Intrathoracic neural tumours
|
|
|
- James Flynn
- 5 years ago
- Views:
Transcription
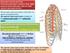
1 Intrathoracic neural tumours K. G. DAVIDSON, P. R. WALBAUM, AND R. J. M. McCORMACK From the Thoracic Surgery Department, City Hospital, Edinburgh, UK Thorax, 1978, 33, Davidson, K. G., Walbaum, P. R., and McCormack, R. J. M. (1978). Thorax, 33, Intrathoracic neural tumours. The experience of one regional thoracic surgical unit in managing intrathoracic neural tumours over a 25-year period is presented. Neural tumour was diagnosed in 55 patients, of whom 41 were asymptomatic. In 11 patients complete resection was not achieved-the reasons for this and its effect on the outcome of the patient are discussed. There were 52 posterior mediastinal and three lateral chest wall tumours. The pathological distribution was as follows-benign nerve sheath tumours (neurofibroma, neurilemoma) 39, ganglioneuroma 13, and neuroblastoma 3. One neurofibroma recurred as a neurosarcoma six years after its apparently complete resection and was removed by an extensive resection at reoperation. One neuroblastoma recurred within the spinal canal four years after incomplete excision at thoracotomy-this patient died subsequently of widespread metastatic neuroblastoma. No other tumour is known to have recurred. Intrathoracic neural tumours are uncommon but account for about 75% of tumours of the posterior mediastinum (Curreri and Gale, 1949). The terminology of these tumours varies throughout the world, and the pathological classification into distinct types on the basis of the cell of origin can be difficult. In this paper the benign tumour arising from the Schwann cell is called neurilemoma and that arising from the nerve sheath is called neurofibroma. Occasionally features of neurilemoma and neurofibroma co-exist, and this mixed pattem is best accepted as a benign nerve sheath tumour without attempting further classification. The malignant form of these two tumours is neurosarcoma. Benign tumours of nerve cell origin, most of which arise from the autonomic nervous system, are called ganglioneuromas. There is, however, a complete spectrum of differentiation between the benign ganglioneuroma and the malignant neuroblastoma. Unfortunately, many of these 359 tumours of nerve cell origin are large and, while in one area the appearances may be quite benign, it is common to find other areas where the cellular pattern is much less differentiated. This is further complicated by the fact that such tumours in young children may show areas of very poor differentiation and may yet behave as benign ganglioneuromas. Tumours of the paraganglion cells-phaeochromocytoma and chemodectoma-have not been included in this series, although embryologically they may originate from neural crest tissue. The presentation and investigation of patients with intrathoracic neural tumours has been fully discussed elsewhere (Cruickshank, 1957; Morrison, 1958; Le Roux, 1960; Oosterwijk and Swierenga, 1968) -they are reviewed only briefly here. The pathological behaviour patterns are looked at in more detail with particular emphasis on those factors that determine outcome. Patients Between 1949 and 1974, 55 patients with intrathoracic neural tumours were seen in this unit. The male to female ratio was 1: 1,3, and the slight female preponderance is typical of that found in other series. The age range at presentation was 7 months to 63 years (average 33 years). The distribution of tumour type within the various age groups is shown in Fig. 1. As would be expected, most tumours of nerve cell origin, both benign and malignant, occurred in the younger age groups, and the average age of this subgroup was 18. The tumours affected left and right sides of the chest with equal frequency and were evenly distributed from apex of thorax to diaphragm (Fig. 2). There were 52 posterior mediastinal neural tumours and three neurofibromas arising from intercostal nerves of the lateral chest wall.
2 360 (A 0 o a males: females * Nerve sheath tumours a Nerve cell tumours 03 Malignant tumours Age Fig. 1 Relative incidence of different types of neural tumour in different age groups. Fig. 2 Presentation Right side 27 Left side 25 Anatomical distribution of neural tumours. In this series 75% of the patients were asymptomatic and their tumour was a chance finding on routine chest radiography (Table 1). Three patients had intrathoracic neurofibromas as manifestations of von Recklinghausen's disease. Neurological disturbances produced by these tumours were uncommon-only four patients complained of pain in the distribution of the nerves affected by their tumour. One baby with a large neuroblastoma in K. G. Davidson, P. R. Walbaum, and R. J. M. McCormack Table 1 Presentation of neural tumours Chance radiographic finding 41 Neurological symptoms Von Recklinghausen's syndrome 3 Pain 4 Pulmonary symptoms Horner's syndrome 2 Dyspnoea 3 Spinal cord pressure 1 Cough 3 the right superior mediastinum presented with Horner's syndrome, as did one adult with a similarly situated benign tumour. One young man presented with symptoms and signs of spinal cord compression at midthoracic level, and was shown to have tumour both in his posterior mediastinum and in his vertebral canal. Respiratory symptoms were also uncommon, being associated mainly with the more bulky type of tumour. Two patients presented with cough and shortness of breath, the tumour in one of these being so large that it had to be cut into three pieces before it could be delivered from the chest. One patient presented with cough as his only symptom and one with breathlessness, but in neither case was the tumour remarkable as regards site or size, and the explanation of these complaints is not clear. Various other symptomatic presentations have been describedpneumonia, empyema, stridor, haemoptysis, hoarseness, and dysphagia, but none of these was seen in any of our patients. Investigations The classical radiographic features of mediastinal neural tumours (Parish, 1957-posterior situation, hair-line margin, uniform density, and D- shaped outline in the lateral projection-were present in most patients (Figs. 3a and b). Ten patients had associated rib deformities adjacent to the lesion, and all ten had benign tumours. Two of these ten patients were also recognised to have vertebral anomalies (Fig. 4). Most patients underwent barium-swallow examination and, as would be expected, oesophageal displacement was occasionally seen in patients with large tumours. A minority in whom there was doubt about the diagnosis were subjected to bronchoscopy, but in no patient was there any bronchoscopic abnormality. In one patient who had an atypical radiographic appearance the diagnosis was made first at mediastinoscopy and confirmed subsequently at thoracotomy. Management The policy of this unit has always been that all patients with suspected intrathoracic neural tumours should have thoracotomy and resection of
3 !: , (a) Thorax: first published as /thx on 1 June Downloaded from (b) Fig. 3(a) and (b) Chest radiographs showing typical posterior mediastinal neural tumour. on 1 October 2018 by guest. Protected by copyright.
