Effect of Vertical or Beveled Chondral Defect Creation on Rim Deformation and Contact
|
|
|
- Gwen Shepherd
- 5 years ago
- Views:
Transcription
1 XXX / CARTILAGEYanke et al. research-article2018 iginal Article Effect of Vertical or Beveled Chondral Defect Creation on Rim Deformation and Contact Cartilage 1 7 The Author(s) 2018 Reprints and permissions: sagepub.com/journalspermissions.nav DOI: journals.sagepub.com/home/car Adam B. Yanke 1, Megan L. Konopka 1, Davietta C. Butty 1, Maximilian A. Meyer 1, Eric J. Cotter 1, Alejandro A. Espinoza 1, and Brian J. Cole 1 Abstract Objective. To determine biomechanical effects of knee cartilage defect perimeter morphology based on cartilage strain and opposing subchondral bone contact. Design. Articular cartilage defects were created in 5 bovine femoral condyles: group 1, 45 inner bevel with 8-mm rim; group 2, vertical with 8-mm rim; and group 3, 45 outer bevel with 8-mm base. Samples were placed into a custom-machined micro computed tomography tube and subjected to 800 N of axial loading. DICOM data were used to calculate cartilage thickness 4 and 6 mm from the center, distance between tibial cartilage surface and femoral subchondral bone, and contact width between tibial cartilage and subchondral bone. Strain 4 mm from the center and both absolute and change in distance (mm) to subchondral bone were compared between groups 1 and 2 using paired t tests. Strain at 6 mm and distance changed, loaded distance, and contact width (mm) were compared between groups using the Friedman test with post hoc analysis using Wilcoxon signed rank test. Results. No significant differences in rim strain were noted between groups 1 and 2 at 4 mm (P = 0.10) and between groups 1, 2, and 3 at 6 mm (P = 0.247) from the defect center. The loaded distance was significantly different between groups 1 and 3 (P = 0.013). No significant change in distance to the subchondral bone was found between groups (P = 0.156). The difference in subchondral bone contact area approached but did not reach significance (P = 0.074). Conclusion. When debriding focal articular cartilage defects, establishment of an inner bevel decreases tissue deformation and contact with opposing subchondral bone. Keywords articular cartilage, debridement, perimeter morphology, bevel Introduction Cartilage defects of the knee cause a significant burden to both the patient by generating pain and society by expediting progression of osteoarthritis. It is estimated that approximately 63% of individuals undergoing arthroscopy have articular cartilage defects. 1 Much of this is due to the inability of cartilage to restore its native structure. 2 While treatments continue to evolve, ranging from simple debridement to cell-based surface treatments, the first step of nearly every cartilage restoration procedure remains preparation of a stable vertical wall at the periphery of the defect. 3,4 Survey data suggests that 97% of surgeons debride cartilage back to a stable layer while performing microfracture. 5 While this is likely advantageous in the setting of microfracture, it is unclear if it is beneficial to perform the procedure in a similar manner when performing debridement alone. Nearly 3 decades ago, the veterinary community explored the effect of peripheral wall morphology in the debridement of articular cartilage defects and concluded that beveled walls may lead to cartilage defect size progression. 6 However, the beveling process in this study necessarily enlarged the defects and therefore clouded accurate assessment of disease progression. This point has not undergone further discussion, and the assumption remains that vertical walls are superior. Clinically, cartilage defects are still commonly debrided as part of a staging arthroscopy or as the first stage of a 2-stage restoration. Yet it remains unclear if debridement to a vertical wall yields biomechanical advantages, such as decreased compressive ability or reduced subchondral bone contact, in comparison 1 Department of thopaedic Surgery, Rush University Medical Center, Chicago, IL, USA Corresponding Author: Brian J. Cole, Department of thopaedic Surgery, Rush University Medical Center, 1611 West Harrison Street, Suite 300, Chicago, IL 60611, USA. bcole@rushortho.com
2 2 Cartilage 00(0) Figure 1. Illustration of the 3 medial femoral condyle defects evaluated in this study.[aq: 3] to an inner or outer bevel. The purpose of this study was to determine the local biomechanical effects of cartilage defect perimeter morphology based on cartilage strain and contact with opposing subchondral bone. The authors hypothesized that increasing the surface diameter of a cartilage defect would increase opposing contact with subchondral bone and that vertical walls would have greater strain resistance than beveled walls. Methods Sample Preparation and Defect Creation Bovine knees (n = 5) were harvested and the articular surface of the medial femoral condyle was exposed. The knee was placed in a vice and Kirschner wires were passed across the joint to maintain native congruity. The center of the medial femoral condyle was harvested using a 30-mm coring reamer, taking care to remain perpendicular to the articular surface. A corresponding core of articular cartilage of the tibial plateau was harvested using the same process. After this was complete, fullthickness cartilage defects were created in the femoral condyle according to the following groups: (1) inner bevel with-8 mm rim, (2) vertical with 8-mm rim, and (3) outer bevel with 8-mm base (Fig. 1). These were created sequentially by starting with a 2-mm skin biopsy punch. For group 1, this was followed by creation of a 45 beveled defect with a custom-machined device, resulting in a 8-mm rim at the chondral surface. This was followed by an 8-mm skin biopsy punch to progress to group 2. In a similar fashion to group 1, a second custom-machined device was used to create 45 beveled walls with an inner base diameter of 8 mm. Figure 2. Illustration of a custom-machined micro computed tomography (µct) tube that allows for controlled axial loading. Sample Testing and Imaging To prepare the samples for computed tomography (CT) imaging, the femoral plug was stained overnight at 4 C with 40% Hexabrix ioxaglate radiological contrast (Guerbet, Roissy, France) and 60% 0.15 M phosphate buffered saline (PBS), which renders articular cartilage surfaces distinguishable by micro-ct. After removing excess solution with gauze, the samples were loaded in apposition to approximate anatomical orientation into a custom-machined micro-ct tube that allowed for controlled axial loading (Fig. 2). To limit variability, all samples were marked to ensure the same
