpreted to mean that the patient has systemic involvement. 9 Identical T-cell clones were detected in the blood and skin of 2 patients in our study, which implies systemic disease involvement and may be a marker of poor prognosis. 21 Data in our study were insufficient to evaluate this possibility. Although limited by their retrospective nature and the inability to standardize or directly compare treatments, other studies 1,2 and ours found that FMF is less responsive to treatment than classic mycosis fungoides. Some investigators 1,22 propose that the deep extension of lymphocytes into the hair follicles limits the response to superficial therapies such as UV-B phototherapy and topical corticosteroids. Other investigators 1 have hypothesized that the lymphocyte biologic characteristics that determine pilotropism also contribute to therapy resistance. We particularly aimed to calculate 5-year overall survival rates given apparent discrepancies among survival data of previous large retrospective studies. 1,2 The present study and the study by van Doorn et al 1 determined 5-year overall survival by measuring the time from diagnosis of mycosis fungoides to death, and these rates were similar (62% and 64%, respectively). Gerami et al 2 used the duration between the time of lesion onset to death. After accounting for a mean time to diagnosis of 4.5 years, the survival rate reported by Gerami et al is similar (67%). Cause-specific mortality rates and time to disease progression could not be calculated because of few cause-specific deaths and our inability to gather accurate data on the timing of disease progression. Our data may have overestimated the severity of FMF because of the tertiary referral nature of our practice and 612
7 the likely possibility that early cases of FMF may not have been recognized. Given the potentially subtle clinical and histopathologic findings in FMF, patients with early stages of the disease may have been unrecognized. The pathogenesis of FMF is not well understood. Heightened expression of intercellular adhesion molecule 1 in perifollicular keratinocytes in FMF, which may be induced by the neoplastic T lymphocytes, may lead to obstruction of the follicle orifice by neoplastic T cells. 4,5,23,24 Skin infection is known to exacerbate mycosis fungoides. 25 In the presence of Staphylococcus aureus superantigens, nonmalignant T lymphocytes stimulate the proliferation of malignant T lymphocytes by molecular cross-talk. 26 Indeed, several patients in our series with evidence of impetiginization had temporary improvement of their FMF after a course of systemic antibiotics. The finding that bacterial toxins worsen mycosis fungoides most likely has implications for FMF, as the follicular ostia are reservoirs of bacteria and pruritus (a stimulus for scratching) and subsequent impetiginization is a common clinical feature of FMF. Accepted for Publication: November 18, Correspondence: Roger H. Weenig, MD, Associated Skin Care Specialists, PA, 7205 University Ave NE, Fridley, MN (rogerweenig@gmail.com). Author Contributions: Dr Weenig had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Lehman, Cook-Norris, Weenig, Gibson, Weaver, and Pittelkow. Acquisition of data: Lehman, Cook-Norris, Weed, Weenig, and Pittelkow. Analysis and interpretation of data: Lehman, Weenig, Gibson, Weaver, and Pittelkow. Drafting of the manuscript: Lehman, Cook-Norris, Weed, Weenig, Weaver, and Pittelkow. Critical revision of the manuscript for important intellectual content: Lehman, Cook-Norris, Weenig, Gibson, Weaver, and Pittelkow. Statistical analysis: Weaver. Administrative, technical, or material support: Weenig, Gibson, and Pittelkow. Study supervision: Lehman, Weed, Weenig, Gibson, and Pittelkow. Financial Disclosure: None reported. Online-Only Material: etables 1 and 2 are available at REFERENCES 1. van Doorn R, Scheffer E, Willemze R. Follicular mycosis fungoides, a distinct disease entity with or without associated follicular mucinosis: a clinicopathologic and follow-up study of 51 patients. Arch Dermatol. ;138(2): Gerami P, Rosen S, Kuzel T, Boone SL, Guitart J. Folliculotropic mycosis fungoides: an aggressive variant of cutaneous T-cell lymphoma. Arch Dermatol. 2008; 144(6): Gerami P, Guitart J. The spectrum of histopathologic and immunohistochemical findings in folliculotropic mycosis fungoides. Am J Surg Pathol. 2007;31 (9): Vergier B, Beylot-Barry M, Beylot C, et al; French Study Group of Cutaneous Lymphomas. Pilotropic cutaneous T-cell lymphoma without mucinosis: a variant of mycosis fungoides? Arch Dermatol. 