4 362 their tumour because of doubt about the diagnosis and the possibility of malignancy. It is also clear that as a tumour enlarges it will produce pressure effects on surrounding structures, which may necessitate its excision. The surgical approach is lateral thoracotomy and the tumour mass, covered by pleura, is easily identified. The lung is not usually adherent to it, and the mass can be mobilised without difficulty. Division of the nerve or nerves of origin will have to be carried out, and division of intercostal arteries may also be required. In the benign tumour there is an easily developed plane between tumour and rib, the latter usually appearing bare of periosteum and often deformed by pressure of the tumour. The objective of complete tumour removal was apparently attained in 80% of patients, and in no patient in this series was the resection accomplished without the division of one or more nerves. Up to four intercostal nerves have needed division, as have the sympathetic trunk and vagus from which tumours were originating. The reasons for failure to achieve complete resection and its effect on the patients are presented in more detail in Table 2. There were found to be three situations in which K. G. Davidson, P. R. Walbaum, and R. J. M. McCormack Fig. 4 Chest radiograph showing large neural tumour with associated rib and vertebral abnormalities. neural tumours were deemed to have been incompletely resected: DIRECT EXTENSION OF TUMOUR INTO INTERVERTEBRAL FORAMINA Eight patients were found to have finger-like processes extending from the main tumour mass into one or more intervertebral foramina. In all of these patients there was residual tumour visible within the foramina after excision of all tumour accessible at thoracotomy. It is of interest that in all eight patients the tumours were of nerve cell origin, seven being ganglioneuromas and one a neuroblastoma. There were four male and five female patients in this group, and their average age was 15. Only one of the patients presented with symptoms that were clearly related to the intervertebral extension of his tumour. This was a young man with symptoms and signs of spinal cord compression at midthoracic level, confirmed by myelography and then laminectomy. Four patients in this group underwent myelography and three of these subsequently came to laminectomy. Intervertebral tumour was found in two of the three patients (cases 1 and 4). In these two cases the tumour was excised, but the outcome was very
5 Intrathoracic neural tumours Table 2 Incomplete resection of neural tumours Case Age Sex Clinicalfeatures Pathology Outcome Follow-up (years) Direct vertebral extension 1 22 M Cord symptoms and signs GN Well F None GN Well F Dyspnoea GN Well F None NB Recurred 4 years Died F Cough and weight loss GN Well M None GN Well M Chest pain GN Well M None GN Well 8 Cervical extension 9 1 F Horner's syndrome NB Well 10 Multiple tumours F None NF Well F None NF Well 5 GN = ganglioneuroma; NB = neuroblastoma; NF = neurofibroma. different. Patient no. 1 is alive and well and in full-time work ten years after surgery. Patient no. 4 remained well for four years after her original thoraco.omy before symptoms of spinal cord compression developed. At laminectomy, dumb-belllike tumour masses extended through the intervertebral foramina on both sides and although complete resection was attempted it was thought that it had probably not been achieved. The pathological appearances were regarded as those of neuroblastoma. Despite the attempted radical surgery, followed by radiotherapy, the tumour advanced, and the patient died of widespread metastases eight years after the original incomplete resection of her mediastinal tumour. The other seven patients in this group are alive and well at follow-up periods ranging from two to 11 years. CERVICAL EXTENSION Only one example of cervical extension was found (Table 2)- a young girl with a Homer's syndrome and a large mass in the posterior mediastinum on chest radiography. At operation, soft tumour filled the upper third of the right hemithorax, and there were long extensions into the neck and brachial plexus. At the posterior end of the first intercostal space was an enlarged soft lymph node that was excised along with all intrathoracic tumour, but the extensions into the neck and brachial plexus were not removed. The pathological appearances were those of neuroblastoma, which was also present in the excised lymph node. The neck and right upper thorax were irradiated subsequently but chemotherapy was not used. Ten years after resection she remains well, though the right upper thorax is shrunken and the overlying skin telangiectatic. There is no clinical or radiological evidence of tumour recurrence. MULTIPLE TUMOURS 363 Of the two patients in this group (Table 2), one (case 10) was recognised to have had generalised neurofibromatosis in childhood and this had been confirmed by biopsy of a cutaneous lesion. Chest radiography, however, had shown the presence of a new mass in the posterior mediastinum and because of the possibility of malignancy it was thought that thoracotomy should be undertaken. Every visible nerve was studded with small tumours, and resection of only the main tumour mass was performed. Three months after thoracotomy she developed back pain and this was put down to a scoliosis, which had been present for several years. Myelography was carried out but did not show any evidence of intraspinal tumour, and it was thought that her symptoms were due to her scoliosis. A spinal fusion was carried out subsequently, and at this operation there was extensive paravertebral tumour, apparently