ORIGINAL ARTICLE. Variables Associated With Feeding Tube Placement in Head and Neck Cancer. cases of head and neck cancer
|
|
|
- Scott Walsh
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Variables Associated With Feeding Tube Placement in Head and Neck Cancer Sara S. Cheng, MD, PhD; Jeffrey E. Terrell, MD; Carol R. Bradford, MD; David L. Ronis, PhD; Karen E. Fowler, MPH; Mark E. Prince, MD; Theodoros N. Teknos, MD; Gregory T. Wolf, MD; Sonia A. Duffy, PhD, RN Objective: To identify clinical factors associated with enteral feeding tube placement in a head and neck cancer population. Design: A self-administered survey was given to patients being treated for head and neck cancer while they were waiting to be seen in 1 of 4 otolaryngology clinics. The post hoc analysis presented here combines survey and chart review data to determine clinical and demographic variables associated with feeding tube placement. Setting: Four otolaryngology clinics. Patients: Otolaryngology clinic patients being treated for head and neck cancer. Main Outcome Measure: Enteral feeding tube placement. Results: Of the 724 patients eligible for this study, 14% (n=98) required enteral feeding tube placement. Multivariate analysis found the following variables to be independently associated with feeding tube placement: oropharynx/hypopharynx tumor site (odds ratio [OR], 2.4; P=.01), tumor stage III/IV (OR, 2.1; P=.03), flap reconstruction (OR, 2.2; P=.004), current tracheotomy (OR, 8.0; P), chemotherapy (OR, 2.6; P), and increased age (OR, 1.3; P=.02). In addition, there was a curvilinear relationship between time since treatment and feeding tube placement, with about 30% having a feeding tube at 1 month posttreatment, tapering down during the first 3 years to about 8% and leveling off thereafter. Conclusions: Identification of factors associated with an increased risk of feeding tube placement may allow physicians to better counsel patients regarding the possibility of feeding tube placement during treatment. Since feeding tube placement has been linked to decreased quality of life in head and neck cancer, such counseling is an integral part of the clinical management of these patients. Arch Otolaryngol Head Neck Surg. 2006;132: Author Affiliations: Departments of Otolaryngology Head and Neck Surgery (Drs Cheng, Terrell, Bradford, Prince, Teknos, Wolf, and Duffy) and Psychiatry (Dr Duffy), University of Michigan Medical School, Veterans Affairs Health Services Research & Development Center for Practice Management & Outcomes Research (Drs Ronis and Duffy and Ms Fowler), Department of Otolaryngology, Veterans Affairs Ann Arbor Healthcare System (Dr Prince), and School of Nursing, University of Michigan (Dr Ronis), Ann Arbor. Dr Cheng is now with the Department of Anesthesiology, University of Colorado Health Sciences Center, Denver. EACH YEAR, NEW cases of head and neck cancer are diagnosed worldwide, with over new cases in the United States alone. In the United States, deaths per year are caused by head and neck cancer. 1 In addition to mortality, head and neck cancer causes significant morbidity related to problems with poor nutrition, decreased communication, pain, and decreased general functional capability. 2,3 Patients with advanced head and neck cancer are often nutritionally depleted at initial presentation. An increasing number of patients with head and neck cancer require enteral feeding supplementation during the course of their treatment because of increasingly aggressive multimodal therapy. Common indications for feeding tube placement in these patients include tumor-related factors (malnutrition or dysphagia) as well as treatment-related factors (dysphagia, odynophagia from surgery or irradiation, repeated aspiration, and pharyngocutaneous fistula). 4,5 Complications arising from gastrostomy tube placement contribute to morbidity, including infection, blockage of the tube, and aspiration pneumonitis. 6,7 More rare but serious complications include gastrointestinal bleeding, peritonitis, and metastasis of the primary tumor to the gastrostomy site. 6,8 Initiation of enteral tube feeding is also a significant cause of head and neck cancer associated decreases in quality of life, 9,10 as documented by a previous study by our group. 11 To aid in prospective identification of patients at risk for prolonged enteral feeding, this study was designed to determine which clinical and demographic variables are associated with enteral feeding tube placement. METHODS This multicenter cross-sectional study was part of a larger study investigating quality of life in patients with head and neck cancer. A research assistant distributed a self-administered questionnaire on quality of life to a convenience sample of patients with head and neck cancer while they were waiting to be seen in 655
2 the otolaryngology clinic. Research assistants helped patients complete the questionnaire as needed. Clinical data were abstracted from medical records. Institutional review board approval was obtained at each site prior to the study. SAMPLING PROCEDURES Subjects were recruited from 4 medical centers including 3 Veterans Affairs (VA) hospitals, in Ann Arbor, Mich, Gainesville, Fla, and Dallas, Tex, and the University of Michigan Hospital from 2000 to Of the 1561 patients initially approached, 62% (n=973) agreed to participate and met all eligibility requirements. The inclusion criterion was presence of cancer of the head and neck. Excluded were patients who, from the time of diagnosis and any time thereafter, were (1) pregnant; (2) younger than 18 years; (3) non-english speaking; or (4) found to have a tumor not arising from the upper aerodigestive tract (such as thyroid, parotid, or skin cancer). An additional 249 subjects had completed the survey less than 1 month after most recent therapy and were excluded from these analyses, leaving a sample size of 724 subjects. A 1-month threshold was chosen because it was thought that within 1 month after treatment, both patients and clinicians would regard enteral tube feeding as a short-term and nonextreme intervention, whereas the physical and psychosocial impact might be perceived as much larger when enteral feeding tube placement is required over an extended period after treatment. MEASURES The independent variables of interest included clinical and demographic variables. The dependent variable was enteral feeding tube placement at the time of the survey. Both nasogastric tubes and gastrostomy tubes were coded as feeding tubes. Some of the feeding tubes were placed prior to initiation of therapy and were coded according to whether they were present or absent at the time of survey. Thus, feeding tubes placed prophylactically, for previous tumor-unrelated treatment, and during the course of head and neck cancer treatment were all coded simply as present at the time of survey. Clinical variables consisted of time since treatment, tumor stage, tumor site, current tracheotomy (excluding laryngectomy stoma), surgery (total laryngectomy, primary site excluding laryngectomy, any flap reconstruction, and/or neck dissection), and adjuvant therapy (chemotherapy and/or radiation). Tumor sites were categorized into 3 groups: oropharynx/ hypopharynx, oral cavity/other, and larynx. These categories were chosen because oropharynx and hypopharynx sites behaved similarly in quality of life data from our previous research, as did oral cavity and other sites. 2,3 The other sites included nasal cavity, nasopharynx, sinus tumors, and unknown primary sites. Tumor stage was classified as stage 0/I/II vs stage III/IV. Flap reconstructions included both free and regional flaps. Nonflap reconstructions included primary closures, skin grafts, local flaps, and healing by secondary intention. Since patients were surveyed at different points in treatment, time since most recent treatment of head and neck cancer was measured in months since treatment. Demographic control variables consisted of age, sex, race, marital status, education, and hospital site. Since there were so few African Americans and other race respondents compared with whites, race was classified into white and nonwhite for analysis. Similarly, marital status was classified as married vs not married (separated, widowed, divorced, or never married). Education was classified as high school or less, some college, or college or more. Hospital site was classified as University of Michigan or 1 of the 3 VA hospitals (Ann Arbor, Dallas, or Gainesville). STATISTICAL ANALYSIS Descriptive statistics (means and frequencies) were computed on all demographic, clinical, and treatment variables. Bivariate analysis was conducted between the independent variables collected and the dependent variable, feeding tube placement. 