Weekly versus every-three-weeks platinumbased chemoradiation regimens for head and neck cancer
|
|
|
- Kory Phelps
- 5 years ago
- Views:
Transcription
1 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 DOI /s x ORIGINAL RESEARCH ARTICLE Weekly versus every-three-weeks platinumbased chemoradiation regimens for head and neck cancer Open Access James M. Melotek 1, Benjamin T. Cooper 2, Matthew Koshy 1,3, Joshua S. Silverman 2 and Michael T. Spiotto 1,3* Abstract Background: The majority of chemoradiation (CRT) trials for locally advanced head and neck squamous cell carcinoma (HNSCC) have relied on platinum-based chemotherapy regimens administered every-3-weeks. However, given the increased utilization of weekly platinum regimens, it remains unclear how different chemotherapy schedules compare regarding efficacy and toxicity. Methods: We retrospectively identified 212 patients with HNSCC who were treated at a single academic medical center with concurrent platinum-based CRT given weekly (N = 68) or every-three-weeks (N = 144). JMP version 10 (SAS Institute) was used for statistical analysis. Discrete variables were compared with the chi-square test and differences in the medians were assessed using the Wilcoxon test. Survival curves were constructed using the Kaplan-Meier method and significance was assessed using the log rank test. For univariate analysis and multivariate analysis, we used Cox proportional hazard or logistic regression models to compare differences in survival or differences in categorical variables, respectively. Results: Patients receiving weekly platinum regimens were more likely to be older (median age 61.4 vs y; P <.001), have high or very high Charlson comorbidity index (45.6% vs. 27.8%; P =.01), and receive carboplatin-based chemotherapy (6.3% vs. 76.5%; P <.001). Weekly and every-3-week platinum regimens had similar locoregional control (HR 1.10; 95% CI ; P =.72), progression-free survival (HR 1.13; 95% CI ; P =.55), and overall survival (HR 1.11; 95% CI ; P =.71). Every-3-weeks platinum regimens were associated with increased days of hospitalization (median: 3 days vs. 0 days; P =.03) and acute kidney injury (AKI) during radiotherapy (5% vs. 22.1%; P <.001). On multivariate analysis, AKI was significantly associated with every-3-weeks regimens (OR: 24.38; 95% CI ; P =.003) and high comorbidity scores (OR: 2.74; 95% CI ; P =.01). Conclusions: Our results suggest that every-3-weeks and weekly platinum-containing CRT regimens have similar disease control but weekly platinum regimens are associated with less acute toxicity. Keywords: Head and neck neoplasm, Concurrent chemoradiotherapy, Acute kidney injury, Cisplatin, Carboplatin Background In patients with locally advanced head and neck squamous cell carcinoma (HNSCC), chemoradiation (CRT) improves locoregional control (LRC) and overall survival (OS) compared to radiotherapy (RT) alone [1]. Typically, CRT schedules use platinum-based regimens given every * Correspondence: mspiotto@radonc.uchicago.edu 1 Department of Radiation and Cellular Oncology, University of Chicago, KCBD 6142, 900 E. 57th St, Chicago, IL 60637, USA 3 Department of Radiation Oncology, University of Illinois at Chicago, Chicago, IL, USA Full list of author information is available at the end of the article three weeks [2 6]. The Head and Neck Intergroup trial and RTOG observed that concurrent CRT with every-3-weeks cisplatin improved LRC and OS for unresectable HNSCC and resectable laryngeal cancers, respectively [2, 4]. Other trials have demonstrated improved outcomes using every-3-weeks platinum-based chemotherapy alone or combined with 5-fluorouracil and/or other drugs during RT [3, 5, 6]. Due to the prevalence of randomized studies, cisplatin at a dose of 100 mg/m 2 given every three weeks remains the recommended systemic therapy option during CRT [7]. However, the The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 2 of 9 addition of this chemotherapy regimen to RT is often associated with significantly increased toxicities including stomatitis, nausea/vomiting, and myelosuppression. For example, rates of grade 3 stomatitis and myelosuppression were 73% and 81% with CRT compared to 42% and 5% with RT alone in RTOG [4]. Thus, there remains a critical need to maintain the efficacy of CRT while minimizing its toxicity. Several groups have investigated the use of a weekly platinum-based chemotherapy schedule during RT to reduce toxicity [8 11]. Data regarding this approach are limited and conflicting. Chan et al. demonstrated an overall survival benefit with the addition of weekly cisplatin to RT in nasopharyngeal carcinoma [12]. However, LRC was not improved, contrary to expectations with the use of radiosensitizing doses of chemotherapy. Additional support for weekly platinum CRT regimens has been extrapolated from two cervical carcinoma trials demonstrating improved OS and progression-free survival (PFS) with weekly cisplatin [13, 14]. However, another trial by the National Cancer Institute of Canada observed no difference in outcomes between RT and CRT with weekly platinum [15]. In the setting of unresectable head and neck cancer, a joint trial performed by the RTOG and ECOG showed no benefit in LRC or OS with the addition of weekly low dose cisplatin at 20 mg/m 2 to RT [16]. Furthermore, retrospective or prospective data comparing the efficacy and toxicity of weekly versus every-3-weeks platinum-based CRT are lacking. We therefore sought to compare the outcomes of patients with HNSCC treated with platinum-based CRT at a single institution using either a weekly or every-3-weeks chemotherapy schedule. Methods Study population Patients were treated at the University of Illinois Medical Center at Chicago between 1992 and This study was approved by the University of Illinois Medical Center IRB protocol in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1999, as revised in The University of Illinois at Chicago IRB waived informed consent given that this study used preexisting medical records and obtaining informed consent on all patients would be impractical given the associated time and cost. Patient data was anonymized and de-identified prior to analysis. We identified 212 consecutive patients with HNSCC from a retrospective database who were treated with concurrent platinum-based CRT given weekly or every-three-weeks. 144 patients received every-3-weeks chemotherapy and 68 patients received weekly chemotherapy. Patients were excluded who did not have documented chemotherapy schedules or received a combination of weekly and every-3-weeks chemotherapy. Of patients receiving every-3-weeks chemotherapy, 3 patients initially received cisplatin for the first 1-2 cycles and were subsequently switched to carboplatin. The anonymized and de-identified dataset is available for review as Additional file 1. Variables Data was collected from all available physical and electronic medical records. All patients were included in this analysis regardless of treatment compliance. During RT, acute toxicities were recorded during weekly ontreatment visits. We approximated comorbidity burden using a modified Charlson Comorbidity Index [17] and performance status using the Karnofsky Performance Status (KPS) [18]. Staging was categorized using the American Joint Committee on Cancer staging system used at the time of diagnosis. We defined RT delay as RT courses that were completed 3 days or longer than the anticipated finish date and RT truncations as RT courses that did not achieve the prescribed radiation dose. Chemotherapy modifications included treatments that did not achieve 3 cycles of every-3-weeks platinum chemotherapy or 6 cycles of weekly platinum chemotherapy, chemotherapy dose reductions, or changes in chemotherapy drugs. We defined the length and number of hospitalizations based on the discharge summary. Creatinine (Cr) values were obtained from patient records and were measured at the start of therapy, during RT at one to two week intervals, and at regular follow-up visits. We defined acute kidney injury (AKI) as a peak Cr concentration during radiotherapy greater than or equal to 0.3 mg/dl over pretreatment Cr levels as it meets one of the three Acute Kidney Injury Network (AKIN) criteria for AKI [19] and Cr increments as small as mg/dl have been associated with increased mortality [20]. Time to LRC, PFS, and OS were determined from last date of RT. Patterns of failure were determined as the first failure with any component of local, regional or distant recurrence, respectively. PFS was calculated as the time to any failure or death. OS was calculated as the time to death. Statistical analysis We used JMP version 10 (SAS Institute) to perform statistical analysis using two-sided tests and defining significance as P <.05. Discrete variables were compared with the chi-square test and differences in the medians were assessed using the Wilcoxon test. Survival curves were plotted using the Kaplan-Meier method and significance was assessed using the log rank test. For univariate analysis (UVA) and multivariate analysis (MVA), we used Cox proportional hazard or logistic regression models to compare differences in survival or differences in categorical variables, respectively. Censoring is assumed to be
