Preoperative Needle Biopsy of Sentinel Lymph Nodes Using Intradermal Microbubbles and Contrast-Enhanced Ultrasound in Patients With Breast Cancer
|
|
|
- Charleen Gordon
- 6 years ago
- Views:
Transcription
1 Women s Imaging Original Research Sever et al. CEUS to Determine SLN Status in Breast Cancer Patients Women s Imaging Original Research Ali R. Sever 1 Philippa Mills 1 Jennifer Weeks 1 Susan E. Jones 2 David Fish 3 Peter A. Jones 2 Willem Mali 4 Sever AR, Mills P, Weeks J, et al. Keywords: axillary lymph node dissection, breast cancer, contrast-enhanced ultrasound, core biopsy, fine-needle aspiration cytology, microbubble contrast agents, preoperative staging, sentinel lymph node biopsy DOI: /AJR Received August 15, 2011; accepted after revision December 16, Department of Radiology, Maidstone Hospital, Hermitage Ln, Maidstone ME16 9QQ, United Kingdom. Address correspondence to A. R. Sever (ali.sever@nhs.net). 2 Department of Surgery, Maidstone Hospital, Maidstone, United Kingdom. 3 Department of Pathology, Maidstone Hospital, Maidstone, United Kingdom. 4 Department of Radiology, University Medical Centre Utrecht, Utrecht, The Netherlands. AJR 2012; 198: X/12/ American Roentgen Ray Society Preoperative Needle Biopsy of Sentinel Lymph Nodes Using Intradermal Microbubbles and Contrast-Enhanced Ultrasound in Patients With Breast Cancer OBJECTIVE. The purpose of this study was to assess whether sentinel lymph nodes (SLNs) that undergo targeted needle biopsy after identification by contrast-enhanced ultrasound (CEUS) using intradermally injected microbubbles results in more node-positive breast cancer patients being diagnosed preoperatively. Furthermore, we sought to determine whether the addition of CEUS to gray-scale sonography of the axilla reduces the number of patients having axillary lymph node (ALN) dissection as a second procedure. SUBJECTS AND METHODS. Intradermal microbubble injection was performed in 136 breast cancer patients who had no abnormal ALNs on routine gray-scale axillary sonography. When an enhancing ALN was visualized, percutaneous sonography-guided fine-needle aspiration cytology or core needle biopsy was performed. Depending on the biopsy results, patients underwent SLN biopsy or ALN dissection. If the putative SLN biopsy was positive or a biopsy tract was seen in the excised SLN, the procedure was defined as successful. RESULTS. SLNs were identified and biopsied in 126 of the 136 cases (93%). Seventeen patients had positive sonography-guided biopsy results (13%) and were treated with immediate ALN dissection. In seven patients, the biopsied node was the only positive node. The remaining 109 patients underwent SLN biopsy. In nine cases (8%), a positive lymph node was identified. Four of these false-negative cases had only micrometastases. CONCLUSION. SLNs can be identified and biopsied using CEUS to increase the accuracy of preoperative axillary staging. If the needle biopsy result is negative, conventional SLN biopsy is indicated. A xillary lymph node (ALN) status provides important staging and prognostic information about patients with invasive breast cancer and may influence treatment decisions [1, 2]. ALN dissection was the gold standard but is associated with significant morbidity [3, 4]. With increased breast cancer awareness, improved imaging systems, and high-quality screening programs, patients now often present with smaller tumors and the incidence of lymph node involvement has decreased. Almost two thirds of breast cancer patients present without axillary metastases [5, 6]. Consequently, sentinel lymph node (SLN) biopsy has replaced ALN dissection as the standard of care for staging the axilla [7, 8]. The SLN is the first lymph node draining the primary tumor, and its histologic status is a reliable indicator of the entire lymph node basin. First pioneered using blue dye in patients with malignant melanoma [9], Giuliano et al. [10] adapted its use in breast cancer and Krag et al. [11] used radiolabeled colloid to identify the SLN. Albertini et al. [12] were the first to use both blue dye and gamma probe guided surgery, leading to an SLN identification rate of more than 95% with false-negative rates between 5% and 10% after subsequent ALN dissection [13]. United States guidelines currently advise completion ALN dissection when the SLN biopsy reveals macro- or micrometastases (> 0.2 mm) [13]. Approximately 50% of patients with positive SLN biopsy findings harbor additional non sentinel ALN metastases. This possibility represents an important drawback of the SLN biopsy procedure because these patients normally require a second operation. More accurate preoperative staging would reduce this need. Clinical examination of the axilla is inaccurate for predicting ALN status [14, 15]. The efficacy of preoperative axillary sonography has been investigated, and the morphologic features of abnormal lymph nodes AJR:198, August
2 Sever et al. have already been described [16]. Particularly when combined with sonography-guided biopsy of abnormal lymph nodes, preoperative axillary sonography has been shown to reduce the need for a second operation in more than 50% of cases [17, 18]. Contrast-enhanced ultrasound (CEUS) is established in clinical practice. IV administration of a contrast agent provides enhanced imaging of tissue microvasculature in many organs. Previously always given IV, microbubbles were initially used mostly for cardiac imaging; their use has been expanded to include hepatic imaging, posttransplant sonography, abdominal trauma scanning, and imaging other areas [19]. Sonographic contrast agents are composed of a dispersion of microbubbles, each of which is smaller than an RBC, that act as reflectors of the ultrasound beam [20, 21]. In 2004, Goldberg et al. [22] showed that microbubbles injected peritumorally in a swine melanoma model were seen to enter lymphatic channels, thus allowing SLNs to be identified accurately using sonography in 90% of cases. After a successful trial of CEUS on a swine model [22] and five patients [23], a validation study was performed. The results of that study showed that this technique can be used to identify the SLN in breast cancer patients [24, 25]. The aim of this study was to investigate the role of preoperative sonography-guided needle biopsy of the enhancing SLN or SLNs after microbubble injection in patients with breast cancer and to determine whether CEUS would be superior to routine grayscale sonography in the preoperative detection of node positivity. Subjects and Methods This prospective study was approved by the local institutional review board and the Medicines and Healthcare Products Regulatory Agency. All patients gave written informed consent. Between November 2009 and December 2010, 136 consecutive consenting patients with breast cancer who were scheduled for primary surgical treatment were recruited into the study. Exclusion criteria were histologically or cytologically proven ALN involvement diagnosed clinically or using standard sonographic imaging and the presence of severe medical comorbidities. All sonographic examinations were performed by a single experienced breast radiologist using an Acuson Sequoia 512 scanner (Siemens Healthcare). This scanner provides conventional gray-scale imaging, pulse-inversion harmonic gray-scale imaging, and contrast-specific sonographic imaging with live dual images of tissue only and contrast agent (Cadence Contrast Pulse Sequencing, Siemens Healthcare). A high-frequency 14-MHz linear-array probe (15L8w, Siemens Healthcare) was used. To reduce microbubble destruction, low-mechanical-index values were applied ( ). All patients with suspected breast carcinoma undergo axillary sonography as part of their initial assessment. Patients with abnormal or suspicious nodes undergo fine-needle aspiration