Microvascular decompression of cranial nerves: lessons learned after 4400 operations
|
|
|
- Alexis Johnston
- 5 years ago
- Views:
Transcription
1 J Neurosurg 90:1 8, 1999 Microvascular decompression of cranial nerves: lessons learned after 4400 operations MARK R. MCLAUGHLIN, M.D., PETER J. JANNETTA, M.D., BRENT L. CLYDE, M.D., BRIAN R. SUBACH, M.D., CHRISTOPHER H. COMEY, M.D., AND DANIEL K. RESNICK, M.D. Department of Neurological Surgery, University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania Object. Microvascular decompression has become an accepted surgical technique for the treatment of trigeminal neuralgia, hemifacial spasm, glossopharyngeal neuralgia, and other cranial nerve rhizopathies. The senior author (P.J.J.) began performing this procedure in 1969 and has performed more than 4400 operations. The purpose of this article is to review some of the nuances of the technical aspects of this procedure. Methods. A review of 4415 operations shows that numerous modifications to the technique of microvascular decompression have occurred during the last 29 years. Of the 2420 operations performed for trigeminal neuralgia, hemifacial spasm, and glossopharyngeal neuralgia before 1990, cerebellar injury occurred in 21 cases (0.87%), hearing loss in 48 (1.98%), and cerebrospinal fluid (CSF) leakage in 59 cases (2.44%). Of the 1995 operations performed since 1990, cerebellar injuries declined to nine cases (0.45%), hearing loss to 16 (0.8%), and CSF leakage to 37 (1.85% p 0.01, test for equality of distributions). The authors describe slight variations made to maximize surgical exposure and minimize potential complications in each of the six principal steps of this operation. These modifications have led to decreasing complication rates in recent years. Conclusions. Using the techniques described in this report, microvascular decompression is an extremely safe and effective treatment for many cranial nerve rhizopathies. KEY WORDS microvascular decompression trigeminal neuralgia hemifacial spasm glossopharyngeal nerve V J. Neurosurg. / Volume 90 / January, 1999 ASCULAR arterial contacts with the dorsal root of the trigeminal nerve were first described in 1929 by Dandy. 5 Although he characterized these findings in subsequent communications, 4,6 it was not until the 1950s that Gardner and Miklos 8 and Taarnhøj 12 reported the beneficial effects of decompressing the trigeminal nerve for tic douloureux. Similar observations of vascular compression of the seventh cranial nerve in patients with hemifacial spasm were first reported by Campbell and Keedy 3 in 1947 and by Laine and Nayrac 10 in Gardner and Sava 9 later extended these descriptions and proposed decompression of the facial nerve for hemifacial spasm in Despite these seminal observations, it took another 10 to 15 years before microvascular decompression became an accepted treatment for cranial nerve syndromes. Early posterior fossa surgery was performed without the aid of magnification or adequate lighting and produced high rates of morbidity and mortality. Initially, procedures were performed with the patient prone, with planned partial or complete nerve section. Over the years, the goals of the operation changed and technological advances, combined with surgical innovations, helped to make this procedure safer and more effective. We review the senior author s (P.J.J.) 29 years of experience in performing this operation, and we detail many of the technical aspects that have contributed to minimize complications. We propose a six-step method of performing microvascular decompression and describe six surgical pearls that make this operation safer and more effective. Important modifications of the initial procedure include patient positioning and the overall goal of surgery. The patient is now surgically treated while in the lateral or park-bench position, and the goal of the surgery is nerve decompression rather than nerve section. Such modifications, in addition to many others described herein, have greatly reduced the attendant risks of operative morbidity and have improved outcome. Operative Technique Step 1. Positioning of the Patient Vertex position dictates cranial nerve exposure (P.J.J.). It has been said that the most important part of a surgical procedure occurs before the skin incision, and much of the ease or difficulty of the microvascular decompression procedure is determined by patient positioning. The patient is placed on the operating room table with the head at the foot of the bed to maximize the surgeon s comfort 1
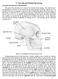
2 M. R. McLaughlin, et al. FIG. 1. Upper: Drawing showing the patient s head placed at the foot of the operating table to allow more leg room for the surgeon during the microsurgical portion of the procedure. The head is secured with three-point fixation and the patient is turned in the lateral decubitus position. The head is rotated slightly away from the affected side and flexed to approximately two finger breadths from the sternum. Lower: Drawings showing how the angle of the vertex is tailored depending on the cranial nerve approach. For trigeminal or cochlear nerve approaches, the vertex of the head is kept parallel to the floor to keep the seventh eighth nerve complex at a more inferior position with respect to the trigeminal nerve. For a seventh or lower cranial nerve approach, the vertex is dropped 15 toward the floor to rotate and expose the proximal aspect of the seventh nerve and to rotate the vestibulocochlear complex more cephalad. during the microsurgical portion of the procedure. Following induction of anesthesia and intubation, a threepoint head-fixation device is applied and the patient is placed in the lateral decubitus position with appropriate padding of pressure points and an axillary roll. The neck is flexed slightly with the chin approximately two finger breadths from the sternum (Fig. 1 upper). The head is rotated approximately 10 away from the affected side. If a trigeminal or cochlear approach is planned, the vertex is kept parallel to the floor to keep the seventh eighth cranial nerve complex at a more inferior position in relation to the trigeminal nerve. If a facial nerve or lower brainstem approach is planned, the vertex is dropped 15 toward the floor to expose the proximal aspect of the seventh nerve and rotate the vestibulocochlear complex more cephalad (Fig. 1 lower). The head holder is secured in the proper position. The patient is taped securely to the table at the hips and chest to allow rotation of the table during the operation. Finally, the patient s shoulder is taped down and placed out of the way. Step 2. Surgical Incision The placement of the incision is variable depending on the size and thickness of the patient s neck (P.J.J.). A 3 3 cm area behind the ear is shaved and bone landmarks are identified by palpation before the patient is prepared for surgery. The mastoid eminence, digastric groove, and inion should be identified and an iniomeatal line drawn to define the transverse