Magnetic Resonance Imaging in the Evaluation of Infantile Torticollis
|
|
|
- Elisabeth Farmer
- 5 years ago
- Views:
Transcription
1 Magnetic Resonance Imaging in the Evaluation of Infantile Torticollis SHITAL N. PARIKH, MD; ALVIN H. CRAWFORD, MD; SAM CHOUDHURY, MD abstract This retrospective study assessed the use of magnetic resonance imaging (MRI) in 58 infants with infantile torticollis. Eighteen patients had nonmuscular causes of torticollis (group 1); MRI identified lesions in 16 patients. Of 40 patients with a diagnosis of congenital muscular torticollis (group 2), 28 had a normal MRI. Five patients had asymmetry of the sternocleidomastoid without noticeable signal changes. Seven patients showed evidence of fibromatosis colli. Asymmetry of the posterolateral skull consistent with plagiocephaly was common. Magnetic resonance imaging did not alter treatment of group 2. Findings of compartment syndrome of sternocleidomastoid were inconsistent. Magnetic resonance imaging is not recommended for asymptomatic patients with infantile torticollis. Infantile torticollis is defined as torticollis in a patient aged 1 year. 1 It can be congenital (present at or soon after birth) or acquired. It may originate from a number of primary etiologies including congenital muscular torticollis, congenital postural torticollis, ocular abnormalities, osseous abnormalities, and neurologic abnormalities Congenital muscular torticollis is the most common cause of torticollis and is the third most common congenital deformity, with hip dysplasia and pes equinovarus being more common. 20 Although many theories of etiology have been proposed, recent reports surmised that compartment syndrome of the sternocleidomastoid may be an etiologic factor in congenital muscular torticollis. 21 The nonmuscular causes of torticollis in children are less common. In a report of 288 patients with torticollis, the estimated prevalence was 18.4%. 2 The previous two decades have resulted in substantial technological advancements in radiographic imaging. New noninvasive imaging modalities have been developed and existing modalities have been refined. Magnetic resonance imaging (MRI) allows improved anatomical visualization of the spine and central nervous system without undue radiation exposure. The ubiquitous availability of MRI, however, may have led to its over use and inappropriate application. Ballock and Song 2 suggested a useful algorithm for evaluation of torticollis in children. Initial evaluation of any patient with torticollis should involve a thorough history and physical examination including neurologic assessment, followed by plain radiographs and ophthalmologic consultation in a step-wise approach. Magnetic resonance imaging should be obtained only when the ophthalmologic evaluation is negative or the initial neurologic examination is abnormal. Most patients with infantile torticollis who underwent MRI at our institution were referred from outside pediatric facilities. We hypothesized that MRI was increasingly used as a general screening study in otherwise asymptomatic patients with infantile torticollis or in the absence of a working clinical diagnosis. This study assessed the use of MRI in evaluating infantile torticollis and identified the signs of compartment syndrome of sternocleidomastoid as a factor in the development of congenital muscular torticollis. MATERIALS AND METHODS A computerized medical recordretrieval system was used to identify all patients referred to our institution from for MRI evaluation of torticollis. The medical records of these patients were screened by the lead author From the Department of Pediatric Orthopedic Surgery, Cincinnati Children s Hospital Medical Center, Cincinnati, Ohio. The authors thank Susan L. Foad for manuscript preparation. Reprint requests: Alvin H. Crawford, MD, Dept of Pediatric Orthopedic Surgery, Cincinnati Children s Hospital Medical Center, 3333 Burnet Ave, Cincinnati, OH MAY 2004 Volume 27 Number 5 509
2 TABLE 1 Patient Data and Rate of Positive MRI Findings Demographic Group 1 Group 2 Total No. patients Mean age SD (mos) Male:Female 10:8 19:21 29:29 Left:Right 8:10 19:21 27:31 Positive MRI findings (%) 16 (89) 12 (30) 28 (48) Positive orthopedic MRI findings (%) 2 (11) 12 (30) 14 (24) Abbreviations: MRI=magnetic resonance imaging and SD=standard deviation. TABLE 2 Clinical and MRI Findings in Group 1 Patients With Infantile Torticollis (n=18) Clinical Presentation/ Diagnosis* No. MRI Findings* No. Seizures 6 Normal 2 Developmental delay 6 Plagiocephaly 7 Facial asymmetry 5 Macrocrania/mild communicating 5 (2 ) hydrocephalus Hydrocephalus 3 Inflammatory cells in mastoid 4 (2 ) Neck mass 2 Corpus callosum hypoplasia 5 Hoarse cry 2 Cervical lymphadenopathy 2 Ptosis 1 Parenchymal volume loss 2 Otorrhea 1 Arnold-Chiari malformation 2 Hemiplegia 1 Parotid hemangioma 2 Right arm paresis 1 Malignant peripheral nerve sheath tumor 1 Hypotonia 1 Middle ear congestion 1 Erb s palsy 1 Brachycephaly 1 Down s syndrome 1 Hyperintense globus pallidus 1 Hairy patch 1 Rhombocephalosynapsis 1 Vomiting 1 Craniosynostosis 1 Post-traumatic 1 C1-C2 rotatory subluxation 1 Spinal canal narrowing 1 Abbreviation: MRI=magnetic resonance imaging. *Patient may have more than one clinical or MRI finding. Incidental finding. TABLE 3 Clinical and MRI Findings in Group 2 Patients With Infantile Torticollis (n=40) Clinical Presentation/Diagnosis* No. MRI Findings* No. Congenital muscular torticollis 40 Normal 28 Facial asymmetry 4 Fibromatosis colli with signal 7 changes Mass within sternocleidomastoid 1 Sternocleidomastoid asymmetry 5 Plagiocephaly 6 Macrocrania/mild communicating 2 hydrocephalus Inflammatory cells in mastoid 2 Abbreviation: MRI=magnetic resonance imaging. *Patient may have more than one clinical or MRI findings. Incidental finding. Congenital muscular torticollis is the most common cause of torticollis and is the third most common congenital deformity. (S.N.P.) to determine their age at initial presentation and initial diagnosis. All patients initially presenting after age 12 months and patients with insufficient documentation were excluded from the study. Eighty-six patients with congenital torticollis who underwent MRI evaluation were initially identified. Twenty-eight patients were excluded because of delayed initial presentation (age 12 months) or inadequate documentation. The remaining 58 patients (29 boys and 29 girls) comprised the study group. Patients were divided into two groups. Group 1 consisted of 18 patients with infantile torticollis with associated specific clinical findings (eg, neurogenic torticollis, osseous anomalies of the cervical spine, or otolaryngology involvement). Group 2 consisted of 40 patients with congenital muscular torticollis. The medical charts of these patients were reviewed for age at presentation, sex, side of involvement, symptoms, clinical findings, imaging studies, and primary diagnosis. The MRI reports were reviewed for the type of examination, procedure comments, MRI findings, and final impression. All MRIs were reviewed, with special attention to bilateral sternocleidomastoid muscles, to identify any comparable asymmetry or signal changes. A clinicopathological correlation was established for both patient groups. All patients had evidence of torticollis from the neonatal period. The majority of MRI examinations were referred by primary care physicians from the communi- 510 ORTHOPEDICS
