MAST CELL RESPONSES TO DANGER SIGNALS
|
|
|
- Philip Norris
- 5 years ago
- Views:
Transcription
1 Department of Medicine, Clinical Immunology and Allergy Unit, Karolinska Institutet, Stockholm, Sweden MAST CELL RESPONSES TO DANGER SIGNALS Mattias Enoksson Stockholm 2012
2 All previously published papers were reproduced with permission from the publisher. Paper I: Copyright S. Karger AG, Basel Paper II: Copyright The American Association of Immunologists, Inc. Published by Karolinska Institutet. Printed by Larserics Digital Print AB Mattias Enoksson, 2012 ISBN
3 A problem solved is a problem caused - Karl Pilkington
4
5 ABSTRACT Detecting and responding to danger is a paramount function of the immune system. Compounds heralding danger can be divided into two groups: exogenous and endogenous danger signals. The former group consists of conserved microbial structures such as lipopolysaccharide (LPS), while the latter consists of host compounds released or exposed by dead or dying cells as a consequence of trauma, stress or infection. Mast cells are long-lived immune cells present in almost all tissues, and are especially numerous at sites facing the external environment, making them ideal responders to danger signals. The aim of the work presented in this thesis was to investigate mast cell responses to danger signals of exogenous and endogenous origin. In Paper I, we investigated mast cell responses to the exogenous danger signal M-TriDAP, a bacterial peptidoglycan degradation product. We found that cord bloodderived mast cells (CBMCs) express NOD1, the receptor for M-TriDAP. Furthermore, M-TriDAP-treatment of CBMCs resulted in degranulation-independent release of cytokines and chemokines such as TNF, IL-8/CXCL8, MIP-1α/CCL3 and MIP-1β/CCL4. Importantly, we observed an augmented response when M-TriDAP was combined with the TLR4 agonist LPS, indicating cooperation between intracellular and extracellular pattern recognition receptors. In Paper II, we investigated mast cell responses to cell injury by subjecting murine mast cells to the supernatant of fibroblasts rendered necrotic by freeze-thawing. We found that mast cells respond to cell injury in this model by initiating a proinflammatory response, characterized by degranulation-independent release of cytokines and leukotrienes. By using genetically modified mice and molecular inhibitors, we found that the recognition of cell injury was MyD88-, T1/ST2- and p38- dependent. Finally, by using RNA-interference, we could pinpoint IL-33 as the necrotic cell compound that was responsible for the mast cell activation. In Paper III, we investigated responses to IL-33 administration in vivo. Here we found that wild-type C57BL/6 mice respond to intraperitoneal IL-33 administration with neutrophil infiltration. This response was not observed in mast cell-deficient mice but could be restored upon mast cell reconstitution, thus demonstrating a mast cell dependent mechanism. In Paper IV, we investigated the hypothesis that mast cells might function as sensors of damaged epithelia by responding to IL-33 during chronic inflammations of the airways, for instance in asthma. We found that IL-33 is released from necrotic airway epithelial cells and that CBMCs respond to the necrotic supernatant of these cells by secreting IL-5, IL-8/CXCL8, TNF and GM-CSF. However, no release of histamine, LTB 4 or PGD 2 could be detected. Interestingly, the exact same mediator release pattern was observed when CBMCs were treated with recombinant IL-33, suggesting that IL-33 might be an important factor released by injured airway epithelial cells that activates mast cells. In conclusion, the work presented in this thesis provides further evidence for important roles of mast cells in innate immune responses. The function of mast cells as sensors of cell injury is highlighted; a role that potentially can be either beneficial or detrimental. Finally, novel evidence is provided for the notion that IL-33 is an important danger signal capable of mast cell activation.
6 LIST OF PUBLICATIONS I. Enoksson M, Ejendal KFK, McAlpine S, Nilsson G, Lunderius-Andersson C Human cord blood-derived mast cells are activated by the Nod1 agonist M-TriDAP to release pro-inflammatory cytokines and chemokines J Innate Immun. 2011;3: II. Enoksson M, Lyberg K, Möller-Westerberg C, Fallon PG, Nilsson G, Lunderius-Andersson C Mast cells as sensors of cell injury through IL-33 recognition J Immunol Feb 15;186(4): III. Enoksson M, Fallon PG, Lunderius-Andersson C, Nilsson G Intraperitoneal influx of neutrophils in response to IL-33 is mast cell dependent Submitted IV. Enoksson M, Andersson C, Heinz G, Chatterjee M, Saluja R, Erjefält J, Nilsson G Human mast cell responses to injured airway epithelial cells implications for chronic airway inflammation Manuscript
7 Publications not included in this thesis Lunderius-Andersson C, Enoksson M, Nilsson G Mast cells respond to cell injury through the recognition of IL-33 Front Immunol. 2012, In press. Review McAlpine SM, Enoksson M, Lunderius-Andersson C, Nilsson G The effect of bacterial, viral and fungal infection on mast cell reactivity in the allergic setting J Innate Immun. 2011;3: Review
8
9 CONTENTS 1 INTRODUCTION Mast cells Mast cell distribution and heterogeneity Mast cell activation and mediator release Mast cell function in health and disease Pattern recognition Toll-like receptors Nod-like receptors C-type lectin receptors Retinoic acid-inducible gene (RIG)-I-like receptors Damage recognition Endogenous danger signals IL IL-33 expression and signaling IL-33 activity IL-33 in health and disease IL-33 as a danger signal THE PRESENT STUDY Aim Methodology Results and discussion Human cord blood-derived mast cells are activated by the Nod1 agonist M-TriDAP to release pro-inflammatory cytokines and chemokines (Paper I) Mast cells as sensors of cell injury through IL-33 recognition (Paper II) Intraperitoneal influx of neutrophils in response to IL-33 is mast cell dependent (Paper III) Human mast cell responses to injured airway epithelial cells implications for chronic airway inflammation (Paper IV) FUTURE PERSPECTIVES POPULÄRVETENSKAPLIG SAMMANFATTNING ACKNOWLEDGEMENTS REFERENCES... 40
10 LIST OF ABBREVIATIONS AHR Airway hyper-responsiveness AIM Absent in melanoma APC Antigen-presenting cell ATP Adenosine triphosphate BMMC Bone marrow-derived mast cell CARD Caspase activation and recruitment domain CBMC Cord blood-derived mast cell CIA Collagen-induced arthritis CLR C-type lectin receptor DAMP Danger-associated molecular pattern DC Dendritic cell ELISA Enzyme linked immunosorbent assay GM-CSF Granulocyte macrophage colony-stimulating factor HMGB1 High-mobility group box 1 protein HSP Heat shock protein IFN Interferon Ig Immunoglobulin IL Interleukin IL-1RAcP IL-1R accessory protein IPAF ICE-protease-activating factor IRF Interferon regulatory factor LGP2 Laboratory of genetics and physiology 2 LPS Lipopolysaccharide LRR Leucine-rich repeat LT Leukotriene MCP Monocyte chemoattractant protein MDA5 Melanoma differentiation associated factor 5 MDP Muramyl dipeptide MEF Mouse embryonal fibroblast MIP Macrophage inflammatory protein NALP NACHT, LRR and PYD-containing protein NBD Nucleotide-binding domain NK Natural killer NLR NOD-like receptor NLRP NACHT, LRR and PYD-containing protein NOD Nucleotide-binding oligomerization domain PAMP Pathogen-associated molecular pattern PBS Phosphate-buffered saline PG Prostaglandin PGN Peptidoglycan PNEC Primary nasal epithelial cell PRR Pattern recognition receptor PYD Pyrin domain qpcr Quantitative real time PCR
11 RA RAGE RIG-I RLR SCF sirna TGF Th TIR TLR TNF Rheumatoid arthritis Receptor for advanced glycation endproducts Retinoic acid-inducible gene I Retinoic acid-inducible gene (RIG)-I-like receptor Stem-cell factor Small interfering RNA Transforming growth factor T helper Toll/IL-1R homology Toll-like receptor Tumor necrosis factor
12
