14RC1-PERRUCHOUD Interventional management of cancer pain
|
|
|
- Dayna Atkinson
- 5 years ago
- Views:
Transcription
1 14RC1-PERRUCHOUD Interventional management of cancer pain Christophe Perruchoud Department of Anaesthesiology and Pain Management, University Hospital Centre and University of Lausanne, Lausanne Background The prevalence of pain amongst cancer patients varies between 30 and 50% and rises to more than 80% of patients with end stage disease. 1 The pain is usually a mixture of nociceptive and neuropathic pain. Metastatic spread of cancer to bone is probably one of the most common causes of cancer pain. 2 Pressure on surrounding organs, stretching hollow viscera and distortion of the capsule of solid organs results in visceral pain, and infiltration of sensory nerves and plexuses causes neuropathic pain, representing important origins of pain. Cancer pain may also be related to adverse effects of anticancer treatment, including chemotherapy, radiotherapy, hormonal therapy or surgery. Opioid therapy remains the mainstay of cancer pain control and adherence to the WHO analgesic threestep ladder achieves pain relief in most patients. 3 However, about one third of cancer patients have inadequate pain relief, often due to unacceptable side-effects of opioids that limit dosage, especially in late stages of disease. 4 For this reason, the inclusion of a fourth step to the WHO analgesic ladder to include advanced interventional approaches has been proposed. However, earlier application of interventional pain management techniques can be recommended before even considering the use of strong opioids. About 20% of oncology patients may benefit from interventional procedures. 5 Interventional therapy ranges from less invasive techniques, such as reversible nerve blocks, to more invasive techniques such as implantable devices or irreversible nerve destruction. Interventional procedures can be divided into procedures affecting the spinal canal, intrathecal or epidural space or neuraxial techniques, and those targeting individual nerves or plexuses, called neurolytic techniques. Neuraxial techniques The main indication for intrathecal and epidural analgesics is failure of oral or transdermal analgesics despite suitable doses. Compared to the systemic administration of opioids, the central route, epidural or intrathecal, provides equal or better pain relief with lower doses and fewer adverse effects. Moreover it allows simultaneous administration of other analgesics, such as bupivacaine or clonidine. Epidural infusion Epidural infusion is a simple method for short-term, i.e. less than three months, use in patients with advanced cancer and difficult-to-control pain. A percutaneous or subcutaneous implantable port can be connected to the catheter. Patients are then discharged with portable infusion pumps. Percutaneous catheters may exit directly at the dorsal site or be tunnelled to the flank areas. The main indication for subcutaneous port implantation is a life expectancy greater than six weeks. The most frequently infused drugs are local anaesthetics, opioids and clonidine. Complications include urinary retention, superficial infections (4-40%), epidural abscess (1-15%) and catheter-related complications such as leakage, obstruction or dislodgment, requiring exchange or removal of the catheter in 15 % of patients. 6 A meta-analysis calculated an incidence of catheter-related infections of 0.4/1000 catheter days. 7 1/7
2 Intrathecal drug delivery Intrathecal (IT) drug administration can be achieved by using an external catheter, a subcutaneous access port or an implantable pump. External catheters and subcutaneous access ports are reserved for patients with short life expectancies. For long-term administration, a pump is implanted surgically in the subcutaneous abdominal tissue and acts as a drug reservoir and delivery mechanism. Although IT drug delivery systems may represent an effective option for pain management, not all patients are appropriate candidates for implants. Selection requires evaluation of comorbidities, psychosocial factors and life expectancy. A cost-effectiveness analysis has shown that implantable systems are better than external pumps if the patient has a life expectancy of at least three months. 