Health care workers (HCWs) are at. Occupational Exposure to Blood and Body Fluids. Review. M Bahadori, 1 G Sadigh 2. Abstract. Keywords.
|
|
|
- Charleen Spencer
- 6 years ago
- Views:
Transcription
1 Review Occupational Exposure to Blood and Body Fluids M Bahadori, 1 G Sadigh 2 Abstract Occupational exposure to blood and body fluids is an important hazard for health care workers, which places them at a high risk for blood-borne infections including hepatitis B virus, hepatitis C virus and human immunodeficiency virus and results in psychological and emotional stresses. Several preventive measures have been proposed including pre-exposure (e.g., education, use of standard precautions, use of needle protective devices, and vaccination) and post-exposure (e.g., post-exposure prophylaxis and early detection of disease) prevention. In this article, the importance of occupational exposure to blood and body fluids and the basic concepts of exposure prevention and management are reviewed. 1 Department of infectious disease, National Iranian Oil Company (NIOC) Hospital, Tehran, Iran 2 Tehran University of Medical Sciences, Tehran, Iran Keywords Occupational disease; Health personnel; Occupational health; Blood-borne pathogens; Prevention; Safety Introduction Health care workers (HCWs) are at risk of exposure to more than 60 different pathogens or species including 26 viruses, 18 bacteria/rickettsia, 13 parasites, and three yeasts 1,2 resulting from contact with blood and body fluids (BBF) from patients. Human immunodeficiency virus (HIV), hepatitis B virus (HBV), and hepatitis C virus (HCV) are the three most important causes of occupational-related infections. 1 An exposure that might place HCWs at risk for these infections can be in the form of either a percutaneous injury (e.g., a needle stick or cut with a sharp object), or contact of mucous membrane or non-intact skin (e.g., exposed skin that is chapped, abraded, or afflicted with dermatitis) with blood, tissue, or other body fluids that are potentially infectious. 3-5 Despite published guidelines and training programs to prevent infection transmission, 6 exposure to BBF remains a major concern in hospitals even in developed countries such as the United States. 7 HCWs include emergency medical service, dental, laboratory, and autopsy personnel, nurses, nursing assistants, physicians, technicians, therapists, pharmacists, students and trainees, contractual staff not employed by the health care facility, and persons not directly involved in patient care but potentially exposed to BBF (e.g., clerical, dietary, housekeeping, maintenance, and volunteer personnel). 3,6 Epidemiology Incidence It has been estimated that more than Correspondence to Gelareh Sadigh, MD, No 2, 5 th West Alley, Ajoudanieh St, Tehran 19567, Iran. Tel: , Fax: gelarehsadigh@yahoo.com Vol 1 Number 1 January,
2 Occupational Exposure to Body Fluids three million HCWs experience percutaneous injuries with contaminated sharp objects each year. 8 Of these exposures, approximately occur in the US. 9 The overall sharps injury rate per HCWs per year ranges from 113 (1%) to 623 (6.2%), with a mean of 405 (4%); 10 however, the Exposure Prevention Information Network (EPINet ) surveillance program reported the rate of percutaneous injury, defined as the number of injuries per 100 occupied beds per year, to be 26.8 in teaching hospitals and 18.7 in nonteaching hospitals. 4 Regarding the Canada Communicable Disease Report (CCDR) on 2621 registered occupational exposures to BBF, needle stick injuries account for the highest BBF exposures among HCWs (65.7%), followed by splashes from patients (13.7%), cuts with sharp objects (8.6%), sticks other than needle stick (7.2%), scratches (1.9%), touching patients directly (1.8%), and bites (1.2%). 11 In the CCDR, hypodermic needles, suture needles, winged needles, venous catheter needles, and blood collection needles caused two-thirds of the percutaneous exposures. 11,12 Of the mucocutaneous exposures, 70.5% occurred on mucous membranes and 22.3% on non-intact skin. 12 While splashes often involved multiple parts of the body, fingers were the most commonly reported anatomical location (77%) for needle stick injuries. 13 The predominant body parts affected by splashes were eyes alone and face or mouth. Bodily fluids (e.g., urine, sweat, blister, and saliva) were the predominant type of splash, followed by blood spatter. 6 Across all health care settings, the needle stick injuries and splashes occurred predominantly at the patient s bedside, 14 while sharp injuries occurred most frequently in the operating rooms. 6 Nurses, medical doctors, and laboratory technicians were the three professional groups that most frequently reported exposures. 7,11 The higher number of reports from nurses partly reflects the relative number of nurses to doctors in health care setting. 15 It also shows the reticence of doctors to report injuries due to potential subsequent restrictions on their practice. 7,15 Moreover, most of the doctors believe that they can handle the issue themselves. 7 Lack of experience in many procedures, insufficient training, work overload and fatigue were the probable causes that led to occupational sharp injuries. 10,14 A recent analysis of needle stick injuries in navy medical personnel from the Naval Safety Center Injury Tracking System (IN- JTRAK) illustrated that most BBF injuries occur among men and HCWs younger than 30 years of age, 13 while other studies reported that female HCWs had more injury rate than their male counterparts. 6,7 Under-reporting For a variety of reasons, it is important that workers report exposures to BBF. HCWs who do not report their exposures run the risk of seroconversion and morbidity and put others, especially their sexual partners, at risk of infection, if timely postexposure medical evaluation and treatment are not sought. Furthermore, if an exposure is not formally documented and reported, an infected worker may not be eligible for workers compensation if a claim is filed. In addition, underestimation of exposure incidence and poor information on risk factors by the employer may decrease his incentive to implement safer equipment or work practices or to seek product engineering upgrades from device manufacturers. 9 The under reporting rate has been es- 2 Vol 1 Number 1; January, 2010
