A Cluster of Cases of Severe Acute Respiratory Syndrome in Hong Kong
|
|
|
- Mary Montgomery
- 6 years ago
- Views:
Transcription
1 original article A Cluster of Cases of Severe Acute Respiratory Syndrome in Hong Kong Kenneth W. Tsang, M.D., Pak L. Ho, M.D., Gaik C. Ooi, M.D., Wilson K. Yee, M.D., Teresa Wang, M.D., Moira Chan-Yeung, M.D., Wah K. Lam, M.D., Wing H. Seto, M.D., Loretta Y. Yam, M.D., Thomas M. Cheung, M.D., Poon C. Wong, M.D., Bing Lam, M.D., Mary S. Ip, M.D., Jane Chan, M.D., Kwok Y. Yuen, M.D., and Kar N. Lai, M.D., D.Sc. abstract background Information on the clinical features of the severe acute respiratory syndrome (SARS) will be of value to physicians caring for patients suspected of having this disorder. methods We abstracted data on the clinical presentation and course of disease in 10 epidemiologically linked Chinese patients (5 men and 5 women 38 to 72 years old) in whom SARS was diagnosed between February 22, 2003, and March 22, 2003, at our hospitals in Hong Kong, China. results Exposure between the source patient and subsequent patients ranged from minimal to that between patient and health care provider. The incubation period ranged from 2 to 11 days. All patients presented with fever (temperature, >38 C for over 24 hours), and most presented with rigor, dry cough, dyspnea, malaise, headache, and hypoxemia. Physical examination of the chest revealed crackles and percussion dullness. Lymphopenia was observed in nine patients, and most patients had mildly elevated aminotransferase levels but normal serum creatinine levels. Serial chest radiographs showed progressive air-space disease. Two patients died of progressive respiratory failure; histologic analysis of their lungs showed diffuse alveolar damage. There was no evidence of infection by Mycoplasma pneumoniae, Chlamydia pneumoniae, or Legionella pneumophila. All patients received corticosteroid and ribavirin therapy a mean (±SD) of 9.6±5.42 days after the onset of symptoms, and eight were treated earlier with a combination of beta-lactams and macrolide for 4±1.9 days, with no clinical or radiologic efficacy. From the University Departments of Medicine (K.W.T., M.C.-Y., W.K.L., P.C.W., B.L., M.S.I., J.C., K.N.L.), Clinical Microbiology (P.K.L., T.W., K.Y.Y.), and Diagnostic Radiology (G.C.O.), University of Hong Kong; the Department of Medicine, Kwong Wah Hospital (W.K.Y.); and the Department of Medicine, Pamela Youde Nethersole Eastern Hospital (L.Y.Y., T.M.C.) all in Hong Kong, China. Address reprint requests to Dr. Lai at the University Department of Medicine, University of Hong Kong, Queen Mary Hospital, Pokfulam, Hong Kong, China. This article was published at on March 31, Copyright 2003 Massachusetts Medical Society. conclusions SARS appears to be infectious in origin. Fever followed by rapidly progressive respiratory compromise is the key complex of signs and symptoms from which the syndrome derives its name. The microbiologic origins of SARS remain unclear. tsang-1
2 in the fall of 2002, there were reports from Guangdong Province in southern China of 305 cases of highly contagious and very severe atypical pneumonia of unknown cause. The condition appeared to be particularly prevalent among health care workers and their household members; many cases were rapidly fatal. 1 On March 13, 2003, as the condition began to spread from China, the World Health Organization (WHO) issued a global alert about the outbreak and instituted worldwide surveillance. In late February the U.S. Centers for Disease Control and Prevention (CDC) termed this condition the severe acute respiratory syndrome (SARS) and provided a clinical case definition. 2 Herein we report the clinical, radiologic, and laboratory features of 10 of our patients with SARS whose cases were epidemiologically linked. Since the microbiology of these cases remains unresolved, we provide the clinical and epidemiologic information for use in case recognition and management. methods patients Between February 22 and March 22, 2003, we identified 10 epidemiologically linked patients (all southern Chinese) whose disease met the CDC case definition of March 17, 2003, of SARS at our hospital cluster (Queen Mary Hospital, Kwong Wah Hospital, and Pamela Youde Nethersole Eastern Hospital) in Hong Kong (Table 1). 2 Patients were interviewed to ascertain their possible contacts with each other, as noted in Figure 1. radiologic assessment The chest radiographs of 10 patients were evaluated without reference to clinical details. Volumetric contrast-enhanced computed tomography (CT) with high-resolution CT scanning of the thorax was available in three patients (Patients 3, 4, and 10), and these were also reviewed. The pattern of opacification was categorized as air space (ground-glass opacification, focal consolidation, lobar consolidation, or patchy consolidation), interstitial (reticular), or diffuse (affecting all lung zones). The presence of pleural effusions was also noted. microbiologic evaluation Respiratory secretions (sputum in all patients and tracheal aspirate and bronchoalveolar-lavage fluid in Patients 1, 2, and 3) were analyzed for conventional bacteria (with blood, chocolate, and MacConkey agars), Legionella pneumophila(with BCYEa medium), and mycobacteria (with LJ medium). Gramstained and auramine-rhodamine stained smears were examined to search for bacterial or acid-fast morphotypes. Single or, when available, paired serum samples were tested for Mycoplasma pneumoniae (Serodia- Myco-II, Fujirebio) and Chlamydia pneumoniae and C. psittaci (MRL microimmunofluorescence kit). Urinary antigen detection (Binax Now test kits, Binax) was performed for L. pneumophila and pneumococcus. Immunofluorescence techniques were used to detect antigens in nasopharyngeal aspirates (and bronchoalveolar-lavage fluid in Patient 1) with commercially available reagents from Dako Diagnostics and Chemicon International. results patients and contact history The mean (±SD) age of the 10 patients (5 men and 5 women) was 52.5±11.0 years (median, 49.5; range, 35 to 72). Except as noted below, all of the patients had unremarkable medical histories. Patient 2 had stable hypertension and benign prostatic hypertrophy, Patient 4 had ischemic heart disease and non-insulin-dependent diabetes mellitus, and Patient 10 had non-insulin-dependent diabetes and resected renal-cell carcinoma of the right kidney. Patient 2 was taking metoprolol and nifedipine; Patient 4 was taking aspirin, diltiazem, and metformin; and Patient 10 was taking gliclazide and metformin. Eight of the 10 patients had never smoked, 1 was a current smoker (25 cigarettes per day), and 1 was a former smoker (20 cigarettes per day) who had stopped five years earlier. The contact history among the patients in this cluster is shown in Figure 1A. Patient 1, who had the first known case of SARS in Hong Kong, was a nephrologist working in a hospital in southern China who had traveled to Hong Kong on February 21, 2003, having first had symptoms five days earlier. On arrival in Hong Kong he felt well enough to sightsee and shop with his brother-in-law, but the next day he sought urgent care and was directly admitted to the intensive care unit (ICU) of Hospital A with respiratory failure. Patient 2, a Hong Kong resident, was the brother-in-law of Patient 1 and had had social contact with Patient 1 for 10 hours while sightseeing and shopping. Patient 3 was a nurse in the accident and emergency department 2-tsang
