Women s Imaging Original Research
|
|
|
- Edward Skinner
- 6 years ago
- Views:
Transcription
1 Women s Imaging Original Research Greenberg et al. Breast Cancer Screening Using 3D DBT Versus 2D DM Women s Imaging Original Research Julianne S. Greenberg 1 Marcia C. Javitt 2 Jason Katzen 1 Sara Michael 3 Agnes E. Holland 1 Greenberg JS, Javitt MC, Katzen J, Michael S, Holland AE Keywords: 3D mammography, breast cancer, breast tomosynthesis, mammography screening DOI: /AJR Received February 4, 2014; accepted after revision March 11, Washington Radiology Associates, PC, 3022 Williams Dr, Ste 200, Fairfax, VA Address correspondence to J. S. Greenberg (jgreenberg@wrapc.com). 2 Department of Medical Imaging, Rambam Health Care Campus, Haifa, Israel. 3 Department of Radiology, Walter Reed National Military Medical Center, Bethesda, MD. AJR 2014; 203: X/14/ American Roentgen Ray Society Clinical Performance Metrics of 3D Digital Breast Tomosynthesis Compared With 2D Digital Mammography for Breast Cancer Screening in Community Practice OBJECTIVE. The objective of our study was to assess the clinical performance of combined 2D-3D digital breast tomosynthesis (DBT), referred to as 3D DBT, compared with 2D digital mammography (DM) alone for screening mammography in a community-based radiology practice. MATERIALS AND METHODS. Performance outcomes measures were assessed for 14 radiologists who interpreted more than 500 screening mammography 3D DBT studies after the initiation of tomosynthesis. Outcomes from screening mammography during the study period between August 9, 2011, and November 30, 2012, using 3D DBT (n = 23,149 patients) versus 2D DM (n = 54,684 patients) were compared. RESULTS. For patients screened with 3D DBT, the relative change in recall rate was 16.1% lower than for patients screened with 2D DM (p > ). The overall cancer detection rate (CDR), expressed as number of cancers per 1000 patients screened, was 28.6% greater (p = 0.035) for 3D DBT (6.3/1000) compared with 2D DM (4.9/1000). The CDR for invasive cancers with 3D DBT (4.6/1000) was 43.8% higher (p = ) than with 2D DM (3.2/1000). The positive predictive value for recalls from screening (PPV1) was 53.3% greater (p = ) for 3D DBT (4.6%) compared with 2D DM (3.0%). No significant difference in the positive predictive value for biopsy (PPV3) was found for 3D DBT versus 2D DM (22.8% and 23.8%, respectively) (p = 0.696). CONCLUSION. In community-based radiology practice, mammography screening with 3D DBT yielded lower recall rates, an increased CDR for cancer overall, and an increased CDR for invasive cancer compared with 2D DM. The PPV1 was significantly greater in the group screened using 3D DBT. S ince the introduction of mammography in the 1960s for the detection of breast cancer, breast screening technology has advanced. Recent controversies have focused attention on the overdiagnosis of clinically insignificant lesions, negative impact of false-positive recalls from screening, and low positive predictive value from biopsy after abnormal screening. Both film-screen mammography and 2D digital mammography (DM) are limited for breast cancer screening by decreased sensitivity in women with dense breasts [1, 2] and by false-positive recalls attributed to overlapping normal breast tissues. Additionally, dense tissues can obscure breast cancers, thereby producing false-negative results. The latest technologic advance in mammography 3D digital breast tomosynthesis (DBT) may provide solutions. First approved by the U.S. Food and Drug Ad- ministration (FDA) on February 11, 2011 [3], combined 2D-3D DBT may decrease the recall rate and increase the cancer detection rate (CDR) for mammographic screening as noted in observer performance studies [4 7]. Initial European population-based screening programs documented improvements in clinical outcomes for 3D DBT [8, 9]. In the United States, Haas et al. [10] recently reported a significant reduction in recall rate with 3D DBT screening. From communitybased practice, Rose et al. [11] reported a significant increase in the detection of invasive cancers and in the positive predictive value for screening recalls (PPV1) with 3D DBT compared with 2D DM alone. As early adopters of 3D DBT in community-based practice, we aimed to retrospectively compare the clinical performance of 3D DBT (combined 2D-3D DM) with conventional 2D DM alone in a high-volume population-based breast cancer screening program. AJR:203, September
2 Greenberg et al. Materials and Methods This retrospective study was performed at a multisite community-based radiology practice that instituted a DBT program in August We compared screening mammography outcomes metrics for 2D DM alone with those of 3D DBT in contemporaneous patient cohorts. The study protocol was approved by Western Institutional Review Board (WIRB), an independent commercial IRB, and was HIPAA compliant. A waiver of written informed consent was obtained. Study Design and Participants We compared mammography audit and patient demographic data for consecutive patients who underwent screening by 2D DM or 3D DBT between August 9, 2011, and November 30, Initially, we began to use our tomosynthesis-capable mammography unit on August 9, 2011, in our Potomac, MD, office. Subsequently, five additional sites (Bethesda, MD; Chevy Chase, MD; Washington, DC; Fairfax, VA; and Sterling, VA) installed DBT units through March Screening mammograms for all patients were obtained with DMcapable and DBT-capable equipment (Selenia or Selenia Dimensions, Hologic) in both the craniocaudal and mediolateral oblique projections. After receiving written material about 3D DBT and a verbal explanation of the technology, all screening mammography patients at our Potomac, MD, office were offered the option of 3D DBT. The first patients who opted for 3D DBT received the examination without additional charge until December 6, 2011 (1147 patients). Thereafter, 3D DBT was offered for an additional $50 fee. As each office installed tomosynthesis, during the 7- to 10-day period of applications training, 3D DBT was performed without charge (1577 patients). Thereafter, a $50 fee was charged. If a patient indicated she was unable to afford the fee, then tomosynthesis was performed free of charge. Of 77,833 women screened, 23,149 patients (29.7%) opted for 3D DBT and 54,684 patients (70.3%) for 2D DM screening. Of our 24 boardcertified radiologists, 10 interpreted relatively few (< 500) 3D DBT. To include only the relatively consistent readers who TABLE 1: Clinical Performance Measures of 2D Digital Mammography (DM) Versus 3D Digital Breast Tomosynthesis (DBT) in Community-Based Practice Measure 2D DM 3D DBT p a No. of screening examinations 38,674 20,943 No. of patients recalled Recall rate (no. of patients recalled per 100 No. of patients LTF after recall from screening 3D DBT 2D DM Relative < ( ) PPV1 without LTF cases (%) ( ) PPV1 with LTF cases (%) ( ) No. of biopsies Biopsy Rate (no./1000) (9.69,33.83) No. of biopsies without cancer Noncancer biopsy rate (no. of biopsies performed per 1000 No. of patients with cancer c No. of patients after biopsy recommendation LTF CDR (no. of cancers per ( ) ( ) PPV3 without LTF cases (%) ( 15.6 to 24.36) PPV3 with LTF cases (%) ( 14.7 to 25.88) Absolute 2.60 ( ) 1.60 ( ) 1.50 ( ) 0.47 (0.21, 0.73) 0.34 ( ) 0.14 ( ) 1.00 ( 3.55 to 5.55) 1.20 ( 3.16 to 5.56) 2D DM 15.5 ( ) 3.0 ( ) 3.0 ( ) 20.8 (18.1, 23.9) 16.0 ( ) 4.9 ( ) 22.8 ( ) 21.5 ( ) Generalized Linear Mixed Model b 3D DBT 13.4 ( ) 4.6 ( ) 4.5 ( ) 25.1 (21.6, 29.0) 19.0 ( ) 6.2 ( ) 23.8 ( ) 22.7 ( ) p Change (%) < ( ) ( ) ( ) (7.77,34.50) ( ) ( ) ( 14.5 to 27.73) ( 13.7 to 29.40) Note All data are for radiologists with experience reading more than 500 3D DBT examinations. Values in parentheses are 95% CIs. LTF = lost to follow-up, PPV1 = positive predictive value for recalls from screening, CDR = cancer detection rate, PPV3 = positive predictive value for biopsy. a Fisher exact test. b For each of the outcome measures, a generalized linear mixed model (PROC Glimmix procedure [SAS software, version 9.3, SAS Institute]) was used to analyze the difference between 2D DM and 3D DBT. The link function was specified as LOGIT. The correlation between reads made by the same radiologists was accounted for by specifying radiologist as the G-side random effect. The adjusted rates were calculated using the fitted model and their 95% CIs were derived using the delta method. c The 190 2D DM cancers include one patient with Hodgkin lymphoma and one patient with non-hodgkin lymphoma. The 131 3D DBT cancers include one patient with sarcoma. These patients are not included in cancer totals for Table AJR:203, September 2014
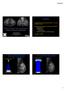