3 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 3 of 9 non-informative. Variables with P value <.1 on UVA were included on MVA. Results Population, tumor, and treatment characteristics As shown in Table 1, median follow-up was not significantly different between groups (21.1 months for every-3- weeks vs months for weekly chemotherapy; P =.40). Patients receiving every-3-weeks chemotherapy were younger (55.5y vs. 61.4y; P <.001) and had lower comorbidity scores (27.8% vs. 45.6% with high comorbidity index; P =.01). There was no difference in gender, performance status, smoking or alcohol use, primary site, tumor stage, or nodal stage. In an analysis limited to patients who received either every-3-weeks cisplatin or weekly carboplatin also shown in Table 1, patients receiving every-3-weeks cisplatin were younger (55.4y vs. 61.9y; P <.001), more likely to be male (81.2% vs. 67.3%; P =.04), and had lower comorbidity scores (26.1% vs. 48.1% with high comorbidity index; P <.01). As shown in Table 2, patients receiving weekly chemotherapy were more often treated in the post-operative setting (44.1% vs 3%; P =.05) and received carboplatin chemotherapy (76.5% vs 6.3%; P <.001). There was no difference in receipt of induction chemotherapy, post-radiation lymph node dissection, alterations in RT course, RT technique (3D-conformal vs. intensity-modulated RT), or chemotherapy dose modification. In an analysis limited to patients who received either every-3-weeks cisplatin or weekly carboplatin also shown in Table 2, there were no significant differences in treatment characteristics other than the chemotherapy agent delivered. Patients in the every-3-weeks cisplatin group received a median cumulative dose of 200 mg/m 2 (interquartile range 200 mg/m mg/m 2 ). Outcomes and toxicity With median follow-up of 23.7 months for the entire cohort, 85 patients experienced disease progression (28 patients in the weekly chemotherapy group and 57 patients in the every-3-weeks chemotherapy group). The majority of failures were due to locoregional progression (20 patients in the weekly chemotherapy group and 38 patients in the every-3-weeks chemotherapy group). At the time of analysis, 63 patients had died (20 patients in the weekly chemotherapy group and 43 patients in the every-3-weeks chemotherapy group). As shown in Fig. 1, weekly chemotherapy in comparison to every-3-weeks chemotherapy was not associated with worse LRC (2y LRC ± SE 65.7 ± 6.4% vs ± 4.4%; HR 1.10; 95% CI ; P =.72), PFS (2y PFS ± SE 50.7 ± 6.4% vs ± 4.6%; HR 1.13; 95% CI ; P =.55), or OS (2y OS ± SE 69.9 ± 6.4% vs ± 4.0%; HR 1.11; 95% CI ; P =.71). As shown in Fig. 2, weekly carboplatin in comparison to bolus cisplatin was not associated with worse LRC (2y LRC ± SE 72.7 ± 6.9% vs ± 4.5%; HR 0.90; 95% CI ; P =.76), PFS (2y PFS ± SE 55.8 ± 7.4% vs ± 4.8%; HR 0.96; 95% CI ; P=.88), or OS (2y OS ± SE 71.2 ± 7.2% vs ± 4.3%; HR 0.96; 95% CI ; P=.89). When only patients treated with definitive RT were analyzed, weekly chemotherapy in comparison to every- 3-weeks chemotherapy was not associated with worse LRC (2y LRC ± SE 55.2 ± 9.6% vs ± 5.7%; HR 1.29; 95% CI ; P =.43), PFS (2y PFS ± SE 39.8 ± 8.7% vs ± 5.5%; HR 1.42; 95% CI ; P =.16), or OS (2y OS ± SE 66.8 ± 8.9% vs ± 5.1%; HR 1.58; 95% CI ; P =.18). When only patients treated with adjuvant RT were analyzed, weekly administration of chemotherapy was also not associated with worse LRC (2y LRC ± SE 77.2 ± 8.3% vs ± 5.2%; HR 1.32; 95% CI ; P =.63), PFS (2y PFS ± SE 63.1 ± 9.4% vs ± 7.5%; HR 0; 95% CI ; P = 0), or OS (2y OS ± SE 74.0 ± 9.2% vs ± 6.9%; HR 2; 95% CI ; P =.67). On UVA (Table 3), every-three-weeks chemotherapy was associated with increased median total hospital days (3 vs. 0; P =.03) and AKI during RT (5% vs. 22.1%; P <.001). By contrast, receipt of every-three-weeks chemotherapy was not associated with acute toxicities such as weight loss, feeding tube during or after RT, tracheotomy dependence after RT, mucositis or dermatitis. On UVA limited to patients who received either every-3- weeks cisplatin or weekly carboplatin also shown in Table 3, every-3-weeks cisplatin was similarly associated with AKI during RT (49.3% vs. 28.9%; P <.01). On MVA (Table 4), AKI during RT was significantly associated with receipt of every-3-weeks chemotherapy (OR: 24.38; 95% CI ; P =.003) and high comorbidity index (OR: 2.74; 95% CI ; P =.01) but not with receipt of cisplatin chemotherapy, post-operative RT, or age. Only high comorbidity index was significantly associated with hospitalizations on MVA (OR: 2.08; 95% CI ; P =.03). Discussion In our cohort of patients with HNSCC treated with different CRT schedules, weekly compared to every-3- weeks platinum-based regimens resulted in similar outcomes and less renal toxicity. The benefit of weekly platinum chemotherapy lies in the ability to titrate the dose to avoid severe acute toxicity. In our series, weekly platinum regimens were more often used in older patients or those with more comorbidity, indicating a potential selection bias. Based on prior data demonstrating improved disease outcomes in younger patients and those with less comorbidity [21, 22], we would expect the selection bias present in our series to result in worse
4 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 4 of 9 Table 1 Patient characteristics Every-3-weeks platinum Weekly platinum P-value Every-3-weeks cisplatinum Weekly carboplatinum P-value (N = 144) (N = 68) (N = 138) (N = 52) Median age (years) < <.001 (IQR) ( ) ( ) ( ) ( ) Median follow-up (months) (IQR) ( ) ( ) ( ) ( ) Gender Male 116 (8%) 49 (72.1%) 112 (81.2%) 35 (67.3%) Female 28 (19.4%) 19 (27.9%) 26 (18.8%) 17 (32.7%) KPS (83.3%) 51 (75.0%) 116 (84.1%) 41 (78.9%) < 70 9 (6.3%) 5 (2.4%) 9 (6.5%) 4 (7.7%) Not stated 15 (1%) 12 (17.7%) 13 (9.4%) 7 (13.5%) Comorbidity index.01 <.01 Medium 104 (72.2%) 37 (54.4%) 102 (73.9%) 27 (51.9%) High 40 (27.8%) 31 (45.6%) 36 (26.1%) 25 (48.1%) Stage I 0 (%) 1 (1.5%) 0 (%) 1 (1.9%) II 10 (6.9%) 3 (4.4%) 9 (6.6%) 2 (3.9%) III 33 (22.9%) 19 (27.9%) 31 (22.6%) 10 (19.2%) IV 101 (70.1%) 45 (66.2%) 97 (7%) 39 (75.0%) Alcohol history drinks/day 76 (52.8%) 33 (48.5%) 73 (52.9%) 25 (48.1%) < 2 drinks/day 36 (25.0%) 21 (30.9%) 35 (25.4%) 17 (32.7%) Not stated 32 (22.2%) 14 (2%) 30 (21.7%) 10 (19.2%) Tobacco history > 10 pack-years 106 (73.6%) 48 (7%) 101 (73.2%) 38 (73.1%) 10 pack-years 33 (22.9%) 19 (27.9%) 32 (23.2%) 13 (25.0%) Not stated 5 (3.5%) 1 (1.5%) 5 (3.6%) 1 (1.9%) Primary site Hypopharynx 5 (3.5%) 4 (5.9%) 5 (3.6%) 3 (5.8%) Larynx 31 (21.5%) 12 (17.7%) 29 (2%) 9 (17.3%) Nasopharynx 14 (9.7%) 5 (7.4%) 14 (10.1%) 3 (5.8%) Oral Cavity 38 (26.4%) 16 (23.5%) 36 (26.1%) 11 (21.2%) Oropharynx 39 (27.1%) 20 (29.4%) 38 (27.5%) 17 (32.7%) Other 17 (11.8%) 11 (16.2%) 16 (11.6%) 9 (17.3%) Tumor Stage T (3%) 26 (38.2%) 41 (29.7%) 22 (42.3%) T3-4b 100 (69.4%) 42 (61.8%) 97 (70.3%) 30 (57.7%) Nodal Stage N0-2a 69 (47.9%) 40 (58.8%) 67 (48.6%) 27 (51.9%) N2b-3 75 (52.1%) 28 (41.2%) 71 (51.5%) 25 (48.1%) P16 status Positive 4 (2.8%) 0 (%) 4 (2.9%) 0 (%) Negative 50 (34.7%) 32 (47.1%) 49 (35.5%) 27 (51.9%) Not stated 90 (62.3%) 36 (52.9%) 85 (61.6%) 25 (48.1%) Cr creatinine, IQR interquartile range, KPS Karnofsky performance status