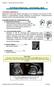
3 MRI EVALUATION OF INFANTILE TORTICOLLIS PARIKH ET AL ty or outside pediatric facilities. The mean age at initial presentation for all 58 patients was 7 months (range: 1-12 months). The majority of MRIs were performed with the patient under sedation, with strict adherence to the hospital sedation policy. Standard technique for softtissue visualization was used, and imaging was performed in coronal, sagittal, and transverse planes. resonance imaging showed anteroposterior narrowing of the cervical spinal canal. A 12-month-old male patient presented with post-traumatic torticollis. Magnetic resonance imaging showed C1-C2 rotatory subluxation; however, this was diagnosed previously on computed tomography (CT). Of 6 patients with developmental delay, The clinical and MRI findings in group 2 patients are summarized in Table 3. The indications for the majority of MRIs were to rule out posterior fossa tumors. All patients in this group had congenital muscular torticollis, which was diagnosed by RESULTS Patient data and rate of positive MRI findings in each group and in the entire study group are summarized in Table 1. The torticollis was left-sided in 27 patients and rightsided in 31 patients. The clinical and MRI findings in group 1 patients are summarized in Table 2. Two of 18 patients had normal MRI studies. A 4-month-old female patient with torticollis and seizures and a 6- month-old female patient with torticollis and vomiting had no abnormal MRI findings. Two patients had evidence of a mass on clinical examination; both had parotid hemangioma diagnosed by MRI. A 3- month-old male patient presented with torticollis and right upper extremity hemiparesis, which was initially diagnosed as Erb s palsy. However, significant worsening of right arm function was noted and MRI revealed an anterior cervical extradural mass in C6-C7; this was diagnosed and histologically confirmed as malignant peripheral nerve sheath tumor. Only 2 (11%) patients had positive orthopedic findings in this group. A 5- month-old female patient with Down s syndrome and torticollis underwent MRI to rule out cord compression. Magnetic Figure 1: Axial MRI of the neck of a 6-week-old infant shows fusiform swelling of intermediate signal density of the right sternomastoid. The clinical and imaging findings suggest fibromatosis colli. Figure 2: Coronal (A) and axial (B) MRIs of the neck of a 4-month-old infant show homogenous asymmetrical enlargement of the left sternocleidomastoid muscle and a slight torticollis to the left. 3 had corpus callosum hypoplasia, 2 had parenchymal white matter loss, and 1 had increased signal intensity in globus pallidus. The most common incidental findings were macrocrania or mild communicating hydrocephalus (2 patients) and inflammatory cells in mastoid (2 patients). Sixteen of 18 patients presenting with infantile torticollis and associated symptoms had positive MRI findings; the clinicopathological correlation was 89%. 1 2A 2B the treating physician. Of 40 patients in this group, 12 (30%) patients had sternocleidomastoid involvement on MRI; 7 patients had fibromatosis colli and 5 patients had sternocleidomastoid asymmetry (Figures 1 and 2). No patient had posterior fossa tumor or other significant pathologic findings. The mean age of these 12 patients was 7.5 months. The clinicopathological correlation was 30%. The most common bony abnormality MAY 2004 Volume 27 Number 5 511
4 was asymmetry of the posterolateral skull consistent with plagiocephaly, which was present in 14 (24%) patients in this series. Except in 1 patient with craniosynostosis, MRI was unable to differentiate between postural plagiocephaly and plagiocephaly due to craniosynostosis. Facial asymmetry was present in 9 (16%) patients. DISCUSSION With the imaging capabilities of MRI, it is possible to examine the spine and central nervous system anatomy with excellent resolution. This has led to a better understanding of the frequency and spectrum of findings that can be present as part of the evaluation for nonmuscular causes of torticollis. Magnetic resonance imaging is a sensitive and specific diagnostic tool, especially for detection of neurogenic causes of torticollis, as evident in the present series. However, errors in clinical decision-making after MRI for infantile torticollis may arise in one of three general areas: 1) the timing of MRI during the patient s clinical course, 2) matching the clinical indications to the optimum investigation, and 3) precise correlation of the abnormalities seen on MRI with the clinical symptoms. The majority of patients with congenital muscular torticollis (group 2) were referred for MRI to rule out posterior fossa tumor. Torticollis has been described as the initial sign of a posterior fossa tumor in several reports. 2,3,5,6,13,15,17,22 However, torticollis secondary to posterior fossa tumor is an acquired cause of torticollis, usually associated with symptoms and presenting in older age groups. Gupta et al 3 reported five patients with torticollis as the initial sign of posterior fossa tumor. Four of five patients had associated symptoms such as headache, nausea, vomiting, or positive neurologic signs. No patient had torticollis in the neonatal period. Ballock and Song 2 reported six children with torticollis and central nervous system lesions. All patients had abnormal neurologic examinations on initial presentation, and the Although sternocleidomastoid tumor of infancy and congenital muscular torticollis often are referred to as different entities, no consensus exists in the literature for distinguishing these two conditions. youngest patient in their series was 17 months old. Kiwak et al 13 reported three patients with syringomyelia and spinal cord tumor, with acquired torticollis as an early finding in each. All three patients had associated scoliosis or abnormal neurologic presentation. Boisen 15 reported three patients with infratentorial tumors who presented with torticollis; all three patients were adults. Marmor et al 17 reported a triad of photophobia, epiphora, and torticollis as initial manifestation of posterior fossa tumors and recommended that children with this triad undergo MRI for evaluation of the posterior fossa. Taboas-Perez and Rivera-Reyes 16 reported three children with torticollis and posterior fossa tumors; all had associated symptoms at presentation. No cases of posterior fossa tumor or other significant pathologic lesion were noted in group 2 patients in the present study. Based on our study and review of the literature, 2 when no sternocleidomastoid tightness or inflammatory process is noted in the head and neck on clinical examination, radiographs are normal, and ophthalmologic examination is negative, or when the initial neurologic examination is abnormal, only then should a child be referred to a neurologist. Magnetic resonance imaging can be obtained at this time. Magnetic resonance imaging is not recommended for an infant with torticollis without any associated symptoms. Wei et al 23 suggested a similar treatment algorithm and recommended that imaging studies be considered only if the torticollis does not resolve by 12 months in patients with congenital muscular torticollis. The other frequent indication for MRI in infantile torticollis is to evaluate a neck mass within the sternocleidomastoid muscle. Sternocleidomastoid tumor of infancy is a unique form of perinatal fibromatosis that results in the formation of a hard mass within the sternocleidomastoid muscle of the neonate. It has been referred to as fibromatosis colli, nodular fasciitis, or pseudotumor of infancy, and it is grouped within the spectrum of disorders collectively known as congenital muscular torticollis. 