Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery?
|
|
|
- Francine Welch
- 5 years ago
- Views:
Transcription
1 Ulster Med J 2019;88(1):10-14 Grand Rounds Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery? Jennifer E Tham 1, Benjamin Tharian 2, Patrick B Allen 1, Gary Spence 1, Tony C Tham 1 Accepted: 12 th of October 2017 Provenance: externally peer-reviewed ABSTRACT For oesophageal cancer patients with potentially curative disease, treatment usually comprises neoadjuvant chemoradiotherapy followed by surgery. Several methods are currently used for nutritional support while patients are undergoing neoadjuvant treatment but these do not relieve dysphagia. Stenting as a bridge to curative surgery has been explored in several case series and a case control study. This is a review of the current literature on the topic. Some small series have shown it to be safe and effective in relieving dysphagia and malnutrition without adverse effect on surgical outcomes, perioperative complications or delay in surgical resection post neoadjuvant therapy. However, there are sufficient concerns about its adverse impact on oncological outcomes such as a reduction in the R0 resection rates, median time to recurrence and 2-3 year overall survival, to not currently recommend its routine use in resectable cancers. INTRODUCTION For patients with potentially curative oesophageal cancer, there is a risk that a compromised nutritional state can extend through the period of tumour staging to the commencement of neoadjuvant treatment, leading to treatment delays, poorer response and an adverse impact on the long term prognosis and surgical outcome 1. Several methods are currently used for nutritional support. These include enteral feeding via nasogastric or nasojejunal tubes, percutaneous gastrostomy (PEG) and jejunostomy (PEG-J) tubes, parenteral nutrition via central venous access, as well as aggressive oral supplementation under dietetic review 1-4. All of these methods have significant limitations as they do not relieve dysphagia, which decreases quality of life. In addition, there is the risk of aspiration pneumonia, surgical compromise of the stomach, dislodgement and risk of central line infection and thrombosis, thrombophlebitis, liver failure and prohibitive cost of parenteral nutrition 2. The concept of employing stents (partially or fully covered self-expanding metal stents (SEMS) or plastic/biodegradable) as a bridge to curative surgery has been explored in several case series and a case control study 5-8. The principle is that the stent will relieve or improve dysphagia allowing an increase in oral intake, an improvement in nutritional status and possibly surgical outcome. There is a general reluctance to stent operable candidates, possibly due to poor knowledge about outcome, which is why we decided to review the literature. METHODS We included only articles on the use of oesophageal stents in operable cancer in the main discussion, though references have been occasionally made to others when there was no relevant information available. Scientific papers published between 1990 and 2015 were searched for in PubMed, EMBASE, Cochrane Library and Medline; the key words were (o) esophageal stent, surgery, resectable cancer and (o)esophageal cancer. In addition, a search of the references within papers was made to identify other studies. English and non-english sources were reviewed, though the relevant studies included were all in English. Manual searching was also done. Grey literature including non-indexed journals, proceedings and posters from international meetings were also included in the initial review. Two independent reviewers (TCKT and JEJT) scrutinised all the studies with regards to the inclusion criteria and quality. The overall results were assessed by all authors for their robustness and conclusions were discussed to avoid any bias before arriving at a consensus. RESULTS We identified 15 studies that evaluated the role of stents as a bridge to surgery 3-5, Three systematic reviews were also available. There are several key questions to be addressed with regards to oesophageal stents being used as a bridge. We have tried to critically review these studies and discuss each question in this context. WHAT IS THE EFFICACY OF OESOPHAGEAL STENTING IN RELIEVING DYSPHAGIA? Dysphagia is the commonest indication for stenting this subgroup of patients, being the predominant indication in up to 95% of patients in some studies 5. It is important to evaluate 1. Division of Gastroenterology and Surgery, Ulster Hospital, Belfast; Northern Ireland 2. University of Arkansas Medical Sciences, Little Rock, USA. Correspondence to: Dr Tony Tham tctham1234@gmail.com
2 Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery? 11 the efficacy of stenting from the point of view of procedural success, and relief of dysphagia. Most of the studies discussed below included subjective scoring of dysphagia at initial presentation, ranging from no dysphagia through solid, mixed and liquid dysphagia to total dysphagia. Alder et al, conducted a prospective non-randomised study of 13 patients who underwent EUS (endoscopic ultrasound) followed by stent placement 15. The dysphagia scores significantly improved post stent insertion. The study concluded that oesophageal stent insertion was safe and permitted adequate oral feeding though at the cost of risk of migration (6 in 13 patients, 43%). Martin, et al performed a small prospective study of 5 patients who received oesophageal stents prior to receiving neoadjuvant chemotherapy 16. Stent placement was successful in all 5 cases (100%) with optimal calorific needs met within 2 hours. Siddiqui et al performed a retrospective, non-randomised study of 6 patients with malignant strictures who underwent oesophageal stent placement before receiving neoadjuvant chemo radiation 21. Of the 6 patients, stent placement was successful in 5 (83%). Pellen et al conducted a study of 16 patients who received a self-expanding removable metal stent (SERMS) during neoadjuvant therapy 10. There was a significant fall in mean dysphagia score from 2.5 (range 1-4) to 1.1 (range 0-3) immediately preoperatively. Langer et al conducted a study of 38 patients, who had stents inserted, before undergoing neo-adjuvant chemo radiotherapy of 38 (97.4%) patients had immediate dysphagia relief. Brown et al prospectively evaluated the use of self-expanding plastic stents (SEPS) during neoadjuvant therapy 12. Lopes et al conducted a study of 11 patients who received SEMS prior to neoadjuvant therapy 13. Dysphagia significantly improved compared to baseline in both these studies. Griffiths, et al 17 evaluated a cohort of 22 patients who received biodegradable oesophageal stents (BD SX ELLA) of whom 9 had oesophageal malignancy. The insertion was successful in 21/22 (96%) of their patients with a significant improvement in dysphagia scores at a median of 47 days. Park, et al 19 evaluated the clinical efficacy of temporary placement of a retrievable expandable metallic stent during preoperative neoadjuvant chemoradiotherapy. Stent placement was technically successful in all patients with 24 of 25 (96%) showing symptomatic