Diagnosis and Treatment of Gastrinomas in Multiple Endocrine Neoplasia Type 1 (MEN-1)
|
|
|
- Adam Terry
- 6 years ago
- Views:
Transcription
1 Cancers 2012, 4, 39-54; doi: /cancers Review OPEN ACCESS cancers ISSN Diagnosis and Treatment of Gastrinomas in Multiple Endocrine Neoplasia Type 1 (MEN-1) Ursula Plöckinger Interdisziplinäres Stoffwechsel-Centrum: Endokrinologie, Diabetes und Metabolismus, Kompetenzzentrum Seltene Stoffwechselkrankheiten, Charité-Universitätsmedizin Berlin, Campus Virchow-Klinikum, Berlin 13353, Germany; ursula.ploeckinger@charite.de; Tel.: ; Fax: Received: 1 December 2011; in revised form: 7 January 2012 / Accepted: 12 January 2012 / Published: 20 January 2012 Abstract: Multiple endocrine neoplasia type 1 (MEN-1) is a rare autosomal-dominant disease. It is associated with a broad range of endocrine tumours, most frequently arising in the parathyroid glands, the pituitary and the pancreas. Most neuroendocrine tumours will be diagnosed in the pancreas as non-functioning neuroendocrine tumours or insulinomas. Forty-two percent of the patients will develop a gastrin-secreting neuroendocrine tumour, a gastrinoma. Gastrinomas in MEN-1 tend to be small, multiple and preferentially located in the duodenum. This paper will focus on the specific characteristics of gastrinomas in the setting of MEN-1 compared to sporadic gastrinomas. The developments in understanding the tumorigenesis of these tumours and the consequences for diagnosis and therapy will be discussed. Keywords: MEN-1; gastrinoma; diagnosis; therapy 1. Introduction Multiple endocrine neoplasia type 1 (MEN-1) is a rare autosomal-dominant disease. MEN-1 is associated with a broad range of endocrine tumours, most frequently arising in the parathyroid glands, the pituitary and the pancreas. Penetrance for neuroendocrine tumours is up to 70% 100%. Half of the patients with MEN-1 will present with a pancreatico-duodenal neuroendocrine tumour at the age of 50 years. Most will arise in the pancreas as non-functioning neuroendocrine tumours or insulinomas. Forty-two percent (range 20% 61%) of the patients will develop a gastrin-secreting neuroendocrine
2 Cancers 2012, 4 40 tumour, a gastrinoma. In contrast to sporadic gastrinomas that occur predominantly in the pancreas, in MEN-1 most of these tumours reside in the duodenum [1]. Duodenal gastrinomas are small, usually below 1 cm in diameter, multiple and show a preference for the proximal duodenum. Pancreatic gastrinomas associated with MEN-1 are very rare [2], as are other uncommon extra-pancreatic, extra-duodenal locations that have been associated with gastrinomas. 2. Pathogenesis and Classification Independent of the tumour location, gastrinomas are well differentiated endocrine carcinomas. Recently, a specific sequence of events has been suggested to occur during tumorigenesis in gastrinomas due to multiple endocrine neoplasia [3,4]. In MEN-1 distinctive proliferative hyperplastic gastrin cells in the non-neoplastic duodenum are interpreted as multicentric precursor lesions. Their spectrum of proliferative changes is compared to those seen in entero-chromaffine-like (ECL)-cells in chronic atrophic gastritis. The first step is supposed to be diffuse hyperplasia of gastrin-positive cells, followed by linear hyperplasia, i.e., chains of more than five gastrin-positive cells and more than two chains per mm. With further proliferation micronodular (30 50 µm) hyperplastic lesions, i.e., nodules of more than 5 gastrin-positive cells within glands or crypts of the mucosa followed by enlarged nodules (> µm) of gastrin-positive cells with solid architecture have been demonstrated. These hyperproliferative and hyperplastic lesions were found only in patients with MEN-1, but were absent in patients with sporadic, not MEN-1 associated duodenal gastrinoma. The occurrence of gastrin cell hyperplasia at various sites in the duodenal mucosa explains the multifocality of gastrinomas in MEN-1. It is however unclear whether additional stimuli, besides the MEN-1 mutation are responsible for the development of hyperplastic lesions. As the next step in the tumorigenesis of MEN-1 associated gastrinomas micro-invasive lesions, small clusters of gastrin-positive cells in the lamina propria between the glands, resulting in micro-tumours (>250 µm) with trabecular growth pattern and fibrosis have been described. In MEN-1 the heterozygous germ line mutations of the MEN-1 gene, a tumour-suppressor gene, are by themselves insufficient for tumour development. According to the two-hit hypothesis of tumour development by Knudson additional somatic inactivation of the wild-type MEN-1 allele on chromosome 11q13 has to occur. This may lead to a loss of a part or all of chromosome 11, termed loss of heterozygosity. By using a combination of fluorescence in situ hybridisation and immuno-fluorescence techniques, Anlauf et al. were able to simultaneously detect allelic deletion and hormone expression in individual duodenal cells [3]. Different tumours from one patient showed different patterns of loss of heterozygosity, suggesting that each gastrinoma arises as a result of an independent second hit. In contrast none of the hyperplastic lesions was found to be positive for loss of heterozygosity. These observations enabled the authors to conclude that the hyperplastic lesions, suggested to be pre-neoplastic, retain both MEN-1 alleles and that allelic loss or other mutation in the wild-type allele inactivating the gene, is responsible for the final development of neoplastic lesions. It still remains to be analysed which factors are responsible for loss of heterozygosity in these individual cells. To summarize, MEN-1 associated duodenal gastrinomas are preceded by gastrin-positive cell hyperplasia. Allelic deletion in these cells results in multifocal gastrin positive neoplastic lesions. MEN-1 associated duodenal gastrinomas show a trabecular and pseudo-glandular pattern; immuno-histochemically they express gastrin and occasionally somatostatin. Interestingly only about
3 Cancers 2012, % of these tumours are functionally active i.e., associated with a Zollinger-Ellison syndrome and thus are gastrinomas per definition [2]. They are characterised according to the WHO classification (i) as well differentiated neuroendocrine tumours, i.e., benign, if non-angioinvasive and below 1 cm in size or (ii) benign or low grade malignant, if confined to the mucosa-submucosa with or without angioinvasion and less than 1 cm in size. With invasion of the muscularis propria and beyond or the development of metastases they are characterized as well differentiated neuroendocrine carcinomas. Tumours with a high grade malignancy are termed poorly differentiated neuroendocrine carcinomas. Recently a TNM classification has been suggested for duodenal tumours by the European Neuroendocrine Tumour Society (ENETS) [5]. 3. Clinical Presentation The penetrance of duodenal gastrinomas in MEN-1 lies between non-functioning pancreatic tumours and insulinomas. Twenty to 40% of patients, between 50 and 70 years of age, are diagnosed with a gastrinoma [6]. Data from the NIH series indicate a slightly earlier diagnosis with a maximum occurring at 40 years, preceded by symptoms of a Zollinger-Ellison syndrome by 5 7 years. In comparison to sporadic gastrinomas, gastrinomas in the setting of MEN-1 are diagnosed 10 years earlier and the primary is more often located in the duodenum. No other lesion than the primary was found at the time of diagnosis in 9% of the patients with MEN-1 as compared to 27% of those with sporadic gastrinomas [7]. While recent data localize most MEN-1 related gastrinomas within the duodenum [2,8], earlier studies reported primary lymph node gastrinomas and significantly more pancreatic gastrinomas than today. This may be due to the high frequency (60 to 80%) of large regional lymph nodes metastases at the time of diagnosis [9,10]. These were either misinterpreted as primary lymph node gastrinomas due to the very small duodenal lesions that have escaped detection in patients with MEN-1, or were possibly considered as pancreatic tumours, especially if they were located at the upper margin of the head of the pancreas [11]. Duodenal gastrinomas may metastasize to the liver in about 10% of the cases, but this occurs rather late in the course of the disease. Fast-growing poorly differentiated and metastasizing duodenal gastrinomas are extremely rare [1,12,13]. The percentage of patients with gastrinomas as part of the MEN-1 syndrome is about 23% (10% 48%) in ten large series compiled by Berna and co-workers [7]. Most patients present with long-standing upper abdominal pain (66%), diarrhoea (76%), heartburn (52%), nausea (38%) and vomiting (24%) or weight loss (12%) similar to patients with sporadic gastrinoma [7,14]. Due to the notion that Zollinger-Ellison syndrome complications occur slightly less in MEN-1 compared to sporadic gastrinomas, the number of patients with bleeding as the presenting symptom of Zollinger-Ellison syndrome was significantly lower (12% vs. 27%) in MEN-1 gastrinomas patients [14]. The widespread use of proton-pump inhibitors may mask the classical symptoms of Zollinger-Ellison syndrome and delay the diagnosis of a gastrinoma [15]. Associated nephrolithiasis [7] occurs more often in MEN-1 patients and cutaneous lesions (angiofibromas and collagenomas) have a sensitivity of 75% and specificity of 95% to predict the presence of MEN-1 in patients with Zollinger-Ellison syndrome [16]. Interestingly, the prevalence and probability of Zollinger-Ellison syndrome in MEN-1 is sex-related, with a probability of developing Zollinger-Ellison syndrome at the age of 60 years of 55% in men and 33% in women [17].
