TRIAGE OF THE DYSPNOEIC CAT : IS YOUR PRACTICE PREPARED?
|
|
|
- Marjorie Ball
- 6 years ago
- Views:
Transcription
1 The Feline Centre Langford and TM working together for the benefit of cats TRIAGE OF THE DYSPNOEIC CAT : Angie Hibbert BVSc CertSAM DipECVIM-CA MRCVS European Veterinary Specialist in Internal Medicine and RCVS Recognised Specialist in Feline Medicine. The arrival of an unstable, dyspnoeic cat is a common emergency in general practice and initial management and stabilisation are critical in patient survival. Here, Angie Hibbert outlines triage of these patients, facilitating a coordinated approach from the whole practice team. Dyspnoea is a relatively common presentation in feline patients. The severity of disease is often particularly advanced at the time of emergency presentation, due to the cat s inherent nature of hiding early signs of illness, in part due to their lifestyles. The patients are typically fragile, therefore careful handling and emergency stabilisation are essential. It is often necessary to delay more extensive diagnostic tests such as radiography or echocardiography, until the patient has been stabilised. Correct management of the dyspnoeic cat is essential since excessive stress or interventions before appropriate stabilisation may precipitate a terminal respiratory crisis. Dyspnoea: difficulty in breathing; often manifests in cats as open-mouth breathing. Tachypnoea: increased rate of breathing. Hyperpnoea: increased depth of breathing, with or without an increase in the rate of breathing. Orthopnoea: adoption of a standing or sternal position to aid respiration. Fig. 1: A dyspnoeic cat receiving flow-by oxygen via facemask. may cause tachypnoea and open-mouth breathing such as pain, fear, anaemia, hyperthyroidism, metabolic acidosis, abdominal distension or neurological disease have to be considered. In the case of primary respiratory disease, it can be be helpful to think about possible causes by location of the affected region of the respiratory tract, dividing it into the upper respiratory tract (nares through to the trachea), lower respiratory tract (bronchial tree), pulmonary parenchyma, pleural space and mediastinum, and thoracic wall (including the ribs, intercostal muscles and diaphragm). Be prepared! In order to deal with any type of emergency presentation, it helps if all members of the veterinary team are familiar with the steps that will need to be taken in the emergency situation and what tasks they will perform. Dyspnoea can be caused by many different conditions and primarily relates to disease originating within the respiratory system, but other processes that As soon as the impending arrival of a cat with breathing difficulties has been logged, equipment should be assembled. 1
2 An open area is ideally used for assessment and stabilisation, preferably with access to oxygen and a crash kit, so that the nurses and vets are in a position to perform cardiopulmonary resuscitation if necessary. Essential items for the crash kit that are important for dealing with respiratory emergencies include a laryngoscope suitable for feline patients (with appropriate blades and functioning light bulb), range of endo-tracheal tubes, suction device (to clear airway secretions), urinary catheter (to connect to oxygen tubing if intubation using an ET tube cannot be achieved quickly), T-piece or an ambu-bag, local anaesthetic spray (e.g. Intubeaze ), tracheostomy kit, drugs (including a bronchodilator e.g. terbutaline or salbutamol), short-acting corticosteroid (e.g. dexamethasone sodium phosphate, hydrocortisone) and furosemide, thoracocentesis kit and a thoracic drain. Monitoring equipment should be easily accessible, ideally this would include an ECG, non-invasive blood pressure monitor, pulse oximetry and capnography. However it is important to remember that much can still be achieved with careful monitoring using clinical observations alone. For all cases, regardless of the cause of dyspnoea, tachypnoea or hyperpnoea, the first steps in an emergency are: 1. Immediately begin supplemental oxygen. 2. Minimise oxygen demands through gentle handling and perform initial cardiorespiratory assessment (if the cat is fractious a hands-off approach is necessary). 