Regional and Topical Anaesthesia for Endotracheal Intubation
|
|
|
- Elijah Thomas
- 6 years ago
- Views:
Transcription
1 REFERENCES 1. V. Patil, G L. Barker, R J. Harwood and N M. Woodall. Training course in local anaesthesia of the airway and fibreoptic intubation using course delegates as subjects. BJA (4): Fu S. Xue, et al. Spray-As-You-Go Airway Topical Anesthesia in Patients with a Difficult Airway: A Randomized, Double-Blind Comparison of 2% and 4% Lidocaine. Anesth Analg 2009; 108: Latorre, F; Otter, W; Kleemann, P.P; Dick, W.; Jage, J. Cocaine or phenylephrine/lignocaine for nasal fibreoptic intubation? EJA Nov 1996 (13) 6 p Chung D C, Mainland P, Kong A. Anesthesia of the airway by aspiration of lidocaine. Can J Anesth 1999 / 46: 3 / pp Graham DR, Hay JG, Clague J, Nisar M, Earis JE. Comparison of three different methods used to achieve local anesthesia for fiberoptic bronchoscopy. Chest 1992; 102: Webb AR, Fernando SSD, Dalton HR, Arrowsmith JE, Woodhead MA, Cummin AR. Local anaesthesia for fibreoptic bronchoscopy: transcricoid injection or the "spray as you go" technique? Thorax 1990; 45: QY. Yang, FS. Xue, X Liao. Topical anaesthesia of the airway using Trachlight TM and MADgic atomizer in patients with predicted difficult tracheal intubation. BJA 2007; 99(6): Williams KA, Barker GL, Harwood RJ, Woodall NM. Combined nebulization and spray-as-you-go topical local anaesthesia of the airway. BJA 2005; 95(4): Ban C. H. Tsui, Cunningham K. Fiberoptic Endotracheal Intubation After Topicalization with In-Circuit Nebulized Lidocaine in a Child with a Difficult Airway. Anesth Analg 2004; 98 (1286 8). 10. Netter F: Atlas of Human Anatomy. Ciba-Geigy Corporation, Brookman CA, Teh HP, Morrison LM: Anticholinergics improve fibreoptic intubating conditions during general anaesthesia. Can J Anaesth 1997; 44: Parkes SB, Butler CS, Muller R: Plasma lignocaine concentration following nebulization for awake intubation. Anaesth Intensive Care 1997; 25: Curran J, Hamilton C, Taylor T: Topical analgesia before tracheal intubation. Anaesthesia 1975; 30: Kundra P, Kutralam S, Ravishankar M: Local anaesthesia for awake fibreoptic nasotracheal intubation. Acta Anaesthesiol Scand 2000; 44: June 2009 Regional and Topical Anaesthesia for Endotracheal Intubation VR Nurbadh Commentator: S Ramsander Moderator: M Soni Department of Anaesthetics Page 24 of 24
2 CONTENTS INTRODUCTION...3 ANATOMY...4 AIRWAY REFLEXES...5 Indications...5 Preparation...6 TOPICALIZATION...9 NERVE BLOCKS...12 GLOSSOPHARYNGEAL NERVE...13 SUPERIOR LARYNGEAL NERVE...16 RECURRENT LARYNGEAL NERVE...18 PALATINE & ANTERIOR ETHMOID NERVES...21 IDEAL TECHNIQUE?...22 CONCLUSION...23 REFERENCES...24 using course delegates as subjects. British Journal of Anaesthesia 89 (4): 586±93 (2002) Patil et al nostril topicalization with 2.5 ml of 5% lidocaine solution containing 0.5% phenylephrine, then spray as you go technique with 4% lignocaine to a maximum dose of topical lidocaine limited to 9 mg kg. Despite their exclusion of anitsialogogiues and anxiolytics, they found this technique acceptable Ban C. H. Tsui, Cunningham K. Fiberoptic Endotracheal Intubation After Topicalization with In-Circuit Nebulized Lidocaine in a Child with a Difficult Airway. Anesth Analg 2004; 98 (1286 8) This case report describes the successful fiberoptic intubation of an uncooperative child with a difficult airway administering 4% end-tidal sevoflurane and simultaneously delivering 4% nebulized lignocaine via a small-volume nebulizer that was connected to the inspiratory limb of the circle system via a T-piece adapter. The implication being, that an in-circuit nebulization system to deliver topical lignocaine may facilitate fiberopticassisted intubation in anaesthetized, spontaneously breathing children with compromised airways. CONCLUSION It is clear that no consensus exists and that further studies will be required. The "ideal" anaesthetic method should be the one that is simple, effective, safe and works best in the anaesthesiologist's "educated hands within the available resources. It may even be a combination of these techniques provided that it is performed with a careful preparation, patience, gentleness, and above all, a close communication with the patient. Page 2 of 24 Page 23 of 24
3 IDEAL TECHNIQUE? Graham DR, Hay JG, Clague J, Nisar M, Earis JE. Comparison of three different methods used to achieve local anesthesia for fiberoptic bronchoscopy. Chest 1992; 102: Graham et al compared transtracheal, spray as you go, and nebulization, and concluded that transtracheal was superior. INTRODUCTION William MacEwen 1880 Webb AR, Fernando SSD, Dalton HR, Arrowsmith JE, Woodhead MA, Cummin AR. Local anaesthesia for fibreoptic bronchoscopy: transcricoid injection or the "spray as you go" technique? Thorax 1990; 45: Patients receiving transcricoid lignocaine coughed less than the patients receiving lignocaine through the bronchoscope despite receiving a lower total dose of lignocaine. Cricothyroid puncture was not associated with any complications and was not unpleasant for the patients. QY Yang, F. S. Xue, X. Liao. Topical anaesthesia of the airway using TrachlightTM and MADgic atomizer in patients with predicted difficult tracheal intubation British Journal of Anaesthesia (6): Yang et al demonstrated favourable intubating conditions using a light wand with they incorporated an atomizer. Williams KA, Barker GL, Harwood RJ, Woodall NM. Combined nebulization and spray-as-you-go topical local anaesthesia of the airway. British Journal of Anaesthesia (4): In his series of 25 subjects, Williams et al concluded that a combined method of nebulization and direct application of lignocaine to the airway was acceptable to this small group of unsedated subjects. It produced good conditions for fibreoptic intubation. V Patil, G. L. Barker, R. J. Harwood and N. M. Woodall. Training course in local anaesthesia of the airway and fibreoptic intubation Page 22 of 24 "On its introduction there was evince considerable excitement, accompanied by a spasmodic fit of coughing which lasted for about a couple of minutes. In order to gain the patient's confidence, he was asked to hold with his own hand the portion of the tube which projected from his mouth, and told that he was at liberty to withdraw it if he felt it necessary half an hour afterward he withdrew the tube..." In recent years, there have been many advances in airway management. One major decision must be made with every procedure: will the patient be intubated while under general anaesthesia, or does the patient need to be awake during intubation? Intubation under general anaesthesia (even with inhalational induction and spontaneous ventilation) carries the inherent risk of losing control of the difficult airway. For this reason, many anaesthesiologists, on recognition of a difficult airway, elect to perform an awake intubation using either fiber optic laryngobronchoscopy or awake direct laryngoscopy. Direct laryngoscopy in an awake, unprepared patient can be extremely challenging. Excessive salivation and gag and cough reflexes can make intubation difficult, if not impossible, under awake conditions. In addition, the stress and discomfort may lead to undesirable elevations in the patient s sympathetic and parasympathetic outflow. Several highly effective topical and regional anaesthesia techniques have been developed to subdue these reflexes and facilitate intubation. Each of these techniques has the common goal of reducing sensation over the specific regions that will be encountered by the fiber optic bronchoscope and endotracheal tube. Page 3 of 24
