Platelet activating factor in allergies
|
|
|
- Eugenia Gibbs
- 6 years ago
- Views:
Transcription
1 600598IJI / International Journal of Immunopathology and PharmacologyPałgan and Bartuzi research-article2015 Letter to the editor Platelet activating factor in allergies Krzysztof Pałgan and Zbigniew Bartuzi International Journal of Immunopathology and Pharmacology 2015, Vol. 28(4) The Author(s) 2015 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: / iji.sagepub.com Abstract The platelet-activating factor (PAF) produced and released by mast cells, basophils, neutrophils, eosinophils, fibroblasts, platelets, endothelial cells, and even cardiac muscle cells plays an important role in inflammatory and thrombotic diseases. PAF has been shown to be an important mediator in anaphylaxis. Serum level of the factor correlates with the severity of systemic reactions. PAF is also involved in asthamatic patients bronchoconstriction, mucus hypersecretion, and inflammation of bronchi. Furthermore, increased plasma levels of PAF have been reported in patients with urticarial. Studies have shown that PAF increases the permeability of skin s capillaries and indices the development of wheals, flare, and inflammatory reactions in the skin. This review focuses on the actions of the PAF on the eosinophiles and mast cells. Following that pathophysiological mechanism of the PAF in anaphylaxis bronchial asthma and urticaria was discussed. Keywords anaphylaxis, bronchial asthma, platelet-activating factor, urticaria Date received: 9 February 2015; accepted: 22 July 2015 Introduction Platelet-activating factor (1-O-alkyl-2-acetyl-snglycero-3-phosphocholine) also known as PAF, was discovered by the French immunologist Jacques Benveniste ( ). In 1972, Benveniste demonstrated that this factor was released from basophils. 1 Further reports have shown that PAF is produced and released by other cells such as neutrophils, eosinophils, fibroblasts, platelets, endothelial cells, and even cardiac muscle cells. 2 Phospholipase A 2 and acetyltransferase are required for the production of PAF in the most common pathway and an acetylhydrolase specific for PAF (PAF acetylhydrolase [PAF-AH]) is responsible for its degradation. The PAF elimination time is short, because its half-life is 3 13 min. 3 It is interesting that most of the cells producing PAF also have receptors for it (PAFR). PAF is a phospholipid which is involved in the regulation of a variety of cells, principally in the immune and nervous systems. The importance of PAF is emphasized in inflammation and coagulation. 4,5 This factor increases inflammation through chemotaxis, stimulation of degranulation, and release of oxygen radicals from leukocytes. Furthermore, it promotes the adhesion of inflammatory cells to the vascular endothelium, which in turn also undergoes increased permeability under the influence of PAF. The group of agents stimulating the release of PAF from the vascular endothelium is particularly large. It has been demonstrated that thrombin, angiotensin II, vasopressin, leukotrienes (LTs), plasmin, interleukin-8 (IL-8), and tumor necrosis factor (TNF) can stimulate the release of this factor from endothelial cells. By contrast, PAF relaxes arterial smooth muscle, as opposed to the uterus The Department of Allergology, Clinical Immunology and Internal Diseases Collegium Medicum Bydgoszcz, Nicolaus Copernicus University in Toruń, Collegium Medicum of L. Rydygier in Bydgoszcz, Poland Corresponding author: Krzysztof Pałgan, Nicolaus Copernicus University, Collegium Medicum in Bydgoszcz, Department of Allergology, Clinical Immunology and Internal Diseases, Ujejskiego 75, Bydgoszcz, Poland. palgank@wp.pl
2 Pałgan and Bartuzi 585 Table 1. Biological properties of PAF. Characteristic Reference Source Mast cells, basophils, eosinophils, monocytes, fixed tissue 1, 2, 3 macrophages, neutrophils, endothelial cells, platelets Inactivation By platelet-activating factor acetylhydrolase (PAF-AH) to 3, 4, 17 lyso-paf Mean plasma level 23.8 pg/ml 16, Half-life of PAF 3 13 min 13, 14 Action Via binding to a specific receptor (PAFR) 5 Chemotaxin for neutrophils and eosinophils 10, 13 Bronchoconstrictor 26, 27, 30 Increases vascular permeability and edema 15 Reduction of coronary blood flow 6, 15 Depression of myocardial contractility 6, 15 Direct arrhythmogenic effect 6, 15 Recent literature indicates that PAF is an important element of allergic reactions, especially anaphylaxis. muscle in which it stimulates contractions. PAF has a pro-arrhythmic and negative inotropic effect on a heart muscle; moreover, it reduces blood flow through the coronary vessels (Table 1). 6 PAF and eosinophils Eosinophils play an important role in allergic diseases. They are activated by numerous cytokines. The factors that significantly regulate the differentiation and maturation of eosinophils include IL-3, IL-5, IL-33, and granulocyte macrophage-colony stimulating factor (GM-CSF). Eotaxin is a chemotactic factor for eosinophils. 7 In addition to these factors, it has been shown that PAF is not only produced by eosinophils, and at the same time it also multidirectionally modulates their function. In vitro studies have shown that PAF is a chemoattractant for eosinophils, and via β 2 integrin it increases their adhesion to vascular endothelium. PAF increases the production of leukotriene C4 (LTC 4 ), oxygen-derived radicals, and degranulation of eosinophils. 8 Very interesting observations by Kato et al. 9 have shown that PAF can activate eosinophils in two stages. Phase one fast activation of eosinophils is carried out by G proteins that, with the participation of phospholipase Cβ (PLCβ), lead to the rapid but short release of oxygen-derived free radicals, and the second phase, which also occurs with the participation of PAF, but eosinophils must be additionally stimulated by cell adhesion involving β 2 integrin. This phase is characterized by a slower but longer release of oxygen-derived radicals. 10 Dyer et al. 8 demonstrated in an animal model that PAF causes the release of factors such as IL-13, eotaxin-1, a protein blocking receptor for IL-1, basic fibroblast growth factor (bfgf), RANTES, IL-9 and platelet-derived growth factor (PDGF) from eosinophils. PAF and mast cells Mast cells, also known as mastocytes, play a key role in type I allergic reactions according to the Gell and Coombs classification. Anaphylactic reactions begin with the activation of these cells. Classic mast cell activation occurs via the FcεRI receptor to which a complex of IgE-allergen is attached. An alternative pathway of mast cell activation is IgE-independent, and may occur under the influence of complement components, chemokines, immune complexes, or factors released during the decomposition of various types of microorganisms. 11 Activated mast cells release a variety of factors involved in allergic inflammation, e.g. cytokines, and factors influencing blood vessels including histamine and enzymes. Mast cells not only produce PAF, but they can also be activated by it. In the case of mast cells located in the skin, exposure to PAF leads to degranulation of their granules via neuropeptides. 12 Kajiwara et al. 13 has demonstrated in vitro that PAF can directly activate mast cells derived from lung tissue through surface PAFRs. An interesting aspect of mast cells that have been highlighted by these studies is that the release of histamine from lung mast cells mastocytes is dependent on the concentration of PAF.