cytology (FNAC) or core biopsy (CB). Rather than FNAC, CB was chosen in some cases when the primary was close to the axilla and in some cases when the node was very enlarged. All patients with normal findings on axillary sonography or negative axillary biopsy results were assessed clinically and patients suitable for routine SLN biopsy were invited to be included in this study. For consenting patients, in order not to delay the surgery, axillary assessment with microbubbles was performed within 1 week of the diagnosis of breast cancer. The microbubble study was also offered to those patients commencing neoadjuvant treatment. The median tumor size was 16 mm (range, mm). Most patients had only a small amount of associated ductal carcinoma in situ. Including the in situ component, the median overall tumor size was 19.5 mm (range, mm). There were six cases of in situ cancer only, 104 cases of invasive ductal cancer, 20 cases of invasive lobular cancer, and six cases of other cancer types. Lymphovascular invasion was seen in 38 cases (28%). The lesions were located in the breast as follows: 76 in the upper outer quadrant, 32 in the upper inner quadrant, 22 in the lower outer quadrant, and six in the lower inner quadrant. The Microbubble Procedure Before microbubble injection, 1 ml of 1% lidocaine was injected into the subcutaneous layer of the areola. The microbubble contrast agent was reconstituted using 2 ml of sterile saline, and the ampoule was shaken vigorously to ensure a homogeneous suspension of bubbles. The ultrasound contrast agent is composed of phospholipid-stabilized microbubbles containing sulfur hexafluoride gas (SonoVue, Bracco Imaging) with a mean diameter of 2.5 μm. Between 0.2 and 0.5 ml of the microbubble suspension was injected into and just under the skin of the areola in the upper outer quadrant using a 1-mL insulin syringe and a 26-gauge needle. Up to three consecutive injections were given intradermally similar to the technique used for radioisotope and blue dye injections in patients undergoing conventional SLN biopsy. A conventional gray-scale ultrasound examination of the axilla was performed before injection of microbubbles, and the positions of the imaged lymph nodes were noted. After injection of the microbubbles, lymphatic channels were visualized immediately on contrast pulse sequencing and were tracked into the axilla. Areas of contrast agent accumulation were then imaged with grayscale or were simultaneously viewed on live dual images to confirm the presence of an architecturally defined lymph node. When no obvious lymphatic filling was seen, the areola area was massaged for seconds and imaging was repeated. If no lymph nodes could be identified after three consecutive injections, the study was abandoned and recorded as a failure. In patients whose nodes were successfully identified, the transit time from injection to arrival in the axillary node was between 15 and 45 seconds. Contrast agent remained in the presumed SLN for up to 3 minutes. Repeating the areola massage often produced a refill of the SLN without the need for a second injection. When an enhancing node was identified in the axilla, a biopsy was performed. The first node to enhance was always biopsied. In most cases there was only one SLN; if two SLNs enhanced simultaneously, both were biopsied. Core biopsy was carried out using a 16-gauge needle and up to three samples were taken and sent for analysis. FNAC was performed with a 21-gauge needle and samples were sent dry on glass slides to cellular pathology where routine H and E staining was carried out followed by cytologic analysis. The entire procedure usually took minutes to perform. Sentinel Lymph Node Biopsy The time between the microbubble study and definitive surgery varied from 5 to 90 days (median, 13 days). Patients with a positive FNAC or CB result underwent ALN dissection. The remaining patients with a negative FNAC or CB result were advised to undergo a standard SLN biopsy using a radioisotope and blue dye. The afternoon before surgery, patients attended the nuclear medicine department for subdermal injection of a radioactive isotope (Nanocoll, GE Healthcare), 40 mbq, in the periareolar upper outer quadrant region. Before surgery and immediately after induction of anesthesia, patients received a 2-mL subdermal injection of blue dye (Bleu Patente V 2.5%, Guerbet) in the periareolar upper outer quadrant region. A standard axillary incision was made, and a gamma probe (Navigator GPS, RMD Instruments) was used to facilitate identification of SLNs. All radioactive lymph nodes that is, all nodes colored blue and, very occasionally, any nodes that looked or felt macroscopically suspicious to the surgeon were excised and sent for standard histologic analysis together with the breast cancer specimen. 466 AJR:198, August 2012
3 CEUS to Determine SLN Status in Breast Cancer Patients TABLE 1: Summary of the 136 Microbubble Procedures Variable Value Total no. of cases 136 Technical failures 10 No lymph nodes identified 4 Inadequate biopsy 4 No biopsy evidence in excised SLNs 2 Technical success, no. (%) of cases 126 (93) True-positive results 17 (13) False-positive results 0 No. of cases treated with SLN biopsy 109 True-negative results 100 False-negative results 9 Sensitivity (%) 65 a Specificity (%) 100 b Positive predictive value (%) 100 c Negative predictive value (%) 92 d Note SLNs = sentinel lymph nodes. a (17 / [17 + 9]). b (100 / [ ]). c (17 / [17 + 0]). d (100 / [ ]). The pathologic assessment of the SLNs was performed according to the Sentinel Lymph Node Biopsy Handbook: New Start guidelines [26]. The pathologist also noted whether there was histologic evidence that the SLN had previously been biopsied by noting the presence of a linear tract of granulation tissue with associated hemorrhage, fat necrosis, or hemosiderin-laden macrophages. Results A total of 136 patients who had a microbubble injection and underwent SLN biopsy or immediate ALN dissection, depending on the results of the procedure, were included in the assessment. There were 135 women and one man with a median age of 62 years (range, years). Of these, 55 patients had screening mammography detected cancers diagnosed by the Maidstone and Tunbridge Wells National Health Service Trust Breast Screening Service and the remaining 81 cases were symptomatic referrals to the breast clinic. There were no adverse events, and a patient survey showed a high level of satisfaction [25]. There were no axillary hematomas found after the axillary needle biopsy. In one patient, microbubbles successfully identified the SLN and the 16-gauge CB was benign, but the surgical SLN biopsy procedure failed to identify any hot or blue nodes. The patient underwent ALN dissection and all nodes were benign. In total, 136 patients underwent SLN biopsy or immediate ALN dissection depending on the results of the preoperative assessment with microbubbles. The microbubble procedure was defined as successful when the following three parameters were met: lymphatic enhancement identified at the site of microbubble injection and followed into the axilla where enhancing lymph nodes were seen; a successful biopsy of these nodes; and pathologic confirmation of the biopsy tract within the excised SLNs. When biopsy of the presumed SLN yielded positive findings, patients proceeded to immediate ALN dissection and these cases were also regarded as successful. The procedure was unsuccessful in 10 patients. In four patients, microbubble injection failed to show any enhancing lymph nodes; therefore, no biopsy was performed. In one of these four cases, the patient had a recent surgical excision and the microbubble contrast agent pooled in the surgical cavity and the lymphatics failed to bypass this area. In two cases the lymphatics were seen but could not