Circulating Epithelial Cells in Intraductal Papillary Mucinous Neoplasms and Cystic Pancreatic Lesions
|
|
|
- Ella Cole
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Circulating Epithelial Cells in Intraductal Papillary Mucinous Neoplasms and Cystic Pancreatic Lesions Katherine E. Poruk, MD,* Vicente Valero, III, MD,* Jin He, MD,* Nita Ahuja, MD,* John L. Cameron, MD,* Matthew J. Weiss, MD,* Anne Marie Lennon, MD, PhD, Michael Goggins, MD, Laura D. Wood, MD, PhD, and Christopher L. Wolfgang, MD, PhD* Objectives: Circulating epithelial cells (CECs) are identified in the blood of patients with intraductal papillary mucinous neoplasms (IPMNs) despite the absence of malignancy. We assessed the blood of patients undergoing resection for IPMN or other benign pancreatic lesions for CECs. Methods: Peripheral blood was collected from 26 patients prior to pancreatic resection and filtered by the ISET (Isolation by Size of Epithelial Tumor Cells) method. Circulating epithelial cells were identified with antibodies to cytokeratin and Pdx1 (pancreas and duodenal homeobox protein 1), a pancreas marker. Results: Nineteen patients underwent resection of an IPMN without associated malignancy. Eleven patients (58%) had cytokeratin-positive CECs. Circulating epithelial cells were significantly more likely to be found in patients with IPMNs with high-grade dysplasia (P = 0.04). In addition, 10 of the 11 patients with cytokeratin-positive CECs also had separate populations of cytokeratin-positive, Pdx1-positive CECs, suggesting a pancreatic source. Dual-staining CECs were more frequently found in patients with high-grade dysplasia (P = 0.04). Patients with IPMNs were significantly more likely to have pan-cytokeratin CECs in the blood compared with those without IPMNs (P =0.01). Conclusions: Circulating epithelial cells staining with potential pancreasspecific markers have been found in patients with IPMNs, even without malignancy. Circulating epithelial cells may help to differentiate patients with high-grade IPMN from lower grades of dysplasia and other pancreatic cysts. Key Words: circulating epithelial cells, grade, intraductal papillary mucinous neoplasms, Pdx1 (Pancreas 2017;46: ) Intraductal papillary mucinous neoplasms (IPMNs) are mucinproducing cystic lesions of the main and branch pancreatic ducts predominantly found in older individuals. While the majority of these lesions are benign, the accumulated evidence strongly supports that IPMNs are precursors to pancreatic ductal adenocarcinoma (PDAC). Several case series have demonstrated From the Departments of *Surgery, Gastroenterology, and Pathology, The Johns Hopkins Hospital, Baltimore, MD. Received for publication June 9, 2016; accepted April 11, Address correspondence to: Christopher L. Wolfgang, MD, PhD, The Johns Hopkins Hospital, 600 N Wolfe St Osler 624, Baltimore, MD (e mail: cwolfga2@jhmi.edu); Laura D. Wood, MD, PhD, CRB2 Room 345, 1550 Orleans St, Baltimore, MD (e mail: ldwood@jhmi.edu). Funding for this study was provided by National Institutes of Health (NIH) grants CA A1 (to K.E.P.), the Sol Goldman Cancer Research Grant (to K.E.P.), NIH SPORE grant CA62924, the Kaya Tuncer Career Development Award in GI Cancer Prevention (to L.D.W.), the AGA- Bernard Lee Schwartz Research Scholar Award in Pancreatic Cancer (to L.D.W.), The Natalie and David Lederman Foundation, Joseph C. Monastra Foundation, Michael Rolfe Pancreatic Cancer Foundation, the Pancreatic Cancer Action Network, and the Sol Goldman Pancreatic Cancer Research Center. The authors declare no conflict of interest. DOI: /MPA that at the time of resection anywhere from 6% to 81% of patients will be found to have an adenocarcinoma associated with their IPMN, especially those with a main-duct IPMN. 1 5 In addition, as many as 38% of patients may progress to PDAC after resection of a benign IPMN even as far out as 10 years postoperatively. 6 Certain risk factors have been identified for the progression to PDAC, thus creating specific criteria for pancreatic resection known as the Sendai Consensus Guidelines. 7 Indications for resection based on these criteria include main-duct IPMN or main-duct mixed with branch-duct IPMN, dilatation of the main duct to at least 10 mm in diameter, an associated solid component within the cyst, branch-duct IPMN greater than 3 cm in size, and individuals who are symptomatic given a higher association with high-grade dysplasia or malignancy. 7 While the goal of these guidelines is to resect lesions in highrisk patients prior to malignant progression, the criteria are neither perfectly sensitive nor perfectly specific, creating a need for further markers to identify and stratify patients for resection at highest risk of associated malignancy and dysplasia. Circulating tumor cells (CTCs) are cells that have been shed from a tumor into the bloodstream. These circulating cells have been identified in numerous malignancies, including patients with PDAC, and are believed to be a potential marker not only for cancer but also for poor prognosis and tumor recurrence. 8 Interestingly, similar circulating epithelial cells (CECs) have been identified in patients with IPMNs despite the absence of any clinically identified malignancy. These cells have been appropriately called CECs, over CTCs, as a reflection of their likely nonmalignant source. A study of 21 patients with cystic neoplasms of the pancreas, including 18 patients with Sendai-negative IPMNs, demonstrated that 33% of patients had CECs based on expression of antibodies to epithelial cell adhesion molecule and pancreas and duodenal homeobox protein 1 (Pdx1), a pancreas-specific transcription factor. 