13 1 INTRODUCTION The immune system has evolved to combat infections, a function that represents a prerequisite for life. Therefore, strict control and regulation of the immune system is paramount, as both excessive and insufficient activation can be fatal, leading to autoimmunity and persistent infections, respectively. Consequently, contextappropriate activation is vital [1], i.e. the nature, magnitude and duration of the immune response need to be appropriate for a given situation and location. In essence, the immune system can be activated by two means: i) by recognizing non-self molecules of infectious agents such as bacteria, virus, parasites and fungi (pathogen-associated molecular patterns; PAMPs) [2] or ii) by recognizing self molecules released by damaged or dying cells (danger-associated molecular patterns; DAMPs) [3]. To face the ever present threat of detrimental pathogens, the immune system has evolved into a highly organized network of organs, cells and molecules that together can be regarded as the barriers, first line-defenders and the heavy artillery of the immune system. Traditionally, the immune system is described to be composed of two branches: the innate and the adaptive branch. While the former is unspecific but fast in onset, the latter is slow but extremely specific. The first obstacles faced by invading pathogens are physical and chemical barriers, which can be considered part of the innate immune system. Such barriers include for example the skin, mucosal surfaces and low gastric ph. Should pathogens circumvent these barriers, the cellular part of the innate immune system will be activated. The cellular part is composed of a variety of cell types including macrophages, monocytes, dendritic cells (DCs), eosinophils, basophils, natural killer cells (NK cells), neutrophils and mast cells. Together, these cells possess the abilities to directly kill pathogens, produce compounds that enhance pathogen elimination and to activate the adaptive branch of the immune system. Most pathogen infestations can be handled by the innate immune cells, but sometimes a more forceful response is needed, and this is where the adaptive branch of the immune system is introduced. Antigen-presenting cells (APCs) of the innate immune system, such as DCs, are specialized in carrying antigens through the lymphatic system to local lymph nodes, where activation of the adaptive immune system takes place. The adaptive immune system is composed of T and B lymphocytes, cells that carry receptors specific for a vast amount of antigens. When activated, these cells expand and participate in pathogen killing by producing mediators and antibodies that enhance pathogen elimination. The adaptive immune system also possesses memory, which facilitates a fast response to reinvading pathogens. In order to fully understand the immune system, and eventually translate this understanding into therapeutical use, detailed knowledge of the various components of the immune system is of great importance. This thesis deals with the activation of such a component; the mast cell. More specifically, activation of mast cells by exogenous and endogenous danger signals is investigated. 1
14 1.1 MAST CELLS The mast cell was discovered in 1878 by the German scientist Paul Ehrlich [4]. Mast cells are most well-known for their role in allergic inflammation, where they act as effector cells which release compounds causing classical allergic symptoms. For many years, mast cells were mostly discussed in the context of allergy, but it is becoming increasingly clear that mast cells have many other functions. We now know that mast cells possess a Dr Jekyll and Mr Hyde -nature, where mast cell responses sometimes are beneficial and sometimes detrimental [5]. Thus, a more complex role for mast cells is emerging, where mast cells are more and more appreciated as important sentinel cells possessing regulatory functions. Key characteristics of mast cells include their granulation, their wide tissue distribution, their long life span, and their ability to selectively release mediators upon activation. In addition, mast cells are endowed with several types of receptors, enabling them to react to a multitude of activators. In this chapter, important aspects of mast cell biology are highlighted Mast cell distribution and heterogeneity Mast cells are evolutionary conserved inflammatory cells; early mast cells are thought to have appeared approximately million years ago [6]. Murine mast cells originate from a pluripotent, hematopoietic stem cell population in the bone marrow and human mast cells derive from a corresponding CD34 + /CD117 + /CD13 + bone marrow population [7-9]. Unlike other cells of the hematopoietic lineage, mast cells exit the bone marrow as immature precursors, circulate in the bloodstream and eventually migrate into peripheral tissues where they mature [7, 9]. Mast cells are commonly found near blood vessels and nerves in vascularized tissues throughout the body, and are especially numerous at sites facing the external environment, such as the skin, the airways and in the gastrointestinal tract [7, 10, 11]. As a result of this tissue distribution, mast cells are among the first cell types to encounter invading pathogens, and are therefore often referred to as gate-keepers, or sentinels, of the immune system. This important function of mast cells will be discussed in more detail in chapter Mast cells represent a heterogeneous cell population, where the tissue microenvironment and growth factor milieu dictates the characteristics of the mature mast cell. Mast cell heterogeneity was originally described by Enerbäck in the 1960s [12, 13]. In this work, mast cells in the intestinal mucosa and submucosa were called mucosal mast cells and connective-tissue mast cells, respectively, depending on their dye-binding properties. In humans, corresponding mast cell populations are referred to as MC T (tryptase containing) and MC TC (tryptase and chymase containing) [9]. However, this division probably represents an oversimplification, as it is more likely that there is a wide spectrum of mast cell variants, depending on localization and local microenvironment. These types of mast cells might also change during inflammation or infection [11]. Interestingly, it has even been suggested that mast cell phenotypes can be reversible under certain conditions [9, 14]. Stem-cell factor (SCF) is the most important growth factor for mast cells. However, other mediators such as interleukin-3 (IL-3), IL-4, IL-5, IL-6, IL-9 and transforming growth factor-1 (TGF-1) can also influence mast cell proliferation and survival [7, 11, 15-17]. The importance of SCF or its receptor c-kit, which is highly expressed by mast cells, is 2
15 demonstrated in mice deficient in c-kit or SCF, as mast cells are almost completely absent in these mice [18, 19] Mast cell activation and mediator release Mast cells are best known for their role in allergic reactions. Therefore, the most extensively studied mast cell reaction is immunoglobulin E (IgE)-dependent mast cell activation [20, 21]. This kind of activation is what underlies an allergic reaction, eventually resulting in classical allergic symptoms, such as sneezing and a runny nose. IgE-dependent mast cell activation is schematically depicted in figure 1. When susceptible individuals come into contact with for example birch pollen, their B cells produce birch-specific IgE antibodies (a process that also requires T cell help). These antibodies will then attach to the surface of mast cells by binding to high affinity IgEreceptors (FcRI). Upon a second exposure to birch pollen, IgE-primed mast cells are activated through FcRI-crosslinking, causing the mast cells to degranulate and thereby release mediators, such as histamine, that cause allergic symptoms. Y B T cell help Ig class switch IgE Y Y Y Y Y Y Y M Y Y Y M Figure 1. IgE-dependent mast cell activation. In this example, birch allergen (black star) induces the production of IgE antibodies from B cells (1). These birch-specific IgE-antibodies attach to mast cells by interacting with the FcεRI receptor (2). When the same birch allergen is encountered a second time, IgE-primed mast cells become activated and degranulate (3), thereby releasing mediators that elicit allergic inflammation. Aside from IgE-dependent mast cell activation, mast cells can become activated through many other means. Mast cell activators derive from a wide variety of sources, including viruses, parasites, cytokines, chemokines, chemicals, venoms, endogenous peptides, complement [21], neuropeptides such as substance P [22], IgG [23, 24] fungal components such as zymosan [25], and CD30/CD30L interactions [26]. Studying alternative or IgE-independent routes of mast cell activation is of great importance in order to better understand the different roles mast cells have in innate immune responses. While considering that there are many different types of signals capable of mast cell activation, it is important to remember that mast cells do not aimlessly release all their content when activated. Instead, mast cells release different mediator profiles depending on the triggering factor [27]. This means that a certain stimuli might cause degranulation, while another might induce release of cytokines or chemokines without triggering degranulation. For example, many pathogen products induce release of 3