3 Yanke et al. 3 Figure 3. Micro computed tomography (µct) images of all defect groups both with and without axial loading. orientation with each subsequent scan. For each sample and defect size, images were obtained in the micro-ct scanner (Scanco uct 50, Bruettisellen, Switzerland) without and then with axial loading (Fig. 3). For all samples, micro-ct was set at scanner, μct40 μct50; voxel size, 40 μm; x-ray tube potential (peak), 70 kvp; x-ray intensity, 114 μa; integration time, 300 [AQ: 1]. The applied load was monitored through a miniature load cell placed inside the tube (Omega LC307-series 1000 N button load-cell, Omegadyne, Inc., Sunbury, OH). The sample was loaded to 800 N using this method. The loaded sample was allowed to relax and equilibrate over the course of 10 minutes, with measurements of decremental load dissipation occurring each minute prior to being introduced to the micro-ct scanner. Scan time was approximately 45 minutes per sample. All testing for a given sample was done without any freeze-thaw cycles in between and completed on the same day. Data Collection and Analysis Raw DICOM (Digital Imaging and Communications in Medicine) data from the micro-ct scanner was imported into OsiriX (Pixmeo SARL, ). Using 3-dimensional (3D) orthogonal reconstructions, sample images were reoriented to the same plane using anatomic landmarks to ensure the same view was analyzed for all groups. Using the coronal reconstructions, the following data were obtained for the loaded and unloaded samples in all groups: cartilage thickness 4 and 6 mm from the center, minimum distance of tibial cartilage surface to the center of exposed femoral subchondral bone, and, if contacting, the width of the contact of the cartilage on the bone. Whenever possible, measurement was made at the center of the defect and checked using 3D reconstructions to minimize variability. Using descriptive statistics (average and standard deviation), the strain applied at 4 and 6 mm from the center was calculated. These peripheral defect measurements were taken at the same respective location on both sides of each defect type within a sample. Strain was calculated using the equation ε = [(d d 0 )/d 0 ] 100. The absolute length and change in distance to the subchondral bone was also calculated (Fig. 4). Using paired t tests, strain at 4 mm was compared between group 1 and group 2. Strain at 6 mm was compared between all groups using first a repeated-measures 1-way analysis of variance; however, the data proved to have an outlier value, so a Friedman test was used given the nonparametric nature of the data. The amount of 2D contact and distance (mm) to the subchondral bone was also compared between all groups using a Friedman test. Significance for all tests was set at P < Statistical calculations were carried out using the SPPS 18.0 (SPSS, Chicago, IL, USA).
4 4 Cartilage 00(0) Figure 4. Schematic of measurements taken. In all cases, d 0 and d correspond to distances measured in the unloaded and loaded conditions, respectively. Given that the subchondral layer is exposed, d 0 and d also equal the distance to subchondral bone in the unloaded and loaded conditions, respectively, when measured from the center of the defect. The 4 mm radius measurements are shown in blue, and the 6 mm measurements are shown in green. In all cases, strain is calculated as ε = [(d d 0 )/d 0 ] 100 to show the strain at the wall height, with d always smaller than d 0. Note that the bevel angle decreases below 45 after the load is applied in groups 1 and 3. Measurement of cartilage wall height at 4 mm radius is not possible for group 3 because that material has already been removed by the bevel. Results Rim strain did not change significantly within groups when moving from 4 to 6 mm from the center of the defect. When comparing rim strain at 4 and 6 mm, there were no significant differences between groups (4 mm, 0.61 ± 0.10 and 0.50 ± 0.16 for groups 1 and 2, respectively; 6 mm, 0.54 ± 0.11, 0.47 ± 0.17, and 0.64 ± 0.17 for Groups 1, 2, and 3, respectively; P > 0.05) (Table 1). On axial loading, a significant difference was shown between group 1 (0.82 ± 0.33), group 2 (0.50 ± 0.41), and group 3 (36 ± 0.44) (P = 0.015). On post hoc analysis using Wilcoxon signed rank test, group 1 exhibited a significantly greater loaded distance compared Table 1. Differences in Rim Strain Between Groups. Group 4-mm Strain 6-mm Strain ± ± ± ± Not applicable 0.64 ± 0.17 P with group 3, that is, changing the wall profile from inner bevel to outer bevel) (P = 0.013) (Table 2). No significant differences were noted between group in the minimum distance of tibial cartilage surface to the center of exposed