be followed into the axilla; in the one remaining case, no lymphatics were identified. In 132 of the 136 cases (97%), a presumed SLN was seen enhancing in the axilla after microbubble injection and a biopsy was performed. CB was performed in 87 patients and FNAC in 83 cases. In 38 cases, both FNAC and CB were performed because of the perceived inadequacy of the FNAC specimen at the time of biopsy. Four biopsies were reported as inadequate because no sufficient cytologic material or lymph node tissue was included within the biopsy specimen. Those cases were also recorded as failures. In 128 cases the biopsy material was adequate. However, in two cases there was no definite histologic evidence of a previous biopsy within the excised SLN, raising the possibility that a lymph node that was not the SLN had been sampled in error. Three of the 10 failed cases (30%) were positive at subsequent SLN biopsy; all were in the group in which microbubble injection failed to show any enhancing lymph nodes. The overall results of the procedure are shown in Table 1. The microbubble procedure was deemed successful in 126 of the 136 cases (93%) when the SLNs were correctly identified and biopsied. In 17 of the 126 cases (13%), histopathologic examination of the needle biopsy sample from the microbubble procedure proved a metastatic deposit in the SLNs and these patients underwent ALN dissection (true-positive biopsy). In seven cases the biopsied node was the only positive node in the axillary specimen (Fig. 1), and in three of those seven cases the only evidence of axillary disease was a micrometastasis ( mm) in the biopsied node. The other 10 patients had more than one involved node in their axillary dissection specimen. In 109 cases there was no evidence of malignancy within the nodal biopsy specimen and these patients underwent SLN biopsy. In nine of the 109 cases (8%), there was malignancy in the excised SLN (false-negative biopsy, Fig. 2). The location of the primary tumor in these nine cases was as follows: seven in the upper outer quadrant, one in the lower outer quadrant, and one in the lower inner quadrant. Eight of the 109 patients (7%) had completion ALN dissection. One patient with micrometastasis declined further axillary surgery. In five of the eight patients (63%) who underwent completion ALN dissection, there were no other involved nodes identified in the axillary specimen. In the remaining three patients, however, the completion ALN dissection specimen contained macrometastatic deposits in the non-slns. In one case, only one of 17 non-slns was positive, containing a 5-mm deposit. The second case had a micrometastasis in the hot and blue SLN containing the biopsy tract and an 8-mm deposit in the other slightly hot, nonblue node, whereas the completion ALN dissection specimen revealed an additional nine of 21 nodes were also involved. In the third case the surgeon removed two SLNs: The hot and blue node was negative and contained a biopsy tract in keeping with the microbubble-enhanced node and the other SLN was nonhot and nonblue but hard and contained an 11-mm metastasis with extracapsular spread. In this patient, the completion ALN dissection specimen showed an additional five of 15 nodes were involved. In most of the cases, the lymphatics were readily followed into the axilla and microbubbles highlighted, by their enhanced reflection, a single axillary node. However, in some cases a second or third node was also noted enhancing subsequently via the efferent lymphatics connecting the first node to the others. In such cases the initial enhancing node was accepted as the true presumed SLN and the remaining nodes were not biopsied. In 16 of the 123 patients (13%) two nodes were identified by simultaneous enhancement and both nodes were biopsied. Three patients in this group were proven to AJR:198, August
4 Sever et al. have axillary metastasis and all were treated with immediate ALN dissection. In 76 of the 136 patients (56%) the enhancing lymph node or nodes were also seen on gray-scale imaging before the microbubble injection. However, in 55 cases (40%) the presumed SLN could be identified as a lymph node by sonography only after the microbubble enhancement. It was otherwise not visible on gray-scale imaging either because of its deep location or because it had a very thin cortex and a prominent fatty hilum and therefore was obscured by the surrounding axillary fat. In five cases (4%), there was a focal collection of contrast agent in the axilla but gray-scale imaging failed to identify a nodal architecture corresponding to the site of enhancement, raising the possibility of contrast pooling rather than true nodal enhancement. Three patients underwent the microbubble procedure before commencing neoadjuvant chemotherapy. Two had a negative SLN FNAC and at surgery had a negative SLN biopsy. The third patient had a positive CB of the presumed SLN after microbubble injection and her final postchemotherapy ALN dissection revealed (residual) isolated tumor cells (< 0.2 mm) in one node. A C Fig year-old woman with grade II invasive ductal carcinoma. A, Contrast-enhanced ultrasound image obtained using contrast-specific mode (Cadence Pulse Sequencing, Siemens Healthcare) reveals nodal enhancement (arrows). B, Conventional gray-scale image shows same node (arrows) as A. C, After sentinel lymph node was identified with microbubbles, core biopsy sample was taken of this node (short arrows) using 16-gauge biopsy needle (long arrows). Discussion SLN biopsy has become the standard procedure for axillary staging in breast cancer patients. However, if metastases are detected in the SLNs, then completion ALN dissection is advised. Preoperative diagnosis of lymph node metastases reduces this need. In most United Kingdom based centers, the routine use of intraoperative assessment of the SLNs with frozen-section or touch imprint cytology has not been adopted for logistical reasons. Many units do not have an onsite histopathology or cytology service. False-negative rates are well recognized for both techniques and the reported patientbased sensitivities are highly variable; a meta-analysis reported a sensitivity of 75% (95% CI, 65 84%) and 63% (95% CI, 57 69%) for frozen-section and touch imprint cytology, respectively [27, 28]. Accurate preoperative axillary staging has many potential benefits. These benefits not only avoid a second operation, but also facilitate better theater scheduling, allow precise patient consenting, and may influence decisions regarding neoadjuvant chemotherapy. In 2004 and more recently in 2011, Goldberg et al. [22, 29] showed that in a swine melanoma model, microbubbles had the potential to identify the sentinel nodes. A subsequent clinical study showed, for the first time, that in breast cancer patients a microbubble contrast agent injected intradermally readily entered breast lymphatic channels and traveled into the draining SLNs and that enhancement was clearly visualized by CEUS [24, 25]. This current study describes how sonography-guided biopsy of the enhancing node has the potential to identify malignancy within otherwise normal-looking SLNs preoperatively and therefore may select patients in whom an SLN biopsy would be futile. Preoperative axillary gray-scale sonography and biopsy of abnormal axillary nodes are becoming routine practice in breast units. A meta-analysis of five studies showed axillary sonography with sonography-guided biopsy to be moderately sensitive (45.4%) and highly specific (99.6%) for the diagnosis of axillary metastases [30]. Others have emphasized the limitations of gray-scale sonography, showing that normal axillary sonography misses involved axillae in 16 29% of cases [31, 32]. These figures are consistent with our audit of data from 2005 to 2008, in which 503 patients with a normal axillary sonography underwent SLN biopsy and B 468 AJR:198, August 2012