9 However, this study was not able to confirm cyst type or the absence of pancreatic malignancy, because no patient underwent resection of the cystic lesion. A similar analysis of 21 patients with IPMNs demonstrated 13 (62%) had CECs identified based on the presence of cells with malignant-appearing morphology after Giemsa staining. 10 However, a recent study from our group suggests that identification of CECs based on morphology alone may not be accurate for the identification of these cells in PDAC. 8 With this study, we assessed the blood of patients prior to resection of an IPMN or other cystic pancreatic neoplasm for the presence of CECs utilizing specific antibodies with comparison to patient and tumor characteristics. We demonstrate the presence of CECs in the blood of patients with IPMN but not patients with other cystic pancreatic neoplasms. MATERIALS AND METHODS Patient Selection This study included 19 consecutive patients with IPMN, 5 patients with solid pseudopapillary neoplasms (SPN), 1 patient Pancreas Volume 46, Number 7, August
2 Poruk et al Pancreas Volume 46, Number 7, August 2017 with a mucinous cystic neoplasm (MCN), and 1 patient with benign pancreatic lobular proliferation who underwent surgical resection at The Johns Hopkins Hospital between June 2013 and October These patients all consented for peripheral blood collection prior to surgical resection by written consent. Between 5 and 10 ml of venous and/or arterial blood was collected prior to surgical incision. Medical charts for all patients were reviewed, and data were collected regarding patient demographics, tumor histopathology, preoperative imaging, and perioperative factors. The pathology of all 26 patients was reviewed by a clinical pathologist and included an assessment of size, location, number, margin status, and, when applicable, grade of the lesion. This study was performed with the approval of the institutional review board at The Johns Hopkins Hospital. Circulating Epithelial Cell Filtration and Identification by Immunofluorescence Blood samples were processed using the Isolation by Size of Epithelial Tumor Cells (ISET) method (Rarecells, Paris, France), which involved mixing approximately 5 to 10 ml of patient blood with specially prepared ISET buffer and formaldehyde. This mixture was then filtered onto special membranes by the ISDT machine for further analysis. After filtration, samples were stored at 20 C until staining. Immunofluorescence was performed by rehydrating ISET membranes with 1X Tris-buffered saline prior to permeabilization with 0.2% Triton. After removal of the Triton, membranes were incubated in a 5% milk-based blocking buffer. Membranes were then incubated for 2 hours with conjugated antibodies to pan-cytokeratin (1:100, fluorescein isothiocyanate; Millipore, Danvers, Mass) and Pdx1 (1:100, Alexa Fluor 647; Abcam, Cambridge, Mass) diluted in 5% milk-based blocking buffer. Finally, membranes were washed in 1X Tris-buffered saline and affixed to glass microscope slides with 4,6-diamidino- 2-phenylindole (DAPI; Life Technologies, Carlsbad, Calif) before analysis by fluorescence microscope. All antibodies were appropriately tested using known positive and negative controls. All slides were viewed under 20 magnification with the entire membrane viewed for CECs. Circulating epithelial cells were counted manually by a single user across the entire membrane, with separate counts for patients with DAPI-positive, cytokeratinpositive, Pdx1-negative CECs and patients with DAPI-positive, cytokeratin-positive, Pdx1-positive CECs. Initial exposure times were automatically identified using the Nikon NIS Elements imaging program (version bit; Melville, NY) and corresponded to 600 milliseconds for DAPI, 1 second for cytokeratin, and 3 seconds for Pdx1. These exposure times were consistent for all 24 patients included in this study. All sections of each membrane were viewed with each separate wavelength corresponding to DAPI, cytokeratin, and Pdx1. When a candidate CEC was identified, an image under each specific wavelength was captured and saved. A CEC was defined as a cell with nuclear staining of DAPI with a diameter greater than 15 μm and cytoplasmic labeling for cytokeratin. Circulating epithelial cells were also noted for the presence or absence of Pdx1, which in the CECs identified stained predominantly in the cytoplasm. Although predominantly a nuclear transcription factor, cytoplasmic expression in pancreatic cells has been noted under certain conditions Statistical Analysis Statistics for individual patient groups and the entire patient cohort are presented using frequencies and percentages for categorical variables and as mean values with ranges for continuous TABLE 1. Comparison of Characteristics Between Patients With and Without Cytokeratin-Positive CECs Characteristic All Patients (n = 19) Pan-Cytokeratin + CTC (n = 11) No CTC (n = 8) P Age, y 66.1 (27 82) 66.1 (27 80) 66.1 (46 82) 0.99 Sex 0.37 Male 10 (53) 7 (64) 3 (37) Female 9 (47) 4 (36) 5 (63) No. of IPMNs 1.3 (1 4) 1.4 (1 4) 1.1 (1 2) 0.56 IPMN size, cm 2.6 (1 9.0) 3.0 ( ) 2.0 (1 4) 0.27 Grade (highest) 0.04 Low 3 (16) 0 (0) 3 (37) Intermediate 12 (63) 7 (64) 5 (63) High 4 (21) 4 (36) 0 (0) Grade (binary) 0.10 Low/intermediate 15 (79) 7 (64) 8 (100) High 4 (21) 4 (36) 0 (0) Location 0.99 Side duct 9 (47) 5 (45.5) 4 (50) Main duct 2 (11) 1 (9) 1 (13) Mixed 8 (42) 5 (45.5) 3 (37) Margin 0.99 Positive (mucin) 5 (26) 3 (27) 2 (25) Negative 14 (74) 8 (73) 6 (75) Associated pancreatic intraepithelial neoplasia 1.00 Yes 7 (37) 4 (36) 3 (37) No 12 (63) 7 (64) 5 (63) Data are presented as either n (%) or mean (range). Bold values are statistically significant with P < Wolters Kluwer Health, Inc. All rights reserved.