16 cytokines and chemokines from mast cells, but do not induce degranulation [11]. The ability of mast cells to selectively produce and release mediators means that they can tailor responses as required for a certain situation. This is of particular importance for their role as sentinel cells, as it gives them the opportunity to fine tune mediator release depending on the invading pathogen. In the same way as mast cells can be activated by many different triggers, they also produce and release many different mediators. To simplify, mast cell mediators can be divided into two groups; i) mediators that are preformed and stored in granules and ii) mediators that are synthesized upon activation [21]. Mediators belonging to the first group are released immediately during degranulation, while mediators of the second group can be released minutes to hours following mast cell activation. Mast cell mediators are summarized in figure 2. Activator M Pre-stored Proteases Histamine Heparin Serotonin Cytokines VEGF FGF2 Lipid mediators LTB 4 LTC 4 PGD 2 PGE 2 PAF Figure 2. Examples of mast cell mediators. Cytokines & Chemokines TNF IL-1 IL-6 IL-10 IL-13 IFN- IFN- IFN- GM-CSF IL-8/CXCL8 MCP-1/CCL2 MIP-1/CCL3 MIP-1/CCL4 RANTES/CCL5 MIP-2/CXCL2 KC/CXCL1 Of the pre-stored mediators, different proteases (including tryptases, chymases and carboxypeptidases) constitute the largest group. Other pre-stored mediators include histamine, serotonin, heparin and tumor necrosis factor (TNF) [11, 21, 27]. Mediators synthesized upon activation include lipid mediators such as leukotriene B 4 (LTB 4 ), LTC 4, prostaglandin D 2 (PGD 2 ) and PGE 2 [11] and many different cytokines and chemokines, including TNF, IL-1, IL-3, IL-4, IL-5, IL-6 IL-8/CXCL8, IL-9, IL-10, IL-13, IL-16, GM-CSF, MCP-1/CCL2, MIP-1α/CCL3, IFN-α, IFN-β and IFN-γ [11, 27]. In addition, mast cells can also produce and release antimicrobial peptides such as LL-37 [28]. The ability to selectively release different mediators depending on the activating stimuli underlies the fact that mast cells participate in, and help orchestrate, many different 4
17 responses. These can be beneficial or detrimental, depending on the circumstances. The impact of various mast cell responses are discussed in chapter Mast cell function in health and disease In 2007, Mitch Leslie published a News article in Science entitled Mast cells show their might, in which Leslie stated: Once dismissed as allergy cells, mast cells have proven crucial for immunity. But they ve also shown a dark side [5]. Today, it is clear that mast cells can be beneficial, detrimental, or even fatal, depending on the current setting that they are present in, a fact that renders them particularly interesting targets of research. An overview of mast cell roles in health and disease is depicted in figure 3. In order to understand mast cell function in health and disease, the use of mast celldeficient mice has been an invaluable tool. The two most commonly used strains are referred to as WBB6F1-Kit W/W-v [29] and C57BL/6-Kit W-sh/W-sh [30]. These mice almost completely lack mast cells due to mutations in the c-kit gene, which encodes the receptor for SCF. Comparing results in wild-type mice, mast cell-deficient mice and mast cell knock-in mice has provided important knowledge concerning the role of mast cells in different diseases [31, 32]. In addition, reconstituting mast cell-deficient mice with mast cells deficient in a certain mediator facilitates studies on the role of mast cellderived mediators, for instance TNF [9, 33]. In addition to Kit-mutant mice, two novel mouse models were recently generated in which mast cells are selectively targeted and eradicated using genetic engineering [34, 35], allowing for more precise future studies of mast cell roles in the immune system. When considering the mast cell s characteristics, it is easy to understand why they are now recognized as important sentinel cells. By being pre-positioned in tissues, longlived and able to selectively release inflammatory mediators, mast cells are well equipped for being first hand-responders to different pathogens [36]. The importance of mast cells in bacterial defense has been extensively studied. For instance, mast cells have been shown to be of vital importance in acute bacterial peritonitis models [37], as well as in bacterial clearance after intraperitoneal challenge with enterobacteria [38]. In addition, mast cells protect against other bacteria, such as Helicobacter [39], Pseudomonas [40] and Mycoplasma [41]. Mast cells also seem to have important roles in the defence against viruses and fungi. For instance, mast cells are activated by poly(i:c) (a dsrna analogue), reovirus [42] and dengue virus [43]. In addition, fungal products such as zymosan and fungal extract (from Malassezia sympodialis) also activate mast cells [25, 44, 45]. Supporting a role for mast cells in the recognition of virus and fungi, mast cells express receptors important for the recognition of such pathogens, including toll-like receptor-(tlr)3, TLR7, TLR9 [46], Dectin-1 [25, 44, 45] and Mincle [44]. Pattern recognition receptors (PRRs) such as these are discussed in more detail in chapter 1.2. Even though mast cells have been shown to be able to phagocytose bacteria [38, 47], release antimicrobial peptides [28, 48], form extracellular traps [49] and even act as antigen-presenting cells [11, 50-52], one of their most important functions in host defense might be to promote inflammation. This is achieved for instance by facilitating the recruitment of effector cells such as neutrophils by releasing pro-inflammatory 5
18 cytokines, chemokines and lipid mediators. Examples of when mast cell-derived mediators are important for inflammation are numerous. For instance, TNF derived from mast cells is important for neutrophil infiltration in peritonitis [53], and mast cellderived lipid mediators such as LTB 4 and LTC 4 contribute to early neutrophil influx during bacterial infection [54]. In addition, chemokines secreted by activated mast cells, such as KC/CXCL1, play important roles in mediating neutrophil recruitment during skin inflammation [55]. Due to the same characteristics that renders mast cells efficient in recognizing and responding to pathogens, mast cells are also ideal contributors to wound healing. Indeed, mast cells have been suggested to participate in various stages of wound healing [56]. Aside from their already mentioned ability to initiate inflammation, mast cells are involved in other important aspects of wound healing as well, such as angiogenesis [57] and matrix remodeling [58]. Furthermore, early wound closure is delayed in mast cell deficient-mice, while wound closure, extravasation and neutrophil recruitment are restored upon mast cell reconstitution in these mice [59]. Mast cells are not only important in facilitating processes required for tissue repair; they are also important in actually sensing cell injury. The function of mast cells as sensors of cell injury was suggested already in 1958 by G.B. West [60], but has surprisingly not yet been completely explored. The role of mast cells as sensors of cell injury is discussed in Papers II and IV of this thesis. Beneficial Harmful Effector cell recruitment Allergy & Asthma Parasite & fungal defense Viral defense Bacterial defense Wound healing Venom resistance Homeostasis Inflammation M Anaphylaxis Autoimmunity Skin inflammation Cancer Cardiovascular disease Mastocytosis Inflammation Figure 3. Mast cells can be helpful or detrimental, depending on localization, environment, triggering stimuli, infections and inflammation and other factors. Listed here are some processes where mast cells are involved. Even though mast cell responses are beneficial in many instances, there is also a darker side to mast cell biology, most commonly linked to their involvement in allergies, anaphylactic reactions and asthma, but mast cells are also believed to be involved in diseases such as multiple sclerosis and rheumatoid arthritis (RA) [61]. In addition, mast cells are involved in the development of heart disease and cancer by, for instance, promoting atherosclerosis [62-64] and tumor growth [61], respectively. Evidence has also been presented that connects mast cells to the development of diabetes and dietinduced obesity [65]. 6