3 Breast Cancer Screening Using 3D DBT Versus 2D DM 54,684 2D DM 77,833 Screening mammography studies 23,149 3D DBT 59,617 Screening studies were read by radiologists who had interpreted > 500 3D DBT studies during the study period 38,674 2D DM 20,943 3D DBT had presumably overcome the learning effects of new technology, we evaluated only the data for the 14 radiologists who interpreted more than 500 3D DBT screening mammography studies during the study period. Therefore, 59,617 patients were included in two patient cohorts: 38,674 patients who underwent 2D DM and 20,943 patients who underwent 3D DBT (Fig. 1 and Table 1). The 14 study group radiologists had previously been trained to interpret DM. All had completed the required 8-hour tomosynthesis training mandated by the Mammography Quality Standards Act (MQSA) [12]. They had 2 38 years of postresidency or fellowship clinical experience in breast imaging (average, 18.6 years). Four of the radiologists had completed fellowship training in breast imaging and 10 had spent at least 75% of their clinical practice in breast imaging. Audit Data and Outcomes Measures Aggregate mammography audit and patient demographic data were acquired from our MQSAcompliant radiology information system (RIS) (Merge RIS, Merge Healthcare) and mammography information system (MIS) (MagView Mammography Information System, MagView). The RIS recorded which patients underwent 2D DM and which underwent 3D DBT. The MIS provided the following information: patient age, breast density, family history of breast cancer, use of hormones, and whether the study was a baseline study or a subsequent mammography study. Cancer diagnoses were determined by review of pathology reports from needle and surgical biopsies and from surgical treatment procedures for cancers. These reports were obtained as part of our routine data acquisition for our MQSA-mandated internal audit of mammography outcomes. Cancer Analysis For all cancers diagnosed in the two patient cohorts, we recorded the screening and recall dates, Fig. 1 Of 77,833 studies, there were 23,149 studies in 3D digital breast tomosynthesis (DBT) cohort and 54,684 in 2D digital mammography (DM) cohort. Only data for 14 radiologists who had interpreted more than 500 3D DBT during study period were included, leaving 59,617 studies in two patient cohorts for comparative analysis. biopsy dates with pathology results, and number of additional mammographic views for recall examinations. Biopsy and final surgical pathology results were recorded for cancer cases. Surgical biopsy results for patients with initial diagnoses of atypia or other high-risk lesions based on needle biopsy were obtained whenever possible to determine upgrades to cancer diagnoses. If breast MRI or ultrasound were performed for further workup of patients with abnormal screening mammography findings, then the MRI or ultrasound findings resulting in cancer diagnoses were included in the CDRs. Cancers diagnosed more than 120 days after screening mammography were excluded from the screening-detected cancer analysis. Clinical Performance Metrics Key clinical outcomes measures of recall rates from screening mammography, overall CDR (number of cancers per 1000 and CDR for invasive cancer and in situ cancer detection, positive predictive value from screening (PPV1), positive predictive value for biopsy after BI-RADS category 4 or 5 assessment (PPV3), and overall and noncancer biopsy rates (number of biopsies performed per 1000 were calculated for the aggregate 2D DM and 3D DBT patient cohorts for radiologists who read more than 500 3D DBT screening examinations. Positive predictive values are expressed as percentages. The recall rate was calculated as the percentage of screening patients for whom additional imaging was requested (BI-RADS category 0 assessment). Technical recalls were included in the study but were not calculated in the radiologists recall rates. For patients with multiple cancers, the most severe lesion was chosen from the patient s record (e.g., invasive cancer took precedence over in situ cancer) and that patient was counted only once in the CDR. Lesions upgraded to cancers from initial pathology findings of atypia or high-risk lesion were included in the CDR and positive predictive value calculations. Statistical Analysis Statistical software (SAS, version 9.3, SAS Institute) was used to analyze differences between 2D DM and 3D DBT patient cohorts for each of the outcome measures. The Fisher exact test and a generalized linear mixed model were used for all analyses except patient age to determine statistical significance. The Wilcoxon rank sum test was used for patient age. A p value of < 0.05 was considered significant, and all tests were two-sided. For the generalized linear mixed model, the reading radiologist was assumed to be random. Proportions from each group and their differences after factoring in random radiologist effects were taken into account for analyses of outcomes measures (PROC Glimmix procedure, SAS Institute) used to assess differences between 2D DM and 3D DBT cohorts. Results Clinical performance measures comparing 3D DBT with 2D DM are summarized in Table 1. Recall From Screening Of the 38,674 patients screened with 2D DM, 6247 were recalled for additional imaging, whereas 2845 of 20,943 patients screened with 3D DBT were recalled. The recall rate for 2D DM was 16.2% and for 3D DBT, 13.6%. The difference in recall rates is a statistically significant relative reduction of 16.1% or an absolute reduction of 2.6% for screening with 3D DBT versus screening with 2D DM alone (p < ). The generalized linear mixed model also shows a significant recall reduction (estimate, 13.60%; p < ). Biopsy Rates Eight hundred thirty-five biopsies were performed in the 2D DM cohort compared with 551 biopsies in the 3D DBT cohort (Table 1). The overall biopsy rate per 1000 patients screened was significantly higher for the 3D DBT cohort (26.3/1000, p = ) compared with 2D DM (21.6/1000) cohort. The generalized linear mixed model estimated increase in biopsy rate was 20.39% (p = ). The noncancer biopsy rate was also greater (p = 0.003) for 3D DBT (20.1/1000) compared with 2D DM (16.7/1000). Cancer Detection Rates and Positive Predictive Values The 835 biopsies resulted in 190 patients diagnosed with cancer in the 2D DM cohort (Table 1). In the 3D DBT co- AJR:203, September
4 hort, the 551 biopsies resulted in 131 patients diagnosed with cancer. The CDR for 2D DM alone was 4.9/1000 and for 3D DBT, 6.3/1000. This difference in CDR is a statistically significant 28.6% relative increase in CDR for patients screened with 3D DBT (p = 0.035). The generalized linear mixed model estimated increase was 27.11% (p = 0.041). There was a large significant (p = ) difference in the PPV1 for 3D DBT (4.6%) compared with 2D DM (3.0%) screening. This difference constitutes a 53.3% relative increase in PPV1 for an abnormal finding on 3D DBT screening mammography compared with 2D DM screening. The generalized linear mixed model estimated PPV1 increase was 51.14% (p = ). Thus, the likelihood that an abnormal screening examination will result in a cancer diagnosis was greater for the women screened with 3D DBT than for those screened with 2D DM. The PPV3 was similar for the two groups: 23.8% for 3D DBT and 22.8% for 2D DM, with no significant difference (p = 0.696) by the Fisher exact test and by the generalized linear mixed model analysis (p = 0.662). Patient Characteristics The differences between the 2D DM and 3D DBT groups are shown in Table 2. There was no significant difference in age between the 2D DM and 3D DBT cohorts. Mean age was 59.5 and 59.6 years for the 2D DM and 3D DBT groups, respectively (p = 0.695). There was no difference in the number of patients with multiple breast cancers (p = 0.39). In both groups, 12 patients had multiple breast cancers diagnosed. A comparison of the distributions of breast density between the two groups showed no significant differences (p = 0.081). Likewise, between the two cancer cohorts, there were no significant differences regarding family history of breast cancer (p = 0.899), history of hormone use (p = 0.221), or if the screening study was a baseline study or a subsequent study (p = 1.000). Number of Mammographic Views for Recall An analysis of the frequency distributions for the number of additional views obtained at recall (Table 2) shows fewer additional mammographic views were obtained for women diagnosed with breast cancer who underwent 3D DBT as compared with 2D DM screening (p < 0.001). For screening recalls resulting in cancer diagnoses, Greenberg et al. TABLE 2: Patient Characteristics for Cancers Diagnosed by 2D Digital Mammography (DM) Versus 3D Digital Breast Tomosynthesis (DBT) Screening Characteristic 2D DM 3D DBT p a 74.1% of 3D DBT patients underwent two or fewer mammographic views versus 51.0% of 2D DM patients. Additionally, 35.1% of patients in the 3D DBT group required no additional mammographic views versus 6.3% in the 2D DM group. 95% CI of Difference Between 2D DM and 3D DBT b No. of patients with cancer detected Age of patients with cancer detected (y) to 2.34 Mean (SD) 59.5 (11.44) 59.6 (10.31) Median Minimum Maximum BI-RADS breast density category, no. (%) of patients 1 7 (3.7) 2 (1.5) 1.25 to (37.4) 48 (36.6) 10.0 to (53.7) 80 (61.1) 18.3 to (5.3) 1 (0.8) No. of additional mammographic views, no. < (%) of patients 0 12 (6.3) 46 (35.1) 37.7 to (2.6) 6 (4.6) 6.19 to (42.1) 45 (34.4) 2.99 to (30.5) 20 (15.3) (12.1) 11 (8.4) 2.93 to (5.8) 3 (2.3) 0.69 to (0.5) 0 (0.0) 0.50 to 1.56 No. (%) of patients with multiple 12 (6.3) 12 (9.2) to 3.19 breast cancers Family history of breast cancers c, no. (%) to 9.27 of patients Yes 51 (26.8) 36 (27.5) No 139 (73.2) 95 (72.5) History of hormone therapy c, no. (%) to 3.70 of patients Yes 54 (28.4) 46 (35.1) No 136 (71.6) 85 (64.9) Baseline screening c, no. (%) of patients to 3.09 Yes 5 (2.6) 3 (2.3) No 185 (97.4) 128 (97.7) Note All data are for radiologists with experience reading more than 500 3D DBT examinations. a The Wilcoxon rank sum test was used for age, and Fisher exact tests were used for all other categoric variables. b The difference was calculated as 2D DM 3D DBT. A 95% CI of the difference of the means was calculated for age. c The 95% CIs were calculated for the difference between groups in the percentages of Yes responses. Screening-Detected Cancers Table 3 shows the grade and histologic type of the screening-detected cancers for the two patient cohorts. Multiple cancers were treated independently in this analysis. There were no significant differences in the 690 AJR:203, September 2014