separate from the mediastinal tumour. Eight years later she remains well, having no further treatment. The other patient in this group (case 11) was not known to have generalised neurofibromatosis and was found to have a posterior mediastinal opacity. At thoracotomy, however, a tumour mass extended from the pleural dome to the azygos vein and nodules were present down the entire course of the vagus nerve to the diaphragm. The upper pole of the main tumour mass extended into the neck along the expected course of the vagus nerve. A low right cervical incision showed tumour along the vagus nerve to the level of the hyoid bone, above which the nerve appeared normal. The vagus was divided at this level and the main tumour removed. The mediastinal tissues were also apparently infiltrated by tiny nodules, and several of these were taken for biopsy. All specimens were neurofibromas, and there were multiple minute
6 364 neurofibromas throughout all the tissues. This case is unique in our experience in that other than the described tumour there was no evidence of generalised neurofibromatosis. She remains well five years after operation with no evidence of generalised neurofibromatosis or recurrent or residual tumour. Results and complications In this series over 70% of tumours were benign nerve sheath tumours neurofibromas (45%) neurilemomas (13%), and a mixed pattern with both neurofibroma and neurilemoma elements in them (13%). The remainder were all nerve cell tumours; benign ganglioneuromas (24%) and neuroblastomas (5%) (Table 3). The overall incidence of malignancy was only 6%-well within the reported range of 3% (Blades, 1946) to 19% (Morrison, 1958). The results and complications related to the excision of these tumours are presented in Table 4. Table 3 Relative frequency of neural tumours Nerve sheath tumours Nerve cell tumours Neurofibroma 25 Ganglioneuroma 13 Neurilemoma 7 Neuroblastoma 3 Mixed pattern 7 Total 55 Table 4 Results and complications Deaths Recurrence after Related to neural complete resection 1 tumour I Horner's syndrome 5 Unrelated I Sympathectomy of arm 3 Incomplete resection Brachial plexus signs 2 Vertebral extension 8 Left recurrent nerve Cervical extension 1 paralysis I Multiple tumours 2 Of the 52 patients whose benign neural tumours were excised, none is known to have died as a consequence of tumour recurrence. One patient, however, had a benign neurilemoma excised from her right posterior mediastinum in 1957, and ten years later she presented with irresectable oat cell carcinoma of the bronchus. She died soon after presentation, and at necropsy there was no evidence of recurrence of her neural tumour. Eleven patients with mediastinal neural tumours, which it proved impossible to resect completely, have already been described. One of these, case 4, died as a consequence of recurrence of her neuroblastoma. The two patients with generalised neurofibromatosis are unchanged. None of the other eight K. G. Davidson, P. R. Walbaum, and R. J. M. McCormack patients is known to have tumour recurrence. One of the three patients with lateral chest wall neurofibromas, an asymptomatic man of 28, whose tumour was apparently completely resected, developed multiple opacities in the same area six years after his original operation. Re-exploration showed two hard tumours adherent to the angles of the 4th and 5th ribs and a third lump adherent to or possibly even within the apical segment of the left lower lobe. All tumour tissue, along with 8-cm lengths of the 4th and 5th ribs, the intercostal muscles, and a portion of the apical segment of the left lower lobe, were resected. The pathologist reported that all three tumour masses were quite different from the original benign neurofibroma and now showed undoubted neurosarcoma. After operation the patient developed an empyema that needed further surgical treatment but he remains well at present with no evidence of tumour recurrence, though the follow-up period is only one year. Two of the three patients with neuroblastomas have already been presented in the group of incomplete resections (cases 4 and 9). The third such tumour was in an 18-month-old boy who was found to have an abnormal chest radiograph during the investigation of diarrhoea, later shown to be due to salmonella infection. At thoracotomy, a tumour filled one third of the left hemithorax, and there was a posterior mediastinal pedicle extending from the 4th to the 9th intercostal bundles. Contributions to the pedicle came from four of these intercostal bundles, all of which required division, and resection appeared to be complete. The pathological features were those of neuroblastoma, in parts quite well differentiated. Four years later, without further treatment, he was well, with no clinical or radiological evidence of recurrence. There were few complications of the surgical procedure itself, and these were mainly the predictable ones produced by division of the nerve, or nerves from which the tumours originated. Thus, excision of five tumours from the superior mediastinum at the thoracic inlet (Fig. 5) produced Horner's syndrome. Three of these five were noted to have had a sympathectomy of the homolateral arm, and two of the same group also suffered damage to the anterior primary rami of the first and second thoracic nerves. One patient was found at operation to have a large left superior mediastinal tumour originating from the vagus nerve (Figs. 6a and b) and, inevitably, had a left recurrent nerve palsy after excision of the tumour. The lesion was reported to be a benign neurilemoma. No other major complications have been recorded in this series.
