Chemotherapy After Portal Vein Embolization to Protect Against Tumor Growth During Liver Hypertrophy Before Hepatectomy
|
|
|
- Magdalen Day
- 5 years ago
- Views:
Transcription
1 Research Original Investigation to Protect Against Tumor Growth During Liver Hypertrophy Before Hepatectomy Catha Fischer, MD; Laleh G. Melstrom, MD; Dean Arnaoutakis, MD; William Jarnagin, MD; Karen Brown, MD; Michael D Angelica, MD; Anne Covey, MD; Ronald DeMatteo, MD; Peter Allen, MD; T. Peter Kingham, MD; Scott Tuorto; Nancy Kemeny, MD; Yuman Fong, MD IMPORTANCE Portal vein embolization improves the safety of liver resection by increasing the size of residual liver, but the embolization may increase tumor growth during the waiting period before definitive hepatectomy. OBJECTIVE To determine whether the administration of chemotherapy mitigates tumor growth after portal vein embolization (PVE) performed before major hepatectomy for metastatic colorectal cancer. DESIGN, SETTING, AND PARTICIPANTS Review of prospectively collected data at Memorial-Sloan Kettering Cancer Center was conducted. The database included patients subjected to PVE before major hepatectomy for metastatic colorectal cancer. MAIN OUTCOMES AND MEASURES Lesions in both the embolized and nonembolized lobes of the liver before and 1 month after PVE were measured and Response Evaluation Criteria in Solid Tumors were applied to assess disease status. Assessment of survival was based on receipt of post-pve chemotherapy and then stratified by subsequent resectability. RESULTS Two hundred eight tumors were measured in 64 patients; 53 tumors were in patients undergoing post-pve chemotherapy. Approximately one-third of the lesions progressed after PVE when no chemotherapy was administered. This did not differ significantly according to whether tumors were ipsilateral or contralateral to the PVE. When chemotherapy was administered, there was a significantly lower rate of progression (18.9%, P =.3). In long-term follow-up, treatment with post-pve chemotherapy was also independently associated with improved survival (P <.6). CONCLUSIONS AND RELEVANCE Chemotherapy does not retard growth of the liver after PVE and may prevent cancer progression. Thus, the combination of PVE and chemotherapy may enhance both oncologic and operative safety. JAMA Surg. 213;148(12): doi:1.11/jamasurg Published online October 3, 213. Author Affiliations: Department of Surgery, Memorial Sloan-Kettering Cancer Center, New York, New York (Fischer, Melstrom, Arnaoutakis, Jarnagin, D Angelica, DeMatteo, Allen, Kingham, Tuorto, Fong); Department of Radiology, Memorial Sloan-Kettering Cancer Center, New York, New York (Brown, Covey, Fong); Department of Medicine, Memorial Sloan-Kettering Cancer Center, New York, New York (Kemeny). Corresponding Author: Yuman Fong, MD, Department of Surgery, Memorial Sloan-Kettering Cancer Center, 1275 York Ave, New York, NY 165 (FongY@mskcc.org). 113
2 Research Original Investigation Portal vein embolization (PVE) has become a standard technique for increasing residual liver mass before major hepatectomy 1-3 and has been shown to improve clinical outcome. 2 This technique was first proposed by Makuuchi et al 4 for improving the outcome of patients needing major hepatectomy for hilar cholangiocarcinoma. Portal vein embolization has proven to be a very safe procedure 5,6 with few major periprocedural complications. One concern raised regarding PVE is whether local factors stimulating growth of liver parenchyma after PVE will also stimulate growth of local macroscopic and microscopic tumors (Table 1) Metastatic colorectal cancer is the tumor most commonly resected by hepatectomy in Western populations. In this disease, great advancements in chemotherapy have been made recently, including the development and approval for use of irinotecan, 14 oxaliplatin, 15 cetuximab, 16 and bevacizumab. 17 These agents are often used to produce reduction of tumor bulk in initially unresectable cases to switch patients status to candidates for potentially curative resections. 18 Many other patients also receive these agents as neoadjuvant therapy before liver resection. We 2 previously demonstrated that PVE can be performed while the patient is continuing neoadjuvant or downstaging chemotherapy and results in growth of the liver to enhance subsequent hepatectomy. In the present study, we assessed tumor growth in the liver during the first month after PVE to determine whether concurrent neoadjuvant chemotherapy will influence the pace of tumor progression after PVE. Methods Patients We examined 64 consecutive PVEs performed in patients with metastatic colorectal cancer between September 1999 and September 24. An extended liver resection ( 4 segments of liver) was anticipated in all of these patients. Those receiving chemotherapy after PVE (n = 25) were compared with patients who did not receive chemotherapy after PVE (n = 5). Portal Vein Embolization The techniques of PVE at our institution have been described. 19 Briefly, an ipsilateral puncture of the portal vein is performed to decrease the likelihood of iatrogenic damage to the liver intended to be the remnant after resection. Embolization was performed using polyvinyl alcohol particles (2-3 μm). 6 Metallic coils were avoided to prevent interference with a concurrent protocol using magnetic resonance spectroscopy for assessment of liver function. Assessments Volumetric analysis of liver hypertrophy and atrophy was performed by computed tomography (CT) volumetrics comparing pre-embolization scans and scans performed 1 month later. All CT scanning was performed with a helical scanner, and the CT data were transferred to an independent workstation for assessment. Table 1. Previous Publications on Portal Vein Embolization and Tumor Growth Source Pamecha et al, 7 29 Pamecha et al, 8 29 Hayashi et al, 9 27 Barbaro et al, 1 23 Kokudo et al, Elias et al, Tumor Type (No. of Patients [PVE/Control]) CRC liver metastasis (42 [22/2]) CRC liver metastasis HCC (6); CCC (2) Primary colon liver metastasis (5); rectal lesions (1); carcinoid tumors (unchanged) (3) CRC liver metastasis (47 [18/29]) Metastasis in left liver lobe (5) Variable CT/MRI volumetry; mitotic rate; proliferation index (Ki67) Tumor mitotic rate; proliferation markers CT volumetry Spiral CT; nontumorous parenchymal volume ratio Hepatic parenchymal fraction; tumor volume and percent tumor volume; disease-free survival CT and CT arterial portography Abbreviations: CCC, cholangiocellular carcinoma; CRC, colorectal cancer; CT, computed tomography; HCC, hepatocellular carcinoma; MRI, magnetic resonance imaging; PVE, portal vein embolization;, increased. All tumors visible by CT were assessed. Tumors were measured along the longest axis and compared before and 1 month after PVE. Volume of the right and left sides of the liver was determined by semiautomated contouring of the scans. This was performed on serial transverse scans. On each section, the total liver was outlined and the sum of the sections was calculated by integrated software techniques using density threshold. This was repeated solely for the right side of the liver according to the plane of the middle hepatic vein. The difference between total liver volume and the volume of the right side of the liver was considered the volume of the left side. Results were recorded as percentage of volume change of the right and left sides of the liver. Clinical Data Clinical data, including complications and long-term survival, were collected and evaluated. This review of data was approved by the Memorial Sloan-Kettering Cancer Center institutional review board. All patients were reviewed and classified using a preoperative Clinical Risk Score (CRS) prognostic scoring system defined for colorectal metastasis. 