Pathogenesis of septic shock in Pseudomonas aeruginosa pneumonia
|
|
|
- Amos Marvin Davis
- 6 years ago
- Views:
Transcription
1 Pathogenesis of septic shock in Pseudomonas aeruginosa pneumonia Kiyoyasu Kurahashi, 1 Osamu Kajikawa, 2 Teiji Sawa, 1 Maria Ohara, 1 Michael A. Gropper, 1,3 Dara W. Frank, 4 Thomas R. Martin, 2 and Jeanine P. Wiener-Kronish 1,5,6 1 Department of Anesthesia and Perioperative Care, University of California San Francisco, San Francisco, California 94143, USA 2 Medical Research Service, Seattle Veterans Affairs Medical Center and the Division of Pulmonary and Critical Care Medicine, Department of Medicine, University of Washington School of Medicine, Seattle, Washington 98108, USA 3 Department of Physiology, University of California San Francisco, San Francisco, California 94143, USA 4 Department of Microbiology and Molecular Genetics, Medical College of Wisconsin, Milwaukee, Wisconsin 53226, USA 5 Department of Medicine, University of California San Francisco, California 94143, USA 6 Cardiovascular Research Institute, University of California San Francisco, California 94143, USA Address correspondence to: Jeanine P. Wiener-Kronish, Department of Anesthesia and Perioperative Care, University of California San Francisco, San Francisco, California , USA. Phone: (415) ; Fax: (415) ; WienerKJ@Anesthesia.ucsf.edu. Received for publication April 19, 1999, and accepted in revised form August 2, The pathogenesis of septic shock occurring after Pseudomonas aeruginosa pneumonia was studied in a rabbit model. The airspace instillation of the cytotoxic P. aeruginosa strain PA103 into the rabbit caused a consistent alveolar epithelial injury, progressive bacteremia, and septic shock. The lung instillation of a noncytotoxic, isogenic mutant strain (PA103 UT), which is defective for production of type III secreted toxins, did not cause either systemic inflammatory response or septic shock, despite a potent inflammatory response in the lung. The intravenous injection of PA103 did not cause shock or an increase in TNF-α, despite the fact that the animals were bacteremic. The systemic administration of either anti TNF-α serum or recombinant human IL-10 improved both septic shock and bacteremia in the animals that were instilled with PA103. Radiolabeled TNF-α instilled in the lung significantly leaked into the circulation only in the presence of alveolar epithelial injury. We conclude that injury to the alveolar epithelium allows the release of proinflammatory mediators into the circulation that are primarily responsible for septic shock. Our results demonstrate the importance of compartmentalization of inflammatory mediators in the lung, and the crucial role of bacterial cytotoxins in causing alveolar epithelial damage in the pathogenesis of acute septic shock in P. aeruginosa pneumonia. J. Clin. Invest. 104: (1999). Introduction Nosocomial pneumonia is a leading cause of mortality among critically ill patients (1 3). The most common gram-negative organism associated with nosocomial pneumonia is Pseudomonas aeruginosa (4 6). Patients with P. aeruginosa pneumonia are also more likely to develop multiple organ failure and to die than patients with other types of pneumonia(7, 8). One explanation for the poor prognosis associated with P. aeruginosa pneumonia is that some P. aeruginosa strains cause acute lung epithelial injury and disseminate into the circulation (4, 7, 8). A tight alveolar epithelium is the barrier that prevents the dissemination of inhaled organisms into the systemic circulation. We have determined the mechanisms for dissemination of P. aeruginosa from the lung into the circulation. First, cytotoxic P. aeruginosa causes necrosis of epithelial cells (9, 10). Instilled P. aeruginosa bacteria disseminate across the injured epithelium (11 14), and production of type III secreted toxins by P. aeruginosa leads to acute epithelial injury and bacterial dissemination (14, 15). The role of circulating proinflammatory cytokines in the pathogenesis of septic shock has been well described (16, 17). In animal experiments, the sepsis syndrome is frequently mimicked by intravenous administration of bacteria or LPS. However, patients with sepsis are frequently not bacteremic, yet have severe hemodynamic instability (18). We therefore hypothesized that septic shock associated with P. aeruginosa pneumonia was secondary to the leak of mediators generated in the lungs crossing the injured epithelial barrier into the circulation. To test this hypothesis, we used a noncytotoxic isogenic mutant, PA103 UT. This strain was genetically engineered to be defective in the production of the known type III secreted toxins, and is thus unable to cause alveolar epithelial injury. We also compared the ability of PA103 to produce septic shock when administered by airspace instillation or intravenous infusion. We used anti-cytokine therapies to test whether cytokine-dependent mechanisms were involved in the development of septic physiology in P. aeruginosa pneumonia. Finally, using radiolabeled TNF-α instilled in the lung, we tested whether the leakage of TNF-α from the lung into the circulation depended on the presence of alveolar epithelial injury. Methods Culture conditions. Parental P. aeruginosa PA103 and its isogenic mutant PA103 exouexot:tc (PA103 UT) were used in this study (19, 20). PA103 UT was engineered by allelic replacement techniques to contain an insertion within exot and a deletion of exou (21). The bacterial suspension The Journal of Clinical Investigation September 1999 Volume 104 Number 6 743
2 was prepared as described previously (10). The number of bacteria in the solution was confirmed by serial dilution followed by culture on sheep-blood agar plates. In-vitro cytotoxicity assay. A human bronchial epithelial cell line immortalized by adenovirus-12-sv40 hybrid virus (BEAS-2B; American Type Culture Collection, Rockville, Maryland, USA) was used for the cytotoxicity assay, as reported previously (22). Either PA103 or PA103 UT was mixed with RPMI-1640 medium buffered with 25 mm HEPES without serum or antibiotics, and applied to the BEAS-2B cells in 1 of 2 bacterial concentrations (10 8 or 10 7 CFU/mL). Bacterialinduced cytotoxicity after 4 hours was quantified by counting the number of live and dead cells per field, using trypan blue dye to stain the cells. Two hundred cells were counted, and viability was calculated as the percentage of live cells. Animal investigation protocol. The protocol for all animal experiments was approved by the Animal Research Committee of the University of California San Francisco. Pathogen free male New Zealand white rabbits (range of body weight kg; Western Oregon Rabbit, Philomath, Oregon, USA) were used for all animal experiments. Animal preparation and general protocol. Anesthesia was induced with intravenous sodium pentobarbital (25 mg/kg) and maintained with halothane. A tracheotomy was done, and an endotracheal tube (4.0-mm inner diameter) was inserted. Mechanical ventilation was maintained with a constant-volume pump (Harvard Apparatus Inc., Holliston, Massachusetts, USA), with an inspired oxygen fraction of 1.0 at a tidal volume of 20 ml/kg body weight; positive end-expiratory pressure of 3 cm H 2 O was applied. The respiratory rate was adjusted to maintain an arterial CO 2 level between 35 and 45 mmhg. A polyethylene tube (0.86-mm inner diameter) was inserted through the endotracheal tube into the right lower lung, for subsequent instillation of a bacterial suspension or a vehicle solution. The right carotid artery was catheterized for measurement of blood pressure and sampling of arterial blood. A thermodilution catheter was inserted through the right femoral vein into the pulmonary artery. Then the rabbits were placed in the right lateral decubitus position and were observed for a minimum of 30 minutes before taking baseline measurements. In all experiments, pressures were monitored regularly as reported (14). All animals received an intravenous infusion of lactated Ringer s solution (L/R; 4 ml/kg per hour) throughout the experimental period. Blood (700 µl) was sampled every 15 minutes for quantitative cultures of bacteria, for quantitation of the efflux of the airspace-protein tracer into the circulation, and for measurements of cytokines. Experimental groups. Table 1 summarizes the experimental groups and treatments. Twenty-eight rabbits were used in experiments comparing hemodynamics and quantities of plasma mediators. Four rabbits (control) received an airspace instillate that did not contain bacteria. Five rabbits (PA103) received an airspace instillate that contained