The diagnosis of lung cancer is often confirmed by
|
|
|
- Philip Craig
- 5 years ago
- Views:
Transcription
1 Original Articles Diagnostic Concordance of Histologic Lung Cancer Type Between Bronchial Biopsy and Cytology Specimens Taken During the Same Bronchoscopic Procedure Melanie K. Sackett, MD; Diva R. Salomão, MD; Janis L. Donovan, BS; Eunhee S. Yi, MD; Marie Christine Aubry, MD N Context. The diagnosis of lung cancer is often confirmed by cytology and biopsy specimens obtained during a bronchoscopic procedure. At our institution, these specimens are read by different pathologists, and the rate of concordance was not known. Objectives. To evaluate the concordance rate in the diagnosis of lung cancer types between cytology and biopsy specimens and to correlate discordance with patient outcome. Design. Specimens obtained during the same procedure, between January 1, 2000, and December 31, 2005, were identified. Cases with cytology and biopsy specimens positive for cancer were evaluated for concordance of histologic type, small cell versus non small cell lung carcinoma. Cases with different types were considered discordant, and slides were reviewed. Results. Of 231 cases, 225 (97.4%) had concordant diagnoses. Discordance was the result of misinterpretation of undifferentiated carcinoma, overinterpretation of squamous dysplasia, interpretation of suboptimal specimens with necrosis and crush artifact, and sampling error. Conclusions. Even though the cytology and biopsy specimens were reviewed by different pathologists, the concordance rate for histologic type at our institution was high, emphasizing that this is a safe practice. The few discordant cases did not affect the patient s outcome. (Arch Pathol Lab Med. 2010;134: ) The diagnosis of lung cancer is often confirmed by cytology and biopsy specimens obtained during a bronchoscopic procedure. An important step in guiding treatment is determining the histologic type of cancer. Distinguishing small cell lung carcinoma (SCLC) from non small cell lung carcinoma (NSCLC) is critical because the treatment modalities and prognosis differ greatly. At our institution, NSCLC represents approximately 89% of all lung cancer diagnoses. 1 The mainstays of therapy for limited-stage SCLC are chemotherapy and radiotherapy; extensive-stage SCLC is treated primarily with chemotherapy. The role of surgery in SCLC is still under investigation, although it may be of value in treating limited disease. 2 In contrast, surgery remains the cornerstone of treatment for NSCLC and the only hope for cure, especially for stage I and II disease. Adjuvant chemotherapy offers some benefit for stage II tumors. 2 For advanced disease, treatment relies on a combination of radiotherapy, chemotherapy, and other novel therapies. 3 5 The response rate to chemotherapy and radiotherapy is lower in NSCLC than in SCLC, but the survival rates are better. 2 6 Therefore, accurate subtyping of lung cancer is critical. Accepted for publication January 15, From the Division of Anatomic Pathology, Mayo Clinic, Rochester, Minnesota. The authors have no relevant financial interest in the products or companies described in this article. Reprints: Diva R. Salomão, MD, Division of Anatomic Pathology, Mayo Clinic, 200 First St SW, Rochester, MN ( salomao. diva@mayo.edu). Usually, biopsy and cytology specimens are taken during the same diagnostic bronchoscopic procedure. At our institution, the biopsy and cytology specimens are processed separately in different laboratories, become available for review at different times daily, and are reported separately by 2 different pathologists; therefore, correlation between both specimens is not routinely done. Discordances between histologic types have occurred in our practice, which occasionally caused clinical challenges and required resolution. However, the frequency of this type of discordance and the causes were unknown, and whether there was a need to modify our practice remained unclear. Previous studies have shown that the accuracy in differentiating between SCLC and NSCLC on cytology specimens ranged from 94% to 100%, with average error rates of 9% (range, 0% 33%) for SCLC and 2% (range, 1% 7%) for NSCLC, 7 when compared with the resection or autopsy specimen. The accuracy for bronchoscopic biopsy specimens in differentiating between histologic types of lung carcinomas ranges from 62% to 97.5%, when compared with the resection or autopsy specimen, taking into account discrepancies between subtypes of NSCLC The correlation between cytology and biopsy diagnoses is not well known. The purpose of this study was to evaluate the rate of concordance of histologic types of lung cancer diagnosed in cytology and biopsy specimens obtained during a single bronchoscopic procedure, to evaluate the cause of discordance, and to correlate discordance with patient outcome Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al
2 Table 1. Demographics, Radiologic Information, and Outcomes for Different Cytology/Biopsy Diagnosis Categories and Overall Group for Same Bronchoscopic Procedure Specimens Characteristic Cytology/Biopsy Diagnosis Positive/Positive Positive/Negative Negative/Positive Negative/Negative Cases, No. (%) 231 (27) 44 (5) 90 (10) 493 (57) 858 (100) Age, mean (SD), y 67.0 (11.0) 65.6 (10.7) 65.3 (11.9) 60.5 (15.1) 63 (13.9) Male, No. (%) 151 (65) 25 (57) 49 (54) 264 (54) 489 (57) Radiologic information Type of lesion, No. (%) Mass lesion 198 (86) 29 (66) 70 (78) 122 (25) 419 (49) Localized infiltrate 9 (3.9) 5 (11.4) 4 (4.4) 110 (22) 128 (15) Bilateral infiltrates 4 (1.7) 1 (2.3) 1 (1.1) 159 (32) 165 (19) Lymphadenopathy 7 (3.0) 4 (9.1) 4 (4.4) 28 (6) 43 (5) NA 13 (5.6) 5 (11.4) 11 (12) 74 (15) 103 (12) Size of lesion, mean (SD), cm Location, No. (%) Central 148 (64) 18 (41) 53 (59) 113 (23) 332 (39) Peripheral 24 (10) 12 (27) 4 (4.4) 68 (14) 108 (13) Diffuse 2 (0.9) 0 (0) 0 (0) 88 (18) 90 (10) Midlung or NS 57 (25) 14 (32) 33 (37) 224 (45) 328 (38) Outcomes Died, No. (%) Of lung cancer 91 (39) 14 (32) 38 (42) 25 (5) 168 (20) Of other causes 6 (2.6) 2 (4.5) 5 (5.6) 66 (13) 79 (9) Of unknown cause 0 (0) 2 (4.5) 0 (0) 4 (0.8) 6 (0.7) Alive, No. (%) With lung cancer 114 (49) 19 (43) 31 (34) 19 (4) 183 (21) Without lung cancer 20 (9) 6 (13.6) 14 (16) 343 (70) 383 (45) With unknown cancer status 0 (0) 1 (2.3) 2 (2.2) 36 (7) 39 (5) Abbreviations: NA, nonspecific changes or no imaging studies; NS, not specified. Total MATERIALS AND METHODS With Mayo Clinic institutional review board approval, a computer search of pathology files was performed to identify all cases for which biopsy and cytology specimens were obtained during the same diagnostic bronchoscopic procedure between January 1, 2000, and December 31, 2005, at Mayo Clinic, Rochester, Minnesota, our institution. The specimens included in this study were from patients who provided consent for their information to be used for research purposes. Cytology specimens were classified as negative, atypical, suspicious, or positive for malignancy. For the final analysis, atypical cases were considered negative, and suspicious cases were considered positive. Biopsy specimens showing dysplasia, carcinoma in situ, invasive carcinoma, or other malignancies were considered positive. Biopsy specimens with atypia (reactive or not otherwise specified) were considered negative. The positive cases were further evaluated for concordance of SCLC versus NSCLC between cytology and biopsy specimens. Clinical and radiologic data were abstracted from computerized medical files and included age, sex, and clinical outcome. Outcome was based on the last clinical note or the reported date of death, and duration of follow-up was calculated from the date of the patient s bronchoscopic procedure. Abstracted radiologic information included lesion type, size, and location. Lesions were divided into infiltrates or nodule/mass and unilateral or bilateral. The location of lesions as central or peripheral was recorded when assessed. Slides for discordant cases were reviewed independently by a cytopathologist (D.R.S.) and a pulmonary pathologist (M.C.A.) who were blinded to the clinical data and original diagnosis. Immunohistochemical studies were performed to support the diagnostic impression when there was disagreement on the original diagnosis or disagreement between the reviewing pathologists. Cytologic and histologic diagnoses were then compared, and cases with remaining discordance were submitted for independent evaluation to a second pulmonary pathologist (E.S.Y.) who was blinded not only to the clinical data and original diagnosis but also to the opinions of the other 2 pathologists. A consensus diagnosis was then made on the basis of all the available data. Factors contributing to the discordance were noted. RESULTS During the study period, 858 patients underwent a bronchoscopic procedure in which both cytology and biopsy specimens were obtained (Table 1). Of these, 493 patients (57%) had negative results for malignancy on both cytology and biopsy specimens. In a few patients, a positive result was detected either in the cytology specimen (44 patients [5%]) or in the biopsy specimen (90 patients [10%]) alone. The remaining 231 patients (27%) had both positive cytology and positive biopsy findings, and these composed our study group. Most patients were men (151 of 231; 65%) with a mean age of 67 years. The primary reason for biopsy in these patients was a central lung mass (198 of 231; 86%). For 225 of the 231 cases (97.4%), the cytology and the biopsy specimens yielded a concordant diagnosis. The findings in the 6 discordant cases are summarized in Table 2, and details of their clinical histories are provided as individual case reports. The effect of the discrepancy on each patient outcome was classified as harm, near-miss, and no-harm, using the scale proposed by the Institute of Medicine Case 1 A 64-year-old woman presented with a 6-cm central lung mass. Original diagnoses were combined SCLC and NSCLC for the cytology specimen and SCLC for the Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al 1505