2 This 5-point preoperative clinical scale evaluates the condition of patients by (1) disease-free interval of less than 12 months, (2) carcinoembryonic antigen greater than 2 ng/dl, (3) lymph node positive primary, (4) more than 1 hepatic lesion, and (5) hepatic lesion larger than 5 cm. Statistical Analysis Comparisons were performed by an unpaired t test and by χ 2 test as indicated. Nonparametric factors were compared by the Mann-Whitney test. 21 Survival probabilities were estimated using the Kaplan- Meier method. 22 Univariate associations between potential risk factors and survival were assessed using the log-rank test. Independent predictors of survival were determined using a proportional hazards regression model JAMA Surgery December 213 Volume 148, Number 12 jamasurgery.com
3 Original Investigation Research Table 2. Demographics of Patients Subjected to Preoperative PVE Characteristic Value Sex, No. Male 38 Female 26 Age, y Mean (SE) 55 (2) Median (range) 55 (29-79) Embolizations, No. Right 55 Left 9 Chemotherapy received after PVE before hepatectomy, No. 25 (39) (%) Fluorouracil/leucovorin 2 FOLFIRI 4 FOLFOX 8 FOLFOX/avastin 1 CPT11/oxaliplatin 2 Floxuridine/FOLFOX 2 Floxuridine/FOLFIRI 2 Floxuridine/irinotecan/oxaliplatin 4 Abbreviations: FOLFIRI, folinic acid, fluorouracil, and irinotecan; FOLFOX, folinic acid, fluorouracil, and oxaliplatin; PVE, portal vein embolization. Results Demographics The demographics of the study patients are listed in Table 2 and Table 3. There were 38 men and 26 women. The age of the patients was typical for this disease, with a median of 55 years. Most embolizations were right PVE (n = 55) in preparation for right-sided resections. Twenty-five of the patients received chemotherapy in the month after PVE. The regimens of chemotherapy used were varied and included systemic chemotherapy in only 17 cases (68%) and regional plus systemic chemotherapy in 8 cases (32%). The demographics of the patients (age, sex, or CRS) were similar in patients not receiving chemotherapy and those receiving chemotherapy (Table 3). Changes in Tumor Size In these 64 patients, 28 lesions were assessed. Forty-seven of the lesions were contralateral to the side of PVE, and 161 lesions were ipsilateral to the PVE. For patients who did not receive chemotherapy, 34.2% of lesions progressed by Response Evaluation Criteria in Solid Tumors criteria 24 in the month after PVE (Table 4) and did not differ significantly whether the lesion was ipsilateral or contralateral to the PVE. The changes in tumor size in centimeters are shown in Figure 1. Tumors in patients undergoing chemotherapy after PVE had suppressed growth compared with lesions in patients not subjected to chemotherapy (P <.1). For patients not receiving chemotherapy, the tumors had a mean (SD) growth of 8% (3%) in size, and the lesions in patients receiving chemotherapy had a 13% (8%) mean regression in size (P <.1). Table 3. Comparison of Patients Between Groups No Characteristic Chemotherapy (n = 39) Chemotherapy (n = 25) P Value Age, mean (SE), y 54 (4) 55 (3) NS Sex, No. NS Male Female Clinical Risk Score NS Median (range) 3 (1-4) 3 (-5) Contralateral liver hypertrophy, mean (SE), % 19 (3) 2 (7) NS No. not resected 16 9 NS No. resected Abbreviation: NS, not significant. Table 4. Changes in Tumor Size According to Side of Liver Tumor and Peri Portal Vein Embolization Chemotherapy a Characteristic No Chemotherapy Chemotherapy P Value Ipsilateral tumor, No. (%) Stable or response 74 (64.3) 36 (78.3) Progression 41 (35.7) 1 (21.7) Contralateral, No. (%) Stable or response 28 (7.) 7 (1.) Progression 12 (3.) All tumors, No. (%) Stable or response 12 (65.8) 43 (81.1).3 Progression 53 (34.2) 1 (18.9) a Response criteria are by Response Evaluation Criteria in Solid Tumors. Changes in Liver Size and Complications of PVE Overall, patients subjected to PVE experienced minimal adverse effects; 42% of the patients (n = 27) developed a temperature above 38 C (41% in the no-chemotherapy group and 44% in the chemotherapy group). The fever usually occurred on day 1 after embolization and was self-limiting. Twentyseven percent (n = 17) of the patients had leukocytosis (white blood cells >11 /μl [to convert to cells 1 9 /L, multiply by.1]; no chemotherapy, 26%; and chemotherapy, 28%). Neither of these effects was associated with infection. No other complications were noted. Within 3 days, the mean growth of the side of the liver contralateral to the side embolized was 22% (4%) in the no-chemotherapy group and 24% (.5%) in the chemotherapy group (P >.99). Perioperative Outcome Thirty-six patients (56%) in this series underwent resection (no chemotherapy, 53% [27]; chemotherapy, 69% [16]). The reason jamasurgery.com JAMA Surgery December 213 Volume 148, Number
4 Research Original Investigation Figure 1. Box Plots for Changes of Tumor Size 8 Figure 2. Kaplan-Meier Overall Survival Curves 1. Change in Size, cm Survival Chemotherapy after PVE No chemotherapy after PVE 4 No Chemotherapy After PVE Chemotherapy After PVE Months Results are shown for the tumors in patients who did and did not undergo chemotherapy after portal vein embolization (PVE) (P <.1). Boxes represent upper and lower quartiles of data; horizontal line in the box, median value; limit lines, maximum and minimum values excluding outliers; and solid circles, outliers (more or less than 3/2 times the upper or lower quartiles). for unresectable disease was identification of occult additional disease in all cases. Operative procedures for the 2 groups were similar (no chemotherapy, 8 trisectionectomy plus contralateral minor procedures and 12 lobectomies plus contralateral minor procedures; chemotherapy, 7 trisectionectomies plus and 9 lobectomies plus contralateral minor procedures). The complication rate overall was 24% (no chemotherapy, 3%; chemotherapy, 19%). The complications experienced by the nochemotherapy group included 1 deep vein thrombosis, 1 intraabdominal abscess, 3 wound infections, and 1 chemotherapy pump misperfusion. The complications experienced by the chemotherapy group included 1 wound infection and 2 pump misperfusions. Survival Analysis Thirty of the 64 patients died. The median survival of those who died was 15 months, and the median follow-up of survivors was 51 months. The long-term survival of the patients is shown in Figure 2. Even though the 2 groups were equivalent according to age, sex, CRS, and resectability (Table 1), patients subjected to chemotherapy after PVE had a significantly better survival (median: no chemotherapy, 23.7 months vs chemotherapy, 5.1 months; 5-year survival: no chemotherapy, 24% vs chemotherapy, 49%) (P =.6). The survival for patients separated by resectability is shown in Figure 3. To determine whether chemotherapy after PVE may be an independent predictor of outcome, we used multivariate analysis to examine the influence of chemotherapy and high CRS (Table 5). Use of chemotherapy remained highly correlated with improved outcome. Discussion Results are shown for patients after liver resection analyzed according to whether they received or did not receive chemotherapy after portal vein embolization (PVE) (P <.6). Portal vein embolization was first proposed 2 years ago as an effective means of increasing the functional residual liver by inducing liver hypertrophy in the unembolized lobe. 4 Originally, this procedure was proposed for use in hilar cholangiocarcinoma, in which a very large amount of liver is usually removed for a very small tumor. With the safety of PVE becoming well documented, this procedure is increasingly used for patients with metastatic colorectal cancer because of the increasing extent of resections surgeons are willing to undertake to eradicate disease. It is also becoming important in treatment of metastatic colorectal cancer because the various preoperative chemotherapeutic regimens often produce liver parenchymal damage and hinder posthepatectomy recovery. 