Correlation of Parasite Load Determined by Quantitative PCR to Clinical Outcome in a Heart Transplant Patient with Disseminated Toxoplasmosis
|
|
|
- Peregrine Chambers
- 5 years ago
- Views:
Transcription
1 JOURNAL OF CLINICAL MICROBIOLOGY, July 2010, p Vol. 48, No /10/$12.00 doi: /jcm Copyright 2010, American Society for Microbiology. All Rights Reserved. Correlation of Parasite Load Determined by Quantitative PCR to Clinical Outcome in a Heart Transplant Patient with Disseminated Toxoplasmosis Solène Patrat-Delon, 1 Jean-Pierre Gangneux, 2 Sylvain Lavoué, 1 Bernard Lelong, 3 Claude Guiguen, 2 Yves le Tulzo, 1 and Florence Robert-Gangneux 2 * Service de Réanimation Médicale et Maladies Infectieuses, 1 Laboratoire de Parasitologie-Mycologie, 2 and Service de Cardiologie, 3 Centre Hospitalier et Universitaire de Rennes, Rennes, France Received 8 February 2010/Returned for modification 22 March 2010/Accepted 30 April 2010 Disseminated toxoplasmosis is a life-threatening infection in transplant recipients, which results either from reactivation of latent infection or from organ-transmitted primary infection. Preventive measures and diagnostic screening methods differ between countries and are related to the seroprevalence of Toxoplasma spp. in the general population. Here we report a case of disseminated toxoplasmosis in a heart transplant recipient with previous immunity that occurred after cotrimoxazole prophylaxis for the prevention of Pneumocystis jirovecii pneumonia was stopped. Quantitative PCR proved useful for the diagnosis and monitoring of Toxoplasma infection. Decreasing parasitic burdens in sequential samples of cerebrospinal fluid, blood, and bronchoalveolar lavage fluid correlated with a favorable outcome and allowed modulation of the immunosuppressive drug regimen. The duration of anti-toxoplasma treatment and the need for maintenance prophylaxis are discussed, as well as prophylaxis for solid-organ transplant recipients. Although a rare event in heart transplant recipients, Toxoplasma reactivation must be investigated promptly, since early treatment improves the prognosis. Toxoplasmosis is a worldwide parasitic disease caused by the intracellular protozoan Toxoplasma gondii. After infection, acquired mostly through contaminated vegetables or undercooked meat, the parasite can persist for life, encysted in different sites such as the muscles, heart, brain, eye, and, more rarely, other organs. Whereas clinical symptoms are usually absent or mild in primarily infected immunocompetent individuals, the infection is life-threatening for immunocompromised patients (17). In transplant patients, severe or disseminated toxoplasmosis can result either from reactivation of latent infection in the recipient or from organ-transmitted infection from a seropositive donor to a seronegative recipient (6, 29), a situation where heart transplants carry the highest risk (16, 19, 22, 32). Reactivation of a chronic infection may occur in the recipient irrespective of the type of graft, but the risk is closely related to the duration and degree of immunosuppression. The risk also differs according to the immunosuppression protocol and therefore according to the graft, with hematopoietic stem cell transplantation (HSCT) carrying the highest risk (10). Furthermore, the incidence of Toxoplasma reactivation is greater in countries with higher seroprevalences. The diagnosis of acute toxoplasmosis in immunocompromised patients relies on PCR detection of parasite DNA in blood, cerebrospinal fluid (CSF), bronchoalveolar lavage (BAL) samples, or biopsy specimens. Serology performs poorly in the * Corresponding author. Mailing address: Laboratoire de Parasitologie-Mycologie, Centre Hospitalier et Universitaire de Rennes, Université Rennes 1 IFR 140/IRSET, 2 rue Henri Le Guilloux, Rennes, France. Phone: Fax: florence.robert-gangneux@univ-rennes1.fr. Published ahead of print on 12 May diagnosis of reactivation of infection, due to a lack of sensitivity (in HSCT patients) or poor correlation with clinical reactivation (for solid-organ transplantation [SOT]). Here we report a case of disseminated toxoplasmosis in a previously seropositive heart transplant recipient who underwent several severe infectious complications leading to interruption of cotrimoxazole prophylaxis and subsequently to Toxoplasma reactivation. After the initial diagnosis, the infection was monitored by quantitative PCR on blood, CSF, and pulmonary samples. A decrease in parasite load correlated with a favorable clinical outcome upon treatment. Quantitative PCR is considered to be a valuable tool for the diagnosis and monitoring of acute toxoplasmosis in SOT recipients. Our results reemphasize the need to monitor Toxoplasma reactivation in seropositive recipients, particularly in countries with high seroprevalences. Potential drug regimens for anti-toxoplasma chemoprophylaxis in heart transplant patients are discussed. CASE REPORT A 57-year-old man underwent a heart transplant following ischemic cardiomyopathy with severe heart failure. The patient was seropositive for anti-toxoplasma antibodies before transplantation (Table 1), as was the donor (IgG level, 43 IU/ml; no IgM detected). Both serological results were indicative of past infection. Primary preventive treatment with cotrimoxazole (40 and 200 mg/day) for Pneumocystis jirovecii pneumonia prophylaxis was started on the first postoperative day (day 1 [D1]), continued until D27, and was then stopped because of intolerance (aggravation of thrombocytopenia from 62 g/liter to 39 g/liter, aggravation of leucopenia from 6 g/liter to 3 g/liter, and acute renal failure). Immunosuppressive therapy was started 2541
2 2542 PATRAT-DELON ET AL. J. CLIN. MICROBIOL. TABLE 1. Results of Toxoplasma serological follow-up and Toxoplasma DNA detection by quantitative PCR Date of sample collection a Titer of anti-toxoplasma antibody b IgG (IU/ml) IgM (ELISA index) IgM (ISAGA index) T. gondii burden (no. of parasites/ml of sample) by quantitative PCR c Whole blood CSF BAL fluid Day Day Day Day , ,000 Day 119 1,000 Day Day Day 129 2, Day Day 164 Undet. Day 185 2, Day a From the day of transplantation. b Positivity thresholds were 9 for IgG (Platelia Toxo IgG ELISA; Bio-Rad), 1 for IgM by the Platelia Toxo IgM ELISA (Bio-Rad), and 9 to 12 for IgM by the IgM ISAGA (biomérieux)., not done. c Undet., undetectable. on D1 to D3 with mofetil mycophenolate (MFM) at 3 g/day, methylprednisolone hemisuccinate (440 mg/day on D1, 410 mg/day on D2, and 240 mg/day on D3), and thymoglobulin. The dose of methylprednisolone hemisuccinate was then reduced progressively to 30 mg/day on D30, without any change in the MFM regimen, and cyclosporine was introduced on D3 with residual rates ranging from 100 to 200 ng/ml. The postoperative evolution was marked by several infectious and cardiovascular complications. During the early postoperative days (D3), the patient presented with mixed cardiogenic and septic shock due to Escherichia coli, which required circulatory assistance and antibiotherapy with imipenem and gentamicin. On D28, he developed invasive pulmonary aspergillosis, diagnosed by positive BAL fluid cultures and the presence of circulating galactomannan antigen, which was successfully treated with voriconazole. In the following days, he developed catheter-related bacteremia due to Enterococcus faecalis and Staphylococcus epidermidis, which was treated with vancomycin. He was readmitted to the intensive care unit (ICU) from D45 to D87 for severe successive infectious complications, including extended-spectrum -lactamase (ESBL) E. coli bacteremia and a Scarpa s triangle abscess treated with imipenem, and pneumopathy due to Enterobacter aerogenes, probably acquired through mechanical ventilation, which had a favorable outcome upon cefotaxime antibiotherapy. Everolimus was introduced on D46 in order to optimize the immunosuppressive regimen and reduce the cyclosporine dose. However, due to the lack of improvement of renal function, everolimus was stopped on D70. Cyclosporine was replaced by tacrolimus on D78, in combination with methylprednisolone hemisuccinate and MFM, because of the onset of thrombotic microangiopathy. On D104, the patient finally left the ICU with stable hemodynamics, despite