3 Case No. Table 2. Age, y/sex Discordant Cytology and Histology Types for the Same Bronchoscopic Procedure Cytology and Biopsy Specimens Original Diagnosis Review Diagnosis Cytology Biopsy Cytology Biopsy Cause of Discordance 1 64/F Combined SCLC- NSCLC SCLC SCLC SCLC, moderate severe dysplasia Interpretation 2 62/M Sec: NSCLC SCLC Sec: SCLC, SCLC Interpretation (SQCC); TBNA: dysplasia; SCLC TBNA: SCLC 3 76/M NSCLC SCLC NSCLC NSCLC Interpretation 4 81/F SCLC NSCLC SCLC NSCLC Suboptimal specimen 5 39/M NSCLC NEC with NSCLC with Carcinoid tumor Suboptimal SCLC possible SCLC specimen features component 6 72/M SCLC Combined SCLC- NSCLC SCLC Combined SCLC- NSCLC Sampling error Effect on Patient Outcome a Followup, mo Outcome No harm 12 DOD No harm 12 AWD Harm 26 DOD No harm 18 DOD Harm None NA No harm None NA Abbreviations: AWD, alive with disease; DOD, died of disease; NA, not available; NEC, neuroendocrine carcinoma; NSCLC, non small cell lung carcinoma; SCLC, small cell lung carcinoma; Sec, secretion; SQCC, squamous cell carcinoma; TBNA, transbronchial needle aspiration. a The effect of the discrepancy on each patient outcome was classified as harm, near-miss, and no-harm, using the scale proposed by the Institute of Medicine. 13 biopsy specimen. The patient was treated for SCLC and had an initial complete response to chemotherapy and radiotherapy, but liver metastasis developed 9 months later. She died of lung cancer 12 months after initial diagnosis. The review diagnosis for the cytology specimen was SCLC, with a possible, but questionable, squamous cell carcinoma component (Figure 1, A). Review of the biopsy specimen concurred with the original diagnosis of SCLC. Squamous metaplasia with severe dysplasia was noted on the biopsy specimen (Figure 1, B). The consensus diagnosis was SCLC. The discordance was considered an interpretive error. The squamous dysplasia was interpreted as squamous cell carcinoma on the original cytology diagnosis. This was a no-harm type of error because it did not affect treatment; combined SCLC- NSCLC is treated as SCLC. Case 2 A 62-year-old man presented with localized pulmonary infiltrates and a history of esophageal squamous cell carcinoma, treated with esophagogastrectomy the prior year. The original diagnoses were NSCLC favoring squamous cell carcinoma for the bronchial secretion specimen, SCLC for the transbronchial needle aspirate, and SCLC for the bronchial biopsy specimen. Nine months later, metastatic SCLC was diagnosed in a liver fine-needle aspiration biopsy specimen, and the patient underwent chemotherapy and radiotherapy, but the disease progressed, and metastasis developed in the right cerebellum. The patient was alive with persistent lung cancer after 12 months of follow-up. The review diagnosis for the bronchial secretion specimen was SCLC with associated squamous dysplasia. The biopsy specimen showed extensive crush artifact and Figure 1. Case 1. Small cell lung carcinoma and squamous metaplasia with moderate to severe dysplasia. A, The cytology specimen shows small cell lung carcinoma (left) and clusters of squamous cells with dysplasia (right upper). B, Biopsy with small cell lung carcinoma and moderate squamous dysplasia in the overlying epithelium (Papanicolaou stain, original magnification 3400 [A]; hematoxylin-eosin, original magnification 3400 [B]) Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al
4 extensive necrosis. The histologic features of the viable cells suggested SCLC. Immunohistochemical studies performed on the biopsy demonstrated that the tumor was strongly positive for TTF-1, positive in a perinuclear dotlike pattern for cytokeratin AE1/AE3, and negative for cytokeratin 903, p63, and desmoglein 3, further supporting the diagnosis of SCLC and ruling out squamous cell carcinoma. The consensus diagnosis for this case was SCLC. This was considered an interpretive error, similar to that in case 1. Squamous dysplasia led to the interpretation of all the tumor cells as squamous cell carcinoma on the bronchial secretion specimen. This was a no-harm type error because it did not affect treatment for this patient. Case 3 A 76-year-old man had a history of limited SCLC treated by chemotherapy and radiotherapy and had been free of disease for 8 years when he presented with a new lung mass and diffuse brain metastasis. The original bronchoscopic diagnoses of this new lung mass were NSCLC for the cytology specimen and SCLC for the biopsy specimen. Clinically, he was believed to have recurrent SCLC and was treated accordingly. The patient ultimately died of lung cancer 26 months later. The review diagnoses for both the cytology and biopsy specimens were NSCLC (M.S.,M.C.A.,D.R.S.). The smears showed a few clusters of neoplastic cells, intermixed with benign bronchial epithelial cells. In some clusters, the neoplastic cells were stripped of their cytoplasm, showed hyperchromatic nuclei, and occasional molding. In other clusters, where the cells were better preserved, eosinophilic cytoplasm and distinct small nucleoli were visible. Some cells showed a finely granular chromatin pattern characteristic of neuroendocrine tumors (Figure 2, A). On the basis of the cytologic features observed in the preserved cells, this neoplasm was thought to be better characterized as an NSCLC. Because of the discrepancy with the previous history and clinical assumption, both cytology and biopsy specimens were rereviewed along with material from the previous tumor (M.C.A.,D.R.S.). On rereview, the biopsy specimen showed a poorly differentiated carcinoma. Atypical cells had a moderate amount of cytoplasm without nuclear molding, but the nuclei had a homogenous chromatin and no nucleoli, similar to the nuclear features observed in SCLC (Figure 2, B). Immunohistochemical studies of the biopsy specimen demonstrated that the tumor cells were positive for cytokeratin AE1/AE3, showing predominantly cytoplasmic staining. TTF-1, CD56, and synaptophysin results were also positive, and chromogranin staining was negative. The case was then reviewed by the third pathologist (E.S.Y.) who favored a diagnosis of SCLC. Interestingly, all 3 (M.C.A.,D.R.S.,E.S.Y.) pathologists believed that the original tumor was NSCLC and that it looked slightly different from the current tumor, although it had a similar immunoprofile (Figure 2, C). Ultimately, the 3 pathologists could not reach a consensus, and the differential diagnosis between SCLC and NSCLC with neuroendocrine differentiation was unresolved. Because differences in treatment could potentially affect the patient outcome, this was considered a harm type error. Figure 2. Case 3. A, High-power photomicrograph of the cytology specimen. B, Corresponding biopsy specimen. Both specimens show an undifferentiated malignancy composed of moderate to large-sized cells with the presence of cytoplasm. Cytologically, the nuclei do not show extensive molding and have an open chromatin and a small punctate nucleoli. Histologically, the nuclei have more molding and more uniform, dark chromatin. C, The biopsy specimen taken 8 years previously when lung cancer was initially diagnosed (Papanicolaou stain, original magnification 3600 [A]; hematoxylin-eosin, original magnifications 3400 [B and C]). Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al 1507