4 ANATOMY Three major neural pathways supply sensation to airway structures: 3.5 Structural injuries - surrounding structures, including the posterior tracheal wall and vocal cords can be damaged, especially if the needle is not stabilized during injection of the local anaesthetic, or not removed immediately. 3.6 Intravascular injection. Aspiration should be performed prior to the injection of local anaesthetic. PALATINE & ANTERIOR ETHMOID NERVES 1. Anatomy and innervation: The greater and lesser palatine nerves innervate the nasal turbinates and the posterior two thirds of the nasal septum. The anterior ethmoid nerve innervates the remainder of the nasal passage. Terminal branches of the ophthalmic and maxillary divisions of the trigeminal nerve supply the nasal cavity and turbinates. The oropharynx and posterior third of the tongue are supplied by the glossopharyngeal nerve. 2. Technique: The sensory input of these nerves can be blocked by topical application of the local anaesthetic into nasal passages. This can be accomplished noninvasively by taking a cotton-tipped applicator soaked in local anaesthetic and passing it along the upper border of the middle turbinate to the posterior wall of the nasopharnx, where it is left for 5 10 minutes. If this proves inadequate, however, regional blockade of the palatine nerves can be accomplished by blocking the pterygopalatine ganglion from which both nerves arise. This is technically difficult, and not usually necessary as topicalization of this region is all that is needed. Page 4 of 24 Page 21 of 24
5 Branches of the vagus nerve innervate the epiglottis and more distal airway structures: - superior laryngeal nerve The internal branch of the superior laryngeal nerve provides sensory innervation to the base of the tongue, posterior surface of the epiglottis, aryepiglottic fold, and the arytenoids. The external branch of the SLN supplies the motor innervation to the cricothyroid muscle. - recurrent laryngeal nerve provides sensory innervation of the vocal folds and trachea and motor function of all intrinsic laryngeal muscles except the cricothyroid supplied by the external branch of the superior laryngeal nerve. 3. Specific technique related complications: 3.1 Direct blockade of the recurrent laryngeal nerve is contraindicated. This is because it may result in the upper airway obstruction, since the recurrent laryngeal nerve provides motor innervation for all the muscles of the larynx except the cricothyroid. In contrast, unilateral blockade typically manifests only as transient hoarseness. 3.2 This technique is possibly contraindicated in patients with high risk of gastric aspiration, but is believed by most authorities to actually decrease the risk, by decreasing risk of coughing and gag reflex during intubation. 3.3 This block usually rapidly results in a fit of coughing, which should be considered in patients whom coughing is undesirable or contraindicated. This block is contraindicated in patients diagnosed with an unstable neck, because it induces coughing. During performance of the block, the patient should not talk, swallow, or cough, if possible. 3.4 Vascular injury the needle does not need to be far off the midline of the cricothyroid membrane to encounter significant arterial and venous vessels. Pressure should be held over the injection site with an alcohol wipe after injection to prevent haematoma formation and subcutaneous emphysema Page 20 of 24 AIRWAY REFLEXES The aforementioned nerves participate in several brainstem-mediated reflex arcs: 1. Gag reflex triggered by mechanical and chemical stimulation of areas innervated by the glosso-pharyngeal nerve, the efferent motor arc being provided by the vagus nerve and its branches to the pharynx and larynx. 2. Glottic closure reflex elicited by selective stimulation of the superior laryngeal nerve, and efferent arc is the recurrent laryngeal nerve. Exaggeration of this reflex is called laryngospasm. 3. Cough the cough receptors located in the larynx and trachea receive afferent and efferent fibers from the vagus nerve. Indications Indicated primarily to obtund reflexes in patients with airway compromise, trauma to the upper airway, or cervical instability, where procedures that involve manipulation of the airway are necessary, these include; awake laryngoscopy, nasal intubation, and fiberoptic intubation. Page 5 of 24
6 Preparation 1. Explanation: The adult patient is prepared by giving an explanation of the need for awake intubation, nasal endoscopy or other airway procedure, and will be more cooperative once they understand the rationale for any uncomfortable procedures that must be performed. I refer to you to the following table which appears in the BJA in an article by Patil et al Entitled Detailed subjective description of endoscopy and intubation, which you may modify during your counselling depending upon your local practice: There is obviously a degree of apprehension associated with anticipation of an awake intubation. Before consenting for an awake intubation you will need to understand what is involved, the risks of the procedure and exactly how you can expect to feel during and afterwards. This method of airway anaesthesia has been used repeatedly on patients, by doctors who are competent at performing this technique. Method We observe a 6 hour fast before the procedure, but despite this it is advisable to ensure an empty bladder as the whole procedure may take an hour. The procedure takes place in an operating theatre with full resuscitation facilities available. You will be settled in the supine position with head elevated on a fairly comfortable operating table. Monitoring will be applied ± NIBP, ECG and pulse oximetry. Oxygen will be administered by nasal cannulae. After a period of stabilization to give you time to settle down, a small cannula will be inserted into the back of your hand or the antecubital fossa, whichever you prefer. This is followed by the i.v. administration of glycopyrrolate 200±400 mg. Over the following 10 min the glycopyrrolate will produce a dry mouth. Sedation may be used. Early preparation includes the application of a vasoconstrictor to the nose, this is a little uncomfortable