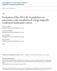
3 Pancreas Volume 46, Number 7, August 2017 Circulating Epithelial Cells in IPMNs FIGURE 1. Circulating epithelial cells staining positive for cytokeratin. Circulating epithelial cell stains included for (A) all stains merged, (B) DAPI only, (C) pan-cytokeratin only, and (D) absence of Pdx1. variables. Differences in patient characteristics between dichotomous cohorts were calculated utilizing Fisher's exact test. All statistical analyses were performed using STATA version 13.0 (StataCorp, College Station, Tex). Statistical significance was set at P <0.05. RESULTS Assessment of CECs in Patients With IPMN During the study period, 19 patients without a prior history of malignancy underwent pancreatic resection of an IPMN. Patient characteristics are given in Table 1. The average patient age was 66.1 years (range, years), and 53% of patients were male. The average and median size of the IPMN were 2.6 and 2.1 cm (range, cm), and the majority of patients (n = 15 [88%]) had only 1 IPMN by pathological analysis. The majority of patients underwent pancreaticoduodenectomy (n = 12 [63%]), followed by distal pancreatectomy with splenectomy (n = 4 [21%]), central pancreatectomy (n = 2 [11%]), or total pancreatectomy (n = 1 [5%]). More than half of all patients (n = 10 [53%]) had involvement of the main pancreatic duct. Of note, no patient with an IPMN had an associated PDAC, nor did any patient have a personal history of a concurrent or prior malignancy. The presence of CECs was assessed by staining patient blood samples with pan-cytokeratin, an epithelial marker, and Pdx1, a pancreas specific marker. First, samples were assessed for CECs positive only for cytokeratin. Eleven patients (58%) with IPMNs were found to have CECs that stained positive for pan-cytokeratin and DAPI, a nuclear marker (Fig. 1). Differences in characteristics between patients with and without pan-cytokeratin positive CECs are given in Table 1. There was no significant difference between any patient or tumor characteristic in patients with CECs, including IPMN size, number, or location (all P > 0.05). However, all patients with IPMNs with high-grade dysplasia were found to have pan-cytokeratin positive CECs, and patients with CECs were significantly more likely to have high-grade dysplasia present at the time of surgery (P = 0.04). The presence of CECs with pancreas-specific markers was then assessed by identifying CECs with both pan-cytokeratin and Pdx1. Ten patients (53%) were found to have cells that stained positive for both pan-cytokeratin and Pdx1 (Fig. 2). All 10 patients were also found to have pan-cytokeratin positive, Pdx1-negative CECs during the same analysis, whereas 1 patient had only cytokeratin-positive CECs without any staining for Pdx1. The remaining 7 patients did not have CECs of either type. Differences in characteristics between patients with and without cytokeratinpositive, Pdx1-positive CECs are given in Table 2. Similar to the previous analysis, there was no significant difference between any patient or tumor characteristic in patients with cytokeratinpositive, Pdx1-positive CECs, including IPMN size, number, or location (all P > 0.05) except for grade of dysplasia. All patients with high-grade IPMNs were found to have pan-cytokeratin positive, Pdx1-positive CECs, and patients with CECs were significantly more likely to have high-grade dysplasia present at the time of surgery (P = 0.04). In addition, there was a trend toward high-grade dysplasia in patients with pan-cytokeratin positive, Pdx1-positive CECs compared with low- or moderategrade dysplasia (P = 0.09). CECs in Non-IPMN Patients Seven patients who underwent pancreatic resection for non- IPMN cystic disease were assessed for the presence of pancytokeratin CECs. This included 5 patients with SPNs, 1 patient with an MCN, and 1 patient with concern for IPMN who was found at resection to have benign lobular proliferation. Average and median ages for these patients were 56.4 and 63 years, respectively (range, years), and 43% of patients were male. Average and median sizes of the cystic lesions were 5.1 and 3.5 cm, respectively (range, 1 17 cm). None of the 7 patients were found to have CECs as assessed by the presence of pan-cytokeratin staining. A comparison of CECs demonstrated that patients with IPMNs were significantly more likely to have pan-cytokeratin positive CECs in the blood compared with patients without IPMNs (P = 0.01). The sensitivity and specificity for diagnosis were 58% and 100%, respectively. DISCUSSION The identification of CECs in patients with malignancy has become an exciting potential mechanism for early detection, treatment stratification, and prediction of prognosis. However, the detection of these cells in the blood of patients without a documented cancer has led to uncertainty about the origin and significance of these cells. Multiple patient series have identified the FIGURE 2. Circulating epithelial cell staining positive for cytokeratin and Pdx1. Circulating epithelial cell stains included for (A) all stains merged, (B) DAPI only, (C) pan-cytokeratin only, and (D) Pdx1 only Wolters Kluwer Health, Inc. All rights reserved
