CLINICAL PATHOLOGY CONFERENCE
|
|
|
- Anis Berry
- 6 years ago
- Views:
Transcription
1 CLINICAL PATHOLOGY CONFERENCE DEPARTMENT OF MEDICINE JANUARY 13, 2006 Alex Esana MD
2 Case 43 y/o Caucasian female referred to Endocrinology clinic in July 2005 from Orthopedics for evaluation of recurrent stress fractures. First fractures in 2000-bilateral femur stress fractures requiring an intra- medullary rod on the left
3 Case DEXA in 2000 showed T-score +1.4 at L2- L4 T-score -0.4 at femoral neck Treated with: Fosamax 70 mg weekly for 2 years without follow up studies. Calcium supplements 600 mg (with vitamin D) daily
4 Case Lab work in 2000 revealed: Unremarkable CBC Comprehensive metabolic profile within normal limits with serum calcium=9.8 mg/dl and reduced alkaline phosphatase=8 IU/L [normal ] Normal serum immunoelectrophoresis
5 Case In October 2004, she was stepping over a fence and suffered a right fifth metatarsal stress fracture which was casted. In February 2005, she suffered a traumatic left fifth metatarsal fracture managed with a orthopedic boot. She had mild residual left foot and right femur aching not requiring narcotic analgesia.
6 Past Medical History History of hypothyroidism treated with L-L thyroxine mg daily for 25 years with normal TSH values on therapy Hysterectomy without oophorectomy in 1998 but was not experiencing hot flashes No history of joint laxity or kidney stones She lost her baby teeth at age 4 and had multiple root canals in the past with history of widened pulp spaces
7 Family History No history of osteoporosis No history suggestive of malabsorption or steatorrhea No history of hypercortisolism.
8 Physical Exam Basically unremarkable Normal sclera No bony tenderness No goiter with clinically euthyroid appearance
9 Laboratory Studies Normal serum calcium, 25-hydroxy hydroxy-vitamin D and 1,25-dihydroxy dihydroxy-vitamin D levels Serum phosphorus was 5.2 mg/dl [ mg/dl] PTH level was 15 pg/dl [6-40 pg/dl] 24-hour urine calcium was 228 mg Urine free cortisol was 7 mcg [ mcg] Serum TSH was 1.9 [ ]
10 Further Work-up Repeat DEXA showed: L1-4 4 T-score T was +1.6 (1.4) Right femoral neck T-score T was +0.3 (-( 0.4) A diagnostic study was obtained and a treatment approach was decided.
11 Significant case findings Dexa.multiple fx, with Nl bone density Low Alk Phos, Normal calcium, NL SPEP Hypothyroidism Tx,...? Euthyroid Hysterectomy.Ovaries intact, (Estrogen problem) No family history of osteoporosis (congenital) No history suggestive of malabsorption or steatorrhea No hypercortisolism No joint laxity No history of nephrolithiasis Lost her baby teeth at age 4
12 Regulation of bone cell function Parathyroid hormone The most important regulator of calcium homeostasis Maintains serum calcium concentrations by stimulating bone resorption, increasing renal tubular calcium reabsorption, and increasing renal calcitriol production Stimulates bone formation when given intermittently, but inhibits collagen synthesis at high concentrations Stimulates bone resorption when given (or secreted) continuously, a process mediated by osteoclasts
13 Regulation of bone cell function Calcitriol Increases intestinal calcium and phosphorus absorption, thereby promoting bone mineralization At high concentrations, under conditions of calcium and phosphate deficiency, it also stimulates bone resorption, thereby helping to maintain the supply of these ions to other tissues Stimulates osteoclastogenesis in cell cultures, but animals lacking vitamin D have relatively normal bone growth and remodeling during development
14 Regulation of bone cell function Calcitonin inhibits osteoclasts and therefore bone resorption in pharmacologic doses. However, its physiologic role is minimal in the adult skeleton. Growth hormone and IGFs The GH/IGF-1 1 system and IGF-2 2 are important for skeletal growth, especially growth at the cartilaginous end plates and endochondral bone formation. Glucocorticoids have both stimulatory and inhibitory effects on bone cells. Inhibition of bone formation is the major cause of glucocorticoid-induced induced osteoporosis and may be due to accelerated apoptosis of osteoblasts and osteocytes
15 Bone Remodeling The renewal of bone is responsible for bone strength throughout our life. Old bone is removed (resorption) and new bone is created (formation). During childhood and the beginning of adulthood, bone becomes larger, heavier and denser.
16 Bone Remodeling The Bone Mass increases until the ages of where it reaches its maximum value: the Peak Bone Mass (Maximum Bone Density and Strength). The higher the Peak Bone Mass is, the lower the risk of osteoporosis. Bone Mass remains stable for a few years (for women, till about 45 years old): a perfect equilibrium between bone formation and resorption exists. After a certain age, bone mass starts to decrease. For women, this bone loss starts a few years before menopause and becomes more and more important until death.
