Approaches To Midfoot Degenerative Joint Disease
|
|
|
- Abigayle Norton
- 6 years ago
- Views:
Transcription
1 CHAPTER I O Approaches To Midfoot Degenerative Joint Disease Stepben J. Miller, DPM. INTRODUCTION The joints of the midfoot are susceptible to degenerative changes as a resuit of a variety of forces, including biomechanical faults, frank trauma, and Charcot neuropathy. Such degeneration may be accelerated by concurrent osteoarthritis, or compensation for a functional foot deformity such as equinus. Diagnosis can be elusive until radiographic changes ate evident. Conservative treatment is effective only while symptoms are tolerable, while surgical intervention becomes the treatment of choice in order to achieve pain free function. ANATOMICAL CONSIDERATIONS The joints of the midfoot include LisFranc's (tarsometatarsal) joint, Chopart's (midtarsal) joint, and the joints in between. Because of its unique function (which is more in tandem with the subtalar joint), the midtarsal joint will not be addressed in this paper. The tarsometatarsal loints consist of the first, second, and third metatarsocuneiform joints, as well as the fourth and fifth metatarsocuboid joints. This is an intricate nefwork of articulations which make up the transverse arch of the foot, where the keystone is the second metatarsal and cuneiform. The transverse arch is connected by dorsal, plantar, and interosseus ligaments which bond all metatarsal-cuneiform/cuboid articulations except for the first and second metatarsal bases. Although the bases of these two metatarsals have no ligamentous attachment between them, the second metatarsal is stabilized by an extremely strong ligament from the medial cuneiform bone (LisFranc's ligament). The intertarsal joints consist of the first, second, and third naviculocuneiform articulations, as well as the adjacent interfaces between the first and second cuneiform bones, the second and third cuneiform bones, and the third cuneiform-cuboid bones. Motion is limited to each rzy as well as adjacent afticulations. The shapes of the joints allow only limited motion, making them pafiicularly susceptible to jamming injuries, which are exaggerated in the Charcot foot. The midfoot is the interface between the rearfoot function (subtalar and midtarsal joints) and forefoot function (metatarsais and digits). In addition, there is a limited amount of inteftarsal motion. PATTIOPHYSIOLOGY Midfoot degenerative joint disease is the product of trauma, biomechanical abnormalities, or neuropathy (Figs. 1A, 1B). Trauma can include blunt or crush injuries, contusions, or high veloci$z impact. Tarsometatarsal joint dislocations or fracitre/dislocations can be devastating injuries which rapidly progress to degenerative joint disease. Injury to this group of afiiculations can also involve other midfoot bones and joints, as well as the base of the metatarsals (particularly the second). \fith luauma, there is direct afiicular damage which causes significant joint degeneration over time. Underlfng biomechanical deformrties can fufiher accelerate afihrosis. Figure 1A. A 67 year-old female with non-traumatic degeneration of the tarsometatarsal joint.
2 42 CHAPTER 10 Figure 18. Note the point of sagittal plane collapse on the latency racliograph. Figure 2A. Lesser tarsus joint destruction aggravated by an equinus deformity. Note the point of compensation at the talonavicular 1oint. The most common biomechanical deformity that can cause midfoot jamming is pronation. Once the subtalar joint pronates and unlocks the midtarsal joint, the distal joints, including those of the midfoot, tend to lose their inherent functional stability as a rigid lever. \7ith a loss of stability, the joints are in malalignment and reach an early functional end range of motion. This causes significant jamming as the weight of the body continues to propulse across them. Such forces result in significant degenerative changes where the impact of the joint is greatest, which is usually dorsally. In pes ca\.lrs, there is a significant supination deformity which again causes midfoot jammlng, but by a slightly different mechanism. The joints are inherently stable, but have no available end range of motion. This results in significant cafiilage degeneration, pafiicularly at the dorsal margins of the joints. Compensation deformities can include forefoot or rearfoot varus, forefoot valgus, and equinus (Figs. 2A, 2B). Fusion, by way of triple, pantalar, or even single hindfoot joint arthrodesis, causes increased stress on the surrounding joints as they attempt to compensate for the lost motion. This too can result in joint jamming and destruction. Perhaps the most dramatic manifestation of midfoot stresses is in the neuropathic foot. Loss of shock absorption mechanisms results in rapid joint destruction, and fractures accelerated by biomechanical deformities such as equinus. Conditions which predispose patients to degenerative joint disease of the midfoot include overuse, obesity, osteoporosis, rheumatologic disorders, biomechanical deformities, and neurologic disorders. Figure 28. The point of compensation is at the naviculocuneiform loint. DIAGNOSIS Stiffness, midfoot fatigue, and difficulty wearing shoes, especially if they are tight over the midfoot area, ate all early symptoms of developing degenerative joint disease. The pain is usually of a dull aching nature, and is located more dorsally than plantarly. Pain is due to subchondral osseous damage after there is loss of articular cartilage. There may also be locaiized synovitis. Pain becomes more severe during weight bearing, resulting in difficulty with walking. It may present as poststatic dyskinesia, and the patient may repofi a significant increase in symptoms when there are temperature or weather changes. Usually there is very little swelling, but often warmth is present at the affected afiiculations. The patient may often present with an antalgic gait. Palpation reveals tenderness along the joint lines dorsally where osteophyes may be evident. There are seldom significant clicks or crepitus, since there is insufficient motion in these joints to produce such signs. Careful and deep palpation of the midfoot from the plantar approach will also often
