Radiation Treatment Breaks and Ulcerative Mucositis in Head and Neck Cancer Gregory Russo, Robert Haddad, Marshall Posner and Mitchell Machtay
|
|
|
- Polly Heath
- 5 years ago
- Views:
Transcription
1 Radiation Treatment Breaks and Ulcerative Mucositis in Head and Neck Cancer Gregory Russo, Robert Haddad, Marshall Posner and Mitchell Machtay The Oncologist published online August 13, 2008 The online version of this article, along with updated information and services, is located on the World Wide Web at: citation Downloaded from by guest on February 26, 2014
2 The Oncologist Radiation Oncology Radiation Treatment Breaks and Ulcerative Mucositis in Head and Neck Cancer GREGORY RUSSO, a ROBERT HADDAD, b MARSHALL POSNER, b MITCHELL MACHTAY a a Department of Radiation Oncology, Jefferson Medical College, Philadelphia, Pennsylvania, USA; b Department of Medical Oncology, Dana-Farber Cancer Institute/Harvard Medical School, Boston, Massachusetts, USA Key Words. Head and neck cancer Concurrent chemoradiation Radiation mucositis Radiation treatment breaks Radiation toxicity Disclosure: The content of this article has been reviewed by independent peer reviewers to ensure that it is balanced, objective, and free from commercial bias. No financial relationships relevant to the content of this article have been disclosed by the authors, planners, independent peer reviewers, or staff managers of the article. LEARNING OBJECTIVES After completing this course, the reader will be able to: 1. Evaluate the role of mucositis in treatment breaks and the influence of the radiotherapy regimen on mucositis and treatment breaks. 2. Discuss the recent literature (published from 2000 to the present) on the prevalence of treatment breaks during radiotherapy for head and neck cancer, and the effect of treatment breaks on clinical outcomes. 3. Examine strategies to prevent mucositis and reduce treatment breaks, including alternative radiotherapy regimens and pharmacologic agents. CME This article is available for continuing medical education credit at CME.TheOncologist.com. ABSTRACT Unplanned radiation treatment breaks and prolongation of the radiation treatment time are associated with lower survival and locoregional control rates when radiotherapy or concurrent chemoradiotherapy is used in the curative treatment of head and neck cancer. Treatment of head and neck cancer is intense, involving high-dose, continuous radiotherapy, and often adding chemotherapy to radiotherapy. As the intensity of treatment regimens has escalated in recent years, clinical outcomes generally have improved. However, more intensive therapy also increases the incidence of treatment-related toxicities, particularly those impacting the mucosal lining of the oral cavity, pharynx, and cervical esophagus, and results in varying degrees of ulcerative mucositis. Ulcerative mucositis is a root cause of unscheduled radiation treatment breaks, which prolongs the total radiation treatment time. Alterations in radiotherapy and chemotherapy, including the use of continuous (i.e., 7 days/week) radiotherapy to ensure constant negative proliferative pressure, may improve efficacy outcomes. However, these approaches also increase the incidence of ulcerative mucositis, thereby increasing the incidence of unplanned radiation treatment breaks. Con- Correspondence: Mitchell Machtay, M.D., Department of Radiation Oncology, Jefferson Medical College, 111 South 11th Street, Philadelphia, Pennsylvania , USA. Telephone: ; Fax: ; Mitchell.machtay@jeffersonhospital. org Received January 31, 2008; accepted for publication May 14, 2008; first published online in THE ONCOLOGIST Express on August 13, AlphaMed Press /2008/$430.00/0 doi: /theoncologist The Oncologist 2008;13:
3 2 Ulcerative Mucositis in Head and Neck Cancer versely, the reduction of ulcerative mucositis to minimize unplanned breaks in radiotherapy may enhance not only tolerability, but also efficacy outcomes. Several strategies to prevent ulcerative mucositis in radiotherapy for head and neck cancer have been evaluated, but none have demonstrated strong efficacy. Continued investigation is needed to identify superior radiation treatment regimens, technology, and supportive care that reduce unplanned radiation treatment breaks with the goal of improving clinical outcomes in head and neck cancer. The Oncologist 2008;13: INTRODUCTION Squamous cell carcinoma of the head and neck occurs in a substantial number of patients: projections for 2007 in the U.S. alone included approximately 45,660 new cases and 11,210 deaths for cancer of the oral cavity, pharynx, and larynx [1]. Patients who present with local disease are typically treated with a single-modality approach using surgery or radiotherapy. However, approximately 65% of patients with head and neck tumors present with locally advanced disease [2], which typically requires a multidisciplinary approach [2 7]. Concurrent chemoradiotherapy (CRT) can result in a superior treatment response and survival outcome compared with radiotherapy alone in these patients [3], and it has become the standard of care for locally advanced disease and organ preservation. However, 3 years after concurrent CRT, 30% 40% of patients will experience locoregional recurrences, and 20% 30% will develop distant metastases [3 6]. Additionally, the combination of chemotherapy and radiotherapy may improve survival to a lesser extent than it improves local treatment response and control, while adding to acute toxicity [4, 5]. The major limitation to continuous, uninterrupted radiotherapy and concurrent CRT in the management of head and neck cancer is ulcerative mucositis. Unplanned radiation treatment breaks resulting from ulcerative mucositis and the associated acute side effects negatively impact treatment outcomes for many types of tumors, but the detrimental effect appears greatest in head and neck cancer [4]. Ulcerative mucositis is difficult to assess because it occurs not only in the oral cavity but also in areas that cannot be easily observed, such as the esophagus and hypopharynx. The secondary acute effects of oral mucositis include acute and chronic aspiration, inanition, infection, and severe pain. These lead to significant morbidity requiring treatment interruptions. The objective of this article is to review data on the clinical consequences of radiation treatment breaks, the association between ulcerative mucositis and radiation treatment breaks, and possible strategies to prevent radiation treatment breaks by reducing ulcerative mucositis in the management of head and neck cancer. A literature search (published from the year 2000 to the present) was performed in the MEDLINE, Embase, Biosis, Ovid Journals Full Text, and Conference Papers Index databases. The search strategy consisted of text words and synonyms for treatment breaks, survival analysis, treatment outcomes, radiotherapy, chemotherapy, breast cancer, head and neck cancer, lung cancer, colorectal cancer, and hematological neoplasm. Literature references were selected by the authors on the basis of their relevance to current clinical practice for the treatment of head and neck cancer. BIOLOGIC CONSEQUENCES OF RADIATION TREATMENT BREAKS Studies in radiation biology have demonstrated that there is a higher risk for proliferation by residual tumor cells when local radiotherapy is delayed or interrupted. The biological basis for the negative effects of unplanned radiation treatment breaks on clinical outcomes has been attributed to tumor stem cells, cells that can reproduce indefinitely and can therefore cause recurrence [6]. In contrast, most cells in a tumor have a limited life span. Approximately 2 4 weeks after the initiation of radiotherapy, surviving tumor stem cell repopulation in head and neck cancer accelerates and occurs continually during radiation [6, 7]. The accelerated repopulation by tumor stem cells is a consequence of radiotherapy-induced killing of tumor cells; the surviving cells cycle faster during the time the radiation is not being applied. Additionally, surgery interrupting radiotherapy may trigger accelerated tumor regrowth by enhancing the growth environment during healing. The molecular mechanisms underlying accelerated repopulation by tumor cells receiving sublethal doses of radiotherapy likely involve pre-existing signal transduction pathways that have the potential to stimulate cellular proliferation [8]. During accelerated repopulation, the estimated tumor stem cell doubling time may shorten from approximately 60 days to 4 days [6]. Tarnawski et al. [7] retrospectively estimated repopulation rates for 1,502 patients with carcinoma of the larynx or pharynx who were treated with radiotherapy alone. The probability of tumor control significantly correlated with radiation dose, tumor node metastasis stage, overall radiation treatment time, and
4 Russo, Haddad, Posner et al. 3 gap duration. Ninety percent of these patients had unplanned radiation treatment breaks (mean break of 9 days), and accelerated repopulation of tumor cells occurred more rapidly during a break than during normal days of radiotherapy. During the radiation treatment break, the proliferation rate was equal to 0.75 cell doubling per day versus 0.2 cell doubling per day during days with irradiation, which means that the clonogens are capable of proliferating three times faster on days when no radiotherapy is given than on days when radiotherapy is given. This higher rate strongly demonstrates the cellular basis for the impact of planned and unplanned radiation treatment delays on locoregional control, as confirmed in clinical studies. CLINICAL CONSEQUENCES OF RADIATION TREATMENT BREAKS Studies quantifying the adverse clinical consequences of unplanned radiation treatment breaks and the resulting prolongation of the overall radiation treatment time are summarized in Table 1 [9 21]. Unplanned breaks in radiotherapy for head and neck cancer are associated with significantly worse locoregional control [10, 11, 13]. There is evidence that even a short break may have negative consequences; in a retrospective analysis of 2,225 patients from four centers [11], an unplanned break of only 1 day resulted in a 0.68% lower 2-year local control rate. Other authors have estimated that the tumor control rate is at least 1% lower for every day that radiation treatment is interrupted [4, 6]. Unplanned breaks, especially those of several days or more, also have been reported to result in significantly shorter overall survival [9] and relapse-free survival [12] times. After radiotherapy is held for 6 days, every additional day is associated with a 1% 2% lower 5-year relapsefree survival rate [12]. Indirect evidence of the negative consequences of unplanned radiation treatment breaks comes from several studies of total radiation treatment time. Unintended prolongation of the total time of definitive radiotherapy is associated with worse locoregional control [14 16, 18] and survival [12, 17]. In the case of postoperative treatment of head and neck cancer, there can be significant delays in the package time the time from surgery to completion of postoperative radiotherapy. When the package time is prolonged because of operative morbidity, similar negative effects for locoregional control [18 20] and survival [18 20] are observed. There