5 CEUS to Determine SLN Status in Breast Cancer Patients Fig. 2 Photomicrograph (H and E, 4) of histopathologic slide from sentinel lymph node specimen of 62-year-old woman with grade II invasive ductal carcinoma. Micrometastasis (1.4 mm) was identified within node (arrowheads). Hemorrhage from previous biopsy tract was noted a few millimeters away from metastatic deposit (arrows). in 105 patients (21%) the SLN biopsy result was positive and necessitated a subsequent completion ALN dissection [18]. Since the introduction of the microbubble procedure in our routine practice in 2008, the completion ALN dissection rate has dropped from 21% to 8%. Our experience has clearly shown one of the main limitations of gray-scale sonography is that the SLN can be obscured within the axillary fat. Indeed, we report here that 40% of the SLNs could be identified as a lymph node only after microbubble enhancement. In four of the 17 true-positive (24%) and in five of the nine false-negative (56%) cases, the SLNs could not be seen on gray-scale images alone. These results are also consistent with those of Britton et al. [33]; those investigators found that grayscale sonography guided biopsy missed the SLN in 36% of patients and concluded there was a need for more reliable methods of nodal identification. In experimental studies, Goldberg et al. [22] identified filling defects within enhancing SLNs that were successfully correlated with tumor deposits. In our study, we aimed only to identify and biopsy the SLNs and did not attempt to perform such correlation. Axillary lymph nodes are deeper in location in the human axilla compared with those in their animal models, which makes identification of small filling defects difficult. All patients had an initial assessment of the ipsilateral axilla with clinical examination and sonography. Any abnormal or enlarged nodes were biopsied and those with involved nodes were excluded. In the 26 patients who had positive nodes, none was sonographically enlarged. Recognition of the nodal enhancement pattern may be a valuable addition to this technique and perhaps such filling defects could be better seen in lymph nodes with a thickened cortex. Further studies are required to assess this feature. In the aforementioned experimental studies, both groups used different microbubbles, which may be significant. We have noticed that microbubbles do not last long in the lymph nodes and their persistence is related to the duration of sonography scanning. More robust microbubbles may provide a more homogeneous filling of the lymph nodes and may enhance longer, enabling a more detailed assessment of any filling defects. In patients undergoing neoadjuvant chemotherapy, identification of the SLN using microbubbles may be particularly valuable. Neoadjuvant treatment lowers the rate of SLN identification possibly because of fibrosis within the axilla [34, 35]. In our series, 10 patients underwent neoadjuvant therapy and microbubble assessment. In seven cases the microbubble assessment was performed after completion of neoadjuvant chemotherapy. In three patients the microbubble assessment preceded neoadjuvant chemotherapy. In one of these three patients, a positive node was proven on CB after microbubble assessment and subsequently was found to have only isolated tumor cells in the ALN dissection specimen, indicating a partial response. Although we have no such case in our series of patients with proven metastases on CB after microbubble assessment and later deemed negative after ALN dissection, we acknowledge that this false positivity can occur after a complete pathologic response on axillary nodal disease. In such cases it is possible for the pathologist to identify fibrous scarring in the node where the metastasis had been previously proven. Insertion of a marker into or next to the microbubble-enhancing SLN in these patients may help in identifying the node later if conventional techniques fail. Similarly, patients treated by mastectomy for widespread ductal carcinoma in situ or for risk reduction may benefit from a deployed marker to facilitate subsequent SLN biopsy if any unsuspected invasive component is identified histologically. In four patients microbubble injection failed to show any enhancing lymph nodes, and therefore no biopsy was performed. Three of these four cases had a positive SLN biopsy. It is well established that lymph nodes totally replaced by metastases can be associated with a falsenegative SLN biopsy because these nodes may fail to take up blue dye or radioactive isotope when the lymphatics are obstructed [36]. In such cases microbubble enhancement may also fail. In patients who have no enhancing nodes, cautious gray-scale imaging particularly at the site where abrupt lymphatic visualization stops may help to identify abnormal lymph nodes. Such cases also highlight the importance of having an experienced surgeon who can recognize these involved nodes by the naked eye at operation. A few limitations of this study merit comment. The data are from a single unit and a single radiologist. The procedure has a learning curve not only in identification, but also in the biopsy technique. For this reason we have not included the results of two other radiologists who have recently started performing this technique and validating their results. It is important to differentiate contrast pooling from actual nodal enhancement. In five cases we encountered this problem: An obvious lymph node was not clearly recognizable on the gray-scale images corresponding to the site of enhancement. In four of these cases the biopsy was inadequate, raising the possibility of lymphatic pooling rather than nodal enhancement. This shortcoming was recognized early in the study. Massage frequently overcame the problem; however, if no lymph node was recognizable on gray-scale images after massage, the procedure was regarded as a failure. Another limitation relates to the false-negative biopsy results in nine cases. A similar drawback was recognized by Britton et al. [33] when half of the false-negative cases revealed a biopsy tract within the SLN. It might be possible to overcome this sampling error by removing the entire contrast-identified lymph node for detailed histologic analysis. Breast lesions are increasingly being removed under sonography guidance using vacuum-assisted and other devices. It is possible that similar techniques could be used to remove the entire SLN. This would have the potential to obviate conventional SLN biopsy and replace it with a percutaneous outpatient procedure. In conclusion, SLNs may be identified and biopsied preoperatively using CEUS after injection of microbubbles. Using this technique increases the number of patients proven to have involved ALNs preoperatively, thereby reducing the futile SLN biopsy rate by AJR:198, August
