We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
|
|
|
- Laurence Lee
- 5 years ago
- Views:
Transcription
1 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3, , M Open access books available International authors and editors Downloads Our authors are among the 151 Countries delivered to TOP 1% most cited scientists 12.2% Contributors from top 500 universities Selection of our books indexed in the Book Citation Index in Web of Science Core Collection (BKCI) Interested in publishing with us? Contact book.department@intechopen.com Numbers displayed above are based on latest data collected. For more information visit
2 Chapter 2 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going Adrianna Ranger, Navjot Chaudhary and Jonathan Lau Additional information is available at the end of the chapter 1. Introduction In North merica and Europe, cancer involving the central nervous system (CNS) ranks second as the most common malignancy seen in infancy through adolescence, second only to leukaemia [1-7]. Consistent with this are figures on cancer-related mortality. In the year 2004, for example, there were 566 confirmed cases of leukemia-related death among children in the United States, followed by 555 CNS cancer-related deaths; these numbers accounted for 25.5% and 25.0% of the total number of cancer deaths in individuals less than 20 years old, respectively [4]. In general, survival from cancer has improved dramatically over the past forty years, presumably due to a combination of improved treatments and earlier detection. This is especially true in the paediatric population, among whom the overall long-term survival rate across all cancers has risen from under 50% to roughly 70% [4;8;9]. Even with brain cancer, the prognosis in children has improved, such that long-term survival is now achieved in more than half of patients [10]. This being said, the neoplasm originates in the brainstem in roughly 10-20% of children with CNS cancer [7;11-13], accounting for 150 to 300 new cases per year in the U.S. [11;13] and thus rendering it more common in children and adolescents than in adults [14;15]. nd in this subset of children, the prognosis generally is considered extremely bleak, akin to that of glioblastoma multiforme [1;4;14;16-19]. Despite a continued poor prognosis, much has changed over the past several decades like how paediatric brainstem tumours are diagnosed and classified, if and when surgery is considered, approaches to surgery, the use of adjunct therapies like radiation and chemotherapy, and the evolution of several new therapeutic options. Once lumped together as a single 2014 The Author(s). Licensee InTech. This chapter is distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
3 32 Tumors of the Central Nervous System Primary and Secondary entity that was considered inoperable and, hence, completely incurable, recent developments in imaging and surgical techniques have led to the classification of several different types of brainstem tumour; and, for some of these, surgical resection is considered the treatment of choice [16;18;20]. This chapter reviews the historical progression of understanding of paediatric brainstem tumours, including evolving beliefs regarding their classification, diagnosis, management, prognosis and prognosticators, dating from the 1970s to current times. It then describes current diagnostic and management protocols for these tumours, ending with a glance forwards towards potentially promising treatments and technologies and how they might, hopefully within the near future, favourably alter outcomes in these patients, both in terms of their survival and quality of life. 2. Where we have been 2.1. Definitions, diagnosis and classification The brainstem has been defined as extending from the midbrain (tectal plate) to the medullary cervical junction [7]. rain stem tumours are, by definition, tumours that involve the brainstem. However, they include tumours not just in the brainstem per se, but also in the upper cervical spine [16]. In the paediatric population, posterior fossa tumours significantly outnumber those that are supratentorial [10;21;22], and brainstem tumours account for roughly 25% of all tumours found within the posterior fossa [16;23]. The vast majority of these are primary lesions, since just 3 to 5% of all brain metastases are found in the brainstem [24]. The most common paediatric posterior fossa tumours are cerebellar astrocytomas, medulloblastomas, ependymomas and brainstem gliomas [25]. Traditionally, the term brainstem glioma has been used to incorporate all brainstem tumours, largely because biopsies often were not performed and the majority of brainstem tumours in childhood are, in fact, of glial cell origin [26;27]. However, other histological forms of tumours do exist, though they comprise but a small percentage of brainstem tumours, and generally tend to be exophytic, growing either external to the brainstem or on its surface. Even among such exophytic tumours, gliomas form the clear majority. In their series of 75 paediatric patients with exophytic tumours seen between 1970 and 1990, Pierre-Kahn et al. [28] noted 69 glial tumours (92% of the total), of which 58 were astrocytomas and 11 oligodendrogliomas. The remaining six non-glial tumours were two ependymomas; two primitive neuroectodermal tumours (PNET); one ganglioglioma; and one of unknown histology [28]. In a much more recent review of non-glial brainstem tumours, other brainstem lesions noted to occur anecdotally included medulloblastomas invading the brainstem, cavernomas, lymphomas, haemangioblastomas, and other ganglionic and mixed tumors [29]. Nonetheless, many continue to use the term brainstem glioma generically, given that the vast majority of brainstem tumours are glial cell based. Up until the development of advanced imaging techniques like computed tomography (CT) and, to an even greater extent, magnetic resonance imaging (MRI) brainstem tumours
4 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 33 tended to be lumped together as a single clinical entity and considered uniformly inoperable [30]. Since they were presumed gliomas and surgery was deemed contraindicated, there was no call even to biopsy them, except in certain instances in which the diagnosis was in doubt. For example, in 1969, Matson wrote: brainstem gliomas must be classified as malignant tumors since their location in itself renders them inoperable [21]. nd as late as 1984, Tomita et al. [31] wrote: Since biopsy specimens often misrepresent the true pathology... surgery undertaken to obtain precise histological verification of brain stem gliomas is futile. Instead, these latter authors recommended computed tomography (CT) with high-resolution metrizamide CT cisternography to distinguish surgically resectable extra-axial tumors adjacent to the brain stem from non-resectable intrinsic brain stem gliomas. Such sentiments that tumours only were worth a biopsy if they were either completely exterior to brainstem tissue or, at worst, on the surface were echoed by others [32]. Consequently, early classification of brainstem tumours often subdivided lesions into those that were exclusively or primarily intraaxial, and those that were exclusively or primarily extra-axial. Meanwhile, brainstem tumours were collectively contrasted against those involving the midbrain or thalamus, both of which exhibited considerably superior prognoses [33]. This being said, there were early reports of certain patients with brainstem tumours who survived long-term. For example, in 1971, Lassiter et al. reported on 37 patients with presumed brainstem gliomas (22 of them children), among whom there were four children with large, surgically-drained neoplastic cysts who achieved long-term survival: two of these children died 7½ and 13 years later, and two still were alive 8½ and 9 years post diagnosis, one of them going on to graduate from college and the other with residual hemiparesis and mental retardation [34]. In 1975, Hara et al. reviewed the cases of 24 brainstem