Trigeminal neuralgia is a debilitating facial pain disorder,
|
|
|
- Coral Mabel Little
- 5 years ago
- Views:
Transcription
1 CLINICAL ARTICLE Tentorial sling for microvascular decompression in patients with trigeminal neuralgia: a description of operative technique and clinical outcomes Jeffrey A. Steinberg, MD, Jayson Sack, MD, Bayard Wilson, MD, MAS, David Weingarten, MD, Bob Carter, MD, PhD, Alexander Khalessi, MD, MS, Sharona Ben-Haim, MD, and John Alksne, MD Department of Neurosurgery, University of California, San Diego, California OBJECTIVE Trigeminal neuralgia is a debilitating pain disorder most often caused by arterial compression of the trigeminal nerve, although there are other etiologies. Microvascular decompression (MVD) remains the most definitive treatment for this disorder, with cure rates reported between 60% and 80%. Traditional MVD techniques involve a retrosigmoid craniotomy with placement of an inert foreign material, such as Teflon, between the nerve and compressive vessel. Recurrence of trigeminal neuralgia after MVD has been associated with vessel migration, adhesion formation, and arterial pulsation against the Teflon abutting the nerve. Additionally, foreign materials such as Teflon have been reported to trigger inflammatory responses, resulting in recurrence of trigeminal pain. An alternative method for decompression involves the use of a sling to transpose the compressive vessel away from the nerve. Results of various sling techniques as a decompressive strategy are limited to small series and case reports. In this study, the authors present their experience utilizing a tentorial sling for MVD in patients with trigeminal neuralgia. METHODS Institutional review board approval was obtained in order to contact patients who underwent MVD for trigeminal neuralgia via the tentorial sling technique. Clinical outcomes were assessed utilizing the Barrow Neurological Institute (BNI) pain intensity score immediately after surgery and at the time of the study. RESULTS The tentorial sling technique was performed in 45 patients undergoing MVD for trigeminal neuralgia. In 41 of these patients, this procedure was their first decompressive surgery. Immediate postoperative relief of pain (BNI score I) was achieved in 80% of patients undergoing their first decompressive procedure. At last follow-up, 73% of these patients remained pain free. Three patients experienced recurrent trigeminal pain, with surgical exploration demonstrating an intact tentorial sling. The complication rate was 6.6%. CONCLUSIONS Transposition techniques for MVD have been described previously in small series and case reports. This study represents the largest experience in which the utilization of a tentorial sling for MVD in patients with trigeminal neuralgia is described. The technique represents a novel method for decompression of the trigeminal nerve by transposition of the offending vessel without the use of foreign material. Although the authors preliminary results parallel the historical cure rate, further outcome data are required to assess long-term durability of this method. KEYWORDS tentorial sling; microvascular decompression; trigeminal neuralgia; MVD; Teflon granuloma; surgical technique; pain Trigeminal neuralgia is a debilitating facial pain disorder, with an annual incidence of 4 5 per 100,000 and a slightly higher occurrence in females. 6,16 The most commonly accepted etiology for classic trigeminal neuralgia is vascular compression at or near the root entry zone. Microvascular decompression (MVD) is considered the most definitive and durable treatment for trigeminal neuralgia, 6 as patients who undergo MVD can have complete resolution of pain immediately after surgery. Traditional decompressive methods involve placing foreign material between the nerve and the compressive blood vessel to maintain distance between the 2 structures. In this method, the foreign material acts as a cushion or buttress interposed between the 2 structures. Teflon is most ABBREVIATIONS BNI = Barrow Neurological Institute; MVD = microvascular decompression; SCA = superior cerebellar artery. SUBMITTED April 22, ACCEPTED October 6, INCLUDE WHEN CITING Published online April 20, 2018; DOI: / JNS AANS 2018, except where prohibited by US copyright law 1
2 J. A. Steinberg et al. often used, but other materials such as cotton, small pieces of muscle, Gelfoam (Pfizer), Ivalon sponges (Fabco), and others have also been used. 4,10,11 Long-term cure rates for trigeminal neuralgia after MVD range from 60% to 80%. 2 4,8 In a large study by Barker et al., 1185 patients underwent MVD for trigeminal neuralgia; 75% of these patients were pain free at 1 year, and 64% were pain free 10 years after surgery. 1 Historically, recurrent pain has been attributed to a number of factors: vessel migration back toward the nerve, adhesion formation, foreign material impingement against the nerve, blood vessel/teflon complex pulsations abutting the nerve, and general failure of the operative technique. 4,9 Teflon is the most used material for decompression of the trigeminal nerve because it is considered an inert substance. 12,13,15 However, numerous reports of inflammatory reactions related to Teflon use have been described within the neurosurgical literature, as well as within other surgical subspecialties. 2,4,5,9,10,15 It has been proposed that Teflon granuloma formation is the cause of delayed recurrence of facial pain after initial surgical success. 2,4,5,9,10,15 Other foreign materials used in MVD procedures have also been found to cause inflammatory reactions. 13 Alternative decompressive techniques for trigeminal neuralgia are described in the literature, including the use of a slinging method to reposition the compressive vessel away from the trigeminal nerve. The first report of this method was described by Fukushima in 1982, in which a Dacron sling technique was used. 7 Other case reports and small case series describe similar methods, with various sling materials used to transpose the offending vessel away from the nerve. These studies have predominantly used foreign materials for sling creation, including Dacron, suture, Gore-Tex tape, aneurysm clips, and gelatin sponge. 9,13 However, Melvill and Baxter described the use of an autologous dural sling created from the underside of the tentorium. 