3. Prepare equipment for placement of an intravenous catheter; this will be necessary for drug administration and in case of deterioration of respiratory function leading to a requirement for intubation for ventilation or resuscitation. Suggested Technique Equipment and set up Advantages Disadvantages flow rate Flow-by ± Connect breathing system 2-3 litres/min. Quick to set up. Poorly tolerated by some cats. facemask or tubing to oxygen cylinder. Suitable for immediate Short-term unless patient is Attach clear facemask and supplementation unconscious or recumbent as hold over nose or in during triage. restraint is required. proximity to face; if mask is Equipment readily Wastes oxygen. poorly tolerated try with available. Risk of carbon dioxide tubing only. accumulation if tight-fitting mask applied. Oxygen Specially designed chambers 3-10 litres/min Allows hands-off approach Delay in reaching tent/cage (e.g. Kruuse) and cage doors depending on without restraint, minimising inspired oxygen are available. Alternatively cage size. stress. concentrations. cover front of a cage with Suitable for conscious Very difficult to maintain clear plastic and run oxygen dyspnoeic patients on oxygen levels if patient through front. Second-hand immediate arrival. requires intervention and paediatric incubators hands-on monitoring. work well. High flow rates required. Risk of Hyperthermia; monitor for overheating. Oxygen Cover the bottom 80% of litres/min. Allows hands-off approach May not be tolerated by hood the front of an Elizabethan without restraint, some patients. collar with cling film; place minimising stress. Risk of hyperthermia and on cat. Run oxygen tubing Suitable for conscious carbon dioxide acculumulation through the back of the collar. dyspnoeic patients on arrival. reduced by leaving gap at Cheap. the top of the front of the collar. Nasal Instil local anaesthetic ml/kg/min; Highly effective. Insertion can be stressful catheter (e.g. proxymetacaine) into nares; slowly increase If tolerated, can apply two - do not attempt if the cat wait 1-2 minutes. Take a 4-6 Fr flow rate to catheters to maximise struggles. soft feeding tube catheter and desired level over maximum oxygen Often poorly tolerated. measure to level of medial canthus. 3-5 minutes. supplementation. Contraindicated if Apply sterile lubricant and insert A gradual increase coagulopathy, nasal disease or tube via ventral meatus to level is generally well raised intracranial pressure. of medial canthus. Secure in place tolerated, reducing Oxygen should be humidified to hair with tape and spot of risk of inducing if possible to prevent nasal super glue. Nasal catheter can be sneezing and mucosa irritation. connected to a T-piece using a 5ml dislodging the syringe and ET tube connector. catheter. Table 1: Oxygen supplementation methods Reproduced with permission from the BSAVA Manual of Feline Practice. BSAVA. 2
3 Oxygen supplementation Techniques for oxygen supplementation are detailed in Table 1. The most suitable technique for supplementation will be dependent upon several factors including whether the patient is collapsed, whether the cat will tolerate flow-by oxygen sitting on a table or the bottom half of a carrier and the number of personnel available to assist. In many patients triage can be performed on a table or in the bottom half of the cat carrier whilst the cat receives flow-by oxygen (Fig.1). However if the cat struggles with administration of flow-by oxygen or you are alone with the patient, setting up an oxygen hood or cage (Fig.2) are the next safest options. Placement of the cat within an oxygen enriched cage allows time for the cat to settle but remember it will take a significantly longer period of time for oxygen levels to rise, it is therefore The effectiveness of oxygen delivery can be determined by: 1. Clinical evaluation Change in rate and depth of respiration. General demeanour - the patient should look less anxious and be more aware of its surroundings. Heart rate, mucous membrane colour +/- blood pressure. 2. Pulse oximetry Measures oxygen saturation of haemoglobin. Cats may tolerate placement of the probe across the pinna or phalanx; peripheral vasoconstriction (e.g. due to shock), skin pigmentation and administration of oxyglobin interfere with readings. Hypoxia = PaO 2 of <80mmHg. A PaO 2 of 80mmHg approximates to a SpO 2 of 95%. Fig. 2: Oxygen cages typically used in the management of dyspnoea. important to minimise opening of the cage door and start with high flow rates of oxygen. Oxygen supplementation is indicated where the PaO 2 <60 mmhg which approximates to a SpO 2 of 90% and below, but aim to maintain >95%. Arterial blood gas analysis allows measurement of the partial pressure of dissolved oxygen in the plasma (PaO 2 ) but sampling is technically much more demanding in cats and the risk in a dyspnoeic conscious patient is not warranted. Methaemoglobinaemia (e.g. paracetamol toxicity) and carboxyhaemoglobinaemia (e.g. carbon monoxide toxicity) interfere with haemoglobin saturation, however they would not be detected by regular pulse oximetry. If oxygen saturation fails to improve to acceptable levels with non-invasive methods of oxygen supplementation, intubation for manual ventilation may be required. Examination Initially only a limited examination may be possible in the dyspnoeic patient. A