3 M. Bahadori, G. Sadigh timated between 26% and 85% in previous studies. 15 Reasons for not reporting exposures have included the belief that the risk of infection was low, being too busy, not knowing the reporting procedure, and not wanting to appear careless. 9 A clear inverse association between the frequency of recent injury and reporting likelihood was documented in a recent study. 7 In a study by Lymer, et al, of 1181 incidents of injury, only 9% had been officially reported. 16,17 There was a significant difference between various professional groups with regard to the frequency of incident reporting. Physicians reported only 3% of the incidents whereas medical laboratory technicians reported almost 36% of them. 16 This finding was confirmed in other studies. 7 In a study by Askarian, et al, on medical, dental, nursing and midwifery students in Shiraz University of Medical Sciences, Iran, 82% (401 of 489) of all needle stick injuries went unreported; most of which attributed to the uncertainty of the injured student about the reporting process. 14 Similarly, another Iranian study reported that 80% of the surgeons had never or rarely reported their needle stick injuries. 18 Economic impact A recent economic analysis of the costs associated with the management of occupational exposure to BBF including post-exposure prophylaxis (PEP) showed that the overall cost ranged from US$ Moreover, HCWs experience such a significant fear, anxiety and emotional distress following a needle stick injury that sometimes results in occupational and behavioral changes. 20 According to O Malley, et al, the mean total costs varied greatly by the infection status of the source patient. The overall mean cost for exposures to HIV-infected source patients (including those co-infected with HBV or HCV) was US$ 2456 (range: US$ ), for exposures to source patients with unknown or negative infection status, was US$ 376 (range: US$ ), and for source patients infected with HCV was US$ 650 (range: US$ ). 19 The risk of transmission of blood-borne pathogens Hepatitis B The risk of HBV infection is primarily related to the level of contact with blood and also to the hepatitis B e antigen (HBe Ag) status of the source person. According to the Center for Disease Control and Prevention (CDC) report, the risk of developing clinical hepatitis after percutaneous exposure to a blood sample positive for both hepatitis B surface antigen (HBs Ag) and HBe Ag is 22% to 31%, whereas the risk of developing serologic evidence of HBV infection is 37% to 62%. However, the risk of developing clinical hepatitis from a needle contaminated with HBs Ag-positive, HBe Ag-negative blood is 1% to 6%, and the risk of developing serologic evidence of HBV infection is 23% to 37%. 5 Blood contains the highest HBV titers of all body fluids. Therefore, blood is the most important vehicle for transmission of HBV in the health care setting; other body fluids, including breast milk, bile, cerebrospinal fluid, feces, nasopharyngeal washings, saliva, semen, sweat and synovial fluid are not efficient vehicles for transmission because they contain low amounts of infectious HBV, despite the presence of HBs Ag. 5 Hepatitis C HCV is not easily transmitted through Vol 1 Number 1; January,
4 Occupational Exposure to Body Fluids TAKE-HOME MESSAGE The needlestick injuries and splashes occurred predominantly at the patient s bedside, while sharp injuries occurred most frequently in the operating rooms. Lack of experience in many procedures, insufficient training, work overload and fatigue were the main causes that led to occupational sharp injuries. exposure to blood. The mean incidence of anti-hcv seroconversion after accidental percutaneous exposure from an HCV-positive patient is 1.8% (range: 0% in those with negative HCV-PCR to 10% in those with positive PCR). 1,5 One study showed that the transmission occurred only by hollow-bore needles rather than other sharps. Transmission rarely occurs from mucous membrane exposures to blood no transmission in HCWs has been reported from intact or non-intact skin exposures to blood. The risk for transmission from exposure to fluids or tissues other than HCVinfected blood though has not been measured yet, is expected to be low. 5 HIV The average risk for HIV transmission after a percutaneous exposure to a blood sample positive for HIV is approximately 0.3%. It is almost 0.09% after a mucous membrane exposure. Although episodes of HIV transmission after non-intact skin exposure have been reported, the average risk for transmission by this route has not been quantified yet. However, the risk is estimated to be less than that for mucous membrane exposures. Besides, the risk for transmission after exposure to fluids or tissues other than HIV-infected blood is considerably lower than for blood exposures. 3 Numerous studies suggest that multiple factors might influence the risk for HIV transmission after an occupational exposure. These factors include the volume of blood inoculated (e.g., deep needle stick, injury caused by a visibly bloody device, and injury caused by a needle that had been directly in the source patient s blood vessel) or the number of infective agents (high viral load such as in newly-infected patients or those in a terminal stage illness). 1,3,4,21 Documented occupationallyacquired infections The overall number of HCWs annually exposed to sharp injuries contaminated with HCV, HBV, and HIV was estimated to reach , 2.1 million, and , respectively. 8 Nonetheless, there are minimal data collected on occupational transmission of these infections. In 1987, the CDC estimated that each year, app roximately HCWs were becoming occupationally infected with HBV in the US. Among these people 700 to 1200 would become chronic carriers, and 200 to 300 deaths would occur as a result of infection. 1 However, in 1995, there were 800 occupationally HBV-infected HCWs in the US, showing a sharp decline of 95% since implementation of the vaccination program in At the same time, there were no reported cases of hepatitis B in the UK. 15 There is no comprehensive registry for documented cases of HCWs occupationally infected with hepatitis C. Between July 1997 and December 1999, 360 cases of occupational exposure to hepatitis C were reported in England and Wales, with only one known seroconversion. Over the same 4 Vol 1 Number 1; January, 2010
