Extent of Lumpectomy for Breast Cancer After Diagnosis by Stereotactic Core Versus Wire Localization Biopsy
|
|
|
- Charlotte Wilcox
- 6 years ago
- Views:
Transcription
1 Annals of Surgical Oncology, 6(4): Published by Lippincott Williams & Wilkins 1999 The Society of Surgical Oncology, Inc. Extent of Lumpectomy for Breast Cancer After Diagnosis by Stereotactic Core Versus Wire Localization Biopsy Saif S. Al-Sobhi, MD, Mark A. Helvie, MD, Helen A. Pass, MD, and Alfred E. Chang, MD Background: Stereotactic core biopsy of mammographically defined breast abnormalities is an alternative to wire localization biopsy. The purpose of this study was to evaluate the extent of lumpectomy in patients diagnosed by stereotactic core versus wire localization biopsy. Methods: A total of 67 consecutive patients diagnosed with invasive cancers or ductal carcinoma in situ (DCIS) were retrospectively reviewed. Thirty-four were diagnosed by core biopsy and the remaining 33 by wire localization biopsy. Results: Approximately 65% of patients subsequently had breast-conserving surgical therapy. Seventy-nine percent of patients undergoing wire localization biopsies had positive surgical margins. Achievement of negative surgical margins for lumpectomies performed after wire localization or stereotactic core biopsies was 100% and 89%, respectively, which was not significantly different. However, the total volume of breast tissue removed for breast conservation in patients undergoing lumpectomy after wire localization versus core biopsies was 183 cm 3 and 104 cm 3, respectively, which was significantly different (P.003). Conclusions: Diagnosis by stereotactic core biopsies resulted in less tissue removal to achieve margin-negative lumpectomies for breast conservation. Stereotactic core biopsy is the method of choice for biopsying nonpalpable, suspicious breast lesions. Key Words: Breast cancer Mammography Biopsy Breast conservation. Received August 13, 1998; accepted November 6, From the Division of Surgical Oncology (SSA-S, HAP, AEC), University of Michigan Cancer Center, Ann Arbor, MI, and the Breast Imaging Division (MAH), Department of Radiology, University of Michigan, Ann Arbor, Michigan. Address correspondence to: Alfred E. Chang, 3302 Cancer Center, 1500 E. Medical Center Dr., Ann Arbor, MI ; Fax: The use of annual screening mammography has increased the detection of nonpalpable breast lesions requiring biopsy. It is estimated that approximately 500,000 of these lesions are detected annually in the United States. 1 Most of these mammographic abnormalities prove to be benign, but approximately 15% are found to be malignant. 2 There are different biopsy techniques available for studying these nonpalpable lesions. 3 Stereotactic larger core biopsy, an alternative method to diagnose mammographic abnormalities, was first described in 1990 by Parker and coworkers. 4 This biopsy technique has been adopted by many practitioners. It costs less than a surgical biopsy 5 7 and has been reported to have a high sensitivity and specificity rate in diagnosis. 8,9 However, there are some difficulties in differentiating between atypical ductal hyperplasia and breast carcinoma. Wire localization biopsy of nonpalpable breast lesions detected mammographically has been the gold standard method for the last three decades. It remains the only technique available in centers where stereotactic core facilities are not available. It is more invasive than stereotactic core biopsy, because it requires an operative approach and leaves a scar. In this report, we compared the utility of these biopsy procedures in patients subsequently diagnosed with breast cancer. Specifically, we examined the surgical outcomes of patients who went on to receive lumpectomies for breast conservation. MATERIALS AND METHODS Subjects A total of 337 patients identified as having moderately to highly suspicious mammographic lesions underwent biopsies during the period from April 1996 to April
2 BIOPSY TECHNIQUES FOR BREAST CANCER 331 at the University of Michigan Medical Center. Of those patients, 147 and 190 patients had either stereotactic core or wire localization biopsies, respectively. A total of 67 of these patients (20%) who were found to have invasive or noninvasive cancers made up the group analyzed in this study. Patients diagnosed with lobular carcinoma in situ only were excluded from the study. Four surgical oncologists within the Division of Surgical Oncology performed the wire localization biopsies and definitive surgical procedures. The decision whether to perform a wire localization biopsy versus a stereotactic core biopsy was made jointly by the surgeons in consultation with the mammographers. If a mammographic lesion could be biopsied by either technique, the surgeon presented the options to the individual patient to allow the patient to make an informed choice. In our early experience with the stereotactic core biopsy apparatus, fewer attempts were made by the mammographers to biopsy microcalcifications in contrast to mass lesions. This was not the case in the latter part of the study period after more experience with the technique had been acquired. The decision of what definitive surgical procedure should be performed (breast conservation versus mastectomy) was made by the patient after consultation with the multidisciplinary team of healthcare providers at the Breast Care Center of the University of Michigan Cancer Center. Medical records were reviewed for patient demographics, mammographic findings, pathological characteristics, and the definitive surgical procedures. Wire Localization The skin surface closest to the lesion was chosen, The breast was compressed with the patient in a sitting position, and an alphanumeric fenestrated paddle was placed over the suspicious abnormality. Coordinates were transferred onto the skin, and a 21-gauge hook-wire apparatus (Kopans Spring Hook Localizer Needle, Wire Loc Cook, Bloomington, IN) was inserted into the breast following local anesthesia with 1% lidocaine. After needle placement, orthogonal views were obtained to determine the correct depth. A hook-wire was then deployed through the needle, which was subsequently withdrawn. The hook-wire usually was placed with the reinforced portion within the lesion and the tip of the wire extending beyond it. Craniocaudal and lateral mammographic views were obtained with the hook-wire in place. These views were labeled and submitted with the patient to the surgeon for subsequent operative procedure. The excisional biopsy was performed in an operating room suite using a combination of a local anesthetic and intravenous sedation. Specimen radiography was performed to confirm lesion excision. Stereotactic Core Biopsy The breast was suspended through the aperture of a dedicated prone digital breast biopsy table. Following compression and identification of the suspicious abnormality, stereotactic pairs of images were obtained at 15 off center. The suspicious lesion was identified on both stereotactic images on a video terminal, and its location was determined using the software package employing geometric formulas that assess the relative movement of the index lesion on the stereotactic pairs. A 14- or 11- gauge vacuum-assisted needle (Core Needles Biopsys Mammotome TM needle, Biopsys Medical, Irvine, CA) was then inserted into the compressed breast at the correct coordinates following local anesthesia with lidocaine. A prefire stereotactic pair was obtained to document correct needle location. This was followed by postfire stereotactic pairs after the needle had been advanced mechanically through the lesion. Following confirmation of needle location, vacuum-assisted core biopsy samples of the lesion were obtained. Generally, at least 12 samples were taken. If calcifications were present, a specimen radiograph was obtained to confirm retrieval. Mammographic/pathologic concordance was determined when the pathology results were available. Discordant results led to recommendation for wire-localized surgical biopsy. Local Breast Excision Techniques Wire localization biopsies were performed for diagnostic purposes. A radius of at least 1 cm to 2 cm of breast tissue from the wire was excised. A specimen radiograph was performed to confirm that an adequate sample of tissue had been obtained. In the setting of a confirmed diagnosis of malignancy (i.e., after stereotactic core or wire localization biopsy) a margin-negative lumpectomy was attempted in patients deemed to be candidates for breast conservation. This entailed a wire localization lumpectomy for patients previously diagnosed by stereotactic core biopsy. The technique is similar to that described above in which breast tissue was excised in an effort to achieve negative surgical margins. For patients who had had a prior wire localization biopsy in whom the malignant lesion involved the surgical margin, a re-excision lumpectomy was performed. This procedure involved excising the previous biopsy skin incision in continuity with the underlying breast tissue surrounding the biopsy site, with an effort made not to enter the biopsy cavity. All breast excision specimens were inked for evaluation of the margin status. Tumor cells present at the margin or less than 3 mm away from the margin were considered positive.