is indirect evidence that adding chemotherapy during planned treatment breaks alternating chemotherapy and radiation therapy can minimize the time factor found to be so critical. In a phase III study from Italy that randomized patients between standard radiation therapy and alternating chemotherapy and radiation therapy (three cycles of cisplatin plus 5-fluorouracil [5-FU] alternating with three 2-week courses of standard fractionated radiation therapy), the patients in the combination therapy arm had superior response, 3-year and 5-year survival, diseasefree survival, and local control rates, and there was no difference in the acute high-grade mucositis rates [22, 23]. The total treatment time for the alternating chemotherapy and radiation therapy arm was 10 weeks. This suggests that the adverse effect of a longer treatment time may be less relevant when additional negative growth pressure (i.e., chemotherapy) is applied to tumor clonogens during breaks, and permit healing of normal tissues. RADIATION TREATMENT BREAKS AND ALTERED FRACTIONATION SCHEDULES Just as unplanned radiation treatment breaks are known to have clinical consequences, planned radiation treatment breaks may explain some of the observed results in controlled clinical trials of altered fractionation schedules (Table 2) [24 31]. Planned radiation treatment breaks have the potential benefit of improving radiation tolerability and quality of life by reducing mucositis and its consequences, but they may come at the expense of poorer tumor control. In an early controlled study of altered fractionation for head and neck cancer [24], hyperfractionation (1.15 Gy twice daily, 5 days/week for 7 weeks) was well tolerated and resulted in significantly better locoregional tumor control, but was not associated with a statistically significant survival benefit compared with standard radiotherapy (2.0 Gy once daily, 5 days/week for 7 weeks). A subsequent larger randomized phase III study [25] in 1,073 patients with head and neck cancer compared standard once-a-day radiotherapy (2.0 Gy once daily, 5 day/ week for 7 weeks), hyperfractionation (1.2 Gy twice daily, 5 days/week for 7 weeks), accelerated hyperfractionation with a break (1.6 Gy twice daily, 5 days/week for 6 weeks including a 2-week rest after 38.4 Gy), and accelerated fractionation with a concomitant boost (1.8 Gy once daily, 5 days/week for 6 weeks, plus an additional 1.5 Gy once daily to a boost field during the last 12 radiation treatment days). Hyperfractionation and accelerated fractionation with a concomitant boost resulted in better locoregional tumor control but did not alter survival significantly. The combination of accelerated hyperfractionation with a break did not affect locoregional tumor control or survival outcomes when compared with the standard treatment arm oncedaily, standard fractionated radiotherapy. This finding may have been a result of the inclusion of the planned 2-week break, which appears to negate the benefits of hyperfrac-
5 4 Ulcerative Mucositis in Head and Neck Cancer Table 1. Radiotherapy: effects of unplanned radiation treatment breaks and prolonged radiation treatment time on efficacy outcome Study Regimen n of patients Efficacy outcome Unplanned radiation treatment breaks Herrmann et al. (1994) [9] RT (63% postoperative, 37% as primary treatment) Robertson et al. (1998) [10] RT was primary treatment for all patients; 3% had prior surgery Robertson et al. (1998) [11] RT (various schedules) 2,225 (retrospective, 4 institutions) 192 LRC closely correlated with survival: 95% of deaths within 5 yrs were from recurrent carcinoma; breaks in RT resulted in lower 5-yr survival rate (p.001); no breaks, 61% survival rate; breaks during first 3 wks, 65% survival rate; breaks during middle 2 wks, 25% survival rate; breaks during last 2 wks, 18% survival rate 352 Breaks of 3 days resulted in poorer local control relative to no breaks (HR, 1.75; 95% CI, ); position of breaks did not matter Break or prolongation by 1 day associated with lower 2-yr local control rate by 0.68% per day Suwinski et al. (2003) [12] Postoperative RT 868 (retrospective) Breaks 6 days did not influence RFS; longer breaks were associated with 1% 2% lower RFS rate per day Groome et al. (2006) [13] Overall radiation treatment time Barton et al. (1992) [14] 90% received RT alone as initial therapy Definitive RT for larynx carcinoma 491 stage T1N0; 213 stage T2N0 (population-based) Fowler et al. (1992) [15] RT 3,834 (literature review, 12 reports) Withers et al. (1995) [16] RT (various dose fractionation patterns) Local failure associated with stage T1N0 disease: 4 RT interruption days RR, 2.43; 95% CI, ; stage T2N0 disease: late RT breaks (i.e., after day 28) RR, 2.19; 95% CI, ,012 (retrospective) OTT significantly affected local control (p.02 when adjusted for influence of stage and laryngeal subsite): hazard of local relapse 4.8% higher per day of interruption (p.006), resulting in lower local control rate by 1.4% per day if uncompensated OTT correlated with local control (p.05 for 10 of 12 reports); median loss of local control was 14% per wk (range, 3% 25%) 676 (retrospective) Tumor control probability 1% lower per day with longer OTT (continued)
6 Russo, Haddad, Posner et al. 5 Table 1. (Continued) Study Regimen n of patients Efficacy outcome Alden et al. (1996) [17] Induction CT (5-FU cisplatin); definitive RT-std 41 Elapsed RT treatment time was highly predictive of survival (p.02); 5-yr rates (median times): RT 55 days, 56% (98 mos); RT days, 46% (57 mos); RT 66 days, 15% (15 mos) Rosenthal et al. (2002) [18] Postoperative RT 208 (retrospective) RT treatment time was associated with locoregional failure (p.03) Suwinski et al. (2003) [12] Postoperative RT 868 (retrospective) Prolongation of RT treatment time by 10 days was related to a 10% 20% lower 5-yr RFS rate Package time (time between surgery and completion of radiotherapy) Parsons et al. (1997) [19] Postoperative RT 134 Unfavorable tumors ( 4 indications for RT and/or invasive at margins): LRC higher for package time 100 days (60% versus 14%; p.04); favorable tumors: no significant effect of package time on LRC Ang et al. (2001) [20] Rosenthal et al. (2002) [18] Postoperative RT delivered in 5 versus 7 wks Surgery plus postoperative RT 151 high-risk patients The 5-yr actuarial LRC rate for package time 11 wks was 76%, compared with 62% for wks and 38% for 13 wks (p.002); the 5-yr survival rate for package time 11 wks was 48%, compared with 27% for wks and 25% for 13 wks (p.003) 208 (retrospective) Package time associated with locoregional failure (p.13); package time predicted survival (p.021) Abbreviations: 5-FU, 5-fluorouracil; CI, confidence interval; HR, hazard ratio; LRC, locoregional control; N, node stage; OTT, overall treatment time; RFS, recurrence-free survival; RR, relative risk; RT, radiotherapy; RT-std, standard radiotherapy; T, tumor stage. tionation and acceleration. Support for this theory comes from a secondary analysis of 501 patients treated with splitcourse (n 191) or continuous (n 310) radiotherapy in two randomized trials of the Danish Head and Neck Cancer Group [32], in which the overall 5-year locoregional control rate was lower for split-course radiotherapy (30% versus 41%; p.007), particularly among well-differentiated tumors (21% versus 38%; p 0.001; Fig. 1). Conversely, reducing or eliminating planned radiation treatment breaks and reducing the overall treatment time has been shown to lead to better tumor control. Overgaard et al. [26] demonstrated that administration of a sixth weekly dose, either alone on day 6 or as a second dose on day 5, and reducing the total radiation treatment time from 6.5 to 5.5 weeks resulted in better locoregional tumor control; however, it did not affect survival and it resulted in a higher incidence of acute morbidity (Fig. 2). Maciejewski et al. [33] eliminated all treatment breaks and administered standard fractionated radiotherapy 7 days a week for five consecutive weeks in a noncontrolled study; however, this regimen resulted in unacceptable acute morbidity and consequential late morbidity. By using the 7 days/week schedule for 5 weeks but decreasing the daily dose from 2.0 Gy to 1.8 Gy in a small controlled trial [27, 28], the investigators were
7 6 Ulcerative Mucositis in Head and Neck Cancer Table 2. Selected randomized trials and meta-analyses of altered fractionation schedules: efficacy and toxicity outcomes Study Regimen n of patients Efficacy outcome Toxicity Horiot et al. (1992) [24] RT-std or RT-hf yr local control rate was better with RT-hf (59% versus 40%; p.02); trend toward longer survival with RT-hf (p.08) Fu et al. (2000) [25] Overgaard et al. (2003) [26] Skladowski et al. (2000, 2006) [27, 28] Dische et al. (1997) [29] Bourhis et al. (2006) [30] Budach et al. (2006) [31] Budach et al. (2006) [31] RT-std, RT-hf, RT-accel (split), or RT-accel (boost) 1,073 RT-hf and RT-accel (boost) associated with better LRC (p.045 and p.050) compared with RT-std; no significant differences in OS among regimens; RT-hf and RT-accel (boost) trend toward higher DFS rate (p.067 and p.054) relative to RT-std RT-6 or RT-std 1,476 5-yr LRC rate, 70% for RT-6 and 60% for RT-std (p.0005); DFS rate, 73% for RT-6 and 66% for RT-std (p.01) CAIR or RT-std yr local control rate, 82% for CAIR versus 37% (p.0001); 5-yr local control rate, 75% for CAIR versus 33% (p.00004); actuarial 3-yr OS rate, 78% for CAIR versus 32% (p.0001); 5-yr OS rate for CAIR also better (p.00005) CHART or RT-std 918 No difference between the arms in LRC, primary tumor control, nodal control, disease-free interval, metastasis-free survival, and overall survival; CHART was more effective in younger patients (p.041); RTstd was more effective for poorly differentiated tumors (p.030) RT-std, RT-accel, or RT-hf RT-std or RTaccel 6,515 (15 trials) LRC benefit (6.4% at 5 yrs; p.0001) favored RT-accel/RT-hf; absolute overall 5-yr survival benefit versus RT-std of 8% for RT-hf, 2% for RT-accel 4,702 (9 trials) No survival benefit for RT-accel in 8/9 studies; overall, no OS benefit for RT-accel RT-std or RT-hf 1,523 (4 trials) RT-hf provided OS benefit of 14.2 mos (95% CI, ; p.0001) Grade 3 diffuse ulcerative mucositis: RT-std, 49%; RT-hf, 66.5%; no difference in late effects Grade 3 mucous membrane toxicity: RTstd, 25%; RT-hf, 42%; RT-accel (boost), 47%; RT-accel (split), 41%; no significant difference in late effects Confluent ulcerative mucositis, 53% versus 33% (p.0001) Confluent ulcerative mucositis occurred more often with CAIR (94% versus 53%; p.00001) and had a longer duration (mean, 4.2 versus 1.5 wks) Osteoradionecrosis in 0.4% of patients after CHART and 1.4% of patients after conventional radiotherapy; late morbidities were less severe with CHART, but acute ulcerative mucositis was more severe and started earlier Abbreviations: CAIR, continuous accelerated irradiation for 7 days/week; CHART, continuous hyperfractionated accelerated radiotherapy; CI, confidence interval; DFS, disease-free survival; LRC, locoregional control; OS, overall survival; RT, radiotherapy; RT-6, standard radiotherapy plus a sixth dose on Friday or Saturday; RT-accel, accelerated fractionation radiotherapy; RT-alt, altered fractionation; RT-hf, hyperfractionated radiotherapy; RT-std, standard radiotherapy.
