American College of Radiology ACR Appropriateness Criteria Breast Cancer Screening
|
|
|
- Dominic Parrish
- 6 years ago
- Views:
Transcription
1 Revised 2017 American College of Radiology ACR Appropriateness Criteria Breast Cancer Screening Variant 1: Breast cancer screening. Average-risk women: women with <15% lifetime risk of breast cancer. Procedure Appropriateness Category Relative Radiation Level Mammography screening Usually Appropriate Digital breast tomosynthesis screening Usually Appropriate US breast May Be Appropriate O MRI breast without and with IV contrast Usually Not Appropriate O MRI breast without IV contrast Usually Not Appropriate O FDG-PEM Usually Not Appropriate Tc-99m sestamibi MBI Usually Not Appropriate Variant 2: Breast cancer screening. Intermediate-risk women: women with personal history of breast cancer, lobular neoplasia, atypical ductal hyperplasia, or 15% to 20% lifetime risk of breast cancer. Procedure Appropriateness Category Relative Radiation Level Mammography screening Usually Appropriate Digital breast tomosynthesis screening Usually Appropriate MRI breast without and with IV contrast May Be Appropriate O US breast May Be Appropriate O FDG-PEM Usually Not Appropriate Tc-99m sestamibi MBI Usually Not Appropriate MRI breast without IV contrast Usually Not Appropriate O Variant 3: Breast cancer screening. High-risk women: women with a BRCA gene mutation and their untested first-degree relatives, women with a history of chest irradiation between 10 to 30 years of age, women with 20% or greater lifetime risk of breast cancer. Procedure Appropriateness Category Relative Radiation Level Mammography screening Usually Appropriate Digital breast tomosynthesis screening Usually Appropriate MRI breast without and with IV contrast Usually Appropriate O US breast May Be Appropriate O FDG-PEM Usually Not Appropriate Tc-99m sestamibi MBI Usually Not Appropriate MRI breast without IV contrast Usually Not Appropriate O ACR Appropriateness Criteria 1 Breast Cancer Screening
2 BREAST CANCER SCREENING Expert Panel on Breast Imaging: Martha B. Mainiero, MD a ; Linda Moy, MD b ; Paul Baron, MD c ; Aarati D. Didwania, MD d ; Roberta M. diflorio-alexander, MD, MS e ; Edward D. Green, MD f ; Samantha L. Heller, MD, PhD g ; Anna I. Holbrook, MD h ; Su-Ju Lee, MD i ; Alana A. Lewin, MD j ; Ana P. Lourenco, MD k ; Kara J. Nance, MD l ; Bethany L. Niell, MD, PhD m ; Priscilla J. Slanetz, MD, MPH n ; Ashley R. Stuckey, MD o ; Nina S. Vincoff, MD p ; Susan P. Weinstein, MD q ; Monica M. Yepes, MD r ; Mary S. Newell, MD. s Summary of Literature Review Introduction/Background Other than skin cancer, breast cancer is the most common cancer diagnosis and the second leading cause of cancer death in women. Since the advent of screening mammography in the United States, breast cancer mortality has decreased 36% between 1989 and 2012, after slowly increasing before that time [1]. Long-term follow-up analysis of populations before and after the institution of screening mammography attributes the decrease in mortality to screening of the general population [2]. In addition to mortality reduction, early detection allows for a wider range of less invasive treatment options. The sensitivity of mammography is dependent upon breast density, where sensitivity decreases with the increase of breast density. Breast density is reported on mammography as: A = almost entirely fatty, B = scattered areas of fibroglandular density, C = heterogeneously dense, or D = extremely dense, where heterogeneously dense and extremely dense (C and D categories) are considered dense [3]. Discussion of Procedures by Variant Variant 1: Breast cancer screening. Average-risk women: women with <15% lifetime risk of breast cancer. Mammography and DBT In follow-up of randomized controlled trials of screening mammography in women 40 to 74 years of age, there continues to be a highly significant decrease in mortality in those randomized to invitation to screening mammography [4]. Because breast cancer incidence increases with age, more women among the younger age group (40-50) will need to be screened for each life saved than for women 50 years of age or older. However, because younger women have a longer life expectancy, life years gained for the women diagnosed with breast cancer by screening in their 40s is higher than in the 50- to 70-year-old population [5]. The age at which various organizations recommend beginning screening mammography and the frequency at which mammography is recommended in different age groups varies based upon the weight given to the perceived risks (false-positive examinations and the possibility of over-diagnosis) and benefits of screening (mortality reduction and less invasive treatment options). Some groups recommend screening for all women starting at age 50, with screening recommended between 40 to 50 years of age dependent upon patient preference [6] or risk [7]. However, personalized screening in the 40 to 49 year age group would cause the majority of screen-detected cancers to be excluded from detection [8,9]. Groups also vary on whether screening mammography is recommended as an annual or biennial examination. Based on a review of the randomized trials and subsequent meta-analyses, the ACR recommends annual screening beginning at 40 years of age [10]. There is no upper age limit established for screening mammography, but as the benefits of screening mammography may take years to be fully realized, screening recommendations should take into account life expectancy and comorbid conditions, with screening mammography remaining appropriate when a woman s life expectancy exceeds 5 to 7 years [10,11]. a Principal Author, Alpert Medical School of Brown University, Providence, Rhode Island. b Panel Vice-Chair, NYU Clinical Cancer Center, New York, New York. c Roper St. Francis Physician Partners Breast Surgery, Charleston, South Carolina; American College of Surgeons. d Northwestern University Feinberg School of Medicine, Chicago, Illinois; American College of Physicians. e Dartmouth-Hitchcock Medical Center, Lebanon, New Hampshire. f The University of Mississippi Medical Center, Jackson, Mississippi. g New York University School of Medicine, New York, New York. h Emory University Hospital, Atlanta, Georgia. i University of Cincinnati Medical Center, Cincinnati, Ohio. j New York University School of Medicine, New York, New York. k Alpert Medical School of Brown University, Providence, Rhode Island. l Wellessence MD, Schaumburg, Illinois; American College of Physicians. m H. Lee Moffitt Cancer Center and Research Institute, Tampa, Florida. n Beth Israel Deaconess Medical Center, Boston, Massachusetts. o Women and Infants Hospital, Providence, Rhode Island; American Congress of Obstetricians and Gynecologists. p Hofstra Northwell School of Medicine, Manhasset, New York. q Perelman School of Medicine of the University of Pennsylvania, Philadelphia, Pennsylvania. r University of Miami, Miami, Florida. s Panel Chair, Emory University Hospital, Atlanta, Georgia. The American College of Radiology seeks and encourages collaboration with other organizations on the development of the ACR Appropriateness Criteria through society representation on expert panels. Participation by representatives from collaborating societies on the expert panel does not necessarily imply individual or society endorsement of the final document. Reprint requests to: publications@acr.org ACR Appropriateness Criteria 2 Breast Cancer Screening
3 Digital breast tomosynthesis (DBT) can address some of the limitations encountered with standard mammographic views. In addition to planar images, DBT allows for creation and viewing of thin-section reconstructed images that may decrease the lesion-masking effect of overlapping normal tissue and reveal the true nature of potential false-positive findings without the need for recall. Several studies confirm that in a screening setting, the cancer detection rate is increased with use of DBT compared with 2-D mammography alone [12-27]. Additionally, the rate of recall for benign findings (false-positives) can be decreased [12,14-17,20-25,27-30]. Some authors found these advantages to be especially pronounced in women under age 50 [20,31], in those with dense breasts [31,32], and with lesion types including spiculated masses [33] and asymmetries [28]. Interpretation time for DBT images is greater than for standard mammography [14,34]. Additionally, dose is increased if standard 2-D images are obtained in addition to DBT images. However, synthesized reconstructed images (a virtual planar image created from the tomographic dataset) may replace the need for a 2-D correlative view; current data suggest that these synthetic images perform as well as standard full-field digital images [35,36]. DBT is almost always performed as part of an examination that also includes digital mammography. The digital mammography part of the examination may be in the form of traditional projection mammography or synthesized image from the DBT data. US The presence of dense breast tissue lowers the sensitivity of mammography and increases breast cancer risk when compared with patients with fatty breasts [37]. Adding hand-held or automated breast ultrasound (US) to mammography in women with dense breasts increases the cancer detection rate but also substantially increases the false-positive rate [38-40]. In the initial clinical experience with screening breast US after