Protocol. This trial protocol has been provided by the authors to give readers additional information about their work.
|
|
|
- Letitia Janis Howard
- 6 years ago
- Views:
Transcription
1 Protocol This trial protocol has been provided by the authors to give readers additional information about their work. Protocol for: Quintero E, Castells A, Bujanda L, et al. Colonoscopy versus fecal immunochemical testing in colorectal-cancer screening. N Engl J Med 2012;366:
2 Colorectal cancer screening in the average-risk population: a pragmatic, multicentre, randomised, controlled trial comparing colonoscopy and faecal immunochemical testing (COLONPREV Study) Grupo Cooperativo para el Cribado del Cáncer Colorrectal en España Study Protocol Date: June 2 nd, 2008
3 INDEX 1. EXECUTIVE SUMMARY 3 2. BACKGROUND AND CURRENT STATUS OF THE ISSUE 4 3. OBJECTIVES Primary objective Secondary objectives Additional objectives 7 4. STUDY METHODOLOGY Study type Scope Target population Study groups, randomisation, and stratification Sample size calculation Processes of selecting and inviting the population to be screened Determination of faecal occult blood Technical characteristics of colonoscopies Quality assurance program DEVELOPMENT OF THE STUDY Screening phases Organisation and management of the project DEFINITIONS Classification of colorectal polyps Treatment of malignant polyps Classification of colorectal cancer STATISTICAL ANALYSIS PLAN CHRONOGRAM ETHICAL QUESTIONS RESEARCH PROJECT TEAM REFERENCES 24 2
4 1. EXECUTIVE SUMMARY Introduction Colorectal cancer (CRC) is one of the most common malignancies in Western nations, and the second most common in Spain after lung cancer in men and breast cancer in women. Its incidence is estimated at 25,000 new cases per year, and it is the second leading cause of cancer death. Although the efficacy of CRC screening in the prevention of this cancer is well established, the most appropriate procedure for screening has not yet been identified. Primary objective To measure CRC-specific mortality at 10 years after screening using biennial faecal immunochemical testing (FIT) compared to screening by one-time colonoscopy in an average-risk population (asymptomatic individuals aged years with no personal or family history of CRC). Study design A pragmatic, non-inferiority, multicentre, randomised, controlled trial in eight Autonomous Regions of Spain (Aragon, Canary Islands, Catalonia, Galicia, Madrid, Murcia, Basque Country, and Valencia). Methodology Inclusion criteria: Asymptomatic men and women between the ages of 50 and 69. Exclusion criteria: 1) Having previously undergone CRC screening within the prescribed period; 2) Belonging to high-risk groups due to family history (hereditary nonpolyposis colorectal cancer, familial adenomatous polyposis, other hereditary polyposis syndromes, first-degree relatives with CRC) or personal history (inflammatory bowel disease, adenoma, or prior CRC); 3) Symptoms suggestive of colorectal disease; 4) Having undergone a total colectomy; or 5) Individuals suffering from a serious illness. Study groups Group 1: Screening using biennial FIT (latex agglutination, OC-Sensor, cut-off point: 75 ng Hb/ml), and performance of colonoscopy in patients with a positive result. Group 2: Screening using one-time colonoscopy. The study design allowed for cross-over between both screening strategies. Sample size calculation With an alpha risk of and a beta risk of 0.20, using one-sided test of proportions, 27,749 subjects are required in each trial arm (total: 55,498) accepting a non-inferiority condition if the absolute difference was below 1.6 in the CRCspecific mortality rate at 10 years according to the intention to screen analysis (primary objective of the study). 3
5 2. BACKGROUND AND CURRENT STATUS OF THE ISSUE Colorectal cancer (CRC) is the second most common cause of cancer death in Spain, accounting for more than 11,000 deaths annually. Its rate of incidence makes it the second most common cancer after lung cancer in men and breast cancer in women, but it is the most common cancer if figures for both genders are combined, with more than 25,000 new cases detected each year (1). The mean survival rate for CRC in Spain is only 48% at 5 years after diagnosis (2). This may be because diagnosis is made late, in most cases as a result of a lack of screening programmes. Several prestigious medical societies and clinical guidelines based on scientific evidence recommend screening for all individuals over the age of 50 even if no additional risk factors are present, as well as for members of high-risk population groups (hereditary CRC syndromes, individuals with first-degree relatives with CRC, and patients suffering from inflammatory bowel disease) (3-12). For screening in high-risk populations, the strategy of choice is colonoscopy, performed at various intervals depending on the clinical situation (6,12). However, it is not known which screening method (annual or biennial faecal occult blood testing [FOBT], sigmoidoscopy every 5 years, or colonoscopy every 10 years) is the most suitable for the average-risk population. Of all the possible strategies, the most evaluated to date is annual or biennial FOBT screening. Several randomised controlled trials have shown that FOBT screening with a chemical test (guaiac) reduced mortality from CRC by approximately 15-30% (13-15) and also reduced its incidence (16).However, this method has been disputed because of its low sensitivity, with a detection rate of 30-50% in a single round of screening for CRC (15.17), and of less than 20% for advanced adenoma (18,19). Other disadvantages of screening with the guaiac-based FOBT method are that it needs to be repeated every 1-2 years, that it requires dietary restrictions to ensure the reliability of the test, and that three consecutive samples must be collected, thereby greatly reducing compliance. On the other hand, there are faecal immunochemical tests (FIT) that are more sensitive than chemical methods (20). Such methods specifically detect human haemoglobin, and therefore do not require dietary restrictions and only need a single sample to be taken. However, they have been insufficiently tested in Western countries, and there are no studies on the costeffectiveness of CRC screening using this procedure. In the past 15 years several pilot studies have been carried out in Spain for early detection of CRC in average-risk populations (21-25). Most of them used the chemical FOBT method as a screening test, followed by colonoscopy in individuals with a positive result. In total, these studies included more than 12,000 participants, with an average participation rate of 56% and an average detection rate of early stage CRC of 80%. Although these studies are not comparable from the methodological point of view, and were performed at different times, the results suggest an acceptable level of participation in the Spanish population, and high efficacy in the early detection of CRC. However, no studies have been conducted in Spain assessing the efficacy of screening in terms of mortality or incidence over the long-term. In a recent study conducted in Tenerife (25), the acceptance, efficacy, and costeffectiveness of a new FIT (latex agglutination, OC-Light ) was compared to the hemofec chemical test for the detection of advanced adenoma and CRC. The study showed that the immunological method is more sensitive than the chemical test for detection of advanced adenoma (51% vs. 18%), CRC (100% vs. 52%) or both (57% vs. 22%). Specificity with the immunological method was 97% for advanced adenoma, 93% for CRC, and 95% for both, while with the chemical test it was 97% for 4
6 either advanced adenoma or CRC, and 98% for both. This study also showed that the probability of detecting advanced cancers (advanced adenoma or CRC) in individuals with a positive immunological test (OR: 13; 95% CI: ) was four times higher than that for those in whom the chemical test was positive (OR: 3.17; 95% CI: ). The immunological method was also more cost-effective than the chemical test in the detection of CRC or advanced adenoma. The chemical FOBT test achieved a cost-effectiveness ratio of 3.573/QALY gained, reducing CRC-caused mortality by 20%, while for the immunological test the ratio was 2,224/QALY gained, with a reduction in mortality of 52%. These data suggest that the FIT should replace the chemical method in future CRC screening campaigns in average-risk population. Colonoscopy is the most accurate method that exists for the early detection and prevention of CRC. Although studies evaluating the effect of screening with this test on CRC-caused mortality in average-risk populations have not yet been published, its implementation is recommended based on the following evidence: 1) studies have demonstrated that colonoscopy with polypectomy reduces the incidence of CRC by 40-90% (27,28); 2) At least two case-control studies suggest that screening by flexible sigmoidoscopy significantly reduces the risk of death from distal CRC (29,30), an effect that lasts for more than 5 years (30) which has enabled extrapolation of its effectiveness to colonoscopy; 3) The prevalence of adenomas in cross-sectional studies of screening by colonoscopy is twice that observed for sigmoidoscopy (18,19,31,32), with colonoscopy also found to be more sensitive than the barium enema or virtual colonoscopy for detecting polyps and CRC (26); 4) Approximately two out of three patients with advanced cancers of the proximal colon do not show neoplasia distal to the splenic flexure, meaning that it would not be detectable in screening by sigmoidoscopy (33,34). This is particularly relevant if one considers that 40% of CRCs are located proximal to the splenic flexure (35). An additional benefit of colonoscopy every 10 years compared to other screening strategies in an average-risk population is that it allows a long period of protection, which can help improve compliance in the population. It also facilitates diagnosis and treatment in one session, which decreases the risk of the loss of patients to follow-up that occurs with tests that are purely diagnostic. The primary limiting factors for the use of colonoscopy in screening an average-risk population are its invasive nature, including a possible risk of potentially serious complications such as perforation or post-polypectomy bleeding (1-2 per 2,000 examinations), and a higher cost than other screening methods such as the FOBT test. Despite the proven beneficial effect of secondary prevention on morbidity and mortality from CRC, there are significant obstacles that hinder the implementation of large-scale CRC screening programmes. First, there is still no agreement as to what constitutes an optimal screening strategy. Secondly, there is little compliance with them by the target population. This is due mainly to a significant lack of information among the target population, and among healthcare managers and staff themselves (36-38). Finally, the organisation and resources needed to ensure the safety and efficacy of a programme of this nature are not currently available. An essential requirement for the implementation of any population screening programme for a particular disease is to be cost-effective. Several studies have confirmed that CRC screening is cost-effective regardless of the strategy applied (39-41), with the cost in terms of quality-adjusted life years (QALY) being lower than screening for other cancers such as breast or cervical cancer (40). These findings were corroborated in a recent analysis by the Evaluation and Planning Unit of the Canary Islands Health Service (unpublished data), which found that the costs of CRC screening using FIT or colonoscopy every 10 years would be significantly lower 5