5 M. Bahadori, G. Sadigh period in Scotland, 41 exposures to hepatitis C with no known seroconversions were reported. 15 In 2001, 43 occupational seroconversions for HCV were documented in France. 1 Occ upational transmission of HIV is divided into definite cases (i.e., confirmed occupational transmission) and possible cases (i.e., no identified risk of infection other than occupational exposure). 15 A total of 106 definite and 238 possible cases of occupationally-acquired HIV had been reported worldwide by the end of December ,2 The November 2002 World Health Report revealed that 2.5% of hepatitis B and 40% of hepatic C cases among HCWs worldwide were the result of occupational exposure. 8,22 Similarly, 4.4% of HIV cases among HCWs are thought to be attributed to occupational exposures. 7 Finally, the annual number of infections attributable to sharp injuries among HCWs worldwide in year 2000 was almost (range: ) for HCV, (range: ) for HBV, and 1000 (range: ) for HIV. These infections are thought to result in 145 (range: ) premature deaths from HCV, 261 (range: ) deaths from HBV and 736 (range: ) deaths from HIV in HCWs between the years 2000 and 2030; 8 half of these deaths would occur in Sub-Saharan Africa. Prevention Primary prevention of occupational exposures is an important issue, and preventive efforts should not be only focused on post-exposure prevention. Although PEP may substantially reduce the risk of transmission following an occupational exposure to an infected patient, it does not eliminate the risk of transmission. Furthermore, it cannot completely relieve the anxiety that many HCWs experience following an exposure. 4 It is suggested that prevention of sharp injuries be aimed at nurses and doctors. 15 Health care organizations should provide an appropriate system to their personnel and make available suitable written protocols for prompt reporting, evaluation, counseling, treatment, and follow-up of those occupational exposures that might place them at risk for acquiring a bloodborne infection. 5 Effective prevention of needle stick injury include administrative and work practice controls such as educating workers about hazards, implementing standard precautions (e.g., hand hygiene and the use of personnel protective equipment such as gloves, gowns, and face mask), eliminating needle recapping, providing sharps containers for easy access that are within sight and arm s reach 4,6,8,21 and the introduction of needle protective devices. 15 In a study involving three hospitals in Virginia, US, Jagger reported a 59% reduction in intravenous (IV) access needle injuries after establishment of an educational program and implementation of standard precautions. There was also an 84% reduction in injuries after implementation of a safety IV catheter. 21 Surprisingly, the CDC identified that over a four-year period within a group of hospitals, 5% of all sharp injuries were sustained while using a needle protective device. This finding underlines the fact that these devices do not provide complete protection. 15 Poor compliance with standard precautions has been found to be associated with factors such as inaccessibility or discomfort of the protective equipment, how urgent the patients needs are, influence of co-workers, and sub-optimal working Vol 1 Number 1; January,
6 Occupational Exposure to Body Fluids conditions. 17 In a study conducted in 2007, Moghimi, et al, reported that only 74 (12.9%) of 574 surgeons in Iran always used double gloves, 18 demonstrating poor compliance with the standard precautions among Iranian surgeons and the need for education. Any person who performs tasks involving contact with blood, blood-contaminated body fluids, other body fluids, or sharps should be vaccinated against hepatitis B free of charge. 5,6,8 Pre-vaccination serologic screening for previous infection is not indicated for persons being vaccinated because of occupational risk, unless the hospital or health care organization considers screening cost-effective. 5 The ongoing vaccination program against HBV has led to considerable reduction in the use of hightiter immunoglobulin against HBV which is an expensive treatment and decreased the anxiety of HCWs after needle stick and sharp injuries. 7 HCWs who have contact with patients or blood, and are at ongoing risk for percutaneous injuries should be tested 1 2 months after completion of the three dose vaccination series for anti-hbs. 5 Once the appropriate antibody level achieved, booster doses of hepatitis B vaccine are not necessary, and periodic serologic testing to monitor antibody levels after completion of the vaccine series is not recommended. 5 According to Prüss-Ustün, et al, regional estimates for the coverage of hepatitis B immunization among HCWs worldwide ranges between 18% and 77%. 8 According to a study conducted by Moghimi, et al, although 93.3% of surgeons in Iran are vaccinated against HBV, only 56.8% had checked their anti-hbs level. 18 This study shows an acceptable coverage rate of hepatitis B immunization among HCWs in Iran. We suggest that HCWs should be tested free of charge for anti-hbs 1 2 months after completion of vaccination, so that the antibody response to vaccine is being assessed. This will decrease the anxiety and psychological stress after exposure to BBF, when the HCW knows his/her antibody response. Additionally, it will be more costeffective when the PEP is administrated and unnecessary administration of immunoglobulin against HBV is prevented. Unlike hepatitis B there is no immunization available for HIV or HCV. 21 Post-exposure management The first step in post-exposure management is to wash wounds and skin sites that have been in contact with BBF with soap and water; mucous membranes should be flushed with water. No evidence exists in favor of using antiseptics for wound care or expressing fluid by squeezing the wound in order to reduce the risk of blood-borne pathogen transmission; while the use of antiseptics is not contraindicated, they are not injected into the wounds. 