renal failure requiring dialysis three times a week and encephalopathy attributed to anti-calcineurins. On D113, he presented with febrile respiratory distress, hypoxemia, and persistent encephalopathy, leading to orotracheal intubation for invasive mechanical ventilation. Pulmonary radiography revealed bilateral pulmonary infiltrates. BAL fluid was positive for T. gondii trophozoites by direct microbiological examination and negative for bacteria and viruses by culture and/or PCR. Cerebral tomodensitometry gave a normal result, and lumbar puncture yielded a clear CSF sample, with moderate hyperproteinorachia (0.56 g/liter) and normoglycorachia without hypercellularity ( 1 leukocyte/ l), which was negative for bacteria and parasites by direct examination. PCR allowed the detection of high levels of Toxoplasma DNA in blood, BAL fluid, and CSF. An endomyocardial biopsy sample taken on D124 did not reveal the presence of cysts or signs of acute rejection. Toxoplasma serology was checked concomitantly and showed strong serological reactivation, with high titers of both IgG and IgM antibodies. Anti-Toxoplasma treatment was introduced immediately (D113) with pyrimethamine at 50 mg/ day and sulfadiazine at 3 g/day; the latter was replaced on D118 by clindamycin (2,400 mg/day) because of premature hematotoxicity. Because Toxoplasma DNA could still be detected 2 weeks after the onset of therapy, the immunosuppressive regimen was reduced until D131 by stopping MFM and decreasing methylprednisolone hemisuccinate to 10 mg/day and tacrolimus to a 3-ng/ml residual rate (versus 15 to 20 ng/ml before). At the same time, the lymphocyte count increased from 0.02 g/liter on D113 to 0.4 g/liter on D138. This decrease in immunosuppression was accompanied by a decrease in the parasitic burden. Definitive clearance of parasites from the different fluids was checked on D164. The patient s fever started to decrease from D142, and he was completely apyrexial on D149 (i.e., 36 days after beginning specific therapy and 18 days after a change in the immunosuppressive regimen). Extubation was delayed on D159 because of critical neuromyopathy. After 48 days of antiparasitic treatment with a curative dose regimen, secondary prophylaxis was continued with pyrimethamine at 25 mg/day and clindamycin at 1,200 mg/day. On D180, echocardiography showed a strong alteration of systolic function, leading to an endomyocardial biopsy, which confirmed the diagnosis of acute rejection. Immunosuppressive therapy was optimized with an increase in the dose of prednisone to 20 mg/day and the progressive reintroduction of MFM in addition to tacrolimus. Toxoplasma secondary prophylaxis was modified with pyrimethamine (25 mg/day) and cotrimoxazole (160 and 800 mg at the end of each dialysis, three times a week). The patient left the cardiology unit 206 days after transplantation with terminal chronic renal failure, major malnutrition, and reduced mobility. His immunosuppressive regimen was maintained with MFM at 1,000 mg/day (reduced to 750 mg/day on D214), prednisone at 20 mg/day, and tacrolimus with a residual rate of 5.9 to 7.5 mg/liter. Secondary antiparasite prophylaxis was continued. The patient is still in a rehabilitation center 1 year after transplantation. MATERIALS AND METHODS Clinical samples. Sequential serum, whole-blood, CSF, and pulmonary samples (BAL fluid) were collected for diagnostic purposes (i.e., serology, direct examination [BAL fluid], and quantitative PCR [whole blood, CSF, BAL fluid]). After centrifugation, serum was removed and stored at 20 C until serological
3 VOL. 48, 2010 PCR MONITORING OF DISSEMINATED TOXOPLASMOSIS 2543 testing. Slides were prepared from BAL fluid after cytocentrifugation at 91 g for 5 min and were stained using Giemsa stain. All samples for DNA extraction were frozen at 80 C. Serology. Specific anti-toxoplasma IgG and IgM antibodies were detected using the Platelia Toxo IgG and Platelia Toxo IgM enzyme-linked immunosorbent assays (ELISAs) (Bio-Rad, Marnes-la-Coquette, France) and an immunosorbent agglutination assay (ISAGA) (IgM ISAGA; biomérieux, Marcy l Etoile, France). Parasite DNA detection. DNA was extracted using QIAamp DNA minikit tissue extraction columns (Qiagen, Courtaboeuf, France) after an initial step of overnight proteinase K digestion at 56 C for whole blood. Real-time PCR was performed using TaqMan probes on a Step One Plus system (Applera, Villebon, France). The PCR assay targeted the highly repetitive sequence REP-529 (GenBank accession no. AF487550) with primers 270F (5 -AGAGACACCG GAATGCGATCT) and 318R (5 -TTCGTCCAAGCCTCCGACT) and with probe 310T, labeled with 6-carboxyfluorescein (6-FAM) and 6-carboxytetramethylrhodamine (TAMRA) (5 -TCGTGGTGATGGCGGAGAGAATT GA). Amplification was performed as described previously (28), after a decontamination step with uracil-dna glycosylase. All DNA samples were tested in duplicate, with and without an internal control consisting of a small amount (5 copies/ml) of parasite genomic DNA from strain RH added to the well. A standard curve was established using serial dilutions of Toxoplasma strain RH recovered and purified from peritoneal lavage fluid from an infected mouse. The sensitivity of the PCR assay has been evaluated previously; it can detect 2 to 5 parasites/ml (data not shown) and is evaluated annually in the framework of the quality control program of the Centre National de Référence de la Toxoplasmose ( The parasitic load of each sample was evaluated from the standard curve. Mouse inoculation (in vivo culture). With the aim of isolating parasites for genotyping, two Swiss IOPS female mice were inoculated intraperitoneally with 0.5 ml of BAL fluid. Mice were subjected to serological examination 5 weeks later by using an hemagglutination assay (Toxoscreen; biomérieux), according to the manufacturer s instructions. As expected, serological testing gave positive results, and infection was confirmed in mice by the presence of cerebral cysts in brain tissue on microscopic examination. The remaining brain tissue was sent to the Centre National de Référence de la Toxoplasmose (Biological Resource Center, Reims-Limoges, France) for genotyping. RESULTS The serological and parasitological results for the sequential samples are shown in Table 1. Parasite DNA was concomitantly detected in BAL fluid, CSF, and whole-blood samples on D112 posttransplantation. Because tachyzoites were visible on Giemsa-stained smears of BAL fluid, two Swiss IOPS mice were immediately inoculated with the remaining fluid. The isolated Toxoplasma strain was typed as genotype II. After the initiation of specific treatment, the parasite load in whole blood was carefully monitored by quantitative PCR. On D12 post-initiation of therapy, parasites could still be detected at decreasing but nevertheless significant numbers in whole blood and BAL fluid (Table 1), leading clinicians to perform another lumbar puncture that still gave a low-level positive result on D14 posttherapy. A new blood sample obtained after 21 days of treatment had a residual parasite DNA load of 6 tachyzoites/ml and was associated with clinical improvement and a decrease in fever. Total clearance of parasite DNA from blood was demonstrated 1 month later (Table 1). Toxoplasma serology showed stable IgG and IgM antibody titers until 3 weeks before the dissemination of the parasite. The patient had persistent IgM detection, probably related to chronic residual IgM from a past infection, as demonstrated by a previous serological result, obtained 1 year before transplantation (Table 1). IgG and IgM antibody titers began to rise dramatically from the day of parasite isolation, reaching a peak 2 months after the episode and decreasing slowly over the next 4 months. DISCUSSION Disseminated toxoplasmosis is a well-known life-threatening infectious complication in transplant recipients, although it is a rare event in SOT patients. It usually results from a mismatch between the serological Toxoplasma statuses of the donor and the recipient (seropositive donor to seronegative recipient) and the transplantation of a graft containing encysted Toxoplasma (16, 19). Heart and heart-lung transplants carry the highest risk of Toxoplasma graft transmission to a seronegative recipient (32), which