8 Russo, Haddad, Posner et al. 7 Figure 1. Locoregional control of well/moderately differentiated squamous cell carcinoma of the pharynx and the supraglottis treated with continuous radiotherapy and with splitcourse radiotherapy. Reprinted from Hansen O, Overgaard J, Hansen HS et al. Importance of overall treatment time for the outcome of radiotherapy of advanced head and neck carcinoma: Dependency on tumor differentiation. Radiother Oncol 1997;43:47 51, with permission from Elsevier. Figure 2. Administration of a sixth weekly dose, either alone on day 6 or as a second dose on day 5, plus a reduction in the total radiation treatment time from 6.5 to 5.5 weeks resulted in better locoregional tumor control. There was no difference in survival and there was a higher incidence of acute morbidity. Reprinted from Overgaard J, Hansen HS, Specht L et al. Five compared with six fractions per week of conventional radiotherapy of squamous-cell carcinoma of head and neck: DAH- ANCA 6 and 7 randomised controlled trial. Lancet 2003;362: , with permission from Elsevier. able to reduce morbidity to a manageable level and demonstrated a highly significant greater 5-year locoregional tumor control rate of 75% for continuous accelerated irradiation, versus 33% with standard fractionation. One approach that has been examined in clinical trials is the use of short-course, continuous hyperfractionated accelerated radiotherapy (CHART), whereby 36 fractions of radiotherapy are administered three times daily for 12 consecutive days (compared with 5 7 weeks of therapy for most radiotherapy regimens). In the initial report of a multicenter comparison of CHART and conventional radiotherapy in 918 patients, the locoregional tumor control rate was comparable between the radiation treatments, but late radiation morbidity favored CHART [29]. However, a subsequent analysis of data from the study [34] reported that CHART was associated with a greater incidence (75% versus 44%) and peak prevalence (60% versus 34%) of confluent ulcerative mucositis. Highly significant relationships between ulcerative mucositis grade and dysphagia, odynophagia, and prescribed narcotics were also observed. Two meta-analyses of randomized altered fractionation trials [30, 31] addressed the relative efficacy of accelerated versus hyperfractionated schedules. Both meta-analyses demonstrated significantly longer survival times for hyperfractionated radiotherapy relative to accelerated radiotherapy. However, the authors noted that the modest benefits of most altered radiotherapy schedules may be offset by higher incidences of acute and chronic radiation treatment related morbidity. RADIATION TREATMENT BREAKS AND CONCURRENT CRT The addition of concurrent chemotherapy to radiotherapy has been shown to lead to better organ preservation, locoregional control, and survival in randomized trials and meta-analyses in head and neck cancer [31, 35 43], but not surprisingly, the combination therapy resulted in greater toxicity (Table 3). For example, in the Intergroup phase III trial of unresectable head and neck cancer [35], standard radiation was compared with two different CRT regimens: bolus cisplatin with continuous radiotherapy and a split course with cisplatin plus 5-FU. The bolus cisplatin regimen resulted in significantly better locoregional tumor control and a longer overall survival time compared with radiotherapy alone; split-course treatment (despite having more aggressive chemotherapy) was not statistically different from radiotherapy alone. The survival rate at 3 years was 23%, 27%, and 37%, respectively, for radiotherapy alone, split-course CRT, and continuous CRT with bolus cisplatin, but rates of grade 3 toxicity in the CRT groups were significantly greater (52%, 77%, and 89%, respectively). In contrast to the body of data delineating the negative consequences of radiation treatment breaks and longer total radiation treatment times in radiotherapy alone for head and neck cancer, there is a paucity of data regarding the influence of the radiation treatment time on outcomes when concurrent CRT is used. The influence of the overall radiation time was specifically evaluated in 88 patients undergoing definitive CRT for head and neck cancer [44]. Patients were treated with two cycles of induction chemotherapy (cisplatin and 5-FU) followed by concurrent CRT with cisplatin and 5-FU in conjunction with
9 8 Ulcerative Mucositis in Head and Neck Cancer Table 3. Selected randomized trials and meta-analyses of concurrent chemoradiotherapy versus radiotherapy alone: efficacy and toxicity outcomes Study Regimen n of patients Efficacy outcome Toxicity Adelstein et al. (2003) [35] Bernier et al. (2004) [36] A, RT-std; B, RT-std cisplatin; C, split-course RT cisplatin and 5-FU A, postoperative RT; B, postoperative RT with concurrent cisplatin 295 (unresectable) 3-yr projected OS: A, 23%; B, 37% (p.014 versus A); C, 27% (NS versus A) 334 Estimated 5-yr cumulative incidence of local or regional relapses favored arm B (31% versus 18%; p.007); survival advantage for arm B after median follow-up of 60 mos OS: death HR, 0.70; p.02; PFS: progression HR, 0.75; p.04 Brizel et al. (1998) [37] RT-hf or RT-hf concurrent PF 116 evaluable 3-yr LRC favored PF (70% versus 44%; p.01); 3-yr OS favored PF (55% versus 34%; p.07); PF resulted in greater RFS rate (61% versus 41%; p.08) Calais et al. (1999) [38], Denis et al. (2004) [39] Cooper et al. (2004) [40] Forastiere et al. (2003) [41] Staar et al. (2001) [42] Budach et al. (2006) [31] Pignon et al. (2000) [43] A, RT-std; B, concurrent RT carboplatin and 5-FU A, Postoperative RT; B, RT concurrent cisplatin A, induction cisplatin 5-FU followed by RT; B, concurrent cisplatin RT; C, RT alone RT-hf (accel) with or without CT (5-FU carboplatin) 1A, RT-std with or without concurrent CT; 1B, RT-hf and/or RT-accel with or without concurrent CT; 1C, imbalanced RT regimens with or without concurrent or alternating CT Locoregional therapy with or without CT (adjuvant, neoadjuvant, or concurrent) yr LRC favored arm B (48% versus 25%; p.002); 5-yr OS rate favored arm B (22% versus 16%; p.05); 5-yr DFS rate favored arm B (27% versus 15%; p.01) 459 After median follow-up of 45.9 mos, LRC favored group B (HR for recurrence, 0.61; p.01); OS was not significantly different; DFS time was longer for group B (HR for disease or death, 0.78; p.04) 547 (larynx preservation) Intact larynx at 2 yrs: A, 75%; B, 88% (p.005 versus A; p.001 versus C); C, 70%; local control rate at 2 yrs: A, 64%; B, 80%; C, 58%; OS similar in all 3 groups 240 (unresectable) After median 22.3 mos, 1- and 2-yr rates were 69% and 51% (CRT) and 58% and 45% (RT) (p 0.05); 1-yr survival with local control (primary endpoint): 58% for CRT versus 44% for RT (p.05); p.01 for oropharyngeal and NS for hypopharyngeal; 1-yr OS rate of 66% for CRT versus 60% for RT; 2-yr OS rate of 58% for CRT versus 39% for RT Meta-analysis: 10 trials (n 2,197); 6 trials (n 1,301); 3 trials (n 502) Meta-analysis: 63 trials (n 10,741) OS benefit favored CT (p.0001 for all 3 groups): 12.0-, 12.0-, and 7.9-mo benefits for 1A, 1B, and 1C Absolute OS benefit of 4% at 5 yrs (p.0001) in favor of CT; for concurrent CT, absolute OS benefit was 8% at 5 yrs Toxicity grade 3: A, 52%; B, 89% (p.0001 versus A); C, 77% (p.001 versus A) AEs grade 3 more frequent in arm B (41% versus 21%; p.001); types of severe mucosal AEs and incidence of late AEs similar between arms Confluent ulcerative mucositis rates were comparable (75% for PF versus 77%) Acute grade 3 ulcerative mucositis more frequent in arm B (71% versus 39%; p.005); late grade 3 effects more common in arm B (56% versus 30%; NS) Acute grade 3 AEs higher in arm B (77% versus 34%; p.001); grade 3 mucous membrane AEs higher in arm B (62% versus 37%); no significant difference in late effects Grade 3 mucosal (stomatitis) effects: A, 24%; B, 43%; C, 24% Higher mucosal toxicity after CRT (68% grade 3 4 ulcerative mucositis versus 52%; p.01); 30% of survivors 2 yrs remained dependent on feeding tubes; more patients treated with CRT had swallowing problems and continuous use of feeding tubes (51% versus 25%; p.02) Abbreviations: 5-FU, 5-fluorouracil; AE, adverse event; CRT, chemoradiotherapy; CT, chemotherapy; HR, hazard ratio; NS, not significant; OS, overall survival; PF, cisplatin/5-fluorouracil; PFS, progression-free survival; RFS, recurrence-free survival; RT, radiotherapy; RT-accel, accelerated fractionation radiotherapy; RT-hf, hyperfractionated radiotherapy; RT-std, standard radiotherapy. once-daily radiotherapy to a planned total dose of Gy. After 2 years, the 61 patients with overall radiation times 60 days had significantly better local control (89% versus 59%; p.04) and neck control (95% versus 72%; p.02) than the 27 patients with overall radiation times 60 days. Likewise, Keane et al. [45] reported the results of a randomized trial involving 212 patients treated with either concurrent chemotherapy (mitomycin C and 5-FU) and 50 Gy radiotherapy over 28 days with a 4-week rest at the midpoint or radiotherapy alone. After a median follow-up of 4.4 years, no significant differences in the local and regional relapse-free rates or overall survival rate were observed between the CRT arm and radiotherapy alone. These studies provide indirect evidence that prolonged radiation treatment breaks in concurrent CRT regimens, whether planned or unplanned, may decrease the beneficial effect of the addition of chemotherapy to radiotherapy.
