Epidermal Langerhans cells are specialized members of the
|
|
|
- Isabella Kelley
- 5 years ago
- Views:
Transcription
1 The Human Hair Follicle: A Reservoir of CD40 B7-Deficient Langerhans Cells that Repopulate Epidermis After UVB Exposure Anita C. Gilliam,* Inger B. Kremer,* Yuichi Yoshida,* Seth R. Stevens,* Elena Tootell,* Marcel B.M. Teunissen, Craig Hammerberg,* and Kevin D. Cooper* *Department of Dermatology, Case Western Reserve University and University Hospitals of Cleveland, Cleveland, U.S.A.; Academic Medical Center, University of Amsterdam, Amsterdam, The Netherlands; School of Medicine, Kyushu University, Japan; VA Medical Center, Cleveland, Ohio, U.S.A. The ability of skin to maintain its protective structural and functional integrity depends on both resident and circulating cells. Until now, it was thought that dendritic antigen presenting cells of epidermis (Langerhans cells) were replaced by circulating bone marrow derived precursors. Here we show by immunostaining studies of timed biopsies taken from human skin after ultraviolet exposure, that hair follicle is a critical reservoir of Langerhans cells that repopulate epidermis depleted of Langerhans cells by a single four minimal erythema dose of ultraviolet B. Immunostaining with antibodies to thymidine dimers showed that ultraviolet B only penetrated the superficial hair follicle opening, whereas deeper follicle was relatively protected. Langerhans cells migrat- ing from hair follicle into epidermis 72 h after ultraviolet exposure have a partial deficiency of molecules important to T cell costimulation. We used four color flow cytometry to show that Langerhans cells isolated from epidermis 72 h after ultraviolet B can upregulate CD40 but not B7 1 or B7 2 expression in culture, suggesting a different phenotype of hair follicle Langerhans cells. Therefore, the hair follicle is a specialized immune compartment of the skin that serves as an intermediate reservoir of Langerhans cells between bone marrow and epidermis, and that may play a critical role in immune surveillance. Key words: antigen presenting cells/costimulatory molecules/dendritic cells. J Invest Dermatol 110: , 1998 Epidermal Langerhans cells are specialized members of the human cutaneous bone marrow derived dendritic cell population (Silberberg-Sinakin et al, 1976; Katz et al, 1979; Volc-Platzer et al, 1984; Breathnach, 1991), and are critical antigen presenting cells for initiating primary T cell mediated immune processes (i.e., delayed type hypersensitivity and contact hypersensitivity) (Rowden et al, 1977; Toews et al, 1980; Romani et al, 1991; Stingl and Shevach, 1991; Teunissen et al, 1997). They normally are present as highly dendritic cells with processes interdigitating between epidermal keratinocytes, with a cell density of about 2%. Langerhans cells are found in many epithelia, where contact with the external environment occurs (Rowden et al, 1977), as well as in follicular epithelium (Breathnach, 1963), although follicular Langerhans cells are poorly characterized. Other human leukocyte antigen (HLA) class II positive dendritic cells are found in the dermis (Murphy et al, 1986; Breathnach, 1991), some of which are of the dendritic antigen presenting cell lineage (Meunier et al, 1993) that may represent resident perivascular Langerhans cell variants, Langerhans cell precursors migrating into skin, or activated Langerhans cells migrating from skin. Upon activation, the Langerhans cell phenotype changes from a cell that efficiently takes up and processes antigen into one that efficiently Manuscript received August 29, 1997; revised December 4, 1997; accepted for publication December 23, Reprint requests to: Dr. Anita C. Gilliam, Department of Dermatology, Lakeside Hospital, Case Western Reserve University/University Hospitals of Cleveland, Euclid Avenue, Cleveland, OH presents antigen to naïve T cells (Schuler and Steinman, 1985; Teunissen et al, 1997). This maturation is accompanied by the inducible expression of several costimulatory molecules and the enhanced expression of HLA class II molecules. Recently, dendritic cells with features of Langerhans cells have been generated in vitro from human neonatal cord blood stem cell precursors (Caux et al, 1992) and from peripheral blood precursors (Sallusto and Lanzavecchia, 1994) using specialized culture conditions [granulocyte-macrophage colony stimulating factor, interleukin (IL)-4, and tunor necrosis factor-α]; however, the source (resident dermal precursors or blood derived dendritic cells) of Langerhans cells in epidermis in vivo and their maturation steps are not known. A useful model for the study of Langerhans cell entry into skin and phenotype after functional challenge is ultraviolet B (UVB) exposed skin (Cruz and Bergstresser, 1991). After UVB exposure, epidermal Langerhans cells are decreased in density and altered in morphology, becoming less dendritic (Toews et al, 1980). At 72 h, CD1a Langerhans cells are markedly decreased in numbers in UVB exposed epidermis and do not begin to reappear in large numbers until days 4 6 (Toews et al, 1980; Aberer et al, 1981); their disappearance is closely related in time to the development of an immunosuppressive environment and antigen specific tolerance to epicutaneous hapten (Streilein et al, 1980; Cooper et al, 1992). By 72 h, depletion of cells bearing HLA-DR but not OKT6 from epidermal suspensions reduces T cell proliferation in allogeneic epidermal cell-lymphocyte reactions, showing indirectly that at that time, Langerhans cells are not significantly contributing to induction of T cell proliferation by UV exposed skin (Cooper et al, 1985). At the same time that Langerhans cells disappear from the epidermis, infiltration of first the dermis and later the epidermis by IL X/98/$10.50 Copyright 1998 by The Society for Investigative Dermatology, Inc. 422
2 VOL. 110, NO. 4 APRIL 1998 HUMAN HAIR FOLLICLE producing CD11b monocyte/macrophages (Kang et al, 1994) 1 that are deficient in CD40, B7, and IL-12 2 and that induce T cell proliferation well is seen. We report here that the hair follicle is a reservoir for epidermal Langerhans cells after UVB injury to human skin. (This follicular reservoir paradigm is also seen in cutaneous thermal injury and in the autoimmune disease vitiligo, in which follicular keratinocytes and melanocytes replenish epidermal cell populations.) After UVB, Langerhans cells in follicular epithelium divide and appear to migrate from follicular infundibulum into surrounding epidermis. In addition, the early repopulating epidermal Langerhans cells present 72 h after UVB show an altered phenotype compared with Langerhans cells from unirradiated epidermis. These Langerhans cells have a selectively reduced capacity to express the costimulatory markers B7 1 and B7 2, but not CD40, in culture compared with Langerhans cells from unexposed control skin, suggesting an intermediate maturation step in the transition from hair follicle to epidermis with possible implications for T cell activation. Because of the demonstrated linkage of susceptibility in animals (Kripke and Fisher, 1976) and humans (Yoshikawa et al, 1990) to UVB induced skin tumors with development of an immunosuppressive state in UVB exposed skin, our data suggest the importance of a mechanism for a more rapid recovery of the protective cutaneous immune system after UVB than may be possible from blood precursors alone. MATERIALS AND METHODS Subjects Healthy adult volunteers (n 8) participated in the study after Institutional Review Board approval of the protocol and informed consent. As described previously (Cooper et al, 1992), four minimal erythema dose (MED) was delivered to buttock skin from Westinghouse FS20 bulbs at different time points. At the final time point, punch biopsies or keratomes were obtained from all UVB exposed and nonirradiated control sites. Immunohistochemical studies Antibodies Immunostaining was performed at least three times on each specimen with the following primary mouse monoclonal antibodies: CD1a (B , IgG2a; Immunotech, Westbrook, ME), CD11b (anti-mac-1/bear 1, IgG1; Immunotech), Ki-67 (Ki-S5, IgG1; Boehringer, Indianapolis, IN), and antibodies to cyclobutane pyrimidine dimers (TDM-2, IgG2a; gift of Dr. Osamu Nikaido, Kanazawa University, Japan). Secondary antibodies used for immunoperoxidase studies were biotin conjugated goat anti-mouse IgG1 or IgG2a (Caltag, San Francisco, CA) followed by peroxidase labeled streptavidin (Kirkegaard & Perry, Gaithersburg, MD). Double immunofluorescence staining for Ki-67 and CD1a was performed using fluorescein isothiocyanate conjugated goat anti-mouse IgG1 for Ki-67 (Boehringer), and biotin conjugated goat antimouse IgG2a for CD1a followed by Rhodamine Red-x conjugated avidin (Neutr-Avidin, Molecular Probes, Leiden, The Netherlands). Immunohistochemical procedures Six micrometer frozen sections were blocked with 10% goat serum, treated with primary antibody or its isotype control immunoglobulin, treated with biotin conjugated secondary antibody, peroxidase conjugated streptavidin (Kirkegaard & Perry), then detected with Diaminobenzidine Reagent Set (DAB) (Kirkegaard & Perry) and counterstained with hematoxylin. Before staining frozen tissue sections with antibodies to cyclobutane thymidine dimers (TDM-2), nuclear DNA was denatured with 70 mm NaOH in 70% ethanol for 2 min, followed by neutralization for 1 min in 100 mm Tris-HCL, ph 7.5 in 70% ethanol, three washes of 70% ethanol, and two washes of phosphate buffered saline (Chadwick et al, 1995). Microscopy and photography Images from immunostaining experiments were obtained using a Zeiss (Thornwood, NY) Axiophot microscope and Kodak (Rochester, NJ) Ektachrome 160T film (bright field studies) or P1600 film (immunofluorescence studies). These were scanned (SprintScan, Polaroid, Cambridge, MA) and formatted as tiff images in Adobe Photoshop and Illustrator. Analysis: quantitation of CD1a cells CD1a cells in the upper area of the 1 Gilliam AC, Moser A, Tootell E, Kang K, Cooper KD: Distinct physical and temporal compartments of antigen-presenting cells and IL-10 and TNFα expression in human UV-exposed skin by in situ hybridization and immunostaining. J Invest Dermatol 108:638, 1997 (abstr.) 