Oral tacrolimus for pediatric steroid-resistant ulcerative colitis
|
|
|
- Marion McCormick
- 5 years ago
- Views:
Transcription
1 Journal of Crohn's and Colitis (2014) 8, Available online at ScienceDirect Oral tacrolimus for pediatric steroid-resistant ulcerative colitis V.M. Navas-López, J. Blasco Alonso, M.J. Serrano Nieto, F. Girón Fernández-Crehuet, M.D. Argos Rodriguez, C. Sierra Salinas Pediatric Gastroentrology and Nutrition Unit, Hospital Materno Infantil, Málaga, Spain Received 21 November 2012; received in revised form 12 March 2013; accepted 13 March 2013 KEYWORDS Ulcerative colitis; Tacrolimus; Surgery; Steroids; Children; Paediatric Abstract Background: Ulcerative colitis (UC) occurring during childhood is generally extensive and is associated with severe flares that may require intravenous steroid treatment. In cases of corticosteroid resistance is necessary to introduce a second-line treatment to avoid or delay surgery. Aims: To describe the efficacy and safety of oral tacrolimus for the treatment of severe steroid-resistant UC. Methods: We performed a retrospective study that included all patients under age 18 suffering from severe steroid-resistant UC treated with oral tacrolimus during the period January 1998 to October 2012 and with a follow-up period after treatment of 24 months or more. Results: A total of ten patients were included. The age at baseline was 9.4 ± 4.9 years, and the time from diagnosis was 1.3 months (IQR, 1 5.7). Seven of the patients were in their first flare of disease. All of them received an oral dose of 0.12 mg/kg/day of tacrolimus divided in two doses. Trough plasma levels of tacrolimus were maintained between 4 and 13 ng/ml. Response was seen in 5/10 patients at 12 months, colectomy was eventually performed in 60% of patients during the follow-up period. Conclusions: Tacrolimus is useful in inducing remission in patients with severe steroid-resistant UC, preventing or delaying colectomy, and allowing the patient and family to prepare for a probable surgery. Tacrolimus may also be used as a treatment bridge for corticosteroid-dependent patients until the new maintenance therapy takes effect European Crohn's and Colitis Organisation. Published by Elsevier B.V. All rights reserved. Conference presentation: ECCO 2012, Barcelona, Spain. Corresponding author at: Pediatric Gastroenterology and Nutrition Unit, Hospital Materno Infantil, Avda. Arroyo de los Ángeles s/n Málaga, Spain. Tel.: (mobile). addresses: victor.navas@gmail.com (V.M. Navas-López), javierblascoalonso@yahoo.es (J. Blasco Alonso), serranonieto@hotmail.com (M.J. Serrano Nieto), currogiron@gmail.com (F. Girón Fernández-Crehuet), mdargos@gmail.com (M.D. Argos Rodriguez), csierra@wanadoo.es (C. Sierra Salinas) /$ - see front matter 2013 European Crohn's and Colitis Organisation. Published by Elsevier B.V. All rights reserved.
2 Oral tacrolimus for pediatric steroid-resistant ulcerative colitis Introduction Ulcerative colitis (UC) occurring during childhood is generally extensive and is associated with severe flares that may require intravenous steroid treatment. Approximately 60 70% of patients that fail to respond to oral steroid treatment with prednisone will respond to intravenous treatment. Steroidresistant UC is defined as a lack of response to intravenous steroid treatment at adequate doses in the 3 10 days following the onset of treatment; it is usually found in 34% patients with severe UC. 1 In such cases, it is necessary to initiate a second-line treatment to avoid or delay surgery. Treatment modalities include tacrolimus, cyclosporine (CyA) and antitnf. 2,3 Tacrolimus is a macrolide that is structurally similar to rapamycin, has a potent immunosuppressive effect and is isolated from the fungus Streptomyces tsukubaensis. Its mechanism of action is similar to that of CyA; both bind to a cytosolic protein denoted FK BP12, creating a complex of FK BP12-tacrolimus, calcium, calmodulin, and calcineurin and leading to the inhibition of calcineurin phosphatase activity and prevention of the generation of the nuclear factor of activated T cells (NF-AT), a protein that initiates the transcription of cytokine genes. This, in turn, induces blockage of IL-2 synthesis and consequently the proliferation of T-cells, clonal expansion, and production of the cytokines involved in the immunological chain. 4 Tacrolimus has been used successfully in liver, intestine, lung, heart, pancreas, and renal transplantation, 5 7 in the prevention of graft-versus-host disease after bone marrow transplantation, and in nephrotic syndrome. 8 Its use has also been extended to treat autoimmune chronic hepatitis, 9 primary sclerosing cholangitis, autoimmune enteropathy, 10 and refractory inflammatory bowel disease (IBD). 11 We provide our experience on the efficacy and safety of oral tacrolimus treatment in children with severe steroid-resistant UC. 2. Patients and method This was a retrospective study that included patients under age 18 suffering from severe steroid-resistant UC treated with oral tacrolimus during the period January 1998 to October 2012 and with a follow-up period after treatment of 24 months or more Inclusion criteria In those patients treated before 2007, a severe flare of UC was considered if there was a bad general condition, intense abdominal pain, and loose bloody stools greater in number than five in 24 hours. For patients included after the year 2007, the Pediatric Ulcerative Colitis Activity Index (PUCAI) 12,13 was used; the flare was considered severe if PUCAI 65 points Exclusion criteria Active intestinal infection, toxic megacolon, intestinal perforation or peritonitis. Before beginning the treatment, stool samples were obtained for culture and research of Salmonella, Shigella, Yersinia, Campylobacter, Escherichia coli, and the presence of Clostridium difficile A and B toxins in all cases. Other determinations were the following: blood count, erythrocyte sedimentation rate, C-reactive protein (CRP), sodium, potassium, chloride, transaminases, urea, creatinine, calcium, phosphorus, magnesium and coagulation tests. Active cytomegalovirus (CMV) infection was also excluded. In all cases, informed consent was obtained. Tacrolimus were administered as an off-label medication. All patients received an oral dose of 0.12 mg/kg/day of tacrolimus (Prograf, Astellas Pharma, Madrid, Spain) divided in two doses. Daily monitoring during admission included measurement of blood count, urea/creatinine, transaminases, magnesium, blood pressure, and tacrolimus trough levels until the levels reached those expected (5 10 ng/ml). Once such levels were reached, measurements were taken weekly during the first month, every 15 days during the second month and each month thereafter. We administered oral magnesium in cases of hypomagnesemia. The data collected included age, sex, duration of illness to initiation of treatment with tacrolimus, number of flares, medication administered prior to treatment with tacrolimus, trough levels of tacrolimus (ng/ml), clinical response, duration of treatment, need for surgery, time elapsed until surgery, immunomodulation therapy after tacrolimus in noncolectomised patients and adverse effects observed. We considered that the patient was responding when the number and characteristics of the stools normalised, the abdominal pain disappeared, the acute phase reactants decreased the hemoglobin increased or when PUCAI dropped over 20 points. The extent of the disease was defined according to the Montreal Classification. 14,15 3. Statistical analysis Variables are expressed as the median and interquartile range (IQR) or as the mean and standard deviation based on whether the variables followed a normal distribution. For normally distributed variables, we utilised the Kolmogorov Smirnoff test. For the comparison of different variables, we used the Fisher exact test, Pearson Chi-square test, or Kruskall Wallis test. The survival plots were drawn with the Kaplan Meier method. We considered a p b 0.05 as statistically significant. 4. Results Atotaloftenpatientswereincluded,sevenofwhichwere females (Table 1); seven of the patients were in their first flare of disease. The age at baseline was 9.4 ± 4.9 years, and the time from diagnosis was 1.3 months (IQR, 1 5.7). An initial clinical response was achieved in six patients; non-responders required colectomy and, in these cases, surgery was performed in a median of 9 days (IQR, ). In the subgroup that initially responded, two of the six patients required colectomy, one at ten months after starting treatment and the other at six years and four months in conjunction with the suspension of immunomodulation therapy and the emergence of a new flare refractory to medical treatment. The three patients who were not in their first flare of the disease responded to tacrolimus. In four patients, surgery was avoided; these patients currently remain in clinical remission with immunomodulation therapy,
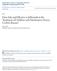