5 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 5 of 9 Table 2 Treatment characteristics Every-3-weeks platinum Weekly platinum P-value Every-3-weeks cisplatinum Weekly carboplatinum P-value (N = 144) (N = 68) (N = 138) (N = 52) RT timing Post-operative 44 (3%) 30 (44.1%) 44 (31.9%) 22 (42.3%) Definitive 100 (69.4%) 38 (55.9%) 94 (68.1%) 30 (57.7%) Induction chemotherapy Yes 41 (28.5%) 17 (25.0%) 37 (26.8%) 16 (3%) No 103 (71.5%) 51 (75.0%) 101 (73.2%) 36 (69.2%) Post-radiation lymph node dissection Yes 19 (13.2%) 5 (7.4%) 18 (13.0%) 4 (7.7%) No 81 (56.3%) 33 (48.5%) 76 (55.1%) 26 (5%) Not stated 44 (3%) 30 (44.1%) 44 (31.9%) 22 (42.3%) RT technique D-conformal 25 (17.4%) 14 (2%) 23 (16.7%) 10 (19.2%) IMRT 119 (82.6%) 54 (79.4%) 115 (83.3%) 42 (8%) Type of chemotherapy <.001 <.001 Cisplatin 138 (95.8%) a 16 (23.5%) 138 (10%) 0 (%) Carboplatin 9 (6.3%) 52 (76.5%) 0 (%) 52 (10%) Alterations in RT course None 82 (56.9%) 40 (58.8%) 78 (56.5%) 31 (59.6%) Delay 43 (29.9%) 21 (30.9%) 41 (29.7%) 15 (28.9%) Truncations 19 (13.2%) 7 (10.3%) 19 (13.8%) 6 (11.5%) Chemotherapy dose modification Yes 76 (52.8%) 32 (47.1%) 73 (52.9%) 25 (48.1%) No 68 (47.2%) 36 (52.9%) 65 (47.1%) 27 (51.9%) RT radiotherapy, IMRT intensity modulated radiotherapy a Three patients were treated with CDDP and switched to carboplatin. All were treated according to an every-3-weeks regimen outcomes for patients treated with weekly chemotherapy. However, weekly chemotherapy was similarly efficacious for patients with these worse prognostic features. Additionally, patients treated with weekly chemotherapy had significantly fewer AKI events compared to those receiving an every-3-weeks regimen. Thus, even with more adverse features, patients treated with weekly platinumbased CRT had similar disease control and survival rates with less toxicity. In our study, similar rates of treatment compliance likely facilitated similar LRC and OS rates for weekly and every-3-weeks chemotherapy that were comparable to previously reported outcomes [2, 3]. Previously, it has been suggested that a weekly chemotherapy may be Locoregional Control Bolus P =.72 Weekly a Progression-Free Survival b Bolus P =.55 Weekly Overall Survival Bolus P =.71 Weekly Fig. 1 Kaplan-Meier curves for (a) locoregional control, (b) progression-free survival, and (c) overall survival in patients receiving weekly versus every-3-weeks chemoradiation regimens. The log rank test was used to assess for differences in outcomes c
6 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 6 of 9 Locoregional Control Bolus cisplatin Weekly carboplatin P =.76 a Progression-Free Survival b Bolus cisplatin Weekly carboplatin P =.88 Overall Survival Bolus cisplatin Weekly carboplatin P =.89 Fig. 2 Kaplan-Meier curves for (a) locoregional control, (b) progression-free survival, and (c) overall survival in patients receiving weekly carboplatin versus every-3-weeks cisplatin chemoradiation regimens. The log rank test was used to assess for differences in outcomes c Table 3 Toxicity Every-3-weeks platinum Weekly platinum P-value Every-3-weeks cisplatinum Weekly carboplatinum P-value (N = 144) (N = 68) (N = 138) (N = 52) Median total hospital days (IQR) (0 9) (0 4) (0 9) (0 4) Hospitalizations Yes 62 (43.1%) 28 (41.2%) 60 (43.5%) 21 (4%) No 49 (34.0%) 33 (48.5%) 46 (33.3%) 26 (5%) Not stated 33 (22.9%) 7 (10.3%) 32 (23.2%) 5 (9.6%) Feeding tube during RT Yes 72 (5%) 26 (38.2%) 67 (48.6%) 18 (34.6%) No 72 (5%) 42 (61.8%) 71 (51.5%) 34 (65.4%) Weight loss >10% Yes 72 (5%) 30 (44.1%) 71 (51.4%) 23 (44.2%) No 36 (25.0%) 24 (35.3%) 33 (23.9%) 21 (4%) Not stated 36 (25.0%) 14 (2%) 34 (24.6%) 8 (15.4%) Grade 3 mucositis Yes 35 (24.3%) 19 (27.9%) 33 (23.9%) 17 (32.7%) No 85 (59.0%) 36 (52.9%) 83 (60.1%) 28 (53.8%) Not stated 24 (16.7%) 13 (19.1%) 22 (15.9%) 7 (13.5%) Grade 3 dermatitis Yes 6 (4.2%) 4 (5.9%) 6 (4.3%) 3 (5.8%) No 115 (79.9%) 51 (75.0%) 111 (8%) 42 (8%) Not stated 23 (16.0%) 13 (19.1%) 21 (15.2%) 7 (13.5%) Feeding tube at last follow-up Yes 43 (29.9%) 17 (25.0%) 41 (29.7%) 10 (19.2%) No 101 (70.1%) 51 (75.0%) 97 (70.3%) 42 (8%) Tracheotomy at last follow-up Yes 20 (13.9%) 8 (11.8%) 20 (14.5%) 4 (7.7%) No 124 (86.1%) 60 (88.2%) 118 (85.5%) 48 (92.3%) AKI during RT <.001 <.01 Yes 72 (5%) 15 (22.1%) 68 (49.3%) 15 (28.9%) No 40 (27.8%) 40 (58.8%) 39 (28.3%) 29 (55.8%) Not stated 32 (22.2%) 13 (19.1%) 31 (%) 8 (15.4%) AKI acute kidney injury, IQR interquartile range, RT radiotherapy
7 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 7 of 9 Table 4 Multivariate analysis for factors impacting toxicity Odds ratio (95% CI) AKI during RT Hospitalizations High comorbidity index 2.74 ( ) 2.08 (5 4.21) P value Every-3-weeks chemotherapy ( ) 1.16 (1 3.26) P value Post-operative RT 0 (9 1.24) 6 ( ) P value Cisplatin 6.38 ( ) 1.94 (7 5.78) P value Age (9 1.22) 1.64 (5 3.23) P value AKI acute kidney injury, CI confidence interval, RT radiotherapy inferior to every-3-week chemotherapy as it is less likely to achieve cumulative doses 200 mg/m 2 for cisplatin or 5 weekly cycles [23, 24]. Tsan et al. demonstrated that only 62.5% of patients treated with weekly cisplatin achieved cumulative doses of 200 mg/m 2 compared to 88.5% of patients receiving every-3-weeks chemotherapy [24]. Similarly, previous retrospective studies reported that % of patients receiving weekly cisplatin achieved 5 or more weekly chemotherapy cycles resulting in cumulative doses 200 mg/m 2 [23, 25, 26]. By contrast, trials using every-3 weeks cisplatin achieved cumulative doses of 200 mg/m 2 in 79 84% of patients [2, 4]. Treatment compliance in our study is more compatible with prior trials using every-3-weeks chemotherapy, as 78.1% of patients treated in our study received at least 5 weekly chemotherapy cycles. In our study, patients in the every-3-weeks cisplatin group received a median cumulative dose of 200 mg/m 2. However, we cannot adequately report the cumulative dose for patients treated with weekly chemotherapy as the majority of these patients were treated with carboplatin typically at an AUC of 1.5. Nevertheless, the number of patients receiving weekly chemotherapy cycles was greater in our study than previously reported and may partially account for similar efficacy between different chemotherapy schedules. Furthermore, we observed that fewer patients experienced AKI when treated with weekly platinum regimens compared to every-3-weeks. While we did not observe significant differences in other acute or late toxicities, nephrotoxicity remains a dose-limiting complication of platinum-based chemotherapies. Our rate of AKI approached 50% with every-3-weeks chemotherapy and appears substantially higher than previously reported rates of severe acute nephrotoxicity. However, this discrepancy lies in the use of different definitions for clinically meaningful renal toxicity. Previous trials using every-3-weeks cisplatin which report grade 3 nephrotoxicity rates of % [2, 4, 27] use clinical criteria for renal failure to define such acute severe nephrotoxicity, including the need for dialysis and/or Cr elevations greater than mg/dl among others. However, these criteria for renal failure likely underestimate small but clinically relevant renal insults. In our study, a Cr rise of 0.3 mg/dl was used per the Acute Kidney Injury Network definition of AKI [19] and has been associated with a 4.1-fold increased risk of mortality [20]. Furthermore, relative changes in Cr, rather than absolute rises, likely capture changes in renal function that better reflect individual differences in body mass. Thus, compared to every-3-weeks platinum, we observed that weekly platinum regimens were associated with fewer renal injuries that may not constitute renal failure but potentially impact patient survival. Our study is limited by its retrospective nature and heterogeneous population. In this study, patients receiving weekly chemotherapy were more likely to be treated in the post-operative setting and receive carboplatin, whereas patients receiving every-3-weeks chemotherapy were more likely to be treated in the definitive setting and receive cisplatin. Previous reports including a Hellenic Cooperative Group Trial by Fountzilas et al. and a more recent study by Rades et al. have suggested