Exposure of Primary Orbital Implants in Postenucleation Retinoblastoma Patients
|
|
|
- Lisa Norris
- 6 years ago
- Views:
Transcription
1 Exposure of Primary Orbital Implants in Postenucleation Retinoblastoma Patients Vickie Lee, FRCOphth, 1 Ian Subak-Sharpe, MBBS, 1 John L. Hungerford, FRCS, FRCOphth, 1 Nigel P. Davies, FRCOphth, 1 Sanjay Logani, MD 2 Purpose: To determine significant factors influencing the exposure of primary orbital implants in patients with retinoblastoma. Design: Retrospective noncomparative case series. Participants: One hundred nine consecutive patients (110 sockets) who had undergone enucleation for retinoblastoma from January 1993 to December Methods: Two patients with recurrence of orbital retinoblastoma were excluded from further analysis, leaving 107 patients (108 sockets). The parameters analyzed included the patient s age; gender; ocular diagnosis; surgeon; type, covering, and size of the implant; the use of chemotherapy or radiotherapy; and the timing of these treatments in relation to enucleation. Study patients were divided into two main groups: the treated group patients who had undergone adjuvant external beam radiotherapy or chemotherapy, and the untreated group patients had undergone enucleation with or without cryotherapy, laser thermotherapy, or brachytherapy to the index or fellow eye. The following additional parameters were noted in the patients with exposed implants: time to exposure from date of enucleation and treatment of exposure. Main Outcome Measure: Exposure of orbital implants. Results: There were two exposures caused by orbital recurrence of retinoblastoma. The rate of nontumor recurrence exposure was 28% (30 of 108). The median time to exposure was 136 days (range, days). There were 18 exposures (35%,18 of 51) in the treated group, with a 34% exposure rate (13 of 38) in the chemotherapy group. The exposure rate was 21% (12 of 57) in the untreated group. The rates of exposure according to implant were: Vicryl mesh wrapped hydroxyapatite (2 of 18, 11%), Medpor (8 of 13, 53%), plain polymethylmethacrylate (PMMA) (4 of 50, 8%), Mersilene-wrapped PMMA (9 of 17, 53%) and Castroviejo (7 of 10, 70%). Eight of the exposures (27%) were managed conservatively; the remainder required surgical repair. Conclusions: Results suggested that implant type and covering (P 0.000) had a highly significant effect on the rate of exposure in postenucleation retinoblastoma patients. There was no statistical evidence that age, gender, ocular diagnosis, surgeon, size of the implant, or radiotherapy had an effect on implant exposure. There was an increased rate of exposure in the chemotherapy group, although this did not achieve statistical significance (P 0.058), but a detrimental effect could not be excluded. Ophthalmology 2000;107: by the American Academy of Ophthalmology. The goal of enucleation of an eye with retinoblastoma and insertion of a primary orbital implant is to remove the diseased globe, to stop extraocular spread, and to provide acceptable cosmesis. Clinical management of retinoblastoma is changing with the advent of new integrated implants and the increasing use of chemotherapy. 1 4 We have noted a significant number of exposures of primary orbital implants Originally received: November 8, Accepted: January 13, Manuscript no Ocular Oncology Service, St. Bartholomew s Hospital & Moorfields Eye Hospital, London, England. 2 Department of Ophthalmology, University of Southern California/Doheny Eye Institute, Los Angeles, California. Presented in part at the annual meeting of the American Academy of Ophthalmology, New Orleans, Louisiana, November The authors have no financial or proprietary interest in any of the materials used in this study. Reprint requests to Mr. J. L. Hungerford, FRCS, Ocular Oncology Service, St. Bartholomew s Hospital, West Smithfield, London England, EC1A7BE. in postenucleation retinoblastoma patients. This study attempts to identify any causes of this phenomenon during this period of transition. Methods The Ocular Oncology Service is the major tertiary referral center for retinoblastoma in England. One hundred nine records (110 sockets) of consecutive patients who had undergone enucleation for retinoblastoma from January 1993 to December 1997 with a minimum of 3 months follow-up were available for review. Before January 1993, chemotherapy had usually been reserved for advanced intraocular 1 and extraocular disease; after this date, chemotherapy became gradually more widely used as a first-line treatment for intraocular disease. Protocols of Patient Follow-Up When the patients underwent external beam radiotherapy, they were followed up with an examination under anesthesia 6 to 8 weeks after the initial radiotherapy, then every three months until by the American Academy of Ophthalmology ISSN /00/$ see front matter Published by Elsevier Science Inc. PII S (00)
2 Lee et al Exposure of Orbital Implants in Retinoblastoma Patients the age of 2, and then every four months from the age of 2 to 4. After the age of 4, they would usually be examined awake in the clinic. Patients undergoing chemotherapy had examinations done under anesthesia after every two cycles of chemotherapy until the end of the treatment regimen, when they would proceed with the follow-up arrangements according to age, as detailed previously. If a patient had undergone treatment for a relapse or new tumor, an examination with the patient under anesthesia would be arranged 1 month after the treatment. Treatment for Retinoblastoma Enucleation was undertaken as a primary treatment if there was anterior segment involvement by tumor or if there was extensive vitreous disease at presentation and after the failure of conservative treatment. Other treatment modalities included cryotherapy, thermotherapy, brachytherapy, and external beam radiotherapy (using the whole eye or a lens-sparing technique). Chemotherapy was used as first-line treatment for intraocular disease since January The first-line regimen was JOE (consisting of vincristine, etoposide, and carboplatin), described in an earlier publication. 1 After January 1993, most patients with bilateral retinoblastoma had chemotherapy initiated within days of the enucleation of the fellow eye. They normally underwent six to eight courses of chemotherapy at 3-week intervals to allow for the recovery of the platelet count between the courses. Chemotherapy was also begun after a report of adverse histologic findings in the enucleation specimen. This included extension of the tumor beyond the cut end of the optic nerve, deep choroidal invasion, or extrascleral extension. These patients usually underwent four courses of adjuvant JOE chemotherapy. Second-line chemotherapy was initiated for a variety of indications the most common being vitreous relapse in an eye after the patient had already undergone the JOE regimen earlier in the treatment. Treatment Undertaken for Exposure Conservative treatment consisted of topical antibiotics and modification of the prosthesis, generally with increased vaulting of the posterior surface. Resuturing of conjunctival dehiscence: the wound was revised by mobilizing all anterior adhesions to the exposed implant and resuturing with generous closure of Tenon s capsule and the conjunctiva in two separate layers. Implant exchange: The exposed implant was replaced with a buried nonintegrated plain polymethylmethacrylate (PMMA) sphere with no rectus attachments. Removal of implant: An implant was replaced only in cases in which there was significant fibrosis causing contracture or pre-existing infection, causing a high risk of exposure in the new implant, or when there had been a history of recurrent implant exposures. Excision of suture granulomas: suture granulomas were excised because they caused poor fitting of the prosthesis and the wound resutured. Parameters. The parameters included the patient s age at enucleation, ocular diagnosis (unilateral or bilateral, sporadic, or familial), type (Castroviejo, Medpor, hydroxyapatite, or PMMA) and covering of the implant (Mersilene mesh, Vicryl mesh, or none), size of the implant, the surgeon, use of chemotherapy or radiotherapy, and timing of these treatments in relation to enucleation. In the group of patients with exposed implants, the following were noted: time to first signs of exposure from date of enucleation, any cause for exposure, and treatment of exposure. The sockets were divided into two main groups. The first group consisted of untreated sockets (these included patients who had previously undergone cryotherapy, thermotherapy, or brachytherapy (it was calculated that orbital tissue receives 0 to 200 cgy in a properly shielded iodine plaque so effects of orbital radiation from brachytherapy should be minimal.) 