5 The person whose BBF is the source of an occupational exposure should be evaluated for HBV, HCV, and HIV infection. If the exposure source is unknown or cannot be tested, information about where and under what conditions the exposure has occurred should be assessed epidemiologically for the likelihood of transmission of HBV, HCV, or HIV. Testing of needles or other sharp instruments implicated in an exposure, regardless of whether the source is known or unknown, is not recommended. 5 We recommend an anti-hcv and anti-hiv testing after exposure to a source patient who has been considered likely to have HCV/HIV infection. In this way, a previously-infected HCW can be differentiated from one who acquires infection after an occupational exposure to BBF. 6 Vol 1 Number 1; January, 2010
7 M. Bahadori, G. Sadigh Post-exposure prophylaxis Effectiveness of PEP varies from 75% to >90% to prevent HBV infection; 14 however, PEP for HIV is generally considered to reduce the risk of transmission by approximately 80%; 4 there is no known way for preventing HCV acquisition following BBF exposure. 14 HBV PEP for unvaccinated HCWs following an exposure includes initiating vaccine series. When the source patient is HBs Ag-positive, one dose of hepatitis B immunoglobulin should be additionally administered. A previously-vaccinated HCW who is a known responder (serum anti-hbs 10 miu/ml 1 2 months after completion of three doses of vaccination) does not need any PEP. A previously-vaccinated HCW who is a known non-responder or has an unknown antibody response does not need any PEP after exposure to HBs Ag-negative patients; however, after exposure to HBs Ag-positive or unknown source patient, the non-responders should receive either one dose of hepatitis B immunoglobulin plus revaccination or two doses of hepatitis B immunoglobulin (if they have previously completed a second three-dose series of vaccination). HCWs with unknown antibody response should be tested for serum antibody titer. If the titer is inadequate, they should receive a booster dose and in case of HBs Ag-positive source patient, they should also receive one dose of hepatitis B immunoglobulin. 5 As it will be timeconsuming to wait for the serum antibody titer results, the authors suggest beginning with a booster dose and one dose of hepatitis B immunoglobulin to reduce the stress of the exposed HCW which may influence his/her private and occupational life and decrease his/her efficacy at work. It can then be waited for the test results to choose the appropriate PEP according to the CDC guidelines. When hepatitis B immunoglobulin or vaccine is indicated, it should be administered as soon as possible after the exposure (preferably within 24 hours). The effectiveness of hepatitis B immunoglobulin when administered more than seven days after exposure is unknown. 5 HCV There is no immunoglobulin or postexposure use of antiviral agents (e.g., interferon with or without ribavirin) available to prevent HCV infection. The present data suggests that an established infection might need to be present before interferon can be treated as an effective treatment. 5 While there is no PEP for HCV, recommendations for post-exposure management are intended to achieve early identification of chronic disease and, if present, referral for evaluation of treatment options. 5 HIV PEP should be initiated in HCWs who have been exposed to a source patient with suspected HIV infection. If the source is found to be HIV-negative after the initiation of PEP, it should be discontinued. Although concerns have been expressed regarding HIV-negative sources being in the window period for seroconversion, no case of transmission involving an exposure source during the window period has been reported in the US. 3 Normally, a two-drug (basic) or threedrug (expanded) PEP regimens, depending on the level of risk for HIV transmission as determined by the level of exposure (e.g., type and severity of exposure, the source patient s HIV status and/or risk factors for HIV infection, and the prevalence of Vol 1 Number 1; January,
8 Occupational Exposure to Body Fluids HIV in the local population [if source patient s HIV status is unknown]) 4 is recommended. 3 When the source person s virus is known or suspected to be resistant to one or more of the drugs considered for the PEP regimen, choosing those drugs to which the source person s virus is unlikely to be resistant is recommended. Combinations which can be used for PEP include zidovudine (ZDV) and lamivudine (3TC) or emtricitabine (FTC); stavudine (d4t) and 3TC or FTC; and tenofovir (TDF) and 3TC or FTC. Addition of a third or even a fourth drug should be considered for exposures that pose an increased risk of transmission or that involve a source patient in whom antiretroviral drug resistance is likely. 3 PEP should be initiated immediately, preferably within one hour of exposure 3,21,23 and continued for a month to be most effective; 21 starting PEP even after two weeks post-exposure may still be beneficial. 23 Nonetheless, some reports indicate that if PEP is delayed more than 72 hours, it is not effective. 5,21 If a question arises concerning which antiretroviral drugs to be used, or whether to use a basic or expanded PEP regimen, the basic regimen should be started immediately and not delay the PEP administration. 3 Reevaluation of the exposed HCW should be strongly encouraged within 72 hours after the exposure, especially as additional information about the nature of the exposure or source person becomes available. HCWs with occupational exposure to HIV should receive follow-up counseling, post-exposure testing, and medical evaluation regardless of whether they receive PEP. HIV-antibody testing by enzyme-linked immunosorbant assay (ELISA) should be used to monitor HCWs for seroconversion six months after occupational HIV exposure. After baseline tests at the time of exposure, follow-up tests could be performed at six weeks, 12 weeks, and six months post-exposure. 