3 332 S. S. AL-SOBHI ET AL. TABLE 1. Mammographic and histologic characteristics Core biopsy (n 34) Wire localization (n 33) Characteristic No. (%) No. (%) Mammographic findings Mass 23 (68) 14 (42) Microcalcifications 7 (21) 14 (42) Mass with microcalcifications 4 (11) 4 (12) Architectural distortion 1 (4) Histologic findings IDC 21 (62) 15 (45) IDC DCIS 5 (15) 5 (15) DCIS 6 (18) 13 (39) DCIS with microinvasion 2 (5) DCIS, ductal carcinoma in situ; IDC, infiltrating ductal carcinoma Statistical Analysis Comparisons were analyzed by the Student s t-test. These analyses were performed with the aide of the StatView statistical software (Abacus Concepts, Inc., Berkeley, CA). RESULTS Mammographic Findings, Biopsy Results, and Surgical Therapy A total of 67 patients were evaluated in this study; 34 underwent stereotactic core biopsy and 33 had wire localization biopsy. The median ages of the patients diagnosed by stereotactic core and wire localization biopsy were 59 years (range, years) and 58 years (range, years), respectively, and were not statistically different. Table 1 summarizes the mammographic findings of both groups. In the stereotactic core biopsy group there were 27 (79%) patients with masses with or without microcalcifications and 7 (21%) with microcalcifications only. By contrast, in the wire localization group, 18 (54%) patients presented with masses with or without microcalcifications, 14 (42%) with microcalcifications only, and 1 (4%) with architectural distortion. In the stereotactic core biopsy group, there were 26 (77%) patients who had invasive carcinoma, 5 of whom had an intraductal component (Table 1). Eight patients were diagnosed as having DCIS, with two of these patients having evidence of microinvasion. In the wire localization group, 20 (60%) patients had invasive carcinoma, of whom 5 had an intraductal component; and 13 (39%) patients had DCIS without evidence of microinvasion. The correlation between the mammographic findings and the subsequent biopsy results is summarized in Table 2. Among the 45 patients who presented with a mass with or without evidence of microcalcifications, 40 (89%) were found to have infiltrating ductal carcinoma with or without an intraductal component. By contrast, among the 21 patients who presented with microcalcifications, 16 (76%) were diagnosed with DCIS. The operative procedures performed after biopsy are summarized in Table 3. Among the 34 patients diagnosed by stereotactic core biopsy, 33 patients had their definitive surgical procedure performed at the University of Michigan. Nineteen (57%) of these patients underwent breast conservation; the remaining 14 (43%) had mastectomies. Among the 33 patients diagnosed by wire localization biopsy, six patients had no further surgery at the University of Michigan. Among these six patients, four had DCIS with negative surgical margins and went on to receive radiotherapy; one patient had DCIS with a focally positive surgical margin and had radiotherapy without re-excision; and one patient had positive margins and went on to have surgical therapy at another institution. The remaining 27 patients of the 33 diagnosed by wire localization biopsy had a subsequent surgical procedure performed (see Table 3). Of the 32 patients diagnosed by wire localization biopsy and treated at the University of Michigan, 23 (72%) underwent breast conservation and the remaining nine had mastectomies. There was no significant difference between the two biopsy techniques in the proportion of patients undergoing breast conservation ( 2, P.17). Combining all 65 patients diagnosed and treated at our institution, 42 (65%) of patients underwent breast conservation. Surgical Margins in Patients Undergoing Breast Conservation The status of the surgical margins among the 33 patients undergoing wire localization biopsy was evaluated. TABLE 2. Correlation of mammographic findings with histologic diagnosis Histology Mass (n 37) Microcalcifications (n 21) Mass with microcalcifications (n 8) Architectural distortion (n 1) IDC IDC DCIS DCIS DCIS with microinvasion IDC, infiltrating ductal carcinoma; DCIS, ductal carcinoma in situ.