4 Cancers 2012, Diagnosis 4.1. Biochemical Diagnosis The diagnosis of Zollinger-Ellison syndrome is made by demonstrating an increased gastrin concentration in fasting patients in the presence of proven hyperchlorhydria. In a large prospective investigation in 309 patients with Zollinger-Ellison syndrome (including 30% MEN-1 patients), Berna et al. compared their findings with 2,209 cases from the literature [7]. Both, normal or very high concentrations (>100-fold normal) of gastrin concentrations in fasting patients were uncommon (0.3% 3% and 4.9% 9%, respectively). Forty to 60% of gastrinoma patients in the fasting state had a gastrin concentration below 10 times normal and this overlaps with gastrin concentrations seen in Helicobacter pylori infection. No difference could be detected between sporadic and MEN-1 associated gastrinoma patients. This increase of the gastrin concentration in fasting patients overlaps with hypergastrinaemia seen in fasting patients with idiopathic peptic disease or gastro-oesophageal reflux disease. Furthermore an increased gastrin concentration in fasting patients is observed in patients with pernicious anaemia or on proton pump inhibitor medication. However in both conditions gastric acid secretion is reduced in contrast to gastrinoma patients. In 20% 30% of these patients the gastrin concentration can be up to five times normal, comparable to the gastrin concentration seen in 60% of Zollinger-Ellison syndrome patients. As expected increased basal acid output, tumour location (pancreas > duodenum), tumour size (large > small) and extent (liver metastases > local disease) all were positively correlated to the basal gastrin concentration. Proton pump inhibitors have to be stopped at least 1 week prior to the determination of the gastrin concentration and this may pose a serious problem in terms of pain and risk of bleeding in symptomatic patients [7]. While histamine H2 receptor antagonists are needed in higher doses to achieve symptom control in Zollinger-Ellison syndrome compared to idiopathic ulcer disease, this is not the case with proton pump inhibitors. Thus, the use of proton pump inhibitors can delay the diagnosis of Zollinger-Ellison syndrome because of symptom control with conventional dosage. Hypercalcaemia (due to hyperparathyroidism in MEN-1 patients, which predeces the manifestation of gastrinoma in most patients) has been shown to increase the serum gastrin concentration in fasting patients with Zollinger-Ellison syndrome. However, in the NIH series no correlation between hypercalcaemia and the gastrin concentration in fasting patients was observed, probably due to the low tumour load in MEN-1 patients. Hypochlorhydria will increase gastrin secretion. Patients with atrophic gastritis, pernicious anaemia, post-vagotomy patients or patients on proton pump inhibitors can be excluded due to the high intragastric ph or low basal acid-output. On the other hand patients with hyperchlorhydria and hypergastrinaemia due to Helicobacter pylori infection, antral G-cell hyperfunction, short bowel syndrome or those with renal failure have to be differentiated from those with Zollinger-Ellison syndrome. Thus, while the gastrin concentration in fasting patients with proven hyperchlorhydria is increased, in most Zollinger-Ellison syndrome patients functional testing is recommended due to the large overlap with other pathological conditions with hypergastrinaemia. Gastrin stimulation tests use either secretin or calcium to demonstrate a pathological increase in gastrin. A meal stimulation test is no
5 Cancers 2012, 4 43 longer used due to its insufficient specificity to diagnose a Zollinger-Ellison syndrome. Using a delta gastrin of 200 pg/ml, the secretin test has a sensitivity and specificity of 82% and 100% for the diagnosis of Zollinger-Ellison syndrome. The sensitivity can be increased to 94%, if a delta gastrin of 120 pg/ml is used [18]. For the calcium infusion test the corresponding numbers are 54% and 100%, respectively for a delta gastrin concentration of 396 pg/ml, while a 50% increase of the gastrin concentration after calcium stimulation resulted in a sensitivity and specificity of 78% and 83%. In those Zollinger-Ellison syndrome patients with a negative secretin test the calcium infusion test is positive in 38% 50% of the patients. Due to potential complications the calcium stimulation test is rarely used in most centres. Interestingly, there is no correlation of the secretin-stimulated gastrin response with the calcium-stimulated response. While the calcium stimulated increase in gastrin secretion has been shown to be due to a calcium sensing receptor [19], the secretin-stimulated responses have to rely on the presence of secretin receptors. It has been demonstrated that the secretin response is significantly related to the presence and density of secretin receptors in gastrinoma cells [20]. The diagnosis of Zollinger-Ellison syndrome may be further impeded due to technical difficulties with the determination of the correct gastrin concentration. Gastrin circulates not as a single molecule but as several peptides of various lengths and amino acid modifications. Moreover circulating gastrins in Zollinger-Ellison syndrome may deviate from that in healthy controls. Rehfeld et al. demonstrated that seven of twelve commercially available assays (radioimmunoassay and enzyme-linked immunosorbent assays) failed to accurately measure the plasma gastrin concentration [21] Tumour Localisation Once the diagnosis has been biochemically established by fasting and stimulated gastrin concentration, localization and staging of the tumour are mandatory. Here results differ considerably for patients with sporadic or MEN-1 associated tumours. Conventional imaging studies localize 10% 40%, angiography 20% 50% and somatostatin receptor scintigraphy 60% 70% of sporadic pancreatic gastrinomas. Somatostatin receptor scintigraphy is comparable to all conventional studies combined and changes the management in 15% 45% of the patients. However, sensitivity is dependent on tumour size and tumours below 1 cm are missed in about 50% of cases. As gastrinomas in MEN-1 are mostly very small duodenal lesions they are frequently missed [22]. In a prospective study in 80 patients with Zollinger-Ellison syndrome, with 22% of the patients with an associated MEN-1, somatostatin receptor scintigraphy was the most sensitive method, but had no influence on long-term survival and intra-operatively 33% additional lesions were found [23]. The guidelines for the diagnosis of MEN-1 [24] explicitly state that somatostatin receptor scintigraphy still lacks full evaluation in MEN-1. Thus, due to the small size of duodenal gastrinomas in MEN-1, these will mostly be missed by somatostatin receptor scintigraphy or conventional imaging. The highest chance for detecting these tumours will be by using multi-slice CT scanners. This technique is superior to state of the art MRI, due to its potential for acquiring an entire anatomic region continuously without gaps [25,26]. Endoscopic ultrasound, while highly effective for the detection of small pancreatic lesions fails to localize tumours in the duodenal wall. Intraoperative evaluation of the duodenum is still superior to preoperative imaging techniques, especially so when intraoperative ultrasound combined with duodenotomy are used [27].
6 Cancers 2012, 4 44 It can be safely assumed that after a biochemical diagnosis of Zollinger-Ellison syndrome in MEN-1, multiple small tumours are probably located in the duodenum. At surgical exploration duodenotomy is essential to detect up to one-half of duodenal tumours. Intra-operative transillumination of the duodenum is frequently used to help identify the site for the duodenotomy. Intra-operative ultrasound should be routinely used to assess and identify pancreatic lesions [22]. Diagnostic imaging in gastrinoma associated with MEN-1 should preferentially aim to diagnose metastatic disease. Lymph node metastases occur in 45% to 85% of duodenal gastrinomas in MEN-1 [28]. The sensitivity and specificity of somatostatin receptor scintigraphy for lymph node metastasis as well as liver metastasis is high and somatostatin receptor scintigraphy can be highly recommended. However its sensitivity is dependent on tumours size, thus somatostatin receptor scintigraphy will miss up to 50% of small gastrinoma lesions <1 cm [29]. Metastatic disease does influence therapeutic decisions. When additional non-functioning pancreatic neuroendocrine tumours are diagnosed, any lesion in the liver can either be a metastasis of the pancreatic tumours or the gastrinoma. The prevalence of distant metastatic disease in MEN-1 due to gastrinoma is rather low and no specific data are available for the sensitivity of conventional imaging. The frequency of liver metastases from gastrinomas in MEN-1 is less by 62% compared with patients who have sporadic gastrinomas [28]. Hepatic metastatic lesions can be detected with state of the art equipment starting from 1 mm in size [26]. Yet still this does not clarify if the metastasis is due to a parallel existing non-functioning neuroendocrine pancreatic tumours or the duodenal gastrinoma. Intraoperative selective intra-arterial secretin stimulation and venous sampling of gastrin may be helpful in localising small sporadic gastrinomas. However, the procedure is not easy to perform and experience is limited, especially in patients with MEN Therapy Therapy in MEN-1 associated gastrinoma aims at the treatment of (i) acid hypersecretion, (ii) the gastrinoma and (iii) the treatment of gastric neuroendocrine tumours type Medical Treatment of Acid Hypersecretion Histamine H2-inhibitors (cimetidine, ranitidine, famotidine) have been substituted due to the need of frequent and high dosing required to control acid hypersecretion. The H1-K1 ATPase inhibitors, like omeprazole, lansoprazole, or pantoprazole, are now the drugs of choice. Acid secretion can be controlled in all patients due to the long duration of action and potency of the drugs. Most patients will need dosing once or twice and only occasionally three times a day. Acid secretion can be successfully controlled during long-term therapy with a mean omeprazole dosage of 65 mg per day or equivalent dosing of other PPI. Theses drugs are well tolerated and side effects are rare. As hypercalcaemia due to hyperparathyroidism in MEN-1 patients may exacerbate acid secretion, these patients may need higher doses of proton pump inhibitors. It is recommended to additionally address therapeutic options for hyperparathyroidism. It should, however, not be assumed that an asymptomatic patient has adequate control of gastric acid secretion [30]. Thus, to establish the correct dosage of proton pump inhibitors acid secretion has to be determined by either measuring basic acid output 1 h prior to the next dose of anti-secretory drug
7 Cancers 2012, 4 45 or by 24-h ambulatory ph-metry. If acid secretion is suppressed to 0.10 mu/h, or 0.5 mu/h in patients with previous gastric resection or severe reflux, peptic ulcers will heal and further peptic complications will be prevented [31 34]. As has been already discussed at the diagnostic section, the hypercalcaemia of hyperparathyroidism increases gastrin secretion and, by a mechanism unknown, reduces the sensitivity of acid secretion to anti-secretory medication. Successful parathyroidectomy reduces basic acid output, gastrin secretion in fasting patients and increases the sensitivity towards anti-secretory medication allowing to reduce the dosage of anti-secretory drugs [34]. In patients with Zollinger-Ellison syndrome with MEN-1 and hypercalcaemia omeprazole 40 mg b.i.d. or equivalent is recommended as a staring dose and followed by a reduction to 20 mg b.i.d. if possible Surgical Therapy of the Gastrinoma There has been no general recommendation for the therapy of the primary in MEN-1 associated Zollinger-Ellison syndrome. Due to the recent notion that gastrinoma in MEN-1 is a multiple tumour disease, and that most primaries are located in the duodenum, all recommendations referring to pancreatic tumours may be obsolete. The cure rate for gastrinomas within the setting of MEN-1 has been very low and this may be due to treatment strategies, which aimed at pancreatic tumours [35 38]. Further complicating the process of therapeutic decision making is the paucity of prognostic data and the synchronous existence of the gastrinoma and malignant non-functioning pancreatic neuroendocrine tumours. It is therefore difficult to discern the effect of the gastrinoma on morbidity and mortality. Thus controversies exist concerning almost every aspect of surgical therapy in gastrinoma in patients with MEN-1. Should patients controlled by proton pump inhibitors be operated at all? If surgery is considered necessary what is the optimal time-point? Should patients be operated at the diagnosis of Zollinger-Ellison syndrome or after the tumour has reached a predefined size? Should surgery be performed to control pancreaticoduodenal disease by preventing the development of metastasis? Should surgery aim at cure from Zollinger-Ellison syndrome and thus use aggressive techniques or should only individual tumours be operated on. What kind of surgery should be performed? Overall, data compiled by Jensen demonstrate that long-term survival after diagnosis is considerably longer in patients with MEN-1 associated gastrinoma (93% at 15 years) compared to patients with sporadic gastrinoma (68% at 15 years) [34]. The analysis of eighty-one patients with MEN-1 and Zollinger-Ellison syndrome reported 100% 15 year survival with small (<2.5 cm) pancreatic tumours, as well as 100% survival in those with a single, surgically removed tumour <6 cm, but only 89% survival in those with surgery for more than two tumours or one tumour larger than 6 cm [39]. The presence of lymph node metastases does not influence, but liver metastases will shorten survival [27]. Due to the fact that liver metastases due to gastrinoma are rare in patients with MEN-1 compared to sporadic gastrinoma (2% vs. 21%), the percentage of patients that will develop more aggressive disease is not known. However, it has been shown that liver metastases occurred in 3% of Zollinger-Ellison syndrome patients treated surgically compared to 23% of those with only medical therapy [40]. A recent review covering 72 patients with gastrinoma (N = 15, 22% MEN-1) gave a median survival of 6.6 years. Two of 15 deaths were due to metastatic gastrinoma, with no gastrinoma related death in the MEN-1 population [41]. Goudet et al. investigated the risk of death according to lesions in a large cohort of 758 MEN-1 patients and found that the presence of a gastrinoma increased the risk of death
8 Cancers 2012, 4 46 (Hazard ratio 1.89, p = 0.022). The Hazard ratio was lower than for non-functioning pancreatic tumours (Hazard ratio 3.43, p = 0.001), but higher than the non-significant risk due to pituitary, bronchial tumours or insulinomas [42]. In addition considering that metastatic disease from non-functioning pancreatic tumours may be the major determinant of long-term survival, the importance of surgical therapy for gastrinoma in MEN-1 is further reduced. Is aggressive surgery for gastrinoma without metastases justified? A retrospective analysis of surgery for Zollinger-Ellison syndrome in twelve MEN-1 patients using different surgical approaches over a period from 1970 to 2008 failed to demonstrate biochemical cure in any of the patients treated [43]. In a recent study 11 patients with Zollinger-Ellison syndrome as part of a MEN-1 syndrome were analyzed prospectively. Cure of Zollinger-Ellison syndrome was defined as a normal gastrin concentration in fasting patients and a negative secretin test. Seven of the eleven (77%) gastrinoma patients were biochemically cured after a median follow-up for 123 months ( months). Four of these seven patients cured by surgery underwent pylorus-preserving pancreatico-duodenectomy. In contrast, four of the eleven patients with recurrent Zollinger-Ellison syndrome underwent local excision of duodenal gastrinomas as the initial procedure. None of these four patients had developed metastatic disease [38]. The authors therefore argue for a more aggressive therapeutic approach in duodenal-pancreatic tumours associated with MEN-1. Their objective is to detect and remove potentially malignant tumour in asymptomatic patients before malignant transformation, in an effort to reduce the death rate in those patients who undergo early surgery. Data from Skogseid and other groups support this hypothesis [38,44,45]. The high rate of post-operatively normalised basal and stimulated gastrin concentration (77%) is probably related to the use of pylorus-preserving pancreatico-duodenectomy and this is confirmed by others [1,46 54]. Pylorus-preserving pancreatico-duodenectomy may therefore be justified if there is a biochemical diagnosis of Zollinger-Ellison syndrome in MEN-1 and the source of gastrin can be regionalized by preoperative selective arterial secretin injection to the head of the pancreas [27,55]. Arguing against this approach are the difficult nature of this procedure, a possible high rate of morbidity and mortality, the unknown long-term consequences of pylorus-preserving pancreatico-duodenectomy as well as the problem of possible reoperation that may be rendered more difficult after pylorus-preserving pancreatico-duodenectomy than after duodenal excision or distal pancreatectomy. A more conservative surgical approach has been to interfere only after a diagnosed lesion suggested to be a gastrinoma has surpassed a given diameter. Recommendations depend on the estimated risk for the development of metastatic disease and range from lesions larger than 1 cm, 2.5 cm or 3 cm [24,34]. The procedure most often used in these patients has been pancreatico-duodenectomy. However, Gibril and co-workers could not confirm the relationship between the incidence of liver metastases and the size of the primary tumour [56]. In addition the number of patients with both duodenal and pancreatic gastrin secreting tumours, justifying pancreatico-duodenectomy, is probably rather low [57]. A recent overview on the results of pancreatico-duodenectomy for gastrinoma in MEN-1 indicated a high cure rate (77% 100%). However most cited reports included only one or two patients, only two studies had six and thirteen patients, respectively [28]. A new option may be pancreas-preserving total duodenectomy that has been recently reported by Imamura and co-workers [57 59] in patients with multiple gastrinomas as part of MEN-1 syndrome.
