Telithromycin Treatment of Chronic Chlamydia pneumoniae Infection in C57BL/6J mice
|
|
|
- Grace Golden
- 6 years ago
- Views:
Transcription
1 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2004, p Vol. 48, No /04/$ DOI: /AAC Copyright 2004, American Society for Microbiology. All Rights Reserved. Telithromycin Treatment of Chronic Chlamydia pneumoniae Infection in C57BL/6J mice Liisa Törmäkangas, 1 * Hannu Alakärppä, 1 Denise Bem David, 2 Maija Leinonen, 1 and Pekka Saikku 3 National Public Health Institute 1 and Department of Medical Microbiology, University of Oulu, 3 Oulu, Finland, and Medical Affairs, Aventis Pharma International, Paris, France 2 Received 19 February 2004/Returned for modification 14 March 2004/Accepted 16 May 2004 Chronic Chlamydia pneumoniae infections have been associated with atherosclerosis, but clear knowledge about how these infections should be treated is lacking. We studied the effect of a new ketolide antibiotic, telithromycin, on chronic C. pneumoniae lung infection. Female C57BL/6J mice on a 0.2% cholesterol diet were inoculated intranasally with C. pneumoniae either two or three times every fourth week. Telithromycin was given to the mice subcutaneously at 75 mg/kg of body weight once daily for 5 or 10 days, starting at 3 days after the last inoculation. Samples were taken at 4 and 12 weeks after the last inoculation. The presence of C. pneumoniae DNA in lung tissue was demonstrated by PCR and the detection of lipid accumulation in the aortic sinus by Oil-Red-O staining. C. pneumoniae DNA positivity and inflammatory reactions in the lung tissue of the mice inoculated twice were significantly affected by treatment after both inoculations or only after the second inoculation at 12 weeks. Intimal lipid accumulation in the aortic sinus was also slightly but significantly less abundant in the mice treated after both inoculations compared to the levels in those treated only after the second inoculation for 10 days (geometric means, 823 and 4,324 m 2, respectively; P 0.033). No differences between the infected, untreated controls and the group inoculated three times and treated for 5 days were seen. We conclude that telithromycin is effective in preventing the development of chronic C. pneumoniae infection and intimal lipid accumulation in C56BL/6J mice when the treatment is given after each inoculation. * Corresponding author. Mailing address: National Public Health Institute, P.O. Box 310, FIN Oulu, Finland. Phone: Fax: liisa.tormakangas@ktl.fi. Chlamydia pneumoniae is an obligate intracellular bacterium that causes infections of both the upper and the lower respiratory tracts. Similar to the other chlamydial species, it has a tendency to cause persistent infections. Persistent C. pneumoniae infection has been associated with several chronic diseases, such as asthma (24), chronic obstructive pulmonary disease (53), and coronary heart disease (CHD) (13), in several studies. C. pneumoniae is susceptible to macrolides and tetracyclines (12, 29), which are commonly used for the treatment of acute chlamydial infections. Fluoroquinolones (25), rifampin (21), and most recently, ketolides (34, 45) have also been found to be effective. At present, knowledge of the successful therapies for the treatment of latent and persistent infections is limited. The definition and development of appropriate and effective treatments and means of eradication of chronic C. pneumoniae infection would, however, be very important, especially if such treatments turned out to have an effect on the development of the associated chronic diseases. Previous animal models have shown that repeated inoculations of chlamydia increase the presence and persistence of chlamydial DNA in several mouse tissues (10, 36). C. pneumoniae also causes atherosclerotic changes in rabbits (18, 31) and hyperlipidemic mice (27, 36), although controversial findings have been published from studies with murine models (1, 9). In addition, early treatment of C. pneumoniae-infected rabbits with macrolide antibiotics has been shown to prevent the development of atherosclerosis (17, 39), while in apolipoprotein E-deficient mice, azithromycin did not decrease the progression of lipid lesions (47). The first two small-scale antibiotic treatment trials with CHD patients (22, 23) gave promising results concerning the decreased incidence of cardiovascular events. In a more recent study, patients with acute unstable angina or non-q-wave myocardial infarction were treated with clarithromycin for 3 months, which led to a significant reduction in cardiovascular events during monitoring for an average of 555 days (49). In the Azithromycin in Coronary Artery Disease: Elimination of Myocardial Infection with Chlamydia (ACADEMIC) study, however, 3 months of azithromycin treatment of patients with stable coronary artery disease improved inflammatory markers but did not decrease C. pneumoniae antibody levels at 6 months (3) and did not reduce ischemic events during the 2-year period of monitoring (38). Very recently, two large-scale azithromycin treatment trials with adequate patient series reported negative results for the whole patient population as well: the WIZARD trial included 7,747 patients with previous myocardial infarction and elevated C. pneumoniae antibody levels (40), and the Azithromycin in Acute Coronary Syndrome (AZACS) trial included 1,439 patients with unstable angina or myocardial infarction (11). The ongoing large trials of antibiotics and CHD patients may yield new information on the possible preventive effects of antibiotics on cardiovascular events. On the other hand, more animal models are needed to determine whether antimicrobial drugs can eradicate chronic C. pneumoniae infection, to establish the effect of antibiotic treatment on atherosclerosis, and to determine the optimal drug or combination of drugs as well as the dosage and timing of treatment. In previous studies with mice, multiple C. pneumoniae inoc- 3655
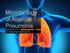
2 3656 TÖRMÄKANGAS ET AL. ANTIMICROB. AGENTS CHEMOTHER. ulations caused only inflammatory reactions and no atherosclerotic changes in the aortas or aortic sinuses of C57BL/6J mice fed normal chow (7). Mice of this strain, however, have been shown to be susceptible to intimal lipid accumulation when they are fed a high-fat, high-cholesterol diet (41), and with this kind of diet C. pneumoniae inoculations have been shown to increase atherosclerotic changes significantly (6). In the present study, we investigated the development of chronic infection and inflammatory reactions in mice without the possible confounding effects of a high-fat diet and genetic modifications. Therefore, we used normal C57BL/6J mice fed a 0.2% cholesterol diet to study the effects of a ketolide antibiotic, telithromycin, on the treatment and eradication of chronic C. pneumoniae infections and on the development of lipid lesions in the aortic sinuses of these mice. MATERIALS AND METHODS Organism and inoculum. C. pneumoniae isolate Kajaani 7 (K7), a Finnish epidemic strain (15) grown in HL cells, was used in the study. Infected cells were harvested with sterile glass beads and disrupted by ultrasonication. The cell debris was separated by low-speed centrifugation, followed by sonication and two cycles of high-speed centrifugation, to purify the chlamydial particles. Finally, the pellet obtained was resuspended in sucrose-phosphate-glutamic acid buffer for storage. The number of inclusion-forming units (IFU) of viable organisms per milliliter was determined by culture in HL cells. Briefly, HL cells were infected with 10-fold dilutions of the chlamydia stock culture by centrifugation and incubated at 35 C in5%co 2 for 72 h. Culture medium (RPMI 1640) contained 7% fetal bovine serum, 1% L-glutamate, 20 g of streptomycin per ml, and 0.5 g of cycloheximide per ml. The inoculum dose was estimated on this basis, and the infectious dose given to the animals was confirmed by culture in HL cells, as described above. Animal model and treatment. Six-week-old female inbred C57BL/6J mice were purchased from M&B A/S, Ry, Denmark. Normal feeding (1324; Altromin, Lage, Denmark) with 0.2% cholesterol supplement was started when the animals arrived at the facilities. After 2 weeks on a cholesterol-supplemented diet, each mouse was inoculated intranasally with IFU of C. pneumoniae K7 while the mouse was under inhaled methoxyflurane (Metofane; Schering-Plough, Bloomfield, N.J.) anesthesia. One or two reinfections were given similarly 4 weeks (dose, IFU/mouse) and 8 weeks (dose, IFU/mouse) after the primary inoculation. Telithromycin was given to the mice subcutaneously at 75 mg/kg of body weight once daily for 5 or 10 days, starting on the third day after intranasal inoculation. Telithromycin was dissolved with glacial acetic acid and further diluted with phosphate-buffered saline (PBS) solution (final acetic acid concentration, 0.1%). The telithromycin dose used was chosen on the basis of preliminary studies (52), in which doses of 25, 50, and 100 mg/kg for the treatment of FIG. 1. Diagram of study design. treatm., treatment; w, weeks. acute C. pneumoniae lung infection were tested. Telithromycin doses of 50 and 100 mg/kg have been used in other mouse models as well (43, 51), and such high doses are apparently needed in mice with high metabolic and elimination rates to achieve good treatment responses. Previously, Bonnefoy et al. (8) was able to measure telithromycin levels for 8 h after intravenous or oral administration of 10 mg of the drug per kg to Swiss mice, and the half-life was reported to be 1.2 h by the intravenous route of administration. The mice were divided into three treatment groups and two placebo-control groups, with 20 mice in each group. Groups 1 and 2 were inoculated with chlamydia twice. Group 1 was treated for 10 days after both inoculations, and group 2 was treated for 10 days after the last inoculation, i.e., postinfection (p.i.). The placebo group (group 3) was given diluent after both inoculations. Group 4 was inoculated three times and was treated only after the last inoculation for 5 days (although the intent had been to treat them for 10 days). The other placebo group (group 5) was inoculated three times and received diluent after the last inoculation for 5 days, similar to group 4. Samples were taken at 4 and 12 weeks p.i. The inoculation and treatment regimens are also presented in Fig. 1. The Animal Care and Use Committee of the National Public Health Institute, Helsinki, Finland, approved all procedures involving animals. Measurement of C. pneumoniae antibody titers. Antibody titers were measured by the microimmunofluorescence test (originally described elsewhere [55]) by using purified, formalin-fixed whole elementary bodies of K7 as the antigen. Immunoglobulin G (IgG) antibodies were detected in serum by using fluorescein isothiocyanate-conjugated anti-mouse IgG [F(ab ) 2 fragments; Serotec]. Culture of lung tissue. Lobes from the right lung were mechanically homogenized in 2 ml of sucrose-phosphate-glutamic acid buffer. The tissue suspensions were centrifuged to remove the debris, and the supernatant was collected and frozen at 70 C. The remaining lung tissue debris was stored for C. pneumoniae DNA detection. The lungs of the mice were assayed at 4 weeks p.i. for the presence of viable C. pneumoniae organisms. All analyses were performed in duplicate. HL cells infected with different dilutions of the homogenates were centrifuged at 490 g for 1 h and incubated at 35 C under 5% CO 2 for 72 h, after which the plates were centrifuged again as described above, new culture media were added, and the cultures were grown for another 72 h. Finally, the cells were washed with PBS solution, fixed with methanol, and stained with a Chlamydia genus-specific monoclonal antibody conjugated to fluorescein isothiocyanate (Pathfinder; Sanofi Diagnostics Pasteur, Redmond, Wash.). Detection of C. pneumoniae DNA in lung tissues. Lung tissue debris (50 mg) was lysed with proteinase K (Qiagen) in tissue lysis buffer (Qiagen). After incubation at 56 C overnight, DNA was purified with a commercially available QIAamp tissue kit, according to the instructions of the manufacturer (Qiagen). The purified DNA was kept frozen at 20 C. The PCR primers were synthesized at the Institute of Biotechnology, Helsinki, Finland. The sequences for the primers used for DNA amplification (135-bp product), primer HB1 (5 -ATAG TCTCCGTAAAATCCAGCACG-3 ) and biotinylated primer HB2 (5 -CCTGT AGGGAACCCTTCTGATC-3 ), were derived from the C. pneumoniae omp1 gene. PCR was performed with a mixture of 400 M each deoxynucleoside triphosphate, 4.0 mm MgCl 2, 50 mm Tris-HCl (ph 8), 100 mm NaCl, 0.1 mm EDTA, 1 mm dithiothreitol, 50% glycerol, 1% Triton X-100, 1.0 U of Taq polymerase (PromegaTag), 50 pmol of each primer, and 10 l of DNA isolated