a dense breast notification law was enacted on a state-wide level, the cancer detection rate increased but the number of short interval follow-up recommendations increased substantially and the positive predictive value of a biopsy recommendation was much lower [41,42]. For women with dense breasts tissue but no additional risk factors, US may be useful as an adjunct to mammography for incremental cancer detection [10], but the balance between increased cancer detection and the increased risk of a false-positive examination should be considered in the decision. There are no data to support the use of US for average-risk women with nondense breasts [43]. MBI and FDG-PEM Supplementing mammography with molecular breast imaging (MBI) in women with dense breasts increases the cancer detection rate [44,45]. However, there have been no large population studies of MBI for screening, and the whole-body radiation dose with this technique is concerning [46]. Positron emission mammography with fluorine fluoro-2-deoxy-D-glucose (FDG-PEM) is similarly limited by radiation dose and lack of evidence in large screening populations. MRI There is insufficient evidence to support the use of magnetic resonance imaging (MRI) for screening women of average risk. Variant 2: Breast cancer screening. Intermediate-risk women: women with personal history of breast cancer, lobular neoplasia, atypical ductal hyperplasia, or 15% to 20% lifetime risk of breast cancer. Some women with an intermediate risk of breast cancer may benefit by beginning screening mammography earlier than 40 years of age and may also benefit from supplemental screening. The recommendations for supplemental screening for women at intermediate risk of breast cancer, including those with a personal history of breast cancer, a history of lobular carcinoma in situ or ADH, those with an intermediate family history and a lifetime risk of 15% to 20%, or women with dense breasts continues to be an area of debate [47]. Mammography and DBT Annual screening mammography is recommended for women with biopsy-proven lobular neoplasia or atypical ductal hyperplasia beginning at diagnosis, but not when <30 years of age [11]. Women who have a prior history of breast cancer are recommended to have mammography every 12 months (and 6 to 12 months post-radiation if the breast is conserved) [11]. The sensitivity of mammography is dependent upon breast density, with sensitivity decreasing with increasing breast density. DBT can address some of the limitations encountered with standard mammographic views. In addition to planar images, DBT allows for creation and viewing of thin-section reconstructed images that can decrease the lesion-masking effect of overlapping normal tissue and reveal the true nature of potential falsepositive findings without the need for recall. Several studies confirm that in a screening setting, cancer detection ACR Appropriateness Criteria 3 Breast Cancer Screening
4 rate is increased with the use of DBT compared to 2-D mammography alone [12-27]. Additionally, the rate of recall for benign findings (false-positives) can be decreased [12,14-17,20-25,27-30]. Some authors found these advantages to be especially pronounced in women under age 50 [20,31], in those with dense breasts [31,32], and with lesion types including spiculated masses [33] and asymmetries [28]. Interpretation time for DBT images is greater than for standard mammography [14,34]. Additionally, dose is increased if standard 2-D images are obtained in addition to DBT images. However, synthesized reconstructed images (a virtual planar image created from the tomographic dataset) may replace the need for a 2-D correlative view; current data suggest that these synthetic images perform as well as standard full-field digital images [35,36]. DBT is almost always performed as part of an examination that also includes digital mammography. The digital mammography part of the examination may be in the form of traditional projection mammography or synthesized from the DBT data. US In women with dense breasts and increased risk of breast cancer, mammography sensitivity can be as low as 50%; supplementing mammography screening with US will significantly increase cancer detection, although falsepositive rates are also substantially increased [48,49]. In intermediate-risk women with dense breasts, supplemental US screening is an option [48,49]. MRI The American Cancer Society considers there to be insufficient evidence for or against MRI as an adjunct to mammography in women at intermediate risk of breast cancer [47]. However, recent studies support the use of screening MRI in certain subsets of this population, including women with a history of lobular carcinoma in situ [50,51] or a personal history of breast cancer [52,53]. MBI and FDG-PEM Supplementing mammography with MBI in women with dense breasts increases the cancer detection rate [44,45]. However, there have been no large population studies of MBI for screening and whole body radiation dose with this technique is concerning [46]. FDG-PEM is similarly limited by radiation dose and lack of evidence in large screening populations. Variant 3: Breast cancer screening. High-risk women: women with a BRCA gene mutation and their untested first-degree relatives, women with a history of chest irradiation between 10 to 30 years of age, women with 20% or greater lifetime risk of breast cancer. Women at high risk for breast cancer include those with BRCA or other known genetic predispositions, women with a very strong family history placing them at more than a 20% lifetime risk of breast cancer, and those with prior mantle radiation therapy between 10 to 30 years of age [47]. In addition to beginning screening mammography earlier than the general population, women in this high-risk group benefit from supplemental screening. Mammography and DBT Annual mammography is recommended starting 8 years after radiation therapy but not before age 25 for women who received mantle radiation between 10 to 30 years of age [10,11]. As there is some concern about young women with an inherited cancer predisposition having increased sensitivity to radiation, women with a genetic predisposition are recommended for annual screening beginning 10 years earlier than the affected relative at the time of diagnosis but not before age 30 [11]. The sensitivity of mammography is dependent upon breast density, with sensitivity decreasing with increasing breast density. DBT can address some of the limitations encountered with standard mammographic views. In addition to planar images, DBT allows for creation and viewing of thin-section reconstructed images that may decrease the lesion-masking effect of overlapping normal tissue and reveal the true nature of potential falsepositive findings without the need for recall. Several studies confirm that in a screening setting, the cancer detection rate is increased with use of DBT compared to 2-D mammography alone [12-27]. Additionally, the rate of recall for benign findings (false-positives) can be decreased [12,14-17,20-25,27-30]. Some authors found these advantages to be especially pronounced in women under age 50 [20,31], in those with dense breasts [31,32], and those with lesion types including spiculated masses [33] and asymmetries [28]. Interpretation time for DBT images is greater than for standard mammography [14,34]. Additionally, dose is increased if standard 2-D images are obtained in addition to DBT images. However, synthesized reconstructed images (a virtual planar image created from the tomographic dataset) may replace the need for a 2-D correlative view; and current data suggest that these synthetic images perform as well as standard full-field digital images [35,36]. DBT is almost always ACR Appropriateness Criteria 4 Breast Cancer Screening
5 performed as part of an examination that also includes digital mammography. The digital mammography part of the examination may be in the form of traditional projection mammography or synthesized image from the DBT data. MRI Breast MRI in high-risk women has a higher sensitivity than mammography, and the combination of mammography and MRI in this population has the highest sensitivity [54-61]. In a high-risk population, MRI and mammography combined have a higher sensitivity (92.7%) than US and mammography combined (52%) [49,62]. Therefore, in high-risk women for whom supplemental screening is indicated, MRI is recommended when possible. Screening MRI is recommended in women with BRCA gene mutations and their untested first-degree relatives as well as women with a lifetime risk of breast cancer of ~20% or greater. Also included in this high-risk group are women who have received radiation therapy to the chest between 10 to 30 years of age as well as women with other genetic syndromes that increase the risk of breast cancer. Screening high-risk women with breast MRI is cost-effective, and the cost-effectiveness of screening MRI increases with increasing breast cancer risk [63,64]. The American Cancer Society recommends breast-screening MRI in high-risk women [47], and the ACR and the Society of Breast Imaging endorse those recommendations [10]. US Screening US is indicated in high-risk patients who cannot tolerate MRI. Mammography alone does not perform as well as mammography plus supplemental screening in high-risk women, especially those with a genetic predisposition, and supplemental screening US is indicated in high-risk patients