9 Cancers 2012, 4 47 This challenging new technique awaits further investigations before it can be used as an alternative to pylorus-preserving pancreatico-duodenectomy. In summary, no definite recommendations for surgical therapy are possible at this time for patients with MEN-1 related gastrinomas. Due to the new patho-physiological insight into the development of gastrinoma in MEN-1 with multiple very small tumours in the duodenum and a rare tumour manifestation in the pancreas Pylorus preserving pancreatico-duodenectomy may be the adequate procedure. All surgery should be performed according to oncological criteria, i.e., the inclusion of lymph node resection. However, in patients with additional non-functioning neuroendocrine pancreatic tumours an individualized approach with resection of pancreatic tumours is probably indicated as part of a strategy to prevent the development of hepatic metastases. This approach may be independent of the size of the pancreatic lesions. In contrast in the patient with a sporadic gastrinoma the indication for surgery is given and the type of surgery is dictated by the localisation of the tumour and the necessary extend of surgery. 6. Treatment of Metastasized Gastrinoma The most important predictor of poor survival is the presence of hepatic metastases. There are no controlled surgical trials for curative surgery in metastatic gastrinoma. Most data reported stem from mono-centric retrospective analysis in patients with functional/non-functional pancreatic neuroendocrine tumours. Major hepatic surgery with a curative approach may be justified if all or at least 90% of tumour tissue can be removed. Norton and co-workers report their results in a study with 19 gastrinoma patients. In 17 patients curative resection was performed and 5-year survival was 85%. During follow-up of 5.5 years five patients remained disease-free [60]. However, inclusion bias may have influenced the outcome of this investigation. Recently peptide-radio receptor therapy has become available. The use of 90 Yttrium- or 177 Luthetium-labelled somatostatin analogues offers combination therapies to further improve outcome [61,62]. It has been suggested that peptide-radio receptor therapy is especially effective in metastasized gastrinoma with partial remission in 47% of patients with gastrinomas, insulinomas or vipomas [63]. A recent publication on the outcome of peptide-radio receptor therapy ( 90 Yttrium- or 177 Lutetium-DOTATOC) in eleven sporadic gastrinomas showed complete response in one (9%) patient, partial tumour response in 5/11 (45%), and tumour stabilization in 5/11 (45%) patients, respectively. In seven patients the anti-tumour effect persisted for 14 months, while four patients died of disease with a mean survival time after the last peptide-radio receptor therapy of 14 ± 6.9 months [64]. No prospective, randomized investigations referring to one specific tumour entity in the context of MEN-1 are available. Octreotide therapy has been investigated in malignant gastrinomas but no data are available for its effectiveness in the setting of MEN-1. In seven of 15 patients (47%) tumour stabilization was demonstrated, and tumour size decreased in one patient (6%). The mean duration of response was 25.0 ± 6.1 months (range, months). During follow-up (range, 4 8 years), 25% of the responders died compared with 71% of the non-responders, a difference that approached statistical significance (p = 0.10) [64]. Alternatively systemic chemotherapy with streptozotocin and 5-fluorouracil or doxorubicin can be offered to the patients [34,65].
10 Cancers 2012, Gastric Neuroendocrine Tumours Type 2 Gastric neuroendocrine tumours are currently classified according to their differentiation as well differentiated tumours, mainly composed by enterochromaffine-like cells or gastrin-producing cells. Subtyping these enterochromaffine-like cell tumours (carcinoids) classifies those associated with chronic atrophic gastritis as type 1, those associated with hypertrophic gastropathy due to Zollinger-Ellison syndrome with MEN-1 as type 2 tumours [66]. Gastric neuroendocrine tumours develop in 13% 30% of patients with Zollinger-Ellison syndrome and MEN-1. The mean age at diagnosis is 50 years [67,68]. Hypergastrinaemia is associated with entero-chromaffine-like cell hyperplasia and is seen in 90% of Zollinger-Ellison syndrome patients with MEN-1. Loss of heterozygosity at the MEN-1 locus on chromosome 11q has been clearly established in these type 2 gastric neuroendocrine tumours in contrast to type 1 gastric neuroendocrine tumours that are related to hypergastrinaemia due to atrophic gastritis [69 71]. Gastric neuroendocrine tumours type 2 occur in equal frequencies in both sexes, 70% are smaller than 1.5 cm, are multicentric in 90% and show invasion of the gastric wall limited to the mucosa and submucosa [67]. Metastases to lymph nodes occurred in 30% and distal metastases in 10%. However, only one patient s death was related to the course of gastric neuroendocrine tumours type 2. While no definite recommendation can be made regarding the therapy of theses tumours, it seems justified to take a more conservative approach, following and treating these patients endoscopically as long as the lesion is below 1 cm. Whether a more aggressive approach with surgical treatment for those tumours with a size between 1 to 2 cm, or even gastrectomy in tumours larger than 2 cm is justified is currently unclear [67,72]. In addition there are no data on the effect of surgical cure, i.e., abolishment of hypergastrinaemia by surgical treatment of duodenal gastrinomas, on growth and progression of gastric neuroendocrine tumours type Conclusions It has been demonstrated recently that gastrinomas associated with MEN-1 are preferentially located in the duodenum, arise from gastrin cell hyperplasia, so-called precursor lesions that develop to micro-tumours after loss of heterozygosity. The diagnosis of MEN-1 is made biochemically by determination of the fasting and secretin-stimulated gastrin concentration. Clinically hypergastrinaemia results in Zollinger-Ellison syndrome and signs and symptoms are comparable to sporadic gastrinoma. Proton pump inhibitor medication is the therapy of choice to control acid secretion in virtually all patients. Due to the small size of the primaries imaging fails to demonstrate most of these tumours, while lymph node and liver metastases may be demonstrated by somatostatin receptor scintigraphy and CT. The classical surgical approach by pancreatico-duodenectomy failed to cure most of these patients due to a possible misinterpretation of pancreatic tumours as gastrin secreting primaries. After localization of gastrin secretion to the head of the pancreas pylorus preserving pancreatico-duodenectomy has been suggested after biochemical diagnosis of Zollinger-Ellison syndrome, with a biochemical cure rate in about two-thirds of the patients. However, as most patients will harbour additional non-functioning neuroendocrine pancreatic tumours surgical strategies will have to be individualized. In metastatic gastrinomas treatment schedules follow those for sporadic gastrinomas.