improvement. Stents were removed electively 32 days after starting neoadjuvant chemoradiotherapy or after stent migration and exit through the anus. The dysphagia score improved from 3.1 by 3 days after stent placement to 1.3 and was maintained up to 1 month after stent removal. Van den Berg, et al 20 included 10 patients who underwent biodegradable stent placement (BD ELLA) before neoadjuvant chemoradiotherapy. Technical and clinical success rates were 100% each. Mean dysphagia score improved significantly, 3 to 1.13 pre and post stent insertion, p < A systematic review and meta-analysis conducted by Nagaraja, et al 22 found a substantial decrease in dysphagia scores (standard error 0.15, 95% CI, -1.1 to -0.51). This review included nine of our fifteen studies. Are oesophageal stents effective in management of malnutrition? Van den Berg et al showed that although biodegradable stent placement as a bridge to surgery prior to neoadjuvant treatment resulted in improved dysphagia scores, it appeared to hamper oral intake, resulting in significant weight loss, needing additional nutritional interventions 20. In contrast Siddiqui, et al 4 showed that albumin levels and weight increased significantly with both plastic stent (PS) and surgical jejunostomy (JT). There were no significant differences between groups in the procedural success rates (PS 92% vs. JT 100%, P = 0.33), complication rates (PS 22% vs. JT 4%, P = 0.11), mean increase in weight (PS 4.4 kg vs. JT 4.2 kg, P = 0.59), and mean increase in serum albumin (PS 0.62 g/dl vs. JT 0.44 g/dl, P = 0.05). In a review of a prospective database by Bower, et al, the silicone stent group demonstrated greater mean improvement in albumin levels (0.14 g/dl vs g/dl vs g/dl, P<.001) and less percentage body weight loss (1.5% vs. 4.2% vs. 5.5%, P<.001) compared with the groups with feeding tubes and oral nutrition. Nagaraja et al conducted a meta-analysis of the literature. They found a substantial increase in weight (SE 0.434, 95% CI, to 1.442) and albumin (SE 0.271, 95% CI, to 0.881) standard difference in means 22. WHAT ARE THE COMPLICATIONS OF STENTING RESECTABLE OESOPHAGEAL CANCER? Stent migration varied from 20% in the study by Martin, et al (removed without complication at the time of operation 16 to 60% in the study by Siddiqui, et al (all successfully removed endoscopically or at the time of surgery) 22. Stentrelated morbidity occurred in 4/16 (25%) patients and migration occurred in 7/16 (44%) in the study by Pellen, et al, though all were resolved endoscopically with no stentrelated mortality 10. A meta-analysis of stents for resectable oesophageal cancer concluded that stent migration occurred in 1 patient causing jejunal perforation (2.6%), tracheooesophageal fistula in 2 (5.2%) and significant bleeding 1 (2.6%); delayed complications occurred in three (7.89%) ie tracheo-oesophageal fistula and recurrent dysphagia 22. Griffiths, et al reported of 9 patients who had biodegradable stents, one (11%) required reinsertion of a self expanding metal stent at 2 months and 2 (22%) required supplementary feeding via jejunostomy and a fine bore nasojejunal tube within 12 weeks of stenting. Van den Berg, et al 20 used biodegradable stents, with an adverse event rate of 70%. Retrosternal pain developed in 6 patients and persisted for a median of 12 days. Stent obstruction occurred in one patient because of necrotic tissue.
3 12 The Ulster Medical Journal Table: Summary of the results of the use of self expanding stents as a bridge to surgery in oesophageal cancer SEMS = Self expanding metal stent; SEPS = Self expanding plastic stent, BDS = Biodegradable stent, REMS = Retrievable expandable metallic stent Author Year Type of stent Number of patients Number who had surgical resection (%) Number of stent related complications (%) Mariette SEMS (100%) Not reported Krokidis SEPS 11 1 (9%) 5 (45%) Pellen SEMS (63%) 8 (50%) Siddiqui SEMS 55 8 (15%) 19 (35%) Brown SEPS (63%) 10 (31%) Lopes SEMS 11 2 (18%) 5 (45%) Langer SEMS-25, SEPS (53%) 18 (47%) Adler SEPS 13 3 (23%) 6 (46%) Bower SEPS (56%) 6 (24%) Martin SEPS 5 Not reported 1 (20%) Siddiqui SEPS 12 Not reported 4 (33%) Griffiths BDS 9 3 (33%) 3 (33%) Kjaer SEMS 63 All R0 (this was the group from which the patients who had stents were identified) Not reported Park REMS 25 Not reported Not reported Van den Berg BDS 10 7 (70%) 7 (70%) Siddiqui SEPS 6 100% 3 (60%) The systemic review by Nagaragi et al noted the incidence of major adverse events including stent migration as 32% and chest discomfort as 51.4% 22. The authors in this review recommend stents for dysphagia prior to or during neoadjuvant chemotherapy but seem to underestimate the impact of the complications and did not adequately assess the disadvantages of stenting preoperatively as they considered stent migration not to be a disadvantage but rather an indicator of tumour reduction. A review by Jones and Griffiths 23 came to the conclusion that there can be significant complications in a small proportion of patients which can compromise opportunity for curative surgery. HAS STENTING BEEN COMPARED TO STANDARD OPTIONS SUCH AS NASOGASTRIC OR NASOJEJUNAL FEEDING AND GASTROSTOMY OR JEJUNOSTOMY? Only two studies to date have compared stenting to standard treatments. Bower, et al conducted a retrospective study comparing nutritional support methods in patients undergoing neoadjuvant chemo radiotherapy 3. This study compared the outcomes of oesophageal stenting, feeding tubes and oral diets. 25 patients received stents, 19 patients had feeding tubes inserted and 14 patients were maintained on oral diet only. The group of patients who received oesophageal stents had a lower rate of interruption of chemo radiotherapy (8% vs. 29% vs. 47%, P=0.011), greater mean improvement of albumin (0.14 g/dl vs g/dl vs g/dl, P<0.001), less percentage body weight loss (1.5% vs. 4.2% vs. 5.5%, P<0.001) and a reduction in major operative complications (20% vs. 47% vs. 43% among stent, feeding tube, and oral nutrition respectively (P=0.130). As mentioned earlier, Siddiqui, et al showed that plastic stents were a safe and effective alternative to surgical jejunostomy for maintaining nutrition in this subset of patients undergoing neoadjuvant chemo radiotherapy 4. DOES STENTING COMPROMISE SUBSEQUENT SURGERY AND ONCOLOGICAL OUTCOMES? Studies have shown that interval disease progression as a direct consequence of SEMS could adversely affect the treatment plan of 30 to 85%. 3,12,14 Mariette et al conducted a retrospective study of 2944 patients in a multicentre European cohort, who underwent oesophageal resection over a period of ten years 5. They evaluated the oncologic impact of covered SEMS when used as a bridge to surgery. A total of 38 patients had SEMS inserted. SEMS insertion was complicated by perforation in 2 cases. The study also found that postoperative mortality (13.2% vs 8.6%) and morbidity rates (63.2% vs 59.2%) were increased in the SEMS group compared to the control group respectively. They found a significant reduction in the R0 resection rate (71% vs 85.5%; p=0.041), median time to recurrence (6.5 vs 9 months) and the 3-year overall survival (25% vs 44%) in the SEMS group compared to the control.
