Contributions from plasma NEFA, diet and de novo lipogenesis-derived fatty. acids to fasting VLDL-triglycerides
|
|
|
- Conrad Patrick
- 5 years ago
- Views:
Transcription
1 Contributions from plasma NEFA, diet and de novo lipogenesis-derived fatty acids to fasting VLDL-triglycerides via the delayed secretory pathway in humans Aruna Vedala 1, Wei Wang 1, Richard A. Neese 1, Mark P. Christiansen 1, and Marc K. Hellerstein 1, 2 1 Department of Nutritional Sciences and Toxicology, University of California at Berkeley, Division of Endocrinology and Metabolism, San Francisco General Hospital, University of California, San Francisco, California, Running title: Contributions from plasma NEFA, diet and de novo lipogenesis-derived fatty acids to fasting VLDL-TG via storage pool Correspondence to: Marc K. Hellerstein, MD, PhD, Dept of Nutritional Sciences and Toxicology, 309 Morgan Hall, University of California, Berkeley, CA , USA; Tel: ; FAX: ; march@nature.berkeley.edu Abbreviations: Apo B, apolipoprotein B; CAD, coronary artery disease; DNL, de novo lipogenesis; FA, fatty acids; FAME, fatty acid methyl esters; GC, gas chromatography; GCRC, General Clinical Research Center; HDL C, HDL-cholesterol; HPTG, hypertriglyceridemic; IR, insulin resistance; k s, fractional replacement rates; M 0 and M 1, parent mass and mass +1; MPE, molar percent excess; MS, mass spectrometric; m/z, MH0507ch2 1
2 mass/charge; NPRQ, non protein respiratory quotient; TG, triglyceride; TRL, TG-rich lipoprotein; DHA, docosahexaenoic acid; EM 2 /EM 1, ratio of excess double-labeled to single labeled species; EPA, eicosapentaenoic acid; LPL, lipoprotein lipase; MIDA, mass isotopomer distribution analysis. MH0507ch2 2
3 Abstract Newly synthesized hepatic triglyceride (TG) may exit the liver as VLDL-TG immediately or be stored in the cytosol and secreted after a delay. We quantified in humans the contribution from plasma NEFA, diet and de novo lipogenesis (DNL)- derived fatty acids (FA) to fasting VLDL-TG via the immediate and delayed secretory pathways by a stable isotope labeling approach. Five lean, normolipidemic subjects; six obese, hypertriglyceridemic non-diabetic (HPTG) subjects; and six obese, diabetic HPTG subjects were studied. Intravenous [ 2 H 31 ]-palmitate and [1-13 C 1 ]- acetate and oral [ 2 H 35 ]-stearate were administered during the 30 hour period preceding an overnight fast. [1,2,3,4-13 C 4 ]-palmitate was infused intravenously during the subsequent 12 hr overnight fasting period. The contributions from plasma NEFA via the immediate secretory pathway were 64±15%, 33±6% and 58±2% in control, HPTG and diabetic HPTG groups, respectively. Dietary FA contributed 2.0±0.9%, 2.5±1% and 12±2%, while DNL provided 3±0.3%, 14±3% and 13±4%, in the three groups. The summed delayed pathway contribution from all measured sources was 20±3%, 36±7% and 56±5% in the three groups, leaving unaccounted (unlabeled) contributions of 25±13%, 32±11% and <0%. VLDL-TG production rates and the absolute input rate from the delayed pool were significantly higher in both HPTG and diabetic HPTG than controls. In conclusion, we provide kinetic evidence for an hepatic TG storage pool in humans and document its sources and its importance in HPTG. The turnover time of this pool is shorter and the metabolic sources of TG differ in diabetic HPTG than in non-diabetic HPTG, however. These differences may have therapeutic implications. MH0507ch2 3
4 Key words: Hypertriglyceridemia; diabetes; obesity; TG production; hepatic cytosolic pool; stable isotopes; mass spectrometry. MH0507ch2 4
5 Introduction Hypertriglyceridemia (HPTG) is associated with diabetes [1], obesity [2] and coronary artery disease (CAD) [3]. Most studies have evaluated the relationship between fasting plasma triglyceride (TG) concentrations and CAD [4, 5]. Other workers have demonstrated correlations between postprandial TG elevations and CAD [5, 7, 8], however, consistent with the proposal [6] that atherogenesis is a postprandial phenomenon. Correlations between fasting plasma TG concentrations and the magnitude and duration of postprandial TG response have also been reported [9, 10]. Couillard et al [9], for example, found that fasting plasma TG, insulin and HDL levels showed a strong correlation with postprandial TG-rich lipoprotein (TRL) concentrations. High fasting TG and low HDL-cholesterol (HDL C ) concentrations have also been associated with elevated postprandial TRL levels [10, 11]. Although plasma NEFA are considered to be the major source of VLDL-TG [12-14], dietary fatty acids (FA) carried in chylomicrons and FA synthesized by hepatic de novo lipogenesis (DNL) can also affect VLDL-TG metabolism in a number of ways. FA released from lipolysis of chylomicrons may escape uptake by peripheral tissues and enter the plasma NEFA pool [15-19]. This increased substrate supply may then stimulate hepatic TG production. Persistence of TRL particles into the fasting state [23, 24] may continue to provide FA for fasting VLDL-TG production. Also, remnants of TRL are taken up by a receptor-mediated mechanism in the liver and hydrolyzed in hepatic lysosomes, releasing FA into the cytosol [20, 21]. It is estimated that as much as 50% of dietary fat is taken up as remnant TG by the liver [22]. The hepatic cytosolic TG MH0507ch2 5
6 storage pool may then contribute to VLDL-TG released during the fasted state, via a delayed secretory pathway (Fig. 1). Hepatic DNL is also known to contribute newly synthesized FA to VLDL-TG in both fasting and postprandial states [25, 26]. The literature on DNL contribution to VLDL-TG has focused on the secretion-coupled or immediate secretory pathway, rather than the delayed secretory pathway. The DNL contribution to fasting VLDL-TG is small [23, 25-27], typically providing at most 5-10% of palmitate to fasting VLDL-TG, with somewhat higher values in the fed state [26]. Conflicting results exist as to the fate of FA newly synthesized by DNL in the liver. Duerden et al [28] found that the TG-FA produced via DNL in cultured rat hepatocytes were partitioned preferentially to VLDL for secretion rather than into the cytosolic storage pool. Evidence for delayed input of DNL-derived FA in humans comes from Hudgins et al [29], who found that, during a 39-hour [1-13 C]-acetate infusion, measured DNL contribution was higher on the second morning than the first. This progressive increase in contribution during a long labeling period suggests filling of delayed, or cytosolic, pool with labeled FA (Fig. 1). The most widely accepted pathogenic model [14, 30, 31] for fasting HPTG invokes overproduction of VLDL-TG due to increased rates of lipolysis and FFA flux into the liver [32, 33] in the fasting state. This pathogenic model does not provide a mechanism, however, for linking postprandial metabolic events with overproduction of TG in the fasting state. In the present study we asked whether the hepatic cytosolic TG storage pool could provide such a link between postprandial and fasting TG metabolism. MH0507ch2 6
7 Existence of a hepatic cytosolic TG pool has been demonstrated in vivo and in vitro [36-38]. Obese humans often exhibit higher levels of fat in the liver [39-41], correlating with insulin resistance (IR) [40], dyslipidemia [40, 41] and metabolic syndrome [39]. Metabolic studies of FA sources of VLDL-TG in obese and HPTG subjects have reported a substantial percentage of VLDL-TG FA that are not accounted by circulating [23, 42] or splanchnic [34, 43, 44] NEFA. Additionally, a multicompartmental model of VLDL-TG transport in humans [45] suggested that VLDL-TG secretion is best explained by fast (immediate) and slow (delayed) pathways. In patients with clinically diagnosed hepatic steatosis, Donnelly et al. [46] measured metabolic sources of hepatic TG and fasting VLDL-TG but the contributions from delayed vs. immediate secretory pathways to fasting VLDL-TG were not assessed. In the present study, we tested the hypothesis that a delayed TG storage pool [36-38] makes an important contribution to fasting VLDL-TG in humans and contributes to fasting HPTG (Fig. 1). Contributions from NEFA, DNL and dietary FA to fasting VLDL-TG by the delayed pathway were measured, in addition to contributions from NEFA by the direct pathway, by combining a prelabeling and a direct labeling stable isotope approach. Non-diabetic HPTG, diabetic HPTG and normolipidemic subjects were compared. Methods Human subjects. Subjects were recruited by advertisement and gave written informed consent before enrolling in the study. All study protocols received prior approval from MH0507ch2 7
8 the University of California at San Francisco and University of California at Berkeley human ethical committees. Subjects were recruited from three groups: A) Controls (lean, normolipidemic); B) HPTG (obese, non-diabetic); C) diabetic HPTG (obese with type 2 diabetes mellitus). The selection criteria were as follows: fasting TG concentration <100 mg/dl for control group and mg/dl for HPTG and diabetic HPTG groups; BMI <25 kg/m 2 for controls and kg/ m 2 for HPTG and diabetic HPTG groups; body fat >30% for HPTG and diabetic HPTG groups. Diabetic HPTG subjects had fasting blood glucose concentrations mg/dl and hemoglobina 1 C 7-10%. Additional criteria in control and HPTG groups included having no current or previous diagnosis of diabetes, no family history of diabetes in mother or father, no other significant medical conditions or use of medications and no abnormalities on screening blood tests. The subjects in the diabetic HPTG group were being managed clinically on either insulin therapy or sulfonylurea hypoglycemic agents but not metformin or thiazolidinediones, and were not taking any other medication known to alter lipid or carbohydrate metabolism, e.g. β-blockers, thiazide diuretics, glucocorticoids, hypolipidemic agents, phenytoin, androgens or estrogens. Diabetic HPTG subjects had no other significant medical conditions or abnormalities on screening blood tests. Body composition was measured by bioelectric impedance analysis (model 1990B; Valhalla Scientific Inc., San Diego, California, USA), using manufacturer s equations. Waist and hip circumferences were measured at level of umbilicus and point of greatest circumference around the hip, respectively. MH0507ch2 8
9 Study Design. For 2 weeks prior to the metabolic study, subjects received weight maintaining, controlled diets administered on an out-patient basis from the San Francisco General Hospital s General Clinical Research Center (GCRC) diet kitchen, in order to avoid effects of recent dietary differences between groups. Diets were calculated to be eucaloric and of identical macronutrient composition, consisting of 50% carbohydrate, 35% fat and 15% protein. Each subject s daily dietary requirements were estimated by GCRC dieticians, based on the basal metabolic rate of each individual by the Harris-Benedict equation and dietary records. Diet was adjusted by up to 100 Kcal/day to maintain constant body weight. Diets were composed of foods normally consumed by the subjects. All meals, beverages and snacks were prepared by the staff at the metabolic diet kitchen of the GCRC. Each subject reported to the GCRC 3-5 days per week to be interviewed by the study staff, get weighed and to consume either dinner or breakfast. Food to be consumed until the next visit was packed and given to subjects for consumption. Subjects were instructed to consume all the study food and not to consume any other food during this period. At the end of the 2-week weight maintenance period, subjects were admitted to the GCRC at noon on day 1 of the study. The metabolic infusion study was started at 1800 (Fig. 2). Metabolic Infusion Protocol. All labeled substrates were >98% enriched and were sterile and pyrogen free. The metabolic study was started at 1800 of day 1 (Fig. 2). Venous catheters were inserted into the anticubital vein in each arm for separate blood drawing and administration of infusates. The decision to administer [ 2 H 31 ]-palmitate and [1-13 C 1 ]- acetate for the 30-hour period prior to the fasting state was based on previous data from our laboratory [29] which MH0507ch2 9