5 Yanke et al. 5 Table 2. Differences in Distance to Subchondral Bone Between Groups. Group 1 Group 2 Group 3 P Loaded distance (mm) 0.82 ± ± ± a Distance change (mm) 1.09 ± ± ± Contact (mm) 0 ± ± ± a Group 1 versus group 3 had a P value = in post hoc analysis using Wilcoxon signed rank test. femoral subchondral bone. Group 1 defects did not display any contact with opposing subchondral bone. However, no significant difference was noted in the amount of opposing subchondral bone contact area between groups. Discussion This study resulted from the basic assumption that, just as a car tire traveling over a pothole may experience different amounts of deformation based on the size and morphology of the hole, similar effects may be noticed with cartilage defects (Fig. 5). Specifically, the increased surface diameter may be more predictive of deformation and contact of the healthy cartilage with the opposing subchondral bone. The findings of this study suggest that keeping an inner bevel of tissue may decrease tissue contact with the opposing subchondral bone. Proposed clinical consequences of preserving subchondral bone from contact and subsequent sclerosis include decreased pain after debridement, as articular cartilage is aneural, as well as improved success rates for downstream cartilage restoration strategies, such as autologous chondrocyte implantation. 7,8 Further human studies are needed to determine the extent to which contact with subchondral bone affects pain and functional outcomes. While not significant, there was a trend toward the ability of vertical walls to shield the neighboring tissue from strain. Prior work has demonstrated that there is a critical defect size at which rim stress increases significantly. Brown et al. 9 demonstrated that the critical strain size for canine models is 2 mm. Similarly, Guettler et al. 10 demonstrated no change in surrounding peak stress in human knees until defects were >8 mm in diameter, with a 64% increase in 10-mm defects. Interestingly, there was no increased peak stress when moving from 10- to 20-mm defects. Our study therefore chose to evaluate an inner and outer bevel from this 8-mm critical value since bovine knees are similar to human knees in overall size. However, while moving from group 2 to group 3 increased the lesion surface radius from 4 to 6 mm, there was no significant change in strain at 6 mm. This suggests that at this size there was no effect of protecting the cartilage from deformation, while it did decrease the amount of deformation on the contralateral surface. The results of this study are revealing when evaluated in the setting of the work by Rudd et al. 6 Specifically, while Figure 5. Deformation of a car tire depends largely on the size and shape of the pothole that it passes over. Similarly, debridement of cartilage defects to either beveled (top) or vertical (bottom) walls may alter biomechanical properties such as deformation, strain, and contact with subchondral bone. the authors did not see defect size progression with beveling defects, they reported increased erosion on the surface opposing the beveled defects. The authors attribute this finding to be more related to the overall superficial diameter of the defect than to the morphology of the rim itself. In this light, this is why there was more effect on strain when moving from group 2 to 3 as opposed to moving from group 1 to 2. Beveling may also have the effect of increased sliding strain magnitudes as compared to nonbeveled defects. 11
6 6 Cartilage 00(0) Limitations This study has several limitations, including the limitations of any in vitro analysis. This study is limited with regard to the variability in the bovine knee contour and specific location of the defect. While each statistical comparison was made within the same knee, there is still increased variability that is imposed on the system due to these differences. However, the authors still felt that this model is more clinically relevant than a pure finite element analysis simulation without this variability. Furthermore, in order to create 3 distinct groups, the beveling process necessarily removed differing amounts of tissue for each group, which may confound interpretation of local strain results. However, in order to analyze 3 potential debridement strategies for a roughly 8-mm defect in a clinically relevant fashion, such differences in volume removed were considered unavoidable. While all attempts were made to apply uniform loading, it was not possible to monitor this during the scanning procedure. Also, the tissue used was healthy and therefore the properties of degenerative tissue left at the base of the defect may not be represented. This property has been described by Nelson et al. 12 where they demonstrated no difference in rim stress in fresh canine defects and in those filled with fibrocartilage. Finally, the methods employed with µct are novel and provide different information than pressure sensors that have shown to have an error ranging from 11.7% to 20%. 13 Conclusion Though this study could not evaluate degenerative tissue, the findings suggest that the establishment of an inner bevel in the treatment of articular cartilage defects in the knee provides unique biomechanical advantages, namely decreasing tissue deformation and subsequent contact with opposing subchondral bone. Clinical studies are needed to determine if these advantages translate to clinically relevant decreases in patient pain after debridement. As expected, there does not appear to be a role for an outer bevel into healthy adjacent cartilage tissue. Acknowledgments and Funding The research was conducted at Rush University Medical Center. The study was internally funded. Declaration of Conflicting Interests The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: ABY reports research support from Anthrax, Inc. and NuTech Medical and serves as a paid consultant for JRF tho. BJC reports the following disclosures: Aesculap/B.Braun, research support; American Journal of thopedics, editorial or governing board; American thopaedic Society for Sports Medicine, board or committee member; American Shoulder and Elbow Surgeons, board or committee member; Arthrex, Inc., intellectual property royalties, paid consultant, research support; Arthroscopy, editorial or governing board; Arthroscopy Association of North America, board or committee member; Athletico, other financial or material support; Cytori, research support; Elsevier Publishing, intellectual property royalties; International Cartilage Repair Society, board or committee member; Journal of Bone and Joint Surgery American, editor; Journal of Shoulder and Elbow Surgery, editor; Journal of the American Academy of thopaedic Surgeons, editor; National Institutes of Health (NIAMS and NICHD), research support; Ossur, other financial or material support; Regentis, paid consultant, stock or stock options; Saunders/Mosby-Elsevier, publishing royalties, financial or material support; Smith & Nephew, other financial or material support; Tornier, other financial or material support. Ethical Approval Ethical approval for this study was obtained from *NAME OF ETHICS COMMITTEE OR INSTITUTIONAL REVIEW BOARD (APPROVAL NUMBER/ID)*.