9 ; and those who had orbital implant exposure develop before their chemotherapy or radiotherapy (because these treatments could not have been a factor influencing exposure). The second group consisted of treated sockets: patients who had undergone chemotherapy and/or received 4000 to 5000 cgy in external beam radiotherapy before or at the time of exposure. Because we were specifically concerned about the effects of chemotherapy, we also analyzed our results with regard to a chemotherapy sockets group within this second set of patients. Statistical Methods The outcome was defined as exposed or not exposed. All data were described as the median and range. The chi-squared test or the Fisher s exact test was used for categorical data. Quantitative data such as age were analyzed by use of a rank sum test. P 0.05 was considered significant. Factors found to be significant on univariate analysis were entered into a linear logistic regression. Enucleation Technique All the enucleations were performed by surgeons in the Ocular Oncology Service and all used the technique detailed later, which had been consistent over this period. The surgery was performed with the patient under general anesthesia. We first made a 360- degree peritomy at the limbus. The Tenon s fascia was divided using blunt dissection in all four quadrants to isolate the rectus muscles, which were then hooked and tagged with 5/0 catgut sutures before they were cauterized and cut near to the insertion leaving a 1-mm stump. The stump was then anchored with a 4/0 silk suture on a cutting needle, avoiding penetration of the globe. The oblique muscles were hooked, cauterized, and then cut. The silk sutures from the stumps of the four recti were then gathered and twisted together and clipped by an artery forceps to allow even distribution of tension on the globe. The globe was gently maneuvered out of the socket to allow the insertion of a snare, which was introduced as posteriorly as possible into the orbit to obtain a good length of optic nerve. The snare was tightened to cut the nerve and the globe was removed. The socket was firmly compressed with wet gauze and digital pressure for 5 to 10 minutes for hemostasis. All implants were placed as far posteriorly as possible in the muscle cone. This was facilitated by the use of a strip of plastic drape as a tubular sheath for the introduction of the implant to prevent dragging of the Tenon s capsule. With implants to which the recti could be sutured, the muscle attachments were anteriorized so that thick and more viable layers of Tenon s capsule and conjunctiva could be meticulously closed in two separate layers. We generally put in the largest implant (84% of the implants were 16 mm or more) over the conjunctiva, and the Tenon s could be closed adequately to avoid replacement of the implant with orbital growth. Plain PMMA sphere (baseball implant): The rectus muscles were not attached to this implant. Mersilene-wrapped PMMA sphere: The recti were advanced 3 to 5 mm from the apex of the implant and sutured onto the mesh. Castroviejo implant: The recti were sutured onto the anterior hapten. Vicryl mesh wrapped hydroxyapatite: The implant was left spherical and not modified. The recti were attached in an anteriorized position described earlier. None of our patients have undergone pegging of their hydroxyapatite implants. Medpor (Porex Surgical Inc, Georgia): Four small grooves were made at the apex of the implant with a Bard-Parker blade to allow for the suturing of the recti directly onto the implant. No covering was used with this implant, as recommended by the manufacturer. 941
3 Implant Ophthalmology Volume 107, Number 5, May 2000 Table 1. Types of Implants and Exposure Rates Treated Chemotherapy Untreated Unexposed Exposed Unexposed Exposed Unexposed Exposed Rate of Implant Exposure Odds Ratio for Exposure Compared with PMMA Castroviejo %(7/10) 20.7 (P 0.001) Medpor %(8/13) 12.0 (P 0.003) Baseball % (4/50) Mersilene/baseball %(9/17) 16.0 (P 0.00) Hydroxyapatite/Vicryl mesh %(2/18) 1.10 (P 0.93) Total % (30/108) PMMA polymethylmethacrylate. A conformer was placed between the lids and the bulbar conjunctiva, and a firm pressure bandage was applied overnight. The patient was normally reviewed in clinic on the first postoperative day and 3 weeks after surgery to evaluate the wound and histologic findings of the enucleated specimen. The patient was referred to an ocularist 4 to 6 weeks after enucleation, when measurements were taken for a permanent prosthesis. A temporary prosthesis was supplied in the interim. None of our patients in this series has had peg placement of their Medpor or hydroxyapatite implants. Results One hundred nine records were reviewed (110 sockets). There were 55 males and 54 females. There were 48 right eyes and 62 left eyes. The median age at diagnosis was 19.0 months (range, birth 136 months). The median age at enucleation was 24.0 months (range, months). The frequency of various orbital implants and their sizes, ocular diagnosis, and gender with respect to exposure rate are shown in Tables 1 to 4. The median follow-up was 21.6 months (range, months) after enucleation. Patient Treatment The two patients (one male and female) with orbital retinoblastoma causing secondary exposure of the implants were excluded from further statistical analysis. There were 50 patients (51 sockets) in the treated group. Of these, 13 patients (14 sockets) underwent enucleation with adjuvant chemotherapy and external beam radiotherapy, 23 (24 sockets) had only adjuvant chemotherapy, and 12 (13 sockets) had only adjuvant radiotherapy. There were 57 patients (57 sockets) in the untreated group. There were three patients (three eyes) in the untreated group who had undergone plaque brachytherapy, whereas in the treated group seven patients (eight eyes) had undergone plaque brachytherapy. Rates of Exposure in Treated and Untreated Sockets A total of 30 patients (30 sockets, 28%) had exposure of their orbital implants. There were 18 females and 12 males. Twelve (40%) patients had symptoms of excessive discharge from the socket. There was a 35% (18 of 51) exposure rate in the treated group (with 13 of 38 [34%] exposures in the chemotherapy group). There was a 20% (12 of 57) exposure rate in the untreated group. Timing of Exposure In the untreated socket group, the median time from enucleation to exposure was 153 days (range, days). In the treated socket group, the median time was 118 days (range, days). Two patients in each group had implant exposure in the first 30 days after surgery. Eighty seven percent of all exposures (26 of 30) occurred in the first year after enucleation. Management of Exposed Implant In the untreated socket group, two resolved with conservative management, six were resutured, and four patients required implant exchange. In the treated socket group, four resolved with conservative management, four were resutured, and 10 required eventual implant removal. Two patients with conjunctival thinning but no actual implant exposure underwent removal of the original implant and replacement with a hydroxyapatite implant because of problems of fitting a prosthetic eye. Five of the seven exposed Castroviejo implants needed to be removed. Three of the exposed plain PMMA implants were managed conservatively, and one was removed. Four of the Mersilene-wrapped PMMA implants were resutured, four were removed, and one exposure resolved after conservative treatment. Both hydroxyapatite implants were resutured. Of the Medpor implants, four were resutured, two were removed, and two were exchanged. Table 2. Exposure of Different Sizes of Implant Treated Chemotherapy Untreated Implant Size (mm) Unexposed Exposed Unexposed Exposed Unexposed Exposed Castroviejo (one size) Not recorded
