Uveitis in the internist s office: Are a patient s eye symptoms serious?
|
|
|
- Ira Chapman
- 5 years ago
- Views:
Transcription
1 REVIEW CME CREDIT RULA A. HAJJ-ALI, MD Department of Rheumatic and Immunologic Disease, Center for Vasculitis Care and Research, The Cleveland Clinic Foundation CAREEN LOWDER, MD, PhD Cole Eye Institute, The Cleveland Clinic Foundation BRIAN F. MANDELL, MD, PhD Vice-Chairman of Medicine for Educational Affairs; Department of Rheumatic and Immunologic Diseases, Center for Vasculitis Care and Research, The Cleveland Clinic Foundation; Editor-in-Chief, Cleveland Clinic Journal of Medicine Uveitis in the internist s office: Are a patient s eye symptoms serious? ABSTRACT Uveitis is an inflammatory process that may affect one or several specific areas of the eye. But when a patient presents to an internist with eye symptoms, be it photophobia, floaters, or red eye, the diagnosis is not always clear. If the diagnosis of uveitis is made, internists must search for an underlying cause, such as infection or an autoimmune disease. KEY POINTS Many systemic and regional diseases can cause ocular inflammation. It is critical to rule out infectious disease as the cause of uveitis, because giving immunosuppressive therapy to someone with infective uveitis can be disastrous. Infectious causes of uveitis include toxoplasmosis, cytomegalovirus, herpes simplex virus, tuberculosis, and syphilis. Systemic inflammatory causes include sarcoidosis, juvenile idiopathic arthritis, inflammatory bowel disease, and HLA-B27-associated diseases, especially ankylosing spondylitis and reactive arthritis. If the cause of uveitis is not infectious, treatment includes corticosteroids, given either topically, by periocular injection, or systemically. Immunosuppressive therapy may be required to limit steroid use. This paper discusses therapies that are not approved by the US Food and Drug Administration for the use under discussion. P ATIENTS OFTEN PRESENT to the office with vague eye symptoms, such as photophobia, red eye, or floaters. In most cases the symptoms are minor and do not reflect a serious problem. But in some cases, those symptoms indicate the more serious, visionthreatening condition of uveitis (intraocular inflammation). Diagnosis of uveitis is challenging, and its diagnosis and treatment are best handled collaboratively with an ophthalmologist. Once uveitis is diagnosed, physicians must determine whether it is caused by infection or is a sign of an underlying condition. This article covers the causes of uveitis, how to approach its diagnosis, and recommendations for managing it. UVEITIS IS INFLAMMATION AT ANY SITE The uvea constitutes the middle portion of the eye between the retina and sclera. However, uveitis now commonly refers to intraocular inflammation at any site. The anterior uveal tract consists of the iris. The ciliary body is the intermediate area connecting the iris to the posterior uveal portions of the choroid (FIGURE 1). Anterior uveitis refers to inflammation of the iris (iritis) or both iris and ciliary body (iridocyclitis). Inflammation of the ciliary body is termed cyclitis, pars planitis, or intermediate uveitis. Posterior uveitis includes vitritis, choroiditis, retinitis, chorioretinitis, or retinochoroiditis. Panuveitis or diffuse uveitis is the term used when there is both anterior and posterior uveitis. CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
2 UVEITIS HAJJ-ALI AND COLLEAGUES Terms used in the text Cells and flare findings on slit lamp examination: cells imply the presence of leukocytes within the anterior, posterior, or vitreous chambers; flare represents increased protein in the intraocular fluids Uveitis inflammation of the uveal tract (iris, ciliary body, choroid) Synechiae inflammatory adhesions between the iris and cornea (anterior synechiae) or the iris and lens (posterior synechiae) Cornea Anterior chamber Lens Iris Posterior chamber Uveal tract Ciliary body Vitreous chamber Choroid Retina Vitritis Inflammation within the vitreous cavity Retinitis/retinochoroiditis inflammation of the retina (retinitis) with or without contiguous choroidal inflammation (retinochoroiditis) Iritis/cyclitis/iridocyclitis inflammation of the iris (iritis), ciliary body (cyclitis) or both (iridocyclitis) CCF 2005 Choroiditis/chorioretinitis inflammation involving the choroid primarily (choroiditis), with or without contiguous involvement of the retina (chorioretinitis) FIGURE 1. Schematic figure of the different structures of the eye. CLASSIFICATION OF UVEITIS Uveitis is classified according to its: Anatomic location (anterior, intermediate, or posterior) Laterality (unilateral or bilateral) Onset (acute or insidious) Duration (self-limited, chronic, or recurrent) Size and distribution of keratic precipitates ( granulomatous or nongranulomatous ) seen by slit lamp examination. Biopsy of these inflammatory precipitates is rarely performed, but older pathological studies permit the current labeling of the deposits as granulomatous or nongranulomatous on the basis of their magnified (not biopsied) appearance. This classification helps the ophthalmologist develop a differential diagnosis. 4,5 Although many cases are idiopathic, an attempt to categorize by etiology should be made (see below), 4 ie: An infectious disease A localized specific ocular disease A specific systemic inflammatory disease A masquerade syndrome (eg, intraocular tumors). DIFFERENT PATTERNS IN DIFFERENT POPULATIONS Different patterns of uveitis are associated with different ages, genders, and races, mainly because of disease associations. For example, chronic anterior uveitis is associated with pauciarticular juvenile rheumatoid arthritis, and it is more common in young girls. Acute anterior uveitis, associated with ankylosing spondylitis, is more common in men and boys and is an important cause of uveitis in the United States and the United Kingdom. 330 CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL 2005
3 TABLE 1 Features of anterior uveitis that differentiate it from other common causes of red eye No discharge No itching Redness affecting primarily the limbus (FIGURE 2) Poorly reactive pupil Irregularity of the pupil Pain and photophobia Family history of uveitis In Caucasians, in whom the prevalence of uveitis is approximately 17 cases per 100,000 and the peak ages are between 20 and 50 years, 1 anterior uveitis is the most common pattern. 2 In contrast, in Japanese people, posterior uveitis accounts for most cases and is a manifestation of Behçet syndrome or Vogt- Koyanagi-Harada syndrome. 3 5 Ocular sarcoidosis is more common in African Americans, while Behçet disease is much more common in Asians and in people of Middle Eastern descent. 2 IS THIS UVEITIS? The first question the internist must answer is whether a patient with eye symptoms has uveitis and should be referred to an ophthalmologist. Many patients with anterior uveitis have a red eye, but other causes of a red eye that should be distinguished from uveitis include corneal inflammation (keratitis), conjunctival inflammation (conjunctivitis), blood vessel inflammation in the episclera or sclera (episcleritis and scleritis, respectively), or acute closed-angle glaucoma. TABLE 1 summarizes the signs and symptoms that help in recognizing anterior uveitis. Patients with posterior uveitis are more likely to be pain-free but with visual changes such as floaters. The new onset of significant floaters, especially with any haziness of vision, warrants referral to an ophthalmologist. The diagnosis of uveitis is confirmed by slit lamp examination, which can demonstrate inflammatory cells and the flare that results from protein extravasations from inflamed blood vessels into the anterior or posterior chambers. SYMPTOMS DEPEND ON SITE The symptoms of uveitis depend on the site of involvement. Acute anterior uveitis frequently causes pain and photophobia associated with ciliary injection. This is the typical pattern in patients with HLA-B27-associated iridocyclitis. Initially, vision may or may not be affected. Insidious anterior uveitis. If the onset is insidious (eg, in pauciarticular juvenile idiopathic arthritis), patients may experience no symptoms, despite inflammation and intraocular damage, until scarring, loss of vision, and cataracts occur. Posterior uveitis causes floaters and hazy vision. Redness and pain are not usual features of isolated posterior uveitis, although a dull ache may be present. Involvement of the retina may produce blind spots or flashing lights (a major warning sign). CAUSES OF UVEITIS: INFECTIOUS DISEASES FIGURE 2. Congestion of the limbus (the junction between the cornea and the sclera) in anterior uveitis. Although infection is an uncommon cause of uveitis, it is critical to rule out infection because giving immunosuppressive therapy to someone with infective uveitis can be disastrous. Infectious uveitis can occur in immunocompromised or healthy people. It is usually recognized by specific findings on ophthalmologic examination in an immunocompromised patient or after uveitis does not respond to anti-inflammatory therapy. Uveitis may precede the full-blown expression of systemic disease CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