7 Intrathoracic neural tumours Discussion Analysis of this series of intrathoracic neural tumours illustrates some of the difficulties of pathological diagnosis and surgical management in this uncommon group of tumours. Because of doubt about the diagnosis, increasing size of tumour, and the possibility of malignancy, early surgical exploration and resection is a universally accepted policy. Most patients clearly present little problem if this objective is achieved-the asymptomatic patient, usually a young adult with a typical posterior mediastinal opacity, will have this tumour completely excised and its benign nature confirmed by the pathologist. This series suggests that in about 20% of patients complete resection at thoracotomy will not be possible. If there are dumb-bell-like extensions passing into intervertebral foramina, then the lesion is most likely to be a ganglioneuroma originating from the sympathetic trunk and the correct management is excision of all accessible intrathoracic tumour. This can be followed four to eight weeks later by myelography to assess the extent of the intervertebral tumour. Exploration for intraspinal tumour by laminectomy would then be undertaken only if the myelogram showed tumour at the relevant site. If multiple tumours are present they are likely 365 Fig. 5 Chest radiograph showing large posterior neural tumour occupying much of right upper hemithorax. to be neurofibromas and may be manifestations of von Recklinghausen's disease. In this situation it is recommended that the main tumour mass should be excised, but clearly there is no point in attempting to excise multiple neurofibromas, which may well be minute and may affect virtually every nerve within the chest. There will always be a risk that this type of patient may eventually develop a neurosarcoma, but there is no known way of preventing this. In anteriorly situated neural tumours there is a higher incidence of malignancy (Efskind and Liavaag, 1950), but such tumours are very rare (Kent et al., 1944). The difficulties of the pathologist are perhaps greater than those of the surgeon, but the minutiae of pathological interpretation are beyond the scope of this paper and have been fully discussed elsewhere (Russell and Rubinstein, 1969). Nerve sheath tumours of mixed pattern are common, and the appearances may vary from section to section of the same tumour. To the surgeon, the distinction between neurofibroma and neurilemoma is of relatively little importance, although the latter is usually more encapsulated. Histologically, the appearance of the malignant neurosarcoma is usually quite distinctive and does not present a major diagnostic problem to the pathologist. The area of greatest concern in this field
8 (ul) (I)) Fig. 6(a) and (b) Chest radiographs showing ganglioneuroma originating from left vagus nerve.
9 Intrathoracic neural tumours is in the interpretation of the nerve cell tumour, with benign ganglioneuroma at one end of the spectrum and undifferentiated neuroblastoma at the other. Between these two extremes, all varieties of differentiation are found, different degrees being seen in different parts of the same tumour. Prediction of tumour behaviour is particularly difficult in the young child where a certain lack of differentiation may be seen in a tumour that otherwise behaves in a wholly benign manner. The policy of this unit has been that if a neural tumour appears to have been completely excised and is reported as a benign ganglioneuroma no further treatment is offered, and the patient is merely kept under observation for a prolonged period. If, however, a ganglioneuroma has been incompletely resected it is more difficult to be specific about the appropriate managementmyelography should probably be carried out, but laminectomy only if intraspinal tumour is suspected radiologically. Nor is there universal agreement as to management when the excised tumour is reported as a neuroblastoma. When excision appears complete, it would seem reasonable to proceed with close observation, particularly if the patient is a young child, but also to consider either radiotherapy or chemotherapy at that stage. If resection were incomplete, or possibly incomplete, further treatment in the form of radiotherapy or chemotherapy or both is instituted. Following this policy, two of the three patients in this series who had neuroblastomas excised remain well four years and ten years after resection. Both of these were young children, and one was irradiated because of incomplete resection. The third patient with neuroblastoma died eight years after resection despite irradiation, with extensive recurrence of her tumour. The only other patient known to have recurrent tumour had a benign lateral chest wall neurofibroma excised, and this recurred six years later as a neurosarcoma-it was again resected and has not recurred to date. Several authors have pointed out recently that in patients who present with typical posterior mediastinal neural tumours the likelihood of malignancy is low, and a reasonable course of action would be merely to continue with regular observation and perhaps avoid a thoracotomy. We have found, however, that it has not been possible to distinguish clinically or radiologically between benign and malignant tumours. With improvements in radiotherapy and chemotherapy, this distinction is becoming increasingly important. Doubt about the diagnosis and increase in size of the tumour mass remain indications for surgical excision. There has been no mortality from the surgical procedure itself, and the morbidity has been very small-almost entirely complications directly related to the excision of affected nerves. In addition, all three patients with neuroblastomas underwent radical surgery followed by radiotherapy, and in only one of these has the tumour recurred. Although primary intrathoracic neuroblastomas carry a less ominous prognosis than similar intra-abdominal tumours, it has been suggested (Koop et al., 1955) that wide excision, even if incomplete, may lead to increased survival. For these reasons, we consider that the most appropriate management policy for patients with suspected intrathoracic neural tumours remains surgical excision. References 367 Blades, B. (1946). Mediastinal tumors; report of cases treated at Army thoracic surgery centres in the United States. Annals of Surgery, 123, Cruickshank, D. B. (1957). Primary intrathoracic neurogenic tumours. Journal of the Faculty of Radiologists, 8, Curreri, A. R., and Gale, J. W. (1949). Mediastinal tumors. Archives of Surgery, 58, Efskind, L., and Liavaag, K. (1950). Intrathoracic neurogenic tumors. Journal of Thoracic Surgery, 20, Kent, E. M., Blades, B., Valle, A. R., and Graham, E. A. (1944). Intrathoracic neurogenic tumors. Journal of Thoracic Surgery, 13, Koop, C. E., Kiesewetter, W. B., and Horn, R. C. (1955). Neuroblastoma in childhood. Surgery, 38, Le Roux, B. T. (1960). Primary intrathoracic neural tumours. Thorax, 15, Morrison, I. M. (1958). Tumours and cysts of the mediastinum. Thorax, 13, Oosterwijk, W. M., and Swierenga, J. (1968). Neurogenic tumours with an intrathoracic localization. Thorax, 23, Parish, C. (1957). The clinical features of intrathoracic neurogenic tumours. Journal of the Faculty of Radiologists, 8, Russell, D. H., and Rubinstein, L. (1969). Pathology of Tumours of the Nervous System. 2nd edition. Williams and Wilkins, Baltimore. Requests for reprints to: Dr. K. G. Davidson, Thoracic Surgery Department, City Hospital, Edinburgh.