3 a cluster of cases of sars in hong kong Table 1. Characteristics of the Patients on Presentation.* Patient No. Summary Sex M M F M F F F F M M Age (yr) ±11.0 Smoking history Never Never Never Never Never Never Never Never Current Former Symptoms Cough Sputum production + 1+ Dyspnea Pleurisy Sore throat Rhinorrhea + 1+ Malaise Myalgia Rigor Fever (temperature >38 C for 24 hr) Headache Physical signs Crackles Percussion dullness Hemoglobin (g/dl) ±1.22 Leukocyte count ( 10 9 /liter) ±3.1 Lymphocyte count ( 10 9 /liter) ±0.4 Platelet count ( 10 9 /liter) ±77.8 ALT (U/liter) ±54.4 AST (U/liter) ±24.5 Creatinine (µmol/liter) ±27.1 PaCO 2 on room air (kpa) NA NA NA NA 3.8 NA 4.0±0.6 PaO 2 on room air (kpa) NA NA NA NA 11.9 NA 8.8±2.2 Oxygen saturation on room air (%) ±11.8 * Plus minus values are means ±SD. A plus sign indicates that the sign or symptom was present, and a minus sign that it was absent. Normal ranges are as follows: for hemoglobin, 13 to 18 g per deciliter; for the leukocyte count, to per liter; for the lymphocyte count, to per liter; for the platelet count, to per liter; for alanine aminotransferase, 6 to 53 U per liter; for aspartate aminotransferase, 13 to 33 U per liter; for creatinine, 82 to 106 µmol per liter; for the partial pressure of carbon dioxide (PaCO 2 ), 4.7 to 6.0 kpa; and for the partial pressure of oxygen (PaO 2 ), 12 to 17 kpa. To convert values for creatinine to milligrams per deciliter, divide by NA denotes not available. Data were available for seven patients. Data were available for five patients. tsang-3
4 A Shopping and sightseeing together for 10 hr Patient 1 Male/64 yr Died Indirect contact with patient 1 at the resuscitation room at Hospital A Staying on the same floor of Hotel X Close contact Hospital care contact Casual contact Hospital contact Patient 2 Male/53 yr Died Patient 3 Female/35 yr Patient 4 Male/72 yr Nursing patient 2 at the intensive care unit of Hospital A for 6 hr Nursing patient 4 at a general ward of Hospital B for up to 40 hr Visiting patient 4 once at Hotel X, once at Hospital B, and once at Hospital C Sharing same cubicle of a general ward at Hospital B with patient 4 for 5 days Patient 5 Female/56 yr Patient 6 Female/38 yr Patient 7 Female/47 yr Patient 8 Female/54 yr Patient 9 Male/50 yr Patient 10 Male/56 yr B Patient Number February March Zhong Shan, China Hotel X Shopping Hospital A Hospital B Hospital C Hospital D Died Onset of symptoms Beginning of treatment Figure 1. Contact History (Panel A) and Temporal Relation between Contact and the Onset of Symptoms (Panel B) in the 10 Patients with the Severe Acute Respiratory Syndrome. of Hospital A who was present in the same resuscitation room but at least 1 m away from Patient 1, who was being treated by another team of physicians and nurses. Patient 3 had no direct contact with Patient 1 and was wearing a surgical mask at the time. Patient 5 was a health care assistant who worked in the ICU of Hospital A and had unprotected hospital contact (without a mask or gown) with Patient 2 for six hours. Patient 4 was a Chinese-Canadian businessman 4-tsang
5 a cluster of cases of sars in hong kong who had returned to Hong Kong for a family reunion on February 13, He had not traveled outside Toronto for more than 12 months before his return to Hong Kong. His stay at Hotel X overlapped with that of Patient 1 for one day. There was no known direct contact between Patient 1 and Patient 4. Patient 4 could not recollect whether he had seen Patient 1 in the common areas of the hotel. Patients 6, 7, and 8 were nurses who worked at Hospital B, where Patient 4 was admitted and remained for six days for treatment of pneumonia before he was transferred to Hospital C. During this period, the nurses spent five eight-hour shifts stationed on the general ward on which Patient 4 was hospitalized. The three nurses recalled a close encounter with Patient 4 during which they cleaned him when he had fecal incontinence after an episode of diarrhea on March 3, The nurses did not wear masks or gowns during their routine nursing care of any patients on the ward. Patient 9 was the nephew of Patient 4 and visited him once at Hotel X, once at Hospital B, and once in the ICU of Hospital C, each time for 10 minutes. At the last of these visits, Patient 4 was receiving noninvasive positivepressure ventilation. Patient 10 stayed in the same cubicle (with six beds) on the same ward of Hospital B as Patient 4 for a total of five days while recovering uneventfully from a total nephrectomy for a resectable right renal-cell carcinoma. Another bed separated them from one another. There was no social or other contact between the two patients, who were both largely bedridden. Apart from these contacts, and with the exception of Patient 1, none of the patients had any known contacts with anyone with respiratory illness or had traveled to southern China, Vietnam, or Singapore for at least three months. Figure 1B shows the temporal relation between contact and the onset of symptoms in the 10 patients. The incubation period, calculated as the number of days between likely exposure and the onset of symptoms, 3 could be precisely determined only for Patients 2, 3, 4, and 5 (two, two, six, and two days, respectively), since the other patients had multiple contacts with the source patients. The ranges of possible incubation periods were 1 to 6, 5 to 11, 5 to 11, 1 to 5, and 2 to 7 days for Patients 6, 7, 8, 9, and 10, respectively. clinical and other features All 10 patients presented with fever (temperature, >38 C for more than 24 hours), and all but 1 also had rigor (Table 1). There was a median interval of five days (range, three to seven) from the onset of fever to the occurrence of dyspnea. All patients remained febrile until the initiation of empirical treatment with corticosteroids and ribavirin. Over half the patients also reported a nonproductive cough, dyspnea, malaise, and headache on presentation. On physical examination of the chest, crackles and dullness on percussion were detected in most patients. The results of cardiovascular, abdominal, and neurologic examination were normal in all patients given their known preexisting conditions. Mild leukocytosis and leukopenia were each observed in two patients at initial presentation. Lymphopenia (less than 1500 cells per cubic millimeter) was observed in nine patients; clinically significant thrombocytopenia (less than 50,000 platelets per cubic millimeter) was not observed. The aspartate aminotransferase level, alanine aminotransferase level, or both were elevated slightly (to less than four times the