5 Figure 3. Case 4. Non small cell lung carcinoma with extensive necrosis. A, The cytology specimen shows an extremely necrotic tumor with scant cells interpreted as a small cell lung carcinoma. B, The biopsy specimen comprises mostly hyperchromatic crushed and necrotic cells. C, Intermediate magnification of the biopsy specimen. D, High-power magnification of the biopsy specimen. Both C and D show a focal viable tumor with mild to moderately abundant cytoplasm interpreted as non small cell lung carcinoma (Papanicolaou stain, original magnification 3200 [A]; hematoxylin-eosin, original magnifications 3200 [B and C] and 3400 [D]). Case 4 An 81-year-old woman presented with a large central lung mass. The original diagnoses were SCLC for the cytology specimen and NSCLC for the biopsy specimen. The patient was not a good candidate for surgery and was treated for NSCLC with radiotherapy. Bilateral adrenal masses developed, and the patient died of lung cancer 18 months after the initial diagnosis. The review diagnoses for both the cytology and biopsy specimens concurred with their respective original diagnoses. Both specimens showed extensive necrosis. In the biopsy specimen, viable tumor cells contained a moderate amount of cytoplasm without nuclear molding (Figure 3, B through D), supporting a diagnosis of NSCLC. The cytology specimen was paucicellular, with rare clusters of cells, showing scant or no cytoplasm, and with elongated nuclei with no nucleoli, suggestive of SCLC (Figure 3, A). The cells seen in the cytology specimen were thought to correspond to the small hyperchromatic cells seen in the biopsy specimen. However, based on the well-preserved tumor cells in the biopsy, the final consensus diagnosis for 1508 Arch Pathol Lab Med Vol 134, October 2010 this case was NSCLC. Rendering diagnosis in a suboptimal paucicellular specimen with extensive necrosis was identified as the cause of the discordance. This error did not affect patient care; the patient s treatment was based on the biopsy findings, which were confirmed in our review. Therefore, it was considered a no-harm type of error. Case 5 A 39-year-old man, with a complex medical history, was first seen 4 years earlier for treatment of a thymic tumor, a diagnosis made outside our institution and not reviewed before treatment. Because of extensive regional invasion, he was treated with neoadjuvant therapy followed by surgery. A diagnosis of grade 3 (of 4) thymic neuroendocrine carcinoma was made on the surgical specimen, and the patient was treated with additional chemotherapy, followed by radiotherapy and chemotherapy for metastases in the left supraclavicular lymph nodes. A central lung mass then developed. The original diagnoses were NSCLC for the cytology specimen and a grade 3 (of 4) neuroendocrine carcinoma with SCLC features for the Lung Biopsy and Cytology Concordance Sackett et al
6 Figure 4. Case 5. A, The biopsy specimen shows prominently crushed, small, hyperchromatic cells but no necrosis. The chromogranin is diffusely positive (image not shown). B, The MIB-1 labeling index is low. C, On review, the previous mediastinal specimen shows a marked artifact with crushing and a fixation effect. D, Focally, areas more typical of carcinoid tumor can be seen. E, The cytology specimen has scant cellularity, but the features are consistent with carcinoid tumor (hematoxylin-eosin, original magnifications 3200 [A], 3100 [C], and 3600 [D]; original magnification 3200 [B]; Papanicolaou stain, original magnification 3600 [E]). biopsy specimen. Clinically, the patient was considered to have recurrent high-grade thymic neuroendocrine carcinoma. The review diagnosis of the cytology specimen was NSCLC with a possible neuroendocrine (carcinoid or SCLC) component. On review, the lung biopsy was Arch Pathol Lab Med Vol 134, October 2010 composed of a single, small fragment of bronchial wall involved by small, hyperchromatic, crushed tumor cells (Figure 4, A). No necrosis was seen. The differential diagnosis was between SCLC and carcinoid tumor. In immunohistochemical results, the neoplastic cells were strongly and diffusely positive for chromogranin and Lung Biopsy and Cytology Concordance Sackett et al 1509
7 synaptophysin and showed a low proliferation index of 15% on the MIB-1 tests (Figure 4, B). Therefore, the diagnosis of carcinoid tumor was favored, which prompted review of the prior mediastinal excision. This specimen also showed focal crushed areas, along with a fixation artifact that distorted the neuroendocrine architecture (Figure 4, C). The tumor had no extensive necrosis and few mitotic figures (,10/10 high-power fields), but cellular atypia was present. Areas with typical features of carcinoid tumor were few (Figure 4, D). Diffuse and strong positive immunoreactivity for chromogranin and synaptophysin was also present. These features supported a diagnosis of atypical thymic carcinoid tumor, including the mitotic count. With this information, the cytologic specimen was rereviewed. The specimen was scant. The few tumor cell clusters did have neuroendocrine features and, in the absence of necrosis, were believed to be consistent with carcinoid tumor (Figure 4, E). The final consensus diagnosis was, therefore, carcinoid tumor. The error in this case was based on interpretation of scant material with a prominent artifact. The pitfall of distinguishing carcinoid tumor from SCLC was not avoided on initial diagnosis, possibly because of bias based on the historical diagnosis and no documentation of rereview of material. Furthermore, this error was compounded by not reviewing another institution s material before the initial surgery. Because of the aggressive nature of the tumor, treatment would not have differed for this patient, although confusing carcinoid tumor for SCLC is considered a harm type of error. Case 6 A 72-year-old man presented with a 5-cm central mass. Original diagnoses were SCLC for the cytology specimen and combined SCLC-NSCLC for the biopsy specimen. Clinically, there was no reconciliation of the results, and the patient was considered by the oncologist as having SCLC and was treated as such. It was interesting to note in the clinical records that the pulmonologist thought this patient had NSCLC. No follow-up was available for this patient. The review diagnosis for the cytology specimen was SCLC with extensive necrosis (Figure 5, A). Review of the biopsy specimen concurred with the original diagnosis of combined SCLC-NSCLC, further supported by the immunohistochemical study that showed strong TTF-1 immunoreactivity in the SCLC component, and CK903 highlighted the squamous cell carcinoma component (Figure 5, B through D). The consensus diagnosis was combined SCLC, with the NSCLC component not represented in the cytology specimen. The cause of discordance was considered to be attributable to sampling. This error did not affect patient care; therefore, it was considered a no-harm type error because the SCLC component, which determined treatment, was recognized. Summary of Cases In summary, 3 of these errors were interpretive: squamous dysplasia, interpreted as squamous cell carcinoma on cytology in cases 1 and 2; and distinguishing SCLC with larger-cell cytology from NSCLC with neuroendocrine differentiation in case 3. Poor quality of the material, either because of extensive tumor necrosis or crushing artifact, and the scantiness of the tumor cells were thought to be the causes of error in cases 4 and 5. Sampling error was the cause in case 6. COMMENT Our study showed that the concordance rate between the cytologic and histologic diagnoses distinguishing SCLC from NSCLC by different pathologists in our practice is high. This likely reflects that, in general, pathologists are highly accurate in the subtyping of lung cancer on cytology and biopsy bronchoscopic specimens In a study done in the 1980s, Matsuda et al 9 compared tumor types in specimens obtained from brushing and bronchial biopsy; the discordant rate for SCLC versus NSCLC was 2.57%. This similar discordance rate to our study, 2 decades later, suggests that, even with refinement in diagnostic tools and addition of ancillary studies, we have not improved on the rate of concordance. The high rate of concordance on histologic type supports the practice as safe and adequate. Because of the retrospective nature of our study, we were unable to account for an inherent bias caused by informal, undocumented correlation occurring at the time of sign-out of difficult cases, although we suspect this undocumented correlation occurs infrequently. Studies addressing cytologic-histologic correlation have more often been related to gynecologic than nongynecologic specimens Classically, the discrepancies have been classified as the result of sampling or misinterpretation. 20,21 In a recent study 16 analyzing the root cause of error in cases detected by cytologic-histologic correlation, the authors proposed a no-fault system based on specimen interpretability. Discrepancies between cytology and biopsy specimens, considered either benign or malignant, were classified on the basis of the quality of the specimen and the amount of neoplastic cells present in the specimen. 16 In our study, we focused on the discrepancies in the interpretation of tumor types; therefore, not all cases fell neatly into one of the subgroups proposed by those authors. 16 In our study, we believe that misinterpretation was the most common cause of discrepancy affecting 3 of 6 cases (50%). In cases 1 and 2, the interpretation of squamous dysplasia as NSCLC in the cytology specimen was the cause of the discrepancy. These 2 cases raise the issue of overinterpreting squamous dysplasia in cytologic specimens as squamous cell carcinoma. Several articles have addressed this issue of misinterpreting benign or atypical reactive cells as carcinoma in pulmonary cytology specimens. However, to our knowledge, squamous dysplasia has not been studied as having potential for misinterpretation. In our 2 cases, the finding of several squamous dysplastic cells made us overlook the other tumor cells present in the background. These were misinterpreted as poorly differentiated cells of invasive squamous cell carcinoma. In case 3, a consensus could not be achieved; this lack of agreement represents a recognized challenge: the distinction between SCLC and NSCLC in some cases. Unfortunately, immunohistochemical study plays a small role in this distinction, with the exception of SCLC versus squamous cell carcinoma. In the latter, a panel of immunostains, comprising TTF-1, p63, and high-molecular-weight keratin, usually distinguishes these 2 carcinomas, with SCLC expressing TTF-1, but not p63 and high Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al