3 CHAPTER reveal tenderness. One should be able to anatomically identify the exact ioint(s) affected before consulting radiographs. In terms of diagnostic tests, blood studies are not usually helpful, with the possible exception of the ESR which is a nonspecific marker for inflammation. Radiographs show a loss of joint space, often with complete joint obliteration. If the x-ray is not pointed at the coffect angle, visualization of the joint may be obscured. Repeat films with adjusted central ray angles may be necessary. Radiographic findings include narrowing of the joints, subchondral sclerosis, erosions, and periarlicular osteophyes (Figs. 3,{, 3B). Subluxation and dislocation may be evident in the most severe cases, especially in the Charcot foot. A CT scan is indicated only if joint damage is extensive, and if the information gained would influence the treatment. Flgure 38. Note hor. the change in the angle of the central radiograph beam "opens" various midfoot joints. ing is necessary in order to effect sufficient rest for relief of symptoms. Intra-articular corticosteroid injections can provide a variable duration of relief, but are genera1ly effective in relieving symptoms. A soluble steroid should be utiiized for the initial test injection. If this is successful, the longer acting crystalline steroid salts should be utilized. There is relatively low risk of further joint damage since the hyaiine cartilage has already been destroyed by the degenerative process. SURGICAL TREATMENT Figure 3A. An example of clegenerative changes in the midfoot. C ONSERVAITVE TREATMENT Early intervention is most beneficial if initiated prior to radiographic evidence of degenerative joint disease. Treatment modalities include compression, heat, NSAIDs, and physical therapy. Heat delivered via ultrasound or a paraffin wax bath is the most effective treatment. Orthotic support is also essential. Occasionally, a short period of cast- Persistent pain and disability in spite of conservative care is the primary indication for surgical interwention. However, the patient should not be immediately scheduled for surgery merely due to marked joint destruction on the initial radiograph. The nature of the pathology, prognosis with and without treatment, and the alternatives for non-operative and operative care should be clearly delieated to the patient before surgical intelention is attempted. Midfoot degenerative joint disease frequently occurs in the geriatric population. Because it is often impossible to keep this patient non-weight bearing during recovery from arthrodesis, alternative procedures may be considered. One such procedure is the osteoarthrotomy. This involves
4 44 CHAPTER 10 resecting one side of a joint (usually the more mobile side), such as the bases of the metatarsals at the tarsometatarsal junctions. Complete medial to lateral resection of the midfoot should not be attempted, however, one or two joints may be addressed at a lime. The patient must be made awate of the fact that a bone graft afihrodesis may be necessary in the future, if the procedure fails to produce painfree ambulation. Silastic implant material can serve as an interface at the osteoafihrotomy site. High density silicone polymer can be fashioned from a solid block, and shaped to fit in the appropriate space. Again, the patient must be prepared for possible failure and the need for further afihrodesis at the site. There are no long-term studies relative to the effectiveness of silastic fi:raterial in these pafiicular locations. Postoperative management includes the use of a closed suction drain and a surgical shoe. 'Weight bearing is allowed immediately as necessary. A common and effective procedure for relief of midfoot degenerative joint disease is arlhrodesis of either a single joint or a combination of joints, depending on the degree of pathology. Whether the bones need to be fused, at their side-to-side interfaces depends again on the pathology presented. Usually the bones within eachray can be fused, and it is not imperative to fuse the bones in between the rays, unless there is severe joint destruction present (Figs. 44, 4B). The more mobile the joint, the greater the chance for non-union. Therefore, mobile afiiculations such as the first metatarsocuneiform joint require greater stabilization. Incision Planning Incision placement requires careful planning due to the many anatomical structures thatlay between the scalpel and the affected joints. Each layer houses neryes and vessels, including the superficial peroneal nerve branches and the dorsalis pedis/deep peroneal neurovascular bundle, which lies on the periosteum of the midfoot. One should use a skin scribe to carefully draw the target articulations and the vital structures in the area before making an incision. The incision should be oriented to provide the best exposure with the least amount of scarring. Figure 4A. Preoperative radiograph of a 54 year-old female with painful degeneration of the lesser tarsal joints. Figure 48. Complete relief of painful symptoms in medial lesser tarsal joints, resolved by fusion. Postoperative radiograph following arthrodesis of the first and second tarsometatarsal,oints. The patient had complete resolution of pain fo1- lowing successful fusion.