2 Tests were used for categorical variables, t tests for interval level variables. Logistic regression was used to conduct multivariate analyses to determine the predictors of feeding tube placement as well as to determine the probability of having a current feeding tube given the number of predictor variables present. Owing to power limitations, not all of the variables that were statistically significant in the bivariate analysis could be included in the multivariate analysis. Therefore, variables that showed the strongest statistical associations with feeding tube placement in the bivariate analysis were chosen, including tumor site, tumor stage, flap reconstruction, current tracheotomy, irradiation, and chemotherapy. While age was not significant in the bivariate analysis, it is known to be associated with swallowing and was hence included in the analysis. Since a curvilinear relationship was observed between time since treatment and likelihood of feeding tube placement, a time-squared variable was included in the multivariate analysis. While sex and race have been significant predictors in other head and neck cancer studies, they were omitted from the multivariate analysis because they were highly correlated with hospital site (VA vs university hospital) and were not significant in the bivariate analysis. The data were entered into a Microsoft Access database and analyzed using SAS software (SAS Institute Inc, Cary, NC). Since all the respondents did not answer all of the questions, sample size varied for different analyses. For all tests, a 2-tailed P value of less than.05 was considered statistically significant. The probability of having an enteral feeding tube if 1 or more of the significant clinical (but not demographic) risk factors were present was calculated using a logistic regression. The 5 clinical variables included in this analysis were oropharyngeal and/or hypopharyngeal site, stage III or IV cancer, any flap reconstruction, current tracheotomy, and chemotherapy. Count variables were created based on the sum of predictor variables present for each subject (0, 1, 2, 3, 4, or 5). The count variables were then used in a logistic regression to generate the probability of having a feeding tube given the number of predictor variables. It should be noted that only 1 subject had all 5 chosen clinical variables. This did not provide enough data to accurately assess the probability if all 5 variables were present; therefore, no estimate of probability is given for 5 variables. Age was not included in this model because it was considered a demographic rather than a clinical variable. In addition, an arbitrary cutoff between younger and older was difficult to justify. RESULTS UNIVARIATE ANALYSIS Descriptive statistics are reported in Table 1 and Table 2. Fourteen percent (n=98) of patients in the study had an enteral feeding tube in place at the time of the survey. Tumor sites were evenly distributed among hypopharynx/oropharynx, oral cavity/other, and larynx. Almost two thirds of patients (64%; n=449) were classified as stage III/IV. Almost three quarters of the study population (71%; n=516) underwent some type of head and neck surgery (excluding biopsies) as part of their overall treatment. About one fifth of all study patients (21%; 656
3 Table 1. Clinical Characteristics of Patients With Head and Neck Cancer at Least 1 Month After Treatment* Clinical Characteristic Patients, No. (%) Enteral feeding tube in place at time of survey Yes 98 (14) No 626 (86) Tumor site Hypopharynx/oropharynx 230 (32) Oral cavity/other 230 (32) Larynx 264 (36) Tumor stage (n = 704) 0/I/II 255 (36) III/IV 449 (64) Surgical procedure (any head and neck surgery) 516 (71) Total laryngectomy 127 (18) Primary site procedure other than laryngectomy 370 (51) Any flap reconstruction 153 (21) Free flap reconstruction 98 (14) Regional flap reconstruction 62 (9) Neck dissection (any) 376 (52) Tracheotomy at time of survey Yes 28 (4) No 696 (96) Irradiation Yes 567 (78) No 157 (22) Chemotherapy Yes 178 (25) No 546 (75) Irradiation and chemotherapy Yes 168 (23) No 556 (77) *Unless otherwise indicated, n = 724. n=153) received some form of surgical flap reconstruction (either regional or free). A small percentage of patients had a tracheotomy at the time of survey (4%; n=28). About three quarters of patients (78%; n=567) underwent radiation therapy. Of the patients who received chemotherapy (25%; n=178), most also received irradiation (n=168) (Table 1). The mean age of the patients surveyed was 61 years at the time of survey. The mean number of months since most recent treatment was 35 months. Most of the patients were male (84%; n=611) and white (89%, n=634). Slightly less than two thirds of study patients were married (61%; n=440). Most of the study patients had only a high school degree or less education (52%; n=374), with a smaller percentage attending some college (32%; n=227) or obtaining a 4-year college degree or more (16%; n=116). Just over half were treated at the University of Michigan (56%; n=409), the rest at a VA hospital. BIVARIATE ANALYSIS Table 2. Demographic Characteristics of 724 Patients With Head and Neck Cancer at Least 1 Month After Treatment* Demographic Characteristic Patient Data* Age, mean (range), y 61 (27-87) Time since most recent treatment, mean (range), mo 35 (1-399) Sex Male 611 (84) Female 113 (16) Race (n = 715) White 634 (89) Nonwhite 81 (11) Marital status (n = 718) Married 440 (61) Not married 278 (39) Educational level (n = 717) High school or less 374 (52) Some college 227 (32) College or more 116 (16) Hospital site University of Michigan 409 (56) Ann Arbor, Mich VAMC 117 (16) Gainesville, Fla VAMC 80 (11) Dallas, Tex VAMC 118 (16) Abbreviation: VAMC, Veterans Affairs medical center. *Unless otherwise indicated, data are reported as number (percentage) of patients. SD = 11. SD = 46. Clinical variables associated with statistically significant increases in rate of enteral feeding tube placement were tumor site of oropharynx/hypopharynx, tumor stage of III/ IV, flap reconstruction, tracheotomy, irradiation, and chemotherapy (Table 3 and Table 4). Age did not show a significant association with feeding tube placement in the bivariate analysis. There was a curvilinear relationship between time since most recent treatment and feeding tube placement. Although 14% of the entire population required a feeding tube, the frequency was greatest 1 to 3 months after treatment and then declined dramatically during the first 2 years after treatment, leveling off at about 8% after that time (Figure). Sex, race, marital status, educational level, and hospital site did not have a statistically significant impact on feeding tube placement. MULTIVARIATE ANALYSIS While the cancer sites of oropharynx/hypopharynx and oral cavity/other compared with larynx were both significant predictors of feeding tube placement in the bivariate analysis, only oropharynx/hypopharynx remained significant in the multivariateanalysis(oddsratio[or], 2.4; P=.01)(Table 5). Stage III/IV disease continued to show a significant association with feeding tube placement(or, 2.1; P=.03). Both flap reconstruction(or, 2.2; P=.004) and tracheotomy(or, 8.0; P) remained significant in the multivariate analysis, with current tracheotomy being the strongest predictor of feeding tube placement of all the independent variables. Irradiation was no longer significant in the multivariate analysis (OR, 1.9; P=.12); however, chemotherapy did remain significantly associated with feeding tube placement (OR, 2.6; P). While increased age was not a significant predictor of feeding tube placement in the bivariate analysis, in the multivariate analysis each decade of age was associated with a 30% greater odds of enteral feeding tube dependence (OR, 1.3; P=.02). Time and time-squared since most recent treatment showed statistically significant associations with the likelihood of feeding tube placement (OR, 0.98; P and OR, 4.6; P, respectively). While the odds 657
4 Table 3. Bivariate Analysis of Patients With Head and Neck Cancer at Least 1 Month After Treatment* Characteristic Patients, No. Clinical Patients With Feeding Tube, % P Value Tumor site Oropharynx/hypopharynx Oral cavity/other Larynx Tumor stage 0/I/II III/IV Surgical procedure (any head and neck surgery) Yes No Primary site procedure other than laryngectomy Yes No Laryngectomy Yes No Any flap reconstruction (regional and free) Yes No Neck dissection Yes No Tracheotomy at time of survey Yes No Irradiation Yes No Chemotherapy Yes No Irradiation and chemotherapy Yes No Demographic Sex Male Female Race White All others Marital status Married Not married Educational level High school or less Some college College or more Hospital site University of Michigan Ann Arbor, Mich VAMC Gainesville, Fla VAMC Dallas, Tex VAMC Abbreviation: VAMC, Veterans Affairs medical center. Table 4. Bivariate Analysis of Patients With Head and Neck Cancer With and Without a Feeding Tube in Place at Least 1 Month After Treatment Demographic Characteristic* ratio of 1.9 for irradiation was not significant, smaller odds ratios for age and time since treatment were significant because each of these was tested against its own standard error, which was influenced by the scaling of the variables and by correlations with other predictors. When the significant clinical (nondemographic) predictors were used in the logistic regression analysis to predict the probability of having an enteral feeding tube, the probability ranged from 0.6% if none of the predictors were present to 59% if 4 of the clinical predictors were present (Table 6). The 5 clinical predictors were oropharyngeal/ hypopharyngeal site, stage III/IV cancer, any flap reconstruction, current tracheotomy, and chemotherapy. COMMENT In this head and neck cancer patient population, statistically higher odds of having enteral feeding tubes at least 1 month after completion of therapy were found in patients with 1 or more of the following variables: oropharyngeal/ hypopharyngeal site, advanced stage, flap reconstruction, current tracheotomy, chemotherapy, increased age, and decreased time since treatment. While at least 2 small studies have attempted to identify clinical variables that predict feeding tube placement in patients with head and neck cancer, 12,13 to our knowledge this study is the first to examine data from a very large cross section of patients that allowed analysis of a greater number of independent variables. TUMOR SITE Feeding Tube in Place Yes (n = 98) No (n = 626) P Value Mean age, y Mean time since treatment, mo Patients With Feeding Tube, % mo 4-6 mo 7-12 mo 1-2 y 2-3 y 3-5 y 5-10 y >10 y Time Since Most Recent Treatment Figure. Percentage of patients with a feeding tube in place by time since most recent treatment (n=724). Multivariate analysis revealed that patients with tumors of the oropharynx/hypopharynx had roughly twice the odds of requiring feeding tube placement when compared with patients with laryngeal tumors. These re- 658