significant amount of information can be gleaned by: observing the patient s respiratory pattern (see overleaf). assessing the mucous membranes (include capillary refill time, colour and note petechiation etc). assessing peripheral pulses bilaterally, noting quality and deficits. auscultating the heart, noting any murmurs, arrhythmias (especially gallop rhythms) or displacement of the apex beat. auscultating and percussing all lung fields of the thorax in a gentle, systematic manner. At this stage the aim is to simply to look for clues as to whether the patient has signs of primary cardiac, respiratory or metabolic disease (e.g. anaemia) and to assess baseline vital parameters (mucous membrane colour, respiratory rate, heart and pulse rate). (continued) 3
4 Examination (continued) Normal Breathing Patterns Normal rate 12-30bpm for cats. No visible effort should be noticed. Expiration and inspiration usually of similar duration, often with an end expiratory pause. Thoracic movement: Inspiration - The ribs move cranially and dorsally to expand the thorax. At the same time, the diaphragm contracts, which displaces the cranial abdominal organs caudally. This appears as an increase in the size of the cranial abdomen. - Thoracic and abdominal walls move out. Expiration - The ribs move caudoventrally, with passive intercostal muscle recoil, reducing the volume of the thorax. The diaphragm relaxes, moving cranially and the cranial abdomen returns to normal size. - Thoracic and abdominal walls move in. Panting vs. open-mouth breathing due to dyspnoea - Rapid rate, minimal thoracic wall excursion, body position not restricted. Respiratory features to assess: Rate. Presence of any respiratory noise. Stertor - soft, snorting or snoring noise, localises to the oropharynx or nasopharynx. Stridor - harsh high-pitched sound localises to the larynx or trachea. Wheezing - typically due to airflow through narrowed airways. Crackles - heard when an airway reopens after being blocked by fluid. Whether any increased effort is associated with inspiration or expiration. Whether inspiratory or expiratory phase are of similar duration. Co-ordination of movement of the thoracic and abdominal wall. Paradoxical breathing - Describes movement of either the thoracic or abdominal wall in the opposite direction to what is expected. - Inward movement of the abdominal wall during inspiration can be associated with diaphragmatic weakness and pleural space disease. - Decreased outward movement of the thoracic wall during inspiration can occur with intercostal muscle paralysis. A flail chest-segment of the thoracic wall (when present) moves inward during inspiration. Abdominal breathing - Increased abdominal effort on expiration. - Contraction of the abdominal muscles increases intra-abdominal pressure and forces the diaphragm cranially; may be seen with bronchial disease. Signs of extreme dyspnoea and life-threatening respiratory failure include cyanosis, gasping, serous fluid visible at the nares (could suggest fulminant pulmonary oedema), marked distress with open mouth breathing (thrashing in carrier or cage) or severe hypoventilation with only intermittent breaths. Causes of dyspnoea and ABnormal breathing patterns Assessment of respiratory patterns can be helpful in located between the nares and tracheal bifurcation. deciding what area of the respiratory tract is affected in Typically causes increased inspiratory effort a dyspnoeic patient. The animal will make compensations (prolonged duration of inspiratory phase) in the rate and/or depth of breathing to try to maintain with minimally increased rate. appropriate levels of oxygen delivery to the lungs. Two main problems can occur that limit airflow into the alveoli of the lungs; obstruction of the airways or restriction to inflation of the lungs. Airway disease (nose to trachea) Large airway obstruction Causes inspiratory dyspnoea when the problem is Large airway obstruction is often associated with respiratory noise such as stridor or stertor. Obstruction of the lower airways e.g. chronic bronchitis, feline asthma, causes expiratory dyspnoea, which may manifest with abdominal effort and wheezing may be heard over the lower airways. (continued) 4