11 This method was used in 7 patients with a follow-up period ranging from 1 to 8 months. Although the series is small and with short follow-up, the authors reported success, with 6 patients achieving complete cure of facial pain and 1 patient with significant improvement in facial pain. Here, we report the largest series of patients who underwent MVD for trigeminal neuralgia in which a tentorial-based sling was used for vessel transposition. Methods Institutional review board approval was obtained from the University of California, San Diego, to review charts of patients who underwent MVD for trigeminal neuralgia by the senior author during the period of All patients were older than 18 years and treated at University of California, San Diego, Medical Center. Prior to surgery, patients were evaluated in the clinic and gave their consent to undergo MVD for trigeminal neuralgia. We reviewed the operative reports to assess whether the tentorial sling method was used for MVD. A total of 45 patients underwent MVD with the use of a tentorial sling during a 2.5-year period starting in late 2013 and ending in During this time period, any patient undergoing MVD for trigeminal neuralgia and with a compressive artery amenable to tentorial sling transposition underwent this procedure. Patients who underwent MVD for trigeminal neuralgia with use of the tentorial sling were contacted to complete a clinical outcome questionnaire. Study outcomes included postoperative facial pain status, current medication usage for facial pain, subsequent interventions for facial pain, and complications. The Barrow Neurological Institute (BNI) pain intensity score, described by Rogers et al., 14 was used to assess facial pain status (Table 1). Operative Technique A standard retrosigmoid approach is performed. The junction of the tentorium and petrous bone is identified, and the petrosal veins are cauterized, as is standard practice in both our traditional and tentorial sling MVD procedures. Once the subjacent arachnoid is dissected off of the trigeminal nerve, the region is explored for vascular compression with specific focus on the nerve root entry zone. As part of the inclusion criteria for this study, a compressive artery must have been present and in a location amenable to slinging. Once the offending vessel is identified, it is dissected free from the trigeminal nerve and mobilized away from the nerve. Attention is then turned toward creation of the tentorial sling (Fig. 1). A view of the underside of the tentorium in relation to the trigeminal nerve and compressive vessel is shown in Fig. 1A. Using a 15 blade, a 3- to 4-mm split-thickness incision is made along the underside of the superficial/lateral aspect of the tentorium (Fig. 1B). Blunt dissection continues between the 2 layers of the tentorium (Fig. 1C). A second incision is then carried out perpendicular to the initial incision, directed toward the medial edge of the tentorium. This perpendicular incision is created using microscissors, cutting within the split-thickness dural plane (Fig. 1D and E). Care is taken to avoid injury to the trochlear nerve while making the distal cut in this location (Fig. 1D and E). The tentorium is often highly vascular, and hemostasis can be accomplished with use of Surgicel and limited bipolar cauterization, as excessive cautery will shrink the tentorial sling. A third cut, parallel to the second, is completed, creating a 3- to 4-mm split-thickness strip of dura with a pedicle at the medial and deep aspect of the inferior tentorium (Fig. 1F). We found the optimal sling length to be cm. The dural sling is then wrapped around the compressive vessel, TABLE 1. Barrow Neurological Institute (BNI) pain intensity score Score I II III IV V No trigeminal pain, no medication Occasional pain, not requiring medication Some pain, adequately controlled with medication Some pain, not adequately controlled with medication Severe pain/no pain relief Reprinted from Int J Radiat Oncol Biol Phys, vol 47, issue 4, Rogers CL, Shetter AG, Fiedler JA, Smith KA, Han PP, Speiser BL, Gamma knife radiosurgery for trigeminal neuralgia: the initial experience of the Barrow Neurological Institute, pp , copyright 2000, with permission from Elsevier. 2
3 J. A. Steinberg et al. FIG. 1. Creation of a right-sided tentorial sling. A: View of the cerebellopontine angle, including the underside of the tentorium (Tent). The SCA is seen looping inferiorly, compressing the medial/superior aspect of the trigeminal nerve (TN). B: An initial 3-mm transverse incision is made using a 15 blade. C: Dissection is carried out in a split-thickness plane of the dura. D: Microscissors are used to cut perpendicular to the initial incision. E: A parallel cut, approximately cm long, is made to complete the tentorial sling (SL). F: A view of the tentorial sling prior to wrapping around the compressive vessel. *Tentorial incision. Figure is available in color online only. with care to preserve any perforators, as too much tension may cause avulsion (Fig. 2A C). Once the tentorial sling is wrapped around the compressive vessel, the complex is brought back up to the tentorium, thereby transposing the vessel away from the trigeminal nerve. The free edge of the tentorial sling is secured to the uppermost aspect of the sling or to the free cut edge of the tentorium with a Weck (Teleflex) clip (Fig. 2D). Once displaced away from the nerve, the vessel is inspected to ensure pulsatility and continued blood flow while also inspecting the nerve to ensure adequate decompression (Fig. 2E and F). Photographs obtained before and after vessel transposition utilizing the tentorial sling technique are directly contrasted, as shown in Fig. 3. A video of the tentorial sling microsurgical technique demonstrates the procedure performed in a cadaveric specimen (Video 1). VIDEO 1. Video clip demonstrating the tentorial sling technique for decompression of the trigeminal nerve in a cadaveric specimen. CN = cranial nerve. Copyright Jeffrey A. Steinberg. Published with permission. Click here to view. The dura is closed in a watertight fashion if permissible, with use of dural substitute as needed, followed by use of bone cement to fill the craniectomy defect. The soft tissue is then closed in sequential layers. Results A total of 45 patients met inclusion criteria for our study, having undergone MVD for trigeminal neuralgia with the use of a tentorial sling. Thirteen other patients underwent MVD for trigeminal neuralgia during the same period without the tentorial sling method. This included 5 patients who underwent revision MVD (3 from outside FIG. 2. Utilization of the tentorial sling to transpose the compressive vessel away from the nerve. A: The tentorial sling is mobilized toward the compressive vessel. B: The vessel is lifted to allow the tentorial sling to be positioned around it. C: The sling is manipulated around the vessel. D: The free edge of the sling is secured to the tentorium using a Weck clip. E: The transposed vessel is inspected to ensure no constriction of blood flow and adequate decompression of the nerve. F: Final view of the vessel repositioned away from the trigeminal nerve by the tentorial sling. The motor rootlet (MR) of the trigeminal nerve is now visible. Figure is available in color online only. 3