25 There is no doubt that PVE has improved our ability to safely resect colorectal cancer that has metastasized to the liver. Two studies found that patients who had PVE prior to resection had survival rates equivalent to those in patients who did not have PVE despite the fact that patients who underwent PVE had more severe disease. 5,26 The present study examined a series of patients with advanced hepatic metastases (median CRS, 3) and demonstrated the role that PVE may play in complex multimodality treatment strategies. Recent data have been reassuring for the immediate periprocedural safety of PVE. Although there had been concerns regarding potential detrimental effects of PVE on liver function, clinical data clearly have shown PVE not to have major negative effects on hepatic function. 27 Our study 2 on the safety of these procedures showed PVE to be associated with only mild postembolization syndrome (fever, thrombocytopenia, and local pain). However, there remains concern regarding the potential for PVE to stimulate tumor growth. It has been hypothesized that by increasing portal blood flow to the unembolized lobe and inducing local growth factors, tumors in this lobe would enlarge. Many small studies 3,7-12 have shown conflicting results, with some studies demonstrating tumor growth by size 7 or DNA measurements. 8 In the present study, we demonstrated that, after PVE, one-third of the tumors grow sufficiently in the first month to be considered progression. We also showed that simultaneous administration of chemotherapy retarded such tumor progression and was associated with improved long-term survival. 116 JAMA Surgery December 213 Volume 148, Number 12 jamasurgery.com
5 Original Investigation Research Figure 3. Analysis of Survival According to Post Portal Vein Embolization Chemotherapy (PVE) Stratified by Subsequent Resectability Resected Not Resected Chemotherapy after PVE Chemotherapy after PVE Survival.5 No chemotherapy after PVE Survival Follow-up, mo Follow-up, mo No chemotherapy after PVE Results are shown for patients survival according to whether they received or did not receive chemotherapy after PVE(P <.7). Table 5. Multivariate Cox Proportional Hazards Regression Analysis of Survival Characteristic P Value Relative Risk a Peri-PVE chemotherapy.1.26 Resection.2.34 CRS > Sex NS Abbreviations: CRS, Clinical Risk Score; NS, not significant; PVE, portal vein embolization. a Relative risk not determined for sex because it was not a significant variable. Even without these new data, the use of chemotherapy with PVE has practical value. Many patients arrive for evaluation by the hepatic surgeon while receiving neoadjuvant chemotherapy. Furthermore, of patients with unresectable hepatic colorectal metastases, approximately 15% are now routinely converted to resectable cases by chemotherapy. If stopping chemotherapy for 3 to 6 weeks is necessary for PVE and waiting 4 to 6 weeks afterward is necessary to allow adequate hypertrophy, then patients with metastatic disease will need to be without cancer treatment for at least 7 to 12 weeks prior to hepatectomy. That is why Covey et al 2 and others 28 had previously examined the possibility of performing PVE while the patient is receiving chemotherapy. Initially, it was thought that neoadjuvant chemotherapy would impede liver hypertrophy. Thus, it was stopped several weeks before embolization, allowing for a period of time when potential for tumor growth was uninhibited. Beal et al 29 conducted a small retrospective study looking at 15 patients and showed that hypertrophy does occur in those who received PVE and chemotherapy. However, this occurred to a lesser extent than in patients who underwent only PVE. In a slightly larger study, Goéré et al 28 demonstrated no significant difference in hypertrophy response when chemotherapy was continued after PVE. Interestingly, they also showed no increase in postoperative complications among patients who continued chemotherapy. Most recently, Covey et al, 2 in one of the largest studies to date with a series of 1 patients, concluded that chemotherapy had no negative effects on hypertrophy. They further showed that patients who underwent PVE before resection had improved outcomes measured by reduced need for transfusion and reduced hospital stay after resection. From these and similar studies, it is evident that chemotherapy after PVE does not have a negative effect on liver hypertrophy. The present study shows that not only are the combination of PVE and chemotherapy safe and effective from a liver hypertrophy standpoint, it is associated with retarded tumor growth and improved long-term survival. Although recent advances in chemotherapy have been a major improvement in treatment for metastatic colorectal cancer, chemotherapy performed before hepatectomy is also producing new challenges for the liver surgeon. With this increasing experience with chemotherapy, a clinically apparent syndrome of liver injury has been noted chemotherapy-associated steatohepatitis. 3 This is not only a pathologic entity but one associated with adverse clini-cal outcomes. 25 Portal vein embolization was first introduced for cases in which very small liver remnants were anticipated 31,32 and for patients with liver parenchymal injury from hepatitis 33 ; it is now increasingly used in resections involving parenchymal damage from chemotherapy. 2 With the knowledge that the liver can still hypertrophy in a toxic environment, we can safely continue a modality that will shrink tumor burden while also using a strategy to produce more functional residual liver. This dual strategy of neoadjuvant chemotherapy and PVE allows physicians to make use of different approaches simultaneously, providing maximal benefit to our patients. If chemotherapy does not have to be halted after PVE, it eliminates the concern of tumor progression during the standard 3- to 4-week time until resection; moreover, as we have shown, chemotherapy can slow progression of disease. jamasurgery.com JAMA Surgery December 213 Volume 148, Number