upper limit of the reference range in seven patients); serum creatinine levels were normal in eight patients. Five patients presented with hypoxemia, and three (Patients 4, 6, and 8) had infrequent diarrhea in the first three days after the onset of fever. The onset of diarrhea could not be attributed to antibiotic therapy in Patients 6 and 8, since they had not received such treatment before its onset. microbiologic assessment The sputum culture yielded only commensal species (Table 2). Acid-fast staining of all respiratory secretions was negative in each patient. Examination of nasopharyngeal aspirates for rapid viral antigen detection of influenzavirus A and B, parainfluenzavirus 1, 2, and 3, respiratory syncytial virus, and adenovirus was negative. The serologic titers of C. pneumoniae, C. psittaci, and M. pneumoniae showed no significant increase over a period of 7 to 10 days in the entire cohort. Urinary antigen detection for L. pneumophila and pneumococcus was negative in all cases. At this time, the microbiologic origin of SARS is unknown. radiologic assessment All patients except Patient 2 had abnormal chest radiographs on presentation. The primary abnormality on the initial chest radiograph was air-space shadowing: ground-glass opacities (in Patients 4, 5, and 10), focal consolidation (in Patients 3 and 9), or patchy consolidation (Patients 6, 7, and 8) (Fig. 2A). No interstitial pattern was found on the chest radiographs. Opacities were predominantly in the lower lung zones in eight patients (Patients 2, 3, tsang-5
6 Table 2. Results of Microbiologic Assessement in 10 Patients with the Severe Acute Respiratory Syndrome.* Patient No. Sputum Culture Sputum AFB Smear NPA Serologic Analysis Urinary Antigen Detection C. pneumoniae C. psittaci M. pneumoniae S. pneumoniae L. pneumophila 1 C <1:32 <1:32 <1:40 ND ND 2 C <1:32 <1:32 <1:40 ND ND 3 C <1:32 <1:32 <1:40 ND ND 4 C NA NA <1:32 <1:32 <1:40 5 C <1:32 <1:32 <1:40 ND ND 6 C 1:32 <1:32 <1:40 7 C <1:32 <1:32 <1:40 8 C <1:32 1:32 <1:40 9 C 1:32 <1:32 <1:40 10 C NA NA 1:128 <1:32 <1:40 * C denotes commensals, AFB acid-fast bacilli, NPA nasopharyngeal aspirate for rapid viral antigen detection, NA not available, and ND not done. 5, 6, 7, 8, 9, and 10) and in upper zones in one (Patient 4). None of the patients had pleural effusions. The air-space opacities increased in size, extent, and severity in seven patients (Patients 3, 4, 5, 6, 7, 9, and 10) within the first 10 days after admission. The chest radiograph of Patient 1 did not show clinically significant changes from presentation to death; a diffuse miliary nodulation was noted throughout. In Patient 2, the chest radiograph remained unremarkable for more than a week, after which diffuse opacification appeared (Fig. 2B); a similar course was observed in Patient 5. Among the survivors, six patients (Patients 3, 4, 6, 8, 9, and 10) had some improvement of the air-space opacities, with variable residual reticular opacities, within two weeks after presentation. Predominant abnormalities found on initial CT scans were subpleural focal consolidation with air bronchograms and ground-glass opacities. These occurred mostly, but not exclusively, in the posterior aspects of the lower lobes (Fig. 2C). No pleural effusions, mediastinal nodes, or central pulmonary embolisms were found. treatment and outcome All of the patients were treated empirically with corticosteroids and ribavirin, as noted below. Before this combination was administered, all patients except Patients 7 and 8 received a combination of a beta-lactam (Augmentin, Rocephin, or Maxipime) and a macrolide (clarithromycin or azithromycin) for a mean (and median) of four days (range, two to six), which had no effect on the overall clinical course, fever, or radiographically evident profusion of disease (Table 2 and Fig. 2 and 3). Empirical treatment consisted of a combination of intravenous ribavirin (8 mg per kilogram of body weight every eight hours) or oral ribavirin (1.2 g every eight hours, in Patient 4 only) and intravenous corticosteroids (hydrocortisone at a dose of 4 mg per kilogram every eight hours tapered to 200 mg every eight hours or methylprednisolone at a dose of 240 to 320 mg daily) in all patients (Fig. 3). There was a mean of 9.6±5.42 days (median, 12.5; range, 3 to 22) between the onset of symptoms and treatment with the combination of corticosteroids and ribavirin. Figure 3 shows the response in temperature, heart rate, oxygen saturation, and total leukocyte, lymphocyte, and platelet counts after the beginning of therapy. There was resolution of fever and improvement in heart rate within the first two days of starting treatment. There was also an increasing trend toward improved lymphocyte and platelet counts after eight days of treatment. In Patients 1 and 2 there was a steady deterioration in gas exchange despite an increase in ventilory support from noninvasive support to intubation and mechanical pressure-controlled ventilation with high positive end-expiratory pressures and a fraction of inspired oxygen of 1.0. Despite intensive physio- 6-tsang
7 a cluster of cases of sars in hong kong logical support, both patients died. Postmortem examination of the lungs of Patient 1 revealed marked alveolar edema with foci of hemorrhage and hyaline membrane formation. There was desquamation of pneumocytes, but there were few free inflammatory cells, either polymorphonuclear or mononuclear cells in the alveolar spaces. There were scattered foci of alveolar myxoid fibroblastic tissue, a finding consistent with the early organization phase of progressive pneumonia. Interalveolar septa were mildly thickened, with a mild mononuclear infiltrate. There was no tissue necrosis, viral inclusions, fungi, or bacteria on the sections. These features were considered to reflect severe diffuse alveolar damage. Patient 2 underwent a biopsy by videoassisted thoracoscopy on day 5 that showed only mild diffuse alveolar damage. From the onset of disease to the time of this writing, only Patient 3 has had a complete clinical recovery (no supplementary oxygen as of day 12) and radiographic recovery (resolution of right-lowerlobe consolidation on day 18), leading to her discharge on day 20. This patient has continued to have nonspecific malaise, even on day 26. From the onset of symptoms, Patients 4 through 10 have been unwell for 23.1±5.5 days (median, 25.5; range, 18 to 33) and have had a partial radiologic and clinical recovery. Only Patients 4, 7, and 9 are still oxygendependent; the mean oxygen saturation was 95.1± 2.59 percent (median, 96; range, 90 to 99) in the eight survivors. Patient 3 recovered completely and had no exercise restriction, whereas Patients 4, 7, and 9 were able to walk only three to five steps on the level, and Patients 5, 6, 8, and 10 were able to walk on the level without apparent restriction, within the confines of the isolation wards. Patients 4, 6, 7, 8, and 9 still reported dry cough, which was considered subjectively to be milder than that experienced at the onset of