10 demonstrated an increase in the fractional contribution from DNL to VLDL-TG between a 15 hour (overnight) and a 39 hour (two night) infusion of [1-13 C 1 ]-acetate but no further increase from 39 to 63 hour of [1-13 C 1 ]-acetate infusion. The 30-hour lead-in labeling period used here (Fig. 2) started at 1800 on day 1 and continued to 2400 on day 2. An intravenous infusion of [ 2 H 31 ]-palmitate (0.6 mg/kg/hr) and [1-13 C 1 ]-acetate (7mg/kg/hr) was administered to label the hepatic TG storage pool and subsequently measure the contribution from NEFA and DNL, respectively, via the delayed secretory pathway. Subjects were also administered oral [ 2 H 35 ]-stearate (0.45mg/kg/meal) mixed with meals to measure the contribution from chylomicron remnants to fasting VLDL-TG. Hardy- Schmidt and Kien [47] have previously demonstrated that oral administration of lipid emulsion containing 13 C-palmitate with a meal results in incorporation of 13 C-palmitate label into chylomicrons and VLDL-TG. During the label lead-in period, subjects consumed a total of six meals (4 meals and 2 snacks) that were similar in composition to those consumed during the weight maintenance phase. Each breakfast, lunch and dinner contained approximately 28% of total daily calories and an evening snack contained 16% of total calories. Meal times were as follows: breakfast 0800, lunch 1300, dinner 1800 and snack Each meal was accompanied by a single dose of [ 2 H 35 ]-stearate mixed with 25 gm of unsweetened apple sauce. [ 2 H 35 ]-stearate was mixed to account for 10% of the dietary stearate in each meal. Subjects were required to consume all food given to them during the inpatient period. During the infusion study, subjects in the diabetic HPTG group were managed clinically according to their existing medication regimen. No changes in regimen were required in any of the diabetic HPTG subjects. MH0507ch2 10
11 After completion of the 30-hour lead-in period, the infusion of [ 2 H 31 ]-palmitate and [1-13 C 1 ]- acetate was discontinued and subjects were infused with [1,2,3,4-13 C 4 ]- palmitate (0.42mg/kg/hr) and [2-13 C 1 ]-glycerol (18mg/kg/hr) overnight (midnight day 2 to noon day 3). The fractional contribution calculated from infusion of [1,2,3,4-13 C 4 ]- palmitate represents the direct, or immediate, secretory pathway contribution from NEFA to VLDL-TG in the fasting state. During this 12-hour follow-up period, subjects remained fasted and were only allowed noncaloric, non-caffeine containing beverages. Frequent blood samples were drawn during the entire infusion period (Fig. 2). At on the morning of day 3, indirect calorimetry was performed using a Deltatrac Metabolic Cart (Sensor Medix, Yorba Linda, CA) in the hooded mode. The infusion was stopped at noon on day 3, and subjects were discharged to home. Metabolite Isolation. All blood samples were drawn into iced vacutainer tubes containing 1mg/ml EDTA. Plasma was separated by centrifugation (1,500g) at 4ºC for 20 min and stored at -20ºC until further analysis. For VLDL isolation, plasma samples were ultracentrifuged twice in a 50.3 Beckman rotor at 35,000 rpm for 30 min to separate and remove chylomicrons (1.6x106g at 15ºC) [23, 48]. The remaining sample was used to isolate VLDL (d<1.006g/ml) by ultracentrifugation at 40,000 rpm for 17hrs (1.3x108g at 12ºC) [47, 48]. VLDL-TG were trans-esterified and derivatized to fatty acid-methyl esters (FAME) and reconstituted in heptane for gas chromatography (GC)/mass spectrometric (MS) analysis (model 5971 mass spectrometer with a model 5890 GC and autosampler, Hewlett-Packard Co, Palo Alto, CA). The remaining aqueous fraction, after FAME extraction, containing VLDL-TG glycerol was evaporated to dryness under MH0507ch2 11
12 nitrogen and derivatized with pyridine/acetic anhydride to glycerol-triacetate, then reconstituted in ethyl acetate. Plasma NEFA were separated [23, 48] from cholesterol and phospholipids by Silica gel G thin layer chromatography (Analtech, Newark, DE) and derivatized to FAME [48]. Plasma free glycerol was isolated from 350µl of deproteinized plasma by ion exchange chromatography. Glycerol-triacetate from plasma was derivatized by reaction with acetic anhydride : pyridine (1:1) at 60ºC and reconstituted in ethyl acetate [48]. Additionally, TG and FFA in sample meals (made as pairs to the meal consumed) were extracted by Folch solution (choloform:methanol, 2:1), containing 100 nmol pentadecanoic acid as an internal standard, in 1:10 ratio, followed by TLC separation. TG and FFA fractions were then combined and trans-esterified to FAME for GC/MS analysis to confirm the palmitate enrichment of the food given. Enrichments were within +/ MPE of the intended value (10 MPE). Serum lipids and insulin concentrations were measured by standard methods at the Clinical Laboratories of San Francisco General Hospital. Plasma TG concentrations were analyzed at Unilab (San Jose, CA). Mass Spectrometric Analyses. All GC/MS analyses were done in the selected ion monitoring mode. Palmitate and stearate methyl ester were analyzed by GC/MS using a 25 m DBI fused silica column [48] under electron impact ionization. Under the major palmitate methyl-ester GC peak, mass/charge (m/z) and m/z 301 were monitored, to calculate the incorporation of [1,2,3,4-13 C 4 ]-palmitate and [ 2 H 31 ]-palmitate respectively. The [ 2 H 31 ]-palmitate peak exhibited a shift in GC retention time relative to natural abundance palmitate-methyl ester and had to be monitored accordingly. MH0507ch2 12
13 Abundance matched standard curves of [1,2,3,4-13 C 4 ]-palmitate and [ 2 H 31 ]-palmitate were run concurrently to quantify true isotopic enrichment. Under the major stearate methyl-ester GC peak, m/z 298 and 333 were monitored to calculate the incorporation of [ 2 H 35 ]-stearate. The shift in GC retention time for [ 2 H 35 ]-stearate was taken into account. Abundance matched standard curves of [ 2 H 35 ]-stearate were run concurrently to quantify true isotopic enrichment. Concentrations of FA in plasma samples were determined simultaneously while measuring isotopic enrichments, by using a splitter that diverted a portion of GC effluent to a flame ionization detector, with comparison to pentadecanoic acid as an internal standard [48]. Glycerol-triacetate was transesterified, to remove NEFA then the aqueous fraction, then derivatized to glyceroltriacetate, for analysis with a 10 m DB-225 column (chemical ionization mode, using methane). The enrichment was determined by monitoring m/z 159 and 160, representing parent mass and mass +1 (M 0 and M 1 ), with comparison to a concurrently run standard curve of [2-13 C 1 ]-glycerol [48]. Calculations. The contributions from plasma NEFA to VLDL-TG were calculated based on the precursor-product relationship. Plasma NEFA contribution via the immediate secretory pathway to VLDL-TG in the fasting state was calculated as [23]: (Equ.1) [1,2,3,4-13 C 4 ]-palmitate enrichment in VLDL-TG (at isotopic plateau) [1,2,3,4-13 C 4 ]-palmitate in the plasma NEFA pool (average value) The incorporation of [1,2,3,4-13 C 4 ]-palmitate in VLDL-TG reached or approached a plateau by the10th hour of study. Accordingly, the average enrichment over last 3 MH0507ch2 13
14 time points, between , on day 3, was used for calculation of fractional contribution to VLDL-TG. Plasma and VLDL [ 2 H 31 ]-palmitate enrichments were also used to calculate the contribution from plasma NEFA to fasting VLDL-TG via the delayed secretory pathway. The calculation was as follows: (Equ. 2) [ 2 H 31 ]-palmitate enrichment in VLDL-TG (last three time points) [ 2 H 31 ]-palmitate enrichment in plasma (30-hour average) A correction for recycling of FA through the plasma NEFA pool during fasting was included in the calculations. The basis of this correction is as follows. It is possible for some of the labeled FA administered during the prelabeling period (by iv or dietary routes) to enter fasting VLDL-TG via recycling through the plasma NEFA pool during fasting. This could occur by hydrolysis of labeled hepatic TG or VLDL-TG during the fasting period with release of FA into the plasma and incorporation into VLDL-TG via the immediate secretory pathway (Fig 1). Indeed, plasma NEFA enrichments of [ 2 H 31 ]- palmitate and [ 2 H 35 ]-stearate were measurable during the fasting period (see below). Label incorporation by this route is properly classified as immediate pathway input. To correct for recycling through the plasma NEFA pool during fasting, a correction was made to the delayed pathway from [ 2 H 31 ]-palmitate, by subtracting the input from fasting plasma NEFA: VLDL-TG [ 2 H 31 ]-palmitate enrichment - VLDL-TG [ 2 H 31 ]-palmitate enrichment derived from fasting plasma NEFA (Equ. 3) [ 2 H 31 ]-palmitate enrichment in plasma (30-hour average) MH0507ch2 14
15 The VLDL-TG [ 2 H 31 ]-palmitate enrichment derived from fasting plasma NEFA in Equ. 3 was calculated based on the incorporation ratios observed for [1,2,3,4-13 C 4 ]- palmitate (equ. 1). This is illustrated in the following example: assume VLDL-TG [ 2 H 31 ]-palmitate enrichment (last three time points) was 1.13 molar percent excess (MPE); residual plasma [ 2 H 31 ]-palmitate enrichment (after stopping the 30-hour infusion) was 0.55 MPE; average plasma [ 2 H 31 ]-palmitate enrichment during the lead-in period was 3.19 MPE; and the fractional contribution from NEFA to VLDL-TG by the immediate secretory pathway was 54% (calculated from [1,2,3,4-13 C 4 ]-palmitate incorporation). The calculated contribution of label from recycling of VLDL-derived [ 2 H 31 ]-palmitate through plasma NEFA is then 0.55 MPE 0.54= 0.30 MPE and the corrected delayed pathway contribution = ( )/3.19 = 26.1%. The fractional contribution from dietary FA to VLDL-TG during the postprandial period via the immediate secretory pathway was calculated by dividing the enrichment of [ 2 H 35 ]-stearate in VLDL-TG by the [ 2 H 35 ]-stearate enrichment in each meal (10%). [ 2 H 35 ]- stearate enrichments at the last three time points of the follow-up study period ( day 3) were averaged and calculated (with correction for recycling of FA through NEFA) as follows: (Equ.4) VLDL-TG [ 2 H 35 ]-stearate enrichment - VLDL-TG enrichment derived from recycling through fasting plasma NEFA 10% where the correction for VLDL-TG enrichment derived from fasting plasma [ 2 H 35 ]- stearate (i.e., immediate pathway input) was calculated from measured fasting plasma MH0507ch2 15