4 J. A. Steinberg et al. FIG. 3. Left: Initial view of the right trigeminal nerve demonstrating the SCA compressing the superior aspect of the trigeminal nerve root entry zone. Right: Final view after completing the tentorial sling technique for vessel transposition. The motor rootlet of the trigeminal nerve is now visible, as the nerve has been decompressed. Figure is available in color online only. institutions) and 8 patients without a direct arterial compressive vessel. Patient demographics for those who underwent the tentorial sling procedure included 14 males and 31 females. The mean age at the time of surgery was 59 years. Twenty-eight (62%) MVDs were right-sided and 17 (38%) were left-sided. Trigeminal neuralgia in all patients was categorized as classical trigeminal neuralgia as defined by the International Classification of Headache Disorders (13.1.1). The mean length of stay was 3.7 days with a median length of stay of 3 days. For 41 patients (91%), MVD with use of the tentorial sling was the first decompressive procedure for trigeminal neuralgia. Seven of these patients had undergone prior palliative procedures: radiofrequency ablation in 1 patient, Gamma Knife radiosurgery in 2 patients, glycerol injection in 2 patients, balloon compression in 1 patient, and both Gamma Knife radiosurgery and glycerol injection in 1 patient. The other 4 patients had undergone prior MVD, 3 at outside institutions and 1 at the University of California, San Diego, by the senior author. Immediate postoperative clinical outcomes are shown in Table 2 for the 41 patients who underwent their first MVD. Thirty-three patients (80%) achieved complete relief of facial pain (BNI score I). Two other patients had significant symptom relief, with only occasional pain and no medication usage (BNI score II). Two patients reported improvement, but still required medication to manage their facial pain (BNI score III), and 4 patients had minimal to no relief (BNI score IV or V). In the patients who underwent MVD with use of a tentorial sling as their first decompressive procedure (n = 41), the mean follow-up time was 16 months (range 2 36 months). The clinical outcomes for these patients at the time of the study are listed in Table 2. Three patients who were initially free of facial pain developed recurrence of their trigeminal neuralgia at 12, 18, and 36 months. As a result, 73% of patients remained completely pain free without medication use at the last follow-up (BNI score I). Including the 2 patients who maintained significant pain relief with only occasional mild pain (BNI score II), 78% of patients had a favorable result at last follow-up. Of the 7 patients with minimal or no improvement at last follow-up (BNI score IV or V), one had a history of prior glycerol injection and another a history of prior Gamma Knife radiosurgery. 4 Three patients underwent reexploration for continued pain after their initial MVD with a tentorial sling. In one of these patients, no new compressive vessel or lesion was found, and the tentorial sling transposition of the previously compressive artery was intact. Massage of the trigeminal nerve was performed, and the pain decreased to BNI score II postoperatively. Another patient initially had complete resolution of pain for 1 year; however, the pain recurred to a BNI score of IV. Reexploration demonstrated significant adhesions between the dura, cerebellum, trigeminal nerve, and surrounding structures. The tentorial sling vessel construct was intact. After releasing the adhesions, the patient achieved resolution of pain (BNI score I). In the third patient, the sling remained intact; however, a portion of the ectatic vessel had come in contact with the nerve. This portion of the vessel was mobilized away from the nerve, and a small piece of Teflon was placed between the 2 structures. This revision MVD was performed in the only patient in the study in whom foreign material (Teflon) was used, with a final technical result utilizing the tentorial sling in the first procedure and Teflon in the second because of the ectatic vessel anatomy. Postoperatively, the patient s pain improved to a BNI score of II. These 3 patients were all recorded as having a BNI score of IV or V at last follow-up for the study (Table 2). Examining outcomes after these 3 reexploration surgeries, 35 patients (85%) achieved complete pain relief or significant improvement in facial pain (BNI score I or II). Of the 4 patients in the study who had undergone prior MVD without the use of a tentorial sling, 1 patient had a complete cure (BNI score I), and the other 3 achieved moderate improvement in pain (BNI score III). Although each of these patients had undergone prior MVD, a compressive vessel was discovered during the senior author s repeat exploration, which was amenable to decompression by the dural sling transposition method. The overall complication rate for the 45 procedures performed was 6.6%. Complications included 2 CSF leaks (one requiring CSF diversion), and 1 patient had a small cerebellar stroke within the superior cerebellar artery (SCA) territory, resulting in mild dysmetria. This patient had an ectatic, tortuous SCA that looped down around the trigeminal nerve. Mobilization of the vessel involved significant manipulation of the artery to decompress the nerve. The sling portion of the procedure was completed
5 J. A. Steinberg et al. TABLE 2. Immediate postoperative outcome and outcome at last follow-up in patients who underwent MVD as their first decompressive procedure BNI Score Immediate Outcome No. of Patients (n = 41) Outcome at Last Follow-Up I II 2 2 III 2 2 IV 2 4 V 2 3 without complication. The small postoperative stroke was attributed to the significant manipulation of the vessel. No postoperative facial numbness was encountered in any patient. Discussion Microvascular decompression remains the only definitive cure for trigeminal neuralgia. Traditional methods involve placement of a foreign material (most often Teflon) between the compressive vessel and nerve. Multiple studies have demonstrated that inflammatory responses to this material can result in granuloma formation and lead to pain recurrence and failure of the MVD. 4,5,8 In a review by Capelle et al., the authors reviewed their series of 200 patients and found 3 with a Teflon granuloma during reexploration for recurrent facial pain. 4 Additionally, the authors reviewed a small body of literature in which occurrence of Teflon granulomas was reported, citing an overall incidence of 1% 7%. The present study is the first of its size to describe MVD with use of a tentorial sling for vessel transposition. For patients undergoing MVD with the use of a tentorial sling as their initial decompressive procedure, 80% achieved complete pain relief immediately following surgery, defined as a BNI pain score of I. Including the 2 patients who only experienced occasional facial pain after the procedure, 85% had significant improvement postoperatively. However, 3 patients did develop recurrence of pain. At the last follow-up, the cure rate was 73%, with 78% of patients achieving significant