1996;132(6): Pereyo NG, Requena L, Galloway J, Sangüeza OP. Follicular mycosis fungoides: a clinicohistopathologic study. J Am Acad Dermatol. 1997;36(4): Cerroni L, Fink-Puches R, Back B, Kerl H. Follicular mucinosis: a critical reappraisal of clinicopathologic features and association with mycosis fungoides and Sézary syndrome. Arch Dermatol. ;138(2): Hodak E, Feinmesser M, Segal T, et al. Follicular cutaneous T-cell lymphoma: a clinicopathological study of nine cases. Br J Dermatol. 1999;141(2): Flaig MJ, Cerroni L, Schuhmann K, et al. Follicular mycosis fungoides: a histopathologic analysis of nine cases. J Cutan Pathol. 2001;28(10): Olsen E, Vonderheid E, Pimpinelli N, et al; ISCL/EORTC. Revisions to the staging and classification of mycosis fungoides and Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the cutaneous lymphoma task force of the European Organization of Research and Treatment of Cancer (EORTC). Blood. 2007;110(6): Nashan D, Faulhaber D, Ständer S, Luger TA, Stadler R. Mycosis fungoides: a dermatological masquerader. Br J Dermatol. 2007;156(1): Fraser-Andrews E, Ashton R, Russell-Jones R. Pilotropic mycosis fungoides presenting with multiple cysts, comedones and alopecia. Br J Dermatol. 1999; 140(1): Volk AL, Vannucci SA, Cook W, Thompson KA, Listinsky CM. Composite mycosis fungoides and B-cell chronic lymphocytic leukemia. Ann Diagn Pathol. ; 6(3): Vonderheid EC, Bernengo MG, Burg G, et al; ISCL. Update on erythrodermic cutaneous T-cell lymphoma: report of the International Society for Cutaneous Lymphomas. J Am Acad Dermatol. ;46(1): Pinkus H. The relationship of alopecia mucinosa to malignant lymphoma. Dermatologica. 1964;129: Gibson LE, Muller SA, Leiferman KM, Peters MS. Follicular mucinosis: clinical and histopathologic study. J Am Acad Dermatol. 1989;20(3): Mehregan DA, Gibson LE, Muller SA. Follicular mucinosis: histopathologic review of 33 cases. Mayo Clin Proc. 1991;66(4): Gibson LE, Brown HA, Pittelkow MR, Pujol RM. Follicular mucinosis. Arch Dermatol. ;138(12): Campanati A, Giangiacomi M, Goteri G, Penna L, Turtù S, Offidani AM. A case of follicular mycosis fungoides with follicular mucinosis: a rare association. Am J Dermatopathol. ;24(5): Siddiqui J, Hardman DL, Misra M, Wood GS. Clonal dermatitis: a potential precursor of CTCL with varied clinical manifestations [abstract]. J Invest Dermatol. 1997;108(4): Fraser-Andrews EA, Woolford AJ, Russell-Jones R, Seed PT, Whittaker SJ. Detection of a peripheral blood T cell clone is an independent prognostic marker in mycosis fungoides. J Invest Dermatol. 2000;114(1): Beylot-Barry M, Sibaud V, Thiebaut R, et al. Evidence that an identical T cell clone in skin and peripheral blood lymphocytes is an independent prognostic factor in primary cutaneous T cell lymphomas. J Invest Dermatol. 2001;117(4): Klemke CD, Dippel E, Assaf C, et al. Follicular mycosis fungoides. Br J Dermatol. 1999;141(1): Lacour JP, Castanet J, Perrin C, Ortonne JP. Follicular mycosis fungoides: a clinical and histologic variant of cutaneous T-cell lymphoma: report of two cases. J Am Acad Dermatol. 1993;29(2, pt 2): Vejlsgaard GL, Ralfkiaer E, Avnstorp C, Czajkowski M, Marlin SD, Rothlein R. Kinetics and characterization of intercellular adhesion molecule 1 (ICAM-1) expression on keratinocytes in various inflammatory skin lesions and malignant cutaneous lymphomas. J Am Acad Dermatol. 1989;20(5, pt 1): Axelrod PI, Lorber B, Vonderheid EC. Infections complicating mycosis fungoides and Sézary syndrome. JAMA. 1992;267(10): Woetmann A, Lovato P, Eriksen KW, et al. Nonmalignant T cells stimulate growth of T-cell lymphoma cells in the presence of bacterial toxins. Blood. 2007;109 (8):
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
The clinical recognition of a folliculotropic pattern in
 ORIGINAL ARTICLE The Spectrum of Histopathologic and Immunohistochemical Findings in Pedram Gerami, MD and Joan Guitart, MD Background: Since the original designation of folliculotropic mycosis fungoides
ORIGINAL ARTICLE The Spectrum of Histopathologic and Immunohistochemical Findings in Pedram Gerami, MD and Joan Guitart, MD Background: Since the original designation of folliculotropic mycosis fungoides
Cluster of differentiation (CD) markers in erythrodermic patients: A case series study
 Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Microscopic study of the normal skin in cases of mycosis fungoides
 Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
Microscopic study of the normal skin in cases of mycosis fungoides M. El Darouti, S. Marzook, M. Bosseila, O. Abu Zeid, O. El- Safouri, A. Zayed, A. El-Ramly Egyptian Dermatology Online Journal 2 (1):