disease. None of the surviving patients reported any of the other symptoms listed in Table 2. (temperature, >38 C for more than 24 hours) and rigor, followed by dry cough, which may in some cases proceed rapidly to respiratory failure, accompanied by radiographic evidence of air-space disease. The incubation period in our patients was bediscussion Our experience with these 10 epidemiologically linked patients confirms that SARS is a contagious and rapidly progressive infectious disease that can affect otherwise healthy persons, sometimes after even trivial contacts. It is not known why some persons (such as the wife of Patient 4, who stayed in the same hotel room with him throughout) remain asymptomatic despite substantial exposure. SARS presents predominantly with high fever A B C Figure 2. Chest Radiographs of Patient 6 (Panel A), Showing Patchy Consolidation in the Right Lower Zone (Arrows), and Patient 2 (Panel B), Showing Diffuse Involvement of All Lung Zones in Both Lungs, and a High-Resolution CT Scan of Patient 4 (Panel C), Showing Subpleural Areas of Consolidation and Ground-Glass Opacification with Air Bronchogram (Arrow) Affecting the Posterior Aspects of the Lungs, Particularly the Lower Lobes. tsang-7
8 Temperature ( C) Heart Rate (beats/min) Oxygen Saturation (%) Total Leukocyte Count ( 10 9 /liter) Lymphocyte Count ( 10 9 /liter) Platelet Count ( 10 9 /liter) (N=5) 2 (N=6) 1 (N=6) 0 1 (N=10) (N=10) 2 (N=9) 3 (N=9) Day of Treatment 4 (N=8) 5 (N=8) 6 (N=5) 7 (N=4) 8 (N=3) Figure 3. Response to Treatment with an Intravenous Corticosteroid and Ribavirin for the 10 Patients with the Severe Acute Respiratory Syndrome. 8-tsang
9 a cluster of cases of sars in hong kong tween 1 and 11 days, and in most of our clear-cut cases, the patients presented 2 days after exposure. Our experience therefore singles out at-risk exposure (however trivial) to source patients and fever as the most important pointers to the diagnosis of SARS. Indeed, the finding that many people whose condition meets the CDC case definition 2 of SARS do not have respiratory failure important enough to meet WHO criteria 4 suggests that many people with this illness have respiratory insufficiency without frank failure. Although there was no clinical response to combined therapy with a beta-lactam and a macrolide, empirical treatment with a combination of a high-dose corticosteroid and ribavirin coincided with clinical improvement. Most patients appeared to have clinical and radiographic improvement, although the full time course of the illness is not known. It is also of note that the two patients who died did not have multiorgan failure, as is often the case with patients with the acute respiratory distress syndrome. The primary radiologic appearance of SARS is air-space shadowing determined on CT to be subpleural focal consolidation with air bronchograms and ground-glass opacities predominantly affecting the lower lobes. The initial radiographic appearance, however, may be normal. Air-space opacification progresses within a few days of presentation, increasing in size, extent, and severity. In some cases, there is further progression to diffuse opacification suggestive of the acute respiratory distress syndrome. Resolution of air-space shadowing occurs with features suggesting that the disease is entering a fibrotic phase. Radiographically, SARS may be indistinguishable from bacterial bronchopneumonia or viral infections, and more important, it shares CT features with other conditions that result in subpleural air-space disease, such as bronchiolitis obliterans organizing pneumonia and acute interstitial pneumonia. 5-7 In the later stages, particularly with diffuse involvement of the lungs, the radiographic appearance is similar to that of the acute respiratory distress syndrome. The clinical and radiographic features of the disease in our patients and, in particular, its highly contagious nature strongly point to a viral cause of SARS. Most patients with SARS had the onset of symptoms two to five days after exposure to the respective source patients. Such a short incubation period argues against infection with M. pneumoniae or C. pneumoniae. For M. pneumoniae, the reported incubation period ranges from 6 to 32 days, with a median of 14 days. 3 The incubation period for C. pneumoniae is unclear but appears to be long, with estimates ranging from 10 to 30 days. 8 L. pneumophila is not known to be transmitted from human to human and is thus most unlikely to be the causative agent. Our microbiologic tests also showed no evidence of infection by these agents. Research to identify potential viral infective agents in SARS is ongoing. Given the information we present on case transmission, it is important to take appropriate isolation precautions with patients suspected to have SARS. Information on current recommendations can be found at and Because the disease has appeared in many health care workers, they should have a high index of suspicion when fever and features suggestive of SARS develop in them or their family members. In such cases, we believe that health care workers should present themselves for evaluation, to avoid putting others at risk. When the microbiology of SARS is more fully understood, better methods of case identification should follow. We are indebted to Ms. Christina Yan, June Sun, and Christine So for technical assistance and to all the medical and nursing staff members who assisted in the care of these patients. references 1. Acute respiratory syndrome in China update 3: disease outbreak reported. Geneva: World Health Organization, (Accessed March 31, 2003, at don/2003_2_20/en.) 2. Severe acute respiratory syndrome (SARS). Atlanta: Centers for Disease Control and Prevention, (Accessed March 31, 2003, at 3. Mycoplasma. In: Hawker J, Begg N, Blair I, Reintjes R, Weinberg J. Communicable disease control handbook. London: Blackwell Science, 2001: Case definitions for surveillance of severe acute respiratory syndrome (SARS). Geneva: World Health Organization, (Accessed March 31, 2003 at sars/casedefinition.) 5. Muller NL, Staples CA, Miller RR. Bronchiolitis obliterans organizing pneumonia: CT features in 14 patients. AJR Am J Roentgenol 1990;154: Lee KS, Kullnig P, Hartman TE, Muller NL. Cryptogenic organizing pneumonia: CT findings in 43 patients. AJR Am J Roentgenol 1994;162: Primarck SL, Hartman TE, Ikezoe J, Akira M, Sakatani M, Muller NL. Acute interstitial pneumonia: radiographic and CT findings in nine patients. Radiology 1993;188: Jackson LA, Grayston JT. Chlamydia pneumoniae. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas, and Bennett s principles and practices of infectious diseases. 5th ed. Vol. 2. Philadelphia: Churchill Livingstone, 2000: Copyright 2003 Massachusetts Medical Society. tsang-9
Severe Acute Respiratory Syndrome ( SARS )
 Severe Acute Respiratory Syndrome ( SARS ) Dr. Mohammad Rahim Kadivar Pediatrics Infections Specialist Shiraz University of Medical Sciences Slides Designer: Dr. Ramin Shafieian R. Dadrast What is SARS?