improvement of their facial pain. In one of the largest MVD clinical outcome studies for trigeminal neuralgia, Barker et al. reported an 82% rate of pain relief immediately following surgery and a 75% rate at 1 year. 1 Additionally, maintenance of pain relief at 10 years was 64%, demonstrating the continued recurrence of facial pain over time. Four patients underwent MVD with the use of a tentorial sling after previously undergoing traditional MVD. Results for these patients were mixed 1 patient had complete pain relief, and 3 achieved partial pain relief. In general, repeat MVD for trigeminal neuralgia is associated with variable outcome. Additionally, performing repeat MVD utilizing a sling method is only applicable for patients found to have a compressive artery against the nerve. All patients who underwent the tentorial sling procedure were found to have a compressive artery at the nerve root entry zone without other sources of compression. No foreign material was used in any of the patients undergoing MVD with use of the tentorial sling except for a patient who experienced pain recurrence; during reexploration, Teflon was used to augment the previous tentorial sling SCA complex, which remained intact. Although temporal durability of this procedure requires longer-term patient outcome data, we believe that it has 2 main advantages over the traditional MVD method. First, the sling method does not require the use of foreign material, aside from a Weck clip to hold the sling in place. A Weck clip is used to secure the tentorial sling as it provides efficient and permanent fixation. An alternative option of utilizing suture to secure the tentorial sling is possible; however, because of the small corridor and deep location of the site, we believe that this would incur added operative time and challenge. In the absence of foreign material, the likelihood of an inflammatory response is minimized. This may lead to a lower rate of trigeminal pain recurrence over time. Second, by transposing the vessel away from the nerve, there is no vessel/foreign material complex near the trigeminal nerve. Instead, the artery is repositioned, leaving the nerve and root entry zone free from any compression, including that from inserted material. Because the vessel is wrapped, postoperative migration of the vessel back toward the nerve is unlikely. In the 3 patients who underwent reexploration in our study, we found that all tentorial slings were maintained in place with the vessel adequately repositioned and with good pulsatile flow. In one patient, an ectatic portion of the SCA had come in contact with the nerve. Another patient demonstrated significant adhesion formation. During reexploration in the third patient, no compression or adhesions of the nerve were found. Although facial pain recurred in these patients, the tentorial sling remained intact. These cases are a reminder that the pathophysiology of trigeminal neuralgia is complex and incompletely understood. Although our results are similar to those of the traditional MVD technique, the unique tentorial sling method described here provides neurosurgeons an alternative surgical technique that may be used in cases in which buttressing with foreign material alone does not provide enough decompression. The tentorial sling method does have limitations. As with any new procedure, there is a learning curve. Challenges with creating the tentorial sling include tearing of the dura, bleeding, and maintaining a split-thickness pedicle. We found that laying a piece of Gelfoam along the cerebellopontine angle when creating the sling prevents tentorial bleeding from accumulating at this site. Additionally, use of Surgicel and bipolar cautery help control bleeding from the cut edges of the tentorium. Care must be taken not to shrink the dural sling with excessive use of bipolar cautery. The sling procedure adds minutes of surgical time initially when learning the technique; however, after becoming accustomed to the method, the procedure could be performed in approximately 20 minutes. In our practice, we regularly sacrifice the petrosal vein in both the traditional MVD technique and the novel method described here. We have not found that this leads to a higher complication profile, and we believe that sacrifice of the petrosal vein allows for improved operating 5
6 J. A. Steinberg et al. and visualization of the nerve root entry zone without hindrance by bridging veins during the procedure. The sling procedure is not applicable to all MVD procedures for trigeminal neuralgia. As stated in Results, 13 patients were not candidates for the tentorial sling method during the 2.5-year period utilizing this novel method. Five of these patients had prior MVDs and underwent revision procedures for pain recurrence with adherent Teflon discovered at the nerve root entry zone, and the other 8 patients had anatomy that was unfavorable for using the sling method. In these 8 patients veins or venous complexes were found at the nerve root entry zone, which were mobilized and coagulated when appropriate. No Teflon was used in these cases, as no arterial compression was encountered. When no arterial compression is found or when perforator anatomy is unfavorable, the sling method cannot be used. This is a similar challenge encountered with traditional MVD procedures when no evidence of arterial compression is identified. Conclusions This study represents the largest series of patients with trigeminal neuralgia who were treated using a decompressive sling technique. Although the long-term durability of this technique is unknown, it has potential advantages over traditional methods, as it avoids the use of foreign material and achieves complete transposition of the compressive vessel. Limitations include extending the surgical time and potentially dural bleeding. Although Teflon granuloma is reviewed in this study and described in the literature, it should be understood that the rate of complications from Teflon or other foreign material is relatively low, and traditional MVD techniques remain an overall very successful neurosurgical procedure. The tentorial slinging technique provides an alternative decompressive method for neurosurgeons who treat trigeminal neuralgia. We plan to assess clinical follow-up in our patients at 5- and 10-year time points to further assess temporal durability. References 1. Barker FG II, Jannetta PJ, Bissonette DJ, Larkins MV, Jho HD: The long-term outcome of microvascular decompression for trigeminal neuralgia. N Engl J Med 334: , Bobek MP, Sagher O: Aseptic meningitis caused by Teflon implantation for microvascular decompression. Case report. J Neurosurg 90: , Burchiel KJ, Clarke H, Haglund M, Loeser JD: Long-term efficacy of microvascular decompression in trigeminal neuralgia. J Neurosurg 69:35 38, Capelle HH, Brandis A, Tschan CA, Krauss JK: Treatment of recurrent trigeminal neuralgia due