can be prevented by cotrimoxazole prophylaxis (25). In high-risk mismatched heart recipients, the efficacy and safety of cotrimoxazole has been established (2, 18) at the same dose regimen commonly used to prevent P. jirovecii pneumonia, but trimethoprim-sulfamethoxazole (160 and 800 mg) three times a week is also effective (2, 24). In contrast, a combination of pyrimethamine and sulfadoxine (75 mg and 1,500 mg) every 2 weeks has been reported to be ineffective at preventing heart-transmitted infection (13). In cases of intolerance, pyrimethamine alone (25 mg/day) can be a valuable alternative (24, 33). Prevention also relies on serological screening of the donor and the recipient, as well as counseling of seronegative patients to avoid exposure through food (31). In France, where seroprevalence is high, serological screening is mandatory for every organ donor; screening of recipients is strongly recommended; and the risk of graft-transmitted toxoplasmosis is reduced both by prolonged chemoprophylaxis and by careful follow-up of patients in cases of mismatch. However, in countries with low Toxoplasma seroprevalence, guidelines may differ, and serological screening is not routinely recommended for all patients (18, 25, 34). Reactivation of past infection is more frequently observed in HSCT patients than in SOT patients and is associated with a high mortality rate (10, 11). Consequently, some HSCT centers monitor patients carefully for several months by repeated screening for Toxoplasma DNA using quantitative PCR on blood samples, since prompt initiation of therapy is crucial for patients with profound immunodeficiency (7, 14, 20). In heart transplant recipients, disseminated toxoplasmosis due to reactivation is rare and in most cases is favored by enhancement of immunosuppressive regimens in cases of acute rejection. Moreover, the incidence of reactivation is related to the prevalence of toxoplasmosis in the general population, a fact that explains the lack of consensus concerning biological follow-up and anti-toxoplasma chemoprophylaxis for heart transplant patients with infections acquired prior to transplantation (23). Prophylaxis in Toxoplasma-seropositive heart transplant patients is usually ensured by cotrimoxazole in the framework of P. jirovecii pneumonia prevention. The very low incidence of Toxoplasma reactivation in such patients does not justify a specific prophylaxis regimen outside this context (3), but the potential risk of reactivation of latent infection should not be ignored for patients receiving pentamidine for P. jirovecii pneumonia prophylaxis or with interruption of cotrimoxazole prophylaxis (11), as was the case for our patient. In our case, multiple infectious events, although nonviral, that combined to stop prophylaxis could have heightened immunodeficiency and
4 2544 PATRAT-DELON ET AL. J. CLIN. MICROBIOL. favored Toxoplasma reactivation. This case and others (8) raise the question of prolonging prophylaxis for as long as 3 months for patients with latent toxoplasmosis before transplantation, particularly patients with serious complications in the postoperative months. However, cotrimoxazole has been reported to be ineffective at preventing Toxoplasma reactivation in a liver transplant recipient receiving antilymphocytic immunoglobulins for the treatment of acute graft rejection (4), suggesting that other prophylactic regimens could be used for severely immunocompromised patients. An alternative using pyrimethamine-sulfadoxine was proposed as a twice-weekly regimen for the prevention of P. jirovecii pneumonia and toxoplasmic encephalitis in HIV-infected patients (30) or as a onceweekly regimen for bone marrow transplant recipients (12). It is widely agreed that early diagnosis improves the prognosis of patients with disseminated toxoplasmosis, but diagnostic strategies differ from one country to another. In our hospital, Toxoplasma serological follow-up is carried out two or three times during the first year and once a year thereafter. Serological reactivation with significantly increasing IgG titers, even associated with specific IgM detection, can be observed in the absence of any clinical manifestations. Nevertheless, it should prompt the search for Toxoplasma infection. In the present case, serology was unhelpful for diagnosis, since the last serum sample obtained 24 days prior to the finding of Toxoplasma-positive BAL fluid showed no sign of serological reactivation. Quantitative PCR allowed confirmation of cerebral involvement and was useful for monitoring the response to treatment. The doses of immunosuppressive drugs (MFM, methylprednisolone hemisuccinate, and tacrolimus) were temporarily reduced to prompt an immune response against the parasite, and these drugs were then restored at the full doses in order to avoid acute rejection when the infection was under control. The delay before PCR-negative blood results were obtained was quite long (more than 3 weeks), but shorter than that in reports with lethal outcomes (21), probably reflecting the extent of immunodeficiency. The level of parasitemia was similar to that in other reports (6). Furthermore, the isolate obtained from our patient was typed as genotype II, an avirulent genotype widely isolated from both congenitally infected and immunocompromised patients in France (1), a fact that could explain the favorable outcome observed here, in contrast to the poor outcomes reported by Delhaes et al. for two allo- SCT patients infected with virulent genotypes (9). Reactivation of the recipient s own Toxoplasma cysts is the most probable hypothesis, although it has also been suggested that disseminated toxoplasmosis could be due to reinfection with a new strain acquired from the transplanted organ (27). Here no cysts were observed in the myocardial biopsy performed on D124. Despite the lack of sensitivity inherent in the examination of small biopsy samples, this result could suggest peripheral reactivation of the recipient s cysts rather than reactivation of an organ-transmitted strain. Anti-Toxoplasma curative therapy usually relies on a synergistic combination of antimicrobial agents, including pyrimethamine and sulfadiazine or pyrimethamine and clindamycin (15), but cotrimoxazole has also been shown to be effective as the first-line treatment for HIV-infected patients (5). A reduction in immunosuppressive therapy is essential wherever possible and could explain the short delay to a favorable evolution in our case. Curative therapy is generally given at high doses for 6 weeks (31), followed by maintenance therapy. However, data on the duration and drug regimen for secondary prophylaxis are scarce, particularly for transplant patients. Cotrimoxazole (5) or sulfadiazine-pyrimethamine (25 mg and 2 g daily or 50 mg and 2 g three times a week) (26) has been proposed for maintenance therapy of toxoplasma encephalitis in HIV-infected patients. In the present case, secondary prophylaxis with cotrimoxazole at the end of each dialysis and 25 mg of pyrimethamine daily was chosen in order to ensure optimal levels of protective drugs in the serum. The optimal duration of secondary prophylaxis has not been clearly defined, but it should be at least 6 months, depending on the ongoing risk factors for reactivation (31). In conclusion, disseminated toxoplasmosis remains a lifethreatening infection in heart transplant recipients with previous immunity, although it is a rare event that depends mostly on the seroprevalence of Toxoplasma in the general population. Despite its low incidence, Toxoplasma reactivation must be investigated rapidly for patients with neurological signs, unexplained fever, or pulmonary infiltrates, since the prognosis is highly dependent on early treatment. ACKNOWLEDGMENTS We thank the Biological Resources Center of the Centre National de Référence de la Toxoplasmose (Limoges-Reims, France) for strain genotyping and Newmed Publishing Services for English editing. REFERENCES 1. Ajzenberg, D., H. Yera, P. Marty, L. Paris, F. Dalle, J. Menotti, D. Aubert, J. Franck, M. H. Bessières, D. Quinio, H. Pelloux, L. Delhaes, N. Desbois, P. Thulliez, F. Robert-Gangneux, C. Kauffmann-Lacroix, S. Pujol, M. Rabodonirina, M. E. Bougnoux, B. Cuisenier, C. Duhamel, T. H. Duong, D. Filisetti, P. Flori, F. Gay-Andrieu, F. Pratlong, G. Nevez, A. Totet, B. Carme, H. Bonnabau, M. L. Dardé, and I. Villena Genotype of 88 Toxoplasma gondii isolates associated with toxoplasmosis in immunocompromised patients and correlation with clinical findings. J. Infect. Dis. 199: Baden, L. R., J. T. Katz, L. Franck, S. Tsang, M. Hall, R. H. Rubin, and J. Jarcho Successful toxoplasmosis prophylaxis after orthotopic cardiac transplantation with trimethoprim-sulfamethoxazole. Transplantation 75: Baran, D. A., M. M. Alwarshetty, S. Alvi, L. H. Arroyo, S. Lubitz, S. Pinney, A. L. Gass, and M. J. Zucker Is toxoplasmosis prophylaxis necessary in cardiac transplantation? Long-term follow-up at two transplant centers. J. Heart Lung Transplant. 