5 Table 5. Clinical and Demographic Characteristics Associated With Enteral Feeding Tube Placement* Independent Variable sults are consistent with prior studies demonstrating that the site of the primary tumor has a predictable impact on the severity of dysphagia experienced by patients with head and neck cancer. Tumors in the posterior oral cavity, including the base of the tongue, soft palate, retromolar trigone, and tonsillar fossa usually cause more severe dysphagia on surgical excision owing to the critical role that the tongue base and posterior pharyngeal wall play in swallowing. 14,15 This results from the relative contributions of oral and pharyngeal structures to the complex act of swallowing, the extent of resection required at a given site, and the loss of sensation that accompanies the interruption of nerve function with surgery. TUMOR STAGE Multivariate Odds Ratio (95% CI) Advanced-stage cancers are more likely to distort and debilitate the mucosa, muscles, nerves, and other tissues that are critical to the complex physiology of swallowing and thereby be associated with greater risk of pretreatment or subsequent dysphagia. In addition, patients with advanced-stage cancers usually require more aggressive therapy, particularly larger doses of radiation to larger fields, larger resections of tissues for those treated with primary site surgery, more complex flap reconstructions, or more rounds of chemotherapy. FLAP RECONSTRUCTION P Value Clinical Oropharynx/hypopharynx site 2.4 ( ).01 Oral cavity/other site 1.8 ( ).10 Tumor stage III/IV 2.1 ( ).03 Flap reconstruction (any) 2.2 ( ).004 Tracheotomy 8.0 ( ) Irradiation 1.9 ( ).12 Chemotherapy 2.6 ( ) Demographic Age (per decade) 1.3 ( ).02 Time since treatment 0.98 ( ) Time squared since treatment 4.6 ( ) Abbreviation: CI, confidence interval. *For all analyses reported herein, n = 704. Flap reconstructions were found to have an independent association with feeding tubes after controlling for other clinical and demographic variables. Tissue flaps can directly contribute to dysphagia in a number of ways. They may obstruct bolus passage if they are bulky, decrease the amount of propulsive force available, or interfere with the normal sensation needed to guide the bolus down the oropharynx. 16 In addition, the surgical defect created is typically greater in patients who require a flap for closure compared with those who have primary site surgical procedure without a flap. Unfortunately, there were not enough patients who received free flaps or regional Table 6. Probability of Feeding Tube Placement Given Increasing Number of Clinical Predictors* Predictors, No. Patients, No. Probability (95% CI) (0-4) (7-15) (13-24) (19-35) (35-79) Abbreviation: CI, confidence interval. *Probabilities and CIs calculated using the strongest clinical predictors of feeding tube placement identified by this study: oropharyngeal/ hypopharyngeal site, stage III/IV cancer, any flap reconstruction, tracheotomy, and chemotherapy. Only 1 subject had all 5 chosen clinical predictors, which did not provide enough data to assess the probability accurately; therefore, no estimate of probability is given for presence of 5 predictors. flaps to include these groups separately in the multivariate analysis. Thus, we could not determine which kind of flap reconstruction, if any, might be associated with an increased incidence of feeding tube placement. TRACHEOTOMY Several mechanisms may explain the strong association between tracheotomy and feeding tube placement. Increased aspiration risk is an indication for both tracheotomy and feeding tube placement, meaning that if a patient requires one procedure, he or she is very likely to require the other procedure as well. In addition, a large body of literature exists describing the negative effects of tracheotomy on swallowing function. 17,18 Since our survey data simply recorded the presence or absence of a tracheotomy at the time of survey, we are unable to conclude if both short-term and long-term tracheotomies are associated with feeding tube placement. IRRADIATION Patients who underwent irradiation appeared more likely to receive feeding tubes in the bivariate analysis, but this association did not remain significant in the multivariate analysis. This was an unexpected result because it is widely assumed that there is a strong association between radiation therapy and dysphagia in patients with head and neck cancer. 16 This is possibly owing to the exclusion of patients who were less than 1 month out from their most recent treatment, who might have had temporary feeding tubes related to early irradiation adverse effects, whereas those further out from treatment might no longer have had feeding tubes at the time they were surveyed. It is possible that a larger sample size might have detected an association between irradiation and enteral feeding tube placement, but it probably would not be as strong a predictor as the other variables identified in this study. CHEMOTHERAPY Patients undergoing chemotherapy had markedly increased odds of receiving a feeding tube compared with 659
6 patients who did not undergo chemotherapy. However, it should be noted that most chemotherapy protocols use chemotherapy in conjunction with irradiation. Thus, the number of patients in our study receiving chemotherapy alone was very small ( 1%), and the 2.6 OR observed really represents the odds associated with combined chemoradiation treatment (after controlling for the other factors in the analysis, including irradiation). The rate of feeding tube placement in patients undergoing chemoradiation therapy for head and neck cancer has not been carefully documented. In the present study, the observed rate of feeding tube placement in patients receiving chemoradiation was 28.0%. Published rates in patients with head and neck cancer undergoing radiotherapy or chemoradiotherapy range widely from 13% to 85% The incidence of severe (grade 3 or 4) mucositis is increased in patients receiving chemoradiation compared with those receiving radiotherapy alone in several randomized trials, 22 making it probable that higher rates of mucositis and other soft tissue damage noted with chemoradiation therapy are causally related to the higher frequency of enteral feeding tube use in these patients. In fact, our clinical experience indicates that patients with laryngeal or hypopharyngeal tumors develop severe mucositis, stricture, and dysphagia after chemoradiation treatment, and therefore enteral feeding tubes are placed prophylactically in many patients undergoing chemoirradiation. Therefore, the association we have noted between chemoradiation therapy and enteral feeding tubes may be due in part to feeding tubes being placed in anticipation of treatment sequelae. Patients who undergo pretreatment, prophylactic enteral feeding tube placement often have the feeding tubes in place for more than 1 month after completion of therapy and so might have been included in this study. This could have skewed the odds calculation to some degree. AGE Each decade of age was associated with a 30% greater odds of feeding tube placement. This is likely related to an increasing number of medical comorbidities in each successive decade of life as well as the neural, muscular, and structural changes in the pharynx and larynx that occur with aging. TIME SINCE TREATMENT As expected, patients who more recently underwent treatment had a higher rate of feeding tube placement. The percentage of patients with feeding tubes decreased from 30% to about 8% in the first 3 years and leveled off thereafter (Figure). Much of this might be explained by the routine placement of feeding tubes as a part of organ preservation protocols, as noted. Survivorship may also play a role, whereby the patients living the longest had less severe disease, required less aggressive therapies, and had better outcomes from treatment, while patients who were in worse clinical condition may not have survived to be surveyed after completion of their treatment. Also, patients farther out from completion of cancer treatment may be better able to adapt to or minimize their dysphagia with swallowing therapy. A PROBABILITY MODEL Based on the clinical risk factors associated with use of an enteral feeding tube in this study, a probability model for assessing the chance of having a feeding tube inserted was generated (Table 6). Each clinical risk factor was associated with an increased probability of enteral feeding tube dependence in this data set, such that patients with no clinical risk factors were unlikely to have an enteral feeding tube (probability, 0.6%), while those with 1, 2, 3, and 4 clinical risk factors had a much higher probability of requiring a feeding tube (probabilities, 10%, 18%, 26%, and 59%, respectively). This probability model does not take into account patient age or time since treatment because these variables were considered demographic rather than clinical variables and are continuous variables rather than dichotomous (absent/present). Therefore, the model in Table 6 may underestimate the risk of feeding tube placement in elderly patients and overestimate the risk in patients who are farther out from treatment. Nevertheless, we believe that this probability model is conceptually easier to grasp than the odds ratios generated from multivariate analyses. Patients and clinical caregivers can more easily generate a rough approximation of the probability of having an enteral tube placed at a time at least 1 month after therapy using this model. As such, we believe that this may be a valuable tool for clinical teaching, patient education, and outcomes research. While this clinical prediction tool may have utility in predicting feeding tube placements, ideally it should be validated in a prospective study of patients with head and neck cancer to confirm its clinical validity prior to using the model as a predictive tool for an individual patient. LIMITATIONS This cross-sectional study uses data collected from patients at 1 point in time; however, this point in time varied from patient to patient with respect to initiation of treatment. While time was included in our analysis, no actual longitudinal follow-up of an a priori population of patients was conducted. Our results are affected by factors that influence whether a patient comes to the clinic, which include time since diagnosis and the severity of their ongoing clinical problems. While we think that there may be different variables associated with short-term and long-term enteral feeding tube placement, the sample size was not large enough to make this comparison. Because our survey data did not distinguish between prophylactically placed feeding tubes and those placed subsequent to initiation of antitumor therapy, the statistical associations found in this study may reflect at least in part which variables influence clinicians in their assessment of which patients will need a feeding tube. Thus, the clinical variables we have found to be associated with feeding tube placement are not necessarily those that lead to clinically significant dysphagia, but these variables are associated with feeding tube placement in standard clinical management of these patients. Nonetheless, clinicians will continue to place enteral feeding tubes based on their best clinical judgment, and these results are a useful description of current clinical practice. 660