10,23-25 It is present in approximately 0.4% of live births, and approximately 90% of patients have good prognosis with conservative treatment usually by age 1 year. 4,7,10,25 In addition to torticollis, patients may present with lytic clavicular lesions, ipsilateral mandibular asymmetry, plagiocephaly, occipital condyle asymmetry, ipsilateral clavicle and shoulder elevation, facial deformities, and postural cervicothoracic scoliosis. 26,27 Ultrasound has been the procedure of choice for diagnosis; it is used to demonstrate the origin of the mass in sternocleidomastoid muscle and to exclude other conditions mimicking it. 28,29 If unexpected symptoms or physical findings develop, further evaluation with CT, MRI, or fine-needle aspiration biopsy is recommended. 29 Magnetic resonance imaging findings of fibromatosis colli have been described in the literature. 24,30,31 Ablin et al 30 described the MRI findings in a biopsyproven case of fibromatosis colli. The signal intensity of the mass on T2-weighted images was slightly less than on T1- weighted images, consistent with fibrous tissue within the muscle mass. They concluded that MRI was helpful in demonstrating signal characteristics of the mass, localizing the mass to within the sternocleidomastoid muscle, and demonstrating 512 ORTHOPEDICS
5 MRI EVALUATION OF INFANTILE TORTICOLLIS PARIKH ET AL Figure 3: Coronal MRI of an infant with a palpable mass within the right sternocleidomastoid muscle. The patient had a diagnosis of fibromatosis colli. When compared to the normal left sternocleidomastoid, heterogeneous signal and enlargement of the right sternocleidomastoid is noted. Similar findings have been described as compartment syndrome of sternocleidomastoid; however, these findings were not seen in other patients with fibromatosis colli. clear surrounding fascial planes with lack of associated lymphadenopathy, airway compression, vascular encasement, bone involvement, or intracranial extension associated with other neck masses. Jaber and Goldsmith 24 reported two cases with sternocleidomastoid tumor of infancy. Magnetic resonance imaging demonstrated diffuse isointense enlargement of the muscle in one patient and a focal hyperintense mass within the muscle in the other patient. The MRI appearance of these lesions often is variable and nonspecific. This is likely secondary to both the amount of collagen and degree of cellularity of the lesion. 31 Only one patient in the present series had a palpable mass within the muscle. The MRI findings in this patient were suggestive of fibromatosis colli (Figure 3). Although sternocleidomastoid tumor of infancy and congenital muscular torticollis often are referred to as different entities, no consensus exists in the literature for distinguishing these two conditions. It is unknown whether these two entities are distinct pathological conditions or whether they comprise a spectrum of the same muscular abnormality. 23 Porter and Blount 32 defined sternocleidomastoid tumor of infancy when patients were diagnosed between ages 2 and 4 weeks. Similarly, Wei et al 23 considered a diagnosis of pseudotumor of infancy before age 6 weeks, and a diagnosis of congenital muscular torticollis after age 6 weeks. However, similar to the study by Coventry and Harris, 33 we grouped these What is already known on this topic 3 two entities together as congenital muscular torticollis irrespective of the age at presentation. The etiology of congenital muscular torticollis remains a mystery. Davids et al 21 described the characteristic MRI findings in 10 patients with congenital muscular torticollis and proposed that this condition was a sequelae of an intrauterine or perinatal compartment syndrome. Nine of 10 patients were aged between 4 and 12 weeks at imaging, and 4 had a discretely palpable mass in the affected muscle at the time of study. In no case did MRI demonstrate a definite mass in the sternocleidomastoid muscle, but all 9 patients exhibited asymmetry and abnormal signal changes within the muscle changes that were similar to those described for leg and forearm compartment syndrome. In the older patient aged 5 years, MRI produced signals consistent with atrophy and fibrosis of the entire affected muscle, without inflammation or edema. In contrast, light and electron microscopy studies by Tang et al 34 found myoblasts in various stages of differentiation and degeneration in the sternocleidomastoid muscle. They concluded that the Muscular torticollis is the most common cause of infantile torticollis. Initial evaluation of infantile torticollis should include a history, physical examination with careful neurologic assessment, plain radiographs, and ophthalmologic consultation in a step-wise approach. What this article adds Patients with infantile torticollis who have seizures, developmental delay, hydrocephalus, or other neurologic findings should have MRI evaluation based on 89% positive findings in the patient group in our study. Magnetic resonance imaging is not recommended as a screening tool in infants with congenital muscular torticollis. Ultrasound should be considered before MRI for evaluation of patients with sternocleidomastoid tumor of infancy (fibromatosis colli) not responding to conventional treatment measures. Asymmetry of the posterolateral skull (plagiocephaly) was the most common bony abnormality present in 24% of patients. Compartment syndrome of sternocleidomastoid could not be established as an etiologic factor in congenital muscular torticollis. MAY 2004 Volume 27 Number 5 513
6 muscle produced images different from that of compartment syndrome and failed to show any edema and muscle infarction. In our series, of 40 patients in group 2 with a diagnosis of congenital muscular torticollis, sternocleidomastoid involvement on MRI was found in only 12 (30%) patients. Two reasons may be responsible for this inconsistent finding in our series: age and initial diagnosis. In contrast to all 9 patients reported by Davids et al, 21 with age 12 weeks, the mean age of our patients with congenital muscular torticollis (group 2) was 8 months. The MRI findings suggestive of compartment syndrome may be present only during the first few months after birth; with time, the inflammation and edema subsides, replaced by findings suggestive of atrophy and muscle fibrosis. Whyte et al 8 reported the MRI findings suggestive of sternocleidomastoid fibrosis in a case of congenital muscular torticollis, represented by hypointense signals within the affected sternocleidomastoid on T1- and T2-weighted images. Clinically, an infant with congenital muscular torticollis may appear normal at birth. Between age 2 and 3 weeks, a palpable mass can often be appreciated in the midsubstance of the sternocleidomastoid muscle. When not treated, subsequent contracture of the muscle causes the infant to hold its head in a characteristic position of forward flexion, ipsilateral lateral bend, and lateral rotation. The muscle can be felt as a tight band with restricted neck range of movement. It is a limitation of our retrospective study to apply strict criteria for diagnosis of congenital muscular torticollis. All patients in group 2 had an initial diagnosis of congenital muscular torticollis, but it may have included patients with other forms of congenital torticollis, such as congenital postural torticollis, ocular torticollis, or patients with sternocleidomastoid imbalance. The term sternocleidomastoid imbalance was introduced by Golden et al 35 to discern between a muscle mass or contracted sternocleidomastoid on one side, more identifiable with congenital muscular torticollis, versus an apparent sternocleidomastoid imbalance or weakness on the contralateral side. They characterized half of their patients with muscle imbalance as those with decreased ability to actively rotate or laterally flex their head to end range but near normal passive cervical range of motion. As many as 80 different causes of torticollis have been documented in the literature. 