3 586 International Journal of Immunopathology and Pharmacology 28(4) The greater the concentration of this factor in the mast cell environment, the more enhanced is the release of histamine. Mastocytes located between muscle fibers, in the area of blood vessels and myocardial artery intima have been a subject of interest for approximately 20 years. It appears that PAF-activated myocardial mast cells locally release factors responsible for cardiac dysfunction and hypotension that occurs in severe anaphylactic reactions. 14 Anaphylactic reactions and PAF Anaphylaxis is a severe, immediate, life-threatening reaction that occurs in hypersensitive individuals, caused by exposure to a stimulus that is well tolerated by healthy individuals. Anaphylactic reactions are divided into allergic, non-allergic, and idiopathic. The allergic anaphylaxis is mediated by an immunologic mechanism and usually is IgE, IgG, and immunocomplex-component dependent. The non-allergic anaphylaxis is non-immunologic and IgE-independent caused by drugs, physical factors, exercise, and other factors. The cause of idiopathic anaphylaxis is unknown. 15 The main cells involved in the allergic anaphylaxis are mast cells and basophils, which release histamine, serotonin, proteolytic enzymes, cytokines, and lipid mediators such as prostaglandin D2 (PGD2), LTB 4, cysteinyl LTs, LTC 4, LTD 4, LTE 4, and PAF. PAF has recently attracted a large amount of attention and interest, as it is a very important element of pathogenic severe anaphylactic reactions. 16 Examining the concentration of serum PAF in individuals with anaphylaxis, Vadas et al. 17 has found that compared to the control group, it is significantly higher and positively correlated with the severity of anaphylactic reaction. It has been found that in healthy individuals, a serum concentration of PAF is approximately 23.8 pg/ml and in persons with severe anaphylaxis can reach 805 ± 595 pg/ml. Vadas et al. 17 has observed that serum PAF levels in patients with grade 1, 2, and 3 anaphylaxis were 2.5-, 5-, and 10-fold higher than in the control group, respectively. Observations of the activity of PAF-AH, an enzyme neutralizing PAF, are particularly interesting. Acetylhydrolase activity studies have revealed significantly lower activity of this enzyme in people with very severe anaphylaxis caused by eating peanuts. 18 Generally, it has been shown that people with low PAF-AH activity have been characterized by a higher concentration of serum PAF compared to people with normal acetylhydrolase activity. Studies on the biology of this enzyme are interesting. It has been demonstrated that 70% of serum PAF-AH is bound to low-density lipoprotein (LDL), while the remainder is bound to high-density lipoprotein (HDL), moreover it has been found that lowering LDL levels prolongs PAF half-life. Therapy with lovastatin or fenofibrates, in addition to lowering LDL, leads to a proportional reduction in the activity of PAF-AH and can increase the risk of anaphylaxis. 19,20 The significance of PAF in the development of anaphylactic reactions has been confirmed by animal experiments. Anaphylaxis could not be induced in rabbits, mice, and rats in which cellular receptors for PAF were blocked. 21 A comparison of the significance of diagnostic measurements of the concentrations of histamine, tryptase and PAF in anaphylactic reactions, has shown that the levels of serum PAF is the most useful as it correlates most accurately with the severity of the anaphylactic reaction. In the case of histamine, an increase in serum levels has been observed in 35% of patients with a moderate reaction and 61% with a severe reaction. Tryptase levels have correlated slightly better, the serum concentration of which has increased in 55% of patients with a grade 2 anaphylactic reaction and in 75% of patients with severe anaphylaxis. The serum concentration of PAF has been shown to be higher in 100% of patients with severe anaphylaxis. 22 According to the experts guidelines, epinephrine administered intramuscularly is the first-line treatment for anaphylaxis. It is recommended that administration of this drug should occur as soon as possible during the development of anaphylaxis with cardiovascular symptoms. 23 Epinephrine directly affects blood vessels by preventing their dilatation, and it has positive ino- and chronotropic activity on cardiac muscle. Moreover, it causes bronchial smooth muscle relaxation and reduces edema of the respiratory tract epithelium. Epinephrine also blocks the release of histamine and other mediators from mast cells and basophils. In the case of food allergy, it has been demonstrated that delayed administration of epinephrine results in an increased risk of severe anaphylaxis. 24 A hypothesis to explain the role of epinephrine administration timing on the course of anaphylactic shock
4 Pałgan and Bartuzi 587 development has been published by Vadas and Perelman. 25 They have shown in vitro that human vascular smooth muscle cells (HVSMCs) stimulated with PAF release prostaglandin E2 (PGE 2 ), which is a strong smooth muscles relaxing factor. However, pre-incubation of HVSMCs with epinephrine completely abolishes the stimulatory effect of PAF. Furthermore, the authors have noted that the block of PGE 2 release is more effective the quicker epinephrine is added to the HVSMC culture following PAF stimulation. PAF and bronchial asthma PAF produced by several types of inflammatory cells participates in the pathogenesis of bronchial asthma. It has been demonstrated that PAF can directly cause bronchial obstruction in animals under experimental conditions, while in humans it belongs to a group of factors that increase bronchial tree hyper-reactivity. 