3 VOL. 48, 2004 TREATMENT OF CHRONIC C. PNEUMONIAE INFECTION IN MICE 3657 from clinical samples. The total reaction volume was 50 l. After 5 min of denaturation at 94 C, the samples were subjected to 50 cycles of denaturation (94 C, 30 s), annealing (55 C, 30 s), and extension (72 C, 30 s) with a Perkin- Elmer Cetus GeneAmp 9600 thermocycler. A time-resolved fluorescence-based hybridization assay with an Eu-labeled hybridization probe (5 -CCATATTGTA CCATCAATTAA-3 ) (2 ng/100 l) was used to test for the presence of the C. pneumoniae-specific PCR product. The probe was incubated overnight at 37 C, and the reaction was stopped by washing the reaction mixture 10 times. Otherwise, the assay was done as described previously (44). The detection limit of the PCR assay is 0.8 genome equivalents. All samples positive in the first run were assayed twice, and the result was considered positive only if the result was the same in both runs. Lung histopathology. The left lung of each mouse was removed and fixed in 10% buffered formalin. Specimens were embedded in paraffin, and 4- m sections were cut and stained with hematoxylin-eosin (HE). The inflammation detected by HE staining was evaluated for the severity of bronchointerstitial pneumonia and was graded on a scale that ranged from 0 to 4. Grade 0 indicated that no inflammatory reaction is visible. Grade 1 was considered mild inflammation with perivascular and peribronchial lymphocyte and plasma cell infiltration with occasional neutrophilic and eosinophilic granulocytes. Grade 2 was considered moderate inflammation, grade 3 was considered marked inflammation, and grade 4 was considered severe inflammation. Grade 4 also included patchy consolidation of lung tissue with alveolar macrophages and plasma cells, but only grades 0 to 2 were detected in the present study. Aorta and aortic sinus histopathologies. After the lungs had been dissected, the heart and the adjoining aorta were perfused with 1 ml of PBS, removed, and fixed in 10% buffered formalin. The aorta and the heart were cut apart, and the sites where the three carotid arteries branch off were separately embedded in paraffin. Transversal 4- m sections were cut from the branching sites of the aortic arch and stained with HE. The upper half of the heart from five mice per group was also embedded in paraffin, and 4- m sections from the area of the aortic sinus valve cups (as described below) were collected and stained with HE. All sections were evaluated histopathologically for lesions and inflammation. Quantitative analysis of lipid accumulation in aortic sinus. Lipid lesions from 8 to 10 mice in each of the treatment groups were analyzed. The upper half of the formalin-fixed heart was embedded in gelatin and frozen. Sections (thickness, 5 m) were collected from the area of the aortic sinus in which valve cups and valves were clearly present by the method described by Paigen et al. (42) and were stained with Oil-Red-O. Every other section was placed on a slide, for an average total of 24 to 30 sections per mouse, and every third section collected was analyzed. Of these, the area of lipid accumulation from six consecutive sections per mouse was quantified by computer-assisted image analysis. Statistics. The nonparametric Mann-Whitney U test was used for statistical analyses of the lipid accumulation areas. PCR positivity was tested by Pearson s chi-square test or Fisher s exact test, as appropriate, and the lung histopathology findings were tested by the chi-square test for trend (SPSS for Windows, version ). Exact P values were reported as appropriate. RESULTS Clinical observations. No symptoms of respiratory infection were detected in the mice inoculated with chlamydia, and the mice in all groups gained weight steadily throughout the study. For an unknown reason, the mice inoculated three times and treated only after the last inoculation had skin irritation and developed sores at the injection sites on their necks. The skin irritation and sores were detected mostly in the telithromycintreated groups, but they were also detected to some extent in the placebo groups. For this reason, the treatment for these groups had to be terminated after 5 days, after which the sores healed rapidly. Consequently, the treatment time for these mice (group 4) after the last inoculation was only 5 days, whereas it was 10 days in the groups of mice (groups 1 and 2) inoculated twice. Serology. All mice had antibody titers 128, as measured by the microimmunofluorescence method. At 4 weeks p.i., the mice inoculated twice and treated after both inoculations had significantly higher antibody titers (geometric mean of titers FIG. 2. DNA positivity detected by PCR. The bars represent the percentages of positive mice per treatment group. 1, two inoculations and two treatments; 2, two inoculations and one treatment; 3, two inoculations and no treatment; 4, three inoculations and one treatment; 5, three inoculations and no treatment. and, P compared to the results at 4 weeks p.i. (Pearson s chi-square test). per study group, 987) than the placebo group (mean titer, 530) (P 0.025, Mann-Whitney U test). At 12 weeks p.i., the corresponding titers in these two groups were 630 and 461, but the difference was no longer statistically significant. C. pneumoniae culture and detection of DNA from lung tissue. All lung tissue homogenates of the samples taken at 4 weeks p.i. were culture negative. The hybridization assay method that we used with PCR gave a quantitative value for the amount of amplified DNA in the PCR product but not directly for the amount of original DNA in the sample. For this reason, we compared the groups only on the basis of positive and negative results. The positive values therefore refer to the number of DNA-positive mice per group, expressed as a percentage. The C. pneumoniae DNA positivity values at 4 and 12 weeks p.i. for the mice receiving different treatments are shown in Fig. 2. In the mice inoculated twice, the rates of DNA positivity decreased significantly from 4 to 12 weeks p.i. in both treatment groups, whereas the decrease in the placebo-treated group was not significant. The treatment given after both inoculations was most effective, with only 10% (2 of 20) of the mice remaining PCR positive. In the mice inoculated three times, the treatment after the last inoculation did not significantly decrease the rate of DNA positivity, and in the placebotreated control group, the rate of positivity even increased slightly between 4 and 12 weeks p.i. (42 and 59%, respectively). The number of samples with discrepant results (samples positive in the first round of analysis and negative in the second round) was 6 of 60 (10%) samples (excluding samples with negative results) at 4 weeks p.i. and, similarly, 19 of 54 (35%) samples at 12 weeks p.i. Lung histopathology. No marked or severe inflammatory changes (grades 3 and 4, respectively), which are frequently present during acute C. pneumoniae infection in mice, were detected in this study. There were no significant differences between the groups at 4 weeks p.i. (results not shown), but at 12 weeks p.i., earlier treatment with telithromycin clearly decreased the level of inflammation in the lungs of the mice: a moderate inflammatory reaction (grade 2) was present in 50%
4 3658 TÖRMÄKANGAS ET AL. ANTIMICROB. AGENTS CHEMOTHER. FIG. 3. PCR positivity versus histopathology in groups combined by treatment: placebo-treated control groups (A); telithromycintreated groups (B). Black bars, PCR positive; white bars, PCR negative;, significant P value by the chi-square test for trend for increased rates of PCR positivity for lung tissue compared to an increased severity of lung histopathology. TABLE 1. Percentages of mice with different inflammation grades within a treatment group Treatment group a % Mice with the following severity of inflammation b : inoc. 2 treatm c 2 inoc. 1 treatm c 2 inoc. placebo c 3 inoc. 1 treatm inoc. placebo a inoc., inoculations; treatm., treatments. b Inflammatory changes are according to the lung histopathologies for the telithromycin-treated and the control groups. 0, no changes; 1, mild lymphocyte and plasma cell infiltration; 2, moderate changes with perivascular and peribronchial lymphoid reactions. The results were obtained at 12 weeks p.i. c Significant trend (P 0.009) for an increase in the severity if inflammation when only one treatment or no treatment (placebo) was given (chi-square test for trend). FIG. 4. Lipid lesion areas (in micrometers squared) in the aortic sinuses of the mice (and geometric means per group) treated with telithromycin or placebo. Samples were taken at 12 weeks p.i. 1, two inoculations and two treatments; 2, two inoculations and one treatment; 3, two inoculations and no treatment; 4, three inoculations and one treatment; 5, three inoculations and no treatment. A significant difference was detected between groups 1 and 2 by the Mann-Whitney U test. of the untreated mice, 11% of those treated only after the last inoculation, and 5% of the mice treated after both inoculations (P 0.009, chi-square test for trend) (Table 1). The treatments given after all three inoculations had no effect on the inflammatory reactions in the lungs. When the lung histopathology scores were compared to the rates of PCR positivity for the telithromycin-treated mice, more DNA-positive mice were seen among the mice with histology grades 1 and 2 at both time points, and the trends were statistically significant (P at 4 weeks p.i. and P at 12 weeks p.i., chi-square test for trend) (Fig. 3B). For the placebo-treated control mice, a significant trend was seen only at 4 weeks p.i. (P 0.043, chisquare test for trend) (Fig. 3A). Heart and aortic arch histopathologies. The histopathologies of the aortic arch and the aortic sinus showed no abnormal inflammatory reactions on HE staining, nor were any lesions visible in the aortic arches of these mice. Lipid accumulation in aortic sinus. The lipid lesion areas in the mice at 12 weeks p.i. (age 24 weeks) are shown in Fig. 4. In the mice inoculated twice, the lipid lesion areas were significantly smaller in group 1 (treated twice) than in group 2 (treated only once) (P 0.033, Mann-Whitney U test). No difference in the lesion areas between the group treated once and the placebo group was detected, whereas the group treated twice showed decreased lipid lesion areas compared to those for the placebo group, but this difference was not significant. The telithromycin-treated mice inoculated three times showed a trend toward decreased lipid accumulation compared to the level of lipid accumulation in the placebo-treated groups (at age 28 weeks), but no statistically significant differences were detected. The lipid lesion areas detected at the earlier time point, i.e., at 4 weeks p.i. (ages 16 and 20 weeks), were very small, and no differences between any of the groups were