gliomas, and found that the median survival was 9 months, except for one patient who survived beyond 4½ years and another who lived for 14 years and 10 months before succumbing to the disease [35]. Similar isolated cases of long-term survival with brainstem gliomas, especially cystic lesions, were reported as far back as 1937 and 1940 through the mid nineteen seventies and early eighties [36-42]. nd, contrary to conventional wisdom, even then, some neurosurgeons were routinely performing biopsies and surgery on select patients with brainstem gliomas [27;40;41;43-46]. In the nineteen sixties and early nineteen seventies, angiography and pneumoencephalograms were largely used to identify brain and brainstem tumours [47-50]. These imaging modalities were replaced in the mid nineteen seventies as computed tomography (CT) emerged as the imaging tool of choice for the detection and diagnosis of both supra-and infra-tentorial lesions, including brainstem tumours [51-54]. y this point, some surgeons were starting to distinguish outcomes between different subsets of patient who were able to undergo either partial or radical resection of brainstem cancers [27;40;41;43-45]. The first to propose what he termed a staging system for brainstem gliomas was Epstein, in 1985, who first categorized tumours as intrinsic, exophytic and disseminated; and then subcategorized intrinsic (actual brainstem) tumours as either diffuse, focal or cervico-medullary [43]. In 1986 and again in 1988, Epstein et al. published series of paediatric patients undergoing surgery for brainstem cancer, again classifying patients as focal, diffuse or cervico-medullary; in the latter report, they added a
5 34 Tumors of the Central Nervous System Primary and Secondary category for cystic lesions [27;44]. What these authors noted was uniformly dismal outcomes in children with diffuse lesions, but often favourable outcomes in those patients with any one of the three other classifications. In the 1988 report, co-authored by Wisoff [27], among 66 children with intrinsic brainstem gliomas diagnosed between 1980 and 1986 who underwent radical surgical resection and either CT, MRI or both pre-operatively, 27 (41%) were found to have diffuse tumors, all of whom died within 12 to 18 months of surgery with malignant neoplasms that had not benefitted from surgery. However, five of nine children with cystic tumors, three of five with focal tumors, and twenty of twenty-four with cervicomedullary tumors were discovered to have a histopathologically low-grade lesion, and these 28 children all remained alive between one and six years post-operatively. The authors proposed criteria combining clinical and neuroradiological findings to predict which patients with brainstem tumors were likely to benefit from radical surgical intervention [27]. Since that time, several additional and very different classification systems have been proposed for brainstem tumours, including those by Stroink et al., arkovich et al., lbright, Fischbein et al., Choux et al., Fisher et al., Mehta et al. and, most recently, Ramos et al. [45;55-61]. (See Table 1) The system proposed by Stroink et al., published in 1987, was born out of a study of 16 children (9 girls, 7 boys; age range 1½-12 years) with dorsally exophytic transependymal benign brainstem gliomas diagnosed between 1962 and 1985 at Sick Kids Hospital in Toronto, Canada [45]. Of these, 13 were low-grade (grade I-II) astrocytomas, one a grade III astrocytoma, and two gangliogliomas. ll 16 patients underwent subtotal resection of their tumours, and seven had post-operative radiation therapy. One died 18 months after surgery, but the remaining 15 remained alive an average of eight years post-operatively (median=7 years; range=8 months to 23 years). ased upon these results, Stroink et al. proposed dorsal exophytic gliomas (Type I) as a distinct clinical entity, to differentiate them from hypo-dense, nonenhancing intrinsic tumours (Type IIa); hyper-dense, contrast-enhancing exophytic intrinsic tumours (Type IIb); focal, enhancing cystic intrinsic tumours (Type III); and focal iso-dense and contrast-enhancing intrinsic tumours (Type IV) [45]. Author(s) Year Published Imaging Classification System Epstein [43] 1985 CT, MRI Intrinsic - diffuse; focal, cervicomedullary Exophytic - anterolateral; posterolateral Disseminated - positive cytology; positive myelography Epstein et al. [44] 1986 CT, MRI Diffuse Focal Cervicomedullary Epstein et al. [27] 1988 CT, MRI Diffuse Focal Cervicomedullary Cystic
6 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 35 Author(s) Year Published Imaging Classification System Stroink et al. [45] 1987 CT with contrast Type I: dorsal exophytic glioma Type II intrinsic brainstem tumour * IIa - hypodense with no contrast enhancement IIb - hyperdense with contrast enhancement, exophytic Type III: focal cystic tumour with contrast enhancement Type IV: focal isodense tumour with contrast enhancement Barkovich et al. [55] 1990 MRI Tumours characterized by - (1) Location - midbrain, pons, medulla (2) Focality - focal or diffuse (3) Direction & extent of tumour growth (4) Degree of brainstem enlargement (5) Presence/absence of exophytic growth (6) Presence/absence of haemorrhage or necrosis (7) Evidence of hydrocephalus Albright [58] 1996 MRI Focal - midbrain; pons; medulla Diffuse Fischbein et al. [56] 1996 MRI Midbrain - diffuse; focal; tectal Pons - diffuse; focal Medulla - diffuse; focal; dorsal and exophytic Choux et al. [57] 2000 MRI Type I - diffuse Type II - intrinsic and focal Type III - intrinsic and exophytic Type IV - cervicomedullary Fisher et al. [59] 2000 MRI Pilocytic astrocytomas Fibrillary astrocytomas Other tumors Mehta et al. [60] 2009 MRI Intrinsic tumours - expanding; diffuse infiltrative; purely ventral Extrinsic tumours Ramos et al. [61] 2013 MRI Diffuse intrinsic/diffusely infiltrative Posterior exophytic/cervicomedullary gliomas; other focal tumours Dorsal exophytic tumours Cervicomedullary tumours Focal tectal tumours Table 1. Classification Systems for Brain Stem Tumours-1985 to Present
7 36 Tumors of the Central Nervous System Primary and Secondary It was in the mid to late nineteen-eighties that magnetic resonance imaging (MRI) started to replace CT as the imaging modality of choice for the diagnosis and classification of brainstem tumours [62]. s such, it was based upon MRI studies that arkovich et al. proposed their criteria for brainstem tumours in 1990 [55]. Their criteria were derived from the results of retrospectively-reviewed MRI studies for 87 paediatric patients with brainstem gliomas. T2- weighted images were deemed most appropriate for use, given that they were the most accurate at demonstrating the extent of tumour. In this much more elaborate classification scheme, tumours were characterized in terms of (1) their location of origin, into midbrain, pons and medulla; (2) their degree of focality (whether diffuse of focal); (3) the direction and extent of tumour growth; (4) the degree of brainstem enlargement; (5) the degree of exophytic growth; (6) the presence or absence of cysts, necrosis or hemorrhage; and (7) the presence or absence of hydrocephalus. This classification scheme was never scientifically validated to determine its ability to predict outcomes, however, and failed to achieve widespread acceptance. Likely reasons for this failure were how cumbersome the system was, and the lack of any firm guidelines as to its use. s such, subsequent classification schemes have been much simpler, starting with those proposed by lbright, in 1996, who returned to the very simple categorization of lesions as being either focal (further distinguished by location, into midbrain, pons or medulla) or diffuse [58]; and Fischbein et al., also in 1996, who again categorized lesions as focal or diffuse, but categorized both forms of lesion by location again into midbrain, pons or medulla [56]. Harkening back to the four-category system initially proposed by Epstein in 1985 [43], Freeman et al., in 1998, and Choux et al., in 2000, adopted the four relatively straight-forward categories largely in use today: diffuse intrinsic; focal intrinsic; focal exophytic, and cervicomedullary [18;57]. In 2009, Mehta et al. proposed a modified sub-categorization of intrinsic tumours, into expanding, diffuse infiltrative, and pure ventral varieties, achieving good surgical results and reasonable survival with the first of the three subtypes [60]. Then, most recently, Ramos et al. adopted yet another classification system that included diffuse intrinsic and diffusely infiltrative as a single category, followed by four additional categories of various focal lesions [61]. The authors conclusion was that brainstem tumors are a heterogeneous group of tumors. Clearly then, in terms of how brainstem tumours are now perceived, there has been a 180 degree reversal from early statements [21;30;31] about their homogeneity and the inappropriateness of biopsies for brainstem tumours. The questions remain, however: Who warrants such biopsies? nd how could biopsies and surgery influence outcomes? 