25: Barcán, L. A., M. L. Dallurzo, L. O. Clara, A. Valledor, S. Macias, E. Zorkin, S. Gerona, and B. Livellara Toxoplasma gondii pneumonia in liver transplantation: survival after a severe case of reactivation. Transpl. Infect. Dis. 4: Béraud, G., S. Pierre-François, A. Foltzer, S. Abel, B. Liautaud, D. Smadja, and A. Cabié Cotrimoxazole for treatment of cerebral toxoplasmosis: an observational cohort study during Am. J. Trop. Med. Hyg. 80: Botterel, F., P. Ichai, C. Feray, P. Bouree, F. Saliba, R. Tur Raspa, D. Samuel, and S. Romand Disseminated toxoplasmosis, resulting from infection of allograft, after orthotopic liver transplantation: usefulness of quantitative PCR. J. Clin. Microbiol. 40: Bretagne, S., J. M. Costa, F. Foulet, L. Jabot-Lestang, F. Baud-Camus, and C. Cordonnier Prospective study of toxoplasma reactivation by polymerase chain reaction in allogeneic stem-cell transplant recipients. Transpl. Infect. Dis. 2: Castagnini, M., S. Bernazzali, C. Ginanneschi, B. Marchi, M. Maccherini, C. Tsioulpas, and P. Tanganelli Fatal disseminated toxoplasmosis in a cardiac transplantation with seropositive match for Toxoplasma: should prophylaxis be extended? Transpl. Immunol. 18: Delhaes, L., J.-C. Mraz, E. Fréalle, I. Durand-Joly, L. Magro, D. Ajzenberg, M.-L. Dardé, E. Dei-Cas, and I. Yakoub-Agha. 13 July Severe pulmonary toxoplasmosis after allo-sct in two patients: from Toxoplasma genotyping to clinical management. Bone Marrow Transplant. doi: / bmt Derouin, F., A. Devergie, P. Auber, E. Gluckman, B. Beauvais, Y. J. F. Garin, and M. Lariviere Toxoplasmosis in bone marrow-transplant recipients: report of seven cases and review. Clin. Infect. Dis. 15:
5 VOL. 48, 2010 PCR MONITORING OF DISSEMINATED TOXOPLASMOSIS Derouin, F., and H. Pelloux Prevention of toxoplasmosis in transplant patients. Clin. Microbiol. Infect. 14: Foot, A. B., Y. J. Garin, P. Ribaud, A. Devergie, F. Derouin, and E. Gluckman Prophylaxis of toxoplasmosis infection with pyrimethamine/sulfadoxine (Fansidar) in bone marrow transplant recipients. Bone Marrow Transplant. 14: Fricker-Hidalgo, H., J. P. Brion, M. Durand, O. Chavanon, M. P. Brenier- Pinchart, and H. Pelloux Disseminated toxoplasmosis with pulmonary involvement after heart transplantation. Transpl. Infect. Dis. 7: Fricker-Hidalgo, H., C. E. Bulabois, M. P. Brenier-Pinchart, R. Hamidfar, F. Garban, J. P. Brion, J. F. Timsit, J. Y. Cahn, and H. Pelloux Diagnosis of toxoplasmosis after allogeneic stem cell transplantation: results of DNA detection and serological techniques. Clin. Infect. Dis. 48:e9 e Fung, H. B., and H. L. Kirschenbaum Treatment regimens for patients with toxoplasmic encephalitis. Clin. Ther. 18: Gallino, A., M. Maggiorini, W. Kiowski, X. Martin, W. Wunderli, J. Schneider, M. Turina, and F. Follath Toxoplasmosis in heart transplant recipients. Eur. J. Clin. Microbiol. Infect. Dis. 15: Goebel, W. S., J. H. Conway, P. Faught, S. Vakili, and P. R. Haut Disseminated toxoplasmosis resulting in graft failure in a cord blood stem cell transplant recipient. Pediatr. Blood Cancer 48: Gourishankar, S., K. Doucette, J. Fenton, D. Purych, K. Kowalewska-Grochowska, and J. Preiksaitis The use of donor and recipients screening for Toxoplasma in the era of universal trimethoprim sulfamethoxazole prophylaxis. Transplantation 85: Luft, B. J., Y. Naot, F. G. Araujo, E. B. Stinson, and J. S. Remington Primary and reactivated Toxoplasma infection in patients with cardiac transplants. Clinical spectrum and problems in diagnosis in a defined population. Ann. Intern. Med. 99: Martino, R., S. Bretagne, H. Einsele, J. Maertens, A. J. Ullmann, R. Parody, U. Schumacher, C. Pautas, K. Theunissen, C. Schindel, C. Muňoz, N. Margall, and C. Cordonnier Early detection of Toxoplasma infection by molecular monitoring of Toxoplasma gondii in peripheral blood samples after allogeneic stem cell transplantation. Clin. Infect. Dis. 40: Menotti, J., G. Vilela, S. Romand, Y. J. F. Garin, L. Ades, E. Gluckman, F. Derouin, and P. Ribaud Comparison of PCR-enzyme-linked immunosorbent assay and real-time PCR assay for diagnosis of an unusual case of cerebral toxoplasmosis in a stem cell transplant recipient. J. Clin. Microbiol. 41: Michaels, M. G., E. R. Wald, F. J. Fricker, P. J. del Nido, and J. Armitage Toxoplasmosis in pediatric recipients of heart transplants. Clin. Infect. Dis. 14: Montoya, J. G., L. F. Giraldo, B. Efron, E. B. Stinson, P. Gamberg, S. Hunt, N. Giannetti, J. Miller, and J. S. Remington Infectious complications among 620 consecutive heart transplant patients at Stanford University Medical Center. Clin. Infect. Dis. 33: Muñoz, P., J. Arencibia, C. Rodríguez, M. Rivera, J. Palomo, J. Yañez, and E. Bouza Trimethoprim-sulfamethoxazole as toxoplasmosis prophylaxis for heart transplant recipients. Clin. Infect. Dis. 36: Orr, K. E., F. K. Gould, G. Short, J. H. Dark, C. J. Hilton, P. A. Corris, and R. Freeman Outcome of Toxoplasma gondii mismatches in heart transplant recipients over a period of 8 years. J. Infect. 29: Podzamczer, D., J. M. Miró, E. Ferrer, J. M. Gatell, J. M. Ramón, E. Ribera, G. Sirera, A. Cruceta, H. Knobel, P. Domingo, R. Polo, M. Leyes, J. Cosin, M. C. Fariñas, J. Arrizabalaga, J. Martínez-Lacasa, and F. Gudiol Thrice-weekly sulfadiazine-pyrimethamine for maintenance therapy of toxoplasmic encephalitis in HIV-infected patients. Spanish Toxoplasmosis Study Group. Eur. J. Clin. Microbiol. Infect. Dis. 19: Robert-Gangneux, F., C. Amrein, V. Lavarde, F. Botterel, and J. Dupouy- Camet Neosynthesized IgG detected by Western blotting in Toxoplasma-seropositive heart or lung transplant recipients. Transpl. Int. 13: Robert-Gangneux, F., P. Dupretz, C. Yvenou, D. Quinio, P. Poulain, C. Guiguen, and J. P. Gangneux Clinical relevance of placenta examination for the diagnosis of congenital toxoplasmosis. Pediatr. Infect. Dis. J. 29: Rogers, N. M., C. A. Peh, R. Faull, M. Pannell, J. Cooper, and G. R. Russ Transmission of toxoplasmosis in two renal allograft recipients receiving an organ from the same donor. Transpl. Infect. Dis. 10: Schürmann, D., F. Bergmann, H. Albrecht, J. Padberg, T. Wünsche, T. Grünewald, M. Schürmann, M. Grobusch, M. Vallée, B. Ruf, and N. Suttorp Effectiveness of twice-weekly pyrimethamine-sulfadoxine as primary prophylaxis of Pneumocystis carinii pneumonia and toxoplasmic encephalitis in patients with advanced HIV infection. Eur. J. Clin. Microbiol. Infect. Dis. 21: Soave, R Prophylaxis strategies for solid-organ transplantation. Clin. Infect. Dis. 33:S26 S Speirs, G. E., M. Hakim, R. Y. Calne, and T. G. Wreghitt Relative risk of donor-transmitted Toxoplasma gondii infection in heart, liver and kidney transplant recipients. Clin. Transplant. 2: Wreghitt, T. G., M. Hakim, J. J. Gray, A. H. Balfour, P. G. Stovin, S. Stewart, J. Scott, T. A. English, and J. Wallwork Toxoplasmosis in heart and heart and lung transplant recipients. J. Clin. Pathol. 42: Wulf, M. W. H., R. van Crevel, R. Portier, C. G. ter Meulen, W. J. G. Melchers, A. van der Ven, and J. M. D. Galama Toxoplasmosis after renal transplantation: implications of a missed diagnosis. J. Clin. Microbiol. 43:
Lecture-7- Hazem Al-Khafaji 2016
 TOXOPLASMOSIS Lecture-7- Hazem Al-Khafaji 2016 TOXOPLASMOSIS It is a disease caused by Toxoplasma gondii which is a protozoan parasite that is infects a variety of mammals and birds throughout the world.
TOXOPLASMOSIS Lecture-7- Hazem Al-Khafaji 2016 TOXOPLASMOSIS It is a disease caused by Toxoplasma gondii which is a protozoan parasite that is infects a variety of mammals and birds throughout the world.