4 Lee et al Exposure of Orbital Implants in Retinoblastoma Patients Table 3. Implant Exposure According to Diagnosis Diagnosis Total Not Exposed Exposed Unilateral sporadic retinoblastoma Unilateral familial retinoblastoma Bilateral sporadic retinoblastoma Bilateral familial retinoblastoma Factors Influencing the Rate of Exposure Results suggested that implant type and covering affected exposure rate (P 0.001), but age at enucleation, sex, diagnosis, surgeon, implant size, and radiotherapy appeared not to have an effect on implant exposure. There was an increased rate of exposure (34%) in the chemotherapy group compared with that (21%) in the untreated group. This did not reach statistical significance on multivariate analysis (P 0.058). Discussion As far as we are aware, this is the largest study examining the rate of exposure of primary implants in retinoblastoma patients. Enucleation is often the definitive treatment of large unilateral retinoblastomas, the worse eye in bilateral disease, and relapsed eyes after failure of other treatment modalities. The aim of insertion of an orbital implant is to replace lost orbital volume. This improves cosmesis and prosthesis motility. In the Ocular Oncology Unit at St. Bartholomew s, our practice has evolved with the increasing choice of different implants and covering. We have consistently avoided using donor sclera, taking into account the United Kingdom Health Service Guidelines. 5 Current management of retinoblastoma involves a multimodal approach incorporating enucleation, cryotherapy, laser thermotherapy, plaque brachytherapy, external beam radiotherapy, and chemotherapy. Survival rates are in excess of 90%, but the burden of coping with permanent visual and systemic morbidity often remains, especially in those with bilateral and/or familial disease. Previously, chemotherapy had been used only in the treatment of relapse after radiotherapy or extraocular extension of the disease, but in recent years, chemotherapy has been widely used with other modalities in the treatment of intraocular disease. 6,7 This has decreased the risk of cosmetic and functional deformities associated with radiation therapy, but the long-term effects have not yet been determined. We were concerned whether the new therapeutic approach of different implants and increasing use of chemotherapy may have an effect on the rate of exposure. Type and Covering of Orbital Implant Results from this study strongly suggest that the main factors influencing exposure are the type and covering of the implant. The search for an ideal orbital implant has evolved over the years. The anophthalmic orbit is physiologically and anatomically different, with decreased metabolic activity and vascularity as demonstrated by thermography, 8 and the tissues undergo trophic changes. Orbital implants have been shown to be beneficial to orbital growth 9 in addition to replacing the volume of the enucleated eye and promoting prosthesis motility. Both hydroxyapatite and plain PMMA implants appear to have lower exposure rates in the pediatric orbit, whereas Medpor, Mersilene-wrapped PMMA, and Castroviejo implants have a greater than 50% exposure rate in our study. The hydroxyapatite implant offers the option of drilling and peg placement for better prosthesis mobility at a later stage and has become the implant of choice in many centers. We have been using the baseball implant for many years with excellent results, as have other clinicians using this implant. Shields et al 10 reported no complications in a series of more than 1000; others noted extrusion rates of 4%. 11 However, it is interesting that wrapping the same implant in Mersilene mesh to allow attachment of the recti causes a much higher rate of exposure. This may have resulted from the rough surface of the Mersilene mesh causing mechanical irritation and subsequent exposure. The Castroviejo implant also had unfavorable results in our series. It is interesting to speculate why high-density porous polyethylene or Medpor, with a long successful history in facial reconstructive procedures 12 and with excellent results reported in adult enucleations, 2 should have such a high rate of exposure in the pediatric retinoblastoma orbit. This is particularly marked in the chemotherapy socket group, with exposures of 86% (5 of 6). Our experience is similar that of Karcioglu and coworkers, 13 who also found this unwrapped implant to have a high rate of exposure (21.6%) in a series of 34 retinoblastoma patients. Our results with Vicryl mesh wrapped hydroxyapatite have been encouraging, although the numbers included in this study are still relatively small. This implant of inorganic salt, first described by Perry, 3 is our current porous implant of choice. Vicryl mesh (polyglactin 910) is an absorbable synthetic copolymer, which is nonantigenic, nonpyogenic, inexpensive, and elicits only a mild tissue reaction clinically. 14 Studies have demonstrated variable success of hydroxyapatite implants with exposure rates for this implant varying from 1% to 28%. 15 Shields & coworkers, 16 in the largest series to date of 250 enucleations (70 for retinoblastoma), had one infection and four exposures (1.6%), which were all in children. Gender Exposed Unexposed Table 4. Gender and Exposure Rate Treated Unexposed Treated Exposed Untreated Unexposed Male Female Total Untreated Exposed 943
5 Ophthalmology Volume 107, Number 5, May 2000 In a prospective study from the same unit of 60 pediatric patients, 51 with retinoblastoma, de Potter et al 4 found no actual exposure in their series. Dutton 17 reported no complications in a series of 50. Buettner and Bartley 18 observed a 22% exposure. Many authors believe that healing is difficult once hydroxyapatite is exposed in the early stages because complete vascularization takes between 6 and 10 months. Some authors have suggested drilling holes to the center of the implant to expedite this process. 19 Reznick and Gilmore 20 have suggested that this implant, despite its chemical similarities to the inorganic bone matrix, behaves like a foreign body in infection. The central unvascularized core can act as a harbor for organisms, leading to chronic fistulization. 21 Misiek and colleagues 22 have also suggested that the degree of microscopic coarseness of the pores may predispose to exposure. Timing of Exposure Causes of orbital implant extrusion can be divided into early and late. 23,24 Early extrusion could be caused by edema, infection, hemorrhage, too large an implant or conformer, or faulty surgical technique. In the mainly adult-based literature, most implants expose in the first 16 weeks in the postoperative period. 18,21,25 Goldberg et al 26 had six hydroxyapatite implants exposed within 4 to 6 weeks after enucleation. A small proportion (13%, 4 of 30) of our exposures occurred in the first 30 days after enucleation. Eighty-seven percent (26 of 30) of our exposures occurred in the first year after enucleation. Friction from a poorly fitting prosthesis may lead to erosion of tissue covering the anterior surface of the implant, leading to late extrusion. This can be due to pressure necrosis with secondary infection or conjunctival downgrowth through the dehiscence. Conjunctival downgrowth may cause epithelialization of the cavity around the implant, with resulting contracture of the orbital tissues. 27 To ensure a good prosthetic fit in a young child, we occasionally undertake molding under anesthesia. Late exposure may also be influenced by orbital growth and remodeling in the pediatric orbit. Effect of Chemotherapy and Radiotherapy on Exposure Rate We have similar findings as previous experimental studies that preimplantation radiotherapy does not appear to have a detrimental effect on the retention of primary orbital implant. 