Comparison of Pencil Beam Scanning Proton- and Photon-Based Techniques for Carcinoma of the Parotid
|
|
|
- Ruby Montgomery
- 5 years ago
- Views:
Transcription
1 Comparison of Pencil Beam Scanning Proton- and Photon-Based Techniques for Carcinoma of the Parotid Samuel Swisher-McClure, MD; Boon-Keng Kevin Teo, PhD; Maura Kirk, MS; Chang Chang, PhD; and Alexander Lin, MD Department of Radiation Oncology, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA, USA Abstract Submitted 16 Feb 2015 Accepted 16 Sep 2015 Published 24 Mar 2016 Corresponding author: Samuel Swisher-McClure 3400 Civic Center Blvd, TRC 4-West Philadelphia, PA 19104, USA Phone: (215) Fax: (215) upenn.edu Original Article DOI /IJPT * cc Copyright 2016 International Journal of Particle Therapy Distributed under Creative Commons CC-BY OPEN ACCESS Purpose: To report the dosimetric advantages of a comparison between pencil beam scanning (PBS) proton therapy versus intensity-modulated radiation therapy (IMRT) for parotid gland cancers. Patients and Methods: This was a retrospective, dosimetric comparison of 8 patients who received external beam radiation therapy at our institution between 2009 and Two separate plans were generated for each patient: 1 IMRT and 1 PBS plan. The prescription dose for each plan was 60 Gy for IMRT and 60 Gy (RBE) for PBS. We measured dose-volume relationships for target volumes and organs at risk with each treatment technique. Dosimetric comparisons for each organ at risk were made by using the Wilcoxon signed rank test. All tests were 2-tailed, with P values,.05 considered statistically significant. Results: The mean patient planning target volume was cm 3 (SD 74.6). Pencil beam scanning, compared to IMRT, significantly reduced the mean dose to the following structures: ipsilateral temporal lobe (2.86 versus 9.59 Gy (RBE), P ¼.01), oral cavity (0.58 versus Gy (RBE), P ¼.01), mandible (V 50 : 7.4% versus 12.8%, P ¼.01), contralateral parotid gland (0.003 versus 4.64 Gy (RBE), P ¼.01), ipsilateral submandibular gland (16.59 versus Gy (RBE), P ¼.03), and contralateral submandibular gland (0.02 versus 5.34 Gy (RBE), P ¼.01). Pencil beam scanning also significantly reduced the maximum dose delivered to the brainstem (7.1 versus 30.9 Gy (RBE), P ¼.01). Conclusion: Pencil beam scanning allows for superior normal tissue sparing while still maintaining excellent target coverage in patients with resected parotid gland cancers. These findings suggest that PBS may allow for an improved therapeutic index for these patients. Clinical outcomes with PBS should be evaluated prospectively, with a focus on disease outcomes as well as treatment-related toxicities and patient quality of life. Keywords: proton therapy; pencil beam scanning; head and neck cancer; parotid cancer Introduction Patients with a diagnosis of malignant major salivary gland carcinomas frequently receive radiation therapy (RT) as part of their treatment either following surgery or as definitive treatment for unresectable disease. In the postoperative setting, doses 56 Gy have been associated with improvements in local control [1]; however, such treatment may also be associated with significant treatment-related toxicity including mucositis;
2 xerostomia; hearing loss; and rarely, temporal lobe necrosis. Proton therapy may offer an improved therapeutic index in this setting by reducing dose to adjacent organs at risk (OARs). Proton therapy may be particularly advantageous in the treatment of parotid carcinomas, compared to other head and neck cancers, given that the treatment fields generally target the unilateral base of skull and upper neck. The sharp dose gradient, possible by virtue of the Bragg peak, may allow for improved avoidance of adjacent structures such as the cochlea, the temporal lobe of the brain, the mandible, or the oral cavity. In addition, reduced integral dose through proton therapy for structures such as the oral cavity, submandibular glands, and contralateral parotid glands may help to reduce or avoid longterm xerostomia for patients. Several studies [2 12] have suggested potential dosimetric advantages associated with the use of proton therapy for other head and neck cancers. However, relatively little has been published regarding the use of protons to treat carcinomas of the major salivary glands. We therefore conducted a retrospective treatment planning study to compare intensity-modulated radiation therapy (IMRT) with pencil beam scanning (PBS) proton therapy in a series of patients receiving treatment for parotid gland carcinoma at our institution. Methods and Materials Study Design and Patient Population This study retrospectively compared dosimetric endpoints by radiation treatment technique among patients receiving treatment for parotid carcinoma. We identified 8 patients receiving external beam radiation therapy (EBRT) for parotid carcinoma at our institution between December 2009 and July Most patients in our study had undergone resection of carcinoma involving the parotid and were recommended to receive adjuvant RT. In addition, we also included 3 patients with disease who received RT alone for disease that was deemed unresectable by our head and neck surgeons. Simulation and Treatment Planning All patients underwent computed tomography (CT) simulation with axial images acquired at 1.5- to 3.0-mm increments. Thermoplastic masks were used for immobilization of the head and neck. Computed tomography images were imported into a commercial treatment planning software (Eclipse, Varian Medical Systems, Palo Alto, California), which was used for both photon and proton treatment planning. Target volumes and normal OARs were contoured by 2 radiation oncologists with significant experience treating head and neck cancer. Gross tumor volumes in patients with unresected disease were based on clinical examination and imaging findings including CT, magnetic resonance imaging, or positron emission tomography/ct. Clinical target volumes (CTVs) were customized for each patient to account for microscopic or subclinical extension of disease. The CTV included the ipsilateral cervical lymph nodes in 3 patients and tracked the facial nerve to the base of skull in 5 patients. Consistent with our institutional policy, each CTV was expanded 3 mm to a planning target volume (PTV) to account for organ motion and setup variation. The PTV was then cropped from the skin by 3 mm for planning optimization purposes. From methods established by Moyers et al [13], proton margins were calculated as 3.5% of the range with an additional 1 mm for beam delivery uncertainty. Owing to the shallow depth of the parotid targets, the largest calculated margin for range uncertainty was 4.5 mm. Since the PTV expansion was a uniform 5 mm from the CTV, which was larger than the calculated range uncertainty margins, the same PTV was used for PBS optimization to be conservative. The proton plans were therefore calculated with a 5-mm range uncertainty margin from the CTV, which is equivalent to the PTV margin for the photon plans. No modifications of OAR contours were made for planning between the 2 modalities. The OARs evaluated for each patient included ipsilateral cochlea, ipsilateral temporal lobe, brainstem, oral cavity, mandible, contralateral parotid gland, and bilateral submandibular glands. The same target and OAR structures in each patient were used for all EBRT treatment plans generated. We developed separate treatment plans for each study patient by using the following techniques: (1) 5-field IMRT and (2) PBS proton beam therapy using a single field. The PBS treatment plans were optimized by using customized bolus to reduce spot size and resultant penumbra [14]. Single-field PBS plans have been used to treat shallow targets with reliable bony alignment such as with the spine field of a craniospinal treatment. For the purposes of the study, a worst-case scenario robustness analysis was performed by forward calculating the nominal plans by using 3-mm isocenter shifts in 6 directions (6x, 6y, 6z) and 6 3.5% shifts in the Hounsfield unit. The minimum CTV D 95 among all parameters of all cases was 95%, and the mean CTV D 95 worst-case scenario from each of the patients was 97% 6 1%. All treatment plans evaluated for the Swisher-McClure et al. (2016), Int J Particle Ther 526