8 An IT trial should be performed before surgical implantation to assess the efficacy and side-effects of the intended drug. The trial may be performed with a single injection, multiple injections or a continuous infusion. Prospective studies have shown that patients randomized to receive an intrathecal drug delivery system (IDDS) or who received it after failure of comprehensive medical management had reduced pain scores, significant relief of most pain, control of drug toxicities, and possibly improved survival, at least for the duration of the trial. 9,10 If monotherapy becomes insufficient and dose escalation is no longer safe, combinations of drugs may maintain effective pain relief. Many drugs, bupivacaine, ropivacaine, hydromorphone, fentanyl, sufentanil, buprenorphine, clonidine, and midazolam, are not licensed for IT use in the USA but are licensed in other countries. Consensus statements suggesting different algorithms for nociceptive or neuropathic pain have been developed to guide physicians. 11 Complications resulting from IT therapy are common and include hypotension, sedation, respiratory depression, inflammatory masses, infection and catheter-related complications, such as migration or leakage, and withdrawal syndrome. Excess mortality, especially in the first days after implantation, has been reported in non-cancer patients due to rapid opioid dose escalation in the absence of proper monitoring. Those observations could be translated to the cancer population. 12 Neurolytic techniques Neurolysis describes intentional injury to a nerve or group of nerves by chemical (absolute alcohol, glycerin or phenol), thermal (heat), surgical or cryogenic (freezing) methods to produce pain relief. Neurolytic agents predominantly affect neuronal axons, not cell bodies. Pain relief, therefore, is temporary secondary to axonal regeneration and neural plasticity. The effects of neurolytic therapy typically persist between 3 6 months, although the response may vary widely. Alcohol was the first agent used in 1902 to treat trigeminal neuralgia. 13 Alcohol usually induces a burning sensation in the region where it is injected. Pre-treatment with a local anaesthetic is recommended strongly. Phenol was then introduced in the 1950s and gained widespread popularity, in part because of its analgesic as well as neurolytic properties. Several sites are described for neurolytic block of sympathetically mediated pain associated with gastrointestinal and genitourinary cancers (Figure 1). Since the recent development of neurodestructive techniques such as cryoablation or radiofrequency, and advances in spinal analgesia with continuous infusion, indications for neurolytic blocks have significantly decreased. 2/7
3 Figure 1 : Possible sites for neurolytic block of sympathetically mediated pain according to tumour location. Coeliac plexus The coeliac plexus is a network of neuronal ganglia located underneath the diaphragmatic crus in the retroperitoneal space, at the level of the first lumbar vertebra. Structures immediately adjacent to the coeliac plexus include the coeliac artery and aorta. The coeliac ganglia contain pre- and post-ganglionic sympathetic efferent fibres, preganglionic parasympathetic fibres and visceral sensory afferent fibres. The role of coeliac plexus block to relieve intractable pain caused by upper abdominal malignancies, such as pancreas, liver and stomach, is well established. Several percutaneous techniques are described to access the coeliac plexus, including three posterior approaches, paravertebral, transdiscal and transaortic, and one anterior approach (Figure 2). Fluoroscopy or CT-scan may be used for all except the anterior approach, which requires CT scan or ultrasound guidance. Neurolytic block of the coeliac plexus can be associated with transient hypotension and diarrhoea from sympathetic block. The most serious complication is paraplegia, occurring in approximately 1% of cases, secondary to alcoholinduced vasospasm or mechanical injury to the artery of Adamkiewicz. A meta-analysis of the efficacy and safety of neurolytic coeliac plexus block showed long-lasting (i.e. greater than three months) benefit for 70%-90% of patients with pancreatic and other intra-abdominal cancers, regardless of the approach used. 14 3/7