4 UVEITIS HAJJ-ALI AND COLLEAGUES FIGURE 4. Cytomegalovirus retinitis. Note the characterisitic retinitis that progresses along the nerve fiber layer (arrows). Inappropriate use of immunosuppressive therapy in infectious uveitis can be disastrous FIGURE 3. Toxoplasmosis. Note the focal area of retiniitis (white arrows) adjacent to scar area (black arrrow). Parasitic infection: toxoplasmosis Toxoplasmosis is a common cause of retinochoroiditis (posterior uveitis) in normal and immunosuppressed patients, 6 accounting for as many as 25% of cases of posterior uveitis in the United States. Retinitis is usually prominent. 7 Most cases of acute toxoplasmic retinochoroiditis in adults are believed to be reactivations of congenital infection. Toxoplasmosis is diagnosed by observing a focal active area of retinitis adjacent to a chorioretinal scar (FIGURE 3), with supportive serologic testing. The finding of antitoxoplasmic antibodies helps in the diagnosis but is not sufficient to confirm active disease, since seropositivity is very common in the general population. 8 Viral infections Cytomegalovirus infection can cause posterior uveitis (retinitis) in immunocompromised people. Patients with acquired immunodeficiency syndrome are the most susceptible, especially those with CD4 cell counts lower than 50 cells/ml. 9 The incidence has decreased in the United States since highly active antiretroviral therapy has become available. 10 The infection is bilateral in 50% of cases. The diagnosis is made by recognizing the characteristic retinitis that progresses along the nerve fiber layers (FIGURE 4) in the setting of systemic cytomegalovirus infection, or by polymerase chain reaction studies of vitreous fluid. Other herpesviruses that can cause retinitis include herpes simplex and herpes zoster. Herpes simplex retinitis usually occurs in immunosuppressed patients or in patients who are congenitally infected. A unique form of rapidly progressive necrotizing retinitis can occur in normal hosts as a result of various herpes infections and is known as the acute retinal necrosis syndrome. 11,12 This is associated with visual loss and can be identified by an ophthalmologist. It warrants immediate highdose antiviral therapy. Bacterial and treponemal diseases Tuberculosis was once the most frequent cause of choroiditis. Now it is found in fewer than 1% of all cases of uveitis in the United States. 13,14 It should be considered as the cause of uveitis in a patient with active systemic tuberculosis. Syphilis can cause anterior or posterior uveitis, usually during the secondary or tertiary stages of infection. 15 Anterior syphilitic uveitis typically presents as acute unilateral iritis or iridocyclitis with involvement of the contralateral eye in half of cases (a pattern not generally found in HLA-B27-associated uveitis see below). Posterior syphilitic uveitis can present as diffuse or localized choroiditis or chorioretinitis, most often in patients with human immunodeficiency virus infection. Half of all cases 332 CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL 2005
5 of syphilitic posterior uveitis are also bilateral. Uveitis due to secondary syphilis often cannot be distinguished from other causes of uveitis on the basis of the ocular manifestations. Other, rare causes of bacterial and spirochetal uveitis include leprosy, leptospirosis, cat scratch disease, Lyme disease, and Whipple disease. CAUSES OF UVEITIS: LOCALIZED OCULAR DISEASES Some inflammatory diseases that are confined to the eye, without systemic associations, manifest as uveitis. Patients may present to their internist, but the specific diagnosis is generally recognized by an ophthalmologist on the basis of special features on examination or by history. Sympathetic ophthalmia is inflammation of the sympathizing eye that results from penetrating trauma or surgery in the contralateral ( exciting ) eye. It is thought to be due to an immune response against an ocular antigen that is exposed after the trauma. 16 Early enucleation of the exciting eye improves the visual outcome in the sympathizing eye; use of systemic corticosteroids and other immunosuppressant agents has also improved the prognosis. Birdshot choroidopathy is a bilateral posterior uveitis characterized by yellowish spots disseminated throughout the fundus at the level of the retinal pigment epithelium or choroid. Also noted are disc edema and numerous inflammatory cells in the vitreous and choroid in a birdshot appearance. Most patients are women in middle age (mean age 50). The disease is strongly associated with HLA-A29 antigen: about 80% to 90% of patients are positive for HLA-A29, compared with 7% of the general population. 19,20 Pars planitis is an idiopathic inflammation of the pars plana of the ciliary body, the portion of the eye between the iris and the choroid. It is known as intermediate uveitis when it is associated with a systemic disease such as multiple sclerosis or sarcoidosis. 17,18 Vision is usually affected, but about half of patients have a mild inflammation and a favorable prognosis. 21 Periodic remissions and exacerbations are typical. CAUSES OF UVEITIS: SYSTEMIC INFLAMMATORY DISEASES HLA-B27-associated diseases Anterior uveitis is associated with the histocompatibility antigen HLA-B27. In the United States and England, where HLA-B27 is relatively common (prevalence 4% 10%), from 30% to 70% of patients with acute anterior uveitis have this antigen. 22,23 Only half of patients with HLA-B27 and anterior uveitis have an associated systemic disease such as ankylosing spondylitis, psoriatic arthritis, reactive arthritis, or inflammatory bowel disease. Of patients with ankylosing spondylitis, 90% have HLA-B27; in reactive arthritis the prevalence is 60%. A patient with ankylosing spondylitis or Reiter syndrome has a 20% to 30% chance of developing iritis during the course of the disease. 24 HLA-B27-associated uveitis is characterized by the acute onset of unilateral iridocyclitis with redness and photophobia. With treatment, the prognosis is good, and the inflammation usually resolves within 2 to 4 months, which permits therapy to be discontinued. Recurrences are frequent, however, and may occur unilaterally in the contralateral eye (a flip-flop pattern). Some patients develop synechiae (scarring). Iritis as a complication of either psoriatic or inflammatory bowel disease is less common, less well characterized, and less frequently associated with HLA-B27. Around 7% of patients with psoriatic arthritis develop uveitis, as do fewer than 5% with inflammatory bowel disease. 25 Iritis associated with ulcerative colitis is frequently unilateral and sudden in onset, but the uveitis associated with Crohn disease is much more variable and is frequently bilateral, posterior, insidious in onset, and chronic in duration. 26 Sarcoidosis To the internist, sarcoidosis is a chronic multisystem disease characterized by lung infiltrates, hilar adenopathy, and lesions of the eye and skin. Eye disease may be the initial or only Trauma to one eye can cause uveitis in the other CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