5 In one series of 53 patients with nonmuscular torticollis, the most frequent diagnosis was Klippel-Feil syndrome followed by ocular torticollis, obstetric palsies, and lesions involving the central nervous system. 2 It was not meaningful to calculate such prevalence rates in our study because of the selective patients undergoing MRI study. Klippel-Feil syndrome can be diagnosed clinically or on plain radiographs, and these patients may not need MRI unless an orthopedic procedure is contemplated or for evaluation of symptoms related to cord compromise or instability. 36 Similarly, patients with ophthalmic conditions may present with torticollis, nystagmus, defects in the visual field, or paralytic disorders of ocular movement. The most common ocular causes of torticollis in infancy are congenital paralytic squint due to superior oblique muscle palsy and congenital nystagmus. 11,37 These children typically present at approximately age 1 year, with a head tilt without rotation. 19 These conditions are diagnosed with formal ophthalmologic consultation and do not need MRI. This explains the absence of such patients in our study. The most common bony abnormality in the present series was asymmetry of the posterolateral skull consistent with plagiocephaly. Torticollis has been associated with 64%-84% of infants born with a normal head who develop positional plagiocephaly. 38,39 Also, torticollis may develop secondary to plagiocephaly, as the infant consistently lies on one side of the head, which may cause shortening or tightening of the sternocleidomastoid muscle. 40 Huang et al 39 recommended diagnostic criteria to distinguish between positional flattening of the parieto-occipital area and synostotic lambdoidal plagiocephaly. Despite the fact that the prognosis and consequently the treatment plan vary directly with the presence or absence of synostoses, clinical evaluation of plagiocephaly should include cephalometry, skull radiographs, or CT. 40,41 In infants aged 1 year with positional plagiocephaly, physiotherapy usually cures the torticollis with regression of the neck symptoms and improvement of skull contours. Active counterpositioning, assisted positioning, head bands, and orthotic helmets have been used to manage positional plagiocephaly. 38,42-44 However, craniosynostosis may require a corrective surgery. 45 Magnetic resonance imaging failed to differentiate between postural and synostotic plagiocephaly in all but one patient in the present series. CONCLUSION Careful clinical assessment in infants with congenital muscular torticollis precludes the necessity of MRI. We emphasize the importance of neurologic evaluation in all patients with infantile torticollis. Although MRI is a safe and effective imaging study, it should be used to confirm the information gathered from history and physical examination and should not be used for general screening or to rule out central nervous system lesions without prior orthopedic, ocular, otolarynologic, and neurologic evaluation. Magnetic resonance imaging should not be used for evaluation of sternocleidomastoid tumor of infancy; ultrasound is the imaging procedure of choice, if required. Magnetic resonance imaging could not differentiate between postural plagiocephaly and craniosynostosis. Routine MRI examination is not recommended for otherwise asymptomatic patients with infantile torticollis. The etiology of congenital muscular torticollis remains a mystery. Although it may represent a sequelae of intrauterine or peri- 514 ORTHOPEDICS
7 MRI EVALUATION OF INFANTILE TORTICOLLIS PARIKH ET AL natal compartment syndrome, other contributing factors may be associated with its development. Only in 30% of infants with congenital muscular torticollis did the MRI exhibit asymmetry or signal changes within sternocleidomastoid muscle; and further these MRI changes were not specific for the diagnosis of compartment syndrome of sternocleidomastoid. REFERENCES 1. Cheng JC, Au AW. Infantile torticollis: a review of 624 cases. J Pediatr Orthop. 1994; 14: Ballock RT, Song KM. The prevalence of non-muscular causes of torticollis in children. J Pediatr Orthop. 1996; 16: Gupta AK, Roy DR, Conlan ES, Crawford AH. Torticollis secondary to posterior fossa tumors. J Pediatr Orthop. 1996; 16: Morrison DL, MacEwen GD. Congenital muscular torticollis: observations regarding clinical findings, associated conditions, and results of treatment. J Pediatr Orthop. 1982; 2: Kiwak KJ. Establishing an etiology for torticollis. Postgrad Med. 1984; 75: Clark RN. Diagnosis and management of torticollis. Pediatr Ann. 1976; 5: Canale ST, Griffin DW, Hubbard CN. Congenital muscular torticollis. A long-term follow-up. J Bone Joint Surg Am. 1982; 64: Whyte AM, Lufkin RB, Bredenkamp J, Hoover L. Sternocleidomastoid fibrosis in congenital muscular torticollis: MR appearance. J Comput Assist Tomogr. 1989; 13: Sty JR, Wells RG, Schroeder BA. Congenital muscular torticollis: computed tomographic observations. Am J Dis Child. 1987; 141: Macdonald D. Sternomastoid tumour and muscular torticollis. J Bone Joint Surg Br. 1969; 51: Williams CR, O Flynn E, Clarke NM, Morris RJ. Torticollis secondary to ocular pathology. J Bone Joint Surg Br. 1996; 78: Saltzman CL, Hensinger RN, Blane CE, Phillips WA. Familial cervical dysplasia. J Bone Joint Surg Am. 1991; 73: Kiwak KJ, Deray MJ, Shields WD. Torticollis in three children with syringomyelia and spinal cord tumor. Neurology. 1983; 33: Raimondi AJ, Tomita T. Hydrocephalus and infratentorial tumors. Incidence, clinical picture, and treatment. J Neurosurg. 1981; 55: Boisen E. Torticollis caused by an infratentorial tumour: three cases. Br J Psychiatry. 1979; 134: Taboas-Perez RA, Rivera-Reyes L. Head tilt: a revisit to an old sign of posterior fossa tumors. Bol Asoc Med P R. 1984; 76: Marmor MA, Beauchamp GR, Maddox SF. Photophobia, epiphora, and torticollis: a masquerade syndrome. J Pediatr Ophthalmol Strabismus. 1990; 27: Visudhiphan P, Chiemchanya S, Somburanasin R, Dheandhanoo D. Torticollis as the presenting sign in cervical spine infection and tumor. Clin Pediatr (Phila). 1982; 21: Loder RT. The cervical spine. In: Morrissy RT, Weinstein SL, eds. Lovell and Winter s Pediatric Orthopaedics. 