that carboplatin-based CRT may be inferior to cisplatinbased CRT [28, 29]. However, Fountzilas et al. was not directly powered to compare cisplatin to carboplatin and Rades et al. used a non-standard every-four-weeks chemotherapy administration schedule. Since we did not observe differences in outcomes between cisplatin and carboplatin, our results suggest that weekly carboplatinbased CRT has similar efficacy as CRT with every-3- weeks cisplatin. Though our sample size may be insufficient to detect small differences in outcomes, treatment decisions balancing potentially small differences in disease control with larger differences in toxicity may still find CRT with weekly carboplatin favorable. The median follow-up of our study sample may also limit conclusions on control and survival that can be drawn between the groups. Nevertheless, our results were sufficient to observe less renal toxicity and less hospitalizations in patients treated with weekly platinum-based regimens. Ultimately, the use of weekly platinum-based concomitant chemotherapy with RT for the treatment of locally advanced HNSCC awaits prospective validation. Additionally, the comparative efficacy and toxicity of platinum chemotherapy versus epidermal growth factor receptor (EGFR) inhibitors, namely cetuximab, as radiosensitizers remains an area of great interest currently being studied in the RTOG 1016 and TROG trials. Lastly, the low level of HPV-positivity in this study, which is consistent
8 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 8 of 9 with prior results from our institution [30], limits the generalizability of our results to populations with higher proportions of HPV-positivity. Conclusions In conclusion, our cohort of HNSCC patients treated with definitive CRT had similar disease control with either every-3-weeks or weekly administration of platinum chemotherapy. By contrast, acute renal toxicity was significantly less in patients receiving weekly chemotherapy. As weekly administration of chemotherapy in this setting awaits prospective validation, we must critically assess the balance between treatment efficacy and toxicity in the management of patients with locally advanced HNSCC. Additional file Additional file 1: Table S1. De-identified patient and treatment characteristics. (XLSX 63 kb) Abbreviations AKI: acute kidney injury; Cr: creatinine; CRT: chemoradiation; HNSCC: head and neck squamous cell carcinoma; KPS: Karnofsky performance status; LRC: locoregional control; MVA: multivariate analysis; OS: overall survival; PFS: progression-free survival; RT: radiotherapy; UVA: univariate analysis Acknowledgements None. Funding M.T.S. was supported by a grant from the Burroughs Wellcome Fund (Grant # ). The funding body played no role in the study design, data collection, data analysis, data interpretation, or writing of the manuscript. Availability of data and materials The anonymized and de-identified dataset is provided for review as Additional file 1. Authors contributions Conceived and designed the experiments: JMM MTS. Performed the experiments: JMM MTS. Analyzed the data: JMM MTS. Wrote the paper: JMM BTC MK JSS MTS. All authors read and approved the final manuscript. Competing interests The authors declare that they have no competing interests. Consent for publication This manuscript does not contain any individual person s data in any form. Patient data was anonymized and de-identified prior to analysis. Ethics approval and consent to participate This study was approved by the University of Illinois Medical Center IRB protocol in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1999, as revised in The University of Illinois at Chicago IRB waived informed consent given that this study used preexisting medical records and obtaining informed consent on all patients would be impractical given the associated time and cost. Author details 1 Department of Radiation and Cellular Oncology, University of Chicago, KCBD 6142, 900 E. 57th St, Chicago, IL 60637, USA. 2 Department of Radiation Oncology, New York University, New York, NY, USA. 3 Department of Radiation Oncology, University of Illinois at Chicago, Chicago, IL, USA. Received: 12 June 2016 Accepted: 17 November 2016 References 1. Pignon JP, le Maitre A, Maillard E, Bourhis J, Group M-NC. Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): an update on 93 randomised trials and 17,346 patients. Radiother Oncol. 2009;92(1): Adelstein DJ, Li Y, Adams GL, et al. An intergroup phase III comparison of standard radiation therapy and two schedules of concurrent chemoradiotherapy in patients with unresectable squamous cell head and neck cancer. J Clin Oncol. 2003;21(1): Calais G, Alfonsi M, Bardet E, et al. Randomized trial of radiation therapy versus concomitant chemotherapy and radiation therapy for advancedstage oropharynx carcinoma. J Natl Cancer Inst. 1999;91(24): Forastiere AA, Zhang Q, Weber RS, et al. Long-term results of RTOG 91-11: a comparison of three nonsurgical treatment strategies to preserve the larynx in patients with locally advanced larynx cancer. J Clin Oncol. 2013;31(7): Lee AW, Lau WH, Tung SY, et al. Preliminary results of a randomized study on therapeutic gain by concurrent chemotherapy for regionally-advanced nasopharyngeal carcinoma: NPC-9901 Trial by the Hong Kong Nasopharyngeal Cancer Study Group. J Clin Oncol. 2005;23(28): Wee J, Tan EH, Tai BC, et al. Randomized trial of radiotherapy versus concurrent chemoradiotherapy followed by adjuvant chemotherapy in patients with American Joint Committee on Cancer/International Union against cancer stage III and IV nasopharyngeal cancer of the endemic variety. J Clin Oncol. 2005;23(27): Pfister DG, Spencer S, Brizel DM, et al. Head and neck cancers, Version Clinical practice guidelines in oncology. J Natl Compr Cancer Netw. 2014;12(10): Chera BS, Amdur RJ, Tepper J, et al. Phase 2 Trial of De-intensified Chemoradiation Therapy for Favorable-Risk Human Papillomavirus- Associated Oropharyngeal Squamous Cell Carcinoma. Int J Radiat Oncol Biol Phys. 2015;93(5): Newlin HE, Amdur RJ, Riggs CE, Morris CG, Kirwan JM, Mendenhall WM. Concomitant weekly cisplatin and altered fractionation radiotherapy in locally advanced head and neck cancer. Cancer. 2010;116(19): Rades D, Seidl D, Janssen S, et al. Comparison of weekly administration of cisplatin versus three courses of cisplatin 100 mg/m(2) for definitive radiochemotherapy of locally advanced head-and-neck cancers. BMC Cancer. 2016;16: Urban D, Corry J, Solomon B, et al. Weekly cisplatin and radiotherapy for low risk, locoregionally advanced human papillomavirus-positive oropharyngeal squamous cell carcinoma. Head Neck. 2016;38 Suppl 1:E Chan AT, Leung SF, Ngan RK, et al. Overall survival after concurrent cisplatin-radiotherapy compared with radiotherapy alone in locoregionally advanced nasopharyngeal carcinoma. J Natl Cancer Inst. 2005;97(7): Keys HM, Bundy BN, Stehman FB, et al. Cisplatin, radiation, and adjuvant hysterectomy compared with radiation and adjuvant hysterectomy for bulky stage IB cervical carcinoma. N Engl J Med. 1999;340(15): Rose PG, Bundy BN, Watkins EB, et al. Concurrent cisplatin-based radiotherapy and chemotherapy for locally advanced cervical cancer. N Engl J Med. 1999;340(15): Pearcey R, Brundage M, Drouin P, et al. Phase III trial comparing radical radiotherapy with and without cisplatin chemotherapy in patients with advanced squamous cell cancer of the cervix. J Clin Oncol. 2002;20(4): Haselow RE. Radiation alone vs. radiation with weekly low dose cisplatinum in unresectable cancer of the head and neck. Toronto: B. C. Decker; Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5): Karnofsky DA, Burchenal J. The Clinical Evaluation of Chemotherapeutic Agents in Cancer. New York: Columbia Univ Press; Mehta RL, Kellum JA, Shah SV, et al. Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care. 2007; 11(2):R Chertow GM, Burdick E, Honour M, Bonventre JV, Bates DW. Acute kidney injury, mortality, length of stay, and costs in hospitalized patients. J Am Soc Nephrol. 2005;16(11): Boje CR, Dalton SO, Primdahl H, et al. Evaluation of comorbidity in 9388 head and neck cancer patients: a national cohort study from the DAHANCA database. Radiother Oncol. 2014;110(1):91 7.
