Deceptive morphologic and epigenetic heterogeneity in diffuse intrinsic pontine glioma
|
|
|
- Julia Harper
- 5 years ago
- Views:
Transcription
1 /, 2017, Vol. 8, (No. 36), pp: Deceptive morphologic and epigenetic heterogeneity in diffuse intrinsic pontine glioma Marianna Bugiani 1,*, Sophie E.M. Veldhuijzen van Zanten 2,3,*, Viola Caretti 4, Pepijn Schellen 3, Eleonora Aronica 5, David P. Noske 3,6, William P. Vandertop 3,7, Gertjan J.L. Kaspers 2,3,8, Dannis G. van Vuurden 2,3, Pieter Wesseling 1,8 and Esther Hulleman 2,3 1 VU University Medical Center, Department of Pathology, Amsterdam, The Netherlands 2 VU University Medical Center, Department of Paediatrics, Division of Oncology/Haematology, Amsterdam, The Netherlands 3 Brain Tumor Center Amsterdam, Cancer Center Amsterdam, VU University Medical Center and Academic Medical Center, Amsterdam, The Netherlands 4 Stanford University School of Medicine, Department of Neurology, Neurosurgery and Pediatrics, Stanford, California, USA 5 Academic Medical Center, Department of Pathology, Amsterdam, The Netherlands 6 VU University Medical Center, Department of Neurosurgery, Amsterdam, The Netherlands 7 VU University Medical Center and Academic Medical Center, Neurosurgical Center Amsterdam, Amsterdam, The Netherlands 8 Prinses Máxima Center for Pediatric Oncology and University Medical Center Utrecht, Utrecht, The Netherlands * These authors have contributed equally to this work Correspondence to: Sophie E.M. Veldhuijzen van Zanten, s.veldhuijzen@vumc.nl Keywords: diffuse intrinsic pontine glioma, histone 3, H3 K27M, trimethylation, intratumoral heterogeneity Received: April 15, 2017 Accepted: June 12, 2017 Published: July 31, 2017 Copyright: Bugiani et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License 3.0 (CC BY 3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. ABSTRACT Historically, the diagnosis of diffuse intrinsic pontine glioma (DIPG) was based on typical imaging findings and clinical characteristics instead of pathology. However, the discovery of ations in histone H3 variants, and the availability of tumor material for molecular analysis, has led to a paradigm shift in DIPG research and clinical practice. Using data from whole-brain autopsies in a series of nine DIPG patients with known histone ational status, we here aim to review histopathological characteristics with special focus on intratumoral heterogeneity (ITH) and histone 3 K27 trimethylation (H3 K27me3). All DIPGs showed marked histologic ITH, with 56% even showing focal areas resembling a WHO grade I phenotype. As expected, H3 K27me3 immunoreactivity was lost in the tumors that were H3 K27M-ated (seven patients; 67% H3.3, 11% H3.1). Strikingly, the H3K27 wildtype tumors (two patients; 22%) also contained H3 K27me3-immunonegative areas. Our study underscores the importance of the choice of the biopsy site, as ITH in DIPGs could theoretically lead to erroneous histological diagnoses with small biopsies. New in this respect is our finding that a substantial number of otherwise typical DIPGs has areas resembling WHO grade I tumors (esp. pilocytic astrocytoma, subependymoma). Furthermore, our study shows that negative H3 K27me3 immunohistochemistry in a DIPG does not imply a H3 K27-ant tumor. Research Paper 60447
2 Table 1: Clinical characteristics of DIPG patients Patient ID Age (y) Gender Symptom duration (w) Treatment at diagnosis Treatment at disease progression M <6 XRT (15x3=45 Gy) F XRT (16x2.8 = 44.8 Gy) Temozolomide F Vincristine, carboplatin M < M <6 XRT (13x3.0=39 Gy) + temozolomide XRT (30x1.8=54Gy) + gemcitabine / HDC / combined targeted therapy PFS (m) OS (m) Temozolomide, imatinib, dichloroacetate M <6 XRT (6x3.0=18 Gy) M <6 XRT (13x3.0=39 Gy) XRT (8x3.0=24 Gy) M <6 XRT (13x3.0=39 Gy) XRT (10x3.0=30 Gy) F <6 XRT (30x1.8=54Gy) + gemcitabine M: male, F: female, y: years, m: months, w: weeks, h: hours, XRT: radiotherapy, HDC: high-dose chemotherapy, PFS: progression-free survival, OS: overall survival INTRODUCTION Diffuse intrinsic pontine glioma (DIPG), one of the deadliest childhood cancers [1], shows marked intratumoral heterogeneity (ITH) in terms of histological phenotype and malignancy grade [2]. Because of this heterogeneity and the possible risks associated with biopsy procedures, DIPG diagnoses have been made solely on clinical and radiological grounds for decades. Owing to the reintroduction of stereotactic and open surgical biopsies and subsequent molecular characterization of these tumors, it was recently demonstrated that over 90% of DIPGs carry a histone H3 K27M ation in the genes encoding H3.3 (H3F3A), H3.2 (HIST2H3C), or H3.1 (HIST1H3B and HIST1H3C). Moreover, it was shown that these ations are spatially conserved and result in both loss of H3 K27 trimethylation (H3 K27me3) and alteration of gene expression profiles, putatively driving gliomagenesis [3]. Since H3 K27 ations are significantly associated with survival, the 2016 World Health Organization (WHO) Classification of Tumours of the Central Nervous System introduced Diffuse midline glioma, H3 K27M-ant as a separate WHO grade IV entity, wherein DIPG is a relatively frequent subgroup [4]. Consequently, immunohistochemistry for H3 K27Mant protein and for H3 K27me3 is now increasingly used to assess the H3 K27 status of DIPGs. Based on these recent discoveries, this study aims to perform integrated morphologic and molecular characterization in a series of DIPG patients in whom whole-brain autopsies were performed. Autopsies were performed according to an established protocol [5] that was approved by the medical ethical committee of the VU University Medical Centre, Amsterdam, The Netherlands. RESULTS Patient characteristics and autopsy procedure All patients fulfilled the diagnostic MRI criteria for DIPG according to Barkovich et al [6], i.e. a T1-weighted hypointense and T2-weighted hyperintense tumor with at least 50% involvement of the pons. Table 1 shows the patient and treatment characteristics. Median age at diagnosis was 9.0 years (range years). In most patients, symptoms preceded