3 Counseling for HCWs after Exposure Counseling the exposed HCWs is a critical component of any evaluation of an occupational exposure to potentially infectious substances. Topics to be considered in the discussion include the risk of acquisition of each of the blood-borne pathogens, side effects of any treatments initiated, measures that can reduce the risk of secondary transmission (e.g., abstinence or use of condoms), signs and symptoms of acute infection, and recommendations for follow-up evaluation and testing. 4 HCWs exposed to HBV- or HCV-infected BBF do not need to take any special precautions to prevent secondary transmission during the follow-up; however, they should refrain from donating blood, plasma, organs, tissue, or semen. The exposed person does not need to modify sexual practices or refrain from becoming pregnant. If an exposed woman is breast feeding, she does not need to discontinue. 5 Conclusion Occupational exposure to BBF is an important and common hazard for HCWs, placing them at risk for blood-borne pathogens (HBV, HCV and HIV) and resulting in psychological stress, occupational diseases and loss of financial and human resources. Pre- and post-exposure management helps in decreasing the incidence of acquisition of infections. Pre-exposure preventions include educating HCWs, using standard precautions, and vaccination. Post-exposure prevention includes PEP and early identification of disease. Early and easy 8 Vol 1 Number 1; January, 2010
9 M. Bahadori, G. Sadigh access to written protocols for prompt reporting, evaluation, counseling, treatment, and follow-up of occupationally-exposed HCWs should be prepared by the health care organization. HCWs should be aware of the support of their employers if an occupational event occurs, so that they can feel secure in their job. Acknowledgements The authors would like to sincerely thank Dorsa Sadigh (BSc) for her help in English editing. This research has been supported by National Iranian Oil Company (NIOC) Hospital and Tehran University of Medical Sciences (TUMS). Conflict of Interest: None declared References 1. Tarantola A, Abiteboul D, Rachline A. Infection risks following accidental exposure to blood or body fluids in health care workers: a review of pathogens transmitted in published cases. Am J Infect Control 2006;34(6): Rapparini C. Occupational HIV infection among health care workers exposed to blood and body fluids in Brazil. Am J Infect Control 2006;34(4): Panlilio AL, Cardo DM, Grohskopf LA, Heneine W, Ross CS. Updated U.S. Public Health Service guidelines for the management of occupational exposures to HIV and recommendations for postexposure prophylaxis. MMWR Recomm Rep 2005;54(RR-9): Calfee DP. Prevention and management of occupational exposures to human immunodeficiency virus (HIV). Mt Sinai J Med 2006;73(6): US Publich Health Sevice. Updated US Public Health Service guidelines for the management of occupational exposures to HBV, HCV, and HIV and recommendations for postexposure prophylaxis. MMWR Recomm Rep 2001;50: Alamgir H, Cvitkovich Y, Astrakianakis G, Yu S, Yassi A. Needlestick and other potential blood and body fluid exposures among health care workers in British Columbia, Canada. Am J Infect Control 2008;36(1): Falagas ME, Karydis I, Kostogiannou I. Percutaneous exposure incidents of the health care personnel in a newly founded tertiary hospital: a prospective study. PLoS ONE 2007;2(2):e Pruss-Ustun A, Rapiti E, Hutin Y. Estimation of the global burden of disease attributable to contaminated sharps injuries among health-care workers. Am J Ind Med 2005;48(6): Boal WL, Leiss JK, Sousa S, Lyden JT, Li J, Jagger J. The national study to prevent blood exposure in paramedics: exposure reporting. Am J Ind Med 2008;51(3): Elliott SK, Keeton A, Holt A. Medical students knowledge of sharps injuries. J Hosp Infect 2005;60(4): CCDR. Update-surveillance of health care workers exposed to blood, body fluids and bloodborne pathogens in Canadian hospital settings: 1 April, 2000, to 31 March, Canada Communicable Disease Report. CCDR 2003;29: Ertem M, Dalar Y, Cevik U, Sahin H. Injury or body fluid splash incidence rate during three months period in elective surgery procedures, at Dicle University Hospital, Diyarbakir, Turkey. Ulus Travma Acil Cerrahi Derg 2008;14(1): Bowman W, Bohnker BK. Needle-stick epidemiology in Navy health care workers based on INJTRAK reports ( ). Mil Med 2005;170(12): Askarian M, Malekmakan L, McLaws Vol 1 Number 1; January,
10 Occupational Exposure to Body Fluids ML, Zare N, Patterson JM. Prevalence of needlestick injuries among medical students at a university in Iran. Infect Control Hosp Epidemiol 2006;27(1): Trim JC, Elliott TS. A review of sharps injuries and preventative strategies. J Hosp Infect 2003;53(4): Lymer UB, Schutz AA, Isaksson B. A descriptive study of blood exposure incidents among healthcare workers in a university hospital in Sweden. J Hosp Infect 1997;35(3): Lymer UB, Richt B, Isaksson B. Blood exposure: factors promoting health care workers compliance with guidelines in connection with risk. J Clin Nurs 2004;13(5): Moghimi M, Marashi SA, Kabir A, et al. Knowledge, Attitude, and Practice of Iranian Surgeons About Blood-Borne Diseases. J Surg Res O Malley EM, Scott RD, 2nd, Gayle J, et al. Costs of management of occupational exposures to blood and body fluids. Infect Control Hosp Epidemiol 2007;28(7): Lee JM, Botteman MF, Xanthakos N, Nicklasson L. Needlestick injuries in the United States. Epidemiologic, economic, and quality of life issues. Aaohn J 2005;53(3): Wilburn SQ. Needlestick and sharps injury prevention. Online J Issues Nurs 2004;9(3): WHO. The world health report reducing risks, promoting healthy life: Geneva: WHO, Peate I. Occupational exposure of staff to HIV and prophylaxis therapy. Br J Nurs 2004;13(19): Vol 1 Number 1; January, 2010
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Needles and Sharps Exposure: How do We Proceed?
 Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
Knowledge, attitude and practices among health care workers on needle-stick injuries
 Kathmandu University Medical Journal (2003) Vol. 1,. 2, 91-94 Original Article Knowledge, attitude and practices among health care workers on needle-stick injuries Gurubacharya DL 1, KC Mathura 2, Karki
Kathmandu University Medical Journal (2003) Vol. 1,. 2, 91-94 Original Article Knowledge, attitude and practices among health care workers on needle-stick injuries Gurubacharya DL 1, KC Mathura 2, Karki
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
19/08/2014. What is Injection Safety?
 Infection Prevention and Control A Foundation Course SAFE INJECTION PRACTICES AND SHARPS MANAGEMENT Fiona Barry IPCN Mercy University Hospital, Cork 2014 Links to CDC Materials http://www.youtube.com/watch%3fv%3d6d0stmoz80k
Infection Prevention and Control A Foundation Course SAFE INJECTION PRACTICES AND SHARPS MANAGEMENT Fiona Barry IPCN Mercy University Hospital, Cork 2014 Links to CDC Materials http://www.youtube.com/watch%3fv%3d6d0stmoz80k
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
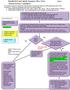 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: F:
 University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
University of Louisville Campus Health Services 401 East Chestnut Street Suite110 P: 502-852-2708 F: 502-852-0660 hlthoff@louisville.edu Training Objectives Understand the OSHA Bloodborne Pathogens Regulation
BAY-ARENAC BEHAVIORAL HEALTH AUTHORITY POLICIES AND PROCEDURES MANUAL
 Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Healthcare Professionals
 EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
Bloodborne Pathogens and Universal Precautions
 Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
Bloodborne Pathogens and Universal Precautions Parkway School District 2012-2013 Revised 9/19/2012 What Are Bloodborne Pathogens(BBPs) Bloodborne pathogens (BBPs) are disease causing microorganisms carried
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
 Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Bloodborne Pathogens Training For School Personnel
 Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV
 Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
NEOMED ACADEMIC POLICY
 (A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
(A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
SLIDE 2: (Opening slide) Good Morning (Afternoon, Evening). Thank you for inviting me to speak to you today about safer needle devices.
 1 SLIDE 2: (Opening slide) Good Morning (Afternoon, Evening). Thank you for inviting me to speak to you today about safer needle devices. 2 SLIDE 3: (Purpose) Since the Bloodborne Pathogens Standard was
1 SLIDE 2: (Opening slide) Good Morning (Afternoon, Evening). Thank you for inviting me to speak to you today about safer needle devices. 2 SLIDE 3: (Purpose) Since the Bloodborne Pathogens Standard was
Healthcare Personnel Immunization Recommendations
 Healthcare Personnel Immunization Recommendations Kathleen Harriman, PhD, MPH, RN California Department of Public Health Immunization Branch Vaccine Preventable Disease Epidemiology Section kathleen.harriman@cdph.ca.gov
Healthcare Personnel Immunization Recommendations Kathleen Harriman, PhD, MPH, RN California Department of Public Health Immunization Branch Vaccine Preventable Disease Epidemiology Section kathleen.harriman@cdph.ca.gov
Public Employees Occupational Safety and Health Alert (Publication No. 21)
 Clifton R. Lacy, M.D. Commissioner Public Employees Occupational Safety and Health Alert (Publication No. 21) James E. McGreevey Governor Albert G. Kroll Commissioner OSHA Revises the Bloodborne Pathogens
Clifton R. Lacy, M.D. Commissioner Public Employees Occupational Safety and Health Alert (Publication No. 21) James E. McGreevey Governor Albert G. Kroll Commissioner OSHA Revises the Bloodborne Pathogens
Bloodborne Pathogens. By Deborah Massarella RN, MSN
 Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
Bloodborne Pathogens By Deborah Massarella RN, MSN 2010, 2014 Objectives At conclusion of in-service learners will: 1. Identify two types of personal protective equipment. 2. Identify two prevention measures
2014 OSHA Blood-borne Pathogens (BBP) Update JHS Annual Mandatory Education
 2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Emergency Department and Receiving Areas CHAPTER 24: Author P. Suri, MD R. Gopaul, MD
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 24: Emergency Department and Receiving Areas Author P. Suri, MD R. Gopaul, MD Chapter Editor Gonzalo Bearman MD, MPH, FACP, FSHEA, FIDSA Topic Outline
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 24: Emergency Department and Receiving Areas Author P. Suri, MD R. Gopaul, MD Chapter Editor Gonzalo Bearman MD, MPH, FACP, FSHEA, FIDSA Topic Outline
Chapter 2 Hepatitis B Overview
 Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Needle Stick. Mr. Fadi J. Zaben RN MSN IMET 2000, Ramallah IMET 2000