sinus. Laterally, over the digastric groove a second line is drawn. The intersection of these lines reveals the junction of the transverse and sigmoid sinuses. This allows the surgeon a mind s eye view of optimal burr hole placement. These external landmarks guide the surgeon to minimize the length of the incision and to allow adequate exposure for burr hole placement (Fig. 2 upper). A vertical incision is drawn 3 to 5 cm long, approximately 0.5 cm posterior (medial) and parallel to the hair line. Identical incisions are used for both upper and lower cranial nerve exposures. A slightly shorter incision is required for thin- and long-necked patients. For short- and thick-necked patients, the incision should be slightly longer with the inferior aspect angled more posteriorly (medially). This angled incision requires slightly more extensive muscle dissection over the mastoid and digastric groove, but positions the thicker neck musculature posteriorly (medially), allowing freer movement of the surgeon s hands and instruments while performing the microsurgery (Fig. 2 lower). Three-quarters of the incision should be drawn inferior to the junction of the transverse and sigmoid sinuses and one-quarter should be above. The area is prepared and draped in the usual fashion and the incision is made down to the occipital bone by using monopolar cautery. The soft tissues are dissected using a periosteal elevator and electrocautery where necessary. The initial periosteal dissection should proceed anteriorly (laterally) before completing the posterior (medial) dissection. This provides better fixation with the Weitlaner retractor. The anterior (lateral) and inferior aspects of the mastoid eminence must be cleared of soft tissue. The nuchal muscles are dissected with electrocautery and the transverse occipital artery is identified, ligated, and divided. The mastoid emissary vein is usually identified and must be waxed in its fossa. An angled Weitlaner cerebellar retractor is put in place. In thin-necked patients a straight Weitlaner retractor often gives adequate exposure and takes up less room within the incisional opening. Step 3. Bone Removal The junction of the transverse and sigmoid sinuses must be visualized before the dural opening (P.J.J.). Before burr hole placement, bone landmarks should be well exposed. The digastric groove should be clearly visualized and the soft tissue should be dissected slightly anterior to this landmark. Often the external aspect of the emissary vein does not lie directly over the sinus; rather, the vein meanders in a rostrolateral direction before entering the proximal sigmoid sinus. Therefore, the mastoid emissary vein is a good landmark for the underlying junction of the transverse and sigmoid sinuses. The asterion location is variable and, thus, is not a reliable landmark for the sinus junction. 7 The burr hole should be placed over 2 J. Neurosurg. / Volume 90 / January, 1999
3 Microvascular decompression complication avoidance FIG. 3. Drawing depicting how bone exposure should demonstrate the junction of the transverse and sigmoid sinuses. Surgical exposure can then be tailored according to the cranial nerve approach desired. sinuses to allow a direct corridor along the petro-tentorial bone. The bone work must be anterior (lateral) enough (usually into mastoid air cells) to allow dural incision and reflection. FIG. 2. Upper: Drawing depicting how the intersection of the digastric groove and the iniomeatal line defines the junction of the transverse and sigmoid sinuses. With a mind s eye view of optimal burr hole placement and craniectomy, an incision is drawn centered over the planned craniectomy. Lower: Drawings showing different surgical incisions based on the size of the patient s neck. Short and thick necked patients require a more posteriorly (medially) directed incision. This angled incision positions the thicker neck musculature more posteriorly (medially) and out of the operative field. This small adjustment is critical in allowing freer movement of the surgeon s hands and instruments while performing the microsurgery. the mastoid emissary vein by using a perforator or highspeed drill. The goal of bone exposure should be to identify the edge of the junction of the transverse and sigmoid sinuses first. A small craniectomy can then be tailored according to the cranial nerve approach desired (Fig. 3). For a trigeminal or cochlear nerve approach, the craniectomy should be shaped as an isosceles triangle with the apex at the junction of the transverse and sigmoid sinuses. For a facial or lower cranial nerve approach, the apex of the triangle should be at the edge of the jugular bulb. It is important to remove a portion of the posterior mastoid air cells and to bevel the craniectomy outward so that no bone overhang will limit the dural opening. Mastoid air cells should be thoroughly waxed. Either a curvilinear or T-shaped incision is made in the dura mater. This incision must expose the most superior and lateral corner of the dura adjacent to the junction of the transverse and sigmoid J. Neurosurg. / Volume 90 / January, 1999 Step 4. Turning the Corner Turning the corner is the most dangerous stage of the operation and must be executed with patience and the utmost care (P.J.J.). After the dura is sutured back, an operative microscope with a 250-mm objective lens is brought into the field. Turning the corner or exposing the cerebellopontine angle may be difficult and hazardous. The surgeon should allow some drainage of cerebrospinal fluid (CSF) before placing the microretractor. Occasionally, gentle advancement of a cottonoid with a rubber dam is required to drain CSF from the cerebellopontine angle before placement of a retractor. All cottonoids are moistened with saline and are paired with an appropriately sized (0.5 2 in) piece of latex cut from a sterile glove. The latex prevents adhesion to the cerebellum and allows easy advancement of cottonoids medially to the cerebellopontine angle. If there is adequate CSF egress, a lumbar drain is not necessary. After the CSF has been drained, the cerebellum should begin to fall away from the petro-tentorial junction. A tapered retractor blade, bent proximally to a 60 angle, is placed over the previously placed rubber dam/cottonoid combination. The retractor should be no longer than necessary (approximately 6 in) because an overly prominent retractor can be bumped accidentally. For trigeminal and cochlear nerve approaches, the blade and cottonoid are placed over the superolateral aspect of the cerebellar surface and the ala of the cerebellum is gently elevated. The goal of retraction for all approaches in this region is always to elevate the cerebellum slightly toward the surgeon and not simply to compress it medially. This facilitates more CSF drainage, thereby minimizing the need for cerebellar retraction. The petrosal vein complex is identified and placed on gentle traction with the retractor. Using microbipolar electrocautery, the vein complex is coagulated and partially divided to verify adequate hemostasis. The complex is then coagulated a sec- 3