17 Bone remodeling Osteoblasts Responsible for bone matrix synthesis Secrete a collagen rich ground substance essential for later mineralization of hydroxyapatite and other crystals Collagen strands to form osteoids: : spiral fibers of bone matrix. Cause calcium salts and phosphorus to precipitate from the blood, Calcium & Phosphorus bond with the newly formed osteoid to mineralize the bone tissue. Contain alkaline phosphatase that is secreted during osteoblastic activity. Have estrogen receptors. Estrogens increase the number of osteoblasts, increasing therefore collagen production.
18 Bone remodeling Osteocytes Osteocytes are osteoblasts that have been trapped in the osteoids produced by surrounding osteoblasts. Function of Osteocytes includes maintain bones, control the extracellular concentration of calcium and phosphate Osteocytes are directly stimulated by calcitonin and inhibited by PTH Their exact role is actually still to be defined.
19 Bone remodeling Osteoclasts OSTEOCLASTS are derive from bone marrow mononuclear cells. Their characteristic feature is a ruffled edge where active resorption takes place. secrete bone-reabsorbing enzymes, which digest bone matrix. The osteoclasts have estrogen receptors Estrogens can inhibit their recruitment.
20 Fracture Risk Bone strength, as estimated indirectly from both bone mineral density and medullary and periosteal diameter of the distal radius, may be a useful predictor of fracture risk. Low serum levels of RANKL (receptor activator of nuclear factor kb ligand; an essential factor for osteoclast, and possibly osteoblast activation) Aortic calcification on CT scan (a marker of atherosclerosis. A previous history of breast cancer (independent of estrogen deficiency)
21 Fracture Risk In spite of being a source of caffeine, tea may have a beneficial effect on bone density. Habitual tea consumption for 10 or more years has been associated with higher bone density. A possible explanation for this observation is that tea contains both flouride and phytoestrogens.
22 Other Aspects of Fracture Risk Previous fracture between the ages of 20 and 50 year History of fracture in a first degree relative Cigarette smoking (men and women) Inflammatory bowel disease Celiac disease (osteopenia in one-third of asymptomatic adults) Cystic fibrosis Previous hyperthyroidism Sedentary life style Consumption of large amounts of caffeine Anxiolytic, anticonvulsant, or neuroleptic drugs Low body weight or weight loss Above average height Type 2 diabetes mellitus
23 Differential Diagnosis Primary Osteoporosis Secondary Osteoporosis Postmenopausal Osteoporosis Juvenile Osteoporosis Drug induced Osteoporosis Hyperthyroidism induced Osteoporosis Rickets/osteomalacia Metabolic bone disease( GI, Pancreatic, hepatobiliary) Vitamin D dependant Rickets Renal Osteodystrophy
24 Differential Diagnosis continued Fanconi Syndrome/Renal Tubular Acidosis Hypophosphatemic syndromes Multiple Myeloma Breast cancer Chronic anemias Mastocytosis Heparin Therapy Pregnancy induced Osteoporosis Osteogenesis Imperfecta
25 Osteoporosis Osteoporosis is the most common bone disease. The estimated cost of osteoporotic fractures in the United States in 1995 was $13.8 billion. Osteoporosis is characterized by low bone mass and micro-architectural loss of bone tissue, leading to enhanced bone fragility and an increase in fracture risk. In practice, one deals mainly with decreased bone density, or osteopenia, without examining bone histology.
26 Osteoporosis WHO has defined normal bone density as a value within one standard deviation of the mean value in young adults of the same sex and race. BMD in any adult that is between 1 and 2.5 standard deviations below the mean is defined as osteopenia, and a value more than 2.5 standard deviations below the mean is defined as osteoporosis. These values are referred to as T-scores. T One standard deviation below the mean at the hip in women is associated with a relative risk of 2.6 for hip fracture One standard deviation below the mean at the femur in women is associated with a relative risk of 2.4 for vertebral fracture.
27 Primary Osteoporosis Defined as the progressive loss of bone with increasing age. Type 1 is related to lack of estrogen and therefore primarily occurs curs in postmenopausal women. It is largely responsible for wrist and vertebral crush fractures. It is estimated that more than 25 percent of all women older than 65 years of age have sustained such a crush fracture. Type 2 or senile osteoporosis is due to progressive loss of bone mass after the age of 35, fractures of the hip, proximal humerus, and pelvis. The prevalence of hip fractures in the United States reaches 15 percent by age 80 and exceeds 25 percent by age 90.
28 Secondary Osteoporosis Results from an underlying medical condition, such as malabsorption, hypogonadism, hyperthyroidism, or multiple myeloma, or to the administration of drugs, primarily corticosteroids. Corticosteroid therapy is the second most common cause of osteoporosis; the cumulative dose correlates with the severity of disease and the fracture incidence, with higher incidence of rib and vertebral fractures. Pathogenesis of glucocorticoid-induced induced osteoporosis is unclear. It most likely involves impaired bone formation, increased bone resorption, and a negative calcium balance.
29 Laboratory tests All standard laboratory values should be normal in the patient with primary osteoporosis. These include measurement of the serum concentrations of calcium, phosphorus, alkaline phosphatase, and parathyroid hormone, tests of thyroid and liver function, and serum and urine protein electrophoresis. If clinically appropriate, tests to assess adreno-cortical function should also be considered.