6 Research Original Investigation ARTICLE INFORMATION Accepted for Publication: March 4, 213. Published Online: October 3, 213. doi:1.11/jamasurg Author Contributions: Drs Fischer and Fong had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Arnaoutakis, Allen, Kingham, Tuorto, Kemeny, Fong. Acquisition of data: Fischer, Arnaoutakis, Jarnagin, Brown, Covey, Tuorto, Fong. Analysis and interpretation of data: Fischer, Melstrom, D Angelica, DeMatteo, Kingham, Tuorto, Fong. Drafting of the manuscript: Fischer, Arnaoutakis, D Angelica, Kingham, Tuorto, Kemeny, Fong. Critical revision of the manuscript for important intellectual content: Fischer, Melstrom, Jarnagin, Brown, Covey, DeMatteo, Allen, Kingham, Tuorto, Fong. Statistical analysis: Fischer, Tuorto, Fong. Obtained funding: Fong. Administrative, technical, and material support: Fischer, Arnaoutakis, Jarnagin, D Angelica, Tuorto, Fong. Study supervision: Allen, Kingham, Kemeny, Fong. Conflict of Interest Disclosures: None reported. Funding/Support: This study was supported in part by US Public Health Service grants RO1CA75416, RO1CA72632, and RO1CA61524 (Dr Fong) from the National Institutes of Health. Role of the Sponsor: The National Institutes of Health had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication. REFERENCES 1. Palavecino M, Chun YS, Madoff DC, et al. Major hepatic resection for hepatocellular carcinoma with or without portal vein embolization: perioperative outcome and survival. Surgery. 29;145(4): Covey AM, Brown KT, Jarnagin WR, et al. Combined portal vein embolization and neoadjuvant chemotherapy as a treatment strategy for resectable hepatic colorectal metastases. Ann Surg. 28;247(3): Ribero D, Abdalla EK, Madoff DC, Donadon M, Loyer EM, Vauthey JN. Portal vein embolization before major hepatectomy and its effects on regeneration, resectability and outcome. Br J Surg. 27;94(11): Makuuchi M, Thai BL, Takayasu K, et al. Preoperative portal embolization to increase safety of major hepatectomy for hilar bile duct carcinoma: a preliminary report. Surgery. 199;17(5): Azoulay D, Castaing D, Krissat J, et al. Percutaneous portal vein embolization increases the feasibility and safety of major liver resection for hepatocellular carcinoma in injured liver. Ann Surg. 2;232(5): Covey AM, Tuorto S, Brody LA, et al. Safety and efficacy of preoperative portal vein embolization with polyvinyl alcohol in 58 patients with liver metastases. AJR Am J Roentgenol. 25;185(6): Pamecha V, Levene A, Grillo F, Woodward N, Dhillon A, Davidson BR. Effect of portal vein embolisation on the growth rate of colorectal liver metastases. Br J Cancer. 29;1(4): Pamecha V, Glantzounis G, Davies N, Fusai G, Sharma D, Davidson B. Long-term survival and disease recurrence following portal vein embolisation prior to major hepatectomy for colorectal metastases. Ann Surg Oncol. 29;16(5): Hayashi S, Baba Y, Ueno K, et al. Acceleration of primary liver tumor growth rate in embolized hepatic lobe after portal vein embolization. Acta Radiol. 27;48(7): Barbaro B, Di Stasi C, Nuzzo G, Vellone M, Giuliante F, Marano P. Preoperative right portal vein embolization in patients with metastatic liver disease: metastatic liver volumes after RPVE. Acta Radiol. 23;44(1): Kokudo N, Tada K, Seki M, et al. Proliferative activity of intrahepatic colorectal metastases after preoperative hemihepatic portal vein embolization. Hepatology. 21;34(2): Elias D, De Baere T, Roche A, Mducreux, Leclere J, Lasser P. During liver regeneration following right portal embolization the growth rate of liver metastases is more rapid than that of the liver parenchyma. Br J Surg. 1999;86(6): de Graaf W, van den Esschert JW, van Lienden KP, van Gulik TM. Induction of tumor growth after preoperative portal vein embolization: is it a real problem?ann Surg Oncol. 29;16(2): Saltz LB, Cox JV, Blanke C, et al; Irinotecan Study Group. Irinotecan plus fluorouracil and leucovorin for metastatic colorectal cancer. N Engl J Med. 2;343(13): Borner MM, Dietrich D, Stupp R, et al. Phase II study of capecitabine and oxaliplatin in first- and second-line treatment of advanced or metastatic colorectal cancer.jclin Oncol. 22;2(7): Cunningham D, Humblet Y, Siena S, et al. Cetuximab monotherapy and cetuximab plus irinotecan in irinotecan-refractory metastatic colorectal cancer. N Engl J Med. 24;351(4): Hurwitz H, Fehrenbacher L, Novotny W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 24;35(23): Adam R, Delvart V, Pascal G, et al. Rescue surgery for unresectable colorectal liver metastases downstaged by chemotherapy: a model to predict long-term survival. Ann Surg.24;24(4): Brown KT, Brody LA, Decorato DR, Getrajdman GI. Portal vein embolization with use of polyvinyl alcohol particles. J Vasc Interv Radiol. 21;12(7): Granger DL, Perfect JR, Durack DT. Virulence of Cryptococcus neoformans regulation of capsule synthesis by carbon dioxide. J Clin Invest. 1985;76(2): Matthews DE, Farewell VT. Understanding Medical Statistics. 2nd ed. New York, NY: Karger; Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. JAmStatAssoc. 1958;53: Barlow WE, Sun WH. Bootstrapped confidence intervals for the Cox model using a linear relative risk form. Stat Med. 1989;8(8): Tuma RS. Sometimes size doesn t matter: reevaluating RECIST and tumor response rate endpoints. J Natl Cancer Inst. 26;98(18): Karoui M, Penna C, Amin-Hashem M, et al. Influence of preoperative chemotherapy on the risk of major hepatectomy for colorectal liver metastases.ann Surg. 26;243(1): Elias D, Santoro R, Ouellet JF, Osmak L, de Baere T, Roche A. Simultaneous percutaneous right portal vein embolization and left liver tumor radiofrequency ablation prior to a major right hepatic resection for bilateral colorectal metastases. Hepatogastroenterology. 24;51(6): van den Esschert JW, de Graaf W, van Lienden KP, et al. Volumetric and functional recovery of the remnant liver after major liver resection with prior portal vein embolization: recovery after PVE and liver resection. J Gastrointest Surg. 29;13(8): Goéré D, Farges O, Leporrier J, Sauvanet A, Vilgrain V, Belghiti J. Chemotherapy does not impair hypertrophy of the left liver after right portal vein obstruction. J Gastrointest Surg. 26;1(3): Beal IK, Anthony S, Papadopoulou A, et al. Portal vein embolisation prior to hepatic resection for colorectal liver metastases and the effects of periprocedure chemotherapy. Br J Radiol. 26;79(942): Fong Y, Bentrem DJ. CASH (chemotherapyassociated steatohepatitis) costs. Ann Surg. 26;243(1): Abdalla EK, Barnett CC, Doherty D, Curley SA, Vauthey JN. Extended hepatectomy in patients with hepatobiliary malignancies with and without preoperative portal vein embolization. Arch Surg. 22;137(6): Hemming AW, Reed AI, Howard RJ, et al. Preoperative portal vein embolization for extended hepatectomy. Ann Surg.23;237(5): Wakabayashi H, Ishimura K, Okano K, et al. Application of preoperative portal vein embolization before major hepatic resection in patients with normal or abnormal liver parenchyma. Surgery. 22;131(1): JAMA Surgery December 213 Volume 148, Number 12 jamasurgery.com
Treatment of Colorectal Liver Metastases State of the Art
 Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy
 Original Article Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy Rebecca C. Auer, MD 1 ; Rebekah R. White, MD 2 ; Nancy E. Kemeny, MD
Original Article Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy Rebecca C. Auer, MD 1 ; Rebekah R. White, MD 2 ; Nancy E. Kemeny, MD
Colon Cancer Liver Metastases: Liver-Directed Therapy
 Colon Cancer Liver Metastases: Liver-Directed Therapy Shishir K. Maithel, MD FACS Assistant Professor of Surgery Division of Surgical Oncology Winship Cancer Institute Emory University August 10, 2014
Colon Cancer Liver Metastases: Liver-Directed Therapy Shishir K. Maithel, MD FACS Assistant Professor of Surgery Division of Surgical Oncology Winship Cancer Institute Emory University August 10, 2014
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D.
 Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options
 State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options Ioannis S. Hatzaras, MD, MPH, FACS Assistant Professor of Surgery Division of Surgical Oncology
State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options Ioannis S. Hatzaras, MD, MPH, FACS Assistant Professor of Surgery Division of Surgical Oncology
Colorectal Liver Metastases Metachronous
 Colorectal Liver Metastases Metachronous Professor Rowan Parks Professor of Surgical Sciences University of Edinburgh No disclosures Natural History of Unresected Untreated Colorectal Metastases Year N
Colorectal Liver Metastases Metachronous Professor Rowan Parks Professor of Surgical Sciences University of Edinburgh No disclosures Natural History of Unresected Untreated Colorectal Metastases Year N
Liver related complications in unresectable disease after portal vein embolization
 Original Article Liver related complications in unresectable disease after portal vein embolization Floor Huisman 1, Kasia P. Cieslak 1, Krijn P. van Lienden 2, Roelof J. Bennink 3, Thomas M. van Gulik
Original Article Liver related complications in unresectable disease after portal vein embolization Floor Huisman 1, Kasia P. Cieslak 1, Krijn P. van Lienden 2, Roelof J. Bennink 3, Thomas M. van Gulik
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer
 Journal of BUON 12: 209-213, 2007 2007 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer N.
Journal of BUON 12: 209-213, 2007 2007 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer N.
Treatment strategy of metastatic rectal cancer
 35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers
 Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers Ching-Wei D. Tzeng, M.D. Assistant Professor Surgical Oncology University of Kentucky Markey Cancer Center Affiliate Network
Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers Ching-Wei D. Tzeng, M.D. Assistant Professor Surgical Oncology University of Kentucky Markey Cancer Center Affiliate Network
Trattamento chirurgico delle lesioni epatiche secondarie difficili. Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica
 Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Quality Improvement for Portal Vein Embolization
 Cardiovasc Intervent Radiol (2010) 33:452 456 DOI 10.1007/s00270-009-9737-x CIRSE GUIDELINES Quality Improvement for Portal Vein Embolization Alban Denys Pierre Bize Nicolas Demartines Frederic Deschamps
Cardiovasc Intervent Radiol (2010) 33:452 456 DOI 10.1007/s00270-009-9737-x CIRSE GUIDELINES Quality Improvement for Portal Vein Embolization Alban Denys Pierre Bize Nicolas Demartines Frederic Deschamps
Evolution of Surgery: Role of the Surgeon in the Molecular and Technology Age. Yuman Fong, MD Memorial Sloan-Kettering Cancer Center Rio 2010
 Evolution of Surgery: Role of the Surgeon in the Molecular and Technology Age Yuman Fong, MD Memorial Sloan-Kettering Cancer Center Rio 2010 Molecular mechanisms for cancer Prevention and screening Molecular
Evolution of Surgery: Role of the Surgeon in the Molecular and Technology Age Yuman Fong, MD Memorial Sloan-Kettering Cancer Center Rio 2010 Molecular mechanisms for cancer Prevention and screening Molecular
Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases
 Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases Universe Leung a, Amber L. Simpson a,b, Lauryn B. Adams a, William R. Jarnagin a, Michael I. Miga b, and T. Peter
Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases Universe Leung a, Amber L. Simpson a,b, Lauryn B. Adams a, William R. Jarnagin a, Michael I. Miga b, and T. Peter
Management of Colorectal Liver Metastases
 Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Sequential preoperative hepatic vein embolization after portal vein embolization for extended left hepatectomy in colorectal liver metastases
 Munene et al. World Journal of Surgical Oncology 2013, 11:134 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Sequential preoperative hepatic vein embolization after portal vein embolization
Munene et al. World Journal of Surgical Oncology 2013, 11:134 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Sequential preoperative hepatic vein embolization after portal vein embolization
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy
 Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy Dr Chan Chung Yip MBBS, M.Med(Surgery), MD, FAMS, FRCSEd Senior Consultant and Head Department of Hepatopancreatobiliary
Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy Dr Chan Chung Yip MBBS, M.Med(Surgery), MD, FAMS, FRCSEd Senior Consultant and Head Department of Hepatopancreatobiliary
ORIGINAL ARTICLE. A Second Liver Resection Due to Recurrent Colorectal Liver Metastases. accepted as the only curative
 ORIGINAL ARTICLE A Second Liver Resection Due to Recurrent Colorectal Liver Metastases Antonio Sa Cunha, MD; Christophe Laurent, MD; Alexandre Rault, MD; Philippe Couderc, MD; Eric Rullier, MD; Jean Saric,
ORIGINAL ARTICLE A Second Liver Resection Due to Recurrent Colorectal Liver Metastases Antonio Sa Cunha, MD; Christophe Laurent, MD; Alexandre Rault, MD; Philippe Couderc, MD; Eric Rullier, MD; Jean Saric,
Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS
 Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS Survival Rates of by Stage of Adenocarcinoma of the Colon Liver Resection New Perspective Colorectal cancer liver
Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS Survival Rates of by Stage of Adenocarcinoma of the Colon Liver Resection New Perspective Colorectal cancer liver
Management of colorectal cancer liver metastases
 Management of colorectal cancer liver metastases Aliakbarian M. M.D. Assistant professor of surgery Organ Transplant & Hepatopancreatobiliary Surgeon SUBJECTS The importance of surgical resection in colorectal
Management of colorectal cancer liver metastases Aliakbarian M. M.D. Assistant professor of surgery Organ Transplant & Hepatopancreatobiliary Surgeon SUBJECTS The importance of surgical resection in colorectal
BACKGROUND: STUDY DESIGN: RESULTS: CONCLUSIONS:
 Improved Survival after Resection of Liver and Lung Colorectal Metastases Compared with Liver-Only Metastases: A Study of 112 Patients with Limited Lung Metastatic Disease Antoine Brouquet, MD, Jean Nicolas
Improved Survival after Resection of Liver and Lung Colorectal Metastases Compared with Liver-Only Metastases: A Study of 112 Patients with Limited Lung Metastatic Disease Antoine Brouquet, MD, Jean Nicolas
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Introduction. Christopher J. Hammond 1 Saadat Ali. Judith I. Wyatt 3 Giles J. Toogood
 Cardiovasc Intervent Radiol (2019) 42:552 559 https://doi.org/10.1007/s00270-018-02159-5 CLINICAL INVESTIGATION VENOUS INTERVENTIONS Segment 2/3 Hypertrophy is Greater When Right Portal Vein Embolisation
Cardiovasc Intervent Radiol (2019) 42:552 559 https://doi.org/10.1007/s00270-018-02159-5 CLINICAL INVESTIGATION VENOUS INTERVENTIONS Segment 2/3 Hypertrophy is Greater When Right Portal Vein Embolisation
Aintree University Hospital
 Aintree University Hospital Liverpool, UK Evolving role of DEBIRI with DC Bead - TACE in mcrc Hassan Z Malik MD FRCS Consultant Hepatobiliary Surgeon Hassan Z Malik is a consultant to Biocompatibles UK
Aintree University Hospital Liverpool, UK Evolving role of DEBIRI with DC Bead - TACE in mcrc Hassan Z Malik MD FRCS Consultant Hepatobiliary Surgeon Hassan Z Malik is a consultant to Biocompatibles UK
TIMOTHY M. PAWLIK, RICHARD D. SCHULICK, MICHAEL A. CHOTI
 The Oncologist Hepatobiliary Expanding Criteria for Resectability of Colorectal Liver Metastases TIMOTHY M. PAWLIK,RICHARD D. SCHULICK,MICHAEL A. CHOTI Department of Surgery, Johns Hopkins University School
The Oncologist Hepatobiliary Expanding Criteria for Resectability of Colorectal Liver Metastases TIMOTHY M. PAWLIK,RICHARD D. SCHULICK,MICHAEL A. CHOTI Department of Surgery, Johns Hopkins University School
Behandeling van colorectale levermetastasen. Rol van beeldvorming van de lever bij colorectaal carcinoom
 Behandeling van colorectale levermetastasen Rol van beeldvorming van de lever bij colorectaal carcinoom B. Op de Beeck Universitair Ziekenhuis Antwerpen bart.op.de.beeck@uza.be 10.12.2016 AZ Turnhout campus
Behandeling van colorectale levermetastasen Rol van beeldvorming van de lever bij colorectaal carcinoom B. Op de Beeck Universitair Ziekenhuis Antwerpen bart.op.de.beeck@uza.be 10.12.2016 AZ Turnhout campus
ORIGINAL ARTICLE. Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases
 ORIGINAL ARTICLE Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases Evan S. Glazer, MD; Karen Beaty, PA-C; Eddie K. Abdalla, MD; J.