[AQ: 2] Ethical approval for this study was waived by *NAME OF ETHICS COMMITTEE OR INSTITUTIONAL REVIEW BOARD* because *REASON FOR WAIVER*. Ethical approval was not sought for the present study because *REASON*. Animal Welfare The present study followed international, national, and/or institutional guidelines for humane animal treatment and complied with relevant legislation. The present study involved client-owned animals; it demonstrated a high standard (best practice) of veterinary care and involved informed client consent. Guidelines for humane animal treatment did not apply to the present study because *REASON*. References 1. Curl WW, Krome J, Gordon ES, Rushing J, Smith BP, Poehling GG. Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy. 1997;13(4): Hunter W. Of the structure and disease of articulating cartilages. Philos Trans R Soc Lond B Biol Sci. 1743;42B: Riboh JC, Cole BJ, Farr J. Particulated articular cartilage for symptomatic chondral defects of the knee. Curr Rev Musculoskelet Med. 2015;8(4): Pascual-Garrido C, McNickle AG, Cole BJ. Surgical treatment options for osteochondritis dissecans of the knee. Sports Health. 2009;1(4): Theodoropoulos J, Dwyer T, Whelan D, Marks P, Hurtig M, Sharma P. Microfracture for knee chondral defects: a survey of surgical practice among Canadian orthopedic surgeons. Knee Surg Sports Traumatol Arthrosc. 2012;20(12):
7 Yanke et al Rudd RG, Visco DM, Kincaid SA, Cantwell HD. The effects of beveling the margins of articular cartilage defects in immature dogs. Vet Surg. 1987;16(5): Minas T, Gomoll AH, Rosenberger R, Royce RO, Bryant T. Increased failure rate of autologous chondrocyte implantation after previous treatment with marrow stimulation techniques. Am J Sports Med. 2009;37(5): Flanigan DC, Harris JD, Brockmeier PM, Siston RA. The effects of lesion size and location on subchondral bone contact in experimental knee articular cartilage defects in a bovine model. Arthroscopy 2010;26(12): Brown TD, Pope DF, Hale JE, Buckwalter JA, Brand RA. Effects of osteochondral defect size on cartilage contact stress. J thop Res. 1991;9(4): Guettler JH, Demetropoulos CK, Yang KH, Jurist KA. Osteochondral defects in the human knee: influence of defect size on cartilage rim stress and load redistribution to surrounding cartilage. Am J Sports Med. 2004;32(6): Gratz KR, Wong BL, Bae WC, Sah RL. The effects of focal articular defects on cartilage contact mechanics. J thop Res. 2009;27(5): Nelson BH, Anderson DD, Brand RA, Brown TD. Effect of osteochondral defects on articular cartilage. Contact pressures studied in dog knees. Acta thop Scand. 1988;59(5): Drewniak EI, Crisco JJ, Spenciner DB, Fleming BC. Accuracy of circular contact area measurements with thin-film pressure sensors. J Biomech. 2007;40(11):
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague Communicator: Josiah Wolf BWIG: David Fiflis BPAG: Zach Wodushek BSAC: Grace Li Client: Dr. Brian Walczak, DO Advisor: Dr. William Murphy,
Osteochondral Transplant Delivery System Team Leader: Alex Teague Communicator: Josiah Wolf BWIG: David Fiflis BPAG: Zach Wodushek BSAC: Grace Li Client: Dr. Brian Walczak, DO Advisor: Dr. William Murphy,
1 Department of Orthopaedic Surgery, Akershus University Hospital,
 483546CARXXX10.1177/1947603513483546CartilageÅrøen et al research-article2013 Article Agreement in Arthroscopic and Arthrotomy Assessment of Full-Thickness Articular Cartilage Lesions of the Knee in a
483546CARXXX10.1177/1947603513483546CartilageÅrøen et al research-article2013 Article Agreement in Arthroscopic and Arthrotomy Assessment of Full-Thickness Articular Cartilage Lesions of the Knee in a
Osteochondral Transplant Delivery System
 Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Osteochondral Transplant Delivery System Team Leader: Alex Teague BPAG: David Fiflis Communicator/BWIG: Alex Babinski BSAC: Zach Wodushek Client: Dr. Brian Walczak, DO Advisor: Dr. Tracy Puccinelli, PhD
Case Report. Byung Ill Lee, MD and Byoung Min Kim, MD Department of Orthopedic Surgery, Soonchunhyang University Hospital, Seoul, Korea
 Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Osteochondral allografting for all other joints is not covered as the evidence is insufficient to determine the
 Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Subchondral Bone Density Distribution in Cam Type Femoroacetabular Impingement Hips
 Subchondral Bone Density Distribution in Cam Type Femoroacetabular Impingement Hips Nozomu Inoue MD, PhD Simon Lee MPH Shane J. Nho MD, MS Department of Orthopedic Surgery Rush University Medical Center
Subchondral Bone Density Distribution in Cam Type Femoroacetabular Impingement Hips Nozomu Inoue MD, PhD Simon Lee MPH Shane J. Nho MD, MS Department of Orthopedic Surgery Rush University Medical Center
Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and. Subchondral Bone Contact of Focal Cartilage Defects of the Knee
 Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and Subchondral Bone Contact of Focal Cartilage Defects of the Knee Undergraduate Research Thesis Presented in Partial Fulfillment
Effects of Meniscus and Defect Size, Location and Orientation on Rim Stress and Subchondral Bone Contact of Focal Cartilage Defects of the Knee Undergraduate Research Thesis Presented in Partial Fulfillment
Disclosures. How to approach cartilage repair. Articular Cartilage Problems: Surface Options
 Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Cartilage Repair Center Brigham and Women s Hospital Harvard Medical School
 Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Brigham and Women s Hospital Harvard Medical School Safety, feasibility, and radiographic outcomes of the anterior meniscal takedown technique to approach chondral defects on the tibia and posterior femoral