2.2. Outcome predictors and indications for surgery Early universal pessimism regarding the fate of children with brainstem tumours has also clearly changed in recent years, with reports of better than 90% five-and ten-year survival rates in children with certain types of tumour [23;63]. The primary objective of all the classification schemes proposed to date has been to identify which patients warrant surgical treatment and how aggressive such treatment should be. Contrary to early years, when all brainstem tumours were considered inoperable [21;30;31], for the past thirty years neurosurgeons have been operating to either de-bulk or completely excise lesions when doing so was felt to be of clinical
8 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 37 benefit, potentially positively influencing quality of life and/or survival. s stated earlier, that a subset of patients existed for whom long-term survival was possible has been suspected for almost eighty years [36;37]. Once again, it was Epstein et al. who first identified diffuse lesions as being the most rapidly fatal, and focal and cystic lesions as being more amenable to treatment and long-term survival [27;43;44]. Since then, other prognostic factors have been identified that can influence the decision to operate (See Table 2). Factor Studies Year Published Imaging Comments Focal (vs. diffuse intrinsic) tumour Sandri et al. [77] 2006 MRI 87.4% 4-year vs. 12.3% 2-year survival Mauffrey [20] 2006 MRI 90% vs. 22% 2-year survival Fried et al MRI 89% vs. 3% 5-year survival Cystic appearance Lassiter et al. [34] 1971 not identified All 4 children with cystic lesions Prolonged pre-diagnosis symptoms Fisher et al. [59] 2000 MRI Cox regression survival w/ symptoms > 6 mo (p =. 004) Shuper et al. [17] 1998 MRI Mean survival 19.5 vs mo with >1 mo symptoms Other than pons location Fisher et al. [59] 2000 MRI Cox regression survival w/ pons involvement (p=. 0002) No presenting eye symptoms/eye palsies Fisher et al. [59] 2000 MRI Cox regression survival w/ abducens palsy (p<.0001) Shuper et al. [17] 1998 MRI Mean survival 17.5 vs mo with no eye symptoms Basilar artery engulfment Fisher et al. [59] 2000 MRI Cox regression survival w/ basilar artery engulfed (p=.006) Tectal location Poussaint et al. [65] 1998 MRI All 32 children with tectal tumours alive after a mean 5 years follow-up Non-enhancing on gadolinium MRI Poussaint et al. [65] 1998 MRI Gadolinium enhancement of tectal lesions increased odds of disease progression x15 Contrast enhancement on MRI Dellaretti et al. [64] 2012 MRI Mean survival with contrast enhancing lesions = 21.7 mo.; with non-enhancing lesions 54.2 months (p <.001) Maximum diameter < 0.5 cm Poussaint et al. [65] 1998 MRI Each 1 cm increase in maximum diameter increased odds of disease progression x5 Neurofibromatosis type 1 Fried et al. [72] 2012 MRI All 7 children with NF-1 had non-focal lesions & long-term survival Other papers Numerous isolated anecdotal reports in other papers Table 2. Factors Predicting Favourable Outcomes in Paediatric Brainstem Tumour Patients
9 38 Tumors of the Central Nervous System Primary and Secondary One of the earliest attempts to empirically look at prognostic factors beyond imaging results was published by Fisher et al. in 2000 [59]. They reported on the results of a study of 77 patients, 21-years old or younger, seen between 1980 and In this study, they sought to identify characteristics statistically associated with poor survival. The factors that they identified were (a) symptom duration less than six months before diagnosis (p=0.004); (b) abducens palsy at presentation (p < ); (c) a pontine location (p=0.0002); and (d) engulfment of the basilar artery (p=0.006). Twenty of their patients were found to have pilocytic astrocytomas, which were associated with a very favorable 5-year overall survival rate of 95%, as well as with location outside the ventral pons (p=0.001) and dorsal exophytic growth (p=0.013). nother histological type they could predict based upon clinic-radiographic findings was fibrillary astrocytoma, of which they had 14 cases. These lesions were associated with symptoms < 6 months (p=0. 006), abducens palsy (p < 0.001), engulfment of the basilar artery (p=0.002), and a one-year survival rate of just 23% (p < ). Shuper et al. also found, in their analysis of 24 children operated upon between 1981 and 1997, that a shorter duration of symptoms (< 4 weeks) and visual symptoms at presentation were associated with shorter survival and lower survival rates [17]. Meanwhile, Dellaretti et al. found that contrast-enhancing lesions on MRI were associated with a significantly shorter mean duration of survival versus non-enhancing lesions (21.7 vs months, p < 0.001); however, on Cox proportional hazards regression analysis, tumour grade was the only significant predictor of survival, suggesting that contrast enhancement in that sample was an indicator of higher tumour grade [64]. Poussaint et al. specifically sought to determine which clinical and imaging findings best correlated with outcomes in children with tumours involving the midbrain tectum, via a retrospective review of the medical records and imaging studies of 32 children (16 boys and 16 girls; mean age, 8 years) with tectal tumours [65]. Of this number, eight children had undergone CT, 11 MRI, and 13 both CT and MRI studies. Over a mean follow-up period of five years (range, 3.6 months to 17 years), all patients experienced hydrocephalus, for which all but one required cerebrospinal fluid (CSF) diversion. The tectum was the centre of the tumour in all cases; and the majority of the tumours appeared iso-dense on CT scans, isointense on T1-weighted MR images, and hyper-intense on T2-weighted images. Twenty patients required no further treatment. In this group, the mean maximum tumour diameter was 1.8 cm, and enhancement occurred in only two cases (10%). t follow-up, 18 tumours were the same size as at baseline, one was larger due to cyst formation in the setting of stable symptoms, and one was smaller. The remaining 12 patients required further treatment (excision and/or radiotherapy) because of disease progression, indicated either by increased tumour size or by worsening symptoms. In this group, the mean maximum tumour diameter was 2.5 cm and contrast enhancement occurred in nine (75%). Further follow-up in this group showed decreased tumour size in eight and stable residual tumor in three. The authors then used regression analysis to calculate and compare the likelihood of a patient requiring further treatment with various-size enhancing versus non-enhancing tumours and identified two trends: larger tumours were more likely to require further treatment; and the same was true for enhancing lesions. Combining these two factors was especially predictive. For example, whereas 31% of lesions with a maximum diameter of 0.5 cm required further treatment, samesized non-enhancing lesions warranted such treatment less than one percent of the time.