7 Despite our efforts to include minority patients by collecting data from 3 VA hospitals, there were still small numbers of minorities (11%) studied. Since a little less than half of the patients were from VA hospitals, whose patient base is largely composed of men, there were fewer women in the study (16%) than are in the general population of patients with head and neck cancer (24%). While we were able to control for time since most recent treatment, all of the patients were not surveyed at the same point in their treatment. Also, the results of this study are only generalizable to patients seen in otolaryngology clinics and not those seen in other settings and practices. Since feeding tube placement is now becoming a standard part of chemoradiation protocols, assessing patients at known times after the completion of their treatment may have given a more accurate picture of the rate of feeding tube dependence after the short-term treatment associated toxic effects have resolved. The number of variables included in our analysis was statistically limited by the sample size, even with the considerable number of patients recruited. Therefore, a number of important clinical distinctions, such as the type of radiotherapy and chemoradiation regimens, were not included in our initial questionnaire. It is certainly likely that increasing irradiation dose would have a positive correlation with the need for feeding tube placement. In addition, there are differences between the amount of mucositis caused by sequential and concomitant chemoradiation treatments. The relationship of these different modalities to the incidence of feeding tube placement would be of interest for further study. In conclusion, in patients with head and neck cancer, statistically higher odds of having enteral feeding tubes in place more than 1 month after completion of therapy was found when 1 or more of 5 clinical factors (oropharyngeal/hypopharyngeal site, advanced stage, flap reconstruction, tracheotomy, and/or chemotherapy) and 2 demographic variables (age and time since most recent treatment) were present. Patients with greater numbers of clinical risk factors had an incrementally greater probability of needing enteral feeding tubes. Since previous work has demonstrated that enteral feeding tube dependence is a strong predictor of large decrements in healthrelated quality of life, these current findings may provide clinicians and patients with some insight into which patients may be at risk for such feeding tube associated decrements in quality of life. Submitted for Publication: March 24, 2005; final revision received November 20, 2005; accepted January 27, Correspondence: Sonia A. Duffy, PhD, RN, Veterans Affairs Ann Arbor Healthcare System, Health Services Research and Development (11H), PO Box , Ann Arbor, MI (sonia.duffy@med.va.gov). Financial Disclosure: None. Funding/Support: This research was supported by grant IIR from the Department of Veterans Affairs, Washington, DC; by GlaxoSmithKline, Research Triangle Park, NC, through the Managed Care Forum; and by the National Institutes of Health, Bethesda, Md, through the University of Michigan s Head and Neck SPORE (Specialized Program of Research Excellence) grant 1 P50 CA Previous Presentation: This research was presented at the Sixth International Conference on Head and Neck Cancer; August 8, 2004; Washington, DC. Acknowledgment: We thank the otolaryngology clinic personnel at the VA hospitals in Ann Arbor, Gainesville, and Dallas and at the University of Michigan Medical Center for their cooperation in the study. We also thank Cynthia Wampler, BS, Lynn Gregory, MSN, Sharon Stephens, RN, and Carol Bishop, MSN, for their participation in data collection and management. Finally, we thank the patients who participated in this study for their time and cooperation. REFERENCES 1. Landis SH, Murray T, Bolden S, Wingo PA. Cancer statistics, CA Cancer J Clin. 1999;49: Terrell JE, Fisher SG, Wolf GT. Long-term quality of life after treatment of laryngeal cancer. Arch Otolaryngol Head Neck Surg. 1998;124: Terrell JE, Nanavati K, Esclamado RM, Bradford CR, Wolf GT. Health impact of head and neck cancer. Otolaryngol Head Neck Surg. 1999;120: RieraL,SandiumengeA,CalvoC,etal.Percutaneousendoscopicgastrostomyinhead and neck cancer patients. ORL J Otorhinolaryngol Relat Spec. 2002;64: Righi PD, Reddy DK, Weisberger EC, et al. Radiologic percutaneous gastrostomy: results in 56 patients with head and neck cancer. Laryngoscope. 1998; 108: Finocchiaro C, Galletti R, Rovera G, et al. Percutaneous endoscopic gastrostomy: a long-term follow-up. Nutrition. 1997;13: Luman W, Kwek KR, Loi KL, Chiam MA, Cheung WK, Ng HS. Percutaneous endoscopic gastrostomy. Singapore Med J. 2001;42: Sinclair JJ, Scolapio JS, Stark ME, Hinder RA. Metastasis of head and neck carcinoma to the site of percutaneous endoscopic gastrostomy: case report and literature review. JPEN J Parenter Enteral Nutr. 2001;25: Padilla GV, Grant MM. Psychosocial aspects of artificial feeding. Cancer. 1985; 55: Roberge C, Tran M, Massoud C, et al. Quality of life and home enteral tube feeding. Br J Cancer. 2000;82: Terrell JE, Ronis DL, Fowler KE, et al. Clinical predictors of quality of life in patients with head and neck cancer. Arch Otolaryngol Head Neck Surg. 2004; 130: Gardine RL, Kokal WA, Beatty JD, Riihimaki DU, Wagman LD, Terz JJ. Predicting the need for prolonged enteral supplementation in the patient with head and neck cancer. Am J Surg. 1988;156: Schweinfurth JM, Boger GN, Feustel PJ. Preoperative risk assessment for gastrostomy tube placement in head and neck cancer patients. Head Neck. 2001; 23: Sessions DG, Zill R, Schwartz SL. Deglutition after conservation surgery for cancer of the larynx and hypopharynx. Otolaryngol Head Neck Surg. 1979;87: Logemann JA, Pauloski BR, Rademaker AW, et al. Speech and swallow function after tonsil/base of tongue resection with primary closure. J Speech Hear Res. 1993;36: Gaziano JE. Evaluation and management of oropharyngeal dysphagia in head and neck cancer. Cancer Control. 2002;9: Nash M. Swallowing problems in the tracheotomized patient. Otolaryngol Clin North Am. 1988;21: Murray KA, Brzozowski LA. Swallowing in patients with tracheotomies. AACN Clin Issues. 1998;9: Newman LA, Vieira F, Schwiezer V, et al. Eating and weight changes following chemoradiation therapy for advanced head and neck cancer. Arch Otolaryngol Head Neck Surg. 1998;124: Adelstein DJ, Saxton JP, Lavertu P, et al. Maximizing local control and organ preservation in stage IV squamous cell head and neck cancer with hyperfractionated radiation and concurrent chemotherapy. J Clin Oncol. 2002;20: Mekhail TM, Adelstein DJ, Rybicki LA, Larto MA, Saxton JP, Lavertu P. Enteral nutrition during the treatment of head and neck carcinoma. Cancer. 2001;91: Calais G, Alfonsi M, Bardet E, et al. Randomized trial of radiation therapy versus concomitant chemotherapy and radiation therapy for advanced-stage oropharynx carcinoma. J Natl Cancer Inst. 1999;91:
Laryngeal Conservation
 Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
Survey of Laryngeal Cancer at SBUH comparing 108 cases seen here from to the NCDB of 9,256 cases diagnosed nationwide in 2000
 Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
Survey of Laryngeal Cancer at comparing 108 cases seen here from 1998 2002 to the of 9,256 cases diagnosed nationwide in 2000 Stony Brook University Hospital Cancer Program Annual Report 2002-2003 Gender
More than 40% of head and neck cancer patients have. Depressive Symptoms, Smoking, Drinking, and Quality of Life Among Head and Neck Cancer Patients
 Depressive Symptoms, Smoking, Drinking, and Quality of Life Among Head and Neck Cancer Patients SONIA A. DUFFY, PH.D., R.N., DAVID L. RONIS, PH.D. MARCIA VALENSTEIN, M.D., KAREN E. FOWLER, M.P.H. MICHAEL
Depressive Symptoms, Smoking, Drinking, and Quality of Life Among Head and Neck Cancer Patients SONIA A. DUFFY, PH.D., R.N., DAVID L. RONIS, PH.D. MARCIA VALENSTEIN, M.D., KAREN E. FOWLER, M.P.H. MICHAEL
MANAGEMENT OF CA HYPOPHARYNX
 MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
MANAGEMENT OF CA HYPOPHARYNX GENERAL TREATMENT RECOMMENDATIONS BASED ON HYPOPHARYNX TUMOR STAGE For patients presenting with early-stage definitive radiotherapy alone or voice-preserving surgery are viable
Percutaneous Endoscopic Gastrostomy Tube Dependence Following Chemoradiation in Head and Neck Cancer Patients
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Percutaneous Endoscopic Gastrostomy Tube Dependence Following Chemoradiation in Head and Neck Cancer Patients
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Percutaneous Endoscopic Gastrostomy Tube Dependence Following Chemoradiation in Head and Neck Cancer Patients
Wojciech K. Mydlarz, M.D. Pharyngocutaneous Fistulas after Salvage Laryngectomy: Need for Vascularized Tissue
 Wojciech K. Mydlarz, M.D. Pharyngocutaneous Fistulas after Salvage Laryngectomy: Need for Vascularized Tissue Disclosures No Relevant Financial Relationships or Commercial Interests Educational Objectives
Wojciech K. Mydlarz, M.D. Pharyngocutaneous Fistulas after Salvage Laryngectomy: Need for Vascularized Tissue Disclosures No Relevant Financial Relationships or Commercial Interests Educational Objectives
Department of Head and Neck Surgery, University of Texas MD Anderson Cancer Center, Houston Texas.