4 BIOPSY TECHNIQUES FOR BREAST CANCER 333 TABLE 3. Operative procedures performed after biopsy Core biopsy (n 34) Wire localization (n 33) Procedure No. (%) No. (%) Lumpectomy 4 (12) 10 (37) Lumpectomy ALND 15 (45) 6 (22) ALND 2 (7) Simple mastectomy 6 (18) 4 (15) Modified radical mastectomy 8 (24) 5 (19) Total 33 (100) 27 (100) ALND, axillary lymph node dissection. Twenty-six (79%) of these patients had positive surgical margins with the wire localization biopsy specimen. Among these 26 patients, 16 proceeded to have a subsequent re-excision lumpectomy for breast-conserving therapy. Re-excision lumpectomy resulted in negative surgical margins in all 16 (100%) of these latter patients (Table 4). Nineteen patients who had stereotactic core biopsies proceeded to a lumpectomy for breast-conserving surgery. Seventeen (89%) of these 19 patients had negative surgical margins (see Table 4). Among the two patients with positive margins, one underwent a re-excision lumpectomy with negative margins and the other patient had a mastectomy. The mastectomy was performed because a second primary cancer (chondrosarcoma) in addition to an invasive ductal carcinoma was found within the lumpectomy specimen. Extent of Lumpectomy We estimated the extent of lumpectomy by calculating the volume of tissue that was excised in cubic centimeters (cm 3 ). These volumes were determined from the pathology reports, where the sizes of the tissues removed were recorded in three dimensions. For re-excision TABLE 4. Procedure Volume of breast tissue excised in patients undergoing breast conservation No. patients No. negative margins (%) Mean tissue volume (SD) a Wire localization biopsy 24 6 (25) 38 (29) Lumpectomy after wire (100) 143 (80) localization biopsy Combination of Groups (83) 1 and 2 b Lumpectomy after core biopsy (89) 104 (59) c a Volumes expressed in cm 3 standard deviation (SD). b Total volume of tissue removed wire localization biopsy volume subsequent lumpectomy volume c P.0001 compared to Group 1; not significantly different compared to Group 2; P.003 compared to Group 3. lumpectomies, the dimensions of the entire specimen, which excluded the biopsy cavity, were used to calculate the volume. The volumes of tissue excised for patients undergoing breast conservation are summarized in Table 4. The mean volume of tissue removed with the wire localization biopsy was 38 cm 3. For those patients undergoing subsequent lumpectomy, the mean volume was 143 cm 3. We combined the amount of tissue removed in each patient by adding the volume removed at wire localization biopsy plus the subsequent lumpectomy volume to derive a mean total volume of breast tissue removed, which was 183 cm 3. For purposes of comparison, the mean volume of tissue removed by lumpectomy after core biopsy was 104 cm 3. When this latter volume of tissue is compared with the total amount of tissue removed for patients undergoing wire localization biopsy followed by lumpectomy, it is clear that the patients who initially had a core biopsy had significantly less breast tissue removed (P.003). Total Number of Surgical Procedures per Patient The number of surgical procedures performed in the operating room suite per patient was calculated for the groups biopsied by stereotactic core versus wire localization biopsy. For the stereotactic core group, there were 38 surgical procedures performed resulting in a mean SD of For the wire localization biopsy group, there were 61 surgical procedures performed, which resulted in a mean SD of ; and was significantly increased (P.001) compared to core biopsy. For the subset of patients undergoing breast conservation after stereotactic core biopsy, there were 23 surgical procedures performed, resulting in a mean of procedures per patient. For the subset of patients diagnosed by wire localization biopsy who subsequently underwent breast conservation, there were 37 procedures performed, which calculated to a mean of procedures per patient. This was significantly greater (P.0001) than patients having stereotactic core biopsies. DISCUSSION The wide use of screening mammography has resulted in the detection of increasing numbers of nonpalpable breast lesions. The recent recommendations by the National Cancer Institute and American Cancer Society that all women over 40 years of age consider annual screening mammograms will add to these numbers. The management of these lesions varies according to the level of suspicion of malignancy identified by the mammographer.
5 334 S. S. AL-SOBHI ET AL. The College of Radiology Breast Imaging Reporting and Data System (BI-RADS) has devised a useful classification scheme for characterizing mammographic findings that has been widely adopted by mammographers. 10 A mammogram that does not demonstrate an abnormality is classified as BI-RADS 1. A mammogram that identifies a benign finding (i.e., calcified fibroadenoma) is classified as BI-RADS 2. Mammographic lesions that are probably benign (BI-RADS 3) and have a less than 2% probability of being malignant should undergo short-term follow-up mammography rather than biopsy. Suspicious lesions (BI-RADS 4) do not have all the characteristic features of breast cancer but are sufficiently suspicious to recommend biopsy. These lesions generally are considered for stereotactic core biopsy because a definitive benign diagnosis would eliminate the need for a surgical biopsy. Lesions highly suggestive of malignancy (BI-RADS 5) have characteristic features of cancer, and have a high probability of being cancer. Several reports have documented these lesions to be cancers in approximately 80% of cases. 9 The role of stereotactic core biopsy has been controversial in this category of patients. Because of the high index of suspicion of these lesions, some clinicians recommend an open biopsy to obtain a definitive diagnosis, because a nondiagnostic reading of a stereotactic core biopsy would not avoid the need for a subsequent open biopsy Our study, as well as reports by others, suggests that there are several reasons why stereotactic core biopsy may be advantageous for even the highly suspicious lesions From the cost standpoint, Yim et al. 1 and Whittin et al. 15 have reported that stereotactic core biopsy reduced the number of surgical procedures performed per patient. We observed the same phenomenon when analyzing the entire group of patients who had core biopsies compared to wire localization biopsies. This has translated to a cost reduction ranging from $1000 to $2000 per patient for individuals undergoing stereotactic core biopsy. 1,15,16 One area in which this cost reduction is realized is the high incidence of positive surgical margins associated with wire localization biopsies. In our series, we observed a 79% incidence of positive margins in wire localization biopsy specimens. This is consistent with other reported series, in which the finding of positive surgical margins after wire localization biopsy has ranged from 55% to 83%. 