presentation by less than 6 weeks. In two patients, symptom duration was longer than three but less than six months. The complaints in the latter cases included gait disturbances and strabismus. All patients except the youngest one received radiotherapy at time of diagnosis (range Gy; Table 1). The median progression-free survival was 5 months (range 1-28 months). At time of progression, three patients received chemotherapy and two underwent re-irradiation. Median overall survival was 11 months (range 4-41 months). Autopsies were performed within 7 hours after death (mean post-mortem time 3 hours). Per autopsy, an average total of 7 tumor samples from the pons, cerebellar peduncles, and cerebellar hemispheres were obtained. Additionally, an average of 27 samples of histopathologically normal tissue were obtained from adjacent areas cranially and caudally within the brainstem and from more distant cerebral regions, resulting in a total of 306 study samples across all patients
3 Table 2: Whole-genome paired-end and Sanger sequencing results Patient ID H3.3 K27M H3.3 G34R/V H3.1 K27M : wildtype, : ant Figure 1: Intratumoral heterogeneity of DIPG (patient VUMC-DIPG-6). (A) axial T2-weighted MR-image; letters correspond to tumor areas illustrated. (B) Gemistocitic morphology of tumor cells and calcifications. (C) High-grade component with necrosis surrounded by pseudopalissading of tumor cells. (C ) In the same area, tumor cells expressing the stem cell markers GFAPδ and CD44. (D) Subependymoma-like component showing negligible mitotic activity (D ), dot-like cytoplasmic immunopositivity for the epithelial membrane antigen (EMA, D ), indicating ependymal differentiation, and immunopositivity for olig2 (D ). (E) High-grade component with microvascular proliferation. (F) Tumor cells infiltrating the gray matter of the pontine nuclei. (G) High-grade component with small cell morphology and brisk mitotic activity (G ). (H) Low-grade component with isolated tumor cells infiltrating the distant white matter and expressing olig2 (H ). In the same area, perivascular clustering of tumor cells immunopositive for neurofilament (NF) kDA (H ). (I) Isolated tumor cells in the distant cerebellar cortex. Bars: 100μm, C 200μm
4 Immunohistochemistry and molecular analysis All DIPGs showed marked histologic ITH including areas with WHO grade II IV histology. Additionally, focal areas were present with a pilocytic astrocytomaand/or subependymoma-like phenotype (3 and 5 cases, respectively), thus resembling WHO grade I lesions (Figure 1). Pilocytic astrocytoma-like regions were characterized by piloid tumor cell processes and presence of Rosenthal fibers, while subependymoma-like areas were paucicellular with marked clustering of tumor cells, some of which showing dot-like EMA-positivity, and some expressing the glial-restricted progenitor cell marker Olig2. Immunohistochemistry confirmed the substantial ITH with respect to astrocytic differentiation and expression of stem cell markers (GFAP, GFAPδ, nestin and CD44), only partly overlapping with the degree of cellular atypia, and revealed at least focal expression of neuronal markers (including synaptophysin and neurofilament kDa). Table 2 shows the results of the whole-genome paired-end sequencing and Sanger sequencing. Six tumors (67%) carried a H3.3 K27M ation, one (11%) carried a H3.1 K27M ation, and two tumors were H3 K27 wildtype (22%). All H3.3 K27M and H3.1 K27M tumors were immunopositive for the ant protein. Strikingly, the H3 K27 wildtype tumors (two patients; 22%) also contained H3 K27me3-immunonegative areas (Figure 2). DISCUSSION Based on our findings in an autopsy series of nine DIPG patients evaluated in the last eight years at the VU University Medical Center Amsterdam, we underscore that DIPG ITH may lead to misinterpretation in biopsy specimens at two distinct levels when using (immuno) histochemistry only: 1. Histologic phenotype.without exception, all DIPGs showed marked histologic ITH. Remarkably, 56% also showed focal areas with a pilocytic astrocytomaand/or subependymoma-like phenotype resembling WHO grade I lesions. This finding is of interest, since many consider WHO grade I lesions not part of the histologic spectrum of DIPG, even in case of typical imaging features. Patients with a WHO grade I lesion upon biopsy were therefore often excluded from clinical DIPG trials. With our results we show that this may have potentially been a false negative decision. Of note, the survival of the patients with WHO grade I-like tumor regions was as poor as that of the others. 2. Immunohistochemical assessment of H3 K27me3/ H3 K27 status. As expected, all H3 K27M tumors (78%) lost H3 K27me3 immunoreactivity, irrespective of histological phenotype and grade. However, the two H3 K27 wildtype neoplasms also contained H3 K27me3- immunonegative areas, which were not clearly related Figure 2: Immunohistochemistry for the H3 K27M-ant protein and H3 K27me3. Patient VUMC-DIPG-6 (H3. 3 K27Mant, left panels) is immunopositive for the ant protein in tumor nuclei and shows H3 K27me3-loss in both high-grade (left) and low-grade (middle-left) components. Patient VUMC-DIPG-1 (H3 K27 wildtype, right panels) is immunonegative for the ant protein in tumor cells, with aspecific microglia staining. Stain against H3 K27me3 shows H3 K27me3-conservation in some areas (middle-right), whereas other areas display H3 K27me3-loss (right). Bars: 100μm