5 VOL. 48, 2004 TREATMENT OF CHRONIC C. PNEUMONIAE INFECTION IN MICE 3659 FIG. 5. (A) Example of an Oil-Red-O-stained section of the aortic sinus of a mouse inoculated three times and treated after the last inoculation. (B) More detail of the intimal lipid accumulation analyzed in this study. The cartilage-like formation with fat staining visible in the bottom left part of panel B was not included in the analyses. detected (data not shown). An example of an analyzed section with intimal lipid accumulation is shown in Fig. 5. DISCUSSION In this study we showed that telithromycin treatment suppresses the pulmonary inflammatory reaction, reduces the number of C. pneumoniae DNA-positive mice (lungs), and affects the lipid accumulation in the aortic sinus in C57BL/6J mice with chronic chlamydial infections when the treatment is given after each inoculation. Treatment after both inoculations decreased the level of C. pneumoniae DNA in mice significantly at 12 weeks p.i., but DNA remained detectable in lung tissue, despite the treatment: at 3 months p.i., the lung tissues of 10% of the mice inoculated and treated twice, 28% of those inoculated twice and treated once after the last inoculation, and 60% of those inoculated three times and treated only after the last inoculation were PCR positive. The proportions of discrepant results detected by PCR analysis were 10% at 4 weeks p.i. and 35% at 12 weeks p.i. The high percentage of inconsistency at 12 weeks may partly be due to the very small amount of chlamydial DNA present, thus leading to problems with sensitivity. Repeats of all analyses more than once would possibly have given even more accurate findings. In agreement with our results, it was shown in a previous study (5) that chlamydial DNA persists for 2 months in 38% of the lung tissues of NMRI mice inoculated once and treated for 7 days with a combination of azithromycin and rifampin early after the infection. In another study, chlamydial DNA remained detectable for 26 weeks in half of ApoE-deficient mice inoculated twice and given delayed treatment with two doses of azithromycin (47). A recent study with humans showed that the persistence of C. pneumoniae DNA in nasopharyngeal swab specimens correlated with the persistence of symptoms (35). Some patients may display persistent infections and prolonged symptoms or relapses with positive culture and/or PCR findings and may not be cured by conventional treatment for 7 to 21 days (16, 26, 35, 46); even prolonged treatment has been ineffective in some cases (16). The C57BL/6J mice used in the study have been shown to be susceptible to chlamydial infection, which results in a selfrestricted pneumonia (54, 57). After secondary inoculation, most of the chlamydiae are eradicated within 3 to 4 weeks in these mice (54), but as shown above, the persistence of bacterial DNA is detected in some animals. In accordance with this, we found no viable chlamydia in the lung tissue by culture at 4 weeks p.i., and successful infection was confirmed by high C. pneumoniae IgG antibody titers. It has been questioned whether the presence of chlamydial DNA can be considered an indicator of a persistent, chronic infection. Previously, culturenegative, persistent C. pneumoniae infection in mice, demonstrated as PCR positivity of lung tissue after the primary inoculation, has been shown to be reactivated by immunosuppressive cortisone treatment (32, 33). In the present study, untreated mice inoculated three times showed a slight increase in PCR positivity during 8 weeks of monitoring (between 4 and 12 weeks p.i.), and only a marginal decrease was seen in a telithromycin-treated group. The persistence of PCR positivity was seen less often in mice that received only two inoculations. This is in accordance with the findings of previous studies (36), which showed that the persistence of DNA increases with repeated inoculations. Lung histopathology detected a moderate inflammatory reaction (grade 2) in 50 and 42% of the mice in the groups inoculated with C. pneumoniae two and three times, respectively, and treated with placebo at 12 weeks p.i. In our preliminary studies, grade 2 inflammation was not seen in mock-inoculated C57BL/6J mice of the same age (L. Törmäkangas, M. Leinonen, and P. Saikku, unpublished data). In addition, in both the telithromycin-treated and the untreated groups, PCR positivity was clearly more common in the mice with grade 1 and 2 lung inflammation than in those with no inflammation. These findings suggest the continuous presence of a chronic, nonculturable form of chlamydia that maintains inflammation in the lung tissue. In vitro studies have shown that C. pneumoniae is able to persist in a metabolically active and viable state in human monocytes and macrophages with the restricted development of infectious progeny (2) and to induce nonreplicating but viable persistent infection when it is exposed to gamma interferon stimulation (4). In vivo, alveolar
6 3660 TÖRMÄKANGAS ET AL. ANTIMICROB. AGENTS CHEMOTHER. and peritoneal macrophages from inoculated mice were shown to be able to transport the infection to uninfected mice (37), and C. pneumoniae is frequently found in circulating mononuclear cells in human peripheral blood samples (50). Furthermore, Gieffers et al. (20) and Yamaguchi et al. (56) recently showed that C. pneumoniae isolates inoculated into circulating human monocytes (20) and mouse primary lymphocytes (56) are resistant to antibiotic treatment. The treatment timing seems to have an influence on the development of chronic infection and atherosclerotic lesions. In a previous study, Rothstein et al. (47) treated ApoE-deficient mice that had been inoculated twice with an oral dose of azithromycin at 2 and 3 weeks p.i. At 26 weeks of age, i.e., 12 weeks p.i., the C. pneumoniae infection increased the sizes of the aortic Oil-Red O-stained lesions in the infected mice, but azithromycin did not reduce their sizes (47). The delay in the beginning of treatment seen in the study by Rothstein et al. (47) may have caused the negative result. This effect was also demonstrated in rabbit models by Muhlestein et al. (39) and Fong et al., who inoculated the rabbits three times and treated them with azithromycin (17) or clarithromycin (17, 19). In the last two studies (17, 19), delayed treatment with clarithromycin slightly diminished the area of atherosclerotic lesion development, whereas all the early treatments in the three studies were significantly effective in decreasing the lesion areas. To our knowledge, the murine model described here is the first to demonstrate that antimicrobial treatment affects the formation of aortic sinus lipid lesions in C. pneumoniae-infected mice. The results must be interpreted with caution because of the wide range of lesion areas in each group. Despite the variability, the effect of the treatment was statistically significant when telithromycin was given after each inoculation compared to the effect obtained when the mice were treated only after the second inoculation in the groups inoculated twice. No statistical difference, however, was found when the results for the group treated twice were compared to those for the placebo-treated control group. It was unfortunate that the treatment of the mice inoculated three times had to be terminated after 5 days due to skin irritation and that the effects of a 10-day treatment on lipid accumulation could not be assessed for this group. The drawbacks of our study are that we were not able to assess the aortic sinuses, where the lesions were detected, for the presence of chlamydial antigen, nor did we have an uninfected control group with which to compare the results for the inoculated, untreated animals. We therefore cannot estimate the direct influence of chlamydiae on the development of atherosclerotic lesions. The repeated inoculations clearly increased the persistence of the pathogen in lung tissue, and treatment decreased this development in the group treated twice, but additional studies with more mice are needed to verify the lipid accumulation results and determine whether the decreased levels of lipid accumulation in our mouse model were really due to the antichlamydial effect of telithromycin. Macrolide antibiotics, especially semisynthetic erythromycin A derivatives (like clarithromycin and roxithromycin), have been shown to possess several anti-inflammatory activities (28, 30, 48). Structurally, telithromycin is derived from erythromycin A (14), but there are no reports on the potential antiinflammatory effects of telithromycin. In our study, some mice were found to be PCR positive even when no inflammation was detected in lung tissue from the telithromycin-treated groups, whereas no chlamydial DNA was detected in lung tissue from the untreated mice without inflammation. This may be due to some anti-inflammatory effect of telithromycin. We cannot exclude the possibility that the decreased lipid accumulation in the treatment groups was partly due to the anti-inflammatory effect as well, although the treatment actually intensified the IgG antibody response to C. pneumoniae. Fong et al. (19) have suggested that the anti-inflammatory action of clarithromycin is not very marked in rabbits, because in noninfected, cholesterol-fed rabbits the decrease in the development of atherosclerotic lesions seen after clarithromycin treatment was minor compared to that seen in chlamydia-inoculated rabbits. The fact that only treatment provided early after infection seems to be effective in preventing the development of chronic infection and decreasing infection-accelerated atherosclerosis in animal models should be kept in mind when considering future human treatment trials. As most antimicrobial agents used to treat chlamydial infections affect only replicating bacteria, their potential to cure chronic infections may be modest. In conclusion, our data suggest that telithromycin has the potential to affect the development of chronic C. pneumoniae infection in a mouse model and that telithromycin treatment may have an effect on decreasing atherosclerotic changes in these mice. These effects were seen only in the groups in which the treatment was given after each inoculation, yet some mice in these groups remained DNA positive. On the basis of the present findings and the findings obtained with other animal models, we hypothesize that the conventional antimicrobial treatments may not be effective in totally eradicating chronic and persistent chlamydiae and that the effects of longer treatment regimens and/or combinations of different antibiotics should be further studied. ACKNOWLEDGMENTS This study was funded by Aventis Pharma, Paris, France. We thank Elise Saario for interpreting the HE staining of the lung tissues and aortas and Aini Bloigu for assistance with the statistical analyses. REFERENCES 1. Aalto-Setala, K., K. Laitinen, L. Erkkila, M. Leinonen, M. Jauhiainen, C. Ehnholm, M. Tamminen, M. Puolakkainen, I. Penttila, and P. Saikku Chlamydia pneumoniae does not increase atherosclerosis in the aortic root of apolipoprotein E-deficient mice. Arterioscler. Thromb. Vasc. Biol. 21: Airenne, S., H. M. Surcel, H. Alakarppa, K. Laitinen, J. Paavonen, P. Saikku, and A. Laurila Chlamydia pneumoniae infection in human monocytes. Infect. Immun. 67: Anderson, J. L., J. B. Muhlestein, J. Carlquist, A. Allen, S. Trehan, C. Nielson, S. Hall, J. Brady, M. Egger, B. Horne, and T. Lim Randomized secondary prevention trial of azithromycin in patients with coronary artery disease and serological evidence for Chlamydia pneumoniae infection: The Azithromycin in Coronary Artery Disease: Elimination of Myocardial Infection with Chlamydia (ACADEMIC) study. Circulation 99: Beatty, W. L., G. I. Byrne, and R. P. Morrison Morphologic and antigenic characterization of interferon gamma-mediated persistent Chlamydia trachomatis infection in vitro. Proc. Natl. Acad. Sci. USA 90: Bin, X. X., K. Wolf, T. Schaffner, and R. Malinverni Effect of azithromycin plus rifampin versus amoxicillin alone on eradication and inflammation in the chronic course of Chlamydia pneumoniae pneumonitis in mice. Antimicrob. Agents Chemother. 44: Blessing, E., L. A. Campbell, M. E. Rosenfeld, N. Chough, and C. C. Kuo Chlamydia pneumoniae infection accelerates hyperlipidemia induced atherosclerotic lesion development in C57BL/6J mice. Atherosclerosis 158: Blessing, E., T. M. Lin, L. A. Campbell, M. E. Rosenfeld, D. Lloyd, and C.