 ORIGINAL ARTICLE Gastrostomy tube placement in patients with hypopharyngeal cancer treated with radiotherapy or chemoradiotherapy: Factors affecting placement and dependence Mihir K. Bhayani, MD, Katherine
ORIGINAL ARTICLE Gastrostomy tube placement in patients with hypopharyngeal cancer treated with radiotherapy or chemoradiotherapy: Factors affecting placement and dependence Mihir K. Bhayani, MD, Katherine
Self-Assessment Module 2016 Annual Refresher Course
 LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
Katsuro Sato. Department of Speech, Language and Hearing Sciences, Niigata University of Health and Welfare, Niigata, Japan
 Report Niigata Journal of Health and Welfare Vol. 12, No. 1 Retrospective analysis of head and neck cancer cases from the database of the Niigata Prefecture Head and Neck Malignant Tumor Registration Committee
Report Niigata Journal of Health and Welfare Vol. 12, No. 1 Retrospective analysis of head and neck cancer cases from the database of the Niigata Prefecture Head and Neck Malignant Tumor Registration Committee
Swallow Preservation Exercises during Chemoradiation Therapy Maintains Swallow Function
 Original Research Head and Neck Surgery Swallow Preservation Exercises during Chemoradiation Therapy Maintains Swallow Function Otolaryngology Head and Neck Surgery 149(6) 878 884 Ó American Academy of
Original Research Head and Neck Surgery Swallow Preservation Exercises during Chemoradiation Therapy Maintains Swallow Function Otolaryngology Head and Neck Surgery 149(6) 878 884 Ó American Academy of
Head and Neck Reirradiation: Perils and Practice
 Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
Head and Neck Reirradiation: Perils and Practice David J. Sher, MD, MPH Department of Radiation Oncology Dana-Farber Cancer Institute/ Brigham and Women s Hospital Conflicts of Interest No conflicts of
NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36
 Cancer of the upper aerodigestive e tract: assessment and management in people aged 16 and over NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36 NICE 2018. All rights reserved. Subject
Cancer of the upper aerodigestive e tract: assessment and management in people aged 16 and over NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36 NICE 2018. All rights reserved. Subject
NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36
 Cancer of the upper aerodigestive e tract: assessment and management in people aged 16 and over NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36 NICE 2018. All rights reserved. Subject
Cancer of the upper aerodigestive e tract: assessment and management in people aged 16 and over NICE guideline Published: 10 February 2016 nice.org.uk/guidance/ng36 NICE 2018. All rights reserved. Subject
Laryngeal Preservation Using Radiation Therapy. Chemotherapy and Organ Preservation
 1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
Geriatric. Care Otolaryngology. Chapter 2. American Academy of Otolaryngology Head and Neck Surgery Foundation
 42 American Academy of Otolaryngology Head and Neck Surgery Foundation American Academy of Otolaryngology Head and Neck Surgery Foundation Geriatric 43 Care Otolaryngology 2006 American Academy of Otolaryngology
42 American Academy of Otolaryngology Head and Neck Surgery Foundation American Academy of Otolaryngology Head and Neck Surgery Foundation Geriatric 43 Care Otolaryngology 2006 American Academy of Otolaryngology
Salivary gland malignancies (SGMs) represent a rare
 Original Research Head and Neck Surgery Feeding Tube Utilization in Patients with Salivary Gland Malignancies Diane Wenhua Chen, MD 1, Jan S. Lewin, PhD 2, Li Xu, PhD 2, Stephen Y. Lai, MD, PhD 2, G. Brandon
Original Research Head and Neck Surgery Feeding Tube Utilization in Patients with Salivary Gland Malignancies Diane Wenhua Chen, MD 1, Jan S. Lewin, PhD 2, Li Xu, PhD 2, Stephen Y. Lai, MD, PhD 2, G. Brandon
Cancer of the upper aerodigestive tract: assessment and management in people aged 16 and over
 Cancer of the upper aerodigestive tract: assessment and management in people aged and over NICE guideline Draft for consultation, March 0 This guideline covers This guideline covers assessing and managing
Cancer of the upper aerodigestive tract: assessment and management in people aged and over NICE guideline Draft for consultation, March 0 This guideline covers This guideline covers assessing and managing
Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer. American Society of Clinical Oncology Clinical Practice Guideline
 Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer American Society of Clinical Oncology Clinical Practice Guideline Introduction ASCO convened an Expert Panel to develop recommendations
Use of Larynx-Preservation Strategies in the Treatment of Laryngeal Cancer American Society of Clinical Oncology Clinical Practice Guideline Introduction ASCO convened an Expert Panel to develop recommendations
Sanguineti s (2)Comment: When it was initially published in 2003 with a median follow-up of 3.8 years (4), the RTOG study led to a change in
 Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
Commento di due Soci AIRO pubblicati su due prestigiose riviste internazionali al Trial della forastiere et al. Long term results of RTOG:91-11 (a cura di Dr. Russi e Dr. Testolin )! Forastiere)et)al.)Long/Term)Results)of)RTOG)91/11:)A)Comparison)of)
Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S.
 Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S. Associate Professor Division of Head and Neck Surgery Department of Otolaryngology-Head and
Head and Neck Cancer in FA: Risks, Prevention, Screening, & Treatment Options David I. Kutler, M.D., F.A.C.S. Associate Professor Division of Head and Neck Surgery Department of Otolaryngology-Head and
Oncologist. The. Outcomes Research. Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis
 The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
The Oncologist Outcomes Research Changes in Survival in Head and Neck Cancers in the Late 20th and Early 21st Century: A Period Analysis DIANNE PULTE, a,b HERMANN BRENNER a a Division of Clinical Epidemiology
FINE NEEDLE ASPIRATION OF ENLARGED LYMPH NODE: Metastatic squamous cell carcinoma
 Case Scenario 1 HNP: A 70 year old white male presents with dysphagia. The patient is a current smoker, current user of alcohol and is HPV positive. A CT of the Neck showed mass in the left pyriform sinus.
Case Scenario 1 HNP: A 70 year old white male presents with dysphagia. The patient is a current smoker, current user of alcohol and is HPV positive. A CT of the Neck showed mass in the left pyriform sinus.
Gourin et al.: Long-Term Outcomes of Larynx Cancer Care in the Elderly
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Short- and Long-Term Outcomes of Laryngeal Cancer Care in the Elderly Christine G. Gourin, MD, MPH; Heather
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Short- and Long-Term Outcomes of Laryngeal Cancer Care in the Elderly Christine G. Gourin, MD, MPH; Heather
ORIGINAL ARTICLE. Predicting the Prognosis of Oral Squamous Cell Carcinoma After First Recurrence
 ORIGINAL ARTICLE Predicting the Prognosis of Oral Squamous Cell Carcinoma After First Recurrence Michael D. Kernohan, FDSRCS, FRCS, MSc; Jonathan R. Clark, FRACS; Kan Gao, BEng; Ardalan Ebrahimi, FRACS;
ORIGINAL ARTICLE Predicting the Prognosis of Oral Squamous Cell Carcinoma After First Recurrence Michael D. Kernohan, FDSRCS, FRCS, MSc; Jonathan R. Clark, FRACS; Kan Gao, BEng; Ardalan Ebrahimi, FRACS;
Quality of life in patients treated for advanced hypopharyngeal or laryngeal cancer
 European Annals of Otorhinolaryngology, Head and Neck diseases (2011) 128, 218 223 ORIGINAL ARTICLE Quality of life in patients treated for advanced hypopharyngeal or laryngeal cancer M. Guibert a, B.
European Annals of Otorhinolaryngology, Head and Neck diseases (2011) 128, 218 223 ORIGINAL ARTICLE Quality of life in patients treated for advanced hypopharyngeal or laryngeal cancer M. Guibert a, B.
Dr. P. Gullane Wharton Chair Head & Neck Surgery Professor Department of Otolaryngology -Head & Neck Surgery University of Toronto
 Wharton Head and Neck Centre The Toronto General Hospital Dr. P. Gullane Wharton Chair Head & Neck Surgery Professor Department of Otolaryngology -Head & Neck Surgery University of Toronto Controversies
Wharton Head and Neck Centre The Toronto General Hospital Dr. P. Gullane Wharton Chair Head & Neck Surgery Professor Department of Otolaryngology -Head & Neck Surgery University of Toronto Controversies
ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER
 ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER Vasu Divi, MD, 1 * Francis P. Worden, MD, 1,2 * Mark E. Prince, MD, 1 Avraham Eisbruch, MD, 3 Julia S. Lee, MD, 4
ORIGINAL ARTICLE CHEMOTHERAPY ALONE FOR ORGAN PRESERVATION IN ADVANCED LARYNGEAL CANCER Vasu Divi, MD, 1 * Francis P. Worden, MD, 1,2 * Mark E. Prince, MD, 1 Avraham Eisbruch, MD, 3 Julia S. Lee, MD, 4
MULTIPLE reports have. Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer ORIGINAL ARTICLE
 ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
Advanced head and neck cancer: surgery and quality of life
 AZIENDA U.L.S.S. 9 TREVISO - UNIVERSITA' DEGLI STUDI DI PADOVA STRUTTURA COMPLESSA CLINICIZZATA DI OTORINOLARINGOIATRIA Centro Regionale per l Oncologia Cervico-Facciale Direttore: Prof.ssa M.C. Da Mosto
AZIENDA U.L.S.S. 9 TREVISO - UNIVERSITA' DEGLI STUDI DI PADOVA STRUTTURA COMPLESSA CLINICIZZATA DI OTORINOLARINGOIATRIA Centro Regionale per l Oncologia Cervico-Facciale Direttore: Prof.ssa M.C. Da Mosto
ESOPHAGEAL STRICTURE AFTER RADIOTHERAPY IN PATIENTS WITH HEAD AND NECK CANCER: EXPERIENCE OF A SINGLE INSTITUTION OVER 2 TREATMENT PERIODS
 ORIGINAL ARTICLE ESOPHAGEAL STRICTURE AFTER RADIOTHERAPY IN PATIENTS WITH HEAD AND NECK CANCER: EXPERIENCE OF A SINGLE INSTITUTION OVER 2 TREATMENT PERIODS Alexander Ahlberg, MD, 1,9 Massoud al-abany,
ORIGINAL ARTICLE ESOPHAGEAL STRICTURE AFTER RADIOTHERAPY IN PATIENTS WITH HEAD AND NECK CANCER: EXPERIENCE OF A SINGLE INSTITUTION OVER 2 TREATMENT PERIODS Alexander Ahlberg, MD, 1,9 Massoud al-abany,
Salvage Laryngectomy. after R T Failure Indications, Complications and Results. Aug
 Salvage Laryngectomy after R T Failure Indications, Complications and Results Aug.3.2013 Acknowledgments I am grateful to the following individuals who have allowed me to use their slides during this presentation:
Salvage Laryngectomy after R T Failure Indications, Complications and Results Aug.3.2013 Acknowledgments I am grateful to the following individuals who have allowed me to use their slides during this presentation:
ORIGINAL ARTICLE. patients with advanced head and neck cancer. Studies have demonstrated
 ORIGINAL ARTICLE Characteristics Associated With Swallowing Changes After Concurrent Chemotherapy and Radiotherapy in Patients With Head and Neck Cancer Joseph K. Salama, MD; Kerstin M. Stenson, MD; Marcy
ORIGINAL ARTICLE Characteristics Associated With Swallowing Changes After Concurrent Chemotherapy and Radiotherapy in Patients With Head and Neck Cancer Joseph K. Salama, MD; Kerstin M. Stenson, MD; Marcy
Head and neck cancer - patient information guide
 Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Head and neck cancer - patient information guide The development of reconstructive surgical techniques in the last 20 years has led to major advances in the treatment of patients with head and neck cancer.