3 66 V.M. Navas-López et al. Table 1 Patients characteristics n, (%). Patients 10 Females 7/10 (70%) Age at tacrolimus started (years) 9.4 ± 4.9 Disease duration (months) 1.3 (IQ 1 5.7) Flare First 7 (70%) Second 1 (10%) Third 2 (20%) Montreal classification E3S3 10 (100%) Baseline PUCAI 68.8 ± 4.8 Previous treatment Corticosteroids 10 (100%) Aminosalicylates 10 (100%) Azathioprine 2 (20%) Infliximab 1 (10%) Days on steroid treatment before 7.1 ± 1.6 starting tacrolimus Tacrolimus trough levels (ng/ml) 4 13 Duration of treatment with tacrolimus 4.7 (IQR, 3.7 6) in responders (months) Maintenance treatment Aminosalicylates 5 (50%) Azathioprine 4 (40%) Mercaptopurine 1 (10%) Surgery during the follow-up 6 (60%) Time to surgery (days) All 20 (IQ, ) Non-responders 9 (IQ, ) more than 24 months after the onset of treatment with tacrolimus. Trough plasma levels of tacrolimus were maintained between 4 and 13 ng/ml. The median duration of treatment with tacrolimus in the responding group was 4.7 months (IQR, 3.7 6) compared to a duration of treatment in the nonresponding group of 0.23 months (IQR ), p = In responding patients, the steroid dose was reduced after 7 10 days of treatment with tacrolimus and immunomodulation maintenance therapy was started (azathioprine or mercaptopurine). During the duration of the triple immunosuppressive therapy (tacrolimus, steroids and thioguanines), the patients received prophylaxis with trimethoprim sulfamethoxazole. Tacrolimus was well tolerated in all cases; we observed no adverse effects except for a slight increase in plasma creatinine levels from baseline in one case. The survival curves (Fig. 1.1) show that, for the patients who initially respond to tacrolimus and whose response is maintained beyond 12 months, the likelihood of colectomy decreases drastically if they continue with immunomodulation therapy. Fig. 1.2 shows that a lack of initial response to tacrolimus inevitably resulted in surgery within the following months; this curve contrasts strikingly with that of the patients who responded initially (p = ). 5. Discusion Several definitions of severe UC have been used in the literature. The first and most widely used of these is the classification of Truelove and Witts. In 1977, Werlin and Grand proposed a modification of Truelove's classification, adapting it to children. 12,16 The application of these criteria has never been validated in children with severe UC. Recently, Turner developed a score of UC activity in children. However, this index not only quantifies the degree of disease activity but also predicts the lack of response to steroid therapy and the need to initiate a second-line treatment for severe flare of UC. 12,13 Steroid-resistant UC is defined as a lack of response to intravenous steroid therapy in adequate doses (1 1.5 mg/kg/day, maximum 60 mg) for 3 10days.Inchildren,corticosteroid resistance is estimated to occur with an incidence of 34% (CI 95%, 27 41%), 17,18 slightly higher than that observed in adults. 1 Corticosteroid resistance is not a stable situation over time, and genetic and environmental factors such as CMV infection have been identified. 22,23 The introduction of a second-line treatment should ideally be based on ability to recognise those patients likely to fail steroid therapy at an early stage. The PUCAI has proven more effective in children than in adults. Given its sensitivity, when calculating the third day of steroid treatment a PUCAI N 45 points forces the health care provider to plan a second-line treatment and to consult a surgeon. Additionally, due to its high specificity, if after 5 days the PUCAI is N65 70, the provider must begin to administer a second-line treatment. 17 Although treatment with second-line drugs is preferred to surgery for children, once the treatment is established it is necessary to inform the family of the possibility of colectomy if drug treatment is not successful. 24 CyA is an inhibitor of calcineurin, a molecule that participates in the synthesis of IL-2. The first published work on the use of CyA in adults dates from ; the first randomised clinical trial of this drug was halted on ethical grounds because the CyA-treated group had a higher response rate. 26 In a recent published open label RCT, CyA was not more effective than infliximab (IFX) in patients with acute severe UC refractory to intravenous steroids. 27 There are few published studies on treatment with CyA in children; if we select the studies that include more than five patients, 86 cases treated with different standards have been reported to date The reported studies are heterogeneous in terms of design, sample size, inclusion criteria, remission, and patient follow-up. Some authors use the oral route initially, while others prefer to begin treatment with CyA intravenously and subsequently switch to the oral route when remission is achieved. Analysis of the published data indicates that approximately 80% of patients (IQR, 95%, 70 87%) respond to treatment, although the percentage of cases that are free of colectomy years later is 45% (IQR, 34 57%). Thus, CyA therapy should be used as a bridge between corticosteroids and thioguanines (azathioprine or 6-mercaptopurine), and its use is for duration longer than 3 4 months is not recommended. In two studies in which thioguanines were used routinely in all patients, the sustained response rate was higher and more prolonged. 29,31 Tacrolimus, which has greater potency than CyA (100 times more in vitro and 10 times more in vivo) due to the high affinity of its complex with FK BP-12 by calcineurin and better bioavailability because its absorption is not hindered by the degree of bowel wall inflammation, was first used in the early 90s as an alternative to CyA in IBD patients. 11 IFX
4 Oral tacrolimus for pediatric steroid-resistant ulcerative colitis 67 Figure 1 Colectomy-free survival Kaplan Meier curve. Colectomy-free survival of all patients regardless of initial response Kaplan Meier curve Colectomy-free survival of patients depending on whether there was initial response (dashed line) or not (solid line). The difference between the survival curves is statistically significant (Log Rank, p = ). can also induce remission in patients with severe UC. 35 There are no published studies comparing tacrolimus with CyA or IFX in children. Experience with tacrolimus in the treatment of pediatric IBD patients is very limited (Table 2). Since the first description by Bousvaros et al. in 1996, 36 a series of studies have been published. Bousvaros et al. 37 conducted a multicentre study that included 14 paediatric patients older than five years old with severe IBD (10 UC, 2 Crohn's disease, and 2 indeterminate colitis) who did not respond to conventional treatment with intravenous steroids. An initial dose of 0.1 mg/kg was administered every 12 h to maintain plasma levels between 10 and 15 ng/ml for 14 days and then between 5 and 10 ng/ml. They found an initial response rate of 65%; the remaining 35% required colectomy. At 12 months follow-up, five patients (38%) were in remission with maintenance therapy and without the need for surgery. The mean duration of treatment in responding patients was 3.4 months. Ziring et al. 38 studied 18 children with UC (nine corticosteroid-resistant and nine corticosteroid-dependent). The initial dose administered was 0.1 mg/kg every 12 h to maintain levels of ng/ml during the first two weeks; thereafter, levels were maintained between 7 and 12 ng/ml. Initially, 94% of patients (17 of 18) responded to tacrolimus. At the time of publication of the study, only 13 of the 18 had had more than one-year follow-up; seven of these (53%) had required colectomy during the first year since the start of tacrolimus. Turner et al. 2 treated six children with severe UC with calcineurin inhibitors (five of these children received tacrolimus and one CyA) following the treatment protocol published by Bousvaros et al. 37 (unpublished data, information provided by the author). Three of the five patients treated with tacrolimus (60%) responded and were discharged without colectomy. One year after discharge, two patients (40%) continued in remission without colectomy. Watson et al. 39 published a report on the largest series of patients to date with severe corticosteroid-resistant UC treated with oral tacrolimus. The regimen followed was similar to that used in a previously published study by these authors. 37 The initial response rate was 89% at two years of follow-up, at which time 54% of the patients were free of colectomy. Table 2 Summary of studies using tacrolimus for the treatment of a severe flare of corticosteroid-resistant ulcerative colitis in children. Adapted from Turner et al. 17 Study N Dose mg/kg/day Pl ng/ml Initial response % Free of colectomy Navas (2013) /10 (60%) 5/10 (50%) at 2 years Watson (2010) /46 (89%) 25/46 (54%) at 2 years Turner (2008) /5 (80%) 2/5 (40%) at one year Ziring (2007) /9 (89%) 0% (b14 months) 7 12 Bousvaros (2000) /9 (55%) 2/9 (22 %) at one year Total (95% IC) 79 79% (68 87%) 43% (32 54%) Pl: plasma levels (ng/ml).