5 CHAPTER Joint Resection Articular osteophytes will be encountered first, and these must be removed along with any loose ossicles. The damaged articdar surfaces must then be resected to expose the underlying cancellous bone. Overaggressive resection of bone should be avoided so as to not make consolidation dfficult or impossible. Fixation Internal interfragmentary compression fixation is the ideal goal for immobilization of the afthrodesis sites. This may be augmented by neutralization plates, such as the one-third tubular plate. A T-plate is well suited for use along the medial surface of the first metatarsocuneiform joint, and can be extended proximally to include the navicular. A smali dynamic compression plate can be placed over the tarsal afticulations dorsaily to provide interfragmentary compression and stabrlization. Howeveq there is a risk of irritation from this plate. Other methods of fixation include cross k-wires, staples, and absorbable pins. Staples should be pre-drilled to prevent fracture into the afihrodesis site. Special considerations are given to the more mobile versus the more stable midfoot joints. Fufihermore, consideration for motion must be made between the stabilized ray and the adjacent mobile ray. This is important when deciding to cross non-damaged joints with internal fixation devices. Due to the anatomical complexities of the midfoot, the approach to fixation is variable in every clinical situation, depending on whether one or more joints are involved, if transverse fusion is required, and the age, bone quality, and activiry level of the patient. Finally, one must address any concurrent structural or functional deformities. Controversy exists regarding the crossing of unaffected joints in the area with screws in order to enhance fixation and stabilization of the arthrodesis sites. There is some concern for joint damage, even if the screws are to remain in place only temporarily. There is also the possibility that shear forces will lead to fracture of the screws. Although some authors have applied these with impunity, there is insufficient evidence to suggest that these joints will not break down over time, once they are damaged by the screws. Bone Grafting Bone grafting material, preferably cancellous bone, should be available for every midfoot arthrodesis procedure. The order of preference for bone grafting is autogenous, aliogeneic, or a bone substitute such as that derived from coral. Bone graft material can be firmly wedged into the afihrodesis site to add some measure of compression to insure consolidation. Postoperative Management 'Ihe patient should be placed in a compression cast until the surgical swelling subsides, usually between three and five days. A non-weight bearing below-knee cast is then applied for six to eight weeks, followed by a walking cast for an additional two weeks. Rehabilitation to pain-free walking in shoes is then instituted. SUMMARY Successful treatment of midfoot degenerative joint disease can be very gratifying to both the patient and the surgeon, since it usually resolves a painful and incapacitating problem. Although normal intertarsal and tarsometatarsal motion is relatively limited, stabilization can be quite challenging, especially the application of internal fixation in order to achieve stable osseous consolidation. Attention to the principles which have been presented will heip achieve these goals. BIBLIOGRAPTry Banks AS, McGlamry ED: Charcot foot. J Am Podicttr lted Assoc 79t2L Goosens M, Destoop N: LisFranc's fracture dislocations: etiology, radiology and results of treatment. Clin Orthop 176t , Harris JR, Brand P\il: Patterns of disintegration of the tarslls in the anacsrherit loor. J Bone.loint SurB 18B: I Horton GA, Olney B$7: Deformity correction and amhrodesis of the midfoot with a medial plate. Foot Ankle 14: , JohnsonJE, Johnson IiA.: Dowel arthrodesis for degenerative afthritis of the Tarsometatarsal (LisFranc) joints. Foot Ankle 5: , LoGerfo FW, Coffman JD: Vascular and microvascular disease of the foot in diabetes. N Eng J Med , Myerson MS, Fisher RT, Burgess AR, Kenzora JE: Fracture dislocations of the tarsometatarsal joints: end results correlated with pathology and treatment. Foot Ankle 6: , Sanjeorzan BJ. Veith RG, Hansen ST: Salvage of LisFranc's tarsometararsal joint by arthrodesis. Foot Ankle 1,0:1,93-200, Sanjeorzan, BJ, Hansen, ST: Early and late posttraumatic foot reconstruction. Clin Orthop 243:86-91, 1989.
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium
 MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
MIDFOOT INJURIES-ARE WE UNDERTREATING IT? Mr Rajiv Limaye Mr Prasad Karpe University Hospital of North Tees 3 rd Foot and Ankle Symposium Introduction Increasing sports injuries RTA and traumatic injuries
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E.
 Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
Jeannie Huh, MD Christopher Gross, MD Alex Lampley, MD Samuel B. Adams, MD James K. DeOrio, MD James A. Nunley II, MD Mark E. Easley, MD Duke University Medical Center Durham, NC Disclosures Predictors
SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT
 C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
C H A P T E R 1 7 SUBTALAR ARTHROEREISIS IN THE OLDER PATIENT William D. Fishco, DPM, MS INTRODUCTION Arthroereisis is a surgical procedure designed to limit the motion of a joint. Subtalar joint arthroereisis
Midfoot - Reduction & Fixation - ORIF - screw fixation - AO Surgery Reference. ORIF - screw fixation
 Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Midfoot - TMT (Lisfranc) injury 1. Diagnosis ORIF - screw fixation Authors Mechanism of the injury Tarso-metatarsal (Lisfranc) injuries may be caused by direct or indirect forces. Direct forces include
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Hany El-Rashidy and Anand Vora
 Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Chapter 194 Lisfranc Injuries Chapter 194 Lisfranc Injuries Hany El-Rashidy and Anand Vora 8 ICD-9 CODE 838.03 Lisfranc (Tarsometatarsal) Fracture-Dislocation Key Concepts The Lisfranc joint represents
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Foot Injuries. Dr R B Kalia
 Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Foot Injuries Dr R B Kalia Overview Dramatic impact on the overall health, activity, and emotional status More attention and aggressive management Difficult appendage to study and diagnose. Aim- a stable
Posterior Tibialis Tendon Dysfunction & Repair
 1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
1 Posterior Tibialis Tendon Dysfunction & Repair Surgical Indications and Considerations Anatomical Considerations: The posterior tibialis muscle arises from the interosseous membrane and the adjacent
Technique Guide. 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot.
 Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Technique Guide 6.5 mm Midfoot Fusion Bolt. For intramedullary fixation of the medial column of the foot. Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Section 3: Foot Subluxations and Dislocations
 Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Section 3: Foot Subluxations and Dislocations Case Study F: Lisfranc s Midfoot Dislocation Clinical History: J.K. a 28 year old female presents complaining of a painful right foot. She sustained an acute
Introduction. The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking.
 The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
The ankle 1 Introduction The primary function of the ankle and foot is to absorb shock and impart thrust to the body during walking. OSTEOLOGRY The term ankle refers primarily to the talocrural joint,
6.5 mm midfoot fusion bolt
 6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
6.5 mm midfoot fusion bolt For intramedullary fixation of the medial column of the foot SurgIcal technique Table of Contents Introduction 6.5 mm Midfoot Fusion Bolt 2 AO Principles 4 Indications 5 Surgical
MULTIPLE APPLICATIONS OF THE MINIRAIL
 C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
C H A P T E R 2 1 MULTIPLE APPLICATIONS OF THE MINIRAIL Thomas J. Merrill, DPM James M. Losito, DPM Mario Cala, DPM Victor Herrera, DPM Alan E. Sotelo, DPM INTRODUCTION The unilateral MiniRail External
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery
 PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
Lisfranc Fracture-Dislocation/ Arthrodesis
 Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Lisfranc Fracture-Dislocation/ Arthrodesis 16 Lawrence A. Di Domenico and Frank A. Luckino Introduction L.A. Di Domenico (*) Ankle and Foot Care Centers, Youngstown, OH, USA Kent State University, College
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment
 Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
Tarsometatarsal Joint Injuries Review of Clinical Presentation and Surgical Treatment S Y Loh, FRCS (Orth)*, J L Soon, MBBS**, W J Verhoeven, FRCS*** *Department of Orthopedic Surgery, Alexandra Hospital,
pedcat Clinical Case Studies
 pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
pedcat Clinical Case Studies C u r v e B e a m 1 7 5 T i t u s A v e, S u i t e 3 0 0 W a r r i n g t o n, P A 1 8 9 7 6 267-4 8 3-8081 w w w. c u r v e b e a m. c o m PedCAT: Clinical Evidence of diagnostic
Complexities surrounding Lisfranc injuries
 Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
Complexities surrounding Lisfranc injuries Lisfranc injuries are commonly associated with sporting injuries and are easily diagnosed with severe midfoot pain, swelling, deformity and inability to bear
LISFRANC FRACTURE-DISLOCATION
 LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
LISFRANC FRACTURE-DISLOCATION Napoleon at Mont St. Bernard, Jacques-Louis David, 1800, Oil on Canvas, Musee du Louvre, Paris. This is Jacques-Louis David s immortal depiction of a young Napoleon Bonaparte,
Long-term follow-up of joint stabilization procedures in the treatment of fixed deformities of feet in leprosy
 Lepr Rev (1996) 67, 126-134 Long-term follow-up of joint stabilization procedures in the treatment of fixed deformities of feet in leprosy M. EBENEZER, S. PARTHEEBARAJAN & S. SOLOMON Branch of Surgery
Lepr Rev (1996) 67, 126-134 Long-term follow-up of joint stabilization procedures in the treatment of fixed deformities of feet in leprosy M. EBENEZER, S. PARTHEEBARAJAN & S. SOLOMON Branch of Surgery
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations
 Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Closed Reduction and Internal Fixation of Lisfranc Fracture Dislocations Anish R. Kadakia, Mark S. Myerson, and Milap Patel Contents Mechanism of Injury... 2 Radiographic Evaluation... 3 Classification...