10 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 39 Corresponding percentages for lesions of maximum diameter 1.0, 1.5, 2.0, 2.5, 3.0, 3.5 and 4.0 cm were 48 and 1%, 67 and 3%, 80 and 6%, 90 and 11%, 95 and 21%, 97 and 36%, and 98 and 54%. y the time a lesion reached 4.5 cm in maximum diameter, virtually all (99 and 70%) required further treatment, irrespective of whether they did or did not enhance. Overall, the odds of surgical or radiation treatment were almost five times greater for each 1 cm increase in maximum tumor diameter (odds ratio, 4.9; 95% confidence interval, ; p=0.015); and 15 times greater when the tumor enhanced versus when it did not (15.0; ; p < 0.003). The investigators thereby concluded that, though paediatric tectal tumors exhibit somewhat variable behavior, patients generally do well, and that larger tumours, and especially those that that enhance with contrast on MRI, are highly likely to be more aggressive [65]. Whether size and contrast-based enhancement on MRI or CT predict the need for treatment or ultimate outcomes with other non-diffuse intrinsic or exophytic brainstem tumours has not yet been demonstrated. nother factor long believed to place individuals at increased risk of brainstem and other CNS malignancies, but also to confer a relatively favorable prognosis, is the presence of type 1 neurofibromatosis (NF-1), though this belief is largely based upon anecdotal reports [66-72]. In the large study of 223 children with brainstem tumours reported by Fried et al., however, there were seven children with concomitant NF-1; and all had low-grade brainstem tumours [72]; the statistical likelihood that this occurred merely by chance, assuming a fifty-fifty split of low-to high-grade lesions (which is roughly what they observed across the sample), is less than one percent. Overall in NF-1 patients, brainstem gliomas comprise a heterogeneous group of lesions, consisting of three main subtypes: (1) diffuse brainstem enlargement; (2) focal enhancing nodules with or without cystic areas; and (3) peri-aqueductal gliomas. ll of these subtypes, including diffuse brainstem enlargement, generally exhibit a very indolent course and do not require treatment, though MRI monitoring is indicated until their indolent course is confirmed. Some lesions even regress on their own [73]. The diffuse brainstem enlargement is somewhat similar in appearance to the unidentified bright objects (U Os) that are the most commonly observed CNS lesions on MRI in patients with NF-1 [74]. Like U Os, they exhibit abnormal signals on T1-weighted images. The major differences are that, as opposed to U Os, there usually is a mass effect, and these lesions also tend to be considerably larger than most U Os. What the diffuse enlargement represents remains controversial. Many presume them to be gliomas, but they exhibit a much more indolent course than brainstem gliomas seen outside of NF-1, such that adjuvant treatment is only required in the minority of patients whose lesions progress. However, ongoing monitoring is required to detect the few who do progress, before neurological deficits ensue, which often are irreversible. Rarely, these gliomas progress to more malignant forms of astrocytoma, including glioblastoma [73;75]. The focal enhancing nodules seen in the brainstem of NF-1 patients, which may occur with or without cystic areas, generally are thought to represent pilocytic astrocytomas, given their imaging characteristics. Like pilocytic astrocytomas elsewhere, they generally are indolent; but their course is unpredictable and the brainstem so susceptible to major deficits, relative to the cerebral hemispheres, that ongoing monitoring is required. Small, focal intrinsic lesions
11 40 Tumors of the Central Nervous System Primary and Secondary may enlarge and then regress spontaneously. Exophytic tumours often are more aggressive and require treatment. Periaqueductal gliomas occur adjacent to the aqueduct of Sylvius between the 3 rd and 4 th ventricles in the midbrain. They typically manifest with late-onset aqueductal stenosis, leading to hydrocephalus. Presumably, they represent low-grade gliomas or glial hamartomas, and typically are indolent. However, because of their location, CSF shunting often is necessary. ut, as with the other two forms of brainstem tumour seen in NF-1 patients, resection usually is unnecessary [73;75]. Table 3 summarizes currently published research on tumour characteristics that predict a favourable outcome. What is most evident is the dearth of confirmatory studies. These findings aside, the brainstem tumour characteristic that is unquestionably the one most likely to dissuade surgeons from operating is evidence that the tumour is intrinsic and diffuse, due both to the known high risks of surgery and to the lack of evidence suggesting any benefit, in terms of either quality of life or survival time [16-18;20]. The corollary to this is that, contrary to thirty years ago when most surgeons preferred to leave all brainstem tumours alone, focal, exophytic and cystic tumours are increasingly being accessed and resected, often with good results [16-18;20;23;60]. Year Study Study subjects 5-year survival Author(s) Published Type N = N = % = Lesniak et al. [76] 2003 Retrospective % Sandri et al. [77] 2006 Retrospective % Mauffrey [20] 2006 Retrospective % Teo et al. [63] 208 Retrospective % Fried et al. [72] 2012 Retrospective % Klimo et al. [23] 2013 Retrospective % OVERALL % Table 3. Survival in Paediatric Patients with Non-Diffuse Intrinsic Brainstem Tumours 2.3. Treatment and outcomes In 1984, Tomita [31] wrote that radiation therapy is the choice of treatment, should CT indicate clear evidence of intrinsic brain stem tumor... posterior fossa craniotomy should be undertaken only for aspiration of cystic intrinsic stem tumors, resection of extra-axial juxtastem tumors and, although rare, in instances when CT is unable to definitively distinguish extra-axial from intra-axial mass for verification of lesion location. Clearly, sentiments have changed; but has the increase in surgical interventions altered outcomes? In 1998, Shuper et al. published the results of their study of 24 children with brainstem tumours operated upon between 1981 and 1997 [17]. The main question they asked was: are we
12 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 41 improving outcomes? tissue diagnosis was achieved in only six of the children. lthough the investigators did not perform inferential statistical analysis, average survival in five patients seen before 1990 was 8.6 months, versus 19.4 months in the five patients seen in 1990 through 1994, and 20.0 months in those seen in 1995 and Moreover, raw data were provided, allowing the current author to perform a statistical comparison of months of survival pre (8.6) versus post (19.7) January 1 st This difference, despite the low numbers, is significant (t=2.379, df 13, p=0.03). However, these patients generally were offered radiation +/-chemotherapy, and not surgery. In addition, other biases might have erroneously generated these results, like alterations in referral patterns or the earlier recognition of tumours as a result of major technological advances in imaging. More recently, several authors have reported survival rates in paediatric patients treated surgically for non-diffuse tumours (Table 3). In 2003, Lesniak et al. [76] retrospectively reviewed the charts of all pediatric patients admitted to Johns Hopkins University Hospital with a diagnosis of a brainstem tumor between January 1985 and December 2000: 89 patients met the inclusion criteria, among whom 57 (64.0%) underwent surgical resection, while 32 (36%) were treated with radiation and/or chemotherapy. Of the surgical candidates, 57 (100%) had an accompanying MRI scan significant for an enhancing lesion in the midbrain, pons or the medulla. The pathology was consistent with juvenile pilocytic astrocytoma in 30 patients (52.6%) and glioblastoma multiforme in 12 patients (21.1%). The remaining cases consisted of ten patients (17.5%) with fibrillary astrocytomas, three (5.3%) with gangliogliomas, one (1.8%) with an oligodendroglioma and one (1.8%) with a primitive neuroectodermal tumor. Total surgical resection was attained in 29 patients, near total resection (>90%) in eight, subtotal resection (50-90%) in 15, and partial resection (<50%) in five. The progression-free survival of all patients, which included the twelve with glioblastomas, was 71.9% at 3 years and 45.6% at 5 years. Excluding the 12 patients with known glioblastomas, all of whom died prior to three years, these survival rates rise to 83 and 53%, comparable