5 68 V.M. Navas-López et al. In our series, six of ten patients (60%) achieved clinical remission with plasma levels of tacrolimus between 4 and 13 ng/ml; after 24 months of follow-up, five of them (50%) had not required surgery. The relation between the tacrolimus dose and plasma trough levels of the drug has been also studied. In a randomised study conducted in 60 adults 40 in which the patients were divided into three groups (plasma levels ng/ml; plasma levels 5 10 ng/ml, and placebo), a higher rate of histologic remission and further steroid dose reduction was observed in patients with high plasma levels of tacrolimus (10 15 ng/ml) versus placebo (p b ). If we compare the two groups treated with tacrolimus the difference was not significant (p = 0.067), this is likely due to the small sample size. Recently, Ogata et al. 41 published a new study of 62 adults comparing treatment with tacrolimus for two weeks versus placebo; they found a higher response rate and clinical and histological remission in the group treated with tacrolimus. Schmidt KJ et al. 42 treated 130 steroidresistant UC adult patients with tacrolimus. Colectomy was avoided in the 86% of the patients in the first 3 months of treatment. The tacrolimus median trough level was 6.85 μg/l (range: ), although it was only measured in the 60% of the patients. Thiopurines given in parallel to tacrolimus tended to limit colectomy and significantly increased remission in the short-term. 42 Based on all of the data that has been published to date, tacrolimus could be indicated as second-line therapy in severe steroid-resistant UC and as bridge therapy in severe steroid-resistant or steroid-dependent UC. Ziring et al. 38 showed that not all patients respond in the same way; six of the nine corticosteroid-resistant patients (66%) in that study were operated on within one year after onset, and all underwent surgery prior to four years after starting tacrolimus treatment, unlike the outcome for the series of corticosteroid-dependent patients (22% needed surgery during the follow-up period). According to the ESPGHAN-ECCO guidelines, CyA or tacrolimus started during an episode of acute severe UC should be discontinued after 4 months, bridging to thiopurines and if disease is still chronically active or frequent flares despite adequate thiopurine treatment, consider IFX therapy (or adalimumab in cases of failure with IFX). 24 In our two patients treated with azathioprine before tacrolimus, we did not use anti-tnf-α because they were not available. Another recently reported aspect of the treatment of UC is the relationship of the presence of a genetic polymorphism to the response to treatment with tacrolimus. Herrilinger et al. 43 found a higher response rate in patients homozygous for some polymorphisms (1236C N T, 2677G N T, A, and 3435C N T) of the ABCB1 gene (7q21.1). If this determination were readily available, it could be used in choosing a second-line treatment. In summary, tacrolimus is useful in inducing remission in patients with severe steroid-resistant UC, preventing or delaying colectomy, and allowing the patient and family to prepare for a probable surgery. Tacrolimus may also be used as a treatment bridge for corticosteroid-dependent patients until the new maintenance therapy takes effect. Conflict of interest statement The authors acknowledge no conflicts of interest. References 1. Turner D, Walsh CM, Steinhart AH, Griffiths AM. Response to corticosteroids in severe ulcerative colitis: a systematic review of the literature and a meta-regression. Clin Gastroenterol Hepatol 2007;5: Turner D, Walsh CM, Benchimol EI, Mann EH, Thomas KE, Chow C, et al. Severe paediatric ulcerative colitis: incidence, outcomes and optimal timing for second-line therapy. Gut 2008;57: Turner D. Severe acute ulcerative colitis: the pediatric perspective. Dig Dis 2009;27: De Oca J, Vilar L, Castellote J, Sánchez Santos R, Parés D, Biondo S, et al. Immunomodulation with tacrolimus (FK 506): results of a prospective, open-label, non-controlled trial in patients with inflammatory bowel disease. Rev Esp Enferm Dig 2003;95: Kelly D, Jara P, Rodeck B, Lykavieris P, Burdelski M, Becker M, et al. Tacrolimus and steroids versus ciclosporin microemulsion, steroids, and azathioprine in children undergoing liver transplantation: randomised European multicentre trial. Lancet 2004;364: Hernández F, López Santamaría M, Gámez M, Murcia J, Leal N, Prieto G, et al. Results of an intestinal transplantation program in Spain. Five years later. Cir Pediatr 2004;17: Plosker GL, Foster RH. Tacrolimus: a further update of its pharmacology and therapeutic use in the management of organ transplantation. Drugs 2000;59(2): Gulati S, Prasad N, Sharma RK, Kumar A, Gupta A, Baburaj VP. Tacrolimus: a new therapy for steroid-resistant nephrotic syndrome in children. Nephrol Dial Transplant 2008;23(3): Larsen FS, Vainer B, Eefsen M, Bjerring PN, Adel Hansen B. Low-dose tacrolimus ameliorates liver inflammation and fibrosis in steroid refractory autoimmune hepatitis. World J Gastroenterol 2007;13: Bousvaros A, Leichtner AM, Book L, Shigeoka A, Bilodeau J, Semeao E, et al. Treatment of pediatric autoimmune enteropathy with tacrolimus (FK506). Gastroenterology 1996;111(1): Chow D, Leong R. The use of tacrolimus in the treatment of inflammatory bowel disease. Expert Opin Drug Saf 2007;6(5): Turner D, Otley AR, Mack D, de Bruijne J, Uusoue K, Walter T, et al. Development and evaluation of a Pediatric Ulcerative Colitis Activity Index (PUCAI): a prospective multicenter study. Gastroenterology 2007;133: Turner D, Hyams J, Markowitz J, Lerer T, Mack DR. Evans J et al Appraisal of the pediatric ulcerative colitis activity index (PUCAI). Inflamm Bowel Dis 2009;15(8): Satsangi J, Silverberg MS, Vermeire S, Colombel JF. The Montreal classification of inflammatory bowel disease: controversies, consensus, and implications. Gut 2006;55: Silverberg MS, Satsangi J, Ahmad T, Arnott ID, Bernstein CN, Brant SR, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a working party of the 2005 Montreal World Congress of Gastroenterology. Can J Gastroenterol 2005;19(Suppl A): Turner D, Seow CH, Greenberg GR, Griffiths AM, Silverberg MS, Steinhart AH. A systematic prospective comparison of noninvasive disease activity indices in ulcerative colitis. Clin Gastroenterol Hepatol 2009;7(10): Turner D, Griffiths A. Acute severe ulcerative colitis in children: a systematic review. Inflamm Bowel Dis 2011;17(1): Turner D, Mack D, Leleiko N, Walters TD, Uusoue K, Leach ST, et al. Severe pediatric ulcerative colitis: a prospective multicenter study of outcomes and predictors of response. Gastroenterology 2010;138(7): De Iudicibus S, Stocco G, Martelossi S, Londero M, Ebner E, Pontillo A, et al. Genetic predictors of glucocorticoid response