7 ( 2,500/QALY and 2,300/QALY, respectively) than screening for breast ( 18,489/QALY), cervical ( 18,646/QALY) or prostate cancers ( 12,647/QALY). It is worth noting that the National Institute for Health and Clinical Excellence (NICE) has recently established that any health intervention that costs less than 30,000/QALY should be considered to be very acceptable from the standpoint of costeffectiveness (42) and has, therefore, recommended its implementation. Given that CRC is a high-priority health issue, and that sufficient evidence exists to show that it is a preventable disease with reasonable economic costs if diagnosed early, the Council of the European Union established guidelines in 2003 (43) so that population screening for CRC would be included as a priority in the health plans of member states. For that reason, the national health plan of the Spanish Ministry of Health and Consumer Affairs includes population screening for CRC as a priority as part of its comprehensive cancer plan (PICA), which is to be implemented before 2007 (43). The Spanish Association of Gastroenterology (AEG) believes that, in order to reduce the mortality and incidence of CRC in Spain, various actions must be taken, among which are publicising the CCR prevention strategies, promotion of their implementation, establishment of mechanisms for assessment, improvement of the efficiency and quality of care levels involved and promotion of comprehensive care for patients with this cancer. This Association, therefore, proposes to conduct a multicentre, controlled study with a scope that covers several Autonomous Regions to establish the efficacy and efficiency of the two principal screening options in the average-risk population. 6
8 3. OBJECTIVES 3.1. Primary objective To assess CRC-specific mortality at 10 years after screening using a FIT method biennially compared to screening by one-time colonoscopy in an average-risk population (asymptomatic individuals aged with no personal or family history of CRC) Secondary objectives To compare diagnostic yield and detection rate of CRC and/or advanced adenomas in each screening strategy at the completion of the first round. To compare the participation rate in each screening strategy at the completion of the first round, and identify the factors influencing it (i.e. demographics, personal and familial characteristics, socio-economic status, etc.). To compare overall diagnostic yield and detection rate of CRC and/or advanced adenomas in each screening strategy at 10 years. To compare the overall adherence rate in each screening strategy at 10 years, and identify the factors influencing it. To assess the cost-effectiveness of each screening strategy. To assess the rate of serious complications in each screening strategy, both at the completion of the first round and overall at 10 years Additional objectives Each Autonomous Region, hospital, and/or health centre participating in the study can propose additional objectives to be performed in its individual data sets. Any proposal should be approved by the Executive Committee of the COLONPREV study. 7
9 4. STUDY METHODOLOGY 4.1. Study type Pragmatic, non-inferiority, multicentre, randomised and controlled Scope The study will be conducted in eight Autonomous Regions: Aragon, Canary Islands, Catalonia, Valencia, Galicia, Madrid, Murcia and Basque Country. The following centres will participate: Hospital Clínico Lozano Blesa (Zaragoza), Hospital Universitario de Canarias (Tenerife),Hospital Clinic de Barcelona, Hospital del Mar (Barcelona), Consorcio Hospitalario de Castelló, Hospital la Fe (Valencia), Complexo Hospitalario Universitario de Vigo, Complexo Hospitalario Universitario de Ourense, Hospital 12 de Octubre (Madrid), Hospital de la Princesa (Madrid), Hospital Puerta de Hierro (Madrid), Hospital Fundación de Alcorcón, Hospital Clínico San Carlos (Madrid), Hospital Universitario Virgen de la Arrixaca (Murcia), Hospital Reina Sofía (Murcia), Hospital de Donostia (San Sebastian), and Instituto Oncológico, Obra Social Kutxa, San Sebastián Target population Inclusion criteria: Asymptomatic men and women between 50 and 69 years of age. This cutoff of age is the recommended by the Spanish Screening Network for the implementation phase of the Spanish CRC screening program. Thereafter, it is planned to increase this age cutoff to 74 years of age when the screening program will be extended to the whole country. Permanent exclusion criteria: All individuals who meet any of the following conditions will be permanently excluded: Personal history of inflammatory bowel disease, colorectal polyps, colorectal adenoma or CRC. Family history of familial adenomatous polyposis syndromes or other hereditary polyposis syndromes, hereditary nonpolyposis colorectal cancer (diagnosed by the presence of germline mutation in DNA repair genes and/or meeting the Amsterdam II criteria), 2 or more first-degree relatives with CRC or 1 first-degree relative with CRC diagnosed before the age of 60. Severe comorbidity that involves a poor short-term prognosis (disease with a mean life expectancy of less than 5 years) or chronic disease that involves major limitation of physical activity (performance status 2). Individuals who have had a total colectomy. Temporary exclusion criteria: All individuals who meet any of the following conditions will be temporarily excluded: Those who have undergone any of the examinations used in CRC screening, regardless of the reason, within the periods specified: history of FOBT screening in the past 2 years, or sigmoidoscopy or colonoscopy within the past 5 years (as long as its validity is documented) (to avoid this eventuality we will seek to conduct the study in a healthcare setting in which the population has not been screened previously). Such individuals may enter the study after the time periods mentioned have expired. 8
10 Those showing symptoms suggestive of colorectal disease (rectal bleeding, altered frequency of bowel movements, constitutional symptoms, anaemia). These individuals may enter the study once their condition has been studied and a colorectal cancer or other pathology that would constitute a cause of permanent disqualification has been excluded, and if any of the abovementioned tests were performed, once the periods mentioned in the previous section have expired Study groups, randomisation, and stratification Asymptomatic men and women aged 50 to 69 years from each participating Autonomous Region will be identified through the corresponding Community Health Registry (CHR) for enrolment into this study. Randomisation will be carried out prior to invitation, with computer-generated lists in blocks of 4 (block randomisation) from the list of health cards, after having previously grouped individuals by household (specified by street address, floor, and apartment number) (see Processes of selecting and inviting the population to be screened section). All eligible patients will be randomised (1:1 ratio) to the two study groups: Group 1: Screening by biennial FIT (latex agglutination, OC-Sensor, cut-off point: 75 ng Hb/ml), and colonoscopy (after no more than 1 month) for patients with a positive result. Determination of FIT will be made using a single faecal sample, without dietary restriction or interruption of normal treatment of the individual, although the habitual use (>1 month) or recent use (last 7-15 days) of NSAIDs, aspirin, anti-platelet drugs and anticoagulants will be recorded. Group 2: Screening by one-time colonoscopy. The ongoing use (>1 month) or recent use (last 7-15 days) of NSAIDs, aspirin, anti-platelet drugs and anticoagulants will also be recorded. Individuals in Group 1 or Group 2 who do not agree to the type of testing assigned to them will be able to receive the alternative test, and must still be followed up in order to carry out efficacy analysis according to the intention to screen analysis. Information on the long-term status of individuals in Group 1 or Group 2 who do not agree to participate in the study will be obtained through population-based registries at the completion of the trial in order to assess efficacy according to the intention to screen analysis Sample size calculation Considerations for calculation of the sample Since there are no study examining the effect of screening with the strategies proposed in our trial on CRC-caused mortality, the calculation of the sample in this case must be based on hypothetical studies of cost-effectiveness that analyse the expected reduction in risk of mortality with biennial FIT or colonoscopy every 10 years. Furthermore, the calculation should be adjusted, when possible, to the local conditions where the strategies are to be implemented. In that sense, it is important to note that no study on this subject have yet been published in Spain. Recently, the Evaluation and Planning Unit of the Canary Islands Health Service has conducted a study of this type based on real data for sensitivity and specificity of the tests in our setting. For a hypothetical population of 100,000 asymptomatic individuals aged 50, the estimated mortality reduction brought about by FIT is 51%, 9