7 VOL. 48, 2004 TREATMENT OF CHRONIC C. PNEUMONIAE INFECTION IN MICE 3661 Kuo Chlamydia pneumoniae induces inflammatory changes in the heart and aorta of normocholesterolemic C57BL/6J mice. Infect. Immun. 68: Bonnefoy, A., M. Guitton, C. Delachaume, P. Le Priol, and A. M. Girard In vivo efficacy of the new ketolide telithromycin (HMR 3647) in murine infection models. Antimicrob. Agents Chemother. 45: Caligiuri, G., M. Rottenberg, A. Nicoletti, H. Wigzell, and G. K. Hansson Chlamydia pneumoniae infection does not induce or modify atherosclerosis in mice. Circulation 103: Campbell, L. A., E. Blessing, M. Rosenfeld, T. Lin, and C. Kuo Mouse models of C. pneumoniae infection and atherosclerosis. J. Infect. Dis. 181(Suppl. 3):S Cercek, B., P. K. Shah, M. Noc, D. Zahger, U. Zeymer, S. Matetzky, G. Maurer, and P. Mahrer Effect of short-term treatment with azithromycin on recurrent ischaemic events in patients with acute coronary syndrome in the Azithromycin in Acute Coronary Syndrome (AZACS) trial: a randomised controlled trial. Lancet 361: Chirgwin, K., P. M. Roblin, and M. R. Hammerschlag In vitro susceptibilities of Chlamydia pneumoniae (Chlamydia sp. strain TWAR). Antimicrob. Agents Chemother. 33: Danesh, J., R. Collins, and R. Peto Chronic infections and coronary heart disease: is there a link? Lancet 350: Douthwaite, S Structure-activity relationships of ketolides vs. macrolides. Clin. Microbiol. Infect. 7: Ekman, M. R., J. T. Grayston, R. Visakorpi, M. Kleemola, C. C. Kuo, and P. Saikku An epidemic of infections due to Chlamydia pneumoniae in military conscripts. Clin. Infect. Dis. 17: Falck, G., J. Gnarpe, and H. Gnarpe Persistent Chlamydia pneumoniae infection in a Swedish family. Scand J. Infect. Dis. 28: Fong, I. W., B. Chiu, E. Viira, D. Jang, M. W. Fong, R. Peeling, and J. B. Mahony Can an antibiotic (macrolide) prevent Chlamydia pneumoniae-induced atherosclerosis in a rabbit model? Clin. Diagn. Lab. Immunol. 6: Fong, I. W., B. Chiu, E. Viira, D. Jang, and J. B. Mahony De novo induction of atherosclerosis by Chlamydia pneumoniae in a rabbit model. Infect. Immun. 67: Fong, I. W., B. Chiu, E. Viira, D. Jang, and J. B. Mahony Influence of clarithromycin on early atherosclerotic lesions after Chlamydia pneumoniae infection in a rabbit model. Antimicrob. Agents Chemother. 46: Gieffers, J., H. Fullgraf, J. Jahn, M. Klinger, K. Dalhoff, H. A. Katus, W. Solbach, and M. Maass Chlamydia pneumoniae infection in circulating human monocytes is refractory to antibiotic treatment. Circulation 103: Gieffers, J., W. Solbach, and M. Maass In vitro susceptibilities of Chlamydia pneumoniae strains recovered from atherosclerotic coronary arteries. Antimicrob. Agents Chemother. 42: Gupta, S., E. W. Leatham, D. Carrington, M. A. Mendall, J. C. Kaski, and A. J. Camm Elevated Chlamydia pneumoniae antibodies, cardiovascular events, and azithromycin in male survivors of myocardial infarction. Circulation 96: Gurfinkel, E., G. Bozovich, E. Beck, E. Testa, B. Livellara, and B. Mautner Treatment with the antibiotic roxithromycin in patients with acute non-q-wave coronary syndromes. The final report of the ROXIS Study. Eur. Heart J. 20: Hahn, D. L., R. W. Dodge, and R. Golubjatnikov Association of Chlamydia pneumoniae (strain TWAR) infection with wheezing, asthmatic bronchitis, and adult-onset asthma. JAMA 266: Hammerschlag, M. R Activity of gemifloxacin and other new quinolones against Chlamydia pneumoniae: a review. J. Antimicrob. Chemother. 45: Hammerschlag, M. R., K. Chirgwin, P. M. Roblin, M. Gelling, W. Dumornay, L. Mandel, P. Smith, and J. Schachter Persistent infection with Chlamydia pneumoniae following acute respiratory illness. Clin. Infect. Dis. 14: Hu, H., G. N. Pierce, and G. Zhong The atherogenic effects of chlamydia are dependent on serum cholesterol and specific to Chlamydia pneumoniae. J. Clin. Investig. 103: Ianaro, A., A. Ialenti, P. Maffia, L. Sautebin, L. Rombola, R. Carnuccio, T. Iuvone, F. D Acquisto, and M. Di Rosa Anti-inflammatory activity of macrolide antibiotics. J. Pharmacol. Exp. Ther. 292: Kuo, C. C., and J. T. Grayston In vitro drug susceptibility of Chlamydia sp. strain TWAR. Antimicrob. Agents Chemother. 32: Labro, M. T Anti-inflammatory activity of macrolides: a new therapeutic potential? J. Antimicrob. Chemother. 41: Laitinen, K., A. Laurila, L. Pyhala, M. Leinonen, and P. Saikku Chlamydia pneumoniae infection induces inflammatory changes in the aortas of rabbits. Infect. Immun. 65: Laitinen, K., A. L. Laurila, M. Leinonen, and P. Saikku Reactivation of Chlamydia pneumoniae infection in mice by cortisone treatment. Infect. Immun. 64: Malinverni, R., C. C. Kuo, L. A. Campbell, and J. T. Grayston Reactivation of Chlamydia pneumoniae lung infection in mice by cortisone. J. Infect. Dis. 172: Miyashita, N., H. Fukano, Y. Niki, and T. Matsushima In vitro activity of telithromycin, a new ketolide, against Chlamydia pneumoniae. J. Antimicrob. Chemother. 48: Miyashita, N., H. Fukano, K. Yoshida, Y. Niki, and T. Matsushima Chlamydia pneumoniae infection in adult patients with persistent cough. J. Med. Microbiol. 52: Moazed, T. C., C. Kuo, J. T. Grayston, and L. A. Campbell Murine models of Chlamydia pneumoniae infection and atherosclerosis. J. Infect. Dis. 175: Moazed, T. C., C. C. Kuo, J. T. Grayston, and L. A. Campbell Evidence of systemic dissemination of Chlamydia pneumoniae via macrophages in the mouse. J. Infect. Dis. 177: Muhlestein, J. B., J. L. Anderson, J. F. Carlquist, K. Salunkhe, B. D. Horne, R. R. Pearson, T. J. Bunch, A. Allen, S. Trehan, and C. Nielson Randomized secondary prevention trial of azithromycin in patients with coronary artery disease: primary clinical results of the ACADEMIC study. Circulation 102: Muhlestein, J. B., J. L. Anderson, E. H. Hammond, L. Zhao, S. Trehan, E. P. Schwobe, and J. F. Carlquist Infection with Chlamydia pneumoniae accelerates the development of atherosclerosis and treatment with azithromycin prevents it in a rabbit model. Circulation 97: O Connor, C. M., M. W. Dunne, M. A. Pfeffer, J. B. Muhlestein, L. Yao, S. Gupta, R. J. Benner, M. R. Fisher, and T. D. Cook Azithromycin for the secondary prevention of coronary heart disease events: the WIZARD study: a randomized controlled trial. JAMA 290: Paigen, B., A. Morrow, C. Brandon, D. Mitchell, and P. Holmes Variation in susceptibility to atherosclerosis among inbred strains of mice. Atherosclerosis 57: Paigen, B., A. Morrow, P. A. Holmes, D. Mitchell, and R. A. Williams Quantitative assessment of atherosclerotic lesions in mice. Atherosclerosis 68: Piper, K. E., M. S. Rouse, J. M. Steckelberg, W. R. Wilson, and R. Patel Ketolide treatment of Haemophilus influenzae experimental pneumonia. Antimicrob. Agents Chemother. 43: Rintamaki, S., A. Saukkoriipi, P. Salo, A. Takala, and M. Leinonen Detection of Streptococcus pneumoniae DNA by using polymerase chain reaction and microwell hybridization with europium-labelled probes. J. Microbiol. Methods 50: Roblin, P. M., and M. R. Hammerschlag In vitro activity of a new ketolide antibiotic, HMR 3647, against Chlamydia pneumoniae. Antimicrob. Agents Chemother. 42: Roblin, P. M., G. Montalban, and M. R. Hammerschlag Susceptibilities to clarithromycin and erythromycin of isolates of Chlamydia pneumoniae from children with pneumonia. Antimicrob. Agents Chemother. 38: Rothstein, N. M., T. C. Quinn, G. Madico, C. A. Gaydos, and C. J. Lowenstein Effect of azithromycin on murine arteriosclerosis exacerbated by Chlamydia pneumoniae. J. Infect. Dis. 183: Scaglione, F., and G. Rossoni Comparative anti-inflammatory effects of roxithromycin, azithromycin and clarithromycin. J. Antimicrob. Chemother. 41: Sinisalo, J., K. Mattila, V. Valtonen, O. Anttonen, J. Juvonen, J. Melin, H. Vuorinen-Markkola, and M. S. Nieminen Effect of 3 months of antimicrobial treatment with clarithromycin in acute non-q-wave coronary syndrome. Circulation 105: Smieja, M., J. Mahony, A. Petrich, J. Boman, and M. Chernesky Association of circulating Chlamydia pneumoniae DNA with cardiovascular disease: a systematic review. BMC Infect. Dis. 2: Thadepalli, H., S. K. Chuah, L. Iskandar, and S. Gollapudi Comparison of telithromycin, a new ketolide, with erythromycin and clarithromycin for the treatment of Haemophilus influenzae pneumonia in suckling, middle aged and senescent mice. Int. J. Antimicrob. Agents 20: Törmäkangas, L., E. Saario, D. Bem David, A. Bryskier, M. Leinonen, and P. Saikku Treatment of acute Chlamydia pneumoniae infection with telithromycin in C57BL/6J mice. J. Antimicrob. Chemother. 53: Von Hertzen, L., H. Alakarppa, R. Koskinen, K. Liippo, H. M. Surcel, M. Leinonen, and P. Saikku Chlamydia pneumoniae infection in patients with chronic obstructive pulmonary disease. Epidemiol. Infect. 118: Vuola, J. M., V. Puurula, M. Anttila, P. H. Makela, and N. Rautonen Acquired immunity to Chlamydia pneumoniae is dependent on gamma interferon in two mouse strains that initially differ in this respect after primary challenge. Infect. Immun. 68: Wang, S. P., and J. T. Grayston Immunologic relationship between genital TRIC, lymphogranuloma venereum, and related organisms in a new microtiter indirect immunofluorescence test. Am. J. Ophthalmol. 70: Yamaguchi, H., H. Friedman, M. Yamamoto, K. Yasuda, and Y. Yamamoto Chlamydia pneumoniae resists antibiotics in lymphocytes. Antimicrob. Agents Chemother. 47: Yang, Z. P., C. C. Kuo, and J. T. Grayston A mouse model of Chlamydia pneumoniae strain TWAR pneumonitis. Infect. Immun. 61:
Effect of Azithromycin plus Rifampin versus That of Azithromycin Alone on the Eradication of Chlamydia pneumoniae
 Antimicrobial Agents and Chemotherapy, June 1999, p. 1491-1493, Vol. 43, No. 6 0066-4804/99/$04.00+0 Copyright 1999, American Society for Microbiology. All rights reserved. Effect of Azithromycin plus
Antimicrobial Agents and Chemotherapy, June 1999, p. 1491-1493, Vol. 43, No. 6 0066-4804/99/$04.00+0 Copyright 1999, American Society for Microbiology. All rights reserved. Effect of Azithromycin plus
Chlamydia pneumoniae Does Not Increase Atherosclerosis in the Aortic Root of Apolipoprotein E Deficient Mice
 Chlamydia pneumoniae Does Not Increase Atherosclerosis in the Aortic Root of Apolipoprotein E Deficient Mice Katriina Aalto-Setälä, Kirsi Laitinen, Leena Erkkilä, Maija Leinonen, Matti Jauhiainen, Christian
Chlamydia pneumoniae Does Not Increase Atherosclerosis in the Aortic Root of Apolipoprotein E Deficient Mice Katriina Aalto-Setälä, Kirsi Laitinen, Leena Erkkilä, Maija Leinonen, Matti Jauhiainen, Christian
Chlamydia pneumoniae infection in adult patients with persistent cough
 Journal of Medical Microbiology (2003), 52, 265 269 DOI 10.1099/jmm.0.04986-0 Chlamydia pneumoniae infection in adult patients with persistent cough Naoyuki Miyashita, Hiroshi Fukano, Koichiro Yoshida,
Journal of Medical Microbiology (2003), 52, 265 269 DOI 10.1099/jmm.0.04986-0 Chlamydia pneumoniae infection in adult patients with persistent cough Naoyuki Miyashita, Hiroshi Fukano, Koichiro Yoshida,
Circulating Chlamydia pneumoniae DNA as a Predictor of Coronary Artery Disease
 Journal of the American College of Cardiology Vol. 34, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00391-5 Circulating
Journal of the American College of Cardiology Vol. 34, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00391-5 Circulating
Progression of Early Carotid Atherosclerosis Is Only Temporarily Reduced After Antibiotic Treatment of Chlamydia pneumoniae Seropositivity