5 Breast Cancer Screening Using 3D DBT Versus 2D DM distributions of cancer grade (grade 1, 2, or 3) for invasive cancers detected by 3D DBT versus 2D DM (p = 0.607). More low- and intermediate-grade in situ cancers were detected by 3D DBT screening (p = 0.045; 95% CI, 39.7 to 2.06). More high-grade in situ cancers were detected in our 2D DM cohort (p = 0.045; 95% CI, ). There were no significant differences in the types (ductal, lobular, or other) of cancers detected by 3D DBT versus 2D DM (p = 0.255). Table 4 shows the CDR subanalysis (tabulated by number of patients) for in situ and invasive cancers. The CDR for invasive cancer was significantly higher (p = 0.006) by 43.8% for patients screened with 3D DBT (4.6/1000) compared with 2D DM (3.2/1000) alone. There was no significant difference (p = 0.753) between the CDR for in situ cancer for 3D DBT (1.6/1000) compared with that of 2D DM (1.7/1000). Discussion Implications for Patient Care Although not the first study of screening outcomes in community-based practice [11] in the United States comparing 2D DM with 3D DBT, ours is the largest report (59,617 patients) to date. Because most American women undergo mammography screening in the community radiology setting, our results may be a bellwether for the impact of tomosynthesis on population-based breast cancer screening. With a 16.1% reduction in recall rate from screening, a 53.3% increase in PPV1 from an abnormal screening examination, a 28.6% increase in the CDR for cancer overall, and a 43.8% increase in the CDR for invasive cancer, standard performance metrics for screening outcomes show the superiority of 3D DBT over 2D DM. The reduction in screening recall rate combined with increased detection of invasive but not in situ cancer is strong evidence that effective screening with 3D DBT may be achieved with significant performance improvement. Our results show that screening with 3D DBT is efficacious and has practical implications for patient care. A decreased probability of recall from screening, a higher rate of cancer detection, and a greater likelihood that fewer mammographic views will be needed to diagnose malignant lesions will significantly influence everyday practice. We report a significant 16.1% lower recall rate for 3D DBT compared with 2D DM for population-based screening in our community practice, which is exactly the setting TABLE 3: Type and Grade of Cancers Diagnosed at 2D Digital Mammography (DM) Versus 3D Digital Breast Tomosynthesis (DBT) Screening Cancer Type or Grade 2D DM 3D DBT p a in which most women in the United States undergo screening. Prior observer performance studies [4, 7, 13] reported 30 40% potential reductions in recall rate. Haas et al. [10] similarly showed an almost 30% reduction in recall rate in their retrospective population-based study in academic practice. In community practice, with a smaller sample size (23,355 ) than ours, Rose et al. [11] reported a 36.8% reduction in recall rate in a subgroup of radiologists who had read more than 500 tomosynthesis studies. Results from our community-based practice are more concordant with the 15% recall reduction reported by Skaane et al. [8] in the Oslo population-based screening program. 95% CI of Difference Between 2D DM and 3D DBT b No. of cancers c Type of cancer, no. (%) of cancers Invasive 126 (62.1) 106 (73.6) 21.4 to 1.73 In situ 75 (36.9) 37 (25.7) Other 2 (1.0) 1 (0.7) Grade of cancers, no. (%) of cancers Invasive d T1 microinvasion 4 (3.2) 2 (1.9) 2.72 to 5.30 Grade 1 20 (15.9) 24 (22.6) 17.0 to 3.44 Grade 2 78 (61.9) 61 (57.5) 8.31 to Grade 3 22 (17.5) 19 (17.9) 10.3 to 9.40 Unknown 2 (1.6) 0 (0.0) In situ Low 3 (4.0) 5 (13.5) 21.4 to 2.36 Intermediate 32 (42.7) 20 (54.1) 31.0 to 8.19 High 40 (53.3) 12 (32.4) Unknown 0 (0.0) 0 (0.0) In situ Low or intermediate 35 (46.7) 25 (67.6) 39.7 to 2.06 High 40 (53.3) 12 (32.4) Type of invasive cancers Ductal 107 (84.9) 82 (77.4) 2.56 to Lobular 16 (12.7) 18 (17.0) 13.5 to 4.93 Other 3 (2.4) 6 (5.7) Note All data are for radiologists with experience reading more than 500 3D DBT examinations. a Fisher exact test. b The difference was calculated as 2D DM 3D DBT. A 95% CI was calculated for the difference between the groups in the percentages of responses at each level. c Includes patients with multiple cancers, thus totals will vary from total patient numbers in Table 1. d For cancer grades, unknowns were not included in the analysis for significance. We observed a significant increase in the CDR for cancer overall (28.6%) and, most importantly, a 43.8% increase in the CDR for invasive cancer for patients screened with 3D DBT versus 2D DM. These detection benefits were achieved with no significant increase in the CDR for in situ cancer for 3D DBT compared with 2D DM (1.6/1000 and 1.7/1000, respectively). Our CDRs for 3D DBT are comparable to those reported by Rose et al. [11] and Skaane et al. [8] but differ from the lesser, nonsignificant increase in CDR of 9.5% reported by Haas et al. [10] in an academic setting. Thus, a reduction in screening recalls can be achieved along with an increase in the detection of invasive, but not in situ, cancer. These results imply that effective AJR:203, September
6 Greenberg et al. TABLE 4: Cancer Detection Rates (CDRs) for In Situ and Invasive Cancers Characteristic 2D DM 3D DBT p a No. of screening examinations No. of patients with in situ cancer CDR for in situ cancers (no. of cancers per 1000 No. of patients with invasive cancer CDR for invasive cancers (no. of cancers per ,674 20, population-based screening with 3D DBT in community radiology practice is feasible without contributing to false-positive recalls or increasing the detection of clinically insignificant noninvasive cancers. Relative ( 45.8 to 34.08) ( ) 3D DBT 2D DM Absolute 0.01 ( 0.08 to 0.06) 0.14 ( ) 2D DM 1.7 ( ) 3.2 ( ) Strengths and Limitations In our study, the relative increase in PPV1 with 3D DBT (53.3%) indicates that the likelihood of an abnormal screening examination resulting in a cancer diagnosis is much greater for women screened by 3D DBT. The superior CDR for 3D DBT compared with 2D DM also illustrates the improved efficacy of screening with 3D DBT. However, our results also showed that once biopsy was recommended, there was the same likelihood of a positive result for women who underwent 2D DM as for those who underwent 3D DBT. The PPV1 and CDR results are in accord with the greater sensitivity and accuracy of 3D DBT reported in a reader performance study by Rafferty et al. [7]. However, the higher biopsy rate may be a prevalence effect from the utilization of new technology for first-round screening. Nevertheless, the accrued advantages for patients screened with 3D DBT in community radiology practice include a decreased probability of recall from screening and a higher rate of cancer detection, particularly for invasive cancers. It is noteworthy that fewer additional mammographic views were obtained at recall examination for patients with cancer diagnoses after 3D DBT versus 2D DM screening. A remarkable 35.1% of 3D DBT patients with cancer diagnoses had no additional mammographic views performed at recall. This finding suggests that recall from 3D DBT screening may result in a more efficient recall assessment compared with 2D DM. Larger studies are needed to assess the recall efficiency for all patients who undergo 3D DBT compared with 2D DM. The limitations of our study include the retrospective and nonrandomized design that could introduce selection bias, particularly with regard to the $50 fee charged for 3D DBT. However patients who could not afford 3D DBT were not charged. For a variety of reasons (see Study Design and Participants section), 11.8% of 3D DBT examinations were performed without charge. Additionally, if patients with known risk factors for developing breast cancer self-selected 3D DBT screening, then this could have contributed to a higher PPV1 and CDR in this cohort. However, analyses of patient