and sometimes makes the eyes water. Nebulized, sprayed, or topically applied 2% lignocaine is used to begin anaesthetising the upper airway. Topical application of local anaesthetic spray to the airway tastes unpleasant, as lignocaine has a bitter taste and produces coughing or gagging. If the endoscope is advanced too early, before satisfactory anaesthesia has been achieved, this can cause swallowing coughing, gagging or retching. When the larynx ceases to react to further increments of local anaesthetic the tracheal tube is passed through the nose. A small tube is used, through the largest nostril or through the mouth. As it passes through the nose you may hear some clicking noise though this is uncommon. In general, the procedure is well tolerated. The tracheal tube position is confirmed. Following the procedure you will be aware of a dry mouth which may outlast the procedure and of nasal stuffiness similar to that which occurs in the early stages of a cold. Page 6 of 24 Then a 22- or 20-gauge needle on a 10-mL syringe with 4mL of 4% Lignocaine 4 % is used. Also, 1% or 2% lignocaine, with or without adrenaline is passed perpendicular to the axis of the trachea and pierces the membrane. (Alternatively, a 20-gauge angiocath can be passed.) While the needle is being advanced, the syringe is continuously aspirated. The needle is advanced until air is freely aspirated, signifying that the needle is now in the larynx. Instillation of local anaesthetic at this point invariably results in coughing. Through coughing, the local anaesthetic is dispersed, diffusely blocking the sensory nerve endings of the recurrent laryngeal nerve and superior laryngeal nerve Page 19 of 24
7 RECURRENT LARYNGEAL NERVE 1. Anatomy and innervation: When oropharyngeal sensation returns to normal we recommend a warm cold-cure drink containing aspirin or paracetamol to deal with the nasal discomfort. This usually settles after 12±14 h. Clearly in a procedure of this kind, it is essential that we exercise utmost caution. For this reason we are explicit about the risks. Risks Trauma to the airway from the nose to main bronchi, including bleeding or perforation and abscess formation. Allergic reactions to lignocaine, glycopyrrolate or phenylephrine. Drug toxicity due to lignocaine resulting in convulsions, myocardial depression or cardiac arrest. Aspiration of gastric contents. Infection: localized or systemic, due to hepatitis B, hepatitis C, HIV, TB, CJD and any other contaminating organisms. The recurrent laryngeal nerve provides sensory innervation of the vocal folds and trachea, and motor function of all intrinsic laryngeal muscles except the cricothyroid, supplied by the external branch of the superior laryngeal nerve. Blockade would abolish the gag reflex; prevent coughing and haemodynamic responses to laryngoscopy or bronchoscopy. With the exception of minor nasopharyngeal trauma, none of these complications has been observed during the preparatory stages. Doses of lignocaine applied to the airway are large (up to 9 mg kg±1). These have been found to be acceptable in patients undergoing bronchoscopy (Efthimiou J, Higenbottam T, Holt D, Cochrane GM. Plasma concentrations of lignocaine during breoptic bronchoscopy. Thorax 1982; 37: 68±71). Awake fibreoptic intubation has been reported to be safe in patients at risk of aspiration (Ovassapian A, Krejcie TC, Yelich SJ, Dykes MHM. Awake fibreoptic intubation in patients at high risk of aspiration. Br J Anaesth 1989; 62: 13±16). 2. Technique: Supine, with neck hyperextended. After sterile skin preparation, the overlying skin is anaesthetized by raising a small skin wheal of local anaesthetic. Page 18 of 24 Page 7 of 24
8 2. Antisialogogues: Antisialogogues are invaluable adjuncts that will improve the effectiveness of topically applied local anaesthesia. Antisialogogues and vasoconstrictors for the nasal mucosa (1% phenylephrine spray) should be used before any airway instrumentation, in the absence of contraindications to either. To be most effective, they should be administered minutes prior to application of the local anaesthetic (often in the holding area) They decrease mucosal secretion production, increase the effectiveness of topically applied local anaesthetics by removing the barrier to mucosal contact, decrease drug dilution and are important to the success of these techniques. Glycopyrrolate 0.4 mg given intramuscularly or intravenously helps to diminish secretions. Alternatively, atropine mg may be used intramuscularly or intravenously to similar effect, Intramuscular administration is favored over intravenous administration to avoid undesired side effects such as tachycardia and, less commonly, psychosis (with atropine). 3. Sedation: It is important that the patient undergoing awake tracheal intubation be sedated, comfortable, and experience minimal anxiety. For this purpose, it is best to use short-acting or reversible agents for sedation or agents that do not cause a considerable degree of respiratory depression. Some examples of commonly used medication for awake intubation include midazolam, alfentanil, and fentanyl. Similarly, dexmedetomidine does not cause respiratory depression and is suitable in this setting. It is equally important that the anxiolytic be carefully administered by titration to a desired effect so that a close communication between the anaesthesiologist and the patient can be maintained during the awake tracheal intubation. The cornu of the hyoid bone is palpated transversally with the thumb and the index finger on the side of the neck immediately beneath the angle of the mandible and anterior to the carotid artery. To facilitate its identification, the hyoid bone is displaced toward the side being blocked. One hand displaces the carotid artery laterally and posteriorly. With the other hand, a 22 or 23 gauge - 25 mm needle is "walked off" the cornu (cartilage) of the hyoid bone in an anterior caudad direction, aiming in the direction of the thyroid ligament, until it can be passed through the ligament. At a depth of 1-2 cm, 2 ml of 2% lignocaine with epinephrine is injected (after negative air and blood aspiration) into the space between the thyrohyoid membrane and the pharyngeal mucosa. An additional 1 ml is injected as needle is withdrawn. The block is repeated on the other side. 3. Specific technique related complications: 3.1 Do not to insert the needle into the thyroid cartilage, since injection of local anaesthetic at the level of vocal cords may cause oedema and airway obstruction. 3.2 Haematoma formation from puncture during needle placement for injection, or vascular structure damage. Maintain pressure long enough to prevent haematoma or continued bleeding. 4. Limitation: Glossopharyngeal nerve block is not adequate as a solo technique to facilitate intubation, but in combination with other techniques it is highly effective. Although a balance of comfort and excessive sedation is a challenge, it is critical to ensure ventilation and oxygenation while minimizing the risk of aspirating stomach contents, particularly in patients who present with a full stomach. The risk of aspiration can be minimized by the administration of pharmacological agents, such as ranitidine, and metoclopramide, prior to intubation. Page 8 of 24 Page 17 of 24