ISPUB.COM. M Duvic, E Olsen PURPOSE OF REVISION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
Clinical and Histopathological Spectrum of Mycosis Fungoides
 Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
Awad Hasan Al-Tarawneh, MD, Jordan Board* Background: Early diagnosis of mycosis fungoides is essential but difficult and can be easily missed because it mimics many inflammatory skin diseases both clinically
Mycosis fungoides (MF) is the most common type of cutaneous
 Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
Mycosis fungoides variants clinicopathologic features, differential diagnosis, and treatment Rein Willemze, MD, PhD Abstract Mycosis fungoides (MF) is the most common type of cutaneous T-cell lymphoma,
Follicular lymphomatoid papulosis revisited: a study of 11 cases, with new histopathological findings
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Follicular lymphomatoid papulosis revisited: a study of 11 cases, with
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Follicular lymphomatoid papulosis revisited: a study of 11 cases, with
Two Clinically Unusual Cases of Folliculotropic Mycosis Fungoides: One with and the Other without Syringotropism
 Folliculotropic and Syringotropic Mycosis Fungoides Ann Dermatol Vol. 26, No. 3, 2014 http://dx.doi.org/10.5021/ad.2014.26.3.385 CASE REPORT Two Clinically Unusual Cases of Folliculotropic Mycosis Fungoides:
Folliculotropic and Syringotropic Mycosis Fungoides Ann Dermatol Vol. 26, No. 3, 2014 http://dx.doi.org/10.5021/ad.2014.26.3.385 CASE REPORT Two Clinically Unusual Cases of Folliculotropic Mycosis Fungoides:
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD
 Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Mycosis Fungoides, then and now Have we travelled?
 USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
Therapeutic Management of Early Cutaneous Mycosis Fungoides
 Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Disclosures. Advisory Board. Consultant. Investigator. MiRagen, Actelion, Celgene, Therakos. Mindera
 Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Mycosis Fungoides and Variants
 Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Mycosis Fungoides and Variants Jennifer Madison McNiff, M.D. Associate Professor, Dermatology and Pathology Yale University School of Medicine Classic mycosis fungoides The most common cutaneous lymphoma
Sezary Syndrome(SS) and other malignancies. Hernani Cualing MD Hematopathologist IHCFLOW Lab
 Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation. Dermatopathology Specialists Needed. Changing Trends
 Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Important Decisions in Dermatopathology: The Clinico- Pathologic Correlation Uma Sundram, MD, PhD Departments of Pathology and Dermatology Stanford University May 29, 2008 Dermatopathology Specialists
Review Article. Cutaneous lymphoproliferative disorders. NJ Trendell-Smith
 Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
OBSERVATION. Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy
 OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
OBSERVATION Psoralen Plus Long-Wave UV-A (PUVA) and Bexarotene Therapy An Effective and Synergistic Combined Adjunct to Therapy for Patients With Advanced Cutaneous T-Cell Lymphoma Karen S. McGinnis, MD;
ISPUB.COM. Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis. E Kim PHYSICAL FINDINGS INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
Int J Clin Exp Pathol 2013;6(4): /ISSN: /IJCEP Tadashi Terada
 Int J Clin Exp Pathol 2013;6(4):749-756 www.ijcep.com /ISSN:1936-2625/IJCEP1301060 Case Report Mycosis fungoides in plaque stage with pronounced eosinophilic infiltration, folliculotropism, and concomitant
Int J Clin Exp Pathol 2013;6(4):749-756 www.ijcep.com /ISSN:1936-2625/IJCEP1301060 Case Report Mycosis fungoides in plaque stage with pronounced eosinophilic infiltration, folliculotropism, and concomitant
Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides
 Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas
 Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Hematopathology / BONE MARROW STAGING IN CUTANEOUS T-CELL LYMPHOMA Bone Marrow Histopathologic and Molecular Staging in Epidermotropic T-Cell Lymphomas Vincent Sibaud, MD, 1,2 Marie Beylot-Barry, MD, PhD,
Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas
 Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Sézary syndrome presenting with leonine facies ajd_560
 285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
Grover s disease: A case report.
