Imaging of sacroiliitis in early seronegative spondylarthropathy: Assessment of abnormalities by MR in comparison with radiography and CT
|
|
|
- Poppy Barber
- 6 years ago
- Views:
Transcription
1 Acta Radiologica ISSN: (Print) (Online) Journal homepage: Imaging of sacroiliitis in early seronegative spondylarthropathy: Assessment of abnormalities by MR in comparison with radiography and CT K. BØcker Puhakka, A. G. Jurik, N. Egund, B. Schiottz-Christensen, K. Stengaard-Pedersen, G. vanovereemhansen & J. VallØ Christiansen To cite this article: K. BØcker Puhakka, A. G. Jurik, N. Egund, B. Schiottz-Christensen, K. Stengaard-Pedersen, G. vanovereemhansen & J. VallØ Christiansen (2003) Imaging of sacroiliitis in early seronegative spondylarthropathy: Assessment of abnormalities by MR in comparison with radiography and CT, Acta Radiologica, 44:2, To link to this article: Published online: 16 Sep Submit your article to this journal Article views: 102 View related articles Citing articles: 2 View citing articles Full Terms & Conditions of access and use can be found at Download by: [ ] Date: 04 January 2018, At: 01:07
2 Acta Radiologica 44 (2003) Copyright # Acta Radiologica 2003 Printed in Denmark. All rights reserved ACTA RADIOLOGICA ISSN IMAGING OF SACROILIITIS IN EARLY SERONEGATIVE SPONDYLARTHROPATHY Assessment of abnormalities by MR in comparison with radiography and CT K. BØCKER PUHAKKA 1,A.G.JURIK 1,N.EGUND 1,B.SCHIOTTZ-CHRISTENSEN 2,K.STENGAARD-PEDERSEN 2, G. van OVEREEM HANSEN 3 and J. VALLØ CHRISTIANSEN 4 Departments of 1 Radiology R and 2 Rheumatology, Aarhus University Hospital, Aarhus Kommunehospital, 3 King Christian X Rheumatological Hospital, Graasten, Aarhus and 4 Department of Radiology, Sönderborg Hospital, Sönderborg, Denmark. Abstract Purpose: To analyze the type and frequency of abnormalities of the sacroiliac joint (SIJ) in early seronegative spondylarthropathy (SpA) by MR in comparison with CT and radiography, assess the most appropriate MR sequences to be used, and introduce a new way of grading MR abnormalities of the SIJ. Material and Methods: The SIJs of 41 patients with early SpA (median duration of inflammatory low back pain of 19 months) were evaluated by MR imaging using STIR, T1, T2, and T1 fat saturated (FS) sequences before and after i.v. Gd contrast medium followed by staging of abnormalities. The findings were compared with those obtained by CT and radiography. Results: MR and CT had equal efficacy superior to radiography in staging of erosions and osseous sclerosis. Only MR allowed visualization and grading of active inflammatory changes in the subchondral bone and surrounding ligaments in addition to bone marrow fatty accumulations. T2-weighted sequences did not contribute to assessment of sacroiliitis. Conclusion: MR of the SIJs is reliable in its visualization of joint erosions in early SpA and allows differentiation between active and chronic sacroiliitis. We recommend the following sequences: semicoronal T1 and both semicoronal and semiaxial STIR. If these images are normal, the examination can be finished; otherwise additional semicoronal T1 FS before and after i.v. contrast has to be performed as well as semiaxial post-contrast T1 FS. Key words: Sacroiliitis; MRI; CT. Correspondence: Katriina Bøcker Puhakka, Barthsgade 9. st. mf. th., DK-8200 Aarhus N, Denmark. FAX þ kbpuh@akh.aaa.dk Accepted for publication 20 November The European Spondylarthropathy Study Group (ESSG) defined seronegative spondylarthropathies (SpA) in SpA is divided into five entities (16): ankylosing spondylitis, psoriatic arthritis, reactive arthritis, arthritis associated with inflammatory bowel diseases, and unclassified SpA. The ESSG classification is based on clinical findings. Radiographic evidence of sacroiliitis is included in the definition but is not necessary for diagnosis of SpA. Despite the use of the SpA criteria, the delay in diagnosis may be up to 9 years (13, 36, 41). As SpA occurs mainly in young patients (11) an early diagnosis would be valuable with regard to therapy, prognosis, and evaluation of working capacity. The sacroiliac joints (SIJs) are involved in most cases of SpA and sacroiliitis is commonly the first manifestation of SpA (13). Diagnosis of arthritis in these joints by radiography, CT, or MR therefore 218
3 IMAGING OF SACROILIITIS plays a central role in establishing the diagnosis of early SpA. Since the publication of the diagnostic criteria in 1991, several studies have emphasized the value of CT and MR in the diagnosis of sacroiliitis (4, 7, 8, 18, 38). Both CT and MR have proved their capability to visualize joint erosions earlier than radiography (5, 6, 10, 12, 13, 17, 20, 24, 31, 40). In addition, MR can detect inflammatory changes of the SIJ before any changes are visible by CT. Further, MR is not, as CT, associated with radiation (3, 12, 30, 40). Despite these advantages, MR has not gained wide acceptance in the diagnosis of SpA. This may be explained by difficulties in interpreting MR images of the SIJ partly due to its complex anatomy, being composed of two compartments: a C-shaped cartilaginous portion that lays inferiorly/anteriorly and a ligamentous portion superiorly/posteriorly (9, 23). Besides, analysis of the diagnostic usefulness of different MR sequences seems to be lacking. There is no well-established method for evaluating pathological MR findings of the SIJ, though the need for this is obvious (35). AHLSTRÖM et al. (1) introduced the first method. They divided the findings into two types, mainly based on signal changes on T1, T2, and phase-contrast sequences: Type I lesions were characterized by a low signal intensity on T1-weighted images and a high signal intensity in both phase-contrast and T2-weighted images. Type II lesions consisted of changes presenting with low signal intensity in all sequences. BRAUN et al. (10) described a grading system for disease activity based on quantitative evaluation of contrast enhancement at dynamic MR, and used the New York criteria for joint destruction (22). Other studies have focused on the presence of subchondral bone marrow edema (31) or whether the pathological findings were uni- or bilateral (28). As no studies have assessed the MR findings in detail according to specific localization of signs and grading, there is a need for a new system that can be used to quantify MR signs of both disease activity and joint destruction. The purposes of this study were to analyze articular abnormalities of the SIJs in early SpA by MR in comparison with findings by radiography and CT, assess the most appropriate MR techniques and sequences to be used, and introduce a new way of grading MR abnormalities of the SIJ. Material and Methods In all, 41 patients were included at two different centers, 25 patients at Aarhus University Hospital (Center A) and 16 at the Rheumatological Hospital, Table 1 Clinical features of the 41 patients included in the study No. of patients Median Range Age Males 24 Females 17 Duration of ILBP, months Schober lumbar spine motion test, cm HLA B27 positive 26 Elevated CRP 8 Ongoing NSAID 23 treatment ILBP ¼ inflammatory low back pain. CRP ¼ C-reactive protein. NSAID ¼ non-steroid inflammatory drugs. Graasten (Center B), after referral from the primary ward for either radiography or evaluation at the rheumatological out-patient clinic (Table 1). Patients with radiographic changes stages 0 3 according to the New York criteria (22) were included. All patients fulfilled the ESSG criteria for SpA localized to the SIJ (16) having inflammatory low back pain (ILBP) with at least four of the following manifestations: 1) onset before the age of 45 years; 2) insidious onset; 3) improvement with exercise; 4) associated morning stiffness; and 5) at least 3 months duration. Patients were not included if they showed evidence or had a clinical history of metabolic diseases or malignancies and/or a positive rheumatoid factor. The patients (24 males and 17 females) had a median age of 26 years (20 45 years). The median duration of ILBP was 19 months (3 156 months). Thirty-four of the 41 patients had a disease duration of 36 months or less. The patients gave informed, written consent to participate in a prospective clinical and radiological investigation of SpA. The study was carried out according to the Helsinki Declaration and was approved by the local ethical committees. The present paper is confined to the results of radiography, CT, and MR of the SIJs, performed on all patients at their inclusion in the investigation, with the exception of CT in 2 patients who refused to participate in that examination. A.p. radiography was obtained with a 20 caudal tube tilt. CT was performed in the supine position with a cranial gantry tilt to obtain semicoronal images through both the cartilaginous and ligamentous portions of the SIJs using a Somatom Plus S and a Somatom Plus S4 unit (Siemens) at Centers A and B, respectively. Examination parameters were: contiguous 5-mm slices using 120 kv/ 330 mas at Centers A, and 140 kv/ mas at 219
4 K. PUHAKKA ET AL. Center B. For image reconstruction a standard bone algorithm was used at Center A and a high resolution algorithm at Center B. MR images were obtained with a 1.0 T unit (Signa Highspeed, GE), in 18 patients from Center A and with a 1.5 T unit (Magneton Vision, Siemens) in 7 patients from Center A and in all patients from Center B. The examinations with the 1.0 T unit were performed with a pelvic array coil and consisted of the following sequences: semicoronal short tau inversion recovery (STIR) (TR/TE/TI 4480/66/ 125 ms), semicoronal T1 (TR/TE 400/16 ms), semicoronal T1 with fat saturation (FS) (TR/TE 660/ 16 ms), semiaxial T2 high resolution (TR/TE 5000/ 95 ms), and after administration of i.v. gadolinium (Gd) (Omniscan, 1 mmol/kg, maximum 100 mmol) semicoronal and semiaxial T1 FS (TR/TE 660/ 16 ms). The slice thickness was 4 mm at all sequences with mm spacing. The examinations with the 1.5 T unit were performed with a body array coil. Similar sequences were used, but the parameters were slightly different: TR/TE/TI 4000/30/150 ms for STIR, TR/TE 405/12 ms for T1, TR/TE 660/12 ms for T1 FS, and TR/TE 4100/ 132 ms for T2. The slice thickness was 4 mm at all sequences with spacing of <1 mm. The slice orientations were standardized: semicoronal slices were placed parallel to a line joining the upper dorsal aspect of S1 and S3, and semiaxial slices were perpendicular to the semicoronal plane (Fig. 1). Assessment and grading of images: The images were assessed blindly by two senior radiologists (A.G.J. and N.E.). The MR and CT examinations were analyzed independently, but with the radiographs available at both evaluations to simulate the daily clinical situation. Radiographic abnormalities of the SIJs (Fig. 2a) were graded according to the New York criteria for sacroiliitis in 5 stages: 1) normal; 2) suspicious changes; 3) minimal abnormality in the form of small areas of erosions or sclerosis without alteration in the joint width; 4) unequivocal abnormality moderate or advanced sacroiliitis consisting of erosions, sclerosis, widening, narrowing, and/or partial ankylosis; and 5) severe abnormality in the form of total ankylosis (22). At CT (Fig. 2b) the SIJs were assessed with regard to 1) erosions (destruction of the joint surface); 2) bone marrow sclerosis (increased density); 3) fat accumulation in bone marrow (decreased density); and 4) irregular surface and/or new bone formation at entheses. These findings were graded as 0¼normal, 1¼minimal, 2¼moderate and 3¼severe. A similar grading was used for joint space narrowing, supplemented by a registration of joint space widening (grade 2*). 220 Fig. 1. Scan planes by MR. a) Drawing showing the semicoronal and semiaxial scan planes at the middle of the sacrum together with a lateral view of the whole sacrum with the joint facet. b) Semicoronal and semiaxial scan planes (patient in Fig. 2). Assessment of the MR examinations (Fig. 2c f) included a similar grading of the following findings: 1) erosions; 2) osseous sclerosis (low signal intensity at T1 and/or T1 FS); 3) fat accumulation in the bone marrow (high signal intensity at T1); 4) irregular surface and/or new bone formation at entheses; 5) joint space width; 6) bone marrow edema/reparative processes (high signal intensity at STIR); 7) Gd contrast enhancement in the bone marrow separated in regions with abnormal low and normal signal intensity at precontrast T1 FS, respectively; 8) Gd contrast enhancement in the cartilaginous and ligamentous joint space; and 9) Gd contrast enhancement at entheses outside the joint. All assessments and gradings by CT and MR were performed at four anatomical sites of each SIJ: the sacral and iliac side of the cartilaginous and ligamentous portions of the joint (Fig. 3). The