6 UVEITIS HAJJ-ALI AND COLLEAGUES Uveitis is common in juvenile idiopathic arthritis manifestation, and it can affect all ocular structures. Sarcoidosis accounts for fewer than 6% of cases of anterior uveitis. 27,28 Sarcoidosis-related uveitis is bilateral in 80% of cases; approximately 85% of cases are anterior and 25% are posterior (10% are both). 29,30 Anterior sarcoidosis-related uveitis is an iridocyclitis characterized on slit-lamp examination by large mutton-fat keratic precipitates. The iridocyclitis can be chronic, bilateral, and recurrent and may lead to posterior synechiae formation. Posterior uveitis can be accompanied by involvement of the retinal vessels, the central nervous system, or both. 30 Occasionally, sarcoid uveitis presents acutely with parotitis, fever, and facial nerve palsy (uveoparotid fever). Asymptomatic lacrimal gland enlargement is common and may provide a clue to the underlying disease. The diagnosis of ocular sarcoidosis is strongly supported by the finding of sterile noncaseating granulomas on biopsy of an affected organ, most commonly the lungs or lymph nodes. Conjunctival biopsy in patients suspected of having ocular sarcoidosis may occasionally be worthwhile; the yield is increased by biopsy of clinically abnormal tissue. Computed tomography of the lungs is superior to chest radiography in demonstrating adenopathy. The angiotensin-convertingenzyme level is a nonspecific test and should not be used diagnostically. Ophthalmologists often make the diagnosis of ocular sarcoidosis on the basis of the clinical appearance and pattern of the inflammatory disease, after excluding alternative diagnoses, in the absence of systemic findings. How often this pattern evolves into systemic sarcoidosis is unknown. Juvenile idiopathic arthritis Juvenile idiopathic arthritis is a group of inflammatory arthritides affecting children younger than 16 years. It can present in four different modes: A systemic onset characterized by fever, polyarthritis, rash, adenopathy, and leukocytosis A polyarticular onset in which more than four joints are involved A pauciarticular onset with involvement of four joints or fewer Spondylitis, often with an initial peripheral arthritis. Uveitis is common in juvenile idiopathic arthritis: the prevalence can reach 20% in children with pauciarticular onset and 5% with polyarticular onset. It is extremely rare in the form with systemic onset. Most often, it occurs in young girls who have early-onset pauciarticular disease, frequently with a positive antinuclear antibody test. However, a recent study suggests that despite the classic teaching, antinuclear antibody positivity may not predict uveitis risk in patients with pauciarticular juvenile idiopathic arthritis. 31 Uveitis is usually asymptomatic and often presents within 5 years of the onset of juvenile idiopathic arthritis. An insidious, bilateral iridocyclitis, it is often completely asymptomatic until complications and loss of vision develop. 32 Reports from the 1970s described visual loss in 66% of patients and blindness in up to 38%. 33,34 Early detection by regular eye screening every 3 to 4 months has dramatically decreased the rate of visual impairment to 16%. 32,35 Children with spondylitis may develop acutely painful recurrent anterior uveitis, similar to adults with HLA-B27-associated uveitis. Behçet disease Behçet disease, most commonly seen in the Mediterranean and eastern rim of Asia, is characterized by recurrent orogenital ulcers, uveitis, thrombosis, vasculitis, and cutaneous manifestations. Uveitis, a dominant feature of the disease, occurs in 80% of patients. 36 Uveitis in Behçet disease typically is chronic and bilateral, and can be anterior or posterior or both. The inflammatory response in the anterior chamber may be so brisk as to elicit a visible meniscus of inflammatory cells, termed hypopyon (FIGURE 5). Blindness can result from a relentlessly progressive occlusive retinal vasculitis that often does not respond to aggressive immunosuppressive therapy CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL 2005
7 Vogt-Koyanagi-Harada syndrome Vogt-Koyanagi-Harada syndrome is a presumed autoimmune disease that can cause bilateral panuveitis and acute serous retinal detachment. It is one of the leading causes of uveitis in Japan. 38 Other manifestations include alopecia, peliosis (whitening of patches of hair), sterile meningitis, and eighth cranial nerve disease. Other systemic causes Other causes of uveitis include tubulointerstitial nephritis, 39 Kawasaki disease, 40 multiple sclerosis, 18,41 relapsing polychondritis, 42 Sjögren syndrome, 43 Wegener granulomatosis, 44 drug or hypersensitivity reactions, 45 and Lyme disease. 46 Uveitis is rarely associated with rheumatoid arthritis or systemic lupus erythematosus. MASQUERADE SYNDROMES A number of noninfectious processes can be mistaken for an inflammatory process and can mimic uveitis. These masquerade syndromes include non-hodgkin lymphoma, leukemia, retinitis pigmentosa, and retinoblastoma. These are often suspected when there is poor response to anti-inflammatory agents that are given to treat assumed uveitis. Lymphomas must be considered when uveitis presents at an older age. They are typically of B-cell origin and confined to the eye and the central nervous system. 47 Other masquerade syndromes include uveal melanoma and metastatic lesions of breast, lung, or renal origin. COMPLICATIONS OF UVEITIS FIGURE 5. Hypopyon in Behçet disease (can also be seen in anterior uveitis of other causes). The major sight-threatening complications of uveitis are cataracts; glaucoma; cystoid macular edema; retinal detachment; subretinal, retinal, and optic nerve neovascularization; and band keratopathy. Cataracts occur in patients with uveitis as a direct result of inflammation as well as treatment of the inflammation with corticosteroids. Uveitis may lead to anterior and posterior synechiae which can impede aqueous outflow and cause glaucoma. Permanent loss of vision can occur with long-standing macular edema, observed most commonly in patients with sarcoidosis, intermediate uveitis, birdshot chorioretinopathy, and retinal vasculitis. Glaucoma may occur if the inflammatory cells and debris clog the trabecular meshwork or from posterior synechiae. Retinal detachment occurs in patients with posterior, intermediate, or diffuse uveitis. It is believed that aggressive reduction of all inflammation will prevent most delayed sequelae of uveitis. APPROACH TO PATIENTS WITH UVEITIS When uveitis is diagnosed, potential causes should be considered. A specific diagnosis for uveitis can be found in approximately 70% of cases, and a systemic disease is associated with uveitis in up to half Infection should be considered when uveitis develops in an immunocompromised patient, or when uveitis fails to respond to anti-inflammatory therapy. The active participation of the internist in the evaluation and management of immunosuppression in patients with uveitis is extremely helpful. If this is uveitis, is it associated with systemic disease? The most helpful tools in the initial search for associated systemic diseases are the patient s history and the general physical examination, coupled with the information given by the ophthalmologist about the ocular pattern of the inflammation. TABLE 2 summarizes systemic conditions and their common associated ocu- Cataracts can be due to inflammation or antiinflammatory treatment CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