Primary mediastinal tumours
 Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
Tumors of the posterior mediastinum, located in the paravertebral
 Technique of Thoracoscopic Resection of Posterior Mediastinal Tumors Michael F. Reed, MD Tumors of the posterior mediastinum, located in the paravertebral sulcus, account for about 25% of all mediastinal
Technique of Thoracoscopic Resection of Posterior Mediastinal Tumors Michael F. Reed, MD Tumors of the posterior mediastinum, located in the paravertebral sulcus, account for about 25% of all mediastinal
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
Tumors of the thoracic apex, even when benign,
 Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Anterior Cervical Transsternal Approach for Resection of Benign Tumors at the Thoracic Inlet George Ladas, MD, Peter H. Rhys-Evans, FRCS, and Peter Goldstraw, FRCS Department of Thoracic Surgery, Royal
Karoline Nowillo, MD. February 1, 2008
 Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Primary chondrosarcoma of lung
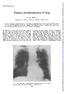 Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
Thorax,(1970), 25, 366. Primary chondrosarcoma of lung G. M. REES Department of Surgery, Brompton Hospital, Lontdonl, S.W.3 A case of primary chondrosarcoma of the lung is described in a 64-year-old man.
Mediastinal Tumors: Imaging
 Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Tumors. Chapter 3. Primary neurogenic tumors. Tumors 27
 Tumors 27 Chapter 3 Tumors MR imaging of the brachial plexus is frequently requested to rule out a tumor in or near the brachial plexus, or to evaluate the extension of a known tumor in the region of the
Tumors 27 Chapter 3 Tumors MR imaging of the brachial plexus is frequently requested to rule out a tumor in or near the brachial plexus, or to evaluate the extension of a known tumor in the region of the
PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE
 Thlorax (1950), 5, 369. PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE BY Fronm the Regional Thoracic Surgery Centre, Shotley Bridge Hospital, Newcastle-upon-Tyne (RECEIVED FOR PUBLICATION
Thlorax (1950), 5, 369. PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE BY Fronm the Regional Thoracic Surgery Centre, Shotley Bridge Hospital, Newcastle-upon-Tyne (RECEIVED FOR PUBLICATION
Paraspinal Venous Malformation Joseph Junewick, MD FACR
 Paraspinal Venous Malformation Joseph Junewick, MD FACR 06/04/2010 History 2 year old with history of fall. Rule out spinal injury. Diagnosis Paraspinal Venous Malformation Additional Clinical CT of the
Paraspinal Venous Malformation Joseph Junewick, MD FACR 06/04/2010 History 2 year old with history of fall. Rule out spinal injury. Diagnosis Paraspinal Venous Malformation Additional Clinical CT of the
CURRENT REVIEW. Tumors
 CURRENT REVIEW Primary Malignant of the Mediastinum Tumors David M. Conkle, M.D., and R. Benton Adkins, Jr., M.D. ABSTRACT Forty-three patients with primary malignant tumors of the rnediastinum are reviewed.
CURRENT REVIEW Primary Malignant of the Mediastinum Tumors David M. Conkle, M.D., and R. Benton Adkins, Jr., M.D. ABSTRACT Forty-three patients with primary malignant tumors of the rnediastinum are reviewed.
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Thoracoscopic surgical resection of thoracic neurogenic tumors
 Neurosurg Focus 7 (5):Article 1, 1999 Thoracoscopic surgical resection of thoracic neurogenic tumors Patrick P. Han, M.D., and Curtis A. Dickman, M.D. Division of Neurological Surgery, Barrow Neurological
Neurosurg Focus 7 (5):Article 1, 1999 Thoracoscopic surgical resection of thoracic neurogenic tumors Patrick P. Han, M.D., and Curtis A. Dickman, M.D. Division of Neurological Surgery, Barrow Neurological
Sectional Anatomy Quiz - III
 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
A Nervous Breakdown: Multimodality Imaging of Thoracic Neurogenic Tumors
 A Nervous Breakdown: Multimodality Imaging of Thoracic Neurogenic Tumors John P. Lichtenberger III, MD, Maj, USAF, MC Assistant Professor, Dept. or Radiology Uniformed Services University of the Health
A Nervous Breakdown: Multimodality Imaging of Thoracic Neurogenic Tumors John P. Lichtenberger III, MD, Maj, USAF, MC Assistant Professor, Dept. or Radiology Uniformed Services University of the Health
THE DESCENDING THORACIC AORTA
 Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Intercostal Arteries and Veins Each intercostal space contains a large single posterior intercostal artery and two small anterior intercostal arteries. The anterior intercostal arteries of the lower spaces
Primary Tumors of Ribs
 Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
Primary Tumors of Ribs Frank E. Schmidt, M.D., and Max J. Trummer, Capt, MC, USN ABSTRACT An analysis of 50 consecutive patients with primary rib tumors operated on at the U.S. Naval Hospital, San Diego,
came from a carcinoma and in 12 from a sarcoma. Ninety lesions were intrapulmonary and the as the chest wall and pleura. Details of the primary
 Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
Thorax 1982;37:366-370 Thoracic metastases MARY P SHEPHERD From the Thoracic Surgical Unit, Harefield Hospital, Harefield ABSTRACI One hundred and four patients are reviewed who were found to have thoracic
PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA
 Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Thor-ax (1954), 9, 304. PULMONARY INFARCTS ASSOCIATED WITH BRONCHOGENIC CARCINOMA W. J. HANBURY, R. J. R. CURETON, AND G. SIMON From St. Bartholomew's Hospital, London BY (RECEIVED FOR PUBLICATION JUNE
Radiation-induced Brachial Plexopathy: MR Imaging
 Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Lateral thoracic meningocele
 Lateral thoracic meningocele A. E. BOOTH J. Neurol. Neurosurg. Psychiat., 1969, 32, 111-115 From the Department of Neurosurgery, The Middlesex Hospital, London A case is reported of a patient with a lateral
Lateral thoracic meningocele A. E. BOOTH J. Neurol. Neurosurg. Psychiat., 1969, 32, 111-115 From the Department of Neurosurgery, The Middlesex Hospital, London A case is reported of a patient with a lateral
Intrathoracic vagus nerve tumours
 Intrathoracic vagus nerve tumours BASIL STRICKLAND and M. K. WOLVERSON Department of Diagnostic Radiology, Brompton Hospital, London SW3 Thorax (1974), 29, 215. Strickland, B. and Wolverson, M. K. (1974).