4 M. R. McLaughlin, et al. FIG. 4. Drawing showing how, in the event of inadvertent petrosal vein avulsion, bleeding can be controlled by gentle pressure and packing of the tentorial side using Surgicel covered with a cottonoid. The retractor can be used for placing gentle pressure on the cottonoid and Surgicel while the surgeon looks for the free end of the avulsed vein. ond time and cut completely. On entering the cerebellopontine angle, the first structure visualized will be the seventh eighth nerve complex, located superficially and caudal to the trigeminal nerve. The trigeminal nerve is located in the most superior and deepest position. The petrosal vein complex usually consists of a confluence of two or three veins draining into the tentorial edge. If bleeding is encountered from this complex, it may be torrential. Occasionally, this can even occur from gentle cerebellar retraction before division of the vein. Bleeding can be controlled by gentle pressure and packing of the tentorial side by using Surgicel and a cottonoid. The retractor can be used to exert gentle pressure while the surgeon looks for the free end of the avulsed vein (Fig. 4). Once the avulsed vein is identified and coagulated, the procedure can continue. If bleeding is severe, a large bore suction tip can be used to allow visualization of the field. Additionally, placing the patient in the reverse Trendelenburg position will decrease venous pressure and bleeding. In the senior author s experience, bleeding can always be controlled, but it may require tamponade for as long as 10 to 30 minutes. For seventh nerve or lower cranial nerve decompressions, an inferior approach is required. The retractor blade is placed over the rubber dam and cottonoid on the inferolateral aspect of the cerebellum and the cerebellar tonsils are gently elevated. The cisterna magna is identified and opened with a bent 25-gauge needle or microscissors. After adequate CSF drainage, the ninth, 10th, and 11th cranial nerves are identified as they enter the jugular foramen. Slightly more superiorly, the seventh eighth nerve complex can be seen. Step 5. Nerve Decompression The pathology lies at the brainstem side of the nerve, but may be more lateral (P.J.J.). Decompression is relatively straightforward if the surgeon keeps two principles in mind at all times: 1) there must be a vessel, and it is my job to find it ; and 2) the FIG. 5. Diagram showing that the dorsal root entry zone of the trigeminal nerve can be variable in length and may extend to a more distal portion of the nerve. dorsal root entry or exit zone can be variable in length, particularly in the case of the trigeminal nerve, and may extend to a more distal portion of the nerve. Therefore, the nerve should be inspected from its origin at the brainstem laterally to its exit from the cerebellopontine angle and all vessels should be treated (Fig. 5). Microvascular decompression of the trigeminal nerve requires sharp dissection of all arachnoid around the trigeminal nerve and superior cerebellar artery. The most common vessel found is a rostroventral superior cerebellar artery loop, which compresses the trigeminal nerve either at the brainstem or distally (Fig. 6). After the arachnoid is dissected and the vessel is freed, the loop can be mobilized to the lateral aspect of the nerve, and a piece of shredded Teflon felt can be placed between the vessel and the nerve (Fig. 7). The most frequent vessel found compressing the cochlear or vestibular nerve is an anterior inferior cerebellar artery loop. Arachnoid dissection in this area requires sharp dissection of the flocculus from the vestibular nerve. This dissection is necessary to visualize the dorsal root entry zone. Changes in the brainstem evoked response (BSER) observed during this part of the procedure are frequently due to traction on the eighth cranial nerve. If BSER changes occur, the retractor should be relaxed somewhat and the surgeon should pause and await return of the BSERs. Frequent visualization of the retractor is paramount because it has a tendency to slip. Unnoticed slips in the retractor may cause rapid and possibly, irreversible damage to the cochlear nerve. Less frequently, decompression of a vessel loop causes impingement on the cochlear nerve and requires manipulation to prevent hearing loss. The facial nerve commonly receives inadequate decompression because of poor exposure of the nerve. This is usually related to improper positioning of the vertex of the head before opening and inadequate inferolateral bone exposure. If the vertex is positioned 15 downward and a wide inferolateral exposure is obtained, the dorsal root exit zone and intrapontine portions of the facial nerve are easily visualized and may be adequately decompressed. The most common vessel causing compression of the facial nerve is the posterior inferior cerebellar artery. This 4 J. Neurosurg. / Volume 90 / January, 1999
5 Microvascular decompression complication avoidance FIG. 6. Drawing of the most common vessel found causing typical trigeminal neuralgia, a rostroventral superior cerebellar artery loop, which compresses the trigeminal nerve either at the brainstem or distally. vessel must be sharply dissected free from the arachnoid and mobilized laterally away from the nerve so that a Teflon implant can be placed. In cases of atypical hemifacial spasm, the pathological vascular entity is almost always located rostral to the nerve or between the seventh and eighth nerves. An anterior inferior cerebellar artery running between the seventh and eighth nerve may have a perforating branch to the pons that must be preserved. Exposure of the lower cranial nerves and lateral medulla oblongata is excellent with inferolateral placement of the retractor. The arachnoid is dissected sharply and the pathological vascular entity can be identified and treated appropriately. Step 6. Surgical Closure Wax the bone edges on the way in and on the way out (P.J.J.). At the conclusion of the decompression procedure, several Valsalva maneuvers are performed to ensure hemostasis. The retractor is then removed and the cerebellar surface is carefully inspected. Valsalva maneuvers are repeated to verify hemostasis. The area is gently irrigated with warm saline bulb irrigation and the durotomy is closed. Syringe irrigation is to be avoided because it may injure the cochlear nerve with a jet of fluid. We are aggressive in performing dural closure in which fascia/muscle grafts from the inferior portion of the incision are used as necessary to ensure watertight closure. The bone edges of the mastoid air cells are thoroughly waxed for a second time. A small pad of cellulose and Gelfoam are then placed over the durotomy, and cranioplasty is performed using methylmethacrylate or wire mesh. The deep and superficial muscles are approximated with interrupted No. 2.0 absorbable sutures, and the fascia is closed with the same type of sutures. The fascial closure must be watertight to prevent any CSF