4 Oesophageal Stents for Potentially Curable Oesophageal Cancer A Bridge to Surgery? 13 Griffiths, et al 17 found that in nine patients who had biodegradable stents, 6 (66%) did not proceed to surgery; 1 (11%) because of disease progression, two (22%) because of failure to gain weight and three (33%) because they became unfit for surgery. The additional 3 (33%) did progress to surgery but were not resected due to the recognition of disseminated disease. In the other biodegradable stent study by van den Berg 20, 4 of 10 patients did not undergo surgery because of fatal pneumonia, liver metastases, poor performance status and insertion of a self expanding metal stent for a post radiation stricture, respectively. A retrospective cohort study from a prospectively maintained national database in Denmark identified all patients treated without neoadjuvant therapy that had an R0 resection 18. Of these 63 patients had a stent as a bridge to surgery. The outcomes from these patients were compared to 211 who did not have a stent. The median survival in the stent group was significantly lower than the non-stent group by 11.6 months and 21.3 months respectively. Non-stent group exhibited a significantly better two year survival with a median recurrence free survival of 9.1 months for the stent group compared with 15.2 months for the non-stent group. ARE THERE ANY DIFFERENCES DEPENDING ON THE TYPES OF STENTS USED? Krokidis, et al conducted a prospective study to evaluate the use of biodegradable oesophageal stents in malignant oesophageal strictures as a bridge to surgery 9. In this study 11 patients had a woven polydioxanone degradable oesophageal stent inserted. Stent deployment was successful in all patients. However, early complications occurred in 3 patients that resulted in failure to restore oral nutrition. Stent dysfunction occurred in 5 of 8 patients (62.5%). In 2 of the 5 patients this was due to a local inflammatory reaction and in the remaining 3, this was due to tumour ingrowth. Subsequently a new metallic stent was inserted in 4 of the 5 patients. At the end of follow-up only 3 of 8 oesophageal stents were patent. This study demonstrates that biodegradable oesophageal stents do not appear to have benefit in malignant strictures. Two other studies on biodegradable stents. 17,20 also do not show good outcomes in terms of surgical resection and stent related complications. Five studies have evaluated self-expanding plastic stents (SEPS) 3,4,15,16,21 and three studies 10,11,13 have evaluated selfexpanding metal stents (SEMS). One study combined both SEPS and SEMS 14. There did not appear to be any differences in outcomes although there are no studies comparing these two. Two studies looked at the concept of removing stents prior to surgery with self expanding plastic stents 19,21 but there was no clear benefit. WHAT ABOUT COST-EFFECTIVENESS? To date, no studies have evaluated cost effectiveness as a bridge to neoadjuvant therapy and surgery in oesophageal cancers. DISCUSSION In summary, although stents are effective in relieving dysphagia in resectable tumours, significant complications are common such as perforation and fistula, with one study showing increased postoperative mortality and morbidity. Although a systematic review 22 found that stents before neoadjuvant therapy result in an increase in weight and albumin, biodegradable stents appear to hamper oral intake resulting in weight loss needing additional nutritional interventions 20. Stent insertion before surgery was found to be a predictor of poor prognosis after adjusting for confounding factors in the study by Mariette, et al 5. The reasons suggested include peri-stent fibrosis secondary to expansive radial forces, compromising the normal planes of dissection and therefore the resectability 24,25 ; fixating spurs causing micro perforations and dissemination 26 ; inability to accurately restage tumours after stent insertion making it difficult to identify the tumours that progress and become unresectable. However this study has limitations. This retrospective study did not evaluate patients who underwent stent insertion and did not benefit from surgery due to tumour progression or stent-related fistula. In addition, it is a small study with only 38 cases of SEMS insertion. The findings from this study are supported by a larger similar study from Denmark 18 of 63 patients who underwent stenting prior to surgery. In this study, only patients who underwent an R0 resection were selected. They too found that the two year survival and recurrence-free survival was decreased in the stent group compared with those who did not have a stent. Although stents appear to be effective in relieving dysphagia prior to surgery, there are major concerns about its adverse impact on oncological outcomes. The European Society of Gastrointestinal Endoscopy (ESGE) clinical guidelines 28 for the use of oesophageal stenting in benign and malignant disease do not recommend the use of stent placement as a bridge to surgery or prior to preoperative chemo-radiotherapy due to a high incidence of adverse events and the availability of safer feeding options. 29. The review by Jones and Griffiths 23 also came to the same conclusion. CONCLUSION With the limited available data on this topic, we can conclude that although stenting appears to be effective in relieving dysphagia and addressing malnutrition prior to surgery, there are currently sufficient concerns about its adverse impact on oncological outcomes, to not recommend its routine use in resectable patients. Well-designed randomised prospective trials are required but are unlikely to happen because of concern about adverse oncological outcome. In our opinion, the use of oesophageal stents as a bridge to surgery should be confined to patients with dysphagia who cannot tolerate tube feeding or where a feeding gastrostomy or jejunostomy is contraindicated or not possible, or in the context of a clinical trial evaluating its role.