4 Poruk et al Pancreas Volume 46, Number 7, August 2017 TABLE 2. Comparison of Characteristics Between Patients With and Without Cytokeratin-Positive, Pdx1-Positive CECs Characteristic Pan-Cytokeratin + /Pdx1 + CTC (n = 10) No Pan-Cytokeratin + /Pdx1 + CTC (n = 9) P Age, y 66.2 (27 80) 66.0 (46 82) 0.97 Sex 0.66 Male 6 (60) 4 (44) Female 4 (40) 5 (56) No. of IPMNs 1.3 (1 4) 1.13 (1 2) 0.89 IPMN size, cm 3.1 (1.4-9) 2.0 (1 4) 0.21 Grade (highest) 0.04 Low 0 (0) 3 (33) Intermediate 6 (60) 6 (67) High 4 (40) 0 (0) Grade (binary) 0.09 Low/intermediate 6 (60) 9 (100) High 4 (40) 0 (0) Location 0.81 Side duct 4 (40) 5 (56) Main duct 1 (10) 1 (11) Mixed 5 (50) 3 (33) Margin 0.99 Positive (mucin) 3 (30) 2 (22) Negative 7 (70) 7 (78) Associated pancreatic intraepithelial neoplasia 0.65 Yes 3 (30) 4 (44) No 7 (70) 5 (56) Data are presented as either n (%) or mean (range). Bold values are statistically significant with P <0.05. presence of epithelial or malignant-appearing cells in the blood of patients with IPMN, but correlation to underlying histopathology has been lacking. This study adds to the literature by further demonstrating the presence of CECs in patients whose absence of malignancy was confirmed by histopathologic review. In addition, our study used a unique method to identify these cells (filtering by size followed by immunofluorescence for epithelial and pancreatic markers), demonstrating that the identification of these cells is not an artifact of a single isolation method. As with 2 prior studies, we identified the presence of CECs through cytokeratin staining in more than half of all patients undergoing resection for an IPMN. Furthermore, none of these patients had any history of malignancy, and complete pathological examination of the resected pancreata did not reveal any malignancy. Almost all of these patients had CECs that also stained for Pdx1, a marker thought to be specific to the pancreas. However, the Pdx1 staining we observed was cytoplasmic, not nuclear. Previous reports of Pdx1 staining in pancreatic neoplasms have focused on nuclear staining, but cytoplasmic staining has been reported in endocrine cells under specific conditions Although Pdx1 expression is suggestive of a pancreatic source, the precise implications of cytoplasmic staining in this particular clinical situation are not known. Still, identification of driver gene mutations in these CECs will be needed to definitively confirm a neoplastic pancreatic source beyond simple staining with Pdx1. Unlike prior studies, this study is the first to compare the presence or absence of CECs with patient and tumor characteristics. Overall, there were no differences in size, number, and location of IPMN between patients with or without CECs. Interestingly, all patients with high-grade dysplasia were found to have CECs staining with pan-cytokeratin, Pdx1, or both. In addition, patients with CECs were significantly more likely to have high- or moderategrade dysplasia compared with patients without CECs. This creates the potential use for CECs to differentiate the degree of underlying dysplasia prior to resection of an IPMN. Further study in a larger number of patients, including those with IPMN-associated adenocarcinoma, is necessary to determine and to further evaluate this potential relationship and identify if CECs are a potential marker for high-grade dysplasia. This study also assessed the presence of CECs in a small population of patients undergoing pancreatic resection for a non- IPMN cystic neoplasm. Many of these patients underwent resection with a high suspicion for an IPMN, only to be discovered to have a different neoplasm such as SPN or MCN or, in 1 patient s case, benign proliferation of lobular pancreatic tissue. While the diagnosis of an IPMN or other neoplasm is often straightforward, in some cases imaging cannot clearly determine the etiology of the lesion. In this study, patients with IPMNs were significantly more likely to have CECs compared with patients without an IPMN. Unlike prior studies, however, no CECs were discovered in patients with non-ipmn cystic neoplasms. This may be related to the small number of patient included in this cohort, as prior research has demonstrated the presence of CECs in patients with MCN. 9 It may be possible that a larger analysis of patients with SPN and MCN would demonstrate individuals with CECs present. Further study in a larger cohort of patients with and without IPMN is needed to determine if CECs have utility as a diagnostic marker for IPMN. In conclusion, this study demonstrates the presence of CECs in the blood of patients with IPMN without associated adenocarcinoma, expanding on prior studies by correlating the presence of these cells to underlying histopathology. In addition, this study identified CECs staining positive for Pdx1, a pancreatic marker, further suggesting a pancreatic origin. Additional study in a larger Wolters Kluwer Health, Inc. All rights reserved.