leakage. Interrupted sutures lend strength to the fascial closure. A second Valsalva maneuver may reveal further egress of CSF through the fascia, necessitating reinforcement of the closure. The subcutaneous tissues are approximated with No. 3.0 interrupted absorbable sutures. A well-approximated subcutaneous layer can also afford protection from CSF leakage. The J. Neurosurg. / Volume 90 / January, 1999 skin is closed with No. 4.0 nylon sutures in a running locked fashion with care taken not to impair the vascular supply to the incision by excessive tension on the skin suture. Postoperative care includes routine overnight observation in the neurosurgical continuous care unit. It is important to monitor blood pressure carefully and to treat hypertension (systolic blood pressure 160 mm Hg) aggressively. We routinely use invasive arterial pressure monitoring in the perioperative period. Intravenous antiemetic medications are administered liberally to minimize postoperative nausea and emesis. Early mobilization of our patients is encouraged, beginning on postoperative Day 1. Provided the postoperative course is uneventful, patients are discharged at 72 hours and frequently at 48 hours. Most patients have some degree of frontal headache or incision pain; however, the presence of severe headache unresponsive to low-dosage narcotic medications necessitates obtaining a computerized tomography scan to rule out hemorrhage. If the scan is negative for hemorrhage we routinely perform a lumbar puncture and drain CSF until the closing pressure is equal to one-half of the opening pressure. We have found that many postoperative headaches are due to temporarily high opening pressures and are definitively treated with one or, rarely, two lumbar punctures performed during the postoperative period. Complication Avoidance We chose to examine trends over time with respect to the three complications thought to be directly related to operative technique during microvascular decompression. The complications evaluated were cerebellar injury, hearing loss, and CSF leakage. These three complications are by no means comprehensive, but are easily defined and determined objectively through routine postoperative clinical, radiographic, and neurophysiological evaluations. Other rare complications of the procedures, such as facial weakness or anesthesia, lower cranial nerve dysfunction, or recurrent symptoms, were not evaluated because of their relative infrequency and because they have been reported in detail in previous communications. 1,2,11 By evaluating cerebellar injury, hearing loss, and CSF leakage, decreases in their occurrence could be detected in operations performed since Of the 4415 operations performed for trigeminal neuralgia, hemifacial spasm, or glossopharyngeal neuralgia performed since 1972, there have been 30 cerebellar injuries (0.68%), 64 hearing deficits (1.45%), and 96 CSF leaks (2.17%) (Table 1). When operations performed before 1990 were compared with those performed since 1990, we found that these rates have decreased. The largest decline was in hearing loss (1.98% compared with 0.8%, p 0.01; test for equality of distributions, Table 1). Although BSERs were used before 1990, the rate of hearing loss includes many operations performed early in our series when use of BSERs was experimental. Thus, use of intraoperative BSERs appears to have contributed significantly to the observed decline in postoperative hearing deficits. Other factors have also contributed to this decline. Hearing loss did not occur following decompression of 5
6 M. R. McLaughlin, et al. FIG. 7. Diagrams depicting how dissection and mobilization of the arterial loop depend on the anatomy of compression. This figure demonstrates the microsurgical movements that are performed when a typical superior cerebellar artery loop is found compressing the trigeminal nerve. The concepts of Teflon felt placement and proximal-to-distal sweeping movements of the felt along the nerve apply for lower cranial nerve decompressions as well. A: Before the vessel can be moved, the arachnoid must be sharply dissected over the entire length of the loop proximally and distally. B: After the vessel is freed, the vascular loop is lifted off the brainstem at the rostral aspect of the nerve and a medium-sized cigar-shaped piece of Teflon felt is placed between the vessel and the nerve. It is very important to position the distal portion of the felt with the tips of the forceps. The Teflon felt should not be pushed into position by holding its proximal portion. C: After the Teflon felt is placed under the loop, the pledget is gently pushed in a proximal-to-distal fashion along the nerve toward Meckel s cave. This movement elevates the arterial loop and causes it to begin to rotate outward from the ventral surface of the nerve. D: A second Teflon felt, approximately the same size, is placed where the first felt was originally positioned. Using the same proximal-to-distal sweeping motion, the felt should be advanced over the length of the nerve toward Meckel s cave. E: As the Teflon pledgets are advanced, the vascular loop progressively rotates from the ventral aspect of the nerve to the dorsal side. F: A third Teflon pledget is placed where the first felt was originally positioned and, again, a proximal-to-distal sweeping movement along the trigeminal nerve flips the vascular loop to the dorsal aspect of the nerve. G: After the vascular loop is flipped to the dorsal surface of the nerve, pledgets are placed between the vessel and the nerve. 6 J. Neurosurg. / Volume 90 / January, 1999
7 Microvascular decompression complication avoidance TABLE 1 Incidence of complications during microvascular decompression of cranial nerves Before 1990 Since 1990 Total Complications (2420 ops) (1995 ops) (4415 ops) cerebellar injury 21 (0.87%) 9 (0.45%) 30 (0.68%) eighth nerve injury 48 (1.98%) 16 (0.80%) 64 (1.45%) CSF leak 59 (2.44%) 37 (1.85%) 96 (2.17%) TABLE 2 Incidence of hearing loss following microvascular decompression of cranial nerves* Decom Before 1990 Since 1990 Total CN V 22 of 1659 (1.33%) 9 of 1537 (0.59%) 31 of 3196 (0.97%) CN VII 26 of 692 (3.76%) 6 of 377 (1.59%) 32 of 1069 (2.99%) CN IX/X 0 of 69 (0.0%) 0 of 81 (0.0%) 0 of 150 (0.0%) total 48 of 2420 (1.98%) 15 of 1995 (0.75%) 63 of 4415 (1.43%) * CN = cranial nerve; decom = decompression procedure. the ninth and 10th cranial nerve, and the rate after decompression of the fifth cranial nerve was much less than that observed after treatment of hemifacial spasm (Table 2). The approach turning the corner to the ninth and 10th nerves, discussed previously, involves elevation of the cerebellar tonsils and a corridor along the floor of the occiput. This places no retraction on the seventh eighth nerve complex. A common error is to approach the ninth and 10th nerves too superiorly, exposing the seventh and eighth nerves prematurely before moving inferior to the ninth and 10th nerves. This route requires retraction of the cerebellum at the level of the seventh and eighth cranial nerves, often