1,15,17 No attempt at achieving negative margins, such as the use of touch preps, was made because these were diagnostic procedures. By contrast, the incidence of positive surgical margins for breast lumpectomy after a diagnosis was established by stereotactic core biopsy was significantly lower. In this setting, we observed an 11% incidence of positive margins. Whittin et al. reported a 29% incidence of positive margins in similar patients. 15 In the series reported by Yim et al., where patients with DCIS only were excluded, the incidence of positive margins after stereotactic core biopsy was 6%. 1 These observations indicate that a definitive lumpectomy can be performed as a single procedure in the majority of cases when the diagnosis has been established by core biopsy. The use of touch preparation cytology at the time of lumpectomy may be useful in increasing the rate of negative-margin specimens. 18 In patients who are potential candidates for breastsparing surgery, resection of the primary tumor with the least amount of tissue removal and achievement of negative surgical margins obviously is desirable. We have been able to document that a reduced volume of tissue is removed at the definitive surgical procedure in patients diagnosed by stereotactic core biopsy compared to the total volume of tissue removed in patients diagnosed by wire localization biopsy. The volume of tissue removed for lumpectomy after core biopsy was significantly greater than the volume of the initial wire localization biopsy. Similar results were observed by Whittin et al. 15 Moreover, the volume of tissue removed for patients undergoing re-excision after wire localization biopsy was equivalent to that removed for lumpectomy after core biopsy. This translated to a significantly greater total volume of tissue removed in the wire localization biopsy group than in the core biopsy group. Some clinicians advocate performing definitive lumpectomies or segmental mastectomies on highly suspicious mammographic lesions (BI-RADS 5), which would result in obtaining a diagnosis of malignancy as well as achieving a negative surgical margin in the majority of patients with just one procedure. 17,18 However, 10% to 20% of patients in this group will be found to have no malignancy and thus would have undergone an unnecessarily more aggressive procedure to achieve a diagnosis. The patients determined to have invasive cancers still will require a staging procedure such as an axillary lymph node dissection or lymphatic mapping. Hence, the number of surgical procedures per patient will not be reduced in that subset of patients. Moreover, lymphatic mapping may be compromised by the large volume of breast parenchyma removed at the initial lumpectomy procedure. These issues argue in favor of obtaining a tissue diagnosis up front with the least invasive procedure, such as an image-guided needle or core biopsy. One concern with this approach is the possible implantation of tumor cells along the needle or core track. Longer follow-up will be needed to determine if there is a higher incidence of in-breast recurrences in
6 BIOPSY TECHNIQUES FOR BREAST CANCER 335 patients undergoing breast conservation surgery initially diagnosed by image-guided needle or core biopsy. When we perform a definitive lumpectomy, we excise the skin puncture site and track at the same time whenever possible. This requires close interaction with the mammographer so that core biopsy sites are placed appropriately at locations that will traverse the least amount of tissue to the lesion. Subsequent lumpectomy by the wire localization technique then requires placement of a wire along the previous core or needle biopsy track. Cooperation among surgeons, radiologists, and primary physicians is very important in the management of patients with mammographically detected lesions. Accordingly, the best method for following or biopsying these lesions should be determined by this team. The advantages and disadvantages should be explained to the patient. We favor stereotactic core biopsy for suspicious (BI-RADS 4) and highly suspicious (BI-RADS 5) suspicious mammographic lesions. This approach would result in a reduction of the amount of breast tissue removed at the time of definitive lumpectomy for patients desiring breast conservation, with the advantage of a potentially improved cosmetic result. In addition, stereotactic core biopsy is a more cost-effective method of making a diagnosis of a mammographically detected lesion. Acknowledgments: The authors thank Sally Smith, Patricia Reineman, and Leslie McBride for their efforts in data retrieval and preparation of this manuscript REFERENCES 1. Yim JH, Barton P, Weber B, et al. Mammographically detected breast cancer. Benefits of stereotactic core versus wire localization biopsy. Ann Surg 1996;6: Osteen RT, Cady B, Chmiel JS, et al national survey of carcinoma of the breast by the Commission on Cancer. J Am College of Surg 1994;3: Bear HD. Image-guided breast biopsy how, when, and by whom? (Guest Editorial). J Surg Onc 1997;67: Parker SH, Lovin JD, Jube WE, Luethke JM, Hopper KD, Yakes WF, Burke BJ. Stereotactic breast biopsy with a biopsy gun. Radiol 1990;176: Doyle AJ, Murray KA, Nelson EW, Bragg DG. Selective use of image-guided large-core needle biopsy of the breast: Accuracy and cost-effectiveness. Am J Radiol 1995;2: Berg WA, Krebs TL, Campassi C, Magder LS, Sun CC. Evaluation of 14- and 11-gauge directional, vacuum-assisted biopsy probes and 14-gauge biopsy guns in a breast parenchymal model. Radiol 1997;1: Liberman L, LaTrenta LR, Dershaw DD, et al. Impact of core biopsy on the surgical management of the impalpable breast cancer. Am J Radiol 1997;2: Parker SH, Burbank F, Jackman RJ, et al. Percutaneous large-core breast biopsy: a multi-institutional study. Radiol 1994;2: Nguyen M, McCombs MM, Ghandehari S, et al. An update on core needle biopsy for radiologically detected breast lesions. Cancer 1996;11: American College of Radiology (ACR). Breast imaging reporting and data system (BI-RADS ). 2nd ed. Reston, VA: American College of Radiology, Morrow M. Management of nonpalpable breast lesions. Prin Pract Oncol Updates 1990;4: Morrow M, Schmidt R, Cregger B, Hassett C, Cox S. Preoperative evaluation of abnormal mammographic findings to avoid unnecessary breast biopsies. Arch Surg 1994;10: Sullivan DC. Needle core biopsy of mammographic lesions. Am J Radiol 1994;3: Liberman L, Dershaw DD, Rosen PP, Cohen MA, Hann LE, Abramson AF. Stereotaxic core biopsy of impalpable spiculated breast masses. Am J Radiol 1995;3: Whitten TM, Wallace TW, Bird RE, Turk PS. Image-guided core biopsy has advantages over needle localization biopsy for the diagnosis of nonpalpable breast cancer. Am Surgeon 1997;12: Cross MJ, Evans WP, Peters GN, Cheek JH, Jones RC, Krakos P. Stereotactic breast biopsy as an alternative to open excisional biopsy. Ann Surg Onc 1995;3: Ngai JH, Zelles GW, Rumore GJ, Sawicki JE, Godfrey RS. Breast biopsy techniques and adequacy of margins. Arch Surg 1991;126: Cox CE, Ku NN, Reintgen DS, Greenberg HM, Nicosia SV, Wangensteen S. Touch preparation cytology of breast lumpectomy margins with histologic correlation. Arch Surg 1991;126: Balch CM. The needle biopsy should replace open excisional biopsy... but will the surgeon s role in coordinating breast cancer be diminished? (Editorial). Ann Surg Onc 1995;3:191 2.