who cannot tolerate MRI [49,62]. MBI and FDG-PEM Supplementing mammography with MBI in women with dense breasts increases the cancer detection rate [44,45]. However, there have been no large population studies of MBI for screening and the whole-body radiation dose with this technique is concerning [46]. FDG-PEM is similarly limited by radiation dose and lack of evidence in large screening populations. Summary of Recommendations For average-risk women, annual screening mammography or DBT (with accompanying planar or synthesized 2-D images) is recommended beginning at age 40. For women with dense breasts, US may also be considered, but the balance between increased cancer detection and the increased risk of a false-positive examination should be considered in the decision. For intermediate-risk women, breast mammography or DBT (with accompanying planar or synthesized 2-D images) is recommended. MRI may be considered as an adjunct to mammography or DBT (with accompanying planar or synthesized 2-D images) depending upon risk factors. For women with dense breasts, US may be an option, but the balance between increased cancer detection and the increased risk of a falsepositive examination should be considered in the decision. For high-risk women, mammography or DBT (with accompanying planar or synthesized 2-D images) is recommended. MRI is recommended as an adjunct to screening mammography or DBT (with accompanying planar or synthesized 2-D images). US is recommended when the patient cannot tolerate MRI. Summary of Evidence Of the 65 references cited in the ACR Appropriateness Criteria Breast Cancer Screening document, all of them are categorized as diagnostic references including 12 well-designed studies, 12 good-quality studies, and 22 quality studies that may have design limitations. There are 18 references that may not be useful as primary evidence. There is one reference that is a meta-analysis study. The 65 references cited in the ACR Appropriateness Criteria Breast Cancer Screening document were published from 2005 to While there are references that report on studies with design limitations, 24 well-designed or good-quality studies provide good evidence. ACR Appropriateness Criteria 5 Breast Cancer Screening
6 Appropriateness Category Names and Definitions Appropriateness Category Name Appropriateness Rating Usually Appropriate 7, 8, or 9 May Be Appropriate 4, 5, or 6 May Be Appropriate (Disagreement) Usually Not Appropriate 1, 2, or 3 5 Appropriateness Category Definition The imaging procedure or treatment is indicated in the specified clinical scenarios at a favorable riskbenefit ratio for patients. The imaging procedure or treatment may be indicated in the specified clinical scenarios as an alternative to imaging procedures or treatments with a more favorable risk-benefit ratio, or the risk-benefit ratio for patients is equivocal. The individual ratings are too dispersed from the panel median. The different label provides transparency regarding the panel s recommendation. May be appropriate is the rating category and a rating of 5 is assigned. The imaging procedure or treatment is unlikely to be indicated in the specified clinical scenarios, or the risk-benefit ratio for patients is likely to be unfavorable. Relative Radiation Level Information Potential adverse health effects associated with radiation exposure are an important factor to consider when selecting the appropriate imaging procedure. Because there is a wide range of radiation exposures associated with different diagnostic procedures, a relative radiation level (RRL) indication has been included for each imaging examination. The RRLs are based on effective dose, which is a radiation dose quantity that is used to estimate population total radiation risk associated with an imaging procedure. Patients in the pediatric age group are at inherently higher risk from exposure, both because of organ sensitivity and longer life expectancy (relevant to the long latency that appears to accompany radiation exposure). For these reasons, the RRL dose estimate ranges for pediatric examinations are lower as compared to those specified for adults (see Table below). Additional information regarding radiation dose assessment for imaging examinations can be found in the ACR Appropriateness Criteria Radiation Dose Assessment Introduction document [65]. Relative Radiation Level* Relative Radiation Level Designations Adult Effective Dose Estimate Range Pediatric Effective Dose Estimate Range O 0 msv 0 msv <0.1 msv <0.03 msv msv msv 1-10 msv msv msv 3-10 msv msv msv *RRL assignments for some of the examinations cannot be made, because the actual patient doses in these procedures vary as a function of a number of factors (eg, region of the body exposed to ionizing radiation, the imaging guidance that is used). The RRLs for these examinations are designated as Varies. Supporting Documents For additional information on the Appropriateness Criteria methodology and other supporting documents go to References 1. Siegel RL, Miller KD, Jemal A. Cancer Statistics, CA Cancer J Clin. 2017;67(1):7-30. ACR Appropriateness Criteria 6 Breast Cancer Screening
7 2. Reduction in breast cancer mortality from organized service screening with mammography: 1. Further confirmation with extended data. Cancer Epidemiol Biomarkers Prev. 2006;15(1): D'Orsi CJ, Sickles EA, Mendelson EB, et al. ACR BI-RADS Atlas, Breast Imaging Reporting and Data System. Reston, VA, American College of Radiology; Tabar L, Vitak B, Chen TH, et al. Swedish two-county trial: impact of mammographic screening on breast cancer mortality during 3 decades. Radiology. 2011;260(3): Hendrick RE, Helvie MA. Mammography screening: a new estimate of number needed to screen to prevent one breast cancer death. AJR Am J Roentgenol. 2012;198(3): Siu AL. Screening for Breast Cancer: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2016;164(4): Schousboe JT, Kerlikowske K, Loh A, Cummings SR. Personalizing mammography by breast density and other risk factors for breast cancer: analysis of health benefits and cost-effectiveness. Ann Intern Med. 2011;155(1): Destounis SV, Arieno AL, Morgan RC, et al. Comparison of breast cancers diagnosed in screening patients in their 40s with and without family history of breast cancer in a community outpatient facility. AJR Am J Roentgenol. 2014;202(4): Price ER, Keedy AW, Gidwaney R, Sickles EA, Joe BN. The Potential Impact of Risk-Based Screening Mammography in Women Years Old. AJR Am J Roentgenol. 2015;205(6): Lee CH, Dershaw DD, Kopans D, et al. Breast cancer screening with imaging: recommendations from the Society of Breast Imaging and the ACR on the use of mammography, breast MRI, breast ultrasound, and other technologies for the detection of clinically occult breast cancer. J Am Coll Radiol. 2010;7(1): Monticciolo DL, Newell MS, Hendrick RE, et al. Breast Cancer Screening for Average-Risk Women: Recommendations From the ACR Commission on Breast Imaging. J Am Coll Radiol. 2017;14(9): Ciatto S, Houssami N, Bernardi D, et al. Integration of 3D digital mammography with tomosynthesis for population breast-cancer screening (STORM): a prospective comparison study. Lancet Oncol. 2013;14(7): Bernardi D, Caumo F, Macaskill P, et al. Effect of integrating 3D-mammography (digital breast tomosynthesis) with 2D-mammography on radiologists' true-positive and false-positive detection in a population breast screening trial. Eur J Cancer. 2014;50(7): Bernardi D, Ciatto S, Pellegrini M, et al. Application of breast tomosynthesis in screening: incremental effect on mammography acquisition and reading time. Br J Radiol. 2012;85(1020):e Caumo F, Bernardi D, Ciatto S, et al. Incremental effect from integrating 3D-mammography (tomosynthesis) with 2D-mammography: Increased breast cancer detection evident for screening centres in a population-based trial. Breast. 2014;23(1): Friedewald SM, Rafferty EA, Rose SL, et al. Breast cancer screening using tomosynthesis in combination with digital mammography. JAMA. 2014;311(24): Greenberg JS, Javitt MC, Katzen J, Michael S, Holland AE. Clinical performance metrics of 3D digital breast tomosynthesis compared with 2D digital mammography for breast cancer screening in community practice. AJR Am J Roentgenol. 2014;203(3): Houssami N, Macaskill P, Bernardi D, et al. Breast screening using 2D-mammography or integrating digital breast tomosynthesis (3D-mammography) for single-reading or double-reading--evidence to guide future screening strategies. Eur J Cancer. 2014;50(10): Lei J, Yang P, Zhang L, Wang Y, Yang K. Diagnostic accuracy of digital breast tomosynthesis versus digital mammography for benign and malignant lesions in breasts: a meta-analysis. Eur Radiol. 2014;24(3): McCarthy AM, Kontos D, Synnestvedt M, et al. Screening outcomes following implementation of digital breast tomosynthesis in a general-population screening program. J Natl Cancer Inst. 2014;106(11). 21. Rafferty EA, Park JM, Philpotts LE, et al. Assessing radiologist performance using combined digital mammography and breast tomosynthesis compared with digital mammography alone: results of a multicenter, multireader trial. Radiology. 2013;266(1): Rafferty EA, Park JM, Philpotts LE, et al. Diagnostic accuracy and recall rates for digital mammography and digital mammography combined with one-view and two-view tomosynthesis: results of an enriched reader study. AJR Am J Roentgenol. 2014;202(2): Rose SL, Tidwell AL, Ice MF, Nordmann AS, Sexton R, Jr., Song R. A reader study comparing prospective tomosynthesis interpretations with retrospective readings of the corresponding FFDM examinations. Acad Radiol. 2014;21(9): ACR Appropriateness Criteria 7 Breast Cancer Screening