2 Kremer IB, Cooper KD, Teunissen MBM, Stevens SR: Diminished CD40 expression on macrophages infiltrating UV-exposed skin is responsible for IL- 2Rα T cell activation. J Invest Dermatol 108:538, 1997 (abstr.) follicle and in the epidermis adjacent to the follicle were counted in unirradiated control skin and in skin 72 h after UVB using an ocular micrometer grid with 200 magnification. The compartments are delineated as A E with the areas of A, B1 B2, C1 C2, D1 D2, and E1 E2, each corresponding to mm 2 (Fig 4). After counting the number of CD1a cells in three sections per individual specimen (n 3), CD1a cells in UVB irradiated skin were expressed as a percentage ( SEM) of the mean count in the equivalent compartment in unirradiated control skin. Flow cytometry Antibodies For flow cytometry, the following mouse monoclonal antibodies were used: biotin conjugated anti-hla-dr (IgG2a; Becton Dickinson, Mountain View, CA), fluorescein isothiocyanate conjugated anti-cd1a (IgG1; Ortho, Raritan, NJ), and anti-cd40 (IgG1; Pharmingen, San Diego, CA), phycoerythrin conjugated anti-cd1a (OKT6; IgG1; Ortho), anti-b7 1 (CD80; IgG1; Becton Dickinson), anti-b7 2 (CD86; IgG1; Ancell, Bayport, MN), or isotype matched control antibodies from the same companies. Cascade-Bluestreptavidin was purchased from Molecular Probes (Eugene, OR). Flow cytometry protocol Keratome biopsies were obtained 72 h after four MED of UVB as previously described (Meunier et al, 1993). Epidermis was separated from dermis by incubation in dispase, digested in trypsin, and dissociated in 0.1% DNase (Sigma, St Louis, MO) in Hanks balanced salt solution containing 10% fetal bovine serum (Hyclone, Logan, UT). The suspension was filtered through 100 µm nylon mesh and cultured for 24 h in vitro in RPMI with 10% heat inactivated human AB serum (North American Biology, Miami, FL) to allow costimulatory molecule expression. Cells were incubated with human IgG (Sigma) to prevent nonspecific Fc receptor binding. Dead cells were identified by addition of ethidium monoazide (Molecular Probes) for 10 min under visible light for cross-linkage to DNA. Flow cytometry was performed using an Epics Elite (Coulter Cytometry). RESULTS Human hair follicle is a reservoir for Langerhans cells in skin depleted of epidermal Langerhans cells by UVB When human skin is exposed to four MED of UVB, interfollicular epidermal Langerhans cells (Fig 1a d, arrows) become less dendritic and are decreased in number after 24 h, with almost complete disappearance of CD1a cells at 72 h. Note the occasional CD1a dermal Langerhans cell-like cells in control unirradiated skin (Fig 1a) but not in irradiated skin. Lower power views of skin specimens from a single subject show numerous CD1a Langerhans cells in both follicular epithelium and epidermis in control tissue (Fig 2a, arrows). At later time points after UVB (48, 72, 96 h, Fig 2b d, respectively), CD1a cells are absent in interfollicular epidermis and dermis, but appear in and adjacent to follicles. At 96 h (Fig 2d), there are clearly increased numbers of CD1a cells in the follicular orifice and in the adjacent epidermis. At the same time, the epidermis and dermis at some distance from follicles showing prominent UVB injury (necrosis of epidermal keratinocytes) still lack CD1a cells. The CD1a cells in perifollicular epidermis adjacent to follicles at 48, 72, and 96 h may represent either Langerhans cells that are migrating from follicle to epidermis, or Langerhans cells left in the epidermis after UVB injury; the immunostaining results of this time course showing CD1a cells at progressive distances from the follicular orifice, suggest that Langerhans cells are migrating from follicle to epidermis. These changes can be appreciated in the low power view of a biopsy taken 72 h after UVB exposure from another subject (n 3, Fig 3a). The immunostaining results presented here are representative of those in all biopsies from all patients. Immunostaining of sections containing follicles from the same specimen with CD11b/CD18 (Mac-1) (Fig 3b) highlights the unique character of follicular epithelium and of epidermis adjacent to follicles after UVB; numerous infiltrating Mac-1 macrophages are seen in epidermis and dermis at some distance from but not adjacent to or within follicles, presenting the reverse image of CD1a staining (Fig 3a). Therefore, the hair follicle appears to be a relatively protected environment for and serves as a source of Langerhans cells that begin to replenish the epidermis 48 h after four MED UVB. Meanwhile, the epidermis at some distance from the follicle is injured, without CD1a cells, and is a site for migration of and infiltration by Mac-1 macrophages. Further support of follicular Langerhans cells as a reservoir for epidermal Langerhans cells is the observation that the other possible
3 424 GILLIAM ET AL THE JOURNAL OF INVESTIGATIVE DERMATOLOGY Figure 1. UVB-induced changes in epidermal Langerhans cells. Interfollicular CD1a epidermal Langerhans cells in human skin irradiated with four MED UVB change in morphology and numbers, becoming less dendritic at 6 h (b), depleted in number at 24h(c), and completely absent by 72 h (d), compared with control unirradiated skin (a). Immunoperoxidase staining with CD1a (brown staining cells, arrows) of tissue collected at time points after UVB. Note occasional CD1a dermal cells in control skin (a) but not in irradiated skin. Scale bar, 43 µm. Figure 2. UVB-induced changes in hair follicle Langerhans cells. CD1a Langerhans cells (brown staining cells, arrows) at time points after four MED UVB [(a) control unirradiated skin, (b) 48h,(c)72h,(d) 96 h] are present in progressively increased numbers in the follicular opening, whereas interfollicular epidermis distant from the hair follicle becomes devoid of CD1a cells. Sclae bar, 138 µm. Figure 3. Langerhans cells and macrophages occupy different compartments in UV-exposed skin. Lower power views of a biopsy specimen of skin 72 h after four MED UVB stained with CD1a (a) or CD11b (b) show that CD1a Langerhans cells and CD11b macrophages are present in distinctly different compartments in the skin after UVB. Scale bar, 344 µm. source of Langerhans cells migrating to the epidermis (papillary dermis) contains few if any CD1a cells at 48, 72, or 96 h after UVB (Fig 2b d, 3a). To quantitatively document that follicular epithelium contains increased numbers of Langerhans cells 72 h after UVB, we counted CD1a cells in epidermal compartments (n 3, inset, Fig 4). Epithelium at the follicular orifice (inset: A, B1 B2) contains significantly more CD1a cells than the immediately adjacent epidermis (C1 C2, D1 D2, and E1 E2). As Fig 4 shows, the numbers of Langerhans cells decrease with increasing distance from the hair follicle, with 100% representing control unirradiated skin. Deep follicular epithelium is protected from UVB It has been shown that UVB only reaches the epidermis and superficial dermis (Bruls et al, 1984). To evaluate the depth of direct UVB exposure in our skin samples and to show that follicular epithelium is relatively photoprotected, we performed immunostaining of biopsy tissue taken from buttock skin 10 min after UVB with antibodies to cyclobutane pyrimidine dimers (Qin et al, 1994; Vink et al, 1996). We confirmed that fewer thymidine dimers are found at increasing depth in the epidermis. Figure 5(a) shows no staining in control unirradiated skin, whereas Fig 5(b) shows numerous positive cells in the epidermis and superficial papillary dermis but not in the deeper follicle, with a sharp line of demarcation in the superficial portion of the hair follicle, showing that infundibulum and deep follicular epithelium are indeed protected from UVB radiation. Proliferating Langerhans cells are found in the hair follicle Immunostaining with Ki-67, which stains nuclei of cells in cycle (Gerdes et al, 1984), identifies numerous proliferating cells in follicular epithelium 72 h after UVB. Double-staining immunofluorescence studies using anti-ki-67 (fluorescein isothiocyanate) and anti- CD1a (rhodamine) (Fig 6) show that admixed with the green nuclei of Ki-67 proliferating keratinocytes are occasional cells with yellow