Cerebral Toxoplasmosis in HIV-Infected Patients. Ahmed Saad,MD,FACP
 Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Performance of the BioPlex 2200 flow immunoassay (Bio- Rad) in critical cases of serodiagnosis of toxoplasmosis
 CVI Accepts, published online ahead of print on 29 January 2014 Clin. Vaccine Immunol. doi:10.1128/cvi.00624-13 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 3 Performance
CVI Accepts, published online ahead of print on 29 January 2014 Clin. Vaccine Immunol. doi:10.1128/cvi.00624-13 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 3 Performance
REVIEW. Prevention of toxoplasmosis in transplant patients F. Derouin 1 and H. Pelloux 2, on behalf of the ESCMID Study Group on Clinical Parasitology
 REVIEW 10.1111/j.1469-0691.2008.02091.x Prevention of toxoplasmosis in transplant patients F. Derouin 1 and H. Pelloux 2, on behalf of the ESCMID Study Group on Clinical Parasitology 1 Laboratory of Parasitology
REVIEW 10.1111/j.1469-0691.2008.02091.x Prevention of toxoplasmosis in transplant patients F. Derouin 1 and H. Pelloux 2, on behalf of the ESCMID Study Group on Clinical Parasitology 1 Laboratory of Parasitology
Toxoplasmosis in heart and heart and lung transplant recipients
 J Clin Pathol 1989;42:194-199 Toxoplasmosis in heart and heart and lung transplant recipients T G WREGHITT,* M HAKIM,* J J GRAY,* A H BALFOUR,t P G I STOVIN,4 SUSAN STEWART,: J SCOTT, T A H ENGLISH,II
J Clin Pathol 1989;42:194-199 Toxoplasmosis in heart and heart and lung transplant recipients T G WREGHITT,* M HAKIM,* J J GRAY,* A H BALFOUR,t P G I STOVIN,4 SUSAN STEWART,: J SCOTT, T A H ENGLISH,II
Coccidia. Eucoccidioside
 Coccidia Kingdom Sub-Kingdom Phylum Class Order Family Genus Species Protista Protozoa Apicomplexa Sporozoasida Eucoccidioside Sarcocystidae Toxoplasma gondii 1 Toxoplasma gondii (life cycle) Sexual cycle
Coccidia Kingdom Sub-Kingdom Phylum Class Order Family Genus Species Protista Protozoa Apicomplexa Sporozoasida Eucoccidioside Sarcocystidae Toxoplasma gondii 1 Toxoplasma gondii (life cycle) Sexual cycle
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Severe Pulmonary Toxoplasmosis Mimicking Viral Pneumonitis after a Third Allogeneic Stem Cell Transplantation in a Man with Acute Lymphoblastic Leukemia Masahiko Sumi 1, Satoru Hata 2, Keijiro
CASE REPORT Severe Pulmonary Toxoplasmosis Mimicking Viral Pneumonitis after a Third Allogeneic Stem Cell Transplantation in a Man with Acute Lymphoblastic Leukemia Masahiko Sumi 1, Satoru Hata 2, Keijiro
Utility of Immunoblotting for Early Diagnosis of Toxoplasmosis Seroconversion in Pregnant Women
 CLINICAL AND VACCINE IMMUNOLOGY, Nov. 2011, p. 1908 1912 Vol. 18, No. 11 1556-6811/11/$12.00 doi:10.1128/cvi.05303-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Utility of
CLINICAL AND VACCINE IMMUNOLOGY, Nov. 2011, p. 1908 1912 Vol. 18, No. 11 1556-6811/11/$12.00 doi:10.1128/cvi.05303-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. Utility of
Toxoplasma gondii. Definitive Host adult forms sexual reproduction. Intermediate Host immature forms asexual reproduction
 Toxoplasma gondii cosmopolitan distribution seropositive prevalence rates vary generally 20-75% generally causes very benign disease in immunocompetent adults tissue cyst forming coccidia predator-prey
Toxoplasma gondii cosmopolitan distribution seropositive prevalence rates vary generally 20-75% generally causes very benign disease in immunocompetent adults tissue cyst forming coccidia predator-prey
TELEFAX. Toxoplasma Serology Laboratory (TSL) DATE: TO: FAX: FROM:
 TELEFAX DATE: TO: FAX: FROM: Toxoplasma Serology Laboratory RE: SPECIMEN REQUIREMENTS AND TESTING INFORMATION (effective 1/15/16) THIS TRANSMISSION CONSISTS OF 16 PAGES INCLUDING THIS COVER PAGE. IF THERE
TELEFAX DATE: TO: FAX: FROM: Toxoplasma Serology Laboratory RE: SPECIMEN REQUIREMENTS AND TESTING INFORMATION (effective 1/15/16) THIS TRANSMISSION CONSISTS OF 16 PAGES INCLUDING THIS COVER PAGE. IF THERE
Pneumocystis. Pneumocystis BIOL Summer Introduction. Mycology. Introduction (cont.) Introduction (cont.)
 Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Toxoplasma gondii. Jarmila Kliescikova, MD 1. LF UK
 Toxoplasma gondii Jarmila Kliescikova, MD 1. LF UK Toxoplasma gondii Apicomplexa, Koccidia Obligate intracellular parasite Distribution: cosmopolite Transmission: alimentary transplacentary (transfusions,
Toxoplasma gondii Jarmila Kliescikova, MD 1. LF UK Toxoplasma gondii Apicomplexa, Koccidia Obligate intracellular parasite Distribution: cosmopolite Transmission: alimentary transplacentary (transfusions,
PUO in the Immunocompromised Host: CMV and beyond
 PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
Human toxoplasmosis in Europe. Parasitology, Paris Descartes University, Cochin Hospital, Paris, France
 Human toxoplasmosis in Europe Prof Jean Dupouy-Camet Parasitology, Paris Descartes University, Cochin Hospital, Paris, France Toxoplasma gondii, discovered in 1908, by Nicolle at Institut Pasteur de Tunis,
Human toxoplasmosis in Europe Prof Jean Dupouy-Camet Parasitology, Paris Descartes University, Cochin Hospital, Paris, France Toxoplasma gondii, discovered in 1908, by Nicolle at Institut Pasteur de Tunis,
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
This article was downloaded by: Publisher: KKG Publications Registered office: 18, Jalan Kenanga SD 9/7 Bandar Sri Damansara, Malaysia
 This article was downloaded by: Publisher: KKG Publications Registered office: 18, Jalan Kenanga SD 9/7 Bandar Sri Damansara, 52200 Malaysia Key Knowledge Generation Publication details, including instructions
This article was downloaded by: Publisher: KKG Publications Registered office: 18, Jalan Kenanga SD 9/7 Bandar Sri Damansara, 52200 Malaysia Key Knowledge Generation Publication details, including instructions
A 39 years old HIV-positive black African woman with previously treated cerebral
 1 Abstract A 39 years old HIV-positive black African woman with previously treated cerebral toxoplasmosis experienced a foetal intra-uterine death due to congenital toxoplasmosis. This case demonstrates
1 Abstract A 39 years old HIV-positive black African woman with previously treated cerebral toxoplasmosis experienced a foetal intra-uterine death due to congenital toxoplasmosis. This case demonstrates
Significance of a positive Toxoplasma Immunoglobulin M test result. in the United States
 JCM Accepted Manuscript Posted Online 9 September 2015 J. Clin. Microbiol. doi:10.1128/jcm.01663-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Significance of a positive
JCM Accepted Manuscript Posted Online 9 September 2015 J. Clin. Microbiol. doi:10.1128/jcm.01663-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 Significance of a positive
PCR Detection of Toxoplasma gondii DNA in Blood and Ocular Samples for the
 JCM Accepts, published online ahead of print on 10 September 2014 J. Clin. Microbiol. doi:10.1128/jcm.01793-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 PCR Detection
JCM Accepts, published online ahead of print on 10 September 2014 J. Clin. Microbiol. doi:10.1128/jcm.01793-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 PCR Detection
EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS
 EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS DR LOW CHIAN YONG MBBS, MRCP(UK), MMed(Int Med), FAMS Consultant, Dept of Infectious Diseases, SGH Introduction The incidence of invasive fungal
EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS DR LOW CHIAN YONG MBBS, MRCP(UK), MMed(Int Med), FAMS Consultant, Dept of Infectious Diseases, SGH Introduction The incidence of invasive fungal
Opportunistic infections
 Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Opportunistic infections Opportunistic infections Decrease in number of CD4 lymphocytes is condition for development of opportunistic infections Risk is started, when number of CD4 lymphocytes drops to
Ocular Toxoplasmosis - A Laboratory View. Chatterton JMW* Evans R. Ho-Yen DO
 Ocular Toxoplasmosis - A Laboratory View Chatterton JMW* Evans R Ho-Yen DO Scottish Toxoplasma Reference Laboratory Microbiology Department Raigmore Hospital Inverness IV UJ * corresponding author Introduction
Ocular Toxoplasmosis - A Laboratory View Chatterton JMW* Evans R Ho-Yen DO Scottish Toxoplasma Reference Laboratory Microbiology Department Raigmore Hospital Inverness IV UJ * corresponding author Introduction
Tijana Štajner, 1 Zorica Vasiljević, 2 Dragana Vujić, 2,3 Marija Marković, 1 Goran Ristić, 2
 JCM Accepts, published online ahead of print on 12 June 2013 J. Clin. Microbiol. doi:10.1128/jcm.01077-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 ORIGINAL ARTICLE 2 3
JCM Accepts, published online ahead of print on 12 June 2013 J. Clin. Microbiol. doi:10.1128/jcm.01077-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 ORIGINAL ARTICLE 2 3
Received 8 April 1996/Returned for modification 19 June 1996/Accepted 15 July 1996
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1996, p. 2526 2530 Vol. 34, No. 10 0095-1137/96/$04.00 0 Copyright 1996, American Society for Microbiology Study of Abbott Toxo IMx System for Detection of Immunoglobulin
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1996, p. 2526 2530 Vol. 34, No. 10 0095-1137/96/$04.00 0 Copyright 1996, American Society for Microbiology Study of Abbott Toxo IMx System for Detection of Immunoglobulin
Comparison of immunoblotting, Goldmann-Witmer coefficient and real-time. PCR on aqueous humor for diagnosis of ocular toxoplasmosis.