3 Table 1. Characteristics of the study population. Patient No. Primary histologic profile T stage N stage PTV volume, cm 3 Neck targeted Facial nerve targeted to base of skull Unresectable disease 1 Cutaneous squamous cell carcinoma Tx N2a No Yes Yes 2 Adenoid cystic carcinoma T1 N0 49 No Yes No 3 Recurrent acinic cell carcinoma T4a N No Yes No 4 Recurrent pleomorphic adenoma T1 N No No No 5 Cutaneous squamous cell carcinoma Tx N2b Yes Yes No 6 Cutaneous basal cell carcinoma T4 N No Yes No. 7 High-grade mucoepidermoid carcinoma T4b N Yes Yes Yes 8 Carcinoma ex pleomorphic adenoma T4b N2b Yes No Yes Abbreviation: PTV, planned target volume. purposes of the study were developed by a single physicist with experience in both head and neck cancer and proton treatment planning (B.-K.K.T.). The prescription dose for each plan was 60 Gy for photon plans or 60 Gy (RBE) for proton plans, using a conversion factor of 1.1 relative biological effectiveness (RBE) [15]. This uniform dose was selected for the sake of simplicity in the study, with the understanding that patients with positive surgical margins or unresectable disease will typically receive EBRT doses. 60 Gy. In all cases, plans provided dose coverage such that 95% of the planning target volume received at least 95% of the prescription dose. Analysis We measured dose-volume relationships for target volumes, and OAR (ipsilateral cochlea, ipsilateral temporal lobe, brainstem, mandible, oral cavity, contralateral parotid gland, bilateral submandibular glands) with each treatment technique. Using Wilcoxon signed rank test, we performed pair-wise comparisons of dose parameters with PBS versus IMRT for each OAR. All tests were 2-tailed and P values,.05 were considered statistically significant. Statistical analyses were conducted by using Stata version 12 (College Station, Texas). Results Characteristics of the Study Population The characteristics of the study population are displayed in Table 1. Five patients (63%) were treated for a primary parotid carcinoma, while 3 patients (37%) received treatment for cutaneous malignancies involving the parotid gland. Three patients received RT for disease that was unresectable owing to base of skull involvement. The facial nerve was specifically targeted to the base of skull (stylomastoid foramen) in 6 patients (75%). The mean patient PTV volume was cm 3 (SD 74.6). Comparison of Dose to Normal Structures Using IMRT versus PBS The comparative distribution of dose to normal structures for all study patients, using IMRT and PBS, is shown in Figure 1. A representative comparison of dose distribution and dose-volume histograms between IMRT and PBS treatment plans for a single study patient can be seen in Figure 2. Descriptive statistics and the results of univariate statistical comparisons are shown in Table 2. Ipsilateral Cochlea Pencil beam scanning did not result in a statistically significant reduction in the mean dose to the ipsilateral cochlea when compared to IMRT (P ¼.16). The average mean cochlear dose was 1.49 Gy (RBE) with IMRT and 1.10 Gy (RBE) with PBS. Ipsilateral Temporal Lobe The PBS technique resulted in a statistically significant reduction in the mean dose to the ipsilateral temporal lobe when compared to IMRT (P ¼.012). The average mean temporal lobe dose was 9.59 Gy (RBE) with IMRT versus 2.86 Gy (RBE) Swisher-McClure et al. (2016), Int J Particle Ther 527
4 Figure 1. Comparative distributions of doses to normal structures, using IMRT versus PBS proton therapy. Abbreviations: IMRT, intensity-modulated radiation therapy; PBS, pencil beam scanning. with PBS. The average maximum temporal lobe dose was also reduced with PBS compared to IMRT (25.0 Gy (RBE) versus Gy (RBE), respectively). However, this reduction was not statistically significant (P ¼.09). Oral Cavity Dose to the oral cavity was nearly eliminated when using PBS (Figure 1). The average mean oral cavity dose with PBS was 0.58 Gy (RBE), compared to Gy (RBE) with IMRT. Pencil beam scanning resulted in a statistically significant reduction in the mean oral cavity dose when compared to IMRT (P ¼.01). Brainstem Similarly, dose to the brainstem was minimal when using PBS. The average maximum brainstem dose was 7.1 Gy (RBE) with PBS, compared to 30.9 Gy (RBE) when using IMRT. Pencil beam scanning resulted in a statistically significant reduction in the maximum brainstem dose when compared to IMRT (P ¼.01). Mandible The maximum point doses to the mandible for each patient, using IMRT and PBS, were similar. The average maximum dose to 0.03 cm 3 of the mandible was Gy (RBE) with IMRT and Gy (RBE) with PBS. There was no statistically significant difference in the maximum mandibular dose between IMRT and PBS (P ¼.67). The mandibular V 50 (volume of the organ Swisher-McClure et al. (2016), Int J Particle Ther 528
5 Table 2. Comparison of doses to normal structures using IMRT and PBS proton therapy. IMRT PBS Dose, Gy (RBE) Dose, Gy (RBE) P value Ipsilateral cochlea Mean dose 1.49 (1.64) 1.10 (2.00).16 Ipsilateral temporal lobe Mean dose 9.59 (12.59) 2.86 (7.02).01 Maximum dose 25.0 (26.0) (22.72).09 Brainstem Maximum dose (10.34) 7.10 (15.44).01 Oral cavity Mean dose (6.53) 0.58 (1.61).01 Mandible Dose to 0.03 cm (2.18) (1.62).16 V 50, % 12.8 (8.62) 7.4 (5.34).01 Contralateral parotid Mean dose 4.64 (2.13) (0).01 Ipsilateral submandibular gland Mean dose (14.24) (8.64).03 Contralateral submandibular gland Mean dose 5.34 (3.21) 0.02 (0.06).01 Abbreviations: IMRT, intensity-modulated radiation therapy; PBS, pencil beam scanning. a Doses reported in the table reflect the arithmetic mean of each dose parameter for the respective normal structures. Standard deviations are provided in parentheses. P values reflect the results of the Wilcoxon signed rank test for each comparison. receiving 50 Gy (RBE) was 12.8% with IMRT, compared to 7.4% when using PBS. Pencil beam scanning resulted in a statistically significant reduction in the mandibular V 50 when compared to IMRT (P ¼.01) Contralateral Parotid Gland Contralateral parotid dose was nearly eliminated when using PBS. The average mean dose to the contralateral parotid gland was 4.64 Gy (RBE) with IMRT and Gy (RBE) with PBS. The PBS technique resulted in a statistically significant reduction in the mean dose to the contralateral parotid gland when compared to IMRT (P ¼.01). Ipsilateral Submandibular Gland In 2 patients, the ipsilateral submandibular glands were located entirely within the treatment target volume. Therefore, doses were only compared for the remaining 6 patients in whom at least a portion of the submandibular gland was located outside the treatment target volume. Pencil beam scanning resulted in a statistically significant reduction in the mean dose to the ipsilateral submandibular gland when compared to IMRT (P ¼.03). The average mean dose to the ipsilateral submandibular gland was Gy (RBE) with IMRT, compared to Gy (RBE) when using PBS. Contralateral Submandibular Gland Pencil beam scanning again nearly eliminated dose to the contralateral submandibular gland. The average mean dose to the contralateral submandibular gland was 5.34 cgy with IMRT versus 0.02 Gy (RBE) with PBS. Pencil beam scanning resulted in a statistically significant reduction in the mean dose to the contralateral submandibular gland when compared to IMRT (P ¼.01). Discussion Our study demonstrates that in patients receiving radiation therapy for cancers of the parotid, treatment with a PBS protonbased approach delivers significantly less radiation exposure to adjacent normal OARs than an IMRT photon-based approach. This study is the first of its kind to compare the most advanced technique of both proton and photon therapy for the treatment of parotid malignancies. Swisher-McClure et al. (2016), Int J Particle Ther 529