 Progression of Early Carotid Atherosclerosis Is Only Temporarily Reduced After Antibiotic Treatment of Chlamydia pneumoniae Seropositivity Dirk Sander, MD; Kerstin Winbeck, MD; Jürgen Klingelhöfer, MD;
Progression of Early Carotid Atherosclerosis Is Only Temporarily Reduced After Antibiotic Treatment of Chlamydia pneumoniae Seropositivity Dirk Sander, MD; Kerstin Winbeck, MD; Jürgen Klingelhöfer, MD;
Prevalence and Persistence of Chlamydia pneumoniae Antibodies in Healthy Laboratory Personnel in Finland
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, May 2005, p. 654 659 Vol. 12, No. 5 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.5.654 659.2005 Copyright 2005, American Society for Microbiology. All Rights
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, May 2005, p. 654 659 Vol. 12, No. 5 1071-412X/05/$08.00 0 doi:10.1128/cdli.12.5.654 659.2005 Copyright 2005, American Society for Microbiology. All Rights
Myocardial infarction and unstable angina derive from
 Clinical Investigation and Reports Effect of 3 Months of Antimicrobial Treatment With Clarithromycin in Acute Non Q-Wave Coronary Syndrome Juha Sinisalo, MD; Kimmo Mattila, MD; Ville Valtonen, MD; Olli
Clinical Investigation and Reports Effect of 3 Months of Antimicrobial Treatment With Clarithromycin in Acute Non Q-Wave Coronary Syndrome Juha Sinisalo, MD; Kimmo Mattila, MD; Ville Valtonen, MD; Olli
Chlamydia pneumoniae and Cardiovascular Disease
 Chlamydia pneumoniae and Cardiovascular Disease Lee Ann Campbell, Cho-Chou Kuo, and J. Thomas Grayston University of Washington, Seattle, Washington, USA Chlamydia pneumoniae is a ubiquitous pathogen that
Chlamydia pneumoniae and Cardiovascular Disease Lee Ann Campbell, Cho-Chou Kuo, and J. Thomas Grayston University of Washington, Seattle, Washington, USA Chlamydia pneumoniae is a ubiquitous pathogen that
The obligate intracellular pathogen Chlamydia pneumoniae. Clinical Investigation and Reports
 Clinical Investigation and Reports Chlamydia pneumoniae Infection in Circulating Human Monocytes Is Refractory to Antibiotic Treatment Jens Gieffers, MD; Henriette Füllgraf; Jürgen Jahn, MD; Matthias Klinger,
Clinical Investigation and Reports Chlamydia pneumoniae Infection in Circulating Human Monocytes Is Refractory to Antibiotic Treatment Jens Gieffers, MD; Henriette Füllgraf; Jürgen Jahn, MD; Matthias Klinger,
Presence of Chlamydia pneumoniae in Human Symptomatic and Asymptomatic Carotid Atherosclerotic Plaque
 Presence of Chlamydia pneumoniae in Human Symptomatic and Asymptomatic Carotid Atherosclerotic Plaque Ronald LaBiche, PhD; Deloris Koziol, PhD; Thomas C. Quinn, MD; Charlotte Gaydos, DrPH; Salman Azhar,
Presence of Chlamydia pneumoniae in Human Symptomatic and Asymptomatic Carotid Atherosclerotic Plaque Ronald LaBiche, PhD; Deloris Koziol, PhD; Thomas C. Quinn, MD; Charlotte Gaydos, DrPH; Salman Azhar,
Antibiotic Treatment of Chlamydia pneumoniae after Acute Coronary Syndrome
 The new england journal of medicine original article Antibiotic Treatment of Chlamydia pneumoniae after Acute Coronary Syndrome Christopher P. Cannon, M.D., Eugene Braunwald, M.D., Carolyn H. McCabe, B.S.,
The new england journal of medicine original article Antibiotic Treatment of Chlamydia pneumoniae after Acute Coronary Syndrome Christopher P. Cannon, M.D., Eugene Braunwald, M.D., Carolyn H. McCabe, B.S.,
Key words: Chlamydia pneumoniae, acute upper resiratory infections, culture, micro-if method
 Key words: Chlamydia pneumoniae, acute upper resiratory infections, culture, micro-if method Table 1 Prevalence of antibodies to C. pneumoniae in patients and control group There was no statistically significant
Key words: Chlamydia pneumoniae, acute upper resiratory infections, culture, micro-if method Table 1 Prevalence of antibodies to C. pneumoniae in patients and control group There was no statistically significant
Effects of Repeated Chlamydia pneumoniae Inoculations on Aortic Lipid Accumulation and Inflammatory Response in C57BL/6J Mice
 INFECTION AND IMMUNITY, Oct. 2005, p. 6458 6466 Vol. 73, No. 10 0019-9567/05/$08.00 0 doi:10.1128/iai.73.10.6458 6466.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. Effects
INFECTION AND IMMUNITY, Oct. 2005, p. 6458 6466 Vol. 73, No. 10 0019-9567/05/$08.00 0 doi:10.1128/iai.73.10.6458 6466.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved. Effects
Performance of Three Microimmunofluorescence Assays for Detection of Chlamydia pneumoniae Immunoglobulin M, G, and A Antibodies
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 2002, p. 833 839 Vol. 9, No. 4 1071-412X/02/$04.00 0 DOI: 10.1128/CDLI.09.4.833 839.2002 Copyright 2002, American Society for Microbiology. All Rights
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 2002, p. 833 839 Vol. 9, No. 4 1071-412X/02/$04.00 0 DOI: 10.1128/CDLI.09.4.833 839.2002 Copyright 2002, American Society for Microbiology. All Rights
ORIGINAL ARTICLE /j x
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01898.x Acute Chlamydia pneumoniae infections in asthmatic and non-asthmatic military conscripts during a non-epidemic period R. Juvonen 1, A. Bloigu 2, M. Paldanius
ORIGINAL ARTICLE 10.1111/j.1469-0691.2007.01898.x Acute Chlamydia pneumoniae infections in asthmatic and non-asthmatic military conscripts during a non-epidemic period R. Juvonen 1, A. Bloigu 2, M. Paldanius
Outbreak of Respiratory Tract Infections on an Islet in Korea: Possible Chlamydia pneumoniae Infection
 Jpn. J. Infect. Dis., 59, 294-298, 2006 Original Article Outbreak of Respiratory Tract Infections on an Islet in Korea: Possible Chlamydia pneumoniae Infection Kwang-Jun Lee, Su-Jin Kwon, Bo-Ram Choi,
Jpn. J. Infect. Dis., 59, 294-298, 2006 Original Article Outbreak of Respiratory Tract Infections on an Islet in Korea: Possible Chlamydia pneumoniae Infection Kwang-Jun Lee, Su-Jin Kwon, Bo-Ram Choi,
Chlamydia pneumoniae Eradication from Carotid Plaques. Results of an Open, Randomised Treatment Study
 Eur J Vasc Endovasc Surg 18, 355 359 (1999) Article No. ejvs.1999.0915 Chlamydia pneumoniae Eradication from Carotid Plaques. Results of an Open, Randomised Treatment Study G. Melissano 1, F. Blasi 2,
Eur J Vasc Endovasc Surg 18, 355 359 (1999) Article No. ejvs.1999.0915 Chlamydia pneumoniae Eradication from Carotid Plaques. Results of an Open, Randomised Treatment Study G. Melissano 1, F. Blasi 2,
Can acute Chlamydia pneumoniae respiratory tract infection initiate chronic asthma?
 Can acute Chlamydia pneumoniae respiratory tract infection initiate chronic asthma? David L Hahn, MD, MS* and Roberta McDonald, BS Background: Chlamydia pneumoniae infection can cause acute respiratory
Can acute Chlamydia pneumoniae respiratory tract infection initiate chronic asthma? David L Hahn, MD, MS* and Roberta McDonald, BS Background: Chlamydia pneumoniae infection can cause acute respiratory
Inflammation plays a major role in atherogenesis and rapid
 Effect of Treatment for Chlamydia pneumoniae and Helicobacter pylori on Markers of Inflammation and Cardiac Events in Patients With Acute Coronary Syndromes South Thames Trial of Antibiotics in Myocardial
Effect of Treatment for Chlamydia pneumoniae and Helicobacter pylori on Markers of Inflammation and Cardiac Events in Patients With Acute Coronary Syndromes South Thames Trial of Antibiotics in Myocardial
Growth Cycle-Dependent Pharmacodynamics of Antichlamydial Drugs
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2005, p. 1852 1856 Vol. 49, No. 5 0066-4804/05/$08.00 0 doi:10.1128/aac.49.5.1852 1856.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, May 2005, p. 1852 1856 Vol. 49, No. 5 0066-4804/05/$08.00 0 doi:10.1128/aac.49.5.1852 1856.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
The Microimmunofluorescence Test for Chlamydia pneumoniae Infection: Technique and Interpretation
 S421 The Microimmunofluorescence Test for Chlamydia pneumoniae Infection: Technique and Interpretation San-pin Wang Department of Pathobiology, University of Washington, Seattle A brief description of
S421 The Microimmunofluorescence Test for Chlamydia pneumoniae Infection: Technique and Interpretation San-pin Wang Department of Pathobiology, University of Washington, Seattle A brief description of
Association of Chlamydia pneumoniae IgA antibodies with
 Epidemiol. Infect. (1996), 117, 513-517 Copyright K 1996 Cambridge University Press Association of Chlamydia pneumoniae IgA antibodies with recently symptomatic asthma D. L. HAHN'*, T. ANTTILA AND P. SAIKKU2'3
Epidemiol. Infect. (1996), 117, 513-517 Copyright K 1996 Cambridge University Press Association of Chlamydia pneumoniae IgA antibodies with recently symptomatic asthma D. L. HAHN'*, T. ANTTILA AND P. SAIKKU2'3
A New Primer Pair for Detection of Chiamydia pneumoniae by Polymerase Chain Reaction
 A New Primer Pair for Detection of Chiamydia pneumoniae by Polymerase Chain Reaction Microbiol. Immunol., 40(1), 27-32, 1996 Yoshifumi Kubota Division of Respiratory Diseases, Department of Medicine, Kawasaki
A New Primer Pair for Detection of Chiamydia pneumoniae by Polymerase Chain Reaction Microbiol. Immunol., 40(1), 27-32, 1996 Yoshifumi Kubota Division of Respiratory Diseases, Department of Medicine, Kawasaki
Infection and Atherosclerosis: Evidence for Possible Associations
 Cardiovascular Disease Infection and Atherosclerosis: Evidence for Possible Associations I.W. Fong, MB, BS, FRCPC, Department of Medicine, Division of Infectious Diseases, University of Toronto, St. Michael
Cardiovascular Disease Infection and Atherosclerosis: Evidence for Possible Associations I.W. Fong, MB, BS, FRCPC, Department of Medicine, Division of Infectious Diseases, University of Toronto, St. Michael
Bacteria belonging to genus Chlamydia have a. Comparison of Individuals With and Without Specific IgA Antibodies to Chlamydia pneumoniae*
 Comparison of Individuals With and Without Specific IgA Antibodies to Chlamydia pneumoniae* Respiratory Morbidity and the Metabolic Syndrome Göran Falck, MD, PhD; Judy Gnarpe, PhD; Lars-Olof Hansson, MD,
Comparison of Individuals With and Without Specific IgA Antibodies to Chlamydia pneumoniae* Respiratory Morbidity and the Metabolic Syndrome Göran Falck, MD, PhD; Judy Gnarpe, PhD; Lars-Olof Hansson, MD,
Endovascular Presence of Viable Chlamydia pneumoniae Is a Common Phenomenon in Coronary Artery Disease
 JACC Vol. 31, No. 4 March 15, 1998:827 32 827 CORONARY ARTERY DISEASE Endovascular Presence of Viable Chlamydia pneumoniae Is a Common Phenomenon in Coronary Artery Disease MATTHIAS MAASS, MD, CLAUS BARTELS,
JACC Vol. 31, No. 4 March 15, 1998:827 32 827 CORONARY ARTERY DISEASE Endovascular Presence of Viable Chlamydia pneumoniae Is a Common Phenomenon in Coronary Artery Disease MATTHIAS MAASS, MD, CLAUS BARTELS,
The Prevalence of Chlamydia pneumoniae
 152 JACC Vol. 33, No. 1 The Prevalence of Chlamydia pneumoniae in Atherosclerotic and Nonatherosclerotic Blood Vessels of Patients Attending for Redo and First Time Coronary Artery Bypass Graft Surgery
152 JACC Vol. 33, No. 1 The Prevalence of Chlamydia pneumoniae in Atherosclerotic and Nonatherosclerotic Blood Vessels of Patients Attending for Redo and First Time Coronary Artery Bypass Graft Surgery
Rabbit Model for Chlamydia pneumoniae Infection
 JOURNAL OF CLINICAL MICROBIOLOGY, Jan. 1997, p. 48 52 Vol. 35, No. 1 0095-1137/97/$04.00 0 Copyright 1997, American Society for Microbiology Rabbit Model for Chlamydia pneumoniae Infection IGNATIUS W.