5 Causes of dyspnoea and abnormal breathing patterns (continued) Other aspects of the patient s history may also help to localise the problem for the veterinarian e.g. presence of a cough (type, onset, duration and whether nature has changed), exercise tolerance and whether there is dysphonia (feature of laryngeal disease). Lung disease (Bronchial tree and pulmonary parenchyma) Dyspnoea associated with lung diseases can be considered by the mechanisms affecting normal ventilation. The disease may be: Primarily obstructive e.g. feline asthma due to bronchospasm and increased luminal secretions. Primarily restrictive e.g. pulmonary fibrosis, pulmonary oedema whereby the pulmonary changes reduce lung compliance, making it more difficult for the patient to inflate the lungs. A combination of obstructive and restrictive mechanism; this occurs most commonly and examples include pulmonary oedema and bronchopneumonia. Pattern of breathing Obstructive lung disease results in relatively prolonged and effortful expiration. Restrictive lung disease results in an increased frequency of respiration with rapid shallow inspirations. With progression animals frequently adopt postural efforts to maximise ventilation (e.g. head and neck extension, sternal position with elbows abducted) and are reluctant to lie in lateral recumbency. Respiratory fatigue may develop quickly. The distinction between obstructive and restrictive lung breathing patterns are much more subtle than patterns associated with upper airway obstructions - the most important thing is to look and make some sort of assessment of how the cat is breathing and decide whether any abnormal respiratory noise is present, often it will not be possible to strictly categorise the respiration into a single pattern. Auscultation Expiratory wheezes may be heard in obstructive lung disease due to asthma or bronchitis. Crackles are more common with restrictive lung disease such as pulmonary oedema or bronchopneumonia. Gallop or heart murmurs - consider cardiac disease and pulmonary oedema. Historical features that may be relevant to consider A history of coughing (cats do not typically cough with cardiac disease). Whether there have been prior episodes of openmouth breathing. Signs of exercise tolerance e.g. panting or openmouth breathing after exertion. Pleural space and mediastinal disease Due to the presence of pleural effusion, pneumothorax or space occupying lesions (e.g. diaphragmatic rupture, mediastinal mass). Auscultation using a grid pattern can help to detect and localise decreased or absent lung sounds in the presence of a pleural effusion or pneumothorax. Cardiac sounds may be muffled by the presence of pleural effusion. Remember to check a cranial rib spring - decreased compliance can occur with mediastinal masses, and pleural effusions. Breathing pattern Typically consistent with a restrictive pattern. Increased rate with rapid shallow inspiration. Exaggerated abdominal motion may be seen during inspiration. Some cats with pleural effusions will have paradoxical breathing, with the abdominal wall sucked in on inspiration. In severe pneumothorax the intercostal muscles may be seen to be sucked inwards as the ribs forcibly expand, due to the presence of an intra-thoracic vacuum. Diaphragmatic weakness or paralysis Causes include phrenic nerve injury or degeneration and generalised myopathies (e.g. botulism). If only the phrenic nerve and diaphragm are affected, compensation will occur by increasing the respiratory rate and inspiratory excursion of the thoracic wall. May see paradoxical abdominal wall movement (inwards during inspiration). Thoracic wall disease Traumatic (e.g. rib fractures) or non-traumatic (e.g. neuropathy, myopathy or motor unit disorder) causes affect intercostal muscle function and therefore rib movement. Reduced thoracic wall movement or paradoxical movement (thoracic wall moving in during inspiration) +/- tachypnoea. 5
6 Additional stabilisation TECHNIQUES/TREATMENTs for dyspnoeic patients As stated earlier, oxygen supplementation, cage rest and minimising stressful handling are important until the dyspnoeic patient is stable enough to undergo further diagnostic investigations. In many situations empirical therapy may be necessary on the basis of the patient s history, presenting signs and examination findings alone. The following details how some of the more common causes of dyspnoea may be managed empirically. Upper airway dyspnoea e.g. due to laryngeal oedema, laryngitis Low-dose sedation may be useful to reduce anxiety and promote more effective ventilation. Butorphanol ( mg/kg i.v. or i.m.) is often effective. Cooling the patient is important if hyperthermia (>40 C) has developed, to try to reduce respiratory work Wetting the coat and applying fans is usually effective. Anti-inflammatory doses of short-acting corticosteroid are indicated if airway swelling is possible e.g. dexamethasone sodium phosphate mg/kg i.v. or i.m or hydrocortisone 2mg/kg i.v. Intubate as necessary for ventilation if dyspnoea becomes severe. Ensure nares are free of discharge and debris. Steam nebulisation can be helpful if discharge is causing obstruction. Pulmonary disease Lower airway disease e.g. feline asthma Administration of a bronchodilator e.g. terbutaline (0.015mg/kg i.v. or i.m) or salbutamol via inhalational chamber is essential. Anti-inflammatory