4 VOL. 110, NO. 4 APRIL 1998 HUMAN HAIR FOLLICLE 425 Figure 4. The numbers of CD1a cells 72 h after four MED UVB are high in the hair follicle and in the adjacent epidermis and form a gradient inversely related to distance from the follicle. The numbers of CD1a cells per square grid ( mm 2 ) in the upper area of the follicle and in the epidermis near the follicle were counted in unirradiated control skin and in skin 72 h after UVB using an ocular micrometer grid under the microscope. The image in the right corner shows the square compartments (A E) defined for counting. The percentage of CD1a cells SEM in each compartment (mean of three experiments) at 72 h versus control unirradiated skin (100%) is presented. Figure 6. Proliferating Langerhans cells are found in the hair follicle. Occasional proliferating Langerhans cells are seen in the follicular epithelium when double stained for CD1a (red staining dendritic cell bodies) and for Ki- 67 (yellow nuclei, white arrows) at 72 h after UVB. The remainder of Ki-67 cell nuclei staining green represent keratinocytes in the cell cycle. Scale bar,26 µm. Figure 5. Deep follicular epithelium is protected from UVB. The depth of penetration ( ) of UV in skin collected 10 min after a single dose of four MED UVB is shown by the presence of thymidine dimers (brown staining keratinocyte nuclei) in the epidermis and the upper follicular epithelium. Protected follicular epithelium deep to the infundibulum shows no thymidine dimers. Scale bar, 138 µm; inset, 72 µm. double-staining nuclei (white arrow) and red dendritic cell bodies that are positive for both CD1a and Ki-67, representing proliferating Langerhans cells. Therefore, although the majority of proliferating cells in the follicular epithelium of UVB irradiated skin are keratinocytes, there are also proliferating Langerhans cells. Hair follicles in control skin also showed a few CD1a Ki-67 cells (not shown); the numbers in both UV and control conditions are small. Newly migrating follicular Langerhans cells are deficient in upregulation of B7 but not of CD40 costimulatory molecules We next asked if the Langerhans cells present in UVB exposed epidermis 72 h after UVB, which are predominantly associated with the hair follicle (Figs 2b d, 3a, 4), are normal Langerhans cells. The ability of Langerhans cells to stimulate T cells depends on the presence of surface costimulatory molecules such as B7 and CD40 (Foy et al, 1996; Lenschow et al, 1996). Therefore, we investigated the expression of these costimulatory molecules using flow cytometry of Langerhans cells purified from control or UVB irradiated epidermis 72 h after four MED UVB, when Langerhans cells present in cell suspensions are likely to be those that have migrated from the hair follicle. [We verified that in routine histology of intact keratome and in dispase-split epidermal and dermal components of the keratome, the upper region of the hair follicle stays with the epidermis (not shown).] Epidermal cell suspensions were cultured in vitro for 24 h to mimic the maturation process observed when Langerhans cells migrate from the skin to the lymph nodes (Schuler and Steinman, 1985). After 1 d of culture, as expected, Langerhans cells from control skin strongly expressed B7 1, B7 2, and CD40 (Fig 7a, left panels, b). In contrast, Langerhans cells from UVB irradiated skin essentially failed to upregulate B7 1 or B7 2 during culture, but were clearly positive for newly expressed CD40 removed by trypsinization (Fig 7a, right panels, b), evidence for a partial deficit in costimulatory molecule expression. Although migration in this ex vivo model cannot be directly studied, together these data suggest that follicular Langerhans cells are sources for replenishment of epidermal Langerhans cells after a single dose of UVB, and that additional not yet characterized maturation steps occur after their migration into epidermis.
5 426 GILLIAM ET AL THE JOURNAL OF INVESTIGATIVE DERMATOLOGY DISCUSSION This study demonstrates the critical and unique role of hair follicles in the immune system of the skin. We show that Langerhans cells proliferate in and migrate from the hair follicle into UVB exposed epidermis, beginning to repopulate the epidermis as early as 48 h after a single dose of four MED UVB. The ability of Langerhans cells to divide and migrate is known (Miyauchi and Hashimoto, 1987); the factors that induce Langerhans cell division, maintain Langerhans cell/ keratinocyte ratios in epidermis, and initiate migration are not well characterized. Based on bone marrow transplantation studies of lethally irradiated mice and humans, in which repopulation of epidermis by Langerhans cells was shown to be entirely by cells with donor phenotype (Katz et al, 1979; Volc-Platzer et al, 1984), the route of entry into skin appeared to be via blood borne precursors originating in bone marrow. Whether these precursors take up residence in the perivascular dermis, enter directly into the epidermis, or enter the epidermis via the hair follicle is unknown. The present data using a physiologic skin challenge of a single four MED of UVB, which results in almost complete depletion of interfollicular epidermal CD1a cells, indicate that one pathway for repopulation of epidermal Langerhans cells is a local one via the hair follicle. This study suggests that newly emigrated follicular Langerhans cells have a different phenotype than interfollicular epidermal Langerhans cells, in that they are able to induce CD40 but not B7 expression in culture; the properties acquired in culture are thought to model the functional changes that occur during stimulated Langerhans cell migration from the epidermis to regional lymph nodes. The afferent pathway of Langerhans cell trafficking from blood and tissue into epidermis is less well understood; our data identifying follicular Langerhans cells as a resource for epidermal Langerhans cells will be useful for dissecting out that differentiation pathway. Because T cell activation in the absence of B7 costimulation can result in antigen specific unresponsiveness (Gimmi et al, 1993), the presence of B7 deficient Langerhans cells in UV exposed skin is likely to have consequences for immune activation and tolerance induction. Changes in the cytokine environment in UVB irradiated skin, such as the presence of IL-10 producing UV macrophages, will also influence the phenotype of Langerhans cells repopulating the epidermis from the hair follicle, because IL-10 can directly downregulate B7 expression (Ding et al, 1993; Ozawa et al, 1996). Therefore, Langerhans cells in the hair follicle may be exposed to different microenvironments of cytokines and growth factors as they migrate to the epidermis following UVB. Further studies of the follicular and epidermal microenvironments in which Langerhans cells reside will provide important information about possible mechanisms of Langerhans cell maturation and function, and roles in immune surveillance. Note added in proof: Follicular infundibular Langerhans cells may also replenish epidermis in chronically UV-exposed human skin (Murphy et al, 1998). We thank the many volunteers who donated skin biopsies and keratomes for these studies. We appreciate also the excellent secretarial assistance of Virginia Ehrbar with this manuscript. This work was supported in part by grants from the Dermatology Foundation (ACG, Mary Kay Cosmetics Grant; SRS, Procter and Gamble Fellowship); Ohio Regents Pilot Study Grant (ACG); National Alopecia Areata Foundation (ACG; 44); Netherlands Organization for Scientific Research Fellowship, Dutch Cancer Figure 7. Langerhans cells in skin 72 h after four MED UVB are deficient in their ability to upregulate B7 1 and B7 2, but not CD40. Epidermal cells were isolated from UV exposed and nonirradiated control keratomes obtained 72 h after UV exposure and analyzed by four color flow cytometry. (a) Representative flow diagrams of B7 1, B7 2, and CD40 expression on CD1a HLA-DR ethidium monoazide (viable) Langerhans cells. The left panels show Langerhans cells from control skin (C-Langerhans cells), the right panels show Langerhans cells from UV-exposed skin (UV-Langerhans cells). Percentages of positive cells are given in the upper right boxes in each panel. Only 2% of UV-Langerhans cells express B7 1, compared with 50% of C-Langerhans cells. Similarly, only 19% of UV-Langerhans cells express B7 2, compared with 86% of C-Langerhans cells. In contrast, the percentage of UV- Langerhans cells expressing CD40 is almost the same as that of C-Langerhans cells (71 and 76%, respectively). (b) Mean values of B7 1, B7 2, and CD40 expression (delta mean fluorescence) for four experiments. Delta mean fluorescence for B7 1 and B7 2 was significantly lower for Langerhans cells from UV irradiated skin (y) as compared with nonirradiated control skin (j); * indicated p 0.05.