to rates observed in a subsequent study by Sandri et al. [77]. In 2006, Sandri et al. [77] published their series of 31 children admitted to their institution from 1995 to 2003, 14 of whom were classified on MRI as having diffuse and 17 as having focal brainstem tumours. Patients with diffuse lesions were treated with locoregional radiotherapy (1.8 Gy/day for 54 Gy) and weekly vincristine for radiosensitization (1.5 mg/sm for six total doses). Meanwhile, patients with focal tumours underwent surgical resection, with adjunct chemotherapy and/or radiotherapy considered on a case-by-case basis. mong the 14 with diffuse tumours, ten experienced a partial response, three exhibited stabilization of their disease, and one progressed. General and/or neurological symptoms improved in more than 80% of these patients. However, the median time from diagnosis to progression and from diagnosis to death were just 8 (range of 3-13) and 13 (range of 4-25) months, respectively, with a 2-year overall survival rate of just 12.3%. Conversely, among the 17 children with focal lesions, gross total removal was achieved in 4/17 cases, subtotal removal in 7/17, and partial removal in 6/17. There was one surgery-related death. Eight out of 17 patients had adjuvant chemo-and/or radiotherapy after progression, among whom six remained free of neurological symptoms and two died secondary to tumor progression. The 4-year overall and disease-free
13 42 Tumors of the Central Nervous System Primary and Secondary survival rates were 87.4 (SE 8.4) and 58.8% (SE 11.9), respectively, with the extent of resection identified as the best predictor of survival (p=0.012) [77]. lso in 2006, Mauffrey reported on his retrospectively reviewed series of 27 paediatric patients admitted to hospital in Turin, Italy with a diagnosis of brainstem glioma [20]. Thirteen patients had a diffuse pontine tumour on MRI scan, while fourteen had other brainstem gliomas. Those in the first group had a shorter mean duration of symptoms prior to diagnosis (2.6 vs months), never demonstrated gadolinium enhancement of their tumour on MRI (vs. 78.6% in the other group), and were much more likely to have symptoms or findings indicating cranial nerve involvement (77.0 vs. 28.5%). None of the 13 with diffuse gliomas underwent radical surgery, whereas it was the treatment of choice in the remaining 14. Two-year survival rates were 25% and 90%, respectively, and 60% of the latter remained alive at five years [20]. In 2008, Teo and Siu [63] reported on their results with 34 consecutive patients between 3 and 16 years of age who underwent endoscope-assisted microsurgery for focal brainstem gliomas with the intent of radial resection between 1999 and More than 90% tumour resection was achieved in 31patients, while >50% was attained in the remainder. There was no perioperative mortality and the average follow-up was 46 months. Twenty-three patients (74%) harboured low-grade and 11 (26%) high-grade gliomas. Kaplan-Meier survival analysis revealed marked differences in the 5-year survival rates between the two groups (100% vs. 33%). Multivariate analysis demonstrated that the degree of tumour resection was not associated with poor outcome at 6 months. Two papers published over the past couple of years are those by Fried et al. [72], based at The Hospital for Sick Children in Toronto Canada, and Klimo et al., based at George Washington University in Washington, DC [23]. The latter study, like all those described previously, was relatively small, with just 52 patients (32 boys), all with radiographically-confirmed, low-grade focal brainstem gliomas seen from 1986 to The median duration of follow-up was 10.0 years, and the median age at diagnosis 6.5 years (range 1-17 years). Tumors were located in the midbrain (n=22, 42%), pons (n=15, 29%), and medulla (n=15, 29%). Surgical extirpation was the primary treatment in 25 patients (48%). Five-and 10-year event-free survival and overall survival rates were 59% and 98%, and 52% and 90%, respectively. Surprisingly, children with intrinsic tumors trended towards slightly higher event-free survival at 5 years than those with exophytic tumors (p=0.054), but not at 10 years (p=0.147). No other variables were predictive of event-free survival [23]. The retrospective study by Fried et al. is by far the largest to date, assessing a total of 223 children with brainstem tumours (12% of all CNS tumours seen) followed at The Hospital for Sick Children in Toronto over the preceding 25 years [72]. Ninety-five of these tumours were diffuse and an additional 17 were high-grade astrocytomas (grade III or IV). The investigators made several novel observations. First, whereas 75% of tumors involving the pons were highgrade, 98% of tumours lacking pontine involvement were low-grade (p = ). Second, residual tumour after surgery, even when visualized, did not adversely alter either progression-free survival or overall survival. nd, among those requiring further treatment, 5-year progression-free and overall survival were comparable between those receiving chemotherapy (53 and 93%) and those administered radiotherapy (66 and 83%) (p = 0.26 and 0.30, respective
14 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 43 ly). mong those with focal lesions, five-year progression-free survival (PFS) and overall survival (OS) were 57% and 89%. Combining the results of these last seven studies (Table 3), in which children with non-focal brainstem tumours were identified and treated, either surgically or non-surgically, there were 282 such children, of whom 223 (79.1%) survived long-term (beyond 4 years and most beyond 5 years). In the largest study, which had 108 such children [72], 90% remained alive 10 years post diagnosis. Several comments are warranted. First, every one of the above-mentioned studies had significant methodological issues, not the least being that they all were retrospective. Moreover, because patients were selected for surgery, it is not possible to rule out the possibility that the characteristics that made them surgical candidates in the first place (e.g., a focal vs. diffuse tumour) were responsible for their survival, rather than the surgery itself. Nonetheless, what is clear is that long-term survival among children with non-diffuse tumours clearly is not at all uncommon. In fact, it seems likely for four out of five such children, making it the rule and not the exception, which is radically distant from both the beliefs and outcomes of thirty and forty years ago, and considerably improved from survival rates in at least one older study in which those with non-diffuse tumours were identified but not offered surgery [78]. Fried et al. concluded that children with non-diffuse brainstem tumours do well even with conservative management; but their conservative management appears to have consisted of surgical resection in most cases, with adjuvant chemotherapy or radiation considered more aggressive [72]. Ideally, from a purely methodological standpoint, future studies would randomize surgery-eligible patients to surgery versus non-surgery groups. Practically, however, this author considers it unlikely that most parents would consent to allow their children to be randomly assigned to one group or the other when surgery offers at least the potential of cure. The good news, then, irrespective of methodological questions regarding the true effectiveness of surgery, is that children with several types of brainstem tumour appear to do well. The bad news is that the majority of brainstem tumours in children continue to be either diffuse intrinsic lesions or high-grade astrocytomas [72], and the prognosis for either remains dismal, with only about 10% of children alive two years after diagnosis [79;80]. One major challenge currently facing researchers and clinicians is to identify non-surgical ways to better target these otherwise poorly responsive tumours. 3. Where we are and where we are going Clearly, the past forty years have brought about substantial changes in the way brainstem tumours are both perceived and managed. No longer is the term brainstem glioma used to lump all brainstem lesions together as homogenous, untreatable and ultimately fatal. Now, either three or four heterogeneous classes of tumour are described, and all but one is considered to be an indication for aggressive, often surgical treatment. Some investigators sub-classify lesions further, related to their anatomical location (e.g., midbrain, pons, medulla). In essence, though, irrespective of the number of tumour types proposed, all categorization systems ultimately separate diffuse intrinsic lesions from all others.