8 24. Skaane P, Bandos AI, Gullien R, et al. Prospective trial comparing full-field digital mammography (FFDM) versus combined FFDM and tomosynthesis in a population-based screening programme using independent double reading with arbitration. Eur Radiol. 2013;23(8): Skaane P, Bandos AI, Gullien R, et al. Comparison of digital mammography alone and digital mammography plus tomosynthesis in a population-based screening program. Radiology. 2013;267(1): Svahn TM, Chakraborty DP, Ikeda D, et al. Breast tomosynthesis and digital mammography: a comparison of diagnostic accuracy. Br J Radiol. 2012;85(1019):e Takamoto Y, Tsunoda H, Kikuchi M, et al. Role of breast tomosynthesis in diagnosis of breast cancer for Japanese women. Asian Pac J Cancer Prev. 2013;14(5): Durand MA, Haas BM, Yao X, et al. Early clinical experience with digital breast tomosynthesis for screening mammography. Radiology. 2015;274(1): Lourenco AP, Barry-Brooks M, Baird GL, Tuttle A, Mainiero MB. Changes in recall type and patient treatment following implementation of screening digital breast tomosynthesis. Radiology. 2015;274(2): Rose SL, Tidwell AL, Bujnoch LJ, Kushwaha AC, Nordmann AS, Sexton R, Jr. Implementation of breast tomosynthesis in a routine screening practice: an observational study. AJR Am J Roentgenol. 2013;200(6): Haas BM, Kalra V, Geisel J, Raghu M, Durand M, Philpotts LE. Comparison of tomosynthesis plus digital mammography and digital mammography alone for breast cancer screening. Radiology. 2013;269(3): Mun HS, Kim HH, Shin HJ, et al. Assessment of extent of breast cancer: comparison between digital breast tomosynthesis and full-field digital mammography. Clin Radiol. 2013;68(12): Lang K, Andersson I, Zackrisson S. Breast cancer detection in digital breast tomosynthesis and digital mammography-a side-by-side review of discrepant cases. Br J Radiol. 2014;87(1040): Dang PA, Freer PE, Humphrey KL, Halpern EF, Rafferty EA. Addition of tomosynthesis to conventional digital mammography: effect on image interpretation time of screening examinations. Radiology. 2014;270(1): Skaane P, Bandos AI, Eben EB, et al. Two-view digital breast tomosynthesis screening with synthetically reconstructed projection images: comparison with digital breast tomosynthesis with full-field digital mammographic images. Radiology. 2014;271(3): Zuley ML, Guo B, Catullo VJ, et al. Comparison of two-dimensional synthesized mammograms versus original digital mammograms alone and in combination with tomosynthesis images. Radiology. 2014;271(3): Winkler NS, Raza S, Mackesy M, Birdwell RL. Breast density: clinical implications and assessment methods. Radiographics. 2015;35(2): Brem RF, Tabar L, Duffy SW, et al. Assessing improvement in detection of breast cancer with threedimensional automated breast US in women with dense breast tissue: the SomoInsight Study. Radiology. 2015;274(3): Chae EY, Kim HH, Cha JH, Shin HJ, Kim H. Evaluation of screening whole-breast sonography as a supplemental tool in conjunction with mammography in women with dense breasts. J Ultrasound Med. 2013;32(9): Giuliano V, Giuliano C. Improved breast cancer detection in asymptomatic women using 3D-automated breast ultrasound in mammographically dense breasts. Clin Imaging. 2013;37(3): Hooley RJ, Greenberg KL, Stackhouse RM, Geisel JL, Butler RS, Philpotts LE. Screening US in patients with mammographically dense breasts: initial experience with Connecticut Public Act Radiology. 2012;265(1): Parris T, Wakefield D, Frimmer H. Real world performance of screening breast ultrasound following enactment of Connecticut Bill 458. Breast J. 2013;19(1): Gartlehner G, Thaler KJ, Chapman A, et al. Adjunct ultrasonography for breast cancer screening in women at average risk: a systematic review. Int J Evid Based Healthc. 2013;11(2): Rhodes DJ, Hruska CB, Conners AL, et al. Journal club: molecular breast imaging at reduced radiation dose for supplemental screening in mammographically dense breasts. AJR Am J Roentgenol. 2015;204(2): Rhodes DJ, Hruska CB, Phillips SW, Whaley DH, O'Connor MK. Dedicated dual-head gamma imaging for breast cancer screening in women with mammographically dense breasts. Radiology. 2011;258(1): Holbrook A, Newell MS. Alternative screening for women with dense breasts: breast-specific gamma imaging (molecular breast imaging). AJR Am J Roentgenol. 2015;204(2): ACR Appropriateness Criteria 8 Breast Cancer Screening
9 47. Saslow D, Boetes C, Burke W, et al. American Cancer Society guidelines for breast screening with MRI as an adjunct to mammography. CA Cancer J Clin. 2007;57(2): Berg WA, Blume JD, Cormack JB, et al. Combined screening with ultrasound and mammography vs mammography alone in women at elevated risk of breast cancer. JAMA. 2008;299(18): Berg WA, Zhang Z, Lehrer D, et al. Detection of breast cancer with addition of annual screening ultrasound or a single screening MRI to mammography in women with elevated breast cancer risk. JAMA. 2012;307(13): Friedlander LC, Roth SO, Gavenonis SC. Results of MR imaging screening for breast cancer in high-risk patients with lobular carcinoma in situ. Radiology. 2011;261(2): Sung JS, Malak SF, Bajaj P, Alis R, Dershaw DD, Morris EA. Screening breast MR imaging in women with a history of lobular carcinoma in situ. Radiology. 2011;261(2): Lehman CD, Lee JM, DeMartini WB, et al. Screening MRI in Women With a Personal History of Breast Cancer. J Natl Cancer Inst. 2016;108(3). 53. Brennan S, Liberman L, Dershaw DD, Morris E. Breast MRI screening of women with a personal history of breast cancer. AJR Am J Roentgenol. 2010;195(2): Hagen AI, Kvistad KA, Maehle L, et al. Sensitivity of MRI versus conventional screening in the diagnosis of BRCA-associated breast cancer in a national prospective series. Breast. 2007;16(4): Kriege M, Brekelmans CT, Boetes C, et al. Differences between first and subsequent rounds of the MRISC breast cancer screening program for women with a familial or genetic predisposition. Cancer. 2006;106(11): Kuhl CK, Schrading S, Leutner CC, et al. Mammography, breast ultrasound, and magnetic resonance imaging for surveillance of women at high familial risk for breast cancer. J Clin Oncol. 2005;23(33): Leach MO, Boggis CR, Dixon AK, et al. Screening with magnetic resonance imaging and mammography of a UK population at high familial risk of breast cancer: a prospective multicentre cohort study (MARIBS). Lancet. 2005;365(9473): Saadatmand S, Vos JR, Hooning MJ, et al. Relevance and efficacy of breast cancer screening in BRCA1 and BRCA2 mutation carriers above 60 years: a national cohort study. Int J Cancer. 2014;135(12): Sardanelli F, Podo F, D'Agnolo G, et al. Multicenter comparative multimodality surveillance of women at genetic-familial high risk for breast cancer (HIBCRIT study): interim results. Radiology. 2007;242(3): Kuhl C, Weigel S, Schrading S, et al. Prospective multicenter cohort study to refine management recommendations for women at elevated familial risk of breast cancer: the EVA trial. J Clin Oncol. 2010;28(9): Weinstein SP, Localio AR, Conant EF, Rosen M, Thomas KM, Schnall MD. Multimodality screening of high-risk women: a prospective cohort study. J Clin Oncol. 2009;27(36): Berg WA. Tailored supplemental screening for breast cancer: what now and what next? AJR Am J Roentgenol. 2009;192(2): Plevritis SK, Kurian AW, Sigal BM, et al. Cost-effectiveness of screening BRCA1/2 mutation carriers with breast magnetic resonance imaging. JAMA. 2006;295(20): Taneja C, Edelsberg J, Weycker D, Guo A, Oster G, Weinreb J. Cost effectiveness of breast cancer screening with contrast-enhanced MRI in high-risk women. J Am Coll Radiol. 2009;6(3): American College of Radiology. ACR Appropriateness Criteria Radiation Dose Assessment Introduction. Available at: Accessed September 1, The ACR Committee on Appropriateness Criteria and its expert panels have developed criteria for determining appropriate imaging examinations for diagnosis and treatment of specified medical condition(s). These criteria are intended to guide radiologists, radiation oncologists and referring physicians in making decisions regarding radiologic imaging and treatment. Generally, the complexity and severity of a patient s clinical condition should dictate the selection of appropriate imaging procedures or treatments. Only those examinations generally used for evaluation of the patient s condition are ranked. Other imaging studies necessary to evaluate other co-existent diseases or other medical consequences of this condition are not considered in this document. The availability of equipment or personnel may influence the selection of appropriate imaging procedures or treatments. Imaging techniques classified as investigational by the FDA have not been considered in developing these criteria; however, study of new equipment and applications should be encouraged. The ultimate decision regarding the appropriateness of any specific radiologic examination or treatment must be made by the referring physician and radiologist in light of all the circumstances presented in an individual examination. ACR Appropriateness Criteria 9 Breast Cancer Screening
ACR Appropriateness Criteria Breast Cancer Screening EVIDENCE TABLE. See Last Page for Key Revised 2017 Mainiero Page 1.