to Teflon granuloma. J Headache Pain 11: , Chen J, Lee S, Lui T, Yeh Y, Chen T, Tzaan W: Teflon granuloma after microvascular decompression for trigeminal neuralgia. Surg Neurol 53: , Cruccu G, Gronseth G, Alksne J, Argoff C, Brainin M, Burchiel K, et al: AAN-EFNS guidelines on trigeminal neuralgia management. Eur J Neurol 15: , Fukushima T: [Posterior cranial fossa neurovascular decompression (Jannetta method) for trigeminal neuralgia and facial spasm.] No Shinkei Geka 10: , 1982 (Jpn) 8. Masuoka J, Matsushima T, Inoue K, Nakahara Y, Takase Y, Kawashima M: Outcome of microvascular decompression for trigeminal neuralgia treated with the stitched sling retraction technique. Neurosurg Rev 38: , Masuoka J, Matsushima T, Kawashima M, Nakahara Y, Funaki T, Mineta T: Stitched sling retraction technique for microvascular decompression: procedures and techniques based on an anatomical viewpoint. Neurosurg Rev 34: , Matsushima T, Yamaguchi T, Inoue TK, Matsukado K, Fukui M: Recurrent trigeminal neuralgia after microvascular decompression using an interposing technique. Teflon felt adhesion and the sling retraction technique. Acta Neurochir (Wien) 142: , Melvill RL, Baxter BL: A tentorial sling in microvascular decompression for trigeminal neuralgia. Technical note. J Neurosurg 84: , Meybodi AT, Habibi Z, Miri M, Tabatabaie SAF: Microvascular decompression for trigeminal neuralgia using the stitched sling retraction technique in recurrent cases after previous microvascular decompression. Acta Neurochir (Wien) 156: , Mitsos AP, Georgakoulias N, Lafazanos SA, Konstantinou EA: The hanging technique of vascular transposition in microvascular decompression for trigeminal neuralgia: technical report of four cases. Neurosurg Rev 31: , Rogers CL, Shetter AG, Fiedler JA, Smith KA, Han PP, Speiser BL: Gamma knife radiosurgery for trigeminal neuralgia: the initial experience of the Barrow Neurological Institute. Int J Radiat Oncol Biol Phys 47: , Yang DB, Jiang DY, Chen HC, Wang ZM: Second microvascular decompression for trigeminal neuralgia in recurrent cases after microvascular decompression. J Craniofac Surg 26: , Zakrzewska JM, Linskey ME: Trigeminal neuralgia. BMJ 348:g474, 2014 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: Steinberg, Sack, Weingarten, Alksne. Acquisition of data: Steinberg, Wilson. Analysis and interpretation of data: Steinberg, Sack, Wilson, Alksne. Drafting the article: Steinberg, Sack, Alksne. Critically revising the article: Steinberg, Sack, Ben-Haim, Alksne. Reviewed submitted version of manuscript: all authors. Approved the final version of the manuscript on behalf of all authors: Steinberg. Study supervision: Steinberg, Sack, Weingarten, Carter, Khalessi, Alksne. Supplemental Information Videos Video 1. Previous Presentations Preliminary data from this paper were presented as an oral abstract at the North American Skull Base Society 27th Annual Meeting, New Orleans, Louisiana, March 4, Correspondence Jeffrey A. Steinberg: University of California, San Diego, CA. j1steinberg@ucsd.edu. 6
Il dolore nelle nevralgie e trattamento chirurgico
 Il dolore nelle nevralgie e trattamento chirurgico F. TOMASELLO Clinica Neurochirurgica, Università di Messina Napoli, 28 Maggio 2012 NEUROVASCULAR COMPRESSION SYNDROMES Trigeminal neuralgia (V cranial
Il dolore nelle nevralgie e trattamento chirurgico F. TOMASELLO Clinica Neurochirurgica, Università di Messina Napoli, 28 Maggio 2012 NEUROVASCULAR COMPRESSION SYNDROMES Trigeminal neuralgia (V cranial
Clinical features and surgical treatment of trigeminal neuralgia caused solely by venous compression
 Acta Neurochir (2011) 153:1037 1042 DOI 10.1007/s00701-011-0957-x CLINICAL ARTICLE Clinical features and surgical treatment of trigeminal neuralgia caused solely by venous compression Wenyao Hong & Xuesheng
Acta Neurochir (2011) 153:1037 1042 DOI 10.1007/s00701-011-0957-x CLINICAL ARTICLE Clinical features and surgical treatment of trigeminal neuralgia caused solely by venous compression Wenyao Hong & Xuesheng
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
Shanghai Jiao Tong University, School of Medicine, Shanghai Ninth People s Hospital, Department of Neurosurgery, Shanghai, China
 DOI: 10.5137/1019-5149.JTN.23513-18.1 Received: 16.04.2018 / Accepted: 02.07.2018 Published Online: 19.11.2018 Turk Neurosurg, 2018 Original Investigation Effects of Microvascular Decompression Plus Longitudinal
DOI: 10.5137/1019-5149.JTN.23513-18.1 Received: 16.04.2018 / Accepted: 02.07.2018 Published Online: 19.11.2018 Turk Neurosurg, 2018 Original Investigation Effects of Microvascular Decompression Plus Longitudinal
Two types of posterior fossa veins are involved in. FOCUS Neurosurg Focus 45 (1):E2, 2018
 NEUROSURGICAL FOCUS Neurosurg Focus 45 (1):E2, 2018 Bridging veins and veins of the brainstem in microvascular decompression surgery for trigeminal neuralgia and hemifacial spasm Hiroki Toda, MD, PhD,
NEUROSURGICAL FOCUS Neurosurg Focus 45 (1):E2, 2018 Bridging veins and veins of the brainstem in microvascular decompression surgery for trigeminal neuralgia and hemifacial spasm Hiroki Toda, MD, PhD,
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Fleece-Bound Tissue Sealing in Microvascular Decompression
 DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve
 Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve Pages with reference to book, From 140 To 143 Nawab Mohammad Khan, Mohammad Afzal Khan, Fazal Karim Aasi ( Department
Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve Pages with reference to book, From 140 To 143 Nawab Mohammad Khan, Mohammad Afzal Khan, Fazal Karim Aasi ( Department
H emifacial spasm (HFS) is an infrequent disorder with
 1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... J Neurol Neurosurg Psychiatry 2005;76:1574 1580. doi: 10.1136/jnnp.2004.056861
1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... J Neurol Neurosurg Psychiatry 2005;76:1574 1580. doi: 10.1136/jnnp.2004.056861
H emifacial spasm (HFS) is an infrequent disorder with
 1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... See end of article for authors affiliations... Correspondence to: Dr Amin Kassam,
1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... See end of article for authors affiliations... Correspondence to: Dr Amin Kassam,
Perforating branches from ovending arteries in hemifacial spasm: anatomical correlation with vertebrobasilar configuration
 J Neurol Neurosurg Psychiatry 1999;67:73 77 73 Department of Neurosurgery, Nagoya University School of Medicine, Nagoya, Japan T Nagatani S Inao Y Suzuki J Yoshida Correspondence to: Dr T Nagatani, Department
J Neurol Neurosurg Psychiatry 1999;67:73 77 73 Department of Neurosurgery, Nagoya University School of Medicine, Nagoya, Japan T Nagatani S Inao Y Suzuki J Yoshida Correspondence to: Dr T Nagatani, Department
Tumor-related trigeminal neuralgia (TRTN) is