16 [ 2 H 35 ]-stearate enrichments and the fractional incorporation from [1,2,3,4-13 C 4 ]- palmitate, as described above for equ 3. Mass isotopomer distribution analysis (MIDA) was used to calculate the fractional contribution from DNL to fasting VLDL-TG palmitate and the isotopic enrichment of the true precursor pool, hepatic acetyl CoA [49, 50]. Based on the principle of combinatorial probabilities, the enrichment of acetyl CoA was inferred from the ratio of excess doublelabeled to single labeled species (EM 2 /EM 1 ). The precursor-product relationship was then applied to calculate the fractional contribution from DNL to VLDL-TG FA during fasting as well as postprandial periods. The average of the last three time points in the morning of day 3 was used to calculate the fractional contribution from DNL to fasting VLDL-TG via the delayed secretory pathway. The VLDL-TG synthetic rate in fasting state was calculated from the incorporation curves of [1,2,3,4-13 C 4 ]-palmitate and [2-13 C 1 ]-glycerol into VLDL-TG. Fractional replacement rates (k s ) were calculated by modeling the rise toward plateau enrichment of [1,2,3,4-13 C 4 ]-palmitate and [2-13 C 1 ]-glycerol in VLDL-TG. The data were fit to the equation y = A x [1-e -ks (t-c) ], where y = VLDL-TG enrichment, A = the plateau value of VLDL-TG enrichment, t = time in hours and c = lag period before isotope incorporation into secreted VLDL-TG. The half-life of VLDL in plasma, t 1/2 (hour) was calculated by dividing by k s [51]. Absolute VLDL synthesis rate (g/hr) was then calculated as: (Equ.5) k s (hr -1 ) x TG concentration (g/dl) x estimated plasma volume (dl) MH0507ch2 16
17 Plasma volume was estimated to be 5% of the lean body weight. Absolute contributions (g/hr) from NEFA, dietary and DNL-derived FA to VLDL-TG were calculated as follows: (Equ.6) fractional contribution VLDL-TG synthesis rate (g/hr) Non protein respiratory quotient (NPRQ), energy expenditure and whole body oxidation of fat and carbohydrate were calculated by indirect calorimetry according to standard equations [52]. Statistical Analysis. All data are expressed as means ± SEM. The statistical significance of differences was determined by Kruskal-Wallis 1-way analysis of variance, where P value <0.05 was defined to be statistically significant. If statistically significant, these results were followed up using Bonferroni techniques at a 5% procedure-wise error rate (10% for insulin) in conjunction with the Mann-Whitney U- Wilcoxon test. SPSS for UNIX, Release 6.14 (Sunos) was used for the analysis. Results Subject Characteristics and Lipid Profile. Subject characteristics and metabolic profiles of the three groups are shown in Table 1. Control subjects were younger than the HPTG and diabetic HPTG subjects, as we had difficulty recruiting normal control subjects in the 50-year old range. Diabetic HPTG subjects were more obese than the HPTG subjects. Lipid profile was assessed from the samples collected at baseline on day 1 of metabolic infusion study. TG and VLDL cholesterol concentrations were MH0507ch2 17
18 significantly higher in HPTG and diabetic HPTG groups compared to the control group. HPTG and diabetic HPTG subjects had significantly higher fasting insulin concentrations compared to the control group (p<0.033). TG concentrations followed a circadian rhythm in all three groups (Fig. 3), with a decrease during fasting followed by an increase during the postprandial period. The TG concentrations were similar in the HPTG and diabetic HPTG groups and were constantly higher than in the control group throughout the study. The TG concentrations at nadir were 58±6, 144±18 and 156±27 mg/dl in control, HPTG and diabetic HPTG groups, respectively, while the observed peak values were 96±12, 293±44 and 289±34 mg/dl in control, HPTG and diabetic HPTG groups, respectively. VLDL-TG synthesis. The rate of synthesis of VLDL-TG was calculated by kinetic modeling of incorporation curves of [2-13 C 1 ]-glycerol (Table 2). VLDL-TG synthesis rates were 0.38±0.03, 1.28±0.20 and 1.04±0.23 g/hr in control, HPTG and diabetic HPTG groups, respectively. The rates of synthesis were significantly higher in HPTG and diabetic HPTG groups compared to the control group (p<0.011). VLDL-TG half life was non-significantly longer in the diabetic HPTG group compared to control and HPTG groups (Table 2). The rate of appearance of glycerol in the fasting state was nonsignificantly higher in the diabetic HPTG group than in control and HPTG groups (average values were 1.3±0.2, 1.8±0.1 and 3.0±0.6 µmol/kg/min in control, HPTG and diabetic HPTG groups, respectively, p>0.055). Immediate Pathway Contribution from NEFA to VLDL-TG. The fractional contribution from NEFA to VLDL-TG via the immediate pathway was calculated from the precursor-product relationship. The [1,2,3,4-13 C 4 ]-palmitate MH0507ch2 18
19 enrichment in plasma NEFA reached a plateau by 2 hours of infusion and leveled off thereafter. The [1,2,3,4-13 C 4 ]-palmitate enrichment time course in VLDL-TG is shown in Fig. 4. The fractional contribution from NEFA to fasting VLDL-TG via the immediate secretory pathway was 64±15%, 33±6% and 58±2% in control, HPTG and diabetic HPTG groups, respectively (Table 2). The fractional contribution was significantly lower in the HPTG group compared to the diabetic HPTG group. There was no significant difference between the three groups in absolute contribution from NEFA to VLDL-TG by the immediate secretory pathway (Table 3). The absolute contribution rates averaged 0.23±0.10, 0.44±0.12 and 0.61±0.14 g/hr in control, HPTG and diabetic HPTG groups, respectively. Delayed Pathway Contribution from NEFA to VLDL-TG. [ 2 H 31 ]-palmitate enrichment in the plasma NEFA pool reached plateau within 2-3 hour of infusion and leveled off during the 30-hour lead-in period (Fig. 5). Within an hour of stopping the infusion at midnight of day 2, plasma enrichments fell to near zero levels in all three groups. [ 2 H 31 ]-palmitate enrichment in VLDL-TG increased progressively until 14 hours (8 AM) on day 2 and stayed at near plateau levels for the rest of the labeling period in control and HPTG groups (Fig. 6). In the diabetic HPTG group there was a further increase until 24hours (6 PM) on day 2. After the infusion was stopped, the VLDL-TG palmitate enrichment decreased gradually in all three groups and reached stable values by the final 2-3 hours of the fasting period. It is possible that some of the labeled FA incorporated into VLDL-TG during the 30-hour lead-in period were released into the plasma NEFA pool by lipolysis of circulating TG or hepatic TG stores, then MH0507ch2 19
20 reincorporated into VLDL-TG during the subsequent fasting period via the immediate secretory pathway (Fig. 1). Accordingly, this input was corrected for (see methods). At the end of the fasting period, the fractional corrected contribution from NEFA to VLDL-TG via the delayed secretory pathway was non-significantly higher in the diabetic HPTG group compared to the control and HPTG groups, with average values of 15±4%, 20±4% and 30±3% in control, HPTG and diabetic HPTG groups, respectively (Table 2). Absolute contributions from NEFA to VLDL-TG via the delayed secretory pathway were 1.2±0.5, 6.7±2.5 and 7.0±1.1 g/day in control, HPTG and diabetic HPTG groups, respectively (Table 3, p<0.05 for control vs. HPTG and diabetic HPTG). Contribution from Dietary FA to VLDL-TG in the fasting state. [ 2 H 35 ]-stearate enrichments in plasma NEFA and VLDL-TG are shown in Fig. 7 and Fig. 8, respectively. At all time points, [ 2 H 35 ]-stearate enrichments in NEFA and VLDL-TG were higher in the diabetic HPTG group. Because dietary fat absorption and chylomicron clearance should be long completed by hours after the last snack at 8 PM on day-2, the persistent elevation of plasma [ 2 H 35 ]-stearate enrichment through noon of the next day, during the follow-up period, implies recycling of FFA released into plasma from lipolysis of circulating VLDL-TG or stored hepatic TG (for which a correction was made - see methods). The corrected fractional contributions from dietary FA to fasting VLDL-TG via the delayed secretory pathway were 2.0±0.9%, 2.5±1% and 12±2% in control, HPTG and diabetic HPTG groups (Table 2), respectively. The absolute contribution from dietary FA to VLDL-TG in the fasting period via the delayed secretory pathway is estimated to be 2.0±0.9, 2.5±1.0 and 12±2.0 g/day, respectively (Table 3). The absolute contribution MH0507ch2 20
21 was higher in the diabetic HPTG group compared to the control group and the HPTG group (p< 0.01) Contribution from Dietary FA to VLDL-TG in the postprandial state. To estimate the contribution from dietary FA to VLDL-TG in the postprandial state, we averaged the enrichments of [ 2 H 35 ]-stearate in VLDL-TG at 2 and 4 hours after ingestion of the last meal on days 1 and 2 to represent the postprandial state (Fig 8). The fractional contributions from dietary FA to VLDL-TG during the postprandial period were: 4%, 2% and 7% (day 1) and 4%, 4% and 21% (day 2), in control, HPTG and diabetic HPTG groups, respectively ( diabetic HPTG significantly different from control and HPTG groups, p<0.05). Contribution from Dietary FA to NEFA pool. During the postprandial period (see above), averaged [ 2 H 35 ]-stearate enrichments in plasma during the evening of day 1 were 0.67%±0.21%, 1.05%±0.32% and 1.69%±0.39%, respectively in control, HPTG and diabetic HPTG groups. [ 2 H 35 ]-stearate enrichments in plasma increased to 0.93%±0.48%, 1.78%±0.40% and 2.12%±0.55%, respectively, in control, HPTG and diabetic HPTG groups on day 2. These enrichment values represent the entry of a fraction of [ 2 H 35 ]-stearate from the diet (10% enrichment) into the NEFA pool. Thus, during the postprandial period, approximately 7%, 10% and 17% on day 1 and 9%, 18% and 21% on day 2 of the FA in plasma NEFA were derived from recent diet in control, HPTG and diabetic HPTG groups, respectively (control group significantly different from both HPTG and diabetic HPTG groups, p<0.05). Contribution from DNL to VLDL-TG in the fasting state. MH0507ch2 21
22 The percent of VLDL-TG FA derived from DNL during the12-hour follow-up period is shown in Fig. 9. The fractional contributions from DNL to fasting VLDL-TG via the delayed secretory pathway were 3±0.3%, 14±3% and 13±4% in control, HPTG and diabetic HPTG groups, respectively (Table 2). Estimated absolute contributions were 0.3±0.03, 4.5±1.2 and 2.8±0.8 g/day (Table 3). The absolute contribution was significantly higher in the HPTG and diabetic HPTG groups compared to the control group (p <0.011). The fractional contribution from DNL was highly variable in the diabetic HPTG group, though consistent within each individual, and ranged from 3-25% (Fig. 10). It was not possible to identify any clinical or metabolic variables that correlated with the differences in lipogenesis among the diabetic HPTG subjects. Contribution from DNL to VLDL-TG in the postprandial state. The percent of newly synthesized FA by DNL during the postprandial period is shown in Fig. 9. Midnight of day 1 and 2 represent two consecutive postprandial periods. The peak values of fractional DNL, at midnight 1, were 6%±2.1%, 9%±1.2% and 8%±2.2% in control, HPTG and diabetic HPTG groups, respectively. In the control group, following the peak at midnight 1, DNL decreased gradually during the fasting period until the consumption of breakfast on day 2. During the daytime, DNL then increased somewhat but stayed at a relatively constant value, only to increase once again during the evening of day 2. In the HPTG group, DNL followed the same pattern as in the control group until after breakfast, followed by a steady increase until midnight of day 2. In the diabetic HPTG group, however, DNL increased progressively from the start of the study to a peak at midnight of day 2. The peak fractional contributions at midnight of day 2 increased to 7%±2.9%, 20%±1.9% and 20%±4.9% in control, HPTG and diabetic MH0507ch2 22