6 Oral tacrolimus for pediatric steroid-resistant ulcerative colitis 69 in pediatric patients with inflammatory bowel diseases. J Clin Gastroenterol 2011;45(1):e De Iudicibus S, Franca R, Martelossi S, Ventura A, Decorti G. Molecular mechanism of glucocorticoid resistance in inflammatory bowel disease. World J Gastroenterol 2011;17(9): Kabakchiev B, Turner D, Hyams J, Mack D, Leleiko N, Crandall W, et al. Gene expression changes associated with resistance to intravenous corticosteroid therapy in children with severe ulcerative colitis. PLoS One 2010;5(9):e13085 [pii]. 22. Lawlor G, Moss AC. Cytomegalovirus in inflammatory bowel disease: pathogen or innocent bystander? Inflamm Bowel Dis 2010;16(9): Ayre K, Warren BF, Jeffery K, Travis SP. The role of CMV in steroid-resistant ulcerative colitis: a systematic review. JCrohns Colitis 2009;3(3): Turner D, Travis SP, Griffiths AM, Ruemmele FM, Levine A, Benchimol EI, et al. Consensus for managing acute severe ulcerative colitis in children: a systematic review and joint statement from ECCO, ESPGHAN, and the Porto IBD Working Group of ESPGHAN. Am J Gastroenterol 2011;106(4): Gupta S, Keshavarzian A, Hodgson HJ. Cyclosporin in ulcerative colitis. Lancet 1984;2(8414): Lichtiger S, Present DH, Kornbluth A, Gelernt I, Bauer J, Galler G, et al. Cyclosporine in severe ulcerative colitis refractory to steroid therapy. N Engl J Med 1994;330(26): Laharie D, Bourreille A, Branche J, Allez M, Bouhnik Y, Filippi J, et al. Ciclosporin versus infliximab in patients with severe ulcerative colitis refractory to intravenous steroids: a parallel, open-label randomised controlled trial. Lancet 2012;380(9857): Castro M, Papadatou B, Ceriati E, Knafelz D, De Angelis P, Ferretti F, et al. Role of cyclosporin in preventing or delaying colectomy in children with severe ulcerative colitis. Langenbecks Arch Surg 2007;392(2): Ramakrishna J, Langhans N, Calenda K, Grand RJ, Verhave M. Combined use of cyclosporine and azathioprine or 6- mercaptopurine in pediatric inflammatory bowel disease. J Pediatr Gastroenterol Nutr 1996;22(3): Socha P, Wawer Z, Ryzko J, Orłowska E, Szczepański M, Kierkus J, et al. Efficacy and safety of cyclosporine in the treatment of inflammatory bowel disease in children a retrospective study. Med Wieku Rozwoj 2006;10(2): Barabino A, Torrente F, Castellano E, Gandullia P, Calvi A, Cucchiara S, et al. The use of ciclosporin in paediatric inflammatory bowel disease: an Italian experience. Aliment Pharmacol Ther 2002;16(8): Treem WR, Cohen J, Davis PM, Justinich CJ, Hyams JS. Cyclosporine for the treatment of fulminant ulcerative colitis in children. Immediate response, long-term results, and impact on surgery. Dis Colon Rectum 1995;38(5): Benkov KJ, Rosh JR, Schwersenz AH, Janowitz HD, LeLeiko NS. Cyclosporine as an alternative to surgery in children with inflammatory bowel disease. J Pediatr Gastroenterol Nutr 1994;19(3): Kirschner BS, Whitington PF, Malfeo-Klein R. Experience with cyclosporine A (CyA) in severe non-specific ulcerative colitis. Pediatr Res 1989;25:A Hyams J, Damaraju L, Blank M, Johanns J, Guzzo C, Winter HS, et al. Induction and maintenance therapy with infliximab for children with moderate to severe ulcerative colitis. Clin Gastroenterol Hepatol 2012;10(4): Bousvaros A, Wang A, Leichtner AM. Tacrolimus (FK-506) treatment of fulminant colitis in a child. J Pediatr Gastroenterol Nutr 1996;23(3): Bousvaros A, Kirschner BS, Werlin SL, Parker-Hartigan L, Daum F, Freeman KB, et al. Oral tacrolimus treatment of severe colitis in children. J Pediatr 2000;137(6): Ziring DA, Wu SS, Mow WS, Martin MG, Mehra M, Ament ME. Oral tacrolimus for steroid-dependent and steroid-resistant ulcerative colitis in children. J Pediatr Gastroenterol Nutr 2007;45(3): Watson S, Pensabene L, Mitchell P, Bousvaros A. Outcomes and adverse events in children and young adults undergoing tacrolimus therapy for steroid-refractory colitis. Inflamm Bowel Dis 2011;17(1): Ogata H, Matsui T, Nakamura M, Iida M, Takazoe M, Suzuki Y, et al. A randomised dose finding study of oral tacrolimus (FK506) therapy in refractory ulcerative colitis. Gut 2006;55: Ogata H, Kato J, Hirai F, Hida N, Matsui T, Matsumoto T, et al. Double-blind, placebo-controlled trial of oral tacrolimus (FK506) in the management of hospitalized patients with steroid-refractory ulcerative colitis. Inflamm Bowel Dis 2012;18(5): Schmidt KJ, Herrlinger KR, Emmrich J, Barthel D, Koc H, Lehnert H, et al. Short-term efficacy of tacrolimus in steroid-refractory ulcerative colitis experience in 130 patients. Aliment Pharmacol Ther 2013;37(1): Herrlinger KR, Koc H, Winter S, Teml A, Stange EF, Fellermann K, et al. ABCB1 single-nucleotide polymorphisms determine tacrolimus response in patients with ulcerative colitis. Clin Pharmacol Ther 2011;89(3):422 8.
Clinical Course of Infliximab Treatment in Korean Pediatric Ulcerative Colitis Patients: A Single Center Experience
 pissn: 2234-8646 eissn: 2234-8840 http://dx.doi.org/10.5223/pghn.2014.17.1.31 Pediatric Gastroenterology, Hepatology & Nutrition 2014 March 17(1):31-36 Original Article PGHN Clinical Course of Infliximab
pissn: 2234-8646 eissn: 2234-8840 http://dx.doi.org/10.5223/pghn.2014.17.1.31 Pediatric Gastroenterology, Hepatology & Nutrition 2014 March 17(1):31-36 Original Article PGHN Clinical Course of Infliximab
Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients
 Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients Tamás Molnár 1, Klaudia Farkas 1, Tibor Nyári 2, Zoltán Szepes 1, Ferenc Nagy 1,
Response to First Intravenous Steroid Therapy Determines the Subsequent Risk of Colectomy in Ulcerative Colitis Patients Tamás Molnár 1, Klaudia Farkas 1, Tibor Nyári 2, Zoltán Szepes 1, Ferenc Nagy 1,
Moderately to severely active ulcerative colitis
 Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Algorithm for managing severe ulcerative colitis
 Tropical Gastroenterology 2014;Suppl:S40 44 Algorithm for managing severe ulcerative colitis Vineet Ahuja 1, Ajay Kumar 2, Rakesh Kochhar 3 ABSTRACT Dept of Gastroenterology, 1 All India Institute of Medical
Tropical Gastroenterology 2014;Suppl:S40 44 Algorithm for managing severe ulcerative colitis Vineet Ahuja 1, Ajay Kumar 2, Rakesh Kochhar 3 ABSTRACT Dept of Gastroenterology, 1 All India Institute of Medical
Protocol for the management of acute severe ulcerative colitis in children
 Protocol for the management of acute severe ulcerative colitis in children Introduction: Paediatric UC is severe and more extensive than adult onset UC with 6-8% presenting as pancolitis (1,2) Within five
Protocol for the management of acute severe ulcerative colitis in children Introduction: Paediatric UC is severe and more extensive than adult onset UC with 6-8% presenting as pancolitis (1,2) Within five
 Tacrolimus therapy as an alternativ Titlemaintaining remission in patients w colitis. Author(s) Yamamoto, Shuji; Nakase, Hiroshi; M Masuda, Satohiro; Inui, Ken-ichi; C Citation Journal of clinical gastroenterolog
Tacrolimus therapy as an alternativ Titlemaintaining remission in patients w colitis. Author(s) Yamamoto, Shuji; Nakase, Hiroshi; M Masuda, Satohiro; Inui, Ken-ichi; C Citation Journal of clinical gastroenterolog
Optimizing the effectiveness of anti-tnf therapy in paediatric IBD
 Optimizing the effectiveness of anti-tnf therapy in paediatric IBD Anne Griffiths MD, FRCPC Co-Lead, Inflammatory Bowel Disease Center Northbridge Chair in IBD Hospital for Sick Children, Professor of
Optimizing the effectiveness of anti-tnf therapy in paediatric IBD Anne Griffiths MD, FRCPC Co-Lead, Inflammatory Bowel Disease Center Northbridge Chair in IBD Hospital for Sick Children, Professor of
CLINICAL TRIAL PROTOCOL
 CLINICAL TRIAL PROTOCOL Azathioprine maintenance therapy in steroid-refractory Ulcerative Colitis responsive to i.v. Cyclosporine A: Is a therapeutic bridge with oral Cyclosporine A necessary? Miquel A.