8 Figure 5. Case 6. Combined small cell lung carcinoma and squamous cell carcinoma. A, Cytology specimen shows only the small cell lung carcinoma component. B, Both the small cell lung carcinoma component and the squamous cell carcinoma component are visualized on the biopsy specimen. C, High-molecular-weight keratin (CK903) is strongly positive in the squamous cell carcinoma component only. D, TTF-1 showed strong nuclear positivity in the small cell component only (Papanicolaou stain, original magnification 3600 [A]; hematoxylin-eosin, original magnification 3400 [B]; original magnifications 3400 [C and D]). molecular-weight keratin, and squamous cell carcinoma having the opposite profile.26 Otherwise, up to 25% of NSCLCs show expression of neuroendocrine markers, such as chromogranin, synaptophysin, and CD56, and by definition, all large cell neuroendocrine carcinomas should have expression of a neuroendocrine marker, thus overlapping with SCLC.27 A small percentage of SCLCs may be negative for all neuroendocrine markers.27 The pattern of staining with keratin markers may differ between SCLC and NSCLC, where the keratin in SCLCs often has dotlike perinuclear staining, whereas NSCLCs show more diffuse cytoplasmic staining, but otherwise, the distinction still relies mostly on cytologic and histologic features. This distinction is inherently subjective and can show overlap and thus lead to disagreements, even among experts.28 Fortunately, this lack of agreement occurs in only a small percentage of SCLCs.29 In cases 4 and 5, the poor quality of the material caused the discrepancy. In case 4, the discordance was attributed to the poor quality of the specimens, which had extensive necrosis and prominent crush artifact on both the cytology Arch Pathol Lab Med Vol 134, October 2010 and the biopsy specimens. However, the biopsy specimen had a cluster of viable tumor cells that allowed the diagnosis of NSCLC. Although pathologists recognize the shortcomings in making a diagnosis in specimens with necrosis and other artifacts, little data indicating how a marked artifact or necrosis affects the concordance rate between cytology and biopsy interpretation are available in the literature. Catalun a et al8 showed that the presence of necrosis significantly affected the concordance rate between biopsy and surgical specimens. Indeed, 30% of the biopsy specimens harboring necrosis were discordant in contrast to 11% of biopsy specimens without necrosis (P 5.02).8 In case 5, misinterpretation was attributed to historical bias. Although the clinical history usually helps achieve the correct diagnosis,30 in this particular case, not reviewing the prior surgical specimens and being swayed by the prior diagnosis of grade 3 (of 4) thymic neuroendocrine carcinoma led to an incorrect diagnosis. Similar to the recommendations of other authors,31 we recommend that prior material, especially with unusual features or a rare Lung Biopsy and Cytology Concordance Sackett et al 1511
9 diagnosis, be reviewed in the current clinical context to avoid this type of misinterpretation. In case 6, in which a sampling error occurred, the review biopsy diagnosis was combined SCLC-NSCLC; only SCLC was present in the cytology specimen. Combined SCLC-NSCLC is an uncommon diagnosis, and discordance between cytology and biopsy specimens is reported, to our knowledge, in only 2 prior studies. 9,32 Matsuda et al 9 reported 1 case of combined SCLC-NSCLC in which interpretation of the biopsy specimen was accurate, but the brushing cytology interpretation was not. Pilotti et al 32 reported 2 cases of combined SCLC- NSCLC in which the cytology specimen was classified as not otherwise specified in both cases. Recognizing and confirming the presence of SCLC in at least one of the specimens, cytology or biopsy, in a possible combined SCLC or NSCLC, remains crucial because the standard of care for combined SCLC-NSCLC is to treat as SCLC. Our study focused on discordances in distinguishing NSCLC from SCLC because pathologists have not been asked before to further classify the lung cancer type in cytology specimens. However, with the advent of novel therapies, we are facing the need to further subclassify NSCLC on cytology and biopsy specimens. 33,34 Previous studies have shown that SCLC and NSCLC can be distinguished with high accuracy (range, 94% 100%) in cytology specimens, 7 but this accuracy drops to a range from 66% to 91% when subclassification of NSCLC into squamous cell carcinoma, adenocarcinoma, and large cell neuroendocrine carcinoma is performed. 9,11,32 Ancillary studies may play a role as new biomarkers are discovered, and further studies to assess concordance in subclassification of NSCLC will need to be performed. CONCLUSIONS At our institution, the concordance rate for cytologichistologic diagnosis regarding lung cancer type is high (97.4%), despite these specimens being interpreted independently by different pathologists. Therefore, we believe this practice is safe. Discordance was the result of interpreting suboptimal specimens, misinterpreting squamous dysplasia as squamous cell carcinoma on the cytology specimen, misinterpreting a poorly differentiated neoplasm, and not recognizing a second component of a combined SCLC-NSCLC. Challenging cases, an unusual diagnosis, and suboptimal specimens should prompt reconciliation of findings between cytology and biopsy specimens, as well as with pertinent, previous histologic specimens before finalizing the diagnosis. References 1. Yang P, Allen MS, Aubry MC, et al. Clinical features of 5,628 primary lung cancer patients: experience at Mayo Clinic from 1997 to Chest. 2005; 128(1): Scott WJ, Howington J, Feigenberg S, et al. Treatment of non-small cell lung cancer stage I and stage II: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3)(suppl):234S 242S. 3. Robinson LA, Ruckdeschel JC, Wagner H Jr, et al. Treatment of non-small cell lung cancer-stage IIIA: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3)(suppl):243S 265S. 4. Jett JR, Schild SE, Keith RL, Jett JR, Schild SE, Keith RL, Kesler KA; American College of Chest Physicians. Treatment of non-small cell lung cancer, stage IIIB: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007; 132(3)(suppl):266S 276S. 5. Socinski MA, Crowell R, Hensing TE, et al. Treatment of non-small cell lung cancer, stage IV: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3)(suppl):277S 289S. 6. Simon GR, Turrisi A; American College of Chest Physicians. Management of small cell lung cancer: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3)(suppl):324S 339S. 7. Rivera MP, Mehta AC; American College of Chest Physicians. Initial diagnosis of lung cancer: ACCP evidence-based clinical practice guidelines (2nd edition). Chest. 2007;132(3)(suppl):131S 148S. 8. Cataluna JJ, Perpina M, Greses JV, Calvo V, Padilla JD, Paris F. Cell type accuracy of bronchial biopsy specimens in primary lung cancer. Chest. 1996; 109(5): Matsuda M, Horai T, Nakamura S, et al. Bronchial brushing and bronchial biopsy: comparison of diagnostic accuracy and cell typing reliability in lung cancer. Thorax. 1986;41(6): Rudd RM, Gellert AR, Boldy DA, et al. Bronchoscopic and percutaneous aspiration biopsy in the diagnosis of bronchial carcinoma cell type. Thorax. 1982;37(6): Clee MD, Duguid HL, Sinclair DJ. Accuracy of morphological diagnosis of lung cancer in a department of respiratory medicine. J Clin Pathol. 1982;35(4): Payne CR, Hadfield JW, Stovin PG, Barker V, Heard BE, Stark JE. Diagnostic accuracy of cytology and biopsy in primary bronchial carcinoma. J Clin Pathol. 1981;34(7): Committee on Quality of Healthy Care in America, Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Washington, DC: National Academy Press; 2001: Raab SS, Nakhleh RE, Ruby SG. Patient safety in anatomic pathology: measuring discrepancy frequencies and causes. Arch Pathol Lab Med. 2005; 129(4): Kohn LT, Corrigan JM, Donaldson MS, editors. To err is human: building a safer health system. Washington, DC: National Academy Press; 2000: Raab SS, Stone CH, Wojcik EM, et al. Use of a new method in reaching consensus on the cause of cytologic-histologic correlation discrepancy. Am J Clin Pathol. 2006;126(6): Saha R, Thapa M. Correlation of cervical cytology with cervical histology. Kathmandu Univ Med J (KUMJ). 