Management of Glenoid and Humeral Bone Loss in Shoulder Instability
 Short Stem and Long Stem Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics Today Short Stem
Short Stem and Long Stem Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox and Bulls Chief Medical Editor, Orthopaedics Today Short Stem
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Three-dimensional printing improves osteochondral allograft placement in complex cases
 https://doi.org/10.1007/s00167-018-4849-y KNEE Three-dimensional printing improves osteochondral allograft placement in complex cases Kelechi R. Okoroha 1 Timothy J. Evans 1 Jeffrey P. Stephens 2 Eric
https://doi.org/10.1007/s00167-018-4849-y KNEE Three-dimensional printing improves osteochondral allograft placement in complex cases Kelechi R. Okoroha 1 Timothy J. Evans 1 Jeffrey P. Stephens 2 Eric
Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status
 # 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
# 154134 Survivorship After Meniscal Allograft Transplantation According To Articular Cartilage Status Jun-Gu Park, Seong-Il Bin, Jong-Min Kim, Bum Sik Lee Department of Orthopaedic Surgery, Asan Medical
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri
 In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
In-vivo Evaluation Of The Kinematic Behavior Of An Artificial Medial Meniscus Implant: A Pilot Study Using Open-mri Tineke De Coninck, MD 1, Jonathan J. Elsner, PhD 2, Maoz Shemesh, MSc 2, Michiel Cromheecke,
Nabeel Salka, MSE & John A. Grant, MD, PhD, FRCSC. MedSport, Department of Orthopedic Surgery University of Michigan, Ann Arbor, MI
 Contralateral Lateral Femoral Condyle Allografts Provide an Acceptable Surface Match for Simulated Osteochondritis Dissecans Lesions of the Medial Femoral Condyle Nabeel Salka, MSE & John A. Grant, MD,
Contralateral Lateral Femoral Condyle Allografts Provide an Acceptable Surface Match for Simulated Osteochondritis Dissecans Lesions of the Medial Femoral Condyle Nabeel Salka, MSE & John A. Grant, MD,
Cole Research. Evolving Modern Medicine
 Cole Research Evolving Modern Medicine Cole Research Brian Cole M.D., M.B.A. Professor, Department of Orthopedics, Department of Anatomy and Cell Biology; Section Head, Cartilage Restoration Center at
Cole Research Evolving Modern Medicine Cole Research Brian Cole M.D., M.B.A. Professor, Department of Orthopedics, Department of Anatomy and Cell Biology; Section Head, Cartilage Restoration Center at
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Quantitative Analysis of Vascular Canals in Vertebral Endplate
 Quantitative Analysis of Vascular Canals in Vertebral Endplate Kristine Tan 1, Won C. Bae, PhD 1, Tomonori Yamaguchi, MS 1,2, Kelli Xu, BS 1, Iris Shieh, BS 1, Jade He, BS 1, Robert L. Sah, MD, ScD 1,
Quantitative Analysis of Vascular Canals in Vertebral Endplate Kristine Tan 1, Won C. Bae, PhD 1, Tomonori Yamaguchi, MS 1,2, Kelli Xu, BS 1, Iris Shieh, BS 1, Jade He, BS 1, Robert L. Sah, MD, ScD 1,
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Arthroscopy / MRI Correlation Conference. Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16
 Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
Arthroscopy / MRI Correlation Conference Department of Radiology, Section of MSK Imaging Department of Orthopedic Surgery 7/19/16 Case 1: 29 YOM with recurrent shoulder dislocations Glenoid Axial T1FS
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Meniscal Allograft Transplantation in the Adolescent Population
 Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Meniscal Allograft Transplantation in the Adolescent Population Jonathan C. Riboh, M.D., Annemarie K. Tilton, B.S., Gregory L. Cvetanovich, M.D., Kirk A. Campbell, M.D., and Brian J. Cole, M.D., M.B.A.
Public Disclosure Information for Selected Customers
 Page 1 of 9 h Jeffrey S Abrams, MD: Submitted on: 10/07/2017 Arthrocare: Stock or stock Options Cayenne Medical: Stock or stock Options ConMed Linvatec: Paid consultant Ingen Medical: Stock or stock Options;
Page 1 of 9 h Jeffrey S Abrams, MD: Submitted on: 10/07/2017 Arthrocare: Stock or stock Options Cayenne Medical: Stock or stock Options ConMed Linvatec: Paid consultant Ingen Medical: Stock or stock Options;
OCD: Beyond Microfracture. Disclosures. OCD Talus: My Approach 2/23/2018
 OCD: Beyond Microfracture Gregory C Berlet MD, FRCS(C), FAOA Orthopedic Foot and Ankle Center Columbus Ohio Disclosures Consultant/Speaker Bureau/Royalties/ Stock: Wright Medical, Stryker, ZimmerBiomet,
OCD: Beyond Microfracture Gregory C Berlet MD, FRCS(C), FAOA Orthopedic Foot and Ankle Center Columbus Ohio Disclosures Consultant/Speaker Bureau/Royalties/ Stock: Wright Medical, Stryker, ZimmerBiomet,
Why do they fail?? TOM MINAS MD MS. The Management of Failed Cartilage Repair Procedures PALM BEACH FL
 The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement
 016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
016625 REVISION R INVISION Total Ankle Replacement System with PROPHECY Preoperative Navigation Revision of a Failed Agility Total Ankle Replacement CASE STUDY Patient History The patient was a 65-year-old
Specimen. Humeral Head. Femoral Head. Objective. Femoral Condyle (medial) Supplementary Figure 1
 A B Specimen Humeral Head 2 1 µm 76 µm Femoral Head Objective Femoral Condyle (medial) Supplementary Figure 1 A Femoral Head Global Cell Density Superficial Cell Density Cell Number at 1 µm Nuclei /.1
A B Specimen Humeral Head 2 1 µm 76 µm Femoral Head Objective Femoral Condyle (medial) Supplementary Figure 1 A Femoral Head Global Cell Density Superficial Cell Density Cell Number at 1 µm Nuclei /.1
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Using the depth probe, determine the appropriate implant size (thickness) for use. The
Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique
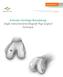 Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique PATIENT CONDYLE PREPARATION Step 1: Perform a parapatellar arthrotomy, and retract the patella to expose the condyle.