11 and involves a cost of 2,101/QALY. For the strategy of colonoscopy, the estimate is a reduction in mortality of 75% at a cost of 2,188/QALY. With an alpha risk of and a beta risk of 0.20 using one-sided test of proportions, 27,749 subjects are required in each arm of the clinical trial (total: 55,498) accepting a non-inferiority condition if the absolute difference was below 1.6 in the CRC-specific mortality rate at 10 years according to the intention to screen analysis and with an expected overall compliance of 30%. Estimates of recruitment by Autonomous Region According to the established sample size, the number of individuals to be recruited in each Autonomous Region is 6, Processes of selecting and inviting the population to be screened In each Autonomous Region, randomisation will be done prior to sending the invitation letter (Zelen s design) in order to properly assess the participation in each screening group and perform the intention to screen analysis of the results. The selection process will be the same as the one used in the Nottingham study (14), in which compliance with the programme reached 60%. Briefly, target population will be identified from the Community Health Registry (CHR) of each Autonomous Region. The CHR is based on the population registry, and includes unique identification for each person, such as name, date of birth, social security number, and contact address, and it is updated regularly to account for population migration, deaths and changes in personal details This list will be refined using cancer registries or other sources of information (primary care medical records, hospital databases, etc.) in order to eliminate individuals who meet exclusion criteria (i.e. CRC and colorectal adenoma) or who have died. Prior to randomisation, individuals will be clustered by household. With such an approach, it is hoped to ensure that all individuals in one household will be assigned to the same study group. All individuals will receive an initial, pre-invitation letter by mail (which may be signed by their primary care doctor or an area specialist, or the person responsible for the Autonomous Regions screening programme) with information regarding the relevance of CRC as a health problem, the possibility of preventing it by means of screening, and the impending start up of a pilot programme (presentation letter), along with an informative leaflet which explains existing measures for CRC prevention. They will later be sent a second letter (also signed by their primary care doctor or area specialist, or the person responsible for the Autonomous Regions screening programme) in which they are invited to participate in the study (invitation letter) and includes an appointment to the Local Screening Office (LSO) and a contact telephone number. In the invitation letter, individuals will also be informed of the screening option that applies to them, the characteristics of the test and its possible adverse effects. This whole process will be performed by the LSO (who may be assisted by staff of the project data manager). Individuals who do not respond will receive a reminding letter at 3-4 months after sending of the introduction letter. Individuals who do not respond to it will receive a second reminding letter 2 months later. The content of the two letters will be identical in all Autonomous Regions. However, translation into official languages and the use of logos, institutional images or letterheads of each Autonomous Regions is permitted. 10
12 The frequency of sending invitation letters will be adapted to the capacity of each LSO to attend individuals wishing to participate in order to diminish the lag time between randomisation and participation to less than 3 weeks. At the Health Centre, the functions of staff responsible for the study (including physicians and nurses of the centre and the data-collector in charge of the study) will be: 1) To track selected individuals in the sample who do not respond or who do not come to the appointment; 2) For those who come to the appointment, to confirm their suitability to participate in the study (compliance with inclusion/exclusion criteria); 3) To provide more detailed and exhaustive information about the study objective and the strategy they have been assigned in order to facilitate their participation; 4) To identify high-risk individuals, and assign them an appointment for a high-risk clinic of the reference hospital or the corresponding genetic counselling unit (see below); 5) To obtain written informed consent for participation in the study; 6) To complete the questionnaire with the data of all individuals contacted and include them in the project database; and 7) To provide a FIT kit (Group 1) or formalise the appointment at the hospital CRC prevention unit assigned to perform the colonoscopy (Group 2). In the event that an attending individual refuses to participate in the study, the baseline questionnaire will be completed and the reasons for the refusal of the invitation will be recorded. They will also be informed that even if they are not examined during screening, they will be contacted periodically in order to monitor the state of their health Determination of faecal occult blood Reading of the FIT tests will be done in a centralised manner in each Autonomous Regions. Individuals participating in the FIT arm will be advised of returning the completed kit to the LSO within 5 working days, and maintaining it in their refrigerator until such a moment. From the LSO to the centralized laboratory kits will be transported in insulated cooler bags once a day Technical characteristics of colonoscopies All colonoscopies performed in a screening programme must be of the highest quality to avoid false negative results and to minimize potential complications. Results of colonoscopy will determine the interval until next endoscopic examination, which is 10 years if no neoplastic lesions are detected, according to current recommendations. Colonoscopies will be performed by experienced staff in the centres involved in the study, which should be able to make correct diagnoses and carry out proper treatment of different types of neoplastic lesions. In addition, these examinations will be performed in specific work modules with sufficient resources to offer the quality required. In that sense, it is important to keep in mind that more than half of the examinations performed to confirm a positive FIT are associated with a therapeutic procedure, most often polypectomy. The period of time between acceptance to participate and performance of colonoscopy in individuals allocated to colonoscopy (Group 2) or between a positive FIT result and performance of colonoscopy in individuals allocated to FIT (Group 1) will be established in less than one month. Endoscopic procedures will be recorded in the appropriate databases, including high quality digital photographs of all lesions detected. The report should contain the parameters for quality assessment (caecal intubation, insertion and withdrawal times, quality of cleanliness for each colorectal segment, number of polyps 11
13 identified, removed and recovered for histological examination, retroflexion manoeuvre in the rectum, immediate complications, etc.). Proper cleansing should be another pillar of colonoscopy in the screening programme. Whichever method is used, part of the preparation should be administered a few hours before the procedure, since in various studies this pattern has resulted in not only better quality cleansing, but also a greater proportion of patients with polyps detected. Any of the commercially available methods can be used (polyethylene glycol [Bohm solution] or disodium hydrogen phosphate [Fosfosoda ]), whether combined or not with bisacodyl (Dulco Laxo ), taking care to provide the last dose for cleansing as close to the time of the colonoscopy as possible. All colonoscopies will be performed under sedation. In patients treated with anti-platelet agents, both for those in Group 1 with a positive FIT test (positive predictive value for colorectal neoplasia greater than 40%) and in Group 2 (positive predictive value of 5-7%), withdrawal or changes in medication will be assessed 7-10 days before testing. However, it is important to note that, according to current scientific recommendations, it is not necessary to discontinue anti-platelet agents to perform a polypectomy. Anti-coagulated patients (dicoumarol) should be changed, when possible, to subcutaneous administration of LMW heparin. Finally, the usefulness of metal clips has been described for the prophylaxis and treatment of post-polypectomy bleeding in at-risk groups, including in anti-coagulated patients. The American Heart Association does not recommend the use of antibiotics prior to completion of endoscopic procedures (including colonoscopy and polypectomy) for prophylaxis of infectious endocarditis ( CIRCULATIONAHA ). Biopsy of the polyp will be sought before polypectomy, especially for patients in whom it is anticipated that it will be difficult to obtain after the procedure. This measure aims to reduce the number of polyps not histologically studied. In cases where colon cleansing is not adequate, the colonoscopy will be repeated. In cases of failure to achieve complete colonoscopy, the procedure will be repeated or a CT-colonography will be offered. Quality standards will be established for all the above requirements according to the recommendations made by the Quality Assurance Task Group of the National Colorectal Cancer Roundtable (44), which shall be subject to internal auditing during the course of the study. This will be the responsibility of the Quality Committee created specifically for this purpose (see below) Quality assurance programme A specific program will be designed to assure the quality of the whole process. It will include the following measures: A communication plan based in a comprehensive informative campaign designed and launched by the Spanish Alliance for CRC Prevention involving national and local media. Data will be registered in a centralized, safe database accessible online ( Quality of FIT measurements will be assured by daily calibration at each reference laboratory, and external validation with samples provided by the manufacturer every 6 months. 12