 1. Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin. 2017;67(1):7-0. Type Review/Other- N/A To estimate the numbers of new cancer cases and deaths that will occur in the United
1. Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin. 2017;67(1):7-0. Type Review/Other- N/A To estimate the numbers of new cancer cases and deaths that will occur in the United
Dense Breasts, Get Educated
 Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document
 RSNA, 2013 Appendix E1 Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document 1. I have been getting more questions
RSNA, 2013 Appendix E1 Frequently Asked Questions about Breast Density, Breast Cancer Risk, and the Breast Density Notification Law in California: A Consensus Document 1. I have been getting more questions
Scenarios for Clinicians
 Breast Density, Breast Cancer Risk and Wisconsin Breast Density Notification Law (2017 Wisconsin Act 201) Scenarios for Clinicians Content adapted from the California Breast Density Information Group,
Breast Density, Breast Cancer Risk and Wisconsin Breast Density Notification Law (2017 Wisconsin Act 201) Scenarios for Clinicians Content adapted from the California Breast Density Information Group,
Disclosures. Breast Cancer. Breast Imaging Modalities. Breast Cancer Screening. Breast Cancer 6/4/2014
 : Information for the Primary Care Physician Disclosures No financial relationships with commercial entities producing health care products/services. Roxsann Roberts, MD Section Chief, MRI Erlanger/EmCare
: Information for the Primary Care Physician Disclosures No financial relationships with commercial entities producing health care products/services. Roxsann Roberts, MD Section Chief, MRI Erlanger/EmCare
BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography
 BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography Poster No.: C-0562 Congress: ECR 2017 Type: Scientific Exhibit Authors:
BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography Poster No.: C-0562 Congress: ECR 2017 Type: Scientific Exhibit Authors:
6 OBG Management August 2015 Vol. 27 No. 8 obgmanagement.com
 Dense breasts are composed of a lot of fibrous and glandular tissue, with less adipose tissue. Heterogeneously dense and extremely dense breast tissue (as illustrated here) make it difficult to detect
Dense breasts are composed of a lot of fibrous and glandular tissue, with less adipose tissue. Heterogeneously dense and extremely dense breast tissue (as illustrated here) make it difficult to detect
WHAT TO EXPECT. Genius 3D MAMMOGRAPHY Exam. The most exciting advancement in mammography in over 30 years
 WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
Breast density: imaging, risks and recommendations
 Breast density: imaging, risks and recommendations Maureen Baxter, MD Radiologist Director of Ruth J. Spear Breast Center Providence St. Vincent Medical Center Alison Conlin, MD/MPH Medical Oncologist
Breast density: imaging, risks and recommendations Maureen Baxter, MD Radiologist Director of Ruth J. Spear Breast Center Providence St. Vincent Medical Center Alison Conlin, MD/MPH Medical Oncologist
BR 1 Palpable breast lump
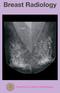 BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
Current Status of Supplementary Screening With Breast Ultrasound
 Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Supplemental Screening for Dense Breasts. Reagan Leverett, MD, MS
 Supplemental Screening for Dense Breasts Reagan Leverett, MD, MS Outline Anatomy and Density Risk of dense breasts Theory of Supplemental Screening Options for supplemental screening Tomosynthesis Ultrasound
Supplemental Screening for Dense Breasts Reagan Leverett, MD, MS Outline Anatomy and Density Risk of dense breasts Theory of Supplemental Screening Options for supplemental screening Tomosynthesis Ultrasound
Breast cancer screening: Does tomosynthesis augment mammography?
 REVIEW TRACI A. TAKAHASHI, MD, MPH Director, Seattle VA Women Veterans Clinic at VA Puget Sound Health Care System, Seattle, WA; Associate Professor of Medicine, University of Washington, Seattle CHRISTOPH
REVIEW TRACI A. TAKAHASHI, MD, MPH Director, Seattle VA Women Veterans Clinic at VA Puget Sound Health Care System, Seattle, WA; Associate Professor of Medicine, University of Washington, Seattle CHRISTOPH
Since its introduction in 2000, digital mammography has become
 Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
TOMOSYNTHESIS. Daniela Bernardi. U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy
 TOMOSYNTHESIS Daniela Bernardi U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy BACKGROUND early detection through screening MAMMOGRAPHY is associated with reduced breast cancer morbidity
TOMOSYNTHESIS Daniela Bernardi U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy BACKGROUND early detection through screening MAMMOGRAPHY is associated with reduced breast cancer morbidity
Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET
 Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET SAM Questions 1. 21 year old female presenting with left breast palpable mass, what is the most appropriate
Management of Palpable Abnormalities in the Breast Katerina Dodelzon, MD July 31, 2018, 7:00pm ET SAM Questions 1. 21 year old female presenting with left breast palpable mass, what is the most appropriate
Outline. Digital Breast Tomosynthesis: Update and Pearls for Implementation. Tomosynthesis Dataset: 2D/3D (Hologic Combo Acquisition)
 Outline Digital Breast Tomosynthesis (DBT) the new standard of care Digital Breast Tomosynthesis: Update and Pearls for Implementation Emily F. Conant, M.D. Professor, Chief of Breast Imaging Department
Outline Digital Breast Tomosynthesis (DBT) the new standard of care Digital Breast Tomosynthesis: Update and Pearls for Implementation Emily F. Conant, M.D. Professor, Chief of Breast Imaging Department
Breast Density. Update 2018: Implications for Clinical Practice
 Breast Density Update 2018: Implications for Clinical Practice Matthew A. Stein, MD Assistant professor Breast Imaging Department of Radiology and Imaging Sciences University of Utah Health Disclosures
Breast Density Update 2018: Implications for Clinical Practice Matthew A. Stein, MD Assistant professor Breast Imaging Department of Radiology and Imaging Sciences University of Utah Health Disclosures
Challenges to Delivery of High Quality Mammography
 Challenges to Delivery of High Quality Mammography Overview of Current Challenges Barbara Monsees, Washington University Geographic Access, Equity and Impact on Quality Tracy Onega, Dartmouth Medical School
Challenges to Delivery of High Quality Mammography Overview of Current Challenges Barbara Monsees, Washington University Geographic Access, Equity and Impact on Quality Tracy Onega, Dartmouth Medical School
The Dilemma of Breast Density in Screening
 The Dilemma of Breast Density in Screening Priscilla J. Slanetz MD, MPH, FACR, FSBI Associate Professor of Radiology, Harvard Medical School Beth Israel Deaconess Medical Center, Boston, MA No financial
The Dilemma of Breast Density in Screening Priscilla J. Slanetz MD, MPH, FACR, FSBI Associate Professor of Radiology, Harvard Medical School Beth Israel Deaconess Medical Center, Boston, MA No financial
Breast Imaging! Ravi Adhikary, MD!
 Breast Imaging! Ravi Adhikary, MD! ACS Estimated Cancers Statistics 2014! Breast! New Cases in Women! 232,670 (+67,570 in situ)! Deaths in Women! 40,000! Colon! 48,380! 24,040! Cervical! 12,360! 4,020!
Breast Imaging! Ravi Adhikary, MD! ACS Estimated Cancers Statistics 2014! Breast! New Cases in Women! 232,670 (+67,570 in situ)! Deaths in Women! 40,000! Colon! 48,380! 24,040! Cervical! 12,360! 4,020!
Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer 3/10/16
 Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer Policy Number: MCP-270 Revision Date(s): Original Effective Date: 3/10/16 Review Date: 6/22/17, 3/8/18 MCPC Approval Date: 3/8/18 DISCLAIMER
Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer Policy Number: MCP-270 Revision Date(s): Original Effective Date: 3/10/16 Review Date: 6/22/17, 3/8/18 MCPC Approval Date: 3/8/18 DISCLAIMER
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk
 The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
The best way of detection of and screening for breast cancer in women with genetic or hereditary risk Ingrid Vogelaar Introduction Each year almost 1.2 million women are diagnosed with breast cancer worldwide.
