43. Guidelines on Needle stick Injury
|
|
|
- Hugh Robinson
- 5 years ago
- Views:
Transcription
1 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency Virus (HIV) published in Material that has been added by ODNS has been placed in italics. The full text of this is available on our website on the downloads page. Background Dry needling involves the use of sterile single use needles, which penetrate the body wall of humans to achieve therapeutic results. Of necessity, this exposes the therapist to the body fluids of the patient, specifically blood and blood products. The HI virus is transmitted through exposure to blood and some other body fluids. Body fluids include semen, vaginal secretions or other fluids contaminated with visible blood, such as are encountered when using needle therapy. (Note that saliva, tears, sweat, urine and breast milk are not associated with the risk of HIV transmission in an occupational setting). Thus the therapist practicing dry needling will be exposed to an increased risk of contracting HIV through contact with infected blood. The average risk of HIV infection from all types of reported percutaneous exposure to HIV infected blood is 0.3%. Although this increased risk is small, it behooves the therapist to take reasonable precautions to minimize this risk both before and after potential exposure. The risk increases with the amount of bleeding and depth to which the needle is inserted (superficial needling carries less risk than deep needling), but the risk is much less for solid needles, such as are used in Dry Needing, than it is for hollow needles which are typically used for Venepuncture or administration of medication. This document is written to summaries the official government position on Postexposure prophylaxis (PEP), and should be read together with the guidelines on needle safety, which are also contained in this manual. Remember that if you keep to the safety guidelines on how to needle safely (i.e. how to keep yourself safe), you will probably not need to follow the post exposure guidelines, as you will not get pricked. ODNS
2 The use of any trade names in this document is for identification only and does not imply endorsement by either Optimal Dry Needling Solutions, or the Department of Health. Health department recommendations: Management of occupational exposure to blood or body fluids (adapted for dry needling) 1. Know your own status now. Be tested after any suspect exposure. 2. For all exposures, immediately clean the affected area with an antiseptic agent and water and irrigate. Mucous membrane and eye exposures should be rinsed and flushed extensively with water. Get yourself treated first before worrying about the patient s status. 3. Evaluate the exposure as follows: 3.1 The potential exposures that should be considered for PEP A blood contaminated needle stick injury (i.e. dry needling, esp. deep needling) An injury with a blood-contaminated sharp instrument or similar Instruments contaminated with semen, CSF, pleural or other serous fluid (excluding urine and faces An exposure to the mucous membranes (eye, mouth) with the above fluids A blood contamination of compromised or diseased skin (such as a Weeping eczema) Prolonged exposure to a large volume of blood on normal skin 3.2 Determine the HIV status of the exposure source If there is no record of the HIV status of the source patient, then an attempt should be made to obtain blood from the patient for this purpose. This should be according to existing guidelines for HIV testing and include pre- and post-test counseling. An approved rapid HIV test could be performed and later confirmed by routine HIV testing procedures. Do not wait for the result of such a test before beginning ARV treatment If the patient refuses HIV testing, if there is no record of a recent HIV test result, or if HIV testing is not possible or available, then a doctor caring for the patient should be consulted as to the likelihood of the patient being HIV positive. Clinical signs indicating possible HIV infection include: TB infection, signs of immune deficiency such as oral thrush (candidiasis) and/or oral hairy cell leukoplakia on the tongue, recent herpes zoster or molluscum contagiosum infection, Kaposi sarcoma, recurrent infectious conditions such as diarrhoeal diseases, pneumonia, meningitis, skin sepsis; or unexplained weight loss, seborrhoeic dermatitis or persistent glandular lymphadenopathy. Using these clinical ODNS