5 IMAGING OF SACROILIITIS a b c d e f Fig. 2. A 27-year-old HLA B27 positive man with 2 years of ILBP associated with psoriatic skin and nail changes. a) Radiograph of the SIJs showing bilateral sacroiliitis grade 3. b) Semicoronal CT demonstrating bilateral erosions and sclerosis with irregular joint spaces and a slightly decreased density in the sacral bone compatible with fatty marrow changes. c) Semicoronal T1-weighted sequence showing erosions, sclerosis, fatty marrow changes (white arrows) and joint width alteration. d) T1-weighted sequence with FS more clearly visualizes the erosions (white arrows). e) Semicoronal STIR sequence illustrating bone marrow edema (open arrow). f) Semicoronal T1 FS after i.v. Gd demonstrating contrast enhancement in the bone marrow (arrows) and the joint space. 221
6 K. PUHAKKA ET AL. a b c d e Fig. 3. Drawing of the two joint compartments of the sacroiliac joints showing the frequency of the different grades of pathological changes at the various joint positions by CT and MR. Number of patients. a) Erosions. b) Sclerosis. c) Fat accumulation in bone marrow. d) Joint width alteration and contrast enhancement. e) Bone marrow edema and contrast enhancement. severity of erosions, sclerosis, and fat accumulation in bone marrow were calculated as a sum of the score for the abnormality in each position, the total maximal score for each abnormality being 12 for each joint, and 24 for a patient. Similarly, a total score for alteration of joint space width and Gd contrast enhancement in the joint space was obtained, resulting in a total maximal score of 6 222
7 IMAGING OF SACROILIITIS Table 2 Scoring system for MR abnormalities based on assessment at 8 osseous positions (the iliac and sacral sides of the cartilaginous and ligamentous portions of the joints, respectively) and 4 joint space positions (cartilaginous and ligamentous joint spaces), as demonstrated in Fig. 3. An osseous joint position or a joint space One SIJ: 4 osseous positions; 2 joint spaces A patient: 8 osseous positions; 4 joint spaces MR abnormalities Grade range Score range Score range Erosion Sclerosis Joint space width Overall joint destruction score 0 60 Bone marrow edema Gd enhancement in bone marrow Gd enhancement in joint space Overall activity score 0 60 for a joint and 12 for a patient. Widening of the joint space (grade 2*) was given a value of 2. Finally, for MR, an overall score for joint destruction was calculated as a sum of the scores for erosions, sclerosis, and joint width (maximum 60 per patient). Similarly, an overall score for inflammatory activity was calculated as a sum of the scores for bone marrow edema, Gd contrast enhancement in the bone marrow, and in the joint space (maximum score 60 per patient) (Table 2). An overall stage of sacroiliitis with regard to joint destruction and enthesopathy graded 0 4 corresponding to the New York criteria for sacroiliitis (22) was also recorded for each joint at CT and MR to facilitate the comparison with radiography. The MR sequences used were assessed with regard to their capability to visualize the articular and osseous abnormalities of sacroiliitis. Statistics: SPSS software (version 10.0) was used to perform the following tests: McNemar test for differences in frequencies of two variables and nonparametric paired samples t-test to compare means. Kappa test with regard to agreement and McNemar test for disagreement were used to estimate the interand intraobserver variations. A value of p<0.05 was considered significant. Results The distribution and severity of sacroiliitis assessed by radiography is displayed in Table 3, which also shows the frequency of unilateral and bilateral changes as well as symmetric and asymmetric changes. The interobserver agreement for the evaluation of radiographs was 89% with a kappa value of 0.63 and a non-significant McNemar test. Osseous changes in the ligamentous portion of the SIJs were rare by CT and MR (Fig. 3). Therefore, assessment of interobserver agreement at CT and MR was only performed for the evaluation of the Table 3 Frequencies, distribution, and severity of sacroiliitis by radiography, CT, and MR. Radiography and MR data are based on 41 and CT on 39 patients. The MR findings are divided into those related to joint destruction (MRI joint) and activity (MR activ.) and based on the New York criteria and our new MR scoring, respectively No. of patients Grading of changes, maximal stage; no. of patients Sacroiliitis stage Sacroiliitis unilat. bilat. sym. asym Mean New York Radiography CT MR joint New scoring MR joint MR activ unilat., unilateral sacroiliitis. bilat., bilateral sacroiliitis. sym., symmetric sacroiliitis. asym., asymmetric sacroiliitis. 223
8 K. PUHAKKA ET AL. cartilaginous portion of the joint, and the results, based on evaluation of all patients, are shown in Table 4. For both CT and MR there was a poor agreement in the assessment of the joint width. The interobserver agreement for the other CT and MR parameters varied between 71% and 94% with kappa values of MR for sclerosis and inflammatory activity evaluated the lowest agreements. The McNemar test was significant for erosions, sclerosis, edema, contrast enhancement, and overall activity score by MR, and for erosions and alteration of the joint width by CT (Table 4). This was not due to a trend of any of the observers to score more joint abnormalities than the other. There was a tendency for N.E. to assess more erosions by CT and MR and more joint width alterations by CT than A.G.J., while A.G.J. had a tendency to assess more sclerosis, bone marrow edema, and enhancement by MR than N.E. Assessment of the intraobserver agreement of A.G.J. was made blindly with approximately 1 year between the first and the second evaluations. The intraobserver agreements varied between 93% and 100% with kappa values between 0.84 and 1.0 and no significant McNemar tests (Table 4). The intraobserver agreement for the radiographs was 95% (kappa¼0.64, p¼1.0). The following findings are based on the evaluation of A.G.J., instead of an amalgam of the two observers, because of the high inter- and intraobserver agreements. The results of CT and MR appear in Fig. 3. Erosions: were observed in 34 patients by CT and in 33 patients by MR. The distribution of erosions in the different positions and the frequency of the different grades of erosions are shown in Fig. 3a. Except in 1 patient, who had erosions in the ligamentous portion of both joints by CT, erosions were only found in the cartilaginous portion of the joints where they predominated on the iliac side. The mean total joint score for erosions was 1.31 by CT, 1.32 by MR for the 39 patients examined by CT, and 1.29 for all patients (Table 5). Sclerosis was observed in 30 patients by CT and in 29 patients by MR. The distribution of sclerosis in the different positions and the different grades of sclerosis are shown in Fig. 3b. Sclerosis was most often seen in the cartilaginous portion of the joint. The mean total joint score for sclerosis was 1.12 by CT and 1.19 by MR for the 39 patients examined by CT (Table 5). Subchondral osseous sclerosis in the cartilaginous portion of the SIJ graded >2 by CT occurred in 21 positions. In all those positions there was decreased signal intensity on T1 FS before contrast injection. In 19 positions there was additional increased signal intensity by STIR and/or contrast enhancement (18 had both). Increased signal intensity by T1 (sign of fat accumulation in bone marrow) occurred in 15 of the 21 positions, in combination with marrow edema and contrast enhancement in 12. Decreased signal intensity on T1 FS before contrast injection occurred in a further 73 positions, in 37 of which there was osseous sclerosis grade 1 by CT. In 16 of the remaining 36 positions Table 4 Inter- and intraobserver (A.G.J.) agreement for each sign in the cartilaginous portion of the SIJ assessed by MR and CT; McNemar (p) and kappa ( k) tests values Pathological findings MR agreement, % Interobserver p k CT agreement, % p k MR agreement, % Intraobserver p k CT agreement, % Erosion Sclerosis Fat accumulation in bone marrow Alterations of joint width Bone marrow edema Enhancement in bone Enhancement in joint space Sacroiliitis (joint stage) Sacroiliitis (joint score) Sacroiliitis (activity score) p k 224
9 IMAGING OF SACROILIITIS Table 5 Mean and median values for the total joint scores representing the sum of the gradings in each position of the joints. By MR for all joints and for the 78 joints compared with CT MR, 82 joints MR, 78 joints CT, 78 joints MR/CT, 78 joints mean median range mean median range mean median range difference p-value Erosion Sclerosis Fatty marrow < Joint width <0.01 Edema Enhancement, bone Enhancement, joint space there was increased signal intensity by T1 (fat accumulation in bone marrow). Fat accumulation in bone marrow was observed in 2 patients by CT and in 26 patients by MR. The distribution in the different joint positions and the division into grades appear in Fig. 3c. The changes mainly affected the cartilaginous portion of the joint. The mean total joint score was 0.04 by CT and 1.19 by MR (p<0.0001) (Table 5). New bone formation at entheses was observed in 13 patients by CT and in 1 patient by MR (Fig. 4). The new bone formation observed by CT was in all 13 patients located at the insertion of the dorsal ligaments, but 1 patient had additional changes anteriorly which were also visible by MR (Fig. 4). Alterations in joint width: Changes in joint width, either narrowing or widening, were observed in 34 patients by CT and in 26 patients by MR. The distribution in the different joint portions, including a separation between narrowing and widening and a division into grades appears in Fig. 3d. The changes were mainly seen in the cartilaginous portion of the joint. The mean total score for joint alteration was significantly higher by CT than by MR, the values being 1.15 and 0.82, respectively, for the patients evaluated by both modalities (p<0.01) (Table 5). Bone marrow edema was present in 35 patients by MR. The distribution and division into grades appear from Fig. 3e. Marrow edema predominantly occurred in the cartilaginous portion and at the iliac side of the joint. The mean total joint score for edema was 2.11 (Table 5). Enhancement of bone was observed in 37 patients by MR with a joint distribution as shown in Fig. 3e. Enhancement was seen in both the ligamentous and the cartilaginous portions of the joint, but most often in the latter and on the iliac side. The grading of changes appears in Fig. 3e. The mean total joint score for bone enhancement was 1.89 (Table 5). Correlation between bone marrow edema and enhancement: There was a significant association between the occurrence of bone marrow edema and contrast enhancement, both when looking at all joint positions (p<0.001) and when analyzing only the cartilaginous portion of the joints (p<0.001). Bone marrow edema and contrast enhancement occurred simultaneously in 91 and were absent in 55 of the 164 cartilaginous joint positions, corresponding to an agreement of 89%. Enhancement was observed in 8 positions without signs of edema, and lack of enhancement occurred in 10 positions with an edema. Enhancement in the joint space was seen in 26 patients by MR with a joint distribution and different grades of enhancement as shown in Fig. 3d. It occurred in both joint portions, but more frequently in the cartilaginous than in the ligamentous portion of the joint. The mean total joint score for enhancement was Enhancement at entheses outside the joint occurred in 9 patients (Fig. 4). The agreement and discrepancy of CT and MR to detect erosions, sclerosis, and fat accumulation in bone marrow, and alterations of joint width was analyzed statistically corresponding to the cartilaginous portion only, due to the rare occurrence of abnormalities in the ligamentous portion (Fig. 3). The results based on the 39 patients undergoing both examinations, are given in Table 6. Erosions, sclerosis, and sacroiliitis (stage of joint destruction) were recorded equally often by the two examinations, while MR significantly more often than CT demonstrated fat accumulation in bone marrow (p<0.0001). The agreement between CT and MR in displaying joint width alteration approached significance (p¼0.08) in the favor of CT. CT was able to demonstrate new bone formation at entheses, which was only the case in 1 patient by MR (Fig. 4). MR, on the other hand, detected signs 225