26,27 The use of PAF receptor blockers has been shown to abolish the bronchoconstriction effect of this factor. Moreover, it has also been demonstrated that PAF increases bronchial epithelial structure mucus production, and increases the permeability of pulmonary blood vessels. Howard 28 suggests that PAF is an important driver of inflammation in the bronchial epithelium. The production of PAF increases in inflammatory cells both during exposure to inhaled allergens, as well as during infection. As mentioned above, PAF is a chemotactic factor for neutrophils and it increases the release of oxygen-derived radicals from both neutrophils and eosinophils. Proinflammatory PAF activity is also manifested by the stimulation of LTB4 production. It is additionally suspected that PAF may be involved in the stimulation of bronchial tree remodeling. Studies on salbutamol, (short-acting β2-adrenergic receptor agonist [SABA]), have revealed that inhalation of the drug results in the release of PAF, which in turn stimulates smooth muscle proliferation. 29,30 Obesity is an important factor that negatively affects the control of asthma in patients with bronchial asthma. A study by Grotta et al. 31 of obese children and young adults suffering from bronchial asthma has shown that they have an increased serum concentration of PAF in addition to leptin, eotaxin, RANTES, and TNF-α. These factors are responsible for chemotaxis and activation of inflammatory cells, particularly eosinophils. According to the authors, PAF is one of the factors responsible for poor control of bronchial asthma. PAF and urticaria Urticaria is characterized by formation of wheals and erythema on the skin. From an etiological point of view, urticaria is divided into three types: allergic, non-allergic, and idiopathic. Based on the duration of the lesions the urticaria is described as either acute or chronic. 32 Activation of mast cells either directly (e.g. chemical, physical factors) or indirectly (e.g. anaphylatoxins, eicosanoids, plasmin, Hageman factor) can result in degranulation of mast cells and formation of the skin lesions. 33 Mastocytes play a central role in both acute and chronic urticaria. Mediators released from these cells, such as histamine, serotonin, proteolytic enzymes, proteoglycans, TNF-α, IL-6, and LTs directly or indirectly affect the development of wheals and erythema. Histamine plays a key role in the development of wheals. It has been also noted that vascular endothelial growth factor (VEGF) and PAF play an important role in patients with urticaria. These factors complement pathogenetic changes by increasing the permeability of capillaries in the skin and enhancing the development of wheals. 34 Moreover, PAF can also intensify the inflammation process by chemotactic action on other cells involved in inflammation such as eosinophils, neutrophils, and macrophages. This effect is especially noticeable in chronic urticaria. Studies on volunteers have shown that PAF injected subcutaneously induces typical urticarial wheals. 35 Urticaria etiology is very diverse and therefore treatment of this type of lesions is troublesome and often ineffective. Drugs that act mainly on mast cells by blocking the H 1 -receptor are recommended including first and second generation antihistamines and H 2 receptor blockers as adjunctive therapy. Drugs not registered for the treatment of urticarial diseases (e.g. sulfasalazine, montelukast, methotrexate, cyclosporine) have been used in attempt to find a therapy without success. A large therapeutic efficacy in urticaria has been shown by rupatadine, a second generation antihistamine having blocking activity on both H 1 and PAF receptors on the surface of mast cells. 36 Recent investigations have confirmed the efficacy of this drug in the therapy of both acute and chronic urticarial. 37,38 In turn, promising results have been shown in a
5 588 International Journal of Immunopathology and Pharmacology 28(4) study of omalizumab at doses of 150 or 300 mg delivered subcutaneously. Interestingly, omalizumab is a monoclonal antibody against the C3 fragment of the IgE heavy chain and the main indication for this drug is severe asthma that is poorly controlled with the use of classical treatment. 39 Conclusion In summary, we conclude that an important role is emerging for PAF in allergic reactions, particularly of the first type. Studies on anaphylaxis have shown that PAF contributes to the development of anaphylactic shock. In bronchial asthma PAF can directly and indirectly enhances obstructive changes of bronchi, by stimulation of allergic inflammation of the respiratory tract epithelium. Studies that have looked into the role of PAF in urticaria pathogenesis have shown that this factor is capable of causing wheals and erythema, and it can increase skin lesions by acting on inflammatory cells. Declaration of conflicting interests The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article. Funding This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors. References 1. Benveniste J (1974) Platelet-activating factor, a new mediator of anaphylaxis and immune complex deposition from rabbit and human basophils. Nature 249(457): Singh P, Singh IN, Mondal SC, et al. (2013) Plateletactivating factor (PAF)-antagonists of natural origin. Fitoterapia 84: Stafforini DM, McIntyre TM, Zimmerman GA, et al. (2003) Platelet-activating factor, a pleiotrophic mediator of physiological and pathological processes. Critical Reviews in Clinical Laboratory Sciences 40: Chao W and Olson MS (1993) Platelet-activating factor: Receptors and signal transduction. Biochemical Journal 292: Nakamura M, Honda Z and Izumi T (1991) Molecular cloning and expression of platelet-activating factor receptor from human leukocytes. Journal of Biological Chemistry 266: Montrucchio G, Alloatti G and Camussi G (2000) Role of platelet-activating factor in cardiovascular pathophysiology. Physiological Reviews 80: Dziedziczko A and Pałgan K (2004) Eosinophil apoptosis and asthma. Polski Merkuriusz Lekarski 17(97): Dyer KD, Percopo CM, Xie Z, et al. (2010) Mouse and human eosinophils degranulate in response to PAF and lysopaf via a PAF-receptor independent mechanism: Evidence for a novel receptor. Journal of Immunology 184(11): Kato M, Kimura H, Motegi Y, et al. (2002) Plateletactivating factor activates two distinct effector pathways in human eosinophils. Journal of Immunology 169(9): Kato M, Yamaguchi T, Tachibana A, et al. (2005) An atypical protein kinase C, PKC ζ, regulates human eosinophil effector functions. Immunology 116(2): Pałgan K, Kołakowska J and Zbikowska-Gotz M (2000) The role of mast cells in inflammatory reactions. Pneumonologia i Alergologia Polska 68: Nilsson G and Schwartz LB (1995) Mast cell heterogeneity: structure and mediators. In: Busse WW, Holgate ST, editors. Asthma and Rhinitis. Boston: Blackwell Science, p Kajiwara N, Sasaki T, Bradding P, et al. (2010) Activation of human mast cells through the plateletactivating factor receptor. Journal of Allergy and Clinical Immunology 125(5): e Petersen LJ, Church MK and Skov PS (1997) Plateletactivating factor induces histamine release from human skin mast cells in vivo, which is reduced by local nerve blockade. Journal of Allergy and Clinical Immunology 99(5): Triggiani M, Patella V, Staiano RI, et al. (2008) Allergy and the cardiovascular system. Clinical and Experimental Immunology 153 Suppl 1: Kruszewski J, Błażowski Ł, Grzelewska- Rzymowska I, et al. (2009) Anaphylaxis. The stance of the expert panel of the Polish Society of Allergology. In: Kruszewski J (ed.) Medycyna Praktyczna. Krakow. 