age, breast density, family history, number of patients with multiple breast cancers, history of hormone use, and baseline screening status showed no significant differences between the 2D DM and 3D DBT cancer cohorts. As a result, we believe neither these risk factors nor the $50 fee introduced clinically relevant selection bias. Furthermore, these factors and fee are unlikely to account for the large differences in outcome performance metrics between the two cohorts. Generalized Linear Mixed Model b 3D DBT 1.6 ( ) 4.6 ( ) The sequential inclusion of office sites as they acquired DBT in our tristate practice could have introduced systematic bias; however, we believe that this possibility is unlikely given the diverse urban-suburban population we serve across these locales. The lack of comparison with performance metrics for 2D DM outcomes in the period preceding introduction of 3D DBT may also limit our study. Recall rates may have changed spuriously because of the novelty or uncertainty of new technology. We believe that learning curve effects were minimized by the analysis of screening data for only experienced radiologists who had interpreted more than 500 3D DBT. We report recall rates of 16.2% for 2D DM and of 13.6% for 3D DBT. The ceiling for recommended recall rate is no greater than 14% [14]. Our 2D DM recall rate is higher than 14%, and the 3D DBT recall rate is just below that benchmark. One recent report showed that approximately 30% of 52 facilities had recall rates that failed to comply with recommended benchmarks and that most had values above the benchmark range [14]. Although we acknowledge that our recall rate for 2D DM was high, we believe that 3D DBT is helping us to achieve more desirable recall rates. Future Directions A detailed analysis of the characteristics of cancers detected by DBT is a subject for future research, including evaluation of lesion size, descriptive imaging characteristics of p Change (%) ( 40.5 to 41.30) ( ) Note All data are for radiologists with experience reading more than 500 3D DBT examinations. Values in parentheses are 95% CIs. a Fisher exact text. b For each of the outcome measures, a generalized linear mixed model (PROC Glimmix procedure [SAS software, version 9.3, SAS Institute]) was used to analyze the difference between 2D DM and 3D DBT. The link function was specified as LOGIT. The correlation between reads made by the same radiologists was accounted for by specifying radiologist as the G-side random effect. The adjusted rates were calculated using the fitted model and their 95% CIs were derived using the delta method. 692 AJR:203, September 2014
7 Breast Cancer Screening Using 3D DBT Versus 2D DM malignant lesions, and TNM pathology staging. Also, analyses stratified by patient age and breast density may yield useful information concerning which patient subgroups will benefit most from 3D DBT screening. Although the effect of repeat screening with 3D DBT (incidence effect) is unknown, future investigations will determine whether interval CDRs are lower for subsequent screening rounds with 3D DBT than what we have reported. Our PPV3 (for biopsy) values were essentially the same for the 2D DM and 3D DBT cohorts. Surprisingly, both overall and noncancer biopsy rates were higher in the 3D DBT group. The paradox of a higher PPV1, an equivalent PPV3, and a higher biopsy rate for 3D DBT may be because first-round screening with tomosynthesis may facilitate detection not only of small or obscured cancers but also of small or obscured benign or high-risk lesions such as isodense fibroadenomas or distortions due to radial scars. Detection of these benign lesions at the outset of a 3D DBT screening program may yield an initially lower positive predictive value for biopsy after screening than would be expected given the higher positive predictive value for screening recall; no similar results have been reported previously to date. Whether 3D DBT yields more diagnoses of atypia or other high-risk or nonobligate precursor lesions, such as radial scars, will be the subject of future investigation. Conclusion Three-dimensional DBT showed significantly improved performance metrics for breast cancer screening when compared with 2D DM in community radiology practice. Population-based screening with 3D DBT results in the detection of more breast cancers, especially invasive cancers, and reduces the recall rate from screening. Acknowledgments We thank Mary McCarthy, RN, for assistance with data collection, Donna Titzer for administrative assistance, and Kathleen Willison for logistical help. References 1. Rosenberg RD, Hunt W, Williamson MR, et al. Effects of age, breast density, ethnicity, and estrogen replacement therapy on screening mammographic sensitivity and stage at diagnosis: review of 183,134 screening mammograms in Albuquerque, New Mexico. Radiology 1998; 209: Pisano ED, Acharyya S, Cole EB, et al. Cancer cases from ACRIN Digital Mammographic Imaging Screening Trial: radiologist analysis with use of a logistic regression model. Radiology 2009; 252: U.S. Food and Drug Administration website. Summary of safety and effectiveness data of Selenia Dimensions 3D System. cdrh_docs/pdf8/p080003b.pdf. Published February 11, Accessed January 29, Gur D, Abrams GG, Chough DM, et al. Digital breast tomosynthesis: observer performance study. AJR 2009; 193: Gennaro G, Toledano A, di Maggio C, et al. Digital breast tomosynthesis versus digital mammography: a clinical performance study. Eur Radiol 2010; 20: Wallis MG, Moa E, Zanca F, Leifland K, Danielsson M. Two-view and single-view tomosynthesis versus full-field digital mammography: high resolution x-ray imaging observer study. Radiology 2012; 262: Rafferty EA, Park JM, Philpotts LE, et al. Assessing radiologist performance using combined digital mammography and breast tomosynthesis compared with digital mammography alone: results of a multicenter, multireader trial. Radiology 2013; 266: Skaane P, Bandos AI, Gullien R, et al. Comparison of digital mammography alone and digital mammography plus tomosynthesis in a population-based screening program. Radiology 2013; 267: Ciatto S, Houssami N, Bernardi D, et al. Integration of 3D digital mammography with tomosynthesis for population breast-cancer screening (STORM): a prospective study. Lancet Oncol 2013; 14: Haas BM, Kaira V, Geisel J, Raghy M, Durand M, Philpotts LE. Comparison of tomosynthesis plus digital mammography and digital mammography alone for breast cancer screening. Radiology 2013; 269: Rose SL, Tidwell AL, Bujnoch LJ, Kushwaha AC, Nordmann AS, Sexton R. Implementation of breast tomosynthesis in a routine screening practice: an observational study. AJR 2013; 200: U.S. Food and Drug Administration website. Radiation-emitting products: MQSA facility certification extension requirements for digital breast tomosynthesis (DBT) system. Updated May 30, Accessed November 20, Poplack SP, Tosteson TD, Kogel CA, Nagy HM. Digital breast tomosynthesis: initial experience in 98 women with abnormal digital screening mammography. AJR 2007; 189: Rauscher GH, Murphy AM, Orsi JM, Dupuy DM, Grabler PM, Weldon CB. Beyond the Mammography Quality Standards Act: measuring the quality of breast cancer screening programs. AJR 2014; 202: AJR:203, September
Women s Imaging Original Research
 Women s Imaging Original Research Brandt et al. DBT for Screening Recalls Without Calcifications Women s Imaging Original Research FOCUS ON: Kathleen R. Brandt 1 Daniel A. Craig 1 Tanya L. Hoskins 2 Tara
Women s Imaging Original Research Brandt et al. DBT for Screening Recalls Without Calcifications Women s Imaging Original Research FOCUS ON: Kathleen R. Brandt 1 Daniel A. Craig 1 Tanya L. Hoskins 2 Tara
Implementation of Breast Tomosynthesis in a Routine Screening Practice: An Observational Study
 Women s Imaging Original Research Rose et al. Tomosynthesis in Routine Screening Women s Imaging Original Research Stephen L. Rose 1 Andra L. Tidwell Louis J. Bujnoch Anne C. Kushwaha Amy S. Nordmann Russell
Women s Imaging Original Research Rose et al. Tomosynthesis in Routine Screening Women s Imaging Original Research Stephen L. Rose 1 Andra L. Tidwell Louis J. Bujnoch Anne C. Kushwaha Amy S. Nordmann Russell
Financial Disclosures
 Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
Financial Disclosures 3D Mammography: The Latest Developments in the Breast Imaging Arena I have no financial disclosures Dr. Katharine Lampen-Sachar Breast and Body Radiologist Radiology Associates of
Comparison of Tomosynthesis Plus Digital Mammography and Digital Mammography Alone for Breast Cancer Screening 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer 3/10/16
 Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer Policy Number: MCP-270 Revision Date(s): Original Effective Date: 3/10/16 Review Date: 6/22/17, 3/8/18 MCPC Approval Date: 3/8/18 DISCLAIMER
Subject: Digital Breast Tomosynthesis (DBT) for Breast Cancer Policy Number: MCP-270 Revision Date(s): Original Effective Date: 3/10/16 Review Date: 6/22/17, 3/8/18 MCPC Approval Date: 3/8/18 DISCLAIMER
Breast cancer screening: Does tomosynthesis augment mammography?