Intrathoracic vagus nerve tumours BASIL STRICKLAND and M. K. WOLVERSON Department of Diagnostic Radiology, Brompton Hospital, London SW3 Thorax (1974), 29, 215. Strickland, B. and Wolverson, M. K. (1974).
FDG PET/CT in Lung Cancer Read with the experts. Homer A. Macapinlac, M.D.
 FDG PET/CT in Lung Cancer Read with the experts Homer A. Macapinlac, M.D. Patient with suspected lung cancer presents with left sided chest pain T3 What is the T stage of this patient? A) T2a B) T2b C)
FDG PET/CT in Lung Cancer Read with the experts Homer A. Macapinlac, M.D. Patient with suspected lung cancer presents with left sided chest pain T3 What is the T stage of this patient? A) T2a B) T2b C)
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
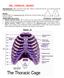 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
AJCC-NCRA Education Needs Assessment Results
 AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
Region: 11. Clinic6patholo cal Studies
 Tumors of the Thvmus and ThVIIliC Region: 11. Clinic6patholo cal Studies on Hodgkin s Disease of Re Thymus N. P. Bergh, M.D., P. Gatzinsky, M.D., S. Larsson, M.D., P. Lundin, M.D., and B. Ridell, M.D.
Tumors of the Thvmus and ThVIIliC Region: 11. Clinic6patholo cal Studies on Hodgkin s Disease of Re Thymus N. P. Bergh, M.D., P. Gatzinsky, M.D., S. Larsson, M.D., P. Lundin, M.D., and B. Ridell, M.D.
Tumour size as a prognostic factor after resection of lung carcinoma
 Tumour size as a prognostic factor after resection of lung carcinoma A. S. SOORAE AND R. ABBEY SMITH Thorax, 1977, 32, 19-25 From the Cardio-Thoracic Unit, Walsgrave Hospital, Clifford Bridge Road, Coventry
Tumour size as a prognostic factor after resection of lung carcinoma A. S. SOORAE AND R. ABBEY SMITH Thorax, 1977, 32, 19-25 From the Cardio-Thoracic Unit, Walsgrave Hospital, Clifford Bridge Road, Coventry
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
An Update: Lung Cancer
 An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
The Value of Adjuvant Radiotherapy in Pulmonary and Chest Wall Resection for Bronchogenic Carcinoma
 The Value of Adjuvant Radiotherapy in Pulmonary and Chest Wall Resection for Bronchogenic Carcinoma G. A. Patterson, M.D., R. Ilves, M.D., R. J. Ginsberg, M.D., J. D. Cooper, M.D., T. R. J. Todd, M.D.,
The Value of Adjuvant Radiotherapy in Pulmonary and Chest Wall Resection for Bronchogenic Carcinoma G. A. Patterson, M.D., R. Ilves, M.D., R. J. Ginsberg, M.D., J. D. Cooper, M.D., T. R. J. Todd, M.D.,
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Imaging Of Cystic Paravertebral Masses:
 Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA
 89 Lymphology 28 (1995) 89-94 Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA ABSTRACT The anatomy of the posterior intercostal lymphatics and lymph
89 Lymphology 28 (1995) 89-94 Division of Diagnostic Imaging, The University of Texas M.D. Anderson Cancer Center, Houston, Texas, USA ABSTRACT The anatomy of the posterior intercostal lymphatics and lymph
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
Wilms Tumor and Neuroblastoma
 Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Wilms Tumor and Neuroblastoma Wilm s Tumor AKA: Nephroblastoma the most common intra-abdominal cancer in children. peak incidence is 2 to 3 years of age Biology somatic mutations restricted to tumor tissue
Primary sarcoma of the lung
 Thorax (1975), 30, 516. Primary sarcoma of the lung E. W. J. CAMERON Thoracic Surgical Unit, The Royal Infirmary, Edinburgh Cameron, E. W. J. (1975). Thorax, 30, 516-520. Primary sarcoma of the lung. Primary
Thorax (1975), 30, 516. Primary sarcoma of the lung E. W. J. CAMERON Thoracic Surgical Unit, The Royal Infirmary, Edinburgh Cameron, E. W. J. (1975). Thorax, 30, 516-520. Primary sarcoma of the lung. Primary
Lobectomy with sleeve resection in the
 Thorax (970), 25, 60. Lobectomy with sleeve resection in the treatment of bronchial tumours G. M. REES and M. PANETH Brompton Hospital, London, S.W3 Fortysix patients with malignant tumours involving the
Thorax (970), 25, 60. Lobectomy with sleeve resection in the treatment of bronchial tumours G. M. REES and M. PANETH Brompton Hospital, London, S.W3 Fortysix patients with malignant tumours involving the
Supraphrenic herniation of perinephric fat
 Thorax (1965), 20, 376. Supraphrenic herniation of perinephric fat B. T. LE ROUX From the Thoracic Surgical Unit, The Royal Infirmary, Edinburgh The diagnosis attached pre-operatively to wellcircumscribed
Thorax (1965), 20, 376. Supraphrenic herniation of perinephric fat B. T. LE ROUX From the Thoracic Surgical Unit, The Royal Infirmary, Edinburgh The diagnosis attached pre-operatively to wellcircumscribed
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
In the Last Three Lectures We Already Discussed the Importance of the Thoracic Cage.