19 After allergen-specific IgE-binding and subsequent cross-linking of FcRI-receptors, mast cells are activated and release their content. This causes an immediate or early phase reaction, which has an impact on epithelial, endothelial and smooth muscle cells due to the actions of released histamine, proteoglycans, lipid mediators, tryptase and other mediators. The release of such mediators cause increased vascular permeability, mucus production and smooth muscle contraction [66]. Sometimes, this leads to an anaphylactic shock, which can have fatal outcomes. The immediate phase is followed by late-phase reactions, which are, partly, caused by mediators de novo synthesized and subsequently released by mast cells, such as leukotrienes, prostaglandins and cytokines such as IL-5 and IL-13 [9, 61, 66]. Mast cells also play a fundamental role in asthma, which is a chronic inflammatory disease of the airways characterized by bronchoconstriction, mucus secretion, edema and tissue remodeling. Mast cells contribute to these symptoms by releasing mediators that initiate and sustain inflammation in the airways [67]. Conclusively, mast cells are heterogeneous cells shaped and adapted by their local milieu. They can be activated by a multitude of triggers, and produce selective responses tailored to a certain stimuli. Mast cell activation can sometimes have detrimental effects, but they also function as important pathogen sensors, and are among the first cells to encounter invading pathogens. Aside from their longevity, their ability to rapidly produce pro-inflammatory mediators and their favorable tissue distribution, mast cells are also endowed with a multitude of receptors for sensing pathogens. Such receptors are collectively referred to as PRRs, and constitute an essential part of the innate immune system. 1.2 PATTERN RECOGNITION Germline-encoded PRRs constitute an essential part of the innate immune system, as they allow for the detection of microorganisms. This is achieved by recognizing conserved microbial structures, referred to as PAMPs [2, 68]. The discovery that PAMP recognition by PRRs is essential for the induction of immune responses, made by Charles Janeway [68], represents a key finding in immunology research. There is also accumulating evidence that PRRs are involved in the recognition of endogenous molecules released by damaged cells, so called DAMPs. Up to date, four classes of PRRs have been identified [69]. These include the TLRs, C-type lectin receptors (CLRs), NOD-like receptors (NLRs) and Retinoic acid-inducible gene (RIG)-I-like receptors (RLRs). As an undisputable testament to the importance of PRRs, the discovery of TLRs by Bruce A. Beutler and Jules A. Hoffman was awarded the Nobel Prize in Physiology or Medicine in 2011 (The prize was shared with Ralph M. Steinman for his discovery of DCs) Toll-like receptors TLRs were the first PRRs to be discovered and are thus most extensively studied. So far, 10 TLRs have been identified in humans and 12 in mice, each recognizing PAMPs derived from a wide variety of sources, including bacteria, virus, fungi and parasites [70]. TLRs are expressed both extracellularly (TLR1, TLR2, TLR4, TLR5 and TLR6) and intracellularly in endosomes and lysosomes (TLR3, TLR7, TLR8 and TLR9) [69, 7
20 71]. The TLRs that are expressed extracellularly are involved in the recognition of bacterial membrane components such as lipopolysaccharide (LPS) (TLR4), peptidoglycan (PGN) (TLR2) and flagellin (TLR5). TLR2 also forms heterodimers with TLR1 or TLR6, where TLR2/TLR1 and TLR2/TLR6 recognize triacyl and diacyl lipoproteins, respectively [69]. Intracellular TLRs are implicated in the recognition of nucleic acids such as dsrna (TLR3), ssrna (TLR7 and TLR8) and DNA (TLR9). This is of particular importance for the initiation of antiviral responses, as the triggering of intracellular TLRs often result in the production of type I interferons (IFNs). TLRs are composed of N-terminal leucine-rich repeats (LRRs), followed by a transmembrane region and a cytoplasmic Toll/IL-1R homology (TIR) domain [69]. Upon recognition of a certain PAMP, TLRs initiate signaling events starting with the recruitment of a TIR-domain-containing adaptor molecule such as MyD88, TRIF, TRAM or TIRAP. All TLRs signal through MyD88, except TLR3 which utilizes TRIF, to eventually activate transcription factors such as nuclear factor kappa-light-chainenhancer of activated B cells (NFB) and interferon regulatory factor-(irf)3 to induce production of pro-inflammatory cytokines and IFNs, respectively [70, 72]. TLRs have been mostly studied in APCs such as dendritic cells, but it is becoming increasingly clear that TLRs play important roles in a wide range of cell types, including B cells and mast cells. For instance, it has been demonstrated that mast celldeficient mice reconstituted with TLR-mutated bone marrow-derived mast cells (BMMCs) display higher mortality than mice reconstituted with wild-type BMMCs after cecal-ligation and puncture-induced peritonitis [73]. Furthermore, the TLR4 ligand LPS has been shown to induce production of several cytokines in mast cells, such as IL-1, TNF-, IL-6, IL-10 and IL-13 [73-75], while treatment of mast cells with the TLR2 ligand PGN induces TNF, IL-4, IL-5 and IL-13, but not IL-1 [75]. These types of cytokine responses have also been shown to be synergistically enhanced during IgE cross-linking [74]. It has also been shown in one study that TLR2- but not TLR4-dependent mast cell activation results in degranulation [75]. This further exemplifies that mast cell responses can be fine-tuned depending on stimuli type [75]. While many studies on TLRs and mast cells have been conducted in a murine system, it has also been described that human cord blood-derived mast cells (CBMCs) express mrna for TLR1, TLR2 and TLR6, but not TLR4 [76]. CBMCs do not respond to LPS [76] unless primed by IL-4 [77], and this also requires the presence of serum components such as CD Nod-like receptors The NLRs are cytosolic sensors of PAMPs and DAMPs, and they can be divided into three subgroups: NODs (nucleotide-binding oligomerization domain), NLRPs/NALPs (NACHT, LRR and PYD-containing domain) and IPAFs (ICE-protease-activating factor) [78]. Some NLRs form large cytoplasmatic complexes termed inflammasomes, and are involved in proteolytic activation of the inflammatory cytokines IL-1 and IL-18. Proteins of the NLR family utilize LRRs (similarly to TLRs), as well as nucleotide-binding domains (NBD) which are thought to be involved in PAMP recognition [79]. Other domains common to NLR proteins include the caspase activation and recruitment domains (CARDs) and pyrin domains (PYDs). Two of the 8
21 first NLRs to be described, and thus most widely studied, are NOD1 and NOD2 [78-81]. NOD1 and NOD2 function as intracellular PRRs and recognize PGN, a component of bacterial cell walls. NOD1 recognizes muropeptides (ie-daps), found mainly in PGN of Gram-negative bacteria, while NOD2 recognizes muramyl dipeptide (MDP), found in both Gram-positive and Gram-negative bacteria [78]. Interestingly, it was recently demonstrated that ssrna activates NOD2 [82], indicating that new NOD ligands from different sources are likely to be found in the future. Both NOD1 and NOD2 recruit the kinase RIP2 upon activation, which subsequently activates NFB, and eventually results in production of pro-inflammatory cytokines [79]. As stated above, several members of the NLR family form cytosolic multiprotein complexes called inflammasomes [83, 84]. Examples of inflammasomes are NACHT, LRR and PYD-containing protein-(nlrp)1, NLRP3 and Absent in melanoma-(aim)2, which function as sensors of endogenous or exogenous PAMPs and DAMPs. In general, inflammasomes are though to be activated by a wide range of compounds, including DAMPs (uric acid crystals, adenosine triphosphate (ATP)), PAMPs (bacteria, virus, parasites) and environmental agents (silica, asbestos, alum) [78]. It is not yet completely understood how inflammasomes are activated in vivo, but inflammasome activation is thought to be achieved in two steps [79, 85], and is best studied in the NLRP3 inflammasome (which belongs to the NALP subgroup of NLRs). The first step is though to be provided by TLR and/or NLR signaling, which initiates expression of NLRP3, as well as transcription of important components such as pro-caspase-1, proil-1 and proil-18 [79]. The second step, which is not yet fully understood, involves interactions between the activator and the inflammasome, and result in inflammasome assembly which eventually drives the release of active IL-1 and IL-18. Very little is known about the role for NLRs in mast cells responses, but it has been demonstrated that mouse mast cells express inflammasome components: Casp1 and Asc are constitutively expressed in BMMCs, while Nlrp3 and Il1b are inducible by LPS treatment [86]. In humans, it has been shown that the numbers of intestinal NOD2 + mast cells are significantly increased in patients with Crohn s disease [87]. The role of NOD1 in human CBMCs is discussed in Paper I in this thesis. Given the roles of mast cells in innate immunity, it is clear that in time, much will be learned about the role of NLRs in mast cells C-type lectin receptors The term C-type lectin was originally used to separate Ca 2+ -dependent and independent carbohydrate binding lectins. CLRs initiate responses to pathogens by recognizing mannose, fucose and glucan carbohydrate structures. Thus, CLRs can recognize several types of pathogens including virus, fungi, mycobacteria and helminths [88]. For instance, mannose-structures are present in virus, fungi and bacteria, fucose structures in helminths (and some bacteria), and glucans are present in cell walls of fungi, plants and mycobacteria. Since all pathogens express different sets of PAMPs, these PAMP profiles elicit different immune responses. This is reflected also in CLR signaling, where activation can lead to direct gene expression through NFκB activation, or to modulation of for instance TLR signaling mechanisms [88-91]. Pathogen recognition 9