6 Figure 2. A representative comparison of dose distribution and dose-volume histograms between intensity-modulated radiation therapy and pencil beam scanning proton plans for a single study patient. Unlike more common malignancies of the head and neck, salivary gland cancers are relatively rare, with an overall incidence in the population of 0.9 to 4.0 cases per persons per year [16]. Therefore, the ability to perform large-scale, comparative randomized trials in this population is limited, and dosimetric comparisons such as this may be helpful in determining the optimal radiation approach for treating these patients. The treatment of other types of head and neck cancer with external-beam photon-based RT can cause severe late effects [17 23] and impact posttreatment quality of life [19]. A pencil-beam proton-based approach for parotid cancers, we believe, is currently the optimal approach to minimize potential acute and long-term side effects for those requiring RT. There are several limitations to our study that warrant mention. This study describes a PBS-based approach and compares its dosimetric results to an IMRT plan. However, the safe clinical implementation of PBS requires stringent technical and quality assurance, with issues such as daily variation in patient positioning [24], anatomic changes that occur during the course of treatment [25], and the inherent uncertainties associated with proton beam delivery. The intensity-modulated proton therapy technique was not used for this planning study owing to its sensitivity to treatment uncertainties [26 28], and a more robust uniform dose technique was used. Additionally, the question of whether significant decreases in doses to OARs with proton Swisher-McClure et al. (2016), Int J Particle Ther 530
7 therapy leads to improvement in patient outcomes remains unanswered and requires clinical follow-up. However, given that previous level 1 evidence demonstrated that improved salivary gland sparing with IMRT (versus conventional RT) reduced the severity of xerostomia and consequently improved quality of life [29], we would expect that the improved normal tissue sparing seen with PBS should produce similar benefits. In summary, given the demonstrated dosimetric advantages achievable with PBS proton therapy, we would advocate for the clinical implementation of such a technique in the treatment of patients with parotid malignancies. Careful attention needs to be made to ensure treatment quality assurance, as well as reporting of long-term clinical outcomes. ADDITIONAL INFORMATION AND DECLARATIONS Conflicts of Interest: The authors have no conflicts to disclose. References 1. Garden AS, Weber RS, Morrison WH, Ang KK, Peters LJ. The influence of positive margins and nerve invasion in adenoid cystic carcinoma of the head and neck treated with surgery and radiation. Int J Radiat Oncol Biol Phys. 1995;32: Quan EM, Liu W, Wu R, Li Y, Frank SJ, Zhang X, Zhu XR, Mohan R. Preliminary evaluation of multifield and single-field optimization for the treatment planning of spot-scanning proton therapy of head and neck cancer. Med Phys. 2013;40: Kandula S, Zhu X, Garden AS, Gillin M, Rosenthal DI, Ang KK, Mohan R, Amin MV, Garcia JA, Wu R, Sahoo N, Frank SJ. Spot-scanning beam proton therapy vs intensity-modulated radiation therapy for ipsilateral head and neck malignancies: a treatment planning comparison. Med Dosim. 2013;38: Ramaekers BL, Grutters JP, Pijls-Johannesma M, Lambin P, Joore MA, Langendijk JA. Protons in head-and-neck cancer: bridging the gap of evidence. Int J Radiat Oncol Biol Phys. 2013;85: Liu SW, Li JM, Chang JY, Yu JM, Chen Q, Jiang QA, Mu XK, Zhao MH, Tian Y, Wei QL. A treatment planning comparison between proton beam therapy and intensity-modulated x-ray therapy for recurrent nasopharyngeal carcinoma. J Xray Sci Technol. 2010;18: Simone CB II, Ly D, Dan TD, Ondos J, Ning H, Belard A, O Connell J, Miller RW, Simone NL. Comparison of intensitymodulated radiotherapy, adaptive radiotherapy, proton radiotherapy, and adaptive proton radiotherapy for treatment of locally advanced head and neck cancer. Radiother Oncol. 2011;101: van de Water TA, Lomax AJ, Bijl HP, de Jong ME, Schilstra C, Hug EB, Langendijk JA. Potential benefits of scanned intensity-modulated proton therapy versus advanced photon therapy with regard to sparing of the salivary glands in oropharyngeal cancer. Int J Radiat Oncol Biol Phys. 2011;79: van der Laan HP, van de Water TA, van Herpt HE, Christianen ME, Bijl HP, Korevaar EW, Rasch CR, van t Veld AA, van der Schaaf A, Schilstra C, Langendijk JA. The potential of intensity-modulated proton radiotherapy to reduce swallowing dysfunction in the treatment of head and neck cancer: a planning comparative study. Acta Oncol. 2013;52: Chera BS, Malyapa R, Louis D, Mendenhall WM, Li Z, Lanza DC, Yeung D, Mendenhall NP. Proton therapy for maxillary sinus carcinoma. Am J Clin Oncol. 2009;32: Cozzi L, Fogliata A, Lomax A, Bolsi A. A treatment planning comparison of 3D conformal therapy, intensity modulated photon therapy and proton therapy for treatment of advanced head and neck tumours. Radiother Oncol. 2001;61: Steneker M, Lomax A, Schneider U. Intensity modulated photon and proton therapy for the treatment of head and neck tumors. Radiother Oncol. 2006;80: Widesott L, Pierelli A, Fiorino C, Dell oca I, Broggi S, Cattaneo GM, Di Muzio N, Fazio F, Calandrino R, Schwarz M. Intensity-modulated proton therapy versus helical tomotherapy in nasopharynx cancer: planning comparison and NTCP evaluation. Int J Radiat Oncol Biol Phys. 2008;72: Moyers MF, Miller DW, Bush DA, Slater JD. Methodologies and tools for proton beam design for lung tumors. Int J Radiat Oncol Biol Phys. 2001;49: Both S, Shen J, Kirk M, Lin L, Tang S, Alonso-Basanta M, Lustig R, Lin H, Deville C, Hill-Kayser C, Tochner Z, McDonough J. Development and clinical implementation of a universal bolus to maintain spot size during delivery of base of skull pencil beam scanning proton therapy. Int J Radiat Oncol Biol Phys. 2014;90: Swisher-McClure et al. (2016), Int J Particle Ther 531
8 15. Gerweck LE, Kozin SV. Relative biological effectiveness of proton beams in clinical therapy. Radiother Oncol. 1999;50: Pinkston JA, Cole P. Incidence rates of salivary gland tumors: results from a population-based study. Otolaryngol Head Neck Surg. 1999;120: Dorresteijn LD, Kappelle AC, Boogerd W, Klokman WJ, Balm AJ, Keus RB, van Leeuwen FE, Bartelink H. Increased risk of ischemic stroke after radiotherapy on the neck in patients younger than 60 years. J Clin Oncol. 2002;20: Eisbruch A, Lyden T, Bradford CR, Dawson LA, Haxer MJ, Miller AE, Teknos TN, Chepeha DB, Hogikyan ND, Terrell JE, Wolf GT. Objective assessment of swallowing dysfunction and aspiration after radiation concurrent with chemotherapy for head-and-neck cancer. Int J Radiat Oncol Biol Phys. 2002;53: Lin A, Kim HM, Terrell JE, Dawson LA, Ship JA, Eisbruch A. Quality of life after parotid-sparing IMRT for head-and-neck cancer: a prospective longitudinal study. Int J Radiat Oncol Biol Phys. 2003;57: Smith GL, Smith BD, Buchholz TA, Giordano SH, Garden AS, Woodward WA, Krumholz HM, Weber RS, Ang KK, Rosenthal DI. Cerebrovascular disease risk in older head and neck cancer patients after radiotherapy. J Clin Oncol. 