9 Melotek et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:62 Page 9 of Pignon JP, Bourhis J, Domenge C, Designe L. Chemotherapy added to locoregional treatment for head and neck squamous-cell carcinoma: three meta-analyses of updated individual data. MACH-NC Collaborative Group. Meta-Analysis of Chemotherapy on Head and Neck Cancer. Lancet. 2000; 355(9208): Osman N, Elamin YY, Rafee S, et al. Weekly cisplatin concurrently with radiotherapy in head and neck squamous cell cancer: a retrospective analysis of a tertiary institute experience. Eur Arch Otorhinolaryngol. 2014; 271(8): Tsan DL, Lin CY, Kang CJ, et al. The comparison between weekly and threeweekly cisplatin delivered concurrently with radiotherapy for patients with postoperative high-risk squamous cell carcinoma of the oral cavity. Radiat Oncol (London, England). 2012;7: Ho KF, Swindell R, Brammer CV. Dose intensity comparison between weekly and 3-weekly Cisplatin delivered concurrently with radical radiotherapy for head and neck cancer: a retrospective comparison from New Cross Hospital, Wolverhampton, UK. Acta Oncol (Stockholm, Sweden). 2008;47(8): Homma A, Inamura N, Oridate N, et al. Concomitant weekly cisplatin and radiotherapy for head and neck cancer. Jpn J Clin Oncol. 2011;41(8): Nguyen-Tan PF, Zhang Q, Ang KK, et al. Randomized Phase III Trial to Test Accelerated Versus Standard Fractionation in Combination With Concurrent Cisplatin for Head and Neck Carcinomas in the Radiation Therapy Oncology Group 0129 Trial: Long-Term Report of Efficacy and Toxicity. J Clin Oncol. 2014;32(34): Fountzilas G, Ciuleanu E, Dafni U, et al. Concomitant radiochemotherapy vs radiotherapy alone in patients with head and neck cancer: a Hellenic Cooperative Oncology Group Phase III Study. Med Oncol (Northwood, London, England). 2004;21(2): Rades D, Ulbricht T, Hakim SG, Schild SE. Cisplatin superior to carboplatin in adjuvant radiochemotherapy for locally advanced cancers of the oropharynx and oral cavity. Strahlenther Onkol. 2012;188(1): Liu G-FF, Ranck MC, Solanki AA, et al. Racial parities in outcomes after radiotherapy for head and neck cancer. Cancer. 2014;120(2): Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Self-Assessment Module 2016 Annual Refresher Course
 LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view. Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium
 HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium DISCLOSURE OF INTEREST Nothing to declare HEAD AND NECK CANCER -HPV
HPV INDUCED OROPHARYNGEAL CARCINOMA radiation-oncologist point of view Prof. dr. Sandra Nuyts Dep. Radiation-Oncology UH Leuven Belgium DISCLOSURE OF INTEREST Nothing to declare HEAD AND NECK CANCER -HPV
Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice?
 Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Locally advanced head and neck cancer
 Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Nasopharyngeal Cancer:Role of Chemotherapy
 Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
De-Escalate Trial for the Head and neck NSSG. Dr Eleanor Aynsley Consultant Clinical Oncologist
 De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
Outcomes for patients with head and neck squamous cell carcinoma presenting with N3 nodal disease
 Witek et al. Cancers of the Head & Neck (2017) 2:8 DOI 10.1186/s41199-017-0027-z Cancers of the Head & Neck RESEARCH Open Access Outcomes for patients with head and neck squamous cell carcinoma presenting
Witek et al. Cancers of the Head & Neck (2017) 2:8 DOI 10.1186/s41199-017-0027-z Cancers of the Head & Neck RESEARCH Open Access Outcomes for patients with head and neck squamous cell carcinoma presenting
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review
 The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy
 TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy Anurag K. Singh, MD Professor of Medicine University at Buffalo School of Medicine Professor of Oncology Director of Radiation Research Roswell Park
TREATMENT TIME & TOBACCO: TWIN TERRORS Of H&N Therapy Anurag K. Singh, MD Professor of Medicine University at Buffalo School of Medicine Professor of Oncology Director of Radiation Research Roswell Park
Head and Neck Reirradiation: Perils and Practice
 Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
Title. CitationInternational Journal of Clinical Oncology, 20(6): 1. Issue Date Doc URL. Rights. Type. File Information
 Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Neoplasie del laringe Diagnosi e trattamento
 Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Laryngeal Preservation Using Radiation Therapy. Chemotherapy and Organ Preservation
 1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER
 ORIGINAL ARTICLE TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER Dirk Rades, MD, 1 Fabian Fehlauer, MD, 2 Mashid Sheikh-Sarraf,
ORIGINAL ARTICLE TOXICITY OF TWO CISPLATIN-BASED RADIOCHEMOTHERAPY REGIMENS FOR THE TREATMENT OF PATIENTS WITH STAGE III/IV HEAD AND NECK CANCER Dirk Rades, MD, 1 Fabian Fehlauer, MD, 2 Mashid Sheikh-Sarraf,
Adjuvant Therapy in Locally Advanced Head and Neck Cancer. Ezra EW Cohen University of Chicago. Financial Support
 Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck. Mei Tang, MD
 Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
A new score predicting the survival of patients with spinal cord compression from myeloma
 Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Douglas et al. BMC Cancer 2012, 12:425 RESEARCH ARTICLE Open Access A new score predicting the survival of patients with spinal cord compression from myeloma Sarah Douglas 1, Steven E Schild 2 and Dirk
Nasopharyngeal Cancer/Multimodality Treatment
 Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER
 CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER Jean-Pascal Machiels Department of medical oncology Institut I Roi Albert II Cliniques universitaires Saint-Luc Université catholique de Louvain, Brussels,
CURRENT STANDARD OF CARE IN NASOPHARYNGEAL CANCER Jean-Pascal Machiels Department of medical oncology Institut I Roi Albert II Cliniques universitaires Saint-Luc Université catholique de Louvain, Brussels,
Predictors and Outcomes for Chronic Tracheostomy After Chemoradiation for Advanced Laryngohypopharyngeal Cancer
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Predictors and Outcomes for Chronic Tracheostomy After Chemoradiation for Advanced Laryngohypopharyngeal
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Predictors and Outcomes for Chronic Tracheostomy After Chemoradiation for Advanced Laryngohypopharyngeal
ORIGINAL ARTICLE. Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer
 ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
Saptarshi Ghosh*, Pamidimukkala Brahmananda Rao, P Ravindra Kumar, Surendra Manam
 RESEARCH ARTICLE Concurrent Chemoradiation with Weekly Cisplatin for the Treatment of Head and Neck Cancers: an Institutional Study on Acute Toxicity and Response to Treatment Saptarshi Ghosh*, Pamidimukkala
RESEARCH ARTICLE Concurrent Chemoradiation with Weekly Cisplatin for the Treatment of Head and Neck Cancers: an Institutional Study on Acute Toxicity and Response to Treatment Saptarshi Ghosh*, Pamidimukkala
ORIGINAL ARTICLE. Harold Lau, MD; Tien Phan, MD; Jack MacKinnon, MD; T. Wayne Matthews, MD
 ORIGINAL ARTICLE Absence of Planned Neck Dissection for the N2-N3 Neck After Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck Harold Lau, MD; Tien Phan, MD; Jack MacKinnon,
ORIGINAL ARTICLE Absence of Planned Neck Dissection for the N2-N3 Neck After Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck Harold Lau, MD; Tien Phan, MD; Jack MacKinnon,
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer
 Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
Effectiveness of Chemoradiotherapy for T1b-T2 Glottic Carcinoma
 Research Article imedpub Journals http://www.imedpub.com Head and Neck Cancer Research ISSN 2572-2107 DOI: 10.21767/2572-2107.100011 Abstract Effectiveness of Chemoradiotherapy for T1b-T2 Glottic Carcinoma
Research Article imedpub Journals http://www.imedpub.com Head and Neck Cancer Research ISSN 2572-2107 DOI: 10.21767/2572-2107.100011 Abstract Effectiveness of Chemoradiotherapy for T1b-T2 Glottic Carcinoma
Ghadjar et al. Radiation Oncology (2015) 10:21 DOI /s y
 Ghadjar et al. Radiation Oncology (2015) 10:21 DOI 10.1186/s13014-014-0319-y RESEARCH Open Access Impact of weight loss on survival after chemoradiation for locally advanced head and neck Cancer: secondary
Ghadjar et al. Radiation Oncology (2015) 10:21 DOI 10.1186/s13014-014-0319-y RESEARCH Open Access Impact of weight loss on survival after chemoradiation for locally advanced head and neck Cancer: secondary
EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA
 ORIGINAL ARTICLE EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA Raymond King Yin Tsang, FRCSEd, Joseph Chun Kit Chung, MRCSEd, Yiu Wing
ORIGINAL ARTICLE EFFICACY OF NECK DISSECTION FOR LOCOREGIONAL FAILURES VERSUS ISOLATED NODAL FAILURES IN NASOPHARYNGEAL CARCINOMA Raymond King Yin Tsang, FRCSEd, Joseph Chun Kit Chung, MRCSEd, Yiu Wing
Accepted 28 April 2005 Published online 13 September 2005 in Wiley InterScience ( DOI: /hed.