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer
 Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
Simultaneous Integrated Boost or Sequential Boost in the Setting of Standard Dose or Dose De-escalation for HPV- Associated Oropharyngeal Cancer Dawn Gintz, CMD, RTT Dosimetry Coordinator of Research and
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX
 QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
Persistent tracheostomy after primary chemoradiation for advanced laryngeal or hypopharyngeal cancer
 ORIGINAL ARTICLE Persistent tracheostomy after primary chemoradiation for advanced laryngeal or hypopharyngeal cancer Paul A. Tennant, MD, * Elizabeth Cash, PhD, Jeffrey M. Bumpous, MD, Kevin L. Potts,
ORIGINAL ARTICLE Persistent tracheostomy after primary chemoradiation for advanced laryngeal or hypopharyngeal cancer Paul A. Tennant, MD, * Elizabeth Cash, PhD, Jeffrey M. Bumpous, MD, Kevin L. Potts,
Pharyngoesophageal Strictures in Head and Neck Cancer
 Pharyngoesophageal Strictures in Head and Neck Cancer Barbara P. Messing, M.A., CCC-SLP, BRS-S, S, John Saunders, M.D., Patrick K. Ha, M.D., Marshall Levine, M.D., Ray Blanco, M.D., Eva Zinreich, M.D.,
Pharyngoesophageal Strictures in Head and Neck Cancer Barbara P. Messing, M.A., CCC-SLP, BRS-S, S, John Saunders, M.D., Patrick K. Ha, M.D., Marshall Levine, M.D., Ray Blanco, M.D., Eva Zinreich, M.D.,
The management of advanced supraglottic and
 ORIGINAL ARTICLE ORGAN PRESERVATION FOR ADVANCED LARYNGEAL CARCINOMA Robert L. Foote, MD, 1 R. Tyler Foote, 1 Paul D. Brown, MD, 1 Yolanda I. Garces, MD, 1 Scott H. Okuno, MD, 2 Scott E. Strome, MD 3 1
ORIGINAL ARTICLE ORGAN PRESERVATION FOR ADVANCED LARYNGEAL CARCINOMA Robert L. Foote, MD, 1 R. Tyler Foote, 1 Paul D. Brown, MD, 1 Yolanda I. Garces, MD, 1 Scott H. Okuno, MD, 2 Scott E. Strome, MD 3 1
Reconstruction of Hypopharynx and Cervical Oesophagus for Treatment of Advanced Hypopharyngeal Carcinoma and Recurrent Laryngeal Carcinoma
 Original Article Reconstruction of Hypopharynx and Cervical Oesophagus for Treatment of Advanced Hypopharyngeal Carcinoma and Recurrent Laryngeal Carcinoma Guo-Hua Hu, Shi-Xun Zhong, Qing Xiao, 1 Yi Qian,
Original Article Reconstruction of Hypopharynx and Cervical Oesophagus for Treatment of Advanced Hypopharyngeal Carcinoma and Recurrent Laryngeal Carcinoma Guo-Hua Hu, Shi-Xun Zhong, Qing Xiao, 1 Yi Qian,
ORIGINAL ARTICLE. Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx
 ORIGINAL ARTICLE Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx Sandro J. Stoeckli, MD; Andreas B. Pawlik, MD; Margareta Lipp, MD; Alexander Huber, MD;
ORIGINAL ARTICLE Salvage Surgery After Failure of Nonsurgical Therapy for Carcinoma of the Larynx and Hypopharynx Sandro J. Stoeckli, MD; Andreas B. Pawlik, MD; Margareta Lipp, MD; Alexander Huber, MD;
Accepted 12 August 2010 Published online 15 December 2010 in Wiley Online Library (wileyonlinelibrary.com). DOI: /hed.21624
 ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
ORIGINAL ARTICLE IMPACT OF EARLY PERCUTANEOUS ENDOSCOPIC GASTROSTOMY TUBE PLACEMENT ON NUTRITIONAL STATUS AND HOSPITALIZATION IN PATIENTS WITH HEAD AND NECK CANCER RECEIVING DEFINITIVE CHEMORADIATION THERAPY
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX
 QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
Implementation of the Dance Head and Neck Clinical Pathway
 Implementation of the Dance Head and Neck Clinical Pathway Barbara Messing, MA, CCC-SLP, BCS-S, FASHA & Head and Neck Team GBMC Head and Neck Grand Rounds Acknowledgements Acknowledgements Background Evidence
Implementation of the Dance Head and Neck Clinical Pathway Barbara Messing, MA, CCC-SLP, BCS-S, FASHA & Head and Neck Team GBMC Head and Neck Grand Rounds Acknowledgements Acknowledgements Background Evidence
Title. CitationInternational Journal of Clinical Oncology, 20(6): 1. Issue Date Doc URL. Rights. Type. File Information
 Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
ORIGINAL ARTICLE. Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation
 ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
Oral Cavity and Oropharynx Cancer Trends
 Oral Cavity and Oropharynx Cancer Trends Darien Weatherspoon, DDS, MPH Diplomate, American Board of Dental Public Health Program Officer, National Institute of Dental and Craniofacial Research National
Oral Cavity and Oropharynx Cancer Trends Darien Weatherspoon, DDS, MPH Diplomate, American Board of Dental Public Health Program Officer, National Institute of Dental and Craniofacial Research National
Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy
 OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
OPERATIVE TECHNIQUES PICTORIAL ESSAY Bidirectional esophageal dilatation in pharyngoesophageal stenosis postradiotherapy Haim Gavriel, MD,* Cuong Duong, MB, BS, PhD, FRACS, John Spillane, MB, BS, FRACS,
RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS. Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1.
 RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1. 550 000 NEW PATIENTS/YEAR WITH HEAD AND NECK CANCER ALL
RADIO- AND RADIOCHEMOTHERAPY OF HEAD AND NECK TUMORS Zoltán Takácsi-Nagy PhD Department of Radiotherapy National Institute of Oncology, Budapest 1. 550 000 NEW PATIENTS/YEAR WITH HEAD AND NECK CANCER ALL
SITE OF DISEASE AND TREATMENT PROTOCOL AS CORRELATES OF SWALLOWING FUNCTION IN PATIENTS WITH HEAD AND NECK CANCER TREATED WITH CHEMORADIATION
 SITE OF DISEASE AND TREATMENT PROTOCOL AS CORRELATES OF SWALLOWING FUNCTION IN PATIENTS WITH HEAD AND NECK CANCER TREATED WITH CHEMORADIATION Jeri A. Logemann, PhD, 1,3 Alfred W. Rademaker, PhD, 2,3 Barbara
SITE OF DISEASE AND TREATMENT PROTOCOL AS CORRELATES OF SWALLOWING FUNCTION IN PATIENTS WITH HEAD AND NECK CANCER TREATED WITH CHEMORADIATION Jeri A. Logemann, PhD, 1,3 Alfred W. Rademaker, PhD, 2,3 Barbara
Surgery in Head and neck cancers.principles. Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer
 Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Pharyngocutaneous Fistula Following Laryngectomy
 Pharyngocutaneous Fistula Following Laryngectomy Pages with reference to book, From 130 To 132 Iqbal H.U daipurwala, Khalid Iqbal ( Department of Otolaryngology and Cervico-facial Surgery, Dow Medical
Pharyngocutaneous Fistula Following Laryngectomy Pages with reference to book, From 130 To 132 Iqbal H.U daipurwala, Khalid Iqbal ( Department of Otolaryngology and Cervico-facial Surgery, Dow Medical
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol
 New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura
 Accepted Manuscript Radiation-induced laryngeal angiosarcoma: Case report Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura PII: S2468-5488(18)30005-5
Accepted Manuscript Radiation-induced laryngeal angiosarcoma: Case report Hiroyuki Hanakawa, Nobuya Monden, Kaori Hashimoto, Aiko Oka, Isao Nozaki, Norihiro Teramoto, Susumu Kawamura PII: S2468-5488(18)30005-5
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
The following slides are from a. presentation given by. H. Worth Boyce, M.D. on. Specialized Studies on Diseases of the Esophagus.