8 UVEITIS HAJJ-ALI AND COLLEAGUES TABLE 2 Systemic conditions and their associated ocular pattern of inflammation SYSTEMIC DISEASE PATTERN OF UVEITIS Ankylosing spondylitis Acute unilateral anterior uveitis; may flip-flop between eyes Reactive arthritis Acute unilateral anterior uveitis Inflammatory bowel disease Acute unilateral anterior uveitis * Juvenile idiopathic pauciarticular arthritis Sarcoidosis Behçet syndrome Vogt-Koyanagi-Harada syndrome Chronic insidious bilateral uveitis Chronic insidious bilateral anterior or posterior uveitis, retinal involvement Chronic insidious bilateral anterior or posterior uveitis Chronic insidious bilateral anterior or posterior uveitis, retinal detachment *Uveitis associated with Crohn disease may be bilateral, posterior, insidious in onset, and chronic in duration The new onset of floaters and hazy vision warrants referral to an ophthalmologist lar pattern of inflammation. Once the inflammation is localized to either anterior or posterior segment, and the onset (acute or insidious) and the symmetry (unilateral or bilateral) have been established, clues from the history and physical examination can direct the diagnosis and workup (TABLE 3). Are there specific considerations in the uveitis workup? The diagnostic evaluation of patients with uveitis should be tailored to fit the history and physical findings. Chest radiography, computed tomography, or both are mandatory when pulmonary symptoms are elicited. However, imaging can still be considered if there are no pulmonary symptoms and if a cause of uveitis is not obvious, since thoracic sarcoidosis is frequently asymptomatic. This approach has not been demonstrated to influence outcomes in patients with otherwise asymptomatic sarcoidosis, however. Symptoms of spondyloarthropathy may be atypical in female patients, and radiographic evaluation of the sacroiliac joints can be helpful if this diagnosis is considered. 51 A normal sacroiliac radiograph does not exclude spondyloarthropathy, since radiographs may be normal early in the disease. 52 However, the ultimate clinical value of routine spine or sacroiliac radiographs in the absence of axial symptoms is not established. 53 HLA typing can occasionally help determine the prognosis of anterior uveitis. HLA-B27 is associated with both spondyloarthropathy and isolated anterior uveitis. Seventy-one percent of patients with acute-onset unilateral nongranulomatous (the ophthalmologic term based on the slitlamp appearance of the eye) anterior uveitis are HLA-B27-positive. 54 HLA typing is not indicated if a patient presents with acute unilateral uveitis and the diagnosis of spondyloarthropathy is already established, however. HLA-B27 testing is also not helpful when the uveitis is posterior or bilateral, since in this setting the relation to HLA-B27 is not clear. Testing may be most useful when a patient presents with acute unilateral anterior uveitis without a clear explanation by history and physical examination. In such cases, detecting HLA-B27 would direct the diagnosis away from sarcoidosis or syphilis and would suggest that the disease is likely to respond to intermittent local therapy with steroid drops, although it will likely recur. 24 Typing for HLA-A29 strongly supports the 336 CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL 2005
9 TABLE 3 Important clues to systemic inflammatory diseases POSSIBLE DIAGNOSE CLUES WORKUP Spondyloarthropathy Asymmetric peripheral arthritis Sacroiliac radiography Dactylitis, enthesitis HLA-B27 testing if diagnosis Morning back stiffness is unclear Sarcoidosis Cough, dyspnea Chest radiography Lacrimal gland enlargement Computed tomography Parotid gland enlargement Behçet disease Oral or genital ulcers Rule out infectious cause (eg, herpes viruses) Inflammatory bowel disease Gastrointestinal symptoms Colonoscopy Heme-positive stools HIV infection Opportunistic infections HIV testing Malignancy Abnormal white blood cell count CD40 count Cancer therapy Thrombocytopenia diagnosis of birdshot retinopathy, a serious chronic chorioretinitis that is usually suggested by the clinical appearance of the retina. 19,20 Antinuclear antibody testing is not recommended in cases of unexplained uveitis, because the test has poor diagnostic value for lupus (or any other specific diagnosis) in the absence of specific diagnostic concern suggested by the history, laboratory evaluation, or physical examination. A positive antinuclear antibody test in the setting of isolated uveitis does not warrant the diagnosis of systemic lupus erythematosus. Some pediatric rheumatologists use the antinuclear antibody test in young patients with pauciarticular juvenile inflammatory arthritis to help predict prognosis, but as noted, this practice has recently been questioned. 31 Serologic tests for syphilis should be considered in patients with unexplained uveitis. Venereal Disease Research Laboratory (VDRL) testing may be negative but the fluorescent treponemal antibody absorption test is usually positive in syphilis-related eye disease. 4 This is especially important in patients infected with human immunodefieciency virus. TREATMENT IS MULTIDISCIPLINARY Uveitis is best managed in collaboration with an ophthalmologist. Inflammatory eye disease is a distinct subspecialty of ophthalmology, and a uveitis specialist may need to be consulted in complex cases. Often, an internist or rheumatologist manages dosing and monitors the toxicity of immunotherapy, while an ophthalmologist assesses disease activity and ocular damage, dictating the need for increased or decreased intensity of therapy. Treatment of infectious diseases Viral infections, particularly cytomegalovirus infection and herpetic acute retinal necrosis, should be treated very aggressively with antiviral agents to prevent retinal damage. Syphilitic uveitis should be treated as neurosyphilis. Toxoplasma infection is usually treated with the combination of sulfadiazine, pyrimethamine, and folinic acid. Corticosteroid therapy Corticosteroids are the mainstay of therapy for noninfectious causes of uveitis; the route depends on the location of inflammation, the severity, the degree of visual disability, and the presence or absence of systemic disease. Topical corticosteroids are used in anterior uveitis but are not recommended in posterior uveitis because of poor penetration and thus limited efficacy. The frequency of doses A positive antinuclear antibody test does not establish lupus or anything else CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
10 UVEITIS HAJJ-ALI AND COLLEAGUES depends on disease severity; hourly application may be needed at first. Topical steroids may worsen viral or other infections and delay the appropriate therapy. Thus, it is imperative to communicate with an ophthalmologist before starting topical corticosteroid therapy. Periocular corticosteroid injections are used for posterior disease. They have the advantage of achieving high intraocular levels of steroids while avoiding the systemic side effects of oral corticosteroids. Globe perforation, ptosis, and glaucoma are potential risks. Systemic corticosteroid therapy, may be effective in controlling anterior uveitis, but is generally reserved for patients with bilateral disease that is refractory to local medication or for those with major ocular disability or retinitis. Systemic or topical corticosteroids usually elicit a therapeutic response, but some inflammatory conditions do not fully respond or require unacceptably high doses and long-term use. Although untreated uveitis can cause cataracts and glaucoma, these are also recognized complications of steroid therapy. Other immunosuppressive medications used in steroid-dependent or refractory uveitis include methotrexate, sulfasalazine, azathioprine, cyclosporine, mycophenolate, chlorambucil, and tacrolimus Few randomized trials of these agents have been performed. Recent reports showed promising results with anti-tumor necrosis factor agents in some forms of inflammatory uveitis Immunosuppressive medications should be managed by physicians experienced in their use, given the wide range of potential toxicity, and in collaboration with an ophthalmologist skilled in the management of uveitis. Adjunctive therapies, including mydriatic/cycloplegic agents, are used mainly to prevent adhesion of the pupillary margins to the anterior lens capsule and to relieve painful ciliary spasm. REFERENCES 1. Rosenbaum JT. An algorithm for the systemic evaluation of patients with uveitis: guidelines for the consultant. Semin Arthritis Rheum 1990; 19: Banares A, Jover JA, Fernandez-Gutierrez B, et al. Patterns of uveitis as a guide in making rheumatologic and immunologic diagnoses. Arthritis Rheum 1997; 40: Darrell RW, Wagener HP, Kurland LT. Epidemiology of uveitis. Arch Ophthalmol 1962; 68: Baarsma GS. The epidemiology and genetics of endogenous uveitis: a review. Curr Eye Res 1992; 11S: Mishima S, Masuda K, Izawa Y, Mochizuki M, Namba K. Behçet s disease in Japan: ophthalmological aspects. Trans Am Ophthalmol Soc 1979; 76: Ongkosuwito JV, Bosch-Driessen EH, Kijlstra A, Rothova A. Serologic evaluation of patients with primary and recurrent ocular toxoplasmosis for evidence of recent infection. Am J Ophthalmol 1999; 128: Henderley DE, Genstler AJ, Smith RE, Rao NA. Changing patterns of uveitis. Am J Ophthalmol 1987; 103: Weiss MJ, Velazquez