30 Imaging studies Plain radiography reveal changes in bone density in patients with at least 30 percent loss of bone mass and therefore do not detect early disease. Characteristic changes in vertebral bodies, such as "codfishing" and compression and crush fractures, may also be observed.
31 Imaging studies Bone densitometry Quantitative x-ray x densitometry may be utilized to help determine the fracture risk and the need for therapeutic intervention. A single bone mass measurement has a far greater predictive value for fracture than the presence of any other single risk factor or combination of factors. Candidates for densitometric measurement include menopausal women in whom hormone replacement therapy is being considered, patients with either demonstrable radiographic changes or primary hyperparathyroidism, and those administered glucocorticoid therapy.
32 Osteomalacia A disorder of mineralization of newly formed organic matrix In children, abnormal calcification of matrix results in rickets The requirements for mineralization of newly formed bone include Normal concentrations of calcium and phosphate in blood The presence of alkaline phosphatase and mature bone matrix The absence of excess quantities of inhibitors of mineralization
33 Causes of osteomalacia Vitamin D deficiency Negative calcium balance, hypophosphatemia, and mild hypocalcemia occur in the absence of sufficient quantities of calciterol (1,25 dihydroxycholecalciferol), the active metabolite of vitamin D. Secondary hyperparathyroidism may contribute to the defective mineralization. Malnutrition and intestinal malabsorption are the most common causes of vitamin D deficiency.
34 Causes of osteomalacia Hypophosphatemia Marked hypophosphatemia results in defective mineralization of bone. In addition to vitamin D deficiency, hypophosphatemia leading to osteomalacia occurs with primary renal tubular wasting of phosphate in disorders such as: oncogenic osteomalacia, sporadic and X-linked X hypophosphatemic rickets, Fanconi syndrome.
35 Osteomalacia Clinical findings and diagnosis Major symptom of osteomalacia is diffuse, dull, aching skeletal pain that is worsened by activity. Muscle weakness, usually involving the proximal musculature, is often present Most common radiologic finding is reduced bone density Other abnormalities include Looser's zones or pseudofractures.
36 Osteomalacia Clinical findings and diagnosis The most common abnormalities-not not present in osteoporosis: Hypophosphatemia Elevation in serum alkaline phosphatase Hypophosphatemia with hypocalcemia usually indicates vitamin D deficiency, Isolated hypophosphatemia is most consistent with a renal tubular phosphate wasting syndrome.
37 Hyperparathyroidism Results in osteitis fibrosa cystica, characterized by marrow fibrosis, woven osteoid, expansion of osteoid surfaces, and numerous collections of osteoclasts. The finding of osteopenia alone may be a characteristic radiographic finding in primary hyperparathyroidism. The diagnosis is made by the combination of hypercalcemia and an inappropriately elevated serum parathyroid hormone concentration. The findings are different in patients with secondary hyperparathyroidism due to renal failure. The serum calcium is usually reduced or normal, the serum phosphate is elevated, and serum PTH is markedly increased.
38 Vitamin D deficiency Osteomalacia can occur with an impairment of vitamin D metabolism. Causes of vitamin D deficiency dietary deficiency gastrointestinal disease reduced exposure to sunlight Incidence Gastrectomy 43 percent Celiac sprue 26 percent Intestinal bypass 15 percent Intestinal resection 8 percent Chronic pancreatitis 4 percent Primary biliary cirrhosis 4 percent
39 Intestinal malabsorption Intestinal malabsorption with impaired vitamin D absorption frequently seen with: celiac disease regional enteritis, scleroderma, Whipple's syndrome, intestinal lymphoma, amyloidosis, and blind-loop loop syndrome.
40 Intestinal Malabsorption Diagnosis: Hypoalbuminemia, Increased stool fat, and Characteristic changes on jejunal biopsy Low levels of calcidiol are low or low normal Low levels of calcitriol or inappropriately normal in the face of elevated levels of PTH and hypophosphatemia.
41 Intestinal malabsorption Osteomalacia occurs as a complication of hepatocellular disorders, is infrequent in pancreatic disorders. The increasing life expectancy in patients with cystic fibrosis may lead to a rising incidence of osteomalacia. The major cause osteomalacia in these disorders is malabsorption of vitamin D. Hypoparathyroidism and pseudohypoparathyroidism are associated with low levels of calcitriol.. Rarely, there is associated osteomalacia which responds to calcitriol therapy. Metabolic bone disease, including osteomalacia,, has also been described after gastric bypass surgery for obesity.
42 The Kidney Chronic renal failure Bone disease in renal insufficiency occurs because of: reduced formation of calcitriol, metabolic acidosis, administration of aluminum (phosphate binder), and secondary hyperparathyroidism.
43 The Kidney Renal tubular acidosis Osteomalacia or rickets is most often seen with proximal (type 2) renal tubular acidosis. Acidosis leads to proximal phosphate wasting, increased calcium loss due, Secondary hyperparathyroidism. Similar findings can occur with the acidosis seen after ureterosigmoidostomy.
44 Other causes Fibrogenesis imperfecta A sporadic, idiopathic disorder with defective bone matrix formation. Symptoms begin in adult life with pain, fractures and weakness. Effects the entire skeleton and is characterized pathologically by the absence of normal birefringent collagen fibrils.