 clinical article J Neurosurg 125:838 844, 2016 Gamma Knife surgery for tumor-related trigeminal neuralgia: targeting both the tumor and the trigeminal root exit zone in a single session Sung Kwon Kim,
clinical article J Neurosurg 125:838 844, 2016 Gamma Knife surgery for tumor-related trigeminal neuralgia: targeting both the tumor and the trigeminal root exit zone in a single session Sung Kwon Kim,
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
ABSTRACT INTRODUCTION
 /, 2017, Vol. 8, (No. 27), pp: 44819-44823 After microvascular decompression to treat trigeminal neuralgia, both immediate pain relief and recurrence rates are higher in patients with arterial compression
/, 2017, Vol. 8, (No. 27), pp: 44819-44823 After microvascular decompression to treat trigeminal neuralgia, both immediate pain relief and recurrence rates are higher in patients with arterial compression
Management of medically refractory trigeminal neuralgia in patients with multiple sclerosis
 Neurosurg Focus 18 (5):E13, 2005 Management of medically refractory trigeminal neuralgia in patients with multiple sclerosis JASON S. CHENG, B.S., RENE O. SANCHEZ-MEJIA, M.D., MARY LIMBO, B.A., MARIANN
Neurosurg Focus 18 (5):E13, 2005 Management of medically refractory trigeminal neuralgia in patients with multiple sclerosis JASON S. CHENG, B.S., RENE O. SANCHEZ-MEJIA, M.D., MARY LIMBO, B.A., MARIANN
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression
 MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
Tr i g e m i n a l neuralgia is a form of facial pain that. Trigeminal neuralgia in young adults. Clinical article
 J Neurosurg 114:1306 1311, 2011 Trigeminal neuralgia in young adults Clinical article Di a a Ba h g a t, M.D., Di b y e n d u K. Ray, M.B.B.S., M.S., M.Ch., Ahm e d M. Ra s l a n, M.D., Sh i r l e y McCa
J Neurosurg 114:1306 1311, 2011 Trigeminal neuralgia in young adults Clinical article Di a a Ba h g a t, M.D., Di b y e n d u K. Ray, M.B.B.S., M.S., M.Ch., Ahm e d M. Ra s l a n, M.D., Sh i r l e y McCa
Microvascular decompression (MVD) is an important ENDOSCOPE-ASSISTED MICROSURGERY FOR MICROVASCULAR COMPRESSION SYNDROMES CLINICAL STUDIES
 CLINICAL STUDIES ENDOSCOPE-ASSISTED MICROSURGERY FOR MICROVASCULAR COMPRESSION SYNDROMES Ramin Rak, M.D. Department of Neurosurgery, North Shore University Hospital, Great Neck, New York Laligam N. Sekhar,
CLINICAL STUDIES ENDOSCOPE-ASSISTED MICROSURGERY FOR MICROVASCULAR COMPRESSION SYNDROMES Ramin Rak, M.D. Department of Neurosurgery, North Shore University Hospital, Great Neck, New York Laligam N. Sekhar,
Microvascular decompression of cranial nerves: lessons learned after 4400 operations
 J Neurosurg 90:1 8, 1999 Microvascular decompression of cranial nerves: lessons learned after 4400 operations MARK R. MCLAUGHLIN, M.D., PETER J. JANNETTA, M.D., BRENT L. CLYDE, M.D., BRIAN R. SUBACH, M.D.,
J Neurosurg 90:1 8, 1999 Microvascular decompression of cranial nerves: lessons learned after 4400 operations MARK R. MCLAUGHLIN, M.D., PETER J. JANNETTA, M.D., BRENT L. CLYDE, M.D., BRIAN R. SUBACH, M.D.,
Microvascular Decompression of the Vestibulocochlear Nerve
 JOURNAL OF CASE REPORTS 2015;5(1):182-186 Microvascular Decompression of the Vestibulocochlear Nerve Henry Emanuel, Zakier Hussain Department of Neurosurgery, Waikato Hospital, Hamilton, New Zealand. Abstract:
JOURNAL OF CASE REPORTS 2015;5(1):182-186 Microvascular Decompression of the Vestibulocochlear Nerve Henry Emanuel, Zakier Hussain Department of Neurosurgery, Waikato Hospital, Hamilton, New Zealand. Abstract:
Long-Term Therapeutic Effect of Microvascular Decompression for Trigeminal Neuralgia: Kaplan-Meier Analysis in a Consecutive Series of 425 Patients
 DOI: 10.5137/1019-5149.JTN.18322-16.1 Received: 02.06.2016 / Accepted: 05.08.2016 Published Online: 22.08.2016 Original Investigation Long-Term Therapeutic Effect of Microvascular Decompression for Trigeminal
DOI: 10.5137/1019-5149.JTN.18322-16.1 Received: 02.06.2016 / Accepted: 05.08.2016 Published Online: 22.08.2016 Original Investigation Long-Term Therapeutic Effect of Microvascular Decompression for Trigeminal
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM
 INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
Classification of Facial Pain. Surgical Treatment of Facial Pain. Typical trigeminal neuralgia. Atypical trigeminal neuralgia
 Surgical Treatment of Facial Pain Nicholas M. Barbaro, MD University of California at San Francisco Classification of Facial Pain Trigeminal neuralgia Atypical trigeminal neuralgia Neuropathic facial pain
Surgical Treatment of Facial Pain Nicholas M. Barbaro, MD University of California at San Francisco Classification of Facial Pain Trigeminal neuralgia Atypical trigeminal neuralgia Neuropathic facial pain
Copyright, 1996, by the Massachusetts Medical Society
 Copyright, 996, by the Massachusetts Medical Society Volume 334 APRIL 5, 996 Number 7 THE LONG-TERM OUTCOME OF MICROVASCULAR DECOMPRESSION FOR TRIGEMINAL NEURALGIA FRED G. BARKER II, M.D., PETER J. JANNETTA,
Copyright, 996, by the Massachusetts Medical Society Volume 334 APRIL 5, 996 Number 7 THE LONG-TERM OUTCOME OF MICROVASCULAR DECOMPRESSION FOR TRIGEMINAL NEURALGIA FRED G. BARKER II, M.D., PETER J. JANNETTA,
Stereotactic Radiosurgery for Glossopharyngeal Neuralgia: An International Multicenter Study
 Stereotactic Radiosurgery for Glossopharyngeal Neuralgia: An International Multicenter Study University of Pittsburgh Hideyuki Kano, MD, PhD L. Dade Lunsford, MD Hospital Na Homolce, Prague Dusan Urgosik,
Stereotactic Radiosurgery for Glossopharyngeal Neuralgia: An International Multicenter Study University of Pittsburgh Hideyuki Kano, MD, PhD L. Dade Lunsford, MD Hospital Na Homolce, Prague Dusan Urgosik,
Centerline Carpal Tunnel Release
 Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
Centerline Endoscopic Carpal Tunnel Release Surgical Technique Centerline Carpal Tunnel Release Centerline Endoscopic Carpal Tunnel Release Surgical Set Up The patient is positioned supine on the operating
Trigeminal Neuralgia Involving All Three Branches Of Trigeminal Nerve Treated By Peripheral Neurectomy: An Interesting Case Report
 ISPUB.COM The Internet Journal of Dental Science Volume 10 Number 2 Trigeminal Neuralgia Involving All Three Branches Of Trigeminal Nerve Treated By Peripheral Neurectomy: An Interesting Case Report K
ISPUB.COM The Internet Journal of Dental Science Volume 10 Number 2 Trigeminal Neuralgia Involving All Three Branches Of Trigeminal Nerve Treated By Peripheral Neurectomy: An Interesting Case Report K
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Adamec I., Grahovac G., Krbot Skorić M., Chudy D., Hajnšek S, Habek M. (2014) Tongue somatosensory-evoked potentials in microvascular decompression treated trigeminal neuralgia.
Središnja medicinska knjižnica Adamec I., Grahovac G., Krbot Skorić M., Chudy D., Hajnšek S, Habek M. (2014) Tongue somatosensory-evoked potentials in microvascular decompression treated trigeminal neuralgia.