2005;3(3): Pradhan B, Pradhan SB, Mital VP. Correlation of Pap smear findings with clinical findings and cervical biopsy. Kathmandu Univ Med J (KUMJ). 2007;5(4): Jones BA, Novis DA. Cervical biopsy-cytology correlation: a College of American Pathologists Q-Probes study of 22,439 correlations in 348 laboratories. Arch Pathol Lab Med. 1996;120(6): Clary KM, Silverman JF, Liu Y, et al. Cytohistologic discrepancies: a means to improve pathology practice and patient outcomes. Am J Clin Pathol. 2002; 117(4): Renshaw AA. Measuring and reporting errors in surgical pathology: lessons from gynecologic cytology. Am J Clin Pathol. 2001;115(3): Ogino S, Franks TJ, Yong M, Koss MN. Extensive squamous metaplasia with cytologic atypia in diffuse alveolar damage mimicking squamous cell carcinoma: a report of 2 cases. Hum Pathol. 2002;33(10): Crapanzano JP, Zakowski MF. Diagnostic dilemmas in pulmonary cytology. Cancer. 2001;93(6): DeMay RM. The Art and Science of Cytopathology. Chicago, IL: ASCP Press; Naryshkin S, Young NA. Respiratory cytology: a review of non-neoplastic mimics of malignancy. Diagn Cytopathol. 1993;9(1): Wu M, Wang B, Gil J, et al. p63 and TTF-1 immunostaining: a useful marker panel for distinguishing small cell carcinoma of lung from poorly differentiated squamous cell carcinoma of lung. Am J Clin Pathol. 2003;119(5): Lyda MH, Weiss LM. Immunoreactivity for epithelial and neuroendocrine antibodies are useful in the differential diagnosis of lung carcinomas. Hum Pathol. 2000;31(8): Marchevsky AM, Gal AA, Shah S, Koss MN. Morphometry confirms the presence of considerable nuclear size overlap between small cells and large cells in high-grade pulmonary neuroendocrine neoplasms. Am J Clin Pathol. 2001;116(4): Travis WD, Gal AA, Colby TV, Klimstra DS, Falk R, Koss MN. Reproducibility of neuroendocrine lung tumor classification. Hum Pathol. 1998;29(3): Raab SS, Oweity T, Hughes JH, et al. Effect of clinical history on diagnostic accuracy in the cytologic interpretation of bronchial brush specimens. Am J Clin Pathol. 2000;114(1): Tsung JS. Institutional pathology consultation. Am J Surg Pathol. 2004; 28(3): Pilotti S, Rilke F, Gribaudi G, Spinelli P. Cytologic diagnosis of pulmonary carcinoma on bronchoscopic brushing material. Acta Cytol. 1982;26(5): Sandler A. Bevacizumab in non small cell lung cancer. Clin Cancer Res. 2007;13(15, pt 2):s4613 s Cabebe E, Wakelee H. Role of anti-angiogenesis agents in treating NSCLC: focus on bevacizumab and VEGFR tyrosine kinase inhibitors. Curr Treat Options Oncol. 2007;8(1): Arch Pathol Lab Med Vol 134, October 2010 Lung Biopsy and Cytology Concordance Sackett et al
Respiratory Tract Cytology
 Respiratory Tract Cytology 40 th European Congress of Cytology Liverpool, UK Momin T. Siddiqui M.D. Professor of Pathology and Laboratory Medicine Director of Cytopathology Emory University Hospital, Atlanta,
Respiratory Tract Cytology 40 th European Congress of Cytology Liverpool, UK Momin T. Siddiqui M.D. Professor of Pathology and Laboratory Medicine Director of Cytopathology Emory University Hospital, Atlanta,
Lung Cytology: Lessons Learned from Errors in Practice
 Lung Cytology: Lessons Learned from Errors in Practice Stephen S. Raab, M.D. Department of Laboratory Medicine Eastern Health and Memorial University of Newfoundland, St. John s, NL and University of Washington,
Lung Cytology: Lessons Learned from Errors in Practice Stephen S. Raab, M.D. Department of Laboratory Medicine Eastern Health and Memorial University of Newfoundland, St. John s, NL and University of Washington,
Neuroendocrine Lung Tumors Myers
 Diagnosis and Classification of Neuroendocrine Lung Tumors Jeffrey L. Myers, M.D. A. James French Professor Director, Anatomic Pathology & MLabs University of Michigan, Ann Arbor, MI myerjeff@umich.edu
Diagnosis and Classification of Neuroendocrine Lung Tumors Jeffrey L. Myers, M.D. A. James French Professor Director, Anatomic Pathology & MLabs University of Michigan, Ann Arbor, MI myerjeff@umich.edu
DIAGNOSTIC DILEMMA. Case Reports Clinical history. Materials and Methods
 DIAGNOSTIC DILEMMA A Metastatic Renal Carcinoid Tumor Presenting as Breast Mass: A Diagnostic Dilemma Farnaz Hasteh, M.D., 1 Robert Pu, M.D., Ph.D., 2 and Claire W. Michael, M.D. 2 * We present clinicopathological
DIAGNOSTIC DILEMMA A Metastatic Renal Carcinoid Tumor Presenting as Breast Mass: A Diagnostic Dilemma Farnaz Hasteh, M.D., 1 Robert Pu, M.D., Ph.D., 2 and Claire W. Michael, M.D. 2 * We present clinicopathological
Objectives. Atypical Glandular Cells. Atypical Endocervical Cells. Reactive Endocervical Cells
 2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
2013 California Society of Pathologists 66 th Annual Meeting San Francisco, CA Atypical Glandular Cells to Early Invasive Adenocarcinoma: Cervical Cytology and Histology Christina S. Kong, MD Associate
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy.
 November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
November 2015 Case of the Month A 53 year-old woman with a lung mass, right hilar mass and mediastinal adenopathy. Contributed by: Rasha Salama, M.D., IU Department of Pathology and Laboratory Medicine
The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia
 MALIGNANCIES OF THE THYMUS The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia Maureen F. Zakowski, MD, James Huang, MD, and Matthew P. Bramlage, MD Background:
MALIGNANCIES OF THE THYMUS The Role of Fine Needle Aspiration Cytology in the Diagnosis and Management of Thymic Neoplasia Maureen F. Zakowski, MD, James Huang, MD, and Matthew P. Bramlage, MD Background:
LUNG CANCER PATHOLOGY: UPDATE ON NEUROENDOCRINE LUNG TUMORS
 LUNG CANCER PATHOLOGY: UPDATE ON NEUROENDOCRINE LUNG TUMORS William D. Travis, M.D. Attending Thoracic Pathologist Memorial Sloan Kettering Cancer Center New York, NY PULMONARY NE TUMORS CLASSIFICATION
LUNG CANCER PATHOLOGY: UPDATE ON NEUROENDOCRINE LUNG TUMORS William D. Travis, M.D. Attending Thoracic Pathologist Memorial Sloan Kettering Cancer Center New York, NY PULMONARY NE TUMORS CLASSIFICATION
Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000
 Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000 Thomas A. Bonfiglio, M.D. Professor Emeritus, Pathology and Laboratory Medicine University of Rochester Disclosures In the past 12 months,
Hyperchromatic Crowded Groups: What is Your Diagnosis? Session 3000 Thomas A. Bonfiglio, M.D. Professor Emeritus, Pathology and Laboratory Medicine University of Rochester Disclosures In the past 12 months,
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Problem 1: Differential of Neuroendocrine Carcinoma 3/23/2017. Disclosure of Relevant Financial Relationships
 Differential of Neuroendocrine Carcinoma Alain C. Borczuk,MD Weill Cornell Medicine Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control
Differential of Neuroendocrine Carcinoma Alain C. Borczuk,MD Weill Cornell Medicine Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control
Objectives. Salivary Gland FNA: The Milan System. Role of Salivary Gland FNA 04/26/2018
 Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics. Mercè Jordà, University of Miami
 Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics Mercè Jordà, University of Miami Mortality Lung cancer is the most frequent cause of cancer incidence and mortality
Cytological Sub-classification of Lung Cancer: Morphologic and Molecular Characteristics Mercè Jordà, University of Miami Mortality Lung cancer is the most frequent cause of cancer incidence and mortality
Neuroendocrine neoplasms of the lung
 Neuroendocrine neoplasms of the lung M Papotti, L Righi, & M Volante University of Turin at San Luigi Hospital TORINO NETs OF THE LUNG Menu - Spectrum of NE lung tumors - CARCINOID TUMORS - SCLC /LCNEC
Neuroendocrine neoplasms of the lung M Papotti, L Righi, & M Volante University of Turin at San Luigi Hospital TORINO NETs OF THE LUNG Menu - Spectrum of NE lung tumors - CARCINOID TUMORS - SCLC /LCNEC
Diagnostic accuracy of cytology and biopsy in
 Thorax, 1979, 34, 294-299 Diagnostic accuracy of cytology and biopsy in primary bronchial carcinoma C R PAYNE, P G I STOVIN, V BARKER, S McVITTIE, AND J E STARK From Papworth Hospital, Papworth Everard,
Thorax, 1979, 34, 294-299 Diagnostic accuracy of cytology and biopsy in primary bronchial carcinoma C R PAYNE, P G I STOVIN, V BARKER, S McVITTIE, AND J E STARK From Papworth Hospital, Papworth Everard,
5/1/2009. Squamous Dysplasia/CIS AAH DIPNECH. Adenocarcinoma
 Pathological Assessment of Diagnostic Specimens Keith Kerr Department of Pathology Aberdeen University Medical School Aberdeen Royal Infirmary Foresterhill, Aberdeen, Scotland, UK Tumours of the Lung:
Pathological Assessment of Diagnostic Specimens Keith Kerr Department of Pathology Aberdeen University Medical School Aberdeen Royal Infirmary Foresterhill, Aberdeen, Scotland, UK Tumours of the Lung:
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung
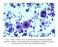 Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung masses. Specimen shown is from a tap of the pleural effusion.