5th ed. Philadelphia, Pa: Lippincott Williams & Wilkins; 2001: Wirth CJ, Hagena FW, Wuelker N, Siebert WE. Biterminal tenotomy for the treatment of congenital muscular torticollis. Long-term results. J Bone Joint Surg Am. 1992; 74: Davids JR, Wenger DR, Mubarak SJ. Congenital muscular torticollis: sequela of intrauterine or perinatal compartment syndrome. J Pediatr Orthop. 1993; 13: Krauss JK, Seeger W, Jankovic J. Cervical dystonia associated with tumors of the posterior fossa. Mov Disord. 1997; 12: Wei JL, Schwartz KM, Weaver AL, Orvidas LJ. Pseudotumor of infancy and congenital muscular torticollis: 170 cases. Laryngoscope. 2001; 111: Jaber MR, Goldsmith AJ. Sternocleidomastoid tumor of infancy: two cases of an interesting entity. Int J Pediatr Otorhinolaryngol. 1999; 47: Thomsen JR, Koltai PJ. Sternomastoid tumor of infancy. Ann Otol Rhinol Laryngol. 1989; 98: Rondinella LJ, Tom LW. An unusual presentation of the sternocleidomastoid tumor of infancy. Otolaryngol Head Neck Surg. 1997; 117:S181-S Sartoris DJ, Mochizuki RM, Parker BR. Lytic clavicular lesions in fibromatosis colli. Skeletal Radiol. 1983; 10: Eich GF, Hoeffel JC, Tschappeler H, Gassner I, Willi UV. Fibrous tumours in children: imaging features of a heterogeneous group of disorders. Pediatr Radiol. 1998; 28: Cakmakci H, Kovanlikaya A. MRI of fibromatosis colli. Turk J Pediatr. 1999; 41: Ablin DS, Jain K, Howell L, West DC. Ultrasound and MR imaging of fibromatosis colli (sternomastoid tumor of infancy). Pediatr Radiol. 1998; 28: Snitzer EL, Fultz PJ, Asselin B. Magnetic resonance imaging appearance of fibromatosis colli. Magn Reson Imaging. 1997; 15: Porter SB, Blount BW. Pseudotumor of infancy and congenital muscular torticollis. Am Fam Physician. 1995; 52: Coventry MB, Harris LE. Congenital muscular torticollis in infancy; some observation regarding treatment. J Bone Joint Surg Am. 1959; 41: Tang S, Liu Z, Quan X, Qin J, Zhang D. Sternocleidomastoid pseudotumor of infants and congenital muscular torticollis: finestructure research. J Pediatr Orthop. 1998; 18: Golden KA, Beals SP, Littlefield TR, Pomatto JK. Sternocleidomastoid imbalance versus congenital muscular torticollis: their relationship to positional plagiocephaly. Cleft Palate Craniofac J. 1999; 36: Tachdjian MO. Disorders of the neck. In: Herring JA, ed. Tachdjian s Pediatric Orthopaedics. Philadelphia, Pa: WB Saunders Co; 2002: Bixenman WW. Diagnosis of superior oblique palsy. Journal of Clinical Neuro Ophthalmology. 1981; 1: Loveday BP, de Chalain TB. Active counterpositioning or orthotic device to treat positional plagiocephaly? J Craniofac Surg. 2001; 12: Huang MH, Gruss JS, Clarren SK, et al. The differential diagnosis of posterior plagiocephaly: true lambdoid synostosis versus positional molding. Plast Reconstr Surg. 1996; 98: Mulliken JB, Vander Woude DL, Hansen M, LaBrie RA, Scott RM. Analysis of posterior plagiocephaly: deformational versus synostotic. Plast Reconstr Surg. 1999; 103: Raco A, Raimondi AJ, De Ponte FS, et al. Congenital torticollis in association with craniosynostosis. Childs Nerv Syst. 1999; 15: Carson BS, Munoz D, Gross G, et al. An assistive device for the treatment of positional plagiocephaly. J Craniofac Surg. 2000; 11: Vles JS, Colla C, Weber JW, Beuls E, Wilmink J, Kingma H. Helmet versus nonhelmet treatment in nonsynostotic positional posterior plagiocephaly. J Craniofac Surg. 2000; 11: Bridges SJ, Chambers TL, Pople IK. Plagiocephaly and head binding. Arch Dis Child. 2002; 86: Imai K, Komune H, Toda C, et al. Cranial remodeling to treat craniosynostosis by gradual distraction using a new device. J Neurosurg. 2002; 96: MAY 2004 Volume 27 Number 5 515
Interesting Case Series. The Danger of Posterior Plagiocephaly
 Interesting Case Series The Danger of Posterior Plagiocephaly Susan Orra, BA, a,b Kashyap Komarraju Tadisina, BS, a Bahar Bassiri Gharb, MD, PhD, a Antonio Rampazzo, MD, PhD, a Gaby Doumit, MD, a and Francis
Interesting Case Series The Danger of Posterior Plagiocephaly Susan Orra, BA, a,b Kashyap Komarraju Tadisina, BS, a Bahar Bassiri Gharb, MD, PhD, a Antonio Rampazzo, MD, PhD, a Gaby Doumit, MD, a and Francis
Operative treatment of congenital torticollis
 Operative treatment of congenital torticollis J. S. Shim, H. P. Jang From Sungkyunkwan University School of Medicine, Seoul, Korea There were 47 patients with congenital muscular torticollis who underwent
Operative treatment of congenital torticollis J. S. Shim, H. P. Jang From Sungkyunkwan University School of Medicine, Seoul, Korea There were 47 patients with congenital muscular torticollis who underwent
Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head?
 Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head? S. David Moss, M.D. Phoenix Children's Hospital, Phoenix, Arizona Plagiocephaly
Nonsurgical, nonorthotic treatment of occipital plagiocephaly: what is the natural history of the misshapen neonatal head? S. David Moss, M.D. Phoenix Children's Hospital, Phoenix, Arizona Plagiocephaly
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2012; 36: 320-327 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2012.36.3.320 Annals of Rehabilitation Medicine Magnetic Resonance Imaging as a Determinant
Original Article Ann Rehabil Med 2012; 36: 320-327 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2012.36.3.320 Annals of Rehabilitation Medicine Magnetic Resonance Imaging as a Determinant
MEDICAL POLICY MEDICAL POLICY DETAILS POLICY STATEMENT POLICY GUIDELINES. Page: 1 of 5. Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.
 Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.32 Category Equipment/Supplies Effective Date 10/18/01 Revised Date 06/27/02, 07/24/03, 06/24/04,
Page: 1 of 5 MEDICAL POLICY MEDICAL POLICY DETAILS Medical Policy Title CRANIAL ORTHOTICS Policy Number 1.01.32 Category Equipment/Supplies Effective Date 10/18/01 Revised Date 06/27/02, 07/24/03, 06/24/04,
Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment
 Name of Policy: Dynamic Orthotic Cranioplasty (DOC) Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment Policy Grade: D Background: As a general rule, benefits are payable under
Name of Policy: Dynamic Orthotic Cranioplasty (DOC) Policy #: 008 Latest Review Date: May 2007 Category: Durable Medical Equipment Policy Grade: D Background: As a general rule, benefits are payable under
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2013;37(2):183-190 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.2.183 Annals of Rehabilitation Medicine The Cervical Range of Motion as a Factor
Original Article Ann Rehabil Med 2013;37(2):183-190 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.2.183 Annals of Rehabilitation Medicine The Cervical Range of Motion as a Factor
Prevention Diagnosis
 Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
South Korea c Department of Physical & Rehabilitation Medicine, Samsung Medical Center, Sungkyunkwan University, School of Medicine,
 Journal of Pediatric Surgery (2011) 46, 1526 1531 www.elsevier.com/locate/jpedsurg Clinical features and outcome of physiotherapy in early presenting congenital muscular torticollis with severe fibrosis
Journal of Pediatric Surgery (2011) 46, 1526 1531 www.elsevier.com/locate/jpedsurg Clinical features and outcome of physiotherapy in early presenting congenital muscular torticollis with severe fibrosis
Table 1: Helmet vs Conservative Treatment