9 4. Limitation: Glossopharyngeal nerve block is not adequate as a solo technique to facilitate intubation, but in combination with other techniques it is highly effective. SUPERIOR LARYNGEAL NERVE 1. Anatomy and innervation: The internal branch of the superior laryngeal nerve provides sensory innervation to the base of the tongue, posterior surface of the epiglottis, aryepiglottic fold, and the arytenoids. The external branch of the SLN supplies the motor innervation to the cricothyroid muscle. The recurrent laryngeal nerve provides sensory innervation of the vocal folds and trachea, and motor function of all intrinsic laryngeal muscles except the cricothyroid supplied by the external branch of the superior laryngeal nerve. 2. Technique: Anaesthetist is positioned on the ipsilateral side of the neck. TOPICALIZATION Topicalization of the airway is the spreading of local anaesthetic over a region of mucosa to achieve local uptake and neural blockade of that region. Topicalization is the simplest method for anaesthetizing the airway. Adequate time allocation is needed to achieve optimal conditions. 1. Agents The choice of the local anaesthetic agent largely depends on its availability, clinical efficacy, and safety. Currently, lignocaine and cocaine are probably the most commonly used local anaesthetics for topical anaesthesia. Fu et al concluded that both 2% and 4% lignocaine administered topically by a spray-as-you-go technique can provide clinically acceptable intubating conditions for awake FOI in sedated patients with a difficult airway. As compared with 4% lignocaine, however, 2% lignocaine requires a smaller dosage and results in lower plasma concentrations. Cocaine compares favourably with lignocaine, because of its topical anaesthetic and vasoconstricting properties, making it useful for nasotracheal intubation. However, cocaine should be used with caution because of its addictive potential and possibility for abuse, as well as its inherent toxicity, particularly with higher concentrations. Phenylephrine is available to us in our daily practice, to be used with good effect with lignocaine 2%. 2. Modes of application 2.1 Spray & aspiration Local anaesthetic can be sprayed directly onto the desired mucosa, or may be aspirated. In the aspiration technique, the patient lies supine, traction is applied to the tongue, and the anaesthetic solution is simply dripped on to the tongue without any attempt to direct it at specific anatomical landmarks. Traction on the tongue is a most important maneuver in this technique as it modifies the act of swallowing and prevents the epiglottis from protecting the airway from aspiration. Page 16 of 24 Page 9 of 24
10 2.2 Gel Local anaesthetic gel can be placed on tongue blade and patient "sucks" on this for several minutes. Topically, peak onset is usually within 15 minutes. 2.3 Soaked swab Anaesthetic-soaked cotton can be applied to targeted mucosal surfaces for 5 15 minutes to effect selective blockade of underlying nerves. Vasoconstrictors such as adrenaline (1:200,000) or phenylephrine (0.05%) can be added to the solution to reduce mucosal bleeding. These are soaked in either viscous or aqueous solutions of local anaesthetic and then left for 5 15 minutes on the region of mucosa that requires anaesthesia. The cotton acts as a reservoir for the anaesthetic agent, producing a dense block. This technique is especially effective in the nasal passages. 2.4 Gargle Viscous lignocaine 2-4 ml may also be used as a gargle (swish and swallow) for approximately 30 sec. 2.5 Inhalation Inhalation of aerosolized local anaesthetic is another simple technique to achieve oropharyngeal anaesthesia. Using deep pressure, the styloid process is palpated just posterior to the angle of the jaw along this line, and a short, small-gauge needle is seated against the styloid process. The needle is then withdrawn slightly and directed posteriorly off of the styloid process. As soon as bony contact is lost, 5 7ml of local anaesthetic solution are injected after careful aspiration for blood. 3. Specific technique related complications: Because of the high vascularity of the palatoglossal arch, accidental vascular injection is an ever-present risk. Careful aspiration helps to reduce this risk, but it cannot be avoided entirely. In addition, significant absorption of local anaesthetic can be expected in this region. The addition of adrenaline to the local anaesthetic solution helps to vasoconstrict the blood vessels in the region, reducing absorption as well as assisting in the diagnosis of intravascular injection by heart rate monitoring. To perform this technique, local anaesthetic is added to a standard nebulizer with a mouthpiece or face mask attached. The patient is then asked to inhale the local anaesthetic vapor deeply. After a period of approximately minutes, the patient should have inhaled a sufficient Page 10 of 24 As with any injection into a highly vascular region, this technique may be contraindicated in patients with coagulopathies or anticoagulation. This block has been reported as painful, and may result in a persistent hematoma. Page 15 of 24
11 quantity of local anaesthetic to achieve a reasonably good level of topical anaesthesia throughout the oropharynx and trachea. The palatopharyngeal fold (posterior tonsillar pillar) is identified, and a tongue depressor, held with the non-dominant hand, is introduced into the mouth to displace the tongue medially (contralateral side) creating a gutter between the tongue and the teeth. A 25g spinal needle is inserted into the membrane near the floor of the mouth at the base of the cul-de-sac and advanced slightly ( cm). An aspiration test is performed. If air is aspirated, the needle has passed through the membrane (through and through). If blood is aspirated, the needle is redirected more medially. Then, 2 ml of 1% Lignocaine can be injected into the anterior tonsillar pillar 0.5 cm lateral to the base of the tongue. This most readily blocks the lingual branch. This block has been reported as painful, and may result in a persistent hematoma. To perform the peristyloid approach to the glossopharyngeal block, the patient is placed supine and a line is drawn between the angle of the mandible and the mastoid process. Focused aerosolized local anaesthetic from an atomizer is ideal for nasal intubation. A number of disposable commercially available syringe-powered atomizers are available but are deficient in achieving small particle size unless outfitted with a side-stream air/oxygen flow to enhance dispersion by virtue of the Venturi principle. For these techniques, lignocaine in concentrations of 0.5% 4% has been suggested; however, quicker and denser blockade is achieved by using concentrations in the range of 2 4%. This technique has a proven clinical track record of safety; however, little data are available regarding the blood levels of local anaesthetic that are achieved using these techniques or regarding metabolism of swallowed local anaesthetics. Parkes et al.