Case 1. Slide 1 History: 65 year old male presents with bilateral pleural effusions, a 40 pack year smoking history and peripheral and hilar lung masses. Specimen shown is from a tap of the pleural effusion.
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Basaloid Carcinoma of the Lung: A Really Dismal Histologic Variant?
 Carcinoma of the Lung: A Really Dismal Histologic Variant? Dae Joon Kim, MD, Kil Dong Kim, MD, Dong Hwan Shin, MD, Jae Y Ro, MD, and Kyung Young Chung, MD Departments of Thoracic and Cardiovascular Surgery,
Carcinoma of the Lung: A Really Dismal Histologic Variant? Dae Joon Kim, MD, Kil Dong Kim, MD, Dong Hwan Shin, MD, Jae Y Ro, MD, and Kyung Young Chung, MD Departments of Thoracic and Cardiovascular Surgery,
Case # year old man with a 2 cm right kidney mass
 Case # 4. 52 year old man with a 2 cm right kidney mass Figure 1 Figure 2 Figure 3 Figure 4 Diagnosis: Negative/Non-diagnostic Normal kidney tissue Fine needle aspiration (FNA) of the kidney is performed
Case # 4. 52 year old man with a 2 cm right kidney mass Figure 1 Figure 2 Figure 3 Figure 4 Diagnosis: Negative/Non-diagnostic Normal kidney tissue Fine needle aspiration (FNA) of the kidney is performed
Root Cause Analysis of Problems in the Frozen Section Diagnosis of In Situ, Minimally Invasive, and Invasive Adenocarcinoma of the Lung
 Root Cause Analysis of Problems in the Frozen Section Diagnosis of In Situ, Minimally Invasive, and Invasive Adenocarcinoma of the Lung Ann E. Walts, MD; Alberto M. Marchevsky, MD Context. Frozen sections
Root Cause Analysis of Problems in the Frozen Section Diagnosis of In Situ, Minimally Invasive, and Invasive Adenocarcinoma of the Lung Ann E. Walts, MD; Alberto M. Marchevsky, MD Context. Frozen sections
Immunohistochemical Profile of Lung Tumors in Image Guided Biopsies
 Original Article DOI: 10.21276/APALM.1342 Immunohistochemical Profile of Lung Tumors in Image Guided Biopsies T. Pavithra 1 *, A. Dhanalakshmi 1, C. Lalitha 1, K.B. Lavanya 1 and S. Shifa 2 Department
Original Article DOI: 10.21276/APALM.1342 Immunohistochemical Profile of Lung Tumors in Image Guided Biopsies T. Pavithra 1 *, A. Dhanalakshmi 1, C. Lalitha 1, K.B. Lavanya 1 and S. Shifa 2 Department
Cellular Dyscohesion in Fine-Needle Aspiration of Breast Carcinoma Prognostic Indicator for Axillary Lymph Node Metastases?
 natomic Pathology / PROGNOSTIC INDICTOR FOR XILLRY LYMPH NODE METSTSES Cellular Dyscohesion in Fine-Needle spiration of reast Carcinoma Prognostic Indicator for xillary Lymph Node Metastases? nne. Schiller,
natomic Pathology / PROGNOSTIC INDICTOR FOR XILLRY LYMPH NODE METSTSES Cellular Dyscohesion in Fine-Needle spiration of reast Carcinoma Prognostic Indicator for xillary Lymph Node Metastases? nne. Schiller,
EBUS-TBNA Diagnosis and Staging of Lung Cancer
 EBUS-TBNA Diagnosis and Staging of Lung Cancer Nirag Jhala MD, MIAC Professor of Pathology and Lab Med. Director of Anatomic Pathology and Cytopathology Lewis Katz School of Medicine@ Temple University
EBUS-TBNA Diagnosis and Staging of Lung Cancer Nirag Jhala MD, MIAC Professor of Pathology and Lab Med. Director of Anatomic Pathology and Cytopathology Lewis Katz School of Medicine@ Temple University
Reparatory system 18 lectures Heyam Awad
 Reparatory system 18 lectures 8-10 Heyam Awad These lectures cover the following topics 1. Diffuse hemorrhagic syndromes 2. Lung tumors important: theses slides are your study source for these lectures.
Reparatory system 18 lectures 8-10 Heyam Awad These lectures cover the following topics 1. Diffuse hemorrhagic syndromes 2. Lung tumors important: theses slides are your study source for these lectures.
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches
 Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
Salivary gland tumor cytologic and histologic correlation: Algorithmic and risk stratification based approaches Christopher C. Griffith, MD, PhD Raja R. Seethala, MD 1. Salivary gland tumor cytology: A
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
THYMIC CARCINOMAS AN UPDATE
 THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
Medullary Thyroid Carcinoma. This case was provided by Treant Hospital, Bethesda, Hoogeveen, The Netherlands
 Medullary Thyroid Carcinoma This case was provided by Treant Hospital, Bethesda, Hoogeveen, The Netherlands ADS-01504 Rev. 001 2016 Hologic, Inc. All rights reserved. Overview Medullary Thyroid Carcinoma
Medullary Thyroid Carcinoma This case was provided by Treant Hospital, Bethesda, Hoogeveen, The Netherlands ADS-01504 Rev. 001 2016 Hologic, Inc. All rights reserved. Overview Medullary Thyroid Carcinoma
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE. Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University
 EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
NPQR Quality Payment Program (QPP) Measures 21_18247_LS.
 NPQR Quality Payment Program (QPP) Measures 21_18247_LS MEASURE ID: QPP 99 MEASURE TITLE: Breast Cancer Resection Pathology Reporting pt Category (Primary Tumor) and pn Category (Regional Lymph Nodes)
NPQR Quality Payment Program (QPP) Measures 21_18247_LS MEASURE ID: QPP 99 MEASURE TITLE: Breast Cancer Resection Pathology Reporting pt Category (Primary Tumor) and pn Category (Regional Lymph Nodes)
SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES)
 SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES) Dr. Mariamma Joseph Professor of Pathology Division Head Cytopathology Department of Pathology and Laboratory Medicine LHSC and Western University
SELECTED DILEMMAS IN RESPIRATORY CYTOPATHOLOGY (2 CASES) Dr. Mariamma Joseph Professor of Pathology Division Head Cytopathology Department of Pathology and Laboratory Medicine LHSC and Western University
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events
 Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
CYTOPATHOLOGIC AND MOLECULAR DIAGNOSTIC ISSUES IN LUNG CYTOPATHOLOGY
 COMPANION MEETING Four Ps of Pulmonary Cytopathology: Procedural, Predictive, Personalized and Participatory CYTOPATHOLOGIC AND MOLECULAR DIAGNOSTIC ISSUES IN LUNG CYTOPATHOLOGY Prof. Fernando Schmitt
COMPANION MEETING Four Ps of Pulmonary Cytopathology: Procedural, Predictive, Personalized and Participatory CYTOPATHOLOGIC AND MOLECULAR DIAGNOSTIC ISSUES IN LUNG CYTOPATHOLOGY Prof. Fernando Schmitt
International Journal of Pharma and Bio Sciences CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY.
 Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Case Report Pathology International Journal of Pharma and Bio Sciences ISSN 0975-6299 CHROMOPHOBE VARIANT OF RENAL CELL CARCINOMA MASQUARDING AS RENAL ONCOCYTOMA ON CYTOLOGY. DR.MAMATHA K*, DR. ARAKERI
Pancreatic malignant tumors are the fifth leading cause of cancerrelated
 44 CANCER CYTOPATHOLOGY Cytologic Criteria for Well Differentiated Adenocarcinoma of the Pancreas in Fine-Needle Aspiration Biopsy Specimens Fan Lin, M.D., Ph.D. 1 Gregg Staerkel, M.D. 2 1 Department of
44 CANCER CYTOPATHOLOGY Cytologic Criteria for Well Differentiated Adenocarcinoma of the Pancreas in Fine-Needle Aspiration Biopsy Specimens Fan Lin, M.D., Ph.D. 1 Gregg Staerkel, M.D. 2 1 Department of
Accuracy of cell typing in nonsmall cell lung cancer by EBUS/EUS FNA cytological samples
 Eur Respir J 2011; 38: 911 917 DOI: 10.1183/09031936.00176410 CopyrightßERS 2011 Accuracy of cell typing in nonsmall cell lung cancer by EBUS/EUS FNA cytological samples W.A.H. Wallace* and D.M. Rassl
Eur Respir J 2011; 38: 911 917 DOI: 10.1183/09031936.00176410 CopyrightßERS 2011 Accuracy of cell typing in nonsmall cell lung cancer by EBUS/EUS FNA cytological samples W.A.H. Wallace* and D.M. Rassl
Immunohistochemical Evaluation of Necrotic Malignant Melanomas
 Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Anatomic Pathology / EVALUATION OF NECROTIC MALIGNANT MELANOMAS Immunohistochemical Evaluation of Necrotic Malignant Melanomas Daisuke Nonaka, MD, Jordan Laser, MD, Rachel Tucker, HTL(ASCP), and Jonathan
Reparatory system lectures Heyam Awad
 Reparatory system lectures 8-10 Heyam Awad note These lectures cover the following topics 1. Diffuse hemorrhagic syndromes 2. Lung tumors important: theses slides are your study source for these lectures.