10 K. PUHAKKA ET AL. a b c Fig. 4. HLA B27 negative 45-year-old man with ILBP for 5 years and a family history of psoriasis. a) CT images showing new bone formation at the attachment of the posterior ligaments to the sacrum and bridging of new bone formation anteriorly (arrows). b) Semicoronal and (c) semiaxial T1-weighted FS sequences after i.v. Gd demonstrating ligamentous enhancement posteriorly and bridging bone formation anteriorly without accompanying enhancement (arrows). Table 6 Agreement and discrepancy between CT and MR in the detection of pathological changes in the cartilaginous portion of the SIJs of 39 patients No. of locations/ joints Erosion Sclerosis Fat accumulation in bone marrow Changes of joint width Sacroiliitis, joint destruction 226 Agreement CT/MR MR pos. CT neg. CT pos. MR neg. p-value McNemar n % <
11 IMAGING OF SACROILIITIS of inflammation in the form of contrast enhancement at entheses outside the joint in 9 patients (Fig. 4) and also inflammatory changes in the bone and joint spaces, not visible by CT (Fig. 2). Based on the 39 patients undergoing all three examination modalities, MR was found to grade the overall changes of joint destruction significantly higher than either radiography (p<0.001) or CT (p<0.01) (Table 3). Of the 2 patients not evaluated by CT, 1 had bilateral, symmetrical joint destruction stage 2 by both radiography and MR, and a bilateral activity stage of 3 by MR. The other patient had unilateral joint destruction stage 1 by radiography and no signs of activity by MR. By MR the mean overall activity score for all 41 patients was 10.3 (0 37), while the similar mean overall destruction score was 6.5 (0 16). Evaluation of the MR sequences used disclosed that the STIR sequence in all patients was valuable for the detection of inflammation. The postcontrast T1 FS gave further information due to higher contrast resolution and a better delineation of the anatomical structures and visualization of vascularized inflammation. Except in 3 patients, the T1 sequence was considered to give information about fat accumulation in bone marrow that could not be achieved by the other sequences. In all but 2 patients, the transverse slices (T2 and postcontrast T1 FS) gave additional information compared to the semicoronal slices due to a better visualization of the ligamentous portion of the joint, but the T2 sequence never gave additional information compared to the postcontrast T1 FS. Discussion In the course of sacroiliitis both acute and chronic changes can occur, separately or at the same time in different areas of the same joint. Acute inflammatory activity presents with bone marrow edema, which is known to be an early and unspecific sign of various abnormalities in bone marrow (37), and contrast enhancement caused by increased vascularization (25). Erosions, sclerosis, and changes of joint width are regarded as signs of chronicity (13), as well as fat deposition in the bone marrow, which can be regarded as a sign of degeneration and healing (21, 26). Chronic bone changes can be detected and graded by both CT and MR, and our data showed that no essential information is lost by using MR instead of CT. We found that the overall stage of joint destruction using the New York criteria (22) was evaluated higher by MR than by CT, probably because MR was better than CT at detecting fat accumulation in the bone marrow. CT demonstrated osseous proliferation in the ligamentous portion that could not be identified by MR. However, MR was capable of detecting inflammation, so the final diagnosis of sacroiliitis was usually established. Only 1 of the present patients was recorded to have possible sacroiliitis (stage 1) by both conventional radiography and CT, but had no detectable joint destruction or signs of activity by MR. At follow-up a year later there were signs of both joint destruction and activity at MR (33). The advantages of MR compared with CT are that it visualizes active inflammatory changes in the form of bone marrow edema and contrast enhancement, making it possible to diagnose sacroiliitis by MR before definite joint destruction, detectable by CT and radiography, occu (3, 5, 6, 10, 12, 13, 24, 30, 31, 40). To our knowledge, six studies comparing MR and CT of the SIJs with regard to sacroiliitis have been published (1, 3, 30, 34, 39, 40). The number of patients included in these studies varied from 17 to 50 (mean 38). The duration of symptoms was not mentioned in any of these studies, but as most of the patients included had defined SpA, it seems likely that our patients were examined at an earlier stage of the disease as they were referred from the primary ward and most had a relative short disease duration. In one of the six studies, MR and CT were not evaluated independently (1). In the remaining studies different sequences and scan parameters were used, and postcontrast MR images were only obtained in one study (40). The results of the five comparative studies are in agreement with those of the present study, finding that MR is equally good or even better than CT at detecting overall SIJ changes. When looking at different signs of sacroiliitis, CT has been reported superior to MR in detecting sclerosis (40) and bone production (20). The latter finding was consistent with that of the present analysis, but sclerosis, in our study, was detected with nearly equal frequency by CT and MR. The present study included an analysis of the signal intensities by MR corresponding to areas disclosing definite sclerosis by CT. The results of one observer (A.G.J.) showed that the sclerosis detected by CT corresponded to a mixture of inflammation, fatty marrow changes, and/or increased osseous tissue or marrow fibrosis by MR. An explanation for the low interobserver agreement regarding sclerosis may be the consideration of one observer (N.E.) that contrast enhancement in bone marrow with low signal intensity at the precontrast T1 sequence may indicate that there is not any increased amount of trabecular bone. 227
12 K. PUHAKKA ET AL. The great advantage of MR compared with CT is the capability to detect inflammation, which in addition to joint destruction is a sign of sacroiliitis. Besides, MR enables a clear distinction of the two portions of the SIJ based upon a well-delineated differentiation between fatty tissue in the ligamentous portion and cartilage in the cartilaginous portion (32). CT only identifies the two portions of the SIJ by their orientation and position (14). This, combined with the ability of MR to detect inflammatory changes, provides an opportunity to analyze pathological inflammatory changes in the ligamentous portion of the joint that would not be detected by CT. This can be important for the diagnosis of early inflammatory changes in patients where the changes are mainly situated in the ligamentous portion. However, chronic changes in that region in the form of new bone formation at entheses are better visualized by CT than by MR, reflected by the fact that new bone formation seen in 13 of the present patients at CT was only visualized in 1 patient by MR (Fig. 4). This patient had changes both at the attachment of the posterior ligaments and anteriorly. The bridging bone formation anteriorly may, however, be due to bridging osteophytes, as seen in degenerative disease. In concordance with our findings, in a recent study (29) CT was found to be optimal in the detection of erosions and was capable of visualizing calcifications in the ligamentous portion of the SIJ. Taking all aspects of sacroiliitis into consideration, MR has only been found significantly inferior to CT for the diagnosis of sacroiliitis in one study (34). An explanation for the different results could be that study (34) was based on comparison of a high resolution CT technique (slice thickness of 2 mm and 480 mas) and MR performed with a body coil and only T1- and T2-weighted sequences. The capability of MR to distinguish between acute and chronic changes and to estimate the degree of disease activity can be beneficial in monitoring the effect of pharmacological treatment (2). The use of dynamic contrast-enhanced MR to evaluate the level of inflammatory activity has been reported of value (7, 38). This method is, however, difficult to apply in routine clinical practice because the assessment is time-consuming, and reproduction of the findings may be difficult. Most reports on MR examinations of SIJs are obtained with semicoronal sectioning. In this study we added a semiaxial sequence providing obvious advantages, as the anatomy of the ventral and dorsal margins of the cartilaginous portion of the joint only can be assessed by this view (32). Semiaxial views also give a good characterization of the ligamentous portion of the SIJ. A proper examination 228 of the joint should therefore contain both semicoronal and semiaxial views. Based on the present analysis we recommend the following sequences for examination of the SIJs with regard to sacroiliitis: semicoronal T1 and both semicoronal and semiaxial STIR. If the images of these two sequences are normal, the examination is completed; otherwise, additional semicoronal T1 FS before and after i.v. contrast has to be performed as well as semiaxial postcontrast T1 FS. CT of the SIJs is associated with radiation exposure. Although optimal machine settings, the use of only a few slices (15, 19), or a semicoronal scan plane (27) can reduce the radiation dose, it is more desirable to avoid radiation completely. This can be achieved by replacing CT with MR, though still keeping in mind the situations in which CT is superior to MR, i.e., detection of chronic bone changes in the ligamentous portion of the joint (29). The present study described a new way of assessing and grading MR abnormalities of the SIJ in early SpA, which can be used for quantifying both the inflammatory activity and the joint destruction. The method has to be further analyzed before it can be used in daily routine. Conclusion: MR and CT are nearly equally good in detecting joint destruction as part of sacroiliitis in the cartilaginous portion of the SIJ. MR in addition visualizes early active inflammatory changes and is not associated with radiation exposure. When available, MR of the SIJs should therefore be the first choice in suspected early SpA, and we recommend semicoronal T1 and both semicoronal and semiaxial STIR sequences. If the images of these sequences are normal, the examination can be completed; otherwise, additional semicoronal T1 FS before and after i.v. contrast has to be performed as well as semiaxial postcontrast T1 FS. ACKNOWLEDGMENTS We gratefully acknowledge the Danish Rheumatism Association and A.P. Møller og Hustru Chastine Mc-Kinney Møllers Fond til almene Formaal for financial support. We also thank Nycomed Denmark A/S for providing the contrast agent, and engineer, Ph.D. Peter Vestergaard Poulsen for technical assistance in providing the MR sequences. REFERENCES 1. Ahlström H, Feltelius N, Nyman R, Hällgren R. Magnetic resonance imaging of sacroiliac joint inflammation. Arthritis Rheum. 1990; 33: Antoni C, Dechant C, Ogilvie A, Kalden-Nemeth D, Kalden JR, Manger B. Successful treatment of psoriatic arthritis with infliximab in a MRI controlled study. J. Rheumatol. 2000; 27: Battafarano DF, West SG, Rak KM, Fortenbery EJ, Chantelois AE. Comparison of bone scan, computed