6 VOL. 110, NO. 4 APRIL 1998 HUMAN HAIR FOLLICLE 427 Foundation, and Christine Buisman Foundation (IBK); NIAID #AI (KDC); Case Western Reserve University Skin Disease Research Center, NIAMS (ACG and SRS), and the Veterans Administration Hospital (KDC). REFERENCES Aberer G, Schuler G, Stingl G, Hönigsmann H, Wolff K: Ultraviolet light depletes surface markers of Langerhans cells. J Invest Dermatol 76: , 1981 Breathnach AS: The distribution of Langerhans cells within the human hair follicle and some observations on its staining properties with gold chloride. J Anat 97:73 80, 1963 Breathnach SM: Origin cell lineage ontogeny tissue distribution, kinetics of Langerhans cells. In: Schuler G (ed.). Epidermal Langerhans Cells, CRC Press, Boca Raton, 1991, pp Bruls WAG, Slaper H, Van Der Leun JC, Berrens L: Transmission of human epidermis and stratum corneum as a function of thickness in the ultraviolet and visible wavelengths. Photochem Photobiol 40: , 1984 Caux C, Dezutter-Dambuyant C, Schmitt D, Banchereau J: GM-CSF and TNF-alpha cooperate in the generation of dendritic Langerhans cells. Nature 360: , 1992 Chadwick CA, Potten CS, Nikaido O, Matsunaga T, Proby C, Young AR: The detection of cyclobutane thymine dimers (6 4) photolesions and the Dewar photoisomers in sections of UV-irradiated human skin using specific antibodies, and the demonstration of depth penetration effects. J Photochem Photobiol 28: , 1995 Cooper KD, Fox P, Neises G, Katz SI: Effects of ultraviolet radiation on human epidermal cell alloantigen presentation: Initial depression of Langerhans cell-dependent function is followed by the appearance of T6- Dr cells that enhance epidermal alloantigen presentation. J Immunol 134: , 1985 Cooper KD, Oberhelman L, Hamilton TA, et al: UV exposure reduces immunization rates and promotes tolerance to epicutaneous antigens in humans: Relationship to dose, CD1a-DR epidermal macrophage induction, and Langerhans cell depletion. Proc Natl Acad Sci USA 89: , 1992 Cruz PD Jr, Bergstresser PR: The influence of ultraviolet radiation and other physical and chemical agents on epidermal Langerhans cells. In: Schuler G (ed.). Epidermal Langerhans Cells, CRC Press, Boca Raton, 1991, pp Ding L, Linsley PS, Huang L-Y, Germain RN, Shevach EM: IL-10 inhibits macrophage costimulatory activity by selectively inhibiting the up-regulation of B7 expression. J Immunol 151: , 1993 Foy TM, Aruffo A, Bajorath J, Buhlmann JE, Noelle RJ: Immune regulation by CD40 and its ligand gp39. Annu Rev Immunol 14: , 1996 Gerdes J, Lemke H, Baisch H, Wacker H-H, Schwab U, Stein H: Cell cycle analysis of a cell proliferation-associated human nuclear antigen defined by the monoclonal antibody Ki-67. J Immunol 133: , 1984 Gimmi CD, Freeman GJ, Gribben JG, Gray G, Nadler LM: Human T-cell clonal anergy is induced by antigen presentation in the absence of B7 costimulation. Proc Natl Acad Sci USA 90: , 1993 Kang K, Hammerberg C, Meunier L, Cooper KD: CD11b macrophages that infiltrate human epidermis after in vivo ultraviolet exposure potently produce IL-10 and represent the major secretory source of epidermal IL-10 protein. J Immunol 153: , 1994 Katz SI, Tamaki K, Sachs DH: Epidermal Langerhans cells are derived from cells originating in bone marrow. Nature 282: , 1979 Kripke ML, Fisher MS: Immunologic parameters for ultraviolet carcinogenesis. J Natl Cancer Inst 57: , 1976 Lenschow DJ, Walunas TL, Bluestone JA: CD28/B7 system of T cell costimulation. Annu Rev Immunol 14: , 1996 Meunier L, Gonzalez-Ramos A, Cooper KD: Heterogeneous populations of class II MHC cells in human dermal cell suspensions. Identification of a small subset responsible for potent dermal antigen-presenting cell activity with features analogous to Langerhans cells. J Immunol 151: , 1993 Miyauchi S, Hashimoto K: Epidermal Langerhans cells undergo mitosis during the early recovery phase after ultraviolet-b irradiation. J Invest Dermatol 88: , 1987 Murphy GF, Messadi D, Fonferko E, Hancock WW: Phenotypic transformation of macrophages to Langerhans cells in the skin. Am J Pathol 123: , 1986 Murphy GF, Katz S, Kligman AM: Topical tretinoin replenishes CD1a-positive epidermal Langerhans cells in chronically photo-damaged human skin. J Cutan Pathol 25:30 34, 1998 Ozawa H, Aiba S, Nakagawa S, Tagami H: Interferon-gamma and interleukin-10 inhibit antigen presentation by Langerhans cells for T helper type 1 cells by suppressing their CD80 (B7 1) expression. Eur J Immunol 26: , 1996 Qin X, Zhang S, Nakatsuru Y, Oda H, Yamazaki Y, Suzuki T, Nikaido O, Ishikawa T: Detection of active UV-photoproduct repair in monkey skin in vivo by quantitative immunohistochemistry. Cancer Lett 83: , 1994 Romani N, Schuler G, Fritsch P: Identification and phenotype of epidermal Langerhans cells. In: Schuler G (ed.). Epidermal Langerhans Cells, CRC Press, Boca Raton, 1991, pp Rowden G, Lewis MG, Sullivan AK: Ia antigen expression on human epidermal Langerhans cells. Nature 268: , 1977 Sallusto F, Lanzavecchia A: Efficient presentation of soluble antigen by cultured human dendritic cells is maintained by granulocyte/macrophage colony -stimulating factor plus interleukin 4 and downregulated by tumor necrosis factor alpha. J Exp Med 179: , 1994 Schuler G, Steinman RM: Murine epidermal Langerhans cells mature into potent immunostimulatory dendritic cells in vitro. J Exp Med 161: , 1985 Silberberg-Sinakin I, Thorbecke GJ, Baer RL, Rosenthal SA, Berezowsky V: Antigenbearing Langerhans cells in skin, dermal lymphatics and in lymph nodes. Cell Immunol 25: , 1976 Stingl G, Shevach EM: Langerhans cells as antigen-presenting cells. In: Schuler G (ed.). Epidermal Langerhans Cells, CRC Press, Boca Raton, 1991, pp Streilein JW, Toews GT, Gilliam JN, Bergstresser PR: Tolerance or hypersensitivity to 2,4-dinitro-1-fluorobenzene: the role of Langerhans cell density within epidermis. J Invest Dermatol 74: , 1980 Teunissen MBM, Kapsenberg ML, Bos JD: Langerhans cells and related skin dendritic cells. In: Bos JD (ed.). Skin Immune System, 2nd edn, CRC Press, Boca Raton, 1997, pp Toews GB, Bergstresser PR, Streilein JW, Sullivan S: Epidermal Langerhans cell density determines whether contact hypersensitivity or unresponsiveness follows skin painting with DNFB. J Immunol 124: , 1980 Vink AA, Strickland FM, Bucana C, Cox PA, Roza L, Yarosh DB, Kripke ML: Localization of DNA damage and its role in altered antigen-presenting cell function in ultravioletirradiated mice. J Exp Med 183: , 1996 Volc-Platzer B, Stingl G, Wolff K, Hinterberger W, Schnedl W: Cytogenetic identification of allogeneic epidermal Langerhans cells in a bone-marrow-graft recipient. [letter]. N Engl J Med 310: , 1984 Yoshikawa T, Rae V, Bruins-Slot W, Van den Berg J-W, Taylor JR, Streilein JW: Susceptibility to effects of UVB radiation on induction of contact hypersensitivity as a risk factor for skin cancer in humans. J Invest Dermatol 95: , 1990