17. Vadas P, Gold M, Perelman B, et al. (2008) Plateletactivating factor, PAF acetylhydrolase, and severe anaphylaxis. New England Journal of Medicine 358(1): Zheng GH, Xiong SQ, Mei LJ, et al. (2012) Elevated plasma platelet activating factor, platelet activating factor acetylhydrolase levels and risk of coronary heart disease or blood stasis syndrome of coronary heart disease in Chinese: A case control study. Inflammation 35:
6 Pałgan and Bartuzi Srinivasan P and Bahnson BJ (2010) Molecular model of plasma PAF acetylhydrolase-lipoprotein association: Insights from the structure. Pharmaceuticals (Basel) 3(3): Guerra R, Zhao B, Mooser V, et al. (1997) Determinants of plasma platelet activating factor acetylhydrolase: Heritability and relationship to plasma lipoproteins. Journal of Lipid Research 38: Finkelman FD, Rothenberg ME, Brandt EB, et al. (2005) Molecular mechanisms of anaphylaxis: Lessons from studies with murine models. Journal of Allergy and Clinical Immunology 115: Vadas P, Perelman B and Liss G (2013) Plateletactivating factor, histamine, and tryptase levels in human anaphylaxis. Journal of Allergy and Clinical Immunology 131(1): Järvinen KM and Celestin J (2014) Anaphylaxis avoidance and management: Educating patients and their caregivers. Journal of Asthma and Allergy 7: Banerji A, Rudders SA, Corel B, et al. (2010) Repeat epinephrine treatments for food-related allergic reactions that present to the emergency department. Allergy and Asthma Proceedings 31(4): Vadas P and Perelman B (2012) Effect of epinephrine on platelet-activating factor stimulated human vascular smooth muscle cells. Journal of Allergy and Clinical Immunology 129: Cuss FM, Dixon CMS and Barnes PJ (1986) Effects of inhaled platelet-activating factor on pulmonary function and bronchial responsiveness in man. Lancet 8500: Pretolani M and Vargaftig BB (1993) From lung hypersensitivity to bronchial hyperreactivity. What can we learn from studies on animal models? Biochemical Pharmacology 45(4): Howard KM (2009) Differential expression of plateletactivating factor acetylhydrolase in lung macrophages. American Journal of Physiology Lung Cellular and Molecular Physiology 297(6): L1141 L Bae R, Arteaga A, Raj JU, et al. (2012) Albuterol isomers modulate platelet-activating factor synthesis and receptor signaling in human bronchial smooth muscle cells. International Archives of Allergy and Immunology 158(1): Kasperska-Zajac A, Brzoza Z and Rogala B (2008) Platelet-activating factor (PAF): A review of its role in asthma and clinical efficacy of PAF antagonists in the disease therapy. Recent Patents on Inflammation & Allergy Drug Discovery 2(1): Grotta MB, Squebola-Cola DM, Toro AA, et al. (2013) Obesity increases eosinophil activity in asthmatic children and adolescents. BMC Pulmonary Medicine 13(1): Jain S (2014) Pathogenesis of chronic urticaria: An overview. Dermatology Research and Practice 2014: Aktar S, Akdeniz N, Ozkol HU, et al. (2015) The relation of autologous serum and plasma skin test results with urticarial activity score, sex and age in patients with chronic urticaria. Postepy Dermatologii i Alergologii 32(3): Spickett G (2014) Urticaria and angioedema. Journal of the Royal College of Physicians of Edinburgh 44(1): Bossi F, Frossi B, Radillo O, et al. (2011) Mast cells are critically involved in serum-mediated vascular leakage in chronic urticaria beyond high-affinity IgE receptor stimulation. Allergy 66(12): Mullol J, Bousquet J, Bachert C, et al. (2008) Rupatadine in allergic rhinitis and chronic urticaria. Allergy 63 Suppl 87: Nettis E, Delle Donne P, Di Leo E, et al. (2013) Rupatadine for the treatment of urticaria. Expert Opinion on Pharmacotherapy 14(13): Rihoux JP, Fadel R and Juhlin L (1991) Plateletactivating factor-induced immediate and late cutaneous reactions. International Archives of Allergy and Applied Immunology 94: Durack A and Matin RN (2014) Omalizumab for the treatment of chronic idiopathic or spontaneous urticaria: A critical appraisal. British Journal of Dermatology 171(1):
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Sporadic Antihistamine-Resistant Angioedema Potential Pathophysiological Mechanisms
 Sporadic Antihistamine-Resistant Angioedema Potential Pathophysiological Mechanisms Massimo Triggiani, MD, PhD Division of Allergy and Clinical Immunology University of Salerno HAWK Consensus Meeting Gargnano,
Sporadic Antihistamine-Resistant Angioedema Potential Pathophysiological Mechanisms Massimo Triggiani, MD, PhD Division of Allergy and Clinical Immunology University of Salerno HAWK Consensus Meeting Gargnano,
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
INFLAMMATION & REPAIR
 INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
Cell-Derived Inflammatory Mediators
 Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Determinants of Severe and Fatal Anaphylaxis
 Determinants of Severe and Fatal Anaphylaxis Peter Vadas MD PhD Chief, Division of Allergy and Clinical Immunology St. Michael s Hospital University of Toronto The Problem Peanut the most common cause
Determinants of Severe and Fatal Anaphylaxis Peter Vadas MD PhD Chief, Division of Allergy and Clinical Immunology St. Michael s Hospital University of Toronto The Problem Peanut the most common cause
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host.
 Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Immunologic Mechanisms of Tissue Damage. (Immuopathology)
 Immunologic Mechanisms of Tissue Damage (Immuopathology) Immunopathology Exaggerated immune response may lead to different forms of tissue damage 1) An overactive immune response: produce more damage than
Immunologic Mechanisms of Tissue Damage (Immuopathology) Immunopathology Exaggerated immune response may lead to different forms of tissue damage 1) An overactive immune response: produce more damage than
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Anaphylaxis: The Atypical Varieties
 Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
Innate vs Adaptive Response
 General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October
 Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October Allergic Reactions ( Immediate Hypersensitivity ) Hay fever, food, drug & animal allergies, reactions to bee stings, etc. Symptoms may include
Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October Allergic Reactions ( Immediate Hypersensitivity ) Hay fever, food, drug & animal allergies, reactions to bee stings, etc. Symptoms may include
Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October
 Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October Allergic Reactions ( Immediate Hypersensitivity ) Hay fever, food, drug & animal allergies, reactions to bee stings, etc. Symptoms may include
Immunology 2011 Lecture 23 Immediate Hypersensitivity 26 October Allergic Reactions ( Immediate Hypersensitivity ) Hay fever, food, drug & animal allergies, reactions to bee stings, etc. Symptoms may include
Anaphylactic response in rabbit Part II
 Anaphylactic response in rabbit Part II Introduction Four types of hypersensitivity reactions: Type I: allergy Type II: antibodies Type III: immune complex Type IV: T-cells Type I Hypersensitivity ALLERGY
Anaphylactic response in rabbit Part II Introduction Four types of hypersensitivity reactions: Type I: allergy Type II: antibodies Type III: immune complex Type IV: T-cells Type I Hypersensitivity ALLERGY
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Mast Cell Mediators. Updates on Chronic Urticaria 11/1/2016. Urticaria: What happens in the skin?
 Urticaria: What happens in the skin? Updates on Chronic Urticaria Kent Woo, MD (USA) Allergy/Immunology Internal Medicine C A U S E MC, mast cell IgE Fc eri MC Release of Mediators Activation Vasodilation
Urticaria: What happens in the skin? Updates on Chronic Urticaria Kent Woo, MD (USA) Allergy/Immunology Internal Medicine C A U S E MC, mast cell IgE Fc eri MC Release of Mediators Activation Vasodilation
Immunology. Lecture- 8
 Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Respiratory Pharmacology PCTH 400 Asthma and β-agonists
 Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Hypersensitivity diseases
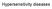 Hypersensitivity diseases Downloaded from: StudentConsult (on 18 July 2006 11:40 AM) 2005 Elsevier Type-I Hypersensitivity Basic terms Type-I = Early= IgE-mediated = Atopic = Anaphylactic type of hypersensitivity
Hypersensitivity diseases Downloaded from: StudentConsult (on 18 July 2006 11:40 AM) 2005 Elsevier Type-I Hypersensitivity Basic terms Type-I = Early= IgE-mediated = Atopic = Anaphylactic type of hypersensitivity
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
contact activation in formation diseases 67 endothelial cells and kinin formation 73 processing and degradation 68 70
 Subject Index Adenosine, mast cell activation modulation 60 Age, risk factor 17, 18 Allergen elicitors 9, 10 insects, see Insect venom-induced microarrays for 136 overview of characteristics 23 recognition
Subject Index Adenosine, mast cell activation modulation 60 Age, risk factor 17, 18 Allergen elicitors 9, 10 insects, see Insect venom-induced microarrays for 136 overview of characteristics 23 recognition
U N I V E R S I T Ä T S M E D I Z I N B E R L I N
 U N I V E R S I T Ä T S M E D I Z I N B E R L I N Chronic Urticaria: the role of mast cells and basophils Marcus Maurer Allergie-Centrum-Charité Department of Dermatology and Allergy Charité - Universitätsmedizin
U N I V E R S I T Ä T S M E D I Z I N B E R L I N Chronic Urticaria: the role of mast cells and basophils Marcus Maurer Allergie-Centrum-Charité Department of Dermatology and Allergy Charité - Universitätsmedizin
Inflammation in the clinic
 Inflammation in the clinic Stephen T. Holgate MRC Clinical Professor of Immunopharmacology ILSI Europe Workshop, Seville, May 14-15 2012 The immune system acts in four general ways to ensure host defence
Inflammation in the clinic Stephen T. Holgate MRC Clinical Professor of Immunopharmacology ILSI Europe Workshop, Seville, May 14-15 2012 The immune system acts in four general ways to ensure host defence