 DEFINING RISK LEVELS IN LOCALLY ADVANCED HEAD AND NECK CANCERS: A COMPARATIVE ANALYSIS OF CONCURRENT POSTOPERATIVE RADIATION PLUS CHEMOTHERAPY TRIALS OF THE EORTC (#22931) AND RTOG (#9501) Jacques Bernier,
DEFINING RISK LEVELS IN LOCALLY ADVANCED HEAD AND NECK CANCERS: A COMPARATIVE ANALYSIS OF CONCURRENT POSTOPERATIVE RADIATION PLUS CHEMOTHERAPY TRIALS OF THE EORTC (#22931) AND RTOG (#9501) Jacques Bernier,
Oral cavity cancer Post-operative treatment
 Oral cavity cancer Post-operative treatment Dr. Christos CHRISTOPOULOS Radiation Oncologist Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Important issues RT -techniques Patient selection
Oral cavity cancer Post-operative treatment Dr. Christos CHRISTOPOULOS Radiation Oncologist Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Important issues RT -techniques Patient selection
Weekly Versus Triweekly Cisplatin-Based Chemotherapy Concurrent With Radiotherapy in the Treatment of Cervical Cancer
 REVIEW ARTICLE Weekly Versus Triweekly Cisplatin-Based Chemotherapy Concurrent With Radiotherapy in the Treatment of Cervical Cancer A Meta-Analysis Xingxing Chen, MD,* Haizhou Zou, MD,Þ Huifang Li, MD,*
REVIEW ARTICLE Weekly Versus Triweekly Cisplatin-Based Chemotherapy Concurrent With Radiotherapy in the Treatment of Cervical Cancer A Meta-Analysis Xingxing Chen, MD,* Haizhou Zou, MD,Þ Huifang Li, MD,*
Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit
 Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
SAMO MASTERCLASS HEAD & NECK CANCER. Nicolas Mach, PD Geneva University Hospital
 SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
5/20/ ) Haffty GB: Concurrent chemoradiation in the treatment of head and neck cancer. Hematol. Oncol. Clin: North Am.
 Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
Emerging Role of Immunotherapy in Head and Neck Cancer
 Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Scottish Medicines Consortium
 Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Laryngeal and hypopharyngeal cancers
 Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
Head and Neck Cancer:
 Head and Neck Cancer: Robert Haddad M.D. Clinical Director Head and Neck Oncology Program Dana Farber Cancer Institute Boston, MA Predictive Biomarkers: HPV Abstract 6003: Survival Outcomes By HPV Status
Head and Neck Cancer: Robert Haddad M.D. Clinical Director Head and Neck Oncology Program Dana Farber Cancer Institute Boston, MA Predictive Biomarkers: HPV Abstract 6003: Survival Outcomes By HPV Status
Oncologist. The. Outcomes Research. Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis
 The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer
 The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
State of the art for radiotherapy of SCCHN
 State of the art for radiotherapy of SCCHN Less side effects Cured More organ & function preservation Head & neck cancer = 42 000 new cases / year in Europe Not cured Local failure Distant failure More
State of the art for radiotherapy of SCCHN Less side effects Cured More organ & function preservation Head & neck cancer = 42 000 new cases / year in Europe Not cured Local failure Distant failure More
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer
 Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer. Dr P Vijay Anand Reddy Director Apollo Cancer Hospital
 Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Practice teaching course on head and neck cancer management
 28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Nicolas Magné France
28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Nicolas Magné France
Accepted 20 April 2009 Published online 25 June 2009 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.21179
 ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
The clinicopathological features and treatment modalities associated with survival of neuroendocrine cervical carcinoma in a Chinese population
 Zhang et al. BMC Cancer (2019) 19:22 https://doi.org/10.1186/s12885-018-5147-2 RESEARCH ARTICLE Open Access The clinicopathological features and treatment modalities associated with survival of neuroendocrine
Zhang et al. BMC Cancer (2019) 19:22 https://doi.org/10.1186/s12885-018-5147-2 RESEARCH ARTICLE Open Access The clinicopathological features and treatment modalities associated with survival of neuroendocrine
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Guillaume Janoray, Yoann Pointreau, Pascal Garaud, Sophie Chapet, Marc Alfonsi, Christian Sire, Eric Jadaud, Gilles Calais
 JNCI J Natl Cancer Inst (016) 108(4): djv368 doi:10.1093/jnci/djv368 First published online December 16, 015 Article Long-Term Results of a Multicenter Randomized Phase III Trial of Induction Chemotherapy
JNCI J Natl Cancer Inst (016) 108(4): djv368 doi:10.1093/jnci/djv368 First published online December 16, 015 Article Long-Term Results of a Multicenter Randomized Phase III Trial of Induction Chemotherapy
New Paradigms for Treatment of. Erminia Massarelli, MD, PHD, MS Clinical Associate Professor
 New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers
 Original Research Article Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers Kuppa Prakash 1*, A. Ravi Chandran 2, M.
Original Research Article Comparison of acute toxicities and response of standard chemo radiation versus hyper fractionated radiotherapy in head and neck cancers Kuppa Prakash 1*, A. Ravi Chandran 2, M.