23 HPTG groups, respectively. The increase in fractional DNL from midnight of day 1 to day 2 was significant in the HPTG and diabetic HPTG groups (p<0.05). Fractional DNL appeared to have reaching a plateau value by midnight of day 2 in all the three groups. Fractional DNL was highly variable in the diabetic HPTG group, with the peak values ranging from 3-17% and 5-37% on day 1and 2 respectively (Fig. 10). Energy Expenditure. There was non-significantly higher resting energy expenditure in HPTG and diabetic HPTG groups compared to the control group. Resting energy expenditure was 1.31±0.08, 1.34±0.05 and 1.45±0.14 Kcal/min in control, HPTG and diabetic HPTG groups, respectively. NPRQ were 0.80±0.01, 0.82±0.02 and 0.74±0.09, respectively. Fat and glucose oxidation did not differ significantly in three groups. Fat oxidation was 0.080±0.01, 0.074±0.01 and 0.13±0.06 g/min, respectively. Glucose oxidation was 0.097±0.01, 0.12±0.02 and 0.10±0.05 g/min, respectively. Discussion We present here kinetic evidence confirming a significant contribution from a delayed secretory pathway (or hepatic cytosolic TG storage pool) to fasting VLDG-TG. The relative and absolute inputs from plasma NEFA, diet and DNL-derived FA to fasting VLDL-TG from this delayed pathway were quantified in normolipidemic controls and in HPTG subjects with or without type 2 diabetes. Earlier studies have provided indirect estimates of the contribution from the hepatic cytosolic pool, ranging from 0-50%, based on difference from the direct NEFA contribution in the fasted state [23, 42, 44]. Also, Diraison et al [44] showed a higher rate of VLDL-TG secretion than plasma NEFA esterification in the postabsorptive state, MH0507ch2 23
24 implying that the remaining FA must have originated from the hepatic TG storage pool. Isotopic studies have confirmed TG storage from NEFA in the livers of human subjects [46] [56]. Direct demonstration of a delayed input of labeled NEFA into fasting VLDL- TG had not previously been available, however. The contribution from the delayed pathway (TG storage pool) to fasting VLDL-TG was measured here by pre-labeling the TG storage pool for 30 hrs. Overall, plasma NEFA contributed 15-20% of VLDL-TG FA in the control and non-diabetic HPTG groups via the delayed pathway, whereas the fractional contribution was higher in the diabetic HPTG group. In contrast, the fractional contribution from NEFA by the immediate secretory pathway was 58-64% in the diabetic HPTG and control groups, respectively,, both of which were higher than the contribution in the non-diabetic HPTG group (33%). These results demonstrate differences in the pathways by which plasma NEFA enter VLDL-TG not only between HPTG and normolipidemic subjects, but between diabetic and non-diabetic HPTG subjects. In humans, acute elevation of plasma NEFA stimulates VLDL production [14]. In our study, NEFA contributed 15%-30% of the VLDL-TG FA via the delayed secretory pathway and 33%-64% via the immediate secretory pathway. Accordingly, plasma NEFA was a major contributor of FA to fasting VLDL-TG, particularly when the delayed pathway input is included, in all the groups that we studied. As it is possible that there is dilution of labeled NEFA by FA in the portal circulation, our estimation of NEFA contribution is, if anything, an underestimation of the true contribution to VLDL-TG. The measured contribution from NEFA to fasting VLDL-TG via the immediate secretory pathway was lower in the non-diabetic HPTG than in the control and diabetic MH0507ch2 24
25 HPTG groups. It has previously been shown that the contribution from plasma NEFA to VLDL-TG is lower in HPTG than normotriglyceridemic subjects [23]. Barter and Nestle also reported that a substantial percentage of VLDL-TG were not derived from plasma NEFA in obese subjects [42] and that elevated BMI correlated with lower contribution from NEFA to VLDL-TG. Visceral (portal) input of NEFA are diluting and are not measured as systemic plasma NEFA contribution, but appear as unaccounted input in our protocol. Accordingly, these observations are consistent with a larger contribution from either the delayed pathway (the TG storage pool) or visceral-fat derived (portal vein) NEFA, or both, in obese, HPTG subjects. The diabetic HPTG group exhibited the highest fractional contribution from NEFA to VLDL-TG via the delayed pathway and the contribution via the immediate pathway was also higher than in the non-diabetic HPTG group. The explanation for significantly different fractional contributions through both the immediate and delayed secretory pathways from NEFA between the HPTG and diabetic HPTG groups (Table 2) is not certain. Whole-body oxidation rates of fats were not significantly different, so cannot account for differences in fractional NEFA contribution to stored TG. The most likely unifying explanation is a difference in the turnover time of the delayed (cytosolic) TG pool, with more rapid release of stored TG from the liver in diabetic HPTG subjects. There was no unaccounted FA in the diabetic HPTG group, whereas 32% of FA in fasting VLDL-TG remained unlabeled from all sources (i.e., unaccounted for) in the HPTG group,. Interestingly, Donnelly et al. [46] reported that >60% of hepatic TG remained unlabeled from all sources even after 4-days of labeling in non-diabetic HPTG subjects with fatty liver. Although we did not characterize whether steatosis was present MH0507ch2 25
26 in our HPTG subjects, these results are all consistent with the presence of a slow turnover, persistently unlabeled TG pool in the liver of non-diabetic HPTG subjects that is evidently not present in diabetic HPTG subjects. Our results also demonstrate that dietary fat is a source of FA in VLDL-TG in fasting as well as postprandial states. Dietary fat contribution via the delayed pool accounted for 2-12% of fasting VLDL-TG in the three groups, so this route was not a major contributor of FA to VLDL-TG during fasting. The fractional contribution was highest in the diabetic HPTG group (12%). As dietary energy and fat intakes were similar in HPTG and diabetic HPTG groups, the higher fractional contribution observed in the diabetic HPTG group is probably not due to the influence of recent diet. Another novel finding here was that dietary-derived NEFA can persist in the circulation for a long time after a meal. We demonstrated the entry of dietary FA into the NEFA pool soon after ingestion of a meal, as shown by appearance of [ 2 H 35 ]- stearate in plasma FFA. On day 1, 2-4 hour after the last meal, dietary stearate constituted 7-17% of NEFA and on day 2, dietary fats accounted for 9-21% of the plasma NEFA pool. These results are compatible with recent reports[17], [18], [57], [58]. Roust et al [17], showed that meal FA rapidly appear in plasma NEFA and up to 33% of meal triglyceride FA entered the plasma NEFA pool. Frayn et al [18], have also shown that FA generated by the action of LPL on circulating TG are released directly into venous plasma. The persistence of [ 2 H 35 ]- stearate in plasma well into the fasted state in our study (Fig 7) also indicates that dietary FA are extensively recycled.. DNL peaked twice during the lead-in period, first at midnight of day 1 then at midnight of day 2. The peak value at midnight 2 appeared to represent a plateau or MH0507ch2 26
27 near-plateau in all the three groups. The results observed here with [ 2 H 31 ]-palmitate prelabeling were similar, with apparent plateau values not approached until at least 30 hours of infusion. In a previous study, Hudgins et al [29] observed that DNL in plasma VLDL-TG after the second evening was higher than after first evening, but that no further increases in DNL occurred after the third evening (63 hour of 13 C 1 - acetate infusion). Donnelly et al. (46) also reported that plateau values are reached for DNL in VLDL-TG after 1-2 days. Continued unaccounted input may still exist after that time, however (Table 2), even after an apparent plateau was reached. This may reflect persistent diluting sources (e.g., visceral NEFA input) or lower turnover of a subfraction of the hepatic TG pool (e.g., PL-FA or a slow-turnover TG sub-compartment). It is also possible that a subpopulation of plasma VLDL-TG that does not turnover is present, as a source of label dilution, although turnover of VLDL-TG was nearly complete during fasting. Taking these findings together, one can speculate that plateau labeling of the hepatic TG pool requires an infusion of at least hours, which should include 2 evening feeding periods, but that unlabeled TG may still be present. Higher fractional DNL values in HPTG and diabetic HPTG groups in this study are compatible with previous reports wherein DNL was elevated in obesity and in insulin resistant states [25, 59, 60]. Higher DNL in HPTG and diabetic HPTG groups may be explained by high levels of insulin [61]. Fractional DNL was, however, highly variable within the diabetic HPTG and the non-diabetic HPTG groups. Highly variable fractional DNL in the setting of carbohydrate induced HPTG was also found by Hudgins et al [29]. The metabolic or genetic basis for this inter-individual variability will be worth exploring in future studies. MH0507ch2 27
28 These findings provide an integrated accounting of the metabolic sources of FA in the liver that contribute to fasting VLDL-TG. The summed contributions from plasma NEFA, diet and DNL to fasting VLDL-TG FA were 83±19%, 68±11% and 113±4%, leaving 17±19%, 32±11% and <0% FA unaccounted for, in the control, non-diabetic HPTG and diabetic HPTG groups, respectively. These findings may be explicable based on the known actions of insulin on lipid metabolism. Insulin is well established to inhibit fasting VLDL production by the liver acutely in humans [12, 14, 62, 63]. This effect appears to be independent of NEFA suppression induced by hyperinsulinemia [14]. In experimental systems, insulin promotes synthesis of TG by the liver but prevents its secretion, by preferentially partitioning newly synthesized TG into the intracellular storage pool [61]. FA released by hepatic lysosomal lipolysis of cytosolic TG [64] appear to contribute to VLDL-TG [37]. It is possible that lipolysis in the hepatocyte is inhibited by insulin, leading to suppression of TG secretion [64]. Insulin also impairs the association of apolipoprotein B (apo B) with TG [65] and causes a reduction in the translational activity of apo B mrna in HepG2 cells [66] while stimulating degradation of newly synthesized apo B [67]. Severely insulin-resistant states like type 2 diabetes may be characterized by resistance to the acute inhibitory effect of insulin on VLDL production [12, 62]. One might speculate that, as human subjects undergo transition from obesity associated HPTG states to frank diabetes with HPTG, there is a progressive loss of sensitivity to this action of insulin on hepatocytes and a reduced hepatic TG pool size. The higher insulin concentrations in the diabetic HPTG group may have been in part contributed by their drug therapy. Whether or not higher insulin levels are due to MH0507ch2 28
29 pharmacotherapy should not change the physiologic actions or impact, however. We considered discontinuing anti-hyperglycemic therapy in the diabetics, but concluded that this would introduce greater uncertainty if cessation was for less than several weeks (due to the possible non-steady-state, as glycemia and lipids deteriorated) and would certainly not be in the patients interest if continued for many weeks. We specifically excluded metformin and thiazolidinedione treatments, since these agents may have direct actions independent of insulin, and might thereby have introduced confounding effects. Moreover, untreated dyslipidemic diabetics are not as relevant to clinical diabetic dyslipidemia, for which the most relevant clinical context is when it persists in the face of standard anti-hyperglycemic therapy. The explanation for a total contribution somewhat >100% in diabetic HPTG is also uncertain. Perhaps the fact that dietary stearate input was added to endogenous palmitate inputs could have contributed to this result (i.e., if their relative oxidation vs incorporation rates are not identical) or it may reflect small systematic errors. The possible impact of potential complicating factors on our model can be estimated. Measurement of circulating NEFA enrichments corrects for recycling of label via adipose tissue or lipoprotein TG. Admixture of portal and systemic blood flow makes the true precursor pool enrichment for hepatic uptake of plasma NEFA complex, but dilution by portal/visceral FA appears in the model as unaccounted input. For the other input sources, the true precursor pool enrichment is known (DNL by MIDA and diet directly). Finally, differential oxidation of stearate and palmitate could influence the additivity of dietary input with other sources, but the dietary contribution was relatively small. Thus, the impact of these factors is not known, but is unlikely to be quantitatively significant. MH0507ch2 29