Severe Acute Respiratory Syndrome ( SARS ) Dr. Mohammad Rahim Kadivar Pediatrics Infections Specialist Shiraz University of Medical Sciences Slides Designer: Dr. Ramin Shafieian R. Dadrast What is SARS?
A Major Outbreak of Severe Acute Respiratory Syndrome in Hong Kong
 The new england journal of medicine original article A Major Outbreak of Severe Acute Respiratory Syndrome in Hong Kong Nelson Lee, M.D., David Hui, M.D., Alan Wu, M.D., Paul Chan, M.D., Peter Cameron,
The new england journal of medicine original article A Major Outbreak of Severe Acute Respiratory Syndrome in Hong Kong Nelson Lee, M.D., David Hui, M.D., Alan Wu, M.D., Paul Chan, M.D., Peter Cameron,
Avian Influenza Clinical Picture, Risk profile & Treatment
 Avian Influenza Clinical Picture, Risk profile & Treatment Jantjie Taljaard Adult ID Unit Tygerberg Academic Hospital University of Stellenbosch jjt@sun.ac.za 083 419 1452 CLINICAL PICTURE The clinical
Avian Influenza Clinical Picture, Risk profile & Treatment Jantjie Taljaard Adult ID Unit Tygerberg Academic Hospital University of Stellenbosch jjt@sun.ac.za 083 419 1452 CLINICAL PICTURE The clinical
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Chapter. Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong. Epidemiology-University Hospital Experience
 content Chapter Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong 3 Nelson Lee, Joseph JY Sung Epidemiology-University Hospital Experience Diagnosis of SARS Clinical
content Chapter Severe Acute Respiratory Syndrome (SARS) Outbreak in a University Hospital in Hong Kong 3 Nelson Lee, Joseph JY Sung Epidemiology-University Hospital Experience Diagnosis of SARS Clinical
LEARNING FROM OUTBREAKS: SARS
 LEARNING FROM OUTBREAKS: SARS IFIC - APECIH 2017 KATHRYN N. SUH, MD, FRCPC 29 SEPTEMBER 2017 www.ottawahospital.on.ca Affiliated with Affilié à SEVERE ACUTE RESPIRATORY SYNDROME (SARS) Nov 2002 southern
LEARNING FROM OUTBREAKS: SARS IFIC - APECIH 2017 KATHRYN N. SUH, MD, FRCPC 29 SEPTEMBER 2017 www.ottawahospital.on.ca Affiliated with Affilié à SEVERE ACUTE RESPIRATORY SYNDROME (SARS) Nov 2002 southern
Radiographic Features of SARS in Paediatric Patients: A Review of Cases in Singapore
 340 Original Article Radiographic Features of SARS in Paediatric Patients: A Review of Cases in Singapore Jaiman V Emmanuel, 1 MBBS, FRCR, Uei Pua, 1 MBBS, FRCR, Gervais KL Wansaicheong, 1 FRCR, M Med,
340 Original Article Radiographic Features of SARS in Paediatric Patients: A Review of Cases in Singapore Jaiman V Emmanuel, 1 MBBS, FRCR, Uei Pua, 1 MBBS, FRCR, Gervais KL Wansaicheong, 1 FRCR, M Med,
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
MERS CoV Outbreak Riyadh, July-Aug 2015
 MERS CoV Outbreak Riyadh, July-Aug 2015 What is MERS-CoV? Middle East Respiratory Syndrome Coronavirus Virus causes severe acute respiratory illness associated with high mortality First identified in Jeddah,
MERS CoV Outbreak Riyadh, July-Aug 2015 What is MERS-CoV? Middle East Respiratory Syndrome Coronavirus Virus causes severe acute respiratory illness associated with high mortality First identified in Jeddah,
Early February Surveillance of severe atypical pneumonia in Hospital Authority in Hong Kong. Initiate contacts in Guangdong
 SARS: Aetiology JSM Peiris The University of Hong Kong & Queen Mary Hospital WHO SARS Laboratory Network Hospital Authority and Department of Health, HK Early February 2003 Surveillance of severe atypical
SARS: Aetiology JSM Peiris The University of Hong Kong & Queen Mary Hospital WHO SARS Laboratory Network Hospital Authority and Department of Health, HK Early February 2003 Surveillance of severe atypical
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Management of Severe Acute Respiratory Syndrome The Hong Kong University Experience
 Clinical Commentary Management of Severe Acute Respiratory Syndrome The Hong Kong University Experience Kenneth W. Tsang and Wah K. Lam University Department of Medicine, Division of Respiratory and Critical
Clinical Commentary Management of Severe Acute Respiratory Syndrome The Hong Kong University Experience Kenneth W. Tsang and Wah K. Lam University Department of Medicine, Division of Respiratory and Critical
SARS: A new infectious disease for a new century
 THEME: Systemic viral infections SARS: A new infectious disease for a new century BACKGROUND A new infectious disease swept the world in early 2003, causing restrictions on international travel and economic
THEME: Systemic viral infections SARS: A new infectious disease for a new century BACKGROUND A new infectious disease swept the world in early 2003, causing restrictions on international travel and economic
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Pneumonia. Dr. Rami M Adil Al-Hayali Assistant professor in medicine
 Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Pneumonia Dr. Rami M Adil Al-Hayali Assistant professor in medicine Definition Pneumonia is an acute respiratory illness caused by an infection of the lung parenchyma, associated with recently developed
Middle East Respiratory Syndrome-Coronavirus Infection: A Case Report of Serial Computed Tomographic Findings in a Young Male Patient
 Case Report Thoracic Imaging http://dx.doi.org/10.3348/kjr.2016.17.1.166 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2016;17(1):166-170 Middle East Respiratory Syndrome-Coronavirus Infection: A Case
Case Report Thoracic Imaging http://dx.doi.org/10.3348/kjr.2016.17.1.166 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2016;17(1):166-170 Middle East Respiratory Syndrome-Coronavirus Infection: A Case
Health Board Logo. Post SARS Outbreak Surveillance. Report of possible or probable cases (Form version 1) February 11 th 2004
 Post SARS Outbreak Surveillance Report of possible or probable cases (Form version 1) February 11 th 2004 This form is to be used for persons who fit the surveillance case definition of possible or probable
Post SARS Outbreak Surveillance Report of possible or probable cases (Form version 1) February 11 th 2004 This form is to be used for persons who fit the surveillance case definition of possible or probable
Surveillance Protocol for SARS - Draft
 Surveillance Protocol for SARS - Draft Note: This draft is dated June 06, 2003. Information about SARS is changing rapidly. Make certain you have the most current guidance. For your convenience all major
Surveillance Protocol for SARS - Draft Note: This draft is dated June 06, 2003. Information about SARS is changing rapidly. Make certain you have the most current guidance. For your convenience all major
NCCID RAPID REVIEW. 1. What are the case definitions and guidelines for surveillance and reporting purposes?