3 parameters in the absence of an HIV test is far from ideal and many HIV positive persons will be asymptomatic. [In situations where there is a high suspicion that the patient may be in the window period, then an HIV PCR or HIV p24 antigen test could be considered.] 4. Recommendations for PEP 4.1 PEP is recommended for any high-risk exposure (see table 1). Deep dry needling falls in this category. 4.2 ZVD in combination with Lamivudine is recommended for high-risk exposures. Single therapy with ZVD may be effective and is preferable to no PEP but is likely to be less effective than therapy with more than one drug. Single ZVD PEP therapy is not recommended by any recognized international authority. 4.3 Indinavir can be added for very high risk exposures. Very high risk exposures include: 1) large volume of blood; 2) deep injury; and, 3) if the source patient has been on ZVD for more than 6 months. 4.4 PEP should be initiated promptly, preferably within 1-2 hours after the exposure. The interval after which there is no benefit from using PEP is not yet defined, however most experts recommend PEP within 24 hours after exposure. Some experts may still consider PEP 7-14 days after the exposure in cases where there is highest risk exposure. To avoid delays in starting PEP, starter packs of recommended drugs should be available in all health care settings. 4.5 PEP should be continued for 4 weeks. PEP should be discontinued if there are serious toxicities or intolerance and should be continued even in the presence of mild side effects. 4.6 Exposures such as small blood volumes or other body fluid contact on normal healthy skin are considered very low risk. PEP is not recommended in these cases but can be assessed on a case by case basis. For exposures to urine or faeces, PEP is not recommended unless these are contaminated with blood. 4.7 If the source patient s HIV status is not known, initiating PEP should be decided upon on a case-by-case basis, and based on circumstances including the likelihood of HIV infection in the source patient. 4.8 PEP is recommended if: 1) the source patient is HIV positive; 2) the rapid HIV test is positive; or, 3) or if there is a high index of suspicion that the source patient is HIV positive. 4.9 An Elisa HIV test should be done and documented on the exposed health care worker at baseline (i.e. within 24 hours of the injury), at 6 weeks, 12 weeks and at 6 months. In rare instances sero-conversion can take place over a period longer than 6 months Tests for occupational exposure to Hepatitis B and C, syphilis, malaria, etc. should also be considered if deemed appropriate. PCR and p24 antigen tests ODNS
4 are not routinely recommended as false positive and negative tests are not infrequent and these tests are costly Supportive counseling should be available to the health care worker. The health care worker should consider using a barrier method for safer sex. Avoidance of pregnancy in female health care workers is also recommended until sero-conversion is excluded. Pregnancy in health care workers should not preclude the use of PEP If HIV sero-conversion occurs the health care worker should be referred for appropriate counseling and treatment and informed about compensation claims (see Appendix 2) An appropriate and confidential reporting system should exist within health facilities to document all occupational exposures and details on the source patient, and health care worker for medico-legal purposes and for possible compensation and insurance claims. All HIV related occupational exposures, irrespective of whether PEP is recommended, should be reported to health facilities Health care facilities should delegate responsible officials to oversee the reporting and recording of occupational HIV exposures If the HIV test on the source patient is negative, it can be assumed that there is a low risk of exposure to HIV unless there is reasonable information to suggest that the source patient is in the window period. In these cases PEP is not recommended. REFERENCES (for Needlestick Guidelines) 1. CDC. Case Control study of HIV sero-conversion In healthcare workers after percutaneous exposure to HIV infected blood in France, United Kingdom and United States, January 1988-August 1994.MMWR 1995;44: Gerberding JL. Management of occupational exposures to blood borne viruses. N Eng J Med 1995;332: Jochimsen EM. Failures of Zidovudine Post exposure Prophylaxis. Am J Med 1997;102 (5b) CDC. Case control study of HIV sero-conversion in healthcare workers after percutaneous exposure to HIV infected blood. France, United Kingdom and United States, January 1988-August 1994.MMWR 1995;44: Connor EM, Sperling RS, Gelber R, et al. Reduction of maternal-infant transmission of HIV type 1 with Zidovudine treatment. N Eng J Med 1994; 331: CDC. Thailand Collaborative Perinatal HIV Prevention Study 7. Saag MS. Candidate Antiretroviral Agents for Use in Post Exposure Prophylaxis. Am J Med 1997;102( (5b): ibid 9. Centers for Disease Control and Prevention. Update: Provisional recommendations for chemoprophylaxis after 10. Jochimsen EM. Failures of Zidovudine Post Exposure Prophylaxis. Am J Med 1997;102 (5b) U.S. Department of health and Human Services, Centers for Disease Control and Prevention (CDC). Public health Service Guidelines for the Management of Health-Care Worker Exposure to HIV and Recommendations for Post Exposure Prophylaxis. May /Vol47/N0.RR7 page Centres for Disease Control and Prevention. Update: Provisional recommendations for chemoprophylaxis after 13. Personal Communication with Dr Des Martin, National Institute of Virology 14. Centers for Disease Control and Prevention. Update: Provisional recommendations for chemoprophylaxis after 15. B Schoub. Virus SA. 1997: Guidelines to the Management of Occupational Exposure to HIV. National Institute of Virology. 16. Tokars JI, Marcus R, Culver DH, et al. Surveillance of HIV infection and Zidovudine use among health care workers after occupational exposure to HIV infected blood. Ann Intern Med 1993;118: Centres for Disease Control and Prevention. Update: Provisional recommendations for chemoprophylaxis after occupational exposure to human immunodeficiency virus MMWR. 1996;45: Adapted from Centres for Disease Control and Prevention. Update: Provisional recommendations for chemoprophylaxis after occupational exposure to Human Immunodeficiency Virus MMWR. 1996; 45: , and from B Schoub. Virus SA Guidelines to the Management of Occupational Exposure to HIV. National Institute of Virology ODNS
5 Type of occupational exposure, risk of exposure, HIV status of the source and recommendations for PEP Percutaneous injury Risk of exposure Recommendation for PEP Superficial injury, solid needle (Superficial dry needling) Skin puncture, visible blood on the needle, hollow needle Needle used in a vein or artery Deep intra-muscular injury or injection into the body (Deep dry needling) Some risk High risk Highest risk Highest risk Recommend Basic Regimen Recommend Basic Regimen, Consider Expanded Regimen Recommend Basic Regimen, Consider Expanded Regimen Mucosal and skin contacts Risk of exposure Recommendation for PEP Unbroken healthy skin Low risk Not recommended Compromised skin, small volume and brief contact Compromised skin, large volume and/or prolonged contact Low risk Increased risk Recommend Basic Regimen HIV Status of Source Risk of exposure Recommendation for PEP Negative Very Low Not recommended Positive, Clinical AIDS and/or a low CD4 cell count and /or a high viral load Low for small volumes or short duration on intact skin HIV Positive, Clinical AIDS and/or a low CD4 cell count and /or a high viral load Unknown High risk for percutaneous injuries Recommend basic or expanded regimen depending on the severity of injury Consider PEP on a case-bycase basis ODNS
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
HIV Occupational Transmission and Exposure. Marsh Gelbart 2010
 HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
HIV Occupational Transmission and Exposure Marsh Gelbart 2010 Rationale for Post Exposure Prophylaxis (PEP) It was estimated that the risk for HIV transmission after percutaneous exposures involving larger
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
FAMILY HIV CENTER NJ CARES SANE
 HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
10/17/2015. Chapter 55. Care of the Patient with HIV/AIDS. History of HIV. HIV Modes of Transmission
 Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
MICROBIOLOGY 211: HIV AND DENTISTRY
 ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
ICROBIOLOGY 211: 2006-2007 Dr. Gillian ccarthy Room 00022 DSB Tel 661 2111 Ext 86122; E-mail: gillian.mccarthy@schulich.uwo.ca HIV AND DENTISTRY OBJECTIVES: The student will be able to discuss - The epidemiology
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
You will now begin the Bloodborne Pathogen Refresher Training.