28 There is an increased rate of exposure in the chemotherapy group, 34% compared with 21% in the untreated group, although this does not attain statistical significance (P 0.058). However, this study has the limitation of retrospective analysis, with all the resulting difficulties of drawing conclusions from a large series of patients treated with different methods. The ideal would be prospective randomized study of orbital implants in chemotherapy sockets, but to obtain the number of patients necessary in these complicated cases would be impracticable as well as unethical because it would involve jeopardizing patient care by withholding adjuvant treatment from some groups. Acknowledgments We thank Ms. Catey Bunce, of the Glaxo Institute of Epidemiology, Moorfields Eye Hospital, for her statistical advice. References 1. Kingston JE, Hungerford JL, Madreperla SA, Plowman PN. Results of combined chemotherapy and radiotherapy for advanced intraocular retinoblastoma. Arch Ophthalmol 1996; 114: Karesh JW, Dresner SC. High density porous polyethylene (Medpor) as a successful anophthalmic socket implant. Ophthalmology 1994;101: Perry AC. Integrated orbital implants. Adv Ophthalmic Plast Reconstr Surg 1990;8: De Potter P, Shields CL, Shields JA, Singh AD. Use of the hydroxyapatite ocular implant in the pediatric population. Arch Ophthalmol 1994;112: NHS Executive. Guidance on the microbiological safety of human tissues and organs used in transplantation. HSG(96)26.25/3/ Murphree AL, Villablanca JG, Deegan WF III, et al. Chemotherapy plus local treatment in the management of intraocular retinoblastoma. Arch Ophthalmol 1996;114: Gallie BL, Budning A, DeBoer G, et al. Chemotherapy with focal therapy can cure intraocular retinoblastoma without radiotherapy. Arch Ophthalmol 1996;114: Soll DB. Evolution and current concepts in the treatment of the anophthalmic orbit. In: Smith BC, ed. Ophthalmic Plastic and Reconstructive Surgery. St. Louis: Mosby, 1987; v. 2, chap 73, Kaste SC, Chen G, Fontanesi J, et al. Orbital development in long-term survivors of retinoblastoma. J Clin Oncol 1997;15: Shields CL, Shields JA, De Potter P. Hydroxyapatite orbital implant after enucleation. Experience with initial 100 consecutive cases. Arch Ophthalmol 1992;110: Troutman RC. End results of implant surgery. Trans Am Acad Ophthalmol Otolargyngol 1952;56: Rubin LR, ed. Biomaterials in Reconstructive Surgery. St. Louis: Mosby, 1983; chap Karcioglu ZA, Al-Mesfer SA, Mullaney PB. Porous polyethylene orbital implant in patients with retinoblastoma. Ophthalmology 1998;105: Jordan DR, Ells A, Brownstein S et al. Vicryl-mesh wrap for the implantation of hydroxyapatite orbital implants: an animal model. Can J Ophthalmol 1995;30: Kaltreider SA, Newman SA. Prevention and management of complications associated with the hydroxyapatite implant. Ophthal Plast Reconstr Surg 1996;12: Shields CL, Shields JA, De Potter P, Singh AD. Problems with the hydroxyapatite orbital implant: experience with 250 consecutive cases. Br J Ophthalmol 1994;78: Dutton JJ. Coralline hydroxyapatite as an ocular implant. Ophthalmology 1991;98: Buettner H, Bartley GB. Tissue breakdown and exposure associated with orbital hydroxyapatite implants. Am J Ophthalmol 1992;113: Ferrone PJ, Dutton JJ. Rate of vascularisation of coralline hydroxyapatite ocular implants. Ophthalmology 1992; 99: Reznick JB, Gilmore WC. Host response to infection of a subperiosteal hydroxyapatite implant. Oral Surg Oral Med Oral Pathol 1989;67:
6 Lee et al Exposure of Orbital Implants in Retinoblastoma Patients 21. Remulla HD, Rubin PA, Shore JW, et al. Complications of porous spherical orbital implants. Ophthalmology 1995;102: Misiek DJ, Kent JN, Carr RF. Soft tissue responses to hydroxyapatite particles of different shapes. J Oral Maxillofac Surg 1984;42: Levine MR. Extruding orbital implant: prevention and treatment. Ann Ophthalmol 1980;12: Oberfeld S, Levine MR. Diagnosis and treatment of complications of enucleation and orbital implant surgery. Adv Ophthal Plast Reconstr Surg 1988;8: Nunery WR, Heinz GW, Bonnin JM, et al. Exposure rate of hydroxyapatite spheres in the anophthalmic socket: histopathologic correlation and comparison with silicone sphere implants. Ophthal Plast Reconstr Surg 1993;9: Goldberg RA, Holds JB, Ebrahimpour J. Exposed hydroxyapatite orbital implants. Report of six cases. Ophthalmology 1992;99: Dryden R, Leibsohn J. Postenucleation orbital implant extrusion. Arch Ophthalmol 1978;96: Martin RT, Nunery WR, Bonnin JM, Rate WR. Effects of radiation on the use of hydroxyapatite for orbital reconstruction in the rabbit. Ophthal Plast Reconstr Surg 1993; 9:
Early ocular prosthesis insertion improves quality of life after enucleation
 Optometry (2006) 77, 71-75 Early ocular prosthesis insertion improves quality of life after enucleation Kimberly Chin, O.D., a Charles B. Margolin, M.B.A., a and Paul T. Finger, M.D. a,b,c a The New York
Optometry (2006) 77, 71-75 Early ocular prosthesis insertion improves quality of life after enucleation Kimberly Chin, O.D., a Charles B. Margolin, M.B.A., a and Paul T. Finger, M.D. a,b,c a The New York
Mobility of Hydroxyapatite Orbital Implant Covered With Autologous Sclera
 Mobility of Hydroxyapatite Orbital Implant Covered With Autologous Sclera Shin-ichiro Kawai, Tsuneko Suzuki and Katsuhito Kawai Department of Ophthalmology, Saitama Medical Center, Saitama Medical School,
Mobility of Hydroxyapatite Orbital Implant Covered With Autologous Sclera Shin-ichiro Kawai, Tsuneko Suzuki and Katsuhito Kawai Department of Ophthalmology, Saitama Medical Center, Saitama Medical School,
Integrated Hydroxyapatite Implant and Non-integrated Implants in Enucleated Asian Patients
 Original Article 477 Integrated Hydroxyapatite Implant and Non-integrated Implants in Enucleated Asian Patients CT Chuah, 1 FRCS, M Med (Ophth), SP Chee, 2 FRCS, M Med, FRC (Ophth), KS Fong, 1 FRCS, M
Original Article 477 Integrated Hydroxyapatite Implant and Non-integrated Implants in Enucleated Asian Patients CT Chuah, 1 FRCS, M Med (Ophth), SP Chee, 2 FRCS, M Med, FRC (Ophth), KS Fong, 1 FRCS, M
REMOVAL OF an eye for treatment
 Intraorbital Implants After Enucleation and Their Complications A 10-Year Review CLINICAL SCIENCES Nancy J. Christmas, MD; Craig D. Gordon; Timothy G. Murray, MD; David Tse, MD; Thomas Johnson, MD; Scott
Intraorbital Implants After Enucleation and Their Complications A 10-Year Review CLINICAL SCIENCES Nancy J. Christmas, MD; Craig D. Gordon; Timothy G. Murray, MD; David Tse, MD; Thomas Johnson, MD; Scott
Clinical Study Standard Enucleation with Aluminium Oxide Implant (Bioceramic) Covered with Patient s Sclera
 The Scientific World Journal Volume 2012, Article ID 481584, 4 pages doi:10.1100/2012/481584 The cientificworldjournal Clinical Study Standard Enucleation with Aluminium Oxide Implant (Bioceramic) Covered
The Scientific World Journal Volume 2012, Article ID 481584, 4 pages doi:10.1100/2012/481584 The cientificworldjournal Clinical Study Standard Enucleation with Aluminium Oxide Implant (Bioceramic) Covered
Effect of Basic Fibroblast Growth Factor on Fibrovascular Ingrowth into Porous Polyethylene Anophthalmic Socket Implants
 Korean J Ophthalmol Vol. 19:1-8, 2005 Effect of Basic Fibroblast Growth Factor on Fibrovascular Ingrowth into Porous Polyethylene Anophthalmic Socket Implants Won Chan Park, MD, Soo Kyung Han, MD, Nam
Korean J Ophthalmol Vol. 19:1-8, 2005 Effect of Basic Fibroblast Growth Factor on Fibrovascular Ingrowth into Porous Polyethylene Anophthalmic Socket Implants Won Chan Park, MD, Soo Kyung Han, MD, Nam
Use of hollow polymethylmethacrylate as an orbital implant
 VOL. 9 NO. PHILIPPINE JOURNAL OF Ophthalmology MARCH ORIGINAL ARTICLE 00 Archimedes Lee D. Agahan, MD Alexander D. Tan, MD Department of Ophthalmology and Visual Sciences University of the Philippines
VOL. 9 NO. PHILIPPINE JOURNAL OF Ophthalmology MARCH ORIGINAL ARTICLE 00 Archimedes Lee D. Agahan, MD Alexander D. Tan, MD Department of Ophthalmology and Visual Sciences University of the Philippines
James W. Gigantelli, M.D.