14 Colonoscopy quality will be ensured following the guidelines of the Spanish Gastroenterological Association and the Spanish Society for Digestive Endoscopy. A specific Quality Committee will be created to oversee the quality assurance programme all over the study. This committee will meet in a periodical basis and will monitor by means of periodic audits the three main phases of the study (recruitment process, FIT determinations and colonoscopy). 13
15 5. DEVELOPMENT OF THE STUDY This research project is included within the population-based screening programme of each Autonomous Region. This screening programme will ensure the recall of individuals for appointments in successive rounds of screening, while also continuing the strategy assigned to them during the randomisation of the study. The investigators will also be responsible to electronically or manually transfer to the LSO the information derived from the study that is of interest to the population screening programme. Each Autonomous Region is committed with recruiting the same number of individuals regardless of the number of participating health centres or hospitals in each region. The dynamics of the study are summarised as follow: Participants in Group 1 with a negative FIT will remain in their assigned group, and will be offered the next round of screening at 2 year intervals until the age of 69. All of them will be sent a letter informing them of the test result and the date of the next round of screening. Individuals who enter the study at the age of 68 or 69 will undergo a single round of screening. Participants in Group 1 with a positive FIT will be contacted by phone and sent a letter informing them of the test result and the date of their appointment with the primary care physician (or specialist) or the person responsible for the screening programme, depending on the Autonomous Region They may be assisted in this task by the project staff. During the visit they will be informed about the colonoscopy procedure and will be scheduled for this procedure. Participants in Group 1 with a positive FIT but who have normal colonoscopies or in whom only non-neoplastic disease is detected will remain in the FIT arm and will be offered the next round of screening using the biennial FOBT test at 10 years after performance of the colonoscopy. Participants in Group 2 who are found to be negative in colonoscopy or in whom only non-neoplastic disease is detected, will remain in the colonoscopy arm and will be offered a new colonoscopy at 10 years after performance of the baseline colonoscopy. Surveillance colonoscopy for patients with adenomas will be carried out according to the Joint Guideline from the US Multi-Society Task Force (USMTF) (45). Participants in either Group 1 or Group 2 in whom only 1 or 2 non-advanced adenomas (low-risk adenomas) are detected, will be included in a surveillance programme and offered a new colonoscopy at 5 years. Participants in either Group 1 or Group 2 in whom 3 or more non-advanced adenomas or 1 or more advanced adenomas (high-risk adenomas) are detected will be included in a surveillance programme and offered a new colonoscopy after 3 years. Participants in either Group 1 or Group 2 in whom >10 adenomas are detected in a single examination will be scheduled for surveillance colonoscopy in less than 3 years. Participants in either Group 1 or Group 2 in whom a large sessile adenoma is detected and removed by piecemeal resection will undergo a colonoscopy in 2-6 months to verify complete removal. 14
16 The interval between subsequent surveillance colonoscopies will depend on the findings of the earlier examinations. In general, if a neoplastic lesion is detected, the above-mentioned criteria will be applied. On the other hand, if the examination is normal or if only non-neoplastic disease is detected, the next colonoscopy will be performed 5 years later. For participants in either Group 1 or Group 2 in whom a malignant polyp is detected (pt1n0m0) and for whom endoscopic polypectomy is deemed sufficient (see criteria below), a new colonoscopy will be performed with biopsy of the resected area within a period of no more than 2-3 months to confirm that complete resection of the lesion was achieved. Subsequently, new colonoscopies will be performed after 1 and 3 years. Participants in either Group 1 or Group 2 in whom an invasive CRC is detected will be treated and followed up according to the specific protocol of each centre, but always including a colonoscopy 1 year after the resection, and every 3 years thereafter. Any individual may refuse the screening examination assigned and request an alternative method. Any such individual will be assessed according to the group to which he/she was randomised for the intention to screen analysis, and according to the procedure actually performed in the as-screened analysis. These same criteria will be applied when any screening examination is performed (FOBT, colonoscopy, CT-colonography, or colonic capsule) and that is not foreseen in the study, regardless of the reason. All randomised subjects, whether the appropriate screening strategies have been performed or not, will be followed up for the purpose of tracking changes in the state of their health. Individuals who are not contacted will be registered for calculation of the invited population. For subsequent screening rounds, the same system of invitation will be used and according to each Autonomous Region policy. The CRC prevention units will ensure the performance of colonoscopies no more than 4 weeks after the procedure is indicated. Patients in whom any neoplastic colorectal lesion is detected will be treated and followed up properly. The treatment of lesions detected in any screening examination will be conducted according to the specific protocol of each centre Screening phases Phase 1: It begins when the presentation letter, containing information on the CRC screening programme and the rationale of the study, is sent. Four weeks later, the invitation letter indicating in which screening strategy the indidivual has been allocated, is sent. It ends with receipt of the FIT test results (and performance of colonoscopy in those individuals with a positive result) (Group 1), or after completion of colonoscopy (Group 2). 15
17 Phase 2 (individuals who require retesting): In Group 1, it begins with repetition of the FIT test in patients for whom the previous test was invalid, and ends when it is delivered and properly read. In Group 2, it begins with repetition of colonoscopy in cases in which the bowel preparation was inadequate, or repetition of colonoscopy or performance of CTcolonography when the colonoscopy was incomplete. Phase 3: includes all Group 1 respondents for phases I and II who are included in the subsequent biennial rounds until completion of the 10 years. In Group 2, phase III will be completed 10 years after completion of the first examination Organisation and management of the project To ensure the viability and effectiveness of this project the following is necessary: 1) Ensuring specific CRC prevention units (CRCPU) in the gastroenterology departments of each participating hospitals; 2) Effective coordination between hospital CRCPU, LSO and primary care physicians; 3) Implementation of an educational programme for the general population and primary care physicians; 4) Assurance of the development of the above-mentioned field work and an effective system for recording the results of the programme in order to determine its true impact and to correct potential malfunctions; and 5) The provision of the financial resources required for ensuring the viability of the project. CRC prevention units (CRCPU) These units will be located in the Gastroenterology Departments of each participant hospitals. They will have a coordinator and will work with a separate agenda in order not to interfere with the regular activity of the endoscopy units. People with a positive FIT as well as all participants in the Group 2 that accepted colonoscopy will be received in these CRCPU. These units should warrant a correct diagnosis, treatment and surveillance of participants. Finally, CRCPU will give assistance to individuals identified as having a high risk for developing CRC. Coordination between Local Screening Offices and primary care physicians The LSO will have a person responsible for the study. There will be also a study coordinator in each Health Care Centre participating in the study, who will be responsible for its development. Moreover, it will be a data collector in charge of the information task and recruitment; this data collector could be located at the LSO, Health Centre or CRCPU. Educational programme and measures for improving study participation The educational programme is aimed to improve the knowledge of the target population and primary care physicians on natural history of CRC, symptoms, treatment, prognosis, and diagnostic tests in order to improve participation in the study. This aspect is critical to achieve a high adherence with screening. Possible actions include: informative leaflets about CRC screening, campaign in the media (TV, radio and press), programme web page, organization of a "CRC prevention awareness day", among others (see Quality assurance programme). Data recording Demographic data, results of diagnostic tests, treatments and pathological data will be recovered in an online, centralized and protected database ( 16