ORIGINAL ARTICLE Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases Evan S. Glazer, MD; Karen Beaty, PA-C; Eddie K. Abdalla, MD; J.
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma
 Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Future Liver Remnant (FLR) Increase in Patients with Colorectal Liver Metastases Is Highest the First Week After Portal Vein Occlusion
 Journal of Gastrointestinal Surgery https://doi.org/10.1007/s11605-018-4031-3 ORIGINAL ARTICLE Future Liver Remnant (FLR) Increase in Patients with Colorectal Liver Metastases Is Highest the First Week
Journal of Gastrointestinal Surgery https://doi.org/10.1007/s11605-018-4031-3 ORIGINAL ARTICLE Future Liver Remnant (FLR) Increase in Patients with Colorectal Liver Metastases Is Highest the First Week
How to deal with synchronous primary and liver metastases
 How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
Surgical treatment of colorectal liver metastases
 Review Article Page 1 of 9 Surgical treatment of colorectal liver metastases Amanda B. Cooper, Steven A. Curley Department of Surgical Oncology, The University of Texas M.D. Anderson Cancer Center, Houston,
Review Article Page 1 of 9 Surgical treatment of colorectal liver metastases Amanda B. Cooper, Steven A. Curley Department of Surgical Oncology, The University of Texas M.D. Anderson Cancer Center, Houston,
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan
 State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan Consultant GI Medical Oncologist National Cancer Centre Singapore Clinician Scientist, Genome Institute of Singapore OS (%) Overall survival
State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan Consultant GI Medical Oncologist National Cancer Centre Singapore Clinician Scientist, Genome Institute of Singapore OS (%) Overall survival
General summary GENERAL SUMMARY
 General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
LiverGroup.org. Case Report Form (CRF) for STAGED procedures
 Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver
 Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver Risa Small BA, Nir Lubezky MD and Menahem Ben-Haim MD Liver Surgery Unit, Department of Surgery B, Tel Aviv
Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver Risa Small BA, Nir Lubezky MD and Menahem Ben-Haim MD Liver Surgery Unit, Department of Surgery B, Tel Aviv
Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in Patients with Colorectal Liver Metastases
 Ann Surg Oncol DOI 1.1245/s1434-9-887-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in with Colorectal Liver Metastases
Ann Surg Oncol DOI 1.1245/s1434-9-887-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in with Colorectal Liver Metastases
Liver metastases: treatment planning. PJ Valette
 Liver metastases: treatment planning PJ Valette Liver metastases removal December 2010 April 2011 : after chemotherapy June 2011 : after resection of left lobe mets & portal embol. Sept 2011 : 1 year after
Liver metastases: treatment planning PJ Valette Liver metastases removal December 2010 April 2011 : after chemotherapy June 2011 : after resection of left lobe mets & portal embol. Sept 2011 : 1 year after
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Radiation Therapy for Liver Malignancies
 Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
Introduction. Case Report
 Case Report A patient who showed a pathologically complete response after undergoing treatment with XELOX plus bevacizumab for synchronous liver metastasis of grade H2 from sigmoid colon cancer Yasuhito
Case Report A patient who showed a pathologically complete response after undergoing treatment with XELOX plus bevacizumab for synchronous liver metastasis of grade H2 from sigmoid colon cancer Yasuhito
COLORECTAL CANCER 44
 COLORECTAL CANCER 44 Colorectal Cancer Highlights from the 2009 Annual Meeting of the American Society of Clinical Oncology Edited by Stuart M. Lichtman, MD Memorial Sloan-Kettering Cancer Center Commack,
COLORECTAL CANCER 44 Colorectal Cancer Highlights from the 2009 Annual Meeting of the American Society of Clinical Oncology Edited by Stuart M. Lichtman, MD Memorial Sloan-Kettering Cancer Center Commack,
The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative Chemotherapy: Is the Treatment Worthwhile?