Articular Cartilage Resurfacing Single Osteochondral Allograft Plug Surgical Technique PATIENT CONDYLE PREPARATION Step 1: Perform a parapatellar arthrotomy, and retract the patella to expose the condyle.
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation
 Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation A Comparative Matched Group Analysis Rachel M. Frank,* y MD, Simon Lee, z MD, MPH, Eric
Outcomes of Osteochondral Allograft Transplantation With and Without Concomitant Meniscus Allograft Transplantation A Comparative Matched Group Analysis Rachel M. Frank,* y MD, Simon Lee, z MD, MPH, Eric
5:05 6:05 pm Live Surgery: office based Arthroscopy (Trice Medical) (1 hr) Surgeon: Sean McMillan, DO Moderator: Chris Uggen, MD
 AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Horizon Scanning Centre November Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects
 Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Disclosures: C.B. Raub: None. B.C. Hansen: None. T. Yamaguchi: None. M.M. Temple-Wong: None. K. Masuda: None. R.L. Sah: None.
 En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
En Face Microscopy of Rabbit Knee Articular Cartilage Following Anterior Cruciate Ligament Transection Reveals Early Matrix Damage, Chondrocyte Loss and Cloning Christopher B. Raub, PhD, Bradley C. Hansen,
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Meniscus Reconstruction: Trough Surgical Technique
 Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Meniscus Reconstruction: Trough Surgical Technique Technique Consultant Jeffrey L. Halbrecht, M.D. San Francisco, CA ABOUT THE TROUGH TECHNIQUE The trough technique for meniscal allograft reconstruction
Osteochondral regeneration. Getting to the core of the problem.
 Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
Osteochondral regeneration. Getting to the core of the problem. TM TM Bio-mimetic, biointegratable and resorbable Flexible and easy to shape Straightforward one-step procedure Promotes a guided osteo-chondral
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
3/9/2018. Algorithm for Massive RCT s. Massive Rotator Cuff Tears: When is Reverse TSA the only option?
 Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Massive Rotator Cuff Tears: When is Reverse TSA the only option? Anthony A. Romeo, MD Professor, Department of Orthopedics Head, Section of Shoulder and Elbow Surgery Team Physician, Chicago White Sox
Predicting the Position of the Femoral Head Center
 The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
The Journal of Arthroplasty Vol. 14 No. 1 1999 Predicting the Position of the Femoral Head Center Nobuhiko Sugano, MD, Philip C. Noble, PhD, and Emir Kamaric, MS Abstract: To find an accurate method to
Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement
 Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement Gary J. Farkas, BS 1, Marc Haro, MD 1, Simon Lee, MPH 1, Philip Malloy 2, Alejandro A.
Hip Center Edge Angle and Alpha Angle Morphological Assessment Using Gait Analysis in Femoroacetabular Impingement Gary J. Farkas, BS 1, Marc Haro, MD 1, Simon Lee, MPH 1, Philip Malloy 2, Alejandro A.
The Impact of Age on Knee Injury Treatment
 The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver
 Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
Direct Measurement of Graft Tension in Anatomic Versus Non-anatomic ACL Reconstructions during a Dynamic Pivoting Maneuver Scott A. Buhler 1, Newton Chan 2, Rikin Patel 2, Sabir K. Ismaily 2, Brian Vial
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation
 First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
Why the dog? Analogy of the anatomy
 Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Why the dog? Analogy of the anatomy Surgically Induced canine OA models: Anterior (cranial) cruciate ligament transection model Pond MJ, Nuki G. Ann Rheum Dis 1973 (and > 100 others) Meniscal disruption
Where to Draw the Line:
 Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Where to Draw the Line: Anatomical Measurements Used to Evaluate Patellofemoral Instability Murray Grissom, MD 1 Bao Do, MD 2 Kathryn Stevens, MD 2 1 Santa Clara Valley Medical Center, San Jose, CA 2 Stanford
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Chondral Injuries in the Athlete
 Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Bone&JointAppraisal Vol
 Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Bone&JointAppraisal Vol 01 No 03 December 2016 COBLATION Chondroplasty Versus Mechanical Debridement: Randomized Controlled Trial with 10-Year Outcomes -Year Four-Year Ten-Year Group A COBLATION technology
Corporate Medical Policy
 Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Corporate Medical Policy Continuous Passive Motion in the Home Setting File Name: Origination: Last CAP Review: Next CAP Review: Last Review: continuous_passive_motion_in_the_home_setting 9/1993 6/2018
Tibial Cartilage Defects
 Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Tibial Cartilage Defects Kevin C. Wang 1 Rachel M. Frank 2 Brian J. Cole 3 Email brian.cole@rushortho.com 1 2 3 Department of Orthopedics, Icahn School of Medicine at Mount Sinai, New York, NY, USA Department
Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation for the Repair of Chondral Defects of the Knee
 International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
Surgical Navigation for Articular Cartilage Repair: Motivation, Development, and Validation. Thesis
 Surgical Navigation for Articular Cartilage Repair: Motivation, Development, and Validation Thesis Presented in Partial Fulfillment of the Requirements for the Degree of Master of Science in the Graduate
Surgical Navigation for Articular Cartilage Repair: Motivation, Development, and Validation Thesis Presented in Partial Fulfillment of the Requirements for the Degree of Master of Science in the Graduate
Where Is the Natural Internal-External Rotation Axis of the Tibia?