22 through CLRs leads to pathogen internalization, followed by degradation and subsequent antigen presentation. Therefore, CLRs have so far mainly been studied in DCs. The mannose receptor [92] and Langerin [93] recognize high-mannose and fucose, and these were among the first CLRs to be shown to detect pathogens [91]. Since then, many different CLRs have been described, including Mincle, dectin-1, dectin-2 and DC-SIGN. Dectin-1 recognizes β-glucans in fungal cell walls, while dectin-2 binds high-mannose and α-mannans, for instance in C. albicans, M. tuberculosis and S. cerevisiae. DC-SIGN is expressed by myeloid DCs and can recognize many different pathogens such as mycobacteria, C. albicans and Leishmania spp. through mannose and fucose recognition. SIGNR3 is the closest mouse homologue of human DC-SIGN. Mincle is a CLR mainly expressed by macrophages, and recognizes α-mannans which allows for recognition of for instance C. albicans and Malasezzia spp [91]. Interestingly, Mincle is a PRR capable of responding also to endogenous danger signals. For instance, it has been demonstrated that Mincle-expressing cells respond to SAP130, a small nuclear ribonucleoprotein released by dead cells [94]. In addition, DNGR-1 (also known as CLEC9A) is a CLR with no known PAMP ligand, but binds a yet uncharacterized endogenous ligand released upon necrosis [91, 95]. Currently, the knowledge about CLRs in mast cells is very limited. However, human mast cells have been shown to express Mincle [44], and the mrna levels were upregulated upon treatment with M. sympodialis extract. Likewise, human mast cells express dectin-1 [25, 44], and respond to treatment with zymosan and A. fumigatus hyphae with leukotriene production and IgE-independent degranulation [96], respectively Retinoic acid-inducible gene (RIG)-I-like receptors RLRs are cytoplasmatic PRRs implicated in antiviral immunity as important sensors of viral RNA, but represent the least characterized class of the PRRs. RLR detection of viral components leads to signaling mechanisms eventually resulting in IFN production required for controlling virus infections. To date, only three RLRs have been identified: retinoic acid-inducible gene I (RIG-I), melanoma differentiation associated factor 5 (MDA5) and laboratory of genetics and physiology 2 (LGP2) [97]. RIG-I and MDA5 are expressed in many tissues and share several structural domains, including CARD, a RNA helicase domain, and a C-terminal repressor domain. LGP2 lacks CARD, and is thought to function as a regulator of RIG-I and MDA5 [97, 98]. RIG-I detects many different viruses, including members of Paramyxoviridae, Orthomyxoviridae, Coronaviridae and Caliciviridae, and also DNA viruses such as Epstein-Barr virus, while MDA5 responds to Picornaviridae. There are also some viruses that are detected by both receptors, including West Nile virus, reovirus and dengue virus [97]. RLR signaling is to date not fully understood, but both RIG-I and MDA5 form CARD-CARD interactions with IPS-1 (an adaptor protein) upon recognition of viral PAMPs. IPS-1 forms a signalosome complex with IRF3 and IRF7, which together with NFκB mediate production of type I IFNs [97]. 10
23 As is the case with mast cells and CLRs, the functions of RLRs in mast cells are to date largely unknown. However, some studies have emerged in which this issue is addressed. For instance, mast cells have been shown to be activated by dengue virus [43, 99]. In a recent study by St John et al., it was shown that both RIG-I and MDA5 were activated in mast cells treated with dengue virus and that this led to mast cell degranulation and de novo synthesis of TNF and IFN [99]. In addition, mast celldeficient mice infected sub-cutaneously with dengue virus displayed increased viral burdens in lymph nodes compared to mast cell-sufficient mice, suggesting mast cells to be important in fighting the viral infection. PRR-mediated recognition of PAMPs represents a cornerstone in immunology, as it is a prerequisite for innate responses to pathogens and also represents an important step in the induction of adaptive immune responses. Importantly, it is becoming increasingly clear that mast cells participate in pathogen recognition by utilizing PRRs such as those described in this chapter. While individual functions of the four classes of PRRs are becoming better and better characterized, much remains to be learned concerning their cross-talk, and how these receptors modulate and regulate each other. When a pathogen is encountered, many different PAMPs are detected by different sets of PRRs. Therefore, it is now clear that cross-talk between different PRRs is essential in order to mount proper immune responses to a given pathogen. 1.3 DAMAGE RECOGNITION While pathogen recognition through PRRs initiates inflammatory responses, pathogens are not the only cause of inflammation; damage, or trauma, is another one. Blunt trauma is a good example, where inflammation is rapidly initiated without pathogens having entered the body. The question is how the immune system can respond to injured cells, thus initiating repair mechanisms and eventually restoring tissue homeostasis? Polly Matzinger, a pioneer in the field of immunology in general, and DAMPs in particular, once stated that the immune system needs to concern itself with two questions when faced with a threat; i) to respond or not, and ii) if the answer is yes, what kind of response should be initiated [100]? During the years, different models have been proposed to answer such questions [3]. One important model was the Infectious-nonself model, proposed by Janeway in 1989 [68]. This model stated that APCs, such as DCs, are not constantly active, but are resting until activated by PAMP recognition utilizing different PPRs. Thus, this model described how APCs could discriminate between infectious-nonself and noninfectious-self [3, 101]. However, as pointed out by Matzinger, this model does not answer questions concerning why transplants are rejected, why alum works as an adjuvant (since it is non-microbial), or what induces autoimmunity. In an attempt to provide a model capable of answering such questions, Matzinger, in 1994, proposed the Danger model [102]. This model suggested that the immune system is more concerned about recognizing damagecausing substances rather than only foreign substances. Importantly, it was proposed that APCs can be activated not only by PAMPs, but also by danger/alarm signals released by cells undergoing for instance mechanical injury or injury caused by pathogen exposure [3]. 11
24 In 2000, Shi et al. found that injecting dead/dying cells provided a strong adjuvant activity, and that the adjuvant activity was present in the cytosol, releasable for instance by mechanical rupture [103, 104]. This finding emphasizes the concept underlying the Danger model, and indeed, during the last decade, many different endogenous danger signals (or DAMPs) have been characterized, providing additional validity to the danger model. Different DAMPs are discussed in chapter Endogenous danger signals A paramount function of the immune system is to monitor the health status of different cells. In this context, cell death (other than apoptotic death) is heralding trouble; a sign of alarm that needs to be recognized and responded to. Responses to injured or killed cells, aiming at repair and a return to tissue homeostasis, can be initiated by the recognition of intracellular molecules exposed as a result of cell injury or death. Thus, an important characteristic of endogenous danger signals is that they should not be released by healthy cells. Of all DAMPs characterized so far, high-mobility group box 1 protein (HMGB1) is perhaps most extensively studied. HMGB1 functions as a chromatin-binding nuclear factor, but can also be secreted and initiate inflammatory responses [105]. Importantly, release of HMGB1 by necrotic cells has been demonstrated to generate an inflammatory response [106]. Here, bone marrow cells were challenged with dead wild-type or HMGB1 -/- fibroblasts. Interestingly, while treatment with dead wild-type fibroblasts triggered a TNF response, this was not observed using HMGB1 -/- fibroblasts, or apoptotic wild-type fibroblasts, clearly demonstrating that HMGB1 released from necrotic cells initiates inflammation. In parallel, another group demonstrated similar findings, where also HMGB1-blocking reduced activation induced by necrotic cells [107]. As mentioned in chapter 1.3, Shi and colleagues demonstrated that dead cells possessed adjuvant activity of unknown identity [103]. In a later study by the same group, the cytosol of irradiated 3T3 fibroblasts was fractionated and individual fractions were tested for adjuvant activity [108]. One single fraction was responsible for most of the activity, and identified as uric acid by using mass spectrometry. In line with this finding, the adjuvant activity of necrotic fibroblasts could be decreased if the cells were pre-treated with allopurinol (an inhibitor of uric acid formation) or uricase [108]. Thus, the authors of this study identified uric acid as an important endogenous danger signal released by necrotic cells. Aside from HMGB1 and uric acid, several additional compounds of different origin have been described as endogenous danger signals. For instance, necrotic cells have been shown to release heat shock proteins (HSPs) such as HSP70 [109], and SAP130 (a ribonucloprotein recognized by Mincle) [94]. Also DNA [110], RNA [111] and ATP [112] can act as DAMPs. 12