Midfoot arthritis, a specific complaint in adults,
 A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
A Review Paper Midfoot Arthritis Siraj A. Sayeed, MD, Fazel A. Khan, MD, Norman S. Turner III, MD, and Harold B. Kitaoka, MD Abstract Foot and ankle complaints are commonly encountered in orthopedic practice.
Ankle Arthritis and Ankle Replacement
 Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
CHARLOTTE Lisfranc. Recontruction System SURGICAL TECHNIQUE
 CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
CHARLOTTE Lisfranc Recontruction System SURGICAL TECHNIQUE Contents Preface 3 Chapter 1 4 Chapter 2 4 4 4 4 4 Chapter 3 5 5 5 6 6 6 7 7 8 Chapter 4 8 8 9 10 Appendix 10 Introduction Indications and Contraindications
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries
 Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Temporary bridge plating of the medial column in Chopart and Lisfranc injuries by Alaa Mansour DPM 1*, Lawrence Fallat DPM, FACFAS 2 The Foot and Ankle Online Journal 10 (1): 5 Severe traumatic injuries
Peggers Super Summaries: Foot Injuries
 Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Lisfranc Injury ANATOMY Roman arch with recessed 2 nd MT base AP medial side of intermediate cuneiform to 2 nd MT base Oblique medial side of lateral cuneiform with 3 rd MT base and 4 th with medial boarder
Managing Tibialis Posterior Tendon Injuries
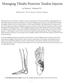 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA
 Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Surgical Technique. Customer Service:
 Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Patent and Patent Pending CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Axis Charcot Fixation System in diameters of 5.5, 6.5 and 7.5mm
Lisfranc and Midfoot Fracture
 Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
Lisfranc and Midfoot Fracture AO Advanced Principles of Fracture Management Middelfart, 11.-14. april 2016 Overlæge Marianne Vestergaard Lind Traumesektionen Ortopædkirurgisk Klinik Rigshospitalet What
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
Case. 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms. Your diagnosis?
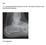 Case 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms Your diagnosis? Diagnosis: Calcaneo-navicular tarsal coalition. C sign Talar beaking Ant eaters nose
Case 15 Y old boy presented with pain in the foot. No history of injury or any constitutional symptoms Your diagnosis? Diagnosis: Calcaneo-navicular tarsal coalition. C sign Talar beaking Ant eaters nose
TIBIAXYS ANKLE FUSION
 TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
TIBIAXYS ANKLE FUSION SURGICAL TECHNIQUE TIBIAXYS Ankle Fusion Plate features Anatomically contoured plates The plates are designed to approximate the patient s bony and soft tissue anatomy The plate designs
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity
 Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
Results of Calcaneal Osteotomy & Flexor Digitorum Longus transfer in Stage II Acquired Flatfoot Deformity Mr Amit Chauhan Mr Prasad Karpe Ms Maire-claire Killen Mr Rajiv Limaye University Hospital of North
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle September 4-6, 2014 Goodlett Farms Innovation
Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury
 Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
Section Editor: Steven F. Harwin, MD Dorsal Multiple Plating Without Routine Transarticular Screws for Fixation of Lisfranc Injury Richard E. Stern, MD; Mathieu ssal, MD bstract: Following a Lisfranc joint
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 7/28/2012 Radiology Quiz of the Week # 83 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
TENDON TRANSFER IN CAVUS FOOT
 TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
TENDON TRANSFER IN CAVUS FOOT Cavovarus deformity is defined by fixed equinus of the forefoot on the hindfoot, resulting in a pathologic elevation of the longitudinal arch, with either a fixed or flexible
Rehabilitation after Total Elbow Arthroplasty
 Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
Rehabilitation after Total Elbow Arthroplasty Total Elbow Atrthroplasty Total elbow arthroplasty (TEA) Replacement of the ulnohumeral articulation with a prosthetic device. Goal of TEA is to provide pain
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures
 FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
FOOT/ ANKLE RETROSPECTIVE STUDYIC S Retrospective Study of Surgical Outcomes for Combined Ankle and Subtalar Joint Arthrodesis, Cavovarus Deformity Correction and Ankle Fractures Adult & Pediatric Deformity
Avascular Necrosis of the Foot. Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada.