 -This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
-This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
Small Cell Lung Cancer
 Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
Small Cell Lung Cancer Small cell lung cancer (SCLC) affects 15% of all lung cancer patients. SCLC is the most aggressive type of lung cancer. It may be treated with chemotherapy and radiation. SCLC has
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
and Nicholas T. Zervas, M.D.
 Combined Approach to "Dumbbell" Intrathoracic and Intraspinal Neurogenic Tumors Hermes C. Grillo, M.D., Robert G. Ojemann, M.D., J. Gordon Scannell, M.D., and Nicholas T. Zervas, M.D. ABSTRACT The unexpected
Combined Approach to "Dumbbell" Intrathoracic and Intraspinal Neurogenic Tumors Hermes C. Grillo, M.D., Robert G. Ojemann, M.D., J. Gordon Scannell, M.D., and Nicholas T. Zervas, M.D. ABSTRACT The unexpected
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Open surgery for posterior mediastinal neurogenic tumors
 Review Article Page 1 of 5 Open surgery for posterior mediastinal neurogenic tumors Erkan Kaba 1, Mazen Rasmi Alomari 2, Alper Toker 2 1 Department of Thoracic Surgery, Istanbul Bilim University Medical
Review Article Page 1 of 5 Open surgery for posterior mediastinal neurogenic tumors Erkan Kaba 1, Mazen Rasmi Alomari 2, Alper Toker 2 1 Department of Thoracic Surgery, Istanbul Bilim University Medical
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Radiological Anatomy of Thorax. Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem
 Radiological Anatomy of Thorax Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem Indications for Chest x - A chest x-ray may be used to diagnose and plan treatment for various conditions, including: Diseases/Fractures
Radiological Anatomy of Thorax Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem Indications for Chest x - A chest x-ray may be used to diagnose and plan treatment for various conditions, including: Diseases/Fractures
Dana Alrafaiah. - Moayyad Al-Shafei. -Mohammad H. Al-Mohtaseb. 1 P a g e
 - 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
- 6 - Dana Alrafaiah - Moayyad Al-Shafei -Mohammad H. Al-Mohtaseb 1 P a g e Quick recap: Both lungs have an apex, base, mediastinal and costal surfaces, anterior and posterior borders. The right lung,
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Understanding surgery
 What does surgery for lung cancer involve? Surgery for lung cancer involves an operation, which aims to remove all the cancer from the lung. Who will carry out my operation? In the UK, we have cardio-thoracic
What does surgery for lung cancer involve? Surgery for lung cancer involves an operation, which aims to remove all the cancer from the lung. Who will carry out my operation? In the UK, we have cardio-thoracic
Lung Cancer Resection
 Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
PDF created with pdffactory Pro trial version
 Neuroblastoma Tumor derived from neural crest cell that form the sympathetic ganglia&adrenal medulla. Causes *unknown. *familial neuroblastoma has been reported but is rare. * The incidence is 1:100,000
Neuroblastoma Tumor derived from neural crest cell that form the sympathetic ganglia&adrenal medulla. Causes *unknown. *familial neuroblastoma has been reported but is rare. * The incidence is 1:100,000
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Intercostal Muscles LO4
 Intercostal Muscles LO4 4 List the structures, from superficial to deep, in an intercostal space. Describe their relationships to each other, to the associated neurovascular bundle and to the pleural cavity.
Intercostal Muscles LO4 4 List the structures, from superficial to deep, in an intercostal space. Describe their relationships to each other, to the associated neurovascular bundle and to the pleural cavity.
PLEURAL TUM:OURS. required thoracoscopy, were referred to this unit. During the period when 3,000 patients with
 Thorax (1962), 17, 111. PLEURAL TUM:OURS BY B. T. LE ROUX From the Department of Clinical Surgery, University of Edinburgh The commonest pleural tumour is a metastasis, and the commonest source of such
Thorax (1962), 17, 111. PLEURAL TUM:OURS BY B. T. LE ROUX From the Department of Clinical Surgery, University of Edinburgh The commonest pleural tumour is a metastasis, and the commonest source of such
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Thyroid INTRODUCTION ANATOMY SUMMARY OF CHANGES
 AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
AJC 7/14/06 1:19 PM Page 67 Thyroid C73.9 Thyroid gland SUMMARY OF CHANGES Tumor staging (T) has been revised and the categories redefined. T4 is now divided into T4a and T4b. Nodal staging (N) has been
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Hodgkin s Disease of the Mediastinum
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 3 NUMBER 4 APRIL 1967 Hodgkin s Disease of the Mediastinum William A. Burke,
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 3 NUMBER 4 APRIL 1967 Hodgkin s Disease of the Mediastinum William A. Burke,
March The patients, two men and nine. an average of 54 years. In 10 of these patients. the cervical trachea was affected.