13 IMAGING OF SACROILIITIS tomography, and magnetic resonance imaging in the diagnosis of active sacroiliitis. Semin. Arthritis Rheum. 1993; 23: Bigot J, Loeuille D, Chary Valckenaere I, Pourel J, Cao MM, Blum A. Détermination des meilleurs critères diagnostiques des sacro-iliites en IRM. J. Radiol. 1999; 80: Blum U, Buitrago-Tellez C, Mundinger A, et al. Magnetic resonance imaging (MRI) for detection of active sacroiliitis a prospective study comparing conventional radiography, scintigraphy, and contrast enhanced MRI. J. Rheumatol. 1996; 23: Bollow M, Braun J, Biedermann T, et al. Use of contrastenhanced MR imaging to detect sacroiliitis in children. Skeletal Radiol. 1998; 27: Bollow M, Braun J, Hamm B, et al. Early sacroiliitis in patients with spondyloarthropathy: evaluation with dynamic gadolinium-enhanced MR imaging. Radiology 1995; 194: Bollow M, König H, Hoffmann C, Schilling A, Wolf KJ. Erste Erfahrungen mit der dynamischen Magnetresonanztomographie in der Diagnostik entzündlicher Erkrankungen der Sakroiliakagelenke. RÖFO 1993; 159: Bowen V, Cassidy JD. Macroscopic and microscopic anatomy of the sacroiliac joint from embryonic life until the eighth decade. Spine 1981; 6: Braun J, Bollow M, Eggens U, König H, Distler A, Sieper J. Use of dynamic magnetic resonance imaging with fast imaging in the detection of early and advanced sacroiliitis in spondylarthropathy patients. Arthritis Rheum. 1994; 37: Braun J, Bollow M, Remlinger G, et al. Prevalence of spondylarthropathies in HLA-B27 positive and negative blood donors. Arthritis Rheum. 1998; 41: Braun J, Sieper J. The sacroiliac joint in the spondyloarthropathies. Curr. Opin. Rheumatol. 1996; 8: Braun J, Sieper J, Bollow M. Imaging of sacroiliitis. Clin. Rheumatol. 2000; 19: Carrera GF, Foley WD, Kozin F, Ryan L, Lawson TL. CT of sacroiliitis. AJR 1981; 136: Damilakis J, Prassopoulos P, Persinakis K, Faflia C, Gourtsoyiannis N. CT of the sacroiliac joints. Dosimetry and optimal settings for a high-resolution technique. Acta Radiol. 1997; 38: Dougados M, van der Linden S, Juhlin R, et al. The European Spondylarthropathy Study Group preliminary criteria for the classification of spondylarthropathy. Arthritis Rheum. 1991; 34: Fenlon HM, Casserly I, Sant SM, Breatnach E. Plain radiographs and thoracic high-resolution CT in patients with ankylosing spondylitis. AJR 1997; 168: Friedburg H, Meske S, Hennig J, Billmann P, Peter HH, Wenz W. Die Kernspintomographie des Sakroiliakagelenkes. Eine neue Untersuchungstechnik zur Differentialdiagnose rheumatischer Erkrankungen im lumbosacralen Übergang. Radiologe 1987; 27: Friedman L, Silberberg PJ, Rainbow A, Butler R. A limited, low-dose computed tomography protocol to examine the sacroiliac joints. Can. Assoc. Radiol. J. 1993; 44: Geijer M, Sihlbom H, Göthlin JH, Nordborg E. The role of CT in the diagnosis of sacroiliitis. Acta Radiol. 1998; 39: Gillams AR, Chaddha B, Carter AP. MR appearances of the temporal evolution and resolution of infectious spondylitis. AJR 1996; 166: Gofton JP, Bennett PH, Bremner JM, et al. Report from the Subcommittee on Diagnostic Criteria for Ankylosing Spondylosis. 1966: Goss CM. Gray s Anatomy. Lea & Febiger, 1973: Hanly JG, Mitchell MJ, Barnes DC, MacMillan L. Early recognition of sacroiliitis by magnetic resonance imaging and single photon emission computed tomography. J. Rheumatol. 1994; 21: Hurley JV. Inflammation. In: Muir s Textbook of Pathology. London: Edward Arnold, Jevtic V, Rozman B, Kos-Golja M, Watt I. MR-Bildgebung bei seronegativen Spondyloarthritiden. Radiologe 1996; 36: Jurik AG, Hansen J, Puhakka KB. Effective radiation dose from semicoronal CT of the sacroiliac joints in comparison with axial CT and conventional radiography. Eur. Radiol. 2002; 12: Lee SH, Jee WH, Kim WU, et al. Association of sacroiliac MR findings with disease activity in patients with ankylosing spondylitis. Arthritis Rheum. 1999; 42: Mester AR, Makó EK, Karlinger K, et al. Enteropathic arthritis in the sacroiliac joint. Imaging and differential diagnosis. Eur. J. Radiol. 2000; 35: Murphey MD, Wetzel LH, Bramble JM, Levine E, Simpson KM, Lindsley HB. Sacroiliitis. MR imaging findings. Radiology 1991; 180: Oostveen J, Prevo R, den Boer J, van de Laar M. Early detection of sacroiliitis on magnetic resonance imaging and subsequent development of sacroiliitis on plain radiography. A prospective, longitudinal study. J. Rheumatol. 1999; 26: Puhakka KB, Egund N, Melsen F, et al. MR imaging of the normal sacroiliac joint with correlation to histology. Skeletal Radiol. 2003; Puhakka KB, Jurik AG, Egund N, et al. The course of sacroiliitis in early seronegative spondylarthropathy. A radiological and clinical follow-up study. Scand. J. Rheum., in press. 34. Rémy M, Bouillet P, Bertin P, et al. Evaluation of magnetic resonance imaging for the detection of sacroiliitis in patients with early seronegative spondylarthropathy. Rev. Rhum. Engl. Ed. 1996; 63: Stone M, Salonen D, Lax M, Payne U, Lapp V, Inman R. Clinical and imaging correlates of response to treatment with infliximab in patients with ankylosing spondylitis. J. Rheumatol. 2001; 28: Underwood MR, Dawes P. Inflammatory back pain in primary care. Br. J. Rheumatol. 1995; 34: Vahlensieck M, Reiser M. Knochenmarködem in der MRT. Radiologe 1992; 32: Wittram C, Whitehouse GH, Bucknall RC. Fat suppressed contrast enhanced MR imaging in the assessment of sacroiliitis. Clin. Radiol. 1996; 51: Wittram C, Whitehouse GH, Williams JW, Bucknall RC. A comparison of MR and CT in suspected sacroiliitis. J. Comput. Assist. Tomogr. 1996; 20: Yu W, Feng F, Dion E, Yang H, Jiang M, Genant HK. Comparison of radiography, computed tomography and magnetic resonance imaging in the detection of sacroiliitis accompanying ankylosing spondylitis. Skeletal Radiol. 1998; 27: Zink A, Braun J, Listing J, Wollenhaupt J. Disability and handicap in rheumatoid arthritis and ankylosing spondylitis results from the German rheumatological database. German Collaborative Arthritis Centers. J. Rheumatol. 2000; 27:
The Clinical Usefulness of Multidetector Computed Tomography of the Sacroiliac Joint for Evaluating Spondyloarthropathies
 The Korean Journal of Internal Medicine : 22:171-177, 2007 The Clinical Usefulness of Multidetector Computed Tomography of the Sacroiliac Joint for Evaluating Spondyloarthropathies You-Hyun Lee, M.D.,
The Korean Journal of Internal Medicine : 22:171-177, 2007 The Clinical Usefulness of Multidetector Computed Tomography of the Sacroiliac Joint for Evaluating Spondyloarthropathies You-Hyun Lee, M.D.,
MRI of the sacroiliac joints: what to report and its pitfalls
 MRI of the sacroiliac joints: what to report and its pitfalls Poster No.: C-1920 Congress: ECR 2016 Type: Educational Exhibit Authors: J. Goncalves, A. Y. Aihara, C. Longo, H. Guidorizzi, P. Aguiar, 1
MRI of the sacroiliac joints: what to report and its pitfalls Poster No.: C-1920 Congress: ECR 2016 Type: Educational Exhibit Authors: J. Goncalves, A. Y. Aihara, C. Longo, H. Guidorizzi, P. Aguiar, 1
ARD Online First, published on October 11, 2005 as /ard
 ARD Online First, published on October 11, 2005 as 10.1136/ard.2005.044206 Combining information obtained from MRI and conventional radiographs in order to detect sacroiliitis in patients with recent-onset
ARD Online First, published on October 11, 2005 as 10.1136/ard.2005.044206 Combining information obtained from MRI and conventional radiographs in order to detect sacroiliitis in patients with recent-onset
Imaging and intervention of sacroiliac joint. Dr Ryan Lee Ka Lok Associate Consultant Prince of Wales Hospital
 Imaging and intervention of sacroiliac joint Dr Ryan Lee Ka Lok Associate Consultant Prince of Wales Hospital Introduction 15%-25% of low back pain is related to sacroiliac joint (SIJ) pain SIJ pain is
Imaging and intervention of sacroiliac joint Dr Ryan Lee Ka Lok Associate Consultant Prince of Wales Hospital Introduction 15%-25% of low back pain is related to sacroiliac joint (SIJ) pain SIJ pain is
T he spondyloarthritides (SpA) comprise five subtypes:
 1305 EXTENDED REPORT Magnetic resonance imaging of the spine and the sacroiliac joints in ankylosing spondylitis and undifferentiated spondyloarthritis during treatment with etanercept M Rudwaleit*, X
1305 EXTENDED REPORT Magnetic resonance imaging of the spine and the sacroiliac joints in ankylosing spondylitis and undifferentiated spondyloarthritis during treatment with etanercept M Rudwaleit*, X
MRI of the Sacroiliac Joints in Patients with Moderate to Severe Ankylosing Spondylitis
 MRI of Sacroiliac Joints in Patients with nkylosing Spondylitis Musculoskeletal Imaging Original Research M E D E N T U R I L I M G I N G JR 2006; 187:1420 1426 0361 803X/06/1876 1420 merican Roentgen
MRI of Sacroiliac Joints in Patients with nkylosing Spondylitis Musculoskeletal Imaging Original Research M E D E N T U R I L I M G I N G JR 2006; 187:1420 1426 0361 803X/06/1876 1420 merican Roentgen
Update - Imaging of the Spondyloarthropathies. Spondyloarthropathies. Spondyloarthropathies
 Update - Imaging of the Spondyloarthropathies Donald J. Flemming, M.D. Dept of Radiology Penn State Hershey Medical Center Spondyloarthropathies Family of inflammatory arthritides of synovium and entheses
Update - Imaging of the Spondyloarthropathies Donald J. Flemming, M.D. Dept of Radiology Penn State Hershey Medical Center Spondyloarthropathies Family of inflammatory arthritides of synovium and entheses
ORIGINAL ARTICLE INTRODUCTION
 Arthritis & Rheumatism (Arthritis Care & Research) Vol. 53, No. 5, October 15, 2005, pp 703 709 DOI 10.1002/art.21445 2005, American College of Rheumatology ORIGINAL ARTICLE Spondyloarthritis Research
Arthritis & Rheumatism (Arthritis Care & Research) Vol. 53, No. 5, October 15, 2005, pp 703 709 DOI 10.1002/art.21445 2005, American College of Rheumatology ORIGINAL ARTICLE Spondyloarthritis Research
37 year old male with several year history of back pain
 37 year old male with several year history of back pain Inflammatory Low Back Pain Clues onset before the age of 40 years insidious onset, chronic (>3 months) pain morning stiffness for longer than 30
37 year old male with several year history of back pain Inflammatory Low Back Pain Clues onset before the age of 40 years insidious onset, chronic (>3 months) pain morning stiffness for longer than 30
Department of Radiology, Aarhus University Hospital, Aarhus, Denmark; 4. Key words MRI, sacroiliitis, ankylosing spondylitis, axial spondyloarthritis.