5 14 The Ulster Medical Journal REFERENCES 1. Mariette C, De Botton ML, Piessen G. Surgery in esophageal and gastric cancer patients: what is the role for nutrition support in your daily practice? Ann Surg Oncol. 2012;19(7): Tessier W, Piessen G, Briez N, Boschetto A, Sergent G, Mariette C. Percutaneous radiological gastrostomy in esophageal cancer patients: a feasible and safe access for nutritional support during multimodal therapy. Surg Endosc. 2013;27(2): Bower M, Jones W, Vessels B, Scoggins C, Martin R. Nutritional support with endoluminal stenting during neoadjuvant therapy for esophageal malignancy. Ann Surg Oncol. 2009;16(11): Siddiqui AA, Glynn C, Loren D, Kowalski T. Self-expanding plastic esophageal stents versus jejunostomy tubes for the maintenance of nutrition during neoadjuvant chemoradiation therapy in patients with esophageal cancer: a retrospective study. Dis Esophagus. 2009;22(3): Mariette C, Gronnier C, Duhamel A, Mabrut J-Y, Bail J-P, Carrere N, et al. Self-expanding covered metallic stent as a bridge to surgery in esophageal cancer: impact on oncologic outcomes. J Am Coll Surg. 2015;220(3): Duron V, Fadeku A, White R. Stent placement in esophageal cancer as a bridge to surgery: Short-term outcomes. Chest. 2011;140(4 Suppl):830A. 7. Sabbagh C, Browet F, Diouf M, Cosse C, Brehant O, Bartoli E, et al. Is stenting as a bridge to surgery an oncologically safe strategy for the management of acute, left-sided, malignant, colonic obstruction? A comparative study with a propensity score analysis. Ann Surg. 2013;258(1): Vleggaar FP. Stent placement in esophageal cancer as a bridge to surgery. Gastrointest Endosc. 2009;70(4): Krokidis M, Burke C, Spiliopoulos S, Gkoutzios P, Hynes O, Ahmed I, et al. The use of biodegradable stents in malignant oesophageal strictures for the treatment of dysphagia before neoadjuvant treatment or radical radiotherapy: a feasibility study. Cardiovasc Intervent Radiol. 2013;36(4): Pellen MGC, Sabri S, Razack A, Gilani SQ, Jain PK. Safety and efficacy of self-expanding removable metal esophageal stents during neoadjuvant chemotherapy for resectable esophageal cancer. Dis Esophagus. 2012;25(1): Siddiqui AA, Sarkar A, Beltz S, Lewis J, Loren D, Kowalski T, et al. Placement of fully covered self-expandable metal stents in patients with locally advanced esophageal cancer before neoadjuvant therapy. Gastrointest Endosc. 2012;76(1): Brown RE, Abbas AE, Ellis S, Williams S, Scoggins CR, McMasters KM, et al. A prospective phase II evaluation of esophageal stenting for neoadjuvant therapy for esophageal cancer: optimal performance and surgical safety. J Am Coll Surg. 2011;212(4):582 8; discussion Lopes TL, Eloubeidi MA. A pilot study of fully covered self-expandable metal stents prior to neoadjuvant therapy for locally advanced esophageal cancer. Dis Esophagus. 2010;23(4): Langer FB, Schoppmann SF, Prager G, Tomaselli F, Pluschnig U, Hejna M, et al. Temporary placement of self-expanding oesophageal stents as bridging for neo-adjuvant therapy. Ann Surg Oncol. 2010;17(2): Adler DG, Fang J, Wong R, Wills J, Hilden K. Placement of Polyflex stents in patients with locally advanced esophageal cancer is safe and improves dysphagia during neoadjuvant therapy. Gastrointest Endosc. 2009;70(4): Martin R, Duvall R, Ellis S, Scoggins CR. The use of self-expanding silicone stents in esophageal cancer care: optimal pre-, peri-, and postoperative care. Surg Endosc Mar;23(3): Griffiths EA, Gregory CJ, Pursnani KG, Ward JB, Stockwell RC. The use of biodegradable (SX-ELLA) oesophageal stents to treat dysphagia due to benign and malignant oesophageal disease. Surg Endosc. 2012;26(8): Kjaer DW, Nassar M, Jensen LS, Svendsen LB, Mortensen FV. A bridging stent to surgery in patients with esophageal and gastroesophageal junction cancer has a dramatic negative impact on patient survival: A retrospective cohort study through data acquired from a prospectively maintained national database. Dis Esophagus. 2017;30(3): Park JH, Song HY, Shin JH, Kim JH, Kim YH, Kim SB, Kim JH. Preliminary results of temporary placement of retrievable expandable metallic stents during preoperative neoadjuvant chemoradiotherapy in patients with resectable esophageal cancer. J Vasc Interv Radiol. 2015;26(6): van den Berg MW, Walter D, de Vries EM, Vleggaar FP, van Berge Henegouwen MI, van Hillegersberg R, et al. Biodegradable stent placement before neoadjuvant chemoradiotherapy as a bridge to surgery in patients with locally advanced esophageal cancer. Gastrointest Endosc. 2014;80(5): Siddiqui AA, Loren D, Dudnick R, Kowalski T. Expandable polyester silicon-covered stent for malignant esophageal strictures before neoadjuvant chemoradiation: a pilot study. Dig Dis Sci. 2007;52(3): Nagaraja V, Cox MR, Eslick GD. Safety and efficacy of esophageal stents preceding or during neoadjuvant chemotherapy for esophageal cancer: a systemic review and meta-analysis. J Gastrointest Oncol. 