30 In summary, this study represents a first survey of many pathways in three populations of subjects. The analytic intensity of this protocol (monitoring up to 4 tracers in plasma and VLDL every 2 hours for 42 hours) limited the number of subjects that could be studied here. Even with six subjects per group, however, statistically significant results were observed. Future investigations can focus on specific pathways or subject groups, building on the results reported here. Differences between diabetic and nondiabetic HPTG for contributions from diet and NEFA or for turnover time required to fully label the delayed pool, for example, may be of particular interest. MH0507ch2 30
31 Acknowledgments The authors thank the nursing staff of GCRC at San Francisco General Hospital for their help, Doris Dare and Laurie Herraiz for diet planning and Dr. Mark Hudes for statistical analysis. This work was funded by research grant # from the American Diabetes Association (to MKH). MH0507ch2 31
32 Figure Legends Figure 1: Metabolic sources contributing FA to VLDL-TG. The figure shows a simplified model of VLDL-TG synthesis and secretion in the liver. TG may be assembled from FA derived from plasma NEFA, chylomicron remnants or DNL pathways and then either secreted into the circulation as VLDL-TG, via the immediate secretory pathway, or stored in the cytosol and secreted after a delay, via the delayed secretory pathway. Dashed arrows indicate recycling of VLDL-TG FA via the plasma NEFA pool into the liver. FA, fatty acids; VLDL-TG, very low density lipoprotein-triglyceride; NEFA, non-esterified fatty acids; Apo B, apolipoprotein B; DNL, de novo lipogenesis. Figure 2: Metabolic infusion protocol, the 30-hour lead-in and the subsequent 12-hour labeling periods are shown. CHO, carbohydrate. Figure 3: Plasma TG concentrations during the study period. Black diamond = Control group, White square = HPTG group, Black triangle = Diabetic HPTG group. TG, triglyceride. Figure 4: [1,2,3,4-13 C 4 ]-palmitate incorporation in VLDL-TG during the 12-hour followup fasting period. Black diamond = Control group, White square = HPTG group, Black triangle = Diabetic HPTG group. VLDL-TG, very low density lipoproteintriglyceride. Figure 5: [ 2 H 31 ]-palmitate enrichment (%) in the plasma NEFA pool during the 30-hour lead-in and 12-hour follow-up period. Arrow indicates the end of the lead-in period on midnight of day 2. Black diamond = Control group, White square = HPTG group, Black triangle = Diabetic HPTG group. MH0507ch2 32
ASSUMPTIONS AND DETAILS OF CALCULATIONS FOR FATTY ACID KINETICS
 1 1 1 1 1 1 0 1 ASSUMPTIONS AND DETAILS OF CALCULATIONS FOR FATTY ACID KINETICS Our hypothesis was that many sources of palmitate (NEFA, lipogenesis, diet) could contribute to newly-synthesized VLDL-TG
1 1 1 1 1 1 0 1 ASSUMPTIONS AND DETAILS OF CALCULATIONS FOR FATTY ACID KINETICS Our hypothesis was that many sources of palmitate (NEFA, lipogenesis, diet) could contribute to newly-synthesized VLDL-TG
Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences
 Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
The art of tracing dietary fat in humans. Leanne Hodson
 The art of tracing dietary fat in humans Leanne Hodson Dietary fat Other lipoproteins: IDL, LDL, HDL Hodson and Fielding linical Lipidology (2010) Relationship between blood & dietary fatty acids Typically:
The art of tracing dietary fat in humans Leanne Hodson Dietary fat Other lipoproteins: IDL, LDL, HDL Hodson and Fielding linical Lipidology (2010) Relationship between blood & dietary fatty acids Typically:
Chapter (5) Etiology of Low HDL- Cholesterol
 Chapter (5) Etiology of Low HDL- Cholesterol The aim of this chapter is to summarize the different etiological factors mainly the role of life-style and different disease conditions contributing to the
Chapter (5) Etiology of Low HDL- Cholesterol The aim of this chapter is to summarize the different etiological factors mainly the role of life-style and different disease conditions contributing to the
Plasma lipoproteins & atherosclerosis by. Prof.Dr. Maha M. Sallam
 Biochemistry Department Plasma lipoproteins & atherosclerosis by Prof.Dr. Maha M. Sallam 1 1. Recognize structures,types and role of lipoproteins in blood (Chylomicrons, VLDL, LDL and HDL). 2. Explain
Biochemistry Department Plasma lipoproteins & atherosclerosis by Prof.Dr. Maha M. Sallam 1 1. Recognize structures,types and role of lipoproteins in blood (Chylomicrons, VLDL, LDL and HDL). 2. Explain
Lipids digestion and absorption, Biochemistry II
 Lipids digestion and absorption, blood plasma lipids, lipoproteins Biochemistry II Lecture 1 2008 (J.S.) Triacylglycerols (as well as free fatty acids and both free and esterified cholesterol) are very
Lipids digestion and absorption, blood plasma lipids, lipoproteins Biochemistry II Lecture 1 2008 (J.S.) Triacylglycerols (as well as free fatty acids and both free and esterified cholesterol) are very
Unit IV Problem 3 Biochemistry: Cholesterol Metabolism and Lipoproteins
 Unit IV Problem 3 Biochemistry: Cholesterol Metabolism and Lipoproteins - Cholesterol: It is a sterol which is found in all eukaryotic cells and contains an oxygen (as a hydroxyl group OH) on Carbon number
Unit IV Problem 3 Biochemistry: Cholesterol Metabolism and Lipoproteins - Cholesterol: It is a sterol which is found in all eukaryotic cells and contains an oxygen (as a hydroxyl group OH) on Carbon number
Pathophysiology of Lipid Disorders
 Pathophysiology of Lipid Disorders Henry Ginsberg, M.D. Division of Preventive Medicine and Nutrition CHD in the United States CHD is the single largest killer of men and women 12 million have history
Pathophysiology of Lipid Disorders Henry Ginsberg, M.D. Division of Preventive Medicine and Nutrition CHD in the United States CHD is the single largest killer of men and women 12 million have history
Metabolic defects underlying dyslipidemia in abdominal obesity
 Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
Metabolic defects underlying dyslipidemia in abdominal obesity Professor Marja-Riitta Taskinen Department of Medicine, Division of Cardiology Helsinki University Hospital, Finland Disclosures: Honorariums/
1Why lipids cannot be transported in blood alone? 2How we transport Fatty acids and steroid hormones?
 1Why lipids cannot be transported in blood alone? 2How we transport Fatty acids and steroid hormones? 3How are dietary lipids transported? 4How lipids synthesized in the liver are transported? 5 Lipoprotien
1Why lipids cannot be transported in blood alone? 2How we transport Fatty acids and steroid hormones? 3How are dietary lipids transported? 4How lipids synthesized in the liver are transported? 5 Lipoprotien
Sources of fatty acids stored in liver and secreted via lipoproteins in patients with nonalcoholic fatty liver disease
 Related Commentary, page 1139 Research article Sources of fatty acids stored in liver and secreted via lipoproteins in patients with nonalcoholic fatty liver disease Kerry L. Donnelly, 1 Coleman I. Smith,
Related Commentary, page 1139 Research article Sources of fatty acids stored in liver and secreted via lipoproteins in patients with nonalcoholic fatty liver disease Kerry L. Donnelly, 1 Coleman I. Smith,
Quantification of menstrual and diurnal periodicities in rates of cholesterol and fat synthesis in humans
 Quantification of menstrual and diurnal periodicities in rates of cholesterol and fat synthesis in humans D. Faix, R. Neese, C. Kletke, S. Wolden,t D. Cesar, M. Coutlangus, C. H. L. Shackleton, and M.
Quantification of menstrual and diurnal periodicities in rates of cholesterol and fat synthesis in humans D. Faix, R. Neese, C. Kletke, S. Wolden,t D. Cesar, M. Coutlangus, C. H. L. Shackleton, and M.
High density lipoprotein metabolism
 High density lipoprotein metabolism Lipoprotein classes and atherosclerosis Chylomicrons, VLDL, and their catabolic remnants Pro-atherogenic LDL HDL Anti-atherogenic Plasma lipid transport Liver VLDL FC
High density lipoprotein metabolism Lipoprotein classes and atherosclerosis Chylomicrons, VLDL, and their catabolic remnants Pro-atherogenic LDL HDL Anti-atherogenic Plasma lipid transport Liver VLDL FC
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM Lipoprotein Metabolism
 ANSC/NUTR 618 LIPIDS & LIPID METABOLISM Lipoprotein Metabolism I. Chylomicrons (exogenous pathway) A. 83% triacylglycerol, 2% protein, 8% cholesterol plus cholesterol esters, 7% phospholipid (esp. phosphatidylcholine)
ANSC/NUTR 618 LIPIDS & LIPID METABOLISM Lipoprotein Metabolism I. Chylomicrons (exogenous pathway) A. 83% triacylglycerol, 2% protein, 8% cholesterol plus cholesterol esters, 7% phospholipid (esp. phosphatidylcholine)
Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats
 J. Biosci., Vol. 12, Number 2, June 1987, pp. 137 142. Printed in India. Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats P. VALSALA and P. A. KURUP Department
J. Biosci., Vol. 12, Number 2, June 1987, pp. 137 142. Printed in India. Investigations on the mechanism of hypercholesterolemia observed in copper deficiency in rats P. VALSALA and P. A. KURUP Department
Postprandial de novo lipogenesis and metabolic changes induced by a high-carbohydrate, low-fat meal in lean and overweight men 1 3
 Postprandial de novo lipogenesis and metabolic changes induced by a high-carbohydrate, low-fat meal in lean and overweight men 1 3 Iva Marques-Lopes, Diana Ansorena, Iciar Astiasaran, Luis Forga, and J
Postprandial de novo lipogenesis and metabolic changes induced by a high-carbohydrate, low-fat meal in lean and overweight men 1 3 Iva Marques-Lopes, Diana Ansorena, Iciar Astiasaran, Luis Forga, and J
AN OVERVIEW OF FATTY ACID ETHYL ESTERS
 AN OVERVIEW OF FATTY ACID ETHYL ESTERS Michael Laposata, M.D., Ph.D. Director of Clinical Laboratories Massachusetts General Hospital Professor, Harvard Medical School OUTLINE OF PRESENTATION Background
AN OVERVIEW OF FATTY ACID ETHYL ESTERS Michael Laposata, M.D., Ph.D. Director of Clinical Laboratories Massachusetts General Hospital Professor, Harvard Medical School OUTLINE OF PRESENTATION Background
Fig. S1. REGN1500 reduces plasma levels of cholesterol, TG and NEFA in WT and Ldlr -/- mice. (A) WT
 Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL
 Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
Behind LDL: The Metabolism of ApoB, the Essential Apolipoprotein in LDL and VLDL Sung-Joon Lee, PhD Division of Food Science Institute of Biomedical Science and Safety Korea University Composition of Lipoproteins:
"Fatty acid dysregulation in NAFLD" Studying the fasting to fed state transition. Outline
 "Fatty acid dysregulation in NAFLD" STOPNASH Symposium on the Origins and Pathways of Nonalcoholic Steatohepatitis October 7, 25 Elizabeth J Parks, PhD, FAHA Division of Gastroenterology/Hepatology Department
"Fatty acid dysregulation in NAFLD" STOPNASH Symposium on the Origins and Pathways of Nonalcoholic Steatohepatitis October 7, 25 Elizabeth J Parks, PhD, FAHA Division of Gastroenterology/Hepatology Department
Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry
 Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry Learning Objectives 1. Define lipoproteins and explain the rationale of their formation in blood. 2. List different
Lipoproteins Metabolism Reference: Campbell Biochemistry and Lippincott s Biochemistry Learning Objectives 1. Define lipoproteins and explain the rationale of their formation in blood. 2. List different
CHM333 LECTURE 34: 11/30 12/2/09 FALL 2009 Professor Christine Hrycyna
 Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Lipid Metabolism β-oxidation FA Acetyl-CoA Triacylglycerols (TAGs) and glycogen are the two major forms of stored energy in vertebrates Glycogen can supply ATP for muscle contraction for less than an hour
Niacin Metabolism: Effects on Cholesterol
 Niacin Metabolism: Effects on Cholesterol By Julianne R. Edwards For Dr. William R. Proulx, PhD, RD Associate Professor of Nutrition and Dietetics In partial fulfillments for the requirements of NUTR342
Niacin Metabolism: Effects on Cholesterol By Julianne R. Edwards For Dr. William R. Proulx, PhD, RD Associate Professor of Nutrition and Dietetics In partial fulfillments for the requirements of NUTR342
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Lipolysis and fatty acid metabolism in men and women during the postexercise recovery period
 J Physiol 84.3 (27) pp 963 981 963 Lipolysis and fatty acid metabolism in men and women during the post recovery period Gregory C. Henderson, Jill A. Fattor, Michael A. Horning, Nastaran Faghihnia, Matthew
J Physiol 84.3 (27) pp 963 981 963 Lipolysis and fatty acid metabolism in men and women during the post recovery period Gregory C. Henderson, Jill A. Fattor, Michael A. Horning, Nastaran Faghihnia, Matthew
LIPID METABOLISM. Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI
 LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
LIPID METABOLISM Sri Widia A Jusman Department of Biochemistry & Molecular Biology FMUI Lipid metabolism is concerned mainly with fatty acids cholesterol Source of fatty acids from dietary fat de novo
DEVELOPMENT OF A METHOD TO MEASURE VLDL SYNTHESIS RATES
 DEVELOPMENT OF A METHOD TO MEASURE VLDL SYNTHESIS RATES WRITTEN BY DEWI VAN HARSKAMP MASTER THESIS SUPERVISORS: M. T. ACKERMANS (SLVE, AMC) AND W. TH. KOK (HIMS, UVA) JUNE 10, 2011 1. ABSTRACT Obesity
DEVELOPMENT OF A METHOD TO MEASURE VLDL SYNTHESIS RATES WRITTEN BY DEWI VAN HARSKAMP MASTER THESIS SUPERVISORS: M. T. ACKERMANS (SLVE, AMC) AND W. TH. KOK (HIMS, UVA) JUNE 10, 2011 1. ABSTRACT Obesity
Cholesterol metabolism. Function Biosynthesis Transport in the organism Hypercholesterolemia
 Cholesterol metabolism Function Biosynthesis Transport in the organism Hypercholesterolemia - component of all cell membranes - precursor of bile acids steroid hormones vitamin D Cholesterol Sources: dietary
Cholesterol metabolism Function Biosynthesis Transport in the organism Hypercholesterolemia - component of all cell membranes - precursor of bile acids steroid hormones vitamin D Cholesterol Sources: dietary
Currently, the most effective established insulinreplacement
 The Effect of Systemic Versus Portal Insulin Delivery in Pancreas Transplantation on Insulin Action and VLDL Metabolism André Carpentier, 1 Bruce W. Patterson, 4 Kristine D. Uffelman, 1 Adria Giacca, 1,2
The Effect of Systemic Versus Portal Insulin Delivery in Pancreas Transplantation on Insulin Action and VLDL Metabolism André Carpentier, 1 Bruce W. Patterson, 4 Kristine D. Uffelman, 1 Adria Giacca, 1,2
How do we retain emphasis on function?
 Systems Biology Systems biology studies biological systems by systematically perturbing them (biologically, genetically, or chemically); monitoring the gene, protein, and informational pathway responses;
Systems Biology Systems biology studies biological systems by systematically perturbing them (biologically, genetically, or chemically); monitoring the gene, protein, and informational pathway responses;
13/09/2012. Dietary fatty acids. Triglyceride. Phospholipids:
 CARDIOVASCULAR DISEASES (CVD) and NUTRITION Major cause of morbidity & mortality in Canada & other developed countries e.g., majority of approved health claims on food labels relate to lowering CVD Relation
CARDIOVASCULAR DISEASES (CVD) and NUTRITION Major cause of morbidity & mortality in Canada & other developed countries e.g., majority of approved health claims on food labels relate to lowering CVD Relation
Intermediary metabolism. Eva Samcová
 Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
STUDY OVERVIEW KEY TAKEAWAYS
 Avocado fruit on postprandial markers of cardio-metabolic risk: A randomized controlled dose response trial in overweight and obese men and women Britt Burton-Freeman, Eunyoung Park, Indika Edirisinghe
Avocado fruit on postprandial markers of cardio-metabolic risk: A randomized controlled dose response trial in overweight and obese men and women Britt Burton-Freeman, Eunyoung Park, Indika Edirisinghe
Lipoproteins Metabolism
 Lipoproteins Metabolism LEARNING OBJECTIVES By the end of this Lecture, the student should be able to describe: What are Lipoproteins? Describe Lipoprotein Particles. Composition of Lipoproteins. The chemical
Lipoproteins Metabolism LEARNING OBJECTIVES By the end of this Lecture, the student should be able to describe: What are Lipoproteins? Describe Lipoprotein Particles. Composition of Lipoproteins. The chemical
ESPEN Congress Madrid 2018
 ESPEN Congress Madrid 2018 Dysglycaemia In Acute Patients With Nutritional Therapy Mechanisms And Consequences Of Dysglycaemia In Patients Receiving Nutritional Therapy M. León- Sanz (ES) Mechanisms and
ESPEN Congress Madrid 2018 Dysglycaemia In Acute Patients With Nutritional Therapy Mechanisms And Consequences Of Dysglycaemia In Patients Receiving Nutritional Therapy M. León- Sanz (ES) Mechanisms and
The Role of LCPUFA in Obesity. M.Tom Clandinin. The Alberta Institute for Human Nutrition The University of Alberta Edmonton, Alberta, Canada
 The Role of LCPUFA in Obesity by M.Tom Clandinin The Alberta Institute for Human Nutrition The University of Alberta Edmonton, Alberta, Canada How big is the Conceptual Problem? Some assumptions: 150lb
The Role of LCPUFA in Obesity by M.Tom Clandinin The Alberta Institute for Human Nutrition The University of Alberta Edmonton, Alberta, Canada How big is the Conceptual Problem? Some assumptions: 150lb
Blood fatty acids understanding the relevance of different tissue fractions and interpreting circulating concentrations.
 Blood fatty acids understanding the relevance of different tissue fractions and interpreting circulating concentrations Leanne Hodson Fatty acid composition as a biomarker of intake Complements dietary
Blood fatty acids understanding the relevance of different tissue fractions and interpreting circulating concentrations Leanne Hodson Fatty acid composition as a biomarker of intake Complements dietary
Chapter VIII: Dr. Sameh Sarray Hlaoui
 Chapter VIII: Dr. Sameh Sarray Hlaoui Lipoproteins a Lipids are insoluble in plasma. In order to be transported they are combined with specific proteins to form lipoproteins: Clusters of proteins and lipids.
Chapter VIII: Dr. Sameh Sarray Hlaoui Lipoproteins a Lipids are insoluble in plasma. In order to be transported they are combined with specific proteins to form lipoproteins: Clusters of proteins and lipids.
Metabolic integration and Regulation
 Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Food Intake Regulation & the Clock. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD
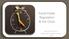 Food Intake Regulation & the Clock Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Circadian disruption affect multiple organ systems: The diagram provides examples of how circadian disruption
Food Intake Regulation & the Clock Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD Circadian disruption affect multiple organ systems: The diagram provides examples of how circadian disruption
Lipid Metabolism Prof. Dr. rer physiol. Dr.h.c. Ulrike Beisiegel
 Lipid Metabolism Department of Biochemistry and Molecular Biology II Medical Center Hamburg-ppendorf 1 Lipids. visceral fat. nutritional lipids 0 1.5 3 4.5 9 h. serum lipids. lipid accumulation in the
Lipid Metabolism Department of Biochemistry and Molecular Biology II Medical Center Hamburg-ppendorf 1 Lipids. visceral fat. nutritional lipids 0 1.5 3 4.5 9 h. serum lipids. lipid accumulation in the
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21953 holds various files of this Leiden University dissertation. Author: Schalkwijk, Daniël Bernardus van Title: Computational modeling of lipoprotein
Cover Page The handle http://hdl.handle.net/1887/21953 holds various files of this Leiden University dissertation. Author: Schalkwijk, Daniël Bernardus van Title: Computational modeling of lipoprotein
Hypertriglyceridemia. Ara Metjian, M.D. Resident s Report 20 December 2002
 Hypertriglyceridemia Ara Metjian, M.D. Resident s Report 20 December 2002 Review of Lipids Chylomicrons (CM): Dietary lipids absorbed through the GI tract are assembled intracellularly into CM. Very Low
Hypertriglyceridemia Ara Metjian, M.D. Resident s Report 20 December 2002 Review of Lipids Chylomicrons (CM): Dietary lipids absorbed through the GI tract are assembled intracellularly into CM. Very Low
PLASMA LIPOPROTEINS AND LIPIDS DETERMINATION OF PLASMA CHOLESTEROL AND TRIGLICERIDE LEVEL
 PLASMA LIPOPROTEINS AND LIPIDS DETERMINATION OF PLASMA CHOLESTEROL AND TRIGLICERIDE LEVEL Lipids are characterized by low polarity and limited solubility in water. Their plasma concentration is about 500-600
PLASMA LIPOPROTEINS AND LIPIDS DETERMINATION OF PLASMA CHOLESTEROL AND TRIGLICERIDE LEVEL Lipids are characterized by low polarity and limited solubility in water. Their plasma concentration is about 500-600
Determination of kinetic parameters of apolipoprotein B metabolism using amino acids labeled with stable isotopes
 Determination of kinetic parameters of apolipoprotein B metabolism using amino acids labeled with stable isotopes Klaus G. Parhofer, P. Hugh R. Barrett,t Dennis M. Bier,* and Gustav Schonfeld Division
Determination of kinetic parameters of apolipoprotein B metabolism using amino acids labeled with stable isotopes Klaus G. Parhofer, P. Hugh R. Barrett,t Dennis M. Bier,* and Gustav Schonfeld Division
Energy metabolism - the overview
 Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Plasma fibrinogen level, BMI and lipid profile in type 2 diabetes mellitus with hypertension
 World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Published by Atom and Cell Publishers All Rights Reserved Available online at: http://www.wjpsonline.org/ Original
World Journal of Pharmaceutical Sciences ISSN (Print): 2321-3310; ISSN (Online): 2321-3086 Published by Atom and Cell Publishers All Rights Reserved Available online at: http://www.wjpsonline.org/ Original
Dietary Lipid Utilization by Haddock (Melanogrammus aeglefinus)
 Dietary Lipid Utilization by Haddock (Melanogrammus aeglefinus) Santosh P. Lall & Dominic A. Nanton National Research Council of Canada Halifax, Canada vis, California ne 23, 2003 Body Components of Wild
Dietary Lipid Utilization by Haddock (Melanogrammus aeglefinus) Santosh P. Lall & Dominic A. Nanton National Research Council of Canada Halifax, Canada vis, California ne 23, 2003 Body Components of Wild
Interactions of exercise and diet in health prevention
 Interactions of exercise and diet in health prevention Dr Jason Gill Institute of Cardiovascular and Medical Sciences University of Glasgow Physical activity and health outcomes does one size fit all?