 The Path to Anophthalmos James W. Gigantelli, MD Ophthalmic Plastic Surgery and Orbital Disease University of Nebraska Medical Center Objectives Understand conditions that result in anophthalmos/microphthalmos
The Path to Anophthalmos James W. Gigantelli, MD Ophthalmic Plastic Surgery and Orbital Disease University of Nebraska Medical Center Objectives Understand conditions that result in anophthalmos/microphthalmos
Retinoblastoma: A Review of Current Treatment Strategies
 Retinoblastoma: A Review of Current Treatment Strategies ABSTRACT: Since the last review of retinoblastoma therapies in the 15 years ago, there has been a significant shift in the approach to treating
Retinoblastoma: A Review of Current Treatment Strategies ABSTRACT: Since the last review of retinoblastoma therapies in the 15 years ago, there has been a significant shift in the approach to treating
The Results of Evisceration with Primary Porous Implant Placement in Patients with Endophthalmitis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(5):279-283 DOI: 10.3341/kjo.2010.24.5.279 Original Article The Results of Evisceration with Primary Porous Implant Placement in Patients with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(5):279-283 DOI: 10.3341/kjo.2010.24.5.279 Original Article The Results of Evisceration with Primary Porous Implant Placement in Patients with
M-Sphere Orbital Implant Surgical Guide
 MOLTENO Orbital Implant Surgical Guide A Step by Step Guide to inserting the Natural Hydroxyapatite Orbital Implant 0316-SG/MS Anthony C. B. Molteno, FRCS, FRACO Copyright Anthony C. B. Molteno Molteno,
MOLTENO Orbital Implant Surgical Guide A Step by Step Guide to inserting the Natural Hydroxyapatite Orbital Implant 0316-SG/MS Anthony C. B. Molteno, FRCS, FRACO Copyright Anthony C. B. Molteno Molteno,
What is so special about Retinoblastoma?
 Definition Retinoblastoma is a primary malignant neoplasm of the retina that arises from immature retinal cells. It is the most common primary intraocular malignancy of childhood. What is so special about
Definition Retinoblastoma is a primary malignant neoplasm of the retina that arises from immature retinal cells. It is the most common primary intraocular malignancy of childhood. What is so special about
Anophthalmic Sockets in Retinoblastoma: A Single Center Experience
 ORIGINAL CLINICAL STUDY Anophthalmic Sockets in Retinoblastoma: A Single Center Experience Preethi Jeyabal, MBBS, and Gangadhara Sundar, DO, FRCSEd, FAMS, AB(USA) Purpose: To evaluate outcomes of anophthalmic
ORIGINAL CLINICAL STUDY Anophthalmic Sockets in Retinoblastoma: A Single Center Experience Preethi Jeyabal, MBBS, and Gangadhara Sundar, DO, FRCSEd, FAMS, AB(USA) Purpose: To evaluate outcomes of anophthalmic
Eye-Preserving Therapy in Retinoblastoma: Prolonged Primary Chemotherapy Alone or Combined with Local Therapy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):219-224 DOI: 10.3341/kjo.2010.24.4.219 Original Article Eye-Preserving Therapy in Retinoblastoma: Prolonged Primary Chemotherapy Alone or
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):219-224 DOI: 10.3341/kjo.2010.24.4.219 Original Article Eye-Preserving Therapy in Retinoblastoma: Prolonged Primary Chemotherapy Alone or
Long-term Surgical Outcomes of the Multi-purpose Conical Porous Synthetic Orbital Implant
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):294-300 http://dx.doi.org/10.3341/kjo.2015.29.5.294 Original Article Long-term Surgical Outcomes of the Multi-purpose Conical Porous Synthetic
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):294-300 http://dx.doi.org/10.3341/kjo.2015.29.5.294 Original Article Long-term Surgical Outcomes of the Multi-purpose Conical Porous Synthetic
Virtual Mentor American Medical Association Journal of Ethics December 2010, Volume 12, Number 12:
 Virtual Mentor American Medical Association Journal of Ethics December 2010, Volume 12, Number 12: 950-954. IMAGES OF HEALING AND LEARNING The Fourth O in Eye Care Ocularists Michael O. Hughes, BCO The
Virtual Mentor American Medical Association Journal of Ethics December 2010, Volume 12, Number 12: 950-954. IMAGES OF HEALING AND LEARNING The Fourth O in Eye Care Ocularists Michael O. Hughes, BCO The
Custom Prosthetic Eyes
 Custom Prosthetic Eyes Todd Cranmore BCO/BADO Licensed Ocularist WELCOME EYE CARE LOSS & HANDLING OCULAR PROSTHETICS SCLERAL SHELLS Realities of Eye Loss Anxiety Depression Fear of Blindness Loss of Depth
Custom Prosthetic Eyes Todd Cranmore BCO/BADO Licensed Ocularist WELCOME EYE CARE LOSS & HANDLING OCULAR PROSTHETICS SCLERAL SHELLS Realities of Eye Loss Anxiety Depression Fear of Blindness Loss of Depth
Tiffany L. Kruger, D.O. Children s Hospital of Michigan Wayne State University/Kresge Eye Institute
 Pediatric Cases Nt Not To Be Missed Tiffany L. Kruger, D.O. Pediatric Ophthalmology Fellow Children s Hospital of Michigan Wayne State University/Kresge Eye Institute Case Presentation CC: Left eye turns
Pediatric Cases Nt Not To Be Missed Tiffany L. Kruger, D.O. Pediatric Ophthalmology Fellow Children s Hospital of Michigan Wayne State University/Kresge Eye Institute Case Presentation CC: Left eye turns
Financial Disclosures
 Retinoblastoma Management: Update Jesse L. Berry, MD Associate Director, Ocular Oncology Service Associate Program Director USC/CHLA, Keck School of Medicine Financial Disclosures Research Support: Bright
Retinoblastoma Management: Update Jesse L. Berry, MD Associate Director, Ocular Oncology Service Associate Program Director USC/CHLA, Keck School of Medicine Financial Disclosures Research Support: Bright
cme Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Educational Objectives
 Article Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Michael S. McCracken, MD; Jonathan D. del Prado, MD; David B. Granet, MD; Leah Levi, MBBS; Don O. Kikkawa, MD Abstract
Article Combined Eyelid and Strabismus Surgery: Examining Conventional Surgical Wisdom Michael S. McCracken, MD; Jonathan D. del Prado, MD; David B. Granet, MD; Leah Levi, MBBS; Don O. Kikkawa, MD Abstract
INTRACONAL IMPLANTS ARE WELL
 LINIL SINS Mechanisms and Treatment of xtruding Intraconal Implants Socket ging and Tissue Restitution (the actus Syndrome ) Mandeep S. Sagoo, M, Ph, MROphth, FRS(din); Geoffrey. Rose, MS, Sc, FRS, FROphth
LINIL SINS Mechanisms and Treatment of xtruding Intraconal Implants Socket ging and Tissue Restitution (the actus Syndrome ) Mandeep S. Sagoo, M, Ph, MROphth, FRS(din); Geoffrey. Rose, MS, Sc, FRS, FROphth