 320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
Primary cutaneous large cell lymphoma CD30+: a case-based review
 Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs
 Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Plasma cell myeloma (multiple myeloma)
 Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Plasma cell myeloma (multiple myeloma) Common lymphoid neoplasm, present at old age (70 years average) Remember: plasma cells are terminally differentiated B-lymphocytes that produces antibodies. B-cells
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma
 Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Granulomatous Slack Skin with an unusually aggressive course due to the subsequent development of a CD30-positive Large Cell Lymphoma Alexandra Papoudou-Bai 1, Eleni Kapsali 2, Ioannis Kostas-Agnantis
Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated with Interferon-Alfa 2a
 Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Burkitt lymphoma. Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8
 Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Heme 8 Burkitt lymphoma Sporadic Endemic in Africa associated with EBV Translocations involving MYC gene on chromosome 8 Most common is t(8;14) Believed to be the fastest growing tumor in humans!!!! Morphology
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides
 Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
ISPUB.COM. Alopecia Areata preceding Mycosis Fungoides. R Creed, J Vu, R Singh, D Jones, M Duvic CASE 1
 ISPUB.COM The Internet Journal of Dermatology Volume 5 Number 2 Alopecia Areata preceding Mycosis Fungoides R Creed, J Vu, R Singh, D Jones, M Duvic Citation R Creed, J Vu, R Singh, D Jones, M Duvic. Alopecia
ISPUB.COM The Internet Journal of Dermatology Volume 5 Number 2 Alopecia Areata preceding Mycosis Fungoides R Creed, J Vu, R Singh, D Jones, M Duvic Citation R Creed, J Vu, R Singh, D Jones, M Duvic. Alopecia
clinical recommendations
 19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin
 Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
STUDY. a group of 6 patients with. with localized alopecia characterized histopathologically
 Follicular Mucinosis STUDY A Critical Reappraisal of Clinicopathologic Features and Association With Mycosis Fungoides and Sézary Syndrome Lorenzo Cerroni, MD; Regina Fink-Puches, MD; Barbara Bäck; Helmut
Follicular Mucinosis STUDY A Critical Reappraisal of Clinicopathologic Features and Association With Mycosis Fungoides and Sézary Syndrome Lorenzo Cerroni, MD; Regina Fink-Puches, MD; Barbara Bäck; Helmut
21/07/2017. Hobnail endothelial cells are not the same as epithelioid endothelial cells
 UPDATE IN CUTANEOUS VASCULAR S DERMATOPATHOLOGY SESSION BELFAST PATHOLOGY JUNE 21/2017 Dr E Calonje St John s Institute of Dermatology, London, United Kingdom THE FAMILY OF VASCULAR S WITH EPITHELIOID
UPDATE IN CUTANEOUS VASCULAR S DERMATOPATHOLOGY SESSION BELFAST PATHOLOGY JUNE 21/2017 Dr E Calonje St John s Institute of Dermatology, London, United Kingdom THE FAMILY OF VASCULAR S WITH EPITHELIOID
Interhospital Dermatology Conference 2013
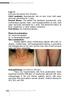 Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Case 21 A 50-year-old woman from Chonburi. Chief complaint: Asymptomatic rash on neck, trunk, both upper and lower extremities for 2 years. Present illness: The patient has developed asymptomatic scaly
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center
 Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary Study
 Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Update in deposition diseases
 Genoa, Italy Update in deposition diseases Prof. Franco Rongioletti, Section of Dermatology, Chair of Dermatopathology, University of Genoa,Italy Cutaneous deposition disorders Endogenous Exogenous Cutaneous