 JCM Accepts, published online ahead of print on 9 April 2008 J. Clin. Microbiol. doi:10.1128/jcm.01900-07 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 9 April 2008 J. Clin. Microbiol. doi:10.1128/jcm.01900-07 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Toxoplasma Seroconversion with Negative or Transient Immunoglobulin M in Women: Myth or Reality? A French Pregnant Multicenter Retrospective Study
 REFERENCES CONTENT ALERTS Toxoplasma Seroconversion with Negative or Transient Immunoglobulin M in Women: Myth or Reality? A French Pregnant Multicenter Retrospective Study H. Fricker-Hidalgo, B. Cimon,
REFERENCES CONTENT ALERTS Toxoplasma Seroconversion with Negative or Transient Immunoglobulin M in Women: Myth or Reality? A French Pregnant Multicenter Retrospective Study H. Fricker-Hidalgo, B. Cimon,
Diagnosis of CMV infection UPDATE ECIL
 UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
Toxoplasmosis Objective :
 Toxoplasmosis Objective : Describe the Life cycle Mention the Infective stages Define Congenital Toxoplasmosis List the Lab.Diagnosis Illustrate the Immunity to Toxoplasmosis Show the relationship between
Toxoplasmosis Objective : Describe the Life cycle Mention the Infective stages Define Congenital Toxoplasmosis List the Lab.Diagnosis Illustrate the Immunity to Toxoplasmosis Show the relationship between
BK Virus (BKV) Management Guideline: July 2017
 BK Virus (BKV) Management Guideline: July 2017 BK virus has up to a 60-80% seroprevalence rate in adults due to a primary oral or respiratory exposure in childhood. In the immumocompromised renal transplant
BK Virus (BKV) Management Guideline: July 2017 BK virus has up to a 60-80% seroprevalence rate in adults due to a primary oral or respiratory exposure in childhood. In the immumocompromised renal transplant
Indirect Enzyme-Linked Immunosorbent Assay for Immunoglobulin G and Four Immunoassays for Immunoglobulin M
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1989, p. 529-535 0095-1137/89/030529-07$02.00/0 Copyright 1989, American Society for Microbiology Vol. 27, No. 3 Indirect Enzyme-Linked Immunosorbent Assay for Immunoglobulin
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 1989, p. 529-535 0095-1137/89/030529-07$02.00/0 Copyright 1989, American Society for Microbiology Vol. 27, No. 3 Indirect Enzyme-Linked Immunosorbent Assay for Immunoglobulin
Toxoplasmosis Seroepidemiology in Serum of Suspected Patients Attending Medical Lab, in 2013
 Journal of Community Health Research. 2015;4(1):47-54. Original Article Toxoplasmosis Seroepidemiology in Serum of Suspected Patients Attending Medical Lab, in 2013 Ali Fattahi Bafghi 1, Roya Anvari 2,
Journal of Community Health Research. 2015;4(1):47-54. Original Article Toxoplasmosis Seroepidemiology in Serum of Suspected Patients Attending Medical Lab, in 2013 Ali Fattahi Bafghi 1, Roya Anvari 2,
Toxoplasmosis. Life cycle Infective stages Congenital Toxoplasmosis Lab.Diagnosis Immunity to Toxoplasmosis Toxoplasmosis & Pregnancy
 Toxoplasmosis Life cycle Infective stages Congenital Toxoplasmosis Lab.Diagnosis Immunity to Toxoplasmosis Toxoplasmosis & Pregnancy Human Toxoplasmosis Toxoplasmosis is a zoonotic disease Caused by Coccidian
Toxoplasmosis Life cycle Infective stages Congenital Toxoplasmosis Lab.Diagnosis Immunity to Toxoplasmosis Toxoplasmosis & Pregnancy Human Toxoplasmosis Toxoplasmosis is a zoonotic disease Caused by Coccidian
PREDICTIVE VALUE OF LATEX AGGLUTINATION TEST IN SEROLOGICAL SCREENING FOR TOXOPLASMA GONDII
 PREDICTIVE VALUE OF LATEX AGGLUTINATION TEST IN SEROLOGICAL SCREENING FOR TOXOPLASMA GONDII Yaowalark Sukthana, Thaiyooth Chintana, Waraporn Supatanapong, Chutatip Siripan, Amorn Lekkla and Rachatawan
PREDICTIVE VALUE OF LATEX AGGLUTINATION TEST IN SEROLOGICAL SCREENING FOR TOXOPLASMA GONDII Yaowalark Sukthana, Thaiyooth Chintana, Waraporn Supatanapong, Chutatip Siripan, Amorn Lekkla and Rachatawan
Comparison of the efficiency of two commercial kits ELFA and Western blot in estimating the phase of Toxoplasma gondii infection in pregnant women
 Annals of Agricultural and Environmental Medicine 2016, Vol 23, No 4, 570 575 www.aaem.pl ORIGINAL ARTICLE Comparison of the efficiency of two commercial kits ELFA and Western blot in estimating the phase
Annals of Agricultural and Environmental Medicine 2016, Vol 23, No 4, 570 575 www.aaem.pl ORIGINAL ARTICLE Comparison of the efficiency of two commercial kits ELFA and Western blot in estimating the phase
Synergistic Activity of Azithromycin and Pyrimethamine or
 ANTMCROBAL AGNTS AND CHMOTHRAPY, May 199, p. 997-11 66-44/9/5997-5$./ Copyright 199, American Society for Microbiology Vol. 36, No. 5 Synergistic Activity of Azithromycin and Pyrimethamine or Sulfadiazine
ANTMCROBAL AGNTS AND CHMOTHRAPY, May 199, p. 997-11 66-44/9/5997-5$./ Copyright 199, American Society for Microbiology Vol. 36, No. 5 Synergistic Activity of Azithromycin and Pyrimethamine or Sulfadiazine
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 2, March 2014
 PRELIMINARY EVALUATION OF CHORUS SYSTEM IN COMPARISON WITH COBAS 6000 SYSTEM FOR DETECTION OF ANTI-TOXOPLASMA-IGM ANTIBODIES BLERTA LAZE* ANILA MITRE** *Dept. of Biology, University Ismail Qemali, Vlora,
PRELIMINARY EVALUATION OF CHORUS SYSTEM IN COMPARISON WITH COBAS 6000 SYSTEM FOR DETECTION OF ANTI-TOXOPLASMA-IGM ANTIBODIES BLERTA LAZE* ANILA MITRE** *Dept. of Biology, University Ismail Qemali, Vlora,
Evaluation of the Immunoglobulin G Avidity Test for Diagnosis of Toxoplasmic Lymphadenopathy
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2004, p. 4627 4631 Vol. 42, No. 10 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.10.4627 4631.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 2004, p. 4627 4631 Vol. 42, No. 10 0095-1137/04/$08.00 0 DOI: 10.1128/JCM.42.10.4627 4631.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
Toxoplasma seroconversion with negative or transient immunoglobulin M in. pregnant women: myth or reality? A French multicentre retrospective study.
 JCM Accepts, published online ahead of print on 24 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.00169-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Toxoplasma seroconversion
JCM Accepts, published online ahead of print on 24 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.00169-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 2 Toxoplasma seroconversion
Evaluation of a new ICT test (LDBIO Diagnostics) to detect toxoplasma IgG. and IgM: comparison with the routine Architect technique.