 1179 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(7): 1179-1186. doi: 10.7150/jca.18091 The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative
1179 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(7): 1179-1186. doi: 10.7150/jca.18091 The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative
UvA-DARE (Digital Academic Repository) Radiological aspects of portal vein embolization van Lienden, K.P. Link to publication
 UvA-DARE (Digital Academic Repository) Radiological aspects of portal vein embolization van Lienden, K.P. Link to publication Citation for published version (APA): van Lienden, K. P. (2012). Radiological
UvA-DARE (Digital Academic Repository) Radiological aspects of portal vein embolization van Lienden, K.P. Link to publication Citation for published version (APA): van Lienden, K. P. (2012). Radiological
Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study
 Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Risk factors for cancer recurrence or death within 6 months after liver resection in patients with colorectal cancer liver metastasis
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.5.257 Annals of Surgical Treatment and Research Risk factors for cancer recurrence or death within 6 months after
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.5.257 Annals of Surgical Treatment and Research Risk factors for cancer recurrence or death within 6 months after
Current Status of Adjuvant Therapy for Colorectal Cancer
 Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
Portal Vein Embolization for Hepatocellular Carcinoma
 2235-1795/0014-0159$38.00/0 159 Review Portal Vein Embolization for Hepatocellular Carcinoma Junichi Shindoh Ching-Wei D. Tzeng Jean-Nicolas Vauthey Department of Surgical Oncology, The University of Texas
2235-1795/0014-0159$38.00/0 159 Review Portal Vein Embolization for Hepatocellular Carcinoma Junichi Shindoh Ching-Wei D. Tzeng Jean-Nicolas Vauthey Department of Surgical Oncology, The University of Texas
Liver surgery for colorectal liver metastases. Keith Roberts, Consultant Liver Transplant and Liver/Pancreas Surgeon University Hospitals Birmingham
 Liver surgery for colorectal liver metastases Keith Roberts, Consultant Liver Transplant and Liver/Pancreas Surgeon University Hospitals Birmingham Introduction: what do we do? UHB Liver Unit: Liver resections
Liver surgery for colorectal liver metastases Keith Roberts, Consultant Liver Transplant and Liver/Pancreas Surgeon University Hospitals Birmingham Introduction: what do we do? UHB Liver Unit: Liver resections
Effect of portal vein embolisation on the growth rate of colorectal liver metastases
 British Journal of Cancer (29) 1, 617 622 & 29 Cancer Research UK All rights reserved 7 92/9 $32. www.bjcancer.com Effect of portal vein embolisation on the growth rate of colorectal liver metastases V
British Journal of Cancer (29) 1, 617 622 & 29 Cancer Research UK All rights reserved 7 92/9 $32. www.bjcancer.com Effect of portal vein embolisation on the growth rate of colorectal liver metastases V
Impact of nutritional status in the era of FOLFOX/FIRI-based chemotherapy
 Okada et al. World Journal of Surgical Oncology (2017) 15:162 DOI 10.1186/s12957-017-1226-0 RESEARCH Open Access Impact of nutritional status in the era of FOLFOX/FIRI-based chemotherapy Shunji Okada,
Okada et al. World Journal of Surgical Oncology (2017) 15:162 DOI 10.1186/s12957-017-1226-0 RESEARCH Open Access Impact of nutritional status in the era of FOLFOX/FIRI-based chemotherapy Shunji Okada,
Five-year Survival following Radiofrequency Ablation of Small, Solitary, Hepatic Colorectal Metastases
 Five-year Survival following Radiofrequency Ablation of Small, Solitary, Hepatic Colorectal Metastases Alice R. Gillams, MBChB, MRCP, FRCR, and William R. Lees, MBBS, FRCR, FRCS PURPOSE: Radiofrequency
Five-year Survival following Radiofrequency Ablation of Small, Solitary, Hepatic Colorectal Metastases Alice R. Gillams, MBChB, MRCP, FRCR, and William R. Lees, MBBS, FRCR, FRCS PURPOSE: Radiofrequency
LIVER SURGERY 2. Case 1. Med 5 Refresher Course (Surgery) 2013/14. Dr Sunny Cheung
 LIVER SURGERY 2 Med 5 Refresher Course (Surgery) 2013/14 24 Jun 2013 Dr Sunny Cheung Case 1 50/M Sudden onset of epigastric pain Abdominal distension Confused HR 120 BP 80/50 Haemocue = 8 What should you
LIVER SURGERY 2 Med 5 Refresher Course (Surgery) 2013/14 24 Jun 2013 Dr Sunny Cheung Case 1 50/M Sudden onset of epigastric pain Abdominal distension Confused HR 120 BP 80/50 Haemocue = 8 What should you
Colorectal liver metastases: making the unresectable resectable using irreversible electroporation for microscopic positive margins acasereport
 Schoellhammer et al. BMC Cancer (2015) 15:271 DOI 10.1186/s12885-015-1279-9 CASE REPORT Open Access Colorectal liver metastases: making the unresectable resectable using irreversible electroporation for
Schoellhammer et al. BMC Cancer (2015) 15:271 DOI 10.1186/s12885-015-1279-9 CASE REPORT Open Access Colorectal liver metastases: making the unresectable resectable using irreversible electroporation for
Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy: A Report of Two Cases
 Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Colorectal Liver Metastases
 J Gastrointest Surg (2013) 17:195 202 DOI 10.1007/s11605-012-2022-3 EVIDENCE-BASED CURRENT SURGICAL PRACTICE Colorectal Liver Metastases Ching-Wei D. Tzeng & Thomas A. Aloia Received: 22 July 2012 /Accepted:
J Gastrointest Surg (2013) 17:195 202 DOI 10.1007/s11605-012-2022-3 EVIDENCE-BASED CURRENT SURGICAL PRACTICE Colorectal Liver Metastases Ching-Wei D. Tzeng & Thomas A. Aloia Received: 22 July 2012 /Accepted:
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Hepatic arterial infusion pump chemotherapy for colorectal liver metastases: an old technology in a new era
 Curr Oncol, Vol. 21, pp. e116-121; doi: http://dx.doi.org/10.3747/co.21.1592 HAI PUMP CHEMOTHERAPY FOR CRC METASTASIS REVIEW ARTICLE Hepatic arterial infusion pump chemotherapy for colorectal liver metastases:
Curr Oncol, Vol. 21, pp. e116-121; doi: http://dx.doi.org/10.3747/co.21.1592 HAI PUMP CHEMOTHERAPY FOR CRC METASTASIS REVIEW ARTICLE Hepatic arterial infusion pump chemotherapy for colorectal liver metastases:
Current Treatment of Colorectal Metastases. Dr. Thavanathan Surgical Grand Rounds February 1, 2005
 Current Treatment of Colorectal Metastases Dr. Thavanathan Surgical Grand Rounds February 1, 2005 25% will have metastases at initial presentation 25-50% 50% will develop metastases later 40% of potentially
Current Treatment of Colorectal Metastases Dr. Thavanathan Surgical Grand Rounds February 1, 2005 25% will have metastases at initial presentation 25-50% 50% will develop metastases later 40% of potentially
Chemotherapy for resectable liver mets: Options and Issues. Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA
 Chemotherapy for resectable liver mets: Options and Issues Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA Chemotherapy regimens in 1 st line mcrc Standard FOLFOX-Bev FOLFIRI-Bev
Chemotherapy for resectable liver mets: Options and Issues Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA Chemotherapy regimens in 1 st line mcrc Standard FOLFOX-Bev FOLFIRI-Bev
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Chemotherapy of colon cancers
 Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Reference No: Author(s) Approval date: 12/05/16. Committee. June Operational Date: Review:
 Reference No: Title: Author(s) Systemic Anti-Cancer Therapy (SACT) Guidelines for Biliary Tract Cancer (BTC) Dr Colin Purcell, Consultant Medical Oncologist on behalf of the GI Oncologists Group, Cancer
Reference No: Title: Author(s) Systemic Anti-Cancer Therapy (SACT) Guidelines for Biliary Tract Cancer (BTC) Dr Colin Purcell, Consultant Medical Oncologist on behalf of the GI Oncologists Group, Cancer
Targeted Therapies in Metastatic Colorectal Cancer: An Update
 Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Management of Stage IV Colorectal Cancer: Expanding the Horizon
 Management of Stage IV Colorectal Cancer: Expanding the Horizon May Tee, MD, MPH and Jan Franko, MD, PhD MercyOne Surgical Group (Mercy Surgical Affiliates) GI Oncology Conference 2019 March 1, 2019 Disclosures