Review Article Clinical Outcomes of Gamma Knife Radiosurgery in the Treatment of Patients with Trigeminal Neuralgia
 Hindawi Publishing Corporation International Journal of Otolaryngology Volume 2012, Article ID 919186, 13 pages doi:10.1155/2012/919186 Review Article Clinical Outcomes of Gamma Knife Radiosurgery in the
Hindawi Publishing Corporation International Journal of Otolaryngology Volume 2012, Article ID 919186, 13 pages doi:10.1155/2012/919186 Review Article Clinical Outcomes of Gamma Knife Radiosurgery in the
Patterns of sensory loss following fractional posterior
 Journal of Neurology, Neurosurgery, and Psychiatry 1982;45:786-790 Patterns of sensory loss following fractional posterior fossa Vth nerve section for trigeminal neuralgia M HUSSEIN,* LA WILSON,t R ILLINGWORTH
Journal of Neurology, Neurosurgery, and Psychiatry 1982;45:786-790 Patterns of sensory loss following fractional posterior fossa Vth nerve section for trigeminal neuralgia M HUSSEIN,* LA WILSON,t R ILLINGWORTH
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
The human brainstem, roughly the size of the thumb,
 TECHNICAL NOTE J Neurosurg 127:1134 1138, 2017 The superior fovea triangle approach: a novel safe entry zone to the brainstem *Kaan Yagmurlu, MD, M. Yashar S. Kalani, MD, PhD, Mark C. Preul, MD, and Robert
TECHNICAL NOTE J Neurosurg 127:1134 1138, 2017 The superior fovea triangle approach: a novel safe entry zone to the brainstem *Kaan Yagmurlu, MD, M. Yashar S. Kalani, MD, PhD, Mark C. Preul, MD, and Robert
Trigeminal neuralgia (TN) is a pain syndrome characterized
 clinical article J Neurosurg 122:1048 1057, 2015 Long-term efficacy and safety of internal neurolysis for trigeminal neuralgia without neurovascular compression Andrew L. Ko, MD, 1 Alp Ozpinar, BA, 1 Albert
clinical article J Neurosurg 122:1048 1057, 2015 Long-term efficacy and safety of internal neurolysis for trigeminal neuralgia without neurovascular compression Andrew L. Ko, MD, 1 Alp Ozpinar, BA, 1 Albert
The Very Long-Term Outcome of Radiosurgery for Classical Trigeminal Neuralgia
 Clinical Study Received: September 16, 2015 Accepted after revision: December 21, 2015 Published online: February 17, 2016 The Very Long-Term Outcome of Jean Régis a Constantin Tuleasca a, d f Noémie Resseguier
Clinical Study Received: September 16, 2015 Accepted after revision: December 21, 2015 Published online: February 17, 2016 The Very Long-Term Outcome of Jean Régis a Constantin Tuleasca a, d f Noémie Resseguier
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
A prospective cost-effectiveness study of trigeminal neuralgia surgery Pollock B E, Ecker R D
 A prospective cost-effectiveness study of trigeminal neuralgia surgery Pollock B E, Ecker R D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on
A prospective cost-effectiveness study of trigeminal neuralgia surgery Pollock B E, Ecker R D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
Stereotactic radiosurgery for idiopathic trigeminal neuralgia
 J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY
 Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Arterial compression of nerve is the primary cause of trigeminal neuralgia
 Neurol Sci (2014) 35:61 66 DOI 10.1007/s10072-013-1518-2 ORIGINAL ARTICLE Arterial compression of nerve is the primary cause of trigeminal Guo-qiang Chen Xiao-song Wang Lin Wang Jia-ping Zheng Received:
Neurol Sci (2014) 35:61 66 DOI 10.1007/s10072-013-1518-2 ORIGINAL ARTICLE Arterial compression of nerve is the primary cause of trigeminal Guo-qiang Chen Xiao-song Wang Lin Wang Jia-ping Zheng Received:
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM
 EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
MVD for trigeminal neuralgia; neuralgia revisited with review of literature
 International Journal of Otorhinolaryngology and Head and Neck Surgery Melkundi RS et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Oct;3(4):849-853 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Melkundi RS et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Oct;3(4):849-853 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Initial experience with endoscopic carpal tunnel release surgery
 Initial experience with endoscopic carpal tunnel release surgery Craig H. Rabb, M.D., and Todd Kuether, M.D. Division of Neurosurgery, Oregon Health Sciences University, Portland, Oregon; and Portland
Initial experience with endoscopic carpal tunnel release surgery Craig H. Rabb, M.D., and Todd Kuether, M.D. Division of Neurosurgery, Oregon Health Sciences University, Portland, Oregon; and Portland
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Journal of Clinical Neuroscience
 Journal of Clinical Neuroscience 20 (2013) 107 111 Contents lists available at SciVerse ScienceDirect Journal of Clinical Neuroscience journal homepage: www.elsevier.com/locate/jocn Clinical Study Preoperative
Journal of Clinical Neuroscience 20 (2013) 107 111 Contents lists available at SciVerse ScienceDirect Journal of Clinical Neuroscience journal homepage: www.elsevier.com/locate/jocn Clinical Study Preoperative
Trigeminal Neuralgia (facial pain)
 Trigeminal Neuralgia (facial pain) Overview Trigeminal neuralgia is an inflammation of the trigeminal nerve, causing extreme pain and muscle spasms in the face. Attacks of intense, electric shock-like
Trigeminal Neuralgia (facial pain) Overview Trigeminal neuralgia is an inflammation of the trigeminal nerve, causing extreme pain and muscle spasms in the face. Attacks of intense, electric shock-like
PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.*
 Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Neurovascular elements of the PCF
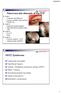 Level I: Neurovascular elements of the PCF Trigeminal and Abducent Superior cerebellar artery and vein Dandy s vein Level II: Facial and Cochleovestibular AICA and internal auditory artery, veins Level
Level I: Neurovascular elements of the PCF Trigeminal and Abducent Superior cerebellar artery and vein Dandy s vein Level II: Facial and Cochleovestibular AICA and internal auditory artery, veins Level
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
doi: /s
 doi: 10.1007/s00701-015-2530-5 Abducent nerve palsy treated by microvascular decompression: a case report and review of the literature TOMOSATO YAMAZAKI, 1,2 TETSUYA YAMAMOTO, 2 TORU HATAYAMA, 3 ALEXANDER
doi: 10.1007/s00701-015-2530-5 Abducent nerve palsy treated by microvascular decompression: a case report and review of the literature TOMOSATO YAMAZAKI, 1,2 TETSUYA YAMAMOTO, 2 TORU HATAYAMA, 3 ALEXANDER
Shin Heon Lee, Taek Kyun Nam, Ki-Su Park, Yong-Sook Park, Seung Won Park, Jeong-Taik Kwon, Young-Baeg Kim
 Original Article eissn2465-891x The Nerve.2016.2(2):42-47 https://doi.org/10.21129/nerve.2016.2.2.42 www.thenerve.net Image-fusion Technique in Microvascular Decompression Surgery with 3D Constructive
Original Article eissn2465-891x The Nerve.2016.2(2):42-47 https://doi.org/10.21129/nerve.2016.2.2.42 www.thenerve.net Image-fusion Technique in Microvascular Decompression Surgery with 3D Constructive
Surgery has been proven to be beneficial for selected patients
 Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Thoracoscopic Lung Volume Reduction Surgery Robert J. McKenna, Jr, MD Surgery has been proven to be beneficial for selected patients with severe emphysema. Compared with medical management, lung volume
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Microsurgical Anatomy and Surgery of the Posterior Cranial Fossa