 Where Is the Natural Internal-External Rotation Axis of the Tibia? Daniel Boguszewski 1, Paul Yang 2, Nirav Joshi 2, Keith Markolf 1, Frank Petrigliano 1, David McAllister 1. 1 University of California
Where Is the Natural Internal-External Rotation Axis of the Tibia? Daniel Boguszewski 1, Paul Yang 2, Nirav Joshi 2, Keith Markolf 1, Frank Petrigliano 1, David McAllister 1. 1 University of California
Experimental Prediction of Contact Area in Hip Replacement and Hemi- Arthroplasty
 Experimental Prediction of Contact Area in Hip Replacement and Hemi- Arthroplasty Qianqian Wang, John Fisher, Sophie Williams. Institute of Medical and Biological Engineering, School of Mechanical Engineering,
Experimental Prediction of Contact Area in Hip Replacement and Hemi- Arthroplasty Qianqian Wang, John Fisher, Sophie Williams. Institute of Medical and Biological Engineering, School of Mechanical Engineering,
Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study
 Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study Natacha Rosa, Fernão D. Magalhães, Ricardo Simões and António Torres Marques Enhanced Bone Healing in intramedullary
Nailing Stability during Tibia Fracture Early Healing Process: A Biomechanical Study Natacha Rosa, Fernão D. Magalhães, Ricardo Simões and António Torres Marques Enhanced Bone Healing in intramedullary
Dimensions of the intercondylar notch and the distal femur throughout life
 Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Dimensions of the intercondylar notch and the distal femur throughout life Poster No.: P-0089 Congress: ESSR 2013 Type: Scientific Exhibit Authors: L. Hirtler, S. Röhrich, F. Kainberger; Vienna/AT Keywords:
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical 2 Assessment 1. Proper implant sizing is determined by placing the appropriate sized trial over the
Medial Meniscal Root Tears: When to rehab? When to repair? When to debride. Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT
 Medial Meniscal Root Tears: When to rehab? When to repair? When to debride Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT Disclosure Consultant Mitek Smith and Nephew-biologic patch Good
Medial Meniscal Root Tears: When to rehab? When to repair? When to debride Christopher Betz, DO Orthopedics Sports Medicine Bristol, CT Disclosure Consultant Mitek Smith and Nephew-biologic patch Good
Roof Impingement Revisited
 Roof Impingement Revisited John A Tanksley MD, Evan J Conte MD, Brian C Werner MD, F Winston Gwathmey MD, Stephen F Brockmeier MD, Mark D Miller MD, University of Virginia, Charlottesville, VA Introduction
Roof Impingement Revisited John A Tanksley MD, Evan J Conte MD, Brian C Werner MD, F Winston Gwathmey MD, Stephen F Brockmeier MD, Mark D Miller MD, University of Virginia, Charlottesville, VA Introduction
YEAR DATA STEP. Proven results in cartilage repair. CARGEL Bioscaffold. Supporting healthcare professionals for over 150 years
 5- YEAR DATA 1 STEP Proven results in cartilage repair CARGEL Bioscaffold Supporting healthcare professionals for over 150 years Proven Performance I Simplicity I Versatility What is CARGEL Bioscaffold?
5- YEAR DATA 1 STEP Proven results in cartilage repair CARGEL Bioscaffold Supporting healthcare professionals for over 150 years Proven Performance I Simplicity I Versatility What is CARGEL Bioscaffold?
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Presented By Dr Vincent VG An MD BSc (Adv) MPhil Dr Murilo Leie MD Mr Joshua Twiggs BEng Dr Brett A Fritsch MBBS FRACS (Orth) FAOrthA.
 A comparison of kinematic and mechanical alignment with regards to bony resection, soft tissue release, and deformity correction in total knee replacement Presented By Dr Vincent VG An MD BSc (Adv) MPhil
A comparison of kinematic and mechanical alignment with regards to bony resection, soft tissue release, and deformity correction in total knee replacement Presented By Dr Vincent VG An MD BSc (Adv) MPhil
CARTIVA. Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING.
 CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
CARTIVA Synthetic Cartilage Implant SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT TABLE OF CONTENTS Introduction... 3 Cartiva
Torn ACL - Anatomic Footprint ACL Reconstruction
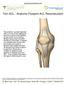 Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Torn ACL - Anatomic Footprint ACL Reconstruction The anterior cruciate ligament (ACL) is one of four ligaments that are crucial to the stability of your knee. It is a strong fibrous tissue that connects
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System
 Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
Knee Series Technique Guide Double Bundle ACL Reconstruction using the Smith & Nephew Outside-In Anatomic ACL Guide System Luigi Adriano Pederzini, MD Massimo Tosi, MD Mauro Prandini, MD Luigi Milandri,
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication
 UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
UvA-DARE (Digital Academic Repository) Treatment of osteochondral defects of the talus van Bergen, C.J.A. Link to publication Citation for published version (APA): van Bergen, C. J. A. (2014). Treatment
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
The cellfree matrix for autoregeneration of articular cartilage defects
 The cellfree matrix for autoregeneration of articular cartilage defects What is Amedrix GmbH? Amedrix GmbH, located in Esslingen near Stuttgart, is a medical biotech company which develops highly innovative
The cellfree matrix for autoregeneration of articular cartilage defects What is Amedrix GmbH? Amedrix GmbH, located in Esslingen near Stuttgart, is a medical biotech company which develops highly innovative
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Lateral Meniscus Transplant
 Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Lateral Meniscus Transplant Using the CONMED Meniscus Allograft Transplant (MAT) Instruments A complete guide to Lateral Meniscus Transplant using the CONMED meniscus allograft transplant Instruments.