N, Hofeldt AJ. Serologic tests in the diagnosis of presumed toxoplasmic retinochoroiditis. Am J Ophthalmol 1990; 109: Jabs DA, Enger C, Barlett JG. Cytomegalovirus retinitis and acquired immunodeficiency syndrome. Arch Ophthalmol 1989; 107: Jabs DA, Bartlett JG. AIDS and ophthalmology: A period of transition. Am J Ophthalmol 1997; 124: Ganatra JB, Chandler D, Santos C, Kuppermann B, Margolis TP. Viral causes of the acute retinal necrosis syndrome. Am J Ophthalmol 2000; 129: Culbertson W, Blumencranz M, Pepose J, Stewart JA, Curtin VT. Varicella zoster virus is a cause of the acute retinal necrosis syndrome. Ophthalmology 1986; 93: Dutt A, Moers D, Stead WW. Short-course chemotherapy for extrapulmonary tuberculosis: nine years experience. Ann Intern Med 1986; 104: Donahue H. Ophthalmic experience in a tuberculosis sanatorium. Am J Ophthalmol 1967; 64: Whitcup S, Raizman M. Spirochetal infections and the eye. In: Alberts D, Jakobiec F, editors. Principles and Practice of Ophthalmology. Philadelphia: W.B. Saunders, 1994: Chu DS, Foster CS. Sympathetic ophthalmia. Int Ophthalmol Clin 2002; 42: Malinowski SM, Pulido JS, Folk JC. Long-term visual outcome and complications associated with pars planitis. Ophthalmology 1993; 100: Zein G, Berta A, Foster CS. Multiple sclerosis-associated uveitis. Ocul Immunol Inflamm 2004; 12: Priem HA, Oosterhuis JA. Birdshot chorioretinopathy: clinical characteristics and evolution. Br J Ophthalmol 1988; 72: LeHoang P, Ozdemir N, Benhamou A, et al. HLA-A29.2 subtype associated with birdshot retinochoroidopathy. Am J Ophthalmol 1992; 113: Newell FW. Intraocular inflammations. Ophthalmology Principles and Concepts. St. Louis: Mosby-Year Book, 1996: Huhtinen M, Karma A. HLA-B27 typing in the categorization of uveitis in a HLA-B27 rich population. Br J Ophthalmol 2000; 84: Linder R, Hoffmann A, Brunner R. Prevalence of spondyloarthritides in patients with uveitis. J Rheumatol 2004; 31: Rosenbaum JT. Acute anterior uveitis and spondyloarthropathies. Rheum Dis Clin North Am 1992; 18: Catsarou-Catsari A, Katsambas A, Theodoropoulos P, Stratigos J. Ophthalmological manifestations in patients with psoriasis. Acta Derm Venereol 1984; 64: Mintz R, Feller ER, Bahr RL, Shah SA. Ocular manifestations of inflammatory bowel disease. Inflamm Bowel Dis 2004; 10: McCannel CA, Holland GN, Helm CJ, Cornell PJ, Winston JV, Rimmer TG. Causes of uveitis in the general practice of ophthalmology. UCLA 338 CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL 2005
11 Community-Based Uveitis Study Group. Am J Ophthalmol 1996; 121: Rodriguez A, Calonge M, Pedroza-Seres M, et al. Referral patterns of uveitis in a tertiary eye center. Arch Ophthalmol 1996; 114: Karma A, Huhti E, Poukkula A. Course and outcome of ocular sarcoidosis. Am J Ophthalmol 1988; 106: Jones NP. Sarcoidosis and uveitis. Ophthalmol Clin North Am 2002; 15: Guillaume S, Prieur AM, Coste J, Job-Deslandre C. Long-term outcome and prognosis in oligoarticular-onset juvenile idiopathic arthritis. Arthritis Rheum 2000; 43: Cabral DA, Petty RE, Malleson PN, Ensworth S, McCormick AQ, Shroeder ML. Visual prognosis in children with chronic anterior uveitis and arthritis. J Rheumatol 1994; 21: Key SN 3rd, Kimura SJ. Iridocyclitis associated with juvenile rheumatoid arthritis. Am J Ophthalmol 1975; 80: Cassidy JT, Sullivan DB, Petty RE. Clinical patterns of chronic iridocyclitis in children with juvenile rheumatoid arthritis. Arthritis Rheum 1977; 20: Sherry DD, Mellins ED, Wedgwood RJ. Decreasing severity of chronic uveitis in children with pauciarticular arthritis. Am J Dis Child 1991; 145: International Study Group for Behçet s Disease. Criteria for diagnosis of Behçet s disease. Lancet 1995; 335: Nussenblatt RB. Uveitis in Behçet s disease. Int Rev Immunol 1997; 14: Rubsamen PE, Gass JDM. Vogt-Koyanagi-Harada syndrome. Clinical course, therapy and long-term visual outcome. Arch Ophthalmol 1991; 109: Mandeville JT, Levinson RD, Holland GN. The tubulointerstitial nephritis and uveitis syndrome. Surv Ophthalmol 2001; 46: Jacob JL, Polomeno RC, Chad Z, Lapointe N. Ocular manifestations of Kawasaki disease (mucocutaneous lymph node syndrome). Can J Ophthalmol 1982; 17: Malinowski SM, Pulido JS, Goeken NE, Brown CK, Folk JC. The association of HLA-B8, B51,DR2 and multiple sclerosis in pars planitis. Ophthalmology 1993; 100: Isaak BL, Liesegang TJ, Michet CJ Jr. Ocular and systemic findings in relapsing polychondritis. Ophthalmology 1986; 93: Rosenbaum JT, Bennett RM. Chronic anterior and posterior uveitis and primary Sjögren s syndrome. Am J Ophthalmol 1987; 104: Hoffman GS, Kerr GS, Leavitt RY, et al. Wegener granulomatosis: an analysis of 158 patients. Ann Intern Med 1992; 116: Shafran SD, Deschenes J, Miller M, Phillips P, Toma E. Uveitis and pseudojaundice during a regimen of clarithromycin, rifabutin and ethambutol. MAC Study Group of the Canadian HIV Trials Network. N Engl J Med 1994; 330: Copeland RA Jr. Lyme uveitis. Int Ophthalmol Clin 1990; 30: Wilson DJ, Braziel R, Rosenbaum JT. Intraocular lymphoma. Immunopathologic analysis of vitreous biopsies. Arch Ophthalmol 1992; 110: Rosenbaum JT. Uveitis. An internist s view. Arch Intern Med 1989; 149: Rothova A, Buitenhuis H, Meeken C, et al. Uveitis and systemic disease. Br J Ophthalmol 1992; 76: Rodriguez A, Calogne M, Pedroza-Seres M, et al. Referral patterns of uveitis in a tertiary eye care center. Arch Ophthalmol 1996; 114: Tay-Kearney ML, Schwam BL, Lowder C, et al. Clinical features and associated systemic diseases of HLA-B27 uveitis. Am J Ophthalmol 1996; 121: Khan MA, van der Linden SM, Kushner I, et al. Spondylitic disease without radiographic evidence of sacroilitis in relatives of HLA-B27 positive ankylosing spondylitis patients. Arthritis Rheum 1985; 28: Austin MW, Clearkin LG. Radiological investigation in the management of uveitis. Eye 1988; 2: Ehlers N, Kissemeyer Nielson F, Kjerbye KE, et al. HLA B27 in acute and chronic uveitis [letter]. Lancet 1974; 1: Munoz-Fernandez S, Hidalgo V, Fernandez-Melon J, et al. Sulfasalazine reduces the number of flares of acute anterior uveitis over a one-year period. J Rheumatol 2003; 30: Jabs DA, Rosenbaum JT, Foster CS, et al. Guidelines for the use of immunosuppressive drugs in patients with ocular inflammatory disorders: recommendations of an expert panel. Am J Ophthalmol 2000; 130: Samson CM, Waheed N, Baltatzis S, Foster CS. Methotrexate therapy for chronic noninfectious uveitis: analysis of a case series of 160 patients. Ophthalmology 2001; 108: Reiff A, Takei S, Sadeghi S, et al. Etanercept in children with treatment-resistant uveitis. Arthritis Rheum 2001; 46: Kruithof E, Kestelyn P, Elewaut C, et al. Successful use of infliximab in a patient with treatment resistant spondyloarthropathy related uveitis. Ann Rheum Dis 2002; 61:470. ADDRESS: Brian Mandell, MD, PhD, Vice-Chairman of Medicine for Educational Affairs, NA20, The Cleveland Clinic Foundation, 9500 Euclid Avenue, Cleveland, OH 44195; mandelb@ccf.org. We Welcome Your Letters WE ENCOURAGE YOU TO WRITE, either to respond to an article published in the Journal or to address a clinical issue of importance to you. You may submit letters by mail, fax, or . MAILING ADDRESS Letters to the Editor Cleveland Clinic Journal of Medicine 9500 Euclid Ave., NA32 Cleveland, OH FAX ccjm@ccf.org Please be sure to include your full address, phone number, fax number, and address. Please write concisely, as space is limited. Letters may be edited for style and length. We cannot return materials sent. Submission of a letter constitutes permission for the Cleveland Clinic Journal of Medicine to publish it in various editions and forms. CLEVELAND CLINIC JOURNAL OF MEDICINE VOLUME 72 NUMBER 4 APRIL
UVEITIS. Dr. Yılmaz ÖZYAZGAN
 UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
UVEITIS Dr. Yılmaz ÖZYAZGAN UVEITIS DEFINITION BY STRICT DEFINITION, UVEITIS IS AN INFLAMMATION OF UVEAL TRACT. BUT IN PRACTICAL, IT IS GENERALLY NOT RESTRICTED TO THE UVEA AND INVOLVES OTHER ADJACENT
Nausheen Khuddus, MD Melissa Elder, MD, PhD
 Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Nausheen Khuddus, MD Melissa Elder, MD, PhD Nausheen Khuddus, MD Pediatric Ophthalmologist and Strabismus Specialist Accent Physicians Gainesville, Florida What Is Uveitis? Uveitis is caused by inflammatory
Head prof. MUDr. E. Vlková, CSc.
 MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
MUDr. Karkanová Michala, Oční klinika LF MU a FN Brno Head prof. MUDr. E. Vlková, CSc. 3 parts: iris (iris) ciliary body (corpus ciliare) choroid (choroidea) Function: regulating the entry of light into
Approach to Pediatric Uveitis. Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service
 Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Approach to Pediatric Uveitis Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Service Epidemiology Uveitis is the 3 rd leading cause of blindness in USA 5-10% of uveitis cases involve children
Diagnosis of uveitis, how to proceed?
 EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
EOS meeting Cairo, 2018 Diagnosis of uveitis, how to proceed? Mohamed G.A Saleh Lecturer of Ophthalmology Assiut University Size of the problem 15/100000 in US every year. 10% of blindness Prevalence varies
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D.
 A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
A Tailored Approach to Uveitis and Associated Systemic Conditions Anthony DeWilde O.D. I. Introduction II. III. IV. A. Why I am giving this talk B. What to take from lecture Diagnosis 1. Better understanding
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
OCCASIONAL COMMUNICATIONS
 UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
UVEITIS: DIAGNOSIS AND MANAGEMENT T. Akerele and S. Lightman, Department of Clinical Ophthalmology, Institute of Ophthalmology, London and Moorfields Eye Hospital, London Uveitis is a generic term which
Management of uveitis
 Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Management of uveitis DR. ANUPAMA KARANTH Anti-inflammatory agents -itis = inflammation Treatment : stop inflammation Use anti-inflammatory drugs Most potent of such agents : Corticosteroids Corticosteroids
Anthony DeWilde, O.D Linwood Blvd. Kansas City, MO x
 Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Anthony DeWilde, O.D. 4801 Linwood Blvd. Kansas City, MO 64128 816-861-4700 x 57411 anthony.dewilde@va.gov Uveitis and Glaucoma: The Seven Reasons Why IOP Can Increase in Uveitis (and What to do About
Uveitis. What is Uveitis?
 Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Uveitis What is Uveitis? Uveitis [u-vee-i-tis] is a term for inflammation of the eye. It can occur in one eye or both eyes and affects the layer of the eye called the uvea [u-vee-uh]. It also can be associated
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 743-748 Methotrexate for uveitis associated with juvenile idiopathic arthritis: Value and requirement for additional anti-inflammatory medication
Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia
 JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
JKAU: Med. Sci., Vol. 19 No. 3, pp: 73-83 (2012 A.D. / 1433 A.H.) DOI: 10.4197/Med. 19-3.6 Pattern of Uveitis in Saudi Female Patients in Western Region of Saudi Arabia Nizamuddin Shaik Hakim Mohammad
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Uveitis of spondyloarthritis in Indian subcontinent: a cross sectional study
 International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
International Journal of Advances in Medicine Ninan F et al. Int J Adv Med. 2017 Oct;4(5):1441-1446 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20174300
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
A Clinical Study of Anterior Uveitis in a Rural Hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 3 Ver. III. (Mar. 2014), PP 55-59 A Clinical Study of Anterior Uveitis in a Rural Hospital
Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis
 Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Haddad and Reddy Journal of Ophthalmic Inflammation and Infection 2014, 4:28 BRIEF REPORT Open Access Double trouble: a patient with both HLA-B27 anterior uveitis and HLA-A29 birdshot chorioretinitis Zeina
Differential diagnosis of posterior uveitis
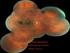 Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Differential diagnosis of posterior uveitis Diagnostic approach 45-year old male. Floaters and decreased vision since 1 week Fever, lymphadenopathy, myalgias, night sweats, two months ago Oral ulcer sporadically
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Update on management of Anterior Uveitis
 Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
Update on management of Anterior Uveitis Parthopratim Dutta Majumder Senior Consultant, Department of Uvea & Intraocular Inflammation Medical Research Foundation, Sankara Nethralaya ABCD of Treating a
o White dot syndromes pattern recognition o Activity and damage o Quality of life o Key points o Idiopathic o Sarcoidosis o Multiple sclerosis
 Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Introduction Clinical Assessment of Posterior Uveitis Philip I. Murray Centre for Translational Inflammation Research University of Birmingham Birmingham and Midland Eye Centre o Classification of uveitis
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE BERNARD H. BLAUSTEIN, O.D., F.A.A.O.
 DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
DIAGNOSIS AND MANAGEMENT OF ANTERIOR UVEITIS POA SPRING CONFERENCE - 2009 Classification of Anterior Uveitis BERNARD H. BLAUSTEIN, O.D., F.A.A.O. A. Anatomic location 1. Iritis Cells and flare mostly in
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Case History. The SEVEN HABITS of Highly Effective Anterior Uveitis Management. SLEx findings: SLEx corneal findings: y.o.
 The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
The SEVEN HABITS of Highly Effective Anterior Uveitis Management Case History! 68 y.o. Caucasian female of photophobia and blurred vision! As well as a headache over right eye for 2 days! Complains Paul
Patterns of uveitis in a Philippine eye clinic
 VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
VOL. NO. PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE - MARCH 5 Harvey S. Uy, MD Irene W. Tam, OD Asian Eye Institute Makati, Philippines Patterns of uveitis in a Philippine eye clinic
Patterns of Uveitis at a Tertiary Referral Center in Southern Iran
 Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
Original Article Patterns of Uveitis at a Tertiary Referral Center in Southern Iran Mansour Rahimi, MD; Ghazaleh Mirmansouri, MD Poustchi Eye Research Center and Ophthalmology Department, Shiraz University
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D.
 WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
WHAT IS YOUR DIAGNOSIS? By ADREA R. BENKOFF M.D. Anterior Chamber Inflammation and Iris Depigmentation Noted 25 Years After Cataract Extraction Decreasing Vision Over a 5- Year Period 64 year old white
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD.
 Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
Glaucoma & Inflammation. Jorge L. Fernandez Bahamonde, MD. Definition. Inflammatory ocular conditions compromise outflow of aqueous humor. Keratitis Episcleritis. Scleritis. Uveitis Glaucoma & Keratitis.
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
COVER FOCUS AT A GLANCE. BY LISA J. FAIA, MD, and KIMBERLY A. DRENSER, MD, PhD
 PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
PEDIATRIC UVEITIS: CHALLENGING FOR OPHTHALMOLOGISTS, PATIENTS, AND PARENTS Management of these complicated diseases differs between pediatric and adult patient populations. BY LISA J. FAIA, MD, and KIMBERLY
2/16/17. 3 main underlying causes are:
 Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
Definition Etiology Signs/Symptoms Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College
What you can expect with OZURDEX
 Important Information About Noninfectious Uveitis Affecting the Back Segment of the Eye and Treatment What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone intravitreal implant) is a prescription
Important Information About Noninfectious Uveitis Affecting the Back Segment of the Eye and Treatment What you can expect with OZURDEX Approved Use OZURDEX (dexamethasone intravitreal implant) is a prescription
Indian Journal of Basic & Applied Medical Research; June 2013: Issue-7, Vol.-2, P
 Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
Original article Clinial Study of different types of Uveitis in Western Maharashtra *Yellambkar ST, *Chavan WM,**Tayade MC *Dept. of Ophthalmology & **Department of Physiology, Rural Medical College, Pravara
10/18/2018. Unraveling Uveitis
 Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Unraveling Uveitis Trenton Cleghern, OD, FAAO VisionAmerica UAB School of Optometry 11/10/2018 1 Disclosure Statement: Nothing to disclose 2 Objectives Classify uveitis Current and new therapeutic options
Bilateral multiple choroidal granulomas and systemic vasculitis as presenting features of tuberculosis in an immunocompetent patient
 Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Kumar et al. Journal of Ophthalmic Inflammation and Infection (2016) 6:40 DOI 10.1186/s12348-016-0109-9 Journal of Ophthalmic Inflammation and Infection BRIEF REPORT Open Access Bilateral multiple choroidal
Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions. April 2018
 Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions This Clinical Practice Guide provides evidence-based information about current best practice in the management
Clinical Practice Guide for the Diagnosis, Treatment and Management of Anterior Eye Conditions This Clinical Practice Guide provides evidence-based information about current best practice in the management
Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior Uveitis in a Korean Population
 J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
J Korean Med Sci 2009; 24: 722-8 ISSN 1011-8934 DOI: 10.3346/jkms.2009.24.4.722 Copyright The Korean Academy of Medical Sciences Clinical Features and Prognosis of HLA-B27 Positive and Negative Anterior
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Ocular Pathology. I. Congenital and/or developmental. A. Trisomy 21. Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea)
 I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
Regional vs. Systemic Therapy. Corticosteroids. Regional vs. Systemic Therapy for Uveitis. Considerations
 Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
Regional vs. Systemic Therapy for Uveitis Nisha Acharya,, M.D., M.S. Director, Uveitis Service F.I. Proctor Foundation University of California, San Francisco December 4, 2010 No financial disclosures
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO
 Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Anterior Segment Disease and the Systemic Link Mile Brujic, OD, FAAO brujic@prodigy.net Summary As optometry s role in health care increases, so does our responsibility to appropriately diagnose and appropriately
Work Sheet And Course Hand Out
 Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
3 main underlying causes are:
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu
Intravitreal Triamcinolone Acetonide for Macular Edema in HLA-B27 Negative Ankylosing Spondylitis
 105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
105 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
!! Definition. !! Etiology. !! Signs/Symptoms. !! Classification/Diagnosis. !! Systemic Associations. !! Lab Testing. !! Treatment. !!