 Microsurgical Anatomy and Surgery of the Posterior Cranial Fossa Toshio Matsushima Microsurgical Anatomy and Surgery of the Posterior Cranial Fossa Surgical Approaches and Procedures Based on Anatomical
Microsurgical Anatomy and Surgery of the Posterior Cranial Fossa Toshio Matsushima Microsurgical Anatomy and Surgery of the Posterior Cranial Fossa Surgical Approaches and Procedures Based on Anatomical
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE
 Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
The translabyrinthine approach has been
 OPERATIVE NUANCES TRANSLABYRINTHINE APPROACH FOR ACOUSTIC NEUROMA John Diaz Day, M.D. Department of Neurosurgery, Drexel University College of Medicine, Philadelphia, Pennsylvania, and Allegheny General
OPERATIVE NUANCES TRANSLABYRINTHINE APPROACH FOR ACOUSTIC NEUROMA John Diaz Day, M.D. Department of Neurosurgery, Drexel University College of Medicine, Philadelphia, Pennsylvania, and Allegheny General
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
06/Μαρ/2013 FUNCTION OF THE ROTATOR CUFF. ARTHROSCOPIC ROTATOR CUFF REPAIR Primarily to stabilize and centralize the humeral head GENERAL GUIDE LINES
 FUNCTION OF THE ROTATOR CUFF ARTHROSCOPIC ROTATOR CUFF REPAIR Primarily to stabilize and centralize the humeral head GENERAL GUIDE LINES Achieved by balancing the force couples in coronal and transverse
FUNCTION OF THE ROTATOR CUFF ARTHROSCOPIC ROTATOR CUFF REPAIR Primarily to stabilize and centralize the humeral head GENERAL GUIDE LINES Achieved by balancing the force couples in coronal and transverse
Antonio De la Cruz, MD 27th Alexandria International Combined ORL Congress Alexandria, Egypt April 8, 2009
 ACOUSTIC NEUROMA TREATMENT OPTIONS 2009 27 th Alexandria International Combined ORL Congress Alexandria, Egypt April 10, 2009 AntonioDelaCruz Cruz, MD House Ear Institute Los Angeles, California Antonio
ACOUSTIC NEUROMA TREATMENT OPTIONS 2009 27 th Alexandria International Combined ORL Congress Alexandria, Egypt April 10, 2009 AntonioDelaCruz Cruz, MD House Ear Institute Los Angeles, California Antonio
T HE direct surgical approach to an aneurysm on
 J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
Trigeminal Neuralgia Future directions. Prof Joanna M. Zakrzewska 18 th International Leksell Gamma Knife Society Amsterdam 2016
 Trigeminal Neuralgia Future directions Prof Joanna M. Zakrzewska 18 th International Leksell Gamma Knife Society Amsterdam 2016 Aims and Objectives objectives Phenotying Outcomes Drugs vs surgery Imaging
Trigeminal Neuralgia Future directions Prof Joanna M. Zakrzewska 18 th International Leksell Gamma Knife Society Amsterdam 2016 Aims and Objectives objectives Phenotying Outcomes Drugs vs surgery Imaging
Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 )
 Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Percutaneous Humeral Fracture Repair Surgical Technique
 Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
Percutaneous Humeral Fracture Repair Surgical Technique Percutaneous Pinning Percutaneous Humeral Fracture Repair Closed reduction followed by percutaneous fixation reduces risk from soft tissue dissection
clinical article J Neurosurg 126: , 2017
 clinical article J Neurosurg 126:391 396, 2017 Prognostic ability of intraoperative electromyographic monitoring during microvascular decompression for hemifacial spasm to predict lateral spread response
clinical article J Neurosurg 126:391 396, 2017 Prognostic ability of intraoperative electromyographic monitoring during microvascular decompression for hemifacial spasm to predict lateral spread response
25/06/2010. Scaricato da 1
 Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
Neurosurgical treatment of glossopharyngeal neuralgia: analysis of 103 cases
 clinical article J Neurosurg 124:1088 1092, 2016 Neurosurgical treatment of glossopharyngeal neuralgia: analysis of 103 cases Yi Ma, MD, Yan-feng Li, MM, Quan-cai Wang, MM, Bin Wang, MM, and Hai-tao Huang,
clinical article J Neurosurg 124:1088 1092, 2016 Neurosurgical treatment of glossopharyngeal neuralgia: analysis of 103 cases Yi Ma, MD, Yan-feng Li, MM, Quan-cai Wang, MM, Bin Wang, MM, and Hai-tao Huang,
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
1 Tentorial Meningiomas Francesco Signorelli
 Meta data Explanation Please review proofs carefully for typographical and factual errors only; mark corrections in the file using the discretion. Please read your chapter carefully to confirm that no
Meta data Explanation Please review proofs carefully for typographical and factual errors only; mark corrections in the file using the discretion. Please read your chapter carefully to confirm that no
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Delayed hemorrhage after microvascular decompression in a hemifacial spasm patient associated with neurosyphilis
 Neurology Asia 2017; 22(4) : 357 362 Delayed hemorrhage after microvascular decompression in a hemifacial spasm patient associated with neurosyphilis * 1 Ji-Qing Qiu PhD, * 2 Yu Cui MD, 3 Li-Chao Sun MD,
Neurology Asia 2017; 22(4) : 357 362 Delayed hemorrhage after microvascular decompression in a hemifacial spasm patient associated with neurosyphilis * 1 Ji-Qing Qiu PhD, * 2 Yu Cui MD, 3 Li-Chao Sun MD,
Constantin Tuleasca, Romain Carron, Noémie Resseguier, Anne Donnet, P Roussel, Jean Gaudart, Marc Levivier, Jean Régis. To cite this version:
 Decreased Probability of Initial Pain Cessation in Classic Trigeminal Neuralgia Treated With Gamma Knife Surgery in Case of Previous Microvascular Decompression: A Prospective Series of 45 Patients With
Decreased Probability of Initial Pain Cessation in Classic Trigeminal Neuralgia Treated With Gamma Knife Surgery in Case of Previous Microvascular Decompression: A Prospective Series of 45 Patients With
Neurosurgery Sample Case
 120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
120 Beulah Road, NE, Suite 200 Vienna, Virginia 22180 Toll Free: 800-336-0332 Fax: 703-255-6134 www.malpracticeexperts.com Neurosurgery Sample Case The patient had an intra-cerebral artery aneurysm operated
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Trigeminal Neuralgia > 1
 Trigeminal Neuralgia Overview Trigeminal neuralgia is an inflammation of the trigeminal nerve causing extreme pain and muscle spasms in the face. Attacks of intense, electric shock-like facial pain can
Trigeminal Neuralgia Overview Trigeminal neuralgia is an inflammation of the trigeminal nerve causing extreme pain and muscle spasms in the face. Attacks of intense, electric shock-like facial pain can
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
SYNTHECEL Dura Repair. Assurance and Versatility for Dura Reconstruction.
 SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
Temporal Bone Magnetic Resonance Imaging Study in Hemifacial Spasm
 Temporal Bone Magnetic Resonance Imaging Study in Hemifacial Spasm Sun Kon Kim, M.D., Jin Ho Kim, M.D., Jin Woo Yang, M.D., Hyun Jeong Lee, M.D., Tae Sub Cheong, M.D.*, Young Ho Sohn, M.D., Jin-Soo Kim,
Temporal Bone Magnetic Resonance Imaging Study in Hemifacial Spasm Sun Kon Kim, M.D., Jin Ho Kim, M.D., Jin Woo Yang, M.D., Hyun Jeong Lee, M.D., Tae Sub Cheong, M.D.*, Young Ho Sohn, M.D., Jin-Soo Kim,
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
AcUMEDr. LoCKING CLAVICLE PLATE SYSTEM
 AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
AcUMEDr LoCKING CLAVICLE PLATE SYSTEM LoCKING CLAVICLE PLATE SYSTEM Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients.
Untangling Cerebral Dural Arteriovenous Fistulas
 Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Literature Review: Neurosurgery
 NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