 NCCID RAPID REVIEW 1. What are the case definitions and guidelines for surveillance and reporting purposes? Middle East Respiratory Syndrome Coronavirus: Ten Questions and Answers for Canadian Public Health
NCCID RAPID REVIEW 1. What are the case definitions and guidelines for surveillance and reporting purposes? Middle East Respiratory Syndrome Coronavirus: Ten Questions and Answers for Canadian Public Health
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Clinical Diagnosis & Management of SARS
 Clinical Diagnosis & Management of SARS Joseph SUNG MD, PhD Department of Medicine & Therapeutics Prince of Wales Hospital The Chinese University of Hong Kong Hospital Authority of Hong Kong SAR Diagnosis
Clinical Diagnosis & Management of SARS Joseph SUNG MD, PhD Department of Medicine & Therapeutics Prince of Wales Hospital The Chinese University of Hong Kong Hospital Authority of Hong Kong SAR Diagnosis
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
Radiological syndroms. Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome
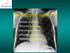 Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Severe adenovirus community-acquired pneumonia in immunocompetent adults: chest radiographic and CT findings
 Original Article Severe adenovirus community-acquired pneumonia in immunocompetent adults: chest radiographic and CT findings Dingyu Tan 1 *, Yangyang Fu 1 *, Jun Xu 1 *, Zhiwei Wang 2, Jian Cao 2, Joseph
Original Article Severe adenovirus community-acquired pneumonia in immunocompetent adults: chest radiographic and CT findings Dingyu Tan 1 *, Yangyang Fu 1 *, Jun Xu 1 *, Zhiwei Wang 2, Jian Cao 2, Joseph
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Novel Coronavirus 2012
 Novel Coronavirus 2012 Susan I. Gerber, MD Respiratory Virus Program Division of Viral Diseases National Center for Immunization and Respiratory Diseases Centers for Disease Control and Prevention Jan.
Novel Coronavirus 2012 Susan I. Gerber, MD Respiratory Virus Program Division of Viral Diseases National Center for Immunization and Respiratory Diseases Centers for Disease Control and Prevention Jan.
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Community-Acquired Pneumonia OBSOLETE 2
 Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
Community-Acquired Pneumonia OBSOLETE 2 Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with respect to appropriate
COPD exacerbation. Dr. med. Frank Rassouli
 Definition according to GOLD report: - «An acute event - characterized by a worsening of the patients respiratory symptoms - that is beyond normal day-to-day variations - and leads to a change in medication»
Definition according to GOLD report: - «An acute event - characterized by a worsening of the patients respiratory symptoms - that is beyond normal day-to-day variations - and leads to a change in medication»
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Radiologic Pattern of Disease in Patients with Severe Acute Respiratory Syndrome: The Toronto Experience 1
 SPECIAL REPORT 553 Radiologic Pattern of Disease in Patients with Severe Acute Respiratory Syndrome: The Toronto Experience 1 Narinder S. Paul, MD Heidi Roberts, MD Jagdish Butany, MD TaeBong Chung, MD
SPECIAL REPORT 553 Radiologic Pattern of Disease in Patients with Severe Acute Respiratory Syndrome: The Toronto Experience 1 Narinder S. Paul, MD Heidi Roberts, MD Jagdish Butany, MD TaeBong Chung, MD
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
and localized ground glass opacities, or bronchiolar focal or multifocal micronodules;
 E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
E1 Chest CT scan and Pneumoniae_YE Claessens et al- Supplementary methods Level of CAP probability according to CT scan - definite CAP: systematic alveolar condensation, or alveolar condensation with peripheral
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Chapter. Introduction. Presentation of SARS patients. Pathological considerations. Digital Radiography and PACS. Chest Radiograph appearances
 content Chapter The Role of Chest Radiographs in the Diagnosis of SARS 5 KT Wong, Gregory E. Antonio, Anil T. Ahuja Introduction Presentation of SARS patients Pathological considerations Role of Imaging
content Chapter The Role of Chest Radiographs in the Diagnosis of SARS 5 KT Wong, Gregory E. Antonio, Anil T. Ahuja Introduction Presentation of SARS patients Pathological considerations Role of Imaging
Nitrofurantoin-Induced Lung Toxicity
 Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Severe Nitrofurantoin-Induced Lung Toxicity Rami Jambeih, M.D. 1, John Flesher, M.D. 1,3, Joe J. Lin, M.D. 2,4 University of Kansas School of Medicine Wichita 1 Department of Internal Medicine 2 Department
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining
 Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Public Health: what is it?