[14] showed plasma concentrations of mg/l in healthy volunteers after inhalation of 10% lignocaine solution. Because these levels were well below the generally accepted 5 mg/l safe level, it can be inferred that inhaling a 2 4% lignocaine for minutes should be safe in most patients, particularly as a stand-alone technique. The major advantage of this technique lies in its simplicity and lack of discomfort. In addition, very little working knowledge of the anatomy of the region is required for its successful implementation. Although this technique may seem ideal, it does have some drawbacks that limit its usefulness. The main disadvantage is that the density of the anaesthesia achieved throughout the airway is highly variable. Page 14 of 24 Page 11 of 24
12 Many patients still experience an intact cough reflex, which can make intubation technically challenging. The rate of onset of this technique is highly dependent on patient compliance. Many patients who need an awake intubation are incapable or unwilling to take deep breaths. GLOSSOPHARYNGEAL NERVE Also, inhalation of local anaesthetic vapors can lead to central nervous system depression in patients whose mental status may already be depressed owing to other disease processes. It should be emphasized that Topicalization alone may be inadequate for awake tracheal intubation in some patients as the stretch receptors at the root of the tongue which cause the gag reflex are submucosal and are not easily blocked and have to be supplemented by nerve bocks. NERVE BLOCKS The essential nerve blocks include those to: 1. Anatomy and innervation: The glossopharyngeal nerve travels anterior along the lateral surface of the pharynx. Its three branches provide sensory innervation to: the posterior third of the tongue, the vallecula, the anterior surface of the epiglottis via the lingual branch; the walls of the pharynx via the pharyngeal branch; and the tonsils via the tonsillar branch. Blockade of the glossopharyngeal nerve facilitates endotracheal intubation by blocking the gag reflex associated with direct laryngoscopy as well as facilitating passage of a nasotracheal tube through the posterior pharynx. The mouth, oropharynx and base of tongue innervated by branches of glossopharyngeal nerve; The hypopharynx, larynx and trachea innervated by branches of vagus nerve; and The nasal mucosa and nasopharynx innervated by branches of trigeminal nerve. Topicalization not completely effective in obliterating the gag reflex. 2. Technique: Intraoral approach is performed with the anaesthetist standing contralateral to the side to be blocked, and the patient s topicalized mouth wide open. Page 12 of 24 Page 13 of 24
AIRWAY BLOCKS. Preparation: It is recommended, that before proceeding with any of these techniques:
 AIRWAY BLOCKS Of all the regional anesthesia techniques, airway blocks are the most critical and should be mastered by all anesthesia providers. These techniques are employed frequently with the diagnosis
AIRWAY BLOCKS Of all the regional anesthesia techniques, airway blocks are the most critical and should be mastered by all anesthesia providers. These techniques are employed frequently with the diagnosis
Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway
 Original Article Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway Khawaja Kamal Nasir, Faraz Mansoor From Department of Anesthesia, Pakistan Institute of Medical Sciences, Islamabad.
Original Article Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway Khawaja Kamal Nasir, Faraz Mansoor From Department of Anesthesia, Pakistan Institute of Medical Sciences, Islamabad.
Anatomy of the Airway
 Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Regional & Topical Anaesthesia of Upper Airways
 Indian Journal of Anaesthesia 2009; 53 (6):641-648 Special Article Regional & Topical Anaesthesia of Upper Airways Summary Nibedita Pani 1, Shovan Kumar Rath 2 A combination of techniques are required
Indian Journal of Anaesthesia 2009; 53 (6):641-648 Special Article Regional & Topical Anaesthesia of Upper Airways Summary Nibedita Pani 1, Shovan Kumar Rath 2 A combination of techniques are required
Training course in local anaesthesia of the airway and breoptic intubation using course delegates as subjects
 British Journal of Anaesthesia 89 (4): 586±93 (2002) Training course in local anaesthesia of the airway and breoptic intubation using course delegates as subjects V. Patil *, G. L. Barker, R. J. Harwood
British Journal of Anaesthesia 89 (4): 586±93 (2002) Training course in local anaesthesia of the airway and breoptic intubation using course delegates as subjects V. Patil *, G. L. Barker, R. J. Harwood
Williams et al. epilepsy, diabetes, asthma, a history of epistaxis, nasal problems, allergy to drugs used during the procedure (xylometolazone, lidoca
 British Journal of Anaesthesia 95 (4): 549 53 (2005) doi:10.1093/bja/aei202 Advance Access publication August 26, 2005 Combined nebulization and spray-as-you-go topical local anaesthesia of the airway
British Journal of Anaesthesia 95 (4): 549 53 (2005) doi:10.1093/bja/aei202 Advance Access publication August 26, 2005 Combined nebulization and spray-as-you-go topical local anaesthesia of the airway
Nicolette Mosinski MPAS, PA-C
 Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
10 cc syringes, 22 and 22 ga needles, 20 ga angiocatheter. alcohol swab, gauze, and Q-tip or pledgets with bayonette forceps, tongue depressor
 Local Anesthesia of the airway Collect equipment: (Drugs listed with each technique below.) Supplemental oxygen (if needed) Antisialogogue if oral topical planned Optimize position: 1) Nasal anesthesia
Local Anesthesia of the airway Collect equipment: (Drugs listed with each technique below.) Supplemental oxygen (if needed) Antisialogogue if oral topical planned Optimize position: 1) Nasal anesthesia
Structure and Nerve Supply of The Larynx
 Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical sciences Structure and Nerve Supply of The Larynx This presentation was originally prepared by: Dr. Kumar Notes were added by:
Kingdom of Bahrain Arabian Gulf University College of Medicine and Medical sciences Structure and Nerve Supply of The Larynx This presentation was originally prepared by: Dr. Kumar Notes were added by:
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
If you suspect airway problems, get a second opinion before you anaesthetise, not after!
 Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients.
 Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
General Medical Procedure. Emergency Airway Techniques (General Airway Protocol)
 General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
Difficult Airway. Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.)
 Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
The Pharynx. Dr. Nabil Khouri MD. MSc, Ph.D
 The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Local Nerve Block Anesthesia for Peroral Endoscopy
 Local Nerve Block Anesthesia for Peroral Endoscopy Tom R. DeMeester, M.D., David B. Skinner, M.D., Richard H. Evans, M.D., and Donald W. Benson, M.D. ABSTRACT Local glossopharyngeal and superior laryngeal
Local Nerve Block Anesthesia for Peroral Endoscopy Tom R. DeMeester, M.D., David B. Skinner, M.D., Richard H. Evans, M.D., and Donald W. Benson, M.D. ABSTRACT Local glossopharyngeal and superior laryngeal
Airway Ma nagement June 2009
 Airway Management June 2009 INDEX: www.developinganaesthesia.org 3 Recognising the difficult airway 4 Regional anaesthesia of the airway 14 Airway management choices 23 Alternative airway devices 30 Laryngoscopy
Airway Management June 2009 INDEX: www.developinganaesthesia.org 3 Recognising the difficult airway 4 Regional anaesthesia of the airway 14 Airway management choices 23 Alternative airway devices 30 Laryngoscopy
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions. 4 May 2012
 SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
The PHARYNX. Dr. Nabil Khouri MD Ph.D
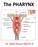 The PHARYNX Dr. Nabil Khouri MD Ph.D PHARYNX Fibromuscular tube lined with mucous membrane extends from base of skull to lower border of cricoid cartilage (C-6). 12-14 cm long At the lower border of cricoid
The PHARYNX Dr. Nabil Khouri MD Ph.D PHARYNX Fibromuscular tube lined with mucous membrane extends from base of skull to lower border of cricoid cartilage (C-6). 12-14 cm long At the lower border of cricoid
LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS. - Our Perspective.
 ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
THE INTERIOR OF THE PHARYNX. By Dr. Muhammad Imran Qureshi
 THE INTERIOR OF THE PHARYNX By Dr. Muhammad Imran Qureshi The Cavity The cavity of the pharynx is divided into: 1. The Nasal part (called Nasopharynx) 2. The Oral part (called the Oropharynx), 3. And the
THE INTERIOR OF THE PHARYNX By Dr. Muhammad Imran Qureshi The Cavity The cavity of the pharynx is divided into: 1. The Nasal part (called Nasopharynx) 2. The Oral part (called the Oropharynx), 3. And the
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Nasotracheal Intubation for Head and Neck Surgery
 Nasotracheal Intubation for Head and Neck Surgery Dr A J Cartwright Introduction History Anatomy Indications for Technique of Complications Contraindications Conclusions History First described in 1902
Nasotracheal Intubation for Head and Neck Surgery Dr A J Cartwright Introduction History Anatomy Indications for Technique of Complications Contraindications Conclusions History First described in 1902
Respiratory System. Functional Anatomy of the Respiratory System
 Respiratory System Overview of the Respiratory System s Job Major Duty Respiration Other important aspects ph control Vocalization Processing incoming air Protection Metabolism (ACE) What structures allow
Respiratory System Overview of the Respiratory System s Job Major Duty Respiration Other important aspects ph control Vocalization Processing incoming air Protection Metabolism (ACE) What structures allow
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Respiratory System. Cambridge University Press Concise Anatomy for Anaesthesia Andreas G. Erdmann Excerpt More information
 Respiratory System 1 The mouth DESCRIPTION The mouth extends from the lips (anterior) to the isthmus of the fauces (posterior). There are two sections: Vestibule slit-like cavity between the cheeks/lips
Respiratory System 1 The mouth DESCRIPTION The mouth extends from the lips (anterior) to the isthmus of the fauces (posterior). There are two sections: Vestibule slit-like cavity between the cheeks/lips
Basic Scope Care and Handling
 Basic Scope Care and Handling Basic principles behind fibre-optic instruments Light and image transfer via coherent(image transmission) and incoherent (light)bundles Fibre coating with lower refractory
Basic Scope Care and Handling Basic principles behind fibre-optic instruments Light and image transfer via coherent(image transmission) and incoherent (light)bundles Fibre coating with lower refractory
How to use the Control-Cric to perform a surgical cricothyrotomy
 TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Anatomy of the Lungs. Dr. Gondo Gozali Department of anatomy
 Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
CHAPTER 22 RESPIRATORY
 pulmonary ventilation move air external respiration exchange gases transportation of gases internal respiration exchange gases CHAPTER 22 RESPIRATORY in / out lungs air - blood blood - cells cell respiration
pulmonary ventilation move air external respiration exchange gases transportation of gases internal respiration exchange gases CHAPTER 22 RESPIRATORY in / out lungs air - blood blood - cells cell respiration
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
NURSE-UP RESPIRATORY SYSTEM
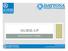 NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
NURSE-UP RESPIRATORY SYSTEM FUNCTIONS OF THE RESPIRATORY SYSTEM Pulmonary Ventilation - Breathing Gas exchanger External Respiration between lungs and bloodstream Internal Respiration between bloodstream