 JCM Accepted Manuscript Posted Online 27 September 2017 J. Clin. Microbiol. doi:10.1128/jcm.01106-17 Copyright 2017 American Society for Microbiology. All Rights Reserved. 1 2 Evaluation of a new ICT test
JCM Accepted Manuscript Posted Online 27 September 2017 J. Clin. Microbiol. doi:10.1128/jcm.01106-17 Copyright 2017 American Society for Microbiology. All Rights Reserved. 1 2 Evaluation of a new ICT test
Molecular diagnosis of toxoplasmosis in immunocompromised patients
 REVIEW C URRENT OPINION Molecular diagnosis of toxoplasmosis in immunocompromised patients Florence Robert-Gangneux a,b and Sorya Belaz a,b Purpose of review Toxoplasmosis in immunocompromised patients
REVIEW C URRENT OPINION Molecular diagnosis of toxoplasmosis in immunocompromised patients Florence Robert-Gangneux a,b and Sorya Belaz a,b Purpose of review Toxoplasmosis in immunocompromised patients
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Lung Abscess due to Clostridium barati in a Patient with Invasive Pulmonary Aspergillosis ACCEPTED
 JCM Accepts, published online ahead of print on 3 January 2008 J. Clin. Microbiol. doi:10.1128/jcm.02446-07 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 3 January 2008 J. Clin. Microbiol. doi:10.1128/jcm.02446-07 Copyright 2008, American Society for Microbiology and/or the Listed Authors/Institutions. All
GUIDELINE FOR THE MANAGEMENT OF TOXOPLASMOSIS ENCEPHALITIS
 GUIDELINE FOR THE MANAGEMENT OF TOXOPLASMOSIS ENCEPHALITIS Full title of guideline Guideline for the management of toxoplasmosis encephalitis Author Dr P Venkatesan (ID consultant) Division and specialty
GUIDELINE FOR THE MANAGEMENT OF TOXOPLASMOSIS ENCEPHALITIS Full title of guideline Guideline for the management of toxoplasmosis encephalitis Author Dr P Venkatesan (ID consultant) Division and specialty
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia)
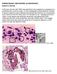 PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
Clinical Policy: Pyrimethamine (Daraprim) Reference Number: ERX.NPA.44 Effective Date:
 Clinical Policy: (Daraprim) Reference Number: ERX.NPA.44 Effective Date: 12.01.15 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Daraprim) Reference Number: ERX.NPA.44 Effective Date: 12.01.15 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical significance of quantifying Pneumocystis jirovecii DNA using real-time. PCR in bronchoalveolar lavage fluid from immunocompromised patients
 JCM Accepts, published online ahead of print on 7 December 2011 J. Clin. Microbiol. doi:10.1128/jcm.06036-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 7 December 2011 J. Clin. Microbiol. doi:10.1128/jcm.06036-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All
Recommendations for VZV management in. Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman
 Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Michael Grimley 1, Vinod Prasad 2, Joanne Kurtzberg 2, Roy Chemaly 3, Thomas Brundage 4, Chad Wilson 4, Herve Mommeja-Marin 4
 Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
Short Video. shows/monsters-inside- me/videos/toxoplasma-parasite/
 The word Toxoplasma Originated from the Greek word toxon, which meant "bow." The Latin word toxicum, which meant "poison." The original Greek meaning is the one used for the word Toxoplasma, meaning "bow
The word Toxoplasma Originated from the Greek word toxon, which meant "bow." The Latin word toxicum, which meant "poison." The original Greek meaning is the one used for the word Toxoplasma, meaning "bow
International Conference on Parasitology August 24-26, 2015 Philadelphia, Pennsylvania, USA
 International Conference on Parasitology August 24-26, 2015 Philadelphia, Pennsylvania, USA SYMPOSIA THE CHALLENGE OF PARASITES AND IMMUNOSUPRESSION: FROM DIAGNOSIS TO TREATMENT from the bench to the bed
International Conference on Parasitology August 24-26, 2015 Philadelphia, Pennsylvania, USA SYMPOSIA THE CHALLENGE OF PARASITES AND IMMUNOSUPRESSION: FROM DIAGNOSIS TO TREATMENT from the bench to the bed
toxoplasmosis Laboratory techniques in the investigation of immunocompromised. Cancer patients, (PCR). Clinical and radiological findings
 Genitourin Med 1992;68:55-59 Public Health Laboratory Service, Toxoplasma Reference Laboratory, St George's Hospital, Blackshaw Road, London, SW17 OQT, UK K F Barker R E Holliman Address correspondence
Genitourin Med 1992;68:55-59 Public Health Laboratory Service, Toxoplasma Reference Laboratory, St George's Hospital, Blackshaw Road, London, SW17 OQT, UK K F Barker R E Holliman Address correspondence
INTERNATIONAL SOCIETY FOR HEART AND LUNG TRANSPLANTATION a Society that includes Basic Science, the Failing Heart, and Advanced Lung Disease
 International Society of Heart and Lung Transplantation Advisory Statement on the Implications of Pandemic Influenza for Thoracic Organ Transplantation This advisory statement has been produced by the
International Society of Heart and Lung Transplantation Advisory Statement on the Implications of Pandemic Influenza for Thoracic Organ Transplantation This advisory statement has been produced by the
Guillain-Barré Syndrome
 Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016
 Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016 Case report 20 months old girl Israeli Arab Muslim family, consanguineous marriage
Let`s go for the diagnosis! Yazeed Toukan, MD Pediatric Pulmonary Institute, Ruth Rappaport Children`s Hospital July 2016 Case report 20 months old girl Israeli Arab Muslim family, consanguineous marriage
Clinical syndromes: experience from the bedside. Professor Rob Miller University College Hospital, London
 Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
2046: Fungal Infection Pre-Infusion Data
 2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients
 DOI 10.1007/s10096-013-1960-3 ARTICLE Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients M. Maillet & D. Maubon & J. P. Brion
DOI 10.1007/s10096-013-1960-3 ARTICLE Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients M. Maillet & D. Maubon & J. P. Brion
CONTRIBUTIONS OF IMMUNOBLOTTING, REAL-TIME PCR AND THE GOLDMANN-WITMER COEFFICIENT TO THE DIAGNOSIS OF ATYPICAL
 JCM Accepts, published online ahead of print on 13 May 2009 J. Clin. Microbiol. doi:10.1128/jcm.00128-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 13 May 2009 J. Clin. Microbiol. doi:10.1128/jcm.00128-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Modification and Evaluation of Avidity IgG Testing for Differentiating of Toxoplasma gondii Infection in Early Stage of Pregnancy
 Original Article Modification and Evaluation of Avidity IgG Testing for Differentiating of Toxoplasma gondii Infection in Early Stage of Pregnancy Mohammad Reza Bonyadi, M.D. 1 *, Parvin Bastani, M.D.
Original Article Modification and Evaluation of Avidity IgG Testing for Differentiating of Toxoplasma gondii Infection in Early Stage of Pregnancy Mohammad Reza Bonyadi, M.D. 1 *, Parvin Bastani, M.D.
Laboratory Diagnosis of Toxoplasma gondii Infection and Toxoplasmosis
 S73 Laboratory Diagnosis of Toxoplasma gondii Infection and Toxoplasmosis Jose G. Montoya Department of Immunology and Infectious Diseases, Research Institute, Palo Alto Medical Foundation, Palo Alto,
S73 Laboratory Diagnosis of Toxoplasma gondii Infection and Toxoplasmosis Jose G. Montoya Department of Immunology and Infectious Diseases, Research Institute, Palo Alto Medical Foundation, Palo Alto,
Comparative evaluation of AxSYM, VIDAS and VIDIA toxoplasmosis reagent performance in a high seroprevalence Latin American country
 Artigo Original / Original Article Comparative evaluation of AxSYM, VIDAS and VIDIA toxoplasmosis reagent performance in a high seroprevalence Latin American country Avaliação comparativa entre o desempenho
Artigo Original / Original Article Comparative evaluation of AxSYM, VIDAS and VIDIA toxoplasmosis reagent performance in a high seroprevalence Latin American country Avaliação comparativa entre o desempenho
Toxoplasmosis in immunocompetent and immunocompromised population of Constanta, Romania
 3rd International Conference on Clinical Microbiology & Microbial Genomics September 24-26, 2014 Valencia, Spain Toxoplasmosis in immunocompetent and immunocompromised population of Constanta, Romania
3rd International Conference on Clinical Microbiology & Microbial Genomics September 24-26, 2014 Valencia, Spain Toxoplasmosis in immunocompetent and immunocompromised population of Constanta, Romania
valganciclovir, 450mg tablets, 50mg/ml powder for oral solution (Valcyte ) SMC No. (662/10) Roche Products Ltd
 valganciclovir, 450mg tablets, 50mg/ml powder for oral solution (Valcyte ) SMC No. (662/10) Roche Products Ltd 17 December 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the
valganciclovir, 450mg tablets, 50mg/ml powder for oral solution (Valcyte ) SMC No. (662/10) Roche Products Ltd 17 December 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of the
WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS?
 WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS? Assoc. Prof. Dr. Serkan SENER Acibadem University Medical School Department of Emergency Medicine, Istanbul Acibadem Ankara Hospital,
WHICH ANTIFUNGAL AGENT IS THE CHOICE FOR SUSPECTED FUNGAL INFECTIONS? Assoc. Prof. Dr. Serkan SENER Acibadem University Medical School Department of Emergency Medicine, Istanbul Acibadem Ankara Hospital,
Extra-intestinal coccidians
 Extra-intestinal coccidians Apicomplexa Coccidia Gregarinea Piroplasmida Eimeriida Haemosporida -Theileriidae - Babesiidae - Eimeriidae - Cryptosporidiidae - Sarcocystidae (Sarcocystis) (Toxoplasma) -Haemosporiidae
Extra-intestinal coccidians Apicomplexa Coccidia Gregarinea Piroplasmida Eimeriida Haemosporida -Theileriidae - Babesiidae - Eimeriidae - Cryptosporidiidae - Sarcocystidae (Sarcocystis) (Toxoplasma) -Haemosporiidae
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals. Taniawati Supali. Department of Parasitology
 Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
Only one take home point for the talk 9/26/2018. Infectious Diseases and Donor Derived Infections. Don t forget about donor-derived infections
 Shane Colombo 1993 2018 Infectious Diseases and Donor Derived Infections Peter Chin-Hong, MD Division of Infectious Diseases UCSF Only one take home point for the talk Don t forget about donor-derived
Shane Colombo 1993 2018 Infectious Diseases and Donor Derived Infections Peter Chin-Hong, MD Division of Infectious Diseases UCSF Only one take home point for the talk Don t forget about donor-derived
The rise of Tropheryma whipplei: a 12- year retrospective study of PCR diagnoses in our. reference center
 JCM Accepts, published online ahead of print on 26 September 2012 J. Clin. Microbiol. doi:10.1128/jcm.01517-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 The rise of Tropheryma
JCM Accepts, published online ahead of print on 26 September 2012 J. Clin. Microbiol. doi:10.1128/jcm.01517-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 The rise of Tropheryma
Identification of Microbes Lecture: 12
 Diagnostic Microbiology Identification of Microbes Lecture: 12 Electron Microscopy 106 virus particles per ml required for visualization, 50,000-60,000 magnification normally used. Viruses may be detected
Diagnostic Microbiology Identification of Microbes Lecture: 12 Electron Microscopy 106 virus particles per ml required for visualization, 50,000-60,000 magnification normally used. Viruses may be detected
Protozoan Infections of the Circulatory System *
 OpenStax-CNX module: m64867 1 Protozoan Infections of the Circulatory System * Geo Lin-Cereghino Based on Parasitic Infections of the Circulatory and Lymphatic Systems by OpenStax This work is produced
OpenStax-CNX module: m64867 1 Protozoan Infections of the Circulatory System * Geo Lin-Cereghino Based on Parasitic Infections of the Circulatory and Lymphatic Systems by OpenStax This work is produced
VIDAS Test for Avidity of Toxoplasma-Specific Immunoglobulin G for Confirmatory Testing of Pregnant Women
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2002, p. 2504 2508 Vol. 40, No. 7 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.7.2504 2508.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, July 2002, p. 2504 2508 Vol. 40, No. 7 0095-1137/02/$04.00 0 DOI: 10.1128/JCM.40.7.2504 2508.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved.