6 Sever et al. more than 50% when compared with the best published detection rates using conventional gray-scale sonography. A negative axillary biopsy does not obviate conventional SLN biopsy. The avoidance of a second operation to complete the ALN dissection should also have cost-saving implications. References 1. Fisher B, Bauer M, Wickerham DL, et al. Relation of number of positive axillary nodes to the prognosis of patients with primary breast cancer: an NSABP update. Cancer 1983; 52: Carter CL, Allen C, Henson DE. Relation of tumor size, lymph node status, and survival in 24,740 breast cancer cases. Cancer 1989; 63: Kuehn T, Klauss W, Darsow M, et al. Long-term morbidity following axillary dissection in breast cancer patients: clinical assessment, significance for life quality and the impact of demographic, oncologic and therapeutic factors. Breast Cancer Res Treat 2000; 64: Leidenius M, Leivonen M, Vironen J, von Smitten K. The consequences of long-time arm morbidity in node-negative breast cancer patients with sentinel node biopsy or axillary clearance. J Surg Oncol 2005; 92: Cady B, Stone MD, Schuler JG, Thakur R, Wanner MA, Lavin PT. The new era in breast cancer: invasion, size, and nodal involvement dramatically decreasing as a result of mammographic screening. Arch Surg 1996; 131: Silverstein MJ, Skinner KA, Lomis TJ. Predicting axillary nodal positivity in 2282 patients with breast carcinoma. World J Surg 2001; 25: Veronesi U, Paganelli G, Galimberti V, et al. Sentinel-node biopsy to avoid axillary dissection in breast cancer with clinically negative lymphnodes. Lancet 1997; 349: McMasters KM, Tuttle TM, Carlson DJ, et al. Sentinel lymph node biopsy for breast cancer: a suitable alternative to routine axillary dissection in multi-institutional practice when optimal technique is used. J Clin Oncol 2000; 18: Morton DL, Wen DR, Wong JH, et al. Technical details of intraoperative lymphatic mapping for early stage melanoma. Arch Surg 1992; 127: Giuliano AE, Kirgan DM, Guenther JM, Morton DL. Lymphatic mapping and sentinel lymphadenectomy for breast cancer. Ann Surg 1994; 220: Krag DN, Weaver DL, Alex JC, Fairbank JT. Surgical resection and radiolocalization of the sentinel lymph node in breast cancer using a gamma probe. Surg Oncol 1993; 2: Albertini JJ, Lyman GH, Cox C, et al. Lymphatic mapping and sentinel node biopsy in the patient with breast cancer. JAMA 1996; 276: Lyman GH, Giuliano AE, Somerfield MR, et al.; American Society of Clinical Oncology. American Society of Clinical Oncology guideline recommendations for sentinel lymph node biopsy in early-stage breast cancer. J Clin Oncol 2005; 23: Sacre RA. Clinical evaluation of axillary lymph nodes compared to surgical and pathological findings. Eur J Surg Oncol 1986; 12: Specht MC, Fey JV, Borgen PI, Cody HS 3rd. Is the clinically positive axilla in breast cancer really a contraindication to sentinel lymph node biopsy? J Am Coll Surg 2005; 200: Bedi DG, Krishnamurthy R, Krishnamurthy S, et al. Cortical morphologic features of axillary lymph nodes as a predictor of metastasis in breast cancer: in vitro sonographic study. AJR 2008; 191: Mainiero MB, Cinelli CM, Koelliker SL, Graves TA, Chung MA. Axillary ultrasound and fine-needle aspiration in the preoperative evaluation of the breast cancer patient: an algorithm based on tumor size and lymph node appearance. AJR 2010; 195: Mills P, Sever A, Weeks J, Fish D, Jones S, Jones P. Axillary ultrasound assessment in primary breast cancer: an audit of 653 cases. Breast J 2010; 16: Wilson SR, Burns PN. Microbubble-enhanced US in body imaging: what role? Radiology 2010; 257: Cosgrove D. Ultrasound contrast agents: an overview. Eur J Radiol 2006; 60: Yang WT, Goldberg BB. Microbubble contrast-enhanced ultrasound for sentinel lymph node detection: ready for prime time? AJR 2011; 196: Goldberg BB, Merton DA, Liu JB, et al. Sentinel lymph nodes in a swine model with melanoma: contrast-enhanced lymphatic US. Radiology 2004; 230: Sever A, Broillet A, Schneider M, et al. Dynamic visualization of lymphatic channels and sentinel lymph nodes using intradermal microbubbles and contrast-enhanced ultrasound in a swine model and patients with breast cancer. J Ultrasound Med 2010; 29: Sever A, Jones S, Cox K, Weeks J, Mills P, Jones P. Preoperative localization of sentinel lymph nodes using intradermal microbubbles and contrast-enhanced ultrasonography in patients with breast cancer. Br J Surg 2009; 96: Sever AR, Mills P, Jones SE, et al. Preoperative sentinel node identification with ultrasound using microbubbles in patients with breast cancer. AJR 2011; 196: Bobrow L, Pinder S. Histopathology and the SLN. In: Bobrow L, Pinder S, eds. Sentinel lymph node biopsy handbook: new start. London, UK: Royal College of Surgeons of England, 2004: Tew K, Irwig L, Matthews A, Crowe P, Macaskill P. Meta-analysis of sentinel node imprint cytology in breast cancer. Br J Surg 2005; 92: Geertsema D, Gobardhan PD, Madsen EV, et al. Discordance of intraoperative frozen section analysis with definitive histology of sentinel lymph nodes in breast cancer surgery: complementary axillary lymph node dissection is irrelevant for subsequent systemic therapy. Ann Surg Oncol 2010; 17: Goldberg BB, Merton DA, Liu JB, et al. Contrast-enhanced ultrasound imaging of sentinel lymph nodes after peritumoral administration of Sonazoid in a melanoma tumor animal model. J Ultrasound Med 2011; 30: Alvarez S, Añorbe E, Alcorta P, López F, Alonso I, Cortés J. Role of sonography in the diagnosis of axillary lymph node metastases in breast cancer: a systematic review. AJR 2006; 186: van Rijk MC, Deurloo EE, Nieweg OE, et al. Ultrasonography and fine-needle aspiration cytology can spare breast cancer patients unnecessary sentinel lymph node biopsy. Ann Surg Oncol 2006; 13: Holwitt DM, Swatske ME, Gillanders WE, et al. Scientific Presentation Award: the combination of axillary ultrasound and ultrasound-guided biopsy is an accurate predictor of axillary stage in clinically node-negative breast cancer patients. Am J Surg 2008; 196: Britton PD, Provenzano E, Barter S, et al. Ultrasound guided percutaneous axillary lymph node core biopsy: how often is the sentinel lymph node being biopsied? Breast 2009; 18: Papa MZ, Zippel D, Kaufman B, et al. Timing of sentinel lymph node biopsy in patients receiving neoadjuvant chemotherapy for breast cancer. J Surg Oncol 2008; 98: Schrenk P, Tausch C, Wölfl S, Bogner S, Fridrik M, Wayand W. Sentinel node mapping performed before preoperative chemotherapy may avoid axillary dissection in breast cancer patients with negative or micrometastatic sentinel nodes. Am J Surg 2008; 196: Carmon M, Olsha O, Rivkin L, Spira RM, Golomb E. Intraoperative palpation for clinically suspicious axillary sentinel lymph nodes reduces the false-negative rate of sentinel lymph node biopsy in breast cancer. Breast J 2006; 12: AJR:198, August 2012
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY
 EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
Study on Efficacy of Preoperative Ultrasonography for Axillary Lymph Node Involvement In Breast Carcinoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
Is Sentinel Node Biopsy Practical?
 Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
Women s Imaging Original Research
 Women s Imaging Original Research Mainiero et al. Ultrasound-Guided FN in Breast Cancer Patients Women s Imaging Original Research WOMEN S IMGING Martha B. Mainiero 1 Christina M. Cinelli 2 Susan L. Koelliker
Women s Imaging Original Research Mainiero et al. Ultrasound-Guided FN in Breast Cancer Patients Women s Imaging Original Research WOMEN S IMGING Martha B. Mainiero 1 Christina M. Cinelli 2 Susan L. Koelliker
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Percutaneous Biopsy and Sentinel Lymphadenectomy: Minimally Invasive. he diagnosis and treatment of nonpalpable. Breast Cancer
 Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Utility of Preoperative Ultrasound for Predicting pn2 or Higher Stage Axillary Lymph Node Involvement in Patients With Newly Diagnosed Breast Cancer
 Women s Imaging Original Research Abe et al. Preoperative Ultrasound to Predict Axillary Lymph Node Involvement Women s Imaging Original Research Hiroyuki Abe 1 David Schacht Charlene A. Sennett Gillian
Women s Imaging Original Research Abe et al. Preoperative Ultrasound to Predict Axillary Lymph Node Involvement Women s Imaging Original Research Hiroyuki Abe 1 David Schacht Charlene A. Sennett Gillian
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Ultrasound or FNA for Predicting Node Positive in Breast Cancer
 Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Eight false negative sentinel node procedures in breast cancer: what went wrong?
 EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT
 PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Sentinel Lymph Node Biopsy Is Valuable For All Cancer. Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner
 Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
Sentinel Lymph Node Biopsy Is Valuable For All Cancer Surgery Grand Rounds Debate October 6, 2008 Joel Baumgartner History Lymphatics first described by Rasmus Bartholin in 1653 Rudolf Virchow postulated
The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer
 Original Article Middle East Journal of Cancer; October 2014; 5(4): 215-220 The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer Sedigheh
Original Article Middle East Journal of Cancer; October 2014; 5(4): 215-220 The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer Sedigheh
The American Society of Breast Surgeons
 The American Journal of Surgery (2008) 196, 477 482 The American Society of Breast Surgeons Scientific Presentation Award: The combination of axillary ultrasound and ultrasound-guided biopsy is an accurate
The American Journal of Surgery (2008) 196, 477 482 The American Society of Breast Surgeons Scientific Presentation Award: The combination of axillary ultrasound and ultrasound-guided biopsy is an accurate
Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study
 [ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
[ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
Original Article. J Fac Med Baghdad 193. Introduction:
 Original Article The value of Gray scale, color doppler and ultrasound guided- FNA in detection metastasis to the axillary lymph node in patient with primary breast cancer. * Qusay A. Fahad* Enam A.Al
Original Article The value of Gray scale, color doppler and ultrasound guided- FNA in detection metastasis to the axillary lymph node in patient with primary breast cancer. * Qusay A. Fahad* Enam A.Al
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
COMPARATIVE ANALYSIS OF COLON AND RECTAL CANCERS IN SENTINEL LYMPH NODE MAPPING
 Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Feasibility of using negative ultrasonography results of axillary lymph nodes to predict sentinel lymph node metastasis in breast cancer patients
 Received: 21 April 2018 Revised: 14 May 2018 DOI: 10.1002/cam4.1606 Accepted: 14 May 2018 ORIGINAL RESEARCH Feasibility of using negative ultrasonography results of axillary lymph nodes to predict sentinel
Received: 21 April 2018 Revised: 14 May 2018 DOI: 10.1002/cam4.1606 Accepted: 14 May 2018 ORIGINAL RESEARCH Feasibility of using negative ultrasonography results of axillary lymph nodes to predict sentinel
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation
 Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Sentinel lymph node (SLN) biopsy is a wellestablished
 ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
Correspondence should be addressed to Donald R. Lannin;
 Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
A Randomized Comparison of Sentinel-Node Biopsy with Routine Axillary Dissection in Breast Cancer
 The new england journal of medicine original article A Randomized Comparison of Sentinel-Node Biopsy with Routine Axillary Dissection in Breast Cancer Umberto Veronesi, M.D., Giovanni Paganelli, M.D.,
The new england journal of medicine original article A Randomized Comparison of Sentinel-Node Biopsy with Routine Axillary Dissection in Breast Cancer Umberto Veronesi, M.D., Giovanni Paganelli, M.D.,
Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection
 456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Targeting Surgery for Known Axillary Disease. Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center
 Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
Pre- operative staging of the axilla
 Pre- operative staging of the axilla Anthony J Maxwell University Hospital of South Manchester Outline Why stage the axilla? Optimising conventional US & needle sampling Other imaging and needle sampling
Pre- operative staging of the axilla Anthony J Maxwell University Hospital of South Manchester Outline Why stage the axilla? Optimising conventional US & needle sampling Other imaging and needle sampling
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection
 The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT
 Axillary Ultrasound Examination in the Selection of Carcinoma of Breast Patients for Sentinel Node Biopsy - A Prospective Study MISRA J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT Background: Axillary lymph
Axillary Ultrasound Examination in the Selection of Carcinoma of Breast Patients for Sentinel Node Biopsy - A Prospective Study MISRA J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT Background: Axillary lymph
Axillary ultrasound is frequently used to assess axillary nodes at
 ORIGINAL ARTICLE Identification and Resection of Clipped Node Decreases the False-negative Rate of Sentinel Lymph Node Surgery in Patients Presenting With Node-positive Breast Cancer (T0 T4, N1 N2) Who
ORIGINAL ARTICLE Identification and Resection of Clipped Node Decreases the False-negative Rate of Sentinel Lymph Node Surgery in Patients Presenting With Node-positive Breast Cancer (T0 T4, N1 N2) Who
ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE
 ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE Yu-Wen Chen, Yung-Chang Lai, Chien-Chin Hsu, and Ming-Feng Hou 1 Departments of Nuclear Medicine and 1 Gastroenteric
ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE Yu-Wen Chen, Yung-Chang Lai, Chien-Chin Hsu, and Ming-Feng Hou 1 Departments of Nuclear Medicine and 1 Gastroenteric
Case Scenario 1 History and Physical 3/15/13 Imaging Pathology
 Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast.
 Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
Diagnosis and staging of breast cancer and multidisciplinary team working
 1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
Role of sentinel lymph node biopsy in assessing the cancer spread to axilla in early breast cancer
 International Surgery Journal Gumber A et al. Int Surg J. 2017 Jan;4(1):53-57 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164445
International Surgery Journal Gumber A et al. Int Surg J. 2017 Jan;4(1):53-57 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20164445
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Sentinel lymph node biopsy under local anesthesia in patients with breast cancer
 Review Article Sentinel lymph node biopsy under local anesthesia in patients with breast cancer Prakasit Chirappapha 1,2, Visnu Lohsiriwat 1,3, Youwanush Kongdan 2, Panuwat Lertsithichai 2, Thongchai Sukarayothin
Review Article Sentinel lymph node biopsy under local anesthesia in patients with breast cancer Prakasit Chirappapha 1,2, Visnu Lohsiriwat 1,3, Youwanush Kongdan 2, Panuwat Lertsithichai 2, Thongchai Sukarayothin
Quality ID #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Quality ID #264: Sentinel Lymph de Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Quality ID #264: Sentinel Lymph de Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes
 Yonsei Med J 49(2):249-254, 2008 DOI 10.3349/ymj.2008.49.2.249 The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes Ki Hong Kim, 1 Eun Ju Son, 1 Eun-Kyung Kim,
Yonsei Med J 49(2):249-254, 2008 DOI 10.3349/ymj.2008.49.2.249 The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes Ki Hong Kim, 1 Eun Ju Son, 1 Eun-Kyung Kim,
The Efficacy of Axillary Ultrasound in the Detection of Nodal Metastasis in Breast Cancer
 Women s Imaging Original Research Lee et al. Ultrasound Detection of Nodal Metastasis Women s Imaging Original Research Belinda Lee 1 Adrian K. Lim 2 Jonathan Krell 1 Keshthra Satchithananda 2 R. Charles
Women s Imaging Original Research Lee et al. Ultrasound Detection of Nodal Metastasis Women s Imaging Original Research Belinda Lee 1 Adrian K. Lim 2 Jonathan Krell 1 Keshthra Satchithananda 2 R. Charles
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
The Value of Intraoperative Examination of Axillary Sentinel Nodes in Carcinoma of the Breast.