JOURNAL OF CLINICAL MICROBIOLOGY, Jan. 1997, p. 48 52 Vol. 35, No. 1 0095-1137/97/$04.00 0 Copyright 1997, American Society for Microbiology Rabbit Model for Chlamydia pneumoniae Infection IGNATIUS W.
The atherogenic effects of chlamydia are dependent on serum cholesterol and specific to Chlamydia pneumoniae
 The atherogenic effects of chlamydia are dependent on serum cholesterol and specific to Chlamydia pneumoniae He Hu, 1 Grant N. Pierce, 2 and Guangming Zhong 1,3 1 Department of Medical Microbiology, 2
The atherogenic effects of chlamydia are dependent on serum cholesterol and specific to Chlamydia pneumoniae He Hu, 1 Grant N. Pierce, 2 and Guangming Zhong 1,3 1 Department of Medical Microbiology, 2
Chlamydial pneumonia in children requiring hospitalization: effect of mixed infection on clinical outcome
 J Microbiol Immunol Infect 2005;38:117-122 Tsai et al Chlamydial pneumonia in children requiring hospitalization: effect of mixed infection on clinical outcome Ming-Han Tsai 1, Yhu-Chering Huang 1, Chih-Jung
J Microbiol Immunol Infect 2005;38:117-122 Tsai et al Chlamydial pneumonia in children requiring hospitalization: effect of mixed infection on clinical outcome Ming-Han Tsai 1, Yhu-Chering Huang 1, Chih-Jung
Effect of Azithromycin Treatment on Endothelial Function in Patients With Coronary Artery Disease and Evidence of Chlamydia pneumoniae Infection
 Effect of Azithromycin Treatment on Endothelial Function in Patients With Coronary Artery Disease and Evidence of Chlamydia pneumoniae Infection Nikhil Parchure, MRCP; Emmanouil G. Zouridakis, MD; Juan
Effect of Azithromycin Treatment on Endothelial Function in Patients With Coronary Artery Disease and Evidence of Chlamydia pneumoniae Infection Nikhil Parchure, MRCP; Emmanouil G. Zouridakis, MD; Juan
Effects of Two Antibiotic Regimens on Course and Persistence of Experimental Chlamydia pneumoniae TWAR Pneumonitis
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Jan. 1995, p. 45 49 Vol. 39, No. 1 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Effects of Two Antibiotic Regimens on Course and Persistence
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Jan. 1995, p. 45 49 Vol. 39, No. 1 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Effects of Two Antibiotic Regimens on Course and Persistence
Epidemiological studies demonstrated an association between
 Reduced Progression of Early Carotid Atherosclerosis After Antibiotic Treatment and Chlamydia pneumoniae Seropositivity Dirk Sander, MD; Kerstin Winbeck, MD; Jürgen Klingelhöfer, MD; Thorleif Etgen, MD;
Reduced Progression of Early Carotid Atherosclerosis After Antibiotic Treatment and Chlamydia pneumoniae Seropositivity Dirk Sander, MD; Kerstin Winbeck, MD; Jürgen Klingelhöfer, MD; Thorleif Etgen, MD;
Received 4 June 2002/Returned for modification 7 August 2002/Accepted 17 September 2002
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Jan. 2003, p. 8 12 Vol. 10, No. 1 1071-412X/03/$08.00 0 DOI: 10.1128/CDLI.10.1.8 12.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Jan. 2003, p. 8 12 Vol. 10, No. 1 1071-412X/03/$08.00 0 DOI: 10.1128/CDLI.10.1.8 12.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
MINIREVIEW Antimicrobial Susceptibility and Therapy of Infections Caused by Chlamydia pneumoniae
 ANTIMICROBiAL AGENTS AND CHEMOTHERAPY, Sept. 1994, p. 1873-1878 0066-4804/94/$04.00+0 Copyright X 1994, American Society for Microbiology Vol. 38, No. 9 MINIREVIEW Antimicrobial Susceptibility and Therapy
ANTIMICROBiAL AGENTS AND CHEMOTHERAPY, Sept. 1994, p. 1873-1878 0066-4804/94/$04.00+0 Copyright X 1994, American Society for Microbiology Vol. 38, No. 9 MINIREVIEW Antimicrobial Susceptibility and Therapy
Comparison of Five Serologic Tests for Diagnosis of Acute Infections by Chlamydia pneumoniae
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2000, p. 739 744 Vol. 7, No. 5 1071-412X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Comparison of Five Serologic
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2000, p. 739 744 Vol. 7, No. 5 1071-412X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Comparison of Five Serologic
322 Chlamydia pneumoniae and Coronary Artery Disease Mayo Clin Proc, March 2003, Vol 78 plaque. 8,9 One theory is that, in certain genetically suscept
 Mayo Clin Proc, March 2003, Vol 78 Chlamydia pneumoniae and Coronary Artery Disease 321 Review Chlamydia pneumoniae and Coronary Artery Disease: The Antibiotic Trials JOHN P. HIGGINS, MD, MPHIL Parallel
Mayo Clin Proc, March 2003, Vol 78 Chlamydia pneumoniae and Coronary Artery Disease 321 Review Chlamydia pneumoniae and Coronary Artery Disease: The Antibiotic Trials JOHN P. HIGGINS, MD, MPHIL Parallel
Antibiotics active against Chlamydia do not reduce the risk of myocardial infarction
 Eur J Clin Pharmacol DOI 10.1007/s00228-005-0059-x PHARMACOEPIDEMIOLOGY AND PRESCRIPTION Lars Bjerrum. Morten Andersen. Jesper Hallas Antibiotics active against Chlamydia do not reduce the risk of myocardial
Eur J Clin Pharmacol DOI 10.1007/s00228-005-0059-x PHARMACOEPIDEMIOLOGY AND PRESCRIPTION Lars Bjerrum. Morten Andersen. Jesper Hallas Antibiotics active against Chlamydia do not reduce the risk of myocardial
Part II Serology Caroline Bax BW.indd 55 Caroline Bax BW.indd : :17
 Part II Serology part II Chapter 4 Comparison of serological assays for detection of Chlamydia trachomatis antibodies in different groups of obstetrical and gynaecological patients C.J. Bax J.A.E.M. Mutsaers
Part II Serology part II Chapter 4 Comparison of serological assays for detection of Chlamydia trachomatis antibodies in different groups of obstetrical and gynaecological patients C.J. Bax J.A.E.M. Mutsaers
A positive association of peripheral arterial occlusive disease (PAD) and Chlamydophila (Clamydia) pneumoniae
 J. Basic Microbiol. 45 (2005) 4, 294 300 DOI: 10.1002/jobm.200410501 (Departments of Microbiology and Surgery 1, University Hospital San Cecilio, University of Granada; Laboratorio Vircell 2 ; Granada,
J. Basic Microbiol. 45 (2005) 4, 294 300 DOI: 10.1002/jobm.200410501 (Departments of Microbiology and Surgery 1, University Hospital San Cecilio, University of Granada; Laboratorio Vircell 2 ; Granada,
Biological Consulting Services
 Biological Consulting Services of North Florida/ Inc. May 13, 2009 Aphex BioCleanse Systems, Inc. Dear Sirs, We have completed antimicrobial efficacy study on the supplied Multi-Purpose Solution. The testing
Biological Consulting Services of North Florida/ Inc. May 13, 2009 Aphex BioCleanse Systems, Inc. Dear Sirs, We have completed antimicrobial efficacy study on the supplied Multi-Purpose Solution. The testing
Background and Current Knowledge of Chlamydia pneumoniae and Atherosclerosis
 S402 Background and Current Knowledge of Chlamydia pneumoniae and Atherosclerosis J. Thomas Grayston Department of Epidemiology, University of Washington, Seattle Attributes of Chlamydia pneumoniae of
S402 Background and Current Knowledge of Chlamydia pneumoniae and Atherosclerosis J. Thomas Grayston Department of Epidemiology, University of Washington, Seattle Attributes of Chlamydia pneumoniae of
Lymphocyte responses to Chlamydia antigens in patients with coronary heart disease
 European Heart Journal (1997) 18, 1095-1101 Lymphocyte respoes to Chlamydia antige in patients with coronary heart disease S. Halme*, H. Syrjalaf, A. Bloigu*, P. Saikku*, M. Leinonen*, J. Airaksinent and
European Heart Journal (1997) 18, 1095-1101 Lymphocyte respoes to Chlamydia antige in patients with coronary heart disease S. Halme*, H. Syrjalaf, A. Bloigu*, P. Saikku*, M. Leinonen*, J. Airaksinent and
on January 10, 2019 by guest
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2000, p. 734 738 Vol. 7, No. 5 1071-412X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Prevalence of Chlamydia
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Sept. 2000, p. 734 738 Vol. 7, No. 5 1071-412X/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Prevalence of Chlamydia
Rifampin Resistance. Charlottesville, Virginia i0w organisms in Trypticase soy broth (BBL Microbiology
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1980, p. 658-662 0066-4804/80/04-0658/05$02.00/0 Vol. 17, No. 14 Treatment of Experimental Staphylococcal Infections: Effect of Rifampin Alone and in Combination
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Apr. 1980, p. 658-662 0066-4804/80/04-0658/05$02.00/0 Vol. 17, No. 14 Treatment of Experimental Staphylococcal Infections: Effect of Rifampin Alone and in Combination
Chlamydia pneumoniae Infection Increases Adherence of Mouse Macrophages to Mouse Endothelial Cells In Vitro and to Aortas Ex Vivo
 INFECTION AND IMMUNITY, Feb. 2008, p. 510 514 Vol. 76, No. 2 0019-9567/08/$08.00 0 doi:10.1128/iai.01267-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae
INFECTION AND IMMUNITY, Feb. 2008, p. 510 514 Vol. 76, No. 2 0019-9567/08/$08.00 0 doi:10.1128/iai.01267-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae
Identification of Chlamydia pneumoniae by DNA Amplification
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 1992, p. 796-800 0095-1137/92/040796-05$02.00/0 Copyright 1992, American Society for Microbiology Vol. 30, No. 4 Identification of Chlamydia pneumoniae by DNA Amplification
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 1992, p. 796-800 0095-1137/92/040796-05$02.00/0 Copyright 1992, American Society for Microbiology Vol. 30, No. 4 Identification of Chlamydia pneumoniae by DNA Amplification
Effects of Corticosteroids and Cyclophosphamide on a Mouse Model of Chlamydia trachomatis Pneumonitis
 INFECTION AND IMMUNITY, Feb. 1982, p. 680-684 0019-9567/82/020680-05$02.00/0 Vol. 35, No. 2 Effects of Corticosteroids and Cyclophosphamide on a Mouse Model of Chlamydia trachomatis Pneumonitis RICHARD
INFECTION AND IMMUNITY, Feb. 1982, p. 680-684 0019-9567/82/020680-05$02.00/0 Vol. 35, No. 2 Effects of Corticosteroids and Cyclophosphamide on a Mouse Model of Chlamydia trachomatis Pneumonitis RICHARD
Chlamydia pneumoniae Infection in Human Monocytes
 INFECTION AND IMMUNITY, Mar. 1999, p. 1445 1449 Vol. 67, No. 3 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae Infection in Human Monocytes
INFECTION AND IMMUNITY, Mar. 1999, p. 1445 1449 Vol. 67, No. 3 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae Infection in Human Monocytes
Key words : Chlamydia trachomatis, Tonsillitis, Rokitamycin
 Key words : Chlamydia trachomatis, Tonsillitis, Rokitamycin Table 1 Distribution of the study population Table 2 Clinical details of patients with tonsillitis *LT =Lingering tonsillitis, RT = Recurrent
Key words : Chlamydia trachomatis, Tonsillitis, Rokitamycin Table 1 Distribution of the study population Table 2 Clinical details of patients with tonsillitis *LT =Lingering tonsillitis, RT = Recurrent
Host immune response to Chlamydia pneumoniae heat shock protein 60 is associated with asthma
 Eur Respir J 21; 17: 178 182 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Host immune response to Chlamydia pneumoniae heat shock protein 6
Eur Respir J 21; 17: 178 182 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Host immune response to Chlamydia pneumoniae heat shock protein 6
JOURNAL OF CLINICAL MICROBIOLOGY, July 2000, p Vol. 38, No. 7. Copyright 2000, American Society for Microbiology. All Rights Reserved.