THE EFFECTS OF REPEATED SUB-ERYTHEMAL EXPOSURES OF UVR ON HUMAN IMMUNITY
 THE EFFECTS OF REPEATED SUB-ERYTHEMAL EXPOSURES OF UVR ON HUMAN IMMUNITY Joanna Narbutt Department of Dermatology Medical University of Lodz, Lodz, Poland Photoimmunosuppression ULTRAVIOLET RADIATION DNA
THE EFFECTS OF REPEATED SUB-ERYTHEMAL EXPOSURES OF UVR ON HUMAN IMMUNITY Joanna Narbutt Department of Dermatology Medical University of Lodz, Lodz, Poland Photoimmunosuppression ULTRAVIOLET RADIATION DNA
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: van Seters M, van Beurden M, ten Kate FJW, et al. Treatment
to Langerhans Cells in the Skin
 401 RAPID COMMUNICATION Ph enotypic Transformation of Macrophages to Langerhans Cells in the Skin GEORGE F. MURPHY, MD, DIANA MESSADI, BDS, MMSc, EILEEN FONFERKO, BS, and WAYNE W. HANCOCK, MD, PhD From
401 RAPID COMMUNICATION Ph enotypic Transformation of Macrophages to Langerhans Cells in the Skin GEORGE F. MURPHY, MD, DIANA MESSADI, BDS, MMSc, EILEEN FONFERKO, BS, and WAYNE W. HANCOCK, MD, PhD From
CHAPTER 3 LABORATORY PROCEDURES
 CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
The Role of Epidermal Langerhans Cells in NB-UVB-Induced Immunosuppression
 Kobe J. Med. Sci., Vol. 59, No. 1, pp. E1-E9, 2013 The Role of Epidermal Langerhans Cells in NB-UVB-Induced Immunosuppression KUMIKO TAGUCHI 1, ATSUSHI FUKUNAGA 1,, KANAKO OGURA 1, and CHIKAKO NISHIGORI
Kobe J. Med. Sci., Vol. 59, No. 1, pp. E1-E9, 2013 The Role of Epidermal Langerhans Cells in NB-UVB-Induced Immunosuppression KUMIKO TAGUCHI 1, ATSUSHI FUKUNAGA 1,, KANAKO OGURA 1, and CHIKAKO NISHIGORI
DEPLETION OF EPIDERMAL LANGERHANS CELLS MOUSE SKIN* BY J. WAYNE STREILEIN, LANYA WHITE LONSBERRY, AND PAUL R. BERGSTRESSER
 Published Online: 1 March, 1982 Supp Info: http://doi.org/10.1084/jem.155.3.863 Downloaded from jem.rupress.org on August 17, 2018 DEPLETION OF EPIDERMAL LANGERHANS CELLS AND Ia IMMUNOGENICITY FROM TAPE-STRIPPED
Published Online: 1 March, 1982 Supp Info: http://doi.org/10.1084/jem.155.3.863 Downloaded from jem.rupress.org on August 17, 2018 DEPLETION OF EPIDERMAL LANGERHANS CELLS AND Ia IMMUNOGENICITY FROM TAPE-STRIPPED
To determine the effect of over-expression and/or ligand activation of. PPAR / on cell cycle, cell lines were cultured as described above until ~80%
 Supplementary Materials and Methods Cell cycle analysis To determine the effect of over-expression and/or ligand activation of PPAR / on cell cycle, cell lines were cultured as described above until ~80%
Supplementary Materials and Methods Cell cycle analysis To determine the effect of over-expression and/or ligand activation of PPAR / on cell cycle, cell lines were cultured as described above until ~80%
Effect of Propecia on the Hair Follicle in Male Androgenetic Alopecia: A Confocal Laser Scanning Microscopy and Video Imaging Study
 Effect of Propecia on the Hair Follicle in Male Androgenetic Alopecia: A Confocal Laser Scanning Microscopy and Video Imaging Study Investigators: Department of Dermatology, University of Minnesota, Minneapolis,
Effect of Propecia on the Hair Follicle in Male Androgenetic Alopecia: A Confocal Laser Scanning Microscopy and Video Imaging Study Investigators: Department of Dermatology, University of Minnesota, Minneapolis,
Soe Janssens, Stan Pavel, Coby Out-Luiting, Rein Willemze and Frank de Gruijl. British Journal of Dermatology 2005; 152:
 4 Normalized UV induction of Langerhans cell depletion and neutrophil infiltrates after artificial UVB hardening of patients with polymorphic light eruption Soe Janssens, Stan Pavel, Coby Out-Luiting,
4 Normalized UV induction of Langerhans cell depletion and neutrophil infiltrates after artificial UVB hardening of patients with polymorphic light eruption Soe Janssens, Stan Pavel, Coby Out-Luiting,
UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication
 UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication Citation for published version (APA): di Nuzzo, S. (2000). Effects of ultraviolet
UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication Citation for published version (APA): di Nuzzo, S. (2000). Effects of ultraviolet
SUPPLEMENTARY INFORMATION
 DOI:.38/ncb3399 a b c d FSP DAPI 5mm mm 5mm 5mm e Correspond to melanoma in-situ Figure a DCT FSP- f MITF mm mm MlanaA melanoma in-situ DCT 5mm FSP- mm mm mm mm mm g melanoma in-situ MITF MlanaA mm mm
DOI:.38/ncb3399 a b c d FSP DAPI 5mm mm 5mm 5mm e Correspond to melanoma in-situ Figure a DCT FSP- f MITF mm mm MlanaA melanoma in-situ DCT 5mm FSP- mm mm mm mm mm g melanoma in-situ MITF MlanaA mm mm
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
SUPPLEMENTARY INFORMATION. Involvement of IL-21 in the epidermal hyperplasia of psoriasis
 SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
DENDRITIC CELL PROGENITORS, mouse, liver, MIGRATION, CHIMERISM
 Transplantation Proceedings (1994) Cell Transplant Society Meeting Minneapolis MN, May 1994 April 21, 1994 DENDRITIC CELL PROGENITORS, mouse, liver, MIGRATION, CHIMERISM PROPAGATION OF DENDRITIC CELL PROGENITORS
Transplantation Proceedings (1994) Cell Transplant Society Meeting Minneapolis MN, May 1994 April 21, 1994 DENDRITIC CELL PROGENITORS, mouse, liver, MIGRATION, CHIMERISM PROPAGATION OF DENDRITIC CELL PROGENITORS
Supplementary Information
 Supplementary Information Figure S1: Follicular melanocytes in the wound peripheral area migrate to the epidermis in response to wounding stimuli. Dorsal skin of Trp2-LacZ mice stained with X-gal and analyzed
Supplementary Information Figure S1: Follicular melanocytes in the wound peripheral area migrate to the epidermis in response to wounding stimuli. Dorsal skin of Trp2-LacZ mice stained with X-gal and analyzed
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels
 Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Post Kala-azar Dermal Leishmaniasis (PKDL) from the field to the cellular and the subcellular levels A M EL Hassan Institute of Endemic Diseases University of Khartoum Introduction PKDL is a VL related
Comparative Anatomical Factors Affecting Topical Delivery
 Comparative Anatomical Factors Affecting Topical Delivery Nancy A. Monteiro-Riviere, Ph.D., Fellow ATS Professor of Investigative Dermatology and Toxicology Center for Chemical Toxicology Research and
Comparative Anatomical Factors Affecting Topical Delivery Nancy A. Monteiro-Riviere, Ph.D., Fellow ATS Professor of Investigative Dermatology and Toxicology Center for Chemical Toxicology Research and
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication
 UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication Citation for published version (APA): di Nuzzo, S. (2000). Effects of ultraviolet
UvA-DARE (Digital Academic Repository) Effects of ultraviolet radiation on cutaneous T cells di Nuzzo, S. Link to publication Citation for published version (APA): di Nuzzo, S. (2000). Effects of ultraviolet
Dendritic Cell Based Immunotherapy for Cancer. Edgar G. Engleman, M.D.