PA103; 4 rabbits ( UT) received an airspace instillate that contained PA103 UT. All 3 of these groups received continuous infusions of L/R (3 ml/kg) that did not contain bacteria. Instillation of P. aeruginosa and airspace-protein tracer. The instillate (3 ml/kg) contained 125 I-labeled human albumin (0.5 µci; Merck Frosst Canada, Kirkland, Quebec, Canada) as the airspace-protein tracer, and 5% BSA in L/R. In designated experiments, bacteria (10 8 CFU/mL of PA103 or PA103 UT) were also added to the instillates. The instillates were administered using a published method, and calculations were done as described previously (12 14). Pretreatment with anti TNF-α serum or recombinant human IL-10. Five additional rabbits (PA103 with anti TNF-α) were pretreated with an intravenous injection of 1 ml goat anti-rabbit TNF-α serum (a generous gift from J.C. Mathison and V. Kravchenco, Scripps Research Institute, San Diego, California, USA) 30 minutes before administration of the airspace instillate containing PA103. The anti TNF-α serum, which was made from blood collected in sterile pyrogen-free and endotoxin-free devices, had more than 10 6 neutralizing units per milliliter. Because the injection of nonimmune serum as a control for the administration of the anti TNF-α serum had no effects on either physiological parameters or cytokine release in our preliminary experiments performed in the rabbits instilled with PA103, we compared the anti TNF-α serum group with the PA103 group that had not received non-immune serum pretreatment. Another 5 rabbits (PA103 with rhil-10) were pretreated with an intravenous injection of 50 µg/kg of recombinant human IL-10 (rhil-10; Schering-Plough Corp., Kenilworth, New Jersey, USA) 30 minutes before the administration of an airspace instillate containing PA103. This dose was found to be effective in blocking the biological effects of TNF-α in a previous investigation using rhil-10 (23). Intravenous injection of P. aeruginosa. Five other rabbits (intravenous PA103) received L/R (3 ml/kg body weight) containing PA103 (10 8 CFU/mL) in an intravenous infusion continuously for 8 hours (i.e., CFU/kg per Figure 1 Cytotoxicity of PA103 and its isogenic mutant, PA103 UT. BEAS- 2B cells ( cells per well) were cultured with (a) 10 8 CFU/mL PA103 or PA103 UT, or (b) 10 7 CFU/mL PA103 or PA103 UT, for 4 hours. Triplicate measurements; mean ± SEM of percent change in cell viability. *P < 0.05 vs. group incubated with PA The Journal of Clinical Investigation September 1999 Volume 104 Number 6
3 Figure 2 MAP, cardiac output, and base excess for 7 hours. (a) Airspace instillation of PA103, PA103 UT, or L/R without bacteria (control group). (b) Pretreatment with intravenously administered anti TNF-α serum or rhil-10 followed by airspace instillation of PA103. (c) Intravenous infusion of PA103 and airspace instillation of vehicle. Mean ± SEM. Cardiac output is expressed as percent change from initial measurements. P < 0.05 vs. control group. *P < 0.05 vs. group instilled with PA103. minute). These rabbits received the same total number of bacteria as the rabbits undergoing the airspace-instillation treatment already described. The rabbits that were given the intravenous infusion of bacteria had their airspaces instilled with vehicle alone (no bacteria). 125 I TNF-α efflux from the airspaces. Seven additional rabbits were used to determine the movement of radiolabeled TNF-α from the airspaces to the circulation. One microcurie of 125 I TNF-α (1,000 Ci/mmol; Amersham International, Little Chalfont, United Kingdom) was added to the airspace instillate along with PA103 (n = 3), PA103 UT (n = 3), or the vehicle solution (n = 1). After the administration of the airspace instillate, blood was collected every 15 minutes for 8 hours, and the efflux of 125 I TNF-α into the circulation was calculated in the same way as the quantitation of airspace-protein tracer efflux was done (see above). One additional rabbit was injected intravenously with both 125 I TNF-α and 131 I- albumin, to compare the clearance rates of those 2 compounds from the circulation. Blood samples were collected repeatedly to measure the elimination half-life of these injected radiolabeled proteins from the circulation. Bronchoalveolar lavage. Another 8 rabbits underwent the same protocol as the above animals, with the addition of bronchoalveolar lavage (BAL). Their right lungs (containing the instillates) were removed and BAL was performed by instilling ice-cold PBS (50 ml) containing 0.1% EDTA. The BAL fluid (BALF) was centrifuged at 3,400 g at 4 C for 20 minutes, and the supernatant was filtered using a 0.2-µm filter. Cultures. To assess bacteremia, arterial blood (100 µl) was obtained every 15 minutes and cultured on tryptic soy The Journal of Clinical Investigation September 1999 Volume 104 Number 6 745
4 Figure 3 Airspace-protein tracer in blood. The quantity of 125 I-albumin that left the lungs and entered the circulation was calculated and shown as a percentage of the initial dose. (a) Airspace instillation of PA103, PA103 UT, or L/R without bacteria (control group). (b) Pretreatment with intravenously administered anti TNF-α serum or rhil-10 followed by airspace instillation of PA103. Mean ± SEM. P < 0.05 vs. control group. *P < 0.05 vs. group instilled with PA103. agar with 5% sheep-blood plates. To assess the quantity of bacteria remaining in the instilled lungs, right lungs were harvested and homogenized. Bacterial colonies were counted after incubation for 12 hours at 37 C. The quantity of bacteria was determined by multiplying counted colonies by the dilution ratio. TNF-α and chemokine assays. A biological TNF-α assay was performed using mouse sarcoma cells (WEHI-13VAR; American Type Culture Collection) as reported (24). TNFα activity of each sample was calculated by comparing absorbance to a standard curve plotted from dilutions of rabbit TNF-α (PharMingen, San Diego, California, USA) between 1.0 pg/ml and 1.0 ng/ml. The lower limit of detection for this assay was 1.0 pg/ml. ELISA assays were performed using goat polyclonal IgG raised against either recombinant rabbit (rrab) IL-8, rrab growth-regulated oncogene (GRO), or rrab monocyte chemotactic protein- 1 (MCP-1), as we have done before (25, 26). The lower limits of detection for the ELISA assays for IL-8, GRO, and MCP-1 were all 100 pg/ml. Statistical analysis. All values obtained incrementally during the 7-hour experimental period were analyzed using 2-way ANOVA with repeated measures followed by a Student s t test. Comparisons at 7 hours are presented. Other data were analyzed with an unpaired Student s t test. Data are presented as mean ± SEM. A value of P < 0.05 was accepted as statistically significant. Results In vitro cytotoxicity of PA103 and its isogenic mutant. The in vitro cytotoxicity of PA103 and PA103 UT was documented using BEAS-2B cells (Figure 1). PA103 UT, an isogenic mutant in which the exot and exou genes have been inactivated, is noncytotoxic. Therefore, PA103 UT could be used to create airspace inflammation without causing alveolar epithelial injury. Comparison of airspace instillation of PA103, PA103 UT, and vehicle. One of the 5 rabbits instilled with PA103 died after 7 hours; therefore, we analyzed the results from all rabbits at 7 hours after treatment. In the control rabbits, which did not receive airspace bacteria, mean arterial pressure (MAP), cardiac output, and base excess remained at baseline values for 7 hours (Figure 2a). Approximately 8% of the airspaceprotein tracer crossed the alveolar epithelium into the circulation over the 7-hour interval (Figure 3a). Bacterial cultures were negative in the blood of these animals, and plasma TNF-α did not exceed the baseline value for 7 hours. In the rabbits instilled with PA103, measurements of MAP, cardiac output, and base excess measurements decreased; all these animals were in septic shock (defined as a 20% decrease in cardiac output from baseline) after 7 hours (Figure 2a). Twenty percent of the airspace-protein tracer had left the lungs and entered the circulation after 7 hours (Figure 3a). Bacteremia increased exponentially after 4 hours and reached 100 CFU/100 µl after 7 hours (Figure 4a). Plasma TNF-α and chemokine levels increased significantly over the duration of the experiment (Figure 5a). TNF-α levels in the BALF were more than 100 times higher than the TNF-α levels in the plasma (Figure 6). In the rabbits instilled with PA103 UT, MAP, cardiac Figure 4 Quantity of bacteria in blood. (a) Airspace instillation of PA103 or PA103 UT. (b) Pretreatment with intravenously administered anti TNF-α serum or rhil-10 followed by airspace instillation of PA103. (c) Intravenous PA103 and airspace instillation of vehicle. Mean ± SEM. *P < 0.05 vs. group instilled with PA The Journal of Clinical Investigation September 1999 Volume 104 Number 6