18 6. DEFINITIONS Pragmatic study: study designed to clarify whether an intervention works under real-life conditions and whether it works in terms that matter to the patient. It is simply concerned with whether the intervention works, not how or why. Target population: year-old individuals with verified address in sanitary card. Invited population: target population excluding non-contacted individuals. Eligible population: target population excluding non-contacted and excluded individuals. Participant population: individuals who returned the FIT test (Group 1) or who completed colonoscopy (Group 2). Screening inclusion data: data of sending the invitation letter. Incomplete colonoscopy: colonoscopy in which caecal intubation is not possible. When an incomplete colonoscopy occurs, this examination must be repeated or completed with a CT-colonography. Inadequate colon cleansing: when less than 90% of colorectal mucosa can be properly evaluated due to the presence of faeces, this examination must be repeated. Non-neoplastic polyp: hyperplastic, hamartomatous or inflammatory polyps. Non-advanced adenoma: any tubular adenoma <1 cm and with low-grade dysplasia. Advanced adenoma: adenoma >1 cm in size, or with high-grade dysplasia, or with villous component (>25%). High-risk adenoma: 3 or more non-advanced adenomas, or any advanced adenoma. Low-risk adenoma: 1 or 2 non-advanced adenomas. Non-invasive colorectal cancer: colorectal carcinoma without submucose invasion (ptis). It includes intramucous carcinoma and intraepithelial carcinoma. Invasive colorectal cancer: colorectal carcinoma beyond the muscularis mucosa (ptnm stages I, II, III and IV). Advanced neoplasia: colorectal advanced adenoma or cancer. Malignant polyp: adenoma that harbours an area of carcinoma invading submucose (pt1). Polyposis: existence of >10 polyps. Depending on the histology, it could be adenomatous, hamartomatous or hyperplastic. Non-neoplastic colorectal diseases: any non-neoplastic disease detected in the colonoscopy (i.e. haemorrhoids, diverticulosis, angiodysplasia, etc.) Classification of colorectal polyps Colorectal polyps will be classified following the Paris classification (protruded, flatelevated and flat-depressed). The size of the polyps will be established ex vivo after resection and before formaldehyde fixation. 17
19 When pathological study is not available because the polyp could not be recovered and pre-resection biopsy was not taken, it will be conservatively considered as adenoma Treatment of malignant polyps Endoscopic polypectomy will be considered definitive treatment of a malignant polyp (pt1) if it fulfils all the following characteristics: Well or moderate differentiation degree, No vascular or lymphatic invasion, and Free resection margin >1 mm In these patients, a new colonoscopy will be performed within 2-3 months with biopsies of the resection area (see Development of the study section) Classification of colorectal cancer CRC patients detected in the study will be classified as: 1) Screening CRC: CRC detected in the screening Groups 1 and 2; 2) Interval CRC: CRC diagnosed after a negative FIT (Group 1) or after a negative colonoscopy (Group 2), or detected after a positive FIT with a negative colonoscopy or if colonoscopy was not accepted by the patient (Group 1); 3) Sporadic CRC: CRC diagnosed in patients that did not accept screening in the study. CRC stage will be established using TNM classification (American Joint Committee on Cancer, 6 th edition): Primary tumour (pt) Tx: It is not possible to evaluate primary tumour T0: There is not evidence of primary tumour Tis (in situ carcinoma): intraepithelial o intramucous tumour T1: Tumour invades submucose T2: Tumour invades muscularis propria T3: Tumour invades subserose or pericolic/perirectal tissues through muscularis propria T4: Tumour invades other organs or perforates the peritoneum Regional lymph nodes (pn) Nx: It is not possible to evaluate regional lymph nodes N0: No metastasis in any regional lymph nodes N1: Metastasis in 1-3 regional lymph nodes N2: Metastasis in 4 or more regional lymph nodes Distant metastasis (pm) Mx: It is not possible to evaluate distant metastasis M0: No distant metastasis M1: Distant metastasis 18
20 Tumour TNM stages Stage 0 Tis N0 M0 Stage I T1-2 N0 M0 Stage IIA T3 N0 M0 Stage IIB T4 N0 M0 Stage IIIA T1-2 N1 M0 Stage IIIB T3-4 N1 M0 Stage IIIC T1-4 N2 M0 Stage IV T1-4 N0-2 M1 19
21 7. STATISTICAL ANALYSIS PLAN (SAP) Because of the study design, which allows for cross-over between both strategies, the main outcomes of the study will be analysed by intention-to-screen, as-screened and per-protocol. Primary end-point: CRC-specific mortality at 10 years Differences in CRC-specific mortality between both strategies will be established by a Cox regression analysis, adjusted by age, gender and participating centre, and reported as hazard ratios (HR) with 95% confidence intervals (95%CI). Data will be presented as probability curves. Secondary end-points: 1. Participation, detection rate, diagnostic yield and complication rate at the completion of the first round and at the end of study (10 years) Definitions of these four key outcomes are as follows: Participation: number of participating individuals (i.e. individuals who completed colonoscopy in the colonoscopy group and individuals who returned the test in the FIT arm) relative to the number of eligible individuals. Detection rate: number of true positives relative to the number of participating individuals. Diagnostic yield: number of true positives relative to the number of eligible individuals. Complication rate: number of major complications (i.e. perforation, postpolypectomy bleeding requiring hospitalization, and cardiovascular/ pulmonary complications requiring medical management) relative to the number of participating individuals. Differences in these four key outcomes between both strategies will be established by logistic regression analysis, adjusted by age, gender and participating centre, and reported as odds ratios (OR) with 95%CI. 2. Overall survival at the end of study (10 years) Differences in overall survival (i.e. any cause of death) between both strategies will be established by a Cox regression analysis, adjusted by age, gender and participating centre, and reported as HR with 95%CI. Data will be presented as probability curves. 3. CRC incidence at the end of study (10 years) Differences in CRC incidence between both strategies will be established by a Cox regression analysis, adjusted by age, gender and participating centre, and reported as HR with 95%CI. Data will be presented as probability curves. 4. Cost-effectiveness analysis Cost-effectiveness will be studied with a Markov s model at the completion of study. Results will be reported in terms of quality-adjusted life years (QALY). 5. Analysis of factors influencing participation in the study Factors associated with participation at the completion of first round and at the end of study (10 years) in each screening strategies will be analyzed by logistic regression analysis and results reported as OR with 95%CI. Parameters analysed will include: demographics, personal and familial characteristics, socio-economic status, etc. 20
22 8. CHRONOGRAM The study will be developed according to the following chronogram: Initial meeting: October 28 th, 2008 Formative meeting for data-collectors and other auxiliary staff: December 12 th, 2008 Informative campaign launched by the Spanish Alliance for CRC Prevention and involving national and local media: from November 2008 to March 2009 Recruitment period will be initiated in June 2009 Quality Committee meetings will be held during the first round according to the following calendar: June 12 th, 2009 December 11 th, 2009 June 11 th, 2010 December 10 th, 2010 First round of screening will be finished in June 2011 First follow-up meeting (first-round interim analysis): July 2011 Other follow-up meetings will be held regularly during the study period, in a biennial basis (date will be announced properly) Other Quality Committee meetings will be held regularly during the study period, in a annual basis (date will be announced properly) Completion of the study: June 2021 Final meeting (final analysis): July 2021 (date will be announced properly) Follow-up conference calls among members of the Executive Committee will be held periodically, every four months, during the study period. 21
23 9. ETHICAL QUESTIONS The study will respect the Helsinki declaration, the European Council Human Rights and Biomedicine, and the UNESCO Universal Declaration about human genome and human rights. Moreover, the study will fulfil established requisites about biomedical investigation, data protection and bioethics of the Spanish law. People included in this study will receive appropriate information about objective, methodology and study procedures. Thereafter, they will provide written informed consent for participating in the study. This study receives the approval of the Ethics Committee of Clinical Investigation and the Research Committee of every of the participant hospitals. 22
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Colon Cancer Screening. Layth Al-Jashaami, MD GI Fellow, PGY 4
 Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
Colon Cancer Screening Layth Al-Jashaami, MD GI Fellow, PGY 4 -Colorectal cancer (CRC) is a common and lethal cancer. -It has the highest incidence among GI cancers in the US, estimated to be newly diagnosed
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Colorectal cancer screening
 26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
Objectives. Definitions. Colorectal Cancer Screening 5/8/2018. Payam Afshar, MS, MD Kaiser Permanente, San Diego. Colorectal cancer background
 Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Northern Ireland Bowel Cancer Screening Programme. Pathways. Version 4 1 st October 2013
 Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
CANCER SCREENING. Er Chaozer Department of General Medicine, Tan Tock Seng Hospital
 CANCER SCREENING Er Chaozer Department of General Medicine, Tan Tock Seng Hospital Introduction Screening average risk patients Benefits and harms from screening Early cancer detection early treatment
CANCER SCREENING Er Chaozer Department of General Medicine, Tan Tock Seng Hospital Introduction Screening average risk patients Benefits and harms from screening Early cancer detection early treatment
Colon Screening in 2014 Offering Patients a Choice. Clark A Harrison MD The Nevada Colon Cancer Partnership
 Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING
 CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer
 Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Guidelines for Colonoscopy Surveillance After Screening and Polypectomy: A Consensus Update by the US Multi-Society Task Force on Colorectal Cancer David A. Lieberman, 1 Douglas K. Rex, 2 Sidney J. Winawer,
Neoplastic Colon Polyps. Joyce Au SUNY Downstate Grand Rounds, October 18, 2012
 Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Early detection and screening for colorectal neoplasia
 Early detection and screening for colorectal neoplasia Robert S. Bresalier Department of Gastroenterology, Hepatology and Nutrition. The University of Texas. MD Anderson Cancer Center. Houston, Texas U.S.A.