B. Correct! As air travels through the nasal cavities, it is warmed and humidified.
 Human Anatomy - Problem Drill 20: The Respiratory System Question No. 1 of 10 1. Which of the following statements about the portion of the respiratory system labeled in the image below is correct? Question
Human Anatomy - Problem Drill 20: The Respiratory System Question No. 1 of 10 1. Which of the following statements about the portion of the respiratory system labeled in the image below is correct? Question
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair. Krista Madden, MSNA. Westminster College
 Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102-6102 1 The Palate The palate forms the roof of the mouth and the floor of the nasal cavity. It is divided into two
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102-6102 1 The Palate The palate forms the roof of the mouth and the floor of the nasal cavity. It is divided into two
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
student handbook BARS handbook September 2012.indd Front Cover 27/11/12 12:08 PM
 student handbook BARS handbook September 2012.indd Front Cover 27/11/12 12:08 PM All materials regarding the Basic Airway Resuscitation Strategy Course were written and developed by Dr. Richard Morris
student handbook BARS handbook September 2012.indd Front Cover 27/11/12 12:08 PM All materials regarding the Basic Airway Resuscitation Strategy Course were written and developed by Dr. Richard Morris
DIFFICULT AIRWAY MANAGMENT. Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr)
 DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
Fiberoptic Intubation. Paul D. Fulling, MD James T. Roberts, MD
 Fiberoptic Intubation Paul D. Fulling, MD James T. Roberts, MD The notion of indirect laryngoscopy was first noted in the 19th century by a professor of singing in Paris named Garcia. Garcia had used dental
Fiberoptic Intubation Paul D. Fulling, MD James T. Roberts, MD The notion of indirect laryngoscopy was first noted in the 19th century by a professor of singing in Paris named Garcia. Garcia had used dental
Respiratory System. Clinical notes. Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz)
 Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
Respiratory System. Student Learning Objectives:
 Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
Respiratory System Student Learning Objectives: Identify the primary structures of the respiratory system. Identify the major air volumes associated with ventilation. Structures to be studied: Respiratory
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Difficult Airway. Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital
 Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Basic Airway Management
 Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Dr. Sami Zaqout Faculty of Medicine IUG
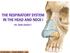 The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
The Nose External Nose Nasal Cavity External Nose Blood and Nerve Supplies of the External Nose Blood Supply of the External Nose The skin of the external nose Branches of the ophthalmic and the maxillary
The Respiratory System
 The Respiratory System Respiration Includes Pulmonary ventilation Air moves in and out of lungs Continuous replacement of gases in alveoli (air sacs) External respiration Gas exchange between blood and
The Respiratory System Respiration Includes Pulmonary ventilation Air moves in and out of lungs Continuous replacement of gases in alveoli (air sacs) External respiration Gas exchange between blood and
Larynx - cartilaginous structure holding the vocal folds which protrude into airstream
 1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
1! Larynx - cartilaginous structure holding the vocal folds which protrude into airstream 2! Flow increase - like thumb over garden hose Pressure drop - narrower space forces pressure drop due to speed
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Respiratory System Structures and Gas Exchange
 A. Respiratory medium the oxygen source 1. Air 2. Water Respiratory Medium Organism Cellular Respiration O 2 CO 2 B. Respiratory surface the structure where exchange of gases with the surrounding environment
A. Respiratory medium the oxygen source 1. Air 2. Water Respiratory Medium Organism Cellular Respiration O 2 CO 2 B. Respiratory surface the structure where exchange of gases with the surrounding environment
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. To study the occurrence of postoperative hyponatremia in paediatric patients under 2 years of age 2. Influence of timing of intravenous fluid therapy on maternal hemodynamics in patients undergoing
S.No. 1. To study the occurrence of postoperative hyponatremia in paediatric patients under 2 years of age 2. Influence of timing of intravenous fluid therapy on maternal hemodynamics in patients undergoing
Akhilesh Agrawal*, Smita S. Lele, Bharati A. Tendolkar
 International Journal of Research in Medical Sciences Agrawal A. Int J Res Med Sci. 2016 Aug;4(8):3224-3228 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162270
International Journal of Research in Medical Sciences Agrawal A. Int J Res Med Sci. 2016 Aug;4(8):3224-3228 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162270
Tony Capizzani, MD, FACS
 Tony Capizzani, MD, FACS Trauma Medical Director Hillcrest Hospital Cleveland Clinic October 2, 2017 No disclosures Goals and Objectives Describe airway anatomy and innervation Recognize the association
Tony Capizzani, MD, FACS Trauma Medical Director Hillcrest Hospital Cleveland Clinic October 2, 2017 No disclosures Goals and Objectives Describe airway anatomy and innervation Recognize the association
Objectives. Module A2: Upper Airway Anatomy & Physiology. Function of the Lungs/Heart. The lung is for gas exchange. Failure of the Lungs/Heart
 Module A2: Upper Airway Anatomy & Physiology Objectives Classify epithelial tissue based on cell type and tissue layers. Identify location of tissue epithelium in the respiratory system. Describe the major
Module A2: Upper Airway Anatomy & Physiology Objectives Classify epithelial tissue based on cell type and tissue layers. Identify location of tissue epithelium in the respiratory system. Describe the major
Chapter 2: Airway Management and Ventilation
 Chapter 2: Airway Management and Ventilation Objectives: Upon completion of this topic, the physician will be able to explain and demonstrate the principles of airway management. Specifically, the physician
Chapter 2: Airway Management and Ventilation Objectives: Upon completion of this topic, the physician will be able to explain and demonstrate the principles of airway management. Specifically, the physician
Anesthesia recommendations for patients suffering from Mucolipidosis II and III
 orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
orphananesthesia Anesthesia recommendations for patients suffering from Mucolipidosis II and III Disease name: Mucolipidosis Type 2 and 3 ICD 10: E77.0 Synonyms: Mucolipidosis type 2 - I-cell disease N-acetyl-glucosamine
(ix) Difficult & Failed Intubation Queen Charlotte s Hospital
 (ix) Difficult & Failed Intubation Queen Charlotte s Hospital Pre-operative Assessment Clinical assessment of airway and risk of difficult intubation: (can be performed in a matter of seconds): 1. Mouth
(ix) Difficult & Failed Intubation Queen Charlotte s Hospital Pre-operative Assessment Clinical assessment of airway and risk of difficult intubation: (can be performed in a matter of seconds): 1. Mouth
Cranial Nerve Monitoring Part II: What do I have to do if cranial nerves are being monitored?