2008; 26: Smith GL, Smith BD, Garden AS, Rosenthal DI, Sherman SI, Morrison WH, Schwartz DL, Weber RS, Buchholz TA. Hypothyroidism in older patients with head and neck cancer after treatment with radiation: a population-based study. Head Neck. 2009;31: Swisher-McClure S, Mitra N, Lin A, Ahn P, Wan F, O Malley B, Weinstein GS, Bekelman JE. Risk of fatal cerebrovascular accidents after external beam radiation therapy for early-stage glottic laryngeal cancer. Head Neck. 2014;36: Tsai CJ, Hofstede TM, Sturgis EM, Garden AS, Lindberg ME, Wei Q, Tucker SL, Dong L. Osteoradionecrosis and radiation dose to the mandible in patients with oropharyngeal cancer. Int J Radiat Oncol Biol Phys. 2013;85: Ahn PH, Ahn AI, Lee CJ, Shen J, Miller E, Lukaj A, Milan E, Yaparpalvi R, Kalnicki S, Garg MK. Random positional variation among the skull, mandible, and cervical spine with treatment progression during head-and-neck radiotherapy. Int J Radiat Oncol Biol Phys. 2009;73: Ahn PH, Chen CC, Ahn AI, Hong L, Scripes PG, Shen J, Lee CC, Miller E, Kalnicki S, Garg MK. Adaptive planning in intensity-modulated radiation therapy for head and neck cancers: single-institution experience and clinical implications. Int J Radiat Oncol Biol Phys. 2011;80: Kraan AC, van de Water S, Teguh DN, Al-Mamgani A, Madden T, Kooy HM, Heijmen BJ, Hoogeman MS. Dose uncertainties in IMPT for oropharyngeal cancer in the presence of anatomical, range, and setup errors. Int J Radiat Oncol Biol Phys. 2013;87: Lomax AJ. Intensity modulated proton therapy and its sensitivity to treatment uncertainties 2: the potential effects of interfraction and inter-field motions. Phys Med Biol. 2008;53: Lomax AJ. Intensity modulated proton therapy and its sensitivity to treatment uncertainties 1: the potential effects of calculational uncertainties. Phys Med Biol. 2008;53: Nutting CM, Morden JP, Harrington KJ, Urbano TG, Bhide SA, Clark C, Miles EA, Miah AB, Newbold K, Tanay M, Adab F, Jefferies SJ, Scrase C, Yap BK, A Hern RP, Sydenham MA, Emson M, Hall E. Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol. 2011;12: Swisher-McClure et al. (2016), Int J Particle Ther 532
Potential Impact of Daily Setup Variation on Pencil-Beam Scanning for Head and Neck Cancer
 Potential Impact of Daily Setup Variation on Pencil-Beam Scanning for Head and Neck Cancer Kanograt Tangsriwong, MD; Maura Kirk, MS; Stefan Both, PhD; and Alexander Lin, MD Department of Radiation Oncology,
Potential Impact of Daily Setup Variation on Pencil-Beam Scanning for Head and Neck Cancer Kanograt Tangsriwong, MD; Maura Kirk, MS; Stefan Both, PhD; and Alexander Lin, MD Department of Radiation Oncology,
Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer
 1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
1 Charles Poole April Case Study April 30, 2012 Evaluation of Whole-Field and Split-Field Intensity Modulation Radiation Therapy (IMRT) Techniques in Head and Neck Cancer Abstract: Introduction: This study
Proton therapy for head and neck cancer: current applications and future directions
 Review Article Proton therapy for head and neck cancer: current applications and future directions Alexander Lin, Samuel Swisher-McClure, Laura Bonner Millar, Maura Kirk, Caitlyn Yeager, Ali Kassaee, Boong-Keng
Review Article Proton therapy for head and neck cancer: current applications and future directions Alexander Lin, Samuel Swisher-McClure, Laura Bonner Millar, Maura Kirk, Caitlyn Yeager, Ali Kassaee, Boong-Keng
Protocol of Radiotherapy for Head and Neck Cancer
 106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
4/25/2018. Proton Therapy for Head and Neck Cancer: The Future is Now. Disclosures. Overview. Physical limitations of photons
 Proton Therapy for Head and Neck Cancer: The Future is Now Michael Chuong, MD Radiation Oncologist Disclosures None Overview Physical limitations of photons Dosimetric/clinical proton data for HNC Proton
Proton Therapy for Head and Neck Cancer: The Future is Now Michael Chuong, MD Radiation Oncologist Disclosures None Overview Physical limitations of photons Dosimetric/clinical proton data for HNC Proton
Martin Stuschke 1,2*, Andreas Kaiser 1,2, Jehad Abu Jawad 1, Christoph Pöttgen 1, Sabine Levegrün 1 and Jonathan Farr 2,3
 Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
Key Words. Proton therapy Head and neck cancer Radiotherapy In silico treatment planning Radiation-induced side effects
 The Oncologist Radiation Oncology The Potential Benefit of Radiotherapy with Protons in Head and Neck Cancer with Respect to Normal Tissue Sparing: A Systematic Review of Literature TARA A. VAN DE WATER,
The Oncologist Radiation Oncology The Potential Benefit of Radiotherapy with Protons in Head and Neck Cancer with Respect to Normal Tissue Sparing: A Systematic Review of Literature TARA A. VAN DE WATER,
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Whoon Jong Kil, MD 1,2 Christina Kulasekere, CMD 1 Craig Hatch, DMD 1 Jacob Bugno, PhD 1 Ronald Derrwaldt, DO 1. Abstract INTRODUCTION CASE REPORT
 Received: 17 January 2017 Revised: 23 February 2017 Accepted: 14 March 2017 DOI: 10.1002/hed.24809 CASE REPORT Tongue-out versus tongue-in position during intensity-modulated radiotherapy for base of tongue
Received: 17 January 2017 Revised: 23 February 2017 Accepted: 14 March 2017 DOI: 10.1002/hed.24809 CASE REPORT Tongue-out versus tongue-in position during intensity-modulated radiotherapy for base of tongue
Clinical Education A comprehensive and specific training program. carry out effective treatments from day one
 Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Protons for Head and Neck Cancer. William M Mendenhall, M.D.
 Protons for Head and Neck Cancer William M Mendenhall, M.D. Protons for Head and Neck Cancer Potential Advantages: Reduce late complications via more conformal dose distributions Likely to be the major
Protons for Head and Neck Cancer William M Mendenhall, M.D. Protons for Head and Neck Cancer Potential Advantages: Reduce late complications via more conformal dose distributions Likely to be the major
Chapter 2. Level II lymph nodes and radiation-induced xerostomia
 Chapter 2 Level II lymph nodes and radiation-induced xerostomia This chapter has been published as: E. Astreinidou, H. Dehnad, C.H. Terhaard, and C.P Raaijmakers. 2004. Level II lymph nodes and radiation-induced
Chapter 2 Level II lymph nodes and radiation-induced xerostomia This chapter has been published as: E. Astreinidou, H. Dehnad, C.H. Terhaard, and C.P Raaijmakers. 2004. Level II lymph nodes and radiation-induced
Intensity-Modulated Proton Therapy Adaptive Planning for Patients with Oropharyngeal Cancer
 Intensity-Modulated Proton Therapy Adaptive Planning for Patients with Oropharyngeal Cancer Richard Y. Wu, MSc 1* and Amy Y. Liu, MSc 1* ; Terence T. Sio, MD, MS 2,4 ; Pierre Blanchard, MD, PhD 2,5 ; Cody
Intensity-Modulated Proton Therapy Adaptive Planning for Patients with Oropharyngeal Cancer Richard Y. Wu, MSc 1* and Amy Y. Liu, MSc 1* ; Terence T. Sio, MD, MS 2,4 ; Pierre Blanchard, MD, PhD 2,5 ; Cody
Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed tomography for non-operative lung cancer during adaptive
 Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
Oncology and Translational Medicine October 2015, Vol. 1, No. 5, P195 200 DOI 10.1007/s10330-015-0054-3 ORIGINAL ARTICLE Dosimetric consequences of tumor volume changes after kilovoltage cone-beam computed
Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy
 Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy Croix C. Fossum, MD 1 ; Chris J. Beltran, PhD 2 ; Thomas J. Whitaker, PhD 2 ; Daniel J. Ma, MD 2 ; Robert
Biological Model for Predicting Toxicity in Head and Neck Cancer Patients Receiving Proton Therapy Croix C. Fossum, MD 1 ; Chris J. Beltran, PhD 2 ; Thomas J. Whitaker, PhD 2 ; Daniel J. Ma, MD 2 ; Robert
IMRT - the physician s eye-view. Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia
 IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer
 Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
A Dosimetric Comparison of Whole-Lung Treatment Techniques. in the Pediatric Population
 A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
Larynx-sparing techniques using intensitymodulated radiation therapy for oropharyngeal cancer.