 You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
For. Correctional. Officers. Your. Health Risks. in Correctional Settings. Facts. About HIV
 For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
2014 OSHA Blood-borne Pathogens (BBP) Update JHS Annual Mandatory Education
 2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Nursing Interventions
 Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
Blood borne Pathogen Exposure Policy for Students
 Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
Blood borne Pathogen Exposure Policy for Students A University of Rhode Island (URI) student or intern who sustains an exposure from a needle stick, instrument stick, or mucous membranes to non-intact
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
BAY-ARENAC BEHAVIORAL HEALTH AUTHORITY POLICIES AND PROCEDURES MANUAL
 Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
Frequently Asked Questions about HIV/AIDS: Transmission and Prevention How is HIV passed from one person to another?
 Frequently Asked Questions about HIV/AIDS: Transmission and Prevention How is HIV passed from one person to another? HIV transmission can occur when blood, semen (including pre-seminal fluid or "pre-cum"),
Frequently Asked Questions about HIV/AIDS: Transmission and Prevention How is HIV passed from one person to another? HIV transmission can occur when blood, semen (including pre-seminal fluid or "pre-cum"),
BLOODBORNE DISEASES. Prevention of transmission for school staff. for staff not directly responsible for providing care or cleaning up blood
 BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
BLOODBORNE DISEASES Prevention of transmission for school staff for staff not directly responsible for providing care or cleaning up blood MASSACHUSETTS DIVISION OF OCCUPATIONAL SAFETY Robert Prezioso,
CMC Annual Review of BLOODBORNE DISEASES. Prevention of Transmission for School Staff
 CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Blood borne Pathogen
 Blood borne Pathogen Training For Certified Nursing Assistants Meets the Blood borne Pathogens & Infection Control Update (Formerly HIV/AIDS) 1 0 In-service Hour Meets the Blood borne Pathogens & Infection
Blood borne Pathogen Training For Certified Nursing Assistants Meets the Blood borne Pathogens & Infection Control Update (Formerly HIV/AIDS) 1 0 In-service Hour Meets the Blood borne Pathogens & Infection
An International Antiviral Society-USA
 Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
NEOMED ACADEMIC POLICY
 (A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
(A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
Chapter 2 Hepatitis B Overview
 Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Chapter 2 Hepatitis B Overview 23 24 This page intentionally left blank. HEPATITIS B OVERVIEW Hepatitis B Virus The hepatitis B virus (HBV) belongs to the Hepadnaviridae family and is known to cause both
Maryland State Department of Education Maryland Department of Health and Mental Hygiene Maryland State School Health Council
 Maryland State Department of Education Maryland Department of Health and Mental Hygiene Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Management of Students with
Maryland State Department of Education Maryland Department of Health and Mental Hygiene Maryland State School Health Council MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINES Management of Students with
EQuIP 5 - This version June 2011 Revision Due June 2014
 Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
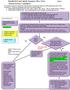 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Hepatitis C Best Practice Guidelines For Local Health Departments
 Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
Hepatitis C Best Practice Guidelines For Local Health Departments LHDs are responsible for investigating and reporting all physician reported cases of acute hepatitis C (HCV). For clients known to have
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 337 N OVEMBER 20, 1997 NUMBER 21 A CASE CONTROL STUDY OF HIV SEROCONVERSION IN HEALTH CARE WORKERS AFTER
The New England Journal of Medicine Copyright, 1997, by the Massachusetts Medical Society VOLUME 337 N OVEMBER 20, 1997 NUMBER 21 A CASE CONTROL STUDY OF HIV SEROCONVERSION IN HEALTH CARE WORKERS AFTER
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
Billing and Coding for HIV Services
 Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
BLOODBORNE PATHOGENS: OR: DO WE REALLY HAVE TO DO THIS AGAIN????