 Gadolinium contrast-enhanced MRI sequence does not have an incremental value in the assessment of sacroiliitis in patients with early inflammatory back pain by using MRI in combination with pelvic radiographs:
Gadolinium contrast-enhanced MRI sequence does not have an incremental value in the assessment of sacroiliitis in patients with early inflammatory back pain by using MRI in combination with pelvic radiographs:
Clinical Study Diagnosis and Progression of Sacroiliitis in Repeated Sacroiliac Joint Computed Tomography
 Arthritis Volume 2013, Article ID 659487, 7 pages http://dx.doi.org/10.1155/2013/659487 Clinical Study Diagnosis and Progression of Sacroiliitis in Repeated Sacroiliac Joint Computed Tomography Mats Geijer,
Arthritis Volume 2013, Article ID 659487, 7 pages http://dx.doi.org/10.1155/2013/659487 Clinical Study Diagnosis and Progression of Sacroiliitis in Repeated Sacroiliac Joint Computed Tomography Mats Geijer,
NIH Public Access Author Manuscript Curr Opin Rheumatol. Author manuscript; available in PMC 2011 January 20.
 NIH Public Access Author Manuscript Published in final edited form as: Curr Opin Rheumatol. 2010 September ; 22(5): 603 607. doi:10.1097/bor.0b013e32833c7255. Early axial spondyloarthritis Robert A Colbert
NIH Public Access Author Manuscript Published in final edited form as: Curr Opin Rheumatol. 2010 September ; 22(5): 603 607. doi:10.1097/bor.0b013e32833c7255. Early axial spondyloarthritis Robert A Colbert
M Bollow, T Fischer, H Reiβhauer, M Backhaus, J Sieper, B Hamm, J Braun
 Ann Rheum Dis 2000;59:135 140 135 Radiology, Klinikum Charité, Humboldt University, Berlin, Germany M Bollow T Fischer B Hamm Pathology, Klinikum Charité, Humboldt University H Reiβhauer Rheumatology and
Ann Rheum Dis 2000;59:135 140 135 Radiology, Klinikum Charité, Humboldt University, Berlin, Germany M Bollow T Fischer B Hamm Pathology, Klinikum Charité, Humboldt University H Reiβhauer Rheumatology and
What is Axial Spondyloarthritis?
 Physiotherapist Module 2 What is Axial Spondyloarthritis? How does it apply to physiotherapists? Claire Harris, Senior Physiotherapist, London North West Healthcare NHS Trust Susan Gurden, Advanced Physiotherapy
Physiotherapist Module 2 What is Axial Spondyloarthritis? How does it apply to physiotherapists? Claire Harris, Senior Physiotherapist, London North West Healthcare NHS Trust Susan Gurden, Advanced Physiotherapy
Sacroiliac Joint Imaging
 Sacroiliac Joint Imaging Jacob Jaremko, MD, PhD Edmonton, Canada SPR, May 2017 Longview, Alberta Overview SI joint anatomy Sacroiliitis pathophysiology Sacroiliitis imaging Disease features Imaging protocols
Sacroiliac Joint Imaging Jacob Jaremko, MD, PhD Edmonton, Canada SPR, May 2017 Longview, Alberta Overview SI joint anatomy Sacroiliitis pathophysiology Sacroiliitis imaging Disease features Imaging protocols
Diagnostic value of pelvic enthesitis on MRI of the sacroiliac joints in spondyloarthritis
 Eur Radiol (2014) 24:866 871 DOI 10.1007/s00330-013-3074-9 MUSCULOSKELETAL Diagnostic value of pelvic enthesitis on MRI of the sacroiliac joints in spondyloarthritis L. Jans & C. van Langenhove & L. Van
Eur Radiol (2014) 24:866 871 DOI 10.1007/s00330-013-3074-9 MUSCULOSKELETAL Diagnostic value of pelvic enthesitis on MRI of the sacroiliac joints in spondyloarthritis L. Jans & C. van Langenhove & L. Van
 www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
SpA non-radiografica: fase precoce di spondilite anchilosante o altro?
 Rheumatology Department of Lucania, S. Carlo Hospital of Potenza and Madonna delle Grazie Hospital of Matera SpA non-radiografica: fase precoce di spondilite anchilosante o altro? Ignazio Olivieri Disclosures
Rheumatology Department of Lucania, S. Carlo Hospital of Potenza and Madonna delle Grazie Hospital of Matera SpA non-radiografica: fase precoce di spondilite anchilosante o altro? Ignazio Olivieri Disclosures
Chapter 2. Overview of ankylosing spondylitis
 Chapter 2 Overview of ankylosing spondylitis The concept and classification of spondyloarthritis The term spondyloarthritis (SpA) comprises AS, reactive arthritis, arthritis/spondylitis associated with
Chapter 2 Overview of ankylosing spondylitis The concept and classification of spondyloarthritis The term spondyloarthritis (SpA) comprises AS, reactive arthritis, arthritis/spondylitis associated with
The evidence for whole-spine MRI in the assessment of axial spondyloarthropathy
 RHEUMATOLOGY Rheumatology 2010;49:426 432 doi:10.1093/rheumatology/kep427 Advance Access publication 11 January 2010 Review The evidence for whole-spine MRI in the assessment of axial spondyloarthropathy
RHEUMATOLOGY Rheumatology 2010;49:426 432 doi:10.1093/rheumatology/kep427 Advance Access publication 11 January 2010 Review The evidence for whole-spine MRI in the assessment of axial spondyloarthropathy
Seronegative spondyloarthropathies : A Pictorial Review
 Seronegative spondyloarthropathies : A Pictorial Review Poster No.: P-0008 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1
Seronegative spondyloarthropathies : A Pictorial Review Poster No.: P-0008 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1
Spondylarthropathies. Outline. Introduction. Spondylarthropathy other than AS. Mimickers of spondylarthropathy. Conclusions.
 Spondylarthropathies Filip M. Vanhoenacker Johan Van Goethem General Hospital St-Maarten Duffel-Mechelen Universities of Antwerp and Ghent Outline Introduction Spondylarthropathy other than AS Mimickers
Spondylarthropathies Filip M. Vanhoenacker Johan Van Goethem General Hospital St-Maarten Duffel-Mechelen Universities of Antwerp and Ghent Outline Introduction Spondylarthropathy other than AS Mimickers
Axial Spondyloarthritis: Issues & Controversies
 Axial Spondyloarthritis: Issues & Controversies Atul Deodhar, MD Professor of Medicine Oregon Health & Science University Portland, OR WRA 2018 Annual Meeting, Leavenworth, WA. 16 th September, 2018 Disclosures:
Axial Spondyloarthritis: Issues & Controversies Atul Deodhar, MD Professor of Medicine Oregon Health & Science University Portland, OR WRA 2018 Annual Meeting, Leavenworth, WA. 16 th September, 2018 Disclosures:
3 Sternoclavicular Joints
 3 Sternoclavicular Joints Anne Grethe Jurik and Flemming Brandt Soerensen 29 Contents 3.1 Introduction.......................................................... 29 3.2 Macroscopic Anatomy.................................................
3 Sternoclavicular Joints Anne Grethe Jurik and Flemming Brandt Soerensen 29 Contents 3.1 Introduction.......................................................... 29 3.2 Macroscopic Anatomy.................................................
COMPUTED TOMOGRAPHY IN THE DIAGNOSIS OF SACROILIITIS
 1479 COMPUTED TOMOGRPHY IN THE DIGNOSIS OF SCROILIITIS FRNKLIN KOZIN, GUILLERMO F. CRRER, LWRENCE M. RYN, DENIS FOLEY, and THOMS LWSON Computed tomography (CT) and conventional radiography of the sacroiliac
1479 COMPUTED TOMOGRPHY IN THE DIGNOSIS OF SCROILIITIS FRNKLIN KOZIN, GUILLERMO F. CRRER, LWRENCE M. RYN, DENIS FOLEY, and THOMS LWSON Computed tomography (CT) and conventional radiography of the sacroiliac
Axial Spondyloarthritis. Doug White, Rheumatologist Waikato Hospital
 Axial Spondyloarthritis Doug White, Rheumatologist Waikato Hospital Disclosures Presentations / Consulting Abbott Laboratories AbbVie MSD Novartis Roche Clinical Trials Abbott Laboratories AbbVie Actelion
Axial Spondyloarthritis Doug White, Rheumatologist Waikato Hospital Disclosures Presentations / Consulting Abbott Laboratories AbbVie MSD Novartis Roche Clinical Trials Abbott Laboratories AbbVie Actelion
symphysis in rheumatic disorders
 Annals of Rheumatic Diseases, 1979, 38, 529-534 A comparative radiological study of the pubic symphysis in rheumatic disorders D. L. SCOTT, C. J. EASTMOND, AND V. WRIGHT From the Rheumatism Research Unit,
Annals of Rheumatic Diseases, 1979, 38, 529-534 A comparative radiological study of the pubic symphysis in rheumatic disorders D. L. SCOTT, C. J. EASTMOND, AND V. WRIGHT From the Rheumatism Research Unit,
UPDATE ON MRI OF SPONDYLOARTHRITIS. PART ONE: THE SACRO-ILIAC JOINT
 JR TR, 2014, 97: 222-227. UPDTE ON MRI OF SPONDYLORTHRITIS. PRT ONE: THE SCRO-ILIC JOINT.C. Vande erg, P. Omoumi,. Larbi, F. Lecouvet, J. Malghem 1 In recent years, there has been an increased trend toward
JR TR, 2014, 97: 222-227. UPDTE ON MRI OF SPONDYLORTHRITIS. PRT ONE: THE SCRO-ILIC JOINT.C. Vande erg, P. Omoumi,. Larbi, F. Lecouvet, J. Malghem 1 In recent years, there has been an increased trend toward
Active (acute) inflammation on MRI highly suggestive of sacroiliitis associated with SpA
 MRI findings of active and chronic sacroiliitis in light of recent ASAS criteria for diagnosing axial spondyloarthritis: what the radiologist should know Poster No.: C-1955 Congress: ECR 2012 Type: Educational
MRI findings of active and chronic sacroiliitis in light of recent ASAS criteria for diagnosing axial spondyloarthritis: what the radiologist should know Poster No.: C-1955 Congress: ECR 2012 Type: Educational
Sacroiliac joints MR: Finally a universal language for the sacroiliitis diagnosis
 Sacroiliac joints MR: Finally a universal language for the sacroiliitis diagnosis Poster No.: C-1836 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. E. Banegas Illescas, C. López Menéndez, M. L.