5 to tumor morphology or grade. Using only H3 K27me3 immunohistochemistry may thus lead to a false positive diagnosis of H3 K27-ant glioma. Focal loss of H3 K27me3 has been reported only once in 2 out of 76 highgrade gliomas [7] and may indicate additional mechanisms underlying the previously described dominant-negative effect of the H3 K27-ant protein on H3 K27me3. Further research investigating these mechanisms may help to better understand the H3 K27 wildtype subgroup, with possible diagnostic and therapeutic consequences. If loss of H3 K27me3 actively contributes to a more malignant course of the disease, H3 K27me3 immunodetection could add important information. Multiple biopsies for multiregional H3 K27me3 immunodetection should then be considered, especially when therapies targeting loss of H3 K27me3 could also be partly effective in patients with H3 K27 wildtype tumors. Notably, interpretation of immunohistochemical staining for the H3 K27-ant protein may be challenging, especially as discriminating positive microglial cells from positive tumor cell nuclei can be difficult. Ideally, molecular analysis should be performed for a definitive assessment the H3 K27 status of the tumor. In conclusion, here we demonstrate that histologic phenotype and immunohistochemical staining for H3 K27 status in small DIPG biopsies can be deceptive. From a diagnostic point of view this means that to make the diagnosis DIPG, typical imaging- and clinical signs remain crucial. And, to make the diagnosis of the (overarching) entity diffuse midline glioma, H3 K27Mant, as defined in the WHO 2016 classification, next generation sequencing/sanger sequencing for now seems more reliable than H3 K27M/H3 K27me3 immunohistochemistry. Future studies are needed to assess the correlation between (heterogeneous) focal loss of H3 K27me3 in H3 K27-wildtype DIPGs and the clinical behavior of these tumors. Last but not least, from a therapeutic point of view, the observed spatial heterogeneity in DIPGs suggests that future chemotherapy should be directed against intratumoral polyclonality using multiple drugs, instead of therapies targeting only a single (putative) target. Moreover, combining this with various administration modalities (i.e. systemic and local drug delivery, such as convection enhanced delivery or ultrasound mediated blood-brain barrier disruption) and (re)irradiation schedules may help to better target the full range of this heterogeneous disease. METHODS Whole-brain autopsy was performed in nine DIPG patients diagnosed based on clinical and MRI features [6] according to the ethical approved protocol [5]. The brainstem and cerebellum were separated from the cerebral hemispheres and cut axially. The cerebral hemispheres were cut coronally. Tumor location and extension via direct parenchymal infiltration and leptomeningeal or intraventricular invasion was evaluated macroscopically. Multiple tissue samples were collected from the pons, cerebellar peduncles, cerebellar hemispheres, medulla oblongata, cervical spinal cord, midbrain, thalami, wall of the third ventricle, subventricular zone, basal nuclei, hippocampi, and all cerebral lobes. Both tumorous and histopathologically normal brain tissue were collected. Four-μm-thick sections of formalin-fixed paraffinembedded material were histochemically stained for Hematoxylin & Eosin (H&E). After heat-induced antigen retrieval in 0.01M citrate buffer (ph6), immunohistochemical staining was performed with antibodies against glial fibrillary acidic protein (GFAP; Sigma, G3893, 1:1000), neurofilaments kda (Monosan, 1:10), oligodendrocyte transcription factor 2 (olig2; Abcam, ab33427, 1:400), Ki67 (Dako, M7240, 1:160), epithelial membrane antigen (EMA; Dako, M0613, 1:100), H3.3 K27M (Merck Millipore, ABE419, 1:500) and H3 K27me3 (Abcam, ab24684, 1:100). Immunopositivity was detected with 3,3 -Diaminobenzidine (DAB) as chromogen. Six-μmthick frozen tissue sections were used for fluorescence immunohistochemistry. Tissue sections were fixed in 4% paraformaldehyde, blocked for 30 minutes in phosphate buffered saline supplemented with 0.1% saponin and 5% normal goat serum, and incubated with antibodies isoform GFAP delta (GFAPδ; kind gift of E. Hol, University Medical Centre Utrecht, 1:250 [8]) and CD44 (Hermes3, 1:100 [8]). After incubating with secondary antibodies (Alexa Fluor 488- or 594-tagged; Molecular Probes, 1:400), sections were counterstained with 4,6-diamidino- 2-phenylindole (DAPI; Molecular Probes, 10 ng/ml) and embedded in Fluoromount G (Southern Biotech). All tissue sections were photographed using a Leica DM6000B microscope (Leica Microsystems). Omitting primary antibodies yielded no significant staining. All nine tumors were molecularly characterized by next generation sequencing, and histone variants were validated with Sanger sequencing. Genomic DNA was isolated from DIPG tumors and from non-affected counterpart brain regionsusing the QIAamp DNA mini isolation kit (Qiagen, USA). Next generation sequencing was executed by whole-genome paired-end sequencing as performed by Complete Genomics [9]. Primary data analysis including variant calling was performed and mapped to reference build hg19. Genomic data was further analyzed using the open source CGAtools ( cgatools.sourceforge.net), generating somatic calls for splice sites or coding exons. For Sanger sequencing, the histone 3 sequences of interest were amplified by PCR andsubsequently sequenced by the dideoxy chaintermination method using the ABI PrismTM BigDye Terminator kit (Perkin Elmer, USA), which was run on the ABI Prism Genetic Analyser 3100 automatic DNA autosequencer (Perkin Elmer) and analysed with ABI 60451
6 sequence Alignment Editor software. Primers were designed using Oligo explorer 1.5 software (Genelink primer sequences available upon request) and blasted against the human genome for specificity (NCBI). Abbreviations DAB 3,3 -diaminobenzidine DIPG diffuse intrinsic pontine glioma EMA epithelial membrane antigen GFAP glial fibrillary acidic protein GFAPδ isoform delta of GFAP HIST2H3C gene encoding H3.2 HIST1H3B gene encoding H3.1 HIST1H3C gene encoding H3.1 H3F3A gene encoding H3.3 H3 K27me3 H3 K27 trimethylation H&E hematoxylin & eosin ITH intratumoral heterogeneity olig2 oligodendrocyte transcription factor 2 WHO World Health Organization Author contributions Marianna Bugiani: performed the autopsies, processed the obtained material, analyzed the results and wrote the main body of the manuscript. Sophie E.M. Veldhuijzen van Zanten: obtained the informed consent for the autopsies from the patients and/ or parents, assisted during the autopsies, analyzed the results and wrote the main body of the manuscript. Viola Caretti: assisted during some autopsies, assisted in data analysis Pepijn Schellen: performed the immunohistochemistry and assisted in data analysis Eleonora Aronica: assisted in data analysis David P. Noske: patient s neurosurgeon, assisted in writing the manuscript. William P. Vandertop: patient s neurosurgeon, assisted in writing the manuscript. Gertjan J.L. Kaspers: patient s physician, assisted in writing the manuscript. Dannis G. van Vuurden: patient s physician, assisted in writing the manuscript. Pieter Wesseling: supervised analysis of the results, analyzed the results, assisted in writing the manuscript. Esther Hulleman: supervised analysis of the results, assisted in writing the manuscript. ACKNOWLEDGMENTS None. CONFLICTS OF INTEREST FUNDING DIPG research in our institute is financially supported by the Semmy Foundation (Stichting Semmy). REFERENCES 1. Kambhampati M, Perez JP, Yadavilli S, Saratsis AM, Hill AD, Ho CY, Panditharatna E, Markel M, Packer RJ, Nazarian J. A standardized autopsy procurement allows for the comprehensive study of DIPG biology ; 6:1-8. doi: /oncotarget Epstein F. A staging system for brain stem gliomas. Cancer. 1985; 56: Jones C, Karajannis MA, Jones DT, Kieran MW, Monje M, Baker SJ, Becher OJ, Cho YJ, Gupta N, Hawkins C, Hargrave D, Haas-Kogan DA, Jabado N, et al. Pediatric high-grade glioma: biologically and clinically in need of new thinking. Neuro Oncol. 2016; 9: Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Ellison DW, Figarella-Branger D, Perry A, Reifenberger G, Von Deimling A. WHO Classification of Tumours of the Central Nervous System. IARC Press, Lyon, Caretti V, Jansen MH, van Vuurden DG, Lagerweij T, Bugiani M, Horsman I, Wessels H, van der Valk P, Cloos J, Noske DP, Vandertop WP, Wesseling P, Wurdinger T, et al. Implementation of a multi-institutional diffuse intrinsic pontine glioma autopsy protocol and characterization of a primary cell culture. Neuropathol Appl Neurobiol. 2013; 39: Barkovich AJ, Krischer J, Kun LE, Packer R, Zimmerman RA, Freeman CR, Wara WM, Albright L, Allen JC, Hoffman HJ. Brain stem gliomas: a classification system based on magnetic resonance imaging. Pediatr Neurosurg. 1990; 16: Bender S, Tang Y, Lindroth AM, Hovestadt V, Jones DT, Kool M, Zapatka M, Northcott PA, Sturm D, Wang W, Radlwimmer B, Højfeldt JW, Truffaux N, et al. Reduced H3K27me3 and DNA hypomethylation are major drivers of gene expression in K27M ant pediatric high-grade gliomas. Cancer Cell. 2013; 24: Bugiani M, Boor I, van Kollenburg B, Postma N, Polder E, van Berkel C, van Kesteren RE, Windrem MS, Hol EM, Scheper GC, Goldman SA, van der Knaap MS. Defective glial maturation in vanishing white matter disease. J Neuropathol Exp Neurol. 2011; 70: Drmanac R, Sparks AB, Callow MJ, Halpern AL, Burns NL, Kermani BG, Carnevali P, Nazarenko I, Nilsen GB, Yeung G, Dahl F, Fernandez A, Staker B. Human genome sequencing using unchained base reads on self-assembling DNA nanoarrays. Science. 2010; 327: None
Deceptive morphologic and epigenetic heterogeneity in diffuse intrinsic pontine glioma
 CHAPTER 5 Deceptive morphologic and epigenetic heterogeneity in diffuse intrinsic pontine glioma Veldhuijzen van Zanten SEM*, Bugiani M*, Caretti V, Schellen P, Aronica E, Noske DP, Vandertop WP, Kaspers
CHAPTER 5 Deceptive morphologic and epigenetic heterogeneity in diffuse intrinsic pontine glioma Veldhuijzen van Zanten SEM*, Bugiani M*, Caretti V, Schellen P, Aronica E, Noske DP, Vandertop WP, Kaspers
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
CLINICAL STUDY. J Neurooncol (2017) 134: DOI /s
 J Neurooncol (2017) 134:231 240 DOI 10.1007/s11060-017-2514-9 CLINICAL STUDY External validation of the diffuse intrinsic pontine glioma survival prediction model: a collaborative report from the International
J Neurooncol (2017) 134:231 240 DOI 10.1007/s11060-017-2514-9 CLINICAL STUDY External validation of the diffuse intrinsic pontine glioma survival prediction model: a collaborative report from the International
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Enterprise Interest None
 Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
Enterprise Interest None Heterogeneous chromosomal profiles in a unique series of DIPG in children and young adults European Congress of Pathology Amsterdam, 6 th September 2017 Charlotte Dufour, Romain
A case of multinodular high-grade neuroepithelial tumor
 Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
Brain Tumor Pathol (2011) 28:253 257 DOI 10.1007/s10014-011-0032-6 CASE REPORT A case of multinodular high-grade neuroepithelial tumor with ependymal differentiation Kensaku Kamada Yuko Tanaka Takayuki
WHY BIOPSY? Diagnosis and Research
 WHY BIOPSY? Diagnosis and Research 9 2 4 1 3 1 1. Diagnosis only by Imaging (like no other tumor) The issue of Typical versus Atypical DIPG T1 FLAIR Gad. T2 Tractography Functional MRI Diffusion/Perfusion
WHY BIOPSY? Diagnosis and Research 9 2 4 1 3 1 1. Diagnosis only by Imaging (like no other tumor) The issue of Typical versus Atypical DIPG T1 FLAIR Gad. T2 Tractography Functional MRI Diffusion/Perfusion
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls. Rob Macaulay Neuropathologist, MCC October 21, 2017
 Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
Classification of Diffuse Gliomas: Progress, Pearls and Pitfalls Rob Macaulay Neuropathologist, MCC October 21, 2017 Objectives Explain why the designation high grade glioma is preferable to GBM for intraoperative
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017
 AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
AMERICAN ASSOCIATION OF NEUROPATHOLOGISTS COMPANION SOCIETY MEETING at the 106 th ANNUAL MEETING OF THE USCAP San Antonio, March 4, 2017 SYLLABUS Papillary Tumor of the Pineal Region and the Differential
Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child
 Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
Case Reports in Oncological Medicine Volume 2013, Article ID 815923, 4 pages http://dx.doi.org/10.1155/2013/815923 Case Report Atypical Presentation of Atypical Teratoid Rhabdoid Tumor in a Child Y. T.