 Public Health: what is it? Joseph JY Sung MD, PhD School of Public Health Chinese University of Hong Kong Center for Emerging Infectious Diseases Common Symptoms of SARS 100 90 Mean incubation period
Public Health: what is it? Joseph JY Sung MD, PhD School of Public Health Chinese University of Hong Kong Center for Emerging Infectious Diseases Common Symptoms of SARS 100 90 Mean incubation period
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
H5N1 / Avian Influenza Essentials. Quick Reference for Providers and Public Health Officials
 H5N1 / Avian Influenza Essentials Quick Reference for Providers and Public Health Officials December 2005 INFLUENZA Family: Orthomyxoviridae Genus: influenza virus Subtypes: A, B, and C Influenza A INFLUENZA
H5N1 / Avian Influenza Essentials Quick Reference for Providers and Public Health Officials December 2005 INFLUENZA Family: Orthomyxoviridae Genus: influenza virus Subtypes: A, B, and C Influenza A INFLUENZA
Supplementary Online Content
 Supplementary Online Content Uranga A, España, Bilbao A, et al. Duration of antibiotic treatment in communityacquired pneumonia: a multicenter randomized clinical trial. JAMA Intern Med. ublished online
Supplementary Online Content Uranga A, España, Bilbao A, et al. Duration of antibiotic treatment in communityacquired pneumonia: a multicenter randomized clinical trial. JAMA Intern Med. ublished online
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Interpretation of Chest Radiographs Paul Christensen, MD 10/21/09. Diagnostic Evaluation. Medical Evaluation & CXR Interpretation.
 Diagnostic Evaluation Medical Evaluation & CXR Interpretation University of Michigan TB Consultant Washtenaw County Medical history Physical examination Testing for TB exposure (previously covered) Radiologic
Diagnostic Evaluation Medical Evaluation & CXR Interpretation University of Michigan TB Consultant Washtenaw County Medical history Physical examination Testing for TB exposure (previously covered) Radiologic
Streptococcus Pneumoniae
 Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
INFLUENZA (Outbreaks; hospitalized or fatal pediatric cases)
 INFLUENZA (Outbreaks; hospitalized or fatal pediatric cases) 1. Agent: Influenza viruses A, B, and C. Only influenza A and B are of public health concern since they are responsible for epidemics. 2. Identification:
INFLUENZA (Outbreaks; hospitalized or fatal pediatric cases) 1. Agent: Influenza viruses A, B, and C. Only influenza A and B are of public health concern since they are responsible for epidemics. 2. Identification:
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
SARS and the Clinical Laboratory
 SARS and the Clinical Laboratory Susan M. Poutanen, MD, MPH, FRCPC Microbiologist, Toronto Medical Labs & Mount Sinai Hosp. Infect. Dis. Clinician, University Health Network & Mount Sinai Hosp. Assistant
SARS and the Clinical Laboratory Susan M. Poutanen, MD, MPH, FRCPC Microbiologist, Toronto Medical Labs & Mount Sinai Hosp. Infect. Dis. Clinician, University Health Network & Mount Sinai Hosp. Assistant
Disclosures. Objectives. Epidemiology. Enterovirus 68. Enterovirus species 9/24/2015. Enterovirus D68: Lessons Learned from the Frontline
 Enterovirus D68: Lessons Learned from the Frontline Disclosures Jennifer Schuster, MD MSCI Children s Mercy Hospital Pediatric Infectious Diseases September 16, 2015 I have nothing to disclose I do not
Enterovirus D68: Lessons Learned from the Frontline Disclosures Jennifer Schuster, MD MSCI Children s Mercy Hospital Pediatric Infectious Diseases September 16, 2015 I have nothing to disclose I do not
Teaching Case of the Month. Round Pneumonias. Burke A. Cunha, MD Arthur Gran, MD Jaime Simon, MD
 Teaching Case of the Month Round Pneumonias Burke A. Cunha, MD Arthur Gran, MD Jaime Simon, MD Infectious Disease Division Winthrop-University Hospital Mineola, New York and State University of New York
Teaching Case of the Month Round Pneumonias Burke A. Cunha, MD Arthur Gran, MD Jaime Simon, MD Infectious Disease Division Winthrop-University Hospital Mineola, New York and State University of New York
Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma
 Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
2009 H1N1 Influenza Infection: Spectrum Of Chest CT Findings, With Radiologic- Pathologic Correlation
 ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 2009 H1N1 Influenza Infection: Spectrum Of Chest CT Findings, With Radiologic- Pathologic Correlation A Nachiappan, E Weihe, B Akkanti, V
ISPUB.COM The Internet Journal of Radiology Volume 12 Number 2 2009 H1N1 Influenza Infection: Spectrum Of Chest CT Findings, With Radiologic- Pathologic Correlation A Nachiappan, E Weihe, B Akkanti, V
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Respiratory Infections
 Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Respiratory Infections NISHANT PRASAD, MD THE DR. JAMES J. RAHAL, JR. DIVISION OF INFECTIOUS DISEASES NEWYORK-PRESBYTERIAN QUEENS Disclosures Stockholder: Contrafect Corp., Bristol-Myers Squibb Co Research
Severe Acute Respiratory Infection (SARI) Guidelines. Chief Public Health Office Department of Health & Wellness
 Severe Acute Respiratory Infection (SARI) Guidelines Chief Public Health Office Department of Health & Wellness 2013 The following document was prepared by the SARI Working Group. Maureen Anderson, Public
Severe Acute Respiratory Infection (SARI) Guidelines Chief Public Health Office Department of Health & Wellness 2013 The following document was prepared by the SARI Working Group. Maureen Anderson, Public
Microbiology of Atypical Pneumonia. Dr. Mohamed Medhat Ali
 Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
FACT SHEET FOR ADDITIONAL INFORMATION CONTACT
 FACT SHEET FOR ADDITIONAL INFORMATION CONTACT Caroline Calderone Baisley, MPH, RS Michael S. Long, MS Director of Health Director of Environmental Services Tel. 203-622-7836 Tel: 203-622-7838 FREQUENTLY
FACT SHEET FOR ADDITIONAL INFORMATION CONTACT Caroline Calderone Baisley, MPH, RS Michael S. Long, MS Director of Health Director of Environmental Services Tel. 203-622-7836 Tel: 203-622-7838 FREQUENTLY
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 25, 2018 0800 EDT NH-HAN 20180825 Cluster of Legionella pneumophila Pneumonia (Legionnaire
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 25, 2018 0800 EDT NH-HAN 20180825 Cluster of Legionella pneumophila Pneumonia (Legionnaire
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
General History. 林陳 珠 Female 69 years old 住院期間 : ~ Chief Complaint : sudden loss of conscious 5 minutes in the morning.