 REVIEW TRACI A. TAKAHASHI, MD, MPH Director, Seattle VA Women Veterans Clinic at VA Puget Sound Health Care System, Seattle, WA; Associate Professor of Medicine, University of Washington, Seattle CHRISTOPH
REVIEW TRACI A. TAKAHASHI, MD, MPH Director, Seattle VA Women Veterans Clinic at VA Puget Sound Health Care System, Seattle, WA; Associate Professor of Medicine, University of Washington, Seattle CHRISTOPH
Recall and Cancer Detection Rates for Screening Mammography: Finding the Sweet Spot
 Women s Imaging Original Research Grabler et al. Optimal Recall and Cancer Detection Rates for Screening Mammography Women s Imaging Original Research Paula Grabler 1 Dominique Sighoko 2 Lilian Wang 3
Women s Imaging Original Research Grabler et al. Optimal Recall and Cancer Detection Rates for Screening Mammography Women s Imaging Original Research Paula Grabler 1 Dominique Sighoko 2 Lilian Wang 3
MRI of the Breast Positron Emission Tomography (PET) Scintimammography/Breast-Specific Gamma Imaging/Molecular Breast Imaging
 6.01.53 Digital Breast Tomosynthesis Section Radiology Subsection Effective Date September 30, 2014 Original Policy Date June 28, 2013 Next Review Date September 2015 Description Digital breast tomosynthesis
6.01.53 Digital Breast Tomosynthesis Section Radiology Subsection Effective Date September 30, 2014 Original Policy Date June 28, 2013 Next Review Date September 2015 Description Digital breast tomosynthesis
Breast Cancer Screening Using Tomosynthesis in Combination With Digital Mammography
 Research Original Investigation Breast Cancer Screening Using in Combination With Sarah M. Friedewald, MD; Elizabeth A. Rafferty, MD; Stephen L. Rose, MD; Melissa A. Durand, MD; Donna M. Plecha, MD; Julianne
Research Original Investigation Breast Cancer Screening Using in Combination With Sarah M. Friedewald, MD; Elizabeth A. Rafferty, MD; Stephen L. Rose, MD; Melissa A. Durand, MD; Donna M. Plecha, MD; Julianne
TOMOSYNTHESIS. Daniela Bernardi. U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy
 TOMOSYNTHESIS Daniela Bernardi U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy BACKGROUND early detection through screening MAMMOGRAPHY is associated with reduced breast cancer morbidity
TOMOSYNTHESIS Daniela Bernardi U.O. Senologia Clinica e Screening mammografico APSS Trento, Italy BACKGROUND early detection through screening MAMMOGRAPHY is associated with reduced breast cancer morbidity
Digital Breast Tomosynthesis
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Outline. Digital Breast Tomosynthesis: Update and Pearls for Implementation. Tomosynthesis Dataset: 2D/3D (Hologic Combo Acquisition)
 Outline Digital Breast Tomosynthesis (DBT) the new standard of care Digital Breast Tomosynthesis: Update and Pearls for Implementation Emily F. Conant, M.D. Professor, Chief of Breast Imaging Department
Outline Digital Breast Tomosynthesis (DBT) the new standard of care Digital Breast Tomosynthesis: Update and Pearls for Implementation Emily F. Conant, M.D. Professor, Chief of Breast Imaging Department
Update of Digital Breast Tomosynthesis. Susan Orel Roth, MD
 Update of Digital Breast Tomosynthesis Susan Orel Roth, MD NCI estimates that : Why DBT? Approximately 20% of breast cancers are missed at mammography screening Average recall rates approximately 10%
Update of Digital Breast Tomosynthesis Susan Orel Roth, MD NCI estimates that : Why DBT? Approximately 20% of breast cancers are missed at mammography screening Average recall rates approximately 10%
Detection and Classification of Calcifications on Digital Breast Tomosynthesis and 2D Digital Mammography: A Comparison
 Women s Imaging Original Research Spangler et al. Digital Breast Tomosynthesis Versus 2D Digital Mammography Women s Imaging Original Research FOCUS ON: M. Lee Spangler 1 Margarita L. Zuley 2 Jules H.
Women s Imaging Original Research Spangler et al. Digital Breast Tomosynthesis Versus 2D Digital Mammography Women s Imaging Original Research FOCUS ON: M. Lee Spangler 1 Margarita L. Zuley 2 Jules H.
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Digital Breast Tomosynthesis Page 1 of 31 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Digital Breast Tomosynthesis Professional Institutional Original Effective
Digital Breast Tomosynthesis Page 1 of 31 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Digital Breast Tomosynthesis Professional Institutional Original Effective
BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography
 BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography Poster No.: C-0562 Congress: ECR 2017 Type: Scientific Exhibit Authors:
BI-RADS classification in breast tomosynthesis. Our experience in breast cancer cases categorized as BI-RADS 0 in digital mammography Poster No.: C-0562 Congress: ECR 2017 Type: Scientific Exhibit Authors:
Jing Zhang, PhD, Lars J. Grimm, MD, MHS, Joseph Y. Lo, PhD, Karen S. Johnson, MD,
 This manuscript has been accepted for publication in Journal of the American College of Radiology. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published
This manuscript has been accepted for publication in Journal of the American College of Radiology. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published
Since its introduction in 2000, digital mammography has become
 Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
Review Article Smith A, PhD email : Andrew.smith@hologic.com Since its introduction in 2000, digital mammography has become an accepted standard of care in breast cancer screening and has paved the way
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: digital_breast_tomosynthesis 3/2011 6/2016 6/2017 11/2016 Description of Procedure or Service Conventional
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: digital_breast_tomosynthesis 3/2011 6/2016 6/2017 11/2016 Description of Procedure or Service Conventional
A comparison of the accuracy of film-screen mammography, full-field digital mammography, and digital breast tomosynthesis
 Clinical Radiology xxx (2012) 1e6 Contents lists available at SciVerse ScienceDirect Clinical Radiology journal homepage: www.clinicalradiologyonline.net A comparison of the accuracy of film-screen mammography,
Clinical Radiology xxx (2012) 1e6 Contents lists available at SciVerse ScienceDirect Clinical Radiology journal homepage: www.clinicalradiologyonline.net A comparison of the accuracy of film-screen mammography,
Challenges to Delivery of High Quality Mammography
 Challenges to Delivery of High Quality Mammography Overview of Current Challenges Barbara Monsees, Washington University Geographic Access, Equity and Impact on Quality Tracy Onega, Dartmouth Medical School
Challenges to Delivery of High Quality Mammography Overview of Current Challenges Barbara Monsees, Washington University Geographic Access, Equity and Impact on Quality Tracy Onega, Dartmouth Medical School
ACR Appropriateness Criteria Breast Cancer Screening EVIDENCE TABLE. See Last Page for Key Revised 2017 Mainiero Page 1.
 1. Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin. 2017;67(1):7-0. Type Review/Other- N/A To estimate the numbers of new cancer cases and deaths that will occur in the United
1. Siegel RL, Miller KD, Jemal A. Cancer Statistics, 2017. CA Cancer J Clin. 2017;67(1):7-0. Type Review/Other- N/A To estimate the numbers of new cancer cases and deaths that will occur in the United
3D Mammography. The most exciting advancement in mammography in over 30 years
 What to Expect 3D Mammography The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense against breast
What to Expect 3D Mammography The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense against breast
Digital Breast Tomosynthesis in the Diagnostic Environment: A Subjective Side-by-Side Review
 Women s Imaging Original Research Hakim et al. Digital Breast Tomosynthesis Women s Imaging Original Research Christiane M. Hakim 1 Denise M. Chough 1 Marie A. Ganott 1 Jules H. Sumkin 1 Margarita L. Zuley
Women s Imaging Original Research Hakim et al. Digital Breast Tomosynthesis Women s Imaging Original Research Christiane M. Hakim 1 Denise M. Chough 1 Marie A. Ganott 1 Jules H. Sumkin 1 Margarita L. Zuley
Corporate Medical Policy. Digital Breast Tomosynthesis (DBT)
 Corporate Medical Policy Digital Breast Tomosynthesis (DBT) Description of Procedure or Service DBT is a three-dimensional (3D) breast imaging technology that uses a rotating X-ray source to acquire multiple
Corporate Medical Policy Digital Breast Tomosynthesis (DBT) Description of Procedure or Service DBT is a three-dimensional (3D) breast imaging technology that uses a rotating X-ray source to acquire multiple
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
the one name in cancer care.
 the one name in cancer care. Landmark study evaluating close to half a million mammography exams published in the Journal of the American Medical Association (JAMA) 1 Hologic 3D Mammography Significantly
the one name in cancer care. Landmark study evaluating close to half a million mammography exams published in the Journal of the American Medical Association (JAMA) 1 Hologic 3D Mammography Significantly
TOMOSYNTHESIS: WORTH ALL THE HYPE?