Sacroiliac joints MR: Finally a universal language for the sacroiliitis diagnosis Poster No.: C-1836 Congress: ECR 2013 Type: Scientific Exhibit Authors: M. E. Banegas Illescas, C. López Menéndez, M. L.
Ankylosing spondylitis: A Pictorial Review
 Ankylosing spondylitis: A Pictorial Review Poster No.: P-0009 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1 2 Hernandez Muñiz,
Ankylosing spondylitis: A Pictorial Review Poster No.: P-0009 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1 2 Hernandez Muñiz,
Concept of Spondyloarthritis (SpA)
 Concept of Spondyloarthritis (SpA) Spondyloarthritis: Characteristic Parameters Used for Diagnosis I Symptoms Inflammatory back pain Imaging Lab ESR/CRP Patient s history Good response to NSAIDs Spondyloarthritis-Characteristic
Concept of Spondyloarthritis (SpA) Spondyloarthritis: Characteristic Parameters Used for Diagnosis I Symptoms Inflammatory back pain Imaging Lab ESR/CRP Patient s history Good response to NSAIDs Spondyloarthritis-Characteristic
Spiral Ct with Three-Dimensional and Multiplanar Reconstruction in the Diagnosis of Anterior Chest Wall Joint and Bone Disorders
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Spiral Ct with Three-Dimensional and Multiplanar Reconstruction in the Diagnosis of
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Spiral Ct with Three-Dimensional and Multiplanar Reconstruction in the Diagnosis of
C. Imaging the spine in arthritis
 C. Imaging the spine in arthritis Poster No.: A-173 Congress: ECR 2010 Type: Invited Speaker Topic: Musculoskeletal - Without Subtopic Authors: A. G. Jurik; Århus C/DK Keywords: arthritis, spondyloarthritis,
C. Imaging the spine in arthritis Poster No.: A-173 Congress: ECR 2010 Type: Invited Speaker Topic: Musculoskeletal - Without Subtopic Authors: A. G. Jurik; Århus C/DK Keywords: arthritis, spondyloarthritis,
Magnetic resonance imaging in ankylosing spondylitis
 REVIEW Magnetic resonance imaging in ankylosing spondylitis Xenofon Baraliakos, Robert Landewé & Juergen Braun Author for correspondence Ruhr-University, Rheumazentrum Ruhrgebiet Herne, Bochum, Germany
REVIEW Magnetic resonance imaging in ankylosing spondylitis Xenofon Baraliakos, Robert Landewé & Juergen Braun Author for correspondence Ruhr-University, Rheumazentrum Ruhrgebiet Herne, Bochum, Germany
Introduction. Natural Progression of AS. Sacroiliac Joint. Clinical Features and Assessment of Ankylosing Spondylitis
 Clinical Features and Assessment of Ankylosing Spondylitis Dr. YIM, Cheuk Wan Specialist in Rheumatology United Christian Hospital Introduction Ankylo=fusion Spondylitis=inflammation of spine Affect 0.1-0.5%
Clinical Features and Assessment of Ankylosing Spondylitis Dr. YIM, Cheuk Wan Specialist in Rheumatology United Christian Hospital Introduction Ankylo=fusion Spondylitis=inflammation of spine Affect 0.1-0.5%
2004 Health Press Ltd.
 ... Ankylosing spondylitis Maxime Dougados MD Professor of Rheumatology Hôpital Cochin René Descartes University Paris, France Désirée van der Heijde MD PhD Professor of Rheumatology University Hospital
... Ankylosing spondylitis Maxime Dougados MD Professor of Rheumatology Hôpital Cochin René Descartes University Paris, France Désirée van der Heijde MD PhD Professor of Rheumatology University Hospital
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29572 holds various files of this Leiden University dissertation. Author: Berg, Rosaline van den Title: Spondyloarthritis : recognition, imaging, treatment
Cover Page The handle http://hdl.handle.net/1887/29572 holds various files of this Leiden University dissertation. Author: Berg, Rosaline van den Title: Spondyloarthritis : recognition, imaging, treatment
of the lumbar facet joints there
 Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Secukinumab for treating ankylosing spondylitis after inadequate response to non-steroidal anti-inflammatory drugs
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Secukinumab for treating ankylosing spondylitis after inadequate response to non-steroidal anti-inflammatory drugs
Demonstration of evolution of hemispherical spondysclerosis by contrast enhanced Gd-DTPA magnetic resonance imaging
 Demonstration of evolution of hemispherical spondysclerosis by contrast enhanced Gd-DTPA magnetic resonance imaging Vladimir Jevtič 1, Natalija Majcen 2 1 Clinical Radiology Institute, University Clinical
Demonstration of evolution of hemispherical spondysclerosis by contrast enhanced Gd-DTPA magnetic resonance imaging Vladimir Jevtič 1, Natalija Majcen 2 1 Clinical Radiology Institute, University Clinical
A mong the inflammatory rheumatic diseases
 659 REVIEW Early referral recommendations for ankylosing spondylitis (including pre-radiographic and radiographic forms) in primary care J Sieper, M Rudwaleit... An earlier diagnosis of ankylosing spondylitis
659 REVIEW Early referral recommendations for ankylosing spondylitis (including pre-radiographic and radiographic forms) in primary care J Sieper, M Rudwaleit... An earlier diagnosis of ankylosing spondylitis
The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint
 i23 The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint B Ejbjerg, F McQueen, M Lassere, E Haavardsholm, P Conaghan, P O Connor, P Bird, C Peterfy, J Edmonds, M Szkudlarek,
i23 The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint B Ejbjerg, F McQueen, M Lassere, E Haavardsholm, P Conaghan, P O Connor, P Bird, C Peterfy, J Edmonds, M Szkudlarek,
Properties of Purdue. Anatomy. Positioning AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS 11/30/2018
 AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis
 CASE ORIGINAL REPORT ARTICLE MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis D J Kotzé, MB ChB L J Erasmus, MB ChB Department of Diagnostic Radiology, University of the Free State, Bloemfontein
CASE ORIGINAL REPORT ARTICLE MRI findings in proven Mycobacterium tuberculosis (TB) spondylitis D J Kotzé, MB ChB L J Erasmus, MB ChB Department of Diagnostic Radiology, University of the Free State, Bloemfontein
Clinical and Imaging Efficacy of Infliximab in HLA B27 Positive Patients With Magnetic Resonance Imaging Determined Early Sacroiliitis
 ARTHRITIS & RHEUMATISM Vol. 60, No. 4, April 2009, pp 946 954 DOI 10.1002/art.24408 2009, American College of Rheumatology Clinical and Imaging Efficacy of Infliximab in HLA B27 Positive Patients With
ARTHRITIS & RHEUMATISM Vol. 60, No. 4, April 2009, pp 946 954 DOI 10.1002/art.24408 2009, American College of Rheumatology Clinical and Imaging Efficacy of Infliximab in HLA B27 Positive Patients With
Sronegative Spondyloarthropathies. Dr. M Jokar
 Sronegative Spondyloarthropathies Dr. M Jokar 1 Definition The spondyloarthropathies are a group of disorders that share certain clinical features and an association with the HLA-B27 allele 2 Spondyloarthropathies
Sronegative Spondyloarthropathies Dr. M Jokar 1 Definition The spondyloarthropathies are a group of disorders that share certain clinical features and an association with the HLA-B27 allele 2 Spondyloarthropathies
A nkylosing spondylitis (AS) is a common chronic
 1046 EXTENDED REPORT Analysing chronic spinal changes in ankylosing spondylitis: a systematic comparison of conventional x rays with magnetic resonance imaging using established and new scoring systems
1046 EXTENDED REPORT Analysing chronic spinal changes in ankylosing spondylitis: a systematic comparison of conventional x rays with magnetic resonance imaging using established and new scoring systems
Seronegative Spondyloarthropathies: A Radiological Persepctive
 Seronegative Spondyloarthropathies: A Radiological Persepctive Poster No.: C-1816 Congress: ECR 2016 Type: Educational Exhibit Authors: K. Shindi, H. Nejadhamzeeigilani, P. Nagtode, C. Nel ; 1 1 2 2 3
Seronegative Spondyloarthropathies: A Radiological Persepctive Poster No.: C-1816 Congress: ECR 2016 Type: Educational Exhibit Authors: K. Shindi, H. Nejadhamzeeigilani, P. Nagtode, C. Nel ; 1 1 2 2 3
Magnetic resonance imaging of femoral head development in roentgenographically normal patients
 Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Introduction SCIENTIFIC ARTICLE
 Skeletal Radiol (2017) 46:633 639 DOI 10.1007/s00256-017-2581-1 SCIENTIFIC ARTICLE Prevalence and clinical significance of lumbosacral transitional vertebra (LSTV) in a young back pain population with
Skeletal Radiol (2017) 46:633 639 DOI 10.1007/s00256-017-2581-1 SCIENTIFIC ARTICLE Prevalence and clinical significance of lumbosacral transitional vertebra (LSTV) in a young back pain population with
ABSTRACT Objective: To validate and refine two sets of candidate criteria for the classification/diagnosis of axial spondyloarthritis
 1 Rheumatology, Med Klinik I, Charité, Campus Benjamin Franklin, Berlin, Germany; 2 Leiden University Medical Center, Leiden, The Netherlands; 3 Maastricht University Medical Center, Maastricht, The Netherlands;
1 Rheumatology, Med Klinik I, Charité, Campus Benjamin Franklin, Berlin, Germany; 2 Leiden University Medical Center, Leiden, The Netherlands; 3 Maastricht University Medical Center, Maastricht, The Netherlands;
Is intra-articular gas within the SI Joints a confounding factor in the false negative diagnosis of sacroiliitis?