 Thomas Jefferson University Jefferson Digital Commons Department of Pathology, Anatomy, and Cell Biology Faculty Papers Department of Pathology, Anatomy, and Cell Biology 11-1-2008 The Value of Intraoperative
Thomas Jefferson University Jefferson Digital Commons Department of Pathology, Anatomy, and Cell Biology Faculty Papers Department of Pathology, Anatomy, and Cell Biology 11-1-2008 The Value of Intraoperative
Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer
 Gynecol Surg (2012) 9:185 191 DOI 10.1007/s10397-011-0712-6 ORIGINAL ARTICLE Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer Daniela Huber &
Gynecol Surg (2012) 9:185 191 DOI 10.1007/s10397-011-0712-6 ORIGINAL ARTICLE Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer Daniela Huber &
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION TYPE:
Quality ID #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Appropriate Use of Healthcare 2019 COLLECTION TYPE:
NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer
 NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer NICE provided the content for this booklet which is
NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer NICE provided the content for this booklet which is
Evaluation of the Axilla Post Z-0011 Trial New Paradigm
 Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Problems in staging breast carcinoma
 Problems in staging breast carcinoma Primary systemic therapy (PST) of breast carcinoma pathologists tasks Dr. Janina Kulka, 2nd Department of Pathology, Semmelweis University Budapest Austro-Hungarian
Problems in staging breast carcinoma Primary systemic therapy (PST) of breast carcinoma pathologists tasks Dr. Janina Kulka, 2nd Department of Pathology, Semmelweis University Budapest Austro-Hungarian
SPECT/CT Imaging of the Sentinel Lymph Node
 IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
Results of the ACOSOG Z0011 Trial
 DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer
 Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
Donna Plecha, MD 1, Shiyu Bai, BS 2, Helen Patterson 3, Cheryl Thompson, PhD 4, and Robert Shenk, MD 5
 Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1
 The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1 Jung Hee Shin, M.D., Asiry Hwang, M.D., Hye-Young Choi, M.D., Seung Yon Baek, M.D. Purpose: We evaluated the
The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1 Jung Hee Shin, M.D., Asiry Hwang, M.D., Hye-Young Choi, M.D., Seung Yon Baek, M.D. Purpose: We evaluated the
Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic score
 De Coninck et al. BMC Medical Imaging (2016) 16:13 DOI 10.1186/s12880-016-0116-1 RESEARCH ARTICLE Open Access Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic
De Coninck et al. BMC Medical Imaging (2016) 16:13 DOI 10.1186/s12880-016-0116-1 RESEARCH ARTICLE Open Access Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic
/pjs
 POLSKI PRZEGLĄD CHIRURGICZNY 05, 87, 6, 9094 0.55/pjs-05-0056 Problems concerning patients qualification for surgical procedures allowing for evaluation of the condition of axillary fossa lymph nodes in
POLSKI PRZEGLĄD CHIRURGICZNY 05, 87, 6, 9094 0.55/pjs-05-0056 Problems concerning patients qualification for surgical procedures allowing for evaluation of the condition of axillary fossa lymph nodes in
ORIGINAL ARTICLE BREAST ONCOLOGY. Ann Surg Oncol (2010) 17: DOI /s x
 Ann Surg Oncol (2010) 17:2690 2695 DOI 10.1245/s10434-010-1052-x ORIGINAL ARTICLE BREAST ONCOLOGY Discordance of Intraoperative Frozen Section Analysis with Definitive Histology of Sentinel Lymph Nodes
Ann Surg Oncol (2010) 17:2690 2695 DOI 10.1245/s10434-010-1052-x ORIGINAL ARTICLE BREAST ONCOLOGY Discordance of Intraoperative Frozen Section Analysis with Definitive Histology of Sentinel Lymph Nodes
Northumbria Healthcare NHS Foundation Trust. Breast Sentinel Lymph Node Biopsy. Issued by the Breast Team
 Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
Surgery for Melanoma and What s on the Horizon
 and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
and What s on the Horizon Giorgos C. Karakousis, M.D. Assistant Professor of Surgery Perelman School of Medicine at the University of Pennsylvania Background/Overview 76,870 cases of melanoma estimated
Sentinel node biopsy in breast cancer patients treated with neoadjuvant chemotherapy
 ONCOLOGY REPORTS 15: 927-931, 2005 927 Sentinel node biopsy in breast cancer patients treated with neoadjuvant chemotherapy YOSUKE TANAKA 1, HIRONORI MAEDA 2, YASUHIRO OGAWA 3, AKIHITO NISHIOKA 3, SATOSHI
ONCOLOGY REPORTS 15: 927-931, 2005 927 Sentinel node biopsy in breast cancer patients treated with neoadjuvant chemotherapy YOSUKE TANAKA 1, HIRONORI MAEDA 2, YASUHIRO OGAWA 3, AKIHITO NISHIOKA 3, SATOSHI
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
T he purpose of axillary node dissection in breast cancer
 546 ORIGINAL ARTICLE Sentinel lymph node biopsy in breast cancer patients after overnight migration of radiolabelled sulphur colloid N Lamichhane, K W Shen, C L Li, Q X Han, Y J Zhang, Z M Shao, Z Z Shen...
546 ORIGINAL ARTICLE Sentinel lymph node biopsy in breast cancer patients after overnight migration of radiolabelled sulphur colloid N Lamichhane, K W Shen, C L Li, Q X Han, Y J Zhang, Z M Shao, Z Z Shen...
The role of the cytologist in breast cancer screening
 The role of the cytologist in breast cancer screening I.Seili-Bekafigo, MD, PhD Clinical cytologist KBC Rijeka Croatian Society for Clinical Cytology Fine needle aspiration (FNA, FNAB, FNAC) Fine needle
The role of the cytologist in breast cancer screening I.Seili-Bekafigo, MD, PhD Clinical cytologist KBC Rijeka Croatian Society for Clinical Cytology Fine needle aspiration (FNA, FNAB, FNAC) Fine needle
ORIGINAL ARTICLE. Characteristics of the Sentinel Lymph Node in Breast Cancer Predict Further Involvement of Higher-Echelon Nodes in the Axilla
 ORIGINAL ARTICLE Characteristics of the Sentinel Lymph Node in Breast Cancer Predict Further Involvement of Higher-Echelon Nodes in the Axilla A Study to Evaluate the Need for Complete Axillary Lymph Node
ORIGINAL ARTICLE Characteristics of the Sentinel Lymph Node in Breast Cancer Predict Further Involvement of Higher-Echelon Nodes in the Axilla A Study to Evaluate the Need for Complete Axillary Lymph Node
Recent Update in Surgery for the Management of Breast Cancer
 Recent Update in Surgery for the Management of Breast Cancer Wonshik Han, MD, PhD Professor, Department of Surgery, Seoul National University College of Medicine Chief of Breast Care Center, Seoul National
Recent Update in Surgery for the Management of Breast Cancer Wonshik Han, MD, PhD Professor, Department of Surgery, Seoul National University College of Medicine Chief of Breast Care Center, Seoul National
Surgery for Breast Cancer
 Surgery for Breast Cancer 1750 Mastectomy - Petit 1894 Radical mastectomy Halsted Extended, Super radical mastectomy 1948 Modified radical mastectomy Patey 1950-60 WLE & RT Baclesse, Mustakallio 1981-85
Surgery for Breast Cancer 1750 Mastectomy - Petit 1894 Radical mastectomy Halsted Extended, Super radical mastectomy 1948 Modified radical mastectomy Patey 1950-60 WLE & RT Baclesse, Mustakallio 1981-85
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Savitri Krishnamurthy, MD 1
 EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
Breast Imaging: Multidisciplinary Approach. Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina
 Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study.
 ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study. Z Sidiropoulou,
ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study. Z Sidiropoulou,
Surgical Issues in Melanoma
 Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
Surgical Issues in Melanoma Mark B. Faries, MD, FACS Director, Donald L. Morton Melanoma Research Program Director, Surgical Oncology Training Program Professor of Surgery John Wayne Cancer Institute Surgical
A Dual-Modality Photoacoustic and Ultrasound Imaging System for Noninvasive Sentinel Lymph Node Detection: Preliminary Clinical Results
 A Dual-Modality Photoacoustic and Ultrasound Imaging System for Noninvasive Sentinel Lymph Node Detection: Preliminary Clinical Results Todd N. Erpelding 1, Alejandro Garcia-Uribe 2, Arie Krumholz 2, Haixin
A Dual-Modality Photoacoustic and Ultrasound Imaging System for Noninvasive Sentinel Lymph Node Detection: Preliminary Clinical Results Todd N. Erpelding 1, Alejandro Garcia-Uribe 2, Arie Krumholz 2, Haixin
Mehmet Eser 1, Metin Kement 1,4*, Levent Kaptanoglu 1, Melin Gecer 2, Evrim Abamor 3, Firat Tutal 1, Salim Balin 1, Necmi Kurt 1 and Huseyin Uzun 1
 Eser et al. BMC Surgery 2013, 13:13 RESEARCH ARTICLE Open Access A prospective comparative study to assess the contribution of radioisotope tracer method to dye-only method in the detection of sentinel
Eser et al. BMC Surgery 2013, 13:13 RESEARCH ARTICLE Open Access A prospective comparative study to assess the contribution of radioisotope tracer method to dye-only method in the detection of sentinel
Journal of IMAB - Annual Proceeding (Scientific Papers) 2007, vol. 13, book 1
 Journal of IMAB - Annual Proceeding (Scientific Papers) 2007, vol. 13, book 1 COMPARATIVE ANALYSIS OF ENDOSCOPICALY SUBMUCOSAL VS. OPEN SURGERY SUB- SEROSAL APPLICATION PATENT BLUE V INTRAOPERATIVE METHOD
Journal of IMAB - Annual Proceeding (Scientific Papers) 2007, vol. 13, book 1 COMPARATIVE ANALYSIS OF ENDOSCOPICALY SUBMUCOSAL VS. OPEN SURGERY SUB- SEROSAL APPLICATION PATENT BLUE V INTRAOPERATIVE METHOD
M D..,., M. M P.. P H., H, F. F A.. A C..S..
 Implications of NSABP B-32 and Loco-Regional Therapy Considerations After Neoadjuvant Chemotherapy Terry Mamounas, M.D., M.P.H, F.A.C.S. Professor of Surgery Northeastern Ohio Medical University Medical
Implications of NSABP B-32 and Loco-Regional Therapy Considerations After Neoadjuvant Chemotherapy Terry Mamounas, M.D., M.P.H, F.A.C.S. Professor of Surgery Northeastern Ohio Medical University Medical
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Effective Health Care Program
 Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy
 Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy Eun Yoon Cho, MD, PhD Department of Pathology and Translational Genomics Samsung Medical Center Sungkyunkwan University
Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy Eun Yoon Cho, MD, PhD Department of Pathology and Translational Genomics Samsung Medical Center Sungkyunkwan University
Imaging Guided Biopsy. Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer
 Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients
 Original Article Radiat Oncol J 4;():-7 http://dx.doi.org/.857/roj.4... pissn 4-9 eissn 4-56 Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients Hee Ji
Original Article Radiat Oncol J 4;():-7 http://dx.doi.org/.857/roj.4... pissn 4-9 eissn 4-56 Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients Hee Ji
Newly Diagnosed Breast Cancer: Preoperative Imaging and Localization
 Newly Diagnosed Breast Cancer: Preoperative Imaging and Localization Debra Monticciolo, MD Professor of Radiology Texas A&M University no disclosures Debra Monticciolo, MD Professor of Radiology Texas
Newly Diagnosed Breast Cancer: Preoperative Imaging and Localization Debra Monticciolo, MD Professor of Radiology Texas A&M University no disclosures Debra Monticciolo, MD Professor of Radiology Texas
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
COPE Library Sample
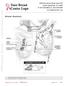 Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Sentinel Node Localisation of Melanoma
 Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
SLN Mapping in Cervical Cancer. Memorial Sloan Kettering Cancer Center New York, USA
 Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Clinical Study Ultrasound Guided Core Biopsy versus Fine Needle Aspiration for Evaluation of Axillary Lymphadenopathy in Patients with Breast Cancer
 ISRN Oncology, Article ID 703160, 9 pages http://dx.doi.org/10.1155/2014/703160 Clinical Study Ultrasound Guided Core Biopsy versus Fine Needle Aspiration for Evaluation of Axillary Lymphadenopathy in
ISRN Oncology, Article ID 703160, 9 pages http://dx.doi.org/10.1155/2014/703160 Clinical Study Ultrasound Guided Core Biopsy versus Fine Needle Aspiration for Evaluation of Axillary Lymphadenopathy in
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration?
 Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration? Poster No.: C-0289 Congress: ECR 2011 Type: Scientific Paper Authors: M. J. Diaz-Ruiz,
Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration? Poster No.: C-0289 Congress: ECR 2011 Type: Scientific Paper Authors: M. J. Diaz-Ruiz,
RESEARCH ARTICLE. Abstract. Introduction
 DOI:http://dx.doi.org/10.7314/APJCP.2013.14.4.2657 Frozen Section Analysis of Sentinel Lymph Nodes for Detection of Breast Cancer Micro Metastasis RESEARCH ARTICLE Accuracy of Frozen Section Analysis of
DOI:http://dx.doi.org/10.7314/APJCP.2013.14.4.2657 Frozen Section Analysis of Sentinel Lymph Nodes for Detection of Breast Cancer Micro Metastasis RESEARCH ARTICLE Accuracy of Frozen Section Analysis of
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Published Ahead of Print on October 13, 2009 as /JCO J Clin Oncol by American Society of Clinical Oncology INTRODUCTION
 Published Ahead of Print on October 13, 2009 as 10.1200/JCO.2009.22.1846 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2009.22.1846 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
Published Ahead of Print on October 13, 2009 as 10.1200/JCO.2009.22.1846 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2009.22.1846 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