Recognition & Management of Anaphylaxis in the Community. S. Shahzad Mustafa, MD, FAAAAI
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
1) Mononuclear phagocytes : 2) Regarding acute inflammation : 3) The epithelioid cells of follicular granulomas are :
 Pathology Second 1) Mononuclear phagocytes : - Are the predominant cells in three day old wounds - Are common in liver, spleen and pancreasd - Produce fibroblast growth factor - Secrete interferon-g -
Pathology Second 1) Mononuclear phagocytes : - Are the predominant cells in three day old wounds - Are common in liver, spleen and pancreasd - Produce fibroblast growth factor - Secrete interferon-g -
Allergy overview. Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital
 Allergy overview Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital Adaptive Immune Responses Adaptive immune responses allow responses against
Allergy overview Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital Adaptive Immune Responses Adaptive immune responses allow responses against
10. Which of the following immune cell is unable to phagocytose (a) neutrophils (b) eosinophils (c) macrophages (d) T-cells (e) monocytes
 Chapter 2. Acute and chronic inflammation(6): 1. In acute inflammation, which events occur in the correct chronological order? (Remembered from 2000, 2004 exam.) p50 (a) transient vasoconstriction, stasis
Chapter 2. Acute and chronic inflammation(6): 1. In acute inflammation, which events occur in the correct chronological order? (Remembered from 2000, 2004 exam.) p50 (a) transient vasoconstriction, stasis
Al ergy: An Overview
 Allergy: An Overview Allergy Type of hypersensitivity reactions of the immune system. Allergy may involve more than one type of reaction. An allergy is a reaction to something that does not affect most
Allergy: An Overview Allergy Type of hypersensitivity reactions of the immune system. Allergy may involve more than one type of reaction. An allergy is a reaction to something that does not affect most
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
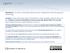 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD)
 WAC2011, Dec 7, 2011 Cancun, Mexico Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD) Hae- Sim Park, MD, Ph D Department of Allergy & Clinical Immunology Ajou University School of
WAC2011, Dec 7, 2011 Cancun, Mexico Eosinophil activation in Aspirin Exacerbated Respiratory Disease (AERD) Hae- Sim Park, MD, Ph D Department of Allergy & Clinical Immunology Ajou University School of
Basis of Immunology and
 Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Etiology and Pathogenesis of Adverse Drug Reactions
 French LE (ed): Adverse Cutaneous Drug Eruptions. Chem Immunol Allergy. Basel, Karger, 2012, vol 97, pp 32 46 Etiology and Pathogenesis of Adverse Drug Reactions O. Hausmann B. Schnyder W.J. Pichler Department
French LE (ed): Adverse Cutaneous Drug Eruptions. Chem Immunol Allergy. Basel, Karger, 2012, vol 97, pp 32 46 Etiology and Pathogenesis of Adverse Drug Reactions O. Hausmann B. Schnyder W.J. Pichler Department
Cytokines, adhesion molecules and apoptosis markers. A comprehensive product line for human and veterinary ELISAs
 Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Respiratory Pharmacology
 Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Innate Immunity: Nonspecific Defenses of the Host
 PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
PowerPoint Lecture Presentations prepared by Bradley W. Christian, McLennan Community College C H A P T E R 16 Innate Immunity: Nonspecific Defenses of the Host Host Response to Disease Resistance- ability
Platelet-Activating Factor, PAF Acetylhydrolase, and Severe Anaphylaxis
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Platelet-Activating Factor, PAF Acetylhydrolase, and Severe Anaphylaxis Peter Vadas, M.D., Ph.D., Milton Gold, M.D., Boris Perelman,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article Platelet-Activating Factor, PAF Acetylhydrolase, and Severe Anaphylaxis Peter Vadas, M.D., Ph.D., Milton Gold, M.D., Boris Perelman,
Hypersensitivity reactions
 Hypersensitivity reactions Prakash Nagarkatti, Ph.D.; e-mail: pnagark@uscmed.sc.edu) COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 19-20 TEACHING OBJECTIVES: 1. Understand the classification
Hypersensitivity reactions Prakash Nagarkatti, Ph.D.; e-mail: pnagark@uscmed.sc.edu) COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 19-20 TEACHING OBJECTIVES: 1. Understand the classification
RESPIRATORY PHARMACOLOGY - ASTHMA. Primary Exam Teaching - Westmead ED
 RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
Hypersensitivity reactions. Immune responses which are damaging rather than helpful to the host.