before visualization of these structures. The same is true for decompression of the fifth cranial nerve. The seventh eighth nerve complex should not be approached directly with subsequent dissection moving superiorly to the fifth cranial nerve. The petrotentorial junction is the proper corridor to approach the fifth nerve and the seventh eighth nerve complex should have little tension from retraction. However, decompression of the fifth cranial nerve does require some retraction, which places tension on the seventh and eighth nerves and, hence, may lead to hearing loss. If during a fifth nerve decompression the BSERs begin to decline, it is often related to the tethering of the arachnoid to the seventh eighth nerve complex. When delays are encountered, the surgeon should continue sharp arachnoidal dissection down to, and slightly below, the seventh eighth nerve complex. This maneuver frequently will relieve the tension on the cochlear nerve and cause improvement in the BSERs. Decompression of the lower cranial nerves, however, places relatively little tension on the seventh eighth nerve complex and is, therefore, associated with a minimal risk of hearing loss (none in our series) (Table 2). Decompression of the seventh or eighth nerve should also be approached from above or below as described previously. This allows good visualization of the seventh and eighth nerves before retracting near their proximal origins. When BSERs change during the procedure, it is usually due to retraction. The first response of the surgeon should be to reduce or remove retraction, or at least change the position of the retractor. We have found this usually improves the BSERs. Constant surveillance of the retractor is imperative because it often shifts and is frequently only millimeters from the eighth cranial nerve. Occasionally the BSERs will change after decompression and is not corrected with alterations in retraction. In these cases, inspection of the entire length of the eighth nerve will often disclose impingement from a Teflon implant or displaced vessel. Appropriate alterations should then be made. Finally, a change in BSERs may occur on closure J. Neurosurg. / Volume 90 / January, 1999 of the dura. Although this happens very rarely, the dura should always be reopened. Opening the dura usually causes the BSERs to return to baseline. In this situation, reexploration of the decompression and the eighth cranial nerve will often disclose tension on the nerve from a Teflon pad or displaced vessels, which somehow worsens after the CSF is replaced and the dura is closed. Manipulation of any impingements on the eighth nerve and closure of the dura can then be safely completed. We have also observed that small amounts of blood or cold saline irrigation on the cochlear nerve may adversely affect BSERs. Cerebellar injuries, including hemorrhage and contusion, have also occurred with less frequency since 1990 (0.87% compared with 0.45%, p 0.01; Table 1). Limitation of the degree and duration of retraction remains essential in avoiding cerebellar injury. The entire decompression procedure (from skin incision to skin closure) generally takes less than 2 hours and requires only a small corridor of exposure between the cerebellum and petrous temporal bone. This corridor is kept to a minimum by adequate exposure of the sigmoid sinus by mastoid bone removal prior to durotomy. This allows a dural incision very close to the sigmoid sinus rather than a more posterior durotomy that requires more cerebellar retraction to permit visualization along the petrous temporal bone. We place rubber dams made from latex gloves on the cerebellar side of all cottonoids so that smooth gentle advancement can be performed. Also, the approach superiorly and inferiorly allows CSF drainage from cisterns prior to significant retraction. An approach that leads straight in requires more cerebellar tissue to be retracted and exposes the seventh eighth nerve complex, rather than a CSF cistern, which can allow further relaxation of the cerebellum. Avoidance of CSF leaks remains problematic after transgression of mastoid air cells and exposure of multiple overlapping tissue planes. Our incidence of CSF leaks has declined since 1990 from 2.44% to 1.85% (p 0.01). Mastoid air cells are frequently opened to obtain adequate visualization of the margin of the sigmoid sinus. Copious amounts of bone wax should be applied before durotomy and after dural closure. The nuchal musculature does not extend above the digastric groove. Therefore, good surgical technique should be applied and the muscular layers approximated before fascial closure. Care should be taken not to include the galea in the deep muscle closure at the inferior aspect of the wound, so that a single layer of fascia is left to close along the entire length of the incision. This should be closed with interrupted sutures. An inverted, interrupted No. 3.0 absorbable closure of the subcuta- 7
8 M. R. McLaughlin, et al. neous tissues should also be watertight and should not be placed until a Valsalva maneuver reveals a watertight galeal closure. Postoperative CSF leaks usually resolve with lumbar drainage, although a minority of cases require operative intervention including reexploration of the dural closure and careful inspection of the mastoid air cells. Conclusions Since the inception of microvascular decompression, the procedure has undergone changes designed to improve safety and efficacy. Implementation of neurophysiological monitoring and meticulous attention to the microsurgical anatomy of the posterior fossa have improved complication rates for cerebellar injury and hearing loss to less than 1%. We believe this six-step approach, combined with the surgical wisdom gained from more than 4400 procedures, remains the key to successful outcomes. References 1. Barker FG II, Jannetta PJ, Bissonette DJ, et al: The long-term outcome of microvascular decompression for trigeminal neuralgia. N Engl J Med 334: , Barker FG II, Jannetta PJ, Bissonette DJ, et al: Microvascular decompression for hemifacial spasm. J Neurosurg 82: , Campbell E, Keedy C: Hemifacial spasm: a note on the etiology in two cases. J Neurosurg 4: , Dandy WE: Concerning the cause of trigeminal neuralgia. Am J Surg 24: , Dandy WE: An operation for the cure of tic douloureux. Partial section of the sensory root at the pons. Arch Surg 18: , Dandy WE: The treatment of trigeminal neuralgia by the cerebellar route. Ann Surg 96: , Day JD, Tschabitscher M: Anatomic position of the asterion. Neurosurgery 42: , Gardner WJ, Miklos MV: Response of trigeminal neuralgia to decompression of the sensory root. Discussion of cause of trigeminal neuralgia. JAMA 170: , Gardner WJ, Sava GA: Hemifacial spasm a reversible pathophysiologic state. J Neurosurg 19: , Laine E, Nayrac P: Hemispasme facial guéri par intervention sur la fossa postérieure. Rev Neurol 80:38 40, Resnick DK, Jannetta PJ, Bissonnette D, et al: Microvascular decompression for glossopharyngeal neuralgia. Neurosurgery 36:64 69, Taarnhøj P: Decompression of the trigeminal root and the posterior part of the ganglion as treatment in trigeminal neuralgia. Preliminary communication. J Neurosurg 9: , 1952 Manuscript received April 14, Accepted in final form September 8, Address reprint requests to: Peter J. Jannetta, M.D., Department of Neurological Surgery, University of Pittsburgh Medical Center, 200 Lothrop Street, Suite B-400 PUH, Pittsburgh, Pennsylvania J. Neurosurg. / Volume 90 / January, 1999