Stereotactic 11-Gauge Vacuum- Assisted Breast Biopsy: A Validation Study
 Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Atypical Ductal Hyperplasia and Ductal Carcinoma In Situ as Revealed by Large-Core Needle Breast Biopsy: Results of Surgical Excision
 Marla L. Rosenfield Darling 1 Darrell N. Smith 1 Susan C. Lester 2 Carolyn Kaelin 3 Donna-Lee G. Selland 1 Christine M. Denison 1 Pamela J. DiPiro 1 David I. Rose 1 Esther Rhei 3 Jack E. Meyer 1 Received
Marla L. Rosenfield Darling 1 Darrell N. Smith 1 Susan C. Lester 2 Carolyn Kaelin 3 Donna-Lee G. Selland 1 Christine M. Denison 1 Pamela J. DiPiro 1 David I. Rose 1 Esther Rhei 3 Jack E. Meyer 1 Received
BI-RADS CATEGORIZATION AND BREAST BIOPSY categorization in the selection of appropriate breast biopsy technique is also discussed. Patients and method
 Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
 Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Percutaneous Biopsy of the Breast
 Percutaneous Biopsy of the Breast Expires Tuesday, March 31, 2020 Radiology Brooke A. Caldwell, M.D. Objectives 1. Describe the pros and cons of surgical biopsy and the reasoning behind the development
Percutaneous Biopsy of the Breast Expires Tuesday, March 31, 2020 Radiology Brooke A. Caldwell, M.D. Objectives 1. Describe the pros and cons of surgical biopsy and the reasoning behind the development
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications
 Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Prone table stereotactic breast biopsy
 JYH Hui LK Chan RLM Chan AWL Lau J Lo JCS Chan HS Lam MEDICAL PRACTICE Prone table stereotactic breast biopsy!"#$%&'()*+, The prone table machine is a mammographic X-ray system specially designed for use
JYH Hui LK Chan RLM Chan AWL Lau J Lo JCS Chan HS Lam MEDICAL PRACTICE Prone table stereotactic breast biopsy!"#$%&'()*+, The prone table machine is a mammographic X-ray system specially designed for use
BI-RADS Categorization As a Predictor of Malignancy 1
 Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Poster No.: C-0466 Congress: ECR 2010 Scientific Exhibit
 Up-right stereotactic vacuum-assisted biopsy (UP-VAB) of non palpable breast lesions: Results and correlations with radiological suspicion (BI-RADS classification) Poster No.: C-0466 Congress: ECR 2010
Up-right stereotactic vacuum-assisted biopsy (UP-VAB) of non palpable breast lesions: Results and correlations with radiological suspicion (BI-RADS classification) Poster No.: C-0466 Congress: ECR 2010
Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods
 Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods Nariya Cho, MD 1 Woo Kyung Moon, MD 1 Joo Hee Cha, MD 1 Sun
Sonographically Guided Core Biopsy of the Breast: Comparison of 14-Gauge Automated Gun and 11-Gauge Directional Vacuum-Assisted Biopsy Methods Nariya Cho, MD 1 Woo Kyung Moon, MD 1 Joo Hee Cha, MD 1 Sun
Effective Health Care Program
 Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
STEREOTACTIC BREAST BIOPSY: CORRELATION WITH HISTOLOGY
 3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy
 Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast
 Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
Sonographically-Guided 14-Gauge Core Needle Biopsy for Papillary Lesions of the Breast Eun Sook Ko, MD Nariya Cho, MD Joo Hee Cha, MD Jeong Seon Park, MD Sun Mi Kim, MD Woo Kyung Moon, MD Index terms:
Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up
 Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up Boo-Kyung Han, MD 1 Yeon Hyeon Choe, MD 1 Young-Hyeh Ko, MD 2 Seok-Jin Nam, MD 3 Jung-Han Kim, MD
Stereotactic Core-Needle Biopsy of Non-Mass Calcifications: Outcome and Accuracy at Long-Term Follow-Up Boo-Kyung Han, MD 1 Yeon Hyeon Choe, MD 1 Young-Hyeh Ko, MD 2 Seok-Jin Nam, MD 3 Jung-Han Kim, MD
Treatment options for the precancerous Atypical Breast lesions. Prof. YOUNG-JIN SUH The Catholic University of Korea
 Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Macrobiopsy under X-Ray Guidance
 Macrobiopsy under X-Ray Guidance C. Balleyguier, B. Boyer Radiology Gustave Roussy, Villejuif, France Breast Intervention Imaging Major domain in breast imaging European guidelines recommend a pre surgical
Macrobiopsy under X-Ray Guidance C. Balleyguier, B. Boyer Radiology Gustave Roussy, Villejuif, France Breast Intervention Imaging Major domain in breast imaging European guidelines recommend a pre surgical
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
National Diagnostic Imaging Symposium 2013 SAM - Breast MRI 1
 National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Learning Curve for Stereotactic Breast Biopsy: How Many Cases Are Enough?
 Laura Liberman 1 Catherine L. Benton D. David Dershaw Andrea F. Abramson Linda R. LaTrenta Elizabeth A. Morris Received July 17, 2000; accepted after revision September 7, 2000. Supported by grant C015709
Laura Liberman 1 Catherine L. Benton D. David Dershaw Andrea F. Abramson Linda R. LaTrenta Elizabeth A. Morris Received July 17, 2000; accepted after revision September 7, 2000. Supported by grant C015709
Imaging-Guided Core Needle Biopsy of Papillary Lesions of the Breast
 Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Is stereotactic large-core needle biopsy beneficial prior to surgical treatment in BI-RADS 5 lesions?
 Report Breast Cancer Research and Treatment 86: 165 170, 2004. Ó 2004 Kluwer Academic Publishers. Printed in the Netherlands. Is stereotactic large-core needle biopsy beneficial prior to surgical treatment
Report Breast Cancer Research and Treatment 86: 165 170, 2004. Ó 2004 Kluwer Academic Publishers. Printed in the Netherlands. Is stereotactic large-core needle biopsy beneficial prior to surgical treatment
Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy of the Breast
 Women s Imaging Original Research Jang et al. Sonographic Breast Biopsy Women s Imaging Original Research WOMEN S IMAGING Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy
Women s Imaging Original Research Jang et al. Sonographic Breast Biopsy Women s Imaging Original Research WOMEN S IMAGING Underestimation of Atypical Ductal Hyperplasia at Sonographically Guided Core Biopsy
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation
 Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions
 Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions.
 Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Image guided core biopsies:
 Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Percutaneous Large Core Breast Biopsy
 256 Percutaneous Large Core Breast Biopsy Steve H. Parker, M.D. Background. Surgical excision biopsy is considered by many to be the gold standard for the diagnosis of breast lesions. Fine needle aspiration
256 Percutaneous Large Core Breast Biopsy Steve H. Parker, M.D. Background. Surgical excision biopsy is considered by many to be the gold standard for the diagnosis of breast lesions. Fine needle aspiration
Stereotactic vacuum-assisted breast biopsy under lateral decubitus position
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.1.16 Annals of Surgical Treatment and Research Stereotactic vacuum-assisted breast biopsy under lateral decubitus
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.1.16 Annals of Surgical Treatment and Research Stereotactic vacuum-assisted breast biopsy under lateral decubitus
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
BREAST MRI. VASILIKI FILIPPI RADIOLOGIST CT MRI & PET/CT Departments Hygeia Hospital, Athens, Greece
 BREAST MRI VASILIKI FILIPPI RADIOLOGIST CT MRI & PET/CT Departments Hygeia Hospital, Athens, Greece Breast ΜR Imaging (MRM) Breast MR imaging is an extremely powerful diagnostic tool, that when used in
BREAST MRI VASILIKI FILIPPI RADIOLOGIST CT MRI & PET/CT Departments Hygeia Hospital, Athens, Greece Breast ΜR Imaging (MRM) Breast MR imaging is an extremely powerful diagnostic tool, that when used in
Percutaneous Biopsy and Sentinel Lymphadenectomy: Minimally Invasive. he diagnosis and treatment of nonpalpable. Breast Cancer
 Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Ductal carcinoma in situ, underestimation, ultrasound-guided core needle biopsy
 Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
Ductal carcinoma in situ diagnosed after an ultrasoundguided 14-gauge core needle biopsy of breast masses: Can underestimation be predicted preoperatively? Poster No.: C-0442 Congress: ECR 2010 Type: Scientific
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES
 RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Breast calcifications are important mammographic features in the
 Diagn Interv Radiol 2012; 18:354 359 Turkish Society of Radiology 2012 BREAST IMAGING ORIGINAL ARTICLE Causes of failure in removing calcium in microcalcification-only lesions using 11-gauge stereotactic
Diagn Interv Radiol 2012; 18:354 359 Turkish Society of Radiology 2012 BREAST IMAGING ORIGINAL ARTICLE Causes of failure in removing calcium in microcalcification-only lesions using 11-gauge stereotactic
CNB vs Surgical Excision
 Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Accuracy of Intraoperative Frozen-Section Analysis of Breast Cancer Lumpectomy-Bed Margins
 Accuracy of Intraoperative Frozen-Section Analysis of Breast Cancer Lumpectomy-Bed Margins Juan C Cendán, MD, FACS, Dominique Coco, MD, Edward M Copeland III, MD, FACS BACKGROUND: STUDY DESIGN: RESULTS:
Accuracy of Intraoperative Frozen-Section Analysis of Breast Cancer Lumpectomy-Bed Margins Juan C Cendán, MD, FACS, Dominique Coco, MD, Edward M Copeland III, MD, FACS BACKGROUND: STUDY DESIGN: RESULTS:
Can magnetic resonance imaging obviate the need for biopsy for microcalcifications?