 Thomas Jefferson University Jefferson Digital Commons Department of Radiation Oncology Faculty Papers Department of Radiation Oncology 1-1-2012 Larynx-sparing techniques using intensitymodulated radiation
Thomas Jefferson University Jefferson Digital Commons Department of Radiation Oncology Faculty Papers Department of Radiation Oncology 1-1-2012 Larynx-sparing techniques using intensitymodulated radiation
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Alexandria University Faculty of Medicine. Alexandria Journal of Medicine.
 Alexandria Journal of Medicine (2013) 49, 379 384 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Three dimensional conformal postoperative
Alexandria Journal of Medicine (2013) 49, 379 384 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE Three dimensional conformal postoperative
Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain
 1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
1 Carol Boyd March Case Study March 11, 2013 Intensity modulated radiotherapy (IMRT) for treatment of post-operative high grade glioma in the right parietal region of brain History of Present Illness:
International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017]
![International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017] International Multispecialty Journal of Health (IMJH) ISSN: [ ] [Vol-3, Issue-9, September- 2017]](/thumbs/84/90586123.jpg) Dosimetric evaluation of carcinoma nasopharynx using Volumetric Modulated Arc Therapy (VMAT): An institutional experience from Western India Dr. Upendra Nandwana 1, Dr. Shuchita Pathak 2, Dr. TP Soni 3,
Dosimetric evaluation of carcinoma nasopharynx using Volumetric Modulated Arc Therapy (VMAT): An institutional experience from Western India Dr. Upendra Nandwana 1, Dr. Shuchita Pathak 2, Dr. TP Soni 3,
Dose variations in tumor volumes and organs at risk during IMRT for head-and-neck cancer
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 13, NUMBER 6, 2012 Dose variations in tumor volumes and organs at risk during IMRT for head-and-neck cancer Mercè Beltran, 1a Mónica Ramos, 2 Juan José
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 13, NUMBER 6, 2012 Dose variations in tumor volumes and organs at risk during IMRT for head-and-neck cancer Mercè Beltran, 1a Mónica Ramos, 2 Juan José
Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal carcinoma
 Wang et al. Radiation Oncology (2015) 10:3 DOI 10.1186/s13014-014-0307-2 RESEARCH Open Access Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal
Wang et al. Radiation Oncology (2015) 10:3 DOI 10.1186/s13014-014-0307-2 RESEARCH Open Access Rules of parotid gland dose variations and shift during intensity modulated radiation therapy for nasopharyngeal
IGRT Solution for the Living Patient and the Dynamic Treatment Problem
 IGRT Solution for the Living Patient and the Dynamic Treatment Problem Lei Dong, Ph.D. Associate Professor Dept. of Radiation Physics University of Texas M. D. Anderson Cancer Center Houston, Texas Learning
IGRT Solution for the Living Patient and the Dynamic Treatment Problem Lei Dong, Ph.D. Associate Professor Dept. of Radiation Physics University of Texas M. D. Anderson Cancer Center Houston, Texas Learning
Treatment Planning (Protons vs. Photons)
 Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Clinical Protontherapy Head and Neck cancer
 Clinical Protontherapy Head and Neck cancer Coen Rasch Department of Radiation Oncology Academic Medical Center Amsterdam No disclosures 1 Introduction Proton vsphotonin the literature Model basedindicationprotocol
Clinical Protontherapy Head and Neck cancer Coen Rasch Department of Radiation Oncology Academic Medical Center Amsterdam No disclosures 1 Introduction Proton vsphotonin the literature Model basedindicationprotocol
Volumetric modulated arc radiotherapy sparing the thyroid gland for early stage glottic cancer: A dosimetrical analysis
 ONCOLOGY LETTERS 7: 1987-1991, 2014 Volumetric modulated arc radiotherapy sparing the thyroid gland for early stage glottic cancer: A dosimetrical analysis EUN SEOK KIM and SEUNG GU YEO Department of Radiation
ONCOLOGY LETTERS 7: 1987-1991, 2014 Volumetric modulated arc radiotherapy sparing the thyroid gland for early stage glottic cancer: A dosimetrical analysis EUN SEOK KIM and SEUNG GU YEO Department of Radiation
SALIVARY GLAND TUMORS TREATED WITH ADJUVANT INTENSITY-MODULATED RADIOTHERAPY WITH OR WITHOUT CONCURRENT CHEMOTHERAPY
 doi:10.1016/j.ijrobp.2010.09.042 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 308 314, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
doi:10.1016/j.ijrobp.2010.09.042 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 308 314, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY
 ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
ONCOLOGY LETTERS 10: , 2015
 ONCOLOGY LETTERS 10: 201-205, 2015 Proton beam therapy for locally advanced and unresectable (T4bN0M0) squamous cell carcinoma of the ethmoid sinus: A report of seven cases and a literature review TAKASHI
ONCOLOGY LETTERS 10: 201-205, 2015 Proton beam therapy for locally advanced and unresectable (T4bN0M0) squamous cell carcinoma of the ethmoid sinus: A report of seven cases and a literature review TAKASHI
Osteoradionecrosis and Radiation Dose to the Mandible in Patients With Oropharyngeal Cancer
 International Journal of Radiation Oncology biology physics www.redjournal.org Clinical Investigation: Head and Neck Cancer Osteoradionecrosis and Radiation Dose to the Mandible in Patients With Oropharyngeal
International Journal of Radiation Oncology biology physics www.redjournal.org Clinical Investigation: Head and Neck Cancer Osteoradionecrosis and Radiation Dose to the Mandible in Patients With Oropharyngeal
Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma
 /, 2017, Vol. 8, (No. 16), pp: 27529-27540 Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma Xiujuan Gai 1,2,*, Yumei Wei 2,*, Hengmin
/, 2017, Vol. 8, (No. 16), pp: 27529-27540 Clinical study of the time of repeated computed tomography and replanning for patients with nasopharyngeal carcinoma Xiujuan Gai 1,2,*, Yumei Wei 2,*, Hengmin
Recurrence of nasopharyngeal carcinoma in the parotid region after parotid-gland-sparing radiotherapy
 Journal of the Formosan Medical Association (2011) 110, 655e660 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com BRIEF COMMUNICATION Recurrence of nasopharyngeal carcinoma
Journal of the Formosan Medical Association (2011) 110, 655e660 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com BRIEF COMMUNICATION Recurrence of nasopharyngeal carcinoma
To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence
 SCIENCE & TECHNOLOGY To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence Alburuj R. Rahman*, Jian Z. Wang, Dr. Z. Huang, Dr. J. Montebello Department of
SCIENCE & TECHNOLOGY To Reduce Hot Dose Spots in Craniospinal Irradiation: An IMRT Approach with Matching Beam Divergence Alburuj R. Rahman*, Jian Z. Wang, Dr. Z. Huang, Dr. J. Montebello Department of
THE INFLUENCE OF NEW IRRADIATION TECHNIQUES OF PAROTID TUMORS FOR ORAL REHABILITATION
 THE INFLUENCE OF NEW IRRADIATION TECHNIQUES OF PAROTID TUMORS FOR ORAL REHABILITATION Dragoş Iancu 1, Roxana Irina Iancu* 2 1 Gr. T. Popa" U.M.Ph. - Iași, Romania, Faculty of Dentistry, Department of Oncology-Radiotherapy
THE INFLUENCE OF NEW IRRADIATION TECHNIQUES OF PAROTID TUMORS FOR ORAL REHABILITATION Dragoş Iancu 1, Roxana Irina Iancu* 2 1 Gr. T. Popa" U.M.Ph. - Iași, Romania, Faculty of Dentistry, Department of Oncology-Radiotherapy
Volumetric variations and the effects of these differences on dosimetry during the course of volumetric modulated arc therapy for head and neck cancer
 Page 1 of 6 Medical & Radiation Oncology Volumetric variations and the effects of these differences on dosimetry during the course of volumetric modulated arc therapy for head and neck cancer S Ozdemir
Page 1 of 6 Medical & Radiation Oncology Volumetric variations and the effects of these differences on dosimetry during the course of volumetric modulated arc therapy for head and neck cancer S Ozdemir
8/1/2016. Motion Management for Proton Lung SBRT. Outline. Protons and motion. Protons and Motion. Proton lung SBRT Future directions
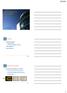 Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Practice teaching course on head and neck cancer management
 28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE LIFE THROUGH MEDICAL MEDICAL EDUCATION EDUCATION www.excemed.org
28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE LIFE THROUGH MEDICAL MEDICAL EDUCATION EDUCATION www.excemed.org
Protocol of Radiotherapy for Breast Cancer
 107 年 12 月修訂 Protocol of Radiotherapy for Breast Cancer Indication of radiotherapy Indications for Post-Mastectomy Radiotherapy (1) Axillary lymph node 4 positive (2) Axillary lymph node 1-3 positive:
107 年 12 月修訂 Protocol of Radiotherapy for Breast Cancer Indication of radiotherapy Indications for Post-Mastectomy Radiotherapy (1) Axillary lymph node 4 positive (2) Axillary lymph node 1-3 positive:
Clinical Oncology xxx (2011) 1e8. Contents lists available at SciVerse ScienceDirect. Clinical Oncology
 Clinical Oncology xxx (2011) 1e8 Contents lists available at SciVerse ScienceDirect Clinical Oncology journal homepage: www.clinicaloncologyonline.net Original Article Adaptive Radiotherapy Using Helical
Clinical Oncology xxx (2011) 1e8 Contents lists available at SciVerse ScienceDirect Clinical Oncology journal homepage: www.clinicaloncologyonline.net Original Article Adaptive Radiotherapy Using Helical
Defining Target Volumes and Organs at Risk: a common language
 Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Department of Radiotherapy & Nuclear Medicine, National Cancer Institute, Cairo University, Cairo, Egypt.
 Original article Res. Oncol. Vol. 12, No. 1, Jun. 2016:10-14 Dosimetric comparison of 3D conformal conventional radiotherapy versus intensity-modulated radiation therapy both in conventional and high dose
Original article Res. Oncol. Vol. 12, No. 1, Jun. 2016:10-14 Dosimetric comparison of 3D conformal conventional radiotherapy versus intensity-modulated radiation therapy both in conventional and high dose
A Case Study: Proton Therapy for Male Breast Cancer with Previous Irradiation
 A Case Study: Proton Therapy for Male Breast Cancer with Previous Irradiation Bosco Q. Giap, BA 1 ; Fantine Giap, BA 2 ; John P. Einck, MD 3 ; Richard LePage, PhD 4 ; Dana M. Blasongame, CMD 4 ; Angela
A Case Study: Proton Therapy for Male Breast Cancer with Previous Irradiation Bosco Q. Giap, BA 1 ; Fantine Giap, BA 2 ; John P. Einck, MD 3 ; Richard LePage, PhD 4 ; Dana M. Blasongame, CMD 4 ; Angela
Overview. Proton Therapy in lung cancer 8/3/2016 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS
 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
Specifics of treatment planning for active scanning and IMPT
 Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Margins in SBRT. Mischa Hoogeman
 Margins in SBRT Mischa Hoogeman MARGIN CONCEPTS Why do we use margins? Target / tumor To a-priori compensate for (unknown) deviations between the intended target position and the real target position during
Margins in SBRT Mischa Hoogeman MARGIN CONCEPTS Why do we use margins? Target / tumor To a-priori compensate for (unknown) deviations between the intended target position and the real target position during
Comparing proton treatment plans of pediatric brain tumors in two pencil beam scanning nozzles with different spot sizes
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Comparing proton treatment plans of pediatric brain tumors in two pencil beam scanning nozzles with different spot sizes John C. Kralik,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 6, 2015 Comparing proton treatment plans of pediatric brain tumors in two pencil beam scanning nozzles with different spot sizes John C. Kralik,
Proton therapy for prostate cancer
 Proton therapy for prostate cancer Shafak Aluwini Radiation oncologist UMCG Protons versus photons Superior beam properties 200 180 Advantage of protons 160 Photons 140 120 100 Spread out Bragg Peak 80
Proton therapy for prostate cancer Shafak Aluwini Radiation oncologist UMCG Protons versus photons Superior beam properties 200 180 Advantage of protons 160 Photons 140 120 100 Spread out Bragg Peak 80
Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment
 Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
Evaluation of three APBI techniques under NSABP B-39 guidelines
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Evaluation of three APBI techniques under NSABP B-39 guidelines Daniel Scanderbeg, a Catheryn Yashar, Greg White, Roger Rice,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 1, WINTER 2010 Evaluation of three APBI techniques under NSABP B-39 guidelines Daniel Scanderbeg, a Catheryn Yashar, Greg White, Roger Rice,
Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD. Barbara Agrimson, BS RT(T)(R), CMD
 Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD Barbara Agrimson, BS RT(T)(R), CMD Disclaimer This presentation will mention equipment by trade name.
Head and Neck Treatment Planning: A Comparative Review of Static Field IMRT RapidArc TomoTherapy HD Barbara Agrimson, BS RT(T)(R), CMD Disclaimer This presentation will mention equipment by trade name.