45 Osteogenesis imperfecta An inherited connective tissue disorder with many phenotypic presentations. Called "brittle bone disease. Severely affected patients suffer multiple fractures with minimal or no trauma, and infants with the worst form of OI die in the perinatal period. Mild forms of OI may be manifested by only premature osteoporosis or severe postmenopausal bone mineral loss.
46 Mild (type I) Types of OI few or no fractures before puberty or numerous fractures throughout their lives. occasionally present in the perinatal period with intrauterine fractures, but usually see fractures when they begin toddling or walking. Adults with OI type I may present with premature osteoporosis or accelerated osteoporosis following menopause. Adults may present with premature hearing loss. Moderate to severe (types III - VII) Hearing loss and osteoporosis. Mothers are prone to accelerated bone loss following pregnancy and a breastfeeding. Lethal perinatal form (type II) Patients with lethal perinatal OI (type II) usually die in utero or in early infancy.
47 Lab findings in OI Elevated levels of serum alkaline phosphatase. Hypercalciuria Decreased urinary excretion of calcium.
48 Bruck syndrome Previously called OI with congenital joint contractures, An autosomal recessive disorder Clinical features that distinguish it from OI include: congenital contractures of the knees, ankles, and feet; webbing of the elbow and knee, clubfoot (talipes equinovarus).
49 Osteoporosis-pseudoglioma pseudoglioma syndrome Previously called the ocular form of OI. An autosomal recessive disorder Caused by deletion of the gene for low-density density- lipoprotein (LDL) receptor-related related protein 5 (LRP-5). Present with: microcephaly; pseudoglioma (inflammatory changes of vitreous body) blindness (with onset in infancy); and hypotonia.
50 Causes of Hypophosphatemia Hungry bone syndrome Parathyroidectomy Associated with marked hypocalcemia and hypo-phosphatemia. phosphatemia. Decreased Intestinal Absorption Normal adults are in phosphate balance. Dietary intake of phosphate usually ranges from 800 to 1500 mg/day, Dietary intake is in excess of gastrointestinal losses, and Variations in intake usually have little effect on phosphate homeostasis. There is little regulation of gut absorption
51 Systemic conditions associated with childhood periodontitis Histiocytosis (Langerhans cell histiocytosis, histiocytosis X, or eosinophilic granuloma) A rare disorder affects infants, children, and young adults Characterized by histiocytic infiltration of the bones, skin, live, or other organs Skin, oral mucosa, bone, and lymph nodes are typical locations for single site involvement.
52 Systemic conditions associated with Leukemia childhood periodontitis Particularly the monocytic type, causes gingival enlargement due to infiltration of the gingival tissues. Typically painless, shiny, red, and edematous. Bleeding is common making oral hygiene difficult. Necrotic ulceration and involvement of the underlying bone can occur. The inflammation may act as a stimulus for further gingival swelling. Additional symptoms include fever, malaise, easy bruising or bleeding, and bone or joint pain.
53 Systemic conditions associated with childhood periodontitis Down Syndrome Papillon-Lefevre Syndrome Characterized by premature loss of the primary and permanent teeth Hyperkeratosis of the palms, soles, and sometimes of the knees and elbows Caused by mutations in the cathepsin C gene (CTSC) on chromosome 11q14.
54 Menopause related bone loss Bone loss, particularly trabecular bone, begins soon after the onset of menopause After the menopause, the ovary secretes little or no estrogen. Undetectable serum estradilo concentrations after menopause correlate with low bone density
55 Menopause related bone loss Data on serum estradiol concentrations and fracture risk are conflicting. Excess bone loss in women can be prevented by estrogen therapy. Estrogen is no longer a first-line therapy for prevention of bone loss, due to its other potential cardiovascular and breast cancer risks. Progestins, SERMs,, and bisphosphonates can also attenuate the loss of bone. Menopause-related bone loss lasts for about 10 years. After this time, the rate of bone loss is diminished to near the rate with aging
56 Pregnancy Bone loss can be seen during pregnancy (sometimes called transient osteoporosis of pregnancy). There does not appear to be an increased risk of fracture after menopause.
57 Lactation Lactation is associated with loss of bone of up to 4.0 percent, Lost bone is regained after lactation ceases; there is no increased risk of fractures in postmenopausal women who lactated earlier in life. PTHrP,, which is secreted by the lactating mammary gland, may play a role in the rapid bone loss that occurs in lactating women. Calcium supplements during lactation have no effect on the lactation-related change in bone turnover.
58 Organ transplant/b12 Glucocorticoids and cyclosporine contribute to post-transplant transplant osteoporosis; an additional factor after renal transplantation is secondary hyperparathyroidism. Vitamin B12 deficiency Vitamin B12 deficiency (pernicious anemia) is associated with an increased risk of osteoporosis, and hip and spine fractures, due to suppression of osteoblast activity as reported in in-vitro studies.
59 Cancer Treatment Osteoporosis in most patients treated for cancer is due to Hypogonadism that results from chemotherapy and radiation therapy, or Glucocorticoid therapy, Direct negative skeletal effects have been described for specific tumors and drug therapies. High-dose methotrexate regimens (eg( eg. Osteosarcoma or ALL) result in osteoporosis and fractures due to: Increase in bone resorption and Inhibition of bone formation, Some children with ALL have osteopenia before the initiation of treatment, suggesting a role for the leukemia itself on bone metabolism.