Genoa, Italy Update in deposition diseases Prof. Franco Rongioletti, Section of Dermatology, Chair of Dermatopathology, University of Genoa,Italy Cutaneous deposition disorders Endogenous Exogenous Cutaneous
Disclosure of Relevant Financial Relationships
 Squamous entities of the thyroid: Reactive to Neoplastic Michelle D. Williams Associate Professor Dept of Pathology, Head & Neck Section University of Texas MD Anderson Cancer Center Disclosure of Relevant
Squamous entities of the thyroid: Reactive to Neoplastic Michelle D. Williams Associate Professor Dept of Pathology, Head & Neck Section University of Texas MD Anderson Cancer Center Disclosure of Relevant
Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants
 Research Article Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants Aarón Kaminsky Award 2007 Alejandra Abeldaño 1, Mariana Arias 2, Karina Ochoa 3, Adriana
Research Article Mycosis fungoides beyond the classical Alibert- Bazin disease: report of seventeen atypical variants Aarón Kaminsky Award 2007 Alejandra Abeldaño 1, Mariana Arias 2, Karina Ochoa 3, Adriana
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis
 Case Reports in Pediatrics Volume 2016, Article ID 8564389, 4 pages http://dx.doi.org/10.1155/2016/8564389 Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis Cláudia Patraquim, 1 Maria
Case Reports in Pediatrics Volume 2016, Article ID 8564389, 4 pages http://dx.doi.org/10.1155/2016/8564389 Case Report Childhood Hypopigmented Mycosis Fungoides: A Rare Diagnosis Cláudia Patraquim, 1 Maria
Cutaneous Mycosis Fungoides (MF), the subtype of cutaneous
 DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
DOI 10. 5001/omj.2012.28 The Histological Spectrum of Early Mycosis Fungoides: A Study of 58 Saudi Arab patients Maha Arafah, Shaesta Naseem Zaidi, Hala Kassouf Kfoury, Ammar Al Rikabi, Khalid Al Ghamdi
The World of Dermatology
 The World of Dermatology, F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates, LTD Objectives Cite the advances in management
The World of Dermatology, F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates, LTD Objectives Cite the advances in management
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia
 CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
Narrow band UVB (311 nm), psoralen UVB (311 nm) and PUVA therapy in the treatment of early-stage mycosis fungoides: a right left comparative study
 Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
Photodermatol Photoimmunol Photomed 2005; 21: 281 286 Blackwell Munksgaard Copyright r Blackwell Munksgaard 2005 Narrow band UVB (311 nm), psoralen UVB (311 nm) and therapy in the treatment of early-stage
88-year-old Female with Lymphadenopathy. Faizi Ali, MD
 88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
88-year-old Female with Lymphadenopathy Faizi Ali, MD Clinical History A 88-year-old caucasian female presented to our hospital with the complaints of nausea, vomiting,diarrhea, shortness of breath and
Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases
 Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Case Report Rare Presentation of Primary Extramedullary Plasmacytoma as Lip Lesion
 Hindawi Case Reports in Oncological Medicine Volume 2017, Article ID 4296802, 5 pages https://doi.org/10.1155/2017/4296802 Case Report Rare Presentation of Primary Extramedullary Plasmacytoma as Lip Lesion
Hindawi Case Reports in Oncological Medicine Volume 2017, Article ID 4296802, 5 pages https://doi.org/10.1155/2017/4296802 Case Report Rare Presentation of Primary Extramedullary Plasmacytoma as Lip Lesion
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Among the benign intraepithelial melanocytic proliferations, Inflamed Conjunctival Nevi. Histopathological Criteria. Resident Short Reviews
 Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Resident Short Reviews Inflamed conjunctival nevi (ICN) may suggest malignancy because of their rapid growth and atypical histology. The objective of this study was to characterize the diagnostic features
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Granulomatous mycosis fungoides (GMF) is
 CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
CASE REPORT Granulomatous mycosis fungoides, a rare subtype of cutaneous T-cell lymphoma Marta Kogut, MD, a Eva Hadaschik, MD, a Stephan Grabbe, MD, b Mindaugas Andrulis, MD, c Alexander Enk, MD, a and
Sézary syndrome. Diagnosis and staging
 CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
STUDY. with a benign clinical course but a malignant appearance
 Lymphomatoid Papulosis STUDY Reappraisal of Clinicopathologic Presentation and Classification Into Subtypes A,, and C Laila El Shabrawi-Caelen, MD; Helmut Kerl, MD; Lorenzo Cerroni, MD Objectives: To analyze
Lymphomatoid Papulosis STUDY Reappraisal of Clinicopathologic Presentation and Classification Into Subtypes A,, and C Laila El Shabrawi-Caelen, MD; Helmut Kerl, MD; Lorenzo Cerroni, MD Objectives: To analyze
CUTANEOUS T-CELL LYMPHOMA PROFORMA
 STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
CUTIS. Do Not Copy. Pityriasis lichenoides is a T cell mediated papular. Pityriasis Lichenoides Chronica in Black Patients. Pediatric Dermatology
 Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
Series Editor: Camila K. Janniger, MD Pityriasis Lichenoides Chronica in Black Patients Tanda N. Lane, MD; Sareeta S. Parker, MD Pityriasis lichenoides chronica (PLC) is a cutaneous disease of unknown
A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature
 Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
SH/EAHP Workshop 2011 Los Angeles, California, USA
 SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective Study
 International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11
 Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Dermatologica Sinica
 DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
DERMATOLOGICA SINICA 31 (2013) 3e Contents lists available at SciVerse ScienceDirect Dermatologica Sinica journal homepage: http://www.derm-sinica.com CASE REPORT Early stage mycosis fungoides with focal
Cutaneous T-cell Lymphoma: An Entry From Thomson Gale's Gale Encyclopedia Of Cancer, 2nd Ed. [HTML] [Digital]
![Cutaneous T-cell Lymphoma: An Entry From Thomson Gale's Gale Encyclopedia Of Cancer, 2nd Ed. [HTML] [Digital] Cutaneous T-cell Lymphoma: An Entry From Thomson Gale's Gale Encyclopedia Of Cancer, 2nd Ed. [HTML] [Digital]](/thumbs/80/80529096.jpg) Cutaneous T-cell Lymphoma: An Entry From Thomson Gale's Gale Encyclopedia Of Cancer, 2nd Ed. [HTML] [Digital] By Michelle, M.S., J.D. Johnson;Rebecca, PhD Frey READ ONLINE If searched for a ebook Cutaneous
Cutaneous T-cell Lymphoma: An Entry From Thomson Gale's Gale Encyclopedia Of Cancer, 2nd Ed. [HTML] [Digital] By Michelle, M.S., J.D. Johnson;Rebecca, PhD Frey READ ONLINE If searched for a ebook Cutaneous
Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified
 NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia. Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE
 Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Title: Erythema annulare centrifugum associated with chronic lymphocytic leukaemia Authors: Helbling I, Walewska R, Dyer MJS, Bamford M, Harman KE Sir, A wide range of conditions have been described as
Supplementary Online Content
 Supplementary Online Content Ross NA, Chung H-J, Li Q, Andrews JP, Keller MS, Uitto J. Pityriasis rubra pilaris: a case series of patients. Published online March 9, 26. JAMA Dermatol. doi:./jamadermatol.26.9.
Supplementary Online Content Ross NA, Chung H-J, Li Q, Andrews JP, Keller MS, Uitto J. Pityriasis rubra pilaris: a case series of patients. Published online March 9, 26. JAMA Dermatol. doi:./jamadermatol.26.9.