5 Figure 5 Concentrations of plasma cytokines. (a) Airspace instillation of PA103 or PA103 UT. (b) Pretreatment with intravenously administered anti TNF-α serum or rhil-10 followed by airspace instillation of PA103. (c) Intravenous PA103 and airspace instillation of vehicle. Mean ± SEM. *P < 0.05 vs. group instilled with PA103. output, and base excess remained at baseline levels for the entire 7-hour interval (Figure 2a). Efflux of the airspace-protein tracer into the circulation was approximately 9%, which was similar to that seen in the control animals, and significantly lower than the efflux seen after the airspace instillation of PA103 (Figure 3a). There was no bacteremia in the rabbits instilled with PA103 UT (Figure 4a). The plasma levels of TNF-α, IL- 8, GRO, and MCP-1 were all significantly lower than those detected in the animals instilled with PA103 (Figure 5a). TNF-α levels in BALF were significantly higher in the animals instilled with PA103 UT than in PA103- instilled animals. When TNF-α levels in plasma and BALF were compared in PA103 UT-instilled animals, there was a 10,000-fold higher level in BALF than in plasma (Figure 6). The TNF-α levels in the BALF confirms that both bacterial strains caused generation of high levels of TNF-α in the airspaces of instilled lungs; however, it appears that the TNF-α remained confined in the lungs of the animals instilled with PA103 UT. Efflux of airspace-instilled 125 I TNF-α from the lungs into the circulation, and clearance of intravenous 125 I TNF-α from the circulation. To compare the efflux of TNF-α from lungs instilled with PA103, PA103 UT, or vehicle (control group), we added 125 I TNF-α to the instillates. The efflux of 125 I TNF-α into the circulation of the rabbits instilled with PA103 was greater than the efflux in the control rabbits or in the rabbits instilled with PA103 UT (Figure 7a). In other rabbits, 125 I TNF-α and 131 I-albumin were injected intravenously to determine the clearance of TNF-α and albumin from the circulation. 125 I TNF-α clears from the circulation significantly faster than does 131 I-albumin (Figure 7b). The half-life for elimination of 125 I TNF-α was only 4 hours, whereas the half-life for elimination of 131 I- albumin was 31 hours. The faster clearance of 125 I TNF-α from the circulation contributed to the differences between the measured plasma levels of 125 I TNF-α (Figure 7a) and 125 I-albumin (Figure 3a). Systemic blockade of TNF-α. To test the hypothesis that the efflux of mediators across the injured epithelium was the cause of the septic shock, animals were pretreated intravenously with anti TNF-α serum or rhil-10. Pretreated animals had significantly improved MAP, cardiac outputs, and base excesses compared with those measurements in The Journal of Clinical Investigation September 1999 Volume 104 Number 6 747
6 Figure 6 Concentrations of cytokines in BALF and plasma. Comparison of instillation with PA103 and instillation with PA103 UT. Mean ± SEM. *P < 0.05 vs. group instilled with PA103. nontreated animals instilled with PA103 (Figure 2b). However, the efflux of the airspace-protein tracer into the circulation was similar in all 3 groups (Figure 3b), indicating a similar degree of alveolar epithelial injury among all 3. As shown in Figure 8, the number of bacteria in the instilled lungs at the end of the experimental period was not affected by the pretreatments. However, bacteremia was significantly improved by pretreatment with rhil-10 before the instillation of PA103 (Figure 4b). TNF-α activity did not exceed baseline levels during the 7-hour period in the animals that were both pretreated with anti TNF-α or rhil-10 and infected with PA103 (Figure 5b). Therefore, both pretreatments significantly decreased TNF-α activity for the duration of the experiment. IL-8 levels similarly did not exceed baseline in the pretreated animals (Figure 5b). MCP-1 levels were also significantly lower in animals pretreated with anti TNF-α or rhil-10 (Figure 5b). However, GRO levels were significantly lowered only by pretreatment with rhil-10. Intravenous infusion of PA103. To determine the effects of PA103 in the circulation in the absence of alveolar epithelial lung injury, intravenous infusions of PA103 were given to animals that had vehicle instilled into their airspaces. Animals receiving infusions of PA103 did not develop septic shock; their MAP, cardiac output, and base excess remained at baseline levels for 7 hours (Figure 2c). All these rabbits survived the duration of the experiments despite constant high-level bacteremia (Figure 4c). Plasma TNF-α levels increased moderately for the first 2 hours and then declined in the animals infused with PA103. After 7 hours, the TNF-α plasma levels in these animals were significantly lower than the TNF-α levels in the animals receiving airspace instillation of PA103 (Figure 5c). The infusion of PA103 did not lead to detectable levels of IL-8 in the plasma. Plasma GRO and MCP-1 levels rose earlier in the animals receiving intravenous PA103 than in animals instilled with PA103; however there were no significant differences in these values after 7 hours (Figure 5c). Discussion We previously documented that strains of P. aeruginosa can be classified as cytotoxic or noncytotoxic to the lungs (19). The airspace instillation of a cytotoxic strain, PA103, consistently produces alveolar epithelial lung injury and bacteremia (14, 15, 20). This experimental paradigm is unique in that septic shock and bacteremia are consistently produced, thereby allowing investigation of the mechanisms causing their development, as well as the relationship of these conditions to lung epithelial injury. Our previous studies documented that instillation of noncytotoxic P. aeruginosa strains into the lungs of mice or rats did not produce lung injury or death when compared with the instillation of cytotoxic strains (10, 19). An isogenic mutant bacteria lacking specific cytotoxins (PA103 UT) was instilled to create lung inflammation without epithelial injury or bacteremia. These investigations showed that instillation of PA103 UT led to significantly elevated levels of TNF-α in Figure I TNF-α tracer studies. (a) 125 I TNF-α was instilled with PA103, PA103 UT, or vehicle. The quantity of 125 I TNF-α in the circulation is shown as a percentage of the initial dose instilled into the airspaces. Mean ± SEM. *P < 0.05 vs. group instilled with airspace PA103. (b) Plasma concentration curves of intravenously injected 125 I TNF-α and 131 I-albumin. Data are percentages of the peak values at 1 minute after the injection. 748 The Journal of Clinical Investigation September 1999 Volume 104 Number 6
7 the BALF of rabbit lungs levels 10,000-fold higher than in the plasma of the same animals. These experiments support our prior observations that lung inflammation can occur without increased epithelial permeability (27, 28). The difference between TNF-α levels in the airspaces and the plasma is consistent with the containment of TNF-α within the lung by an intact epithelial barrier. Further evidence for this comes from the experiments in which radiolabeled TNF-α was instilled along with PA103 or PA103 UT. The efflux of labeled TNF-α was significantly increased only when the cytotoxic PA103 was instilled into the airspaces. However, plasma TNF-α levels resulting from PA103 instillation were much higher than those predicted assuming that the only source of circulating TNF-α was the lung. This suggests that leakage of proinflammatory mediators from the lung into the circulation stimulates systemic TNF-α production. The instillation of PA103 UT also led to the generation of levels of IL-8 in the airspaces that were comparable to those generated in response to instilled PA103. However, IL-8 was undetectable in the circulation of the animals instilled with PA103 UT. This can be explained by the fact that little lung injury occurred, or by the fact that IL-8 coming from the lung was absorbed onto circulating receptors (29). Plasma IL-8 levels were detectable in the animals instilled with PA103; this was consistent with the efflux of airspace IL-8 across the injured epithelium in amounts that exceeded the binding capacity of circulating receptors. A previous investigation by Tutor et al. documented leakage of TNF-α from isolated, perfused rat lungs injured with α-naphthylthiourea (30). Clinical investigations measuring