Managing a Cosmetic Blemish
 192 Kerala Journal of Ophthalmology Vol. XX, No. 2 CONSULTATION S E C T I O N Managing a Cosmetic Blemish Dr. Ani Sreedhar 1 MS, Dr. Gangadhara Sundar 2 MS, Dr. Santosh Honavar 3 MS, Dr. K.R Satish 4 MS,
192 Kerala Journal of Ophthalmology Vol. XX, No. 2 CONSULTATION S E C T I O N Managing a Cosmetic Blemish Dr. Ani Sreedhar 1 MS, Dr. Gangadhara Sundar 2 MS, Dr. Santosh Honavar 3 MS, Dr. K.R Satish 4 MS,
Retinoblastoma, the most common intraocular. Utility of Pupillary Dilation for Detecting Leukocoria in Patients With Retinoblastoma
 Utility of Pupillary Dilation for Detecting Leukocoria in Patients With Retinoblastoma John C. Canzano, MD, and James T. Handa, MD ABSTRACT. In the United States, 50% of all retinoblastoma cases are diagnosed
Utility of Pupillary Dilation for Detecting Leukocoria in Patients With Retinoblastoma John C. Canzano, MD, and James T. Handa, MD ABSTRACT. In the United States, 50% of all retinoblastoma cases are diagnosed
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
A RESOURCE MANUAL MANAGEMENT RETINOBLASTOMA LOW & MIDDLE RESOURCE SETTINGS
 A RESOURCE MANUAL FOR THE MANAGEMENT OF RETINOBLASTOMA IN LOW & MIDDLE RESOURCE SETTINGS UPDATED SEPTEMBER 2017 1 CONTENTS PAGE INTRODUCTION 3 SERVICE LEVEL for Rb MANAGEMENT 4 SCREENING 5 EARLY DIAGNOSIS
A RESOURCE MANUAL FOR THE MANAGEMENT OF RETINOBLASTOMA IN LOW & MIDDLE RESOURCE SETTINGS UPDATED SEPTEMBER 2017 1 CONTENTS PAGE INTRODUCTION 3 SERVICE LEVEL for Rb MANAGEMENT 4 SCREENING 5 EARLY DIAGNOSIS
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique
 Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
Pterygium Excision and Conjunctival-Limbal Autograft Transplantation: A Simplified Technique Kirti Nath Jha Professor of Ophthalmology Mahatma Gandhi Medical College & Research Institute,Pondy-Cuddalore
CLINICAL SCIENCES. with thermotherapy or cryotherapy is an important
 CLINICAL SCIENCES Macular Retinoblastoma Managed With Chemoreduction Analysis of Tumor Control With or Without Adjuvant Thermotherapy in 68 Tumors Carol L. Shields, MD; Arman Mashayekhi, MD; Jacqueline
CLINICAL SCIENCES Macular Retinoblastoma Managed With Chemoreduction Analysis of Tumor Control With or Without Adjuvant Thermotherapy in 68 Tumors Carol L. Shields, MD; Arman Mashayekhi, MD; Jacqueline
Ruthenium-106 plaque brachytherapy in the primary management of ocular medulloepithelioma
 Poon, DS; Reich, E; Smith, VM; Kingston, J; Reddy, MA; Hungerford, JL; Sagoo, MS; (2015) Ruthenium-106 Plaque Brachytherapy in the Primary Management of Ocular Medulloepithelioma. Ophthalmology, 122 (9)
Poon, DS; Reich, E; Smith, VM; Kingston, J; Reddy, MA; Hungerford, JL; Sagoo, MS; (2015) Ruthenium-106 Plaque Brachytherapy in the Primary Management of Ocular Medulloepithelioma. Ophthalmology, 122 (9)
CHEMOREDUCTION FOR RETINOBLASTOMA: ANALYSIS OF TUMOR CONTROL AND RISKS FOR RECURRENCE IN 457 TUMORS
 CHEMOREDUCTION FOR RETINOBLASTOMA: ANALYSIS OF TUMOR CONTROL AND RISKS FOR RECURRENCE IN 457 TUMORS BY Carol L. Shields MD,* Arman Mashayekhi MD, Jacqueline Cater PhD, Abdallah Shelil MD, Anna T. Meadows
CHEMOREDUCTION FOR RETINOBLASTOMA: ANALYSIS OF TUMOR CONTROL AND RISKS FOR RECURRENCE IN 457 TUMORS BY Carol L. Shields MD,* Arman Mashayekhi MD, Jacqueline Cater PhD, Abdallah Shelil MD, Anna T. Meadows
EVIDENCE BASED MANAGEMENT FOR Retinoblastoma
 CLINICAL EVALUATION & STAGING EVIDENCE BASED MANAGEMENT FOR Retinoblastoma Symptoms & Signs : White eye reflex, squint, diminished vision, red eye, proptosis. History - Family history of retinoblastoma
CLINICAL EVALUATION & STAGING EVIDENCE BASED MANAGEMENT FOR Retinoblastoma Symptoms & Signs : White eye reflex, squint, diminished vision, red eye, proptosis. History - Family history of retinoblastoma
Vision Eye Centre, Siri Fort Road, New Delhi
 Oculoplasty Anophthalmic Socket A.K. Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO, Saurbhi Khurana MD, FICO, Shaloo Bageja DNB, Rituraj Baruah MS Vision Eye Centre, Siri Fort Road, New Delhi A nophthalmos
Oculoplasty Anophthalmic Socket A.K. Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO, Saurbhi Khurana MD, FICO, Shaloo Bageja DNB, Rituraj Baruah MS Vision Eye Centre, Siri Fort Road, New Delhi A nophthalmos
Pyogenic Granuloma in an anophthalmic Socket Secondary to ill-fitting Prosthesis- Case Report
 Pyogenic Granuloma in an anophthalmic Socket Secondary to ill-fitting Prosthesis- Dr Sowmya V. 1, Dr Nelly E P Nazareth 2, Dr Vijna B Kamath 3 Abstract Pyogenic granulomas are vaso-proliferative inflammatory
Pyogenic Granuloma in an anophthalmic Socket Secondary to ill-fitting Prosthesis- Dr Sowmya V. 1, Dr Nelly E P Nazareth 2, Dr Vijna B Kamath 3 Abstract Pyogenic granulomas are vaso-proliferative inflammatory
Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques
 Techniques in Ophthalmology 5(3):125 129, 2007 P E D I A T R I C S U R G E R Y Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques David A. Sami, MD Pediatric Subspecialty Faculty
Techniques in Ophthalmology 5(3):125 129, 2007 P E D I A T R I C S U R G E R Y Conjunctival Incisions for Strabismus Surgery: A Comparison of Techniques David A. Sami, MD Pediatric Subspecialty Faculty
Evisceration Techniques and Implant Extrusion Rates: A Retrospective Review of Two Series and a Survey of ASOPRS Surgeons. Don Liu, M.D., F.A.C.S.
 Ophthalmic Plastic and Reconstructive Surgery Vol. 23, No. 1, pp 16 21 2007 The American Society of Ophthalmic Plastic and Reconstructive Surgery, Inc. Evisceration Techniques and Implant Extrusion Rates:
Ophthalmic Plastic and Reconstructive Surgery Vol. 23, No. 1, pp 16 21 2007 The American Society of Ophthalmic Plastic and Reconstructive Surgery, Inc. Evisceration Techniques and Implant Extrusion Rates:
Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO
 Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO If you have questions, please do not hesitate to call Dr. Hsu at Eye Care for Animals, St. Charles at 630-444-0393 or email at stcharlesinfo@eyecareforanimals.com
Ophthalmology Wet Lab Notes - Kimberly Hsu, DVM, MSc, DACVO If you have questions, please do not hesitate to call Dr. Hsu at Eye Care for Animals, St. Charles at 630-444-0393 or email at stcharlesinfo@eyecareforanimals.com
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Outpatient tube removal required. 3 4 (Pain scores are lower following local anesthesia compared to GA.)