Early detection and screening for colorectal neoplasia Robert S. Bresalier Department of Gastroenterology, Hepatology and Nutrition. The University of Texas. MD Anderson Cancer Center. Houston, Texas U.S.A.
Colorectal Cancer Screening. Paul Berg MD
 Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
Colon Cancer Screening & Surveillance. Amit Patel, MD PGY-4 GI Fellow
 Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
EARLY DETECTION OF COLORECTAL CANCER. Epidemiology of CRC
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Colorectal adenocarcinoma leading cancer in developed countries In US, annual deaths due to colorectal adenocarcinoma 57,000.
 Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Colorectal Cancer Screening
 Recommendations from the U.S. Multi-Society Task Force on Colorectal Cancer Colorectal Cancer Screening Rex DK, Boland CR, Dominitz JA, Giardiello FM, Johnson DA, Kaltenbach T, Levin TR, Lieberman D, Robertson
Recommendations from the U.S. Multi-Society Task Force on Colorectal Cancer Colorectal Cancer Screening Rex DK, Boland CR, Dominitz JA, Giardiello FM, Johnson DA, Kaltenbach T, Levin TR, Lieberman D, Robertson
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
05/07/2018. Organisation. The English screening programme what is happening? Organisation. Bowel cancer screening in the UK is:
 Organisation The English screening programme what is happening? Phil Quirke Lead Pathologist Bowel Cancer Screening PHE England Bowel Cancer Screening Pathology Committee Started 2006 with roll out 4 devolved
Organisation The English screening programme what is happening? Phil Quirke Lead Pathologist Bowel Cancer Screening PHE England Bowel Cancer Screening Pathology Committee Started 2006 with roll out 4 devolved
ACG Clinical Guideline: Colorectal Cancer Screening
 ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
Screening for GI Cancer Past Present and Future. Prof. Bob Steele University of Dundee
 Screening for GI Cancer Past Present and Future Prof. Bob Steele University of Dundee Worldwide Cancer Incidence Rates UK Cancer Incidence Rates Screening The detection of disease in asymptomatic subjects
Screening for GI Cancer Past Present and Future Prof. Bob Steele University of Dundee Worldwide Cancer Incidence Rates UK Cancer Incidence Rates Screening The detection of disease in asymptomatic subjects
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
A916: rectum: adenocarcinoma
 General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
Measuring performance and quality indicators of CRC screening
 Measuring performance and quality indicators of CRC screening Ondřej MÁJEK Institute of Biostatistics and Analyses, Masaryk University Institute of Biostatistics and Analyses, Masaryk University, Brno
Measuring performance and quality indicators of CRC screening Ondřej MÁJEK Institute of Biostatistics and Analyses, Masaryk University Institute of Biostatistics and Analyses, Masaryk University, Brno
Updates in Colorectal Cancer Screening & Prevention
 Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
2. Describe pros/cons of screening interventions (including colonoscopy, CT colography, fecal tests)
 Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
Learning Objectives 1. Review principles of colon adenoma/cancer biology that permit successful prevention regimes 2. Describe pros/cons of screening interventions (including colonoscopy, CT colography,
CRC Risk Factors. U.S. Adherence Rates Cancer Screening. Genetic Model of Colorectal Cancer. Epidemiology and Clinical Consequences of CRC
 10:45 11:45 am Guide to Colorectal Cancer Screening SPEAKER Howard Manten M.D. Presenter Disclosure Information The following relationships exist related to this presentation: Howard Manten MD: No financial
10:45 11:45 am Guide to Colorectal Cancer Screening SPEAKER Howard Manten M.D. Presenter Disclosure Information The following relationships exist related to this presentation: Howard Manten MD: No financial
DIGESTIVE SYSTEM SURGICAL PROCEDURES May 1, 2015 INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
Quality Measures In Colonoscopy: Why Should I Care?
 Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Quality Measures In Colonoscopy: Why Should I Care? David Greenwald, MD, FASGE Professor of Clinical Medicine Albert Einstein College of Medicine Montefiore Medical Center Bronx, New York ACG/ASGE Best
Bowel cancer screening and prevention
 Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
Bowel cancer screening and prevention Cancer Incidence and Mortality Victoria 2012 Number 6000 5000 4000 3000 2000 Incidences = 29,387 Mortality = 10,780 Incidence Mortality 1000 0 Prostate Breast Bowel
CENTERS FOR DISEASE CONTROL AND PREVENTION CENTERS FOR DISEASE CONTROL AND PREVENTION. Incidence Male. Incidence Female.
 A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION.
 The West London Medical Journal 2009 Vol No 1 pp 23-31 COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION. Competing interests: None declared ABSTRACT Sarah
The West London Medical Journal 2009 Vol No 1 pp 23-31 COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION. Competing interests: None declared ABSTRACT Sarah
Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests
 Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests Results of a systematic review, Kaiser experience, and implications for the Canton of Vaud Kevin Selby, M.D. Kevin.Selby@hospvd.ch
Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests Results of a systematic review, Kaiser experience, and implications for the Canton of Vaud Kevin Selby, M.D. Kevin.Selby@hospvd.ch
The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean?