doses of glucocorticoid may also be used. Pulmonary oedema If due to congestive heart failure, furosemide (2mg/kg i.v. i.m or s.c.) is the first line treatment. Repeat at 1mg/kg after minutes if only partial improvement. Consider topical nitroglycerine. Avoid intravenous fluids. Bronchopneumonia Broad spectrum intravenous antibiotics are used based on likely bacterial population. Nebulisation can also be beneficial. Contusions Opioid analgesia. Care with intravenous fluids Pleural space disease Pleural effusion Where pleural effusion is suspected from clinical exam findings in a dyspnoeic cat, thoracocentesis can be performed as both a diagnostic and therapeutic measure (i.e. to confirm and relieve the presence of fluid) without first confirming the presence of fluid using radiography. Ultrasound is especially helpful in this setting. Thoracocentesis is usually tolerated without sedation +/- use of local anaesthesia. Pneumothorax Again, thoracocentesis can be considered as a priority in cases where pneumothorax is suspected. Thoracic drain placement may need to be considered if there is on-going air leakage into the pleural space; small bore catheters are well tolerated e.g. Mila. TM Thoracic wall disease Fractured ribs and subcutaneous emphysema can be extremely painful; use of opioid analgesia is necessary. Appropriate management of associated pain will also improve ventilation. Conclusion The key to managing the dyspnoeic cat is to remain calm, provide immediate supplemental oxygen and minimise handling and interventions until the patient stabilises, as indicated by sustained improvement/normalisation of vital parameters. Once stabilisation has been achieved, further investigation into the underlying disease can be undertaken, employing methods that minimise stress and respiratory compromise where possible. Practice and team preparation for receiving dyspnoeic cats will improve the emergency response and therefore aid successful stabilisation of these challenging patients. References and further reading: Beatty J. & Barrs V. (2010) Pleural effusion in the cat: a practical approach to determining aetiology. Journal of Feline Medicine and Surgery 12, Crowe D. (2008) Oxygen therapy. In: Kirk s Current Veterinary Therapy XIV. Eds. J. D. Bonagura and D. C. Twedt. Elsevier Saunders, St. Louis pp Hibbert A. (2013) Dyspnoea, tachypnoea and hyperpnoea In: BSAVA Manual of Feline Practice. Eds. A. Harvey and S. Tasker BSAVA Publications, Gloucester pp Mawby D. (2005) Dyspnoea and tachypnoea In: Textbook of Veterinary Internal Medicine 6th Edn. Eds. S. Ettinger and M. Feldman Elsevier Saunders, St Louis pp Sigrist N.E., Adamik K. N., Doherr M. G. et al. (2011) Evaluation of respiratory parameters at presentation as clinical indicators of the respiratory localisation in dogs and cats with respiratory distress. Journal of Veterinary Emergency and Critical Care 21,1323. Swift S., Dukes-McEwan J., Fonfara S. et al. (2009) Aetiology and outcome in 90 cats presenting with dyspnoea in a referral population. Journal of Small Animal Practice 50, On occasion, reference may be made to drugs which are not licensed for use in animals. The Editor does not take any responsibility for the safety and efficacy of such products. Any persons using these products do so entirely at their own risk. 6
Don t Panic! Dr. Karau s Guide to Respiratory Emergencies November 4, 2018
 Don t Panic! Dr. Karau s Guide to Respiratory Emergencies November 4, 2018 Objectives Oxygen delivery methods Emergent diagnostic tests Differentiating between upper and lower respiratory disease Respiratory
Don t Panic! Dr. Karau s Guide to Respiratory Emergencies November 4, 2018 Objectives Oxygen delivery methods Emergent diagnostic tests Differentiating between upper and lower respiratory disease Respiratory
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Acute Respiratory Distress: The Blue Patient
 E m e rg e n c y M e d i c i n e R E S P I R A T O R Y Peer Reviewed Stacey Leach, DVM, & Deborah Fine, DVM, MS, Diplomate ACVIM University of Missouri Acute Respiratory Distress: The Blue Patient PROFILE
E m e rg e n c y M e d i c i n e R E S P I R A T O R Y Peer Reviewed Stacey Leach, DVM, & Deborah Fine, DVM, MS, Diplomate ACVIM University of Missouri Acute Respiratory Distress: The Blue Patient PROFILE
Difficulty Breathing and Respiratory Distress Basics
 Difficulty Breathing and Respiratory Distress Basics OVERVIEW Difficulty breathing (known as dyspnea ) a subjective term that in human medicine means an uncomfortable sensation in breathing or a sensation
Difficulty Breathing and Respiratory Distress Basics OVERVIEW Difficulty breathing (known as dyspnea ) a subjective term that in human medicine means an uncomfortable sensation in breathing or a sensation
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