4 Figure 2 : Percutaneous approaches for coeliac plexus block at L1 level. Splanchnic plexus The splanchnic nerve block is a useful alternative to paravertebral coeliac plexus block, especially in cases of pancreatic tumours. It targets the splanchnic nerves, branches of the thoracic truncus sympathicus and the nerve supply to the coeliac plexus. The needles are inserted paravertebrally, using a tunnel view, in the direction of the concave mid-portion of the D11 body until bony contact is made. Under lateral view, the needle is advanced to the anterolateral aspect of D11. The tip of the needle should be placed just within the contour of the D11 body in an anteroposterior view, just at the anterior border of the D11 vertebra in a lateral view. Before the neurolytic agent is injected, a small amount of contrast is injected to check dispersion along the anterolateral aspect of the vertebral body. Ganglion Impar (GI) The GI is a retroperitoneal structure usually positioned in the midline at the level of the sacrococcygeal junction. It represents the termination of the paravertebral sympathetic chains. It contains visceral afferent fibres that innervate the perineum, distal part of the rectum, anus, distal urethra, distal third of the vagina and vulva. Several approaches have been described to target the GI. All are performed under fluoroscopy. In the trans-sacrococcygeal approach, the needle is placed midline through the sacrococcygeal ligament into the retroperitoneal space. After proper spread of contrast medium, local anaesthetic or neurolytic agent is injected to ensure block of the GI. 4/7
5 Intrathecal neurolysis Intrathecal neurolysis involves the injection of very small amounts of neurolytic agents, 0.1 ml increments to a total of ml for treatment of one to two dermatomal levels, usually hyperbaric phenol (7-12%) or hypobaric alcohol (50-100%). The aim is to produce segmental sensory block, lasting from weeks to months, without affecting motor function. 15 This is possible because of the separation between sensory and motor fibres in the spinal cord. The dorsal roots carry sensory fibres and the ventral root carries motor and sympathetic fibres. Epidural neurolytic blocks can be used as an alternative approach to intrathecal block, but the degree of analgesia produced is usually less profound. Moreover, intrathecal injections offer greater control over drug spread due to their hypobaricity or hyperbaricity in the cerebrospinal fluid. Potential complications vary from weakness to complete paralysis of the lower limb muscles as well as rectal and bladder sphincter dysfunction. Usually performed at the lumbar level, called a saddle block, some case series describe thoracic and cervical intrathecal neurolysis. Vertebroplasty and Kyphoplasty Percutaneous vertebroplasty (PV) is a radiologically guided procedure in which surgical bone cement is injected into a vertebra under imaging guidance. The aim of PV is to provide pain relief and bone strengthening in painful compression fractures involving the vertebral body. This technique is widely used to treat osteoporotic vertebral fractures and can also be applied to treat fractures caused by metastatic disease. Selected patients should have focal, intense and intractable midline spinal pain at the level of, or within two vertebral levels below the fracture, without evidence of definite radicular signs and symptoms, in which conservative management has failed. 16 Complications are rare, but the main one is caused by cement leaking through cortical defects and causing epidural compression of the spinal cord or neural elements. Kyphoplasty is a modification of PV and involves a balloon being placed percutaneously into the vertebral body. Inflation and deflation of the balloon creates a cavity before the injection of cement. Conclusion Until recently, interventional procedures have been used mostly as a last resort in patients with cancer pain. Several recent publications and guidelines on the management of cancer pain have recommended the use of certain interventional techniques at an earlier stage, possibly even at the stage, where opioid treatment is first being considered. Reserving the use of these techniques until the last few days of life is certainly not a good idea. However, every procedure has its complications. Notwithstanding your best intention, always remember there is no situation, so bad, that you cannot make it worse. 5/7