Abstract. Hematopathology / SÉZARY CELL DETECTION AND QUANTIFICATION
 Hematopathology / SÉZARY CELL DETECTION AND QUANTIFICATION A Comparison of Morphologic Features, Flow Cytometry, Analysis, and TCR-PCR in Qualitative and Quantitative Assessment of Peripheral Blood Involvement
Hematopathology / SÉZARY CELL DETECTION AND QUANTIFICATION A Comparison of Morphologic Features, Flow Cytometry, Analysis, and TCR-PCR in Qualitative and Quantitative Assessment of Peripheral Blood Involvement
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Introduction. Results. Discussion. Histopathologic and immunohistochemical findings. Results. conclusions,
 1/5 2/5 Carcinoma distinctive carcinoma. form erysipeloides (CE), metastasis. which clinically Itfrom has resembles been termed erysipelas, is an uncommon, but may extend It164 toclassically back, presents
1/5 2/5 Carcinoma distinctive carcinoma. form erysipeloides (CE), metastasis. which clinically Itfrom has resembles been termed erysipelas, is an uncommon, but may extend It164 toclassically back, presents
Correlation of pretreatment surgical staging and PET SUV(max) with outcomes in NSCLC. Giancarlo Moscol, MD PGY-5 Hematology-Oncology UTSW
 Correlation of pretreatment surgical staging and PET SUV(max) with outcomes in NSCLC Giancarlo Moscol, MD PGY-5 Hematology-Oncology UTSW BACKGROUND AJCC staging 1 gives valuable prognostic information,
Correlation of pretreatment surgical staging and PET SUV(max) with outcomes in NSCLC Giancarlo Moscol, MD PGY-5 Hematology-Oncology UTSW BACKGROUND AJCC staging 1 gives valuable prognostic information,
Challenging Cases in Dermatopathology. Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania
 Challenging Cases in Dermatopathology Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rosalie Elenitsas
Challenging Cases in Dermatopathology Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Rosalie Elenitsas
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Plenary paper. Introduction
 Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Lymphocytoma Cutis. Cynthia M. Magro MD. Director of Dermatopathology Weill Medical College of Cornell University New York, New York
 Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Follicular Lymphoma: the WHO
 Follicular Lymphoma: the WHO and the WHERE? Yuri Fedoriw, MD Associate Professor of Pathology and Laboratory Medicine Director of Hematopathology University of North Carolina Chapel Hill, NC Disclosure
Follicular Lymphoma: the WHO and the WHERE? Yuri Fedoriw, MD Associate Professor of Pathology and Laboratory Medicine Director of Hematopathology University of North Carolina Chapel Hill, NC Disclosure
Clinicopathologic Self- Assessment S003 AAD 2017
 Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
Clinicopathologic Self- Assessment S003 AAD 2017 Clay J. Cockerell, M.D. Director, Cockerell Dermatopathology Director, Division of Dermatopathology UT Southwestern Medical Center July 2017 No relevant
Mycosis Fungoides Presentation in Emergency
 The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM. Tom Helm, MD
 2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM Tom Helm, MD Case 1 Diagnosis: Pseudoepitheliomatous hyperplasia associated with CD30+ lymphoproliferative disease
2016 AAD SUMMER MEETING SYMPOSIUM S011: CLINICOPATHOLOGIC SELF-ASSESSMENT 7/30/16 2:00 PM Tom Helm, MD Case 1 Diagnosis: Pseudoepitheliomatous hyperplasia associated with CD30+ lymphoproliferative disease
ISPUB.COM. Bexarotene in Tumor stage Mycosis Fungoides. R Talpur, M Duvic INITIAL PRESENTATION TREATMENT COURSE INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Bexarotene in Tumor stage Mycosis Fungoides R Talpur, M Duvic Citation R Talpur, M Duvic. Bexarotene in Tumor stage Mycosis Fungoides. The
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Bexarotene in Tumor stage Mycosis Fungoides R Talpur, M Duvic Citation R Talpur, M Duvic. Bexarotene in Tumor stage Mycosis Fungoides. The
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Fig. 3.1 Fig Past history: She was previously healthy and not taking any medication.
 Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
1/19/2018. Early CTCL: treatment considerations
 Treatment of early stage CTCL Joan Guitart, MD Chicago, IL USA Disclosures: Actelion (grants, consultant), Tetralogic/Medivir (grant, consultant), Solygenix (grant) Therakos (grant) Early CTCL: treatment
Treatment of early stage CTCL Joan Guitart, MD Chicago, IL USA Disclosures: Actelion (grants, consultant), Tetralogic/Medivir (grant, consultant), Solygenix (grant) Therakos (grant) Early CTCL: treatment
CME/SAM. Olga Pozdnyakova, MD, PhD, 1 Svetlana Kondtratiev, MD, 1,2 Betty Li, MS, 1 Karry Charest, 1 and David M. Dorfman, MD, PhD 1.
 Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
Hematopathology / New Mastocytosis Flow Cytometry Approach High-Sensitivity Flow Cytometric Analysis for the Evaluation of Systemic Mastocytosis Including the Identification of a New Flow Cytometric Criterion