11 Cancers 2012, 4 49 References 1. Pipeleers-Marichal, M.; Donow, C.; Heitz, P.U.; Kloppel, G. Pathologic aspects of gastrinomas in patients with Zollinger-Ellison syndrome with and without multiple endocrine neoplasia type I. World J. Surg. 1993, 17, Kloppel, G.; Anlauf, M. Gastrinoma Morphological aspects. Wien. Klin. Wochenschr. 2007, 119, Anlauf, M.; Perren, A.; Henopp, T.; Rudolf, T.; Garbrecht, N.; Schmitt, A.; Raffel, A.; Gimm, O.; Weihe, E.; Knoefel, W.T.; et al. Allelic deletion of the MEN1 gene in duodenal gastrin and somatostatin cell neoplasms and their precursor lesions. Gut 2007, 56, Anlauf, M.; Perren, A.; Kloppel, G. Endocrine precursor lesions and microadenomas of the duodenum and pancreas with and without MEN1: Criteria, molecular concepts and clinical significance. Pathobiology 2007, 74, Rindi, G.; Kloppel, G.; Alhman, H.; Caplin, M.; Couvelard, A.; de Herder, W.W.; Erikssson, B.; Falchetti, A.; Falconi, M.; Komminoth, P.; et al. TNM staging of foregut (neuro)endocrine tumors: A consensus proposal including a grading system. Virchows Arch. 2006, 449, Triponez, F.; Dosseh, D.; Goudet, P.; Cougard, P.; Bauters, C.; Murat, A.; Cadiot, G.; Niccoli-Sire, P.; Chayvialle, J.A.; Calender, A.; et al. Epidemiology data on 108 MEN 1 patients from the GTE with isolated nonfunctioning tumors of the pancreas. Ann. Surg. 2006, 243, Berna, M.J.; Hoffmann, K.M.; Serrano, J.; Gibril, F.; Jensen, R.T. Serum gastrin in Zollinger-Ellison syndrome: I. Prospective study of fasting serum gastrin in 309 patients from the National Institutes of Health and comparison with 2229 cases from the literature. Medicine (Baltimore) 2006, 85, Kloppel, G.; Rindi, G.; Anlauf, M.; Perren, A.; Komminoth, P. Site-specific biology and pathology of gastroenteropancreatic neuroendocrine tumors. Virchows Arch. 2007, 451, S9 S Thompson, J.C.; Lewis, B.G.; Wiener, I.; Townsend, C.M., Jr. The role of surgery in the Zollinger-Ellison syndrome. Ann. Surg. 1983, 197, Weber, H.C.; Venzon, D.J.; Lin, J.T.; Fishbein, V.A.; Orbuch, M.; Strader, D.B.; Gibril, F.; Metz, D.C.; Fraker, D.L.; Norton, J.A.; et al. Determinants of metastatic rate and survival in patients with Zollinger-Ellison syndrome: A prospective long-term study. Gastroenterology 1995, 108, Donow, C.; Pipeleers-Marichal, M.; Schroder, S.; Stamm, B.; Heitz, P.U.; Kloppel, G. Surgical pathology of gastrinoma. Site, size, multicentricity, association with multiple endocrine neoplasia type 1, and malignancy. Cancer 1991, 68, Anlauf, M.; Schlenger, R.; Perren, A.; Bauersfeld, J.; Koch, C.A.; Dralle, H.; Raffel, A.; Knoefel, W.T.; Weihe, E.; Ruszniewski, P.; et al. Microadenomatosis of the endocrine pancreas in patients with and without the multiple endocrine neoplasia type 1 syndrome. Am. J. Surg. Pathol. 2006, 30, Pipeleers-Marichal, M.; Somers, G.; Willems, G.; Foulis, A.; Imrie, C.; Bishop, A.E.; Polak, J.M.; Hacki, W.H.; Stamm, B.; Heitz, P.U.; et al. Gastrinomas in the duodenums of patients with multiple endocrine neoplasia type 1 and the Zollinger-Ellison syndrome. N. Engl. J. Med. 1990, 322,
12 Cancers 2012, Roy, P.K.; Venzon, D.J.; Shojamanesh, H.; Abou-Saif, A.; Peghini, P.; Doppman, J.L.; Gibril, F.; Jensen, R.T. Zollinger-Ellison syndrome. Clinical presentation in 261 patients. Medicine (Baltimore) 2000, 79, Wong, H.; Yau, T.; Chan, P.; Ng, I.O.; Chan, G.; Hui, P.; Law, W.L.; Lo, C.M.; Hedley, A.J.; Epstein, R.J. PPI-delayed diagnosis of gastrinoma: Oncologic victim of pharmacologic success. Pathol. Oncol. Res. 2010, 16, Asgharian, B.; Turner, M.L.; Gibril, F.; Entsuah, L.K.; Serrano, J.; Jensen, R.T. Cutaneous tumors in patients with multiple endocrine neoplasm type 1 (MEN1) and gastrinomas: Prospective study of frequency and development of criteria with high sensitivity and specificity for MEN1. J. Clin. Endocrinol. Metab. 2004, 89, Goudet, P.; Bonithon-Kopp, C.; Murat, A.; Ruszniewski, P.; Niccoli, P.; Menegaux, F.; Chabrier, G.; Borson-Chazot, F.; Tabarin, A.; Bouchard, P.; et al. Gender-related differences in MEN1 lesion occurrence and diagnosis: A cohort study of 734 cases from the Groupe d'etude des Tumeurs Endocrines. Eur. J. Endocrinol. 2011, 165, Berna, M.J.; Hoffmann, K.M.; Long, S.H.; Serrano, J.; Gibril, F.; Jensen, R.T. Serum gastrin in Zollinger-Ellison syndrome: II. Prospective study of gastrin provocative testing in 293 patients from the National Institutes of Health and comparison with 537 cases from the literature. evaluation of diagnostic criteria, proposal of new criteria, and correlations with clinical and tumoral features. Medicine (Baltimore) 2006, 85, Itami, A.; Kato, M.; Komoto, I.; Doi, R.; Hosotani, R.; Shimada, Y.; Imamura, M. Human gastrinoma cells express calcium-sensing receptor. Life Sci. 2001, 70, Long, S.H.; Berna, M.J.; Thill, M.; Pace, A.; Pradhan, T.K.; Hoffmann, K.M.; Serrano, J.; Jensen, R.T. Secretin-receptor and secretin-receptor-variant expression in gastrinomas: Correlation with clinical and tumoral features and secretin and calcium provocative test results. J. Clin. Endocrinol. Metab. 2007, 92, Rehfeld, J.F.; Gingras, M.H.; Bardram, L.; Hilsted, L.; Goetze, J.P.; Poitras, P. The Zollinger-Ellison syndrome and mismeasurement of gastrin. Gastroenterology 2011, 140, Jensen, R.T.; Niederle, B.; Mitry, E.; Ramage, J.K.; Steinmuller, T.; Lewington, V.; Scarpa, A.; Sundin, A.; Perren, A.; Gross, D.; et al. Gastrinoma (duodenal and pancreatic). Neuroendocrinology 2006, 84, Gibril, F.; Reynolds, J.C.; Doppman, J.L.; Chen, C.C.; Venzon, D.J.; Termanini, B.; Weber, H.C.; Stewart, C.A.; Jensen, R.T. Somatostatin receptor scintigraphy: Its sensitivity compared with that of other imaging methods in detecting primary and metastatic gastrinomas. A prospective study. Ann. Intern. Med. 1996, 125, Brandi, M.L.; Gagel, R.F.; Angeli, A.; Bilezikian, J.P.; Beck-Peccoz, P.; Bordi, C.; Conte-Devolx, B.; Falchetti, A.; Gheri, R.G.; Libroia, A.; et al. Guidelines for diagnosis and therapy of MEN type 1 and type 2. J. Clin. Endocrinol. Metab. 2001, 86, Legmann, P.; Vignaux, O.; Dousset, B.; Baraza, A.J.; Palazzo, L.; Dumontier, I.; Coste, J.; Louvel, A.; Roseau, G.; Couturier, D.; Bonnin, A. Pancreatic tumors: Comparison of dual-phase helical CT and endoscopic sonography. Am. J. Roentgenol. 1998, 170, Klose, K.J.; Heverhagen, J.T. Localisation and staging of gastrin producing tumours using cross-sectional imaging modalities. Wien. Klin. Wochenschr. 2007, 119,
13 Cancers 2012, Fendrich, V.; Langer, P.; Waldmann, J.; Bartsch, D.K.; Rothmund, M. Management of sporadic and multiple endocrine neoplasia type 1 gastrinomas. Br. J. Surg. 2007, 94, Jensen, R.T.; Berna, M.J.; Bingham, D.B.; Norton, J.A. Inherited pancreatic endocrine tumor syndromes: Advances in molecular pathogenesis, diagnosis, management, and controversies. Cancer 2008, 113, Alexander, H.R.; Fraker, D.L.; Norton, J.A.; Bartlett, D.L.; Tio, L.; Benjamin, S.B.; Doppman, J.L.; Goebel, S.U.; Serrano, J.; Gibril, F.; et al. Prospective study of somatostatin receptor scintigraphy and its effect on operative outcome in patients with Zollinger-Ellison syndrome. Ann. Surg. 1998, 228, Raufman, J.P.; Collins, S.M.; Pandol, S.J.; Korman, L.Y.; Collen, M.J.; Cornelius, M.J.; Feld, M.K.; McCarthy, D.M.; Gardner, J.D.; Jensen, R.T. Reliability of symptoms in assessing control of gastric acid secretion in patients with Zollinger-Ellison syndrome. Gastroenterology 1983, 84, Maton, P.N.; Frucht, H.; Vinayek, R.; Wank, S.A.; Gardner, J.D.; Jensen, R.T. Medical management of patients with Zollinger-Ellison syndrome who have had previous gastric surgery: A prospective study. Gastroenterology 1988, 94, Metz, D.C.; Pisegna, J.R.; Fishbeyn, V.A.; Benya, R.V.; Feigenbaum, K.M.; Koviack, P.D.; Jensen, R.T. Currently used doses of omeprazole in Zollinger-Ellison syndrome are too high. Gastroenterology 1992, 103, Miller, L.S.; Vinayek, R.; Frucht, H.; Gardner, J.D.; Jensen, R.T.; Maton, P.N. Reflux esophagitis in patients with Zollinger-Ellison syndrome. Gastroenterology 1990, 98, Jensen, R.T. Management of the Zollinger-Ellison syndrome in patients with multiple endocrine neoplasia type 1. J. Intern. Med. 1998, 243, Akerstrom, G. Surgical treatment of carcinoids and endocrine pancreatic tumours. Acta Oncol. 1989, 28, Jensen, R.T.; Fraker, D.L. Zollinger-Ellison syndrome. Advances in treatment of gastric hypersecretion and the gastrinoma. JAMA 1994, 271, Norton, J.A.; Jensen, R.T. Unresolved surgical issues in the management of patients with Zollinger-Ellison syndrome. World J. Surg. 1991, 15, Bartsch, D.K.; Fendrich, V.; Langer, P.; Celik, I.; Kann, P.H.; Rothmund, M. Outcome of duodenopancreatic resections in patients with multiple endocrine neoplasia type 1. Ann. Surg. 2005, 242, Norton, J.A. Surgical treatment and prognosis of gastrinoma. Best Pract. Res. Clin. Gastroenterol. 2005, 19, Fraker, D.L.; Norton, J.A.; Alexander, H.R.; Venzon, D.J.; Jensen, R.T. Surgery in Zollinger-Ellison syndrome alters the natural history of gastrinoma. Ann. Surg. 1994, 220, Wilcox, C.M.; Seay, T.; Arcury, J.T.; Mohnen, J.; Hirschowitz, B.I. Zollinger-Ellison syndrome: Presentation, response to therapy, and outcome. Dig. Liver Dis. 2011, 43, Goudet, P.; Murat, A.; Binquet, C.; Cardot-Bauters, C.; Costa, A.; Ruszniewski, P.; Niccoli, P.; Menegaux, F.; Chabrier, G.; Borson-Chazot, F.; et al. Risk factors and causes of death in MEN1 disease. A GTE (Groupe d'etude des Tumeurs Endocrines) cohort study among 758 patients. World J. Surg. 2010, 34,
14 Cancers 2012, Mortellaro, V.E.; Hochwald, S.N.; McGuigan, J.E.; Copeland, E.M.; Vogel, S.B.; Grobmyer, S.R. Long-term results of a selective surgical approach to management of Zollinger-Ellison syndrome in patients with MEN-1. Am. Surg. 2009, 75, Skogseid, B.; Oberg, K.; Eriksson, B.; Juhlin, C.; Granberg, D.; Akerstrom, G.; Rastad, J. Surgery for asymptomatic pancreatic lesion in multiple endocrine neoplasia type I. World J. Surg. 1996, 20, Norton, J.A.; Jensen, R.T. Resolved and unresolved controversies in the surgical management of patients with Zollinger-Ellison syndrome. Ann. Surg. 2004, 240, Delcore, R.; Friesen, S.R. Role of pancreatoduodenectomy in the management of primary duodenal wall gastrinomas in patients with Zollinger-Ellison syndrome. Surgery 1992, 112, Jordan, P.H., Jr. A personal experience with pancreatic and duodenal neuroendocrine tumors. J. Am. Coll. Surg. 1999, 189, Kato, M.; Imamura, M.; Hosotani, R.; Shimada, Y.; Doi, R.; Itami, A.; Komoto, I.; Kosaka, M.T.T.; Konishi, J. Curative resection of microgastrinomas based on the intraoperative secretin test. World J. Surg. 2000, 24, Lairmore, T.C.; Chen, V.Y.; DeBenedetti, M.K.; Gillanders, W.E.; Norton, J.A.; Doherty, G.M. Duodenopancreatic resections in patients with multiple endocrine neoplasia type 1. Ann. Surg. 2000, 231, Lind, T.; Olbe, L. Long-term follow up of patients with Zollinger-Ellison syndrome (ZES). Acta Chir. Scand. 1989, 155, Norton, J.A.; Alexander, H.R.; Fraker, D.L.; Venzon, D.J.; Gibril, F.; Jensen, R.T. Comparison of surgical results in patients with advanced and limited disease with multiple endocrine neoplasia type 1 and Zollinger-Ellison syndrome. Ann. Surg. 2001, 234, Sarmiento, J.M.; Farnell, M.B.; Que, F.G.; Nagorney, D.M. Pancreaticoduodenectomy for islet cell tumors of the head of the pancreas: Long-term survival analysis. World J. Surg. 2002, 26, Schroder, W.; Holscher, A.H.; Beckurts, T.; Richter, T.H.; Hofler, H.; Siewert, J.R. Duodenal microgastrinomas associated with Zollinger-Ellison syndrome. Hepatogastroenterology 1996, 43, Waddell, W.R.; Coppinger, W.R.; Loughry, R.W. Pancreaticoduodenectomy for Zollinger-Ellison syndrome. Ann. Surg. 1968, 168, Tonelli, F.; Fratini, G.; Falchetti, A.; Nesi, G.; Brandi, M.L. Surgery for gastroenteropancreatic tumours in multiple endocrine neoplasia type 1: Review and personal experience. J. Intern. Med. 2005, 257, Gibril, F.; Venzon, D.J.; Ojeaburu, J.V.; Bashir, S.; Jensen, R.T. Prospective study of the natural history of gastrinoma in patients with MEN1: Definition of an aggressive and a nonaggressive form. J. Clin. Endocrinol. Metab. 2001, 86, Imamura, M.; Komoto, I.; Doi, R.; Onodera, H.; Kobayashi, H.; Kawai, Y. New pancreas-preserving total duodenectomy technique. World J. Surg. 2005, 29, Imamura, M.; Komoto, I.; Ota, S. Changing treatment strategy for gastrinoma in patients with Zollinger-Ellison syndrome. World J. Surg. 2006, 30, 1 11.