 Needle Stick Mr. Fadi J. Zaben RN MSN, Ramallah 1 Objectives: Define Needle Stick. Mention the sharps. Discus the rate of incidence. Identify the person who is at risk. Discus Needle stick and infectious
Needle Stick Mr. Fadi J. Zaben RN MSN, Ramallah 1 Objectives: Define Needle Stick. Mention the sharps. Discus the rate of incidence. Identify the person who is at risk. Discus Needle stick and infectious
Health Care Workers and Viral Hepatitis in Turkey. Bulent Degertekin M.D. Viral Hepatitis Prevention Board Meeting
 Different Aspects of Viral Hepatitis Health Care Workers and Viral Hepatitis in Turkey Bulent Degertekin M.D. Viral Hepatitis Prevention Board Meeting 12 13 November 2009 Istanbul. Turkey Hepatitis B and
Different Aspects of Viral Hepatitis Health Care Workers and Viral Hepatitis in Turkey Bulent Degertekin M.D. Viral Hepatitis Prevention Board Meeting 12 13 November 2009 Istanbul. Turkey Hepatitis B and
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Naval Support Activity Monterey / Naval Postgraduate School
 Background: Bloodborne pathogens are viruses present in human blood and body fluids that can cause disease in humans. Diseases like the hepatitis B virus (HBV), human immunodeficiency virus (HIV) and others
Background: Bloodborne pathogens are viruses present in human blood and body fluids that can cause disease in humans. Diseases like the hepatitis B virus (HBV), human immunodeficiency virus (HIV) and others
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3
 MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
Bloodborne Pathogens: Recognition and Treatment 2011
 Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees
 BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
BLOODBORNE PATHOGENS. 30 Minutes
 BLOODBORNE PATHOGENS 30 Minutes AGENDA Define bloodborne pathogens Recognize OSHA standards related to bloodborne pathogens Identify employer responsibilities related to compliance with OSHA standards
BLOODBORNE PATHOGENS 30 Minutes AGENDA Define bloodborne pathogens Recognize OSHA standards related to bloodborne pathogens Identify employer responsibilities related to compliance with OSHA standards
Hepatitis B and C Overview, Outbreaks, and Recommendations. Viral Hepatitis Language. Types of Viral Hepatitis 7/1/2013
 Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
Hepatitis B and C Overview, Outbreaks, and Recommendations Elizabeth Lawlor, MS Healthy Kansans living in safe and sustainable environments. Viral Hepatitis Language Acute infection is when the infection
Life Threatening Vocational Hazards Diseases and Toxins
 Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Environmental Health and Safety Offices BLOODBORNE PATHOGENS
 Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
Commonly Asked Questions About Chronic Hepatitis C
 Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
FOR INFECTION TO OCCUR: Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV
 OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Introduction to the Need for a Special Focus on Healthcare Worker Safety
 Introduction to the Need for a Special Focus on Healthcare Worker Safety There is still room for improvement in the area of safety and infection control for patients and healthcare workers by lowering
Introduction to the Need for a Special Focus on Healthcare Worker Safety There is still room for improvement in the area of safety and infection control for patients and healthcare workers by lowering
BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens]
![BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens] BLOODBORNEPATHOGENS. CAP Safety Meetings. Revision: CAP Safety Meetings [Bloodborne Pathogens]](/thumbs/73/68341667.jpg) BLOODBORNEPATHOGENS CAP Safety Meetings Revision: 10-2011 2011 Copyright - PEC/Premier Safety Management, Inc. All Rights Reserved Revision: [10-2011] 1 THEBLOODBORNEPATHOGENSSTANDARD The Bloodborne Pathogens
BLOODBORNEPATHOGENS CAP Safety Meetings Revision: 10-2011 2011 Copyright - PEC/Premier Safety Management, Inc. All Rights Reserved Revision: [10-2011] 1 THEBLOODBORNEPATHOGENSSTANDARD The Bloodborne Pathogens
Training Objectives. Provide a basic understanding of:
 Training Objectives Provide a basic understanding of: 1. Bloodborne pathogens (BBP) 2. Common modes of transmission of BBP 3. Methods to prevent transmission of BBP 4. Information to help school staff
Training Objectives Provide a basic understanding of: 1. Bloodborne pathogens (BBP) 2. Common modes of transmission of BBP 3. Methods to prevent transmission of BBP 4. Information to help school staff
Bloodborne Pathogens LVHN s Annual Safety Course
 Slide 1 Bloodborne Pathogens LVHN s Annual Safety Course Nucleus Medical Media (2010). Blood Carries Nutrients. Smart Imagebase. Lehigh Valley Health Network cares about your safety especially about protecting
Slide 1 Bloodborne Pathogens LVHN s Annual Safety Course Nucleus Medical Media (2010). Blood Carries Nutrients. Smart Imagebase. Lehigh Valley Health Network cares about your safety especially about protecting
ADMINISTRATIVE SERVICES MANUAL