10 Russo, Haddad, Posner et al. 9 Table 4. Ulcerative mucositis and associated sequelae in patients receiving radiotherapy for head and neck cancer Literature review [52] Retrospective analysis [53] Study population Systematic analysis of 33 clinical studies (n 6,181) Retrospective analysis of clinical practice (n 450); 83% RT-std, 16% RT-hf, 33% concurrent CRT Incidence of ulcerative mucositis Incidence of grade 3 ulcerative mucositis Weight loss and nutritional support Hospitalization because of ulcerative mucositis Incidence of radiation treatment breaks resulting from ulcerative mucositis RT-std, 97%; CRT, 100%; RT-alt, 89%; CT only, 22% RT-std, 34%; CRT, 43%; RT-alt, 57%; CT only, 0% Feeding tube insertion, 19% (reported in 5 studies; n 819); weight loss, 34% (reported in 8 studies; n 880); weight loss 10%, 17% (reported in 3 studies; n 485) RT-std, 5%; CRT, 6%; RT-alt, 32% Overall, 11% (directly evaluated in 5 studies with 1,267 patients) 83% ulcerative mucositis overall 29% ulcerative mucositis overall Insertion of feeding tube/total parenteral nutrition more common among patients with ulcerative mucositis (p.009) Hospitalization more common among patients with ulcerative mucositis (p.001); incidence of hospitalization correlated with severity of ulcerative mucositis Among patients with mild ulcerative mucositis, 2.4%; among patients with moderate ulcerative mucositis, 15.8%; among patients with severe ulcerative mucositis, 46.8% Abbreviations: CT, chemotherapy; CRT, chemoradiotherapy; RT, radiotherapy; RT-alt, altered fractionation radiotherapy; RT-hf, hyperfractionated radiotherapy; RT-std, standard radiotherapy. The trend has been toward increasing the intensity of chemotherapy in head and neck cancer. Although site-specific information is lacking, supporting data from studies in other types of malignancies (e.g., breast cancer [46, 47] and diffuse large-cell lymphoma [48]) have shown correlations between dose-dense chemotherapy and survival. Dose-dense chemotherapy delivers the same dose of chemotherapy at more frequent time intervals, thus reducing the overall time of chemotherapy delivery. Biologically, the mechanism may be similar to that of accelerated radiation therapy regimens (i.e., more continuous negative growth pressure on tumor clonogens). Similar correlations might be expected for head and neck cancer. In a report of alternating 1-week cycles of CRT (5-FU and hydroxyurea, with or without cisplatin) with 1-week breaks for tissue recovery in patients with advanced head and neck cancer [49], the authors suggested that the usual association between a longer total radiation treatment time and worse outcomes was not applicable when aggressive cell cycle specific chemotherapy was given concomitantly with radiotherapy. Among patients who received radiotherapy doses 59.4 Gy, local control was achieved in 5 of 17 patients who had failed prior local therapy and 30 of 31 patients with no prior local therapy, despite the longer radiotherapy treatment time, weeks total, approximately twice the normal duration of standard radiotherapy. In a subsequent study that also alternated a week-off/week-on schedule of twice-daily radiotherapy with 5-FU plus hydroxyurea for therapy of stage II III disease [50], the 3-year overall survival and progression-free survival rates were 78% and 67%, respectively. The intensive chemotherapy, despite the planned breaks, seemed to exert continued negative growth pressure on tumor stem cells and maintain the benefit of the addition of chemotherapy to radiotherapy by allowing for recovery of acutely responding tissues during the 1-week interruptions. The drawback to this strategy is that the longer overall radiation treatment time and intensity of the chemotherapy requires that patients be compliant with a very long radiation treatment course, and likely may require multiple hospital admissions. It is not clear that this would be feasible in a less controlled environment. This technique is now being tested in the randomized phase III EPIC multicenter trial in combination with cetuximab [51]. As described previously, outcomes are superior when radiotherapy alone is accelerated on a 7 days/week schedule for a shorter total duration with a lower daily dose [28]. Therefore, the Radiation Therapy Oncology Group (RTOG)-0129 protocol was designed to evaluate the effects of concurrent cisplatin therapy with intensified radiotherapy (70 Gy in 35 fractions given 5 days/week for 7 weeks, versus 72 Gy in 42 fractions given 7 days/week for 6 weeks). That trial has completed accrual, but no efficacy data have yet been reported. If the concurrent CRT regimen using concomitant boost radiotherapy is shown to produce significantly better outcomes, this would provide fur-
11 10 Ulcerative Mucositis in Head and Neck Cancer ther support for the importance of minimizing radiation treatment breaks when concomitant chemotherapy is used. ULCERATIVE MUCOSITIS AND RADIATION TREATMENT BREAKS The major limitation to more aggressive radiotherapy and concurrent CRT regimens is locoregional treatment-related toxicities, particularly ulcerative mucositis and the consequences of ulcerative mucositis: aspiration, inanition, and severe pain (Table 4) [52, 53]. A literature review conducted by Trotti et al. [52] found that the overall incidence of ulcerative mucositis was 80% among 6,181 patients in 33 studies that used a variety of grading scales; the overall incidence of grade 3 4 ulcerative mucositis was 39%, with incidences of 43% among patients treated with concurrent CRT and 57% among patients treated with altered fractionation schedules. Five of these studies (1,267 patients) specifically evaluated unplanned interruptions/modifications of radiotherapy and found that 11% of patients (8% 27% in each study) had radiotherapy regimens modified as a result of ulcerative mucositis. A chart review of 450 patients treated by 154 oncologists [53] confirmed the greater risk for ulcerative mucositis associated with intensified therapy either concurrent CRT or higher cumulative radiotherapy doses. Unplanned radiotherapy interruptions were 3.8-fold more common and unplanned chemotherapy breaks were 3.4-fold more common among patients with ulcerative mucositis, and the frequency of radiation treatment breaks was higher with higher grades of ulcerative mucositis. Notably, the incidence of radiation treatment breaks resulting from ulcerative mucositis was greater in this study than in the clinical studies described in the systematic review. Patients with moderate or severe ulcerative mucositis, who comprised the majority of the study population, had 15.8% and 46.8% incidences of radiation treatment breaks resulting from ulcerative mucositis, respectively. This finding is consistent with the theory that radiation treatment breaks resulting from ulcerative mucositis are more common in clinical practice than they are within the controlled setting of clinical trials where there is more support for patients [4]. Although altered radiotherapy schedules and concomitant CRT may enhance the radiation treatment response, they are associated with greater rates of acute toxicity (see Tables 2 and 3). Paradoxically, if the toxicity of the altered radiation treatment or concurrent CRT becomes too great, it could result in more radiation treatment breaks because of ulcerative mucositis, which in turn would lead to worse outcomes and negate the benefits of the altered fractionation radiation treatment. Clearly there is a need for strategies that will reduce ulcerative mucositis and radiation treatment breaks to allow more effective therapies to be administered with minimal planned or unplanned interruptions. STRATEGIES TO REDUCE ULCERATIVE MUCOSITIS AND RADIATION TREATMENT BREAKS Various strategies have been developed to reduce ulcerative mucositis and the associated radiation treatment breaks. The molecularly targeted therapy cetuximab was recently approved by the U.S. Food and Drug Administration in combination with radiation for the de novo treatment of patients with locally advanced head and neck cancers as well as for patients with recurrent, platinum-refractory disease [54]. In a study of high-dose radiotherapy for head and neck cancer, the addition of cetuximab resulted in a lower rate of locoregional progression or death, a longer progressionfree survival time, and a longer overall survival time without exacerbating common adverse events, including ulcerative mucositis [55]. Cetuximab has not been directly compared with cisplatin or other concurrent CRT regimens in a randomized trial, so it is unknown how local-systemic toxicity, survival, and locoregional tumor control rates compare between this newer approach and the standard of care with conventional chemotherapeutic agents. An additional strategy to maintain tumor control without increasing the incidence of ulcerative mucositis is to calculate compensatory doses of radiotherapy for radiation treatment breaks using a linear quadratic model, with the goal of equalizing the biological effective dose between the initially planned and actually delivered radiation doses [10, 11, 56]. Using this model, it is possible to find a solution to recover from early interruptions, but because of the effects of accelerated repopulation, it is almost impossible to recover the dose loss from late radiation treatment breaks. Similarly, compensation after interruptions in altered fractionation is extremely difficult to achieve. Treatment prolongation has a negative impact on locoregional control and can be difficult to achieve in patients whose compliance might be strained by the symptoms associated with ongoing treatment. As described above, the negative consequences typically associated with radiotherapy breaks were not observed in a series of trials that either administered radiotherapy 7 days/week without breaks [27, 28] or used intensive CRT with weekly breaks [49, 50]. Although this approach may preserve the efficacy of radiotherapy for head and neck cancer, it may also lead to greater morbidity. One of the most commonly used strategies to avoid radiation treatment breaks is the prophylactic use of feeding tubes. Feeding tubes allow for continuous feeding even when patients are unable to swallow. This can help to prevent malnutrition and dehydration and some of