 Table 1: Helmet vs Conservative Treatment Author (Year) Title Study Description Data Class, Quality, and Van Wijk et al (2014) Helmet Therapy in Infants with Positional Skull Deformation: Randomized Controlled
Table 1: Helmet vs Conservative Treatment Author (Year) Title Study Description Data Class, Quality, and Van Wijk et al (2014) Helmet Therapy in Infants with Positional Skull Deformation: Randomized Controlled
The Sonographic Correlation between The Sternocleidomastoid Muscle Thickness and the Prognosis of Congenital Muscular Torticollis 1
 J Korean Soc Radiol 2009;60:133-138 The Sonographic Correlation between The Sternocleidomastoid Muscle Thickness and the Prognosis of Congenital Muscular Torticollis 1 Daekeon Lim, M.D., Woocheol Kwon,
J Korean Soc Radiol 2009;60:133-138 The Sonographic Correlation between The Sternocleidomastoid Muscle Thickness and the Prognosis of Congenital Muscular Torticollis 1 Daekeon Lim, M.D., Woocheol Kwon,
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Craniosynostosis. Diagnosis and Treatment
 Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2015;39(1):18-24 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.1.18 Annals of Rehabilitation Medicine Factors That Affect the Rehabilitation Duration
Original Article Ann Rehabil Med 2015;39(1):18-24 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.1.18 Annals of Rehabilitation Medicine Factors That Affect the Rehabilitation Duration
(i) Family 1. The male proband (1.III-1) from European descent was referred at
 1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
1 Supplementary Note Clinical descriptions of families (i) Family 1. The male proband (1.III-1) from European descent was referred at age 14 because of scoliosis. He had normal development. Physical evaluation
Department of Neurosurgery. Differentiating Craniosynostosis from Positional Plagiocephaly
 Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Craniosynostosis and Plagiocephaly
 Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2
 Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Malformations of the cranio-cervical junction: basilar impression Gonzalo Bertullo 1, Viviana Cabrera 2 Abstract Cranio-cervical junction abnormalities are a rare combination of congenital or acquired
Case SCIWORA in patient with congenital block vertebra
 Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
THE EFFICACY OF MANIPULATIVE TREATMENT FOR STERNOMASTOID TUMOURS
 THE EFFICACY OF MANIPULATIVE TREATMENT FOR STERNOMASTOID TUMOURS Y. K. LEUNG, P. C. LEUNG From the Queen Elizabeth Hospital, Hong Kong Sixty-seven patients with sternomastoid tumours have been treated
THE EFFICACY OF MANIPULATIVE TREATMENT FOR STERNOMASTOID TUMOURS Y. K. LEUNG, P. C. LEUNG From the Queen Elizabeth Hospital, Hong Kong Sixty-seven patients with sternomastoid tumours have been treated
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy
 Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Predictive Model for Congenital Muscular Torticollis: Analysis of 1021 Infants With Sonography
 ORIGINAL ARTICLE Predictive Model for Congenital Muscular Torticollis: Analysis of 1021 Infants With Sonography Miao-Ming Chen, MD, Huan-Cheng Chang, MD, MBA, Chuan-Fa Hsieh, MS, Ming-Fang Yen, PhD, Tony
ORIGINAL ARTICLE Predictive Model for Congenital Muscular Torticollis: Analysis of 1021 Infants With Sonography Miao-Ming Chen, MD, Huan-Cheng Chang, MD, MBA, Chuan-Fa Hsieh, MS, Ming-Fang Yen, PhD, Tony
Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal suture
 IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
May have excessive movement in the unfused segment to compensate. Flexion extension better preserved than lateral bend or rotation
 IV CONGENITAL SPINE KLIPPEL FLAIL SYNDROME Prevalence 0.60% Mainly around upper 3 vertebrae [75%] Commonest: C2 3 Lower Cervical spine fusion may be associated with syndromes: Fetal alcohol syndrome Goldenhar
IV CONGENITAL SPINE KLIPPEL FLAIL SYNDROME Prevalence 0.60% Mainly around upper 3 vertebrae [75%] Commonest: C2 3 Lower Cervical spine fusion may be associated with syndromes: Fetal alcohol syndrome Goldenhar
Orthopedic Examination of the Spine, Pelvis, and Extremities, DX 611 Clinical Assessment Protocol
 Orthopedic Examination of the Spine, Pelvis, and Extremities, DX 611 Clinical Assessment Protocol James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic DIAGNOSIS 611 Orthopedics
Orthopedic Examination of the Spine, Pelvis, and Extremities, DX 611 Clinical Assessment Protocol James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic DIAGNOSIS 611 Orthopedics
Orthopedics. Orthopedics. Orthopedics Clinical assessment protocol. Life-Long Long Learners
 Orthopedic Examination of the Spine, Pelvis, and Extremities, DX 611 Clinical Assessment Protocol James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic DIAGNOSIS 611 This lecture
Orthopedic Examination of the Spine, Pelvis, and Extremities, DX 611 Clinical Assessment Protocol James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic DIAGNOSIS 611 This lecture
Interesting Case Series. Ganglion Cyst of the Peroneus Longus
 Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Screening for Torticollis and Plagiocephaly: The Role of the Pediatrician
 Loma Linda University TheScholarsRepository@LLU: Digital Archive of Research, Scholarship & Creative Works Loma Linda University Electronic Theses, Dissertations & Projects 6-2014 Screening for Torticollis
Loma Linda University TheScholarsRepository@LLU: Digital Archive of Research, Scholarship & Creative Works Loma Linda University Electronic Theses, Dissertations & Projects 6-2014 Screening for Torticollis
Original Article Radial club hand deformity The continuing challenges and controversies
 Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 30-34 Original Article Radial club hand deformity The continuing challenges and controversies Banskota AK 1, Bijukachhe B 2, Rajbhandary
Kathmandu University Medical Journal (2005) Vol. 3, No. 1, Issue 9, 30-34 Original Article Radial club hand deformity The continuing challenges and controversies Banskota AK 1, Bijukachhe B 2, Rajbhandary
Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial Plexus Injury
 Send Orders of Reprints at reprints@benthamscience.net 94 The Open Orthopaedics Journal, 2013, 7, 94-98 Open Access Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial
Send Orders of Reprints at reprints@benthamscience.net 94 The Open Orthopaedics Journal, 2013, 7, 94-98 Open Access Extended Long-Term (5 Years) Outcomes of Triangle Tilt Surgery in Obstetric Brachial
General appearance examination
 Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Yorkshire and Humber Neonatal ODN (South) Clinical Guideline
 Yorkshire and Humber Neonatal ODN (South) Clinical Guideline Title: Author: NEONATAL BRACHIAL PLEXUS INJURY Rebecca Musson Date written: January 2011, reviewed January 2016 Review date: January 2019 This
Yorkshire and Humber Neonatal ODN (South) Clinical Guideline Title: Author: NEONATAL BRACHIAL PLEXUS INJURY Rebecca Musson Date written: January 2011, reviewed January 2016 Review date: January 2019 This
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy
 Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses Corporate Medical Policy File name: Adjustable Cranial Orthoses for Positional Plagiocephaly and Craniosynostoses File code:
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Occipital plagiocephaly