 1 of 10 Purpose Scope University of Alaska Anchorage departments will develop plans and procedures to limit occupational exposure to blood and other potentially infectious materials (PIM) in compliance
1 of 10 Purpose Scope University of Alaska Anchorage departments will develop plans and procedures to limit occupational exposure to blood and other potentially infectious materials (PIM) in compliance
ACS BLOOD BORNE PATHOGEN TRAINING
 ACS BLOOD BORNE PATHOGEN TRAINING OBJECTIVE Define Blood borne pathogens Instruct how to recognize exposure to BBP Prevent or reduce risk of BBP exposure Identify high risk groups Review ACS exposure protocol
ACS BLOOD BORNE PATHOGEN TRAINING OBJECTIVE Define Blood borne pathogens Instruct how to recognize exposure to BBP Prevent or reduce risk of BBP exposure Identify high risk groups Review ACS exposure protocol
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
CDM 3 rd Year & Postdocs June 28 th 2017
 Bloodborne Pathogens/Infection Control Tuberculosis Awareness CDM 3 rd Year & Postdocs June 28 th 2017 Biological Safety Officer Environmental Health and Safety Training Outline Infection Control Bloodborne
Bloodborne Pathogens/Infection Control Tuberculosis Awareness CDM 3 rd Year & Postdocs June 28 th 2017 Biological Safety Officer Environmental Health and Safety Training Outline Infection Control Bloodborne
MICROBIOLOGY 211: HIV AND DENTISTRY
 ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
Bloodborne Pathogens. Penn State University Environmental Health & Safety
 Bloodborne Pathogens Penn State University Environmental Health & Safety Diseases of Concern Hepatitis B (Serum Hepatitis) Hepatitis C (non-a non-b Hepatitis) HIV (Human Immunodeficiency Virus aka the
Bloodborne Pathogens Penn State University Environmental Health & Safety Diseases of Concern Hepatitis B (Serum Hepatitis) Hepatitis C (non-a non-b Hepatitis) HIV (Human Immunodeficiency Virus aka the
BLOODBORNE DISEASES. Prevention of transmission for school staff. for staff not directly responsible for providing care or cleaning up blood
 BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
Goldenrod Hills Community Action. Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR
 Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
Hepatitis B Control. Table of Contents
 Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Control Table of Contents 1.0 INTRODUCTION... 1 2.0 GOALS... 1 3.0 DEFINITIONS... 1 4.0 CASE MANAGEMENT... 3 5.0 HEPATITIS B POST- EXPOSURE MANAGEMENT... 4 TABLE 1: HEPATITIS B POST EXPOSURE PROPHYLAXIS...
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training
 Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
Gwynedd Mercy University Bloodborne Pathogen Safety and Awareness Training Education is the KEY Here are Gwynedd Mercy University, we recognize the importance of providing a safe working environment for
Doc: 1.9. Course: Patient Safety Solutions. Topic: Infection prevention and control. Summary
 Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Course: Patient Safety Solutions Topic: Infection prevention and control Summary Health care-associated Infection (HCAI) is defined as an infection acquired in a hospital by a patient who was admitted
Bloodborne Pathogens
 Bloodborne Pathogens Disclaimer This training material presents very important information. Your organization must do an evaluation of all exposures, applicable codes and regulations, and establish proper
Bloodborne Pathogens Disclaimer This training material presents very important information. Your organization must do an evaluation of all exposures, applicable codes and regulations, and establish proper
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens
 Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
CMC Annual Review of BLOODBORNE DISEASES. Prevention of Transmission for School Staff
 CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
Factors Affecting Compliance with the Safety Agenda
 Factors Affecting Compliance with the Safety Agenda Janine Jagger, M.P.H., Ph.D. International Healthcare Worker Safety Center University of Virginia Building the Chain of Safety: Stakeholders Summit College
Factors Affecting Compliance with the Safety Agenda Janine Jagger, M.P.H., Ph.D. International Healthcare Worker Safety Center University of Virginia Building the Chain of Safety: Stakeholders Summit College
Infection Control Program (ICP) ICP Components 1. Exposure Determination 2. Control Methods A. Universal Precautions
 Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV. Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya.
 TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
TRANSMISSION OF BLOODBORNE PATHOGENS: HIV,HBV,HCV Dr Daniel Kimani HIV Prevention Medical Transmission CDC, Kenya. Nevada Hepatitis C Outbreak Tied to Las Vegas Clinic. Thousands Now At Risk for Hepatitis,
Bloodborne Pathogens Training. July 26, 2012
 Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
Bloodborne Pathogens Training July 26, 2012 Introduction As sure as the sun comes up every day, children end up with scraped knees, cuts, and bruises. Students of all ages hurt themselves on the playground,