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Fleece-Bound Tissue Sealing in Microvascular Decompression
 DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY
 NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
NIDCD NATIONAL TEMPORAL BONE, HEARING AND BALANCE PATHOLOGY RESOURCE REGISTRY Guidelines for Removal of Temporal Bones for Pathological Study The temporal bones should be removed as soon as possible. If
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE
 Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
In Situ Fusion L5 to S1
 Chapter 2 In Situ Fusion L5 to S1 Stuart L. Weinstein, M.D. DIAGNOSIS Spondylolisthesis COMMON INDICATIONS n In symptomatic low grade Spondylolysis and listhesis of less than 30 % n Pain unresponsive to
Chapter 2 In Situ Fusion L5 to S1 Stuart L. Weinstein, M.D. DIAGNOSIS Spondylolisthesis COMMON INDICATIONS n In symptomatic low grade Spondylolysis and listhesis of less than 30 % n Pain unresponsive to
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM
 INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
INTRAOPERATIVE NEUROPHYSIOLOGICAL MONITORING FOR MICROVASCULAR DECOMPRESSION SURGERY IN PATIENTS WITH HEMIFACIAL SPASM WILLIAM D. MUSTAIN, PH.D., CNIM, BCS-IOM DEPARTMENT OF OTOLARYNGOLOGY AND COMMUNICATIVE
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
Brain ميهاربا لض اف دمح ا د The Meninges 1- Dura Mater of the Brain endosteal layer does not extend meningeal layer falx cerebri tentorium cerebelli
 .احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
.احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
Surgical Anatomy of the Hip. Joseph H. Dimon
 Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
Surgical Anatomy of the Hip Joseph H. Dimon The hip joint is a deep joint surrounded by large and powerful muscles necessary for its proper function. Essential neurovascular structures lie in front and
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
The translabyrinthine approach has been
 OPERATIVE NUANCES TRANSLABYRINTHINE APPROACH FOR ACOUSTIC NEUROMA John Diaz Day, M.D. Department of Neurosurgery, Drexel University College of Medicine, Philadelphia, Pennsylvania, and Allegheny General
OPERATIVE NUANCES TRANSLABYRINTHINE APPROACH FOR ACOUSTIC NEUROMA John Diaz Day, M.D. Department of Neurosurgery, Drexel University College of Medicine, Philadelphia, Pennsylvania, and Allegheny General
H emifacial spasm (HFS) is an infrequent disorder with
 1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... J Neurol Neurosurg Psychiatry 2005;76:1574 1580. doi: 10.1136/jnnp.2004.056861
1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... J Neurol Neurosurg Psychiatry 2005;76:1574 1580. doi: 10.1136/jnnp.2004.056861
H emifacial spasm (HFS) is an infrequent disorder with
 1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... See end of article for authors affiliations... Correspondence to: Dr Amin Kassam,
1574 PAPER Repeat microvascular decompression for hemifacial spasm J A Engh, M Horowitz, L Burkhart, Y-F Chang, A Kassam... See end of article for authors affiliations... Correspondence to: Dr Amin Kassam,
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve
 Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve Pages with reference to book, From 140 To 143 Nawab Mohammad Khan, Mohammad Afzal Khan, Fazal Karim Aasi ( Department
Neuro Vascular Relationship between Superior Cerebellar Artery and Trigeminal Nerve Pages with reference to book, From 140 To 143 Nawab Mohammad Khan, Mohammad Afzal Khan, Fazal Karim Aasi ( Department
Table of Contents: CARPAL TUNNEL RELEASE SURGICAL TECHNIQUE Knife Assembly... Page 6 VERSION 2.2
 www.s2ssurgical.com Table of Contents: Preparation... Page 1 Dissection... Page 2 Tunneling... Page 3 Release... Page 4 Closure... Page 6 Knife Assembly... Page 6 CARPAL TUNNEL RELEASE SURGICAL TECHNIQUE
www.s2ssurgical.com Table of Contents: Preparation... Page 1 Dissection... Page 2 Tunneling... Page 3 Release... Page 4 Closure... Page 6 Knife Assembly... Page 6 CARPAL TUNNEL RELEASE SURGICAL TECHNIQUE
be very thin and variable. Facial nerve branches that exit the parotid gland are deep to the SMAS.
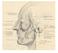 The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
The Superficial musculoaponeurotic system (SMAS) fascia is a fanlike fascia that envelops the face and provides a suspensory sheet which distributes forces of facial expression.. The SMAS is continuous
BICEPTOR Tenodesis System
 BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
BICEPTOR Tenodesis System Sub-Pectoral Biceps Tenodesis A Shoulder Series Technique Guide As described by: Nikhil N. Verma, MD As described by: Nikhil N. Verma, MD Midwest Orthopedics at Rush Chicago,
Extracapsular Repair Monofilament Nylon Suture
 Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Extracapsular Repair Monofilament Nylon Suture Management of the ruptured Cranial Cruciate Ligament (CCL) by placing a non-absorbable suture between the lateral fabella and the proximal, cranial tibia
Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach
 J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Modified Radical Mastectomy
 Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
Modified Radical Mastectomy Valerie L. Staradub, MD, and Monica Morrow, MD S urgical management options for breast cancer include modified radical mastectomy (MRM), MRM with immediate reconstruction, and
THE HUMERUS 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW
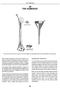 20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
20 THE HUMERUS* CROSS SECTION CROSS SECTION SUPERIOR VIEW The marrow canal of the humerus is funnel-shaped. Its successful pinning is influenced by many factors. With a few exceptions, the entire humerus
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
MIAA. Minimally Invasive Anterior Approach Surgical technique
 MIAA Minimally Invasive Anterior Approach Surgical technique Contents Introduction 3 With-Table MIAA technique 4 A1. Patient positioning/draping 4 A2. Skin incision 4 A3. Muscular dissection 4 A4. Muscle
MIAA Minimally Invasive Anterior Approach Surgical technique Contents Introduction 3 With-Table MIAA technique 4 A1. Patient positioning/draping 4 A2. Skin incision 4 A3. Muscular dissection 4 A4. Muscle
The Transtibial Amputation
 The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
The Transtibial Amputation Site of Previous Surgeries: Amputation indication: four unsuccessful previous surgeries. Patient experiences chronic pain and disfunction along with a limited range of motion.