15 Cancers 2012, Imamura, M.; Komoto, I.; Ota, S.; Hiratsuka, T.; Kosugi, S.; Doi, R.; Awane, M.; Inoue, N. Biochemically curative surgery for gastrinoma in multiple endocrine neoplasia type 1 patients. World J. Gastroenterol. 2011, 17, Norton, J.A.; Doherty, G.M.; Fraker, D.L.; Alexander, H.R.; Doppman, J.L.; Venzon, D.J.; Gibril, F.; Jensen, R.T. Surgical treatment of localized gastrinoma within the liver: A prospective study. Surgery 1998, 124, de Jong, M.; Kwekkeboom, D.; Valkema, R.; Krenning, E.P. Radiolabelled peptides for tumour therapy: Current status and future directions. Plenary lecture at the EANM Eur. J. Nucl. Med. Mol. Imaging 2003, 30, Kwekkeboom, D.J.; Bakker, W.H.; Kam, B.L.; Teunissen, J.J.; Kooij, P.P.; de Herder, W.W.; Feelders, R.A.; van Eijck, C.H.; de Jong, M.; Srinivasan, A.; et al. Treatment of patients with gastro-entero-pancreatic (GEP) tumours with the novel radiolabelled somatostatin analogue [177Lu-DOTA(0),Tyr3] octreotate. Eur. J. Nucl. Med. Mol. Imaging 2003, 30, Kwekkeboom, D. Department of Nuclear Medicine, Erasmus Medical Center, Rotterdam, The Netherlands. Personal communication, Grozinsky-Glasberg, S.; Barak, D.; Fraenkel, M.; Walter, M.A.; Mueller-Brand, J.; Eckstein, J.; Applebaum, L.; Shimon, I.; Gross, D.J. Peptide receptor radioligand therapy is an effective treatment for the long-term stabilization of malignant gastrinomas. Cancer 2011, 117, Shojamanesh, H.; Gibril, F.; Louie, A.; Ojeaburu, J.V.; Bashir, S.; Abou-Saif, A.; Jensen, R.T. Prospective study of the antitumor efficacy of long-term octreotide treatment in patients with progressive metastatic gastrinoma. Cancer 2002, 94, de Herder, W.W.; Lamberts, S.W. Clinical endocrinology and metabolism. Gut endocrine tumours. Best Pract. Res. Clin. Endocrinal. Metab. 2004, 18, Rindi, G.; Bordi, C.; Rappel, S.; La Rosa, S.; Stolte, M.; Solcia, E. Gastric carcinoids and neuroendocrine carcinomas: Pathogenesis, pathology, and behavior. World J. Surg. 1996, 20, Lehy, T.; Cadiot, G.; Mignon, M.; Ruszniewski, P.; Bonfils, S. Influence of multiple endocrine neoplasia type 1 on gastric endocrine cells in patients with the Zollinger-Ellison syndrome. Gut 1992, 33, Cadiot, G.; Laurent-Puig, P.; Thuille, B.; Lehy, T.; Mignon, M.; Olschwang, S. Is the multiple endocrine neoplasia type 1 gene a suppressor for fundic argyrophil tumors in the Zollinger-Ellison syndrome? Gastroenterology 1993, 105, Debelenko, L.V.; Emmert-Buck, M.R.; Zhuang, Z.; Epshteyn, E.; Moskaluk, C.A.; Jensen, R.T.; Liotta, L.A.; Lubensky, I.A. The multiple endocrine neoplasia type I gene locus is involved in the pathogenesis of type II gastric carcinoids. Gastroenterology 1997, 113, Solcia, E.; Bordi, C.; Creutzfeldt, W.; Dayal, Y.; Dayan, A.D.; Falkmer, S.; Grimelius, L.; Havu, N. Histopathological classification of nonantral gastric endocrine growths in man. Digestion 1988, 41,
Surgical treatment and prognosis of gastrinoma
 Best Practice & Research Clinical Gastroenterology Vol. 19, No. 5, pp. 799 805, 2005 doi:10.1016/j.bpg.2005.05.003 available online at http://www.sciencedirect.com 10 Surgical treatment and prognosis of
Best Practice & Research Clinical Gastroenterology Vol. 19, No. 5, pp. 799 805, 2005 doi:10.1016/j.bpg.2005.05.003 available online at http://www.sciencedirect.com 10 Surgical treatment and prognosis of
Gastrinoma: Medical Management. Haley Gallup
 Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Surgical Management of Zollinger-Ellison Syndrome; State of the Art
 Surgical Management of Zollinger-Ellison Syndrome; State of the Art Ellen H. Morrow, MD, JeffreyA. Norton, MD* KEYWORDS Gastrinoma Surgery Diagnosis Localization Outcome MEN-1 Zollinger-Ellison Syndrome
Surgical Management of Zollinger-Ellison Syndrome; State of the Art Ellen H. Morrow, MD, JeffreyA. Norton, MD* KEYWORDS Gastrinoma Surgery Diagnosis Localization Outcome MEN-1 Zollinger-Ellison Syndrome
AN ARGUMENT FOR SURGERY FOR GASTRINOMA. Lauren Wilson R1 General Surgery
 AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
AN ARGUMENT FOR SURGERY FOR GASTRINOMA Lauren Wilson R1 General Surgery WHAT IS A GASTRINOMA? Gastrin secreting cells derived from multipotential stem cells of endodermal origin or enteroendocrine cells
Diagnosis abnormal morphology and /or abnormal biochemistry
 Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
Diagnosis abnormal morphology and /or abnormal biochemistry MEN 1 GEP Tumours Pancreatico-Nodal (-Duodenal) Affects 35-80% of MEN1 patients Functioning or non functioning Hyperplasia microadenoma macrotumours
MINISYMPOSIUM MEN & VHL. N. W. THOMPSON From the Division of Endocrine Surgery, University of Michigan, Ann Arbor, MI, USA
 Journal of Internal Medicine 1998; 243: 495 500 MINISYMPOSIUM MEN & VHL Current concepts in the surgical management of multiple endocrine neoplasia type 1 pancreatic-duodenal disease. Results in the treatment
Journal of Internal Medicine 1998; 243: 495 500 MINISYMPOSIUM MEN & VHL Current concepts in the surgical management of multiple endocrine neoplasia type 1 pancreatic-duodenal disease. Results in the treatment
Surgical treatment of neuroendocrine metastases
 Best Practice & Research Clinical Gastroenterology Vol. 19, No. 4, pp. 577 583, 2005 doi:10.1016/j.bpg.2005.04.003 available online at http://www.sciencedirect.com 6 Surgical treatment of neuroendocrine
Best Practice & Research Clinical Gastroenterology Vol. 19, No. 4, pp. 577 583, 2005 doi:10.1016/j.bpg.2005.04.003 available online at http://www.sciencedirect.com 6 Surgical treatment of neuroendocrine
The role of routine surgical exploration for gastrinoma
 ORIGINAL ARTICLES Surgery Increases Survival in Patients With Gastrinoma Jeffrey A. Norton, MD, Douglas L. Fraker, MD, H. R. Alexander, MD, Fathia Gibril, MD, David J. Liewehr, MS, David J. Venzon, PhD,
ORIGINAL ARTICLES Surgery Increases Survival in Patients With Gastrinoma Jeffrey A. Norton, MD, Douglas L. Fraker, MD, H. R. Alexander, MD, Fathia Gibril, MD, David J. Liewehr, MS, David J. Venzon, PhD,
Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1
 CLINICS 2012;67(S1):173-178 DOI:10.6061/clinics/2012(Sup01)29 REVIEW Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1 Göran Åkerström, Peter Stålberg,
CLINICS 2012;67(S1):173-178 DOI:10.6061/clinics/2012(Sup01)29 REVIEW Surgical management of pancreatico-duodenal tumors in multiple endocrine neoplasia syndrome type 1 Göran Åkerström, Peter Stålberg,
EDUCATION PRACTICE. Diagnosis of the Zollinger Ellison Syndrome. Clinical Scenario. The Problem. Hypergastrinemia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:126 130 EDUCATION PRACTICE Diagnosis of the Zollinger Ellison Syndrome DAVID C. METZ Division of Gastroenterology, Hospital of the University of Pennsylvania,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:126 130 EDUCATION PRACTICE Diagnosis of the Zollinger Ellison Syndrome DAVID C. METZ Division of Gastroenterology, Hospital of the University of Pennsylvania,
Color Codes Pathology and Genetics Medicine and Clinical Pathology Surgery Imaging
 Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Sporadic versus hereditary gastrinomas of the duodenum and pancreas: Distinct clinico-pathological and epidemiological features
 PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 September 14; 12(34): 5440-5446 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. EDITORIAL
PO Box 2345, Beijing 100023, China World J Gastroenterol 2006 September 14; 12(34): 5440-5446 World Journal of Gastroenterology ISSN 1007-9327 wjg@wjgnet.com 2006 The WJG Press. All rights reserved. EDITORIAL
Original Report. Carcinoid Tumors of the Stomach: A Clinical and Radiographic Study
 Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Aaron J. Binstock 1 C. Daniel Johnson 1 David H. Stephens 1 Ricardo V. Lloyd 2 Joel G. Fletcher 1 Received July 25, 2000; accepted after revision September 29, 2000. 1 Department of Radiology, Mayo Clinic,
Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Management of pancreatic neuroendocrine tumors in patients with MEN 1
 Review Article Management of pancreatic neuroendocrine tumors in patients with MEN 1 Samira M. Sadowski 1, Frederic Triponez 2 1 Endocrine Oncology Branch, National Institutes of Health, Bethesda, MD 20892,
Review Article Management of pancreatic neuroendocrine tumors in patients with MEN 1 Samira M. Sadowski 1, Frederic Triponez 2 1 Endocrine Oncology Branch, National Institutes of Health, Bethesda, MD 20892,
Management of Pancreatic Islet Cell Tumors
 Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Management of Pancreatic Islet Cell Tumors Ravi Dhanisetty, MD November 5, 2009 Morbidity and Mortality Conference Case Presentation 42 yr female with chronic abdominal pain. PMHx: Uterine fibroids Medications:
Multiple Endocrine Neoplasia Type 1
 Journal of Surgical Oncology 2005;89:143 150 Multiple Endocrine Neoplasia Type 1 GERARD M. DOHERTY, MD* NW Thompson Professor of Surgery, University of Michigan, Ann Arbor, Michigan Multiple endocrine
Journal of Surgical Oncology 2005;89:143 150 Multiple Endocrine Neoplasia Type 1 GERARD M. DOHERTY, MD* NW Thompson Professor of Surgery, University of Michigan, Ann Arbor, Michigan Multiple endocrine
SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME
 SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME JEFFREY A. NORTON, M.D., DOUGLAS L. FRAKER, M.D., H. RICHARD ALEXANDER, M.D., DAVID J. VENZON, PH.D., JOHN
SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME SURGERY TO CURE THE ZOLLINGER ELLISON SYNDROME JEFFREY A. NORTON, M.D., DOUGLAS L. FRAKER, M.D., H. RICHARD ALEXANDER, M.D., DAVID J. VENZON, PH.D., JOHN
Type 2 gastric neuroendocrine tumor: report of one case
 Case Report Type 2 gastric neuroendocrine tumor: report of one case Yuanliang Li, Xin Su, Huangying Tan Department of Integrative Oncology, China-Japan Friendship Hospital, Beijing 100029, China Correspondence
Case Report Type 2 gastric neuroendocrine tumor: report of one case Yuanliang Li, Xin Su, Huangying Tan Department of Integrative Oncology, China-Japan Friendship Hospital, Beijing 100029, China Correspondence
NEUROENDOCRINE CARCINOID TUMORS PANCREATIC NEUROENDOCRINE TUMORS
 University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
University of Miami Jackson Memorial Hospital Role of the Surgeon in the Approach to Neuroendocrine tumors Dido Franceschi, MD Professor of Surgery University of Miami Karzinoide Siegfried Oberndorfer,
Multiple endocrine neoplasia type 1 (MEN1) is an autosomal
 ORIGINAL ARTICLES Outcome of Duodenopancreatic Resections in Patients With Multiple Endocrine Neoplasia Type 1 Detlef K. Bartsch, MD,* Volker Fendrich, MD,* Peter Langer, MD,* Ilhan Celik, MD, Peter H.