Interactions of exercise and diet in health prevention Dr Jason Gill Institute of Cardiovascular and Medical Sciences University of Glasgow Physical activity and health outcomes does one size fit all?
CHAPTER FORTY FIVE ENDOGENOUS LIPID TRANSPORT PATHWAY: VLDL AND IDL
 CHAPTER FORTY FIVE ENDOGENOUS LIPID TRANSPORT PATHWAY: VLDL AND IDL You will notice that the endogenous pathway is very similar to the exogenous pathway What is the average daily amount of triacylglycerol
CHAPTER FORTY FIVE ENDOGENOUS LIPID TRANSPORT PATHWAY: VLDL AND IDL You will notice that the endogenous pathway is very similar to the exogenous pathway What is the average daily amount of triacylglycerol
Recent Advances in Liver Triacylglycerol and Fatty Acid Metabolism Using Stable Isotope Labeling Techniques
 Recent Advances in Liver Triacylglycerol and Fatty Acid Metabolism Using Stable Isotope Labeling Techniques Elizabeth J. Parks and Marc K. Hellerstein Center for Human Nutrition, University of Texas Southwestern
Recent Advances in Liver Triacylglycerol and Fatty Acid Metabolism Using Stable Isotope Labeling Techniques Elizabeth J. Parks and Marc K. Hellerstein Center for Human Nutrition, University of Texas Southwestern
NEW METHODS FOR ASSESSING SUBSTRATE UTILIZATION IN HORSES DURING EXERCISE
 R. J. Geor 73 NEW METHODS FOR ASSESSING SUBSTRATE UTILIZATION IN HORSES DURING EXERCISE RAYMOND J. GEOR The Ohio State University, Columbus, Ohio There are two major goals in designing diets and feeding
R. J. Geor 73 NEW METHODS FOR ASSESSING SUBSTRATE UTILIZATION IN HORSES DURING EXERCISE RAYMOND J. GEOR The Ohio State University, Columbus, Ohio There are two major goals in designing diets and feeding
Lipid/Lipoprotein Structure and Metabolism (Overview)
 Lipid/Lipoprotein Structure and Metabolism (Overview) Philip Barter President, International Atherosclerosis Society Centre for Vascular Research University of New South Wales Sydney, Australia Disclosures
Lipid/Lipoprotein Structure and Metabolism (Overview) Philip Barter President, International Atherosclerosis Society Centre for Vascular Research University of New South Wales Sydney, Australia Disclosures
Whole Body Synthesis of Docosahexaenoic Acid from Alpha-Linolenic Acid in. Rodents
 Whole Body Synthesis of Docosahexaenoic Acid from Alpha-Linolenic Acid in Rodents By Anthony Frank Domenichiello A thesis submitted in conformity with the requirements for the degree of Doctor of Philosophy
Whole Body Synthesis of Docosahexaenoic Acid from Alpha-Linolenic Acid in Rodents By Anthony Frank Domenichiello A thesis submitted in conformity with the requirements for the degree of Doctor of Philosophy
SUPPLEMENTAL CHOLINE FOR PREVENTION AND ALLEVIATION OF FATTY LIVER IN DAIRY CATTLE
 SUPPLEMENTAL CHOLINE FOR PREVENTION AND ALLEVIATION OF FATTY LIVER IN DAIRY CATTLE Ric R. Grummer and Reinaldo Cooke Department of Dairy Science University of Wisconsin-Madison rgrummer@wisc.edu Fatty
SUPPLEMENTAL CHOLINE FOR PREVENTION AND ALLEVIATION OF FATTY LIVER IN DAIRY CATTLE Ric R. Grummer and Reinaldo Cooke Department of Dairy Science University of Wisconsin-Madison rgrummer@wisc.edu Fatty
ANTIHYPERLIPIDEMIA. Darmawan,dr.,M.Kes,Sp.PD
 ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
ANTIHYPERLIPIDEMIA Darmawan,dr.,M.Kes,Sp.PD Plasma lipids consist mostly of lipoproteins Spherical complexes of lipids and specific proteins (apolipoproteins). The clinically important lipoproteins, listed
3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.
![3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H. 3/20/2011. Body Mass Index (kg/[m 2 ]) Age at Issue (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Mokdad A.H.](/thumbs/82/84935173.jpg) U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
U.S. Adults: 1988 Nineteen states with 10-14% 14% Prevalence of Obesity (*BMI > 30, or ~ 30 lbs overweight for 5 4 woman) Metabolic John P. Cello, MD Professor of Medicine and Surgery, University of California,
Cardiovascular Complications of Diabetes
 VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
Free Glycerol Assay Kit (Colorimetric)
 Product Manual Free Glycerol Assay Kit (Colorimetric) Catalog Number STA-398 100 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Glycerol is the backbone of Triglycerides
Product Manual Free Glycerol Assay Kit (Colorimetric) Catalog Number STA-398 100 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Glycerol is the backbone of Triglycerides
Hypertriglyceridemia: Why, When, and How to Treat. Gregory Cohn, MD, FNLA, FASPC
 Hypertriglyceridemia: Why, When, and How to Treat Gregory Cohn, MD, FNLA, FASPC DISCLOSURES Consultant to Akcea Therapeutics (in the past 12 months). OUTLINE I. Lipoproteins II. Non-HDL-C III. Causes and
Hypertriglyceridemia: Why, When, and How to Treat Gregory Cohn, MD, FNLA, FASPC DISCLOSURES Consultant to Akcea Therapeutics (in the past 12 months). OUTLINE I. Lipoproteins II. Non-HDL-C III. Causes and
Effects of Short-term High-carbohydrate Feeding on. Hypercholesterolaemia*
 Archives of Disease in Childhood, 1970, 45, 393. Effects of Short-term High-carbohydrate Feeding on Serum Triglyceride of Children with Familial Hypercholesterolaemia* M. M. SEGALL, I. TAMIR, AUDREY S.
Archives of Disease in Childhood, 1970, 45, 393. Effects of Short-term High-carbohydrate Feeding on Serum Triglyceride of Children with Familial Hypercholesterolaemia* M. M. SEGALL, I. TAMIR, AUDREY S.
Cholesterol and its transport. Alice Skoumalová
 Cholesterol and its transport Alice Skoumalová 27 carbons Cholesterol - structure Cholesterol importance A stabilizing component of cell membranes A precursor of bile salts A precursor of steroid hormones
Cholesterol and its transport Alice Skoumalová 27 carbons Cholesterol - structure Cholesterol importance A stabilizing component of cell membranes A precursor of bile salts A precursor of steroid hormones
METABOLISM of ADIPOSE TISSUE
 METABOLISM of ADIPOSE TISSUE 2. LF UK Prof. Rudolf Poledne, PhD. TYPES OF ADIPOSE TISSUE brown adipose tissue subcutaneous adipose tissue visceral adipose tissue ADIPOSE TISSUE FUNCTIONS: thermal isolation
METABOLISM of ADIPOSE TISSUE 2. LF UK Prof. Rudolf Poledne, PhD. TYPES OF ADIPOSE TISSUE brown adipose tissue subcutaneous adipose tissue visceral adipose tissue ADIPOSE TISSUE FUNCTIONS: thermal isolation
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
Principles of Anatomy and Physiology 14 th Edition CHAPTER 25 Metabolism and Nutrition Metabolic Reactions Metabolism refers to all of the chemical reactions taking place in the body. Reactions that break
BCH 447. Triglyceride Determination in Serum
 BCH 447 Triglyceride Determination in Serum Introduction: Triglycerides are esters of fatty acids and are hydrolyzed by lipase to glycerol and free fatty acids. Triglyceride determinations when performed
BCH 447 Triglyceride Determination in Serum Introduction: Triglycerides are esters of fatty acids and are hydrolyzed by lipase to glycerol and free fatty acids. Triglyceride determinations when performed
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Triglyceride determination
 Triglyceride determination Introduction: - Triglycerides are esters of fatty acids and are hydrolyzed to glycerol and free fatty acids (by lipase) - Triglyceride determinations when performed in conjunction
Triglyceride determination Introduction: - Triglycerides are esters of fatty acids and are hydrolyzed to glycerol and free fatty acids (by lipase) - Triglyceride determinations when performed in conjunction
Metformin Hydrochloride
 Metformin Hydrochloride 500 mg, 850 mg, 500 mg LA and 750 mg LA Tablet Description Informet is a preparation of metformin hydrochloride that belongs to a biguanide class of oral antidiabetic drugs. Metformin
Metformin Hydrochloride 500 mg, 850 mg, 500 mg LA and 750 mg LA Tablet Description Informet is a preparation of metformin hydrochloride that belongs to a biguanide class of oral antidiabetic drugs. Metformin
Commentary. New mechanisms by which statins lower plasma cholesterol. Henri Brunengraber
 Commentary New mechanisms by which statins lower plasma cholesterol Henri Brunengraber Department of Nutrition Case Western Reserve University Cleveland, OH 44109 Phone: 216 368 6429 Fax: 216 368 6560
Commentary New mechanisms by which statins lower plasma cholesterol Henri Brunengraber Department of Nutrition Case Western Reserve University Cleveland, OH 44109 Phone: 216 368 6429 Fax: 216 368 6560
The New Gold Standard for Lipoprotein Analysis. Advanced Testing for Cardiovascular Risk
 The New Gold Standard for Lipoprotein Analysis Advanced Testing for Cardiovascular Risk Evolution of Lipoprotein Testing The Lipid Panel Total Cholesterol = VLDL + LDL + HDL Evolution of Lipoprotein Testing
The New Gold Standard for Lipoprotein Analysis Advanced Testing for Cardiovascular Risk Evolution of Lipoprotein Testing The Lipid Panel Total Cholesterol = VLDL + LDL + HDL Evolution of Lipoprotein Testing
SCHOOL OF HEALTH SCIENCES DIVISION OF DIETETICS, NUTRITION AND BIOLOGICAL SCIENCES, PHYSIOTHERAPY, PODIATRY, RADIOGRAPHY LEVEL 2 / DIET 1
 SCHOOL OF HEALTH SCIENCES DIVISION OF DIETETICS, NUTRITION AND BIOLOGICAL SCIENCES, PHYSIOTHERAPY, PODIATRY, RADIOGRAPHY LEVEL 2 / DIET 1 D2143/ Nutrition DATE: 28/04/2014 WRITING TIME: 120 minutes TIME:
SCHOOL OF HEALTH SCIENCES DIVISION OF DIETETICS, NUTRITION AND BIOLOGICAL SCIENCES, PHYSIOTHERAPY, PODIATRY, RADIOGRAPHY LEVEL 2 / DIET 1 D2143/ Nutrition DATE: 28/04/2014 WRITING TIME: 120 minutes TIME:
MILK BIOSYNTHESIS PART 3: FAT
 MILK BIOSYNTHESIS PART 3: FAT KEY ENZYMES (FROM ALL BIOSYNTHESIS LECTURES) FDPase = fructose diphosphatase Citrate lyase Isocitrate dehydrogenase Fatty acid synthetase Acetyl CoA carboxylase Fatty acyl
MILK BIOSYNTHESIS PART 3: FAT KEY ENZYMES (FROM ALL BIOSYNTHESIS LECTURES) FDPase = fructose diphosphatase Citrate lyase Isocitrate dehydrogenase Fatty acid synthetase Acetyl CoA carboxylase Fatty acyl
Fat Metabolism, Insulin and MTHFR
 Fat Metabolism, Insulin and MTHFR BCAA, SAMe and ACAT Carolyn Ledowsky Overview of This Presentation 1. Fat Metabolism and MTHFR 2. SAMe and Fat Metabolism 3. Acetyl Co A and Fat Metabolism 4. How to Maintain