Auscultation of the lung
 Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
3/10/15. Summary. Anatomy Larynx. Anatomy Trachea
 Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Foundation in Critical Care Nursing. Airway / Respiratory / Workbook
 Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Nursing the critical care patient part 1: triage
 Nursing the critical care patient part 1: triage EJCAP 26(3) Autumn 2016 P 51 Commissioned paper* Nursing the critical care patient part 1: triage Katherine Howie 1 SUMMARY Good nursing of the emergency
Nursing the critical care patient part 1: triage EJCAP 26(3) Autumn 2016 P 51 Commissioned paper* Nursing the critical care patient part 1: triage Katherine Howie 1 SUMMARY Good nursing of the emergency
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics
 Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics OVERVIEW Partial upper airway obstruction in short-nosed, flat-faced (brachycephalic) breeds of dogs and cats caused
Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics OVERVIEW Partial upper airway obstruction in short-nosed, flat-faced (brachycephalic) breeds of dogs and cats caused
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Bronchospasm & SOB. Kim Kilmurray Senior Clinical Teaching Fellow
 Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
Bronchospasm & SOB Kim Kilmurray Senior Clinical Teaching Fellow LEARNING OBJECTIVES Perform a comprehensive respiratory examination & link clinical signs to underlying pathology Identify the spectrum
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
d) Always ensure patient comfort. Be considerate and warm the diaphragm of your stethoscope with your hand before auscultation.
 Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
THE RESPIRATORY SYSTEM. Pages and
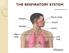 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Chapter 10 Respiration
 1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
BIOE221. Session 5. Examination of Thorax- Respiratory system. Bioscience Department. Endeavour College of Natural Health endeavour.edu.
 BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
Anaesthetic considerations for laparoscopic surgery in canines
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Specialist Referral Service Willows Information Sheets. Laryngeal paralysis
 Specialist Referral Service Willows Information Sheets Laryngeal paralysis Laryngeal paralysis tends to affect middle aged and older animals, especially large breed dogs such as Labrador Retrievers, Golden
Specialist Referral Service Willows Information Sheets Laryngeal paralysis Laryngeal paralysis tends to affect middle aged and older animals, especially large breed dogs such as Labrador Retrievers, Golden
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
NEO 111 Melanie Jorgenson, RN, BSN
 NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
The Respiratory System
 13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
Specialist Referral Service Willows Information Sheets. Brachycephalic Obstructive Airway Syndrome (BOAS)
 Specialist Referral Service Willows Information Sheets Brachycephalic Obstructive Airway Syndrome (BOAS) Brachycephalic breeds include those breeds of dog and cat that have an obvious, characteristic short
Specialist Referral Service Willows Information Sheets Brachycephalic Obstructive Airway Syndrome (BOAS) Brachycephalic breeds include those breeds of dog and cat that have an obvious, characteristic short
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Chapter 39 Oxygenation. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
CAE Healthcare Human Patient Simulator (HPS)
 CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
Chapter 16. The Respiratory System. Mosby items and derived items 2010, 2006, 2002, 1997, 1992 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Northwest Community EMS System Continuing Education Class Credit Questions Respiratory Assessment January 2012
 Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
NHS Training for Physiotherapy Support Workers. Workbook 14 The respiratory system
 NHS Training for Physiotherapy Support Workers Workbook 14 The respiratory system Contents Workbook 14 The respiratory system 1 14.1 Aim 3 14.2 Learning outcomes 3 14.3 The respiratory system 4 14.4 Breathing
NHS Training for Physiotherapy Support Workers Workbook 14 The respiratory system Contents Workbook 14 The respiratory system 1 14.1 Aim 3 14.2 Learning outcomes 3 14.3 The respiratory system 4 14.4 Breathing
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood
 1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
The Respiratory System
 The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
Chapter 13. The Respiratory System.