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
Nathan Lighthizer, O.D., F.A.A.O. Assistant Professor Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Northeastern State University Oklahoma College of Optometry Tahlequah, OK lighthiz@nsuok.edu!!
2/23/18. Disclosures. Rheumatic Diseases of Childhood. Making Room for Rheumatology. I have nothing to disclose. James J.
 Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl
 Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl Pavlina S. Kemp, MD, Susannah Q. Longmuir, MD August 14, 2012 Chief complaint: Central posterior synechiae
Juvenile Idiopathic Arthritis with Associated Bilateral Anterior Uveitis in a Four Year- Old Girl Pavlina S. Kemp, MD, Susannah Q. Longmuir, MD August 14, 2012 Chief complaint: Central posterior synechiae
Case History. Slit lamp exam: Clinical Pearls in the Management of Iritis. 2- injection: Irregular SPK and staining AC: grade 3 cell & flare
 Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
UVEITIS. Uveitis may have different causes. It can be caused by:
 http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
http://www.midwestretina.com Phone: (614)-339-8500 Toll Free: (866)-373-8462 Sugat S. Patel, M.D. Louis J. Chorich III, M.D. Dino D. Klisovic, M.D. Lisa M. Borkowski, M.D. Dominic M. Buzzacco, M.D. Johnstone
Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center
 Original Article Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center Sharad Gupta 1, Dev Narayan Shah 2, Sagun Narayan Joshi 3, Manoj Aryal 4, Lila
Original Article Patterns of Macular Edema in Uveitis as Diagnosed by Optical Coherence Tomography in Tertiary Eye Center Sharad Gupta 1, Dev Narayan Shah 2, Sagun Narayan Joshi 3, Manoj Aryal 4, Lila
Uveitis in patients with Multiple Sclerosis
 Uveitis in patients with Multiple Sclerosis An observational descriptive clinical study submitted in partial fulfillment of Master Degree in Ophthalmology By Dr. Ahmed Mohamed Karara M.B, B Ch. Supervised
Uveitis in patients with Multiple Sclerosis An observational descriptive clinical study submitted in partial fulfillment of Master Degree in Ophthalmology By Dr. Ahmed Mohamed Karara M.B, B Ch. Supervised
Clinical Course of Uveitis in Children in a Tertiary Ophthalmology Center in Northwest Iran
 http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 4, No. 4, October 2017, 200 204 eissn 2148-9696 Clinical Course of Uveitis in Children in a Tertiary
http://www.cjmb.org Open Access Original Article Crescent Journal of Medical and Biological Sciences Vol. 4, No. 4, October 2017, 200 204 eissn 2148-9696 Clinical Course of Uveitis in Children in a Tertiary
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Cases CFEH. CFEH Facebook Case #4
 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
Uveitis Update DISCLOSURE STATEMENT. Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO
 Uveitis Update Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO DISCLOSURE STATEMENT We have no direct financial or proprietary interest in any companies, products or services mentioned in this presentation.
Uveitis Update Featured Speaker: Dr. Kyle Cheatham, FAAO, DIP ABO DISCLOSURE STATEMENT We have no direct financial or proprietary interest in any companies, products or services mentioned in this presentation.
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Various presentations of herpes simplex retinochoroiditis A case series
 Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Review Article Gender and Spondyloarthropathy-Associated Uveitis
 Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
Ophthalmology Volume 2013, Article ID 928264, 6 pages http://dx.doi.org/10.1155/2013/928264 Review Article Gender and Spondyloarthropathy-Associated Uveitis Wendy M. Smith MayoClinic,200FirstStreetSW,Rochester,MN55905,USA
Condition: Herpes Simplex Keratitis
 Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
THE RED EYE Cynthia McNamara, MD Week 25
 THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
THE RED EYE Cynthia McNamara, MD Week 25 Educational Objectives: 1. Know the differential diagnosis and presentation of specific etiologies of the red eye 2. Be able to evaluate patients presenting with
Screening for Uveitis in Children
 Information for patients and parents Manchester Royal Eye Hospital Paediatric Uveitis Service Screening for Uveitis in Children What is uveitis? Uveitis is inflammation of a layer of the eye, called the
Information for patients and parents Manchester Royal Eye Hospital Paediatric Uveitis Service Screening for Uveitis in Children What is uveitis? Uveitis is inflammation of a layer of the eye, called the
Department of Ophthalmology
 Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
Association of Cryptogenic Organizing Pneumonia in Bilateral Anterior Uveitis
 Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: November 13, 2014 1663 2699/14/0053 0365$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Necrotizing retinitis of multifactorial etiology
 Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:49-53 CASE REPORT Necrotizing retinitis of multifactorial etiology Pirvulescu Ruxandra Angela* **, Popa Cherecheanu Alina*
Condition: Herpes Zoster Ophthalmicus (HZO)
 Condition: Herpes Zoster Ophthalmicus (HZO) Description: Herpes zoster represents a reactivation of the varicella zoster virus (VZV) which leads to characteristic skin lesions and, in many cases, ocular
Condition: Herpes Zoster Ophthalmicus (HZO) Description: Herpes zoster represents a reactivation of the varicella zoster virus (VZV) which leads to characteristic skin lesions and, in many cases, ocular
Course, complications, and outcome of juvenile arthritis related uveitis
 Major Articles Course, complications, and outcome of juvenile arthritis related uveitis Kourosh Sabri, MB, ChB, FRCOphth, a Rotraud K. Saurenmann, MD, b,a Earl D. Silverman, MD, FRCPC, b,c and Alex V.
Major Articles Course, complications, and outcome of juvenile arthritis related uveitis Kourosh Sabri, MB, ChB, FRCOphth, a Rotraud K. Saurenmann, MD, b,a Earl D. Silverman, MD, FRCPC, b,c and Alex V.