 166 SECTION 2. 0 its medial wall. Following incision of the nasal mucosa through the osteotomy, the posterior flap of the lacrimal sac is sutured to the posterior nasal mucosa flap. The probe is advanced
166 SECTION 2. 0 its medial wall. Following incision of the nasal mucosa through the osteotomy, the posterior flap of the lacrimal sac is sutured to the posterior nasal mucosa flap. The probe is advanced
Lateral Orbitotomy in the Management of Challenging Exotropia
 Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Lateral Orbitotomy in the Management of Challenging Exotropia Yahalom C (1, 2), Mc Nab A (3), Ben Simon G (3), Kowal L (1). 1- Centre for Eye Research Australia and Ocular Motility Clinic, Royal Victorian
Sub-Tenon Versus Peribulbar Anaesthesia for Cataract Surgery
 Bahrain Medical Bulletin, Vol. 25, No.3, September 2003 Sub-Tenon Versus Peribulbar Anaesthesia for Cataract Surgery Nada Al-Yousuf, FRCSEd * Purpose: The aim of this study is to compare the efficacy of
Bahrain Medical Bulletin, Vol. 25, No.3, September 2003 Sub-Tenon Versus Peribulbar Anaesthesia for Cataract Surgery Nada Al-Yousuf, FRCSEd * Purpose: The aim of this study is to compare the efficacy of
MEDPOR. Oral maxillofacial surgery
 MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR. Oculoplastic surgery
 MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
Medel R, Vásquez LM (eds): Orbital Surgery. ESASO Course Series. Basel, Karger, 2014, vol 5, pp (DOI: / )
 Anophthalmic Socket Christoph Hintschich University Eye Hospital, Ludwig Maximilian University Munich, Munich, Germany Abstract Anophthalmos is defined as an orbit without a clinically detectable eye.
Anophthalmic Socket Christoph Hintschich University Eye Hospital, Ludwig Maximilian University Munich, Munich, Germany Abstract Anophthalmos is defined as an orbit without a clinically detectable eye.
PLEASE SCROLL DOWN FOR ARTICLE
 This article was downloaded by:[canadian Research Knowledge Network] On: 9 September 2007 Access Details: [subscription number 770938029] Publisher: Informa Healthcare Informa Ltd Registered in England
This article was downloaded by:[canadian Research Knowledge Network] On: 9 September 2007 Access Details: [subscription number 770938029] Publisher: Informa Healthcare Informa Ltd Registered in England
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION
 NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
Transvitreal Fine Needle Aspiration Biopsy of Choroidal Melanoma via Pars Plana Vitrectomy
 Surgical Technique Is pars plana vitrectomy a safe method for performing fine needle aspiration biopsy of choroidal melanoma? What are the rates of complications? Clinical Characteristics Do tumor thickness
Surgical Technique Is pars plana vitrectomy a safe method for performing fine needle aspiration biopsy of choroidal melanoma? What are the rates of complications? Clinical Characteristics Do tumor thickness
INTRODUCTION. Trans Am Ophthalmol Soc 2005;103:
 A COMPARISON OF IMPLANT EXTRUSION RATES AND POSTOPERATIVE PAIN AFTER EVISCERATION WITH IMMEDIATE OR DELAYED IMPLANTS AND AFTER ENUCLEATION WITH IMPLANTS BY Don Liu MD ABSTRACT Purpose: To examine implant
A COMPARISON OF IMPLANT EXTRUSION RATES AND POSTOPERATIVE PAIN AFTER EVISCERATION WITH IMMEDIATE OR DELAYED IMPLANTS AND AFTER ENUCLEATION WITH IMPLANTS BY Don Liu MD ABSTRACT Purpose: To examine implant
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Basic microsurgical suturing techniques for beginners
 ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
Plate/Valve Specifications: Thickness: 0.9mm Width: 13.00mm Length: 16.00mm Surface Area: mm 2
 Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
Distribué en France par FCI S.A.S. France Chirurgie Instrumentation SAS 20/22 rue Louis Armand 75015 PARIS Tél. 01.53.98.98.98 / Fax. 01.53.98.98.99 fci@fci.fr / www.fci.fr CATALOGUE DE VENTE Features:
Prospective evaluation of contracted sockets
 Kathmandu University Medical Journal (2007), Vol. 5, No. 3, Issue 19, 391-395 Prospective evaluation of contracted sockets Original Article Adhikari RK 1, Khazai H 2, Usha KD 3 1 Prof National Academy
Kathmandu University Medical Journal (2007), Vol. 5, No. 3, Issue 19, 391-395 Prospective evaluation of contracted sockets Original Article Adhikari RK 1, Khazai H 2, Usha KD 3 1 Prof National Academy
Relationship of regression pattern to recurrence in retinoblastoma
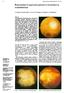 12 BritishJournal ofophthalmology 1993; 77: 12-16 Relationship of regression pattern to recurrence in retinoblastoma A D Singh, D Garway-Heath, S Love, P N Plowman, J Kingston, J L Hungerford Ophthalmology
12 BritishJournal ofophthalmology 1993; 77: 12-16 Relationship of regression pattern to recurrence in retinoblastoma A D Singh, D Garway-Heath, S Love, P N Plowman, J Kingston, J L Hungerford Ophthalmology
A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament
 접수번호 : 2008-087 Korean Journal of Ophthalmology 2009;23:183-187 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.183 A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament Han Woong
접수번호 : 2008-087 Korean Journal of Ophthalmology 2009;23:183-187 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.183 A Cadaveric Anatomical Study of the Levator Aponeurosis and Whitnall s Ligament Han Woong
Retinoblastoma in Great Britain : incidence,
 British Journal of Ophthalmology, 1988, 72, 576-583 Retinoblastoma in Great Britain 1969-80: incidence, treatment, and survival B M SANDERS,' G J DRAPER,' AND J E KINGSTON2 From the 'Childhood Cancer Research
British Journal of Ophthalmology, 1988, 72, 576-583 Retinoblastoma in Great Britain 1969-80: incidence, treatment, and survival B M SANDERS,' G J DRAPER,' AND J E KINGSTON2 From the 'Childhood Cancer Research
1 Eyelids. Lacrimal Apparatus. Orbital Region. 3 The Orbit. The Eye
 1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
1 1 Eyelids Orbital Region 2 Lacrimal Apparatus 3 The Orbit 4 The Eye 2 Eyelids The eyelids protect the eye from injury and excessive light by their closure. The upper eyelid is larger and more mobile
MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE
 Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
Australian and New Zealand Journal of Ouhthalmology 1985; 13: 179-183 MULLERS MUSCLE-CONJUNCTIVAL RESECTION PTOSIS PROCEDURE ALLEN M. PUTTERMAN MD University Of lll~nois Eye and Ear Infirmary, Michael
Clinical Note Clinical Outcome of 285 Medpor Grafts used for Craniofacial Reconstruction PATIENTS AND METHODS
 Clinical Note Clinical Outcome of 285 Medpor Grafts used for Craniofacial Reconstruction Roberto Cenzi, MD,* Antonio Farina, MD, y Luca Zuccarino, MD, z Francesco Carinci, MD Ferrara, Italy Porous polyethylene
Clinical Note Clinical Outcome of 285 Medpor Grafts used for Craniofacial Reconstruction Roberto Cenzi, MD,* Antonio Farina, MD, y Luca Zuccarino, MD, z Francesco Carinci, MD Ferrara, Italy Porous polyethylene
Vitreoretinal surgical management In ocular oncology
 www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
Retinoblastoma. all information provided by:
 basic information & treatment plans of Retinoblastoma all information provided by: Ocular Oncology Service Wills Eye Hospital Philadelphia, PA 840 WALNUT STREET SUITE 1440, PHILADELPHIA, PA 19107 WWW.FIGHTEYECANCER.COM
basic information & treatment plans of Retinoblastoma all information provided by: Ocular Oncology Service Wills Eye Hospital Philadelphia, PA 840 WALNUT STREET SUITE 1440, PHILADELPHIA, PA 19107 WWW.FIGHTEYECANCER.COM
Original Research Article
 STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
Removal of an Eye, Artificial Eyes, and Socket Care
 Removal of an Eye, Artificial Eyes, and Socket Care Introduction: Removal of an eye, or the inside coats of an eye, may be necessary for various reasons. However, regardless of the underlying disorder,
Removal of an Eye, Artificial Eyes, and Socket Care Introduction: Removal of an eye, or the inside coats of an eye, may be necessary for various reasons. However, regardless of the underlying disorder,
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
Outcomes of Cataract Surgery Following Treatment for Retinoblastoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):52-57 https://doi.org/10.3341/kjo.2017.31.1.52 Outcomes of Cataract Surgery Following Treatment for Retinoblastoma Hyeong Min Kim 1,2, Byung
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):52-57 https://doi.org/10.3341/kjo.2017.31.1.52 Outcomes of Cataract Surgery Following Treatment for Retinoblastoma Hyeong Min Kim 1,2, Byung
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page
 The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7412-7417 Mohammad Ahmad Wahdan 1, Abd Allah El Hussainy Shaleel 1, Hossam El Dein Ahmed El Zomor 2, Hossam El Din Hassan El Sayed
The Egyptian Journal of Hospital Medicine (October 2018) Vol. 73 (9), Page 7412-7417 Mohammad Ahmad Wahdan 1, Abd Allah El Hussainy Shaleel 1, Hossam El Dein Ahmed El Zomor 2, Hossam El Din Hassan El Sayed
Beginner (score = 3) Can hold goniolens but hesitates to move to visualize a different angle.