12 Russo, Haddad, Posner et al. 11 their secondary effects. Even with feeding tubes, patients still require narcotic analgesics and topical remedies to treat pain. They can also suffer from local infections that can become systemic as a result of the breakdown of the mucosal barrier and associated immune system. The painful symptoms may respond to oral rinses or systemic opioid therapy; there is limited evidence that some agents (allopurinol mouthwash, GM-CSF, immunoglobulin, or human placental extract) may address the underlying mucositis effectively [57]. The ideal strategy would be to prevent the development of mucositis, thereby maintaining locoregional tumor control without resulting in greater radiotherapy toxicity. Few agents have been proven to be significantly effective in preventing mucositis in head and neck cancer [58]. Small studies suggest that local treatment with oral rinses such as 0.15% benzydamine [59, 60] or vitamin E [61] may prevent mucositis, but large, well-controlled studies of these interventions are sparse. A recent systematic review of the available evidence [58] concluded that a few interventions including hydrolytic enzymes, ice chips, Chinese (herbal) medicine, and amifostine may have some benefit in the prevention of mucositis. Patients receiving amifostine with concurrent CRT in a randomized, phase II trial had a significantly lower incidence of ulcerative mucositis (p.0001) [62], but subsequent results of two phase III trials did not show conclusive evidence of mucosal protection [63, 64]. The authors considered the doses used in the phase III trials to be potentially suboptimal, but the effectiveness of amifostine in the head and neck cancer setting remains questionable. Other radioprotective agents also have shown disappointing results in sufficiently powered randomized trials. For example, in a randomized trial of head and neck cancer patients [65], iseganan failed to produce a lower incidence of ulcerative mucositis or attenuate its clinical sequelae relative to placebo. A meta-analysis of randomized trials of ulcerative mucositis prophylaxis in irradiated head and neck cancer patients [66] showed that, overall, the use of various interventions reduced the odds of developing severe ulcerative mucositis (odds ratio, 0.64; 95% confidence interval, ). However, when the outcome was assessed by patients rather than physicians, no significant difference was seen in outcome between the treatment and control groups. Recently, i.v. administration of the recombinant human keratinocyte growth factor palifermin was shown to reduce the incidence of ulcerative mucositis in patients with hematologic cancers [67]. Its efficacy and safety have not been reported in patients with head and neck cancer; however, phase III trials are currently ongoing in locally advanced head and neck cancer in the U.S. and Europe and may provide evidence regarding the potential effectiveness of this agent in reducing acute CRT-induced mucositis. Additional study is required to identify safe and effective strategies to prevent ulcerative mucositis, thereby preventing unplanned radiation treatment breaks. CONCLUSIONS Treatment intensification improves efficacy outcomes in head and neck cancer but can also lead to a higher incidence of acute adverse events such as ulcerative mucositis, often resulting in unplanned radiation treatment interruptions. For radiotherapy, the biological principle of accelerated repopulation of tumors during breaks has been broadly acknowledged, and the negative clinical consequences have been documented for unplanned radiation treatment breaks. Alteration of radiotherapy schedules to reduce radiation treatment breaks by administering radiotherapy 7 days/ week to eliminate radiation treatment breaks to ensure constant tumor coverage may also improve efficacy outcomes. However, these strategies may simultaneously increase the morbidity of radiotherapy, particularly ulcerative mucositis. The ideal solution would reduce both ulcerative mucositis and unplanned radiation treatment breaks as well as the overall package time, but currently available strategies to achieve this goal have been proven to be inadequate, leaving a very important unmet medical need. Continued investigation of new therapies to attenuate ulcerative mucositis and other associated acute and chronic toxicities should result in the identification of strategies that reduce radiation treatment breaks, thereby improving both the tolerability and efficacy of radiotherapy in head and neck cancer. Awareness of the impact of mucositis and treatment breaks and additional prospective trials, like the RTOG 0435 trial, that evaluate new strategies for reducing mucositis are warranted in order to address these serious impediments to cure. ACKNOWLEDGMENTS The authors take full responsibility for the content of the paper but thank Jonathan Latham, PharmD, and Roberta Connelly, MS, ELS, supported by Amgen, for their assistance in organizing the published literature, writing the first draft of the manuscript, and collating the authors comments. AUTHOR CONTRIBUTIONS Conception/design: Gregory Russo, Robert Haddad, Marshall Posner, Mitchell Machtay Data analysis and interpretation: Gregory Russo, Robert Haddad, Marshall Posner, Mitchell Machtay Manuscript writing: Gregory Russo, Robert Haddad, Marshall Posner, Mitchell Machtay Final approval of manuscript: Gregory Russo, Robert Haddad, Marshall Posner, Mitchell Machtay
13 12 Ulcerative Mucositis in Head and Neck Cancer REFERENCES 1 Jemal A, Siegel R, Ward E et al. Cancer statistics, CA Cancer J Clin 2007;57: National Cancer Institute. Surveillance, Epidemiology, and End Results. Available at Accessed September 20, Posner MR, Haddad RI, Wirth LJ. The evolution of induction chemotherapy and sequential therapy for locally advanced squamous cell cancer of the head and neck. In: American Society of Clinical Oncology (ASCO) Educational Book: 42nd ASCO Annual Meeting, Atlanta, GA, June 2 6, Bese NS, Hendry J, Jeremic B. Effects of prolongation of overall treatment time due to unplanned interruptions during radiotherapy of different tumor sites and practical methods for compensation. Int J Radiat Oncol Biol Phys 2007;68: Chitapanarux I, Lorvidhaya V, Kamnerdsupaphon P et al. Chemoradiation comparing cisplatin versus carboplatin in locally advanced nasopharyngeal cancer: Randomised, non-inferiority, open trial. Eur J Cancer 2007;43: Withers HR, Taylor JM, Maciejewski B. The hazard of accelerated tumor clonogen repopulation during radiotherapy. Acta Oncol 1988;27: Tarnawski R, Fowler J, Skladowski K et al. How fast is repopulation of tumor cells during the treatment gap? Int J Radiat Oncol Biol Phys 2002; 54: Schmidt-Ullrich RK, Contessa JN, Dent P et al. Molecular mechanisms of radiation-induced accelerated repopulation. Radiat Oncol Investig 1999;7: Herrmann T, Jakubek A, Trott KR. The importance of the timing of a gap in radiotherapy of squamous cell carcinomas of the head and neck. Strahlenther Onkol 1994;170: Robertson AG, Robertson C, Perone C et al. Effect of gap length and position on results of treatment of cancer of the larynx in Scotland by radiotherapy: A linear quadratic analysis. Radiother Oncol 1998;48: Robertson C, Robertson AG, Hendry JH et al. Similar decreases in local tumor control are calculated for treatment protraction and for interruptions in the radiotherapy of carcinoma of the larynx in four centers. Int J Radiat Oncol Biol Phys 1998;40: Suwinski R, Sowa A, Rutkowski T et al. Time factor in postoperative radiotherapy: A multivariate locoregional control analysis in 868 patients. Int J Radiat Oncol Biol Phys 2003;56: Groome PA, O Sullivan B, Mackillop WJ et al. Compromised local control due to treatment interruptions and late treatment breaks in early glottic cancer: Population-based outcomes study supporting need for intensified treatment schedules. Int J Radiat Oncol Biol Phys 2006;64: Barton MB, Keane TJ, Gadalla T et al. The effect of treatment time and treatment interruption on tumour control following radical radiotherapy of laryngeal cancer. Radiother Oncol 1992;23: Fowler JF, Lindstrom MJ. Loss of local control with prolongation in radiotherapy. Int J Radiat Oncol Biol Phys 1992;23: Withers HR, Peters LJ, Taylor JM et al. Local control of carcinoma of the tonsil by radiation therapy: An analysis of patterns of fractionation in nine institutions. Int J Radiat Oncol Biol Phys 1995;33: Alden ME, O Reilly RC, Topham A et al. Elapsed radiation therapy treatment time as a predictor of survival in patients with advanced head and neck cancer who receive chemotherapy and radiation therapy. Radiology 1996; 201: Rosenthal DI, Liu L, Lee JH et al. Importance of the treatment package time in surgery and postoperative radiation therapy for squamous carcinoma of the head and neck. Head Neck 2002;24: Parsons JT, Mendenhall WM, Stringer SP et al. An analysis of factors influencing the outcome of postoperative irradiation for squamous cell carcinoma of the oral cavity. Int J Radiat Oncol Biol Phys 1997;39: Ang KK, Trotti A, Brown BW et al. Randomized trial addressing risk features and time factors of surgery plus radiotherapy in advanced head-andneck cancer. Int J Radiat Oncol Biol Phys 2001;51: Fortin A, Bairati I, Albert M et al. Effect of treatment delay on outcome of patients with early-stage head-and-neck carcinoma receiving radical radiotherapy. Int J Radiat Oncol Biol Phys 2002;52: Merlano M, Vitale V, Rosso R et al. Treatment of advanced squamous-cell carcinoma of the head and neck with alternating chemotherapy and radiotherapy. N Engl J Med 1992;327: Merlano M, Benasso M, Corvo R et al. Five-year update of a randomized trial of alternating radiotherapy and chemotherapy compared with radiotherapy alone in treatment of unresectable squamous cell carcinoma of the head and neck. J Natl Cancer Inst 1996;88: Horiot JC, Le Fur R, N Guyen T et al. Hyperfractionation versus conventional fractionation in oropharyngeal carcinoma: Final analysis of a randomized trial of the EORTC cooperative group of radiotherapy. Radiother Oncol 1992;25: Fu KK, Pajak TF, Trotti A et al. A Radiation Therapy Oncology Group (RTOG) phase III randomized study to compare hyperfractionation and two variants of accelerated fractionation to standard fractionation radiotherapy for head and neck squamous cell carcinomas: First report of RTOG Int J Radiat Oncol Biol Phys 2000;48: Overgaard J, Hansen HS, Specht L et al. Five compared with six fractions per week of conventional radiotherapy of squamous-cell carcinoma of head and neck: DAHANCA 6 and 7 randomised controlled trial. Lancet 2003; 362: Skladowski K, Maciejewski B, Golen M et al. Randomized clinical trial on 7-day-continuous accelerated irradiation (CAIR) of head and neck cancer report on 3-year tumour control and normal tissue toxicity. Radiother Oncol 2000;55: Skladowski K, Maciejewski B, Golen M et al. Continuous accelerated 7-days-a-week radiotherapy for head-and-neck cancer: Long-term results of phase III clinical trial. Int J Radiat Oncol Biol Phys 2006;66: Dische S, Saunders M, Barrett A et al. A randomised multicentre trial of CHART versus conventional radiotherapy in head and neck cancer. Radiother Oncol 1997;44: Bourhis J, Overgaard J, Audry H et al. Hyperfractionated or accelerated radiotherapy in head and neck cancer: A meta-analysis. Lancet 2006;368: Budach W, Hehr T, Budach V et al. A meta-analysis of hyperfractionated and accelerated radiotherapy and combined chemotherapy and radiotherapy regimens in unresected locally advanced squamous cell carcinoma of the head and neck. BMC Cancer 2006;6: Hansen O, Overgaard J, Hansen HS et al. Importance of overall treatment time for the outcome of radiotherapy of advanced head and neck carcinoma: Dependency on tumor differentiation. Radiother Oncol 1997;43: Maciejewski B, Skladowski K, Pilecki B et al. Randomized clinical trial on accelerated 7 days per week fractionation in radiotherapy for head and neck cancer. Preliminary report on acute toxicity. Radiother Oncol 1996;40: Bentzen SM, Saunders MI, Dische S et al. Radiotherapy-related early morbidity in head and neck cancer: Quantitative clinical radiobiology as deduced from the CHART trial. Radiother Oncol 2001;60: Adelstein DJ, Li Y, Adams GL et al. An intergroup phase III comparison of standard radiation therapy and two schedules of concurrent chemoradio-
Head and Neck Cancer: Altered Fractionation Schedules
 Head and Neck Cancer: Altered Fractionation Schedules M.I. SAUNDERS Marie Curie Research Wing, Centre for Cancer Treatment, Mount Vernon Hospital, Northwood, Middlesex, United Kingdom Key Words. Head and
Head and Neck Cancer: Altered Fractionation Schedules M.I. SAUNDERS Marie Curie Research Wing, Centre for Cancer Treatment, Mount Vernon Hospital, Northwood, Middlesex, United Kingdom Key Words. Head and
Locally advanced head and neck cancer
 Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
5/20/ ) Haffty GB: Concurrent chemoradiation in the treatment of head and neck cancer. Hematol. Oncol. Clin: North Am.
 Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy
 TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy Anurag K. Singh, MD Professor of Medicine University at Buffalo School of Medicine Professor of Oncology Director of Radiation Research Roswell Park
TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy Anurag K. Singh, MD Professor of Medicine University at Buffalo School of Medicine Professor of Oncology Director of Radiation Research Roswell Park
Laryngeal Preservation Using Radiation Therapy. Chemotherapy and Organ Preservation
 1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER
 THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER Piotr Milecki 1, Grażyna Stryczyńska 1, Aleksandra Kruk-Zagajewska 2 Department of Radiotherapy,
THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER Piotr Milecki 1, Grażyna Stryczyńska 1, Aleksandra Kruk-Zagajewska 2 Department of Radiotherapy,
Oral cavity cancer Post-operative treatment
 Oral cavity cancer Post-operative treatment Dr. Christos CHRISTOPOULOS Radiation Oncologist Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Important issues RT -techniques Patient selection
Oral cavity cancer Post-operative treatment Dr. Christos CHRISTOPOULOS Radiation Oncologist Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Important issues RT -techniques Patient selection
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer
 The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
De-Escalate Trial for the Head and neck NSSG. Dr Eleanor Aynsley Consultant Clinical Oncologist
 De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
Protocol of Radiotherapy for Head and Neck Cancer
 106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
Head and Neck Reirradiation: Perils and Practice
 Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer
 Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit
 Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
Neoplasie del laringe Diagnosi e trattamento
 Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice?
 Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Organ-Preservation Strategies in head and neck cancer. Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari
 Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Yuzuru Niibe 1, Katsuyuki Karasawa 1, Toshio Mitsuhashi 2 and Yoshiaki Tanaka 3 INTRODUCTION. Jpn J Clin Oncol 2003;33(9)
 Jpn J Clin Oncol 2003;33(9)450 455 Hyperfractionated Radiation Therapy for Hypopharyngeal Carcinoma Compared with Conventional Radiation Therapy: Local Control, Laryngeal Preservation and Overall Survival
Jpn J Clin Oncol 2003;33(9)450 455 Hyperfractionated Radiation Therapy for Hypopharyngeal Carcinoma Compared with Conventional Radiation Therapy: Local Control, Laryngeal Preservation and Overall Survival
Adjuvant Therapy in Locally Advanced Head and Neck Cancer. Ezra EW Cohen University of Chicago. Financial Support
 Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Sanguineti s (2)Comment: When it was initially published in 2003 with a median follow-up of 3.8 years (4), the RTOG study led to a change in
 Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review
 The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
Accepted 12 August 2010 Published online 15 December 2010 in Wiley Online Library (wileyonlinelibrary.com). DOI: /hed.21624
 ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
Laryngeal and hypopharyngeal cancers
 Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.128 Research Paper Comparison of
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.128 Research Paper Comparison of
Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers
 Original Research Article Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers Kuppa Prakash 1*, A. Ravi Chandran 2, M.
Original Research Article Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers Kuppa Prakash 1*, A. Ravi Chandran 2, M.
Accepted 28 April 2005 Published online 13 September 2005 in Wiley InterScience ( DOI: /hed.