Fat Metabolism, Insulin and MTHFR BCAA, SAMe and ACAT Carolyn Ledowsky Overview of This Presentation 1. Fat Metabolism and MTHFR 2. SAMe and Fat Metabolism 3. Acetyl Co A and Fat Metabolism 4. How to Maintain
Design and analysis of lipoprotein tracer kinetic studies in humans
 Design and analysis of lipoprotein tracer kinetic studies in humans P Hugh R Barrett, Dick C Chan and Gerald F Watts Metabolic Research Centre, School of Medicine and Pharmacology, University of Western
Design and analysis of lipoprotein tracer kinetic studies in humans P Hugh R Barrett, Dick C Chan and Gerald F Watts Metabolic Research Centre, School of Medicine and Pharmacology, University of Western
Nature Genetics: doi: /ng.3561
 Supplementary Figure 1 Pedigrees of families with APOB p.gln725* mutation and APOB p.gly1829glufs8 mutation (a,b) Pedigrees of families with APOB p.gln725* mutation. (c) Pedigree of family with APOB p.gly1829glufs8
Supplementary Figure 1 Pedigrees of families with APOB p.gln725* mutation and APOB p.gly1829glufs8 mutation (a,b) Pedigrees of families with APOB p.gln725* mutation. (c) Pedigree of family with APOB p.gly1829glufs8
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Glucose. Glucose. Insulin Action. Introduction to Hormonal Regulation of Fuel Metabolism
 Glucose Introduction to Hormonal Regulation of Fuel Metabolism Fasting level 3.5-5 mmol (1 mmol = 18 mg/dl) Postprandial 6-10 mmol Amount of glucose in circulation is dependent on: Absorption from the
Glucose Introduction to Hormonal Regulation of Fuel Metabolism Fasting level 3.5-5 mmol (1 mmol = 18 mg/dl) Postprandial 6-10 mmol Amount of glucose in circulation is dependent on: Absorption from the
History. Aron first proposed that fat may be essential for normal growth Tested on animals-vitamins A,D,E added. Fat deficiency severely affected
 Chapter 5 LIPIDS History 1918 Aron first proposed that fat may be essential for normal growth Tested on animals-vitamins A,D,E added Fat deficiency severely affected Bone growth Reproduction Called Vitamin
Chapter 5 LIPIDS History 1918 Aron first proposed that fat may be essential for normal growth Tested on animals-vitamins A,D,E added Fat deficiency severely affected Bone growth Reproduction Called Vitamin
André J. Tremblay, 1 Benoît Lamarche, 1 Jean-Charles Hogue, 1 and Patrick Couture 1,2. 1. Introduction. 2. Methods
 Diabetes Research Volume 2016, Article ID 2909210, 5 pages http://dx.doi.org/10.1155/2016/2909210 Clinical Study n-3 Polyunsaturated Fatty Acid Supplementation Has No Effect on Postprandial Triglyceride-Rich
Diabetes Research Volume 2016, Article ID 2909210, 5 pages http://dx.doi.org/10.1155/2016/2909210 Clinical Study n-3 Polyunsaturated Fatty Acid Supplementation Has No Effect on Postprandial Triglyceride-Rich
Throughout the day, the human liver responds to
 Original Article Increased Dietary Substrate Delivery Alters Hepatic Fatty Acid Recycling in Healthy Men Maureen T. Timlin, Brian R. Barrows, and Elizabeth J. Parks Sources of fatty acids flowing to the
Original Article Increased Dietary Substrate Delivery Alters Hepatic Fatty Acid Recycling in Healthy Men Maureen T. Timlin, Brian R. Barrows, and Elizabeth J. Parks Sources of fatty acids flowing to the
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
298 Biomed Environ Sci, 2015; 28(4):
 298 Biomed Environ Sci, 2015; 28(4): 298-302 Letter to the Editor Effects of Maternal Linseed Oil Supplementation on Metabolic Parameters in Cafeteria Diet-induced Obese Rats * BENAISSA Nawel 1, MERZOUK
298 Biomed Environ Sci, 2015; 28(4): 298-302 Letter to the Editor Effects of Maternal Linseed Oil Supplementation on Metabolic Parameters in Cafeteria Diet-induced Obese Rats * BENAISSA Nawel 1, MERZOUK
Responses of blood lipids to aerobic and resistance type of exercise
 Responses of blood lipids to aerobic and resistance type of exercise Labros Sidossis, Ph.D. Laboratory of Nutrition and Clinical Dietetics Harokopio University of Athens, Greece Triacylglycerol structure
Responses of blood lipids to aerobic and resistance type of exercise Labros Sidossis, Ph.D. Laboratory of Nutrition and Clinical Dietetics Harokopio University of Athens, Greece Triacylglycerol structure
3-Thia Fatty Acids A New Generation of Functional Lipids?
 Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
BIOL2171 ANU TCA CYCLE
 TCA CYCLE IMPORTANCE: Oxidation of 2C Acetyl Co-A 2CO 2 + 3NADH + FADH 2 (8e-s donated to O 2 in the ETC) + GTP (energy) + Heat OVERVIEW: Occurs In the mitochondrion matrix. 1. the acetyl portion of acetyl-coa
TCA CYCLE IMPORTANCE: Oxidation of 2C Acetyl Co-A 2CO 2 + 3NADH + FADH 2 (8e-s donated to O 2 in the ETC) + GTP (energy) + Heat OVERVIEW: Occurs In the mitochondrion matrix. 1. the acetyl portion of acetyl-coa
Automated Sample Preparation for Profiling Fatty Acids in Blood and Plasma using the Agilent 7693 ALS
 Automated Sample Preparation for Profiling Fatty Acids in Blood and Plasma using the Agilent 7693 ALS Application Note Clinical Research Authors Frank David and Bart Tienpont, Research Institute for Chromatography,
Automated Sample Preparation for Profiling Fatty Acids in Blood and Plasma using the Agilent 7693 ALS Application Note Clinical Research Authors Frank David and Bart Tienpont, Research Institute for Chromatography,
Bachelorarbeit Fructose and weight gain
 Bachelorarbeit Fructose and weight gain Bogner-Strauß, Juliane Gertrude, Assoc.Prof. Mag.rer.nat. Dr.rer.nat. Von Johanna Maria Ticar Mat: 0730208 Graz, 27.07.2011 Abstract The prevalence of obesity is
Bachelorarbeit Fructose and weight gain Bogner-Strauß, Juliane Gertrude, Assoc.Prof. Mag.rer.nat. Dr.rer.nat. Von Johanna Maria Ticar Mat: 0730208 Graz, 27.07.2011 Abstract The prevalence of obesity is
 Glossary For TheFatNurse s For All Ages Series Apolipoprotein B (APOB or ApoB) are the primary apolipoproteins of chylomicrons and low-density lipoproteins (LDL - known commonly by the misnomer "bad cholesterol"
Glossary For TheFatNurse s For All Ages Series Apolipoprotein B (APOB or ApoB) are the primary apolipoproteins of chylomicrons and low-density lipoproteins (LDL - known commonly by the misnomer "bad cholesterol"
Upper-body obesity, especially when associated. Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women
 BRIEF REPORT Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women Esben Søndergaard, 1 Birgitte Nellemann, 1 Lars P. Sørensen, 1 Lars C. Gormsen, 2 Jens S. Christiansen, 1 Erik
BRIEF REPORT Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women Esben Søndergaard, 1 Birgitte Nellemann, 1 Lars P. Sørensen, 1 Lars C. Gormsen, 2 Jens S. Christiansen, 1 Erik
Menopausal Status and Abdominal Obesity Are Significant Determinants of Hepatic Lipid Metabolism in Women
 Menopausal Status and Abdominal Obesity Are Significant Determinants of Hepatic Lipid Metabolism in Women Leanne Hodson, PhD; Rajarshi Banerjee, DPhil; Belen Rial, PhD; Wiebke Arlt, MD, DSc; Martin Adiels,
Menopausal Status and Abdominal Obesity Are Significant Determinants of Hepatic Lipid Metabolism in Women Leanne Hodson, PhD; Rajarshi Banerjee, DPhil; Belen Rial, PhD; Wiebke Arlt, MD, DSc; Martin Adiels,
Index. Page references in bold refer to figures and page references in italic refer to tables.
 Page references in bold refer to figures and page references in italic refer to tables. Adrenaline, high-fat response in post-obese 142 Alcohol absorption 11-12 balance equation 17 and obesity 10-11 thermogenesis
Page references in bold refer to figures and page references in italic refer to tables. Adrenaline, high-fat response in post-obese 142 Alcohol absorption 11-12 balance equation 17 and obesity 10-11 thermogenesis
Upper-body obesity, especially when associated. Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women
 BRIEF REPORT Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women Esben Søndergaard, 1 Birgitte Nellemann, 1 Lars P. Sørensen, 1 Lars C. Gormsen, 2 Jens S. Christiansen, 1 Erik
BRIEF REPORT Similar VLDL-TG Storage in Visceral and Subcutaneous Fat in Obese and Lean Women Esben Søndergaard, 1 Birgitte Nellemann, 1 Lars P. Sørensen, 1 Lars C. Gormsen, 2 Jens S. Christiansen, 1 Erik
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption),
 Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in. obese subjects
 Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
review In vivo regulation of lipolysis in humans Simon W. Coppack, Michael D. Jensen, and John M. Miles
 I review In vivo regulation of lipolysis in humans Simon W. Coppack, Michael D. Jensen, and John M. Miles Endocrine Research Unit, Mayo Clinic, Rochester, M N 55905 and University College London Medical
I review In vivo regulation of lipolysis in humans Simon W. Coppack, Michael D. Jensen, and John M. Miles Endocrine Research Unit, Mayo Clinic, Rochester, M N 55905 and University College London Medical
Free Fatty Acid Assay Kit (Fluorometric)
 Product Manual Free Fatty Acid Assay Kit (Fluorometric) Catalog Number STA-619 100 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Triglycerides (TAG) are a type of lipid
Product Manual Free Fatty Acid Assay Kit (Fluorometric) Catalog Number STA-619 100 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Triglycerides (TAG) are a type of lipid
Figure S1. Comparison of fasting plasma lipoprotein levels between males (n=108) and females (n=130). Box plots represent the quartiles distribution
 Figure S1. Comparison of fasting plasma lipoprotein levels between males (n=108) and females (n=130). Box plots represent the quartiles distribution of A: total cholesterol (TC); B: low-density lipoprotein
Figure S1. Comparison of fasting plasma lipoprotein levels between males (n=108) and females (n=130). Box plots represent the quartiles distribution of A: total cholesterol (TC); B: low-density lipoprotein
2.5% of all deaths globally each year. 7th leading cause of death by % of people with diabetes live in low and middle income countries
 Lipid Disorders in Diabetes (Diabetic Dyslipidemia) Khosrow Adeli PhD, FCACB, DABCC Head and Professor, Clinical Biochemistry, The Hospital for Sick Children, University it of Toronto Diabetes A Global
Lipid Disorders in Diabetes (Diabetic Dyslipidemia) Khosrow Adeli PhD, FCACB, DABCC Head and Professor, Clinical Biochemistry, The Hospital for Sick Children, University it of Toronto Diabetes A Global