 Original Article Can magnetic resonance imaging obviate the need for biopsy for microcalcifications? Shinya Yamamoto, Takashi Chishima Department of Breast Surgery, Yokohama Rosai Hospital, Yokohama 222-0036,
Original Article Can magnetic resonance imaging obviate the need for biopsy for microcalcifications? Shinya Yamamoto, Takashi Chishima Department of Breast Surgery, Yokohama Rosai Hospital, Yokohama 222-0036,
Radioactive Seed Localization of Nonpalpable Breast Lesions
 Subject: Radioactive Seed Localization of Page: 1 of 7 Last Review Status/Date: March 2017 Radioactive Seed Localization of Description Radioactive seed localization is used to detect nonpalpable breast
Subject: Radioactive Seed Localization of Page: 1 of 7 Last Review Status/Date: March 2017 Radioactive Seed Localization of Description Radioactive seed localization is used to detect nonpalpable breast
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
A Decade of Change: An Institutional Experience with Breast Surgery in 1995 and 2005
 ORIGINAL RESEARCH A Decade of Change: An Institutional Experience with Breast Surgery in 1995 and 2005 Amber A. Guth 1, Beth Ann Shanker 1, Daniel F. Roses 1, Deborah Axelrod 1, Baljit Singh 2, Hildegard
ORIGINAL RESEARCH A Decade of Change: An Institutional Experience with Breast Surgery in 1995 and 2005 Amber A. Guth 1, Beth Ann Shanker 1, Daniel F. Roses 1, Deborah Axelrod 1, Baljit Singh 2, Hildegard
Pitfalls and Limitations of Breast MRI. Susan Orel Roth, MD Professor of Radiology University of Pennsylvania
 Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device
 945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
Feasibility of MRI-guided large-core-needle biopsy of suspiscious breast lesions at 3T
 Eur Radiol (2009) 19: 1639 1644 DOI 10.1007/s00330-009-1310-0 BREAST Nicky H. G. M. Peters Carla Meeuwis Chris J. G. Bakker Willem P. Th. M. Mali Arancha M. Fernandez-Gallardo Richard van Hillegersberg
Eur Radiol (2009) 19: 1639 1644 DOI 10.1007/s00330-009-1310-0 BREAST Nicky H. G. M. Peters Carla Meeuwis Chris J. G. Bakker Willem P. Th. M. Mali Arancha M. Fernandez-Gallardo Richard van Hillegersberg
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Fine-needle aspiration cytology (FNAC) and core needle biopsy
 146 CANCER CYTOPATHOLOGY A Comparison of Aspiration Cytology and Core Needle Biopsy in the Evaluation of Breast Lesions Pieter J. Westenend, M.D., Ph.D. 1 Ali R. Sever, M.D. 2 Hannie J. C. Beekman-de Volder
146 CANCER CYTOPATHOLOGY A Comparison of Aspiration Cytology and Core Needle Biopsy in the Evaluation of Breast Lesions Pieter J. Westenend, M.D., Ph.D. 1 Ali R. Sever, M.D. 2 Hannie J. C. Beekman-de Volder
An evaluation of intraoperative digital specimen mammography versus conventional specimen radiography for the excision of nonpalpable breast lesions
 The American Journal of Surgery (2013) 205, 703-710 Clinical Surgery An evaluation of intraoperative digital specimen mammography versus conventional specimen radiography for the excision of nonpalpable
The American Journal of Surgery (2013) 205, 703-710 Clinical Surgery An evaluation of intraoperative digital specimen mammography versus conventional specimen radiography for the excision of nonpalpable
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy
 Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
Prebiopsy Localization of Nonpalpable Breast Lesions
 ORIGINAL ARTICLE Prebiopsy Localization of Nonpalpable Breast Lesions A. Zulfiqar, MMed* v. Param, DMRD** F.A. Meah, FRACS* s. Nair, FRCS** M.A. Siti-Aishah, DCP* A. N orizan, DCP** * Departments of Radiology,
ORIGINAL ARTICLE Prebiopsy Localization of Nonpalpable Breast Lesions A. Zulfiqar, MMed* v. Param, DMRD** F.A. Meah, FRACS* s. Nair, FRCS** M.A. Siti-Aishah, DCP* A. N orizan, DCP** * Departments of Radiology,
Breast ultrasound appearances after Mammotome vacuumassisted
 Breast ultrasound appearances after Mammotome vacuumassisted biopsy. Poster No.: C-1924 Congress: ECR 2011 Type: Educational Exhibit Authors: R. Patel 1, G. R. Kaplan 2 ; 1 London/UK, 2 Herts/UK Keywords:
Breast ultrasound appearances after Mammotome vacuumassisted biopsy. Poster No.: C-1924 Congress: ECR 2011 Type: Educational Exhibit Authors: R. Patel 1, G. R. Kaplan 2 ; 1 London/UK, 2 Herts/UK Keywords:
Here are examples of bilateral analog mammograms from the same patient including CC and MLO projections.