 DEFINING RISK LEVELS IN LOCALLY ADVANCED HEAD AND NECK CANCERS: A COMPARATIVE ANALYSIS OF CONCURRENT POSTOPERATIVE RADIATION PLUS CHEMOTHERAPY TRIALS OF THE EORTC (#22931) AND RTOG (#9501) Jacques Bernier,
DEFINING RISK LEVELS IN LOCALLY ADVANCED HEAD AND NECK CANCERS: A COMPARATIVE ANALYSIS OF CONCURRENT POSTOPERATIVE RADIATION PLUS CHEMOTHERAPY TRIALS OF THE EORTC (#22931) AND RTOG (#9501) Jacques Bernier,
HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view. Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium
 HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium DISCLOSURE OF INTEREST Nothing to declare HEAD AND NECK CANCER -HPV
HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium DISCLOSURE OF INTEREST Nothing to declare HEAD AND NECK CANCER -HPV
MANAGEMENT OF CA HYPOPHARYNX
 MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
Laryngeal Conservation
 Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist
 Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Locally advanced disease & challenges in management
 Gynecologic Cancer InterGroup Cervix Cancer Research Network Cervix Cancer Education Symposium, February 2018 Locally advanced disease & challenges in management Carien Creutzberg Radiation Oncology, Leiden
Gynecologic Cancer InterGroup Cervix Cancer Research Network Cervix Cancer Education Symposium, February 2018 Locally advanced disease & challenges in management Carien Creutzberg Radiation Oncology, Leiden
Oncologist. The. Outcomes Research. Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis
 The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
RT +/- Surgery. Concurrent ChemoRT +/- Surgery
 Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
San Antonio Breast Cancer Symposium 2010 Highlights Radiotherapy
 San Antonio Breast Cancer Symposium 2010 Highlights Radiotherapy Kathleen C. Horst, M.D. Assistant Professor Department of Radiation Oncology Stanford University The Optimal SEquencing of Adjuvant Chemotherapy
San Antonio Breast Cancer Symposium 2010 Highlights Radiotherapy Kathleen C. Horst, M.D. Assistant Professor Department of Radiation Oncology Stanford University The Optimal SEquencing of Adjuvant Chemotherapy
Accepted 20 April 2009 Published online 25 June 2009 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.21179
 ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
Emerging Role of Immunotherapy in Head and Neck Cancer
 Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Pre- Versus Post-operative Radiotherapy
 Postoperative Radiation and Chemoradiation: Indications and Optimization of Practice Dislosures Clinical trial support from Genentech Inc. Sue S. Yom, MD, PhD Associate Professor UCSF Radiation Oncology
Postoperative Radiation and Chemoradiation: Indications and Optimization of Practice Dislosures Clinical trial support from Genentech Inc. Sue S. Yom, MD, PhD Associate Professor UCSF Radiation Oncology
Head and Neck cancer
 Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
SAMO MASTERCLASS HEAD & NECK CANCER. Nicolas Mach, PD Geneva University Hospital
 SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
ORIGINAL ARTICLE. Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer
 ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
Combining chemotherapy and radiotherapy of the chest
 How to combine chemotherapy, targeted agents and radiotherapy in locally advanced NSCLC? Dirk De Ruysscher, MD, PhD Radiation Oncologist Professor of Radiation Oncology Leuven Cancer Institute Department
How to combine chemotherapy, targeted agents and radiotherapy in locally advanced NSCLC? Dirk De Ruysscher, MD, PhD Radiation Oncologist Professor of Radiation Oncology Leuven Cancer Institute Department
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer
 Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Head and NeckCancer: multi-modal therapeuticintegration
 Head and NeckCancer: multi-modal therapeuticintegration P. Ponticelli, L. Lastrucci, R. De Majo, A. Rampini U.O.C. Radioterapia Ospedale S. Donato ASL 8 -AREZZO Summary Biological considerations Clinical
Head and NeckCancer: multi-modal therapeuticintegration P. Ponticelli, L. Lastrucci, R. De Majo, A. Rampini U.O.C. Radioterapia Ospedale S. Donato ASL 8 -AREZZO Summary Biological considerations Clinical
Compliance to Head and Neck Radiotherapy in Our Patient Population
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. VII (April. 2017), PP 48-52 www.iosrjournals.org Compliance to Head and Neck Radiotherapy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 4 Ver. VII (April. 2017), PP 48-52 www.iosrjournals.org Compliance to Head and Neck Radiotherapy
CALGB Thoracic Radiotherapy for Limited Stage Small Cell Lung Cancer
 CALGB 30610 Thoracic Radiotherapy for Limited Stage Small Cell Lung Cancer Jeffrey A. Bogart Department of Radiation Oncology Upstate Medical University Syracuse, NY Small Cell Lung Cancer Estimated 33,000
CALGB 30610 Thoracic Radiotherapy for Limited Stage Small Cell Lung Cancer Jeffrey A. Bogart Department of Radiation Oncology Upstate Medical University Syracuse, NY Small Cell Lung Cancer Estimated 33,000
RANDOMIZED TRIAL ADDRESSING RISK FEATURES AND TIME FACTORS OF SURGERY PLUS RADIOTHERAPY IN ADVANCED HEAD-AND-NECK CANCER
 PII S0360-3016(01)01690-X Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 3, pp. 571 578, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front
PII S0360-3016(01)01690-X Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 3, pp. 571 578, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front
Self-Assessment Module 2016 Annual Refresher Course
 LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
Title. CitationInternational Journal of Clinical Oncology, 20(6): 1. Issue Date Doc URL. Rights. Type. File Information
 Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
TRANSPARENCY COMMITTEE OPINION. 18 October 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
Role of Prophylactic Cranial Irradiation in Small Cell Lung Cancer
 Role of Prophylactic Cranial Irradiation in Small Cell Lung Cancer Kazi S. Manir MD,DNB,ECMO,PDCR Clinical Tutor Department of Radiotherapy R. G. Kar Medical College and Hospital, Kolkata SCLC 15% of lung
Role of Prophylactic Cranial Irradiation in Small Cell Lung Cancer Kazi S. Manir MD,DNB,ECMO,PDCR Clinical Tutor Department of Radiotherapy R. G. Kar Medical College and Hospital, Kolkata SCLC 15% of lung
Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers
 Original Article Free full text available from www.cancerjournal.net Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers Geeta SN, TK Padmanabhan, J Samuel, K Pavithran*,
Original Article Free full text available from www.cancerjournal.net Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers Geeta SN, TK Padmanabhan, J Samuel, K Pavithran*,
Nasopharyngeal Cancer:Role of Chemotherapy
 Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Hypofractionated radiation therapy for glioblastoma
 Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
Hypofractionated radiation therapy for glioblastoma Luis Souhami, MD, FASTRO Professor McGill University Department of Oncology, Division of Radiation Oncology Montreal Canada McGill University Health
TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER
 ORIGINAL ARTICLE TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER Dirk Rades, MD, 1 Fabian Fehlauer, MD, 2 Mashid Sheikh-Sarraf,
ORIGINAL ARTICLE TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER Dirk Rades, MD, 1 Fabian Fehlauer, MD, 2 Mashid Sheikh-Sarraf,
Response Evaluation Of Accelerated Fractionation With Concomitant Boost Chemoradiation In Locally Advanced Squamous Cell Head And Neck Cancer
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. IV (Feb. 2016), PP 27-32 www.iosrjournals.org Response Evaluation Of Accelerated Fractionation
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 2 Ver. IV (Feb. 2016), PP 27-32 www.iosrjournals.org Response Evaluation Of Accelerated Fractionation
Oral Cavity Cancer Combined modality therapy
 Oral Cavity Cancer Combined modality therapy Dr. Christos CHRISTOPOULOS Radiation Oncologist Head and Neck Cancers Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Disclosure slide I have no
Oral Cavity Cancer Combined modality therapy Dr. Christos CHRISTOPOULOS Radiation Oncologist Head and Neck Cancers Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Disclosure slide I have no
RADIATION THERAPY WITH ONCE-WEEKLY GEMCITABINE IN PANCREATIC CANCER: CURRENT STATUS OF CLINICAL TRIALS
 doi:10.1016/s0360-3016(03)00449-8 Int. J. Radiation Oncology Biol. Phys., Vol. 56, No. 4, Supplement, pp. 10 15, 2003 Copyright 2003 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/03/$
doi:10.1016/s0360-3016(03)00449-8 Int. J. Radiation Oncology Biol. Phys., Vol. 56, No. 4, Supplement, pp. 10 15, 2003 Copyright 2003 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/03/$
Nasopharyngeal Cancer/Multimodality Treatment
 Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER
 ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER What is conventional fractionation? Radiation is given at doses of 1.8 to 2.0 Gy delivered once daily, 5 days weekly for 6 to 7 weeks.
ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER What is conventional fractionation? Radiation is given at doses of 1.8 to 2.0 Gy delivered once daily, 5 days weekly for 6 to 7 weeks.
Larynx Hypopharynx. Therapy algorithms. Why larynx preservation at all? State of the art Jean Louis Lefebvre,Lille Jan Klozar,Prague
 Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
September 10, Dear Dr. Clark,
 September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
September 10, 2015 Peter E. Clark, MD Chair, NCCN Bladder Cancer Guidelines (Version 2.2015) Associate Professor of Urologic Surgery Vanderbilt Ingram Cancer Center Nashville, TN 37232 Dear Dr. Clark,
Adjuvant chemo- and radiotherapy for poor prognosis head and neck squamous cell carcinomas
 Critical Reviews in Oncology/Hematology 56 (2005) 353 364 Adjuvant chemo- and radiotherapy for poor prognosis head and neck squamous cell carcinomas Jacques Bernier a,, David G. Pfister b, Jay S. Cooper
Critical Reviews in Oncology/Hematology 56 (2005) 353 364 Adjuvant chemo- and radiotherapy for poor prognosis head and neck squamous cell carcinomas Jacques Bernier a,, David G. Pfister b, Jay S. Cooper
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer. Dr P Vijay Anand Reddy Director Apollo Cancer Hospital
 Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary
 Original article Annals of Oncology 14: 1306 1311, 2003 DOI: 10.1093/annonc/mdg330 Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary A. Argiris
Original article Annals of Oncology 14: 1306 1311, 2003 DOI: 10.1093/annonc/mdg330 Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary A. Argiris
Carcinoma del retto: Highlights
 Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck. Mei Tang, MD
 Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Diagnosis and what happens after referral
 Diagnosis and what happens after referral Dr Kate Newbold Consultant in Clinical Oncology The Royal Marsden Women's cancers Breast cancer introduction 1 Treatment Modalities Early stage disease -larynx
Diagnosis and what happens after referral Dr Kate Newbold Consultant in Clinical Oncology The Royal Marsden Women's cancers Breast cancer introduction 1 Treatment Modalities Early stage disease -larynx
State of the art for radiotherapy of SCCHN
 State of the art for radiotherapy of SCCHN Less side effects Cured More organ & function preservation Head & neck cancer = 42 000 new cases / year in Europe Not cured Local failure Distant failure More
State of the art for radiotherapy of SCCHN Less side effects Cured More organ & function preservation Head & neck cancer = 42 000 new cases / year in Europe Not cured Local failure Distant failure More
Combined Modality Treatment of Anal Carcinoma
 Combined Modality Treatment of Anal Carcinoma F. ROELOFSEN, a H. BARTELINK b a Bethesda Krankenhaus, Essen, Germany; b The Netherlands Cancer Institute/Antoni van Leeuwenhoek Ziekenhuis, Amsterdam, The
Combined Modality Treatment of Anal Carcinoma F. ROELOFSEN, a H. BARTELINK b a Bethesda Krankenhaus, Essen, Germany; b The Netherlands Cancer Institute/Antoni van Leeuwenhoek Ziekenhuis, Amsterdam, The
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: James RD, Glynne-Jones R, Meadows HM, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: James RD, Glynne-Jones R, Meadows HM, et al.