15 44 Tumors of the Central Nervous System Primary and Secondary Current diagnosis largely depends on the use of patient histories and physical findings, especially paying attention to the duration of symptoms prior to diagnosis and the type(s) of neurological deficits identified (e.g., ocular palsies), followed by magnetic resonance imaging, both with and without contrast. Lesions that are intrinsic and diffuse, and lesions that involve the pons are generally considered to be a contraindication to surgery, though many clinicians are now biopsying them to determine if they are high-or low-grade to estimate course and likely survival time [81]. Conversely, lesions that are focal, cystic, and extraphytic are usually considered treatable, with surgery to remove as much of the tumour as possible often considered the treatment of choice. Table 4, utilizing the most recently proposed classification system of Ramos et al. [61], summarizes current general practices. Following the 2013 publication of guidelines promoting the biopsy of diffuse intrinsic brainstem lesions to aid in the development of targeted therapies [82], stereotactic biopsies must now be at least considered standard of care for these patients. Radiation therapy, sometimes combined with chemotherapy, appears to induce brief clinical remissions in patients with diffuse tumours for whom surgery is not indicated, and may prolong survival slightly [83]. With other tumours, surgery often plays the major role; though some patients merely require monitoring and others respond well to radiation or conservative measures like CSF shunting alone. Tumour type Typical location Usual histology Biopsy Surgery Radiatio Chemothera n py 2-year survival Diffuse Intrinsic or Pons grade III-IV gliomas Yes No Yes +/- 10% Diffusely fibrillary Infiltrative astrocytomas Focal Medulla pilocystic astrocytomas Yes Complete resection +/- +/- 90% Brainstem gangliocytomas often possible Dorsal Exophytic Mostly in 4th pilocystic astrocytomas Yes Usually only partial +/- +/- 90% ventricle other low-grade glioma resection is possible Cervicomedullary Epicentre either in medulla or cervical spine pilocystic astrocytomas gangliocytomas Yes Complete resection +/- +/- ~ 100% possible in ~75% of pts Focal Tectal Tectum low-grade gliomas Yes Shunt placement Yes Usually not ~ 100% Resection often unnecessary Table 4. Current Management of Paediatric Brainstem Tumours
16 Paediatric Brainstem Cancers Where We Have Been; Where We Are; Where We Are Going 45 There remains no consensus, however, as to how to best categorize lesions; and the lion s share of brainstem tumours continue to be considered untreatable and to have a dismal prognosis. Consequently, three major challenges that remain are (1) coming to some consensus as to classifying lesions, so as to best predict their course, likely response to treatment and, hence, when and how best to treat them; (2) developing more effective non-surgical treatments to treat the intrinsic diffuse tumours for which all current treatments, including surgery, have been ineffective and the prognosis remains abysmal; and (3) optimizing quality of life in these children and their families, irrespective of long-term prognosis. With a view to these three main objectives, we now briefly explore current and future directions in the detection, diagnosis and classification of brainstem tumours, and in their non-operative and operative management Enhanced diagnostics and classification In few fields have there been as many and as dramatic advances as in the field of diagnostic imaging, and this appears to be having a significant impact upon how brain and brainstem tumours are now detected and diagnosed. Increasing recognition that not all brainstem tumours are a diverse collection of pathological entities with distinct courses and responses to treatment, has led to attempts to distinguish between them using advanced imaging. Typically, for example, diffuse intrinsic fibrillary astrocytomas appear hypo-intense on T1-weighted images, while heterogeneously hyper-intense on T2-weighted images; they also exhibit indistinct margins that reflect the tumour s highly infiltrative nature [61]. eyond distinctions made using different MR sequences, various contrasts are now being used to try to detect lesions that otherwise might be missed [84] and to delineate low-from high-grade lesions [19; 45;56;64;76]. For example, dorsal exophytic tumours often are low-grade pilocytic astrocytomas that, like high-grade fibrillary astrocytomas, may be hypo-intense on T1-weighted images and hyper-intense on T2-weighted images; however, they classically appear well-demarcated. Moreover, after gadolinium infusion, a cystic component often is identified, as only the solid portion of the tumour is enhanced, revealing a hypo-intense centre [61;85;86]. More recent advances in MR scanning like MR spectroscopy, MR perfusion, and diffusion tensor imaging (DTI) are also being utilized to further establish the histopathologic diagnosis of brainstem lesions [18;61]. n additional advantage of these newer MR technologies is that they are better at monitoring for disease recurrence or progression after treatment, since radiationinduced necrosis may be mistaken for tumour re-growth with traditional MRI [87-90]. In addition, functional scans like functional MRI (fmri), positron emission tomography (PET), and single-photon emission computed tomography (SPECT) are emerging as additional imaging tools to identify and characterize lesions in the brain, brainstem and spinal cord [19;91-95]. Further development of these tools may aid in further delineating the various brainstem tumours, even obviating the need for tissue in those patients for whom biopsies pose undue risk. This being said, among the most major imaging advances related to brainstem tumours relates to stereotactic biopsies. stereotactic biopsy utilizes a computer and images performed in at least two planes, first to localize a target lesion, like a tumour, in three-dimensional space; then
17 46 Tumors of the Central Nervous System Primary and Secondary to determine its depth; and finally to guide the removal of tissue for pathological examination. Stereotactic biopsies rely on the underlying principle of parallax, a process that initially was used in astrology to estimate distances between stars [96]. Parallax is the concept of using multiple site lines to visualize the same object relative to objects of known position in front of and behind it. Since objects closer to the observer tend to move more than objects that are more distant when the point of observation changes, measuring the degree of movement of the target lesion relative to reference points, combined with recording the change in viewing angle, permits one to estimate the depth or "Z-dimension" of the target lesion [97]. Long used to aid in the biopsy of breast lesions [98], CT-guided stereotactic biopsies have been used for the diagnosis of brain lesions since the nineteen seventies [99;100], but not with brainstem lesions until more recently. Just this year, Cage et al. reported on their results specifically biopsying diffuse brainstem tumours; they also extensively reviewed the literature [81]. In their own series, nine children with pontine lesions were biopsied, with successful tissue collection achieved in all cases. mong these lesions, four were found to be low-grade (grade I or II) astrocytomas, and five high-grade (grade III or IV) gliomas, demonstrating heterogeneity even among diffuse pontine lesions. Moreover, only one patient experienced any post-operative complication transient seizures and hydrocephalus. In their review of the literature, the same authors identified twenty case series besides their own, ranging in size from a single paediatric patient [101] to 52 children [102]. In this latter series, among 52 paediatric brainstem biopsies, only five patients experienced any post-operative morbidity, in four instances transient; and there were no deaths. iopsy was felt to alter management in 18% of the cases. In another one of the larger series, Kondziolka and Lunsford reported on their use of CT-guided stereotactic biopsies in 40 consecutive patients seen over a 13-year interval [103]. Of this number, 20 patients had midbrain lesions (n=20), 18 pontine lesions, and two medullary lesions. Midline lesions were approached via a coronal, trans-thalamic trajectory; lateral brain stem lesions usually were approached via a trans-cerebellar route. histologic diagnosis was achieved in 38 patients (95%), and no post-biopsy haemorrhages were noted on CT performed immediately after the procedure. Only one patient (2.5%) experienced a complication, which was transient diplopia. ltogether across the twenty-one papers Cage et al. reviewed, there were 294 documented brainstem biopsies in paediatric patients, among whom there were 16 cases of an intra-operative complication (5.4%); 42 cases of increased post-operative morbidity (14.3%) that was transient in the vast majority of cases; 29 inconclusive biopsies (9.9%); and two procedure-related deaths (0.7%) [102]. The authors concluded that brainstem biopsies are safer than widely perceived and that, when used judiciously, might be both safe and of advantage in terms of determining treatment. Stereotactic biopsies have been demonstrated to be superior to MRI alone in accurately diagnosing brainstem lesions [104] Enhanced non-operative management Many have argued against biopsying diffuse intrinsic brainstem lesions, since they cannot be surgically removed or even de-bulked without causing unacceptable neurological deficits because of their location and infiltrating nature, and given the lack of enduring response that the vast majority of patients demonstrate to traditional chemotherapy and radiation. ut this pessimistic outlook may be changing, given emerging knowledge about potential therapeutic
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CHAPTER 11 Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas
 Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas Foolishly, I waited 7 months before I joined this (or any) group. By that time, my son had radiation, chemo, and a recurrence of
Tumors Originating in the Brain Medulloblastomas, PNETs and Ependymomas Foolishly, I waited 7 months before I joined this (or any) group. By that time, my son had radiation, chemo, and a recurrence of
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Prognostic factors in pediatric brain-stem gliomas
 J Neurosurg 65:751-755, 1986 Prognostic factors in pediatric brain-stem gliomas A. LLAND ALBRIGHT, M.D., A. NRMAN GUTHKLCH, M.CH., F.R.C.S., RGR J. PACKR, M.D., RBRT A. PRIC, M.D., AND LUCY B. RURK, M.D.
J Neurosurg 65:751-755, 1986 Prognostic factors in pediatric brain-stem gliomas A. LLAND ALBRIGHT, M.D., A. NRMAN GUTHKLCH, M.CH., F.R.C.S., RGR J. PACKR, M.D., RBRT A. PRIC, M.D., AND LUCY B. RURK, M.D.
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Intrinsic brainstem tumors may be a challenge to the
 J Neurosurg Pediatrics 14:598 603, 2014 AANS, 2014 Neurosurgical treatment of pediatric low-grade midbrain tumors: a single consecutive institutional series of 15 patients Clinical article Tryggve Lundar,
J Neurosurg Pediatrics 14:598 603, 2014 AANS, 2014 Neurosurgical treatment of pediatric low-grade midbrain tumors: a single consecutive institutional series of 15 patients Clinical article Tryggve Lundar,
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Brainstem diffuse gliomas: radiologic findings.
 Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Joana Ramalho, MD C. Ryan Miller, MD, PhD
 Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM EPENDYMOMA Last Revision Date July 2015 1 CNS Site Group Ependymoma Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2.
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Small and Big Operations: New Tools of the Trade for Brain Tumors. Disclosure. Incidence of Childhood Cancer
 Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Small and Big Operations: New Tools of the Trade for Brain Tumors Nalin Gupta MD PhD Chief, Division of Pediatric Neurosurgery Departments of Neurosurgery and Pediatrics University of California San Francisco
Brainstem (BS) tumors in adults focusing on direct microsurgery
 Brainstem (BS) tumors in adults focusing on direct microsurgery Alejandra T. Rabadan MD, PhD Institute of Medical Research A Lanari. University of Buenos Aires UBA & Surgical Team of Buenos Aires ENBA
Brainstem (BS) tumors in adults focusing on direct microsurgery Alejandra T. Rabadan MD, PhD Institute of Medical Research A Lanari. University of Buenos Aires UBA & Surgical Team of Buenos Aires ENBA
STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER
 IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
IJCRR Section: Healthcare Sci. Journal Impact Factor 4.016 Original Article STUDY OFPAEDIATRIC CNS TUMORS IN TERTIARY CARE CENTER Grishma P. Jobanputra Tutor, Department of Pathology, B.J. Medical College,
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management. Timothy M. George, MD, FACS, FAAP
 Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management Timothy M. George, MD, FACS, FAAP PEDIATRIC BRAIN TUMORS BACKGROUND: Incidence: Third most common pediatric tumor type (leukemia, neuroblastoma,
Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management Timothy M. George, MD, FACS, FAAP PEDIATRIC BRAIN TUMORS BACKGROUND: Incidence: Third most common pediatric tumor type (leukemia, neuroblastoma,
Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation
 Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation 2 Case 7 year old girl Initially parents noticed photophobia Then started to complain
Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation 2 Case 7 year old girl Initially parents noticed photophobia Then started to complain
Dosimetry, see MAGIC; Polymer gel dosimetry. Fiducial tracking, see CyberKnife radiosurgery
 Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
TABLES. Table 1: Imaging. Congress of Neurological Surgeons Author (Year) Description of Study Classification Process / Evidence Class
 TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
TABLES Table 1: Imaging Kremer et al (2002) 2 Study Design: Prospective followed case series. Patient Population: Fifty adult patients with NFPA Study Description: Patients underwent MRI before surgery,
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
New Imaging Concepts in Central Nervous System Neoplasms
 New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Tectal Tumors of Childhood: Clinical and Imaging Follow-up
 AJNR Am J Neuroradiol 19:977 983, May 1998 Tectal Tumors of Childhood: Clinical and Imaging Follow-up Tina Young Poussaint, Janis R. Kowal, Patrick D. Barnes, David Zurakowski, Douglas C. Anthony, Liliana
AJNR Am J Neuroradiol 19:977 983, May 1998 Tectal Tumors of Childhood: Clinical and Imaging Follow-up Tina Young Poussaint, Janis R. Kowal, Patrick D. Barnes, David Zurakowski, Douglas C. Anthony, Liliana
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Brainstem Gliomas. Chapter 18. Zhiping Zhou and Mark M. Souweidane. 1. Introduction. 2. Epidemiology
 Chapter 18 Brainstem Gliomas Zhiping Zhou and Mark M. Souweidane Additional information is available at the end of the chapter http://dx.doi.org/10.5772/53887 1. Introduction Brainstem gliomas are a heterogeneous
Chapter 18 Brainstem Gliomas Zhiping Zhou and Mark M. Souweidane Additional information is available at the end of the chapter http://dx.doi.org/10.5772/53887 1. Introduction Brainstem gliomas are a heterogeneous