 Cranial Nerve Monitoring Part II: What do I have to do if cranial nerves are being monitored? Laura Hemmer, M.D., FASA SNACC Neuromonitoring Subcommittee Linda S. Aglio, M.D., M.S. Arne Budde, M.D. Laura
Cranial Nerve Monitoring Part II: What do I have to do if cranial nerves are being monitored? Laura Hemmer, M.D., FASA SNACC Neuromonitoring Subcommittee Linda S. Aglio, M.D., M.S. Arne Budde, M.D. Laura
Emergency ENT Anaesthesia. Richard Semenov
 Emergency ENT Anaesthesia Richard Semenov Emergency ENT Anaesthesia Dr Richard Semenov MBBS (Adel) FRCA (UK) FANZCA Dept of Anaesthesia Royal Adelaide Hospital My Experience in Emergency ENT Anaesthesia
Emergency ENT Anaesthesia Richard Semenov Emergency ENT Anaesthesia Dr Richard Semenov MBBS (Adel) FRCA (UK) FANZCA Dept of Anaesthesia Royal Adelaide Hospital My Experience in Emergency ENT Anaesthesia
HUGE GOITER AND AIRWAY MANAGEMENT
 HUGE GOITER AND AIRWAY MANAGEMENT 1. Introduction 2. Airway challenges in goiter 3. ASA Difficult airway algorithm 4. Different methods to anaesthetic airway management 5. Flexible fiberoptic bronchoscopy
HUGE GOITER AND AIRWAY MANAGEMENT 1. Introduction 2. Airway challenges in goiter 3. ASA Difficult airway algorithm 4. Different methods to anaesthetic airway management 5. Flexible fiberoptic bronchoscopy
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Larynx. Rudimentary. Behind the posterior surface : -stylopharyngeus - salpingopharyngeus -platopharyngeus
 Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Larynx The larynx is an organ that provides a protective sphincter at the inlet of the air passages and is responsible for voice production. It extends from C3-C6: *Posterior: the pharynx *Lateral: the
Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always
 1 3 4 5 6 7 8 9 10 Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always take appropriate Standard measures
1 3 4 5 6 7 8 9 10 Chapter 7, Medication Administration Part 1 Principles and Routes of Medication Administration Caution: Administering medications is business Always take appropriate Standard measures
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
THE RESPIRATORY SYSTEM
 THE RESPIRATORY SYSTEM Functions of the Respiratory System Provides extensive gas exchange surface area between air and circulating blood Moves air to and from exchange surfaces of lungs Protects respiratory
THE RESPIRATORY SYSTEM Functions of the Respiratory System Provides extensive gas exchange surface area between air and circulating blood Moves air to and from exchange surfaces of lungs Protects respiratory
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
CAE Healthcare Human Patient Simulator (HPS)
 CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
CAE Healthcare Human Patient Simulator (HPS) The Human Patient Simulator, HPS, is a tethered simulator that is capable of patient assessment and treatment including mechanical ventilation and anesthesia.
GENERAL ANAESTHESIA AND FAILED INTUBATION
 GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
The Respiratory System
 The Respiratory System If you have not done so already, please print and bring to class the Laboratory Practical II Preparation Guide. We will begin using this shortly in preparation of your second laboratory
The Respiratory System If you have not done so already, please print and bring to class the Laboratory Practical II Preparation Guide. We will begin using this shortly in preparation of your second laboratory
Subdivided into Vestibule & Oral cavity proper
 Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
ORAL CAVITY, ESOPHAGUS AND STOMACH
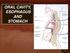 ORAL CAVITY, ESOPHAGUS AND STOMACH 1 OBJECTIVES By the end of the lecture you should be able to: Describe the anatomy the oral cavity, (boundaries, parts, nerve supply). Describe the anatomy of the palate,
ORAL CAVITY, ESOPHAGUS AND STOMACH 1 OBJECTIVES By the end of the lecture you should be able to: Describe the anatomy the oral cavity, (boundaries, parts, nerve supply). Describe the anatomy of the palate,
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia
 DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
MODULE 2 THE LABORATORY RAT
 University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
University Animal Care Committee LABORATORY ANIMAL BIOMETHODOLOGY WORKSHOP MODULE 2 THE LABORATORY RAT SUBSTANCE ADMINISTRATION AND BLOOD COLLECTION Substance Administration: Subcutaneous injection Intramuscular
Cranial Nerves VII to XII
 Cranial Nerves VII to XII MSTN121 - Neurophysiology Session 13 Department of Myotherapy Cranial Nerve VIII: Vestibulocochlear Sensory nerve with two distinct branches. Vestibular branch transmits information
Cranial Nerves VII to XII MSTN121 - Neurophysiology Session 13 Department of Myotherapy Cranial Nerve VIII: Vestibulocochlear Sensory nerve with two distinct branches. Vestibular branch transmits information
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper. Oral vestibule : is slit like space between.
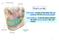 Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Types of Anaesthesia for dermal and lip fillers at Simply Fox
 Types of Anaesthesia for dermal and lip fillers at Simply Fox The Juvederm range we use contains lidocaine- a local anaesthetic, however this does not work instantly as the needle is inserted, it is mixed
Types of Anaesthesia for dermal and lip fillers at Simply Fox The Juvederm range we use contains lidocaine- a local anaesthetic, however this does not work instantly as the needle is inserted, it is mixed
Emergency Cricothyrotomy
 Emergency Cricothyrotomy SWORBHP Live Paramedic Rounds June 15, 2012 Sameer Mal PGY4 Emergency Medicine Dwayne Cottel Regional Paramedic Educator Overview BVM Ventilation Intro to Cricothyrotomy Relevant
Emergency Cricothyrotomy SWORBHP Live Paramedic Rounds June 15, 2012 Sameer Mal PGY4 Emergency Medicine Dwayne Cottel Regional Paramedic Educator Overview BVM Ventilation Intro to Cricothyrotomy Relevant