60 Homocysteine Homocystinuria, a rare autosomal recessive disease in children characterized by high plasma concentrations of homocysteine, lens dislocations, and thromboembolism, is also associated with the early onset of osteoporosis. High homocysteine levels in adults may be a predictor of osteoporotic fracture The mechanism for the effect of high homocysteine concentrations on fracture risk is not known, administering folate and vitamin B12 supplements (that lower serum homocysteine levels) reduce the risk of fracture.
61 Rickets Causes slow growth, bone deformities, elevation of alkaline phosphatase, and in some forms, abnormal tooth formation. Radiographic findings in rickets are characteristic and include: an increased width of the epiphyseal plate, irregular hazy margins of the distal metaphysis and marginal metaphyseal overgrowth that results in a ball- in-cup like appearance. Vitamin D resistant rickets in children, or osteomalacia in adults, may be associated with hypophosphatemia, including, Hereditary hypophasphatemic rickets and tumor induced osteomalacia.
62 Panostotic fibrous dysplasia The extreme form of polyostotic fibrous dysplasia (McCune-Albright syndrome), Caused by a somatic mutation Characterized by cystic or ground glass lesions in all bones.
63 Cole-Carpenter Carpenter syndrome Inheritance pattern of Cole-Carpenter Carpenter syndrome is unknown. Characterized by osteoporosis, short stature, craniosynostosis, hydrocephalus, and proptosis
64 Hypophosphatasia A rare, autosomal disease associated with low levels of alkaline phosphatase. Severe forms are usually inherited as an autosomal recessive trait. Leads to development of osteomalacia and severe periodontal disease. May present in the perinatal period, where it is often lethal, and in infancy.
65 Hypophosphatasia Childhood or adult forms have autosomal dominant traits with variable penetrance and clinical expression. Adults present with dental disease before the onset of symptomatic osteomalacia. Levels of phospho-ethanolamine and pyrophosphate are increased in blood and urine and are useful diagnostically.
66 Hypophosphatasia Caused by mutations in the infantile hypophosphatasia HOPS gene on chromosome 1p36. The phenotypic appearance varies. Results in a deficiency of tissue nonspecific alkaline phosphatase Characterized by abnormal mineralization of bone and dental tissues. The earlier the presentation, the more severe the disease.
67 Hypophosphatasia Leads to complete absence of the cementum, which covers the root structure and helps to prevent teeth from becoming fused to or reabsorped by the adjacent alveolar bone. The absence of cementum prevents normal anchoring of the fibers of the periodontal ligament and leads to premature tooth mobility and loss.
68 Hypophosphatasia Diagnostic findings Low serum alkaline phosphatase concentration Elevated concentrations of phospho- ethanolamine Elevated concentrations of pyrophosphate Increased urinary excretion of phosphoethanolamine.
69 Hypophosphatasia Diagnostic findings-continued Pyridoxal 5 phosphate (PLP) is sensitive and specific X-ray shows stress fx, chondrocalcinosis Enlarged pulp chambers
70 Treatment No uniformly successful treatment Palliative therapy for the infantile form may include correction of hypercalcemia (with calcitonin), reduction of hypercalcuria (with Chlorothiazide), reduction of dietary intake of calcium and vitamin D, reduced exposure to sunlight Prevent secondary rickets with administration of 200 IU IU of vitamin D per day. Serial monitoring of 25-hydroxyvitamin D levels is necessary to monitor and titrate intake.
71 Hypoposphatasia
72 Final diagnosis Hypophosphatasia, Diagnostic Lab test: Phosphoethanolaminuria Pyridoxal 5 phosphate (PLP) X-ray shows: stress fx, chondrocalcinosis
73 The End
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
DISEASES WITH ABNORMAL MATRIX
 DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
Hypophosphatasia. Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX
 Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Hypophosphatasia Tom Blevins, MD Texas Diabetes and Endocrinology Austin, TX Hypophosphatasia Case Teeth 57 y/o male with a hyperlipidemia and hypogonadism. Noted to have an alkaline phosphatase of
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Sachin Soni DNB Pediatrics
 Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Skeletal Manifestations
 Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Diagnosis and Treatment of Osteoporosis. Department of Endocrinology and Metabolism Ajou University School of Medicine.
 Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
Osteoporosis, Osteomalasia & rickets. Bone disorders
 Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Case 4 Generalised bone pain
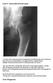 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Osteoporosis. Overview
 v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
OSTEOMALACIA UPDATE. Nothing to Disclose. Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco
 OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
OSTEOMALACIA UPDATE Daniel D Bikle, MD, PhD Professor of Medicine University of California and VA Medical Center San Francisco Nothing to Disclose 1 Case History 59 YO WM referred for evaluation of diffuse
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
Osteoporosis. Treatment of a Silently Developing Disease
 Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
What is Osteoporosis?