 BLOODBORNE PATHOGENS: OR: DO WE REALLY HAVE TO DO THIS AGAIN???? YES THIS YEAR AND EVERY YEAR HEREAFTER REMEMBER: A REVIEW IS NEVER A BAD IDEA YOUR JOBS PUT YOU AT RISK THE DAY YOU KNOW EVERYTHING AND
BLOODBORNE PATHOGENS: OR: DO WE REALLY HAVE TO DO THIS AGAIN???? YES THIS YEAR AND EVERY YEAR HEREAFTER REMEMBER: A REVIEW IS NEVER A BAD IDEA YOUR JOBS PUT YOU AT RISK THE DAY YOU KNOW EVERYTHING AND
CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004)
 CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004) Adults living with HIV/AIDS - 1.1 million Children - 150,000 Number using ART - 24,000 Number needing ARVs - 200,000 National
CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004) Adults living with HIV/AIDS - 1.1 million Children - 150,000 Number using ART - 24,000 Number needing ARVs - 200,000 National
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Sunny Smiles Clinical Guidelines
 Sunny Smiles Clinical Guidelines Accidental Inoculation Injury - Guidance for healthcare professionals on dealing with needle-stick injuries to members Date Written: April 2010 Contents 1 Local Contacts...3
Sunny Smiles Clinical Guidelines Accidental Inoculation Injury - Guidance for healthcare professionals on dealing with needle-stick injuries to members Date Written: April 2010 Contents 1 Local Contacts...3
Bloodborne pathogens and Standard Precautions
 Bloodborne pathogens and Standard Precautions Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may
Bloodborne pathogens and Standard Precautions Teaching plan To use this lesson for self-study, the learner should read the material, do the activity, and take the test. For group study, the leader may
Safety Tips from the WorkSafe People
 Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Bloodborne Pathogens 29 CFR
 Bloodborne Pathogens 29 CFR 1910.1030 Revised OSHA Bloodborne Pathogens Compliance Directive (CPL2-2.44D) Could You Contract a Disease at Work? Administering first aid? Cleaning the restrooms? Using a
Bloodborne Pathogens 29 CFR 1910.1030 Revised OSHA Bloodborne Pathogens Compliance Directive (CPL2-2.44D) Could You Contract a Disease at Work? Administering first aid? Cleaning the restrooms? Using a
June 4, Page 1 of 5 POLICY STATEMENT
 POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
POLICY STATEMENT This policy has been written to inform all staff, clients, relatives and other visitors to the homes of service users about the risks associated with MRSA, AIDS and HIV hazards in the
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Blood Borne Pathogens
 Bloomer School District Blood Borne Pathogens Developed by: Tammy Kornesczuk, RN Act Rather Than Re-act School Staff tend to be nurturing and care-taking people Don t rush to help without putting on gloves
Bloomer School District Blood Borne Pathogens Developed by: Tammy Kornesczuk, RN Act Rather Than Re-act School Staff tend to be nurturing and care-taking people Don t rush to help without putting on gloves
Self-Instructional Packet (SIP)
 Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
Bloodborne Pathogens
 Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
How are Blood borne pathogens harmful? How do you come into contact with Blood-borne pathogens?
 What are Blood borne pathogens? How are Blood borne pathogens harmful? How do you come into contact with Blood-borne pathogens? How do I protect myself? A blood-borne disease is one that can be spread
What are Blood borne pathogens? How are Blood borne pathogens harmful? How do you come into contact with Blood-borne pathogens? How do I protect myself? A blood-borne disease is one that can be spread
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
Supervisors, Department Heads and Principals will:
 The Greater Victoria School District is committed to each student s success in learning within a responsive and safe environment. REGULATION 4213 UNIVERSAL PRECAUTIONS Preamble Universal Precautions are
The Greater Victoria School District is committed to each student s success in learning within a responsive and safe environment. REGULATION 4213 UNIVERSAL PRECAUTIONS Preamble Universal Precautions are
Needles and Sharps Exposure: How do We Proceed?
 Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
Needles and Sharps Exposure: How do We Proceed? UMAYYA MUSHARRAFIEH,MD AMERICAN UNIVERSITY OF BEIRUT MEDICAL CENTER JUNE 14, 2013 Health care workers who use or may be exposed to needles are at increased
What employees should know about UNIVERSAL PRECAUTIONS. They re work practices that help prevent contact with blood and certain other body fluids.
 What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
What are Universal Precautions? What employees should know about UNIVERSAL PRECAUTIONS They re work practices that help prevent contact with blood and certain other body fluids. Universal precautions are:
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
 Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
Original Article Abstract NUJHS Vol. 5, No.4, December 2015, ISSN 2249-7110 Knowledge, awareness and compliance among dental professionals regarding percutaneous exposure incidents as occupational hazard
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids
 Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Blood Borne Pathogens (BBP)
 Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Blood Borne Pathogens (BBP) Healthcare facilities are high-risk areas for exposure to bloodborne pathogens, so protect yourself and remind others to do the same. There are three bloodborne pathogens of
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS.
 SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS February 2012 Version 1.0 1 CONTENTS Section Page 1.0 Introduction 3
SHARPS PROCEDURE PROCEDURE FOR THE SAFE USE & DISPOSAL OF SHARPS AND THE MANAGEMENT OF SHARPS INJURIES AND BLOOD EXPOSURE INCIDENTS February 2012 Version 1.0 1 CONTENTS Section Page 1.0 Introduction 3
patients with blood borne viruses Controlled Document Number: Version Number: 4 Controlled Document Sponsor: Controlled Document Lead:
 CONTROLLED DOCUMENT Procedure for the management of patients with blood borne viruses CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 4 Controlled Document Sponsor: Controlled
CONTROLLED DOCUMENT Procedure for the management of patients with blood borne viruses CATEGORY: CLASSIFICATION: PURPOSE Controlled Document Number: Version Number: 4 Controlled Document Sponsor: Controlled
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
INDIAN JOURNAL OF DENTAL ADVANCEMENTS
 INDIAN JOURNAL OF DENTAL ADVANCEMENTS Journal homepage: www.nacd.in CASE REPORT Prophylaxis Following Occupational Exposure To HIV Manika 1, Shashikant M C 2, Shailaja S 3 Sr. Lecturer 1 & 3 Dept of Oral
INDIAN JOURNAL OF DENTAL ADVANCEMENTS Journal homepage: www.nacd.in CASE REPORT Prophylaxis Following Occupational Exposure To HIV Manika 1, Shashikant M C 2, Shailaja S 3 Sr. Lecturer 1 & 3 Dept of Oral
Greater Glasgow and Clyde. Blood Borne Viruses: Some important basic facts
 Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts A programme developed by Greater Glasgow and Clyde Health
Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts Greater Glasgow and Clyde Blood Borne Viruses: Some important basic facts A programme developed by Greater Glasgow and Clyde Health
Post Blood & Body Fluid Exposure Checklist
 Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Post Blood & Body Fluid Exposure Checklist Employee Name: : First Aid completed (If exposure was to eye, irrigate for 20 minutes at the nearest eye wash station. If exposure was to skin, wash affected
Bloodborne Pathogen Module. Chelmsford Public Schools September, 2016
 Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Bloodborne Pathogen Module Chelmsford Public Schools September, 2016 Why is this important? v OSHA BB Pathogen Standard anyone whose job requires exposure to BB pathogens is required to complete training
Summary of Key Points. WHO Position Paper on Vaccines against Hepatitis B, July 2017
 Summary of Key Points WHO Position Paper on Vaccines against Hepatitis B, July 2017 1 Background l HBV is transmitted by exposure of mucosal membranes or non-intact skin to infected blood, saliva, semen
Summary of Key Points WHO Position Paper on Vaccines against Hepatitis B, July 2017 1 Background l HBV is transmitted by exposure of mucosal membranes or non-intact skin to infected blood, saliva, semen