 The following slides are from a presentation given by H. Worth Boyce, M.D. on Endoscopic Lumen Restoration at the 8 th OESO World Organization for Specialized Studies on Diseases of the Esophagus. Endoscopic
The following slides are from a presentation given by H. Worth Boyce, M.D. on Endoscopic Lumen Restoration at the 8 th OESO World Organization for Specialized Studies on Diseases of the Esophagus. Endoscopic
Locally advanced head and neck cancer
 Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Long Term Toxicities of Head & Neck Cancer Therapies. Faith Mutale Abramson Cancer Center University of Pennsylvania
 Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Persistent Tracheostomy after Organ Preservation Protocol in Patients Treated for Larynx and Hypopharynx Cancer
 THIEME Original Research 377 Persistent Tracheostomy after Organ Preservation Protocol in Patients Treated for Larynx and Hypopharynx Cancer Carlos Miguel Chiesa Estomba Frank Alberto Betances Reinoso
THIEME Original Research 377 Persistent Tracheostomy after Organ Preservation Protocol in Patients Treated for Larynx and Hypopharynx Cancer Carlos Miguel Chiesa Estomba Frank Alberto Betances Reinoso
Information and support
 13 11 20 Information and support Surgery for head and neck cancer Last reviewed June 2012 Contents Types of surgeries Surgery for oral cancer Surgery for salivary gland cancer Surgery for pharyngeal cancer
13 11 20 Information and support Surgery for head and neck cancer Last reviewed June 2012 Contents Types of surgeries Surgery for oral cancer Surgery for salivary gland cancer Surgery for pharyngeal cancer
Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer
 Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer Dylan F. Roden, MD, MPH 1,2 ; David Schreiber, MD 2,3 ; and Babak Givi, MD 1,2 BACKGROUND: Concurrent chemoradiation (CCRT) and upfront
Triple-Modality Treatment in Patients With Advanced Stage Tonsil Cancer Dylan F. Roden, MD, MPH 1,2 ; David Schreiber, MD 2,3 ; and Babak Givi, MD 1,2 BACKGROUND: Concurrent chemoradiation (CCRT) and upfront
The surgical management of subglottic stenosis (SGS)
 Original Research Pediatric Otolaryngology Short- versus Long-term Stenting in Children with Subglottic Stenosis Undergoing Laryngotracheal Reconstruction Otolaryngology Head and Neck Surgery 2018, Vol.
Original Research Pediatric Otolaryngology Short- versus Long-term Stenting in Children with Subglottic Stenosis Undergoing Laryngotracheal Reconstruction Otolaryngology Head and Neck Surgery 2018, Vol.
ELIZABETH CEDARS DR. KOREY HOOD Available September 29
 ELIZABETH CEDARS DR. KOREY HOOD Available September 29 Title and Investigators Optimizing Surgical Management of Thyroid Cancer: Using Surgeon-performed Ultrasound to Predict Extrathyroidal Extension of
ELIZABETH CEDARS DR. KOREY HOOD Available September 29 Title and Investigators Optimizing Surgical Management of Thyroid Cancer: Using Surgeon-performed Ultrasound to Predict Extrathyroidal Extension of
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Thomas Gernon, MD Otolaryngology THE EVOLVING TREATMENT OF SCCA OF THE OROPHARYNX
 Thomas Gernon, MD Otolaryngology THE EVOLVING TREATMENT OF SCCA OF THE OROPHARYNX Disclosures I have nothing to disclose. 3 Changing Role of Surgery N=42,688 Chen Ay et al. Larygoscope. 2007; 117:16-21
Thomas Gernon, MD Otolaryngology THE EVOLVING TREATMENT OF SCCA OF THE OROPHARYNX Disclosures I have nothing to disclose. 3 Changing Role of Surgery N=42,688 Chen Ay et al. Larygoscope. 2007; 117:16-21
Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience
 1 Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience John P. Dahl, MD, PhD, MBA 1,2, *, Patricia L. Purcell, MD 1, MPH, Sanjay R. Parikh, MD, FACS 1, and Andrew F.
1 Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience John P. Dahl, MD, PhD, MBA 1,2, *, Patricia L. Purcell, MD 1, MPH, Sanjay R. Parikh, MD, FACS 1, and Andrew F.
Hypopharynx. 1. Introduction. 1.1 General Information and Aetiology
 Hypopharynx 1. Introduction 1.1 General Information and Aetiology The human pharynx is the part of the throat situated between the nasal cavity and the esophagus and can be divided into three parts: the
Hypopharynx 1. Introduction 1.1 General Information and Aetiology The human pharynx is the part of the throat situated between the nasal cavity and the esophagus and can be divided into three parts: the
Organ-Preservation Strategies in head and neck cancer. Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari
 Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Neck Dissection. Asst Professor Jeeve Kanagalingam MA (Cambridge), BM BCh (Oxford), MRCS (Eng), DLO, DOHNS, FRCS ORL-HNS (Eng), FAMS (ORL)
 Neck Dissection Asst Professor Jeeve Kanagalingam MA (Cambridge), BM BCh (Oxford), MRCS (Eng), DLO, DOHNS, FRCS ORL-HNS (Eng), FAMS (ORL) History radical neck Henry Butlin proposed enbloc removal of upper
Neck Dissection Asst Professor Jeeve Kanagalingam MA (Cambridge), BM BCh (Oxford), MRCS (Eng), DLO, DOHNS, FRCS ORL-HNS (Eng), FAMS (ORL) History radical neck Henry Butlin proposed enbloc removal of upper
BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES
 ORIGINAL ARTICLE BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES Hadi Seikaly, MD, FRCSC, 1,2 Jana Rieger, PhD, 2 Daniel O Connell,
ORIGINAL ARTICLE BEAVERTAIL MODIFICATION OF THE RADIAL FOREARM FREE FLAP IN BASE OF TONGUE RECONSTRUCTION: TECHNIQUE AND FUNCTIONAL OUTCOMES Hadi Seikaly, MD, FRCSC, 1,2 Jana Rieger, PhD, 2 Daniel O Connell,
PRINCIPLES OF RADIATION ONCOLOGY
 PRINCIPLES OF RADIATION ONCOLOGY Ravi Pachigolla, MD Faculty Advisor: Anna Pou, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2000 HISTORY
PRINCIPLES OF RADIATION ONCOLOGY Ravi Pachigolla, MD Faculty Advisor: Anna Pou, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2000 HISTORY
Improving guideline sensitivity and specificity for the identification of proactive gastrostomy placement in patients with head and neck cancer
 ORIGINAL ARTICLE Improving guideline sensitivity and specificity for the identification of proactive gastrostomy placement in patients with head and neck cancer Teresa E. Brown, BSc (Hons), 1 * Jane Crombie,
ORIGINAL ARTICLE Improving guideline sensitivity and specificity for the identification of proactive gastrostomy placement in patients with head and neck cancer Teresa E. Brown, BSc (Hons), 1 * Jane Crombie,
Indications and techniques of surgery for the primary treatment of HNSCC
 Prof. Christian Simon Chef-de-service Service d ORL et chirurgie cervico-faciale Centre Hospitalier Universitaire Vaudois (CHUV) Université de Lausanne Lausanne, Suisse Indications and techniques of surgery
Prof. Christian Simon Chef-de-service Service d ORL et chirurgie cervico-faciale Centre Hospitalier Universitaire Vaudois (CHUV) Université de Lausanne Lausanne, Suisse Indications and techniques of surgery
Locoregional recurrences are the most frequent
 ORIGINAL ARTICLE SECOND SALVAGE SURGERY FOR RE-RECURRENT ORAL CAVITY AND OROPHARYNX CARCINOMA Ivan Marcelo Gonçalves Agra, MD, PhD, 1 João Gonçalves Filho, MD, PhD, 2 Everton Pontes Martins, MD, PhD, 2
ORIGINAL ARTICLE SECOND SALVAGE SURGERY FOR RE-RECURRENT ORAL CAVITY AND OROPHARYNX CARCINOMA Ivan Marcelo Gonçalves Agra, MD, PhD, 1 João Gonçalves Filho, MD, PhD, 2 Everton Pontes Martins, MD, PhD, 2
ORIGINAL ARTICLE. Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer
 ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
ORIGINAL ARTICLE Examining the Need for Neck Dissection in the Era of Chemoradiation Therapy for Advanced Head and Neck Cancer Laura A. Goguen, MD; Marshall R. Posner, MD; Roy B. Tishler, MD, PhD; Lori
RECURRENCE in the neck is a
 ORIGINAL ARTICLE Efficacy of Targeted Chemoradiation and Planned Selective Neck Dissection to Control Bulky Nodal Disease in Advanced Head and Neck Cancer K. Thomas Robbins, MD; Frank S. H. Wong, MD; Parvesh
ORIGINAL ARTICLE Efficacy of Targeted Chemoradiation and Planned Selective Neck Dissection to Control Bulky Nodal Disease in Advanced Head and Neck Cancer K. Thomas Robbins, MD; Frank S. H. Wong, MD; Parvesh
Hypopharyngeal Squamous Cell Carcinoma: Three-Dimensional or Intensity-Modulated Radiotherapy? A Single Institution s Experience
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Hypopharyngeal Squamous Cell Carcinoma: Three-Dimensional or Intensity-Modulated Radiotherapy? A Single Institution
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Hypopharyngeal Squamous Cell Carcinoma: Three-Dimensional or Intensity-Modulated Radiotherapy? A Single Institution
Department of Head and Neck Surgery, University of Texas MD Anderson Cancer Center, Houston Texas.