 The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean? Robert A. Smith, PhD Cancer Control, Department of Prevention and Early Detection American Cancer Society
The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean? Robert A. Smith, PhD Cancer Control, Department of Prevention and Early Detection American Cancer Society
Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative
 Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative Dr. Meryl Oyomno Department of surgery, University of Pretoria INTRODUCTION Screening is the
Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative Dr. Meryl Oyomno Department of surgery, University of Pretoria INTRODUCTION Screening is the
Colorectal Cancer Screening
 Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
Scan for mobile link. Colorectal Cancer Screening What is colorectal cancer screening? Screening examinations are tests performed to identify disease in individuals who lack any signs or symptoms. The
Colorectal Cancer Screening: A Clinical Update
 11:05 11:45am Colorectal Cancer Screening: A Clinical Update SPEAKER Kevin A. Ghassemi, MD Presenter Disclosure Information The following relationships exist related to this presentation: Kevin A. Ghassemi,
11:05 11:45am Colorectal Cancer Screening: A Clinical Update SPEAKER Kevin A. Ghassemi, MD Presenter Disclosure Information The following relationships exist related to this presentation: Kevin A. Ghassemi,
ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009
 ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009 Published by: NHS Cancer Screening Programmes Fulwood House Old Fulwood Road Sheffield S10 3TH Tel: 0114 271 1060 Fax: 0114 271 1089
ADENOMA SURVEILLANCE BCSP Guidance Note No 1 Version 1 September 2009 Published by: NHS Cancer Screening Programmes Fulwood House Old Fulwood Road Sheffield S10 3TH Tel: 0114 271 1060 Fax: 0114 271 1089
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool
 When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
When is a programmed follow-up meaningful and how should it be done? Professor Alastair Watson University of Liverpool Adenomas/Carcinoma Sequence Providing Time for Screening Normal 5-20 yrs 5-15 yrs
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Transition to Fecal Immunochemical Testing (FIT)
 Transition to Fecal Immunochemical Testing (FIT) Frequently Asked Questions for Primary Care Providers October 2017 Version 1.1 Overview Ontario will be transitioning from the guaiac fecal occult blood
Transition to Fecal Immunochemical Testing (FIT) Frequently Asked Questions for Primary Care Providers October 2017 Version 1.1 Overview Ontario will be transitioning from the guaiac fecal occult blood
Increasing Colorectal Cancer Screening in Wyoming. Allie Bain, MPH Outreach & Education Supervisor Wyoming Integrated Cancer Services Program
 Increasing Colorectal Cancer Screening in Wyoming Allie Bain, MPH Outreach & Education Supervisor Wyoming Integrated Cancer Services Program Overview What is colorectal cancer? What are risk factors for
Increasing Colorectal Cancer Screening in Wyoming Allie Bain, MPH Outreach & Education Supervisor Wyoming Integrated Cancer Services Program Overview What is colorectal cancer? What are risk factors for
Colorectal Cancer Screening
 Colorectal Cancer Screening An Integrated Care Pathway of the Collaborative Care Network Subject Matter Expert: Kevin Wolov, DO Pathway Custodian: Pat Czapp, MD First, a Friendly Reminder... This Integrated
Colorectal Cancer Screening An Integrated Care Pathway of the Collaborative Care Network Subject Matter Expert: Kevin Wolov, DO Pathway Custodian: Pat Czapp, MD First, a Friendly Reminder... This Integrated
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
Staging for Residents, Nurses, and Multidisciplinary Health Care Team
 Staging for Residents, Nurses, and Multidisciplinary Health Care Team Donna M. Gress, RHIT, CTR Validating science. Improving patient care. Learning Objectives Introduce the concept and history of stage
Staging for Residents, Nurses, and Multidisciplinary Health Care Team Donna M. Gress, RHIT, CTR Validating science. Improving patient care. Learning Objectives Introduce the concept and history of stage
Pathology in Slovenian CRC screening programme:
 Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Colorectal Cancer Screening and Risk Assessment Workflow. Documentation Guide for Health Center NextGen Users
 Colorectal Cancer Screening and Risk Assessment Workflow Documentation Guide for Health Center NextGen Users Colorectal Cancer Screening and Risk Assessment Workflow and Documentation Guide for Health
Colorectal Cancer Screening and Risk Assessment Workflow Documentation Guide for Health Center NextGen Users Colorectal Cancer Screening and Risk Assessment Workflow and Documentation Guide for Health
COUNCIL RECOMMENDATION of 2 December 2003 on cancer screening (2003/878/EC)
 L 327/34 COUNCIL RECOMMDATION of 2 December 2003 on cancer screening (2003/878/EC) THE COUNCIL OF THE EUROPEAN UNION, Having regard to the Treaty establishing the European Community, and in particular
L 327/34 COUNCIL RECOMMDATION of 2 December 2003 on cancer screening (2003/878/EC) THE COUNCIL OF THE EUROPEAN UNION, Having regard to the Treaty establishing the European Community, and in particular
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Supporting Information 2. ESGE QIC Lower GI Delphi voting process: Round 1 Working Group chair: Michal F. Kaminski, Poland
 Supporting Information 2. ESGE QIC Lower GI Delphi voting process: Round 1 Working chair: Michal F. Kaminski, Poland Population Interventions Comparator Outcome Additional evidence 1.1 Rate of adequate
Supporting Information 2. ESGE QIC Lower GI Delphi voting process: Round 1 Working chair: Michal F. Kaminski, Poland Population Interventions Comparator Outcome Additional evidence 1.1 Rate of adequate
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Colorectal Cancer Screening in Later Life: Blum Center Rounds
 Colorectal Cancer Screening in Later Life: Blum Center Rounds OCTOBER 10, 2018 Agenda CRC Screening and Surveillance Recommendation Screening for Colon Cancer later in life Discussion and listening Families
Colorectal Cancer Screening in Later Life: Blum Center Rounds OCTOBER 10, 2018 Agenda CRC Screening and Surveillance Recommendation Screening for Colon Cancer later in life Discussion and listening Families
Colon and Rectum. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition
 Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an open-label, randomized controlled trial
 Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
FREQUENTLY ASKED QUESTIONS
 FREQUENTLY ASKED QUESTIONS What is CRC? CRC (CRC) is cancer of the large intestine (colon), the lower part of the digestive system. Rectal cancer is cancer of the last several inches of the colon. Together,
FREQUENTLY ASKED QUESTIONS What is CRC? CRC (CRC) is cancer of the large intestine (colon), the lower part of the digestive system. Rectal cancer is cancer of the last several inches of the colon. Together,
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Aberrant crypt foci, chromocolonoscopy for, 539 540 Absorptive stains, for chromocolonoscopy, 522 524 Accessories, for colonoscopy, 680 684
Note: Page numbers of article titles are in boldface type. A Aberrant crypt foci, chromocolonoscopy for, 539 540 Absorptive stains, for chromocolonoscopy, 522 524 Accessories, for colonoscopy, 680 684
Emerging Interventions in Endoscopy. Margaret Vance Nurse Consultant in Gastroenterology St Mark s Hospital
 Emerging Interventions in Endoscopy Margaret Vance Nurse Consultant in Gastroenterology St Mark s Hospital Colon Cancer Colon cancer is common. 1 in 20 people in the UK will develop the disease 19 000
Emerging Interventions in Endoscopy Margaret Vance Nurse Consultant in Gastroenterology St Mark s Hospital Colon Cancer Colon cancer is common. 1 in 20 people in the UK will develop the disease 19 000
PDF // POSITIVE COLON CANCER RESULTS
 01 March, 2018 PDF // POSITIVE COLON CANCER RESULTS Document Filetype: PDF 268.79 KB 0 PDF // POSITIVE COLON CANCER RESULTS This cohort study evaluates the association between time to colonoscopy after
01 March, 2018 PDF // POSITIVE COLON CANCER RESULTS Document Filetype: PDF 268.79 KB 0 PDF // POSITIVE COLON CANCER RESULTS This cohort study evaluates the association between time to colonoscopy after
11/21/13 CEA: 1.7 WNL
 Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Colorectal Cancer. Mark Chapman. MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist
 Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction
 Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
Quality ID #439: Age Appropriate Screening Colonoscopy National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Efficiency DESCRIPTION:
Colorectal Cancer Screening What are my options?