Pre- Versus Post-operative Radiotherapy
 Postoperative Radiation and Chemoradiation: Indications and Optimization of Practice Dislosures Clinical trial support from Genentech Inc. Sue S. Yom, MD, PhD Associate Professor UCSF Radiation Oncology
Postoperative Radiation and Chemoradiation: Indications and Optimization of Practice Dislosures Clinical trial support from Genentech Inc. Sue S. Yom, MD, PhD Associate Professor UCSF Radiation Oncology
Head and Neck cancer
 Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
Protocol of Radiotherapy for Head and Neck Cancer
 106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
106 年 12 月修訂 Protocol of Radiotherapy for Head and Neck Cancer Indication of radiotherapy Indication of definitive radiotherapy with or without chemotherapy (1) Resectable, but medically unfit, or high
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Locally advanced disease & challenges in management
 Gynecologic Cancer InterGroup Cervix Cancer Research Network Cervix Cancer Education Symposium, February 2018 Locally advanced disease & challenges in management Carien Creutzberg Radiation Oncology, Leiden
Gynecologic Cancer InterGroup Cervix Cancer Research Network Cervix Cancer Education Symposium, February 2018 Locally advanced disease & challenges in management Carien Creutzberg Radiation Oncology, Leiden
Sanguineti s (2)Comment: When it was initially published in 2003 with a median follow-up of 3.8 years (4), the RTOG study led to a change in
 Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
RESEARCH ARTICLE. Jia-Xiang Ye 1, Xia Liang 2, Jian Wei 3, Jing Zhou 3, Yu Liao 3, Yu-Lei Lu 3, Xia-Quan Tang 3, An-Yu Wang 3, Yong Tang 1 * Abstract
 DOI:10.22034/APJCP.2018.19.1.115 Treatment Compliance of Stage II IVB Nasopharyngeal Carcinoma RESEARCH ARTICLE Editorial Process: Submission:08/06/2017 Acceptance:12/02/2017 Compliance with National Guidelines
DOI:10.22034/APJCP.2018.19.1.115 Treatment Compliance of Stage II IVB Nasopharyngeal Carcinoma RESEARCH ARTICLE Editorial Process: Submission:08/06/2017 Acceptance:12/02/2017 Compliance with National Guidelines
JOURNAL SCAN FOR IJHNS
 JOURNAL SCAN FOR IJHNS IJHNS Journal Scan for IJHNS Meta-analysis of Chemotherapy in Head and Neck Cancer (MACH-NC): An Update on 93 Randomized Trials and 17,346 Patients Jean-Pierre Pignon A, Aurélie
JOURNAL SCAN FOR IJHNS IJHNS Journal Scan for IJHNS Meta-analysis of Chemotherapy in Head and Neck Cancer (MACH-NC): An Update on 93 Randomized Trials and 17,346 Patients Jean-Pierre Pignon A, Aurélie
Oral Cavity Cancer Combined modality therapy
 Oral Cavity Cancer Combined modality therapy Dr. Christos CHRISTOPOULOS Radiation Oncologist Head and Neck Cancers Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Disclosure slide I have no
Oral Cavity Cancer Combined modality therapy Dr. Christos CHRISTOPOULOS Radiation Oncologist Head and Neck Cancers Centre Hospitalier Universitaire (C.H.U.) de Limoges, France Disclosure slide I have no
ORIGINAL ARTICLE. Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation
 ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
Three Weekly Versus Weekly Cisplatin as Radiosensitizer in Head and Neck Cancer: a Decision Dilemma
 MINI-REVIEW Three Weekly Versus Weekly Cisplatin as Radiosensitizer in Head and Neck Cancer: a Decision Dilemma Preety Negi 1 *, Pamela Alice Kingsley 2, Himanshu Srivastava 3, Surender Kumar Sharma 4
MINI-REVIEW Three Weekly Versus Weekly Cisplatin as Radiosensitizer in Head and Neck Cancer: a Decision Dilemma Preety Negi 1 *, Pamela Alice Kingsley 2, Himanshu Srivastava 3, Surender Kumar Sharma 4
Concomitant Chemoradiotherapy with Altered Cisplatin Regimen in Management of Locally Advanced Head and Neck Cancers
 Research Article imedpub Journals www.imedpub.com DOI: http://www.imedpub.com/brain-behaviour-and-cognitive-sciences/ Concomitant Chemoradiotherapy with Altered Cisplatin Regimen in Management of Locally
Research Article imedpub Journals www.imedpub.com DOI: http://www.imedpub.com/brain-behaviour-and-cognitive-sciences/ Concomitant Chemoradiotherapy with Altered Cisplatin Regimen in Management of Locally
RT +/- Surgery. Concurrent ChemoRT +/- Surgery
 Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer
 Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
Weekly cisplatin with radiotherapy for locally advanced head and neck squamous cell carcinoma
 JBUON 2016; 21(4): 979-988 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Weekly cisplatin with radiotherapy for locally advanced head and neck
JBUON 2016; 21(4): 979-988 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Weekly cisplatin with radiotherapy for locally advanced head and neck
Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers
 Original Article Free full text available from www.cancerjournal.net Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers Geeta SN, TK Padmanabhan, J Samuel, K Pavithran*,
Original Article Free full text available from www.cancerjournal.net Comparison of acute toxicities of two chemotherapy schedules for head and neck cancers Geeta SN, TK Padmanabhan, J Samuel, K Pavithran*,
Combined Modality Therapy State of the Art. Everett E. Vokes The University of Chicago
 Combined Modality Therapy State of the Art Everett E. Vokes The University of Chicago What we Know Some patients are cured (20%) Induction and concurrent chemoradiotherapy are each superior to radiotherapy
Combined Modality Therapy State of the Art Everett E. Vokes The University of Chicago What we Know Some patients are cured (20%) Induction and concurrent chemoradiotherapy are each superior to radiotherapy
Accepted 24 October 2007 Published online 22 January 2008 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.
 ORIGINAL ARTICLE PHASE II STUDY OF GEFITINIB FOR THE TREATMENT OF RECURRENT AND METASTATIC NASOPHARYNGEAL CARCINOMA Daniel T. T. Chua, MD, 1 William I. Wei, MD, 2 Maria P. Wong, MD, 3 Jonathan S. T. Sham,
ORIGINAL ARTICLE PHASE II STUDY OF GEFITINIB FOR THE TREATMENT OF RECURRENT AND METASTATIC NASOPHARYNGEAL CARCINOMA Daniel T. T. Chua, MD, 1 William I. Wei, MD, 2 Maria P. Wong, MD, 3 Jonathan S. T. Sham,
The Role of Neoadjuvant Chemotherapy in Nasopharyngeal Cancer
 1 Review The Role of Neoadjuvant Chemotherapy in Nasopharyngeal Cancer Rong Yang 1, Xuhua Li 2 1 Jiangsu Key Laboratory of Oral Diseases, Nanjing Medical University; Department of Oral and Maxillofacial
1 Review The Role of Neoadjuvant Chemotherapy in Nasopharyngeal Cancer Rong Yang 1, Xuhua Li 2 1 Jiangsu Key Laboratory of Oral Diseases, Nanjing Medical University; Department of Oral and Maxillofacial
Radiotherapy & Cervical Cancer Dr Mary McCormack Consultant Clinical Oncologist University College Hospital, London,UK
 Lead Group Log Radiotherapy & Cervical Cancer Dr Mary McCormack Consultant Clinical Oncologist University College Hospital, London,UK Cervical Cancer treatment Treatment planning should be made on a multidisciplinary
Lead Group Log Radiotherapy & Cervical Cancer Dr Mary McCormack Consultant Clinical Oncologist University College Hospital, London,UK Cervical Cancer treatment Treatment planning should be made on a multidisciplinary
Comparative study of Gemcitabine versus Cisplatin concurrent with radiotherapy for locally advanced head and neck cancer
 Journal of Cancer Treatment and Research 2014; 2(4): 37-44 Published online August 30, 2014 (http://www.sciencepublishinggroup.com/j/jctr) doi: 10.11648/j.jctr.20140204.12 Comparative study of Gemcitabine
Journal of Cancer Treatment and Research 2014; 2(4): 37-44 Published online August 30, 2014 (http://www.sciencepublishinggroup.com/j/jctr) doi: 10.11648/j.jctr.20140204.12 Comparative study of Gemcitabine
KEYWORDS: chemoradiotherapy, efficacy, late toxicity, nasopharyngeal carcinoma, radiotherapy, randomized controlled trial.