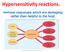 Hypersensitivity reactions. Immune responses which are damaging rather than helpful to the host. 1 Hypersensitivity reaction depends on: 1) chemical nature of allergen 2) route involved in sensitization
Hypersensitivity reactions. Immune responses which are damaging rather than helpful to the host. 1 Hypersensitivity reaction depends on: 1) chemical nature of allergen 2) route involved in sensitization
Pharmacotherapy for Allergic Rhinitis
 Pharmacotherapy for Allergic Rhinitis William Reisacher, MD FACS FAAOA Assistant Professor Weill Cornell Medical College The Impact of Allergic Rhinitis Allergic rhinitis affects approximately 50 million
Pharmacotherapy for Allergic Rhinitis William Reisacher, MD FACS FAAOA Assistant Professor Weill Cornell Medical College The Impact of Allergic Rhinitis Allergic rhinitis affects approximately 50 million
7/25/2016. Use of Epinephrine in the Community. Knowledge Amongst Paramedics. Knowledge Amongst Paramedics survey of 3479 paramedics
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Pharmacology of the Respiratory Tract: Allergy and IgE
 Pharmacology of the Respiratory Tract: Allergy and IgE Tillie-Louise Hackett Assistant Professor, Department of Pharmacology James Hogg Research Centre University of British Columbia Short Synopsis This
Pharmacology of the Respiratory Tract: Allergy and IgE Tillie-Louise Hackett Assistant Professor, Department of Pharmacology James Hogg Research Centre University of British Columbia Short Synopsis This
and its clinical implications
 The Immunology of Allergy and its clinical implications By Dr Priya Bowry Sikand MBBS MRCGP DFFP DIC MSc(Allergy) Back to the Basics. Objectives Understand immunological mechanisms behind Type 1 Hypersensitivity
The Immunology of Allergy and its clinical implications By Dr Priya Bowry Sikand MBBS MRCGP DFFP DIC MSc(Allergy) Back to the Basics. Objectives Understand immunological mechanisms behind Type 1 Hypersensitivity
The Skinny of the Immune System
 The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
Urticaria Moderate Allergic Reaction Mild signs/symptoms with any of following: Dyspnea, possibly with wheezes Angioneurotic edema Systemic, not local
 Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France
 Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France The commonest picture of Allergy Allergy is commonly sensed as an Antibody
Transfusion and Allergy: What is it, and what is it not? Prof. Olivier GARRAUD INTS, Paris Université de Lyon/Saint-Etienne France The commonest picture of Allergy Allergy is commonly sensed as an Antibody
Pharmacology of the Respiratory Tract Lecture 2: Allergy and IgE
 Pharmacology of the Respiratory Tract Lecture 2: Allergy and IgE Dr. Tillie-Louise Hackett Centre for Heart Lung Innovation University of British Columbia tillie.hackett@hli.ubc.ca Learning Objectives
Pharmacology of the Respiratory Tract Lecture 2: Allergy and IgE Dr. Tillie-Louise Hackett Centre for Heart Lung Innovation University of British Columbia tillie.hackett@hli.ubc.ca Learning Objectives
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS
 LECTURE: 15 Title NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Determine the relative percentages in blood for the various types
LECTURE: 15 Title NEUTROPHIL, BASOPHIL, EOSINOPHIL, AND PLATELETS SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Determine the relative percentages in blood for the various types
Five things to know about anaphylaxis
 Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
THE COMPLEMENT SYSTEM OBJECTIVES:
 Dr Mohammed Al- ani THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB)
Dr Mohammed Al- ani THE COMPLEMENT SYSTEM OBJECTIVES: When you finish this section, you should be able to: 1. Describe the effects of complement activation. 2. Outline the Classical, Mannan-Binding (MB)
Case Report. Mechanisms of Anaphylaxis. Case Report. Case Report 37 y/o WF Is this anaphylaxis? What would you do at this point?
 Mechanisms of Anaphylaxis Richard F. Lockey, M.D. Division of Allergy and Immunology Department of Internal Medicine University of South Florida Morsani College of Medicine and James A. Haley Veterans
Mechanisms of Anaphylaxis Richard F. Lockey, M.D. Division of Allergy and Immunology Department of Internal Medicine University of South Florida Morsani College of Medicine and James A. Haley Veterans
Body Defense Mechanisms
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
The Diagnosis and Management of Anaphylaxis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
Learning Outcomes. Systems Pharmacology PHAR3320. Nerves of the Respiratory Tract. Dr Fernandes
 Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Monocast Description Indications
 Monocast Tablet Description The active ingredient of Monocast tablet is Montelukast Sodium INN. Montelukast is a selective and orally active leukotriene receptor antagonist that inhibits the cysteinyl
Monocast Tablet Description The active ingredient of Monocast tablet is Montelukast Sodium INN. Montelukast is a selective and orally active leukotriene receptor antagonist that inhibits the cysteinyl
Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene
 Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene Han-Pin Kuo MD, PhD Department of Thoracic Medicine Chang Gung University Chang Gung Memorial Hospital Taipei, Taiwan Bronchial
Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene Han-Pin Kuo MD, PhD Department of Thoracic Medicine Chang Gung University Chang Gung Memorial Hospital Taipei, Taiwan Bronchial
INFLAMMATION. 5. Which are the main phases of inflammation in their "sequence": 1. Initiation, promotion, progression.
 INFLAMMATION 1. What is inflammation: 1. Selective anti-infective pathological reaction. 2. Pathological process, typical for vascularized tissues. 3. Self-sustained pathological condition. 4. Disease
INFLAMMATION 1. What is inflammation: 1. Selective anti-infective pathological reaction. 2. Pathological process, typical for vascularized tissues. 3. Self-sustained pathological condition. 4. Disease
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network
 Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Anaphylaxis. Perceive the differences between anaphylactic shock and other types of shock. Recognize its nature, causes & characteristics.
 Anaphylaxis Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
Anaphylaxis Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
Topics. Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils
 Topics Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils Immune regulation Idiotypic network 2/15/2005 MICR 415 / 515
Topics Humoral Immune Response Part II Accessory cells Fc Receptors Opsonization and killing mechanisms of phagocytes NK, mast, eosynophils Immune regulation Idiotypic network 2/15/2005 MICR 415 / 515
Hypersensitivity Reactions
 Color code: Important in red Extra in blue Hypersensitivity Reactions For team error adjustments, click here Objectives To know that hypersensitivity reactions are over and excessive immune responses that
Color code: Important in red Extra in blue Hypersensitivity Reactions For team error adjustments, click here Objectives To know that hypersensitivity reactions are over and excessive immune responses that
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders. Allergic Disorders. IgE-dependent Release of Inflammatory Mediators. TH1/TH2 Paradigm
 Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Allergic Disorders Anne-Marie Irani, MD Virginia Commonwealth University Allergic Disorders IgE-mediated immune reactions Clinical entities include: asthma allergic rhinitis atopic dermatitis urticaria
Introduction. Allergic Rhinitis. Seventh Pediatric Asthma Education Conference 5/9/2018
 It Is All One Airway Or How Allergic Rhinitis and Its Management can Affect Asthmatic Patients Stacy Dorris, MD Allergy/Immunology Vanderbilt Medical Center May 9, 2018 Introduction Allergic Rhinitis Allergic
It Is All One Airway Or How Allergic Rhinitis and Its Management can Affect Asthmatic Patients Stacy Dorris, MD Allergy/Immunology Vanderbilt Medical Center May 9, 2018 Introduction Allergic Rhinitis Allergic
Allergic diseases and treatment. Feng Qian ( 钱峰 )
 Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Monocytes must also leave the circulation in response to inflammatory signals, and neutrophils and other granulocytes must be able to do so as well.