proinflammatory mediators in patients with acute lung injury have documented high concentrations of inflammatory mediators in BALF and in pulmonary-edema fluid (31, 32). One investigation that compared mediator levels in a patient s pulmonary-edema fluid to levels in the same patient s plasma found increased concentrations of the inflammatory mediators in the lung fluids, and low concentrations of the same mediators in the plasma (33). Plasma cytokine levels vary markedly in the course of experimental and clinical septic shock; therefore the timing of plasma sampling may explain the discrepancy between those results and our own. Our investigation documents that significant bacterial-induced alveolar epithelial injury causes a progressive increase in circulating TNF-α and IL-8 that is most likely due to leakage from the airspaces. The systemic administration of anti TNF-α serum or rhil-10 blocked the increase of proinflammatory mediators in the circulation, and prevented hypotension and decreased cardiac output. Pretreatment with anti TNF-α serum did not significantly decrease bacteremia; however, shock was prevented. The rhil-10 pretreatment significantly decreased bacteremia without affecting the degree of alveolar epithelial injury. This suggests that the presence of rhil-10 led to improved clearance of circulating bacteria. Thus, Table 1 Classification of experimental groups Figure 8 Number of bacteria in the right lung at the end of experiments (7 hours). The quantity of bacteria in the lungs was determined by multiplying colonies by the dilution ratio. Mean ± SEM. despite the presence of bacteria in the lung and in the circulation, and the development of lung injury, septic physiology did not develop when the systemic effects of the lung-generated inflammatory mediators had been blocked by anti TNF-α or by rhil-10. Finally, intravenous infusion of PA103 did not cause septic shock. The presence of P. aeruginosa in the circulation was not sufficient for the development of septic physiology, even though the concentration of circulating bacteria was greater than that found circulating in the blood of septic patients (34). Notably, the circulatory levels of some of the proinflammatory mediators were different in the PA103-infused animals compared with the PA103-instilled animals. Plasma TNF-α levels in the animals infused with PA103 transiently increased early and then significantly declined later. This phenomenon is similar to the changes observed in serum TNF-α levels after LPS injections in rats (35) and in primates (36). Plasma IL-8 levels were significantly different between treatments; there was no detectable plasma IL-8 in the animals infused with PA103, whereas there was a large increase in plasma IL-8 in the animals instilled with PA103. These results show the crucial importance of a tissue infection, as opposed to bacteremia, in the pathogenesis of septic shock. The results are consistent with the interpretation that mediators leaked from the lung in response to bacterial cytotoxicity and contributed to the development of septic shock. We recently demonstrated that the toxin Treatment group (n) Bacterial strain and route of infection Tracheal instillation Intravenous injection Pretreatment Control 4 L/R L/R None PA103 5 PA103 in L/R L/R None UT 4 PA103 UT in L/R L/R None PA103 with anti TNF-α 5 PA103 in L/R L/R Anti TNF-α serum PA103 with rhil-10 5 PA103 in L/R L/R rhil-10 Intravenous PA103 5 L/R PA103 in L/R None Each group of rabbits received the above combination of tracheal instillation and intravenous injection, with or without pretreatment. Each rabbit was observed for 8 hours under inhalation anethesia with mechanical ventilation, unless the rabbit died within 8 hours. The Journal of Clinical Investigation September 1999 Volume 104 Number 6 749
8 secretion system of P.aeruginosa could be blocked by antibody therapy (37). Therapeutic strategies that decrease or prevent epithelial permeability in patients with pneumonia or lung injury should limit the development of septic shock. Acknowledgments We thank Richard Shanks for his technical assistance. K. Kurahashi especially wishes to thank I. Kudoh and F. Okumura (Department of Anesthesiology, School of Medicine, Yokohama City University, Yokohama, Japan) for providing an opportunity to participate in this project in the USA. This work was supported by grants from the National Institutes of Health (HL and HL to J.P. Wiener- Kronish; AI and AI to D.W. Frank; HL-30542, GM-37696, and AI to T.R. Martin). 1. Fagon, J.Y., et al Nosocomial pneumonia in ventilated patients: a cohort study evaluating attributable mortality and hospital stay. Am. J. Med. 94: Rouby, J.J Nosocomial infection in the critically ill. The lung as a target organ. Anesthesiology. 84: Rouby, J.J Histology and microbiology of ventilator-associated pneumonias. Semin. Respir. Infect. 11: Brewer, S.C., Wunderink, R.G., Jones, C.B., and Leeper, K.V., Jr Ventilator-associated pneumonia due to Pseudomonas aeruginosa. Chest. 109: Craven, D.E., and Steger, K Nosocomial pneumonia in mechanically ventilated adult patients: epidemiology and prevention in Semin. Respir. Infect. 11: Torres, A., et al Incidence, risk, and prognosis factors of nosocomial pneumonia in mechanically ventilated patients. Am. Rev. Respir. Dis. 142: Parrillo, J.E., et al Septic shock in humans. Advances in the understanding of pathogenesis, cardiovascular dysfunction and therapy. Ann. Intern. Med. 113: Taylor, G.D., Buchanan-Chell, M., Kirkland, T., McKenzie, M., and Wiens, R Bacteremic nosocomial pneumonia. A 7-year experience in one institution. Chest. 108: Apodaca, G., et al Characterization of Pseudomonas aeruginosainduced MDCK cell injury: glycosylation-defective host cells are resistant to bacterial killing. Infect. Immun. 63: Sawa, T., et al In vitro cellular toxicity predicts Pseudomonas aeruginosa virulence in lung infections. Infect. Immun. 65: Wiener-Kronish, J.P., Sawa, T., Kurahashi, K., Ohara, M., and Gropper, M.A Pulmonary edema associated with bacterial pneumonia. In Pulmonary edema. M. Matthay and D. Ingbar, editors. Marcel Dekker Inc. New York, NY Wiener-Kronish, J.P., Albertine, K.H., and Matthay, M.A Differential responses of the endothelial and epithelial barriers of the lung in sheep to Escherichia coli endotoxin. J. Clin. Invest. 88: Wiener-Kronish, J.P., et al Alveolar epithelial injury and pleural empyema in acute P. aeruginosa pneumonia in anesthetized rabbits. J. Appl. Physiol. 75: Kudoh, I., Wiener-Kronish, J.P., Hashimoto, S., Pittet, J.F., and Frank, D Exoproduct secretions of Pseudomonas aeruginosa strains influence severity of alveolar epithelial injury. Am. J. Physiol. 267:L551 L Sawa, T., et al IL-10 improves lung injury and survival in Pseudomonas pneumonia. J. Immunol. 159: Beutler, B., and Cerami, A Tumor necrosis, cachexia, shock, and inflammation: a common mediator. Annu. Rev. Biochem. 57: Vassalli, P The pathophysiology of tumor necrosis factors. Annu. Rev. Immunol. 10: Pepe, P.E., Potkin, R.T., Reus, D.H., Hudson, L.D., and Carrico, C.J Clinical predictors of the adult respiratory distress syndrome. Am. J. Surg. 144: Fleiszig, S.M.J., et al Cytotoxic and invasive strains of Pseudomonas aeruginosa are genotypically distinct at the loci encoding exoenzyme S. Infect. Immun. 65: Finck-Barbancon, V., et al ExoU expression by Pseudomonas aeruginosa correlates with acute cytotoxicity and epithelial injury. Mol. Microbiol. 25: Yahr, T.L., Vallis, A.J., Hancock, M.K., Barbieri, J.T., and Frank, D.W ExoY, a novel adenylate cyclase secreted by the Pseudomonas aeruginosa type III system. Proc. Natl. Acad. Sci. USA. 95: Reddel, R.R., et al Transformation of human bronchial epithelial cells by infection with SV40 or adenovirus-12 SV40 hybrid virus, or transfection via strontium phosphate coprecipitation with a plasmid containing SV40 early region genes. Cancer Res. 48: Hurn, R.D., et al Pharmacokinetics and immunomodulatory properties of intravenously administered recombinant human interleukin-10 in healthy volunteers. Blood. 87: Espevik, T., and Nissen-Meyer, J A highly sensitive cell line, WEHI 164 clone 13, for measuring cytotoxic factor/tumor necrosis factor from human monocytes. J. Immunol. Methods. 95: Kajikawa, O., Goodman, R.B., Johnson, M.C., II, Konishi, K., and Martin, T.R Sensitive and specific immunoassays to detect rabbit IL-8 and MCP-1: cytokines that mediate leukocyte recruitment to the lungs. J. Immunol. Methods. 197: Kajikawa, O., Johnson, M.C., II, Goodman, R.B., Frevert, C.W., and Martin, T.R A sensitive immunoassay to detect the α-chemokine GRO in rabbit blood and lung fluids. J. Immunol. Methods. 