 Chapter 13 The Respiratory System https://www.youtube.com/watch?v=hc1ytxc_84a https://www.youtube.com/watch?v=9fxm85fy4sq http://ed.ted.com/lessons/what-do-the-lungs-do-emma-bryce Primary Function of Breathing
Chapter 13 The Respiratory System https://www.youtube.com/watch?v=hc1ytxc_84a https://www.youtube.com/watch?v=9fxm85fy4sq http://ed.ted.com/lessons/what-do-the-lungs-do-emma-bryce Primary Function of Breathing
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Chapter 10 Lecture Outline
 Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning
 CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
MANAGEMENT OF THORACIC TRAUMA. Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA
 MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Anaphylaxis/Latex Allergy
 Children s Acute Transport Service CATS Clinical Guideline Anaphylaxis/Latex Allergy Document Control Information Author D Lutman Author Position Consultant Document Owner E Polke Document Owner Position
Children s Acute Transport Service CATS Clinical Guideline Anaphylaxis/Latex Allergy Document Control Information Author D Lutman Author Position Consultant Document Owner E Polke Document Owner Position
LESSON ASSIGNMENT. Physical Assessment of the Respiratory System. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
Airway management. Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department
 Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
Airway management Dr. Dóra Ujvárosy Medical Unversity of Debrecen Emergency Department Airway management Airway management is the medical process of ensuring there is an open pathway between a patient
MEDICAL EMERGENCIES (PART 1) IDENTIFYING AT RISK PATIENTS AND IDENTIFYING THE CONTENTS OF THE EMERGENCY DRUG KIT
 MEDICAL EMERGENCIES (PART 1) IDENTIFYING AT RISK PATIENTS AND IDENTIFYING THE CONTENTS OF THE EMERGENCY DRUG KIT Aims To explain the categories of patients that may be considered as being at risk during
MEDICAL EMERGENCIES (PART 1) IDENTIFYING AT RISK PATIENTS AND IDENTIFYING THE CONTENTS OF THE EMERGENCY DRUG KIT Aims To explain the categories of patients that may be considered as being at risk during
VAO BASIC SUPPORT CLINICAL APPROACH TO THE PATIENT HANDOUT
 CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia A major cause of perinatal and neonatal
The Blue Baby. Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin
 The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
The Blue Baby Network Stabilisation of the Term Infant Study Day 15 th March 2017 Joanna Behrsin Session Structure Definitions and assessment of cyanosis Causes of blue baby Structured approach to assessing
Cardiorespiratory Physiotherapy Tutoring Services 2017
 VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
RESPIRATORY SYSTEM. A. Upper respiratory tract (Fig. 23.1) Use the half-head models.
 RESPIRATORY SYSTEM I. OVERVIEW OF THE RESPIRATORY SYSTEM AND THORAX A. Upper respiratory tract (Fig. 23.1) Use the half-head models. Nasal cavity Pharynx (fare-rinks) B. Lower respiratory tract (Fig. 23.1)
RESPIRATORY SYSTEM I. OVERVIEW OF THE RESPIRATORY SYSTEM AND THORAX A. Upper respiratory tract (Fig. 23.1) Use the half-head models. Nasal cavity Pharynx (fare-rinks) B. Lower respiratory tract (Fig. 23.1)
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