 Avascular Necrosis of the Foot Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada. Avascular Necrosis: Pathophysiology Ischemia to the bone from oxygen
Avascular Necrosis of the Foot Dr. Hema Choudur MD, FRCPC Associate Professor. Dept. of Radiology. McMaster University, Hamilton, Canada. Avascular Necrosis: Pathophysiology Ischemia to the bone from oxygen
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
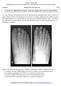 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/29/2012 Radiology Quiz of the Week # 105 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Hallux Rigidus & Silastic Total Implants
 Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Hallux Rigidus & Silastic Total Implants JOSHUA L. MOORE, DPM FACFAS ASSISTANT DEAN OF EDUCATIONAL AFFAIRS TUSPM CLINICAL ASSISTANT PROFESSOR OF SURGERY Definitions Hallux Limitus 1 st MTPJ range of motion
Integra. ADVANSYS Plating System SURGICAL TECHNIQUE
 Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Integra ADVANSYS Plating System SURGICAL TECHNIQUE Table of Contents Dorsal Lisfranc Plate Indications...2 Contraindications...2 Description...2 Surgical Technique...3 Surgical Site Preparation...3 Step
Anatomy 1% 29% 64% 6%
 Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
Mortons Neuroma Perineural fibrosis of the plantar digital nerve Females 8-10 3 rd plantar webspace most commonly effected Burning pain Sensory changes 3&4 digits / interdigital space Etiology Excessive
American Family Physician
 Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Page 1 of 12 American Family Physician Return to Previous Page Jul 1, 1998 Table of Contents Lisfranc Injury of the Foot: A Commonly Missed Diagnosis KEVIN E. BURROUGHS, M.D, Moses Cone Family Practice
Case Report A Case Report of Isolated Cuboid Nutcracker Fracture
 Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Case Reports in Orthopedics Volume 2016, Article ID 3264172, 5 pages http://dx.doi.org/10.1155/2016/3264172 Case Report A Case Report of Isolated Cuboid Nutcracker Fracture Takaaki Ohmori, 1,2 Shinichi
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
Ankle Valgus in Cerebral Palsy
 Ankle Valgus in Cerebral Palsy Freeman Miller Contents Introduction... 2 Natural History... 2 Treatment... 3 Diagnostic Evaluations... 3 Indications for Intervention... 3 Outcome of Treatment... 5 Complications
Ankle Valgus in Cerebral Palsy Freeman Miller Contents Introduction... 2 Natural History... 2 Treatment... 3 Diagnostic Evaluations... 3 Indications for Intervention... 3 Outcome of Treatment... 5 Complications
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
«Foot & Ankle Surgery» 04. Sept THE PAINFUL FLATFOOT. Norman Espinosa, MD
 THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
THE PAINFUL FLATFOOT Norman Espinosa, MD Department of Orthopaedics University of Zurich Balgrist Switzerland www.balgrist.ch WHAT TO DO? INTRINSIC > EXTRINSIC ETIOLOGIES Repetitive microtrauma combined
Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
 Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Injury Extra (2008) 39, 291 295 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/inext CASE REPORT Unusual fracture combination with Charcot arthropathy and juvenile-onset diabetes
Matthew Beuchel MD 2 C. Luke Rust MD 3 Jessica Hooper MD 3
 A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
A Prospective, Randomized,Controlled Trial Comparing Early- Weightbearing vs. Non-Weightbearing Following Modified Lapidus Arthrodesis Intermediate Results - Donald R. Bohay, MD, FACS Professor, Michigan
Index. Clin Podiatr Med Surg 22 (2005) Note: Page numbers of article titles are in boldface type.
 Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Clin Podiatr Med Surg 22 (2005) 309 314 Index Note: Page numbers of article titles are in boldface type. A Abductor digiti minimi muscle, myectomy of, for tailor s bunionette, 243 Achilles tendon, lengthening
Arthritis of the Foot and Ankle
 Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
Arthritis of the Foot and Ankle Arthritis is inflammation of one or more of your joints. It can cause pain and stiffness in any joint in the body, and is common in the small joints of the foot and ankle.
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatric Surgery. Procedure List. As Of.