 ritish Journal of Plastic Surgery (2000), 53, 367 377 9 2000 The ritish ssociation of Plastic Surgeons doi:10.1054/bjps.2000.3329 RITISH JOURNL OF [ ~ ] PLSTIC SURGERY Occipital plagiocephaly D. J. David
ritish Journal of Plastic Surgery (2000), 53, 367 377 9 2000 The ritish ssociation of Plastic Surgeons doi:10.1054/bjps.2000.3329 RITISH JOURNL OF [ ~ ] PLSTIC SURGERY Occipital plagiocephaly D. J. David
Department of Physical Medicine and Rehabilitation, Ajou University School of Medicine, Suwon , 1
 Original Article Ann Rehabil Med 2011; 35: 361-368 pissn: 2234-0645 eissn: 2234-0653 doi: 10.5535/arm.2011.35.3.361 Annals of Rehabilitation Medicine The Thickness of the Sternocleidomastoid Muscle as
Original Article Ann Rehabil Med 2011; 35: 361-368 pissn: 2234-0645 eissn: 2234-0653 doi: 10.5535/arm.2011.35.3.361 Annals of Rehabilitation Medicine The Thickness of the Sternocleidomastoid Muscle as
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic
 Acta Pædiatrica ISSN 0803 5253 REGULAR ARTICLE Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic BL Hutchison (bl.hutchison@auckland.ac.nz),
Acta Pædiatrica ISSN 0803 5253 REGULAR ARTICLE Characteristics, head shape measurements and developmental delay in 287 consecutive infants attending a plagiocephaly clinic BL Hutchison (bl.hutchison@auckland.ac.nz),
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip
 The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
The Efficacy of Pavlik Harness as a Treatment of Developmental Dislocation of the Hip Firas A. Suleiman, MD*, Fadi Al Rousan, MD*, Ahmad Almarzoq, MD *, Razi Altarawneh, MD*, Hidar Soudi, MD* ABSTRACT
Disclosures None. Common Neurosurgical Problems Seen in Office Encounters. Macrocephaly Low Back Pain Sacral Dimple Concussion Chiari Malformation
 Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
Common Neurosurgical Problems Seen in Office Encounters When to Manage, When to Refer Andrew Jea MD FAAP Professor and Chief of Pediatric Neurosurgery Riley Hospital for Children Indiana University School
NYEIS Version 4.3 (ICD) ICD - 10 Codes Available in NYEIS at time of version launch (9/23/2015)
 D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
D82.1 Di George's syndrome E63.9 Nutritional deficiency, unspecified E70.21 Tyrosinemia E70.29 Other disorders of tyrosine metabolism E70.30 Albinism, unspecified E70.5 Disorders of tryptophan metabolism
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
The Acute Calcific Prevertebral Tendinitis : Report of Two Cases
 The Acute Calcific Prevertebral Tendinitis : Report of Two Cases Asian Spine Journal Vol. 4, No. 2, pp 123~127, 2010 doi:10.4184/asj.2010.4.2.123 Dong-Eun Shin 1, Chang-Soo Ahn 2, Jung-Pil Choi 1 1 Department
The Acute Calcific Prevertebral Tendinitis : Report of Two Cases Asian Spine Journal Vol. 4, No. 2, pp 123~127, 2010 doi:10.4184/asj.2010.4.2.123 Dong-Eun Shin 1, Chang-Soo Ahn 2, Jung-Pil Choi 1 1 Department
Pediatric Radiology Update
 Pediatric Radiology Update Douglas Rivard, DO Vice Chairman, Radiology Dept Children s Mercy Hospital Asst Professor of Radiology University of Missouri-Kansas City Objectives Review radiation biology
Pediatric Radiology Update Douglas Rivard, DO Vice Chairman, Radiology Dept Children s Mercy Hospital Asst Professor of Radiology University of Missouri-Kansas City Objectives Review radiation biology
INFANTILE EXOTROPIA. Lionel Kowal
 INFANTILE EXOTROPIA Lionel Kowal INFANTILE XT Usage often imprecise Variation in definitions number of investigators? onset day 1 of life? constant / intermittent Any / large angle? Associated systemic
INFANTILE EXOTROPIA Lionel Kowal INFANTILE XT Usage often imprecise Variation in definitions number of investigators? onset day 1 of life? constant / intermittent Any / large angle? Associated systemic
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound
 Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Prenatal Prediction of The Neurologically Impaired Neonate By Ultrasound Robert H. Debbs, D.O.,F.A.C.O.O.G. Professor of OB-GYN Perelman School of Medicine, University of Pennsylvania Director, Pennsylvania
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012
 Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
Neonatal Hypotonia Guideline Prepared by Dan Birnbaum MD August 27, 2012 Hypotonia: reduced tension or resistance to range of motion Localization can be central (brain), peripheral (spinal cord, nerve,
syndrome Turned head adducted hip truncal curvature
 Archives of Disease in Childhood 1994; 70: 515-519 515 Department of Orthopaedics, Kinki University School of Medicine, Osaka, Japan Chiaki Hamanishi Seisuke Tanaka Correspondence to: Dr Chiaki Hamanishi,
Archives of Disease in Childhood 1994; 70: 515-519 515 Department of Orthopaedics, Kinki University School of Medicine, Osaka, Japan Chiaki Hamanishi Seisuke Tanaka Correspondence to: Dr Chiaki Hamanishi,
Chiari malformations. A fact sheet for patients and carers
 A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip
 Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Clinical Practice & Referral Guideline - Developmental Dysplasia of the Hip *This guideline was developed from the American Academy of Pediatrics Clinical Practice Guideline: Early Detection of Developmental
Triangle Tilt Surgery: Effect on Coracohumeral Distance and External Rotation of the Glenohumeral Joint
 Triangle Tilt Surgery: Effect on Coracohumeral Distance and External Rotation of the Glenohumeral Joint Rahul K. Nath, MD, and Faiz Mahmooduddin, MD Texas Nerve and Paralysis Institute, 6400 Fannin St,
Triangle Tilt Surgery: Effect on Coracohumeral Distance and External Rotation of the Glenohumeral Joint Rahul K. Nath, MD, and Faiz Mahmooduddin, MD Texas Nerve and Paralysis Institute, 6400 Fannin St,
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
DIAGNOSTIC VIDEOFLUOROSCOPY IMPRESSIONS and BIOMECHANICS REPORT
 P.O. Box 6743 New Albany, IN 47151-6743 (812) 945-5515 (812) 945-5632 Fax WWW.KMX.CC DIAGNOSTIC VIDEOFLUOROSCOPY IMPRESSIONS and BIOMECHANICS REPORT Patient Name: Lubna Ibriham Date of Digitization and
P.O. Box 6743 New Albany, IN 47151-6743 (812) 945-5515 (812) 945-5632 Fax WWW.KMX.CC DIAGNOSTIC VIDEOFLUOROSCOPY IMPRESSIONS and BIOMECHANICS REPORT Patient Name: Lubna Ibriham Date of Digitization and
The prevalence of deformational plagiocephaly PEDIATRIC/CRANIOFACIAL
 PEDIATRIC/CRANIOFACIAL Effectiveness of Conservative Therapy and Helmet Therapy for Positional Cranial Deformation Jordan P. Steinberg, M.D., Ph.D. Roshni Rawlani, B.A. Laura S. Humphries, M.D. Vinay Rawlani,
PEDIATRIC/CRANIOFACIAL Effectiveness of Conservative Therapy and Helmet Therapy for Positional Cranial Deformation Jordan P. Steinberg, M.D., Ph.D. Roshni Rawlani, B.A. Laura S. Humphries, M.D. Vinay Rawlani,
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Prevalance of neural axis abnormalities in patients with infantile idiopathic scoliosis
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 12-1-2002 Prevalance of neural axis abnormalities in patients with infantile idiopathic scoliosis Matthew B. Dobbs
Washington University School of Medicine Digital Commons@Becker Open Access Publications 12-1-2002 Prevalance of neural axis abnormalities in patients with infantile idiopathic scoliosis Matthew B. Dobbs
Normal fetal face and neck