Time Scales in Cartilage Impact Injury and Chondrocyte Death
 Time Scales in Cartilage Impact Injury and Chondrocyte Death Lena R. Bartell, Michelle L. Delco, DVM, Lawrence J. Bonassar, Lisa A. Fortier, Itai Cohen. Cornell University, Ithaca, NY, USA. Disclosures:
Time Scales in Cartilage Impact Injury and Chondrocyte Death Lena R. Bartell, Michelle L. Delco, DVM, Lawrence J. Bonassar, Lisa A. Fortier, Itai Cohen. Cornell University, Ithaca, NY, USA. Disclosures:
Adult osteochondritis dissecans (OCD) lesions are
 Clinical Outcomes of Osteochondral Allograft Transplantation for Secondary Treatment of Osteochondritis Dissecans of the Knee in Skeletally Mature Patients Eric J. Cotter, B.S., Rachel M. Frank, M.D.,
Clinical Outcomes of Osteochondral Allograft Transplantation for Secondary Treatment of Osteochondritis Dissecans of the Knee in Skeletally Mature Patients Eric J. Cotter, B.S., Rachel M. Frank, M.D.,
The Aging Athletes Knee
 The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
The Aging Athletes Knee Douglas P Tewes Orthopedic Sports Medicine Lincoln Orthopedic Center 1 Common Sports Knee Injuries Cartilage defects/chondromalacia Meniscal tears ACL tear Articular Cartilage injury/chondromalacia
Subchondral Bone Changes in Patients with Early Degenerative Joint Disease
 Subchondral Bone Changes in Patients with Early Degenerative Joint Disease Eric L. Radin, lgor L. Paul and Marc J. Tolkoff The relationship between early degeneration of articular cartilage and the energyabsorbing
Subchondral Bone Changes in Patients with Early Degenerative Joint Disease Eric L. Radin, lgor L. Paul and Marc J. Tolkoff The relationship between early degeneration of articular cartilage and the energyabsorbing
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
Micro-CT imaging of surgical screw tightening in human trabecular bone
 Micro-CT imaging of surgical screw tightening in human trabecular bone E. Perilli 1, M. Ryan 1, R. Ab-Lazid 1, J.J. Costi 1, K.J. Reynolds 1 1 Medical Device Research Institute, School of Computer Science,
Micro-CT imaging of surgical screw tightening in human trabecular bone E. Perilli 1, M. Ryan 1, R. Ab-Lazid 1, J.J. Costi 1, K.J. Reynolds 1 1 Medical Device Research Institute, School of Computer Science,
Surgical Technique. Poly UHMWPE. Bio Hyaluronic Acid. Advancing Materials. Advancing Outcomes.
 Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
Surgical Technique Bio Hyaluronic Acid Poly UHMWPE Advancing Materials. Advancing Outcomes. Surgical Assessment 1. Proper implant diameter is determined by placing the appropriately sized trial over the
A cadaveric analysis of contact stress restoration after osteochondral transplantation of a cylindrical cartilage defect
 Knee Surg Sports Traumatol Arthrosc (2008) 16:461 468 DOI 10.1007/s00167-008-0494-1 KNEE A cadaveric analysis of contact stress restoration after osteochondral transplantation of a cylindrical cartilage
Knee Surg Sports Traumatol Arthrosc (2008) 16:461 468 DOI 10.1007/s00167-008-0494-1 KNEE A cadaveric analysis of contact stress restoration after osteochondral transplantation of a cylindrical cartilage
Comparative study of the contact pressures in hip joint models with femoroacetabular impingment with different cephalic deformities
 Comparative study of the contact pressures in hip joint models with femoroacetabular impingment with different cephalic deformities Iryna Havenko Instituto Superior Técnico, Universidade de Lisboa, Portugal
Comparative study of the contact pressures in hip joint models with femoroacetabular impingment with different cephalic deformities Iryna Havenko Instituto Superior Técnico, Universidade de Lisboa, Portugal
COR. Precision Targeting Cartilage Repair System. Arthroscopic Technique for Repair of Osteochondral Defects
 COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
COR Precision Targeting Cartilage Repair System Arthroscopic Technique for Repair of Osteochondral Defects Planning the Procedure An 18-gauge spinal needle is initially used to plan a perpendicular approach
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Clinical Policy Title: Autologous chondrocyte implantation
 Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Clinical Policy Title: Autologous chondrocyte implantation Clinical Policy Number: 14.03.07 Effective Date: March 1, 2017 Initial Review Date: February 15, 2017 Most Recent Review Date: February 6, 2018
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Osteochondral Transplant System
 Osteochondral Transplant System Rodrigo Umanzor (Team Leader) Nick Zacharias (BWIG & BSAC) Bilin Loi (BPAG) Eduardo Enriquez (Communicator) Client: Dr. Brian Walczak, DO Advisor: Dr. Kris Saha, PhD February
Osteochondral Transplant System Rodrigo Umanzor (Team Leader) Nick Zacharias (BWIG & BSAC) Bilin Loi (BPAG) Eduardo Enriquez (Communicator) Client: Dr. Brian Walczak, DO Advisor: Dr. Kris Saha, PhD February
CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS
 CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of the Tibia
 Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Case Reports in Orthopedics Volume 2015, Article ID 795759, 5 pages http://dx.doi.org/10.1155/2015/795759 Case Report Arthroscopic Microfracture Technique for Cartilage Damage to the Lateral Condyle of
Osteochondritis Dissecans
 P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
P R O C E D U R E 1 4 Ammar Anbari, Adam B. Yanke, and Brian J. Cole ch014-x4397.indd 221 4/11/2008 10:50:21 AM 222 Treatment Options Conservative management Fixation in situ Elevate the OCD lesion, débride
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions
 Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
Autografts and Allografts in the Treatment of Focal Articular Cartilage Lesions Policy Number: 7.01.78 Last Review: 2/2018 Origination: 8/2002 Next Review: 2/2019 Policy Blue Cross and Blue Shield of Kansas