5 Pancreas Volume 46, Number 7, August 2017 Circulating Epithelial Cells in IPMNs population of patients is needed to determine the effectiveness of CECs for the diagnosis of high-grade dysplasia prior to resection. Circulating epithelial cells may have utility as a diagnostic marker to differentiate IPMNs from other cystic lesions of the pancreas, but prospective assessment in a larger patient cohort is necessary. The presence of circulating cells in patients without cancer is a provocative discovery and creates a potential mechanism to broaden our understanding of the malignant progression. REFERENCES 1. Kim SC, Park KT, Lee YJ, et al. Intraductal papillary mucinous neoplasm of the pancreas: clinical characteristics and treatment outcomes of 118 consecutive patients from a single center. J Hepatobiliary Pancreat Surg. 2008;15: Lee SY, Lee KT, Lee JK, et al. Long-term follow up results of intraductal papillary mucinous tumors of pancreas. J Gastroenterol Hepatol. 2005;20: Nagai K, Doi R, Kida A, et al. Intraductal papillary mucinous neoplasms of the pancreas: clinicopathologic characteristics and long-term follow-up after resection. World J Surg. 2008;32: ; discussion Nara S, Onaya H, Hiraoka N, et al. Preoperative evaluation of invasive and noninvasive intraductal papillary-mucinous neoplasms of the pancreas: clinical, radiological, and pathological analysis of 123 cases. Pancreas. 2009;38: Sadakari Y, Ienaga J, Kobayashi K, et al. Cyst size indicates malignant transformation in branch duct intraductal papillary mucinous neoplasm of the pancreas without mural nodules. Pancreas. 2010;39: He J, Cameron JL, Ahuja N, et al. Is it necessary to follow patients after resection of a benign pancreatic intraductal papillary mucinous neoplasm? JAmCollSurg. 2013;216: ; discussion Tanaka M, Fernández-del Castillo C, Adsay V, et al. International consensus guidelines 2012 for the management of IPMN and MCN of the pancreas. Pancreatology. 2012;12: Poruk KE, Valero V 3rd, Saunders T, et al. Circulating tumor cell phenotype predicts recurrence and survival in pancreatic adenocarcinoma. Ann Surg. 2016;264: Rhim AD, Thege FI, Santana SM, et al. Detection of circulating pancreas epithelial cells in patients with pancreatic cystic lesions. Gastroenterology. 2014;146: Cauley CE, Pitman MB, Zhou J, et al. Circulating epithelial cells in patients with pancreatic lesions: clinical and pathologic findings. JAmCollSurg. 2015;221: Kawamori D, Kajimoto Y, Kaneto H, et al. Oxidative stress induces nucleo-cytoplasmic translocation of pancreatic transcription factor PDX-1 through activation of c-jun NH(2)-terminal kinase. Diabetes. 2003;52: Fujimoto K, Polonsky KS. Pdx1 and other factors that regulate pancreatic beta-cell survival. Diabetes Obes Metab. 2009;11(suppl 4): Macfarlane WM, McKinnon CM, Felton-Edkins ZA, et al. Glucose stimulates translocation of the homeodomain transcription factor PDX1 from the cytoplasm to the nucleus in pancreatic beta-cells. JBiolChem. 1999;274: Park JY, Hong SM, Klimstra DS, et al. Pdx1 expression in pancreatic precursor lesions and neoplasms. Appl Immunohistochem Mol Morphol. 2011;19: Wolters Kluwer Health, Inc. All rights reserved
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
p53 expression in invasive pancreatic adenocarcinoma and precursor lesions
 Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget
 Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center experience with 324 patients who underwent surgical resection
 Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Histopathologic Findings of Multifocal Pancreatic Intraductal Papillary Mucinous Neoplasms on CT
 Gastrointestinal Imaging Original Research Raman et al. CT of Multifocal Pancreatic IPMNs Gastrointestinal Imaging Original Research Siva P. Raman 1 Satomi Kawamoto 1 Amanda Blackford 2 Ralph H. Hruban
Gastrointestinal Imaging Original Research Raman et al. CT of Multifocal Pancreatic IPMNs Gastrointestinal Imaging Original Research Siva P. Raman 1 Satomi Kawamoto 1 Amanda Blackford 2 Ralph H. Hruban
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Cystic pancreatic lesions A proposal for a network approach. Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth
 Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Patient History. A 58 year old man presents with a 16 mm cyst in the pancreatic tail. The cyst is unilocular with a thick wall and no mural nodule.
 Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Intraductal Papillary Mucinous Neoplasm of the Pancreas. Masao Tanaka Editor
 Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas
Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas
Pancreatic intraepithelial
 Pancreatic intraepithelial neoplasia (PanIN) Markéta Hermanová St. Anne s University Hospital Brno Faculty of Medicine, Masaryk University Precursor lesions of invasive pancreatic cancer Pancreatic intraepithelial
Pancreatic intraepithelial neoplasia (PanIN) Markéta Hermanová St. Anne s University Hospital Brno Faculty of Medicine, Masaryk University Precursor lesions of invasive pancreatic cancer Pancreatic intraepithelial
Pancreatic Cysts - Part 2
 REVIEW Pancreatic Cysts - Part 2 Should We Be Less Cyst Centric? Anne Marie Lennon, MD, PhD and Marcia Irene Canto, MD, MHS Abstract: The management of pancreatic cysts is a common problem faced by physicians
REVIEW Pancreatic Cysts - Part 2 Should We Be Less Cyst Centric? Anne Marie Lennon, MD, PhD and Marcia Irene Canto, MD, MHS Abstract: The management of pancreatic cysts is a common problem faced by physicians
According to the international consensus guidelines for
 ORIGINAL ARTICLE Natural History of Branch Duct Intraductal Papillary Mucinous Neoplasm With Mural Nodules A Japan Pancreas Society Multicenter Study Go Kobayashi, MD, PhD,* Naotaka Fujita, MD, PhD,* Hiroyuki
ORIGINAL ARTICLE Natural History of Branch Duct Intraductal Papillary Mucinous Neoplasm With Mural Nodules A Japan Pancreas Society Multicenter Study Go Kobayashi, MD, PhD,* Naotaka Fujita, MD, PhD,* Hiroyuki
Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas
 HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Intraductal Papillary Mucinous Neoplasms: The Bologna Experience
 ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
Pancreatic Cystic Neoplasms: Guidelines and beyond
 Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Case 1. Case 1: EUS Report 5/1/2017. Interesting Cases of Pancreatic Masses
 Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms
 JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
Pancreatico-biliary cytology: a practical approach to diagnosis. Corina Cotoi
 Pancreatico-biliary cytology: a practical approach to diagnosis Corina Cotoi Pancreatico-biliary lesions Solid: Ductal adenocarcinoma Cholangiocarcinoma Acinar cell carcinoma Neuroendocrine tumour / carcinoma
Pancreatico-biliary cytology: a practical approach to diagnosis Corina Cotoi Pancreatico-biliary lesions Solid: Ductal adenocarcinoma Cholangiocarcinoma Acinar cell carcinoma Neuroendocrine tumour / carcinoma
1 Department of Gastroenterology and Pancreatology, Beaujon Hospital, France 3 Department or Radiology, Beaujon Hospital, University Paris 7, Clichy,
 Original Article Accuracy of 2012 International Consensus Guidelines for the prediction of malignancy of branch-duct intraductal papillary mucinous neoplasms of the pancreas United European Gastroenterology
Original Article Accuracy of 2012 International Consensus Guidelines for the prediction of malignancy of branch-duct intraductal papillary mucinous neoplasms of the pancreas United European Gastroenterology
Original article. Introduction!
 382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated Pancreatectomy
 ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
Pancreatic Disorders & Therapy
 ISSN: 2165-7092 rpancreatic Disorders & The apy Review Article Pancreatic Disorders & Therapy Kimura and Tezuka, 2015, 5:1 DOI: 10.4172/2165-7092.1000148 Open Access Acute Pancreatitis is a Predictive
ISSN: 2165-7092 rpancreatic Disorders & The apy Review Article Pancreatic Disorders & Therapy Kimura and Tezuka, 2015, 5:1 DOI: 10.4172/2165-7092.1000148 Open Access Acute Pancreatitis is a Predictive
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Intraductal papillary neoplasms in the bile ducts
 Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case report
 Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
RESEARCH ARTICLE. Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation
 DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
Pancreatobiliary Frozen Section Nightmares
 Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
SYSTEMATIC REVIEWS AND META-ANALYSES
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:913 921 SYSTEMATIC REVIEWS AND META-ANALYSES Fasiha Kanwal, Section Editor Cyst Features and Risk of Malignancy in Intraductal Papillary Mucinous Neoplasms
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:913 921 SYSTEMATIC REVIEWS AND META-ANALYSES Fasiha Kanwal, Section Editor Cyst Features and Risk of Malignancy in Intraductal Papillary Mucinous Neoplasms
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter cohort
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period
 Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics
 Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt, Alexandra Roch, Jennifer Schaffter Stuart, Stuart Sherman, Mohammad A.
 Management of Branch duct Intraductal Papillary Mucinous Neoplasms: A Large Single Center Study to Assess Predictors of Malignancy and Long Term Outcomes Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt,
Management of Branch duct Intraductal Papillary Mucinous Neoplasms: A Large Single Center Study to Assess Predictors of Malignancy and Long Term Outcomes Wiriyaporn Ridtitid, John M.DeWitt, C. Max Schmidt,
Pancreatic Cystic Lesions 원자력병원
 Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
FDG-PET Findings of Intraductal Oncocytic Papillary Neoplasms of the Pancreas: Two Case Reports
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Importance of luminal membrane mesothelin expression in intraductal papillary mucinous neoplasms