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
SUPPLEMENTARY FIG. S2. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of dnscs.
 Supplementary Data SUPPLEMENTARY FIG. S1. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of anpcs. A panel of lineage-specific markers were used
Supplementary Data SUPPLEMENTARY FIG. S1. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of anpcs. A panel of lineage-specific markers were used
Morphological features and genetic alterations
 Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Morphological features and genetic alterations Tutor : Audrey Rousseau Caget Lise: Université d Angers Iorio Vittoria: Seconda Università degli studi di Napoli Manaila Roxana: Iuliu Hatieganu University
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Gliomas in the 2016 WHO Classification of CNS Tumors
 Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma
 From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
From a suspicious cystic pineal gland to pineoblastoma in a patient with familial unilateral retinoblastoma Marcus C de Jong, Annette C Moll, Sophia Göricke, Paul van der Valk, Wijnanda A Kors, Jonas A
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence
 PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
PEDIATRIC RHABDOID MENINGIOMA Anna Maria Buccoliero Department of Biomedicine, Careggi Hospital Florence CLINICAL HISTORY A 3-year-old boy, with a recent history of seizures, was admitted to the Neurosurgery
Challenging Paediatric Brain Tumours. ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin
 Challenging Paediatric Brain Tumours ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin Overview (i) Paediatric malignancy (ii) Central nervous system tumours (iii) Diffuse Intrinsic
Challenging Paediatric Brain Tumours ASP Belfast March 2017 Dr Jane Pears Consultant Paediatric Oncologist, Dublin Overview (i) Paediatric malignancy (ii) Central nervous system tumours (iii) Diffuse Intrinsic
A standardized autopsy procurement allows for the comprehensive study of DIPG biology.
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Pathology Faculty Publications Pathology 1-24-2015 A standardized autopsy procurement allows for the
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Pathology Faculty Publications Pathology 1-24-2015 A standardized autopsy procurement allows for the
Announcing cimpact-now: the Consortium to Inform Molecular and Practical Approaches to CNS Tumor Taxonomy
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2017 Announcing cimpact-now: the Consortium to Inform Molecular and Practical
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2017 Announcing cimpact-now: the Consortium to Inform Molecular and Practical
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Genomic Methods in Cancer Epigenetic Dysregulation
 Genomic Methods in Cancer Epigenetic Dysregulation Clara, Lyon 2018 Jacek Majewski, Associate Professor Department of Human Genetics, McGill University Montreal, Canada A few words about my lab Genomics
Genomic Methods in Cancer Epigenetic Dysregulation Clara, Lyon 2018 Jacek Majewski, Associate Professor Department of Human Genetics, McGill University Montreal, Canada A few words about my lab Genomics
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Human Pontine Glioma Cells Can Induce Murine Tumors
 Chapter 2 Human Pontine Glioma Cells Can Induce Murine Tumors Viola Caretti, A. Charlotte P. Sewing, Tonny Lagerweij, Pepijn Schellen Marianna Bugiani, Marc H. A. Jansen, Dannis G. van Vuurden, Anna C.
Chapter 2 Human Pontine Glioma Cells Can Induce Murine Tumors Viola Caretti, A. Charlotte P. Sewing, Tonny Lagerweij, Pepijn Schellen Marianna Bugiani, Marc H. A. Jansen, Dannis G. van Vuurden, Anna C.
Nature Genetics: doi: /ng.2995
 Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
Supplementary Figure 1 Kaplan-Meier survival curves of patients with brainstem tumors. (a) Comparison of patients with PPM1D mutation versus wild-type PPM1D. (b) Comparison of patients with PPM1D mutation
American Journal of. Medical Case Reports. CAM5.2 Expression in Metastatic Tumours of CNS: A Diagnostic Tool
 American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
American Journal of American Journals of Medical Case Reports http://ivyunion.org/index.php/ajmcr/index Medical Case Reports Mathur SK et al. American Journal of Medical Case Reports 2014, 2:1-8 Vol 2,
Title. CitationBrain Tumor Pathology, 34(4): Issue Date Doc URL. Rights. Type. Additional There Information.
 Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
Title Diencephalic pediatric low-grade glioma harboring th sequential biopsy specimens Ishi, Yukitomo; Hatanaka, Kanako C.; Yamaguchi, Shig Author(s) Terasaka, Shunsuke; Houkin, Kiyohiro CitationBrain
2017 Diagnostic Slide Session Case 3
 2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
2017 Diagnostic Slide Session Case 3 Andrew Gao, MD Lili-Naz Hazrati, MD, PhD Cynthia Hawkins, MD, PhD Hospital for Sick Children and University of Toronto, Toronto, Canada Disclosures: none Clinical History
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case
 OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case --Manuscript Draft-- Manuscript Number: Full Title: Short Title: Article Type: Section/Category:
OMICS PUBLISHING GROUP/Clinical Meningioma with remarkable multiple rosette formation: A diagnostically difficult case --Manuscript Draft-- Manuscript Number: Full Title: Short Title: Article Type: Section/Category:
Explain the laboratory diagnosis of Rabies?
 Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
Explain the laboratory diagnosis of Rabies? The standard test for rabies testing is dfa. This test has been thoroughly evaluated for more than 40 years, and is recognized as the most rapid and reliable
Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum
 Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Case Reports in Pathology Volume 2012, Article ID 718651, 4 pages doi:10.1155/2012/718651 Case Report Complex Form Variant of Dysembryoplastic Neuroepithelial Tumor of the Cerebellum Jesús Vaquero, 1,
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement
 The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
The Open Medical Imaging Journal, 2012, 6, 103-107 103 Open Access Primary Central Nervous System Lymphoma with Lateral Ventricle Involvement Yumi Oie 1,*, Kazuhiro Murayama 1, Shinya Nagahisa 2, Masato
New Imaging Concepts in Central Nervous System Neoplasms
 New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
New Imaging Concepts in Central Nervous System Neoplasms Maarten Lequin Department of Pediatric Radiology Wilhelmina Children s Hospital/University Medical Center Utrecht New Imaging Concepts in Central
CHINESE MEDICAL ASSOCIATION
 Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Zhu et al. Chinese Neurosurgical Journal (2017) 3:22 DOI 10.1186/s41016-017-0087-2 CHINESE NEUROSURGICAL SOCIETY CASE REPORT CHINESE MEDICAL ASSOCIATION Anaplastic pleomorphic xanthoastrocytoma with disseminated
Ma l i g n a n t glial tumors are located most frequently. Exophytic giant cell glioblastoma of the medulla oblongata. Case report.
 J Neurosurg 110:589 593, 2009 Exophytic giant cell glioblastoma of the medulla oblongata Case report Go e t z Lu e tj e n s, 1 M. Java d Mir z aya n, M.D., 1 Al m u t h Br a n d i s, M.D., 2 a n d Jo a
J Neurosurg 110:589 593, 2009 Exophytic giant cell glioblastoma of the medulla oblongata Case report Go e t z Lu e tj e n s, 1 M. Java d Mir z aya n, M.D., 1 Al m u t h Br a n d i s, M.D., 2 a n d Jo a
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
USCAP Neuropathology. Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC
 USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
F-FDG PET standard uptake values of the normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma
 CHAPTER F-FDG PET standard uptake values of the normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma Jansen MHA, Kloet RW, van Vuurden DG, Veldhuijzen van Zanten
CHAPTER F-FDG PET standard uptake values of the normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma Jansen MHA, Kloet RW, van Vuurden DG, Veldhuijzen van Zanten
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or
 monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Tavakoli NP, Wang H, Dupuis M, et al. Fatal case of deer tick
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Tavakoli NP, Wang H, Dupuis M, et al. Fatal case of deer tick
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Supplemental Information. Molecular, Pathological, Radiological, and Immune. Profiling of Non-brainstem Pediatric High-Grade
 Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Cancer Cell, Volume 33 Supplemental Information Molecular, Pathological, Radiological, and Immune Profiling of Non-brainstem Pediatric High-Grade Glioma from the HERBY Phase II Randomized Trial Alan Mackay,
Importance of initial aggressive treatment for pineal parenchymal tumor of intermediate differentiation: A case report and review of literature
 Practical Radiation Oncology (2013) 3, e29 e34 www.practicalradonc.org Teaching Case Importance of initial aggressive treatment for pineal parenchymal tumor of intermediate differentiation: A case report
Practical Radiation Oncology (2013) 3, e29 e34 www.practicalradonc.org Teaching Case Importance of initial aggressive treatment for pineal parenchymal tumor of intermediate differentiation: A case report
In vivo reprogramming reactive glia into ipscs to produce new neurons in the
 In vivo reprogramming reactive glia into ipscs to produce new neurons in the cortex following traumatic brain injury Xiang Gao 1, Xiaoting Wang 1, Wenhui Xiong 1, Jinhui Chen 1, * 1 Spinal Cord and Brain
In vivo reprogramming reactive glia into ipscs to produce new neurons in the cortex following traumatic brain injury Xiang Gao 1, Xiaoting Wang 1, Wenhui Xiong 1, Jinhui Chen 1, * 1 Spinal Cord and Brain
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM LOW GRADE GLIOMAS CNS Site Group Low Grade Gliomas Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING
Prognostic factors in pediatric brain-stem gliomas
 J Neurosurg 65:751-755, 1986 Prognostic factors in pediatric brain-stem gliomas A. LLAND ALBRIGHT, M.D., A. NRMAN GUTHKLCH, M.CH., F.R.C.S., RGR J. PACKR, M.D., RBRT A. PRIC, M.D., AND LUCY B. RURK, M.D.
J Neurosurg 65:751-755, 1986 Prognostic factors in pediatric brain-stem gliomas A. LLAND ALBRIGHT, M.D., A. NRMAN GUTHKLCH, M.CH., F.R.C.S., RGR J. PACKR, M.D., RBRT A. PRIC, M.D., AND LUCY B. RURK, M.D.