REVISITING ICRU VOLUME DEFINITIONS. Eduardo Rosenblatt Vienna, Austria
 REVISITING ICRU VOLUME DEFINITIONS Eduardo Rosenblatt Vienna, Austria Objective: To introduce target volumes and organ at risk concepts as defined by ICRU. 3D-CRT is the standard There was a need for a
REVISITING ICRU VOLUME DEFINITIONS Eduardo Rosenblatt Vienna, Austria Objective: To introduce target volumes and organ at risk concepts as defined by ICRU. 3D-CRT is the standard There was a need for a
Specification of Tumor Dose. Prescription dose. Purpose
 Specification of Tumor Dose George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Prescription dose What do we mean by a dose prescription of 63 Gy? Isocenter dose
Specification of Tumor Dose George Starkschall, Ph.D. Department of Radiation Physics U.T. M.D. Anderson Cancer Center Prescription dose What do we mean by a dose prescription of 63 Gy? Isocenter dose
biij Initial experience in treating lung cancer with helical tomotherapy
 Available online at http://www.biij.org/2007/1/e2 doi: 10.2349/biij.3.1.e2 biij Biomedical Imaging and Intervention Journal CASE REPORT Initial experience in treating lung cancer with helical tomotherapy
Available online at http://www.biij.org/2007/1/e2 doi: 10.2349/biij.3.1.e2 biij Biomedical Imaging and Intervention Journal CASE REPORT Initial experience in treating lung cancer with helical tomotherapy
Proton Stereotactic Radiotherapy: Clinical Overview. Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS
 Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
IMRT/IGRT Patient Treatment: A Community Hospital Experience. Charles M. Able, Assistant Professor
 IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING
 PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System. Prof. Anne Laprie Radiation Oncologist
 The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System Prof. Anne Laprie Radiation Oncologist Disclosure & Disclaimer An honorarium is provided by Accuray for this presentation The views
The PreciseART Approach to Adaptive Radiotherapy with the RADIXACT System Prof. Anne Laprie Radiation Oncologist Disclosure & Disclaimer An honorarium is provided by Accuray for this presentation The views
Long-term parotid gland function after radiotherapy
 Parotid gland sparing radiotherapy, P.M. Braam Chapter 2 Long-term parotid gland function after radiotherapy Pètra M. Braam 1, Judith M. Roesink 1, Marinus A. Moerland 1, Cornelis P.J. Raaijmakers 1, Maria
Parotid gland sparing radiotherapy, P.M. Braam Chapter 2 Long-term parotid gland function after radiotherapy Pètra M. Braam 1, Judith M. Roesink 1, Marinus A. Moerland 1, Cornelis P.J. Raaijmakers 1, Maria
Refresher Course EAR TUMOR. Sasikarn Chamchod, MD Chulabhorn Hospital
 Refresher Course EAR TUMOR Sasikarn Chamchod, MD Chulabhorn Hospital Reference: Perez and Brady s Principles and Practice of radiation oncology sixth edition Outlines Anatomy Epidemiology Clinical presentations
Refresher Course EAR TUMOR Sasikarn Chamchod, MD Chulabhorn Hospital Reference: Perez and Brady s Principles and Practice of radiation oncology sixth edition Outlines Anatomy Epidemiology Clinical presentations
A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM *
 Romanian Reports in Physics, Vol. 66, No. 2, P. 401 410, 2014 A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM * M. D. SUDITU 1,2, D. ADAM 1,2, R. POPA 1,2, V. CIOCALTEI
Romanian Reports in Physics, Vol. 66, No. 2, P. 401 410, 2014 A VMAT PLANNING SOLUTION FOR NECK CANCER PATIENTS USING THE PINNACLE 3 PLANNING SYSTEM * M. D. SUDITU 1,2, D. ADAM 1,2, R. POPA 1,2, V. CIOCALTEI
Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer
 Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer 1- Doaa M. AL Zayat. Ph.D of medical physics, Ayadi-Al Mostakbl Oncology
Dosimetric Comparison of Intensity-Modulated Radiotherapy versus 3D Conformal Radiotherapy in Patients with Head and Neck Cancer 1- Doaa M. AL Zayat. Ph.D of medical physics, Ayadi-Al Mostakbl Oncology
Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente. F. Ricchetti (Negrar, VR)
 Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente F. Ricchetti (Negrar, VR) Adaptive RT for HN SCC day 1 Adaptive RT for HN SCC day 1 day 2 Despite adequate nutritional
Adaptive radiotherapy: le variazioni degli organi a rischio e dell anatomia del paziente F. Ricchetti (Negrar, VR) Adaptive RT for HN SCC day 1 Adaptive RT for HN SCC day 1 day 2 Despite adequate nutritional
Quality of Life of Postoperative Photon versus Proton Radiation Therapy for Oropharynx Cancer
 Quality of Life of Postoperative Photon versus Proton Radiation Therapy for Oropharynx Cancer Sonam Sharma, MD 1 ; Olivia Zhou 2 ; Reid Thompson, MD, PhD 1 ; Peter Gabriel, MD, MSE 1 ; Ara Chalian, MD
Quality of Life of Postoperative Photon versus Proton Radiation Therapy for Oropharynx Cancer Sonam Sharma, MD 1 ; Olivia Zhou 2 ; Reid Thompson, MD, PhD 1 ; Peter Gabriel, MD, MSE 1 ; Ara Chalian, MD
A treatment planning study comparing Elekta VMAT and fixed field IMRT using the varian treatment planning system eclipse
 Peters et al. Radiation Oncology 2014, 9:153 RESEARCH Open Access A treatment planning study comparing Elekta VMAT and fixed field IMRT using the varian treatment planning system eclipse Samuel Peters
Peters et al. Radiation Oncology 2014, 9:153 RESEARCH Open Access A treatment planning study comparing Elekta VMAT and fixed field IMRT using the varian treatment planning system eclipse Samuel Peters
Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D.
 Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D. Radiotherapy and Radiosurgery Dpt. Istituto Clinico Humanitas, Milan, Italy. Higher doses to the tumor Better sparing of
Utilizzo delle tecniche VMAT nei trattamenti del testa collo Marta Scorsetti M.D. Radiotherapy and Radiosurgery Dpt. Istituto Clinico Humanitas, Milan, Italy. Higher doses to the tumor Better sparing of
Management of Salivary Gland Malignancies. No Disclosures or Conflicts of Interest. Anatomy 10/4/2013
 Management of Salivary Gland Malignancies Daniel G. Deschler, MD Director: Division of Head and Neck Surgery Massachusetts Eye & Ear Infirmary Massachusetts General Hospital Professor Harvard Medical School
Management of Salivary Gland Malignancies Daniel G. Deschler, MD Director: Division of Head and Neck Surgery Massachusetts Eye & Ear Infirmary Massachusetts General Hospital Professor Harvard Medical School
Self-Assessment Module 2016 Annual Refresher Course
 LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas
 A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas Reid F. Thompson University of Pennsylvania, Philadelphia, Pennsylvania 1914 Sonal U. Mayekar Thomas
A dosimetric comparison of proton and photon therapy in unresectable cancers of the head of pancreas Reid F. Thompson University of Pennsylvania, Philadelphia, Pennsylvania 1914 Sonal U. Mayekar Thomas
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care
 Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013
 Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes
 Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes Richard Choo, MD 1 ; Bret Kazemba, CMD 1 ; Christopher S. Choo, MD 2 ; Scott C. Lester, MD 1 ; Thomas
Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes Richard Choo, MD 1 ; Bret Kazemba, CMD 1 ; Christopher S. Choo, MD 2 ; Scott C. Lester, MD 1 ; Thomas
Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes
 Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes Richard Choo, MD 1 ; Bret Kazemba, CMD 1 ; Christopher S. Choo, MD 2 ; Scott C. Lester, MD 1 ; Thomas
Proton Therapy for Stage IIA-B Seminoma: A New Standard of Care for Treating Retroperitoneal Nodes Richard Choo, MD 1 ; Bret Kazemba, CMD 1 ; Christopher S. Choo, MD 2 ; Scott C. Lester, MD 1 ; Thomas
Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 12, NUMBER 2, spring 2011 Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma Chris Beltran, a Saumya Sharma, and Thomas
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 12, NUMBER 2, spring 2011 Role of adaptive radiation therapy for pediatric patients with diffuse pontine glioma Chris Beltran, a Saumya Sharma, and Thomas
Chapter 7 General conclusions and suggestions for future work
 Chapter 7 General conclusions and suggestions for future work Radiation therapy (RT) is one of the principle treatment modalities for the management of cancer. In recent decades, advances in the radiation
Chapter 7 General conclusions and suggestions for future work Radiation therapy (RT) is one of the principle treatment modalities for the management of cancer. In recent decades, advances in the radiation
IMRT IN HEAD NECK CANCER
 IMRT IN HEAD NECK CANCER THE SEARCH FOR CONFORMALITY CONVENTIONAL RT Simple field arrangements Uniformly radiate both the target and the surrounding normal tissues. Includes the use of rectangular blocks