205: Martin, T.R., Pistorese, B.P., Chi, E.Y., Goodman, R.B., and Matthay, M.A Effects of leukotriene B4 in the human lung. Recruitment of neutrophils into the alveolar spaces without a change in protein permeability. J. Clin. Invest. 84: Wiener-Kronish, J.P., Albertine, K.H., and Matthay, M.A Differential responses of the endothelial and epithelial barriers of the lung in sheep to Escherichia coli endotoxin. J. Clin. Invest. 88: Darbonne, W.C., et al Red blood cells are a sink for interleukin 8, a leukocyte chemotaxin. J. Clin. Invest. 88: Tutor, J.D., et al Loss of compartmentalization of alveolar tumor necrosis factor after lung injury. Am. J. Respir. Crit. Care Med. 149: Pugin, J., Ricou, B., Steinberg, K.P., Suter, P.M., and Martin, T.R Proinflammatory activity in bronchoalveolar lavage fluids from patients with ARDS, a prominent role for interleukin-1. Am. J. Respir. Crit. Care Med. 153: Goodman, R.B., et al Inflammatory cytokines in patients with persistence of the acute respiratory distress syndrome. Am. J. Respir. Crit. Care. Med. 154: Pugin, J., Verghese, G., Widmer, M.-C., and Matthay, M.A The alveolar space is the site of intense inflammatory and profibrotic reactions in the early phase of acute respiratory distress syndrome. Crit. Care Med. 27: Yagupsky, P., and Nolte, F.S Quantitative aspects of septicemia. Clin. Microbiol. Rev. 3: Nelson, S., et al Compartmentalization of intraalveolar and systemic lipopolysaccharide-induced tumor necrosis factor and the pulmonary inflammatory response. J. Infect. Dis. 159: Leturcq, D.J., et al Antibodies against CD14 protect primates from endotoxin-induced shock. J. Clin. Invest. 98: Sawa, T., et al Active and passive immunization with the Pseudomonas V antigen protects against type III intoxication and lung injury. Nat. Med. 5: The Journal of Clinical Investigation September 1999 Volume 104 Number 6
METHODS. participated in the study. Each subject had a normal physical examination, chest
 METHODS Subjects Thirty-four subjects (20 men and 14 women, mean age 28.5 ± 1.2 yr) participated in the study. Each subject had a normal physical examination, chest radiograph, electrocardiogram, and laboratory
METHODS Subjects Thirty-four subjects (20 men and 14 women, mean age 28.5 ± 1.2 yr) participated in the study. Each subject had a normal physical examination, chest radiograph, electrocardiogram, and laboratory
Intravenous Vitamin C. Severe Sepsis Acute Lung Injury
 Intravenous Vitamin C Severe Sepsis Acute Lung Injury Alpha A. (Berry) Fowler, III, MD Professor of Medicine VCU Pulmonary Disease and Critical Care Medicine I Have No Disclosures Bacterial Sepsis Approximately
Intravenous Vitamin C Severe Sepsis Acute Lung Injury Alpha A. (Berry) Fowler, III, MD Professor of Medicine VCU Pulmonary Disease and Critical Care Medicine I Have No Disclosures Bacterial Sepsis Approximately
Respiratory Research. Open Access. Abstract. BioMed Central
 Respiratory Research BioMed Central Research TLR signaling is essential for survival in acute lung injury induced by virulent Pseudomonas aeruginosa secreting type III secretory toxins Karine Faure 1,
Respiratory Research BioMed Central Research TLR signaling is essential for survival in acute lung injury induced by virulent Pseudomonas aeruginosa secreting type III secretory toxins Karine Faure 1,
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Supplementary Figures
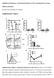 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Stress preconditioning attenuates oxidative injury to the alveolar epithelium of the lung following haemorrhage in rats
 Journal of Physiology (2002), 538.2, pp. 583 597 DOI: 10.1013/jphysiol.2001.013102 The Physiological Society 2002 www.jphysiol.org Stress preconditioning attenuates oxidative injury to the alveolar epithelium
Journal of Physiology (2002), 538.2, pp. 583 597 DOI: 10.1013/jphysiol.2001.013102 The Physiological Society 2002 www.jphysiol.org Stress preconditioning attenuates oxidative injury to the alveolar epithelium
How can human models of ALI inform clinical trials
 How can human models of ALI inform clinical trials Danny McAuley Royal Victoria Hospital and Queen s University of Belfast Critical Care Cananda Forum October 2012 Disclosures GSK; consultancy and participate
How can human models of ALI inform clinical trials Danny McAuley Royal Victoria Hospital and Queen s University of Belfast Critical Care Cananda Forum October 2012 Disclosures GSK; consultancy and participate
from patients with nosocomial pneumonia (1). Despite the use ofpotent antibiotics, the mortality rate ofp. aeruginosa
 Pseudomonas Aeruginosa-induced Lung and Pleural Injury in Sheep Differential Protective Effect of Circulating versus Alveolar Immunoglobulin G Antibody J. F. Pittet, * M. A. Matthay, * G. Pier,t M. Grady,
Pseudomonas Aeruginosa-induced Lung and Pleural Injury in Sheep Differential Protective Effect of Circulating versus Alveolar Immunoglobulin G Antibody J. F. Pittet, * M. A. Matthay, * G. Pier,t M. Grady,
In vitro bactericidal assay Fig. S8 Gentamicin protection assay Phagocytosis assay
 In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
In vitro bactericidal assay Mouse bone marrow was isolated from the femur and the tibia. Cells were suspended in phosphate buffered saline containing.5% BSA and 2 mm EDTA and filtered through a cell strainer.
Trauma Resuscitation: more than just blood products
 Trauma Resuscitation: more than just blood products Benjamin T. Houseman, MD, PhD Assistant Professor in Residence Department of Anesthesia University of California San Francisco Traumatic injury Leading
Trauma Resuscitation: more than just blood products Benjamin T. Houseman, MD, PhD Assistant Professor in Residence Department of Anesthesia University of California San Francisco Traumatic injury Leading
Stimulation of Lung Epithelial Liquid Clearance by Endogenous Release of
 Stimulation of Lung Epithelial Liquid Clearance by Endogenous Release of Catecholamines in Septic Shock in nesthetized Rats J. F. Pittet, J. P. Wiener-Kronish, M. C. McElroy, H. G. Folkesson, and M.. Matthay
Stimulation of Lung Epithelial Liquid Clearance by Endogenous Release of Catecholamines in Septic Shock in nesthetized Rats J. F. Pittet, J. P. Wiener-Kronish, M. C. McElroy, H. G. Folkesson, and M.. Matthay
Routine endotracheal cultures for the prediction of sepsis in ventilated babies
 Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Pathophysiology of Catheter-Related Infection. All sources of infection are potential targets for prevention. Infusates/ drugs. hub/lines Dressing
 Pathophysiology of Catheter-Related Infection All sources of infection are potential targets for prevention catheter hematogeneous Infusates/ drugs hub/lines Dressing skin Critically ill patient: 2-4 vascular
Pathophysiology of Catheter-Related Infection All sources of infection are potential targets for prevention catheter hematogeneous Infusates/ drugs hub/lines Dressing skin Critically ill patient: 2-4 vascular
COPD lungs show an attached stratified mucus layer that separate. bacteria from the epithelial cells resembling the protective colonic
 COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
Aerosolized Antibiotics in Mechanically Ventilated Patients
 Aerosolized Antibiotics in Mechanically Ventilated Patients Gerald C Smaldone MD PhD Introduction Topical Delivery of Antibiotics to the Lung Tracheobronchitis Aerosolized Antibiotic Delivery in the Medical
Aerosolized Antibiotics in Mechanically Ventilated Patients Gerald C Smaldone MD PhD Introduction Topical Delivery of Antibiotics to the Lung Tracheobronchitis Aerosolized Antibiotic Delivery in the Medical
5/1/2015 SEPSIS SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 INFECTION CAN BE CONFIRMED BY:
 SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 Omer Nasiroglu MD Baptist Children s Hospital Pediatric Emergency Department SEPSIS IS A SYSTEMIC INFLAMMATORY RESPONSE SYNDROME
SURVIVING SEPSIS CAMPAIGN HOW TO APPROACH THE POSSIBLE SEPTIC CHILD 2015 Omer Nasiroglu MD Baptist Children s Hospital Pediatric Emergency Department SEPSIS IS A SYSTEMIC INFLAMMATORY RESPONSE SYNDROME
without the permission of the author Not to be copied and distributed to others
 Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Emperor s Castle interior-prato What is the Role of Inhaled Polymyxins for Treatment of Respiratory Tract Infections? Helen Giamarellou CONCLUSIONS: Patients with Pseudomonas and Acinetobacter VAP may
Supplementary Figure 1. Antibiotic partially rescues mice from sepsis. (ab) BALB/c mice under CLP were treated with antibiotic or PBS.