 ONCOLOGY LETTERS 9: 1583-1589, 2015 Importance of luminal membrane mesothelin expression in intraductal papillary mucinous neoplasms TAKAHIRO EINAMA 1,2,3, HIROFUMI KAMACHI 1, HIROSHI NISHIHARA 4, SHIGENORI
ONCOLOGY LETTERS 9: 1583-1589, 2015 Importance of luminal membrane mesothelin expression in intraductal papillary mucinous neoplasms TAKAHIRO EINAMA 1,2,3, HIROFUMI KAMACHI 1, HIROSHI NISHIHARA 4, SHIGENORI
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
International consensus on the management of intraductal papillary mucinous neoplasm of the pancreas
 Review Article Page 1 of 9 International consensus on the management of intraductal papillary mucinous neoplasm of the pancreas Masao Tanaka Shimonoseki City Hospital, 1-13-1 Koyo-cho, Shimonoseki 750-8520,
Review Article Page 1 of 9 International consensus on the management of intraductal papillary mucinous neoplasm of the pancreas Masao Tanaka Shimonoseki City Hospital, 1-13-1 Koyo-cho, Shimonoseki 750-8520,
Genetics of Pancreatic Cancer. October 6, If you experience technical difficulty during the presentation:
 Genetics of Pancreatic Cancer October 6, 2016 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only: 1-408-435-7088
Genetics of Pancreatic Cancer October 6, 2016 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only: 1-408-435-7088
Standardized Terminology in Pancreatobiliary Cytology: The Papanicolaou Society Guidelines
 Standardized Terminology in Pancreatobiliary Cytology: The Papanicolaou Society Guidelines Barbara Ann Centeno. M.D. Vice-Chair, Clinical Services, Anatomic Pathology Assistant Chief, Pathology Service
Standardized Terminology in Pancreatobiliary Cytology: The Papanicolaou Society Guidelines Barbara Ann Centeno. M.D. Vice-Chair, Clinical Services, Anatomic Pathology Assistant Chief, Pathology Service
7th Annual Symposium on Gastrointestinal Cancers " St. Louis, Mo, 9/20/08
 Molecular markers to aid in early diagnosis of pancreatic cancer Michael Goggins, MD Professor of Pathology, Medicine and Oncology Johns Hopkins Medical Institutions, Baltimore, MD 7th Annual Symposium
Molecular markers to aid in early diagnosis of pancreatic cancer Michael Goggins, MD Professor of Pathology, Medicine and Oncology Johns Hopkins Medical Institutions, Baltimore, MD 7th Annual Symposium
Video Microscopy Tutorial 19
 Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Combatting Pancreatic Cancer: Keys to Early Recognition and Diagnosis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/combatting-pancreatic-cancer-keys-earlyrecognition-and-diagnosis/7286/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/combatting-pancreatic-cancer-keys-earlyrecognition-and-diagnosis/7286/
Cystic Pancreatic Lesions: Approach to Diagnosis
 Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Validation of international consensus guideline 2012 for intraductal papillary mucinous neoplasm of pancreas
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/1.4174/astr.216.9.3.124 Annals of Surgical Treatment and Research Validation of international consensus guideline 212 for intraductal
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/1.4174/astr.216.9.3.124 Annals of Surgical Treatment and Research Validation of international consensus guideline 212 for intraductal
A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients
 LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
Pietro Gambitta, Paolo Aseni, Paola Fontana, Emilia Bareggi, Edoardo Forti, Alberto Tringali, Francesco Molteni, Maurizio Vertemati
 Gambitta et al. 100 CASE ORIGINAL REPORT ARTICLE PEER REVIEWED OPEN ACCESS Advantage of endoscopic-ultrasound-fine-needle aspiration associated to Sendai clinical guidelines in detecting the malignant
Gambitta et al. 100 CASE ORIGINAL REPORT ARTICLE PEER REVIEWED OPEN ACCESS Advantage of endoscopic-ultrasound-fine-needle aspiration associated to Sendai clinical guidelines in detecting the malignant
Research Article Surgery for Cystic Pancreatic Lesions in the Post-Sendai Era: A Single Institution Experience
 HPB Surgery Volume 2015, Article ID 847837, 5 pages http://dx.doi.org/10.1155/2015/847837 Research Article Surgery for Cystic Pancreatic Lesions in the Post-Sendai Era: A Single Institution Experience
HPB Surgery Volume 2015, Article ID 847837, 5 pages http://dx.doi.org/10.1155/2015/847837 Research Article Surgery for Cystic Pancreatic Lesions in the Post-Sendai Era: A Single Institution Experience
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES
 ORIGINAL ARTICLE PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES Murat Kılıç,1, Ahmet Erdoğan, Cengiz Ceylan, Barış Saylam and Mesut Tez Department of General Surgery, Numune Training and Research Hospital,
ORIGINAL ARTICLE PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES Murat Kılıç,1, Ahmet Erdoğan, Cengiz Ceylan, Barış Saylam and Mesut Tez Department of General Surgery, Numune Training and Research Hospital,
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Pancreatic Cytopathology: The Solid Neoplasms
 Pancreatic Cytopathology: The Solid Neoplasms Syed Z. Ali, M.D. Professor of Pathology and Radiology Director of Cytopathology The Johns Hopkins Hospital Baltimore, Maryland Pancreatic Cytopathology: Past,
Pancreatic Cytopathology: The Solid Neoplasms Syed Z. Ali, M.D. Professor of Pathology and Radiology Director of Cytopathology The Johns Hopkins Hospital Baltimore, Maryland Pancreatic Cytopathology: Past,
Appendix 4: WHO Classification of Tumours of the pancreas 17
 S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