 Good afternoon. It s my pleasure to be discussing Diagnostic Breast Imaging over the next half hour. I m Wei Yang, Professor of Diagnostic Radiology and Chief, the Section of Breast Imaging as well as
Good afternoon. It s my pleasure to be discussing Diagnostic Breast Imaging over the next half hour. I m Wei Yang, Professor of Diagnostic Radiology and Chief, the Section of Breast Imaging as well as
Amammography report is a key component of the breast
 Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 2010 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 2010 Produced by: BreastScreen Victoria Coordination Unit Level 1, 31 Pelham Street, Carlton South
BreastScreen Victoria Annual Statistical Report 2010 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 2010 Produced by: BreastScreen Victoria Coordination Unit Level 1, 31 Pelham Street, Carlton South
Atypical And Suspicious Categories In Fine Needle Aspiration Cytology Of The Breast
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 15, Issue 1 Ver. III (October. 216), PP 57-61 www.iosrjournals.org Atypical And Suspicious Categories in
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 15, Issue 1 Ver. III (October. 216), PP 57-61 www.iosrjournals.org Atypical And Suspicious Categories in
Breast imaging in general practice
 Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
COPE Library Sample
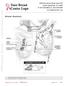 Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass
 Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
PAPER. Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy
 PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
Stereotactic Biopsy of the Breast Using an Upright Unit, a Vacuum-Suction Needle, and a Lateral Arm-Support System
 Dianne Georgian-Smith 1,2 Carl D Orsi 3 Ellen Morris 4 Crandon F. Clark, Jr. 5 Ellen Liberty 3 Constance D. Lehman 1 Received January 8, 2001; accepted after revision October 8, 2001. Presented at the
Dianne Georgian-Smith 1,2 Carl D Orsi 3 Ellen Morris 4 Crandon F. Clark, Jr. 5 Ellen Liberty 3 Constance D. Lehman 1 Received January 8, 2001; accepted after revision October 8, 2001. Presented at the
Metachronic solitary breast metastasis from renal cell carcinoma: case report
 Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, cont
 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Risk of Upgrade
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Risk of Upgrade
Stereotactic vacuum-assisted biopsy (SVAB) of Nonpalpable Breast Microcalcifications: Advantage of clip placement (Prospective study)
 Department of Radiology, University of Ulm Director: Prof. Dr. med. HJ Brambs Stereotactic vacuum-assisted biopsy (SVAB) of Nonpalpable Breast Microcalcifications: Advantage of clip placement (Prospective
Department of Radiology, University of Ulm Director: Prof. Dr. med. HJ Brambs Stereotactic vacuum-assisted biopsy (SVAB) of Nonpalpable Breast Microcalcifications: Advantage of clip placement (Prospective
CURRENT METHODS IN IMAGE GUIDED BREAST BIOPSY
 CURRENT METHODS IN IMAGE GUIDED BREAST BIOPSY Stuart Silver April 24, 2004 OBJECTIVES Review development of current techniques Discuss stereotactic breast biopsy Discuss US guided breast biopsy 1 OBJECTIVES
CURRENT METHODS IN IMAGE GUIDED BREAST BIOPSY Stuart Silver April 24, 2004 OBJECTIVES Review development of current techniques Discuss stereotactic breast biopsy Discuss US guided breast biopsy 1 OBJECTIVES
Original Report. Mucocele-Like Tumors of the Breast: Mammographic and Sonographic Appearances. Katrina Glazebrook 1 Carol Reynolds 2
 Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Department of Radiology, Research Institute of Radiological Science, Yonsei University, College of Medicine, Seodaemun-gu, Seoul, Republic of Korea
 The British Journal of Radiology, 85 (2012), e349 e356 Comparison of the underestimation rate in cases with ductal carcinoma in situ at ultrasound-guided core biopsy: 14-gauge automated core-needle biopsy
The British Journal of Radiology, 85 (2012), e349 e356 Comparison of the underestimation rate in cases with ductal carcinoma in situ at ultrasound-guided core biopsy: 14-gauge automated core-needle biopsy
Breast Health and Imaging Glossary
 Contact: Lorna Vaughan HerSpace Breast Imaging & Biopsy Associates 300 State Route 35 South W. Long Branch, NJ 07764 732-571-9100, ext. 104 lorna@breast-imaging.com Breast Health and Imaging Glossary Women
Contact: Lorna Vaughan HerSpace Breast Imaging & Biopsy Associates 300 State Route 35 South W. Long Branch, NJ 07764 732-571-9100, ext. 104 lorna@breast-imaging.com Breast Health and Imaging Glossary Women
Ana Sofia Preto 19/06/2013
 Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 29 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 29 Produced by: BreastScreen Victoria Coordination Unit Level, 3 Pelham Street, Carlton South Victoria
BreastScreen Victoria Annual Statistical Report 29 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 29 Produced by: BreastScreen Victoria Coordination Unit Level, 3 Pelham Street, Carlton South Victoria
Ductal Carcinoma in Situ (DCIS)
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Ductal Carcinoma in Situ (DCIS) Ductal Carcinoma in Situ DCIS Versions 2002 2017: Audretsch / Blohmer / Brunnert / Budach /
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Ductal Carcinoma in Situ (DCIS) Ductal Carcinoma in Situ DCIS Versions 2002 2017: Audretsch / Blohmer / Brunnert / Budach /
Resection Margins in Breast Conserving Surgery. Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland
 Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
DCIS of the Breast--MRI findings with mammographic correlation.
 DCIS of the Breast--MRI findings with mammographic correlation. Poster No.: C-1560 Congress: ECR 2013 Type: Educational Exhibit Authors: N. B. Ibrahim, P. Morris, S. ANANDAN; Burlington, MA/US Keywords:
DCIS of the Breast--MRI findings with mammographic correlation. Poster No.: C-1560 Congress: ECR 2013 Type: Educational Exhibit Authors: N. B. Ibrahim, P. Morris, S. ANANDAN; Burlington, MA/US Keywords:
Original Article Breast Imaging
 Original Article Breast Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.697 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):697-703 Percutaneous Ultrasound-Guided Vacuum-Assisted Removal versus
Original Article Breast Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.697 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):697-703 Percutaneous Ultrasound-Guided Vacuum-Assisted Removal versus
Needle core biopsy characteristics identify patients at risk of compromised margins in breast conservation surgery
 & 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org Needle core biopsy characteristics identify patients at risk of compromised margins in breast conservation surgery Mary
& 2008 USCAP, Inc All rights reserved 0893-3952/08 $30.00 www.modernpathology.org Needle core biopsy characteristics identify patients at risk of compromised margins in breast conservation surgery Mary
Mammography and Subsequent Whole-Breast Sonography of Nonpalpable Breast Cancers: The Importance of Radiologic Breast Density
 Isabelle Leconte 1 Chantal Feger 1 Christine Galant 2 Martine Berlière 3 Bruno Vande Berg 1 William D Hoore 4 Baudouin Maldague 1 Received July 11, 2002; accepted after revision October 28, 2002. 1 Department
Isabelle Leconte 1 Chantal Feger 1 Christine Galant 2 Martine Berlière 3 Bruno Vande Berg 1 William D Hoore 4 Baudouin Maldague 1 Received July 11, 2002; accepted after revision October 28, 2002. 1 Department
Three-dimensional ultrasound-validated large-core needle biopsy: is it a reliable method for the histological assessment of breast lesions?