 Thorax, 1978, 33, 378-386 Resection of thyroid carcinoma infiltrating the trachea T. ISHIHARA, K. KIKUCHI, T. IKEDA, H. INOUE, S. FUKAI, K. ITO', AND T. MIMURA' From the Department of Surgery, School of
Thorax, 1978, 33, 378-386 Resection of thyroid carcinoma infiltrating the trachea T. ISHIHARA, K. KIKUCHI, T. IKEDA, H. INOUE, S. FUKAI, K. ITO', AND T. MIMURA' From the Department of Surgery, School of
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Pulmonary Neoplasms & Chest Disorders Ahmed Mahmoud
 Pulmonary Neoplasms & Chest Disorders Ahmed Mahmoud Lung Ca ;Pathological types Adenocarcinoma More common in females Peripheral location Spread mainly by blood(brain..) Incidence is increasing (the most
Pulmonary Neoplasms & Chest Disorders Ahmed Mahmoud Lung Ca ;Pathological types Adenocarcinoma More common in females Peripheral location Spread mainly by blood(brain..) Incidence is increasing (the most
Significance of Metastatic Disease
 Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
ANATOMY OF THE PLEURA. Dr Oluwadiya KS
 ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
ANATOMY OF THE PLEURA Dr Oluwadiya KS www.oluwadiya.sitesled.com Introduction The thoracic cavity is divided mainly into: Right pleural cavity Mediastinum Left Pleural cavity Pleural cavity The pleural
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
International Journal of Case Reports (ISSN: ) Totally Cystic Schwannoma in the posterior mediastinum on right side- A rare presentation
 Case Report IJCR (2018) 2:21 International Journal of Case Reports (ISSN:2572-8776) Totally Cystic Schwannoma in the posterior mediastinum on right side- A rare presentation Amarjit singh, K S Sidhu, Shivaji
Case Report IJCR (2018) 2:21 International Journal of Case Reports (ISSN:2572-8776) Totally Cystic Schwannoma in the posterior mediastinum on right side- A rare presentation Amarjit singh, K S Sidhu, Shivaji
Mediastinal cyst containing mural pancreatic tissue
 Thorax, 1977, 32, 512-516 Mediastinal cyst containing mural pancreatic tissue M. J. T. CARR', A. K. DEIRANIYA', AND P. A. JUDD2 From the Cardiothoracic Unit', and Department of Pathology2, Queen Elizabeth
Thorax, 1977, 32, 512-516 Mediastinal cyst containing mural pancreatic tissue M. J. T. CARR', A. K. DEIRANIYA', AND P. A. JUDD2 From the Cardiothoracic Unit', and Department of Pathology2, Queen Elizabeth
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
THORACIC CHORDOMA. G. G. CROWE AND P. B. LL. MULDOON From City General Hospital, Stoke-on-Trent
 Thorax (1951), 6, 403. THORACIC CHORDOMA BY G. G. CROWE AND P. B. LL. MULDOON From City General Hospital, Stoke-on-Trent (RECEIVED FOR PUBLICATION AUGUST 22, 1951) Remnants of the notochord sometimes become
Thorax (1951), 6, 403. THORACIC CHORDOMA BY G. G. CROWE AND P. B. LL. MULDOON From City General Hospital, Stoke-on-Trent (RECEIVED FOR PUBLICATION AUGUST 22, 1951) Remnants of the notochord sometimes become
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
thoracic cage inlet and outlet landmarks of the anterior chest wall muscles of the thoracic wall sternum joints ribs intercostal spaces diaphragm
 Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
Thoracic Wall Lecture Objectives Describe the shape and outline of the thoracic cage including inlet and outlet. Describe the anatomical landmarks of the anterior chest wall. List various structures making
HISTORY SURGERY FOR TUMORS WITH INVASION OF THE APEX 15/11/2018
 30 EACTS Annual Meeting Barcelona, Spain 1-5 October 2016 SURGERY FOR TUMORS WITH INVASION OF THE APEX lung cancer of the apex of the chest involving any structure of the apical chest wall irrespective
30 EACTS Annual Meeting Barcelona, Spain 1-5 October 2016 SURGERY FOR TUMORS WITH INVASION OF THE APEX lung cancer of the apex of the chest involving any structure of the apical chest wall irrespective
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Anatomy of the Lungs. Dr. Gondo Gozali Department of anatomy
 Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Lung Cancer Case Study
 Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD
 PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD Topics 1. Cervical lymphadenopathy 2. Lymphatic malformation 3. Thyroglossal duct cysts 4. Branchial cleft cysts 5. Thyroid masses CASE 1 Case 1 A 2
PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD Topics 1. Cervical lymphadenopathy 2. Lymphatic malformation 3. Thyroglossal duct cysts 4. Branchial cleft cysts 5. Thyroid masses CASE 1 Case 1 A 2
Giant invasive spinal schwannomas: definition and surgical management
 J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