OMT Without An OMT Table Workshop. Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP
 OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Integra. Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE
 Integra Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE Table of Contents Indications... 2 Contraindications... 2 System Description... 2 Features and Benefits... 2 Surgical Site Preparation...3
Integra Endoscopic Gastrocnemius Release System SURGICAL TECHNIQUE Table of Contents Indications... 2 Contraindications... 2 System Description... 2 Features and Benefits... 2 Surgical Site Preparation...3
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
US Patent No. 6,309,396B1. G. David Ritland, M.D.
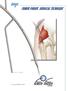 US Patent No. 6,309,396B1 G. David Ritland, M.D. The Femur Finder is designed to direct the guide wire into the medullary canal. Do not use it to manipulate the fracture fragments, reduce the fracture,
US Patent No. 6,309,396B1 G. David Ritland, M.D. The Femur Finder is designed to direct the guide wire into the medullary canal. Do not use it to manipulate the fracture fragments, reduce the fracture,
Open reduction; plate fixation 1 Principles
 Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
Executive Editor: Peter Trafton Authors: Martin Jaeger, Frankie Leung, Wilson Li Proximal humerus 11-A2 Open reduction, plate fixation Search search... Shortcuts All Preparations All Approaches All Reductions
THE ANGULAR TRACT: AN ANATOMICAL
 British Journal of Oral Surgery (1981) 19, 116-120 0 The British Association of Oral Surgeons 0007-117X/81/00170116$02.00 THE ANGULAR TRACT: AN ANATOMICAL OF SURGICAL SIGNIFICANCE STRUCTURE HAITHEM A.
British Journal of Oral Surgery (1981) 19, 116-120 0 The British Association of Oral Surgeons 0007-117X/81/00170116$02.00 THE ANGULAR TRACT: AN ANATOMICAL OF SURGICAL SIGNIFICANCE STRUCTURE HAITHEM A.
The Visible Ear Simulator Dissection Manual.
 The Visible Ear Simulator Dissection Manual. Stereoscopic Tutorialized Version 3.1, August 2017 Peter Trier Mikkelsen, the Alexandra Institute A/S, Aarhus, Denmark Mads Sølvsten Sørensen & Steven Andersen,
The Visible Ear Simulator Dissection Manual. Stereoscopic Tutorialized Version 3.1, August 2017 Peter Trier Mikkelsen, the Alexandra Institute A/S, Aarhus, Denmark Mads Sølvsten Sørensen & Steven Andersen,
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Lecture 4 The BRAINSTEM Medulla Oblongata
 Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Chapter 39. Volar surface incisions
 Chapter 39 EXPLORATION OF AN INJURED HAND OR FOREARM KEY FIGURES: Tourniquet Midlateral finger incisions Brunner zigzag incisions Volar surface incisions Dorsal incisions Proximal and distal extension
Chapter 39 EXPLORATION OF AN INJURED HAND OR FOREARM KEY FIGURES: Tourniquet Midlateral finger incisions Brunner zigzag incisions Volar surface incisions Dorsal incisions Proximal and distal extension
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Abdominal Wall Modification for the Difficult Ostomy
 Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
DEVELOPMENT OF BRAIN
 Ahmed Fathalla OBJECTIVES At the end of the lecture, students should: List the components of brain stem. Describe the site of brain stem. Describe the relations between components of brain stem & their
Ahmed Fathalla OBJECTIVES At the end of the lecture, students should: List the components of brain stem. Describe the site of brain stem. Describe the relations between components of brain stem & their
STAB INCISION GLAUCOMA SURGERY (SIGS)
 STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
STAB INCISION GLAUCOMA SURGERY (SIGS) Dr. Soosan Jacob, MS, FRCS, DNB Senior Consultant Ophthalmologist, Dr. Agarwal's Eye Hospital, Chennai, India dr_soosanj@hotmail.com Videos available in Youtube channel:
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990
 ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990 A 10 minutes transhumeral footprint repair using only sutures AIG Medical GmbH Bonn (Aeratec) Essential for this surgery
ARTHROSCOPIC GIANT NEEDLE ROTATOR CUFF REPAIR AS A ROUTINE PROCEDURE SINCE 1990 A 10 minutes transhumeral footprint repair using only sutures AIG Medical GmbH Bonn (Aeratec) Essential for this surgery
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
BP and Heart Rate by Telemetry
 BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
BP and Heart Rate by Telemetry Version: 1 Modified from: Butz et al. Physiol Genomics. 2001 Mar 8;5(2):89-97. Edited by: Dr. Lynette Bower, UC Davis Summary Reagents and Materials Protocol Reagent Preparation
Anatomy of. External NOSE. By Dr Farooq Aman Ullah Khan PMC
 Anatomy of External NOSE By Dr Farooq Aman Ullah Khan PMC 24 th Nov. 2017 The External Nose Descriptions of the nose always begin with that part of it which is covered by the skin, i.e., the EXPOSED PART
Anatomy of External NOSE By Dr Farooq Aman Ullah Khan PMC 24 th Nov. 2017 The External Nose Descriptions of the nose always begin with that part of it which is covered by the skin, i.e., the EXPOSED PART
1. Introduction: 3. Surgical Procedures. 2. Indications. 3.a. Surgical Instruments. 3.b. Patient Positioning. 3.c. Surgical Technique
 1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
1. Introduction: Luiz Pimenta M.D., Larry T. Khoo M.D. ANTERIOR MICROENDOSCOPIC DISCECTOMY AND FUSION FOR THE CERVICAL SPINE Minimally invasive spine surgery by means of an endoscopic technique has gained
Microvascular Decompression of the Vestibulocochlear Nerve
 JOURNAL OF CASE REPORTS 2015;5(1):182-186 Microvascular Decompression of the Vestibulocochlear Nerve Henry Emanuel, Zakier Hussain Department of Neurosurgery, Waikato Hospital, Hamilton, New Zealand. Abstract:
JOURNAL OF CASE REPORTS 2015;5(1):182-186 Microvascular Decompression of the Vestibulocochlear Nerve Henry Emanuel, Zakier Hussain Department of Neurosurgery, Waikato Hospital, Hamilton, New Zealand. Abstract:
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
Strattice Reconstructive Tissue Matrix used in the repair of rippling
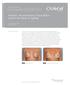 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
OHSU Neurological Surgery Education. Neurosurgical Basics. Copyright Oregon Health & Science University Department of Neurological Surgery
 OHSU Neurological Surgery Education Neurosurgical Basics Chapter 1 Basic Principles: Cranial Three-Point Head Fixation Proper and safe application of a three-point rigid cranial fixation device provides
OHSU Neurological Surgery Education Neurosurgical Basics Chapter 1 Basic Principles: Cranial Three-Point Head Fixation Proper and safe application of a three-point rigid cranial fixation device provides
STEP 1 INCISION AND ELEVATION OF SKIN FLAP STEP 3 SEPARATE PAROTID GLAND FROM SCM STEP 2 IDENTIFICATON OF GREAT AURICULAR NERVE
 STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
Zimmer MIS Mini-Incision THA Anterolateral Approach
 Zimmer MIS Mini-Incision THA Anterolateral Approach Retractor Placement Guide Optimizing exposure and preserving soft tissue during MIS THA Minimally invasive surgery allows you to follow the basic principles
Zimmer MIS Mini-Incision THA Anterolateral Approach Retractor Placement Guide Optimizing exposure and preserving soft tissue during MIS THA Minimally invasive surgery allows you to follow the basic principles
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Technique Guide. Bard MK Hernia Repair. Featuring Modified Onflex Mesh SOFT TISSUE REPAIR. Anterior Approach to a Preperitoneal Inguinal Hernia Repair
 Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Bard MK Hernia Repair Featuring Modified Onflex Mesh Technique Guide Anterior Approach to a Preperitoneal Inguinal Hernia Repair SOFT TISSUE REPAIR Right Procedure. Right Product. Right Outcome. The opinions
Veins that are firm to
 Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
3. The Jaw and Related Structures
 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
The supraclavicular approach to scalenectomy and first rib resection: Description of technique
 The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
The supraclavicular approach to scalenectomy and first rib resection: Description of technique Richard J. Sanders, M.D., and Susan Raymer, Denver, Colo. Supraclavicular first rib resection has been performed
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
OMT FOR CONCUSSIONS KIMBERLY WOLF, D.O. FEBRUARY 17, 2017
 OMT FOR CONCUSSIONS KIMBERLY WOLF, D.O. FEBRUARY 17, 2017 POTENTIAL SEQUENCE Address lymphatics including all transition zones/diaphragms Address somatic dysfunction in spine Focus on upper cervical spine
OMT FOR CONCUSSIONS KIMBERLY WOLF, D.O. FEBRUARY 17, 2017 POTENTIAL SEQUENCE Address lymphatics including all transition zones/diaphragms Address somatic dysfunction in spine Focus on upper cervical spine
Cranial Cavity REFERENCES: OBJECTIVES OSTEOLOGY. Stephen A. Gudas, PT, PhD
 Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.*
 Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Endoscopic Soft Tissue Release System. SafeViewTM 360 Panoramic Visualization Sterile Packaged Fully Disposable
 L O W E R E X T R E M I T Y T E C H N I Q U E G U I D E Endoscopic Soft Tissue Release System SafeViewTM 360 Panoramic Visualization Sterile Packaged Fully Disposable Versatility and Control SafeView is
L O W E R E X T R E M I T Y T E C H N I Q U E G U I D E Endoscopic Soft Tissue Release System SafeViewTM 360 Panoramic Visualization Sterile Packaged Fully Disposable Versatility and Control SafeView is
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM
 EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
This information is intended as an overview only
 This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
This information is intended as an overview only Please refer to the INSTRUCTIONS FOR USE included with this device for indications, contraindications, warnings, precautions and other important information
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
T HE direct surgical approach to an aneurysm on
 J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
J Neurosurg 66:500-505, 1987 Aneurysms of the basilar artery trunk KENICHIRO SUGITA, M.D., SHIGEAKI KOBAYASHI, M.D., TOSHIKI TAKEMAE, M.D., TSUYOSHI TADA, M.D., AND YUICHIRO TANAKA, M.D. Department of
Two types of posterior fossa veins are involved in. FOCUS Neurosurg Focus 45 (1):E2, 2018
 NEUROSURGICAL FOCUS Neurosurg Focus 45 (1):E2, 2018 Bridging veins and veins of the brainstem in microvascular decompression surgery for trigeminal neuralgia and hemifacial spasm Hiroki Toda, MD, PhD,
NEUROSURGICAL FOCUS Neurosurg Focus 45 (1):E2, 2018 Bridging veins and veins of the brainstem in microvascular decompression surgery for trigeminal neuralgia and hemifacial spasm Hiroki Toda, MD, PhD,
Perforating branches from ovending arteries in hemifacial spasm: anatomical correlation with vertebrobasilar configuration
 J Neurol Neurosurg Psychiatry 1999;67:73 77 73 Department of Neurosurgery, Nagoya University School of Medicine, Nagoya, Japan T Nagatani S Inao Y Suzuki J Yoshida Correspondence to: Dr T Nagatani, Department
J Neurol Neurosurg Psychiatry 1999;67:73 77 73 Department of Neurosurgery, Nagoya University School of Medicine, Nagoya, Japan T Nagatani S Inao Y Suzuki J Yoshida Correspondence to: Dr T Nagatani, Department
Meniscus cartilage replacement with cadaveric
 Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Technical Note Meniscal Allografting: The Three-Tunnel Technique Kevin R. Stone, M.D., and Ann W. Walgenbach, R.N.N.P., M.S.N. Abstract: This technical note describes an improved arthroscopic technique
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