 ORIGINAL ARTICLE Gastrostomy tube placement in patients with oropharyngeal carcinoma treated with radiotherapy or chemoradiotherapy: Factors affecting placement and dependence Mihir K. Bhayani, MD, Katherine
ORIGINAL ARTICLE Gastrostomy tube placement in patients with oropharyngeal carcinoma treated with radiotherapy or chemoradiotherapy: Factors affecting placement and dependence Mihir K. Bhayani, MD, Katherine
Scottish Audit of Head and Neck Cancers. A Prospective Audit
 Scottish Audit of Head and Neck Cancers Steering Group Scottish Audit of Head and Neck Cancers A Prospective Audit Report 1999 2002 Edited by David Loeb and Tracey Rapson Statistical Analysis by Tracey
Scottish Audit of Head and Neck Cancers Steering Group Scottish Audit of Head and Neck Cancers A Prospective Audit Report 1999 2002 Edited by David Loeb and Tracey Rapson Statistical Analysis by Tracey
Laryngeal Conservation February 2005
 TITLE: Laryngeal Conservation SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: February 9, 2005 RESIDENT PHYSICIAN: Sarah Rodriguez, MD FACULTY ADVISOR: Shawn Newlands, MD, PhD, MBA
TITLE: Laryngeal Conservation SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: February 9, 2005 RESIDENT PHYSICIAN: Sarah Rodriguez, MD FACULTY ADVISOR: Shawn Newlands, MD, PhD, MBA
American Head and Neck Society - Journal Club Volume 9, December 2016
 - Table of Contents click the page number to go to the summary and full article link. Does resident participation influence otolaryngology-head and neck surgery morbidity and mortality? page 1 Risk of
- Table of Contents click the page number to go to the summary and full article link. Does resident participation influence otolaryngology-head and neck surgery morbidity and mortality? page 1 Risk of
Principles of Management of Head & Neck Cancer. Jinka Sathya Associate professor of Oncology
 Principles of Management of Head & Neck Cancer Jinka Sathya Associate professor of Oncology Oral cavity Oro-pharynx Larynx Hypopharynx Nasophaynx Major sites of Mucosal H&N Cancers Head & Neck Cancer Oral
Principles of Management of Head & Neck Cancer Jinka Sathya Associate professor of Oncology Oral cavity Oro-pharynx Larynx Hypopharynx Nasophaynx Major sites of Mucosal H&N Cancers Head & Neck Cancer Oral
FUNCTIONAL ANALYSIS OF SWALLOWING OUTCOMES AFTER SUPRACRICOID PARTIAL LARYNGECTOMY
 ORIGINAL ARTICLE FUNCTIONAL ANALYSIS OF SWALLOWING OUTCOMES AFTER SUPRACRICOID PARTIAL LARYNGECTOMY Jan S. Lewin, PhD, Katherine A. Hutcheson, MS, Denise A. Barringer, MS, Annette H. May, MA, Dianna B.
ORIGINAL ARTICLE FUNCTIONAL ANALYSIS OF SWALLOWING OUTCOMES AFTER SUPRACRICOID PARTIAL LARYNGECTOMY Jan S. Lewin, PhD, Katherine A. Hutcheson, MS, Denise A. Barringer, MS, Annette H. May, MA, Dianna B.
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Clinical analysis of 29 cases of nasal mucosal malignant melanoma
 1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS
 SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa:
 Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa: 2010-2014 Amanda Kahl, MPH Mary Charlton, PhD, Nitin Pagedar, MD, MPH, Steven Sperry,
Accuracy of the SEER HPV status site specific factor 10 (SSF-10) variable for head and neck cancer (HNC) cases in Iowa: 2010-2014 Amanda Kahl, MPH Mary Charlton, PhD, Nitin Pagedar, MD, MPH, Steven Sperry,
Metastatic Carcinoma to Percutaneous Endoscopic Gastrostomy Tube Sites. A Report of Five Cases
 Metastatic Carcinoma to Percutaneous Endoscopic Gastrostomy Tube Sites A Report of Five Cases Lanjing Zhang, MD, MS, 1,2 Stephanie A. Dean, MD, 1 Emma E. Furth, MD, 1 Gregory S. Weinstein, MD, 3 Virginia
Metastatic Carcinoma to Percutaneous Endoscopic Gastrostomy Tube Sites A Report of Five Cases Lanjing Zhang, MD, MS, 1,2 Stephanie A. Dean, MD, 1 Emma E. Furth, MD, 1 Gregory S. Weinstein, MD, 3 Virginia
Multi-dimensional analysis of oral cavity and oropharyngeal defects following cancer extirpation surgery, a cadaveric study
 Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
Idris et al. Journal of Otolaryngology - Head and Neck Surgery (2018) 47:27 https://doi.org/10.1186/s40463-018-0276-9 ORIGINAL RESEARCH ARTICLE Open Access Multi-dimensional analysis of oral cavity and
LARYNGEAL CANCER IN EGYPT: QUALITY OF LIFE MEASUREMENT WITH DIFFERENT TREATMENT MODALITIES
 ORIGINAL ARTICLE LARYNGEAL CANCER IN EGYPT: QUALITY OF LIFE MEASUREMENT WITH DIFFERENT TREATMENT MODALITIES Ossama A. Hamid, MD, 1 Lobna M. El Fiky, MD, 1 Medani M. Medani, MD, 1 Ayman AbdelHady, MBBCh,
ORIGINAL ARTICLE LARYNGEAL CANCER IN EGYPT: QUALITY OF LIFE MEASUREMENT WITH DIFFERENT TREATMENT MODALITIES Ossama A. Hamid, MD, 1 Lobna M. El Fiky, MD, 1 Medani M. Medani, MD, 1 Ayman AbdelHady, MBBCh,
UPDATE ON RADIOTHERAPY
 1 Miriam Kleiter UPDATE ON RADIOTHERAPY Department for Companion Animals and Horses, Plattform Radiooncology and Nuclear Medicine, University of Veterinary Medicine Vienna Introduction Radiotherapy has
1 Miriam Kleiter UPDATE ON RADIOTHERAPY Department for Companion Animals and Horses, Plattform Radiooncology and Nuclear Medicine, University of Veterinary Medicine Vienna Introduction Radiotherapy has
Speech and Swallowing in KD: Soup to Nuts. Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland
 Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Oral Cancer Risk and Detection
 Oral Cancer Risk and Detection Evan M. Graboyes, MD Assistant Professor Department of Otolaryngology-Head & Neck Surgery Cancer Control Program, Hollings Cancer Center Medical University of South Carolina
Oral Cancer Risk and Detection Evan M. Graboyes, MD Assistant Professor Department of Otolaryngology-Head & Neck Surgery Cancer Control Program, Hollings Cancer Center Medical University of South Carolina
Plain Language Summary: Evaluation of the Neck Mass in Adults
 Plain Language Summary Plain Language Summary: Evaluation of the Neck Mass in Adults Melissa A. Pynnonen, MD, MSc 1, Maria Colandrea, DNP 2,3, Sandra A. Finestone, PsyD 4, and Sarah S. O Connor 5 Otolaryngology
Plain Language Summary Plain Language Summary: Evaluation of the Neck Mass in Adults Melissa A. Pynnonen, MD, MSc 1, Maria Colandrea, DNP 2,3, Sandra A. Finestone, PsyD 4, and Sarah S. O Connor 5 Otolaryngology
PERSISTENT POSTTREATMENT DEPRESSIVE SYMPTOMS IN PATIENTS WITH HEAD AND NECK CANCER
 ORIGINAL ARTICLE PERSISTENT POSTTREATMENT DEPRESSIVE SYMPTOMS IN PATIENTS WITH HEAD AND NECK CANCER Lucy Hynds Karnell, PhD, 1 Gerry F. Funk, MD, 1 Alan J. Christensen, PhD, 2 Eben L. Rosenthal, MD, 3
ORIGINAL ARTICLE PERSISTENT POSTTREATMENT DEPRESSIVE SYMPTOMS IN PATIENTS WITH HEAD AND NECK CANCER Lucy Hynds Karnell, PhD, 1 Gerry F. Funk, MD, 1 Alan J. Christensen, PhD, 2 Eben L. Rosenthal, MD, 3
Transoral robotic total laryngectomy: Report of 3 cases
 CASE REPORT Amy Chen, MD, Section Editor Transoral robotic total laryngectomy: Report of 3 cases Samuel Dowthwaite, MBBS, 1 Anthony C Nichols, MD, 1 John Yoo, MD, 1 Richard V. Smith, MD, 2 Sandeep Dhaliwal,
CASE REPORT Amy Chen, MD, Section Editor Transoral robotic total laryngectomy: Report of 3 cases Samuel Dowthwaite, MBBS, 1 Anthony C Nichols, MD, 1 John Yoo, MD, 1 Richard V. Smith, MD, 2 Sandeep Dhaliwal,
Report prepared on behalf of the Scottish Head and Neck Cancer Networks by the WoSCAN Information Team
 Scottish Head and Neck Cancer Networks Report of the 2011 Clinical Audit Data Presented at the National Head and Neck Cancer Education Day 26th October 2012 Report prepared on behalf of the Scottish Head
Scottish Head and Neck Cancer Networks Report of the 2011 Clinical Audit Data Presented at the National Head and Neck Cancer Education Day 26th October 2012 Report prepared on behalf of the Scottish Head
Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors
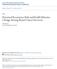 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