 X-Ray Associates of New Mexico, P.C. TOMOSYNTHESIS: WORTH ALL THE HYPE? MICHAEL N. LINVER, MD, FACR MAMMOGRAPHY: THE GOOD, THE PRETTY GOOD, & THE NOT SO GOOD MAMMOGRAPHY: THE GOOD, THE PRETTY GOOD, & THE
X-Ray Associates of New Mexico, P.C. TOMOSYNTHESIS: WORTH ALL THE HYPE? MICHAEL N. LINVER, MD, FACR MAMMOGRAPHY: THE GOOD, THE PRETTY GOOD, & THE NOT SO GOOD MAMMOGRAPHY: THE GOOD, THE PRETTY GOOD, & THE
#46: DIGITAL TOMOSYNTHESIS: What is the Data Really Showing? TERMS (AKA) WHAT IS TOMOSYNTHESIS? 3/3/2014. Digital breast tomosynthesis =
 #46: DIGITAL TOMOSYNTHESIS: What is the Data Really Showing? January K. Lopez, MD Hoag Breast Care Center Newport Beach, CA Disclosures: None TERMS (AKA) Digital breast tomosynthesis = DBT Tomo 3D Full
#46: DIGITAL TOMOSYNTHESIS: What is the Data Really Showing? January K. Lopez, MD Hoag Breast Care Center Newport Beach, CA Disclosures: None TERMS (AKA) Digital breast tomosynthesis = DBT Tomo 3D Full
TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy
 TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy DATE: 26 September 2013 CONTEXT AND POLICY ISSUES Breast cancer is the second leading
TITLE: Digital Tomosynthesis for the Screening and Diagnosis of Breast Cancer: A Review of the Diagnostic Accuracy DATE: 26 September 2013 CONTEXT AND POLICY ISSUES Breast cancer is the second leading
Tomosynthesis and breast imaging update. Dr Michael J Michell Consultant Radiologist King's College Hospital NHS Foundation Trust
 Tomosynthesis and breast imaging update Dr Michael J Michell Consultant Radiologist King's College Hospital NHS Foundation Trust Breast imaging new technology BREAST CANCER FLT PET shows different grades
Tomosynthesis and breast imaging update Dr Michael J Michell Consultant Radiologist King's College Hospital NHS Foundation Trust Breast imaging new technology BREAST CANCER FLT PET shows different grades
WHAT TO EXPECT. Genius 3D MAMMOGRAPHY Exam. The most exciting advancement in mammography in over 30 years
 WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
Breast Tomosynthesis
 Breast Tomosynthesis The Use of Breast Tomosynthesis in a Clinical Setting 2 What s Inside Introduction... 1 Initial Hologic Clinical Trial Purpose and Methodology... 1 Clinical Trial Results... 2 Improved
Breast Tomosynthesis The Use of Breast Tomosynthesis in a Clinical Setting 2 What s Inside Introduction... 1 Initial Hologic Clinical Trial Purpose and Methodology... 1 Clinical Trial Results... 2 Improved
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Current Status of Supplementary Screening With Breast Ultrasound
 Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
2018 PUBLIC REPORTING OF OUTCOMES
 2018 PUBLIC REPORTING OF OUTCOMES The Cancer Committee at Western Maryland Health System s Schwab Family Cancer Center reports annually on program and patient outcomes in compliance with the accreditation
2018 PUBLIC REPORTING OF OUTCOMES The Cancer Committee at Western Maryland Health System s Schwab Family Cancer Center reports annually on program and patient outcomes in compliance with the accreditation
Digital Breast Tomosynthesis
 Digital Breast Tomosynthesis Policy Number: Original Effective Date: MM.05.012 06/28/2013 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 06/28/2013 Section: Radiology Place(s) of Service:
Digital Breast Tomosynthesis Policy Number: Original Effective Date: MM.05.012 06/28/2013 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 06/28/2013 Section: Radiology Place(s) of Service:
Breast Tomosynthesis
 Breast Tomosynthesis The Use of Breast Tomosynthesis in a Clinical Setting 2 What s Inside Introduction... 1 Initial Hologic Clinical Trial Purpose and Methodology... 1 Clinical Trial Results... 2 Improved
Breast Tomosynthesis The Use of Breast Tomosynthesis in a Clinical Setting 2 What s Inside Introduction... 1 Initial Hologic Clinical Trial Purpose and Methodology... 1 Clinical Trial Results... 2 Improved
Additional US or DBT after digital mammography: which one is the best combination?
 Additional US or DBT after digital mammography: which one is the best combination? Poster No.: B-0926 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Elizalde, P. Garcia Barquin, M.
Additional US or DBT after digital mammography: which one is the best combination? Poster No.: B-0926 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Paper A. Elizalde, P. Garcia Barquin, M.
Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features.
 Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features. Poster No.: C-1707 Congress: ECR 2015 Type: Scientific Exhibit Authors: V. Vinci 1, A. Iqbal
Digital breast tomosynthesis (DBT) occult breast cancers: clinical, radiological and histopathological features. Poster No.: C-1707 Congress: ECR 2015 Type: Scientific Exhibit Authors: V. Vinci 1, A. Iqbal
The Radiology Aspects
 REQUIREMENTS FOR INTERNATIONAL ACCREDITATION OF BREAST CENTERS/UNITS The Radiology Aspects Miri Sklair-Levy, Israel RADIOLOGY GUIDELINES FOR QUALITY ASSURANCE IN BREAST CANCER SCREENING AND DIAGNOSIS Radiologists
REQUIREMENTS FOR INTERNATIONAL ACCREDITATION OF BREAST CENTERS/UNITS The Radiology Aspects Miri Sklair-Levy, Israel RADIOLOGY GUIDELINES FOR QUALITY ASSURANCE IN BREAST CANCER SCREENING AND DIAGNOSIS Radiologists
WHAT TO EXPECT. Genius 3D Mammography Exam. The most exciting advancement in mammography in over 30 years
 WHAT TO EXPECT Genius 3D Mammography Exam The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense
WHAT TO EXPECT Genius 3D Mammography Exam The most exciting advancement in mammography in over 30 years Screening for breast cancer Doctors and scientists agree that early detection is the best defense
Screening Options in Dense Breasts. Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging
 Screening Options in Dense Breasts Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging Dense Breasted Women Decreased sensitivity of mammography
Screening Options in Dense Breasts Donna Plecha, M.D. Co-Director UHCMC Breast Centers Associate Professor of Radiology Director of Breast Imaging Dense Breasted Women Decreased sensitivity of mammography
Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in Patients with Dense Breasts
 Original Article Breast Imaging eissn 2005-8330 Korean J Radiol 2019;20(1):58-68 Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in
Original Article Breast Imaging eissn 2005-8330 Korean J Radiol 2019;20(1):58-68 Factors Affecting Breast Cancer Detectability on Digital Breast Tomosynthesis and Two-Dimensional Digital Mammography in
Dense Breasts, Get Educated
 Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Dense Breasts, Get Educated What are Dense Breasts? The normal appearances to breasts, both visually and on mammography, varies greatly. On mammography, one of the important ways breasts differ is breast
Purpose: Materials and Methods: Results: Conclusion: Original Research n Breast Imaging
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Correlation between lesion type and the additional value of digital breast tomosynthesis
 Correlation between lesion type and the additional value of digital breast tomosynthesis Poster No.: C-1604 Congress: ECR 2011 Type: Scientific Exhibit Authors: C. Van Ongeval, L. Cockmartin, A. Van Steen,
Correlation between lesion type and the additional value of digital breast tomosynthesis Poster No.: C-1604 Congress: ECR 2011 Type: Scientific Exhibit Authors: C. Van Ongeval, L. Cockmartin, A. Van Steen,
Innovations in decreasing recall rates for screening mammography
 Tomosynthesis & Screening Moderators: Dr. Stephen A. Feig, Dr. Linda J. Warren Saturday, April 9, 1:30-2:30 p.m. Room: Brazos Innovations in decreasing recall rates for screening mammography CLINICAL RELEVANCE:
Tomosynthesis & Screening Moderators: Dr. Stephen A. Feig, Dr. Linda J. Warren Saturday, April 9, 1:30-2:30 p.m. Room: Brazos Innovations in decreasing recall rates for screening mammography CLINICAL RELEVANCE:
The power and promise of breast tomosynthesis is here. Selenia Dimensions system with Acquisition Workstation 5000
 WOMEN S HEALTH BREAST SOLUTIONS HEALTH The power and promise of breast tomosynthesis is here Selenia Dimensions system with Acquisition Workstation 5000 3D mammography: A new dimension in early breast
WOMEN S HEALTH BREAST SOLUTIONS HEALTH The power and promise of breast tomosynthesis is here Selenia Dimensions system with Acquisition Workstation 5000 3D mammography: A new dimension in early breast
FDA Executive Summary
 Meeting of the Radiological Devices Advisory Panel On October 24, 22, the panel will discuss, make recommendations, and vote on a premarket approval application supplement (P83/S) to expand the indications
Meeting of the Radiological Devices Advisory Panel On October 24, 22, the panel will discuss, make recommendations, and vote on a premarket approval application supplement (P83/S) to expand the indications
What s New in Breast Imaging. Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia
 What s New in Breast Imaging Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia Disclosure Hologic, Inc. Shareholder and research agreement. Volpara Solutions, Ltd. Shareholder
What s New in Breast Imaging Jennifer A. Harvey, M.D., FACR Professor of Radiology University of Virginia Disclosure Hologic, Inc. Shareholder and research agreement. Volpara Solutions, Ltd. Shareholder
Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at Digital Breast Tomosynthesis Screening 1
 Breast Imaging 1954 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at
Breast Imaging 1954 This copy is for personal use only. To order printed copies, contact reprints@rsna.org Strategies to Increase Cancer Detection: Review of True-Positive and False-Negative Results at
WOMEN S HEALTH SOLUTIONS. The power and promise of breast tomosynthesis is here. Selenia Dimensions system with Acquisition Workstation 8000
 WOMEN S HEALTH SOLUTIONS The power and promise of breast tomosynthesis is here Selenia Dimensions system with Acquisition Workstation 8000 3D mammography: A new dimension in early breast cancer detection
WOMEN S HEALTH SOLUTIONS The power and promise of breast tomosynthesis is here Selenia Dimensions system with Acquisition Workstation 8000 3D mammography: A new dimension in early breast cancer detection
Electrical impedance scanning of the breast is considered investigational and is not covered.