 Is intra-articular gas within the SI Joints a confounding factor in the false negative diagnosis of sacroiliitis? Dr. Omar Azmat*, Dr. Zaid Jibri, Dr. Vimarsha Swami, Dr. Babak Maghdoori, Dr. Kent Greep,
Is intra-articular gas within the SI Joints a confounding factor in the false negative diagnosis of sacroiliitis? Dr. Omar Azmat*, Dr. Zaid Jibri, Dr. Vimarsha Swami, Dr. Babak Maghdoori, Dr. Kent Greep,
Imaging of axial spondyloarthritis including ankylosing spondylitis
 Imaging of axial spondyloarthritis including ankylosing spondylitis ACR 2012 Prof. Dr. med. J. Braun Rheumazentrum Ruhrgebiet, Herne Ruhr-Universität Bochum Germany Modified New York Criteria 1984 for
Imaging of axial spondyloarthritis including ankylosing spondylitis ACR 2012 Prof. Dr. med. J. Braun Rheumazentrum Ruhrgebiet, Herne Ruhr-Universität Bochum Germany Modified New York Criteria 1984 for
8/29/2012. Outline Juvenile idiopathic arthritis. 1. Classification-ILAR. 1. Classification-clinical diagnosis. 1. JIA classification
 Outline Juvenile idiopathic arthritis 1. Classification and symptoms (ILAR-International league of Associations for Rheumatology) 2. Imaging J. Herman Kan, M.D. Section chief, musculoskeletal imaging Edward
Outline Juvenile idiopathic arthritis 1. Classification and symptoms (ILAR-International league of Associations for Rheumatology) 2. Imaging J. Herman Kan, M.D. Section chief, musculoskeletal imaging Edward
Dr Tracey Kain. Associate Professor Ed Gane
 Associate Professor Ed Gane New Zealand Liver Transplant Unit Auckland Dr Tracey Kain Consultant Rheumatologist Grace Orthopaedic Centre Tauranga Hospital Tauranga 7:00-7:55 Abbvie Breakfast Session 1.
Associate Professor Ed Gane New Zealand Liver Transplant Unit Auckland Dr Tracey Kain Consultant Rheumatologist Grace Orthopaedic Centre Tauranga Hospital Tauranga 7:00-7:55 Abbvie Breakfast Session 1.
Magnetic Resonance Imaging of Inflammatory Lesions in the Spine in Ankylosing Spondylitis Clinical Trials: Is Paramagnetic Contrast Medium Necessary?
 Magnetic Resonance Imaging of Inflammatory Lesions in the Spine in Ankylosing Spondylitis Clinical Trials: Is Paramagnetic Contrast Medium Necessary? KAY-GEERT A. HERMANN, ROBERT B.M. LANDEWÉ, JÜRGEN BRAUN,
Magnetic Resonance Imaging of Inflammatory Lesions in the Spine in Ankylosing Spondylitis Clinical Trials: Is Paramagnetic Contrast Medium Necessary? KAY-GEERT A. HERMANN, ROBERT B.M. LANDEWÉ, JÜRGEN BRAUN,
Unilateral Sacroiliitis: Differential Diagnosis Between Infectious Sacroiliitis and Spondyloarthritis Based on MRI Findings
 Musculoskeletal Imaging Original Research Kang et al. Use of MRI to Differentiate Infectious Sacroiliitis From Spondyloarthritis Musculoskeletal Imaging Original Research Yusuhn Kang 1 Sung Hwan Hong Ji
Musculoskeletal Imaging Original Research Kang et al. Use of MRI to Differentiate Infectious Sacroiliitis From Spondyloarthritis Musculoskeletal Imaging Original Research Yusuhn Kang 1 Sung Hwan Hong Ji
LUMBOSACRAL RADIOGRAPHIC SIGNS IN PATIENTS WITH PREVIOUS ENTERO- OR UROARTHRITIS
 ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.027086 LUMBOSACRAL RADIOGRAPHIC SIGNS IN PATIENTS WITH PREVIOUS ENTERO- OR UROARTHRITIS (extended report) Antti Mannoja, Johanna Pekkola,
ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.027086 LUMBOSACRAL RADIOGRAPHIC SIGNS IN PATIENTS WITH PREVIOUS ENTERO- OR UROARTHRITIS (extended report) Antti Mannoja, Johanna Pekkola,
COMPUTED TOMOGRAPHY IN THE DIAGNOSIS OF EARLY ANKYLOSING SPONDYLIT-IS
 COMPUTED TOMOGRAPHY IN THE DIAGNOSIS OF EARLY ANKYLOSING SPONDYLITIS ADEL G. FAM, JOEL D. RUBENSTEIN, HYACINTH CHINSANG, and FRANCES Y. K. LEUNG Computed tomography (CT) was compared with plain radiography
COMPUTED TOMOGRAPHY IN THE DIAGNOSIS OF EARLY ANKYLOSING SPONDYLITIS ADEL G. FAM, JOEL D. RUBENSTEIN, HYACINTH CHINSANG, and FRANCES Y. K. LEUNG Computed tomography (CT) was compared with plain radiography
New developments in the diagnosis and treatment of axial spondyloarthritis
 Review: Clinical Trial Outcomes New developments in the diagnosis and treatment of axial spondyloarthritis Clin. Invest. (2013) 3(2), 153 171 Spondyloarthritis (SpA) is an umbrella term for a group of
Review: Clinical Trial Outcomes New developments in the diagnosis and treatment of axial spondyloarthritis Clin. Invest. (2013) 3(2), 153 171 Spondyloarthritis (SpA) is an umbrella term for a group of
Case reports CASE 1. A 67-year-old white man had back pain since the age. our clinic several years later with progressive symptoms.
 Annals of the Rheumatic Diseases, 1982, 41, 574-578 Late-onset peripheral joint disease in ankylosing spondylitis MARC D. COHEN AND WILLIAM W. GINSBURG From the Division ofrheumatology and Internal Medicine,
Annals of the Rheumatic Diseases, 1982, 41, 574-578 Late-onset peripheral joint disease in ankylosing spondylitis MARC D. COHEN AND WILLIAM W. GINSBURG From the Division ofrheumatology and Internal Medicine,
Gender differences in effectiveness of treatment in rheumatic diseases
 Gender differences in effectiveness of treatment in rheumatic diseases Irene van der Horst-Bruinsma Associate Professor Rheumatology Center of Excellence of Axial Spondyloarthritis ARC/VU University Medical
Gender differences in effectiveness of treatment in rheumatic diseases Irene van der Horst-Bruinsma Associate Professor Rheumatology Center of Excellence of Axial Spondyloarthritis ARC/VU University Medical
Disease Characteristics of Filipino Ankylosing Spondylitis Patients in Metro Manila Rheumatology Clinics
 Philippine Journal of Internal Medicine Original Paper Disease Characteristics of Filipino Ankylosing Spondylitis Patients in Metro Manila Rheumatology Clinics Ma. Lucila Dianongco, M.D.*; Marc Gregory
Philippine Journal of Internal Medicine Original Paper Disease Characteristics of Filipino Ankylosing Spondylitis Patients in Metro Manila Rheumatology Clinics Ma. Lucila Dianongco, M.D.*; Marc Gregory
Do HLA-B27 positive patients differ from HLA-B27 negative patients in clinical presentation
 Do HLA-B27 positive patients differ from HLA-B27 negative patients in clinical presentation and imaging? Results from the DESIR cohort of patients with recent onset axial spondyloarthritis Ho Yin Chung
Do HLA-B27 positive patients differ from HLA-B27 negative patients in clinical presentation and imaging? Results from the DESIR cohort of patients with recent onset axial spondyloarthritis Ho Yin Chung
Arthrographic study of the rheumatoid knee.
 Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
Annals of the Rheumatic Diseases, 1981, 40, 344-349 Arthrographic study of the rheumatoid knee. Part 2. Articular cartilage and menisci KYOSUKE FUJIKAWA, YOSHINORI TANAKA, TSUNEYO MATSUBAYASHI, AND FUJIO
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
National Imaging Associates, Inc. Clinical guidelines BONE MARROW MRI Original Date: July 2008 Page 1 of 5 CPT Codes: 77084 Last Review Date: September 2014 NCD 220.2 MRI Last Effective Date: July 2011
HYPEROSTOSIS AND OSSIFICATION IN THE CERVICAL SPINE
 564 RADIOLOGIC VIGNETTE HYPEROSTOSIS AND OSSIFICATION IN THE CERVICAL SPINE DONALD RESNICK A variety of diseases can produce hyperostosis or ossification in the cervical spine. Included among these are
564 RADIOLOGIC VIGNETTE HYPEROSTOSIS AND OSSIFICATION IN THE CERVICAL SPINE DONALD RESNICK A variety of diseases can produce hyperostosis or ossification in the cervical spine. Included among these are
Spine MRI in SpA What is the rheumatologist interested in? Personal use only
 Spine MRI in SpA What is the rheumatologist interested in? 4th Musculoskeletal MRI Meeting 2017: Spine MRI Ospedale Regionale di Lugano May 6th 2017 Ulrich Weber MD Consultant, King Christian 10th Hospital,
Spine MRI in SpA What is the rheumatologist interested in? 4th Musculoskeletal MRI Meeting 2017: Spine MRI Ospedale Regionale di Lugano May 6th 2017 Ulrich Weber MD Consultant, King Christian 10th Hospital,
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
MAGNETIC RESONANCE IMAGING OF SACROILIAC JOINT INFLAMMATION
 1763 MGNETI RESONNE IMGING OF SROILI JOINT INFLMMTION H. HLSTROM, N. FELTELIUS, R. NYMN, and R. HLLGREN consecutive series of 27 patients with symptoms compatible with sacroiliitis underwent magnetic resonance
1763 MGNETI RESONNE IMGING OF SROILI JOINT INFLMMTION H. HLSTROM, N. FELTELIUS, R. NYMN, and R. HLLGREN consecutive series of 27 patients with symptoms compatible with sacroiliitis underwent magnetic resonance
COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP)
 European Medicines Agency Pre-Authorisation Evaluation of Medicines for Human Use London, 23 April 2009 Doc. Ref. CPMP/EWP/4891/03 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL
European Medicines Agency Pre-Authorisation Evaluation of Medicines for Human Use London, 23 April 2009 Doc. Ref. CPMP/EWP/4891/03 COMMITTEE FOR MEDICINAL PRODUCTS FOR HUMAN USE (CHMP) GUIDELINE ON CLINICAL
Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA)
 www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
www.printo.it/pediatric-rheumatology/gb/intro Juvenile Spondyloarthritis / Enthesitis Related Arthritis (SpA-ERA) Version of 2016 1. WHAT IS JUVENILE SPONDYLOARTHRITIS/ENTHESITIS- RELATED ARTHRITIS (SpA-ERA)
Rheumatoid Arthritis. Rheumatoid Arthritis. RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling. Rheumatic Diseases
 RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Rheumatic Diseases The prevalence of rheumatoid arthritis in most Caucasian populations approaches 1% among adults 18 and over and
RCS 6080 Medical and Psychosocial Aspects of Rehabilitation Counseling Rheumatic Diseases The prevalence of rheumatoid arthritis in most Caucasian populations approaches 1% among adults 18 and over and
C hronic low back pain (LBP) is a common problem in
 535 EXTENDED REPORT How to diagnose axial spondyloarthritis early M Rudwaleit, D van der Heijde, M A Khan, J Braun, J Sieper... Ann Rheum Dis 2004;63:535 543. doi: 10.1136/ard.2003.011247 See end of article
535 EXTENDED REPORT How to diagnose axial spondyloarthritis early M Rudwaleit, D van der Heijde, M A Khan, J Braun, J Sieper... Ann Rheum Dis 2004;63:535 543. doi: 10.1136/ard.2003.011247 See end of article
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/43590 holds various files of this Leiden University dissertation Author: Machado, Pedro Title: Health and imaging outcomes in axial spondyloarthritis Issue
Cover Page The handle http://hdl.handle.net/1887/43590 holds various files of this Leiden University dissertation Author: Machado, Pedro Title: Health and imaging outcomes in axial spondyloarthritis Issue
A Patient s Guide to Spondyloarthropathies
 A Patient s Guide to Spondyloarthropathies 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Spondyloarthropathies 763 Larkfield Road 2nd Floor Commack, NY 11725 Phone: (631) 462-2225 Fax: (631) 462-2240 DISCLAIMER: The information in this booklet is compiled from a variety
MUSCULOSKELETAL RADIOLOGY
 MUSCULOSKELETAL RADOLOGY SECTON www.cambridge.org Achilles tendonopathy/rupture Characteristics Describes pathology of the combined tendon of the gastro-soleus complex, which inserts onto the calcaneum.