 Normal fetal face and neck Maria A. Calvo-Garcia, MD. Associate Professor of Radiology Cincinnati Children s Hospital Medical Center Cincinnati, Ohio Disclosure I have no disclosures Goals & objectives
Normal fetal face and neck Maria A. Calvo-Garcia, MD. Associate Professor of Radiology Cincinnati Children s Hospital Medical Center Cincinnati, Ohio Disclosure I have no disclosures Goals & objectives
Congenital Anomaly of the Atlas Misdiagnosed as Posterior Arch Fracture of the Atlas and Atlantoaxial Subluxation
 Case Report Clinics in Orthopedic Surgery 2014;6:96-100 http://dx.doi.org/10.4055/cios.2014.6.1.96 Congenital Anomaly of the Atlas Misdiagnosed as Posterior Arch Fracture of the Atlas and Atlantoaxial
Case Report Clinics in Orthopedic Surgery 2014;6:96-100 http://dx.doi.org/10.4055/cios.2014.6.1.96 Congenital Anomaly of the Atlas Misdiagnosed as Posterior Arch Fracture of the Atlas and Atlantoaxial
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
Clinical Guidance. Neonatal Manual Chapter 10: Musculoskeletal problems
 Clinical Guidance Neonatal Manual Chapter 10: Musculoskeletal problems Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter
Clinical Guidance Neonatal Manual Chapter 10: Musculoskeletal problems Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter
High-frequency ultrasound confirmation of positional plagiocephaly
 J Neurosurg (5 Suppl Pediatrics) 105:413 417, 2006 High-frequency ultrasound confirmation of positional plagiocephaly JAN REGELSBERGER, M.D., GÜNTER DELLING, M.D., MICHAEL TSOKOS, M.D., KNUTH HELMKE, M.D.,
J Neurosurg (5 Suppl Pediatrics) 105:413 417, 2006 High-frequency ultrasound confirmation of positional plagiocephaly JAN REGELSBERGER, M.D., GÜNTER DELLING, M.D., MICHAEL TSOKOS, M.D., KNUTH HELMKE, M.D.,
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University
 The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
Adult Patients with Congenital Muscular Torticollis Treated with Bipolar Release : Report of 31 Cases
 Clinical Article J Korean Neurosurg Soc 60 (1) : 82-88, 2017 https://doi.org/10.3340/jkns.2016.0303.018 pissn 2005-3711 eissn 1598-7876 Adult Patients with Congenital Muscular Torticollis Treated with
Clinical Article J Korean Neurosurg Soc 60 (1) : 82-88, 2017 https://doi.org/10.3340/jkns.2016.0303.018 pissn 2005-3711 eissn 1598-7876 Adult Patients with Congenital Muscular Torticollis Treated with
Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis:
 Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis: Watchful Waiting May Not Be the Best Option for Evaluating Abnormal Head Shape in Infants April, 2016
Effective Treatment of Craniosynostosis and Deformational Plagiocephaly Improves with Early Diagnosis: Watchful Waiting May Not Be the Best Option for Evaluating Abnormal Head Shape in Infants April, 2016
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Neurofibromatosis type 1 (NF-1), or peripheral neurofibromatosis,
 SPINE Volume 38, Number 18, pp 1595 1601 2013, Lippincott Williams & Wilkins SURGERY Does the Presence of Dystrophic Features in Patients With Type 1 Neurofibromatosis and Spinal Deformities Increase the
SPINE Volume 38, Number 18, pp 1595 1601 2013, Lippincott Williams & Wilkins SURGERY Does the Presence of Dystrophic Features in Patients With Type 1 Neurofibromatosis and Spinal Deformities Increase the
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME
 REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME - Case report - TARIQ AL ZAHRANI * Klippel-Feil syndrome (KFS) was first described by Maurice Klippel and Andre Feil in 1912 in a patient with
REVERSE LMA INSERTION IN A NEONATE WITH KLIPPEL-FEIL SYNDROME - Case report - TARIQ AL ZAHRANI * Klippel-Feil syndrome (KFS) was first described by Maurice Klippel and Andre Feil in 1912 in a patient with
Chapter 2 Diagnostic Algorithms. 4 Traumatic Neck Pain Algorithm
 Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
Chapter 2 Diagnostic Algorithms 4 Traumatic Neck Pain Algorithm Patient presents with a traumatic onset of neck pain. In general, radiographs should be ordered with a history of recent, significant trauma.
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Elastofibroma dorsi: 8 case reports and a literature review
 DOI 10.1007/s10195-008-0102-7 BRIEF COMMUNICATION Elastofibroma dorsi: 8 case reports and a literature review F. Muratori M. Esposito F. Rosa F. Liuzza N. Magarelli B. Rossi H.M. Folath F. Pacelli G. Maccauro
DOI 10.1007/s10195-008-0102-7 BRIEF COMMUNICATION Elastofibroma dorsi: 8 case reports and a literature review F. Muratori M. Esposito F. Rosa F. Liuzza N. Magarelli B. Rossi H.M. Folath F. Pacelli G. Maccauro
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
 Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
DOES ALTERED BIOMECHANICS CAUSE BONE MARROW EDEMA?
 DOES ALTERED BIOMECHANICS CAUSE BONE MARROW EDEMA? Alicia M. Yochum RN, DC, DACBR, RMSK DOES ALTERED BIOMECHANICS CAUSE BONE MARROW EDEMA? Mark E. Schweitzer, MD and Lawrence M. White MD Department of
DOES ALTERED BIOMECHANICS CAUSE BONE MARROW EDEMA? Alicia M. Yochum RN, DC, DACBR, RMSK DOES ALTERED BIOMECHANICS CAUSE BONE MARROW EDEMA? Mark E. Schweitzer, MD and Lawrence M. White MD Department of
Clinical Guide. Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses
 Clinical Guide Orthotic Management of Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses STARband Clinical Guide By Dulcey Lima, CO, OTR/L Introduction The number of skull deformities
Clinical Guide Orthotic Management of Pediatric Cranial Deformities using STAR Cranial Remolding Orthoses STARband Clinical Guide By Dulcey Lima, CO, OTR/L Introduction The number of skull deformities
Brain Imaging. Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress
 Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Advanced Animal Imaging Ryan Harrell BS, BS, CNMT
 Advanced Animal Imaging Ryan Harrell BS, BS, CNMT It is a specialized form of x -ray that helps veterinarians determine damage to th e spinal cord. A myelogram can help determine if there is a serious
Advanced Animal Imaging Ryan Harrell BS, BS, CNMT It is a specialized form of x -ray that helps veterinarians determine damage to th e spinal cord. A myelogram can help determine if there is a serious
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
CASE STUDY. Objective: To describe the chiropractic care of an infant with congenital muscular torticollis and plagiocephaly.
 CASE STUDY Improvement in, Plagiocephaly & Breastfeeding Issues in an Infant Following Subluxation Based Chiropractic Care: A Case Study Sian Williams, D.C. 1 Joel Alcantara, D.C. 2 Abstract Objective:
CASE STUDY Improvement in, Plagiocephaly & Breastfeeding Issues in an Infant Following Subluxation Based Chiropractic Care: A Case Study Sian Williams, D.C. 1 Joel Alcantara, D.C. 2 Abstract Objective:
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Normal Value of Skull Base Angle. Using the Modified Magnetic Resonance Imaging Technique in Thai Population
 Open Access Journal of Oral Health and Craniofacial Science Research Article Normal Value of Skull Base Angle ISSN 2573-6191 Using the Modified Magnetic Resonance Imaging Technique in Thai Population Siriporn
Open Access Journal of Oral Health and Craniofacial Science Research Article Normal Value of Skull Base Angle ISSN 2573-6191 Using the Modified Magnetic Resonance Imaging Technique in Thai Population Siriporn