 Immunology Dr. John J. Haddad Chapter 15 Leukocyte Migration and inflammation Lymphocytes must recirculate in the body in search of antigens. Since antigens are brought to lymph nodes and the spleen, the
Immunology Dr. John J. Haddad Chapter 15 Leukocyte Migration and inflammation Lymphocytes must recirculate in the body in search of antigens. Since antigens are brought to lymph nodes and the spleen, the
Ocular allergy pathogenesis and diagnosis
 Ocular allergy pathogenesis and diagnosis Luís Delgado, MD PhD departament of Immunology and Immunoallergology Unit Hospital de S. Joao. Porto (Portugal) Marzo 2006 www.alergomurcia.com Good morning, Mr.
Ocular allergy pathogenesis and diagnosis Luís Delgado, MD PhD departament of Immunology and Immunoallergology Unit Hospital de S. Joao. Porto (Portugal) Marzo 2006 www.alergomurcia.com Good morning, Mr.
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
The Lymphatic System and Body Defenses
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
Introduction to Immunopathology
 MICR2209 Introduction to Immunopathology Dr Allison Imrie 1 Allergy and Hypersensitivity Adaptive immune responses can sometimes be elicited by antigens not associated with infectious agents, and this
MICR2209 Introduction to Immunopathology Dr Allison Imrie 1 Allergy and Hypersensitivity Adaptive immune responses can sometimes be elicited by antigens not associated with infectious agents, and this
Informations on exams
 Informations on exams II year BMC: English or Italian (free choice) I year MBC: Mandatory English EXAM vote: 1.Journal Club presentation 2. Open written exam 1.1 argument free (e-mail) 2.1 argument chosen
Informations on exams II year BMC: English or Italian (free choice) I year MBC: Mandatory English EXAM vote: 1.Journal Club presentation 2. Open written exam 1.1 argument free (e-mail) 2.1 argument chosen
1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50%
 BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
BIOL2030 Huaman A&P II -- Exam 3 -- XXXX -- Form A Name: 1. Lymphatic vessels recover about of the fluid filtered by capillaries. A. ~1% C. ~25% E. ~85% B. ~10% D. ~50% 2. Special lymphatic vessels called
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
The proposal is to add text/statements in red and to delete text/statements with strikethrough: POLICY
 Omalizumab DESCRIPTION Omalizumab is a recombinant DNA-derived humanized IgG1κ monoclonal antibody which selectively binds to immunoglobulin E (IgE). High serum levels of IgE are found in individuals with
Omalizumab DESCRIPTION Omalizumab is a recombinant DNA-derived humanized IgG1κ monoclonal antibody which selectively binds to immunoglobulin E (IgE). High serum levels of IgE are found in individuals with
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
S. Kaiger Basel München Paris London New York Tokyo Sydney
 Mast Cell Activation and Mediator Release Progress in Allergy Vol. 34 Series Editors Kimishige Ishizaka, Baltimore, Md.; Paul Kallds, Helsingborg; Byron H. Waksman, New York, N.Y., and Alain L. de Weck,
Mast Cell Activation and Mediator Release Progress in Allergy Vol. 34 Series Editors Kimishige Ishizaka, Baltimore, Md.; Paul Kallds, Helsingborg; Byron H. Waksman, New York, N.Y., and Alain L. de Weck,
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT. Michael J. Calice MD, FACEP St. Mary Mercy Hospital
 EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
Objectives By the end of lecture the student should:
 Objectives By the end of lecture the student should: Illustrate α oxidation of fatty acids. Understand ω oxidation of fatty acids. List sources and fates of active acetate. Discuss eicosanoids. 2- α Oxidation
Objectives By the end of lecture the student should: Illustrate α oxidation of fatty acids. Understand ω oxidation of fatty acids. List sources and fates of active acetate. Discuss eicosanoids. 2- α Oxidation
ANSC/NUTR 618 Lipids & Lipid Metabolism
 I. Nonessential fatty acids ANSC/NUTR 618 Lipids & Lipid Metabolism A. Synthesized completely by the fatty acid synthase reaction (e.g., myristic and palmitic acid). B. Produced by the modification of
I. Nonessential fatty acids ANSC/NUTR 618 Lipids & Lipid Metabolism A. Synthesized completely by the fatty acid synthase reaction (e.g., myristic and palmitic acid). B. Produced by the modification of
Biologic Agents in the treatment of Severe Asthma
 Biologic Agents in the treatment of Severe Asthma Daniel L Maxwell, D.O., FACOI, FAASM Clinical Assistant Professor of Medicine Michigan State University College of Osteopathic Medicine College of Human
Biologic Agents in the treatment of Severe Asthma Daniel L Maxwell, D.O., FACOI, FAASM Clinical Assistant Professor of Medicine Michigan State University College of Osteopathic Medicine College of Human
Immunology lecture: 14. Cytokines: Main source: Fibroblast, but actually it can be produced by other types of cells
 Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
Immunomodulators: Anti-IgE mab. Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE
 Immunomodulators: Anti-IgE mab Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE Objectives To explain the rationale behind IgE blockade To discuss which
Immunomodulators: Anti-IgE mab Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE Objectives To explain the rationale behind IgE blockade To discuss which
Topic 9 (Ch16_18) Immune Disorders. Allergies. 4 Hypersensitivity Types. Topics - Allergies - Autoimmunity - Immunodeficiency
 Topic 9 (Ch16_18) Immune Disorders Topics - Allergies - Autoimmunity - Immunodeficiency 1 Allergies Allergens (antigens) cause an exaggerated immune response or hypersensitivity 4 types: Type I Type II
Topic 9 (Ch16_18) Immune Disorders Topics - Allergies - Autoimmunity - Immunodeficiency 1 Allergies Allergens (antigens) cause an exaggerated immune response or hypersensitivity 4 types: Type I Type II