Reparatory system lectures 8-10 Heyam Awad note These lectures cover the following topics 1. Diffuse hemorrhagic syndromes 2. Lung tumors important: theses slides are your study source for these lectures.
Fine-Needle Aspiration and Cytologic Findings of Surgical Scar Lesions in Women With Breast Cancer
 148 Fine-Needle Aspiration and Cytologic Findings of Surgical Scar Lesions in Women With Breast Cancer Ehud Malberger, DMD, FIAC,* Yeouda Edoute, MD, PhD,t Osnaf Toledano, MD,* and Dov Sapir, MDS Benign
148 Fine-Needle Aspiration and Cytologic Findings of Surgical Scar Lesions in Women With Breast Cancer Ehud Malberger, DMD, FIAC,* Yeouda Edoute, MD, PhD,t Osnaf Toledano, MD,* and Dov Sapir, MDS Benign
Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms
 Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Updated Molecular Testing Guideline for the Selection of Lung Cancer Patients for Treatment with Targeted Tyrosine Kinase Inhibitors
 Q: How is the strength of recommendation determined in the new molecular testing guideline? A: The strength of recommendation is determined by the strength of the available data (evidence). Strong Recommendation:
Q: How is the strength of recommendation determined in the new molecular testing guideline? A: The strength of recommendation is determined by the strength of the available data (evidence). Strong Recommendation:
Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms
 Hindawi Publishing Corporation Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Hindawi Publishing Corporation Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Update on 2015 WHO Classification of Lung Adenocarcinoma 1/3/ Mayo Foundation for Medical Education and Research. All rights reserved.
 1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
Neuroendocrine (NE) lung tumors represent a broad
 Large Cell Neuroendocrine Carcinoma of the Lung: A 10-Year Clinicopathologic Retrospective Study Massimiliano Paci, MD, Alberto Cavazza, MD, Valerio Annessi, MD, Innocenza Putrino, MD, Guglielmo Ferrari,
Large Cell Neuroendocrine Carcinoma of the Lung: A 10-Year Clinicopathologic Retrospective Study Massimiliano Paci, MD, Alberto Cavazza, MD, Valerio Annessi, MD, Innocenza Putrino, MD, Guglielmo Ferrari,
Villoglandular adenocarcinoma of cervix a tumour with bland cytological features: report of a case missed on cytology
 Malaysian J Pathol 2003; 25(2) : CERVICAL 139 143 VILLOGLANDULAR ADENOCARCINOMA CYTOLOGY CASE REPORT Villoglandular adenocarcinoma of cervix a tumour with bland cytological features: report of a case missed
Malaysian J Pathol 2003; 25(2) : CERVICAL 139 143 VILLOGLANDULAR ADENOCARCINOMA CYTOLOGY CASE REPORT Villoglandular adenocarcinoma of cervix a tumour with bland cytological features: report of a case missed
Human Papillomavirus Testing in Head and Neck Carcinomas
 Human Papillomavirus Testing in Head and Neck Carcinomas Guideline from the College of American Pathologists Early Online Release Publication: Archives of Pathology & Laboratory Medicine 12/18/2017 Overview
Human Papillomavirus Testing in Head and Neck Carcinomas Guideline from the College of American Pathologists Early Online Release Publication: Archives of Pathology & Laboratory Medicine 12/18/2017 Overview
Non Small Cell Lung Cancer Histopathology ד"ר יהודית זנדבנק
 Non Small Cell Lung Cancer Histopathology ד"ר יהודית זנדבנק 26.06.09 Lecture outlines WHO histological classification Macro/Micro assessment Early diagnosis Minimal pathology Main subtypes SCC, AdCa, LCLC
Non Small Cell Lung Cancer Histopathology ד"ר יהודית זנדבנק 26.06.09 Lecture outlines WHO histological classification Macro/Micro assessment Early diagnosis Minimal pathology Main subtypes SCC, AdCa, LCLC
Concordance of cytology and histopathology of intra-thoracic lesions
 Original article: Concordance of cytology and histopathology of intra-thoracic lesions *Dr.Prasanthi cherukuri 1, Dr.B.V.Madhavi 2 1Assitant Proferssor, Gitam institute of Medical sciences and research,visakhapatnam,
Original article: Concordance of cytology and histopathology of intra-thoracic lesions *Dr.Prasanthi cherukuri 1, Dr.B.V.Madhavi 2 1Assitant Proferssor, Gitam institute of Medical sciences and research,visakhapatnam,
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018
 Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Diagnostic accuracy of percutaneous renal tumor biopsy May 10 th 2018 Dr. Tzahi Neuman Dep.Of Pathology Hadassah Medical Center Jerusalem, Israel, (tneuman@hadassah.org.il) Disclosure: 1 no conflicts of
Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT
 Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT during follow- up. ALT, AST, Alk Phos and bilirubin were
Case: The patient is a 62 year old woman with a history of renal cell carcinoma that was removed years ago. A 2.4 cm liver mass was found on CT during follow- up. ALT, AST, Alk Phos and bilirubin were
Combined Large Cell Neuroendocrine Carcinoma and Spindle Cell Carcinoma of the Lung
 Case Reports Jpn J Clin Oncol 2011;41(6)797 802 doi:10.1093/jjco/hyr034 Advance Access Publication 16 March 2011 Combined Large Cell Neuroendocrine Carcinoma and Spindle Cell Carcinoma of the Lung Taichiro
Case Reports Jpn J Clin Oncol 2011;41(6)797 802 doi:10.1093/jjco/hyr034 Advance Access Publication 16 March 2011 Combined Large Cell Neuroendocrine Carcinoma and Spindle Cell Carcinoma of the Lung Taichiro
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Radiology Pathology Conference
 Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Mody. AIS vs. Invasive Adenocarcinoma of the Cervix
 Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
ROBINSON CYTOLOGICAL GRADING OF BREAST CARCINOMA ON FINE NEEDLE ASPIRATION CYTOLOGY- AN OVERVIEW
 Page564 Research Article Biological Sciences ROBINSON CYTOLOGICAL GRADING OF BREAST CARCINOMA ON FINE NEEDLE ASPIRATION CYTOLOGY- AN OVERVIEW Charusheela Rajesh Gore, Chandanwale Shirish S, Ruchika Aggarwal,
Page564 Research Article Biological Sciences ROBINSON CYTOLOGICAL GRADING OF BREAST CARCINOMA ON FINE NEEDLE ASPIRATION CYTOLOGY- AN OVERVIEW Charusheela Rajesh Gore, Chandanwale Shirish S, Ruchika Aggarwal,
Insulinoma-associated protein (INSM1) is a sensitive and specific marker for lung neuroendocrine tumors in cytologic and surgical specimens
 Insulinoma-associated protein (INSM1) is a sensitive and specific marker for lung neuroendocrine tumors in cytologic and surgical specimens Kartik Viswanathan, M.D., Ph.D New York Presbyterian - Weill
Insulinoma-associated protein (INSM1) is a sensitive and specific marker for lung neuroendocrine tumors in cytologic and surgical specimens Kartik Viswanathan, M.D., Ph.D New York Presbyterian - Weill
Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings
 Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings Touhid Uddin Rupom 1, Tamanna Choudhury 2, Sultana Gulshana Banu 3
Study of Fine Needle Aspiration Cytology of Breast Lump: Correlation of Cytologically Malignant Cases with Their Histological Findings Touhid Uddin Rupom 1, Tamanna Choudhury 2, Sultana Gulshana Banu 3
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
INTRODUCTION TO PATHOLOGICAL TECHNIQUES. 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH)
 INTRODUCTION TO PATHOLOGICAL TECHNIQUES 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH) Biopsy-Indications Diffuse/multifocal lesions (neoplastic, inflammatory, etc) Etiology of the
INTRODUCTION TO PATHOLOGICAL TECHNIQUES 1. Types of routine biopsy procedures 2. Special exams (IHC, FISH) Biopsy-Indications Diffuse/multifocal lesions (neoplastic, inflammatory, etc) Etiology of the
Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis
 1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Synchronous squamous cell carcinoma of the breast. and invasive lobular carcinoma
 Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Ground Glass Opacities
 Ground Glass Opacities A pathologist s perspective Marie-Christine Aubry, M.D. Professor of Pathology Mayo Clinic Objectives Discuss the proposed new pathologic classification of adenocarcinoma with historical
Ground Glass Opacities A pathologist s perspective Marie-Christine Aubry, M.D. Professor of Pathology Mayo Clinic Objectives Discuss the proposed new pathologic classification of adenocarcinoma with historical
Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination
 Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Histology: Its Influence on Therapeutic Decision Making
 Histology: Its Influence on Therapeutic Decision Making Mark A. Socinski, MD Professor of Medicine and Thoracic Surgery Director, Lung Cancer Section, Division of Hematology/Oncology Co-Director, UPMC
Histology: Its Influence on Therapeutic Decision Making Mark A. Socinski, MD Professor of Medicine and Thoracic Surgery Director, Lung Cancer Section, Division of Hematology/Oncology Co-Director, UPMC
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens
 ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
CINtec p16 INK4a Staining Atlas
 CINtec p16 INK4a Staining Atlas Rating Rating Positive The rating positive will be assigned if the p16 INK4a -stained slide shows a continuous staining of cells of the basal and parabasal cell layers of
CINtec p16 INK4a Staining Atlas Rating Rating Positive The rating positive will be assigned if the p16 INK4a -stained slide shows a continuous staining of cells of the basal and parabasal cell layers of
Potential Pitfalls for False Suspicion of Papillary Thyroid Carcinoma:
 SUPPLEMENT 1 SPECIAL ISSUE: CYTOPATHOLOGY OF THE THYROID GLAND Guest Editor: Zubair Baloch Potential Pitfalls for False Suspicion of Papillary Thyroid Carcinoma: A Cytohistologic Review of 22 Cases Xin
SUPPLEMENT 1 SPECIAL ISSUE: CYTOPATHOLOGY OF THE THYROID GLAND Guest Editor: Zubair Baloch Potential Pitfalls for False Suspicion of Papillary Thyroid Carcinoma: A Cytohistologic Review of 22 Cases Xin
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT?
 POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
Role of fine needle aspiration cytology and cytohistopathological co-relation in thyroid lesions: experience at a tertiary care centre of North India
 International Journal of Research in Medical Sciences Chandra S et al. Int J Res Med Sci. 2016 Oct;4(10):4552-4556 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20163328
International Journal of Research in Medical Sciences Chandra S et al. Int J Res Med Sci. 2016 Oct;4(10):4552-4556 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20163328
57th Annual HSCP Spring Symposium 4/16/2016
 An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance
 & 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
& 2006 USCAP, Inc All rights reserved 0893-3952/06 $30.00 www.modernpathology.org Intraductal carcinoma of the prostate on needle biopsy: histologic features and clinical significance Charles C Guo 1 and
Pitfalls in thyroid tumor pathology. Prof.Valdi Pešutić-Pisac MD, PhD
 Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Fine-Needle Aspiration Cytology in the Diagnosis of Lymphoma The Next Step
 Fine-Needle Aspiration Cytology in the Diagnosis of Lymphoma The Next Step Linda M. Sandhaus, MD Since 985, almost 2 articles have been published in the medical literature on the subject of fine-needle
Fine-Needle Aspiration Cytology in the Diagnosis of Lymphoma The Next Step Linda M. Sandhaus, MD Since 985, almost 2 articles have been published in the medical literature on the subject of fine-needle
Workshop for O& G trainees and paramedics 17 Dec 2011 Cytological Interpretation
 Workshop for O& G trainees and paramedics 17 Dec 2011 Cytological Interpretation May Yu Director of Cytology Laboratory Service Department of Anatomical & Cellular Pathology Prince of Wales Hospital Cervical
Workshop for O& G trainees and paramedics 17 Dec 2011 Cytological Interpretation May Yu Director of Cytology Laboratory Service Department of Anatomical & Cellular Pathology Prince of Wales Hospital Cervical
Neoplasia 2018 Lecture 2. Dr Heyam Awad MD, FRCPath
 Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
Neoplasia 2018 Lecture 2 Dr Heyam Awad MD, FRCPath ILOS 1. List the differences between benign and malignant tumors. 2. Recognize the histological features of malignancy. 3. Define dysplasia and understand
Prepared By Jocelyn Palao and Layla Faqih
 Prepared By Jocelyn Palao and Layla Faqih The structure of the suspected atypical cell should always be compared to the structure of other similar, benign, cells which are present in the smears. The diagnosis
Prepared By Jocelyn Palao and Layla Faqih The structure of the suspected atypical cell should always be compared to the structure of other similar, benign, cells which are present in the smears. The diagnosis
Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination
 Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE:
Quality ID #395: Lung Cancer Reporting (Biopsy/Cytology Specimens) National Quality Strategy Domain: Communication and Care Coordination 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE:
ACCME/Disclosures. Cribriform Lesions of the Prostate. Case
 Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Gynecologic Cytopathology: Glandular lesions
 Gynecologic Cytopathology: Glandular lesions Lin Wai Fung (MSc, MPH, CMIAC) 17/4/2014 Glandular lesions of the uterus Endocervix Endometrium Normal endocervical cells Sheets, strips well-preserved architecture:
Gynecologic Cytopathology: Glandular lesions Lin Wai Fung (MSc, MPH, CMIAC) 17/4/2014 Glandular lesions of the uterus Endocervix Endometrium Normal endocervical cells Sheets, strips well-preserved architecture:
Predictors of Malignancy in Thyroid Fine-Needle Aspirates Cyst Fluid Only Cases
 Predictors of Malignancy in Thyroid Fine-Needle Aspirates Cyst Fluid Only Cases Can Potential Clues of Malignancy Be Identified? Mohammad Jaragh, MD 1 ; V. Bessie Carydis, MMedSci (Cytol) 1 ; Christina
Predictors of Malignancy in Thyroid Fine-Needle Aspirates Cyst Fluid Only Cases Can Potential Clues of Malignancy Be Identified? Mohammad Jaragh, MD 1 ; V. Bessie Carydis, MMedSci (Cytol) 1 ; Christina
Overview of Indeterminate Cytology
 83 rd Annual Meeting American Thyroid Association Overview of Indeterminate Cytology Scott Boerner MD FRCPC Head Cytopathology, University Health Network University of Toronto DISCLOSURE Nothing to disclose
83 rd Annual Meeting American Thyroid Association Overview of Indeterminate Cytology Scott Boerner MD FRCPC Head Cytopathology, University Health Network University of Toronto DISCLOSURE Nothing to disclose
ORIGINAL ARTICLE. Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population
 ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
ORIGINAL ARTICLE Fine-Needle Aspiration Biopsy of Salivary Gland Lesions in a Selected Patient Population Erik G. Cohen, MD; Snehal G. Patel, MD; Oscar Lin, MD; Jay O. Boyle, MD; Dennis H. Kraus, MD; Bhuvanesh
Abstract. Introduction. Salah Abobaker Ali
 Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology
 New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology United States and Canadian Academy of Pathology 102 nd Annual Meeting Baltimore, Maryland Christina S. Kong, M.D.
New Diagnoses Need New Approaches: A Glimpse into the Near Future of Gynecologic Pathology United States and Canadian Academy of Pathology 102 nd Annual Meeting Baltimore, Maryland Christina S. Kong, M.D.
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma
 Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
Lessons From Cases of Screened Women Who Developed Cervical Carcinoma R. Marshall Austin MD,PhD Magee-Womens Hospital of University of Pittsburgh Medical Center raustin@magee.edu Why Focus Study On Cases
Histological Typing Of Cancer And Precancer Of The Oral Mucosa
 Histological Typing Of Cancer And Precancer Of The Oral Mucosa 1 / 7 2 / 7 3 / 7 Histological Typing Of Cancer And Within the last decade, histologic grading has become widely accepted as a powerful indicator
Histological Typing Of Cancer And Precancer Of The Oral Mucosa 1 / 7 2 / 7 3 / 7 Histological Typing Of Cancer And Within the last decade, histologic grading has become widely accepted as a powerful indicator
Difficult Diagnoses and Controversial Entities in Neoplastic Lung
 Difficult Diagnoses and Controversial Entities in Neoplastic Lung Lynette M. Sholl, M.D. Associate Pathologist, Brigham and Women s Hospital Chief, Pulmonary Pathology Service Associate Professor, Harvard
Difficult Diagnoses and Controversial Entities in Neoplastic Lung Lynette M. Sholl, M.D. Associate Pathologist, Brigham and Women s Hospital Chief, Pulmonary Pathology Service Associate Professor, Harvard
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
DETERMINATION OF A LYMPHOID PROCESS
 Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
Chapter 2 Applications of Touch Preparation Cytology to Intraoperative Consultations: Lymph Nodes and Extranodal Tissues for Evaluation of Hematolymphoid Disorders INTRODUCTION As discussed in Chap. 1,