 069-Colorectal cancer (Rosen) 1/23/04 12:59 PM Page 69 What are my options? Wayne Rosen, MD, FRCSC As presented at the 37th Annual Mackid Symposium: Cancer Care in the Community (May 22, 2003) There are
069-Colorectal cancer (Rosen) 1/23/04 12:59 PM Page 69 What are my options? Wayne Rosen, MD, FRCSC As presented at the 37th Annual Mackid Symposium: Cancer Care in the Community (May 22, 2003) There are
Colorectal Cancer Screening in Canada MONITORING & EVALUATION OF QUALITY INDICATORS RESULTS REPORT
 Colorectal Cancer Screening in Canada MONITORING & EVALUATION OF QUALITY INDICATORS RESULTS REPORT JANUARY 2011 DECEMBER 2012 Acknowledgments The Canadian Partnership Against Cancer would like to gratefully
Colorectal Cancer Screening in Canada MONITORING & EVALUATION OF QUALITY INDICATORS RESULTS REPORT JANUARY 2011 DECEMBER 2012 Acknowledgments The Canadian Partnership Against Cancer would like to gratefully
NHS KINGSTON. Contents
 NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
1101 First Colonial Road, Suite 300, Virginia Beach, VA Phone (757) Fax (757)
 1101 First Colonial Road, Suite 300, Virginia Beach, VA 23454 www.vbgastro.com Phone (757) 481-4817 Fax (757) 481-7138 1150 Glen Mitchell Drive, Suite 208 Virginia Beach, VA 23456 www.vbgastro.com Phone
1101 First Colonial Road, Suite 300, Virginia Beach, VA 23454 www.vbgastro.com Phone (757) 481-4817 Fax (757) 481-7138 1150 Glen Mitchell Drive, Suite 208 Virginia Beach, VA 23456 www.vbgastro.com Phone
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
EU Guidelines for quality assurance in organization, implementation and monitoring of colorectal cancer screening programme. Jožica Maučec Zakotnik
 EU Guidelines for quality assurance in organization, implementation and monitoring of colorectal cancer screening programme Jožica Maučec Zakotnik EU guidelines Luxembourg 2010 EU guidelines - chapters
EU Guidelines for quality assurance in organization, implementation and monitoring of colorectal cancer screening programme Jožica Maučec Zakotnik EU guidelines Luxembourg 2010 EU guidelines - chapters
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care
 Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
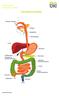 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
COLORECTAL CANCER: A CHALLENGE FOR HEALTHY LIFESTYLE, SCREENING AND PROPER CARE
 COLORECTAL CANCER: A CHALLENGE FOR HEALTHY LIFESTYLE, SCREENING AND PROPER CARE Brno, 29 May 2015: For the fourth time in a row, the second largest city of the Czech Republic will host the European Colorectal
COLORECTAL CANCER: A CHALLENGE FOR HEALTHY LIFESTYLE, SCREENING AND PROPER CARE Brno, 29 May 2015: For the fourth time in a row, the second largest city of the Czech Republic will host the European Colorectal
Cologuard Screening for Colorectal Cancer
 Pending Policies - Medicine Cologuard Screening for Colorectal Cancer Print Number: MED208.056 Effective Date: 08-15-2016 Coverage: I.Cologuard stool DNA testing may be considered medically necessary for
Pending Policies - Medicine Cologuard Screening for Colorectal Cancer Print Number: MED208.056 Effective Date: 08-15-2016 Coverage: I.Cologuard stool DNA testing may be considered medically necessary for
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer
 Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Improving Access to Endoscopy at Safety-Net Hospitals. Lukejohn W. Day MD Assistant Professor of Medicine
 Improving Access to Endoscopy at Safety-Net Hospitals Lukejohn W. Day MD Assistant Professor of Medicine Goals Background Improving Access to Endoscopic Care Electronic referral: ereferral Direct Access
Improving Access to Endoscopy at Safety-Net Hospitals Lukejohn W. Day MD Assistant Professor of Medicine Goals Background Improving Access to Endoscopic Care Electronic referral: ereferral Direct Access
Recommendations on Screening for Colorectal Cancer 2016
 Recommendations on Screening for Colorectal Cancer 2016 Canadian Task Force on Preventive Health Care (CTFPHC) Putting Prevention into Practice Canadian Task Force on Preventive Health Care Groupe d étude
Recommendations on Screening for Colorectal Cancer 2016 Canadian Task Force on Preventive Health Care (CTFPHC) Putting Prevention into Practice Canadian Task Force on Preventive Health Care Groupe d étude
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Citation for published version (APA): Wijkerslooth de Weerdesteyn, T. R. (2013). Population screening for colorectal cancer by colonoscopy
 UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps
 Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps Full guideline Draft for consultation, May 00 0 This guideline
Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn s disease and polyps Full guideline Draft for consultation, May 00 0 This guideline
Cost-effectiveness of adenoma surveillance - the Dutch guidelines -
 Cost-effectiveness of adenoma surveillance - the Dutch guidelines - WEO working group adenoma surveillance 20 May, 2016 Iris Lansdorp-Vogelaar, PhD On behalf of the SAP study-group Introduction Adenoma
Cost-effectiveness of adenoma surveillance - the Dutch guidelines - WEO working group adenoma surveillance 20 May, 2016 Iris Lansdorp-Vogelaar, PhD On behalf of the SAP study-group Introduction Adenoma
Be it Resolved that FIT is the Best Way to Screen for Colorectal Cancer DEBATE
 Be it Resolved that FIT is the Best Way to Screen for Colorectal Cancer DEBATE DEBATE Presenters PRESENTATION MODERATOR Dr. Praveen Bansal -MD, CCFP FCFP Regional Primary Care Lead, Integrated Cancer Screening,
Be it Resolved that FIT is the Best Way to Screen for Colorectal Cancer DEBATE DEBATE Presenters PRESENTATION MODERATOR Dr. Praveen Bansal -MD, CCFP FCFP Regional Primary Care Lead, Integrated Cancer Screening,
Gastric Cancer Histopathology Reporting Proforma
 Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Colorectal Cancer Structured Pathology Reporting Proforma DD MM YYYY
 Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
2017 CANCER ANNUAL REPORT
 2017 CANCER ANNUAL REPORT A WORD FROM OUR LEADERSHIP We are pleased to present our 2017 Annual Report highlighting advances in state of the art cancer care at the Roper St. Francis Cancer Program. Our
2017 CANCER ANNUAL REPORT A WORD FROM OUR LEADERSHIP We are pleased to present our 2017 Annual Report highlighting advances in state of the art cancer care at the Roper St. Francis Cancer Program. Our
Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University WCC, Melbourne
 Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University. 2014 WCC, Melbourne Outline WHO criteria to justify screening Appropriateness: Global variation in incidence
Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University. 2014 WCC, Melbourne Outline WHO criteria to justify screening Appropriateness: Global variation in incidence
WEO CRC SC Meeting. Barcelona, Spain October 23, 2015
 WEO CRC SC Meeting Barcelona, Spain October 23, 2015 THE HEMOGLOBIN CONCENTRATION IN A NEGATIVE RESULT AS A PREDICTOR FOR ADVANCED NEOPLASIA Isabel Portillo, Eunare Arana-Arri, Isabel Idigoras, Lorea Martínez-Indart.
WEO CRC SC Meeting Barcelona, Spain October 23, 2015 THE HEMOGLOBIN CONCENTRATION IN A NEGATIVE RESULT AS A PREDICTOR FOR ADVANCED NEOPLASIA Isabel Portillo, Eunare Arana-Arri, Isabel Idigoras, Lorea Martínez-Indart.
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
The choice of methods for Colorectal Cancer Screening; The Dutch experience
 The choice of methods for Colorectal Cancer Screening; The Dutch experience Monique van Leerdam, Gastroenterologist, NKI-AVL, Amsterdam The Netherlands Colorectal cancer CRC 2 nd cause of cancer related
The choice of methods for Colorectal Cancer Screening; The Dutch experience Monique van Leerdam, Gastroenterologist, NKI-AVL, Amsterdam The Netherlands Colorectal cancer CRC 2 nd cause of cancer related
Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE
 Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE A key mission for family medicine is preserving health and maximizing
Nicolaus Copernicus University in Torun Medical College in Bydgoszcz Family Doctor Department CANCER PREVENTION IN GENERAL PRACTICE A key mission for family medicine is preserving health and maximizing
Dr Alasdair Patrick. Dr Nagham Al-Mozany. 9:45-10:10 Where Are We Up To With Bowel Cancer Screening?
 Dr Alasdair Patrick Gastroenterologist and General Physician Middlemore Hospital Auckland Dr Nagham Al-Mozany Colorectal Surgeon Auckland City Hospital Clinical Senior Lecturer University of Auckland 9:45-10:10
Dr Alasdair Patrick Gastroenterologist and General Physician Middlemore Hospital Auckland Dr Nagham Al-Mozany Colorectal Surgeon Auckland City Hospital Clinical Senior Lecturer University of Auckland 9:45-10:10
11/9/2015 OUTLINE. Quality Indicators for the Doctor Performing Screening Colonoscopy: What you should expect from your Endoscopist
 Quality Indicators for the Doctor Performing Screening Colonoscopy: What you should expect from your Endoscopist Anil K Sharma MD FACP Professor of Clinical Medicine, University of Rochester Chief of Gastroenterology,
Quality Indicators for the Doctor Performing Screening Colonoscopy: What you should expect from your Endoscopist Anil K Sharma MD FACP Professor of Clinical Medicine, University of Rochester Chief of Gastroenterology,