S3.01 The WHO histological tumour type must be recorded. CS3.01a The histological type of the tumour should be recorded based on the current WHO classification 17 (refer to Appendices 4-7). Appendix 4:
Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA
 Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA Jack Yang, MD Department of Pathology, Medical University of South Carolina Objectives Understand the indication of EUS
Pancreatitis: A Potential Pitfall in Endoscopic Ultrasound Guided Pancreatic FNA Jack Yang, MD Department of Pathology, Medical University of South Carolina Objectives Understand the indication of EUS
REVIEW ARTICLE INTRODUCTION SURGICAL MANAGEMENT ABSTRACT
 JOP. J Pancreas (Online) 2015 Sep 08; 16(5):417-424. REVIEW ARTICLE Fate of the Pancreatic Remnant Following Curative Intent Surgical Resection for Intraductal Pancreatic Mucinous Neoplasms: An Overview
JOP. J Pancreas (Online) 2015 Sep 08; 16(5):417-424. REVIEW ARTICLE Fate of the Pancreatic Remnant Following Curative Intent Surgical Resection for Intraductal Pancreatic Mucinous Neoplasms: An Overview
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes
 Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Morphologic features in cystic lesions of pancreas-a retrospective analysis
 International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review
 Case report A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review Martín A. Gómez Z., MD, 1 Cristian Melgar, MD, 2 Germán Junca, MD. 3 1 Gastroenterology Professor,
Case report A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review Martín A. Gómez Z., MD, 1 Cristian Melgar, MD, 2 Germán Junca, MD. 3 1 Gastroenterology Professor,
Population based studies in Pancreatic Diseases. Satish Munigala
 Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
Population based studies in Pancreatic Diseases Satish Munigala 1 Definition Population-based studies aim to answer research questions for defined populations 1 Generalizable to the whole population addressed
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
3/28/2017. Disclosure of Relevant Financial Relationships. GU Evening Subspecialty Case Conference. Differential Diagnosis:
 GU Evening Subspecialty Case Conference Rajal B. Shah, M.D. VP, Medical Director, Urologic Pathology Miraca Life Sciences, Irving, Texas Clinical Associate Professor of Pathology Baylor College of Medicine,
GU Evening Subspecialty Case Conference Rajal B. Shah, M.D. VP, Medical Director, Urologic Pathology Miraca Life Sciences, Irving, Texas Clinical Associate Professor of Pathology Baylor College of Medicine,
Overview. Disclosure. PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes. N. Volkan Adsay, MD
 PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes N. Volkan Adsay, MD Professor and Vice-Chair Director of Anatomic Pathology Emory University and Emory Winship Cancer Institute Atlanta,
PRE INVASIVE NEOPLASIA OF BILIARY TREE New Perspectives on Old Themes N. Volkan Adsay, MD Professor and Vice-Chair Director of Anatomic Pathology Emory University and Emory Winship Cancer Institute Atlanta,
CYTOLOGY OF EUS- GUIDED FNA OF THE PANCREAS AND THE UPPER GI TRACT
 CYTOLOGY OF EUS- GUIDED FNA OF THE PANCREAS AND THE UPPER GI TRACT Barbara A. Centeno, M.D. Vice-Chair, Clinical Services Assistant Chief of Pathology Director of Cytopathology Department of Anatomic Pathology/Moffitt
CYTOLOGY OF EUS- GUIDED FNA OF THE PANCREAS AND THE UPPER GI TRACT Barbara A. Centeno, M.D. Vice-Chair, Clinical Services Assistant Chief of Pathology Director of Cytopathology Department of Anatomic Pathology/Moffitt
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup Periods
 Oncology Volume 2009, Article ID 373465, 6 pages doi:10.1155/2009/373465 Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup
Oncology Volume 2009, Article ID 373465, 6 pages doi:10.1155/2009/373465 Case Report A Case Report of Intraductal Papillary-Mucinous Neoplasm of the Pancreas Showing Morphologic Transformation during Followup
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Three Cases of Concomitant Intraductal Papillary Mucinous Neoplasm and Pancreatic Neuroendocrine Tumour
 CASE SERIES Three Cases of Concomitant Intraductal Papillary Mucinous Neoplasm and Pancreatic Neuroendocrine Tumour Nilanjana Tewari 1, Abed M Zaitoun 2, Daniel Lindsay 2, Areeg Abbas 2, Mohammad Ilyas
CASE SERIES Three Cases of Concomitant Intraductal Papillary Mucinous Neoplasm and Pancreatic Neuroendocrine Tumour Nilanjana Tewari 1, Abed M Zaitoun 2, Daniel Lindsay 2, Areeg Abbas 2, Mohammad Ilyas
Cystic lesions of the pancreas
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Neuro-endocrine and pancreatic non-adenocarcinomas. Marc Engelbrecht, AMC, Amsterdam
 Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Value of EUS in early detection of pancreatic ductal adenocarcinomas in patients with intraductal papillary mucinous neoplasms
 22 Original article Value of EUS in early detection of pancreatic ductal adenocarcinomas in patients with intraductal papillary mucinous neoplasms Authors Ken Kamata 1, Masayuki Kitano 1, Masatoshi Kudo
22 Original article Value of EUS in early detection of pancreatic ductal adenocarcinomas in patients with intraductal papillary mucinous neoplasms Authors Ken Kamata 1, Masayuki Kitano 1, Masatoshi Kudo
MULTIMEDIA ARTICLE - Clinical Imaging. Brian KP Goh 1, Yaw-Fui Alexander Chung 1,4, David CE Ng 2, Sathiyamoorthy Selvarajan 3, Khee-Chee Soo 1,4
 MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts Santhi Swaroop Vege, 1 Barry Ziring, 2 Rajeev
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts Santhi Swaroop Vege, 1 Barry Ziring, 2 Rajeev
Patient with incidental pancreatic cyst
 Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