2014:5(2); Jones CM, Griffiths EA. Should oesophageal stents be used before neoadjuvant therapy to treat dysphagia in patients awaiting oesophagectomy? Best evidence topic (BET). Int J Surg. 12(2014): Sunde B, Ericson J, Kumagai K, Lundell L, Tsai JA, Lindblad M, et al. Relief of dysphagia during neoadjuvant treatment for cancer of the esophagus or gastroesophageal junction. Dis Esophagus. 2015;29(5): Hirdes MM, van Hooft JE, Wijrdeman HK, Hulshof MC, Fockens P, Reerink O, et al. Combination of biodegradable stent placement and single-dose brachytherapy is associated with an unacceptably high complication rate in the treatment of dysphagia from esophageal cancer. Gastrointest Endosc. 2012;76(2): Hirdes MM, Vleggaar FP, de Beule M, Siersema PD. In vitro evaluation of the radial and axial force of self-expanding esophageal stents. Endoscopy. 2013;45(12): Maruthachalam K, Lash GE, Shenton BK, Horgan AF. Tumour cell dissemination following endoscopic stent insertion. Br J Surg. 2007;94(9): Spaander MC, Baron TH, Siersema PD, Fuccio L, Schumacher B, Escorsell À, et al. Esophageal stenting for benign and malignant disease: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Endoscopy. 2016;48(10): Roy A, Kim M, Christein J, Varadarajulu S. Stenting versus gastrojejunostomy for management of malignant gastric outlet obstruction: comparison of clinical outcomes and costs. Surg Endosc. 2012;26(11):
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Biodegradable esophageal stents in benign and malignant strictures a single center experience
 E618 THIEME Biodegradable esophageal stents in benign and malignant strictures a single center experience Authors Institution Dimitrios E. Sigounas, Sandeep Siddhi, John N. Plevris Centre for Liver & Digestive
E618 THIEME Biodegradable esophageal stents in benign and malignant strictures a single center experience Authors Institution Dimitrios E. Sigounas, Sandeep Siddhi, John N. Plevris Centre for Liver & Digestive
Safety and efficacy of esophageal stents preceding or during neoadjuvant chemotherapy for esophageal cancer: a systematic review and meta-analysis
 Meta-Analysis Safety and efficacy of esophageal stents preceding or during neoadjuvant chemotherapy for esophageal cancer: a systematic review and meta-analysis Vinayak Nagaraja, Michael R. Cox, Guy D.
Meta-Analysis Safety and efficacy of esophageal stents preceding or during neoadjuvant chemotherapy for esophageal cancer: a systematic review and meta-analysis Vinayak Nagaraja, Michael R. Cox, Guy D.
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER
 November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
November 2015 DYSPHAGIA MANAGEMENT IN OESOPHAGEAL CANCER 1 Background... 3 2 Dysphagia Grading... 3 3 Dysphagia General Guidelines... 4 4 Modes of Managing Dysphagia... 4 4.1 Modified consistency diet...
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Colonic stenting anno 2014
 Jeanin E. van Hooft, MD, PhD Gastroenterologist Academic Medical Centre Dept. of Gastroenterology and Hepatology Amsterdam, Netherlands Annual meeting of Colonic Stent Safe Procedure Research Group May
Jeanin E. van Hooft, MD, PhD Gastroenterologist Academic Medical Centre Dept. of Gastroenterology and Hepatology Amsterdam, Netherlands Annual meeting of Colonic Stent Safe Procedure Research Group May
Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer
 Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer Authors: Eduardo Rodrigues-Pinto, Pedro Pereira, Todd H. Baron, Guilherme Macedo DOI: 10.17235/reed.2018.5323/2017
Title: Self-expandable metal stents are a valid option in long-term survivors of advanced esophageal cancer Authors: Eduardo Rodrigues-Pinto, Pedro Pereira, Todd H. Baron, Guilherme Macedo DOI: 10.17235/reed.2018.5323/2017
Douglas G. Adler MD. ACG Regional Postgraduate Course - Nashville, TN Copyright 2013 American College of Gastroenterology
 Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
The role of esophageal brachytherapy
 Esophageal cancer is combination with surgery (stents) or EBRT a better solution? Razvan Galalae, MD, PhD Associate Professor, Medical Faculty, Christian Albrecht University Kiel, Germany, and Head of
Esophageal cancer is combination with surgery (stents) or EBRT a better solution? Razvan Galalae, MD, PhD Associate Professor, Medical Faculty, Christian Albrecht University Kiel, Germany, and Head of
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
17. Oesophagus. Upper gastrointestinal cancer
 110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
110 17. Upper gastrointestinal cancer Oesophagus Radical treatment For patients with localised disease, the standard curative approach to treatment is either surgery + perioperative chemotherapy, surgery
Is a Metallic Stent Useful for Non Resectable Esophageal Cancer?
 Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Endoscopic Palliation of Malignant Dysphagia
 Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Endoscopic Palliation of Malignant Dysphagia 1. Scope of the guideline This guidance has been produced to support endoscopic palliation of malignant dysphagia from oesophageal cancer. 2. Guideline background
Colorectal stenting. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
Colorectal stenting Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Metal Stents for Obstructing Colorectal Cancer Dohomoto was credited as the first to report
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
FTS Oesophagectomy: minimal research to date 3,4
 Fast Track Programme in patients undergoing Oesophagectomy: A Single Centre 5 year experience Sullivan J, McHugh S, Myers E, Broe P Department of Upper Gastrointestinal Surgery Beaumont Hospital Dublin,
Fast Track Programme in patients undergoing Oesophagectomy: A Single Centre 5 year experience Sullivan J, McHugh S, Myers E, Broe P Department of Upper Gastrointestinal Surgery Beaumont Hospital Dublin,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
ESOPHAGEAL CANCER. Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds
 ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
ESOPHAGEAL CANCER Dr. Paul Gardiner December 17, 2002 Discipline of Surgery Rounds ESOPHAGEAL CANCER I. EPIDEMIOLOGY INCIDENCE, DIAGNOSIS & STAGING II. TREATMENT OPTIONS Current role of induction therapies
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
Jejunostomy after oesophagectomy, how and why I do it
 Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
CT PET SCANNING for GIT Malignancies A clinician s perspective
 CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
CT PET SCANNING for GIT Malignancies A clinician s perspective Damon Bizos Head, Surgical Gastroenterology Charlotte Maxeke Johannesburg Academic Hospital Case presentation 54 year old with recent onset
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
The Medline search yielded 43 hits, while the search in the CDSR yielded no additional Cochrane reviews.
 KEY QUESTION 5 1. KEY QUESTION 5 a. Wat is de meerwaarde van een stent of deviërend colostoma ten opzichte van acute resectie met of zonder primaire anastomose bij acute obstructie door een linkszijdig
KEY QUESTION 5 1. KEY QUESTION 5 a. Wat is de meerwaarde van een stent of deviërend colostoma ten opzichte van acute resectie met of zonder primaire anastomose bij acute obstructie door een linkszijdig
Wali R Johnson et. al. / International Journal of New Technologies in Science and Engineering Vol. 2, Issue 4, October 2015, ISSN
 Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Enteral Feeding via Percutaneous Endoscopic Gastrojejunostomy(PEGJ) Tubes Decreases Risk of Aspiration and Tube Dislodgement Related Complications Compared to PEGs. Wali R Johnson, MSIV, L Ray Matthews,
Endoscopic Management of Perforations
 Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience
 GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
GENERAL THORACIC Polyflex Expandable Stents in the Treatment of Esophageal Disease: Initial Experience Arjun Pennathur, MD, Andrew C. Chang, MD, Kevin M. McGrath, MD, Gregory Steiner, BS, Miguel Alvelo-Rivera,
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only.
 The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
Adult Trauma Feeding Access Guideline
 Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Title: Use of self-expanding nitinol stents in the pediatric management of refractory esophageal caustic stenosis
 Title: Use of self-expanding nitinol stents in the pediatric management of refractory esophageal caustic stenosis Authors: Verónica Alonso, Devicka Ojha, Harsha Nalluri, Juan Carlos de Agustín DOI: 10.17235/reed.2017.4959/2017
Title: Use of self-expanding nitinol stents in the pediatric management of refractory esophageal caustic stenosis Authors: Verónica Alonso, Devicka Ojha, Harsha Nalluri, Juan Carlos de Agustín DOI: 10.17235/reed.2017.4959/2017
The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial
 Editorial The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial Ian Wong, Simon Law Division of Esophageal and Upper Gastrointestinal Surgery, Department of Surgery,
Editorial The CROSS road in neoadjuvant therapy for esophageal cancer: long-term results of CROSS trial Ian Wong, Simon Law Division of Esophageal and Upper Gastrointestinal Surgery, Department of Surgery,
NICE guideline Published: 24 January 2018 nice.org.uk/guidance/ng83
 Oesophago-gastric cancer: assessment and management in adults NICE guideline Published: 24 January 18 nice.org.uk/guidance/ng83 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Oesophago-gastric cancer: assessment and management in adults NICE guideline Published: 24 January 18 nice.org.uk/guidance/ng83 NICE 18. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases
 Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases Authors Tatsuya Ishii 1,KosukeMinaga 2, Satoshi Ogawa 3, Maiko Ikenouchi 1, Tomoe Yoshikawa 1,TakujiAkamatsu
Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases Authors Tatsuya Ishii 1,KosukeMinaga 2, Satoshi Ogawa 3, Maiko Ikenouchi 1, Tomoe Yoshikawa 1,TakujiAkamatsu
The CREST Trial. Funded by Cancer Research UK and developed by the National Cancer Research Institute
 The CREST Trial A randomised phase III study of stenting as a bridge to surgery in obstructing colorectal cancer. Results of the UK ColoRectal Endoscopic Stenting Trial (CREST). Funded by Cancer Research
The CREST Trial A randomised phase III study of stenting as a bridge to surgery in obstructing colorectal cancer. Results of the UK ColoRectal Endoscopic Stenting Trial (CREST). Funded by Cancer Research
Safety And Efficacy of Stenting In Large Bowel Obstruction - A Review Of Clinical Practice
 Article ID: WMC001512 2046-1690 Safety And Efficacy of Stenting In Large Bowel Obstruction - A Review Of Clinical Practice Corresponding Author: Mr. David C Smith, Specialist Registrar General Surgery,
Article ID: WMC001512 2046-1690 Safety And Efficacy of Stenting In Large Bowel Obstruction - A Review Of Clinical Practice Corresponding Author: Mr. David C Smith, Specialist Registrar General Surgery,
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Can erythropoietin treatment during antiviral drug treatment for hepatitis C be cost effective?
 Below Are Selected Good Abstracts from Digestive Disease Week 2006 Meeting Published in Gut. 2006 April; 55(Suppl 2): A1 A119. http://www.ncbi.nlm.nih.gov/pmc/articles/pmc1859999/?tool=pmcentrez Can erythropoietin
Below Are Selected Good Abstracts from Digestive Disease Week 2006 Meeting Published in Gut. 2006 April; 55(Suppl 2): A1 A119. http://www.ncbi.nlm.nih.gov/pmc/articles/pmc1859999/?tool=pmcentrez Can erythropoietin
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Cancerous esophageal stenosis before treatment was significantly correlated to poor prognosis of patients with esophageal cancer: a meta-analysis
 Original Article Cancerous before treatment was significantly correlated to poor prognosis of patients with cancer: a meta-analysis Han-Yu Deng 1,2#, Guha Alai 1#, Jun Luo 1#, Gang Li 1, Ze-Guo Zhuo 1,
Original Article Cancerous before treatment was significantly correlated to poor prognosis of patients with cancer: a meta-analysis Han-Yu Deng 1,2#, Guha Alai 1#, Jun Luo 1#, Gang Li 1, Ze-Guo Zhuo 1,
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers
 Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
Epidemiology, aetiology and the patient pathway in oesophageal and pancreatic cancers Dr Ian Chau Consultant Medical Oncologist Women's cancers Breast cancer introduction 3 What profession are you in?