CLINICAL TRIAL PROTOCOL Azathioprine maintenance therapy in steroid-refractory Ulcerative Colitis responsive to i.v. Cyclosporine A: Is a therapeutic bridge with oral Cyclosporine A necessary? Miquel A.
Anti-TNF and cyclosporine are identical choices for severe ulcerative colitis refractory to steroid therapy CON Peter Laszlo LAKATOS Semmelweis
 Anti-TNF and cyclosporine are identical choices for severe ulcerative colitis refractory to steroid therapy CON Peter Laszlo LAKATOS Semmelweis University, 1st Department of Medicine Budapest June 13-15,
Anti-TNF and cyclosporine are identical choices for severe ulcerative colitis refractory to steroid therapy CON Peter Laszlo LAKATOS Semmelweis University, 1st Department of Medicine Budapest June 13-15,
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease
 Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Azathioprine for Induction and Maintenance of Remission in Crohn s Disease William J. Sandborn, MD Chief, Division of Gastroenterology Director, UCSD IBD Center Objectives Azathioprine as induction and
Inflammatory Bowel Disease: Clinical updates. Dr Jeff Chao Princess Alexandra Hospital
 Inflammatory Bowel Disease: Clinical updates Dr Jeff Chao Princess Alexandra Hospital Inflammatory bowel disease 2017 Clinical updates and future directions Pathogenesis Treatment targets Therapeutic agents
Inflammatory Bowel Disease: Clinical updates Dr Jeff Chao Princess Alexandra Hospital Inflammatory bowel disease 2017 Clinical updates and future directions Pathogenesis Treatment targets Therapeutic agents
Infliximab (Remicade) for paediatric ulcerative colitis - second line
 Infliximab (Remicade) for paediatric ulcerative colitis - second line September 2011 This technology summary is based on information available at the time of research and a limited literature search. It
Infliximab (Remicade) for paediatric ulcerative colitis - second line September 2011 This technology summary is based on information available at the time of research and a limited literature search. It
IBD in teenagers Biological and Transition
 IBD in teenagers Biological and Transition Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital Chelsea and Westminster Hospital Conflict of Interest None to declare Fee for presentation
IBD in teenagers Biological and Transition Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital Chelsea and Westminster Hospital Conflict of Interest None to declare Fee for presentation
Infliximab as rescue medication for patients with severe ulcerative/indeterminate colitis refractory to tacrolimus
 Infliximab as rescue medication for patients with severe ulcerative/indeterminate colitis refractory to tacrolimus Klaus R. Herrlinger, Daniel N Barthel, Klaus Jürgen Schmidt, Juergen Buening, Christiane
Infliximab as rescue medication for patients with severe ulcerative/indeterminate colitis refractory to tacrolimus Klaus R. Herrlinger, Daniel N Barthel, Klaus Jürgen Schmidt, Juergen Buening, Christiane
Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease
 Gut and Liver, Published online September 9, 2016 ORiginal Article Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease So Yoon
Gut and Liver, Published online September 9, 2016 ORiginal Article Clinical Use of Measuring Trough Levels and Antibodies against Infliximab in Patients with Pediatric Inflammatory Bowel Disease So Yoon
September 12, 2015 Millie D. Long MD, MPH, FACG
 Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Update on Biologic Therapy in 2015 September 12, 2015 Millie D. Long MD, MPH, FACG Assistant Professor of Medicine Inflammatory Bowel Disease Center University of North Carolina-Chapel Hill Outline Crohn
Qualification opinion
 20 January 2016 EMA/CHMP/SAWP/801872/2015 Committee for Medicinal Products for Human Use (CHMP) Draft agreed by scientific advice working party 01 June 2015 Adopted by CHMP for release for consultation
20 January 2016 EMA/CHMP/SAWP/801872/2015 Committee for Medicinal Products for Human Use (CHMP) Draft agreed by scientific advice working party 01 June 2015 Adopted by CHMP for release for consultation
Update on Biologics in Ulcerative Colitis. Scott Plevy, MD University of North Carolina Chapel Hill, NC
 Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
Update on Biologics in Ulcerative Colitis Scott Plevy, MD University of North Carolina Chapel Hill, NC Objectives Discuss the latest advances in the pharmacologic management of ulcerative colitis Describe
abstract STATE-OF-THE-ART REVIEW ARTICLE
 Management of Acute Severe Colitis in Children With Ulcerative Colitis in the Biologics Era Claudio Romano, MD, a Sana Syed, MD, b Simona Valenti, MD, a Subra Kugathasan, PhD b BACKGROUND AND OBJECTIVE:
Management of Acute Severe Colitis in Children With Ulcerative Colitis in the Biologics Era Claudio Romano, MD, a Sana Syed, MD, b Simona Valenti, MD, a Subra Kugathasan, PhD b BACKGROUND AND OBJECTIVE:
Systematic review and meta-analysis of third-line salvage therapy with infliximab or cyclosporine in severe ulcerative colitis
 Systematic review and meta-analysis of third-line salvage therapy with infliximab or cyclosporine in severe ulcerative colitis The Harvard community has made this article openly available. Please share
Systematic review and meta-analysis of third-line salvage therapy with infliximab or cyclosporine in severe ulcerative colitis The Harvard community has made this article openly available. Please share
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals
 Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Latest Treatment Updates for Ulcerative Colitis: Evolving Treatment Goals Stephen Hanauer, MD Professor of Medicine Medical Director, Digestive Disease Center Northwestern Medicine Chicago, Illinois Speaker
Mucosal healing: does it really matter?
 Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does it really matter? Professor Jean-Frédéric Colombel, New York, USA Oxford Inflammatory Bowel Disease MasterClass Mucosal healing: does
Long-term outcome after infliximab for refractory ulcerative colitis
 Journal of Crohn's and Colitis (2008) 2, 219 225 available at www.sciencedirect.com Long-term outcome after infliximab for refractory ulcerative colitis Marc Ferrante a, Séverine Vermeire a, Herma Fidder
Journal of Crohn's and Colitis (2008) 2, 219 225 available at www.sciencedirect.com Long-term outcome after infliximab for refractory ulcerative colitis Marc Ferrante a, Séverine Vermeire a, Herma Fidder
Medical Therapy for Pediatric IBD: Efficacy and Safety
 Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS
 TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
PEDIATRIC INFLAMMATORY BOWEL DISEASE
 PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
PEDIATRIC INFLAMMATORY BOWEL DISEASE Alexis Rodriguez, MD Pediatric Gastroenterology Advocate Children s Hospital Disclosers Abbott Nutrition - Speaker Inflammatory Bowel Disease Chronic inflammatory disease
MEDICAL POLICY. Proprietary Information of YourCare Health Plan
 MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
MEDICAL POLICY Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community.
Indications for use of Infliximab
 Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Indications for use of Infliximab Moscow, June 10 th 2006 Prof. Dr. Dr. Gerhard Rogler Klinik und Poliklinik für Innere Medizin I Universität Regensburg Case report 1989: Diagnosis of Crohn s disease of
Ulcerative colitis (UC) is a chronic inflammatory. Therapeutic Options in Steroid-Refractory Acute Severe Ulcerative Colitis.