25 It is interesting to note that several endogenous danger signals are detected by receptors previously thought to react only to foreign molecules (PAMPs). For example, HMGB1 signals through TLR2, TLR4, TLR9 and RAGE (receptor for advanced glycation endproducts) [113], self RNA-complexes can be detected by TLR7 and TLR8 [111], SAP130 by Mincle [94], hyaluronan fragments by TLR2 [114] and Granulysin by TLR4 [115]. Thus, several PPRs have over-lapping functions and are capable of eliciting inflammatory responses both in response to pathogens, but also in response to endogenous compounds released by necrotic cells. IL-1α is another endogenous danger signal released upon necrosis, and has important functions in subsequent neutrophil recruitment [116] and initiation of inflammation [117]. Interestingly, another cytokine of the IL-1-family, IL-33, has been suggested to function as an alarmin [118, 119]. IL-33 biology, its role in the immune system, and its role as a danger signal is discussed in chapter 1.4. Furthermore, IL-33-mediated mast cell responses are discussed in Papers II-IV. To summarize this chapter, endogenous danger signals are compounds exposed or released by damaged or dead cells as a consequence of infection or trauma. The release of such danger signals functions as a warning signal to the immune system, and allows for damage recognition and actions aiming at containing the damage, and eventually repairing the damaged tissue. Due to their ability to instigate innate responses as well as present antigens to T-cells and thus initiate adaptive responses, recognition and responses to danger signals have largely been studied in DCs. However, a key hypothesis in this thesis is that mast cells also are important sensors of cell injury, based on mast cell characteristics such as a pre-positioning in tissues, their ability to selectively secrete mediators upon activation and their longevity. 1.4 IL-33 IL-33 is a recently discovered member of the IL-1 family of cytokines, and signals through the T1/ST2 receptor [120]. Originally, IL-33 was thought mainly to be involved in induction of T helper 2 (Th2) responses, but many additional functions for this cytokine have been discovered. IL-33 is a potent activator of several immune cells (including mast cells), and is involved in the pathogenesis of several diseases, but it does also mediate protective functions. Interestingly, IL-33 has been shown to function as an endogenous danger signal IL-33 expression and signaling In 2005, IL-33 was characterized by Schmitz et al. [120] as a member of the IL-1 family of cytokines, together with IL-1, IL-18 and IL-1RA. Two years prior to this study, Baekkevold et al. characterized a nuclear factor expressed in high endothelial venules, termed NF-HEV [121], which was later shown to be identical to IL-33 [122]. IL-33 is expressed in many different tissues and organs, especially by structural cell types such as epithelial cells [123], endothelial cells, fibroblasts, keratinocytes [118], airway smooth muscle cells [124] and astrocytes [125]. IL-33 is also expressed in osteoblasts [126, 127], adipocytes [126, 128], monocytes [129] and pancreatic stellate cells [130]. In some cell types, pro-inflammatory stimuli such as LPS can up-regulate IL-33 mrna and protein levels [129]. 13
26 The nuclear role of IL-33 is still incompletely understood. However, it has been demonstrated that IL-33 can associate with heterochromatin in the nucleus, where it exerts transcriptional repression [122]. In addition, IL-33 has been shown to interact with the p65 subunit of NFκB, thus reducing NFκB-triggered gene expression [131]. The recent generation of IL-33 -/- mice [132] will definitively be an important tool in future studies seeking to further investigate nuclear roles of IL-33. The IL-33 receptor consists of two subunits; IL-1R accessory protein (IL-1RAcP) and T1/ST2 [133]. While IL-1RAcP is utilized also by IL-1RI [134], T1/ST2 is specific for IL-33, and was for a long time an orphan receptor until Schmitz et al. identified IL-33 as its ligand [120]. T1/ST2 was originally described as a stable surface marker expressed by Th2 but not Th1 cells, and readily used to distinguish between these cell types [135]. Besides Th2 cells, mast cells were early on shown to strongly express T1/ST2 [136]. Complex formation between T1/ST2 and IL-1RAcP is essential for functional IL-33 signalling [133]. For instance, IL-1RAcP -/- mast cells secrete reduced cytokine levels compared to wild-type mast cells after IL-33 treatment [137], and the use of neutralizing antibodies targeting IL-1RAcP abrogates mast cell responses to IL-33 [138]. The IL-33/ST2 signalling pathway involves recruitment of MyD88, IRAK, IRAK4 and TRAF6, eventually resulting in NFκB activation [120]. TRAF6 has been shown to be a crucial component in this signalling pathway, as activation of NFκB, p38 and JNK was absent when TRAF6 -/- fibroblasts were stimulated with IL-33 [139]. Additionally, JAK2 -/- fibroblasts fail to induce IκBα degradation and NFκB activation upon IL-33 stimulation, suggesting this tyrosine kinase to be of importance in the signalling mechanism of IL-33 [140]. While IL-1β and IL-18, two other members of the IL-1 family of cytokines, both require proteolytical processing by caspase-1 in order to be rendered biologically active [134], this does not seem to be the case for IL-33. Instead, full-length IL-33 (IL , ~30kDa) has been reported by several studies to be biologically active [ ], thus clearly distinguishing IL-33 from IL-1β and IL-18. This characteristic provides one explanation for the proposed role of IL-33 as an endogenous danger signal, a role discussed further in chapter Initially, caspase-1-processing was also thought to be required for IL-33 [120], until several studies demonstrated that IL-33 was a poor substrate for caspase-1 [141, 143, 144]. Consequently, proteolytical processing of IL-33 has been a much debated subject. For instance, one study reported calpain to be mediating IL-33 processing in vivo [145], while another study observed IL-33 release in macrophages treated with inhibitors of both calpain and caspase-8, as well as in caspase-1 -/- cells [146]. Furthermore, IL-33 has even been shown to be inactivated by caspase-1 [142] as well as by the apoptotic caspases caspase-3 and caspase-7 [143]. Many published studies have utilized an artificially truncated form of IL-33 (IL , ~18kDa). While this shorter form of IL-33 can activate T1/ST2 similarly to full-length IL-33 [143], it remains unclear whether the shorter form is produced naturally. 14
Innate Immunity & Inflammation
 Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
2. Innate immunity 2013
 1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
Chapter 3 The Induced Responses of Innate Immunity
 Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Innate Immunity. Chapter 3. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples. Antimicrobial peptide psoriasin
 Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Innate immunity. Abul K. Abbas University of California San Francisco. FOCiS
 1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Innate Immunity. Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016
 Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Role of Innate Immunity in Control of Adaptive Immunity
 Role of Innate Immunity in Control of Adaptive Immunity Innate Immunity The burden of pathogen sensing is placed on the innate immune system Danger hypothesis Missing Self Based on the detection of molecular
Role of Innate Immunity in Control of Adaptive Immunity Innate Immunity The burden of pathogen sensing is placed on the innate immune system Danger hypothesis Missing Self Based on the detection of molecular
Innate Immunity. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples Chapter 3. Antimicrobial peptide psoriasin
 Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