Type of intervention Palliative care. Economic study type Cost-effectiveness analysis.
 Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
Natural course of inoperable esophageal cancer treated with metallic expandable stents: quality of life and cost-effectiveness analysis Xinopoulos D, Dimitroulopoulos D, Moschandrea I, Skordilis P, Bazinis
Oral anti-thrombotic therapy-management in patients requiring endoscopy
 Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Oral anti-thrombotic therapy-management in patients requiring endoscopy Management of anti-thrombotic therapy in patients requiring endoscopy This guideline suggests appropriate management of patients
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Esophageal Stent Placement for the Treatment of Acute Intrathoracic Anastomotic Leak After Esophagectomy
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD
 Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
Michael A. Choti, MD, FACS Department of Surgery Johns Hopkins Medicine, Baltimore, MD Surgical Therapy of Gastric Cancer CLINICAL QUESTIONS 1. How much of the stomach should be removed? 2. How many lymph
Surgery for Gastric and Oesophageal Cancer
 Surgery for Gastric and Oesophageal Cancer Trends in cancer mortality, England and Wales SMR base 1980 Oesophago-Gastric Cancer The National Problem 5 th commonest malignancy 4 th commonest cause of death
Surgery for Gastric and Oesophageal Cancer Trends in cancer mortality, England and Wales SMR base 1980 Oesophago-Gastric Cancer The National Problem 5 th commonest malignancy 4 th commonest cause of death
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines. Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center
 Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
Management of Esophageal Cancer: Evidence Based Review of Current Guidelines Madhuri Rao, MD PGY-5 SUNY Downstate Medical Center Case Presentation 68 y/o male PMH: NIDDM, HTN, hyperlipidemia, CAD s/p stents,
ESOPHAGEAL CANCER. Epidemiology 3/22/2017. Esophageal Carcinoma: subtypes. Esophageal Adenocarcinoma (EAC) Epidemiology.
 ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis
 Review Article Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis Ravi Shridhar 1, Jamie Huston 2, Kenneth L. Meredith 2 1 Department of Radiation
Review Article Accuracy of endoscopic ultrasound staging for T2N0 esophageal cancer: a national cancer database analysis Ravi Shridhar 1, Jamie Huston 2, Kenneth L. Meredith 2 1 Department of Radiation
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings?
 Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
Gastrointestinal Feedings Post Op: What s the deal on beginning oral feedings? Kate Willcutts, DCN, RD, CNSC University of Virginia Health System Charlottesville, VA kfw3w@virginia.edu Objectives 1. Discuss
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
Introduction E178. Background and study aims Fully covered self-expanding
 Original article Treatment of refractory post-esophagectomy anastomotic esophageal strictures using temporary fully covered esophageal metal stenting compared to repeated bougie dilation: results of a
Original article Treatment of refractory post-esophagectomy anastomotic esophageal strictures using temporary fully covered esophageal metal stenting compared to repeated bougie dilation: results of a
WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds
 WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds LUNG Dr. Greenland ESOPHAGUS Dr. Gardiner ESOPHAGEAL CANCER 1200 new
WHO BENEFITS FROM ADJUVANT CHEMOTHERAPY RADIATION CHEMORADIATION? Dr. Paul Gardiner April 23, 2001 Discipline of Surgery Grand Rounds LUNG Dr. Greenland ESOPHAGUS Dr. Gardiner ESOPHAGEAL CANCER 1200 new
Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study
 E89 Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study Authors Institution Agnes N. Reijm, Paul Didden, Marco
E89 Early pain detection and management after esophageal metal stent placement in incurable cancer patients: A prospective observational cohort study Authors Institution Agnes N. Reijm, Paul Didden, Marco
The effect of resection of the primary tumour for stage IV colorectal cancer on patient survival: a systematic review and meta-analysis
 The effect of resection of the primary tumour for stage IV colorectal cancer on patient survival: a systematic review and meta-analysis C.Clancy, J.P. Burke, M. Barry, M.F Kalady, J.C. Coffey Dept. of
The effect of resection of the primary tumour for stage IV colorectal cancer on patient survival: a systematic review and meta-analysis C.Clancy, J.P. Burke, M. Barry, M.F Kalady, J.C. Coffey Dept. of
Is surgical Apgar score an effective assessment tool for the prediction of postoperative complications in patients undergoing oesophagectomy?
 Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Determining Resectability and Appropriate Surgery for Esophageal Cancer
 Determining Resectability and Appropriate Surgery for Esophageal Cancer Peter Baik, DO, FACOS Thoracic Surgery Cancer Treatment Centers of America 1 Esophageal and Esophagogastric Junction Cancers Siewert
Determining Resectability and Appropriate Surgery for Esophageal Cancer Peter Baik, DO, FACOS Thoracic Surgery Cancer Treatment Centers of America 1 Esophageal and Esophagogastric Junction Cancers Siewert
Controversies in management of squamous esophageal cancer
 2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
2015.06.12 12.47.48 Page 4(1) IS-1 Controversies in management of squamous esophageal cancer C S Pramesh Thoracic Surgery, Department of Surgical Oncology, Tata Memorial Centre, India In Asia, squamous
Interventional Endoscopy in PB Malignancy
 Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Y A L E S C H O O L O F M E D I C I N E. This is a CME accredited activity. The presenters and there are no conflicts of interest.