 1 Supplementary Figure 1. Antibiotic partially rescues mice from sepsis. (ab) BALB/c mice under CLP were treated with antibiotic or PBS. (a) Survival curves. WT Sham (n=5), WT CLP or WT CLP antibiotic
1 Supplementary Figure 1. Antibiotic partially rescues mice from sepsis. (ab) BALB/c mice under CLP were treated with antibiotic or PBS. (a) Survival curves. WT Sham (n=5), WT CLP or WT CLP antibiotic
Human Cathepsin D ELISA Kit
 GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Human Cathepsin D ELISA Kit Catalog No. GWB-J4JVV9
GenWay Biotech, Inc. 6777 Nancy Ridge Drive San Diego, CA 92121 Phone: 858.458.0866 Fax: 858.458.0833 Email: techline@genwaybio.com http://www.genwaybio.com Human Cathepsin D ELISA Kit Catalog No. GWB-J4JVV9
Relationship between Cytotoxicity and Corneal Epithelial Cell Invasion by Clinical Isolates of Pseudomonas aeruginosa
 INFECTION AND IMMUNITY, June 1996, p. 2288 2294 Vol. 64, No. 6 0019-9567/96/$04.00 0 Copyright 1996, American Society for Microbiology Relationship between Cytotoxicity and Corneal Epithelial Cell Invasion
INFECTION AND IMMUNITY, June 1996, p. 2288 2294 Vol. 64, No. 6 0019-9567/96/$04.00 0 Copyright 1996, American Society for Microbiology Relationship between Cytotoxicity and Corneal Epithelial Cell Invasion
PATHOGENICITY OF MICROORGANISMS
 PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
Adrenaline aggravates lung injury caused by liver ischemia reperfusion and high-tidal-volume ventilation in rats
 Ota et al. Journal of Intensive Care (2016) 4:8 DOI 10.1186/s40560-016-0130-y RESEARCH Open Access Adrenaline aggravates lung injury caused by liver ischemia reperfusion and high-tidal-volume ventilation
Ota et al. Journal of Intensive Care (2016) 4:8 DOI 10.1186/s40560-016-0130-y RESEARCH Open Access Adrenaline aggravates lung injury caused by liver ischemia reperfusion and high-tidal-volume ventilation
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
DURING one-lung ventilation (OLV), inflammation
 Effect of Therapeutic Hypercapnia on Inflammatory Responses to One-lung Ventilation in Lobectomy Patients Wei Gao, M.D., Dong-Dong Liu, M.D., Di Li, M.D., Guang-xiao Cui, M.D., Ph.D. ABSTRACT Background:
Effect of Therapeutic Hypercapnia on Inflammatory Responses to One-lung Ventilation in Lobectomy Patients Wei Gao, M.D., Dong-Dong Liu, M.D., Di Li, M.D., Guang-xiao Cui, M.D., Ph.D. ABSTRACT Background:
Septic Shock. Rontgene M. Solante, MD, FPCP,FPSMID
 Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Septic Shock Rontgene M. Solante, MD, FPCP,FPSMID Learning Objectives Identify situations wherein high or low BP are hemodynamically significant Recognize complications arising from BP emergencies Manage
Depletion of Alveolar Macrophages by Treatment with 2-Chloroadenosine Aerosol
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, July 1999, p. 452 456 Vol. 6, No. 4 1071-412X/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Depletion of Alveolar Macrophages
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill
 Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Differential Responses of the Endothelial and Epithelial Barriers
 Differential Responses of the Endothelial and Epithelial Barriers of the Lung in Sheep to Escherichia coil Endotoxin J. P. Wioner-Kronish, K. H. Albertine, and M. A. Matthay With the technical assistance
Differential Responses of the Endothelial and Epithelial Barriers of the Lung in Sheep to Escherichia coil Endotoxin J. P. Wioner-Kronish, K. H. Albertine, and M. A. Matthay With the technical assistance
Serum cytokine levels in control and tumor-bearing male and female mice at day 15.
 Supplementary Table 1. Serum cytokine levels in control and tumor-bearing male and female mice at day 15. Male Female Cytokine Control C-26 Control C-26 IL-1β 2.0 ± 0.8 9.6 ± 1.5* 1.8 ± 0.2 6.8 ± 1.4*
Supplementary Table 1. Serum cytokine levels in control and tumor-bearing male and female mice at day 15. Male Female Cytokine Control C-26 Control C-26 IL-1β 2.0 ± 0.8 9.6 ± 1.5* 1.8 ± 0.2 6.8 ± 1.4*
Sepsis Wave II Webinar Series. Sepsis Reassessment
 Sepsis Wave II Webinar Series Sepsis Reassessment Presenters Nova Panebianco, MD Todd Slesinger, MD Fluid Reassessment in Sepsis Todd L. Slesinger, MD, FACEP, FCCM, FCCP, FAAEM Residency Program Director
Sepsis Wave II Webinar Series Sepsis Reassessment Presenters Nova Panebianco, MD Todd Slesinger, MD Fluid Reassessment in Sepsis Todd L. Slesinger, MD, FACEP, FCCM, FCCP, FAAEM Residency Program Director
Biological Consulting Services
 Biological Consulting Services of North Florida/ Inc. May 13, 2009 Aphex BioCleanse Systems, Inc. Dear Sirs, We have completed antimicrobial efficacy study on the supplied Multi-Purpose Solution. The testing
Biological Consulting Services of North Florida/ Inc. May 13, 2009 Aphex BioCleanse Systems, Inc. Dear Sirs, We have completed antimicrobial efficacy study on the supplied Multi-Purpose Solution. The testing
Bacteriemia and sepsis
 Bacteriemia and sepsis Case 1 An 80-year-old man is brought to the emergency room by his son, who noted that his father had become lethargic and has decreased urination over the past 4 days. The patient
Bacteriemia and sepsis Case 1 An 80-year-old man is brought to the emergency room by his son, who noted that his father had become lethargic and has decreased urination over the past 4 days. The patient
Systemic inflammation after myocardial infarction
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Systemic inflammation after myocardial infarction Rudiger, Alain DOI:
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2013 Systemic inflammation after myocardial infarction Rudiger, Alain DOI:
In Vivo Models and Cell Delivery for Lung Indications NO DISCLOSURES
 In Vivo Models and Cell Delivery for Lung Indications Marlowe Eldridge MD Department of Pediatrics and Biomedical Engineering University of Wisconsin School of Medicine and Public Health NO DISCLOSURES
In Vivo Models and Cell Delivery for Lung Indications Marlowe Eldridge MD Department of Pediatrics and Biomedical Engineering University of Wisconsin School of Medicine and Public Health NO DISCLOSURES
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
The epithelium in acute lung injury/acute respiratory distress syndrome Michael A. Gropper a,b and Jeanine Wiener-Kronish a
 The epithelium in acute lung injury/acute respiratory distress syndrome Michael A. Gropper a,b and Jeanine Wiener-Kronish a a Department of Anesthesia and Perioperative Care and b Critical Care Medicine,
The epithelium in acute lung injury/acute respiratory distress syndrome Michael A. Gropper a,b and Jeanine Wiener-Kronish a a Department of Anesthesia and Perioperative Care and b Critical Care Medicine,
Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia (Spain) Pulsion MAB
 State of the Art Hemodynamic Monitoring III CO, preload, lung water and ScvO2 The winning combination! Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia
State of the Art Hemodynamic Monitoring III CO, preload, lung water and ScvO2 The winning combination! Dr. F Javier Belda Dept. Anesthesiology and Critical Care Hospital Clinico Universitario Valencia
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Role of Integrin v 6 in Acute Lung Injury Induced by Pseudomonas aeruginosa
 INFECTION AND IMMUNITY, June 2008, p. 2325 2332 Vol. 76, No. 6 0019-9567/08/$08.00 0 doi:10.1128/iai.01431-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Role of Integrin v
INFECTION AND IMMUNITY, June 2008, p. 2325 2332 Vol. 76, No. 6 0019-9567/08/$08.00 0 doi:10.1128/iai.01431-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Role of Integrin v
New Strategies in the Management of Patients with Severe Sepsis
 New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
TNF-alpha ELISA. For Research Use Only. Not For Use In Diagnostic Procedures.
 TNF-alpha ELISA For the quantitative determination of TNF-alpha in serum, plasma, buffered solution or cell culture medium. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number:
TNF-alpha ELISA For the quantitative determination of TNF-alpha in serum, plasma, buffered solution or cell culture medium. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number:
Evidence-Based. Management of Severe Sepsis. What is the BP Target?
 Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
Evidence-Based Management of Severe Sepsis Michael A. Gropper, MD, PhD Professor and Vice Chair of Anesthesia Director, Critical Care Medicine Chair, Quality Improvment University of California San Francisco
Acute Respiratory Failure. Respiratory Failure. Respiratory Failure. Acute Respiratory Failure. Ventilatory Failure. Type 1 Respiratory Failure
 Acute Respiratory Failure Physiologic Classification Acute Respiratory Failure Type 1 Hypoxemic Type 2 Ventilatory Type 3 Post-op Type 4 Shock Mechanism Shunt Va Atelectasis Cardiac Output Phil Factor,
Acute Respiratory Failure Physiologic Classification Acute Respiratory Failure Type 1 Hypoxemic Type 2 Ventilatory Type 3 Post-op Type 4 Shock Mechanism Shunt Va Atelectasis Cardiac Output Phil Factor,
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
Hemodynamic monitoring beyond cardiac output
 Hemodynamic monitoring beyond cardiac output Prof Xavier MONNET Medical Intensive Care Unit Bicêtre Hospital Assistance publique Hôpitaux de Paris FRANCE Conflicts of interest Lilly GlaxoSmithKline Pulsion
Hemodynamic monitoring beyond cardiac output Prof Xavier MONNET Medical Intensive Care Unit Bicêtre Hospital Assistance publique Hôpitaux de Paris FRANCE Conflicts of interest Lilly GlaxoSmithKline Pulsion
Tuberculosis Intensive
 Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Tuberculosis Pathogenesis Lynn Horvath, MD April 3, 2012 Lynn Horvath, MD has the following disclosures to make: No conflict of interests No relevant
Tuberculosis Intensive San Antonio, Texas April 3 6, 2012 Tuberculosis Pathogenesis Lynn Horvath, MD April 3, 2012 Lynn Horvath, MD has the following disclosures to make: No conflict of interests No relevant
Updates in Sepsis 2017
 Mortality Cases Total U.S. Population/1,000 Updates in 2017 Joshua Solomon, M.D. Associate Professor of Medicine National Jewish Health University of Colorado Denver Background New Definition of New Trials
Mortality Cases Total U.S. Population/1,000 Updates in 2017 Joshua Solomon, M.D. Associate Professor of Medicine National Jewish Health University of Colorado Denver Background New Definition of New Trials
Brief Definitive Report
 Published Online: 1 January, 1989 Supp Info: http://doiorg/101084/jem1691333 Downloaded from jemrupressorg on June 25, 2018 Brief Definitive Report THE COMPLEX PATTERN OF CYTOKINES IN SERUM FROM PATIENTS
Published Online: 1 January, 1989 Supp Info: http://doiorg/101084/jem1691333 Downloaded from jemrupressorg on June 25, 2018 Brief Definitive Report THE COMPLEX PATTERN OF CYTOKINES IN SERUM FROM PATIENTS
Supporting Information
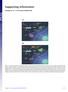 Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Enhanced Extracellular Growth of Staphylococcus aureus
 65 Enhanced Extracellular Growth of Staphylococcus aureus in the Presence of Selected Linear Peptide Fragments of Human Interleukin (IL) 1b and IL-1 Receptor Antagonist Siva Kanangat, 1 Michael S. Bronze,
65 Enhanced Extracellular Growth of Staphylococcus aureus in the Presence of Selected Linear Peptide Fragments of Human Interleukin (IL) 1b and IL-1 Receptor Antagonist Siva Kanangat, 1 Michael S. Bronze,
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections
 ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
Influenza A H1N1 (Swine Flu 2009) Hemagglutinin / HA ELISA Pair Set
 Influenza A H1N1 (Swine Flu 2009) Hemagglutinin / HA ELISA Pair Set Catalog Number : SEK001 To achieve the best assay results, this manual must be read carefully before using this product and the assay
Influenza A H1N1 (Swine Flu 2009) Hemagglutinin / HA ELISA Pair Set Catalog Number : SEK001 To achieve the best assay results, this manual must be read carefully before using this product and the assay
ONLINE SUPPLEMENT Title: CFTR dysfunction induces vascular endothelial growth factor synthesis in airway epithelium
 ONLINE SUPPLEMENT Title: CFTR dysfunction induces vascular endothelial growth factor synthesis in airway epithelium Martin C, Coolen N, Wu YZ, Thévenot G, Touqui L, PrulièreEscabasse V, Papon JF, Coste
ONLINE SUPPLEMENT Title: CFTR dysfunction induces vascular endothelial growth factor synthesis in airway epithelium Martin C, Coolen N, Wu YZ, Thévenot G, Touqui L, PrulièreEscabasse V, Papon JF, Coste
Original Article TLR4 contributes to mechanical ventilation induced lung injury in the rabbits
 Int J Clin Exp Pathol 2017;10(4):4700-4704 www.ijcep.com /ISSN:1936-2625/IJCEP0040416 Original Article TLR4 contributes to mechanical ventilation induced lung injury in the rabbits Hongmei Zhang 1, Pei
Int J Clin Exp Pathol 2017;10(4):4700-4704 www.ijcep.com /ISSN:1936-2625/IJCEP0040416 Original Article TLR4 contributes to mechanical ventilation induced lung injury in the rabbits Hongmei Zhang 1, Pei
2009 H1N1 Influenza ( Swine Flu ) Hemagglutinin ELISA kit
 2009 H1N1 Influenza ( Swine Flu ) Hemagglutinin ELISA kit Catalog Number : SEK001 To achieve the best assay results, this manual must be read carefully before using this product and the assay is run as
2009 H1N1 Influenza ( Swine Flu ) Hemagglutinin ELISA kit Catalog Number : SEK001 To achieve the best assay results, this manual must be read carefully before using this product and the assay is run as
Basics from anatomy and physiology classes Local tissue reactions
 Septicaemia & SIRS Septicaemia is a life-threatening condition that arises when the physical reaction to an infection, causes damage to tissue and organs Basics from anatomy and physiology classes Local
Septicaemia & SIRS Septicaemia is a life-threatening condition that arises when the physical reaction to an infection, causes damage to tissue and organs Basics from anatomy and physiology classes Local
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration
 Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
Fluid bolus of 20% Albumin in post-cardiac surgical patient: a prospective observational study of effect duration Investigators: Salvatore Cutuli, Eduardo Osawa, Rinaldo Bellomo Affiliations: 1. Department
Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery
 Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery Z.-M. Xing*, Z.-Q. Zhang*, W.-S. Zhang and Y.-F. Liu Anesthesia Department, No. 1 People s Hospital of Shunde, Foshan,
Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery Z.-M. Xing*, Z.-Q. Zhang*, W.-S. Zhang and Y.-F. Liu Anesthesia Department, No. 1 People s Hospital of Shunde, Foshan,
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Clearance in Anesthetized Sheep
 Beta-Adrenergic Agonists Increase Lung Liquid Clearance in Anesthetized Sheep Yves Berthiaume, Norman C. Staub, and Michael A. Matthay Cardiovascular Research Institute and Departments ofmedicine and Physiology,
Beta-Adrenergic Agonists Increase Lung Liquid Clearance in Anesthetized Sheep Yves Berthiaume, Norman C. Staub, and Michael A. Matthay Cardiovascular Research Institute and Departments ofmedicine and Physiology,
Buffering a Permissive Hypercapnia The Evidence
 Buffering a Permissive Hypercapnia The Evidence John Laffey Department of Anesthesia, St Michael s Hospital, University of Toronto, CANADA Disclosures Funding European Research Council [FP-7] Health Research
Buffering a Permissive Hypercapnia The Evidence John Laffey Department of Anesthesia, St Michael s Hospital, University of Toronto, CANADA Disclosures Funding European Research Council [FP-7] Health Research
Cell Free Hemoglobin and the Pathogenesis of ARDS
 Cell Free Hemoglobin and the Pathogenesis of ARDS New therapeutic target? Lorraine B. Ware M.D. Vanderbilt University Nashville, TN Financial disclosures: Dr. Ware receives research funding from Boehringer
Cell Free Hemoglobin and the Pathogenesis of ARDS New therapeutic target? Lorraine B. Ware M.D. Vanderbilt University Nashville, TN Financial disclosures: Dr. Ware receives research funding from Boehringer
ARDS and Lung Protection
 ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016
 Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016 Mitchell M. Levy MD, MCCM Professor of Medicine Chief, Division of Pulmonary, Sleep, and Critical Care
Novel pharmacotherapy in ARDS
 Novel pharmacotherapy in ARDS Danny McAuley Royal Victoria Hospital and Queen s University of Belfast Critical Care Cananda Forum October 2012 Disclosures GSK; consultancy and participate in research funded
Novel pharmacotherapy in ARDS Danny McAuley Royal Victoria Hospital and Queen s University of Belfast Critical Care Cananda Forum October 2012 Disclosures GSK; consultancy and participate in research funded
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES
 CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
CHAPTER 4 IMMUNOLOGICAL TECHNIQUES Nitroblue Tetrazolium Chloride (NBT) Reduction test NBT reduction test was evaluated by employing the method described by Hudson and Hay,1989 based upon principle that
Blockage of Arginine Vasopressin Receptor 2 Reduces Increase in Pulmonary Vascular Resistance in Ovine Sepsis Model