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2016 Alberta Health Care Insurance Plan Page i Generated 2016/03/22 TABLE OF CONTENTS As of 2016/04/01 07 PHYSICAL MEDICINE, REHABILITATION,
Product Rationale & Surgical Technique
 Product Rationale & Surgical Technique Contents Surgeon Design Team 8 Introduction 9 1st Metatarsal Fusion Technique 12 Single Joint Fusion Plates Technique 22 Lateral Column Lengthening Plate Technique
Product Rationale & Surgical Technique Contents Surgeon Design Team 8 Introduction 9 1st Metatarsal Fusion Technique 12 Single Joint Fusion Plates Technique 22 Lateral Column Lengthening Plate Technique
Complications of missed or untreated Lisfranc injuries
 Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Foot Ankle Clin N Am 8 (2003) 61 71 Complications of missed or untreated Lisfranc injuries Terry Philbin, DO a,b, *, Gary Rosenberg, MD c, James J. Sferra, MD d a Orthopedic Foot and Ankle, 6200 Cleveland
Traumatic Injuries to the Foot and Ankle
 Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Traumatic Injuries to the Foot and Ankle Dr. Joseph N. Daniel Clinical Associate Professor of Orthopaedic Surgery Foot and Ankle Service, The Rothman Institute Thomas Jefferson University Hospital Philadelphia,
Lisfranc injuries. Mikko Kirjavainen, MD, PhD. Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland
 Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Lisfranc injuries Mikko Kirjavainen, MD, PhD Department of Orthopaedics and Traumatology Helsinki University Central Hospital, Helsinki Finland Lisfranc injuries are midfoot fracture dislocations. The
Interesting Case Series. Ulnolunate Impaction Syndrome
 Interesting Case Series Ulnolunate Impaction Syndrome Saptarshi Biswas, MD, FRCS Westchester University Medical Center, Valhalla, NY Keywords: ulnar impaction, ulnar impaction syndrome, ulnar wrist pain,
Interesting Case Series Ulnolunate Impaction Syndrome Saptarshi Biswas, MD, FRCS Westchester University Medical Center, Valhalla, NY Keywords: ulnar impaction, ulnar impaction syndrome, ulnar wrist pain,
Amputations of the digit, ray and midfoot
 Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Amputations of the digit, ray and midfoot Dane K. Wukich M.D. Chief, Division of Foot and Ankle Surgery Medical Director, UPMC Foot and Ankle Center University of Pittsburgh School of Medicine Disclosure
Sports Injuries of the Foot and Ankle. Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018
 Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Sports Injuries of the Foot and Ankle Mark McEleney, MD University of Iowa College of Medicine Refresher Course for the Family Physician 4/4/2018 I. Objectives A. By the end of the lecture attendees will
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Lecture 10. JOINTS of the FOOT. Dr Farooq Khan Aurakzai. Dated:
 Lecture 10 JOINTS of the FOOT. BY Dr Farooq Khan Aurakzai Dated: 20.02.2018 The joints of the foot are numerous. They are classified: A. Intertarsals B. Tarso metatarsals C. Intermetatarsals D. Metatarsophalangeal
Lecture 10 JOINTS of the FOOT. BY Dr Farooq Khan Aurakzai Dated: 20.02.2018 The joints of the foot are numerous. They are classified: A. Intertarsals B. Tarso metatarsals C. Intermetatarsals D. Metatarsophalangeal
Annual Surgical Conference LisFranc Fractures. Zeeshan S. Husain, DPM, FACFAS, FASPS. Great Lakes Foot and Ankle Institute September 21, 2018
 Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Annual Surgical Conference 2018 LisFranc Fractures Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Jacques LisFranc 1790 1847 History LisFranc
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
1 st MP Arthrodesis. - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA
 1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
1 st MP Arthrodesis - Unraveling The Myths - Craig A. Camasta, DPM Atlanta, Georgia, USA Hallux Limitus Dorsal Bunion Spasm of Short Flexor Immobility of Sesamoids DJD of 1 st MPJ Hallus Limitus Plantar
Surgical Technique Guide
 Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
Guide CAUTION: Federal Law (USA) restricts this device to sale by or on the order of a physician. INDICATIONS FOR USE The Align Anterior Ankle Fusion Plate is intended to facilitate arthrodesis of the
Section 4: Tarsal Coalitions
 Case H (Figure 2): PedCat CBCT transverse plane reconstruction of right Lisfranc midfoot dislocation compared to normal left foot. Clinical Relevance of the PedCat Study: The weight bearing CBCT study
Case H (Figure 2): PedCat CBCT transverse plane reconstruction of right Lisfranc midfoot dislocation compared to normal left foot. Clinical Relevance of the PedCat Study: The weight bearing CBCT study
5 COMMON INJURIES IN THE FOOT & ANKLE
 5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
5 COMMON INJURIES IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA MECHANISM OF INJURY HOW DID IT HAPPEN? HIGH ENERGY VS LOW ENERGY DIRECTION OF FORCES INVOLVED LIVING
Fractures of the Calcaneus
 Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
Fractures of the Calcaneus Anthony T. Sorkin, M.D. Rockford Orthopedic Trauma Service Rajeev Garapati, MD Illinois Bone and Joint Institute Assistant Clinical Professor University of Illinois at Chicago
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
THE JOURNAL OF NUCLEAR MEDICINE Vol. 56 No. 3 March 2015 Rauscher et al.