 Dendritic Cell Based Immunotherapy for Cancer Edgar G. Engleman, M.D. Two main DC subsets Myeloid (mydc) Derived from monocytes Capture/process/present Ag to T cells Activate NK cells and B cells Plasmacytoid
Dendritic Cell Based Immunotherapy for Cancer Edgar G. Engleman, M.D. Two main DC subsets Myeloid (mydc) Derived from monocytes Capture/process/present Ag to T cells Activate NK cells and B cells Plasmacytoid
Supplemental Information. Aryl Hydrocarbon Receptor Controls. Monocyte Differentiation. into Dendritic Cells versus Macrophages
 Immunity, Volume 47 Supplemental Information Aryl Hydrocarbon Receptor Controls Monocyte Differentiation into Dendritic Cells versus Macrophages Christel Goudot, Alice Coillard, Alexandra-Chloé Villani,
Immunity, Volume 47 Supplemental Information Aryl Hydrocarbon Receptor Controls Monocyte Differentiation into Dendritic Cells versus Macrophages Christel Goudot, Alice Coillard, Alexandra-Chloé Villani,
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Anti-DC-SIGN/CD209 murine monoclonal antibodies
 Anti-DC-SIGN/CD209 murine monoclonal antibodies DC-SIGN (DC Specific, ICAM-3 Grabbing, Nonintegrin) / CD209 and L-SIGN (liver/lymph node-specific ICAM-3-grabbing nonintegrin CD299/ DC-SIGNR (DC-SIGN-related
Anti-DC-SIGN/CD209 murine monoclonal antibodies DC-SIGN (DC Specific, ICAM-3 Grabbing, Nonintegrin) / CD209 and L-SIGN (liver/lymph node-specific ICAM-3-grabbing nonintegrin CD299/ DC-SIGNR (DC-SIGN-related
The Skinny of the Immune System
 The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
Immunity. Acquired immunity differs from innate immunity in specificity & memory from 1 st exposure
 Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
Immunity (1) Non specific (innate) immunity (2) Specific (acquired) immunity Characters: (1) Non specific: does not need special recognition of the foreign cell. (2) Innate: does not need previous exposure.
MACROPHAGE "MONOCYTES" SURFACE RECEPTORS
 LECTURE: 13 Title: MACROPHAGE "MONOCYTES" SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the blood monocytes (size, and shape of nucleus). Enumerate some of the monocytes
LECTURE: 13 Title: MACROPHAGE "MONOCYTES" SURFACE RECEPTORS LEARNING OBJECTIVES: The student should be able to: Describe the blood monocytes (size, and shape of nucleus). Enumerate some of the monocytes
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
HHS Public Access Author manuscript J Invest Dermatol. Author manuscript; available in PMC 2015 January 01.
 RNA-seq Permits a Closer Look at Normal Skin and Psoriasis Gene Networks David Quigley 1,2,3 1 Helen Diller Family Comprehensive Cancer Center, University of California at San Francisco, San Francisco,
RNA-seq Permits a Closer Look at Normal Skin and Psoriasis Gene Networks David Quigley 1,2,3 1 Helen Diller Family Comprehensive Cancer Center, University of California at San Francisco, San Francisco,
T Lymphocyte Activation and Costimulation. FOCiS. Lecture outline
 1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
effect on the upregulation of these cell surface markers. The mean peak fluorescence intensity
 SUPPLEMENTARY FIGURE 1 Supplementary Figure 1 ASIC1 disruption or blockade does not effect in vitro and in vivo antigen-presenting cell activation. (a) Flow cytometric analysis of cell surface molecules
SUPPLEMENTARY FIGURE 1 Supplementary Figure 1 ASIC1 disruption or blockade does not effect in vitro and in vivo antigen-presenting cell activation. (a) Flow cytometric analysis of cell surface molecules
were isolated from the freshly drawn blood of healthy donors and ACS patients using the
 Supplemental Figure 1. Quality control of CD4 + T-cell purification. CD4 + T cells were isolated from the freshly drawn blood of healthy donors and ACS patients using the RosetteSep CD4 + T Cell Enrichment
Supplemental Figure 1. Quality control of CD4 + T-cell purification. CD4 + T cells were isolated from the freshly drawn blood of healthy donors and ACS patients using the RosetteSep CD4 + T Cell Enrichment
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells
 Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
Effects of McAb and rhil-2 activated bone marrow on the killing and purging of leukemia cells X.C. Wei, D.D. Yang, X.R. Han, Y.A. Zhao, Y.C. Li, L.J. Zhang and J.J. Wang Institute of hematological research,
CD14 + S100A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer
 CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
SEVENTH EDITION CHAPTER
 Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Third line of Defense. Topic 8 Specific Immunity (adaptive) (18) 3 rd Line = Prophylaxis via Immunization!
 Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
immunity produced by an encounter with an antigen; provides immunologic memory. active immunity clumping of (foreign) cells; induced by crosslinking
 active immunity agglutination allografts immunity produced by an encounter with an antigen; provides immunologic memory. clumping of (foreign) cells; induced by crosslinking of antigenantibody complexes.
active immunity agglutination allografts immunity produced by an encounter with an antigen; provides immunologic memory. clumping of (foreign) cells; induced by crosslinking of antigenantibody complexes.