 A Multicenter, Phase 3, Randomized Trial of Concurrent Chemoradiotherapy Plus Adjuvant Chemotherapy Versus Radiotherapy Alone in Patients With Regionally Advanced Nasopharyngeal Carcinoma: 10-Year Outcomes
A Multicenter, Phase 3, Randomized Trial of Concurrent Chemoradiotherapy Plus Adjuvant Chemotherapy Versus Radiotherapy Alone in Patients With Regionally Advanced Nasopharyngeal Carcinoma: 10-Year Outcomes
RAMY R. GHALI, M.D.*; EMAN EL-SHARAWY, M.D.*; AZZA M. ADEL, M.D.* and SAMER A. IBRAHIM, M.D.**
 Med. J. Cairo Univ., Vol. 79, No. 2, June: 13-18, 2011 www.medicaljournalofcairouniversity.com Induction Docetaxel, Cisplatin and 5 Fluorouracil (TPF) Followed by Concomitant Chemoradiotherapy Versus Concomitant
Med. J. Cairo Univ., Vol. 79, No. 2, June: 13-18, 2011 www.medicaljournalofcairouniversity.com Induction Docetaxel, Cisplatin and 5 Fluorouracil (TPF) Followed by Concomitant Chemoradiotherapy Versus Concomitant
Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients: Patient Characteristics and Type of Chemotherapy
 SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
Head and NeckCancer: multi-modal therapeuticintegration
 Head and NeckCancer: multi-modal therapeuticintegration P. Ponticelli, L. Lastrucci, R. De Majo, A. Rampini U.O.C. Radioterapia Ospedale S. Donato ASL 8 -AREZZO Summary Biological considerations Clinical
Head and NeckCancer: multi-modal therapeuticintegration P. Ponticelli, L. Lastrucci, R. De Majo, A. Rampini U.O.C. Radioterapia Ospedale S. Donato ASL 8 -AREZZO Summary Biological considerations Clinical
J Clin Oncol 22: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 22 NUMBER 5 MARCH 1 2004 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Pelvic Irradiation With Concurrent Chemotherapy Versus Pelvic and Para-Aortic Irradiation for High-Risk Cervical
VOLUME 22 NUMBER 5 MARCH 1 2004 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Pelvic Irradiation With Concurrent Chemotherapy Versus Pelvic and Para-Aortic Irradiation for High-Risk Cervical
Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer
 Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer Dylan F. Roden, MD, MPH 1,2 ; David Schreiber, MD 2,3 ; and Babak Givi, MD 1,2 BACKGROUND: Concurrent chemoradiation (CCRT) and upfront
Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer Dylan F. Roden, MD, MPH 1,2 ; David Schreiber, MD 2,3 ; and Babak Givi, MD 1,2 BACKGROUND: Concurrent chemoradiation (CCRT) and upfront
MANAGEMENT OF CA HYPOPHARYNX
 MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary
 Original article Annals of Oncology 14: 1306 1311, 2003 DOI: 10.1093/annonc/mdg330 Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary A. Argiris
Original article Annals of Oncology 14: 1306 1311, 2003 DOI: 10.1093/annonc/mdg330 Concurrent chemoradiotherapy for N2 or N3 squamous cell carcinoma of the head and neck from an occult primary A. Argiris
The prognostic value of location and size change of pathological lymph nodes evaluated on CT-scan following radiotherapy in head and neck cancer
 Nevens et al. Cancer Imaging (2017) 17:8 DOI 10.1186/s40644-017-0111-y RESEARCH ARTICLE Open Access The prognostic value of location and size change of pathological lymph nodes evaluated on CT-scan following
Nevens et al. Cancer Imaging (2017) 17:8 DOI 10.1186/s40644-017-0111-y RESEARCH ARTICLE Open Access The prognostic value of location and size change of pathological lymph nodes evaluated on CT-scan following
Outcomes and patterns of care of patients with locally advanced oropharyngeal carcinoma treated in the early 21 st century
 Garden et al. Radiation Oncology 2013, 8:21 RESEARCH Open Access Outcomes and patterns of care of patients with locally advanced oropharyngeal carcinoma treated in the early 21 st century Adam S Garden
Garden et al. Radiation Oncology 2013, 8:21 RESEARCH Open Access Outcomes and patterns of care of patients with locally advanced oropharyngeal carcinoma treated in the early 21 st century Adam S Garden
THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER
 THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER Piotr Milecki 1, Grażyna Stryczyńska 1, Aleksandra Kruk-Zagajewska 2 Department of Radiotherapy,
THE IMPACT OF THE TIME FACTOR ON THE OUTCOME OF A COMBINED TREATMENT OF PATIENTS WITH LARYN- GEAL CANCER Piotr Milecki 1, Grażyna Stryczyńska 1, Aleksandra Kruk-Zagajewska 2 Department of Radiotherapy,
Larynx Hypopharynx. Therapy algorithms. Why larynx preservation at all? State of the art Jean Louis Lefebvre,Lille Jan Klozar,Prague
 Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
Analysis of the outcome of young age tongue squamous cell carcinoma
 Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Lymph node ratio as a prognostic factor in head and neck cancer patients
 Chen et al. Radiation Oncology (2015) 10:181 DOI 10.1186/s13014-015-0490-9 RESEARCH Open Access Lymph node ratio as a prognostic factor in head and neck cancer patients Chien-Chih Chen 1*, Jin-Ching Lin
Chen et al. Radiation Oncology (2015) 10:181 DOI 10.1186/s13014-015-0490-9 RESEARCH Open Access Lymph node ratio as a prognostic factor in head and neck cancer patients Chien-Chih Chen 1*, Jin-Ching Lin
Post-Operative Concurrent Chemoradiation with Mitomycin-C for Advanced Head and Neck Cancer
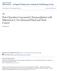 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2006 Post-Operative Concurrent Chemoradiation with Mitomycin-C for
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2006 Post-Operative Concurrent Chemoradiation with Mitomycin-C for
J Clin Oncol by American Society of Clinical Oncology INTRODUCTION
 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Sequencing of Postoperative Radiotherapy and Chemotherapy for Locally Advanced or Incompletely Resected Non Small-Cell Lung Cancer Samual Francis,
JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Sequencing of Postoperative Radiotherapy and Chemotherapy for Locally Advanced or Incompletely Resected Non Small-Cell Lung Cancer Samual Francis,
NICE Single Technology Appraisal of cetuximab for the treatment of recurrent and /or metastatic squamous cell carcinoma of the head and neck
 NICE Single Technology Appraisal of cetuximab for the treatment of recurrent and /or metastatic squamous cell carcinoma of the head and neck Introduction Merck Serono appreciates the opportunity to comment
NICE Single Technology Appraisal of cetuximab for the treatment of recurrent and /or metastatic squamous cell carcinoma of the head and neck Introduction Merck Serono appreciates the opportunity to comment
The management of advanced supraglottic and
 ORIGINAL ARTICLE ORGAN PRESERVATION FOR ADVANCED LARYNGEAL CARCINOMA Robert L. Foote, MD, 1 R. Tyler Foote, 1 Paul D. Brown, MD, 1 Yolanda I. Garces, MD, 1 Scott H. Okuno, MD, 2 Scott E. Strome, MD 3 1
ORIGINAL ARTICLE ORGAN PRESERVATION FOR ADVANCED LARYNGEAL CARCINOMA Robert L. Foote, MD, 1 R. Tyler Foote, 1 Paul D. Brown, MD, 1 Yolanda I. Garces, MD, 1 Scott H. Okuno, MD, 2 Scott E. Strome, MD 3 1
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008
 A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS. Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1.
 RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1. 550 000 NEW PATIENTS/YEAR WITH HEAD AND NECK CANCER ALL
RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1. 550 000 NEW PATIENTS/YEAR WITH HEAD AND NECK CANCER ALL
CACA. Original Article
 Chinese Journal of Cancer Original Article Xing Lu 1,2*, Fei 鄄 Li Wang 1,2*, Xiang Guo 1,2, Lin Wang 1,2, Hai 鄄 Bo Zhang 1,2, Wei 鄄 Xiong Xia 1,2, Si 鄄 Wei Li 1,2, Ning 鄄 Wei Li 1,2, Chao 鄄 Nan Qian 1,2
Chinese Journal of Cancer Original Article Xing Lu 1,2*, Fei 鄄 Li Wang 1,2*, Xiang Guo 1,2, Lin Wang 1,2, Hai 鄄 Bo Zhang 1,2, Wei 鄄 Xiong Xia 1,2, Si 鄄 Wei Li 1,2, Ning 鄄 Wei Li 1,2, Chao 鄄 Nan Qian 1,2
Accepted 12 August 2010 Published online 15 December 2010 in Wiley Online Library (wileyonlinelibrary.com). DOI: /hed.21624
 ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
Diagnosis and what happens after referral
 Diagnosis and what happens after referral Dr Kate Newbold Consultant in Clinical Oncology The Royal Marsden Women's cancers Breast cancer introduction 1 Treatment Modalities Early stage disease -larynx
Diagnosis and what happens after referral Dr Kate Newbold Consultant in Clinical Oncology The Royal Marsden Women's cancers Breast cancer introduction 1 Treatment Modalities Early stage disease -larynx
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
IJC International Journal of Cancer
 IJC International Journal of Cancer Cetuximab or nimotuzumab plus intensity-modulated radiotherapy versus cisplatin plus intensity-modulated radiotherapy for stage II-IVb nasopharyngeal carcinoma Rui You
IJC International Journal of Cancer Cetuximab or nimotuzumab plus intensity-modulated radiotherapy versus cisplatin plus intensity-modulated radiotherapy for stage II-IVb nasopharyngeal carcinoma Rui You
TRANSPARENCY COMMITTEE OPINION. 18 October 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008
 Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Concurrent Chemoradiotherapy with Cisplatin and Docetaxel for Advanced Head and Neck Cancer. A Phase I Study
 Concurrent Chemoradiotherapy with Cisplatin and Docetaxel for Advanced Head and Neck Cancer. A Phase I Study HIDENORI INOHARA 1, TAKEHIRO INOUE 2, SHIRO AKAHANI 1, YOSHIFUMI YAMAMOTO 1, YUKINORI TAKENAKA
Concurrent Chemoradiotherapy with Cisplatin and Docetaxel for Advanced Head and Neck Cancer. A Phase I Study HIDENORI INOHARA 1, TAKEHIRO INOUE 2, SHIRO AKAHANI 1, YOSHIFUMI YAMAMOTO 1, YUKINORI TAKENAKA