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
CLINICAL SCIENCES. Bilateral Simultaneous-Onset Nongranulomatous Acute Anterior Uveitis
 ONLINE FIRST CLINICAL SCIENCES Bilateral Simultaneous-Onset Nongranulomatous Acute Anterior Uveitis Clinical Presentation and Etiology Andrea D. Birnbaum, MD, PhD; Yi Jiang, MD; Roshni Vasaiwala, MD; Howard
ONLINE FIRST CLINICAL SCIENCES Bilateral Simultaneous-Onset Nongranulomatous Acute Anterior Uveitis Clinical Presentation and Etiology Andrea D. Birnbaum, MD, PhD; Yi Jiang, MD; Roshni Vasaiwala, MD; Howard
What prescribers need to know
 HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
Department of Ophthalmology
 Period : 03/July/17 to 07/September/17 Semester : 7 th Semester Department of Ophthalmology Lecture Lesson Plan Sr 1 03.07.17 Uvea-Anatomy, Uvea-Anatomy, Classification of Uveitis Dr R Paranjpe Classification
Period : 03/July/17 to 07/September/17 Semester : 7 th Semester Department of Ophthalmology Lecture Lesson Plan Sr 1 03.07.17 Uvea-Anatomy, Uvea-Anatomy, Classification of Uveitis Dr R Paranjpe Classification
Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Evolving therapies for posterior uveitis. Infliximab (Remicade) Infliximab: pharmacology. FDA-approved monoclonal antibody therapy Target
 Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
Evolving therapies for posterior uveitis Sam Dahr, M.D. September 17, 2005 Midwest Ophthalmology Conference Infliximab (Remicade) FDA approved for Crohn s disease, rheumatoid arthritis, and psoriatic arthritis
UVEITIS A. D. RUEDEMANN, M.D.
 A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
Dr. D. Y. Patil Medical College, Pimpri, Pune
 Dr. D. Y. Patil Medical College, Pimpri, Pune - 411 018 Period : 04/July/16 to 22/September/16 Semester : 7 th Semester Department : Ophthalmology Lecture Lesson Plan Sr No Date Topic Learning objectives
Dr. D. Y. Patil Medical College, Pimpri, Pune - 411 018 Period : 04/July/16 to 22/September/16 Semester : 7 th Semester Department : Ophthalmology Lecture Lesson Plan Sr No Date Topic Learning objectives
Diffuse infiltrating retinoblastoma
 Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Rhegmatogenous retinal detachment in uveitis
 De Hoog et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:22 DOI 10.1186/s12348-017-0140-5 Journal of Ophthalmic Inflammation and Infection ORIGINAL ARTICLE Open Access Rhegmatogenous retinal
De Hoog et al. Journal of Ophthalmic Inflammation and Infection (2017) 7:22 DOI 10.1186/s12348-017-0140-5 Journal of Ophthalmic Inflammation and Infection ORIGINAL ARTICLE Open Access Rhegmatogenous retinal
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Page 1 RED EYES. conjunctivitis keratitis episcleritis / scleritis. Frank Larkin Moorfields Eye Hospital. acute glaucoma anterior uveitis
 The RED EYE and ALLERGIC EYE DISEASE DIAGNOSIS & MANAGEMENT Frank Larkin Moorfields Eye Hospital RED EYES conjunctivitis keratitis episcleritis / scleritis acute glaucoma anterior uveitis post-op. / trauma
The RED EYE and ALLERGIC EYE DISEASE DIAGNOSIS & MANAGEMENT Frank Larkin Moorfields Eye Hospital RED EYES conjunctivitis keratitis episcleritis / scleritis acute glaucoma anterior uveitis post-op. / trauma
White-Spot Syndromes of the Retina Lee Jampol, M.D. Chicago, IL
 Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
Objectives At the conclusion of the program, the attendees will be able to: 1. recognize the various white-spot syndromes of the retina 2. initiate appropriate diagnostic tests of patients with the white-spot
A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated lesion
 Kobayashi et al. BMC Ophthalmology (2018) 18:129 https://doi.org/10.1186/s12886-018-0797-z CASE REPORT Open Access A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated
Kobayashi et al. BMC Ophthalmology (2018) 18:129 https://doi.org/10.1186/s12886-018-0797-z CASE REPORT Open Access A case of scleritis associated rheumatoid arthritis accompanying an intraocular elevated
A Clinical Evaluation of Uveitis-associated Secondary Glaucoma
 A Clinical Evaluation of Uveitis-associated Secondary Glaucoma Tetsuya Takahashi,*, Shinichiro Ohtani,* Kazunori Miyata,* Norio Miyata,* Shiroaki Shirato and Manabu Mochizuki *Miyata Eye Hospital, Miyakonojo,
A Clinical Evaluation of Uveitis-associated Secondary Glaucoma Tetsuya Takahashi,*, Shinichiro Ohtani,* Kazunori Miyata,* Norio Miyata,* Shiroaki Shirato and Manabu Mochizuki *Miyata Eye Hospital, Miyakonojo,
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
The Red Eye: Conjunctivitis, Iritis, or Worse? Sean P. Donahue, MD, PhD
 The Red Eye: Conjunctivitis, Iritis, or Worse? Sean P. Donahue, MD, PhD Sam and Darthea Coleman Chair Vice Chair of Clinical Affairs, Department of Ophthalmology Professor of Pediatrics, Ophthalmology,
The Red Eye: Conjunctivitis, Iritis, or Worse? Sean P. Donahue, MD, PhD Sam and Darthea Coleman Chair Vice Chair of Clinical Affairs, Department of Ophthalmology Professor of Pediatrics, Ophthalmology,
Early detection of Retinoblastoma in children. Max Mantik
 Early detection of Retinoblastoma in children Max Mantik Introduction The most common primary intraocular malignancy of childhood 10 to 15 % of cancers that occur within the first year of life Typical
Early detection of Retinoblastoma in children Max Mantik Introduction The most common primary intraocular malignancy of childhood 10 to 15 % of cancers that occur within the first year of life Typical
Ciliary Body Metastasis Masquerading as Scleritis. Brian J. Lee, MD 1. Careen Y. Lowder, MD, PhD 1. Charles Biscotti, MD 2. Lynn Schoenfield, MD 2
 Ciliary Body Metastasis Masquerading as Scleritis Brian J. Lee, MD 1 Careen Y. Lowder, MD, PhD 1 Charles Biscotti, MD 2 Lynn Schoenfield, MD 2 Arun D. Singh, MD 1 Cole Eye Institute 1 and Department of
Ciliary Body Metastasis Masquerading as Scleritis Brian J. Lee, MD 1 Careen Y. Lowder, MD, PhD 1 Charles Biscotti, MD 2 Lynn Schoenfield, MD 2 Arun D. Singh, MD 1 Cole Eye Institute 1 and Department of
37 year old male with several year history of back pain
 37 year old male with several year history of back pain Inflammatory Low Back Pain Clues onset before the age of 40 years insidious onset, chronic (>3 months) pain morning stiffness for longer than 30
37 year old male with several year history of back pain Inflammatory Low Back Pain Clues onset before the age of 40 years insidious onset, chronic (>3 months) pain morning stiffness for longer than 30
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Rayos Prior Authorization Program Summary
 Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA)
 www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
Kikuchi-Fujimoto Disease with Bilateral Uveitis
 Kikuchi-Fujimoto Disease with Bilateral Uveitis Hope R. Garner 1, Hilary E. Fazzone 1, Daniel E. Meltzer 1* 1. Department of Radiology, St. Luke's-Roosevelt Hospital Center, New York, NY, USA * Correspondence:
Kikuchi-Fujimoto Disease with Bilateral Uveitis Hope R. Garner 1, Hilary E. Fazzone 1, Daniel E. Meltzer 1* 1. Department of Radiology, St. Luke's-Roosevelt Hospital Center, New York, NY, USA * Correspondence:
Imaging in uveitis. Anthony Hall
 Imaging in uveitis Anthony Hall Causes of Vision Loss in Uveitis 1. Cystoid macular oedema 26% 2. Cataract 19% 3. Glaucoma 11% 4. Permanent macular damage 5% Rothova et al BJO 1996; 80: 332-336 Macular
Imaging in uveitis Anthony Hall Causes of Vision Loss in Uveitis 1. Cystoid macular oedema 26% 2. Cataract 19% 3. Glaucoma 11% 4. Permanent macular damage 5% Rothova et al BJO 1996; 80: 332-336 Macular
Masquerade Scleritis CASE REPORT INTRODUCTION
 Ocular Immunology and Inflammation, 13:479 482, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591004133 CASE REPORT Masquerade Scleritis Chrysanthi
Ocular Immunology and Inflammation, 13:479 482, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591004133 CASE REPORT Masquerade Scleritis Chrysanthi