Development of Specific Immunoglobulins G, M, and A Following Primary Toxoplasma gondii Infection in Pregnant Women
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1998, p. 2907 2913 Vol. 36, No. 10 0095-1137/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Development of Specific Immunoglobulins
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1998, p. 2907 2913 Vol. 36, No. 10 0095-1137/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Development of Specific Immunoglobulins
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association
 Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Daraprim) Reference Number: CP.PMN.44 Effective Date: 11.01.15 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Clinical Policy: (Daraprim) Reference Number: CP.PMN.44 Effective Date: 11.01.15 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Nephrology Grand Rounds
 Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
Relationship between pre-existing anti-varicella zoster virus ACCEPTED. (VZV) antibody and clinical VZV reactivation in hematopoietic
 JCM Accepts, published online ahead of print on 11 October 2006 J. Clin. Microbiol. doi:10.1128/jcm.01312-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 11 October 2006 J. Clin. Microbiol. doi:10.1128/jcm.01312-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions. All
GAFFI Fact Sheet. Disseminated histoplasmosis
 F GAFFI Fact Sheet Disseminated histoplasmosis ION NS ACT ALOR ECTIO B O F F L G ND L IN FU NGA FU Disseminated histoplasmosis is a sub- acute infection that may be diagnosed in patients with impaired
F GAFFI Fact Sheet Disseminated histoplasmosis ION NS ACT ALOR ECTIO B O F F L G ND L IN FU NGA FU Disseminated histoplasmosis is a sub- acute infection that may be diagnosed in patients with impaired
Twice-Weekly Maintenance Therapy with Sulfadiazine-Pyrimethamine To Prevent Recurrent Toxoplasmic Encephalitis in Patients with AIDS
 Twice-Weekly Maintenance Therapy with Sulfadiazine-Pyrimethamine To Prevent Recurrent Toxoplasmic Encephalitis in Patients with AIDS Daniel Podzamczer, MD; Jose M. Miro, MD; Ferran Bolao, MD; Jose M. Gatell,
Twice-Weekly Maintenance Therapy with Sulfadiazine-Pyrimethamine To Prevent Recurrent Toxoplasmic Encephalitis in Patients with AIDS Daniel Podzamczer, MD; Jose M. Miro, MD; Ferran Bolao, MD; Jose M. Gatell,
Infectious Complications among 620 Consecutive Heart Transplant Patients at Stanford University Medical Center
 REVIEW ARTICLE Infectious Complications among 620 Consecutive Heart Transplant Patients at Stanford University Medical Center Jose G. Montoya, 1,2 Luis F. Giraldo, 1,2 Bradley Efron, 5 Edward B. Stinson,
REVIEW ARTICLE Infectious Complications among 620 Consecutive Heart Transplant Patients at Stanford University Medical Center Jose G. Montoya, 1,2 Luis F. Giraldo, 1,2 Bradley Efron, 5 Edward B. Stinson,
Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant
 SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
Immunodeficiencies HIV/AIDS
 Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immunocompromised Patients with Cerebral and Extracerebral Toxoplasmosis
 JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 1994, p. 2813-2819 0095-1137/94/$04.00+0 Copyright C) 1994, American Society for Microbiology Vol. 32, No. 11 Value of PCR for Evaluating Occurrence of Parasitemia
JOURNAL OF CLINICAL MICROBIOLOGY, Nov. 1994, p. 2813-2819 0095-1137/94/$04.00+0 Copyright C) 1994, American Society for Microbiology Vol. 32, No. 11 Value of PCR for Evaluating Occurrence of Parasitemia
Bicentric Evaluation of Six Anti-Toxoplasma Immunoglobin G automated. immunoassays and comparison with the LDBio-Toxo II Immunoglobulin G
 CVI Accepts, published online ahead of print on July 00 Clin. Vaccine Immunol. doi:./cvi.001-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
CVI Accepts, published online ahead of print on July 00 Clin. Vaccine Immunol. doi:./cvi.001-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Cytomegalovirus in critically ill patients
 ! Cytomegalovirus in critically ill patients Frédéric Pène Medical ICU, Hôpital Cochin, AP-HP, Paris, France Université Paris Descartes, Sorbonne Paris Cité Institut Cochin, Inserm U1016, CNRS UMR-8104
! Cytomegalovirus in critically ill patients Frédéric Pène Medical ICU, Hôpital Cochin, AP-HP, Paris, France Université Paris Descartes, Sorbonne Paris Cité Institut Cochin, Inserm U1016, CNRS UMR-8104
Toxoplasmosis. Seminar. For personal use. Only reproduce with permission from The Lancet Publishing Group.
 Seminar Toxoplasmosis J G Montoya, O Liesenfeld Toxoplasma gondii is a protozoan parasite that infects up to a third of the world s population. Infection is mainly acquired by ingestion of food or water
Seminar Toxoplasmosis J G Montoya, O Liesenfeld Toxoplasma gondii is a protozoan parasite that infects up to a third of the world s population. Infection is mainly acquired by ingestion of food or water
EBV in HSCT 2015 update of ECIL guidelines
 ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia
 Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Blood stream candidiasis. R. Demeester, D. Famerée, B. Guillaume, JC. Legrand CHU Charleroi SBIMC 8th of November 2012
 Blood stream candidiasis R. Demeester, D. Famerée, B. Guillaume, JC. Legrand CHU Charleroi SBIMC 8th of November 2012 62-year-old man: clinical history Fever for 10 days with peaks above 39 C, cough, orthopnea
Blood stream candidiasis R. Demeester, D. Famerée, B. Guillaume, JC. Legrand CHU Charleroi SBIMC 8th of November 2012 62-year-old man: clinical history Fever for 10 days with peaks above 39 C, cough, orthopnea
Chapter 22: Hematological Complications
 Chapter 22: Hematological Complications 22.1: Perform a complete blood count at least (Not Graded): daily for 7 days, or until hospital discharge, whichever is earlier; two to three times per week for
Chapter 22: Hematological Complications 22.1: Perform a complete blood count at least (Not Graded): daily for 7 days, or until hospital discharge, whichever is earlier; two to three times per week for
ESCMID Online Lecture Library. by author. CASE PRESENTATION ECCMID clinical grand round May Anat Stern, MD Rambam medical center Haifa, Israel
 CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
ABO-incompatible kidney transplantation in elderly patients over 60 years of age
 Int Urol Nephrol (2012) 44:1563 1570 DOI 10.1007/s11255-012-0231-z NEPHROLOGY - ORIGINAL PAPER ABO-incompatible kidney transplantation in elderly patients over 60 years of age Junji Uchida Tomoaki Iwai
Int Urol Nephrol (2012) 44:1563 1570 DOI 10.1007/s11255-012-0231-z NEPHROLOGY - ORIGINAL PAPER ABO-incompatible kidney transplantation in elderly patients over 60 years of age Junji Uchida Tomoaki Iwai
Area Laboratory Service
 THIS IS A CONTROLLED DOCUMENT. DO NOT COPY Organisational Unit: Title: Ref No: Version No: Date Issued: Author: Authorised by: Review date: Area Laboratory Service Microbiology Scottish Toxoplasma Reference
THIS IS A CONTROLLED DOCUMENT. DO NOT COPY Organisational Unit: Title: Ref No: Version No: Date Issued: Author: Authorised by: Review date: Area Laboratory Service Microbiology Scottish Toxoplasma Reference
Disseminated invasive aspergillosis following cytomegalovirus encephalitis in a renal transplant recipient
 CASE REPORT Port J Nephrol Hypert 2008; 22(1): 55-59 Disseminated invasive aspergillosis following cytomegalovirus encephalitis in a renal transplant recipient Patrícia Matias 1, Cristina Jorge 1, Sância
CASE REPORT Port J Nephrol Hypert 2008; 22(1): 55-59 Disseminated invasive aspergillosis following cytomegalovirus encephalitis in a renal transplant recipient Patrícia Matias 1, Cristina Jorge 1, Sância