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2000, p. 2622 2627 Vol. 38, No. 7 0095-1137/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Analytical Sensitivity, Reproducibility
JOURNAL OF CLINICAL MICROBIOLOGY, July 2000, p. 2622 2627 Vol. 38, No. 7 0095-1137/00/$04.00 0 Copyright 2000, American Society for Microbiology. All Rights Reserved. Analytical Sensitivity, Reproducibility
Anti-Chlamydia pneumoniae heat shock protein 10 antibodies in asthmatic adults
 FEMS Immunology and Medical Microbiology 35 (2003) 107^111 www.fems-microbiology.org Anti-Chlamydia pneumoniae heat shock protein 10 antibodies in asthmatic adults Abstract Fotini Betsou, Jean Marie Sueur,
FEMS Immunology and Medical Microbiology 35 (2003) 107^111 www.fems-microbiology.org Anti-Chlamydia pneumoniae heat shock protein 10 antibodies in asthmatic adults Abstract Fotini Betsou, Jean Marie Sueur,
Laboratory diagnosis of congenital infections
 Laboratory diagnosis of congenital infections Laboratory diagnosis of HSV Direct staining Tzanck test Immunostaining HSV isolation Serology PCR Tzanck test Cell scrape from base of the lesion smear on
Laboratory diagnosis of congenital infections Laboratory diagnosis of HSV Direct staining Tzanck test Immunostaining HSV isolation Serology PCR Tzanck test Cell scrape from base of the lesion smear on
CHLAMYDIA PNEUMONIAE, a
 ORIGINAL INVESTIGATION Association Between Chlamydia pneumoniae Antibodies and Intimal Calcification in Femoral Arteries of Nondiabetic Patients Seppo Lehto, MD; Leo Niskanen, MD; Matti Suhonen, MD; Tapani
ORIGINAL INVESTIGATION Association Between Chlamydia pneumoniae Antibodies and Intimal Calcification in Femoral Arteries of Nondiabetic Patients Seppo Lehto, MD; Leo Niskanen, MD; Matti Suhonen, MD; Tapani
ORIGINAL ARTICLE. Chiung-Zuei Chen, 1 Bei-Chang Yang, 2 Tsun-Mei Lin, 3 Cheng-Hung Lee, 1 Tzuen-Ren Hsiue 1 *
 ORIGINAL ARTICLE Chronic and Repeated Chlamydophila pneumoniae Lung Infection can Result in Increasing IL-4 Gene Expression and Thickness of Airway Subepithelial Basement Membrane in Mice Chiung-Zuei Chen,
ORIGINAL ARTICLE Chronic and Repeated Chlamydophila pneumoniae Lung Infection can Result in Increasing IL-4 Gene Expression and Thickness of Airway Subepithelial Basement Membrane in Mice Chiung-Zuei Chen,
Infection of Human Endothelial Cells with Chlamydia pneumoniae Stimulates Transendothelial Migration of Neutrophils and Monocytes
 INFECTION AND IMMUNITY, Mar. 1999, p. 1323 1330 Vol. 67, No. 3 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Infection of Human Endothelial Cells with Chlamydia
INFECTION AND IMMUNITY, Mar. 1999, p. 1323 1330 Vol. 67, No. 3 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Infection of Human Endothelial Cells with Chlamydia
Chlamydia pneumoniae Growth Inhibition in Cells by the Steroid Receptor Antagonist RU486 (Mifepristone)
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, June 2008, p. 1991 1998 Vol. 52, No. 6 0066-4804/08/$08.00 0 doi:10.1128/aac.01416-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Chlamydia
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, June 2008, p. 1991 1998 Vol. 52, No. 6 0066-4804/08/$08.00 0 doi:10.1128/aac.01416-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Chlamydia
Received 19 November 1997/Returned for modification 5 January 1998/Accepted 15 January 1998
 INFECTION AND IMMUNITY, Apr. 1998, p. 1370 1376 Vol. 66, No. 4 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology Characterization of a Strain of Chlamydia pneumoniae Isolated from
INFECTION AND IMMUNITY, Apr. 1998, p. 1370 1376 Vol. 66, No. 4 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology Characterization of a Strain of Chlamydia pneumoniae Isolated from
Expansion of a Novel Pulmonary CD3 CD4 CD8 Cell Population in Mice during Chlamydia pneumoniae Infection
 INFECTION AND IMMUNITY, July 1998, p. 3290 3294 Vol. 66, No. 7 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Expansion of a Novel Pulmonary CD3 CD4 CD8 Cell
INFECTION AND IMMUNITY, July 1998, p. 3290 3294 Vol. 66, No. 7 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Expansion of a Novel Pulmonary CD3 CD4 CD8 Cell
X/01/$ DOI: /CDLI Received 6 November 2000/Returned for modification 6 February 2001/Accepted 27 February 2001
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, May 2001, p. 588 592 Vol. 8, No. 3 1071-412X/01/$04.00 0 DOI: 10.1128/CDLI.8.3.588 592.2001 Comparison of Two Commercial Microimmunofluorescence Kits and
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, May 2001, p. 588 592 Vol. 8, No. 3 1071-412X/01/$04.00 0 DOI: 10.1128/CDLI.8.3.588 592.2001 Comparison of Two Commercial Microimmunofluorescence Kits and
Multi-clonal origin of macrolide-resistant Mycoplasma pneumoniae isolates. determined by multiple-locus variable-number tandem-repeat analysis
 JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
Is atherosclerosis an infectious disease?