ORIGINAL ARTICLES Outcome of Duodenopancreatic Resections in Patients With Multiple Endocrine Neoplasia Type 1 Detlef K. Bartsch, MD,* Volker Fendrich, MD,* Peter Langer, MD,* Ilhan Celik, MD, Peter H.
Multiple endocrine neoplasia type 1: duodenopancreatic tumours
 Journal of Internal Medicine 2003; 253: 590 598 MINISYMPOSIUM Multiple endocrine neoplasia type 1: duodenopancreatic tumours G. M. DOHERTY & N. W. THOMPSON Division of Endocrine Surgery, Department of
Journal of Internal Medicine 2003; 253: 590 598 MINISYMPOSIUM Multiple endocrine neoplasia type 1: duodenopancreatic tumours G. M. DOHERTY & N. W. THOMPSON Division of Endocrine Surgery, Department of
NET und NEC. Endoscopic and oncologic therapy
 NET und NEC Endoscopic and oncologic therapy Classification well-differentiated NET - G1 and G2 - carcinoid poorly-differentiated NEC - G3 - like SCLC well differentiated NET G3 -> elevated proliferation
NET und NEC Endoscopic and oncologic therapy Classification well-differentiated NET - G1 and G2 - carcinoid poorly-differentiated NEC - G3 - like SCLC well differentiated NET G3 -> elevated proliferation
Zollinger-Ellison Syndrome
 Zollinger-Ellison Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Zollinger-Ellison syndrome (ZES)? ZES
Zollinger-Ellison Syndrome National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Zollinger-Ellison syndrome (ZES)? ZES
Endocrine pancreatic tumors: factors correlated with survival
 Original article Annals of Oncology 6: 86 8, 25 doi:.93/annonc/mdi358 Published online 5 August 25 Endocrine pancreatic tumors: factors correlated with survival P. Tomassetti *, D. Campana, L. Piscitelli,
Original article Annals of Oncology 6: 86 8, 25 doi:.93/annonc/mdi358 Published online 5 August 25 Endocrine pancreatic tumors: factors correlated with survival P. Tomassetti *, D. Campana, L. Piscitelli,
Case Report A Perplexing Case of Abdominal Pain That Led to the Diagnosis of Zollinger-Ellison Syndrome
 Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 7636952, 4 pages https://doi.org/10.1155/2017/7636952 Case Report A Perplexing Case of Abdominal Pain That Led to the Diagnosis
Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 7636952, 4 pages https://doi.org/10.1155/2017/7636952 Case Report A Perplexing Case of Abdominal Pain That Led to the Diagnosis
Gastroenteropancreatic Neuroendocrine Tumors in Multiple Endocrine Neoplasia Type 1
 Cancers 2012, 4, 504-522; doi:10.3390/cancers4020504 Review OPEN ACCESS cancers ISSN 2072-6694 www.mdpi.com/journal/cancers Gastroenteropancreatic Neuroendocrine Tumors in Multiple Endocrine Neoplasia
Cancers 2012, 4, 504-522; doi:10.3390/cancers4020504 Review OPEN ACCESS cancers ISSN 2072-6694 www.mdpi.com/journal/cancers Gastroenteropancreatic Neuroendocrine Tumors in Multiple Endocrine Neoplasia
Sonic hedgehog and pancreatic-duodenal homeobox 1 expression distinguish between duodenal and pancreatic gastrinomas
 Endocrine-Related Cancer (2009) 16 613 622 Sonic hedgehog and pancreatic-duodenal homeobox 1 expression distinguish between duodenal and pancreatic gastrinomas Volker Fendrich 1, Ricarda Ramerth 1, Jens
Endocrine-Related Cancer (2009) 16 613 622 Sonic hedgehog and pancreatic-duodenal homeobox 1 expression distinguish between duodenal and pancreatic gastrinomas Volker Fendrich 1, Ricarda Ramerth 1, Jens
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors
 Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Surgical Therapy of GEP-NET: An Overview
 Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Surgical Therapy of GEP-NET: An Overview Pierce K.H Chow MBBS, MMed, FRCSE, FAMS, PhD Professor, Duke-NUS Graduate School of Medicine Senior Consultant Surgeon, Singapore General Hospital Visiting Senior
Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome
 GASTROENTEROLOGY 1987;92;905-12 Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome S. A. WANK, J. L. DOPPMAN, D. L. MILLER,
GASTROENTEROLOGY 1987;92;905-12 Prospective Study of the Ability of Computed Axial Tomography to Localize Gastrinomas in Patients With Zollinger-Ellison Syndrome S. A. WANK, J. L. DOPPMAN, D. L. MILLER,
Lu Hao Feng et al., IJSIT, 2016, 5(6),
 AN UNUSUAL PRESENTATION OF PANCREATIC VASOACTIVE INTESTINAL PEPTIDE TUMOUR (VIP OMAS) WITH GASTROINTESTINAL STROMAL TUMOUR (GIST) WITHOUT HYPOKALEMIA AND HPERCALCEMIA: A CASE REPORT WITH REVIEW ARTICLES
AN UNUSUAL PRESENTATION OF PANCREATIC VASOACTIVE INTESTINAL PEPTIDE TUMOUR (VIP OMAS) WITH GASTROINTESTINAL STROMAL TUMOUR (GIST) WITHOUT HYPOKALEMIA AND HPERCALCEMIA: A CASE REPORT WITH REVIEW ARTICLES
Peptic ulcer disease. Nomin-Erdene. D SOM-531
 Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Imaging and Management of Pancreatic Endocrine Tumors in MEN 1
 October 20, 2008 Imaging and Management of Pancreatic Endocrine Tumors in MEN 1 Marie Elaine Stevens Georgetown University School of Medicine, Year IV Dr. Agenda Discuss Our Patient s Presentation Review
October 20, 2008 Imaging and Management of Pancreatic Endocrine Tumors in MEN 1 Marie Elaine Stevens Georgetown University School of Medicine, Year IV Dr. Agenda Discuss Our Patient s Presentation Review
Lutetium-DOTA TATE Treatment of inoperable GEP NETs
 Logo 177 Lutetium-DOTA TATE Treatment of inoperable GEP NETs Dr. Augusto Llamas-Olier. Nuclear medicine department. Dr. Maria Cristina Martínez*, Dr. Alfonso Lozano** and Dr. Augusto Llamas-Olier*. *Nuclear
Logo 177 Lutetium-DOTA TATE Treatment of inoperable GEP NETs Dr. Augusto Llamas-Olier. Nuclear medicine department. Dr. Maria Cristina Martínez*, Dr. Alfonso Lozano** and Dr. Augusto Llamas-Olier*. *Nuclear
Comparison study of gastrinomas between gastric and non-gastric origins
 Huang et al. World Journal of Surgical Oncology (2015) 13:202 DOI 10.1186/s12957-015-0614-6 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Comparison study of gastrinomas between gastric and non-gastric origins
Huang et al. World Journal of Surgical Oncology (2015) 13:202 DOI 10.1186/s12957-015-0614-6 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Comparison study of gastrinomas between gastric and non-gastric origins
Clinical Outcome Using Lansoprazole in Acid Hypersecretors With and Without Zollinger-Ellison Syndrome: A 13-Year Prospective Study
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:39 48 Clinical Outcome Using Lansoprazole in Acid Hypersecretors With and Without Zollinger-Ellison Syndrome: A 13-Year Prospective Study BASIL I. HIRSCHOWITZ,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:39 48 Clinical Outcome Using Lansoprazole in Acid Hypersecretors With and Without Zollinger-Ellison Syndrome: A 13-Year Prospective Study BASIL I. HIRSCHOWITZ,
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Multiple endocrine neoplasia type 1 (MEN1) is an
 JCEM ONLINE Advances in Genetics Endocrine Care Higher Risk of Aggressive Pancreatic Neuroendocrine Tumors in MEN1 Patients With MEN1 Mutations Affecting the CHES1 Interacting MENIN Domain Detlef K. Bartsch,
JCEM ONLINE Advances in Genetics Endocrine Care Higher Risk of Aggressive Pancreatic Neuroendocrine Tumors in MEN1 Patients With MEN1 Mutations Affecting the CHES1 Interacting MENIN Domain Detlef K. Bartsch,
GI CARCINOID Dr Mussawar Iqbal Consultant Oncologist Hull and East Yorkshire Hospitals NHS Trust
 GI CARCINOID Dr Mussawar Iqbal Consultant Oncologist Hull and East Yorkshire Hospitals NHS Trust Introduction Carcinoid was old term, introduced in 1906 by German pathologist Cancinoma like More recent
GI CARCINOID Dr Mussawar Iqbal Consultant Oncologist Hull and East Yorkshire Hospitals NHS Trust Introduction Carcinoid was old term, introduced in 1906 by German pathologist Cancinoma like More recent
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
CASE REPORT Zollinger-Ellison syndrome: an unusual case of chronic diarrhoea in a child
 Malaysian J Pathol 2016; 38(3) : 321 325 CASE REPORT Zollinger-Ellison syndrome: an unusual case of chronic diarrhoea in a child R GOYAL MD, U DEBI* MD, P DEY** MD, KK PRASAD*** MD, FICPATH and BR THAPA
Malaysian J Pathol 2016; 38(3) : 321 325 CASE REPORT Zollinger-Ellison syndrome: an unusual case of chronic diarrhoea in a child R GOYAL MD, U DEBI* MD, P DEY** MD, KK PRASAD*** MD, FICPATH and BR THAPA
Oberndofer 1907 Illeal Serotonin Secreting Tumor Carcinoid (Karzinoide)
 GEP-NET Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas Oberndofer 1907 Illeal Serotonin Secreting Tumor Carcinoid (Karzinoide) 1 Histogenesis 16 different
GEP-NET Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas Oberndofer 1907 Illeal Serotonin Secreting Tumor Carcinoid (Karzinoide) 1 Histogenesis 16 different
Recent standardization of treatment strategy for pancreatic neuroendocrine tumors
 Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i36.4519 World J Gastroenterol 2010 September 28; 16(36): 4519-4525 ISSN 1007-9327 (print) 2010 Baishideng.
Online Submissions: http://www.wjgnet.com/1007-9327office wjg@wjgnet.com doi:10.3748/wjg.v16.i36.4519 World J Gastroenterol 2010 September 28; 16(36): 4519-4525 ISSN 1007-9327 (print) 2010 Baishideng.
A retrospective analysis of neuroendocrine tumour of pancreas: a single institute study
 International Journal of Research in Medical Sciences Chheda YP et al. Int J Res Med Sci. 2015 Nov;3(11):3041-3045 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150928
International Journal of Research in Medical Sciences Chheda YP et al. Int J Res Med Sci. 2015 Nov;3(11):3041-3045 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150928
Neuroendocrine Tumors
 Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Neuroendocrine Tumors Neuroendocrine tumors arise from cells that release a hormone in response to a signal from the nervous system. Neuro refers to the nervous system. Endocrine refers to the hormones.