 ARBenefits Approval: 09/28/2011 Effective Date: 01/01/2012 Revision Date: Code(s): Medical Policy Title: Electrical Impedance Scanning of the Breast Document: ARB0127 Administered by: Public Statement:
ARBenefits Approval: 09/28/2011 Effective Date: 01/01/2012 Revision Date: Code(s): Medical Policy Title: Electrical Impedance Scanning of the Breast Document: ARB0127 Administered by: Public Statement:
CURRENTLY FDA APPROVED ARE FULL FIELD DIGITAL MAMMOGRAPHY SYSTEMS AND FILM SCREEN STILL BEING USED AT SOME INSTITUTIONS
 ABBY DUROJAYE,M.D CURRENTLY FDA APPROVED ARE FULL FIELD DIGITAL MAMMOGRAPHY SYSTEMS AND FILM SCREEN STILL BEING USED AT SOME INSTITUTIONS BOTH HAVE BEEN SHOWN TO BE EFFECTIVE TOOLS EARLY DETECTION OF BREAST
ABBY DUROJAYE,M.D CURRENTLY FDA APPROVED ARE FULL FIELD DIGITAL MAMMOGRAPHY SYSTEMS AND FILM SCREEN STILL BEING USED AT SOME INSTITUTIONS BOTH HAVE BEEN SHOWN TO BE EFFECTIVE TOOLS EARLY DETECTION OF BREAST
Does the synthesised digital mammography (3D-DM) change the ACR density pattern?
 Does the synthesised digital mammography (3D-DM) change the ACR density pattern? Poster No.: B-0211 Congress: ECR 2015 Type: Scientific Paper Authors: P. MARTÍNEZ MIRAVETE, M. Millor Muruzábal, P. García-
Does the synthesised digital mammography (3D-DM) change the ACR density pattern? Poster No.: B-0211 Congress: ECR 2015 Type: Scientific Paper Authors: P. MARTÍNEZ MIRAVETE, M. Millor Muruzábal, P. García-
Digital Breast Tomosynthesis for Screening and Diagnostic Imaging. Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI
 Digital Breast Tomosynthesis for Screening and Diagnostic Imaging Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI Digital breast tomosynthesis (DBT), which was FDA approved in 2011, is rapidly
Digital Breast Tomosynthesis for Screening and Diagnostic Imaging Authors: Emily F. Conant, MD, FSBI; Liane Philpotts, MD, FSBI Digital breast tomosynthesis (DBT), which was FDA approved in 2011, is rapidly
Women s Imaging Original Research
 Women s Imaging Original Research Women s Imaging Original Research David Gur 1 Andriy I. Bandos 2 Howard E. Rockette 2 Margarita L. Zuley 3 Jules H. Sumkin 3 Denise M. Chough 3 Christiane M. Hakim 3 Gur
Women s Imaging Original Research Women s Imaging Original Research David Gur 1 Andriy I. Bandos 2 Howard E. Rockette 2 Margarita L. Zuley 3 Jules H. Sumkin 3 Denise M. Chough 3 Christiane M. Hakim 3 Gur
Policy Library Clinical Advantages of Digital Breast Tomosynthesis in Symptomatic Patients
 Policy Library Clinical Advantages of Digital Breast Tomosynthesis in Symptomatic Patients Version: 1 Approved by: Faculty of Clinical Radiology Council Date of approval: Click and type: day month and
Policy Library Clinical Advantages of Digital Breast Tomosynthesis in Symptomatic Patients Version: 1 Approved by: Faculty of Clinical Radiology Council Date of approval: Click and type: day month and
BREAST HEALTH SOLUTIONS. See what others miss.
 HMH 3D Mammography BREAST HEALTH SOLUTIONS See what others miss. 2 BREAST HEALTH SOLUTIONS Genius 3D MAMMOGRAPHY exams are clinically proven to detect 41% More invasive breast cancer, while simultaneously
HMH 3D Mammography BREAST HEALTH SOLUTIONS See what others miss. 2 BREAST HEALTH SOLUTIONS Genius 3D MAMMOGRAPHY exams are clinically proven to detect 41% More invasive breast cancer, while simultaneously
Women s Imaging Original Research
 Women s Imaging Original Research Waldherr et al. One-View Breast Tomosynthesis Versus Two-View Mammography Women s Imaging Original Research Christian Waldherr 1 Peter Cerny 1 Hans J. Altermatt 2 Gilles
Women s Imaging Original Research Waldherr et al. One-View Breast Tomosynthesis Versus Two-View Mammography Women s Imaging Original Research Christian Waldherr 1 Peter Cerny 1 Hans J. Altermatt 2 Gilles
WHAT TO EXPECT. Genius 3D MAMMOGRAPHY Exam. The most exciting advancement in mammography in over 30 years
 WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
WHAT TO EXPECT Genius 3D MAMMOGRAPHY Exam The most exciting advancement in mammography in over 30 years 91% of patients agree the quality of care provided by the facility was better with a Genius 3D MAMMOGRAPHY
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM)
 Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Fremtidens rolle for tomosyntese
 Dansk Radiologisk Selskab 9.årsmøde Odense 3.januar, 214 Fremtidens rolle for tomosyntese Professor dr. med. Per Skaane Oslo University Hospital Ullevaal Breast Imaging Center Oslo / Norway PERSKA@ous-hf.no
Dansk Radiologisk Selskab 9.årsmøde Odense 3.januar, 214 Fremtidens rolle for tomosyntese Professor dr. med. Per Skaane Oslo University Hospital Ullevaal Breast Imaging Center Oslo / Norway PERSKA@ous-hf.no
Bianca den Dekker, MD - PhD student. Prof dr R.M. Pijnappel Prof dr H.M. Verkooijen Dr M. Broeders
 Diagnostic value of Three-dimensional UltRasound in breast cancer screening participants referred with a BI-RADS 0 test result: a comparison of imaging strategies (TURBO) Bianca den Dekker, MD - PhD student
Diagnostic value of Three-dimensional UltRasound in breast cancer screening participants referred with a BI-RADS 0 test result: a comparison of imaging strategies (TURBO) Bianca den Dekker, MD - PhD student
Medical Audit of Diagnostic Mammography Examinations: Comparison with Screening Outcomes Obtained Concurrently
 Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
Breast Tomosynthesis
 Breast Tomosynthesis Considerations for Routine Clinical Use Breast Tomosynthesis Considerations for routine clinical use Andrew Smith, Ph.D., Vice President - Imaging Sciences, Hologic This white paper
Breast Tomosynthesis Considerations for Routine Clinical Use Breast Tomosynthesis Considerations for routine clinical use Andrew Smith, Ph.D., Vice President - Imaging Sciences, Hologic This white paper
Pitfalls and Limitations of Breast MRI. Susan Orel Roth, MD Professor of Radiology University of Pennsylvania
 Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
now a part of Electronic Mammography Exchange: Improving Patient Callback Rates
 now a part of Electronic Mammography Exchange: Improving Patient Callback Rates Overview This case study explores the impact of a mammography-specific electronic exchange network on patient callback rates
now a part of Electronic Mammography Exchange: Improving Patient Callback Rates Overview This case study explores the impact of a mammography-specific electronic exchange network on patient callback rates
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis
 Konica Minolta Healthcare Americas, Inc. Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis A WHITEPAPER INTRODUCTION Numerous published studies have shown
Konica Minolta Healthcare Americas, Inc. Exa Mammo A Solution that Overcomes the Challenges of Implementing Digital Breast Tomosynthesis A WHITEPAPER INTRODUCTION Numerous published studies have shown
TMIST: Frequently Asked Questions
 TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
Research Article The Adjunctive Digital Breast Tomosynthesis in Diagnosis of Breast Cancer
 BioMed Research International Volume 2013, Article ID 597253, 7 pages http://dx.doi.org/10.1155/2013/597253 Research Article The Adjunctive Digital Breast Tomosynthesis in Diagnosis of Breast Cancer Tsung-Lung
BioMed Research International Volume 2013, Article ID 597253, 7 pages http://dx.doi.org/10.1155/2013/597253 Research Article The Adjunctive Digital Breast Tomosynthesis in Diagnosis of Breast Cancer Tsung-Lung
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Supplemental Screening for Dense Breasts. Reagan Leverett, MD, MS
 Supplemental Screening for Dense Breasts Reagan Leverett, MD, MS Outline Anatomy and Density Risk of dense breasts Theory of Supplemental Screening Options for supplemental screening Tomosynthesis Ultrasound
Supplemental Screening for Dense Breasts Reagan Leverett, MD, MS Outline Anatomy and Density Risk of dense breasts Theory of Supplemental Screening Options for supplemental screening Tomosynthesis Ultrasound
Breast Cancer Screening and Diagnosis
 Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS
 Screening mammography scrmam_c BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS The radiologist s indication for exam is the primary determinant of whether a mammogram is screening or diagnostic.
Screening mammography scrmam_c BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS The radiologist s indication for exam is the primary determinant of whether a mammogram is screening or diagnostic.
Breast Tomosynthesis. What is breast tomosynthesis?
 Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Significance and Application of Digital Breast Tomosynthesis for the BI-RADS Classification of Breast Cancer
 DOI:http://dx.doi.org/10.7314/APJCP.2015.16.9.4109 Digital Breast Tomosynthesis for Breast Cancer Classification RESEARCH ARTICLE Significance and Application of Digital Breast Tomosynthesis for the BI-RADS
DOI:http://dx.doi.org/10.7314/APJCP.2015.16.9.4109 Digital Breast Tomosynthesis for Breast Cancer Classification RESEARCH ARTICLE Significance and Application of Digital Breast Tomosynthesis for the BI-RADS
Kish chakrabarti, Ph.D. Senior Physicist CDRH/FDA
 Facility Certification Extension Requirements, Quality Assurance and Medical Physicists role for Hologic Selenia Dimensions Digital Breast Tomosynthesis (DBT) System Kish chakrabarti, Ph.D. Senior Physicist
Facility Certification Extension Requirements, Quality Assurance and Medical Physicists role for Hologic Selenia Dimensions Digital Breast Tomosynthesis (DBT) System Kish chakrabarti, Ph.D. Senior Physicist
Supplemental Screening for Women with Dense Breast Tissue. Public Meeting December 13, 2013
 Supplemental Screening for Women with Dense Breast Tissue Public Meeting December 13, 2013 Agenda Meeting Convened 10am-10:15am Presentation of the Evidence and Voting Questions, Q&A 10:15am 11:15am Discussion
Supplemental Screening for Women with Dense Breast Tissue Public Meeting December 13, 2013 Agenda Meeting Convened 10am-10:15am Presentation of the Evidence and Voting Questions, Q&A 10:15am 11:15am Discussion
Nehmat Houssami 1, Kristina Lång 2, Solveig Hofvind 3, Sophia Zackrisson 2, Daniela Bernardi 4, Kylie Hunter 5, Lisa Askie 5, Per Skaane 6
 Study Protocol Effectiveness of digital breast tomosynthesis (3D-mammography) in population breast cancer screening: a protocol for a collaborative individual participant data (IPD) meta-analysis Nehmat
Study Protocol Effectiveness of digital breast tomosynthesis (3D-mammography) in population breast cancer screening: a protocol for a collaborative individual participant data (IPD) meta-analysis Nehmat
Proven clinical effectiveness at low radiation dose
 MicroDose Mammography Solutions Proven clinical effectiveness at low radiation dose Several studies provide evidence that Philips MicroDose Mammography* can provide outstanding image quality at 18% to
MicroDose Mammography Solutions Proven clinical effectiveness at low radiation dose Several studies provide evidence that Philips MicroDose Mammography* can provide outstanding image quality at 18% to
BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases?
 BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases? Poster No.: B-0966 Congress: ECR 2013 Type: Scientific Paper Authors: J. Etxano Cantera, I. Simon-Yarza, G.
BI-RADS 3 category, a pain in the neck for the radiologist which technique detects more cases? Poster No.: B-0966 Congress: ECR 2013 Type: Scientific Paper Authors: J. Etxano Cantera, I. Simon-Yarza, G.
BreastScreen Victoria tomosynthesis screening trial, Maroondah pilot: Preliminary Outcomes
 BreastScreen Victoria tomosynthesis screening trial, Maroondah pilot: Preliminary Outcomes Dr Darren Lockie, Director and Chief Radiologist, Maroondah BreastScreen, Eastern Health Ms Michelle Clemson,
BreastScreen Victoria tomosynthesis screening trial, Maroondah pilot: Preliminary Outcomes Dr Darren Lockie, Director and Chief Radiologist, Maroondah BreastScreen, Eastern Health Ms Michelle Clemson,
Improving Screening Mammography Outcomes Through Comparison With Multiple Prior Mammograms
 Women s Imaging Original Research Hayward et al. Comparing Screening Mammograms With Multiple Prior Mammograms Women s Imaging Original Research Jessica H. Hayward 1 Kimberly M. Ray 1 Dorota J. Wisner
Women s Imaging Original Research Hayward et al. Comparing Screening Mammograms With Multiple Prior Mammograms Women s Imaging Original Research Jessica H. Hayward 1 Kimberly M. Ray 1 Dorota J. Wisner
BI-RADS Categorization As a Predictor of Malignancy 1
 Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Blinded Comparison of Computer-Aided Detection with Human Second Reading in Screening Mammography
 CAD Versus Human for Second Reading in Screening Mammography Women s Imaging Original Research WOMEN S IMAGING Dianne Georgian-Smith 1 Richard H. Moore 2 Elkan Halpern 3 Eren D. Yeh 1 Elizabeth A. Rafferty
CAD Versus Human for Second Reading in Screening Mammography Women s Imaging Original Research WOMEN S IMAGING Dianne Georgian-Smith 1 Richard H. Moore 2 Elkan Halpern 3 Eren D. Yeh 1 Elizabeth A. Rafferty
Can Digital Breast Tomosynthesis(DBT) Perform Better than Standard Digital Mammography Workup in a Breast Cancer Assessment Clinic?
 Can Digital Breast Tomosynthesis(DBT) Perform Better than Standard Digital Mammography Workup in a Breast Cancer Assessment Clinic? Accepted for publication in European Radiology Authors: S Mall, J Noakes,
Can Digital Breast Tomosynthesis(DBT) Perform Better than Standard Digital Mammography Workup in a Breast Cancer Assessment Clinic? Accepted for publication in European Radiology Authors: S Mall, J Noakes,
Disclosures. Breast Cancer. Breast Imaging Modalities. Breast Cancer Screening. Breast Cancer 6/4/2014
 : Information for the Primary Care Physician Disclosures No financial relationships with commercial entities producing health care products/services. Roxsann Roberts, MD Section Chief, MRI Erlanger/EmCare
: Information for the Primary Care Physician Disclosures No financial relationships with commercial entities producing health care products/services. Roxsann Roberts, MD Section Chief, MRI Erlanger/EmCare
Digital Breast Tomosynthesis from a first idea to clinical routine
 International Master Programm Biomedical Engineering Digital Breast Tomosynthesis from a first idea to clinical routine Historical background 2D imaging of 3D objects has important limitations Jörg Barkhausen
International Master Programm Biomedical Engineering Digital Breast Tomosynthesis from a first idea to clinical routine Historical background 2D imaging of 3D objects has important limitations Jörg Barkhausen
Final Evidence Report
 20, 2012 Health Technology Assessment Appropriate Imaging for Breast Cancer Screening in Special Populations Final Evidence Report December 10, 2014 Health Technology Assessment Program (HTA) Washington
20, 2012 Health Technology Assessment Appropriate Imaging for Breast Cancer Screening in Special Populations Final Evidence Report December 10, 2014 Health Technology Assessment Program (HTA) Washington
BREAST DENSITY WHAT IS IT? WHY IS IT IMPORTANT? & What IOWA SF250 Means to Patients and Providers
 BREAST DENSITY WHAT IS IT? WHY IS IT IMPORTANT? & What IOWA SF250 Means to Patients and Providers Arnold Honick, MD Radiology Consultants of Iowa, PLC ahonick@rciowa.com BREAST DENSITY LEGISLATION Nancy
BREAST DENSITY WHAT IS IT? WHY IS IT IMPORTANT? & What IOWA SF250 Means to Patients and Providers Arnold Honick, MD Radiology Consultants of Iowa, PLC ahonick@rciowa.com BREAST DENSITY LEGISLATION Nancy
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI
 Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
Emerging Techniques in Breast Imaging: Contrast-Enhanced Mammography and Fast MRI Lilian Wang, M.D. Breast Imaging Section Department of Radiology Northwestern Medicine Overview Rationale for new imaging
Session 2: The Role of Specialist Radiology Technologists
 Session 2: The Role of Specialist Radiology Technologists Louise M. Henderson, MSPH PhD Assistant Professor, Department of Radiology The University of North Carolina, Chapel Hill Overview Role of the technologist
Session 2: The Role of Specialist Radiology Technologists Louise M. Henderson, MSPH PhD Assistant Professor, Department of Radiology The University of North Carolina, Chapel Hill Overview Role of the technologist
Digital Breast Tomosynthesis Ready for Routine Screening?
 Digital Breast Tomosynthesis Ready for Routine Screening? Sophia Zackrisson MD, PhD, Assoc Prof of Radiology Skåne University Healthcare, Lund University, Sweden 1 Mammography screening 20% reduced breast
Digital Breast Tomosynthesis Ready for Routine Screening? Sophia Zackrisson MD, PhD, Assoc Prof of Radiology Skåne University Healthcare, Lund University, Sweden 1 Mammography screening 20% reduced breast
OPTO-ACOUSTIC BREAST IMAGING
 OPTO-ACOUSTIC BREAST IMAGING Imaging-Pathology Correlation of Opto-Acoustic Features in Benign and Malignant Breast Masses Reni Butler, M.D. F. Lee Tucker, M.D. Philip Lavin, Ph.D. Erin Neuschler, M.D.
OPTO-ACOUSTIC BREAST IMAGING Imaging-Pathology Correlation of Opto-Acoustic Features in Benign and Malignant Breast Masses Reni Butler, M.D. F. Lee Tucker, M.D. Philip Lavin, Ph.D. Erin Neuschler, M.D.
arxiv: v2 [cs.cv] 8 Mar 2018
![arxiv: v2 [cs.cv] 8 Mar 2018 arxiv: v2 [cs.cv] 8 Mar 2018](/thumbs/87/97094636.jpg) Automated soft tissue lesion detection and segmentation in digital mammography using a u-net deep learning network Timothy de Moor a, Alejandro Rodriguez-Ruiz a, Albert Gubern Mérida a, Ritse Mann a, and
Automated soft tissue lesion detection and segmentation in digital mammography using a u-net deep learning network Timothy de Moor a, Alejandro Rodriguez-Ruiz a, Albert Gubern Mérida a, Ritse Mann a, and