 Ultrasound Obstet Gynecol 2004; 23: 393 397 Published online 24 February 2004 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1001 Three-dimensional ultrasound-validated large-core
Ultrasound Obstet Gynecol 2004; 23: 393 397 Published online 24 February 2004 in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/uog.1001 Three-dimensional ultrasound-validated large-core
S. Murgo, MD. Chr St-Joseph, Mons Erasme Hospital, Brussels
 S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
S. Murgo, MD Chr St-Joseph, Mons Erasme Hospital, Brussels? Introduction Mammography reports are sometimes ambiguous and indecisive. ACR has developped the BIRADS. BIRADS consists of a lexicon in order
Detailed Program of the second BREAST IMAGING AND INTERVENTIONS PROGRAM am am : Clinician s requirements from breast imaging
 Detailed Program of the second BREAST IMAGING AND INTERVENTIONS PROGRAM 2012 Day one, 2 nd November BREAST IMAGING AND INTERVENTIONS PROGRAM 2012 9.00 AM 9.10 am Introduction 9.10 am - 9.30 am : Clinician
Detailed Program of the second BREAST IMAGING AND INTERVENTIONS PROGRAM 2012 Day one, 2 nd November BREAST IMAGING AND INTERVENTIONS PROGRAM 2012 9.00 AM 9.10 am Introduction 9.10 am - 9.30 am : Clinician
Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma
 Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds
 215 Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds ratio 719 (100) 305(100) Shape Oval 445 (61.9) 019
215 Table 1. Classification of US Features Based on BI-RADS for US in Benign and Malignant Breast Lesions US Features Benign n(%) Malignant n(%) Odds ratio 719 (100) 305(100) Shape Oval 445 (61.9) 019
Ductal Carcinoma-in-Situ: New Concepts and Controversies
 Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery
 Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery Goal The goal of the Breast Surgery rotation is to develop the knowledge, skills and attitudes necessary to evaluate,
Educational Goals and Objectives for Rotations on: Breast, Wound and Plastic Surgery Goal The goal of the Breast Surgery rotation is to develop the knowledge, skills and attitudes necessary to evaluate,
Radioactive Seed Localization of Nonpalpable Breast Lesions
 Radioactive Seed Localization of Nonpalpable Breast Lesions Policy Number: 6.01.57 Last Review: 11/2017 Origination: 11/2016 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Radioactive Seed Localization of Nonpalpable Breast Lesions Policy Number: 6.01.57 Last Review: 11/2017 Origination: 11/2016 Next Review: 11/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
The Breast Imaging Reporting and Data System (BI-RADS) was
 710 Evaluation of Breast Imaging Reporting and Data System Category 3 Mammograms and the Use of Stereotactic Vacuum-Assisted Breast Biopsy in a Nonacademic Community Practice Angela Mendez, M.D. Fernando
710 Evaluation of Breast Imaging Reporting and Data System Category 3 Mammograms and the Use of Stereotactic Vacuum-Assisted Breast Biopsy in a Nonacademic Community Practice Angela Mendez, M.D. Fernando
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM)
 Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Assessment of extent of disease: digital breast tomosynthesis (DBT) versus full-field digital mammography (FFDM) Poster No.: C-1237 Congress: ECR 2012 Type: Scientific Paper Authors: N. Seo 1, H. H. Kim
Medical Audit of Diagnostic Mammography Examinations: Comparison with Screening Outcomes Obtained Concurrently
 Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology
 Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Underestimation of cancer in case of diagnosis of atypical ductal hyperplasia (ADH) by vacuum assisted core needle biopsy
 reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
PURPOSE IMAGE-GUIDANCE MODALITIES IMAGE-GUIDED BREAST BIOPSY. US-Techniques. Ultrasound. US guided NLOBB. TH. Helbich
 IMAGE-GUIDED BREAST BIOPSY PURPOSE TH. Helbich Department of Radiology Division of Molecular & Gender Imaging Medical University of Vienna Imaging techniques Interventional procedures Quality management
IMAGE-GUIDED BREAST BIOPSY PURPOSE TH. Helbich Department of Radiology Division of Molecular & Gender Imaging Medical University of Vienna Imaging techniques Interventional procedures Quality management
Atypical proliferative lesions diagnosed on core biopsy - 6 year review
 Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions
 Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions Poster No.: C-2870 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Pozzetto, L. Camera,
Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions Poster No.: C-2870 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Pozzetto, L. Camera,
A E K Ibrahim, A C Bateman, J M Theaker, J L Low, B Addis, P Tidbury, C Rubin, M Briley, G T Royle
 J Clin Pathol 2001;54:121 125 121 Departments of Histopathology and Cytopathology,, Tremona Road,, SO16 6YO, UK A E K Ibrahim A C Bateman J M Theaker B Addis P Tidbury Medical Statistics and Computing,
J Clin Pathol 2001;54:121 125 121 Departments of Histopathology and Cytopathology,, Tremona Road,, SO16 6YO, UK A E K Ibrahim A C Bateman J M Theaker B Addis P Tidbury Medical Statistics and Computing,
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2014 September; 17(3): 265-269 Absence of Residual Microcalcifications in Atypical Ductal Hyperplasia Diagnosed via Stereotactic Vacuum-Assisted
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2014 September; 17(3): 265-269 Absence of Residual Microcalcifications in Atypical Ductal Hyperplasia Diagnosed via Stereotactic Vacuum-Assisted
Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery
 Last Review Status/Date: December 2014 Page: 1 of 6 Intraoperative Assessment of Surgical Description Breast-conserving surgery as part of the treatment of localized breast cancer is optimally achieved
Last Review Status/Date: December 2014 Page: 1 of 6 Intraoperative Assessment of Surgical Description Breast-conserving surgery as part of the treatment of localized breast cancer is optimally achieved
Radiologic-pathologic correlation of the mammographic findings retrospectively detected in inflammatory breast cancer: usefulness in clinical practice
 Radiologic-pathologic correlation of the mammographic findings retrospectively detected in inflammatory breast cancer: usefulness in clinical practice Francesca Caumo, Erminia Manfrin, Franco Bonetti,
Radiologic-pathologic correlation of the mammographic findings retrospectively detected in inflammatory breast cancer: usefulness in clinical practice Francesca Caumo, Erminia Manfrin, Franco Bonetti,