Magnetic Resonance Imaging Screening of Women at High Risk for Breast Cancer
 Evidence-Based Series 15-11 Version 2 IN REVIEW A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Magnetic Resonance Imaging Screening of Women at High Risk for
Evidence-Based Series 15-11 Version 2 IN REVIEW A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Magnetic Resonance Imaging Screening of Women at High Risk for
Screening Options in Dense Breasts. Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging
 Screening Options in Dense Breasts Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging Dense Breasted Women Decreased sensitivity of mammography
Screening Options in Dense Breasts Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging Dense Breasted Women Decreased sensitivity of mammography
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Breast Cancer Screening in Women at Higher-Than-Average Risk: Recommendations From the ACR
 ORIGINAL ARTICLE CLINICAL PRACTICE MANAGEMENT Breast Cancer Screening in Women at Higher-Than-Average Risk: Recommendations From the ACR Debra L. Monticciolo, MD a, Mary S. Newell, MD b, Linda Moy, MD
ORIGINAL ARTICLE CLINICAL PRACTICE MANAGEMENT Breast Cancer Screening in Women at Higher-Than-Average Risk: Recommendations From the ACR Debra L. Monticciolo, MD a, Mary S. Newell, MD b, Linda Moy, MD
Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at Digital Breast Tomosynthesis Screening 1
 Breast Imaging 1954 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at
Breast Imaging 1954 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at
Corporate Medical Policy. Digital Breast Tomosynthesis (DBT)
 Corporate Medical Policy Digital Breast Tomosynthesis (DBT) Description of Procedure or Service DBT is a three-dimensional (3D) breast imaging technology that uses a rotating X-ray source to acquire multiple
Corporate Medical Policy Digital Breast Tomosynthesis (DBT) Description of Procedure or Service DBT is a three-dimensional (3D) breast imaging technology that uses a rotating X-ray source to acquire multiple
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Nehmat Houssami 1, Kristina Lång 2, Solveig Hofvind 3, Sophia Zackrisson 2, Daniela Bernardi 4, Kylie Hunter 5, Lisa Askie 5, Per Skaane 6
 Study Protocol Effectiveness of digital breast tomosynthesis (3D-mammography) in population breast cancer screening: a protocol for a collaborative individual participant data (IPD) meta-analysis Nehmat
Study Protocol Effectiveness of digital breast tomosynthesis (3D-mammography) in population breast cancer screening: a protocol for a collaborative individual participant data (IPD) meta-analysis Nehmat
Breast Cancer Screening and Diagnosis
 Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
Dense Breasts. A Breast Cancer Risk Factor and Imaging Challenge
 Dense Breasts A Breast Cancer Risk Factor and Imaging Challenge Renee Pinsky, MD University of Michigan Department of Radiology Division of Breast Imaging No Disclosures QUIZ: ARE YOU DENSE? a. Breast
Dense Breasts A Breast Cancer Risk Factor and Imaging Challenge Renee Pinsky, MD University of Michigan Department of Radiology Division of Breast Imaging No Disclosures QUIZ: ARE YOU DENSE? a. Breast
Fremtidens rolle for tomosyntese
 Dansk Radiologisk Selskab 9.årsmøde Odense 3.januar, 214 Fremtidens rolle for tomosyntese Professor dr. med. Per Skaane Oslo University Hospital Ullevaal Breast Imaging Center Oslo / Norway PERSKA@ous-hf.no
Dansk Radiologisk Selskab 9.årsmøde Odense 3.januar, 214 Fremtidens rolle for tomosyntese Professor dr. med. Per Skaane Oslo University Hospital Ullevaal Breast Imaging Center Oslo / Norway PERSKA@ous-hf.no
SCREENING FOR BREAST CANCER BREAST IMAGING
 SCREENING FOR BREAST CANCER BREAST IMAGING Liane Philpotts, MD, FSBI, FACR Professor, Radiology and Biomedical Imaging Division Chief, Breast Imaging Dec. 5, 2017 Warner, E. NEJM 2011 Screening for
SCREENING FOR BREAST CANCER BREAST IMAGING Liane Philpotts, MD, FSBI, FACR Professor, Radiology and Biomedical Imaging Division Chief, Breast Imaging Dec. 5, 2017 Warner, E. NEJM 2011 Screening for
MANAGEMENT OF DENSE BREASTS. Nichole K Ingalls, MD, MPH NW Surgical Specialists September 25, 2015
 MANAGEMENT OF DENSE BREASTS Nichole K Ingalls, MD, MPH NW Surgical Specialists September 25, 2015 No financial disclosures National Cancer Institute National Cancer Institute Increased Cancer Risk... DENSITY
MANAGEMENT OF DENSE BREASTS Nichole K Ingalls, MD, MPH NW Surgical Specialists September 25, 2015 No financial disclosures National Cancer Institute National Cancer Institute Increased Cancer Risk... DENSITY
Jing Zhang, PhD, Lars J. Grimm, MD, MHS, Joseph Y. Lo, PhD, Karen S. Johnson, MD,
 This manuscript has been accepted for publication in Journal of the American College of Radiology. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published
This manuscript has been accepted for publication in Journal of the American College of Radiology. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published
Additional US or DBT after digital mammography: which one is the best combination?
 Additional US or DBT after digital mammography: which one is the best combination? Poster No.: B-0926 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Elizalde, P. Garcia Barquin, M.
Additional US or DBT after digital mammography: which one is the best combination? Poster No.: B-0926 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Elizalde, P. Garcia Barquin, M.
Breast Cancer Screening Using Tomosynthesis in Combination With Digital Mammography
 Research Original Investigation Breast Cancer Screening Using in Combination With Sarah M. Friedewald, MD; Elizabeth A. Rafferty, MD; Stephen L. Rose, MD; Melissa A. Durand, MD; Donna M. Plecha, MD; Julianne
Research Original Investigation Breast Cancer Screening Using in Combination With Sarah M. Friedewald, MD; Elizabeth A. Rafferty, MD; Stephen L. Rose, MD; Melissa A. Durand, MD; Donna M. Plecha, MD; Julianne
Update in Breast Cancer Screening
 Disclosure information: Update in Breast Cancer Screening Karla Kerlikowske, MDDis Update in Breast Cancer Screening Grant/Research support from: National Cancer Institute - and - Karla Kerlikowske, MD
Disclosure information: Update in Breast Cancer Screening Karla Kerlikowske, MDDis Update in Breast Cancer Screening Grant/Research support from: National Cancer Institute - and - Karla Kerlikowske, MD
Financial Disclosures
 Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
Update in Breast Cancer Screening
 Disclosure information: Update in Breast Cancer Screening Karla Kerlikowske, MDDis Update in Breast Cancer Screening Grant/Research support from: National Cancer Institute and Grail - and - Karla Kerlikowske,
Disclosure information: Update in Breast Cancer Screening Karla Kerlikowske, MDDis Update in Breast Cancer Screening Grant/Research support from: National Cancer Institute and Grail - and - Karla Kerlikowske,
Magnetic Resonance Imaging and Breast Ultrasonography as an Adjunct to Mammographic Screening in High-Risk Patients
 Magnetic Resonance Imaging and Breast Ultrasonography as an Adjunct to Mammographic Screening in High-Risk Patients Huong T. Le-Petross, MD,* and Mahesh K. Shetty, MD, FRCR, FACR Screening mammography
Magnetic Resonance Imaging and Breast Ultrasonography as an Adjunct to Mammographic Screening in High-Risk Patients Huong T. Le-Petross, MD,* and Mahesh K. Shetty, MD, FRCR, FACR Screening mammography
Digital Breast Tomosynthesis for Screening and Diagnostic Imaging. Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI
 Digital Breast Tomosynthesis for Screening and Diagnostic Imaging Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI Digital breast tomosynthesis (DBT), which was FDA approved in 2011, is rapidly
Digital Breast Tomosynthesis for Screening and Diagnostic Imaging Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI Digital breast tomosynthesis (DBT), which was FDA approved in 2011, is rapidly
Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in Patients with Dense Breasts
 Original Article Breast Imaging eissn 2005-8330 Korean J Radiol 2019;20(1):58-68 Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in
Original Article Breast Imaging eissn 2005-8330 Korean J Radiol 2019;20(1):58-68 Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in
Breast Density and Breast Tomosynthesis. How have they changed our lives?
 Breast Density and Breast Tomosynthesis How have they changed our lives? Renee W. Pinsky, MD Associate Professor of Radiology University of Michigan The only thing that is constant is change Heraclitus
Breast Density and Breast Tomosynthesis How have they changed our lives? Renee W. Pinsky, MD Associate Professor of Radiology University of Michigan The only thing that is constant is change Heraclitus
Breast Cancer Imaging
 Breast Cancer Imaging I. Policy University Health Alliance (UHA) will cover breast imaging when such services meet the medical criteria guidelines (subject to limitations and exclusions) indicated below.
Breast Cancer Imaging I. Policy University Health Alliance (UHA) will cover breast imaging when such services meet the medical criteria guidelines (subject to limitations and exclusions) indicated below.