Management of Stage IV Colorectal Cancer: Expanding the Horizon May Tee, MD, MPH and Jan Franko, MD, PhD MercyOne Surgical Group (Mercy Surgical Affiliates) GI Oncology Conference 2019 March 1, 2019 Disclosures
Surgery for hilar cholangiocirconoma
 Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
* * * * Supplementary Figure 1. DS Lv CK HSA CK HSA. CK Col-3. CK Col-3. See overleaf for figure legend. Cancer cells
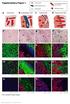 Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma
 Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma Taylor S. Riall, MD, PhD CERCIT Workshop October 19, 2012 Department of Surgery Center for Comparative Effectiveness
Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma Taylor S. Riall, MD, PhD CERCIT Workshop October 19, 2012 Department of Surgery Center for Comparative Effectiveness
Published: Address correspondence to Vidal-Jove Joan:
 Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
New Options in Metastatic Colorectal Cancer. Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka
 New Options in Metastatic Colorectal Cancer Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka 4 th most frequently diagnosed CA in the US 2 nd leading cause of CA death in the US Incidence
New Options in Metastatic Colorectal Cancer Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka 4 th most frequently diagnosed CA in the US 2 nd leading cause of CA death in the US Incidence
Management of Cholangiocarcinoma. Roseanna Lee, MD PGY-5 Kings County Hospital
 Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection of Colorectal Liver Metastases
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2-11-2008 Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2-11-2008 Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection
Lymph node ratio as a prognostic factor in stage III colon cancer
 Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
RESEARCH ARTICLE. Qian Liu, Jian-Jun Bi, Yan-Tao Tian, Qiang Feng, Zhao-Xu Zheng, Zheng Wang* Abstract. Introduction. Materials and Methods
 RESEARCH ARTICLE Outcome after Simultaneous Resection of Gastric Primary Tumour and Synchronous Liver Metastases: Survival Analysis of a Single-center Experience in China Qian Liu, Jian-Jun Bi, Yan-Tao
RESEARCH ARTICLE Outcome after Simultaneous Resection of Gastric Primary Tumour and Synchronous Liver Metastases: Survival Analysis of a Single-center Experience in China Qian Liu, Jian-Jun Bi, Yan-Tao
Cholangiocarcinoma. GI Practice Guideline. Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist)
 Cholangiocarcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist) Approval Date: October 2006 This guideline is a statement of consensus
Cholangiocarcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist) Approval Date: October 2006 This guideline is a statement of consensus
Patient Presentation. 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201
 Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Although the international TNM classification system
 Prognostic Significance of Perioperative Serum Carcinoembryonic Antigen in Non-Small Cell Lung Cancer: Analysis of 1,000 Consecutive Resections for Clinical Stage I Disease Morihito Okada, MD, PhD, Wataru
Prognostic Significance of Perioperative Serum Carcinoembryonic Antigen in Non-Small Cell Lung Cancer: Analysis of 1,000 Consecutive Resections for Clinical Stage I Disease Morihito Okada, MD, PhD, Wataru
Preoperative Percutaneous Transhepatic Portal Vein Embolization With Ethanol Injection
 Vascular and Interventional Radiology Original Research Sakuhara et al. Embolization of Vein With Ethanol Injection Vascular and Interventional Radiology Original Research Yusuke Sakuhara 1 Daisuke Abo
Vascular and Interventional Radiology Original Research Sakuhara et al. Embolization of Vein With Ethanol Injection Vascular and Interventional Radiology Original Research Yusuke Sakuhara 1 Daisuke Abo
Correspondence should be addressed to Roland Andersson,
 Gastroenterology Research and Practice Volume 2012, Article ID 568214, 4 pages doi:10.1155/2012/568214 Research Article Repeated Liver Resection for Colorectal Liver Metastases: A Comparison with Primary
Gastroenterology Research and Practice Volume 2012, Article ID 568214, 4 pages doi:10.1155/2012/568214 Research Article Repeated Liver Resection for Colorectal Liver Metastases: A Comparison with Primary
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Case Conference. Craig Morgenthal Department of Surgery Long Island College Hospital
 Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung
 How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
How to evaluate tumor response? Yonsei University College of Medicine Kim, Beom Kyung End points in research for solid cancers Overall survival (OS) The most ideal one, but requires long follow-up duration
treatment options for primary liver malignancies and metastatic disease
 State of the art treatment options for primary liver malignancies and metastatic disease Peter Huppert Prof. of Radiology and Neuroradiology Klinikum Darmstadt Certified Vascular and Oncologic Center Disclosure
State of the art treatment options for primary liver malignancies and metastatic disease Peter Huppert Prof. of Radiology and Neuroradiology Klinikum Darmstadt Certified Vascular and Oncologic Center Disclosure
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
BACKGROUND. The current study evaluated the effect of bevacizumab added to
 2761 Bevacizumab Improves Pathologic Response and Protects Against Hepatic Injury in Patients Treated With Oxaliplatin-Based Chemotherapy for Colorectal Liver Metastases Dario Ribero, MD 1 Huamin Wang,
2761 Bevacizumab Improves Pathologic Response and Protects Against Hepatic Injury in Patients Treated With Oxaliplatin-Based Chemotherapy for Colorectal Liver Metastases Dario Ribero, MD 1 Huamin Wang,
Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131
 Colorectal cancer: diagnosis and management Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Colorectal cancer: diagnosis and management Clinical guideline Published: 1 November 2011 nice.org.uk/guidance/cg131 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Nomogram for prediction of prognosis in patients with initially unresectable colorectal liver metastases
 Original article Nomogram for prediction of prognosis in patients with initially unresectable colorectal liver metastases K. Imai 1,2,5, M.-A. Allard 1,2,4, C. Castro Benitez 1,2,4,E.Vibert 1,3,4, A. Sa
Original article Nomogram for prediction of prognosis in patients with initially unresectable colorectal liver metastases K. Imai 1,2,5, M.-A. Allard 1,2,4, C. Castro Benitez 1,2,4,E.Vibert 1,3,4, A. Sa
Kaoru Takeshima, Kazuo Yamafuji, Atsunori Asami, Hideo Baba, Nobuhiko Okamoto, Hidena Takahashi, Chisato Takagi, and Kiyoshi Kubochi
 Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Helping you access curative therapies for liver cancer patients
 Metastatic colorectal cancer (mcrc) Helping you access curative therapies for liver cancer patients Biocompatibles Excellence in Interventional Oncology Biocompatibles UK Ltd is a BTG International group
Metastatic colorectal cancer (mcrc) Helping you access curative therapies for liver cancer patients Biocompatibles Excellence in Interventional Oncology Biocompatibles UK Ltd is a BTG International group
Metastatic Liver Cancer
 4 Metastatic Liver Cancer ANDREW J. SMITH, MD, FRCSC RONALD P. DEMATTEO, MD YUMAN FONG, MD, FACS LESLIE H. BLUMGART, MD, FACS, FRCS (ENG, EDIN, GLAS) The management of hepatic metastases has become more
4 Metastatic Liver Cancer ANDREW J. SMITH, MD, FRCSC RONALD P. DEMATTEO, MD YUMAN FONG, MD, FACS LESLIE H. BLUMGART, MD, FACS, FRCS (ENG, EDIN, GLAS) The management of hepatic metastases has become more
Perioperative Chemotherapy With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection
 Original Study Perioperative With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection Anastasia Constantinidou, 1 David Cunningham, 1 Fatima Shurmahi, 1 Uzma
Original Study Perioperative With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection Anastasia Constantinidou, 1 David Cunningham, 1 Fatima Shurmahi, 1 Uzma
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis?
 Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