A case of multicentric gliomas in both supra- and infratentorial regions with different histology: a case report
 Inoue et al. World Journal of Surgical Oncology (2016) 14:152 DOI 10.1186/s12957-016-0907-4 CASE REPORT Open Access A case of multicentric gliomas in both supra- and infratentorial regions with different
Inoue et al. World Journal of Surgical Oncology (2016) 14:152 DOI 10.1186/s12957-016-0907-4 CASE REPORT Open Access A case of multicentric gliomas in both supra- and infratentorial regions with different
Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1.
 Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1. Youngsoo Lee, Sachin Katyal, Yang Li, Sherif F. El-Khamisy, Helen R. Russell, Keith W. Caldecott and Peter J. McKinnon.
Genesis of cerebellar interneurons and the prevention of neural DNA damage require XRCC1. Youngsoo Lee, Sachin Katyal, Yang Li, Sherif F. El-Khamisy, Helen R. Russell, Keith W. Caldecott and Peter J. McKinnon.
IDH1 R132H/ATRX Immunohistochemical validation
 IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
IDH1 R132H/ATRX Immunohistochemical validation CIQC/DSM 2016 12 June 2016 0835-0905 Stephen Yip, M.D., Ph.D., FRCPC University of British Columbia Disclosure Statement I have nothing to disclose I will
21/03/2017. Disclosure. Practice Changing Articles in Neuro Oncology for 2016/17. Gliomas. Objectives. Gliomas. No conflicts to declare
 Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Practice Changing Articles in Neuro Oncology for 2016/17 Disclosure No conflicts to declare Frances Cusano, BScPharm, ACPR April 21, 2017 Objectives Gliomas To describe the patient selection, methodology
Neurocytoma a Rare Intraventricular Tumor
 Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Neurocytoma a Rare Intraventricular Tumor J. A. Mallick,S. A. Ali ( Department of Oncology, Liaquat National Postgraduate Medical Centre, Karachi. ) Introduction Central neurocytoma was first recognized
Gangliogliomas: A Report of Five Cases
 Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
Case Report Gangliogliomas: A Report of Five Cases Nair V, Suri VS, Tatke M, Saran RK, Malhotra V, Singh D* Departments of Pathology and *Neurosurgery, G. B. Pant Hospital, New Delhi, India. Correspondence
BAH1 - Primary Glioblastoma
 BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR
 Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
Gastric Carcinoma with Lymphoid Stroma: Association with Epstein Virus Genome demonstrated by PCR Pages with reference to book, From 305 To 307 Irshad N. Soomro,Samina Noorali,Syed Abdul Aziz,Suhail Muzaffar,Shahid
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas
 The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular entities
 Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
Wood et al. Diagnostic Pathology (2019) 14:29 https://doi.org/10.1186/s13000-019-0802-8 REVIEW Applications of molecular neuro-oncology - a review of diffuse glioma integrated diagnosis and emerging molecular
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Subcutaneous tumor seeding after biopsy in gliomatosis cerebri
 J Neurooncol (2012) 106:431 435 DOI 10.1007/s11060-011-0678-2 LETTER TO THE EDITOR Subcutaneous tumor seeding after biopsy in gliomatosis cerebri Dennis R. Buis Paul van der Valk Philip C. De Witt Hamer
J Neurooncol (2012) 106:431 435 DOI 10.1007/s11060-011-0678-2 LETTER TO THE EDITOR Subcutaneous tumor seeding after biopsy in gliomatosis cerebri Dennis R. Buis Paul van der Valk Philip C. De Witt Hamer
Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma
 Supplementary information for: Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma Rintaro Hashizume 1, Noemi Andor 2, Yuichiro Ihara 2, Robin Lerner 2, Haiyun
Supplementary information for: Pharmacologic inhibition of histone demethylation as a therapy for pediatric brainstem glioma Rintaro Hashizume 1, Noemi Andor 2, Yuichiro Ihara 2, Robin Lerner 2, Haiyun
Cynthia Hawkins. Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada
 Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
Cynthia Hawkins Division of Pathology, Labatt Brain Tumour Research Centre, The Hospital for Sick Children, University of Toronto, Canada To apply a practical diagnostic approach to pediatric high grade
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Clinical significance of genetic analysis in glioblastoma treatment
 Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
Clinical significance of genetic analysis in glioblastoma treatment Department of Neurosurgery, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Koji Yoshimoto Can we get prognostic
Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report
 Int J Clin Exp Med 2018;11(9):10111-10115 www.ijcem.com /ISSN:1940-5901/IJCEM0070674 Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report Qianlei Liang 1*, Xin Chen 2*,
Int J Clin Exp Med 2018;11(9):10111-10115 www.ijcem.com /ISSN:1940-5901/IJCEM0070674 Case Report Intraparenchymal frontal lobe ependymoma without rosettes: a case report Qianlei Liang 1*, Xin Chen 2*,
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma
 Jansen et al. EJNMMI Research 2014, 4:8 ORIGINAL RESEARCH Open Access 18 F-FDG PET standard uptake values of the normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma
Jansen et al. EJNMMI Research 2014, 4:8 ORIGINAL RESEARCH Open Access 18 F-FDG PET standard uptake values of the normal pons in children: establishing a reference value for diffuse intrinsic pontine glioma
Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille
 Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Brainstem diffuse gliomas: radiologic findings.
 Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma
 AJNR Am J Neuroradiol 26:804 808, April 2005 Case Report MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma Sait Albayram, Efsun Urger, Buge Oz, Ali Kafadar, Civan Islak,
AJNR Am J Neuroradiol 26:804 808, April 2005 Case Report MR Imaging of Pial Melanosis Secondary to a Posterior Fossa Melanotic Ependymoma Sait Albayram, Efsun Urger, Buge Oz, Ali Kafadar, Civan Islak,
Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry
 Original Article Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry Badhe Prerna B, Chauhan Pritika P, Mehta Nishaki K Departments of Pathology, Seth G. S. Medical
Original Article Brainstem gliomas A clinicopathological study of 45 cases with p53 immunohistochemistry Badhe Prerna B, Chauhan Pritika P, Mehta Nishaki K Departments of Pathology, Seth G. S. Medical
Joana Ramalho, MD C. Ryan Miller, MD, PhD
 Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
Joana Ramalho, MD C. Ryan Miller, MD, PhD Case 1 3 month old baby girl Presented with new onset of seizures Newborn. Questionable blurring of the gray-white junction within the right occipital lobe. Findings
PROGRESS UPDATE. Evan T. Mandeville DIPG Research Fund
 PROGRESS UPDATE Evan T. Mandeville DIPG Research Fund October 2017 EXECUTIVE SUMMARY Investigators at Dana-Farber Cancer Institute are global leaders in pediatric brain tumor research and patient care,
PROGRESS UPDATE Evan T. Mandeville DIPG Research Fund October 2017 EXECUTIVE SUMMARY Investigators at Dana-Farber Cancer Institute are global leaders in pediatric brain tumor research and patient care,
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
University Journal of Surgery and Surgical Specialties
 University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 DORSAL INTRAMEDULLARY SUBEPENDYMOMA - A RARE CASE REPORT WITH LITERATURE REVIEW BABA DHOULATH KHAN MOHAMEDISMAIL
University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 DORSAL INTRAMEDULLARY SUBEPENDYMOMA - A RARE CASE REPORT WITH LITERATURE REVIEW BABA DHOULATH KHAN MOHAMEDISMAIL
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases
 Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Supratentorial Gangliocytoma Mimicking Extra-axial Tumor: A Report of Two Cases Ho Sung Kim, MD 1 Ho Kyu Lee, MD 1 Ae Kyung Jeong, MD 1 Ji Hoon Shin, MD 1 Choong Gon Choi, MD 1 Shin Kwang Khang, MD 2 We
Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES. VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology
 Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology HANDLING the BRAIN at AUTOPSY: What to FIX vs. what to FREEZE? --no need to be
Vascular Cognitive Impairment-- NEUROPATHOLOGIC ISSUES VCI vs. IVD/DEMENTIA with VASCULAR DISEASE (IVD) advanced pathology HANDLING the BRAIN at AUTOPSY: What to FIX vs. what to FREEZE? --no need to be
HHS Public Access Author manuscript Nat Genet. Author manuscript; available in PMC 2012 September 01.
 Somatic Histone H3 Alterations in Paediatric Diffuse Intrinsic Pontine Gliomas and Non-Brainstem Glioblastomas Gang Wu 1,*, Alberto Broniscer 2,*, Troy A McEachron 3,*, Charles Lu 4, Barbara S Paugh 3,
Somatic Histone H3 Alterations in Paediatric Diffuse Intrinsic Pontine Gliomas and Non-Brainstem Glioblastomas Gang Wu 1,*, Alberto Broniscer 2,*, Troy A McEachron 3,*, Charles Lu 4, Barbara S Paugh 3,
2018 Diagnostic Slide Session Case #8
 2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
2018 Diagnostic Slide Session Case #8 Angela N. Viaene, MacLean P. Nasrallah, and Zissimos Mourelatos Hospital of the University of Pennsylvania AANP June 9, 2018 Disclosures: none Clinical History Healthy,
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A Case Report
 CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
CASE REPORT Brain Tumor Res Treat 2016;4(2):133-137 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.133 A Stable Secondary Gliosarcoma with Extensive Systemic Metastases: A
UW Medicine Neuropathology
 Neuropathology in Patient Care Surgical Neuropathology is that subspecialty of pathology that provides diagnoses on biopsies from the brain, spinal cord, skeletal muscle, peripheral nerve, and eye. In
Neuropathology in Patient Care Surgical Neuropathology is that subspecialty of pathology that provides diagnoses on biopsies from the brain, spinal cord, skeletal muscle, peripheral nerve, and eye. In
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MEDULLOBLASTOMA AND PNET CNS Site Group Medulloblastoma and PNET Author: Dr. Norm Laperriere 1. INTRODUCTION 3 2. PREVENTION
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
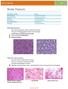 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
An enterogenous cyst with atypical pathological findings and chemical meningitis
 DOI 10.1186/s40064-016-3677-0 CASE STUDY Open Access An enterogenous cyst with atypical pathological findings and chemical meningitis Lu Wang 1, Xiaona Chang 2, Chao Fu 1, Weidong Yu 1 and Xiaoxuan Fang
DOI 10.1186/s40064-016-3677-0 CASE STUDY Open Access An enterogenous cyst with atypical pathological findings and chemical meningitis Lu Wang 1, Xiaona Chang 2, Chao Fu 1, Weidong Yu 1 and Xiaoxuan Fang
Fourth Ventricular Lesions in Metastatic Gliomas: A Rare Predilection?
 CASE REPORT Brain Tumor Res Treat 2017;5(1):24-29 / pissn 2288-2405 / eissn 2288-2413 https://doi.org/10.14791/btrt.2017.5.1.24 Fourth Ventricular Lesions in Metastatic Gliomas: A Rare Predilection? Mohammed
CASE REPORT Brain Tumor Res Treat 2017;5(1):24-29 / pissn 2288-2405 / eissn 2288-2413 https://doi.org/10.14791/btrt.2017.5.1.24 Fourth Ventricular Lesions in Metastatic Gliomas: A Rare Predilection? Mohammed
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
SALSA MLPA probemix P315-B1 EGFR
 SALSA MLPA probemix P315-B1 EGFR Lot B1-0215 and B1-0112. As compared to the previous A1 version (lot 0208), two mutation-specific probes for the EGFR mutations L858R and T709M as well as one additional
SALSA MLPA probemix P315-B1 EGFR Lot B1-0215 and B1-0112. As compared to the previous A1 version (lot 0208), two mutation-specific probes for the EGFR mutations L858R and T709M as well as one additional