 Therapeutic Options in Steroid-Refractory Acute Severe Ulcerative Colitis Wojciech Blonski, MD, PhD, Prashant R. Mudireddy, MD, Anna M. Buchner, MD, PhD, and Gary R. Lichtenstein, MD Abstract Objective:
Therapeutic Options in Steroid-Refractory Acute Severe Ulcerative Colitis Wojciech Blonski, MD, PhD, Prashant R. Mudireddy, MD, Anna M. Buchner, MD, PhD, and Gary R. Lichtenstein, MD Abstract Objective:
Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger
 ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
ORIGINAL ARTICLE: GASTROENTEROLOGY Infliximab Therapy in Pediatric Patients 7 Years of Age and Younger Judith R. Kelsen, Andrew B. Grossman, Helen Pauly-Hubbard, Kernika Gupta, Robert N. Baldassano, and
Summary of SAMEP review
 EVALUATION SUMMARY Infliximab for treatment of immunomodulator-naïve patients for treatment of acute and severe colitis refractory to intravenous corticosteroid therapy South Australian Medicines Evaluation
EVALUATION SUMMARY Infliximab for treatment of immunomodulator-naïve patients for treatment of acute and severe colitis refractory to intravenous corticosteroid therapy South Australian Medicines Evaluation
Previous exposure to biologics and C-reactive protein are associated with the response to tacrolimus in inflammatory bowel disease
 1130-0108/2016/108/9/550-557 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 9, pp. 550-557 ORIGINAL PAPERS Previous exposure
1130-0108/2016/108/9/550-557 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 9, pp. 550-557 ORIGINAL PAPERS Previous exposure
Achieving Success in Ulcerative Colitis: the Role of Infliximab
 Achieving Success in Ulcerative Colitis: the Role of Infliximab Dr Gill Watermeyer IBD clinic Groote Schuur Hospital 17 th August 2012 Inflammatory Bowel Disease Crohn s disease and ulcerative colitis
Achieving Success in Ulcerative Colitis: the Role of Infliximab Dr Gill Watermeyer IBD clinic Groote Schuur Hospital 17 th August 2012 Inflammatory Bowel Disease Crohn s disease and ulcerative colitis
The earliest trough concentration predicts the dose of tacrolimus required for remission induction therapy in ulcerative colitis patients
 Hiraoka et al. BMC Gastroenterology (2015) 15:53 DOI 10.1186/s12876-015-0285-3 RESEARCH ARTICLE Open Access The earliest trough concentration predicts the dose of tacrolimus required for remission induction
Hiraoka et al. BMC Gastroenterology (2015) 15:53 DOI 10.1186/s12876-015-0285-3 RESEARCH ARTICLE Open Access The earliest trough concentration predicts the dose of tacrolimus required for remission induction
young people concise guidance
 Clinical Medicine 2017 Vol 17, No 5: 429 33 CONCISE GUIDELINES Ulcerative colitis: management in adult s, children and young people concise guidance Authors: G lo ria S Z Tun, A Ad a m H a r ris B a nd
Clinical Medicine 2017 Vol 17, No 5: 429 33 CONCISE GUIDELINES Ulcerative colitis: management in adult s, children and young people concise guidance Authors: G lo ria S Z Tun, A Ad a m H a r ris B a nd
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS
 TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
TREATMENT OF INPATIENTS WITH ACUTE SEVERE ULCERATIVE COLITIS Target Audience: Physicians, Physician Assistants, Nurse Practitioners and Nurses impacted by the protocol. Scope/Patient Population: All adult
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Fistulizing Crohn s Disease: The Aggressive Approach
 Fistulizing Crohn s Disease: The Aggressive Approach Bruce E. Sands, MD, MS MGH Crohn s and Colitis Center and Gastrointestinal Unit Massachusetts General Hospital Boston, USA Case Presentation: Summary
Fistulizing Crohn s Disease: The Aggressive Approach Bruce E. Sands, MD, MS MGH Crohn s and Colitis Center and Gastrointestinal Unit Massachusetts General Hospital Boston, USA Case Presentation: Summary
IBD Updates. Themes in IBD IBD management journey. New tools for therapeutic monitoring. First-line treatment in IBD
 IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
IBD Updates Maria T. Abreu, MD University of Miami Miller School of Medicine Miami, Florida Themes in IBD 213 First-line treatment in IBD New tools for therapeutic monitoring Biologic therapy for CD and
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions. Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic
 Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
Perianal and Fistulizing Crohn s Disease: Tough Management Decisions Jean-Paul Achkar, M.D. Kenneth Rainin Chair for IBD Research Cleveland Clinic Talk Overview Background Assessment and Classification
Which is the Safest Strategy to Treat Moderate to Severe IBD?
 Which is the Safest Strategy to Treat Moderate to Severe IBD? David G. Binion, M.D. Co-Director, Inflammatory Bowel Disease Center Director, Translational Inflammatory Bowel Disease Research Visiting Professor
Which is the Safest Strategy to Treat Moderate to Severe IBD? David G. Binion, M.D. Co-Director, Inflammatory Bowel Disease Center Director, Translational Inflammatory Bowel Disease Research Visiting Professor
Epidemiology / Morbidity
 Perianal Crohn s Disease: Current Treatment Approach David A Schwartz, MD Director, Inflammatory Bowel Disease Center Vanderbilt University Medical Center Epidemiology / Morbidity Hellers et al, Gut 1980
Perianal Crohn s Disease: Current Treatment Approach David A Schwartz, MD Director, Inflammatory Bowel Disease Center Vanderbilt University Medical Center Epidemiology / Morbidity Hellers et al, Gut 1980
Treatment Goals. Current Therapeutic Pyramids Crohn s Disease Ulcerative Colitis 11/14/10
 Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
Current Management of IBD: From Conventional Agents to Biologics Stephen B. Hanauer, M.D. University of Chicago Treatment Goals Induce and maintain response/ remission Prevent complications Improve quality
5/2/2018 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD
 5/2/218 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD Grant support for preclinical studies: Janssen, Gusto Global, Vedanta, Artizan BALFOUR SARTOR, MD DISTINGUISHED
5/2/218 SHOULD DEEP REMISSION BE A TREATMENT GOAL? YES! Disclosures: R. Balfour Sartor, MD Grant support for preclinical studies: Janssen, Gusto Global, Vedanta, Artizan BALFOUR SARTOR, MD DISTINGUISHED
Biologics in IBD. Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College
 Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Biologics in IBD Brian P. Bosworth, MD, NYSGEF Associate Professor of Medicine Weill Cornell Medical College Case 30 year old man diagnosed with ulcerative proctitis diagnosed in 2003 Had been maintained
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Assistant Professor of Clinical Pediatrics Division of Gastroenterology,
Minami, Naoki; Yoshino, Takuya; Mat. Madian, Ali; Honzawa, Yusuke; Nakas. Citation BMJ Open Gastroenterology (2015), 2
 Tacrolimus or infliximab for severe Titleterm and long-term data from a retr study Minami, Naoki; Yoshino, Takuya; Mat Author(s) Koshikawa, Yorimitsu; Yamada, Satos Madian, Ali; Honzawa, Yusuke; Nakas
Tacrolimus or infliximab for severe Titleterm and long-term data from a retr study Minami, Naoki; Yoshino, Takuya; Mat Author(s) Koshikawa, Yorimitsu; Yamada, Satos Madian, Ali; Honzawa, Yusuke; Nakas
Management of the Hospitalized IBD Patient. Drew DuPont MD
 Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy
 Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Position of Biologics in IBD Circa 2006: Top Down vs. Step Up Therapy Stephen B. Hanauer, MD University of Chicago Potential Conflicts: Centocor/Schering, Abbott, UCB, Elan, Berlex, PDL Goals of Treatment
Combination of oral antibiotics may be effective in severe pediatric ulcerative colitis: A preliminary report
 Journal of Crohn's and Colitis (2014) 8, 1464 1470 Available online at www.sciencedirect.com ScienceDirect Combination of oral antibiotics may be effective in severe pediatric ulcerative colitis: A preliminary
Journal of Crohn's and Colitis (2014) 8, 1464 1470 Available online at www.sciencedirect.com ScienceDirect Combination of oral antibiotics may be effective in severe pediatric ulcerative colitis: A preliminary
Trust Guideline. for Ciclosporin Treatment & Monitoring for Adult* Patients with Acute, Severe Ulcerative Colitis. (*ie aged 16 years and over)
 Trust Guideline for Ciclosporin Treatment & Monitoring for Adult* Patients with Acute, Severe Ulcerative Colitis (*ie aged 16 years and over) abc A guideline recommended for use In: Gastroenterology/Medical
Trust Guideline for Ciclosporin Treatment & Monitoring for Adult* Patients with Acute, Severe Ulcerative Colitis (*ie aged 16 years and over) abc A guideline recommended for use In: Gastroenterology/Medical
IBD Understanding Your Medications. Thomas V. Aguirre, MD Santa Barbara GI Consultants
 IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
IBD Understanding Your Medications Thomas V. Aguirre, MD Santa Barbara GI Consultants IBD Understanding Your Medications (& Your Doctor) Thomas V. Aguirre, MD Santa Barbara GI Consultants Disclosure I
Anne Griffiths MD, FRCPC. SickKids Hospital, University of Toronto. Buenos Aires, August 16, 2014
 Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
Management and Medical Therapies for Crohn disease: strategies to enhance mucosal healing Anne Griffiths MD, FRCPC SickKids Hospital, University of Toronto Buenos Aires, August 16, 2014 New onset Crohn
DENOMINATOR: All patients aged 18 and older with a diagnosis of inflammatory bowel disease
 Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Measure #270: Inflammatory Bowel Disease (IBD): Preventive Care: Corticosteroid Sparing Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease. David A. Schwartz, MD
 An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
An Update on the Biologic Treatment for Patients with Inflammatory Bowel Disease David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University
CCFA. Crohns Disease vs UC: What is the best treatment for me? November
 CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
CCFA Crohns Disease vs UC: What is the best treatment for me? November 8 2009 Ellen J. Scherl,, MD, FACP,AGAF Roberts Inflammatory Bowel Disease Center Weill Medical College Cornell University New York
Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients with Ulcerative Colitis: A Retrospective Evaluation Study
 Gastroenterology Research and Practice Volume 2016, Article ID 5956316, 6 pages http://dx.doi.org/10.1155/2016/5956316 Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients
Gastroenterology Research and Practice Volume 2016, Article ID 5956316, 6 pages http://dx.doi.org/10.1155/2016/5956316 Clinical Study Tacrolimus for Remission Induction and Maintenance Therapy in Patients
Clinical Study Clinical Study of the Relation between Mucosal Healing and Long-Term Outcomes in Ulcerative Colitis
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2013, Article ID 192794, 6 pages http://dx.doi.org/10.1155/2013/192794 Clinical Study Clinical Study of the Relation between
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2013, Article ID 192794, 6 pages http://dx.doi.org/10.1155/2013/192794 Clinical Study Clinical Study of the Relation between
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 20 October 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 20 October 2010 MEZAVANT LP 1200 mg, prolonged-release gastro-resistant tablets B/60 (CIP code: 378 689-2) Applicant
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 20 October 2010 MEZAVANT LP 1200 mg, prolonged-release gastro-resistant tablets B/60 (CIP code: 378 689-2) Applicant
The Spectrum of IBD. Inflammatory Bowel Disease. Symptoms. Epidemiology. Tests for IBD. CD or UC? Inflamatory Bowel Disease. Fernando Vega, M.D.