Carcinoid Tumors: The Beginning and End. Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011
 Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Endoscopic Ultrasound Is Highly Accurate and Directs Management in Patients With Neuroendocrine Tumors of the Pancreas
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 95, No. 9, 2000 2000 by Am. Coll. of Gastroenterology ISSN 0002-9270/00/$20.00 Published by Elsevier Science Inc. PII S0002-9270(00)01272-7 Endoscopic Ultrasound
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 95, No. 9, 2000 2000 by Am. Coll. of Gastroenterology ISSN 0002-9270/00/$20.00 Published by Elsevier Science Inc. PII S0002-9270(00)01272-7 Endoscopic Ultrasound
Endoscopic Treatment of Duodenal Neuroendocrine Tumors
 CASE REPORT Clin Endosc 2013;46:656-661 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2013.46.6.656 Open Access Endoscopic Treatment of Duodenal Neuroendocrine Tumors Sang
CASE REPORT Clin Endosc 2013;46:656-661 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2013.46.6.656 Open Access Endoscopic Treatment of Duodenal Neuroendocrine Tumors Sang
Gastrointestinal pathology 2018 lecture 4. Dr Heyam Awad FRCPath
 Gastrointestinal pathology 2018 lecture 4 Dr Heyam Awad FRCPath Topics to be covered Peptic ulcer disease Hiatal hernia Gastric neoplasms Peptic ulcer disease (PUD)= chronic gastric ulcer Causes H pylori
Gastrointestinal pathology 2018 lecture 4 Dr Heyam Awad FRCPath Topics to be covered Peptic ulcer disease Hiatal hernia Gastric neoplasms Peptic ulcer disease (PUD)= chronic gastric ulcer Causes H pylori
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL NEUROENDOCRINE GASTRO-ENTERO-PANCREATIC TUMOURS GI Site Group Neuroendocrine gastro-entero-pancreatic tumours Authors: Dr.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL NEUROENDOCRINE GASTRO-ENTERO-PANCREATIC TUMOURS GI Site Group Neuroendocrine gastro-entero-pancreatic tumours Authors: Dr.
Hypochlorhydria and Achlorhydria Are Associated With False-Positive Secretin Stimulation Testing for Zollinger-Ellison Syndrome
 ORIGINAL ARTICLE Hypochlorhydria and Achlorhydria Are Associated With False-Positive Secretin Stimulation Testing for Zollinger-Ellison Syndrome Pari Shah, MD, MSCE,* Maneesh H. Singh, MD,Þ Yu-Xiao Yang,
ORIGINAL ARTICLE Hypochlorhydria and Achlorhydria Are Associated With False-Positive Secretin Stimulation Testing for Zollinger-Ellison Syndrome Pari Shah, MD, MSCE,* Maneesh H. Singh, MD,Þ Yu-Xiao Yang,
Growth rate of small pancreatic neuroendocrine tumors in multiple endocrine neoplasia type 1: results from an endoscopic ultrasound based cohort study
 Growth rate of small pancreatic neuroendocrine tumors in multiple endocrine neoplasia type 1: results from an endoscopic ultrasound based cohort study Authors Wouter F. W. Kappelle 1,GerlofD.Valk 2,MaxLeenders
Growth rate of small pancreatic neuroendocrine tumors in multiple endocrine neoplasia type 1: results from an endoscopic ultrasound based cohort study Authors Wouter F. W. Kappelle 1,GerlofD.Valk 2,MaxLeenders
Diagnosing and monitoring NET
 Diagnosing and monitoring NET Inaccurate or delayed diagnosis of neuroendocrine tumors (NET) is common, because many NET are small and asymptomatic. 1 When symptoms are present, they are usually nonspecific
Diagnosing and monitoring NET Inaccurate or delayed diagnosis of neuroendocrine tumors (NET) is common, because many NET are small and asymptomatic. 1 When symptoms are present, they are usually nonspecific
Staging of digestive endocrine tumours using helical computed tomography and somatostatin receptor scintigraphy
 Original article Annals of Oncology 14: 586 591, 2003 DOI: 10.1093/annonc/mdg160 Staging of digestive endocrine tumours using helical computed tomography and somatostatin receptor scintigraphy F. Panzuto
Original article Annals of Oncology 14: 586 591, 2003 DOI: 10.1093/annonc/mdg160 Staging of digestive endocrine tumours using helical computed tomography and somatostatin receptor scintigraphy F. Panzuto
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID
 ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
CASE REPORT. Introduction. Case Report. Kimitoshi Kubo 1, Noriko Kimura 2, Katsuhiro Mabe 1, Yusuke Nishimura 1 and Mototsugu Kato 1
 doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
Multiple Endocrine Neoplasia Type 1: A Case Report With Review of Imaging Findings
 CASE REPORT Ochsner Journal 18:170 175, 2018 Academic Division of Ochsner Clinic Foundation DOI: 10.31486/toj.17.0019 Multiple Endocrine Neoplasia Type 1: A Case Report With Review of Imaging Findings
CASE REPORT Ochsner Journal 18:170 175, 2018 Academic Division of Ochsner Clinic Foundation DOI: 10.31486/toj.17.0019 Multiple Endocrine Neoplasia Type 1: A Case Report With Review of Imaging Findings
Index. Surg Oncol Clin N Am 15 (2006) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 15 (2006) 681 685 Index Note: Page numbers of article titles are in boldface type. A Ablative therapy, for liver metastases in patients with neuroendocrine tumors, 517 with radioiodine
Surg Oncol Clin N Am 15 (2006) 681 685 Index Note: Page numbers of article titles are in boldface type. A Ablative therapy, for liver metastases in patients with neuroendocrine tumors, 517 with radioiodine
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life.
 B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear
 Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Imaging Pancreatic Neuroendocrine Tumors (PNETs): CT, MRI, EUS, Nuclear Eric Tamm, M.D. Department of Diagnostic Radiology Division of Diagnostic Imaging MD Anderson Cancer Center Houston, TX Disclosure
Endocrine Tumors of the Gastrointestinal System. F. V. Nowak Ohio University March 22, 2005
 Endocrine Tumors of the Gastrointestinal System F. V. Nowak Ohio University March 22, 2005 Gastroenteropancreatic Endocrine System Clear cells of endodermal origin found in the pancreas, stomach, small
Endocrine Tumors of the Gastrointestinal System F. V. Nowak Ohio University March 22, 2005 Gastroenteropancreatic Endocrine System Clear cells of endodermal origin found in the pancreas, stomach, small
Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas
 Yonsei Medical Journal Vol. 47, No. 6, pp. 833-839, 2006 Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas Chang Moo Kang, Se Ho Park, Kyung Sik Kim, Jin Sub Choi, Woo Jung Lee,
Yonsei Medical Journal Vol. 47, No. 6, pp. 833-839, 2006 Surgical Experiences of Functioning Neuroendocrine Neoplasm of the Pancreas Chang Moo Kang, Se Ho Park, Kyung Sik Kim, Jin Sub Choi, Woo Jung Lee,
Case Report. Ameya D. Puranik, MD, FEBNM; Harshad R. Kulkarni, MD; Aviral Singh, MD; Richard P. Baum, MD, PhD ABSTRACT
 Case Report 8-YEAR SURVIVAL WITH A METASTATIC THYMIC NEUROENDOCRINE TUMOR: EMPHASIS ON REDEFINING TREATMENT OBJECTIVES USING PERSONALIZED PEPTIDE RECEPTOR RADIONUCLIDE THERAPY WITH 177 Lu- AND 90 Y-LABELED
Case Report 8-YEAR SURVIVAL WITH A METASTATIC THYMIC NEUROENDOCRINE TUMOR: EMPHASIS ON REDEFINING TREATMENT OBJECTIVES USING PERSONALIZED PEPTIDE RECEPTOR RADIONUCLIDE THERAPY WITH 177 Lu- AND 90 Y-LABELED
Usefulness of somatostatin receptor scintigraphy
 Gutl997;41: 107-114 Presented in part at the AGA meeting in San Francisco, USA, 1996, and published in abstract form as Gastroenterology 1996; 110: 380. CHU Bichat-Claude- Bernard, 46, rue Henri-Huchard,
Gutl997;41: 107-114 Presented in part at the AGA meeting in San Francisco, USA, 1996, and published in abstract form as Gastroenterology 1996; 110: 380. CHU Bichat-Claude- Bernard, 46, rue Henri-Huchard,
Imaging of Neuroendocrine Metastases
 Imaging of Neuroendocrine Metastases Aoife Kilcoyne, Shaunagh McDermott, Colin McCarthy,Manuel Patino, Dushyant Sahani, Michael Blake Abdominal Imaging Division Massachusetts General Hospital Disclosure
Imaging of Neuroendocrine Metastases Aoife Kilcoyne, Shaunagh McDermott, Colin McCarthy,Manuel Patino, Dushyant Sahani, Michael Blake Abdominal Imaging Division Massachusetts General Hospital Disclosure
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Rare GI Malignancies
 Rare GI Malignancies Jordan Karlitz, MD Associate Professor of Medicine, Division of Gastroenterology Director, Hereditary GI Cancer and Genetics Program Tulane University School of Medicine Outline Gastrointestinal
Rare GI Malignancies Jordan Karlitz, MD Associate Professor of Medicine, Division of Gastroenterology Director, Hereditary GI Cancer and Genetics Program Tulane University School of Medicine Outline Gastrointestinal
Neuro-endocrine and pancreatic non-adenocarcinomas. Marc Engelbrecht, AMC, Amsterdam
 Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Neuro-endocrine and pancreatic non-adenocarcinomas Marc Engelbrecht, AMC, Amsterdam Pancreatic Tumors q Epithelial Exocrine q Mesenchymal Ductal Adenocarcinoma (85-95%) Metastasis Lymfoma Acinar Cell Carcinoma
Multifocal Gastric Carcinoid Tumor in a Patient with Pernicious Anemia Receiving Lansoprazole
 Digestive Diseases and Sciences, Vol. 50, No. 3 (March 2005), pp. 509 513 ( C 2005) DOI: 10.1007/s10620-005-2466-3 CASE REPORT Multifocal Gastric Carcinoid Tumor in a Patient with Pernicious Anemia Receiving
Digestive Diseases and Sciences, Vol. 50, No. 3 (March 2005), pp. 509 513 ( C 2005) DOI: 10.1007/s10620-005-2466-3 CASE REPORT Multifocal Gastric Carcinoid Tumor in a Patient with Pernicious Anemia Receiving
Rpts. GENERAL General Schedule (Code GE) Program Prescriber type: Dental Medical Practitioners Nurse practitioners Optometrists Midwives
 Esomeprazole 20mg Name, Restriction, Manner of esomeprazole 20 mg enteric tablet, 30 (8886Q) (029W) Gastric ulcer Peptic ulcer Treatment Phase: Initial treatment The therapy must be for initial treatment
Esomeprazole 20mg Name, Restriction, Manner of esomeprazole 20 mg enteric tablet, 30 (8886Q) (029W) Gastric ulcer Peptic ulcer Treatment Phase: Initial treatment The therapy must be for initial treatment
Community Case. Saeed Awan R5
 Community Case Saeed Awan R5 18 year old presents to ER with history of pain right lower quadrant for three days. Nauseated, denies vomiting and bowel movements normal and no urinary complaint. Admitted
Community Case Saeed Awan R5 18 year old presents to ER with history of pain right lower quadrant for three days. Nauseated, denies vomiting and bowel movements normal and no urinary complaint. Admitted
Is Endoscopic Resection for Type 1 Gastric Neuroendocrine Tumors Essential for Treatment?: Multicenter, Retrospective Long-term Follow-up Results
 ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2016.16.1.13 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2016;16(1):13-18 Is Endoscopic Resection for Type
ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2016.16.1.13 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2016;16(1):13-18 Is Endoscopic Resection for Type
Peptide Receptor Radionuclide Therapy using 177 Lu octreotate
 Peptide Receptor Radionuclide Therapy using 177 Lu octreotate BLR Kam, Erasmus Medical Centre, Rotterdam DJ Kwekkeboom, Erasmus Medical Centre, Rotterdam Legal aspects As 177 Lu-[DOTA 0 -Tyr 3 ]octreotate
Peptide Receptor Radionuclide Therapy using 177 Lu octreotate BLR Kam, Erasmus Medical Centre, Rotterdam DJ Kwekkeboom, Erasmus Medical Centre, Rotterdam Legal aspects As 177 Lu-[DOTA 0 -Tyr 3 ]octreotate
PAPER. Lymph Nodes and Survival in Pancreatic Neuroendocrine Tumors
 PAPER Lymph Nodes and Survival in Pancreatic Neuroendocrine Tumors Geoffrey W. Krampitz, MD; Jeffrey A. Norton, MD; George A. Poultsides, MD; Brendan C. Visser, MD; Lixian Sun, MS; Robert T. Jensen, MD
PAPER Lymph Nodes and Survival in Pancreatic Neuroendocrine Tumors Geoffrey W. Krampitz, MD; Jeffrey A. Norton, MD; George A. Poultsides, MD; Brendan C. Visser, MD; Lixian Sun, MS; Robert T. Jensen, MD
Clinicopathological Characteristics and Prognosis-Related Factors of Resectable Pancreatic Neuroendocrine Tumors
 ORIGINAL ARTICLE Clinicopathological Characteristics and Prognosis-Related Factors of Resectable Pancreatic Neuroendocrine Tumors A Retrospective Study of 104 Cases in a Single Chinese Center Xu Han, MD,*
ORIGINAL ARTICLE Clinicopathological Characteristics and Prognosis-Related Factors of Resectable Pancreatic Neuroendocrine Tumors A Retrospective Study of 104 Cases in a Single Chinese Center Xu Han, MD,*
ENETS Consensus Guidelines for the Standard of Care in
 Neuroendocrinology (DOI:10.1159/000457957) (Accepted, unedited article not yet assigned to an issue) Advanced Release: February 11, 2017 2017 S. Karger AG, Basel www.karger.com/nen Received: December 12,
Neuroendocrinology (DOI:10.1159/000457957) (Accepted, unedited article not yet assigned to an issue) Advanced Release: February 11, 2017 2017 S. Karger AG, Basel www.karger.com/nen Received: December 12,
Practical management and treatment of pancreatic neuroendocrine tumors
 Review Article Practical management and treatment of pancreatic neuroendocrine tumors Naoko Iwahashi Kondo, Yasuharu Ikeda Department of Gastroenterological Surgery, National Hospital Organization Kyushu
Review Article Practical management and treatment of pancreatic neuroendocrine tumors Naoko Iwahashi Kondo, Yasuharu Ikeda Department of Gastroenterological Surgery, National Hospital Organization Kyushu
Intertumor heterogeneity in 60 pancreatic neuroendocrine tumors associated with multiple endocrine neoplasia type 1
 Selberherr et al. Orphanet Journal of Rare Diseases (2019) 14:54 https://doi.org/10.1186/s13023-019-1034-4 RESEARCH Open Access Intertumor heterogeneity in 60 pancreatic neuroendocrine tumors associated
Selberherr et al. Orphanet Journal of Rare Diseases (2019) 14:54 https://doi.org/10.1186/s13023-019-1034-4 RESEARCH Open Access Intertumor heterogeneity in 60 pancreatic neuroendocrine tumors associated
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis.
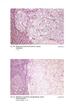 Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
GEP NEN. Personalised approach. Curative and Palliative Surgery. ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano April 2018
 GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
GEP NEN Personalised approach Curative and Palliative Surgery ESMO Preceptorship Programme Neuroendocrine Neoplasms Lugano 13 14 April 2018 Professor Andrea Frilling Department of Surgery and Cancer Imperial
Primary hyperparathyroidism (HPT) has an incidence of
 Dual-Phase Tc-Sestamibi Imaging: Its Utility in Parathyroid Hyperplasia and Use of Immediate/ Delayed Image Ratios to Improve Diagnosis of Hyperparathyroidism Leonie Gordon, MD; William Burkhalter, MD;
Dual-Phase Tc-Sestamibi Imaging: Its Utility in Parathyroid Hyperplasia and Use of Immediate/ Delayed Image Ratios to Improve Diagnosis of Hyperparathyroidism Leonie Gordon, MD; William Burkhalter, MD;
Objectives. Terminology 03/11/2013. Pitfalls in the diagnosis of Gastroenteropancreatic Neuroendocrine Tumors. Pathology Update 2013
 Pitfalls in the diagnosis of Gastroenteropancreatic Neuroendocrine Tumors Pathology Update 2013 Ozgur Mete, MD Consultant in Endocrine Pathology, Department of Pathology, University Health Network Assistant
Pitfalls in the diagnosis of Gastroenteropancreatic Neuroendocrine Tumors Pathology Update 2013 Ozgur Mete, MD Consultant in Endocrine Pathology, Department of Pathology, University Health Network Assistant
Gastric endocrine tumors type I: treatment with long-acting somatostatin analogs
 Endocrine-Related Cancer (2008) 15 337 342 Gastric endocrine tumors type I: treatment with long-acting somatostatin analogs D Campana 1, F Nori 1, R Pezzilli 1, L Piscitelli 1, D Santini 2, E Brocchi 1,
Endocrine-Related Cancer (2008) 15 337 342 Gastric endocrine tumors type I: treatment with long-acting somatostatin analogs D Campana 1, F Nori 1, R Pezzilli 1, L Piscitelli 1, D Santini 2, E Brocchi 1,
KK College of Nursing Peptic Ulcer Badil D ass Dass, Lecturer 25th July, 2011
 KK College of Nursing Peptic Ulcer Badil Dass, Lecturer 25 th July, 2011 Objectives: By the end of this lecture, the students t will be able to: Define peptic pp ulcer Describe the etiology and pathology
KK College of Nursing Peptic Ulcer Badil Dass, Lecturer 25 th July, 2011 Objectives: By the end of this lecture, the students t will be able to: Define peptic pp ulcer Describe the etiology and pathology
An Unexpected Cause of Hypoglycemia
 An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
An Unexpected Cause of Hypoglycemia Stacey A. Milan, MD FACS Surgical Oncology Nothing to disclose Disclosures Objectives Identify indications for workup of hypoglycemia Define work up for hypoglycemic
Original article. M. Cimitan 1 *, A. Buonadonna 2, R. Cannizzaro 3, V. Canzonieri 4, E. Borsatti 1, R. Ruffo 1 & L. De Apollonia 5.
 Original article Annals of Oncology 14: 1135 1141, 2003 DOI: 10.1093/annonc/mdg279 Somatostatin receptor scintigraphy versus chromogranin A assay in the management of patients with neuroendocrine tumors
Original article Annals of Oncology 14: 1135 1141, 2003 DOI: 10.1093/annonc/mdg279 Somatostatin receptor scintigraphy versus chromogranin A assay in the management of patients with neuroendocrine tumors
David Bruyette, DVM, DACVIM Medical Director
 VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
VCAWLAspecialty.com David Bruyette, DVM, DACVIM Medical Director The pancreas is made up of endocrine and exocrine tissue. The endocrine pancreas is composed of islets of Langerhans, which make up approximately
Gastric and Oesophageal Neuroendocrine tumours. Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath
 Gastric and Oesophageal Neuroendocrine tumours Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath Intestinal (and BO) endocrine cells in crypt bases NE cell (granules towards vessels) Paneth
Gastric and Oesophageal Neuroendocrine tumours Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath Intestinal (and BO) endocrine cells in crypt bases NE cell (granules towards vessels) Paneth
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment)
 Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for NET Challenges and specific aspects
 Surgery for NET Challenges and specific aspects Raymond Aerts, MD Department of Abdominal Surgery and Liver Transplantation University Clinics Leuven ESMO Preceptorship on GI neuroendocrine tumours (NETs)
Surgery for NET Challenges and specific aspects Raymond Aerts, MD Department of Abdominal Surgery and Liver Transplantation University Clinics Leuven ESMO Preceptorship on GI neuroendocrine tumours (NETs)
The pathology of neuroendocrine tumours of the gut
 The pathology of neuroendocrine tumours of the gut Professor Neil A Shepherd Gloucester & Cheltenham, UK Histopathology Regional Teaching Bristol May 11 2016 The pathology of neuroendocrine tumours (NETs)
The pathology of neuroendocrine tumours of the gut Professor Neil A Shepherd Gloucester & Cheltenham, UK Histopathology Regional Teaching Bristol May 11 2016 The pathology of neuroendocrine tumours (NETs)
GASTROINTESTINAL AND ANTIEMETIC DRUGS. Submitted by: Shaema M. Ali
 GASTROINTESTINAL AND ANTIEMETIC DRUGS Submitted by: Shaema M. Ali GASTROINTESTINAL AND ANTIEMETIC DRUGS by: Shaema M. Ali There are four common medical conditions involving the GI system 1) peptic ulcers
GASTROINTESTINAL AND ANTIEMETIC DRUGS Submitted by: Shaema M. Ali GASTROINTESTINAL AND ANTIEMETIC DRUGS by: Shaema M. Ali There are four common medical conditions involving the GI system 1) peptic ulcers
PPI-Delayed Diagnosis of Gastrinoma: Oncologic Victim of Pharmacologic Success
 Pathol. Oncol. Res. (2010) 16:87 91 DOI 10.1007/s12253-009-9192-7 PPI-Delayed Diagnosis of Gastrinoma: Oncologic Victim of Pharmacologic Success Hilda Wong & Thomas Yau & Pierre Chan & Irene O. L. Ng &
Pathol. Oncol. Res. (2010) 16:87 91 DOI 10.1007/s12253-009-9192-7 PPI-Delayed Diagnosis of Gastrinoma: Oncologic Victim of Pharmacologic Success Hilda Wong & Thomas Yau & Pierre Chan & Irene O. L. Ng &
A Nationwide Population-Based Study on the Survival of Patients with Pancreatic Neuroendocrine Tumors in The Netherlands
 World J Surg (2018) 42:490 497 DOI 10.1007/s00268-017-4278-y ORIGINAL SCIENTIFIC REPORT A Nationwide Population-Based Study on the Survival of Patients with Pancreatic Neuroendocrine Tumors in The Netherlands
World J Surg (2018) 42:490 497 DOI 10.1007/s00268-017-4278-y ORIGINAL SCIENTIFIC REPORT A Nationwide Population-Based Study on the Survival of Patients with Pancreatic Neuroendocrine Tumors in The Netherlands
SMALL BOWEL ADENOCARCINOMA. Dr. C. Jeske
 SMALL BOWEL ADENOCARCINOMA Dr. C. Jeske Case presentation 54 year old female. Presents with OJ and weight loss. Abdominal examination only reveals a palpable gallbladder. ERCP reveals a circumferential
SMALL BOWEL ADENOCARCINOMA Dr. C. Jeske Case presentation 54 year old female. Presents with OJ and weight loss. Abdominal examination only reveals a palpable gallbladder. ERCP reveals a circumferential
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Coexistence of parathyroid adenoma and papillary thyroid carcinoma. Yong Sang Lee, Kee-Hyun Nam, Woong Youn Chung, Hang-Seok Chang, Cheong Soo Park
 J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
J Korean Surg Soc 2011;81:316-320 http://dx.doi.org/10.4174/jkss.2011.81.5.316 ORIGINAL ARTICLE JKSS Journal of the Korean Surgical Society pissn 2233-7903 ㆍ eissn 2093-0488 Coexistence of parathyroid