 Blockage of Arginine Vasopressin Receptor 2 Reduces Increase in Pulmonary Vascular Resistance in Ovine Sepsis Model Ernesto Lopez MD 1 Osamu Fujiwara MD 1, Baigalmaa Enkhtaivan MD 1, Jose Rojas PhD 2,
Blockage of Arginine Vasopressin Receptor 2 Reduces Increase in Pulmonary Vascular Resistance in Ovine Sepsis Model Ernesto Lopez MD 1 Osamu Fujiwara MD 1, Baigalmaa Enkhtaivan MD 1, Jose Rojas PhD 2,
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach
 Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Wet Lungs Dry lungs Impact on Outcome in ARDS. Charlie Phillips MD Division of PCCM OHSU 2009
 Wet Lungs Dry lungs Impact on Outcome in ARDS Charlie Phillips MD Division of PCCM OHSU 2009 Today s talk Pathophysiology of ARDS The case for dry Targeting EVLW Disclosures Advisor for Pulsion Medical
Wet Lungs Dry lungs Impact on Outcome in ARDS Charlie Phillips MD Division of PCCM OHSU 2009 Today s talk Pathophysiology of ARDS The case for dry Targeting EVLW Disclosures Advisor for Pulsion Medical
Cytomegalovirus in critically ill patients
 ! Cytomegalovirus in critically ill patients Frédéric Pène Medical ICU, Hôpital Cochin, AP-HP, Paris, France Université Paris Descartes, Sorbonne Paris Cité Institut Cochin, Inserm U1016, CNRS UMR-8104
! Cytomegalovirus in critically ill patients Frédéric Pène Medical ICU, Hôpital Cochin, AP-HP, Paris, France Université Paris Descartes, Sorbonne Paris Cité Institut Cochin, Inserm U1016, CNRS UMR-8104
Page 39 of 44. 8h LTA & AT h PepG & AT h LTA
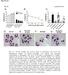 Page 39 of 44 Fig. S1 A: B: C: D: 8h LTA 8h LTA & AT7519 E: F: 8h PepG G: 8h PepG & AT7519 Fig. S1. AT7519 overrides the survival effects of lipoteichoic acid (LTA) and peptidoglycan (PepG). (A) Human
Page 39 of 44 Fig. S1 A: B: C: D: 8h LTA 8h LTA & AT7519 E: F: 8h PepG G: 8h PepG & AT7519 Fig. S1. AT7519 overrides the survival effects of lipoteichoic acid (LTA) and peptidoglycan (PepG). (A) Human
Neue Wirkungsmechanismen von Transfusionsplasma
 Neue Wirkungsmechanismen von Transfusionsplasma Lorenzo ALBERIO Médecin chef Hématologie générale et Hémostase Service et Laboratoire centrale d Hématologie CHUV, Lausanne Trauma patient Bleeding Thrombosis
Neue Wirkungsmechanismen von Transfusionsplasma Lorenzo ALBERIO Médecin chef Hématologie générale et Hémostase Service et Laboratoire centrale d Hématologie CHUV, Lausanne Trauma patient Bleeding Thrombosis
Quantifying Bordetella-induced Neutrophil Infiltration Using a Myeloperoxidase Assay
 Quantifying Bordetella-induced Neutrophil Infiltration Using a Myeloperoxidase Assay Sandra M. Fuentes, Research Scholar Faculty Mentor: Dr. Eric Harvill The Pennsylvania State University Abstract Bacteria
Quantifying Bordetella-induced Neutrophil Infiltration Using a Myeloperoxidase Assay Sandra M. Fuentes, Research Scholar Faculty Mentor: Dr. Eric Harvill The Pennsylvania State University Abstract Bacteria
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
TB Intensive San Antonio, Texas December 1-3, 2010
 TB Intensive San Antonio, Texas December 1-3, 2010 TB Pathogenesis and Transmission Lynn Horvath, MD; TCID December 1, 2010 Tuberculosis Pathogenesis Lynn L. Horvath, MD, FACP, FIDSA Associate Professor
TB Intensive San Antonio, Texas December 1-3, 2010 TB Pathogenesis and Transmission Lynn Horvath, MD; TCID December 1, 2010 Tuberculosis Pathogenesis Lynn L. Horvath, MD, FACP, FIDSA Associate Professor
Effect of Vaccine, Route, and Schedule on Antibody
 APPUED MICROBIOLOGY, Mar. 1969, p. 355-359 Copyright 1969 American Society for Microbiology Vol. 17, No. 3 Printed in U.S.A. Effect of Vaccine, Route, and Schedule on Antibody Response of Rabbits to Pasteurella
APPUED MICROBIOLOGY, Mar. 1969, p. 355-359 Copyright 1969 American Society for Microbiology Vol. 17, No. 3 Printed in U.S.A. Effect of Vaccine, Route, and Schedule on Antibody Response of Rabbits to Pasteurella
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Quantitative Determination of TNFá, a Multipotent Modulator of Immune Response
 Quantitative Determination of TNFá, a Multipotent Modulator of Immune Response 1. Introduction Tumor Necrosis Factor á (TNFá), also known as cachectin, is a polypeptide cytokine produced by monocytes and
Quantitative Determination of TNFá, a Multipotent Modulator of Immune Response 1. Introduction Tumor Necrosis Factor á (TNFá), also known as cachectin, is a polypeptide cytokine produced by monocytes and
Role of Alveolar Macrophages in Candida-Induced Acute Lung Injury
 CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Nov. 2001, p. 1258 1262 Vol. 8, No. 6 1071-412X/01/$04.00 0 DOI: 10.1128/CDLI.8.6.1258 1262.2001 Copyright 2001, American Society for Microbiology. All Rights
CLINICAL AND DIAGNOSTIC LABORATORY IMMUNOLOGY, Nov. 2001, p. 1258 1262 Vol. 8, No. 6 1071-412X/01/$04.00 0 DOI: 10.1128/CDLI.8.6.1258 1262.2001 Copyright 2001, American Society for Microbiology. All Rights
ANWICU knowledge
 ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN
 YK051 Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418 0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
YK051 Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418 0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Use of Blood Lactate Measurements in the Critical Care Setting
 Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Evaluation of Antibacterial Effect of Odor Eliminating Compounds
 Evaluation of Antibacterial Effect of Odor Eliminating Compounds Yuan Zeng, Bingyu Li, Anwar Kalalah, Sang-Jin Suh, and S.S. Ditchkoff Summary Antibiotic activity of ten commercially available odor eliminating
Evaluation of Antibacterial Effect of Odor Eliminating Compounds Yuan Zeng, Bingyu Li, Anwar Kalalah, Sang-Jin Suh, and S.S. Ditchkoff Summary Antibiotic activity of ten commercially available odor eliminating
The promise of nebulized antibiotic therapy
 1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
1 st ATHENA International Conference Athens, 19-20 November 2015 Let s Talk About Inhaled Antibiotics Inhaled Antibiotics: The Story Stijn BLOT Dept. of Internal Medicine Faculty of Medicine & Health Science
Supplementary fig. 1. Crystals induce necroptosis does not involve caspases, TNF receptor or NLRP3. A. Mouse tubular epithelial cells were pretreated
 Supplementary fig. 1. Crystals induce necroptosis does not involve caspases, TNF receptor or NLRP3. A. Mouse tubular epithelial cells were pretreated with zvad-fmk (10µM) and exposed to calcium oxalate
Supplementary fig. 1. Crystals induce necroptosis does not involve caspases, TNF receptor or NLRP3. A. Mouse tubular epithelial cells were pretreated with zvad-fmk (10µM) and exposed to calcium oxalate
The TNF & TNF receptor superfamillies
 TNF Luca Tordella The TNF & TNF receptor superfamillies R.M.Locksley et al.,the TNF and TNF receptor superfamilies: integrating mammalian biology, Cell, 104:487,2001 Late 1800s: Dr William Coley at the
TNF Luca Tordella The TNF & TNF receptor superfamillies R.M.Locksley et al.,the TNF and TNF receptor superfamilies: integrating mammalian biology, Cell, 104:487,2001 Late 1800s: Dr William Coley at the
Postoperative respiratory failure, apparent as hypoxemia,
 Activation of a Neutrophil-Derived Inflammatory Response in the Airways During Cardiopulmonary Bypass Toru Kotani, MD* Yoshifumi Kotake, MD Hiroshi Morisaki, MD Junzo Takeda, MD Hideyuki Shimizu, MD Toshihiko
Activation of a Neutrophil-Derived Inflammatory Response in the Airways During Cardiopulmonary Bypass Toru Kotani, MD* Yoshifumi Kotake, MD Hiroshi Morisaki, MD Junzo Takeda, MD Hideyuki Shimizu, MD Toshihiko
Sepsis and Multiple Organ Failure. J.G. van der Hoeven Radboud University Nijmegen Medical Centre
 Sepsis and Multiple Organ Failure J.G. van der Hoeven Radboud University Nijmegen Medical Centre Sepsis - initiation Microorganism Tissue Damage Pathogen Associated Molecular Pattern (PAMP) Pattern Recognition
Sepsis and Multiple Organ Failure J.G. van der Hoeven Radboud University Nijmegen Medical Centre Sepsis - initiation Microorganism Tissue Damage Pathogen Associated Molecular Pattern (PAMP) Pattern Recognition
Environmental survival of Neisseria meningitidis
 Environmental survival of Neisseria meningitidis Yih-Ling Tzeng, Emory University L.E. Martin, Emory University David Stephens, Emory University Journal Title: Epidemiology and Infection Volume: Volume
Environmental survival of Neisseria meningitidis Yih-Ling Tzeng, Emory University L.E. Martin, Emory University David Stephens, Emory University Journal Title: Epidemiology and Infection Volume: Volume
Vaccination against Pseudomonas aeruginosa Pneumonia in Immunocompromised Mice
 CLINICAL AND VACCINE IMMUNOLOGY, Feb. 2008, p. 367 375 Vol. 15, No. 2 1556-6811/08/$08.00 0 doi:10.1128/cvi.00419-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Vaccination
CLINICAL AND VACCINE IMMUNOLOGY, Feb. 2008, p. 367 375 Vol. 15, No. 2 1556-6811/08/$08.00 0 doi:10.1128/cvi.00419-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Vaccination
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS?
 Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