 What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
Practical Management Of Osteoporosis
 Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Disclosure and Conflicts of Interest Steven T Harris MD Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis
 Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis Steven T Harris MD FACP Clinical Professor of Medicine University of California, San Francisco Disclosure and Conflicts of Interest
Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis Steven T Harris MD FACP Clinical Professor of Medicine University of California, San Francisco Disclosure and Conflicts of Interest
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
PARATHYROID, VITAMIN D AND BONE
 PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
IEHP UM Subcommittee Approved Authorization Guidelines DEXA Scan
 Policy: IEHP UM Subcommittee Approved Authorization Guidelines IEHP considers bone mineral density testing using DEXA medically necessary for members who meet any of the following criteria: Women aged
Policy: IEHP UM Subcommittee Approved Authorization Guidelines IEHP considers bone mineral density testing using DEXA medically necessary for members who meet any of the following criteria: Women aged
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Trebeculae. Step 4. compact bone. Diploë Pearson Education, Inc.
 Trebeculae compact bone Step 4 Diploë Abnormalities in bone growth Fibrodysplasia ossificans progressiva (FOP) autosomal dominant, Codon 206: Arg à Hist 1 : 2, 000, 000 endothelial cells à mesenchymal
Trebeculae compact bone Step 4 Diploë Abnormalities in bone growth Fibrodysplasia ossificans progressiva (FOP) autosomal dominant, Codon 206: Arg à Hist 1 : 2, 000, 000 endothelial cells à mesenchymal
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
بسم هللا الرحمن الرحيم. Rickets
 بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
بسم هللا الرحمن الرحيم Rickets 1 Rickets IS defined as failure of mineralization of growing bone or osteoid tissue due to vitamin D deficiency. Vitamin D appear as rickets in children and as oteomalacia
Bone Remodeling & Repair Pathologies
 Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Bone Remodeling & Repair Pathologies Skeletal system remodels itself to maintain homeostasis Remodeling Maintainence replaces mineral reserves (osteocytes) of the matrix Remodelling recycles (osteoclasts)
Osteoporosis: Risk Factors, Diagnostic Methods And Treatment Options
 ISPUB.COM The Internet Journal of Academic Physician Assistants Volume 1 Number 1 Osteoporosis: Risk Factors, Diagnostic Methods And Treatment Options K Ihrke Citation K Ihrke.. The Internet Journal of
ISPUB.COM The Internet Journal of Academic Physician Assistants Volume 1 Number 1 Osteoporosis: Risk Factors, Diagnostic Methods And Treatment Options K Ihrke Citation K Ihrke.. The Internet Journal of
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Agent(s) FDA Labeled Indications Dosage and Administration. Perinatal/Infantile-onset hypophosphatasia. Juvenile-onset hypophosphatasia
 Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
Strensiq (asfotase alfa) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE Agent(s) FDA Labeled Indications Dosage and Administration Strensiq (asfotase alfa) injection Perinatal/Infantile-onset
The Bare Bones of Osteoporosis. Wendy Rosenthal, PharmD
 The Bare Bones of Osteoporosis Wendy Rosenthal, PharmD Definition A systemic skeletal disease characterized by low bone mass and microarchitectural deterioration of bone tissue, with a consequent increase
The Bare Bones of Osteoporosis Wendy Rosenthal, PharmD Definition A systemic skeletal disease characterized by low bone mass and microarchitectural deterioration of bone tissue, with a consequent increase
New 2010 Osteoporosis Guidelines: What you and your health provider need to know QUESTIONS&ANSWERS
 New 2010 Osteoporosis Guidelines: What you and your health provider need to know QUESTIONS&ANSWERS Wednesday, December 1, 2010 1:00 p.m. to 2:00 p.m. ET 1. I m 55 years old. I ve been taking Fosavance
New 2010 Osteoporosis Guidelines: What you and your health provider need to know QUESTIONS&ANSWERS Wednesday, December 1, 2010 1:00 p.m. to 2:00 p.m. ET 1. I m 55 years old. I ve been taking Fosavance
Overview. Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases. People Centred Positive Compassion Excellence
 Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to
 Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to the Hypothalamus 3. Blood Supply of the Pituitary Gland
Table of Contents Section I Pituitary and Hypothalamus 1. Development of the Pituitary Gland 2. Divisions of the Pituitary Gland and Relationship to the Hypothalamus 3. Blood Supply of the Pituitary Gland
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
AACE Southern States Chapter Lecture. Basics
 AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
AACE Southern States Chapter Lecture Unusual Bone Cases Basics Osteoporosis Osteomalacia Renal Osteodystrophy Multiple Myeloma 1 Osteoporosis Definition Modeling, Bone Remodeling Bone Resorption > Bone
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
TREATMENT OF OSTEOPOROSIS
 TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
Bone Densitometry Pathway
 Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Chapter 39: Exercise prescription in those with osteoporosis
 Chapter 39: Exercise prescription in those with osteoporosis American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 39: Exercise prescription in those with osteoporosis American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Drugs Affecting Bone. Rosa McCarty PhD. Department of Pharmacology & Therapeutics
 Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
Drugs Affecting Bone Rosa McCarty PhD Department of Pharmacology & Therapeutics rmccarty@unimelb.edu.au Objectives At the end of this lecture you should have gained: An understanding of bone metabolism
SKELETAL SYSTEM. Introduction Notes (pt 1)
 SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
SKELETAL SYSTEM Introduction Notes (pt 1) I. INTRODUCTION 1. Bones include active, living tissues: bone tissue, cartilage, dense connective tissue, blood, and nervous tissue. 2. Bones: support and protect
CPT Codes: The following ICD-10-CM codes support the medical necessity of CPT code 82306:
 CPT s: 82306 Vitamin D; 25 hydroxy, includes fraction(s), if performed 82652 Vitamin D; 1, 25 dihydroxy, includes fraction(s), if performed The following ICD-10-CM codes support the medical necessity of
CPT s: 82306 Vitamin D; 25 hydroxy, includes fraction(s), if performed 82652 Vitamin D; 1, 25 dihydroxy, includes fraction(s), if performed The following ICD-10-CM codes support the medical necessity of
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
SKELETAL SYSTEM CHAPTER 07. Bone Function BIO 211: ANATOMY & PHYSIOLOGY I. Body Movement interacts with muscles bones act as rigid bar of a lever
 Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
Page 1 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of
SKELETAL SYSTEM CHAPTER 07 BIO 211: ANATOMY & PHYSIOLOGY I
 BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 CHAPTER 07 SKELETAL SYSTEM Dr. Lawrence G. G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. Some illustrations are courtesy of McGraw-Hill.