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA
 2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Gross Organization I The Brain. Reading: BCP Chapter 7
 Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome to Cutaneous Melanoma
 ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES
 MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
MALIGNANT GLIOMAS: TREATMENT AND CHALLENGES DISCLOSURE No conflicts of interest to disclose Patricia Bruns APRN, CNS Givens Brain Tumor Center Abbott Northwestern Hospital October 12, 2018 OBJECTIVES THEN
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
Chapter 5 Section 3.1
 Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
The Value of a Chest CT in the Evaluation of a Newly Detected Brain Tumor
 Southern Adventist Univeristy KnowledgeExchange@Southern Senior Research Projects Southern Scholars 1999 The Value of a Chest CT in the Evaluation of a Newly Detected Brain Tumor Jennifer L. White John
Southern Adventist Univeristy KnowledgeExchange@Southern Senior Research Projects Southern Scholars 1999 The Value of a Chest CT in the Evaluation of a Newly Detected Brain Tumor Jennifer L. White John
Clinical indications for positron emission tomography
 Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Management of single brain metastasis: a practice guideline
 PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Cerebral Lymphoma: Clinical and Radiological Findings in 90 Cases
 Arch Iranian Med 27; 1 (2): 194 198 Original Article Cerebral Lymphoma: Clinical and Radiological Findings in 9 Cases Alireza Zali MD *, Sohrab Shahzadi MD*, Alireza Mohammad-Mohammadi MD*, Karim Taherzadeh
Arch Iranian Med 27; 1 (2): 194 198 Original Article Cerebral Lymphoma: Clinical and Radiological Findings in 9 Cases Alireza Zali MD *, Sohrab Shahzadi MD*, Alireza Mohammad-Mohammadi MD*, Karim Taherzadeh
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Adult Brain and Spinal Cord Tumors
 Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
CNS Imaging. Dr Amir Monir, MD. Lecturer of radiodiagnosis.
 CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
Adult Central Nervous System Tumors Treatment (PDQ )
 1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
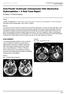 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM ANAPLASTIC GLIOMAS CNS Site Group Anaplastic Gliomas Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Radioterapia no Tratamento dos Gliomas de Baixo Grau
 Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Radioterapia no Tratamento dos Gliomas de Baixo Grau Dr. Luis Souhami University Montreal - Canada Low Grade Gliomas Relatively rare Heterogeneous, slow growing tumors WHO Classification Grade I Pilocytic
Brain Tumors. What is a brain tumor?
 Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Dr.Dafalla Ahmed Babiker Jazan University
 Dr.Dafalla Ahmed Babiker Jazan University Brain tumors are the second commonest malignancy in children Infratentorial tumors are more common As a general rule they do not metastasize out of the CNS, but
Dr.Dafalla Ahmed Babiker Jazan University Brain tumors are the second commonest malignancy in children Infratentorial tumors are more common As a general rule they do not metastasize out of the CNS, but
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry
 Original Article Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry Badhe Prerna B, Chauhan Pritika P, Mehta Nishaki K Departments of Pathology, Seth G. S. Medical
Original Article Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry Badhe Prerna B, Chauhan Pritika P, Mehta Nishaki K Departments of Pathology, Seth G. S. Medical
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Dr Eddie Mee. Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland
 Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
Dr Eddie Mee Neurosurgeon Auckland City Hospital, Ascot Integrated Hospital, MercyAscot Hospitals, Auckland 16:30-17:25 WS #48: Current Management of Brain Bleeds and Tumours 17:35-18:30 WS #58: Current
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia
 A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
A Population-Based Study on the Uptake and Utilization of Stereotactic Radiosurgery (SRS) for Brain Metastasis in Nova Scotia Gaurav Bahl, Karl Tennessen, Ashraf Mahmoud-Ahmed, Dorianne Rheaume, Ian Fleetwood,
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Liver Tumors. Prof. Dr. Ahmed El - Samongy
 Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
Liver Tumors Prof. Dr. Ahmed El - Samongy Objective 1. Identify the most important features of common benign liver tumors 2. Know the risk factors, diagnosis, and management of hepatocellular carcinoma
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Leptomeningeal metastasis: management and guidelines. Emilie Le Rhun Lille, FR Zurich, CH
 Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors
 AJNR Am J Neuroradiol 25:476 480, March 2004 Case Report Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors Atilla Arslanoglu, Nafi Aygun, Deapak Tekhtani, Leslie Aronson, Ken Cohen, Peter C. Burger,
AJNR Am J Neuroradiol 25:476 480, March 2004 Case Report Imaging Findings of CNS Atypical Teratoid/Rhabdoid Tumors Atilla Arslanoglu, Nafi Aygun, Deapak Tekhtani, Leslie Aronson, Ken Cohen, Peter C. Burger,
Scottish Medicines Consortium
 Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
Scottish Medicines Consortium temozolomide 5, 20, 100 and 250mg capsules (Temodal ) Schering Plough UK Ltd No. (244/06) New indication: for the treatment of newly diagnosed glioblastoma multiforme concomitantly
Pediatric Spine Tumors (and other masses)
 Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Ductal Carcinoma-in-Situ: New Concepts and Controversies
 Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Challenging Paediatric Brain Tumours. ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin
 Challenging Paediatric Brain Tumours ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin Overview (i) Paediatric malignancy (ii) Central nervous system tumours (iii) Diffuse Intrinsic
Challenging Paediatric Brain Tumours ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin Overview (i) Paediatric malignancy (ii) Central nervous system tumours (iii) Diffuse Intrinsic
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Case Scenario. 7/13/12 Anterior floor of mouth biopsy: Infiltrating squamous cell carcinoma, not completely excised.
 Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org The Role of Radiosurgery in the Treatment of Gliomas Luis Souhami, MD Professor Department of Radiation
Structural and functional imaging for the characterization of CNS lymphomas
 Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
PROCARBAZINE, lomustine, and vincristine (PCV) is
 RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
RAPID PUBLICATION Procarbazine, Lomustine, and Vincristine () Chemotherapy for Anaplastic Astrocytoma: A Retrospective Review of Radiation Therapy Oncology Group Protocols Comparing Survival With Carmustine
Corporate Medical Policy
 Corporate Medical Policy Brachytherapy, Intracavitary Balloon Catheter for Brain Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_intracavitary_balloon_catheter_for_brain_cancer
Corporate Medical Policy Brachytherapy, Intracavitary Balloon Catheter for Brain Cancer File Name: Origination: Last CAP Review: Next CAP Review: Last Review: brachytherapy_intracavitary_balloon_catheter_for_brain_cancer
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
Oligodendrogliomas & Oligoastrocytomas
 Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
AMERICAN BRAIN TUMOR ASSOCIATION. Oligodendroglioma and Oligoastrocytoma
 AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