 REVIEW STEVEN D. MAWHORTER, MD Department of Infectious Disease, Cleveland Clinic MICHAEL A. LAUER, MD Department of Cardiology, Borgess Medical Center Research Institute, Kalamazoo, Michigan Is atherosclerosis
REVIEW STEVEN D. MAWHORTER, MD Department of Infectious Disease, Cleveland Clinic MICHAEL A. LAUER, MD Department of Cardiology, Borgess Medical Center Research Institute, Kalamazoo, Michigan Is atherosclerosis
Microbiology of Atypical Pneumonia. Dr. Mohamed Medhat Ali
 Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
Gamma Interferon Production by Cytotoxic T Lymphocytes Is Required for Resolution of Chlamydia trachomatis Infection
 INFECTION AND IMMUNITY, Nov. 1998, p. 5457 5461 Vol. 66, No. 11 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Gamma Interferon Production by Cytotoxic T
INFECTION AND IMMUNITY, Nov. 1998, p. 5457 5461 Vol. 66, No. 11 0019-9567/98/$04.00 0 Copyright 1998, American Society for Microbiology. All Rights Reserved. Gamma Interferon Production by Cytotoxic T
De Novo Induction of Atherosclerosis by Chlamydia pneumoniae in a Rabbit Model
 INFECTION AND IMMUNITY, Nov. 1999, p. 6048 6055 Vol. 67, No. 11 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. De Novo Induction of Atherosclerosis by Chlamydia
INFECTION AND IMMUNITY, Nov. 1999, p. 6048 6055 Vol. 67, No. 11 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. De Novo Induction of Atherosclerosis by Chlamydia
Chlamydia pneumoniae in arteries: the facts, their interpretation, and future studies
 J Clin Pathol 1998;51:793 797 793 Leader Imperial College School of Medicine at St Mary s, London W2, UK D Taylor-Robinson B J Thomas Correspondence to: Professor D Taylor-Robinson, Department of Genitourinary
J Clin Pathol 1998;51:793 797 793 Leader Imperial College School of Medicine at St Mary s, London W2, UK D Taylor-Robinson B J Thomas Correspondence to: Professor D Taylor-Robinson, Department of Genitourinary
Association of Chlamj~dia pneumoniae IgA antibodies with recently symptomatic asthma
 E/JI~/PIIIIO~ 111fccr (1996). 117, 513-517 Copyr~ght 0 1996 Cambridge Unlvers~ty Press Association of Chlamj~dia pneumoniae IgA antibodies with recently symptomatic asthma Dc2trri Mcrlical Cc~titcv unrl
E/JI~/PIIIIO~ 111fccr (1996). 117, 513-517 Copyr~ght 0 1996 Cambridge Unlvers~ty Press Association of Chlamj~dia pneumoniae IgA antibodies with recently symptomatic asthma Dc2trri Mcrlical Cc~titcv unrl
Luminescent platforms for monitoring changes in the solubility of amylin and huntingtin in living cells
 Electronic Supplementary Material (ESI) for Molecular BioSystems. This journal is The Royal Society of Chemistry 2016 Contents Supporting Information Luminescent platforms for monitoring changes in the
Electronic Supplementary Material (ESI) for Molecular BioSystems. This journal is The Royal Society of Chemistry 2016 Contents Supporting Information Luminescent platforms for monitoring changes in the
Chlamydia pneumoniae in atheroma: consideration of criteria for causality
 812 School of Pathology, University of the Witwatersrand, South Africa A Shor National Centre for Occupational Health, Johannesburg, South Africa J I Phillips MRC Sexually Transmitted Diseases Research
812 School of Pathology, University of the Witwatersrand, South Africa A Shor National Centre for Occupational Health, Johannesburg, South Africa J I Phillips MRC Sexually Transmitted Diseases Research
Importance of acute Mycoplasma pneumoniae and Chlamydia pneumoniae infections in children with wheezing
 Eur Respir J 2000; 16: 1142±1146 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Importance of acute Mycoplasma pneumoniae and Chlamydia
Eur Respir J 2000; 16: 1142±1146 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Importance of acute Mycoplasma pneumoniae and Chlamydia
Chronic Chlamydophila pneumoniae infection in lung cancer, a risk factor: a case control study
 Journal of Medical Microbiology (2003), 52, 721 726 DOI 10.1099/jmm.0.04845-0 Chronic Chlamydophila pneumoniae infection in lung cancer, a risk factor: a case control study Bekir Kocazeybek Correspondence
Journal of Medical Microbiology (2003), 52, 721 726 DOI 10.1099/jmm.0.04845-0 Chronic Chlamydophila pneumoniae infection in lung cancer, a risk factor: a case control study Bekir Kocazeybek Correspondence
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES
 CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
Human Chlamydia pneumoniae IgG EIA Kit
 Human Chlamydia pneumoniae IgG EIA Kit Cat.No: DEIA1726 Lot. No. (See product label) PRODUCT INFOMATION Intended use General Description Principle Of The Test CD's Chlamydia pneumoniae IgG test is developed
Human Chlamydia pneumoniae IgG EIA Kit Cat.No: DEIA1726 Lot. No. (See product label) PRODUCT INFOMATION Intended use General Description Principle Of The Test CD's Chlamydia pneumoniae IgG test is developed
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR
 Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Chlamydia pneumoniae Expresses Genes Required for DNA Replication but Not Cytokinesis during Persistent Infection of HEp-2 Cells
 INFECTION AND IMMUNITY, Sept. 2001, p. 5423 5429 Vol. 69, No. 9 0019-9567/01/$04.00 0 DOI: 10.1128/IAI.69.9.5423 5429.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Chlamydia
INFECTION AND IMMUNITY, Sept. 2001, p. 5423 5429 Vol. 69, No. 9 0019-9567/01/$04.00 0 DOI: 10.1128/IAI.69.9.5423 5429.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Chlamydia
Study objective: To investigate the clinical presentation of community-acquired Chlamydia
 Clinical Presentation of Community- Acquired Chlamydia pneumoniae Pneumonia in Adults* Naoyuki Miyashita, MD, PhD; Hiroshi Fukano, MD; Niro Okimoto, MD, PhD, FCCP; Hiroki Hara, MD, PhD, FCCP; Koichiro
Clinical Presentation of Community- Acquired Chlamydia pneumoniae Pneumonia in Adults* Naoyuki Miyashita, MD, PhD; Hiroshi Fukano, MD; Niro Okimoto, MD, PhD, FCCP; Hiroki Hara, MD, PhD, FCCP; Koichiro
Phagocytes transmit Chlamydia pneumoniae from the lungs to the vasculature.
 Eur Respir J 2004; 23: 506 510 DOI: 10.1183/09031936.04.00093304 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2004 European Respiratory Journal ISSN 0903-1936 FRONT ROWS OF SCIENCE Phagocytes
Eur Respir J 2004; 23: 506 510 DOI: 10.1183/09031936.04.00093304 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2004 European Respiratory Journal ISSN 0903-1936 FRONT ROWS OF SCIENCE Phagocytes
Supplementary Figures
 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Association of Chlamydia pneumoniae Infection with HLA-B*35 in Patients with Coronary Artery Disease
 CLINICAL AND VACCINE IMMUNOLOGY, Jan. 2008, p. 55 59 Vol. 15, No. 1 1556-6811/08/$08.00 0 doi:10.1128/cvi.00163-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Association of
CLINICAL AND VACCINE IMMUNOLOGY, Jan. 2008, p. 55 59 Vol. 15, No. 1 1556-6811/08/$08.00 0 doi:10.1128/cvi.00163-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Association of
Toshio Kishimoto*, Shuji Ando, Kei Numazaki 1, Kazunobu Ouchi 2, Tsutomu Yamazaki 3, and Chikara Nakahama 4
 Jpn. J. Infect. Dis., 62, 260-264, 2009 Original Article Assay of Chlamydia pneumoniae-specific IgM Antibodies by ELISA Method---Reduction of Non-Specific Reaction and Resetting of Serological Criteria
Jpn. J. Infect. Dis., 62, 260-264, 2009 Original Article Assay of Chlamydia pneumoniae-specific IgM Antibodies by ELISA Method---Reduction of Non-Specific Reaction and Resetting of Serological Criteria
STUDIES OF THE HEMAGGLUTININ OF HAEMOPHILUS PERTUSSIS HIDEO FUKUMI, HISASHI SHIMAZAKI, SADAO KOBAYASHI AND TATSUJI UCHIDA
 STUDIES OF THE HEMAGGLUTININ OF HAEMOPHILUS PERTUSSIS HIDEO FUKUMI, HISASHI SHIMAZAKI, SADAO KOBAYASHI AND TATSUJI UCHIDA The National Institute of Health, Tokyo, Japan (Received: August 3rd, 1953) INTRODUCTION
STUDIES OF THE HEMAGGLUTININ OF HAEMOPHILUS PERTUSSIS HIDEO FUKUMI, HISASHI SHIMAZAKI, SADAO KOBAYASHI AND TATSUJI UCHIDA The National Institute of Health, Tokyo, Japan (Received: August 3rd, 1953) INTRODUCTION
LDL Uptake Cell-Based Assay Kit
 LDL Uptake Cell-Based Assay Kit Item No. 10011125 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
LDL Uptake Cell-Based Assay Kit Item No. 10011125 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL INFORMATION
In vitro assessment of dual drug combinations to inhibit growth of Neisseria gonorrhoeae
 AAC Accepted Manuscript Posted Online 26 January 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.04127-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 In vitro assessment
AAC Accepted Manuscript Posted Online 26 January 2015 Antimicrob. Agents Chemother. doi:10.1128/aac.04127-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 In vitro assessment
Chlamydophila pneumoniae (Chlamydia pneumoniae) accelerates the formation of complex atherosclerotic lesions in Apo E3-Leiden mice
 Cardiovascular Research 56 (2002) 269 276 www.elsevier.com/ locate/ cardiores Chlamydophila pneumoniae (Chlamydia pneumoniae) accelerates the formation of complex atherosclerotic lesions in Apo E3-Leiden
Cardiovascular Research 56 (2002) 269 276 www.elsevier.com/ locate/ cardiores Chlamydophila pneumoniae (Chlamydia pneumoniae) accelerates the formation of complex atherosclerotic lesions in Apo E3-Leiden
Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR (1167)
 From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
LDL Uptake Cell-Based Assay Kit
 LDL Uptake Cell-Based Assay Kit Catalog Number KA1327 100 assays Version: 07 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
LDL Uptake Cell-Based Assay Kit Catalog Number KA1327 100 assays Version: 07 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 Principle of the Assay...
Identification of the Elementary Bodies of Chlamydia trachomatis in the Electron Microscope by an Indirect
 JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1975, p. 327-331 Copyright (D 1975 American Society for Microbiology Vol. 2, No. 4 Printed in U.S.A. Identification of the Elementary Bodies of Chlamydia trachomatis
JOURNAL OF CLINICAL MICROBIOLOGY, Oct. 1975, p. 327-331 Copyright (D 1975 American Society for Microbiology Vol. 2, No. 4 Printed in U.S.A. Identification of the Elementary Bodies of Chlamydia trachomatis
Received 22 February 1999/Returned for modification 17 March 1999/Accepted 26 March 1999
 INFECTION AND IMMUNITY, June 1999, p. 2909 2915 Vol. 67, No. 6 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae Infection of Human Endothelial
INFECTION AND IMMUNITY, June 1999, p. 2909 2915 Vol. 67, No. 6 0019-9567/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Chlamydia pneumoniae Infection of Human Endothelial
Aspirin antagonism in isonizaid treatment of tuberculosis in mice ACCEPTED. Department of Molecular Microbiology & Immunology, Bloomberg School of
 AAC Accepts, published online ahead of print on 4 December 2006 Antimicrob. Agents Chemother. doi:10.1128/aac.01145-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 4 December 2006 Antimicrob. Agents Chemother. doi:10.1128/aac.01145-06 Copyright 2006, American Society for Microbiology and/or the Listed Authors/Institutions.
The value of urine samples from men with nongonococcal
 124 Genitourin Med 1991;67:124-128 The value of urine samples from men with nongonococcal urethritis for the detection of Chlamydia trachomatis P E Hay, B J Thomas, C Gilchrist, H M Palmer, C B Gilroy,
124 Genitourin Med 1991;67:124-128 The value of urine samples from men with nongonococcal urethritis for the detection of Chlamydia trachomatis P E Hay, B J Thomas, C Gilchrist, H M Palmer, C B Gilroy,
Role of Interferon in the Propagation of MM Virus in L Cells
 APPLIED MICROBIOLOGY, Oct. 1969, p. 584-588 Copyright ( 1969 American Society for Microbiology Vol. 18, No. 4 Printed in U S A. Role of Interferon in the Propagation of MM Virus in L Cells DAVID J. GIRON
APPLIED MICROBIOLOGY, Oct. 1969, p. 584-588 Copyright ( 1969 American Society for Microbiology Vol. 18, No. 4 Printed in U S A. Role of Interferon in the Propagation of MM Virus in L Cells DAVID J. GIRON
Instructions for Use. APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests
 3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
Chronic Chlamydia pneumoniae infection and asthma exacerbations in children
 Eur Respir J 1998; 11: 345 349 DOI: 10.1183/09031936.98.11020345 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Chronic Chlamydia pneumoniae
Eur Respir J 1998; 11: 345 349 DOI: 10.1183/09031936.98.11020345 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Chronic Chlamydia pneumoniae
Experimental Infection with Chlamydia pneumoniae in
 INFECTION AND IMMUNITY, Mar. 1990, p. 593-597 0019-9567/90/030593-05$02.00/0 Copyright 1990, American Society for Microbiology Vol. 58, No. 3 Experimental Infection with Chlamydia pneumoniae in Nonhuman
INFECTION AND IMMUNITY, Mar. 1990, p. 593-597 0019-9567/90/030593-05$02.00/0 Copyright 1990, American Society for Microbiology Vol. 58, No. 3 Experimental Infection with Chlamydia pneumoniae in Nonhuman
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