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis. March 15, 2016 Bone ECHO Kate T Queen, MD
 Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Pathophysiology of Postmenopausal & Glucocorticoid Induced Osteoporosis March 15, 2016 Bone ECHO Kate T Queen, MD Review: normal bone formation Bone Modeling Remodeling Peak Bone Mass Maximum bone mass
Aromatase Inhibitors & Osteoporosis
 Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Rama Nada. - Mousa Al-Abbadi. 1 P a g e
 - 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
- 1 - Rama Nada - - Mousa Al-Abbadi 1 P a g e Bones, Joints and Soft tissue tumors Before we start: the first 8 minutes was recalling to Dr.Mousa s duties, go over them in the slides. Wherever you see
Normal Bone Health and Bone Disease. Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017
 Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
Vitamin D Assay Testing For services performed on or after
 2018 MEDICARE LOCAL COVERAGE DETERMINATION (LCD) - L36692 CPT CODES: 82306, 82652 Vitamin D Assay Testing For services performed on or after 2-3-2017 DLS TEST CODE AND NAME 49907 (1,25 DIHYDROXY) (CPT
2018 MEDICARE LOCAL COVERAGE DETERMINATION (LCD) - L36692 CPT CODES: 82306, 82652 Vitamin D Assay Testing For services performed on or after 2-3-2017 DLS TEST CODE AND NAME 49907 (1,25 DIHYDROXY) (CPT
Vitamin D Hormone Du Jour
 Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Hths 2231 Laboratory 13 Alterations in Musculoskeletal
 Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
454 Secondary Causes of Osteoporosis Mayo Clin Proc, May 2002, Vol 77 Table 1. Secondary Causes of Osteoporosis Endocrine disorders Acromegaly Adrenal
 Mayo Clin Proc, May 2002, Vol 77 Secondary Causes of Osteoporosis 453 Review Secondary Causes of Osteoporosis LORRAINE A. FITZPATRICK, MD Secondary causes of bone loss are not often considered in patients
Mayo Clin Proc, May 2002, Vol 77 Secondary Causes of Osteoporosis 453 Review Secondary Causes of Osteoporosis LORRAINE A. FITZPATRICK, MD Secondary causes of bone loss are not often considered in patients
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS
 DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
DIAGNOSING X-LINKED HYPOPHOSPHATEMIA (XLH) BIOCHEMICAL TESTING CONSIDERATIONS XLH IS CHARACTERIZED BY CHRONIC HYPOPHOSPHATEMIA XLH is a hereditary, progressive, lifelong disorder. In children and adults,
CKD-Mineral Bone Disorder (MBD) Pathogenesis of Metabolic Bone Disease. Grants: NIH, Abbott, Amgen, OPKO, Shire
 Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
Pathogenesis of Metabolic Bone Disease Stuart M. Sprague, D.O. Chief, Division of Nephrology and Hypertension Professor of Medicine NorthShore University HealthSystem University of Chicago Pritzker School
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Strensiq (asfotase alfa) Page 1 of 5 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Strensiq (asfotase alfa) Prime Therapeutics will review Prior Authorization
Strensiq (asfotase alfa) Page 1 of 5 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Strensiq (asfotase alfa) Prime Therapeutics will review Prior Authorization
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
nogg Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK
 nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Fragile Bones and how to recognise them. Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey
 Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B.
 Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
Rickets Simple complement 1. What factor influences on vitamin D absorption at the level of small intestine? A. Normal absorption of lipids B. Increased concentration of proteins in foods C. Decreasing
NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT
 NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF OSTEOPOROSIS: OVERVIEW Definitions Risk factors
NEW DEVELOPMENTS IN OSTEOPOROSIS: SCREENING, PREVENTION AND TREATMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF OSTEOPOROSIS: OVERVIEW Definitions Risk factors
Interpreting DEXA Scan and. the New Fracture Risk. Assessment. Algorithm
 Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Osteoporosis. Open Access. John A. Kanis. Diseases, University of Sheffield, UK
 Journal of Medical Sciences (2010); 3(3): 00-00 Review Article Osteoporosis Open Access John A. Kanis WHO Collaborating Centre for Metabolic Bone Diseases, University of Sheffield, UK incorporated into
Journal of Medical Sciences (2010); 3(3): 00-00 Review Article Osteoporosis Open Access John A. Kanis WHO Collaborating Centre for Metabolic Bone Diseases, University of Sheffield, UK incorporated into
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Skeletal Tissue Study Slides. Chapter 6
 Skeletal Tissue Study Slides Chapter 6 Functions of the skeletal system include all of the following, except A. support. B. storage. C. protection. D. blood cell production. E. movement. ANSWER Functions
Skeletal Tissue Study Slides Chapter 6 Functions of the skeletal system include all of the following, except A. support. B. storage. C. protection. D. blood cell production. E. movement. ANSWER Functions
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
OSTEOPOROSIS. QunFang Ding Associate Professor of Geriatric dept.
 OSTEOPOROSIS QunFang Ding Associate Professor of Geriatric dept. A Common Problem in the General Population 200 million people at risk worldwide 88.26 million people with osteoporosis 1.5 million women
OSTEOPOROSIS QunFang Ding Associate Professor of Geriatric dept. A Common Problem in the General Population 200 million people at risk worldwide 88.26 million people with osteoporosis 1.5 million women
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Osteoporosis and Lupus. Andrew Ruthberg, MD University Rheumatologists
 Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Conflict of Interest. Objectives. Learner Outcome
 Foundations of Orthopaedic Nursing Care, Part Four: Metabolic Bone Disease, highlighting Osteoporosis and Paget s Disease Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect
Foundations of Orthopaedic Nursing Care, Part Four: Metabolic Bone Disease, highlighting Osteoporosis and Paget s Disease Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect
Osteoporosis in Men Wendy Rosenthal PharmD. This program has been brought to you by PharmCon
 Osteoporosis in Men Wendy Rosenthal PharmD This program has been brought to you by PharmCon Osteoporosis in Men Speaker: Dr. Wendy Rosenthal, President of MedOutcomes, will be the presenter for this webcast.
Osteoporosis in Men Wendy Rosenthal PharmD This program has been brought to you by PharmCon Osteoporosis in Men Speaker: Dr. Wendy Rosenthal, President of MedOutcomes, will be the presenter for this webcast.
Patients should receive supplemental calcium and vitamin D, if dietary intake is inadequate (see PRECAUTIONS).
 PRODUCT CIRCULAR Tablets Once Weekly 70 mg I. THERAPEUTIC CLASS Bisphosphonates are synthetic analogs of pyrophosphate that bind to the hydroxyapatite found in bone. is a bisphosphonate that acts as a
PRODUCT CIRCULAR Tablets Once Weekly 70 mg I. THERAPEUTIC CLASS Bisphosphonates are synthetic analogs of pyrophosphate that bind to the hydroxyapatite found in bone. is a bisphosphonate that acts as a
Skeletal System worksheet
 Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Skeletal System worksheet Name Section A: Intro to Skeletal System The skeletal system performs vital functions that enable us to move through our daily lives. Support - The skeleton provides support and
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Osseous Tissue and Bone Structure
 6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
6 Osseous Tissue and Bone Structure PowerPoint Lecture Presentations prepared by Jason LaPres Lone Star College North Harris An Introduction to the Skeletal System Learning Outcomes 6-1 Describe the primary
Metabolic Diseases. Nutritional Deficiencies Endocrinopathies In-Born Errors of Metabolism
 Metabolic Diseases Metabolic Diseases Nutritional Deficiencies Endocrinopathies In-Born Errors of Metabolism Endrocrinopathies Anterior Pituitary Posterior Pituitary Thyroid Parathyroid Adrenal Pancreatic
Metabolic Diseases Metabolic Diseases Nutritional Deficiencies Endocrinopathies In-Born Errors of Metabolism Endrocrinopathies Anterior Pituitary Posterior Pituitary Thyroid Parathyroid Adrenal Pancreatic
Regulation of the skeletal mass through the life span
 Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
Regulation of the skeletal mass through the life span Functions of the skeletal system Mechanical protection skull Movement leverage for muscles Mineral metabolism calcium store Erythropoiesis red blood
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
Agents that Affect Bone & Mineral Homeostasis
 Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Prevention and Treatment of OSTEOPOROSIS 骨質疏鬆的預防與治療
 Prevention and Treatment of OSTEOPOROSIS 骨質疏鬆的預防與治療 Gwo Jaw Wang, M.D. 王國照教授 University of Virginia (U.S.A.) & National Cheng Kung University (Taiwan) Learning Objectives Pathophysiology of osteoporosis
Prevention and Treatment of OSTEOPOROSIS 骨質疏鬆的預防與治療 Gwo Jaw Wang, M.D. 王國照教授 University of Virginia (U.S.A.) & National Cheng Kung University (Taiwan) Learning Objectives Pathophysiology of osteoporosis
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OSTEOPOROSIS: PREVENTION AND MANAGEMENT
 OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