Head and Neck Cancer:
 Head and Neck Cancer: Robert Haddad M.D. Clinical Director Head and Neck Oncology Program Dana Farber Cancer Institute Boston, MA Predictive Biomarkers: HPV Abstract 6003: Survival Outcomes By HPV Status
Head and Neck Cancer: Robert Haddad M.D. Clinical Director Head and Neck Oncology Program Dana Farber Cancer Institute Boston, MA Predictive Biomarkers: HPV Abstract 6003: Survival Outcomes By HPV Status
CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER
 CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER Jean-Pascal Machiels Department of medical oncology Institut I Roi Albert II Cliniques universitaires Saint-Luc Université catholique de Louvain, Brussels,
CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER Jean-Pascal Machiels Department of medical oncology Institut I Roi Albert II Cliniques universitaires Saint-Luc Université catholique de Louvain, Brussels,
New Paradigms for Treatment of. Erminia Massarelli, MD, PHD, MS Clinical Associate Professor
 New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
The New England Journal of Medicine HYPERFRACTIONATED IRRADIATION WITH OR WITHOUT CONCURRENT CHEMOTHERAPY FOR LOCALLY ADVANCED HEAD AND NECK CANCER
 HYPERFRACTIONATED IRRADIATION WITH OR WITHOUT CONCURRENT CHEMOTHERAPY FOR LOCALLY ADVANCED HEAD AND NECK CANCER DAVID M. BRIZEL, M.D., MARY E. ALBERS, M.D., SAMUEL R. FISHER, M.D., RICHARD L. SCHER, M.D.,
HYPERFRACTIONATED IRRADIATION WITH OR WITHOUT CONCURRENT CHEMOTHERAPY FOR LOCALLY ADVANCED HEAD AND NECK CANCER DAVID M. BRIZEL, M.D., MARY E. ALBERS, M.D., SAMUEL R. FISHER, M.D., RICHARD L. SCHER, M.D.,
Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer. American Society of Clinical Oncology Clinical Practice Guideline
 Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer American Society of Clinical Oncology Clinical Practice Guideline Introduction ASCO convened an Expert Panel to develop recommendations
Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer American Society of Clinical Oncology Clinical Practice Guideline Introduction ASCO convened an Expert Panel to develop recommendations
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer
 Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER
 ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER Vasu Divi, MD, 1 * Francis P. Worden, MD, 1,2 * Mark E. Prince, MD, 1 Avraham Eisbruch, MD, 3 Julia S. Lee, MD, 4
ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER Vasu Divi, MD, 1 * Francis P. Worden, MD, 1,2 * Mark E. Prince, MD, 1 Avraham Eisbruch, MD, 3 Julia S. Lee, MD, 4
Tumor progression in waiting time for radiotherapy in head and neck cancer
 Radiotherapy and Oncology 84 (27) 5 1 www.thegreenjournal.com Waiting time Tumor progression in waiting time for radiotherapy in head and neck cancer Anni Ravnsbæk Jensen a,b, *, Hanne Marie Nellemann
Radiotherapy and Oncology 84 (27) 5 1 www.thegreenjournal.com Waiting time Tumor progression in waiting time for radiotherapy in head and neck cancer Anni Ravnsbæk Jensen a,b, *, Hanne Marie Nellemann
Radiotherapy for rectal cancer. Karin Haustermans Department of Radiation Oncology
 Radiotherapy for rectal cancer Karin Haustermans Department of Radiation Oncology O U T L I N E RT with TME surgery? Neoadjuvant or adjuvant RT? 5 x 5 Gy or long-course CRT? RT with new drugs? Selection
Radiotherapy for rectal cancer Karin Haustermans Department of Radiation Oncology O U T L I N E RT with TME surgery? Neoadjuvant or adjuvant RT? 5 x 5 Gy or long-course CRT? RT with new drugs? Selection
The efficacy of postoperative radiation therapy in patients with carcinoma of the buccal mucosa and lower alveolus with positive surgical margins
 Original Article The efficacy of postoperative radiation therapy in patients with carcinoma of the buccal mucosa and lower alveolus with positive surgical margins Badakh Dinesh K, Grover Amit H Dr. D.
Original Article The efficacy of postoperative radiation therapy in patients with carcinoma of the buccal mucosa and lower alveolus with positive surgical margins Badakh Dinesh K, Grover Amit H Dr. D.
3/8/2014. Case Presentation. Primary Treatment of Anal Cancer. Anatomy. Overview. March 6, 2014
 Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部
 肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
肺癌放射治療新進展 Recent Advance in Radiation Oncology in Lung Cancer 許峰銘成佳憲國立台灣大學醫學院附設醫院腫瘤醫學部 Outline Current status of radiation oncology in lung cancer Focused on stage III non-small cell lung cancer Radiation
HEAD AND NECK CANCER TREATMENT REGIMENS (Part 1 of 5)
 HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER. Virginie Westeel Chest Disease Department University Hospital Besançon, France
 PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain
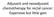 Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Squamous Cell Carcinoma of the Oral Cavity: Radio therapeutic Considerations
 Squamous Cell Carcinoma of the Oral Cavity: Radio therapeutic Considerations Troy G. Scroggins Jr. MD Chairman, Department of Radiation Oncology Ochsner Health Systems 1 Association of Postoperative Radiotherapy
Squamous Cell Carcinoma of the Oral Cavity: Radio therapeutic Considerations Troy G. Scroggins Jr. MD Chairman, Department of Radiation Oncology Ochsner Health Systems 1 Association of Postoperative Radiotherapy
JMSCR Vol 07 Issue 01 Page January 2019
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.58 Pure Accelerated Radiotherapy
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i1.58 Pure Accelerated Radiotherapy
ORIGINAL ARTICLE. Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx
 ORIGINAL ARTICLE Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx Sandro J. Stoeckli, MD; Andreas B. Pawlik, MD; Margareta Lipp, MD; Alexander Huber, MD;
ORIGINAL ARTICLE Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx Sandro J. Stoeckli, MD; Andreas B. Pawlik, MD; Margareta Lipp, MD; Alexander Huber, MD;
Nonsurgical Treatment of Laryngeal Cancer
 correspondence Nonsurgical Treatment of Laryngeal Cancer to the editor: Forastiere and colleagues (Nov. 27 issue) 1 are to be congratulated on their important study of concurrent chemotherapy and radiotherapy
correspondence Nonsurgical Treatment of Laryngeal Cancer to the editor: Forastiere and colleagues (Nov. 27 issue) 1 are to be congratulated on their important study of concurrent chemotherapy and radiotherapy
Scottish Medicines Consortium
 Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Nearly 60% of all cancers currently are diagnosed in patients age
 648 Feasibility and Early Results of Accelerated Radiotherapy for Head and Neck Carcinoma in the Elderly Abdelkarim S. Allal, M.D. 1 Daphné Maire, M.D. 1 Minerva Becker, M.D. 2 Pavel Dulguerov, M.D. 3
648 Feasibility and Early Results of Accelerated Radiotherapy for Head and Neck Carcinoma in the Elderly Abdelkarim S. Allal, M.D. 1 Daphné Maire, M.D. 1 Minerva Becker, M.D. 2 Pavel Dulguerov, M.D. 3
Comparison of Futility Monitoring Methods Using RTOG Clinical Trials. Q. Ed Zhang, PhD
 Comparison of Futility Monitoring Methods Using RTOG Clinical Trials Q. Ed Zhang, PhD 1 Futility Monitoring Definition: Monitoring for early determination that trial results will not be in favor of H 1
Comparison of Futility Monitoring Methods Using RTOG Clinical Trials Q. Ed Zhang, PhD 1 Futility Monitoring Definition: Monitoring for early determination that trial results will not be in favor of H 1
Introduction: Methods: Results: Conclusions: PATIENTS AND METHODS Key Words: 1770
 Original Article Utilization of Hyperfractionated Radiation in Small-Cell Lung Cancer and Its Impact on Survival David Schreiber, MD,* Andrew T. Wong, MD,* David Schwartz, MD,* and Justin Rineer, MD Introduction:
Original Article Utilization of Hyperfractionated Radiation in Small-Cell Lung Cancer and Its Impact on Survival David Schreiber, MD,* Andrew T. Wong, MD,* David Schwartz, MD,* and Justin Rineer, MD Introduction:
Chapter 5 Stage III and IVa disease
 Page 55 Chapter 5 Stage III and IVa disease Overview Concurrent chemoradiotherapy (CCRT) is recommended for stage III and IVa disease. Recommended regimen for the chemotherapy portion generally include
Page 55 Chapter 5 Stage III and IVa disease Overview Concurrent chemoradiotherapy (CCRT) is recommended for stage III and IVa disease. Recommended regimen for the chemotherapy portion generally include
ESRA KAYTAN SAĞLAM, MD Istanbul University Oncology Institute
 USE OF RADIOSENSITIZERS IN ONCOLOGY ESRA KAYTAN SAĞLAM, MD Istanbul University Oncology Institute According to cell type: Radiosensitive tumors (embryojenic tumors, lymphomas) Moderate sensitives (Squamous
USE OF RADIOSENSITIZERS IN ONCOLOGY ESRA KAYTAN SAĞLAM, MD Istanbul University Oncology Institute According to cell type: Radiosensitive tumors (embryojenic tumors, lymphomas) Moderate sensitives (Squamous