 This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy
 OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Characteristics and prognostic factors of synchronous multiple primary esophageal carcinoma: A report of 52 cases Mei Li & Zhi-xiong Lin Department of Radiation
Canena et al. Canena et al. BMC Gastroenterology 2012, 12:70
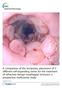 A comparison of the temporary placement of 3 different self-expanding stents for the treatment of refractory benign esophageal strictures: a prospective multicentre study Canena et al. Canena et al. BMC
A comparison of the temporary placement of 3 different self-expanding stents for the treatment of refractory benign esophageal strictures: a prospective multicentre study Canena et al. Canena et al. BMC
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Esophageal Stents What, Why, When and How?
 Esophageal Stents What, Why, When and How? Motility Noon Conference Bill Kessler February 1, 2017 Disclosure Research support from Merit Medical, Inc. Objectives Background Indications Techniques and What?
Esophageal Stents What, Why, When and How? Motility Noon Conference Bill Kessler February 1, 2017 Disclosure Research support from Merit Medical, Inc. Objectives Background Indications Techniques and What?
Nutritional Support in the Perioperative Period
 Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Nutritional Support in the Perioperative Period Topic 17 Module 17.3 Nutritional Support in the Perioperative Period Ken Fearon Learning Objectives Understand the principles behind nutritional care for
Endoscopic biodegradable stents as a rescue treatment in the management of post bariatric surgery leaks: acaseseries
 Endoscopic biodegradable stents as a rescue treatment in the management of post bariatric surgery leaks: acaseseries Authors Abed Al Lehibi, Areej Al Balkhi, Abdullah Al Mtawa, Nawaf Al Otaibi Institution
Endoscopic biodegradable stents as a rescue treatment in the management of post bariatric surgery leaks: acaseseries Authors Abed Al Lehibi, Areej Al Balkhi, Abdullah Al Mtawa, Nawaf Al Otaibi Institution
ROBOTIC VS OPEN RADICAL CYSTECTOMY
 ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Jung-Hoon Park 1 Ho-Young Song 1 Jin Hyoung Kim 1 Deok Ho Nam 2 Jae-Ik Bae 3 Min-Hee Ryu 4 Hwoon-Yong Jung 4
 Vascular and Interventional Radiology Original Research Park et al. Stent Placement to Treat Malignant Jejunal Obstruction Vascular and Interventional Radiology Original Research Jung-Hoon Park 1 Ho-Young
Vascular and Interventional Radiology Original Research Park et al. Stent Placement to Treat Malignant Jejunal Obstruction Vascular and Interventional Radiology Original Research Jung-Hoon Park 1 Ho-Young
Newly Diagnosed Cases Cancer Related Death NCI 2006 Data
 Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
Department of Thoracic Medicine, Chang Gung Memorial Hospital, Lin-Kuo Branch, Chang Gung Medical Foundation; Abstract
 DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
IATROGENIC OESOPHAGEAL PERFORATION
 IATROGENIC OESOPHAGEAL PERFORATION TAOLE MOKOENA DPhil FRCS PROFESSOR OF SURGERY UNIVERSITY OF PRETORIA 17 TH Controversies and Problems in Surgery Symposium 4-5 October 2013 Introduction Perforation of
IATROGENIC OESOPHAGEAL PERFORATION TAOLE MOKOENA DPhil FRCS PROFESSOR OF SURGERY UNIVERSITY OF PRETORIA 17 TH Controversies and Problems in Surgery Symposium 4-5 October 2013 Introduction Perforation of
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
ESD for EGC with undifferentiated histology
 ESD for EGC with undifferentiated histology Jun Haeng Lee, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Biopsy: M/D adenocarcinoma ESD: SRC >>
ESD for EGC with undifferentiated histology Jun Haeng Lee, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Biopsy: M/D adenocarcinoma ESD: SRC >>
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Original article INTRODUCTION
 Diseases of the Esophagus (2007) 20, 466 470 DOI: 10.1111/j.1442-2050.2007.00696.x Blackwell Publishing Asia Original article Superiority of anti-reflux stent compared with conventional stents in the palliative
Diseases of the Esophagus (2007) 20, 466 470 DOI: 10.1111/j.1442-2050.2007.00696.x Blackwell Publishing Asia Original article Superiority of anti-reflux stent compared with conventional stents in the palliative
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE
 22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
22 Main Article ENDOSCOPIC SELF-EXPANDABLE METAL STENTING FOR ADVANCED CARCINOMA OESOPHAGUS: A BETTER PALLIATIVE PROSPECTIVE Swagata Khanna 1, Subhash Khanna 2 ABSTRACT: Endoscopic placement of metal stent
Endoscopic management of sleeve leaks
 Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
Delay in Diagnostic Workup and Treatment of Esophageal Cancer
 J Gastrointest Surg (2010) 14:476 483 DOI 10.1007/s11605-009-1109-y ORIGINAL ARTICLE Delay in Diagnostic Workup and Treatment of Esophageal Cancer Brechtje A. Grotenhuis & Pieter van Hagen & Bas P. L.
J Gastrointest Surg (2010) 14:476 483 DOI 10.1007/s11605-009-1109-y ORIGINAL ARTICLE Delay in Diagnostic Workup and Treatment of Esophageal Cancer Brechtje A. Grotenhuis & Pieter van Hagen & Bas P. L.
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Factors That Affect Stent-Related Complications in Patients with Malignant Obstruction of the Esophagus or Gastric Cardia
 Gut and Liver, Vol. 11, No. 1, January 2017, pp. 47-54 ORiginal Article Factors That Affect Stent-Related Complications in Patients with Malignant Obstruction of the Esophagus or Gastric Cardia Hiroyasu
Gut and Liver, Vol. 11, No. 1, January 2017, pp. 47-54 ORiginal Article Factors That Affect Stent-Related Complications in Patients with Malignant Obstruction of the Esophagus or Gastric Cardia Hiroyasu