Lecture on Innate Immunity and Inflammation
 Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Identification of Microbes
 Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
Structure and Function of Antigen Recognition Molecules
 MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics
 Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Innate Immunity. Jan 8 th Prof. dr. sc. Ivana Novak Nakir 1
 Innate Immunity Jan 8 th 2018. Prof. dr. sc. Ivana Novak Nakir 1 Adaptive Innate 2 Immune system overview 1 st line of defense skin (2m 2 ) and mucosal membranes (~400m 2 ): physical barrier, lymphoid
Innate Immunity Jan 8 th 2018. Prof. dr. sc. Ivana Novak Nakir 1 Adaptive Innate 2 Immune system overview 1 st line of defense skin (2m 2 ) and mucosal membranes (~400m 2 ): physical barrier, lymphoid
Immunology Part II. Innate Immunity. 18. April 2018, Ruhr-Universität Bochum Marcus Peters,
 Immunology Part II Innate Immunity 18. April 2018, Ruhr-Universität Bochum Marcus Peters, marcus.peters@rub.de Conserved structures of pathogens PAMPs are detected by Pattern Recognition Receptors PRRs
Immunology Part II Innate Immunity 18. April 2018, Ruhr-Universität Bochum Marcus Peters, marcus.peters@rub.de Conserved structures of pathogens PAMPs are detected by Pattern Recognition Receptors PRRs
Lecture on Innate Immunity and Inflammation. Innate Immunity: An Evolutionary View
 Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
1. The scavenger receptor, CD36, functions as a coreceptor for which TLR? a. TLR ½ b. TLR 3 c. TLR 4 d. TLR 2/6
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Innate Immunity: (I) Molecules & (II) Cells
 Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Innate Immunity. Natural or native immunity
 Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS
 TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS A/PROF WILLIAM SEWELL ST VINCENT S CLINICAL SCHOOL, UNSW SYDPATH, ST VINCENT S HOSPITAL SYDNEY GARVAN INSTITUTE INNATE VERSUS ADAPTIVE IMMUNE RESPONSES INNATE
TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS A/PROF WILLIAM SEWELL ST VINCENT S CLINICAL SCHOOL, UNSW SYDPATH, ST VINCENT S HOSPITAL SYDNEY GARVAN INSTITUTE INNATE VERSUS ADAPTIVE IMMUNE RESPONSES INNATE
Intrinsic cellular defenses against virus infection
 Intrinsic cellular defenses against virus infection Detection of virus infection Host cell response to virus infection Interferons: structure and synthesis Induction of antiviral activity Viral defenses
Intrinsic cellular defenses against virus infection Detection of virus infection Host cell response to virus infection Interferons: structure and synthesis Induction of antiviral activity Viral defenses
Journal club. Lama Nazzal
 Journal club Lama Nazzal Background Kidney stone disease affects about 12% of men and 5% of women during their lifetimes in the United States Intrarenal nephrocalcinosis is often asymptomatic, but can
Journal club Lama Nazzal Background Kidney stone disease affects about 12% of men and 5% of women during their lifetimes in the United States Intrarenal nephrocalcinosis is often asymptomatic, but can
The Innate Immune Response
 The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Innate immunity. Monika Raulf. Lecture Tasks of the immune system. Body protection against damaging influences
 Innate immunity Monika Raulf Lecture 20.04.2016 Tasks of the immune system Body protection against damaging influences Deployment of a strong defense 2 The line of defence Skin Mucosa Sweat Digestive fluids
Innate immunity Monika Raulf Lecture 20.04.2016 Tasks of the immune system Body protection against damaging influences Deployment of a strong defense 2 The line of defence Skin Mucosa Sweat Digestive fluids
Innate Immunity. Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017
 Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017 Objectives: Explain how innate immune system recognizes foreign substances
Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017 Objectives: Explain how innate immune system recognizes foreign substances
PBS Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs , 27-30
 PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
The Lymphatic System and Body Defenses
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
Immune System. Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka
 Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
JPEMS Nantes, Basic Immunology INNATE IMMUNITY
 JPEMS Nantes, 2014- Basic Immunology INNATE IMMUNITY Teacher: Pr. Régis Josien, Laboratoire d Immunologie and INSERM U1064, CHU Nantes Regis.Josien@univ-nantes.fr 1 Contents 1. General features and specificity
JPEMS Nantes, 2014- Basic Immunology INNATE IMMUNITY Teacher: Pr. Régis Josien, Laboratoire d Immunologie and INSERM U1064, CHU Nantes Regis.Josien@univ-nantes.fr 1 Contents 1. General features and specificity
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity
 1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
1. Overview of Adaptive Immunity
 Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
Chapter 1. Chapter 1 Concepts. MCMP422 Immunology and Biologics Immunology is important personally and professionally!
 MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
Macrophage Activation & Cytokine Release. Dendritic Cells & Antigen Presentation. Neutrophils & Innate Defense
 Macrophage Activation & Cytokine Release Dendritic Cells & Antigen Presentation Neutrophils & Innate Defense Neutrophils Polymorphonuclear cells (PMNs) are recruited to the site of infection where they
Macrophage Activation & Cytokine Release Dendritic Cells & Antigen Presentation Neutrophils & Innate Defense Neutrophils Polymorphonuclear cells (PMNs) are recruited to the site of infection where they
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System Multiple-Choice Questions
 Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
Campbell's Biology: Concepts and Connections, 7e (Reece et al.) Chapter 24 The Immune System 24.1 Multiple-Choice Questions 1) The body's innate defenses against infection include A) several nonspecific
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
Innate Immunity II. Integration. Lindsay Nicholson Advanced Immunology L2
 Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Inflammation: How to Cool the Fire Inside your Gut? REINVENTING DIAGNOSTICS
 Inflammation: How to Cool the Fire Inside your Gut? REINVENTING DIAGNOSTICS Future of Healthcare REINVENTING DIAGNOSTICS Inflammation Gut Inflammation Basis of a Healthy
Inflammation: How to Cool the Fire Inside your Gut? REINVENTING DIAGNOSTICS Future of Healthcare REINVENTING DIAGNOSTICS Inflammation Gut Inflammation Basis of a Healthy
Innate Immunity: (I) Molecules & (II) Cells. Part II: Cells (aka the Sentinels)
 Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
The Adaptive Immune Response. B-cells
 The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
MICR2209. Innate Immunity. Dr Allison Imrie
 MICR2209 Innate Immunity Dr Allison Imrie allison.imrie@uwa.edu.au Synopsis: In this lecture we will review the different mechanisms which consbtute the innate immune response, and examine the major cells
MICR2209 Innate Immunity Dr Allison Imrie allison.imrie@uwa.edu.au Synopsis: In this lecture we will review the different mechanisms which consbtute the innate immune response, and examine the major cells
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Body Defense Mechanisms
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 13 Body Defense Mechanisms Lecture Presentation Anne Gasc Hawaii Pacific University and University of
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology
 Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
Chapter 13 Lymphatic and Immune Systems
 The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
The Chapter 13 Lymphatic and Immune Systems 1 The Lymphatic Vessels Lymphoid Organs Three functions contribute to homeostasis 1. Return excess tissue fluid to the bloodstream 2. Help defend the body against
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD.
 Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
11/25/2017. THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS BARRIER DEFENSES INNATE IMMUNITY OF VERTEBRATES
 THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
Innate Immunity. Natural or native immunity
 Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition. Lipopolysaccharide = Lipid + Polysaccharide
 The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition Lipopolysaccharide = Lipid + Polysaccharide E.coli Cell wall organization Lipopolysaccharide Outer membrane
The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition Lipopolysaccharide = Lipid + Polysaccharide E.coli Cell wall organization Lipopolysaccharide Outer membrane
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host.
 Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Immune System AP SBI4UP
 Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
Immune System AP SBI4UP TYPES OF IMMUNITY INNATE IMMUNITY ACQUIRED IMMUNITY EXTERNAL DEFENCES INTERNAL DEFENCES HUMORAL RESPONSE Skin Phagocytic Cells CELL- MEDIATED RESPONSE Mucus layer Antimicrobial
Understanding basic immunology. Dr Mary Nowlan
 Understanding basic immunology Dr Mary Nowlan 1 Immunology Immunology the study of how the body fights disease and infection Immunity State of being able to resist a particular infection or toxin 2 Overview
Understanding basic immunology Dr Mary Nowlan 1 Immunology Immunology the study of how the body fights disease and infection Immunity State of being able to resist a particular infection or toxin 2 Overview
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Innate Immunity. Bởi: OpenStaxCollege
 Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
General Biology. A summary of innate and acquired immunity. 11. The Immune System. Repetition. The Lymphatic System. Course No: BNG2003 Credits: 3.
 A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
A summary of innate and acquired immunity General iology INNATE IMMUNITY Rapid responses to a broad range of microbes Course No: NG00 Credits:.00 External defenses Invading microbes (pathogens). The Immune
Fc receptors, phagocytosis role 128
 Subject Index Adaptive immunity dependence on innate immunity 9, 10 evolution 10 Aging anti-inflammatory agents in counteraction 202 beneficial polymorphisms 199 201 definition 18, 189 innate immunity
Subject Index Adaptive immunity dependence on innate immunity 9, 10 evolution 10 Aging anti-inflammatory agents in counteraction 202 beneficial polymorphisms 199 201 definition 18, 189 innate immunity
Immune System. Biol 105 Lecture 16 Chapter 13
 Immune System Biol 105 Lecture 16 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Immune System Biol 105 Lecture 16 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Blood and Immune system Acquired Immunity
 Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
Blood and Immune system Acquired Immunity Immunity Acquired (Adaptive) Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
Acquired Immunity Cells are initially and require before they can work Responds to individual microbes
 1 of 10 THE IMMUNE SYSTEM CHAPTER 43; PAGES 898 921 WHY DO WE NEED AN IMMUNE SYSTEM? It s a dirty, dirty world out there and we are vastly outnumbered Bacteria and parasites are everywhere The body has
1 of 10 THE IMMUNE SYSTEM CHAPTER 43; PAGES 898 921 WHY DO WE NEED AN IMMUNE SYSTEM? It s a dirty, dirty world out there and we are vastly outnumbered Bacteria and parasites are everywhere The body has
Unit 5 The Human Immune Response to Infection
 Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
Unit 5 The Human Immune Response to Infection Unit 5-page 1 FOM Chapter 21 Resistance and the Immune System: Innate Immunity Preview: In Chapter 21, we will learn about the branch of the immune system
Internal Defense Notes
 Internal environment of animals provides attractive area for growth of bacteria, viruses, fungi Harm via: 1. destruction of cells 2. production of toxic chemicals To protect against foreign invaders, humans
Internal environment of animals provides attractive area for growth of bacteria, viruses, fungi Harm via: 1. destruction of cells 2. production of toxic chemicals To protect against foreign invaders, humans
Innate Immunity. By Dr. Gouse Mohiddin Shaik
 Innate Immunity By Dr. Gouse Mohiddin Shaik Types of immunity Immunity Innate / inborn Non-specific Acquired / adaptive Specific 3rd line of defense Physical barriers Skin, Saliva, Mucous, Stomach acid,
Innate Immunity By Dr. Gouse Mohiddin Shaik Types of immunity Immunity Innate / inborn Non-specific Acquired / adaptive Specific 3rd line of defense Physical barriers Skin, Saliva, Mucous, Stomach acid,
Immune System. Biol 105 Chapter 13
 Immune System Biol 105 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Immune System Biol 105 Chapter 13 Outline Immune System I. Function of the Immune system II. Barrier Defenses III. Nonspecific Defenses A. Immune system cells B. Inflammatory response C. Complementary
Adaptive Immunity: Humoral Immune Responses
 MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
WHY IS THIS IMPORTANT?
 CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
生命科学基础 (21)- 动物的免疫器官. The Immune System. KE, Yuehai 柯越海. Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院
 生命科学基础 (21)- 动物的免疫器官 The Immune System KE, Yuehai 柯越海 Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院 Outlines The Immune System 1. Innate immunity 2. Adaptive immunity 3. Immune
生命科学基础 (21)- 动物的免疫器官 The Immune System KE, Yuehai 柯越海 Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院 Outlines The Immune System 1. Innate immunity 2. Adaptive immunity 3. Immune
Innate vs Adaptive Response
 General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
General Immunology Innate vs Adaptive Response Innate- non-specific (4 types of barriers) anatomic- ato mechanical ca (skin), ph, mucous, normal flora Physiologic- temperature, ph, chemicals (lysozyme,
Physiology Unit 3. ADAPTIVE IMMUNITY The Specific Immune Response
 Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Gout and Nucleic Acid Metabolism Vol.33 No
 Gout and Nucleic Acid Metabolism Vol.33 No.1 2009 1 1 2 3 in vitro 14 IgM 1 IgM IgM 1 PAMPs Pattern recognition receptors PRRs PRRs PRRs PAMPs Toll Toll-like receptor TLR PAMPs Nod Nod-like receptor NLR
Gout and Nucleic Acid Metabolism Vol.33 No.1 2009 1 1 2 3 in vitro 14 IgM 1 IgM IgM 1 PAMPs Pattern recognition receptors PRRs PRRs PRRs PAMPs Toll Toll-like receptor TLR PAMPs Nod Nod-like receptor NLR
General Overview of Immunology. Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center
 General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
chapter 17: specific/adaptable defenses of the host: the immune response
 chapter 17: specific/adaptable defenses of the host: the immune response defense against infection & illness body defenses innate/ non-specific adaptable/ specific epithelium, fever, inflammation, complement,
chapter 17: specific/adaptable defenses of the host: the immune response defense against infection & illness body defenses innate/ non-specific adaptable/ specific epithelium, fever, inflammation, complement,
The Skinny of the Immune System
 The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases
 محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
Chapter 10 (pages ): Differentiation and Functions of CD4+ Effector T Cells Prepared by Kristen Dazy, MD, Scripps Clinic Medical Group
 FIT Board Review Corner September 2015 Welcome to the FIT Board Review Corner, prepared by Andrew Nickels, MD, and Sarah Spriet, DO, senior and junior representatives of ACAAI's Fellows-In-Training (FITs)
FIT Board Review Corner September 2015 Welcome to the FIT Board Review Corner, prepared by Andrew Nickels, MD, and Sarah Spriet, DO, senior and junior representatives of ACAAI's Fellows-In-Training (FITs)
immunity defenses invertebrates vertebrates chapter 48 Animal defenses --
 defenses Animal defenses -- immunity chapter 48 invertebrates coelomocytes, amoebocytes, hemocytes sponges, cnidarians, etc. annelids basophilic amoebocytes, acidophilic granulocytes arthropod immune systems
defenses Animal defenses -- immunity chapter 48 invertebrates coelomocytes, amoebocytes, hemocytes sponges, cnidarians, etc. annelids basophilic amoebocytes, acidophilic granulocytes arthropod immune systems
D2 inhibits TLR2- initiated 12p40 transcription (-) TLR2 PGN MDP. MyD88 IRAK ECSIT TRAF6 NIK. Smallest unit of PGN muramyl dipeptide IKK.
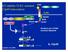 D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
Chapter 21: Innate and Adaptive Body Defenses
 Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Chapter 43. Immune System. phagocytosis. lymphocytes. AP Biology
 Chapter 43. Immune System phagocytosis lymphocytes 1 Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against unwelcome invaders viruses protists
Chapter 43. Immune System phagocytosis lymphocytes 1 Why an immune system? Attack from outside lots of organisms want you for lunch! animals must defend themselves against unwelcome invaders viruses protists