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA
 Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
New Imaging Modalities for better Screening and Diagnosis
 New Imaging Modalities for better Screening and Diagnosis Miri Sklair-Levy, MD Department of Diagnostic Imaging Sheba Medical Center, Sackler School of Medicine, Tel Aviv University Department of Diagnostic
New Imaging Modalities for better Screening and Diagnosis Miri Sklair-Levy, MD Department of Diagnostic Imaging Sheba Medical Center, Sackler School of Medicine, Tel Aviv University Department of Diagnostic
Until recently, when it was surpassed by lung cancer,
 SUPPLEMENT TO Continuing medical education (CME) credit is awarded upon successful completion of the posttest and evaluation. To access the posttest and evaluation, visit www.worldclasscme.com/imagingofthebreast
SUPPLEMENT TO Continuing medical education (CME) credit is awarded upon successful completion of the posttest and evaluation. To access the posttest and evaluation, visit www.worldclasscme.com/imagingofthebreast
Detection to Prediction: Imaging Markers of Breast Cancer Risk
 Detection to Prediction: Imaging Markers of Breast Cancer Risk Carrie B. Hruska, PhD, DABR Associate Professor of Medical Physics Mayo Clinic, Rochester, MN 2017 MFMER slide-1 Disclosure Per agreement
Detection to Prediction: Imaging Markers of Breast Cancer Risk Carrie B. Hruska, PhD, DABR Associate Professor of Medical Physics Mayo Clinic, Rochester, MN 2017 MFMER slide-1 Disclosure Per agreement
MRI of the Breast Positron Emission Tomography (PET) Scintimammography/Breast-Specific Gamma Imaging/Molecular Breast Imaging
 6.01.53 Digital Breast Tomosynthesis Section Radiology Subsection Effective Date September 30, 2014 Original Policy Date June 28, 2013 Next Review Date September 2015 Description Digital breast tomosynthesis
6.01.53 Digital Breast Tomosynthesis Section Radiology Subsection Effective Date September 30, 2014 Original Policy Date June 28, 2013 Next Review Date September 2015 Description Digital breast tomosynthesis
Angela Gilliam, MD University of Colorado Surgical Grand Rounds November 3, 2008
 Angela Gilliam, MD University of Colorado Surgical Grand Rounds November 3, 2008 Breast Cancer Most common cancer in American women 180,000 new cases per year Second most common cause of cancer death 44,000
Angela Gilliam, MD University of Colorado Surgical Grand Rounds November 3, 2008 Breast Cancer Most common cancer in American women 180,000 new cases per year Second most common cause of cancer death 44,000
Update of Digital Breast Tomosynthesis. Susan Orel Roth, MD
 Update of Digital Breast Tomosynthesis Susan Orel Roth, MD NCI estimates that : Why DBT? Approximately 20% of breast cancers are missed at mammography screening Average recall rates approximately 10%
Update of Digital Breast Tomosynthesis Susan Orel Roth, MD NCI estimates that : Why DBT? Approximately 20% of breast cancers are missed at mammography screening Average recall rates approximately 10%
Breast cancer screening: emerging role of new imaging techniques as adjuncts to mammography
 Breast cancer screening: emerging role of new imaging techniques as adjuncts to mammography Nehmat Houssami, Sarah J Lord and Stefano Ciatto Randomised trials of mammography screening have shown that early
Breast cancer screening: emerging role of new imaging techniques as adjuncts to mammography Nehmat Houssami, Sarah J Lord and Stefano Ciatto Randomised trials of mammography screening have shown that early
Why it matters and what to do
 Breast density: Why it matters and what to do Breast density is a frequent topic on social media, in the news and within medical literature - and your patients may be asking you about it. Dense breast
Breast density: Why it matters and what to do Breast density is a frequent topic on social media, in the news and within medical literature - and your patients may be asking you about it. Dense breast
Breast Cancer Screening Clinical Practice Guideline. Kaiser Permanente National Breast Cancer Screening Guideline Development Team
 NATIONAL CLINICAL PRACTICE GUIDELINE Breast Cancer Screening Clinical Practice Guideline Kaiser Permanente National Breast Cancer Screening Guideline Development Team This guideline is informational only.
NATIONAL CLINICAL PRACTICE GUIDELINE Breast Cancer Screening Clinical Practice Guideline Kaiser Permanente National Breast Cancer Screening Guideline Development Team This guideline is informational only.
Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features.
 Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features. Poster No.: C-1707 Congress: ECR 2015 Type: Scientific Exhibit Authors: V. Vinci 1, A. Iqbal
Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features. Poster No.: C-1707 Congress: ECR 2015 Type: Scientific Exhibit Authors: V. Vinci 1, A. Iqbal
American College of Radiology ACR Appropriateness Criteria Breast Pain
 Revised 2018 American College of Radiology ACR Appropriateness Criteria Breast Pain Variant 1: Woman with clinically insignificant breast pain (nonfocal [greater than one quadrant], diffuse, or cyclical)
Revised 2018 American College of Radiology ACR Appropriateness Criteria Breast Pain Variant 1: Woman with clinically insignificant breast pain (nonfocal [greater than one quadrant], diffuse, or cyclical)
Low Dose Molecular Breast Imaging
 Low Dose Molecular Breast Imaging Dr. M.K. O Connor Conflict of Interest Royalties - Gamma Medica Research funding GE Healthcare Research support MTTI Michael O Connor, Ph.D Dept. of Radiology Mayo Clinic
Low Dose Molecular Breast Imaging Dr. M.K. O Connor Conflict of Interest Royalties - Gamma Medica Research funding GE Healthcare Research support MTTI Michael O Connor, Ph.D Dept. of Radiology Mayo Clinic
Title: Ultrasound for Breast Cancer Screening: Clinical Effectiveness. Date: 4 January Context and policy issues:
 Title: Ultrasound for Breast Cancer Screening: Clinical Effectiveness Date: 4 January 2008 Context and policy issues: It is estimated that 22,300 women will be diagnosed with breast cancer and approximately
Title: Ultrasound for Breast Cancer Screening: Clinical Effectiveness Date: 4 January 2008 Context and policy issues: It is estimated that 22,300 women will be diagnosed with breast cancer and approximately
What s New in Breast Imaging. Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia
 What s New in Breast Imaging Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia Disclosure Hologic, Inc. Shareholder and research agreement. Volpara Solutions, Ltd. Shareholder
What s New in Breast Imaging Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia Disclosure Hologic, Inc. Shareholder and research agreement. Volpara Solutions, Ltd. Shareholder
2018 PUBLIC REPORTING OF OUTCOMES
 2018 PUBLIC REPORTING OF OUTCOMES The Cancer Committee at Western Maryland Health System s Schwab Family Cancer Center reports annually on program and patient outcomes in compliance with the accreditation
2018 PUBLIC REPORTING OF OUTCOMES The Cancer Committee at Western Maryland Health System s Schwab Family Cancer Center reports annually on program and patient outcomes in compliance with the accreditation
Effect of Mammographic Screening Modality on Breast Density Assessment: Digital Mammography versus Digital Breast Tomosynthesis
 ORIGINAL RESEARCH BREAST IMAGING Effect of Mammographic Screening Modality on Breast Density Assessment: Digital Mammography versus Digital Breast Tomosynthesis Aimilia Gastounioti, PhD Anne Marie McCarthy,
ORIGINAL RESEARCH BREAST IMAGING Effect of Mammographic Screening Modality on Breast Density Assessment: Digital Mammography versus Digital Breast Tomosynthesis Aimilia Gastounioti, PhD Anne Marie McCarthy,
Ruud Pijnappel Professor of Radiology, UMC Utrecht. Chair Dutch Expert Centre for Screening Board EUSOBI
 Ruud Pijnappel Professor of Radiology, UMC Utrecht Best practice in Breast Imaging: what s new and what women need to know and Update on the Second Implementation Report of the 2003 Council Recommendation
Ruud Pijnappel Professor of Radiology, UMC Utrecht Best practice in Breast Imaging: what s new and what women need to know and Update on the Second Implementation Report of the 2003 Council Recommendation
MEDICAL POLICY SUBJECT: MAMMOGRAPHY: COMPUTER- AIDED DETECTION (CAD) POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: MAMMOGRAPHY: COMPUTER- PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: MAMMOGRAPHY: COMPUTER- PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Literature Review: California Senate Bill 1034 Health Care: Mammograms AT A GLANCE
 Literature Review: California Senate Bill 1034 Health Care: Mammograms Summary to the 2018-2019 California State Legislature, April 16, 2018 AT A GLANCE On February 26, 2018, the Senate Committee on Health
Literature Review: California Senate Bill 1034 Health Care: Mammograms Summary to the 2018-2019 California State Legislature, April 16, 2018 AT A GLANCE On February 26, 2018, the Senate Committee on Health
Improving the Identification of Underserved Women at High Risk for Breast Cancer and Increasing the use of Breast MRI Screening in this Population
 Improving the Identification of Underserved Women at High Risk for Breast Cancer and Increasing the use of Breast MRI Screening in this Population Greenwood HI, Truong L, Price ER. UCSF Department or Radiology
Improving the Identification of Underserved Women at High Risk for Breast Cancer and Increasing the use of Breast MRI Screening in this Population Greenwood HI, Truong L, Price ER. UCSF Department or Radiology
Implementation of Breast Tomosynthesis in a Routine Screening Practice: An Observational Study
 Women s Imaging Original Research Rose et al. Tomosynthesis in Routine Screening Women s Imaging Original Research Stephen L. Rose 1 Andra L. Tidwell Louis J. Bujnoch Anne C. Kushwaha Amy S. Nordmann Russell
Women s Imaging Original Research Rose et al. Tomosynthesis in Routine Screening Women s Imaging Original Research Stephen L. Rose 1 Andra L. Tidwell Louis J. Bujnoch Anne C. Kushwaha Amy S. Nordmann Russell
Breast Density. Information for Health Professionals
 Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
BREAST MRI. Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School
 BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Digital Breast Tomosynthesis Page 1 of 31 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Digital Breast Tomosynthesis Professional Institutional Original Effective
Digital Breast Tomosynthesis Page 1 of 31 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Digital Breast Tomosynthesis Professional Institutional Original Effective
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Early Detection and Diagnosis Early Detection and Diagnosis Version 2005: Junkermann Version 2006 2009: Schreer / Albert Version
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Early Detection and Diagnosis Early Detection and Diagnosis Version 2005: Junkermann Version 2006 2009: Schreer / Albert Version
Tissue Breast Density
 Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
Tissue Breast Density Reporting breast density within the letter to the patient is now mandated by VA law. Therefore, this website has been established by Peninsula Radiological Associates (PRA), the radiologists
Breast Cancer Screening
 Breast Cancer Screening Eileen Rakovitch MD MSc FRCPC Sunnybrook Health Sciences Centre Medical Director, Louise Temerty Breast Cancer Centre LC Campbell Chair in Breast Cancer Research Associate Professor,
Breast Cancer Screening Eileen Rakovitch MD MSc FRCPC Sunnybrook Health Sciences Centre Medical Director, Louise Temerty Breast Cancer Centre LC Campbell Chair in Breast Cancer Research Associate Professor,
Breast Cancer Screening
 Breast Cancer Screening Ravinder S. Legha 1, Jessica Wai Ting Leung After skin cancer, breast cancer is the cancer most diagnosed in U.S. women and has the second highest death rate. Breast cancer will
Breast Cancer Screening Ravinder S. Legha 1, Jessica Wai Ting Leung After skin cancer, breast cancer is the cancer most diagnosed in U.S. women and has the second highest death rate. Breast cancer will
High Risk Screening: A Multimodality Approach
 High Risk Screening: A Multimodality Approach John Lewin, M.D., FACR, FSBI The Women s Imaging Center Denver, Colorado Disclosures Consultant to Hologic Previously received research funds from Hologic
High Risk Screening: A Multimodality Approach John Lewin, M.D., FACR, FSBI The Women s Imaging Center Denver, Colorado Disclosures Consultant to Hologic Previously received research funds from Hologic
Breast Density: Significance and Notification. Carol H. Lee Memorial Sloan-Kettering Cancer Center New York, NY
 Breast Density: Significance and Notification Carol H. Lee Memorial Sloan-Kettering Cancer Center New York, NY Significance of Breast Density Association with increased risk for breast cancer Decreased
Breast Density: Significance and Notification Carol H. Lee Memorial Sloan-Kettering Cancer Center New York, NY Significance of Breast Density Association with increased risk for breast cancer Decreased
Women s Imaging Original Research
 Women s Imaging Original Research Greenberg et al. Breast Cancer Screening Using 3D DBT Versus 2D DM Women s Imaging Original Research Julianne S. Greenberg 1 Marcia C. Javitt 2 Jason Katzen 1 Sara Michael
Women s Imaging Original Research Greenberg et al. Breast Cancer Screening Using 3D DBT Versus 2D DM Women s Imaging Original Research Julianne S. Greenberg 1 Marcia C. Javitt 2 Jason Katzen 1 Sara Michael
Dr Robin Wilson, The Royal Marsden
 Screening: State of the Art High risk and dense breasts Robin Wilson Smart Breast Screening? 1 in 8 women in the will get breast cancer 8 in 9 will not 55% of breast cancers are not screen detected One
Screening: State of the Art High risk and dense breasts Robin Wilson Smart Breast Screening? 1 in 8 women in the will get breast cancer 8 in 9 will not 55% of breast cancers are not screen detected One
WHAT TO EXPECT. Genius 3D Mammography Exam. The most exciting advancement in mammography in over 30 years
 WHAT TO EXPECT Genius 3D Mammography Exam The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense
WHAT TO EXPECT Genius 3D Mammography Exam The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense
Ge elastography cpt codes
 Ge elastography cpt codes Aetna considers digital mammography a medically necessary acceptable alternative to film mammography. Currently, there are no guideline recommendations from leading medical professional
Ge elastography cpt codes Aetna considers digital mammography a medically necessary acceptable alternative to film mammography. Currently, there are no guideline recommendations from leading medical professional
Magnetic resonance imaging (MRI) in high risk women: benefits and problems
 Magnetic resonance imaging (MRI) in high risk women: benefits and problems Poster No.: C-2466 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Pecchi, V. Marchesi, R. Battista, B. Canossi, L. Cortesi,
Magnetic resonance imaging (MRI) in high risk women: benefits and problems Poster No.: C-2466 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Pecchi, V. Marchesi, R. Battista, B. Canossi, L. Cortesi,
Automated breast ultrasound: a novel approach to screening women with dense breasts
 Automated breast ultrasound: a novel approach to screening women with dense breasts Automated breast ultrasound is likely to be a key player in the future of imaging for women with dense breast tissue.
Automated breast ultrasound: a novel approach to screening women with dense breasts Automated breast ultrasound is likely to be a key player in the future of imaging for women with dense breast tissue.
Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis
 Konica Minolta Healthcare Americas, Inc. Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis A WHITEPAPER INTRODUCTION Numerous published studies have shown
Konica Minolta Healthcare Americas, Inc. Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis A WHITEPAPER INTRODUCTION Numerous published studies have shown
National Diagnostic Imaging Symposium 2013 SAM - Breast MRI 1
 National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases?
 BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases? Poster No.: B-0966 Congress: ECR 2013 Type: Scientific Paper Authors: J. Etxano Cantera, I. Simon-Yarza, G.
BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases? Poster No.: B-0966 Congress: ECR 2013 Type: Scientific Paper Authors: J. Etxano Cantera, I. Simon-Yarza, G.
Imaging Surveillance in Women with a History of Treated Breast Cancer. Wei Tse Yang, M.D.
 Imaging Surveillance in Women with a History of Treated Breast Cancer Wei Tse Yang, M.D. Breast Cancer 1. Extent 2. Response 3. Recurrence Surveillance Breast Cancer 1. Extent 2. Response Surveillance
Imaging Surveillance in Women with a History of Treated Breast Cancer Wei Tse Yang, M.D. Breast Cancer 1. Extent 2. Response 3. Recurrence Surveillance Breast Cancer 1. Extent 2. Response Surveillance
Foreword: Radiology Select Volume 8 Breast Imaging: Beyond Mammographic Screening
 Foreword: Radiology Select Volume 8 Breast Imaging: Beyond Mammographic Screening Dear Radiology Select Reader: In 2013, our fourth volume of Radiology Select was introduced, Breast Cancer Screening. This
Foreword: Radiology Select Volume 8 Breast Imaging: Beyond Mammographic Screening Dear Radiology Select Reader: In 2013, our fourth volume of Radiology Select was introduced, Breast Cancer Screening. This
Screening Breast Ultrasound: Past, Present, and Future
 Women s Imaging Review Brem et al. Breast Cancer Screening Ultrasound Women s Imaging Review FOCUS ON: Rachel F. Brem 1 Megan J. Lenihan Jennifer Lieberman Jessica Torrente Brem RF, Lenihan MJ, Lieberman
Women s Imaging Review Brem et al. Breast Cancer Screening Ultrasound Women s Imaging Review FOCUS ON: Rachel F. Brem 1 Megan J. Lenihan Jennifer Lieberman Jessica Torrente Brem RF, Lenihan MJ, Lieberman
BREAST MRI. Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School
 BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
The U.S. Preventive Services Task Force (USPSTF) CLINICAL GUIDELINE
 Annals of Internal Medicine CLINICAL GUIDELINE Screening for Breast Cancer: U.S. Preventive Services Task Force Recommendation Statement Albert L. Siu, MD, MSPH, on behalf of the U.S. Preventive Services
Annals of Internal Medicine CLINICAL GUIDELINE Screening for Breast Cancer: U.S. Preventive Services Task Force Recommendation Statement Albert L. Siu, MD, MSPH, on behalf of the U.S. Preventive Services
TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy
 TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy DATE: 26 September 2013 CONTEXT AND POLICY ISSUES Breast cancer is the second leading
TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy DATE: 26 September 2013 CONTEXT AND POLICY ISSUES Breast cancer is the second leading
the one name in cancer care.
 the one name in cancer care. Landmark study evaluating close to half a million mammography exams published in the Journal of the American Medical Association (JAMA) 1 Hologic 3D Mammography Significantly
the one name in cancer care. Landmark study evaluating close to half a million mammography exams published in the Journal of the American Medical Association (JAMA) 1 Hologic 3D Mammography Significantly
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI
 Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
The potential impact of breast
 Colin Mar, MD, FRCPC, Janette Sam, RTR, Christine Wilson, MD, FRCPC Breast cancer screening in British Columbia: A guide to discussion with patients Primary care providers have an important role to play
Colin Mar, MD, FRCPC, Janette Sam, RTR, Christine Wilson, MD, FRCPC Breast cancer screening in British Columbia: A guide to discussion with patients Primary care providers have an important role to play
Does the synthesised digital mammography (3D-DM) change the ACR density pattern?
 Does the synthesised digital mammography (3D-DM) change the ACR density pattern? Poster No.: B-0211 Congress: ECR 2015 Type: Scientific Paper Authors: P. MARTÍNEZ MIRAVETE, M. Millor Muruzábal, P. García-
Does the synthesised digital mammography (3D-DM) change the ACR density pattern? Poster No.: B-0211 Congress: ECR 2015 Type: Scientific Paper Authors: P. MARTÍNEZ MIRAVETE, M. Millor Muruzábal, P. García-
3D Mammography. The most exciting advancement in mammography in over 30 years
 What to Expect 3D Mammography The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense against breast
What to Expect 3D Mammography The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense against breast