Supplementary Figure 1: Fn14 is upregulated in the epidermis and dermis of mice
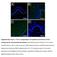 Supplementary Figure 1: Fn14 is upregulated in the epidermis and dermis of mice undergoing AD- and psoriasis-like disease. Immunofluorescence staining for Fn14 (green) and DAPI (blue) in skin of naïve
Supplementary Figure 1: Fn14 is upregulated in the epidermis and dermis of mice undergoing AD- and psoriasis-like disease. Immunofluorescence staining for Fn14 (green) and DAPI (blue) in skin of naïve
NIH Public Access Author Manuscript J Invest Dermatol. Author manuscript; available in PMC 2014 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2013 October ; 133(10): 2311 2314. doi:10.1038/jid.2013.239. Mechanisms of contact sensitization offer insights
NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2013 October ; 133(10): 2311 2314. doi:10.1038/jid.2013.239. Mechanisms of contact sensitization offer insights
Adaptive Immunity. Jeffrey K. Actor, Ph.D. MSB 2.214,
 Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
EFFECTS OF CRUDE OIL AND ULTRAVIOLET RADIATION ON IMMUNITY WITHIN MOUSE SKIN
 u,-.. EFFECTS OF CRUDE OIL AND ULTRAVIOLET RADIATION ON IMMUNITY WITHIN MOUSE SKIN Kim Burnham and Marcie Bey Department of Botany and Microbiology Oklahoma State University E-050 University Center for
u,-.. EFFECTS OF CRUDE OIL AND ULTRAVIOLET RADIATION ON IMMUNITY WITHIN MOUSE SKIN Kim Burnham and Marcie Bey Department of Botany and Microbiology Oklahoma State University E-050 University Center for
Detection of small numbers of immature cells in the blood of healthy subjects
 886 J Clin Pathol 1998;51:886 890 Haematology-Oncology Department, Humboldt University, Berlin, Germany J Oertel B Oertel J Schleicher D Huhn Correspondence to: Dr J Oertel, Hämatologisch-Onkologische
886 J Clin Pathol 1998;51:886 890 Haematology-Oncology Department, Humboldt University, Berlin, Germany J Oertel B Oertel J Schleicher D Huhn Correspondence to: Dr J Oertel, Hämatologisch-Onkologische
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
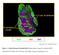 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
IL-34 is a tissue-restricted ligand of CSF1R required for the development of Langerhans cells and microglia
 Supplementary Figures IL-34 is a tissue-restricted ligand of CSF1R required for the development of Langerhans cells and microglia Yaming Wang, Kristy J. Szretter, William Vermi, Susan Gilfillan, Cristina
Supplementary Figures IL-34 is a tissue-restricted ligand of CSF1R required for the development of Langerhans cells and microglia Yaming Wang, Kristy J. Szretter, William Vermi, Susan Gilfillan, Cristina
IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS
 LECTURE: 07 Title: IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS LEARNING OBJECTIVES: The student should be able to: The chemical nature of the cellular surface receptors. Define the location of the
LECTURE: 07 Title: IMMUNE CELL SURFACE RECEPTORS AND THEIR FUNCTIONS LEARNING OBJECTIVES: The student should be able to: The chemical nature of the cellular surface receptors. Define the location of the
Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was
 Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was painted on the shaved back skin of CBL/J and BALB/c mice for consecutive days. (a, b) Phenotypic presentation of mouse back skin
Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was painted on the shaved back skin of CBL/J and BALB/c mice for consecutive days. (a, b) Phenotypic presentation of mouse back skin
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Supplemental Table 1. Primer sequences for transcript analysis
 Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Pathologic Stage. Lymph node Stage
 ASC ASC a c Patient ID BMI Age Gleason score Non-obese PBMC 1 22.1 81 6 (3+3) PBMC 2 21.9 6 6 (3+3) PBMC 3 22 84 8 (4+4) PBMC 4 24.6 68 7 (3+4) PBMC 24. 6 (3+3) PBMC 6 24.7 73 7 (3+4) PBMC 7 23. 67 7 (3+4)
ASC ASC a c Patient ID BMI Age Gleason score Non-obese PBMC 1 22.1 81 6 (3+3) PBMC 2 21.9 6 6 (3+3) PBMC 3 22 84 8 (4+4) PBMC 4 24.6 68 7 (3+4) PBMC 24. 6 (3+3) PBMC 6 24.7 73 7 (3+4) PBMC 7 23. 67 7 (3+4)
Evaluation of Apoptotic Cells Induced by Ultraviolet Light B Radiation in Epidermal Sheets Stained by the TUNEL Technique
 Evaluation of Apoptotic Cells Induced by Ultraviolet Light B Radiation in Epidermal Sheets Stained by the TUNEL Technique Hiroyuki Okamoto, Kana Mizuno, Taketo Itoh, Kiyoji Tanaka,* and Takeshi Horio Department
Evaluation of Apoptotic Cells Induced by Ultraviolet Light B Radiation in Epidermal Sheets Stained by the TUNEL Technique Hiroyuki Okamoto, Kana Mizuno, Taketo Itoh, Kiyoji Tanaka,* and Takeshi Horio Department
Macrophages form functional vascular mimicry channels in vivo. SI Figures and Legend
 Macrophages form functional vascular mimicry channels in vivo Authors: *Faith H. Barnett, *Mauricio Rosenfeld, Malcolm Wood, William Kiosses, Yoshihiko Usui, Valentina Marchetti, Edith Aguilar, and Martin
Macrophages form functional vascular mimicry channels in vivo Authors: *Faith H. Barnett, *Mauricio Rosenfeld, Malcolm Wood, William Kiosses, Yoshihiko Usui, Valentina Marchetti, Edith Aguilar, and Martin
UV and Children s Skin
 UV and Children s Skin Beate Volkmer and Rüdiger Greinert Division of Molecular Cellbiology Center of Dermatology, Elbeklinikum Buxtehude Germany Epidemiological studies indicate that sunburns in childhood
UV and Children s Skin Beate Volkmer and Rüdiger Greinert Division of Molecular Cellbiology Center of Dermatology, Elbeklinikum Buxtehude Germany Epidemiological studies indicate that sunburns in childhood
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells
 CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Afferent lymph-derived T cells and dendritic cells use different CCR7-dependent routes for lymph node entry and intranodal migration
 Braun et al. Supplementary Information 1 Supplementary Information Afferent lymph-derived T cells and dendritic cells use different CCR7-dependent routes for lymph node entry and intranodal migration Asolina
Braun et al. Supplementary Information 1 Supplementary Information Afferent lymph-derived T cells and dendritic cells use different CCR7-dependent routes for lymph node entry and intranodal migration Asolina
L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity
 Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
On the Discovery of the Dendritic Cell and Its Role in Adaptive Immunity
 Jake Noveck Queens College, Biology Senior Ralph M. Steinman, MD (January 14, 1943 September 30, 2011) On the Discovery of the Dendritic Cell and Its Role in Adaptive Immunity Every time that we breathe,
Jake Noveck Queens College, Biology Senior Ralph M. Steinman, MD (January 14, 1943 September 30, 2011) On the Discovery of the Dendritic Cell and Its Role in Adaptive Immunity Every time that we breathe,
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2*
 Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
Ex vivo Human Antigen-specific T Cell Proliferation and Degranulation Willemijn Hobo 1, Wieger Norde 1 and Harry Dolstra 2* 1 Department of Laboratory Medicine - Laboratory of Hematology, Radboud University
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T Cell Activation, Costimulation and Regulation
 1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
Case 3. Ann T. Moriarty,MD
 Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Case 3 Ann T. Moriarty,MD Case 3 59 year old male with asymptomatic cervical lymphadenopathy. These images are from a fine needle biopsy of a left cervical lymph node. Image 1 Papanicolaou Stained smear,100x.
Using the Ch6diak-Higashi Marker
 A Study of the Origin of Pulmonary Macrophages Using the Ch6diak-Higashi Marker Kent J. Johnson, MD, Peter A. Ward, MD, Gary Striker, MD, and Robin Kunkel, MS Using bone marrow reconstitution techniques
A Study of the Origin of Pulmonary Macrophages Using the Ch6diak-Higashi Marker Kent J. Johnson, MD, Peter A. Ward, MD, Gary Striker, MD, and Robin Kunkel, MS Using bone marrow reconstitution techniques
ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko ; IIZUKA, Hajime
 Journal of Dermatology (2011) 38(5):515-517. Granulocyte colony stimulating factor-producing squamous cell carcinoma of the skin ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko
Journal of Dermatology (2011) 38(5):515-517. Granulocyte colony stimulating factor-producing squamous cell carcinoma of the skin ITO, Yasuhiro ; FUJII, Mizue ; SHIBUYA, Takashi ; UEHARA, Jiro ; SATO, Katsuhiko
Product Datasheet. HLA ABC Antibody (W6/32) NB Unit Size: 0.25 mg. Store at -20C. Avoid freeze-thaw cycles. Reviews: 1 Publications: 22
 Product Datasheet HLA ABC Antibody (W6/32) NB100-64775 Unit Size: 0.25 mg Store at -20C. Avoid freeze-thaw cycles. Reviews: 1 Publications: 22 Protocols, Publications, Related Products, Reviews, Research
Product Datasheet HLA ABC Antibody (W6/32) NB100-64775 Unit Size: 0.25 mg Store at -20C. Avoid freeze-thaw cycles. Reviews: 1 Publications: 22 Protocols, Publications, Related Products, Reviews, Research
SUPPLEMENTARY INFORMATION
 Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Supplementary Materials. for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis
 Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
Immune Reconstitution Following Hematopoietic Cell Transplant
 Immune Reconstitution Following Hematopoietic Cell Transplant Patrick J. Kiel, PharmD, BCPS, BCOP Clinical Pharmacy Specialist Indiana University Simon Cancer Center Conflicts of Interest Speaker Bureau
Immune Reconstitution Following Hematopoietic Cell Transplant Patrick J. Kiel, PharmD, BCPS, BCOP Clinical Pharmacy Specialist Indiana University Simon Cancer Center Conflicts of Interest Speaker Bureau
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:!
 LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
LIST OF ORGANS FOR HISTOPATHOLOGICAL ANALYSIS:!! Neural!!!!!!Respiratory:! Brain : Cerebrum,!!! Lungs and trachea! Olfactory, Cerebellum!!!!Other:! Spinal cord and peripheral nerves! Eyes, Inner ear, nasal
Cytokine Complex Expanded Natural Killer Cells Improve Allogeneic Lung. Transplant Function via Depletion of Donor Dendritic Cells
 Cytokine Complex Expanded Natural Killer Cells Improve Allogeneic Lung Transplant Function via Depletion of Donor Dendritic Cells Wolfgang Jungraithmayr, Laura Codarri, Gregory Bouchaud,Carsten Krieg,
Cytokine Complex Expanded Natural Killer Cells Improve Allogeneic Lung Transplant Function via Depletion of Donor Dendritic Cells Wolfgang Jungraithmayr, Laura Codarri, Gregory Bouchaud,Carsten Krieg,
Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c)
 1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder I Nakaya, Kousik
 SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology
 Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Supplemental materials
 Supplemental materials 1 Supplemental Fig. 1 Immunogram This immunogram summarizes patient clinical data and immune parameters at corresponding time points for Patient IMF-32. The top panel illustrates
Supplemental materials 1 Supplemental Fig. 1 Immunogram This immunogram summarizes patient clinical data and immune parameters at corresponding time points for Patient IMF-32. The top panel illustrates
Tolerance 2. Regulatory T cells; why tolerance fails. Abul K. Abbas UCSF. FOCiS
 1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Factors Which Predispose to the Onset of Autoimmune Disease. A Senior Honors Thesis
 Factors Which Predispose to the Onset of Autoimmune Disease A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for graduation with distinction in Biology in the College of Biological
Factors Which Predispose to the Onset of Autoimmune Disease A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for graduation with distinction in Biology in the College of Biological
Basal cell carcinoma 5/28/2011
 Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
Goal of this Presentation A practical approach to the diagnosis of cutaneous carcinomas and their mimics Thaddeus Mully, MD University of California San Francisco To review common non-melanoma skin cancers
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
Supporting Information
 Supporting Information Chan et al. 1.173/pnas.9654916 A Patient B Xenograft C * remaining feature of normal lymph node * * * D lymphocytes Infiltrating transitional carcinoma cells E Enlarged axillary
Supporting Information Chan et al. 1.173/pnas.9654916 A Patient B Xenograft C * remaining feature of normal lymph node * * * D lymphocytes Infiltrating transitional carcinoma cells E Enlarged axillary
VITAMIN D AND THE SKIN JOYCE FARAH MD MS FAAD FARAH DERMATOLOGY AND COSMETICS, LLC ASSISTANT PROFESSOR OF MEDICINE AND ENT UPSTATE MEDICAL UNIVERSITY
 VITAMIN D AND THE SKIN JOYCE FARAH MD MS FAAD FARAH DERMATOLOGY AND COSMETICS, LLC ASSISTANT PROFESSOR OF MEDICINE AND ENT UPSTATE MEDICAL UNIVERSITY VIT D RECEPTORS ROLE IN MAINTAINING NORMAL FOLLICULAR
VITAMIN D AND THE SKIN JOYCE FARAH MD MS FAAD FARAH DERMATOLOGY AND COSMETICS, LLC ASSISTANT PROFESSOR OF MEDICINE AND ENT UPSTATE MEDICAL UNIVERSITY VIT D RECEPTORS ROLE IN MAINTAINING NORMAL FOLLICULAR
The Immune System. by Dr. Carmen Rexach Physiology Mt San Antonio College
 The Immune System by Dr. Carmen Rexach Physiology Mt San Antonio College What is the immune system? defense system found in vertebrates Two categories Nonspecific specific provides protection from pathogens
The Immune System by Dr. Carmen Rexach Physiology Mt San Antonio College What is the immune system? defense system found in vertebrates Two categories Nonspecific specific provides protection from pathogens
Anti-PD-L1 antibody [28-8] ab205921
![Anti-PD-L1 antibody [28-8] ab205921 Anti-PD-L1 antibody [28-8] ab205921](/thumbs/84/91196262.jpg) Anti-PD-L1 antibody [28-8] ab205921 2 Abreviews 16 References 15 Images Overview Product name Anti-PD-L1 antibody [28-8] Description Tested applications Species reactivity Immunogen Rabbit monoclonal [28-8]
Anti-PD-L1 antibody [28-8] ab205921 2 Abreviews 16 References 15 Images Overview Product name Anti-PD-L1 antibody [28-8] Description Tested applications Species reactivity Immunogen Rabbit monoclonal [28-8]
WHY IS THIS IMPORTANT?
 CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
CHAPTER 16 THE ADAPTIVE IMMUNE RESPONSE WHY IS THIS IMPORTANT? The adaptive immune system protects us from many infections The adaptive immune system has memory so we are not infected by the same pathogen
EliScholar A Digital Platform for Scholarly Publishing at Yale
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1990 The effects of interleukin-1, granulocyte macrophage colony-stimulating
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 1990 The effects of interleukin-1, granulocyte macrophage colony-stimulating
Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast
 Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast carcinoma (a) and colon adenocarcinoma (b) were staining
Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast carcinoma (a) and colon adenocarcinoma (b) were staining
Scabies Associated with Radiation Therapy for Cutaneous T-Cell Lymphoma
 Annals of Clinical & Laboratory Science, vol. 31, no. 1, 2001 103 Scabies Associated with Radiation Therapy for Cutaneous T-Cell Lymphoma Douglas H. McGregor, 1 Qinghua Yang, 1 Fang Fan, 1 Robert L. Talley,
Annals of Clinical & Laboratory Science, vol. 31, no. 1, 2001 103 Scabies Associated with Radiation Therapy for Cutaneous T-Cell Lymphoma Douglas H. McGregor, 1 Qinghua Yang, 1 Fang Fan, 1 Robert L. Talley,
INTRODUCTION. Dae-Heui Lee
 Korean J Physiol Pharmacol Vol 16: 243-247, August, 2012 http://dx.doi.org/10.4196/kjpp.2012.16.4.243 Morphologic Evidence of Anti-Tumor Specificity of T Cells Activated by Denritic Cells Derived from
Korean J Physiol Pharmacol Vol 16: 243-247, August, 2012 http://dx.doi.org/10.4196/kjpp.2012.16.4.243 Morphologic Evidence of Anti-Tumor Specificity of T Cells Activated by Denritic Cells Derived from
LYMPHOCYTES & IMMUNOGLOBULINS. Dr Mere Kende, Lecturer SMHS
 LYMPHOCYTES & IMMUNOGLOBULINS Dr Mere Kende, Lecturer SMHS Immunity Immune- protection against dangers of non-self/invader eg organism 3 components of immune system 1 st line: skin/mucosa/cilia/hair/saliva/fatty
LYMPHOCYTES & IMMUNOGLOBULINS Dr Mere Kende, Lecturer SMHS Immunity Immune- protection against dangers of non-self/invader eg organism 3 components of immune system 1 st line: skin/mucosa/cilia/hair/saliva/fatty
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