 General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
SARS Outbreaks in Ontario, Hong Kong and Singapore
 SARS Outbreaks in Ontario, Hong Kong and Singapore DIMACS Workshop on Facing the Challenge of Infectious Diseases in Africa: The Role of Mathematical Modeling September 25-27, 2006 Gerardo Chowell Mathematical
SARS Outbreaks in Ontario, Hong Kong and Singapore DIMACS Workshop on Facing the Challenge of Infectious Diseases in Africa: The Role of Mathematical Modeling September 25-27, 2006 Gerardo Chowell Mathematical
Transmission of Infectious Disease on Aircraft
 Transmission of Infectious Disease on Aircraft Wing Commander Martin Connor MSc MB ChB MRCPath MFPHM DTM&H RAF Consultant in Microbiology and Communicable Diseases RAF Centre of Aviation Medicine Infectious
Transmission of Infectious Disease on Aircraft Wing Commander Martin Connor MSc MB ChB MRCPath MFPHM DTM&H RAF Consultant in Microbiology and Communicable Diseases RAF Centre of Aviation Medicine Infectious
Thin-Section CT Findings in 32 Immunocompromised Patients with Cytomegalovirus Pneumonia Who Do Not Have AIDS
 Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Tomás Franquet 1,2 Kyung S. Lee 3 Nestor L. Müller 1 Received January 27, 2003; accepted after revision April 21, 2003. 1 Department of Radiology, Vancouver Hospital and Health Sciences Center and University
Making the Right Call With. Pneumonia. Community-acquired pneumonia (CAP) is a. Community-Acquired. What exactly is CAP?
 Making the Right Call With Community-Acquired Pneumonia In this article: By Thomas J. Marrie, MD The case of Allyson Allyson, 32, presented to the emergency department with a 48-hour history of anorexia,
Making the Right Call With Community-Acquired Pneumonia In this article: By Thomas J. Marrie, MD The case of Allyson Allyson, 32, presented to the emergency department with a 48-hour history of anorexia,
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Infectivity of Severe Acute Respiratory Syndrome during Its Incubation Period
 BIOMEDICAL AND ENVIRONMENTAL SCIENCES 22, 502 510 (2009) www.besjournal.com Infectivity of Severe Acute Respiratory Syndrome during Its Incubation Period GUANG ZENG *, SHU YUN XIE #, QIN LI, AND JIAN MING
BIOMEDICAL AND ENVIRONMENTAL SCIENCES 22, 502 510 (2009) www.besjournal.com Infectivity of Severe Acute Respiratory Syndrome during Its Incubation Period GUANG ZENG *, SHU YUN XIE #, QIN LI, AND JIAN MING
Description and clinical treatment of an early outbreak of severe acute respiratory syndrome (SARS) in Guangzhou, PR China
 Journal of Medical Microbiology (2003), 52, 715 720 DOI 10.1099/jmm.0.05320-0 Description and clinical treatment of an early outbreak of severe acute respiratory syndrome (SARS) in Guangzhou, PR China
Journal of Medical Microbiology (2003), 52, 715 720 DOI 10.1099/jmm.0.05320-0 Description and clinical treatment of an early outbreak of severe acute respiratory syndrome (SARS) in Guangzhou, PR China
- Mycoplasma pneumoniae (MP): important respiratory pathogen in children that cause many upper and lower respiratory tract diseases, including
 KHOA DICH VU HO HAP - Mycoplasma pneumoniae (MP): important respiratory pathogen in children that cause many upper and lower respiratory tract diseases, including wheezing, coryza, bronchopneumonia. -
KHOA DICH VU HO HAP - Mycoplasma pneumoniae (MP): important respiratory pathogen in children that cause many upper and lower respiratory tract diseases, including wheezing, coryza, bronchopneumonia. -
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Human Infection with Novel Influenza A Virus Case Report Form
 Human Infection with Novel Influenza A Virus Case Report Form Form Approved OMB No. 0920-0004 Exp. Date 6/30/2013 Reporter Information State: Date reported to state/local health department: / / (MM/DD/YYYY)
Human Infection with Novel Influenza A Virus Case Report Form Form Approved OMB No. 0920-0004 Exp. Date 6/30/2013 Reporter Information State: Date reported to state/local health department: / / (MM/DD/YYYY)
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center
 Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
Charles Krasner, M.D. University of NV, Reno School of Medicine Sierra NV Veterans Affairs Medical Center Kathy Peters is a 63 y.o. patient that presents to your urgent care office today with a history
KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA
 KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA Methodology: Expert opinion Issue Date: 8-97 Champion: Pulmonary Medicine Most Recent Update: 6-08, 7-10, 7-12 Key Stakeholders: Pulmonary Medicine,
KAISER PERMANENTE OHIO COMMUNITY ACQUIRED PNEUMONIA Methodology: Expert opinion Issue Date: 8-97 Champion: Pulmonary Medicine Most Recent Update: 6-08, 7-10, 7-12 Key Stakeholders: Pulmonary Medicine,
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
TB In Detroit 2011* Early TB: Smudge Sign. Who is at risk for exposure to or infection with TB? Who is at risk for TB after exposure or infection?
 Those oral antibiotics are just not working! Inpatient Standards of Care & Discharge Planning S/He s in the Hospital: Now What Do I Do? Dana G. Kissner, MD TB Intensive Workshop, Lansing, MI 2012 Objectives:
Those oral antibiotics are just not working! Inpatient Standards of Care & Discharge Planning S/He s in the Hospital: Now What Do I Do? Dana G. Kissner, MD TB Intensive Workshop, Lansing, MI 2012 Objectives:
Current and Emerging Legionella Diagnostics
 Current and Emerging Legionella Diagnostics Nicole Wolter Centre for Respiratory Diseases and Meningitis (CRDM) National Institute for Communicable Diseases nicolew@nicd.ac.za 7 th FIDSSA Conference, Cape
Current and Emerging Legionella Diagnostics Nicole Wolter Centre for Respiratory Diseases and Meningitis (CRDM) National Institute for Communicable Diseases nicolew@nicd.ac.za 7 th FIDSSA Conference, Cape
Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation
 Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Influenza-Associated Pediatric Mortality rev Jan 2018
 rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Viruses, bacteria, fungus, parasites (in rare cases) or other organisms can cause pneumonia.
 1 Pneumonia Pneumonia is an infection which inflames the air sacs either in one or both of the lungs. The air sacs are generally filled with fluid or pus, causing cough along with phlegm or pus, fever,
1 Pneumonia Pneumonia is an infection which inflames the air sacs either in one or both of the lungs. The air sacs are generally filled with fluid or pus, causing cough along with phlegm or pus, fever,