 Supplemental Figure 1 Correlation analysis of tracer between and subsequent as assessed by SUV max in focal lesions (A). x-axis displays quantitative values as obtained by, and y-axis displays corresponding
Supplemental Figure 1 Correlation analysis of tracer between and subsequent as assessed by SUV max in focal lesions (A). x-axis displays quantitative values as obtained by, and y-axis displays corresponding
Foot & Ankle Disorders
 Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Foot & Ankle Disorders Hillingdon PGMC 6-7-2013 Htwe Zaw FRCS (Tr&Orth) Consultant Foot & Ankle and Trauma Surgeon Hillingdon Hospitals NHS Foundation Trust Overview Anatomy: hindfoot-midfoot coupling
Locking Forefoot/Midfoot Plating System
 Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
Locking Forefoot/Midfoot Plating System Locking Forefoot/Midfoot Plating System Acumed is an industry leader in innovative solutions for extremities and trauma. We are dedicated to pioneering solutions
The American Academy of Foot & Ankle Osteosynthesis. presents
 The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle Hyatt DFW Airport Dallas, Texas SCIENTIFIC
The American Academy of Foot & Ankle Osteosynthesis presents Comprehensive Course of Internal Fixation for Reconstructive Surgery and Trauma of the Foot & Ankle Hyatt DFW Airport Dallas, Texas SCIENTIFIC
Arthritis of the Shoulder
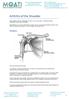 Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
Arthritis of the Shoulder Simply defined, arthritis is inflammation of one or more of your joints. In a diseased shoulder, inflammation causes pain and stiffness. Although there is no cure for arthritis
ABC of Emergency Radiology
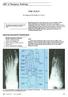 l ja ) $% _2) < j> ~~~~~~~~~~~~~~~~~foot ABC of Emergency Radiology THE FOOT D A Nicholson, D O'Keeffe, P A Driscoll Accurate clinical assessment of injuries to the foot will avoid unnecessary exposure
l ja ) $% _2) < j> ~~~~~~~~~~~~~~~~~foot ABC of Emergency Radiology THE FOOT D A Nicholson, D O'Keeffe, P A Driscoll Accurate clinical assessment of injuries to the foot will avoid unnecessary exposure
InCoreTM Lapidus System
 InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
InCoreTM Lapidus System Precision Guided Correction Surgical Technique InCore TM Lapidus System Precision Guided Correction Tri-Planar Correction Targeting Guide is intended to aid and stabilize angular/rotational
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children
 A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Flatfoot Deformity (Pes Planus) in Children 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled
Lisfranc fracture-dislocations. Disclosures. It s just a foot
 Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
Lisfranc fracture-dislocations Gregory J. Della Rocca, MD, PhD, FACS Associate Professor Co-director, Orthopaedic Trauma Service University of Missouri Disclosures Consultant: Synthes, Bioventus Stock
2017 SAFSA CONGRESS PROGRAMME
 2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
2017 SAFSA CONGRESS PROGRAMME THURSDAY, MAY 25 07h45 07h55: WELCOME & INTRODUCTIONS Forefoot I: Hallux Valgus and Lesser Toes (08h00-10h00 Lectures) 08h00 08h30: Surgical Management of Hallux Valgus Rippstein,
The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus. Alfred D. Grant, M.D. David Feldman, M.D.
 The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus Alfred D. Grant, M.D. David Feldman, M.D. Norman Otsuka, MD M.D. THE PURPOSE OF THIS PRESENTATION IS TO STATE CLEARLY THAT THE VALGUS FOOT
The Valgus Foot in Cerebral Palsy Equinovalgus not Plano-Valgus Alfred D. Grant, M.D. David Feldman, M.D. Norman Otsuka, MD M.D. THE PURPOSE OF THIS PRESENTATION IS TO STATE CLEARLY THAT THE VALGUS FOOT
Common Foot and Ankle Conditions: How Can You Find Relief?
 Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
radiologymasterclass.co.uk
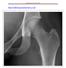 http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
http://radiologymasterclass.co.uk Hip X-ray anatomy - Normal AP (anterior-posterior) Shenton's line is formed by the medial edge of the femoral neck and the inferior edge of the superior pubic ramus Loss
CLAD Error Key. Error Levels: Definite, Possible. Error Procedure Scope. Validation Scope. Location Scope. Violation/Information Text
 CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
CLAD Key s: Definite, Possible Procedure 1 2 3 4 5 6 7 8 9 10 Two or more category 1 procedures Digit Definite 1.6 plus one or more of the following: 2.1.3, 2.1.7, 2.2.2, 2.2.6, and 2.3.4 Side Definite
Index. Clin Sports Med 23 (2004) Note: Page numbers of article titles are in boldface type.
 Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Midfoot Fusion Bolt 6.5 mm. Intramedullary fixation of the medial column of the foot.
 Midfoot Fusion Bolt 6.5 mm. Intramedullary fixation of the medial column of the foot. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
Midfoot Fusion Bolt 6.5 mm. Intramedullary fixation of the medial column of the foot. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