 Instructions: Use one form per trainee For each competency, allocate a score to the trainee s level of execution of said skill: Novice (Score = 2), Beginner (Score = 3), Advanced (Score 4), and Competent
Instructions: Use one form per trainee For each competency, allocate a score to the trainee s level of execution of said skill: Novice (Score = 2), Beginner (Score = 3), Advanced (Score 4), and Competent
Mc Gregor Flap for Lower Eyelid Defect
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. V (April. 2017), PP 69-74 www.iosrjournals.org Mc Gregor Flap for Lower Eyelid Defect
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. V (April. 2017), PP 69-74 www.iosrjournals.org Mc Gregor Flap for Lower Eyelid Defect
From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I.
 TRANSPLANTATION OF THE NAIL: A CASE REPORT By NICHOLAS P. PAPAVASSlI.IOU, M.D. 1 From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I. THE loss of a finger nail may be of
TRANSPLANTATION OF THE NAIL: A CASE REPORT By NICHOLAS P. PAPAVASSlI.IOU, M.D. 1 From the Orthopaedic Department, St. George's Hospital Medical School, London S.W.I. THE loss of a finger nail may be of
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
SYNPOR POROUS POLYETHYLENE IMPLANTS. For craniofacial and orbital augmentation and reconstruction
 SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
SYNPOR POROUS POLYETHYLENE IMPLANTS For craniofacial and orbital augmentation and reconstruction SURGICAL TECHNIQUE TABLE OF CONTENTS INTRODUCTION SYNPOR Porous Polyethylene Implants 2 Indications and
30+ MEDPOR biomaterial. years of proven clinical history
 MEDPOR ENT surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
MEDPOR ENT surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Technique Guide. SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction.
 Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Mechanics of the Ahmed Glaucoma Valve
 Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
Dr. A. Mateen Ahmed President & CEO - New World Medical, Inc. New World Medical, Inc. (NWMI) is a high tech medical device company whose goal is to help humanity lead a better life through improved technology
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING
 PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
Bilateral Retinoblastoma Joseph Junewick, MD FACR
 Bilateral Retinoblastoma Joseph Junewick, MD FACR 06/11/2010 History 17 month old adopted female with proptosis. Diagnosis Bilateral Retinoblastoma Discussion Retinoblastoma is the most common pediatric
Bilateral Retinoblastoma Joseph Junewick, MD FACR 06/11/2010 History 17 month old adopted female with proptosis. Diagnosis Bilateral Retinoblastoma Discussion Retinoblastoma is the most common pediatric
Bilateral retinoblastoma in early infancy
 Saiju R et al Case report Bilateral retinoblastoma in early infancy Saiju R, Duwal S Tilganga Institute of Ophthalmology, Kathmandu, Nepal Abstract Introduction: Retinoblastoma is the most common primary
Saiju R et al Case report Bilateral retinoblastoma in early infancy Saiju R, Duwal S Tilganga Institute of Ophthalmology, Kathmandu, Nepal Abstract Introduction: Retinoblastoma is the most common primary
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM
 SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
SURGICAL TECHNIQUE THE TENDON ANCHOR SYSTEM TABLE OF CONTENTS Introduction PAGE 1 Features and Benefits PAGE 1-2 Applications PAGE 3 Ordering Information PAGE 4 Indications & Contra-indications PAGE 5
Retinal dialysis. procedures. The purpose of the present paper is to report the results of treatment of 62
 Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Humanity s Vision Is Our Focus. The Ahmed Glaucoma Valve
 Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Humanity s Vision Is Our Focus The Ahmed Glaucoma Valve Dr. A. Mateen Ahmed President - New World Medical New World Medical is a high tech medical device company whose goal is to help humanity lead a better
Cytoflex Barrier Membrane Clinical Evaluation
 Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Cytoflex Barrier Membrane Clinical Evaluation Historical Background Guided tissue regeneration is a well established concept in the repair of oral bone defects. The exclusion of soft tissue epithelial
Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
A ptosis repair of aponeurotic defects by the posterior approach
 British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
Retinoblastoma. Protocol applies to retinoblastoma only.
 Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Some of the ophthalmic surgeries
 Some of the ophthalmic surgeries Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary
Some of the ophthalmic surgeries Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
A Legacy of Serving the Surgical Community
 TM A Legacy of Serving the Surgical Community Step By Step Instructions For over half a century, Stryker has been developing products based on the expressed needs of leading practitioners. Introducing
TM A Legacy of Serving the Surgical Community Step By Step Instructions For over half a century, Stryker has been developing products based on the expressed needs of leading practitioners. Introducing
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The O'Connor cinch revisited
 The O'Connor cinch revisited British Journal of Ophthalmology, 1978, 62, 765-769 A. THOMAS WILLIAMS, HENRY S. METZ, AND ARTHUR JAMPOLSKY From the Smith-Kettlewell Institute of Visual Sciences, San Francisco,
The O'Connor cinch revisited British Journal of Ophthalmology, 1978, 62, 765-769 A. THOMAS WILLIAMS, HENRY S. METZ, AND ARTHUR JAMPOLSKY From the Smith-Kettlewell Institute of Visual Sciences, San Francisco,
Plaque Radiotherapy in Recurrent or Incomplete- Excised Conjunctival Squamous Cell Carcinoma and Melanoma
 Plaque Radiotherapy in Recurrent or Incomplete- Excised Conjunctival Squamous Cell Carcinoma and Melanoma Masood Naseripour, MD 1 Mohsen Bahmani-Kashkouli, MD 1 Ramin Jaberi, MS 2 Gholam-Hossein Aghaee,
Plaque Radiotherapy in Recurrent or Incomplete- Excised Conjunctival Squamous Cell Carcinoma and Melanoma Masood Naseripour, MD 1 Mohsen Bahmani-Kashkouli, MD 1 Ramin Jaberi, MS 2 Gholam-Hossein Aghaee,
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Update on Intraocular Oncology
 Update on Intraocular Oncology Suganeswari Ganesan Shri Bhagwan Mahavir Vitreoretinal Services, Sankara Nethralaya Correspondence to: Suganeswari Ganesan, Consultant, Vitreoretinal and Oncology services,
Update on Intraocular Oncology Suganeswari Ganesan Shri Bhagwan Mahavir Vitreoretinal Services, Sankara Nethralaya Correspondence to: Suganeswari Ganesan, Consultant, Vitreoretinal and Oncology services,
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