IMRT IN HEAD NECK CANCER THE SEARCH FOR CONFORMALITY CONVENTIONAL RT Simple field arrangements Uniformly radiate both the target and the surrounding normal tissues. Includes the use of rectangular blocks
Impact of robust treatment planning on single- and multi-field optimized plans for proton beam therapy of unilateral head and neck target volumes
 Cubillos-Mesías et al. Radiation Oncology (2017) 12:190 DOI 10.1186/s13014-017-0931-8 RESEARCH Open Access Impact of robust treatment planning on single- and multi-field optimized plans for proton beam
Cubillos-Mesías et al. Radiation Oncology (2017) 12:190 DOI 10.1186/s13014-017-0931-8 RESEARCH Open Access Impact of robust treatment planning on single- and multi-field optimized plans for proton beam
Outline. Contour quality control. Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT)
 Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT) James Kavanaugh, MS DABR Department of Radiation Oncology Division of Medical Physics Outline Importance
Dosimetric impact of contouring errors and variability in Intensity Modulated Radiation Therapy (IMRT) James Kavanaugh, MS DABR Department of Radiation Oncology Division of Medical Physics Outline Importance
Original Article. Teyyiba Kanwal, Muhammad Khalid, Syed Ijaz Hussain Shah, Khawar Nadeem
 Original Article Treatment Planning Evaluation of Sliding Window and Multiple Static Segments Technique in Intensity Modulated Radiotherapy for Different Beam Directions Teyyiba Kanwal, Muhammad Khalid,
Original Article Treatment Planning Evaluation of Sliding Window and Multiple Static Segments Technique in Intensity Modulated Radiotherapy for Different Beam Directions Teyyiba Kanwal, Muhammad Khalid,
Page 1. Helical (Spiral) Tomotherapy. UW Helical Tomotherapy Unit. Helical (Spiral) Tomotherapy. MVCT of an Anesthetized Dog with a Sinus Tumor
 Helical (Spiral) Tomotherapy Novel Clinical Applications of IMRT Linac Ring Gantry CT Detector X-Ray Fan Beam Binary Multileaf Collimator Binary MLC Leaves James S Welsh, MS, MD Department of Human Oncology
Helical (Spiral) Tomotherapy Novel Clinical Applications of IMRT Linac Ring Gantry CT Detector X-Ray Fan Beam Binary Multileaf Collimator Binary MLC Leaves James S Welsh, MS, MD Department of Human Oncology
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases
 Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
Evaluation of Monaco treatment planning system for hypofractionated stereotactic volumetric arc radiotherapy of multiple brain metastases CASE STUDY Institution: Odette Cancer Centre Location: Sunnybrook
Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI)
 Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI) Tagreed AL-ALAWI Medical Physicist King Abdullah Medical City- Jeddah Aim 1. Simplify and standardize
Treatment Planning Evaluation of Volumetric Modulated Arc Therapy (VMAT) for Craniospinal Irradiation (CSI) Tagreed AL-ALAWI Medical Physicist King Abdullah Medical City- Jeddah Aim 1. Simplify and standardize
Reduced acute toxicity and improved efficacy from intensitymodulated proton therapy (IMPT) for the management of head and neck cancer
 Review Article Page 1 of 12 Reduced acute toxicity and improved efficacy from intensitymodulated proton therapy (IMPT) for the management of head and neck cancer Matthew R. McKeever 1,2, Terence T. Sio
Review Article Page 1 of 12 Reduced acute toxicity and improved efficacy from intensitymodulated proton therapy (IMPT) for the management of head and neck cancer Matthew R. McKeever 1,2, Terence T. Sio
Mick Spillane. Medical. Intensity-Modulated Radiotherapy for Sinonasal Tumors
 Mick Spillane Medical Formatted: Left Intensity-Modulated Radiotherapy for Sinonasal Tumors F Division of Radiotherapy, Department of Oncology (I. M., L. V., W. D. N.), and Division of Head and Neck Surgery,
Mick Spillane Medical Formatted: Left Intensity-Modulated Radiotherapy for Sinonasal Tumors F Division of Radiotherapy, Department of Oncology (I. M., L. V., W. D. N.), and Division of Head and Neck Surgery,
Helical tomotherapy for head and neck squamous cell carcinoma: Dosimetric comparison with linear accelerator-based step-and-shoot IMRT
 Original Article Free full text available from www.cancerjournal.net Helical tomotherapy for head and neck squamous cell carcinoma: Dosimetric comparison with linear accelerator-based step-and-shoot IMRT
Original Article Free full text available from www.cancerjournal.net Helical tomotherapy for head and neck squamous cell carcinoma: Dosimetric comparison with linear accelerator-based step-and-shoot IMRT
Michael F. Gensheimer 1, Matthew Nyflot 2, George E. Laramore 2, Jay J. Liao 2 and Upendra Parvathaneni 2*
 Gensheimer et al. Radiation Oncology (2016) 11:151 DOI 10.1186/s13014-016-0726-3 RESEARCH Open Access Contribution of submandibular gland and swallowing structure sparing to postradiation therapy PEG dependence
Gensheimer et al. Radiation Oncology (2016) 11:151 DOI 10.1186/s13014-016-0726-3 RESEARCH Open Access Contribution of submandibular gland and swallowing structure sparing to postradiation therapy PEG dependence
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer
 A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
IGRT Protocol Design and Informed Margins. Conflict of Interest. Outline 7/7/2017. DJ Vile, PhD. I have no conflict of interest to disclose
 IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
IGRT Protocol Design and Informed Margins DJ Vile, PhD Conflict of Interest I have no conflict of interest to disclose Outline Overview and definitions Quantification of motion Influences on margin selection
Selective partial salivary glands sparing during intensity-modulated radiation therapy for nasopharyngeal carcinoma*
 Oncology and Translational Medicine DOI 10.1007/s10330-017-0219-9 April 2017, Vol. 3, No. 2, P65 P70 ORIGINAL ARTICLE Selective partial salivary glands sparing during intensity-modulated radiation therapy
Oncology and Translational Medicine DOI 10.1007/s10330-017-0219-9 April 2017, Vol. 3, No. 2, P65 P70 ORIGINAL ARTICLE Selective partial salivary glands sparing during intensity-modulated radiation therapy
Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101. Cases from Duke Clinic. Deon Martina Dick
 Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101 Cases from Duke Clinic by Deon Martina Dick Department of Medical Physics Duke University Date: Approved: Joseph Lo, Chair
Knowledge-Based IMRT Treatment Planning for Prostate Cancer: Experience with 101 Cases from Duke Clinic by Deon Martina Dick Department of Medical Physics Duke University Date: Approved: Joseph Lo, Chair
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR
 Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Advanced Technology Consortium (ATC) Credentialing Procedures for 3D Conformal Therapy Protocols 3D CRT Benchmark*
 Advanced Technology Consortium (ATC) Credentialing Procedures for 3D Conformal Therapy Protocols 3D CRT Benchmark* Purpose: To evaluate an institution s 3D treatment planning process and the institution
Advanced Technology Consortium (ATC) Credentialing Procedures for 3D Conformal Therapy Protocols 3D CRT Benchmark* Purpose: To evaluate an institution s 3D treatment planning process and the institution
Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer. William M. Mendenhall, MD
 Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer William M. Mendenhall, MD Meta-Analysis of Probability of Maintaining Erectile Function after Treatment of Localized Cancer Treatment
Erectile Dysfunction (ED) after Radiotherapy (RT) for Prostate Cancer William M. Mendenhall, MD Meta-Analysis of Probability of Maintaining Erectile Function after Treatment of Localized Cancer Treatment
8/3/2016. Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients. Acknowledgement. Overview
 Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients Liyong Lin, PhD, Assistant Professor Department of Radiation Oncology University of Pennsylvania Acknowledgement
Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients Liyong Lin, PhD, Assistant Professor Department of Radiation Oncology University of Pennsylvania Acknowledgement
Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer. Shelby Mariah Grzetic. Graduate Program in Medical Physics Duke University
 Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer by Shelby Mariah Grzetic Graduate Program in Medical Physics Duke University Date: Approved: Joseph Y. Lo, Co-Supervisor Shiva
Multi-Case Knowledge-Based IMRT Treatment Planning in Head and Neck Cancer by Shelby Mariah Grzetic Graduate Program in Medical Physics Duke University Date: Approved: Joseph Y. Lo, Co-Supervisor Shiva
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