MUSCULOSKELETAL RADOLOGY SECTON www.cambridge.org Achilles tendonopathy/rupture Characteristics Describes pathology of the combined tendon of the gastro-soleus complex, which inserts onto the calcaneum.
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R
 The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
Evaluation of MRI diffusion in spondylarthropathy axial skeleton lesions
 Evaluation of MRI diffusion in spondylarthropathy axial skeleton lesions Poster No.: C-2353 Congress: ECR 2012 Type: Scientific Paper Authors: B. Dallaudiere, R. Dautry, A. Felter, J. LINCOT, P. Koch,
Evaluation of MRI diffusion in spondylarthropathy axial skeleton lesions Poster No.: C-2353 Congress: ECR 2012 Type: Scientific Paper Authors: B. Dallaudiere, R. Dautry, A. Felter, J. LINCOT, P. Koch,
Identification of Psoriatic Arthritis and Ankylosing Spondylitis Early Detection to Facilitate Appropriate Care
 Identification of Psoriatic Arthritis and Ankylosing Spondylitis Early Detection to Facilitate Appropriate Care Joy Schechtman D.O. Professor Midwestern University 64C-1876207 Disclosures None 3 64C-1876207
Identification of Psoriatic Arthritis and Ankylosing Spondylitis Early Detection to Facilitate Appropriate Care Joy Schechtman D.O. Professor Midwestern University 64C-1876207 Disclosures None 3 64C-1876207
Magnetic resonance imaging of sacroiliitis in children: frequency of findings and interobserver reliability
 Pediatric Radiology (2018) 48:1621 1628 https://doi.org/10.1007/s00247-018-4185-x ORIGINAL ARTICLE Magnetic resonance imaging of sacroiliitis in children: frequency of findings and interobserver reliability
Pediatric Radiology (2018) 48:1621 1628 https://doi.org/10.1007/s00247-018-4185-x ORIGINAL ARTICLE Magnetic resonance imaging of sacroiliitis in children: frequency of findings and interobserver reliability
Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients
 Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Original Article J Nepal Health Res Counc 2015 Sep - Dec;13(31):196-200 Magnetic Resonance Imaging Findings in Degenerative Disc Disease of Cervical Spine in Symptomatic Patients Karki DB, 1 Gurung G,
Manifestations of Cervical Spine Involvement in Longstanding Ankylosing Spondylitis: Atlantoaxial Ankylosis and Atlantoaxial Subluxation
 Journal of Rheumatic Diseases Vol. 24, No. 1, February, 2017 https://doi.org/10.4078/jrd.2017.24.1.21 Original Article Manifestations of Cervical Spine Involvement in Longstanding Ankylosing Spondylitis:
Journal of Rheumatic Diseases Vol. 24, No. 1, February, 2017 https://doi.org/10.4078/jrd.2017.24.1.21 Original Article Manifestations of Cervical Spine Involvement in Longstanding Ankylosing Spondylitis:
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
SCIENTIFIC DISCUSSION
 European Medicines Agency London, 20 September 2007 Product name: Remicade Procedure number: EMEA/H/C/240/II/95 SCIENTIFIC DISCUSSION 7 Westferry Circus, Canary Wharf, London, E14 4HB, UK Tel. (44-20)
European Medicines Agency London, 20 September 2007 Product name: Remicade Procedure number: EMEA/H/C/240/II/95 SCIENTIFIC DISCUSSION 7 Westferry Circus, Canary Wharf, London, E14 4HB, UK Tel. (44-20)
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Rheumatology. Ankylosing Spondylitis (Bechterew s Disease) Symptoms and Classifications. Definition of Ankylosing Spondylitis. Spondyloarthropathies
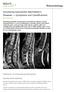 Rheumatology Ankylosing Spondylitis (Bechterew s Disease) Symptoms and Classifications See online here Ankylosing spondylitis, formerly known as Bechterew s disease or Marie- Strümpell disease, is a type
Rheumatology Ankylosing Spondylitis (Bechterew s Disease) Symptoms and Classifications See online here Ankylosing spondylitis, formerly known as Bechterew s disease or Marie- Strümpell disease, is a type
ISPUB.COM. Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay. P Chudgar INTRODUCTION SPINE
 ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay P Chudgar Citation P Chudgar.. The Internet Journal of Radiology.
ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 Spectrum Of MRI Findings In Musculoskeletal Tuberculosis: Pictoral Essay P Chudgar Citation P Chudgar.. The Internet Journal of Radiology.
강직성척추염환자에서대동맥박리를동반한마르팡증후군 1 예
 대한내과학회지 : 제 84 권제 6 호 2013 Http://Dx.Doi.Org/10.3904/Kjm.2013.84.6.873 강직성척추염환자에서대동맥박리를동반한마르팡증후군 1 예 을지대학교의과대학내과학교실 류지원 박지영 송은주 허진욱 A Case of Aortic Dissection with Marfan Syndrome and Ankylosing Spondylitis
대한내과학회지 : 제 84 권제 6 호 2013 Http://Dx.Doi.Org/10.3904/Kjm.2013.84.6.873 강직성척추염환자에서대동맥박리를동반한마르팡증후군 1 예 을지대학교의과대학내과학교실 류지원 박지영 송은주 허진욱 A Case of Aortic Dissection with Marfan Syndrome and Ankylosing Spondylitis
ACR Appropriateness Criteria Chronic Back Pain Suspected Sacroiliitis Spondyloarthropathy EVIDENCE TABLE
 1. Underwood MR, Dawes P. Inflammatory back pain in primary care. Br J Rheumatol. 1995;(11):107-1077.. Sieper J, van der Heijde D, Landewe R, et al. New criteria for inflammatory back pain in patients
1. Underwood MR, Dawes P. Inflammatory back pain in primary care. Br J Rheumatol. 1995;(11):107-1077.. Sieper J, van der Heijde D, Landewe R, et al. New criteria for inflammatory back pain in patients
OSTEOPHYTOSIS OF THE FEMORAL HEAD AND NECK
 908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
Discovertebral (Andersson) lesions in severe ankylosing spondylitis: a study using MRI and conventional radiography
 Clin Rheumatol (2010) 29:1433 1438 DOI 10.1007/s10067-010-1480-9 ORIGINAL ARTICLE Discovertebral (Andersson) lesions in severe ankylosing spondylitis: a study using MRI and conventional radiography Mirjam
Clin Rheumatol (2010) 29:1433 1438 DOI 10.1007/s10067-010-1480-9 ORIGINAL ARTICLE Discovertebral (Andersson) lesions in severe ankylosing spondylitis: a study using MRI and conventional radiography Mirjam
Revised Dec Spine MR Protocols
 Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page
 The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page 2294-2300 Role of Magnetic Resonance Imaging and Ultrasonography in Diagnosis and Follow Up Rheumatoid Arthritis in Hand and Wrist
The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page 2294-2300 Role of Magnetic Resonance Imaging and Ultrasonography in Diagnosis and Follow Up Rheumatoid Arthritis in Hand and Wrist
Sacroiliac joint infection
 Case Report Brunei Int Med J. 2015; 11 (2): 110-114 Sacroiliac joint infection Jon CHUA 1, Kamal JAMIL 1, Kamalnizat IBRAHIM 1, Suraya AZIZ 2 1 Department of Orthopaedic and Traumatology, Faculty of Medicine,
Case Report Brunei Int Med J. 2015; 11 (2): 110-114 Sacroiliac joint infection Jon CHUA 1, Kamal JAMIL 1, Kamalnizat IBRAHIM 1, Suraya AZIZ 2 1 Department of Orthopaedic and Traumatology, Faculty of Medicine,
PROFFESOR THAMER AHMED HAMDAN M.B.CH.B, F.R.C.S(ED), F.R.C.P(ED), F.A.C.S,F.I.C.S CHANCELLOR OF BASRA UNIVERSITY SICOT VICE PRESEDENT
 PROFFESOR THAMER AHMED HAMDAN M.B.CH.B, F.R.C.S(ED), F.R.C.P(ED), F.A.C.S,F.I.C.S CHANCELLOR OF BASRA UNIVERSITY SICOT VICE PRESEDENT DR.RAFID A. ALADAB M.B.CH.B,F.I.C.M.S(ORTHO),SICOT DIPLOMA ORTHOPEDIC
PROFFESOR THAMER AHMED HAMDAN M.B.CH.B, F.R.C.S(ED), F.R.C.P(ED), F.A.C.S,F.I.C.S CHANCELLOR OF BASRA UNIVERSITY SICOT VICE PRESEDENT DR.RAFID A. ALADAB M.B.CH.B,F.I.C.M.S(ORTHO),SICOT DIPLOMA ORTHOPEDIC
The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients
 Bahrain Medical Bulletin, Vol.27, No. 3, September 2005 The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients Jane Kawar, MD* Hisham Al-Sayegh, MD* Objective: To assess
Bahrain Medical Bulletin, Vol.27, No. 3, September 2005 The Relationship Between Clinical Activity And Function In Ankylosing Spondylitis Patients Jane Kawar, MD* Hisham Al-Sayegh, MD* Objective: To assess