 The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
The Spectrum of IBD Inflammatory Bowel Disease Fernando Vega, M.D. Epidemiology CD and UC together 1:400 UC Prevalence 1:500 UC Incidence 6-12K/annum CD Prevalence 1:1000 CD Incidence 3-6K/annum Symptoms
Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested. Philippe Marteau, Paris, France
 Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested Philippe Marteau, Paris, France Sequential vs combined treatments When should one switch? Sequential vs combined treatments
Mild-moderate Ulcerative Colitis Sequential & Combined treatments need to be tested Philippe Marteau, Paris, France Sequential vs combined treatments When should one switch? Sequential vs combined treatments
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Ulcerative colitis: the management of ulcerative colitis Quality standard title: Ulcerative
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children
 Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING FOR THIOPURINE METHYLTRANSFERASE (TPMT) FOR PATIENTS TREATED WITH AZATHIOPRINE (6-MP)
 MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
MEDICAL POLICY SUBJECT: GENOTYPING OR PHENOTYPING PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including
Nutrition as primary therapy in IBD. Dr Clare Donnellan Leeds General Infirmary
 Nutrition as primary therapy in IBD Dr Clare Donnellan Leeds General Infirmary Case GB 34 year old female Diagnosed with Crohn s in 2002? Extent Offered steroids or surgery Declined both GB Represented
Nutrition as primary therapy in IBD Dr Clare Donnellan Leeds General Infirmary Case GB 34 year old female Diagnosed with Crohn s in 2002? Extent Offered steroids or surgery Declined both GB Represented
Personalized Medicine in IBD: Where Are We in 2013
 Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Personalized Medicine in IBD: Where Are We in 2013 David A. Schwartz, MD Director, Inflammatory Bowel Disease Center Associate Professor of Medicine Vanderbilt University Medical Center What is Personalized
Medicine OPEN. Observational Study. 1. Introduction
 Observational Study Medicine OPEN Prospective comparison of preference and efficacy of adalimumab and infliximab for treating ulcerative colitis naive to antitumor necrosis factor therapy Tsutomu Mizoshita,
Observational Study Medicine OPEN Prospective comparison of preference and efficacy of adalimumab and infliximab for treating ulcerative colitis naive to antitumor necrosis factor therapy Tsutomu Mizoshita,
Treatment of Pediatric IBD: What is Different?
 Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
Treatment of Pediatric IBD: What is Different? January 13, 2017 Michael Kappelman MD, MPH University of North Carolina at Chapel Hill Overview Is Pediatric IBD the same disease? Treatment considerations
How Safe and Effective is Infliximab in the Treatment of Children with Moderate to Severe Crohn s disease?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 How Safe and Effective is Infliximab
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 How Safe and Effective is Infliximab
Agenda. Predictive markers in IBD. Management of ulcerative colitis. Management of Crohn s disease
 Agenda Predictive markers in IBD Management of ulcerative colitis Management of Crohn s disease 2 Patients With UC (%) Distribution of UC Disease Severity at Presentation 1 Fulminant disease (9%) 8 6 4
Agenda Predictive markers in IBD Management of ulcerative colitis Management of Crohn s disease 2 Patients With UC (%) Distribution of UC Disease Severity at Presentation 1 Fulminant disease (9%) 8 6 4
Percent Cumulative. Probability. Penetrating. Inflammatory. Stricturing. Months Patients at risk N =
 Fistulizing Crohn s Disease Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology & Hepatology Mayo Clinic Rochester, Minnesota, USA Outline Fistulizing Crohn s Etiology Incidence
Fistulizing Crohn s Disease Edward V. Loftus, Jr., M.D. Professor of Medicine Division of Gastroenterology & Hepatology Mayo Clinic Rochester, Minnesota, USA Outline Fistulizing Crohn s Etiology Incidence
Dr Adele Melton Gastroenterologist MBChB (Otago), FRACP
 Dr Adele Melton Gastroenterologist MBChB (Otago), FRACP (1) Case presentation CMV in IBD (2) Prevalence (3) Treatment (4) Recommendations / Guidelines (5) Questions 60 year old male Background: UC, pancolitis
Dr Adele Melton Gastroenterologist MBChB (Otago), FRACP (1) Case presentation CMV in IBD (2) Prevalence (3) Treatment (4) Recommendations / Guidelines (5) Questions 60 year old male Background: UC, pancolitis
Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease
 Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease The Case for Starting with Anti-TNFα Agents Maria Oliva-Hemker, M.D. Chief, Division of Pediatric Gastroenterology &
Initiation of Maintenance Treatment in Moderate to Severe New Onset Crohn s Disease The Case for Starting with Anti-TNFα Agents Maria Oliva-Hemker, M.D. Chief, Division of Pediatric Gastroenterology &
Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort
 Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Alimentary Pharmacology and Therapeutics Treatment of ulcerative colitis with adalimumab or infliximab: long-term follow-up of a single-centre cohort N. Gies, K. I. Kroeker, K. Wong & R. N. Fedorak Division
Technologies scoping report
 Technologies scoping report In response to an enquiry from NHS Greater Glasgow and Clyde Number 18 October 2013 What is the clinical effectiveness, cost effectiveness and implications for safety of assessing
Technologies scoping report In response to an enquiry from NHS Greater Glasgow and Clyde Number 18 October 2013 What is the clinical effectiveness, cost effectiveness and implications for safety of assessing
Il ruolo degli anticorpi anti farmaco nella pratica clinica
 Il ruolo degli anticorpi anti farmaco nella pratica clinica Daniela Pugliese, MD IBD Unit Complesso Integrato Columbus Gemelli Hospital Catholic University Foundation, Rome - Italy Therapeutic Drug monitoring
Il ruolo degli anticorpi anti farmaco nella pratica clinica Daniela Pugliese, MD IBD Unit Complesso Integrato Columbus Gemelli Hospital Catholic University Foundation, Rome - Italy Therapeutic Drug monitoring
Doncaster & Bassetlaw Medicines Formulary
 Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Doncaster & Bassetlaw Medicines Formulary Section 1.5 Chronic Bowel Disorders (including IBD) Aminosalicylates: Mesalazine 400mg and 800mg MR Tablets (Octasa) Mesalazine 1.2g MR Tablets (Mezavant XL) Mesalazine
Anti-tumour necrosis factor treatment of inflammatory bowel disease in liver transplant recipients
 Alimentary Pharmacology and Therapeutics Anti-tumour necrosis factor treatment of inflammatory bowel disease in liver transplant recipients A. B. Mohabbat*, W. J. Sandborn, E. V. Loftus Jr, R. H. Wiesner
Alimentary Pharmacology and Therapeutics Anti-tumour necrosis factor treatment of inflammatory bowel disease in liver transplant recipients A. B. Mohabbat*, W. J. Sandborn, E. V. Loftus Jr, R. H. Wiesner
Ali Keshavarzian MD Rush University Medical Center
 Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
Mono or Combination Therapy with. Individualized Approach
 Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Mono Combination Therapy with Biologics i in IBD: Developing an Individualized Approach David T. Rubin, MD, FACG Co-Direct, Inflammaty Bowel Disease Center Fellowship Program Direct University of Chicago
Personalized Medicine in IBD
 Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Personalized Medicine in IBD Anita Afzali MD, MPH Assistant Professor of Medicine Director, Inflammatory Bowel Diseases Program University of Washington Harborview Medical Center CCFA April 2 nd, 2016
Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans. Presented by: Richard Veselý. An agency of the European Union
 Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans Presented by: Richard Veselý An agency of the European Union Adalimumab - Crohn s disease Indication: Treatment of severe,
Inflammatory bowel disease (IBD) Overview of the Paediatric investigation plans Presented by: Richard Veselý An agency of the European Union Adalimumab - Crohn s disease Indication: Treatment of severe,
Recent Advances in the Management of Refractory IBD
 Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Recent Advances in the Management of Refractory IBD Raina Shivashankar, M.D. Assistant Professor of Medicine Division of Gastroenterology and Hepatology Thomas Jefferson University Philadelphia, PA Outline
Ulcerative colitis (UC) is a chronic inflammatory
 Induction and Maintenance Therapy with Vedolizumab, a Novel Biologic Therapy for Ulcerative Colitis Feagan BG, Rutgeerts P, Sands BE, et al; GEMINI 1 Study Group. Vedolizumab as induction and maintenance
Induction and Maintenance Therapy with Vedolizumab, a Novel Biologic Therapy for Ulcerative Colitis Feagan BG, Rutgeerts P, Sands BE, et al; GEMINI 1 Study Group. Vedolizumab as induction and maintenance
Guideline Ulcerative colitis: management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel diseases: a real life experience
 Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Outcomes of immunosuppressors and biologic drugs in inflammatory bowel Treatments and therapeutic approaches in IBD are constantly evolving. The newly emerged biologic treatments are one such evolving
Ulcerative colitis (UC), an inflammatory bowel disease, can
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:391 399 Induction and Maintenance Therapy With Infliximab for Children With Moderate to Severe Ulcerative Colitis JEFFREY HYAMS,* LAKSHMI DAMARAJU, MARION
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:391 399 Induction and Maintenance Therapy With Infliximab for Children With Moderate to Severe Ulcerative Colitis JEFFREY HYAMS,* LAKSHMI DAMARAJU, MARION
Endpoints for Stopping Treatment in UC
 Endpoints for Stopping Treatment in UC Jana G. Hashash, MD Assistant Professor of Medicine Inflammatory Bowel Disease Center Division of Gastroenterology, Hepatology, and Nutrition University of Pittsburgh
Endpoints for Stopping Treatment in UC Jana G. Hashash, MD Assistant Professor of Medicine Inflammatory Bowel Disease Center Division of Gastroenterology, Hepatology, and Nutrition University of Pittsburgh
The use of a segmental endoscopic score may improve the prediction of clinical outcomes in acute severe ulcerative colitis
 1130-0108/2016/108/11/697-702 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 11, pp. 697-702 ORIGINAL PAPERS The use of a
1130-0108/2016/108/11/697-702 Revista Española de Enfermedades Digestivas Copyright 2016. SEPD y ARÁN EDICIONES, S.L. Rev Esp Enferm Dig 2016, Vol. 108, N.º 11, pp. 697-702 ORIGINAL PAPERS The use of a
Clinical Study Fecal Calprotectin and Clinical Disease Activity in Pediatric Ulcerative Colitis
 Hindawi Publishing Corporation ISRN Gastroenterology Volume 2013, Article ID 179024, 5 pages http://dx.doi.org/10.1155/2013/179024 Clinical Study Fecal Calprotectin and Clinical Disease Activity in Pediatric
Hindawi Publishing Corporation ISRN Gastroenterology Volume 2013, Article ID 179024, 5 pages http://dx.doi.org/10.1155/2013/179024 Clinical Study Fecal Calprotectin and Clinical Disease Activity in Pediatric
Lessons to learn from Crohn's disease clinical trials: implications for ulcerative colitis
 Lessons to learn from Crohn's disease clinical trials: implications for ulcerative colitis Aránzazu Jáuregui Amézaga, Elena Ricart, Julián Panés Department of Gastroenterology, Hospital Clínic de Barcelona,
Lessons to learn from Crohn's disease clinical trials: implications for ulcerative colitis Aránzazu Jáuregui Amézaga, Elena Ricart, Julián Panés Department of Gastroenterology, Hospital Clínic de Barcelona,
Efficacy and safety of adalimumab in the treatment of Crohn s disease in children
 1130-0108/2013/105/10/579-584 Revista Española de Enfermedades Digestivas Copyright 2013 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid Vol. 105, N.º 10, pp. 579-584, 2013 ORIGINAL PAPERS Efficacy and
1130-0108/2013/105/10/579-584 Revista Española de Enfermedades Digestivas Copyright 2013 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid Vol. 105, N.º 10, pp. 579-584, 2013 ORIGINAL PAPERS Efficacy and
Crohn's Disease. The What, When, and Why of Treatment
 Crohn's Disease The What, When, and Why of Treatment Sunanda Kane, MD, FACG Professor of Medicine Department of Gastroenterology and Hepatology Mayo Clinic Rochester, MN In my lecture today, I will be
Crohn's Disease The What, When, and Why of Treatment Sunanda Kane, MD, FACG Professor of Medicine Department of Gastroenterology and Hepatology Mayo Clinic Rochester, MN In my lecture today, I will be
Incidence of Colectomy During Long-term Follow-up After Cyclosporine-Induced Remission of Severe Ulcerative Colitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:760 765 Incidence of Colectomy During Long-term Follow-up After Cyclosporine-Induced Remission of Severe Ulcerative Colitis DAVID N. MOSKOVITZ, GERT VAN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:760 765 Incidence of Colectomy During Long-term Follow-up After Cyclosporine-Induced Remission of Severe Ulcerative Colitis DAVID N. MOSKOVITZ, GERT VAN
Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts
 Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts Asher Kornbluth, MD Clinical Professor of Medicine The Henry D. Janowitz The Mt. Sinai School of Medicine Refining our Management
Ulcerative Colitis: Refining our Management and Incorporating Newer Concepts Asher Kornbluth, MD Clinical Professor of Medicine The Henry D. Janowitz The Mt. Sinai School of Medicine Refining our Management
Budesonide Use and Hospitalization Rate in Crohn s Disease: Results From a Cohort at a Tertiary Care IBD Referral Center
 Elmer ress Original Article J Clin Med Res. 2016;8(10):705-709 Budesonide Use and Hospitalization Rate in Crohn s Disease: Results From a Cohort at a Tertiary Care IBD Referral Center Jordan Orr a, d,
Elmer ress Original Article J Clin Med Res. 2016;8(10):705-709 Budesonide Use and Hospitalization Rate in Crohn s Disease: Results From a Cohort at a Tertiary Care IBD Referral Center Jordan Orr a, d,