6 Key Learning Points The prevalence of pain among cancer pain is high. About one third of patients suffer from insufficient pain relief. Early adoption of interventional pain procedures can be recommended before even considering the use of strong opioids. Commonly used interventional therapies for cancer pain include spinal administration of analgesics, neurolytic block and vertebroplasty. Proper patient selection and meticulous technique are required to achieve best results and avoid complications 6/7
7 References 1. Bruera E, Lawlor P. Cancer pain management. Acta Anaesthesiologica Scandinavica 1197; 41: Banning A, Sjøgren P, Henriksen H. Treatment outcome in a multidisciplinary cancer pain clinic. Pain 1991; 47: Levy, R.M. Pharmacologic treatment of cancer pain. New England Journal of Medicine 1996; 335: Valeberg BT, Rustoen T, Bjordal K, et al. Self-reported prevalence, etiology, and characteristics of pain in oncology outpatients. European Journal of Pain 2008; 12: De Courcy JG. Interventional techniques for cancer pain management. Clinical Oncology 2011; 23: Sillevis Smitt P, Tsafka A, Van de Zande FT. Outcome and complications of epidural analgesia in patients with chronic cancer pain. Cancer 1998; 83: Ruppen W, Derry S, McQuay HJ, Moore RA. Infection rates associated with epidural indwelling catheters for seven days or longer: systematic review and meta-analysis. BMC Palliative Care 2007; 6:3. 8. Bedder MD, Burchiel K, Larson A. Cost analysis of two implantable narcotic delivery systems. Journal of Pain and Symptom Management 1991; 6: Smith TJ, Staats PS, Deer T, et al. Randomized clinical trial of an implantable drug delivery system compared with comprehensive medical management for refractory cancer pain : impact on pain, drug related toxicity and survival. Journal of Clinical Oncology 2002; 20: Smith TJ, Coyne PJ, Staats PS et al. An implantable drug delivery system (IDDS) for refractory cancer pain provides sustained pain control, less drug-related toxicity, and possibly better survival compared with comprehensive medical management (CMM). Annals of Oncology 2005; 16: Deer TR, Smith HS, Burton AW, et al. Comprehensive consensus based guidelines on intrathecal drug delivery systems in the treatment of pain caused by cancer pain. Pain Physician 2011; 14:E Coffey RJ, Owens ML, Broste SK, et al. Mortality associated with implantation and management of intrathecal opioid drug infusion systems to treat non cancer pain. Anesthesiology 2009; 111: Patt, R.B Cancer Pain. Lippincott. Philadelphia, xxi, 650 p. 14. Eisenberg E, Carr DB, Chalmers TC. Neurolytic celiac plexus block for treatment of cancer pain: a meta-analysis. Anesth Analg 1995; 80: Koyyalagunta D, Burton AW. The role of chemical neurolysis in cancer pain. Current Pain Headache Reports 2010; 14: Kassamali RH, Ganeshan A, Hoey ET, et al. Pain management in spinal metastases: The role of percutaneous vertebral augmentation. Annals of Oncology 2010; 22: /7
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Interventional Techniques for Cancer Pain Management
 Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold Pain Management Center Beth Israel Deaconess Medical Center Disclosure No financial or industry
Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold Pain Management Center Beth Israel Deaconess Medical Center Disclosure No financial or industry
Interventional Techniques for Cancer Pain Management
 Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold - Warfield Pain Center Beth Israel Deaconess Medical Center Boston, MA Disclosure No financial
Interventional Techniques for Cancer Pain Management Musa M. Aner, MD Director, Cancer Pain Service Arnold - Warfield Pain Center Beth Israel Deaconess Medical Center Boston, MA Disclosure No financial
Celiac plexus block. Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care.
 Celiac plexus block Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care. Introduction A celiac plexus block is an injection of local anesthetic into or around the celiac plexus
Celiac plexus block Dr.Kasturi Bhagawati Asst.professor Dept. of Emergency Medicine & Critical care. Introduction A celiac plexus block is an injection of local anesthetic into or around the celiac plexus
Management of Neuropathic pain
 Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
INTERVENTIONAL PAIN MANAGEMENT UPDATE
 INTERVENTIONAL PAIN MANAGEMENT UPDATE Orlando G. Florete Jr.,M.D. Director, Institute of Pain Management Director, Florida Institute of Medical Research Jacksonville, FL HIPPOCRATIC OATH I I will prescribe
INTERVENTIONAL PAIN MANAGEMENT UPDATE Orlando G. Florete Jr.,M.D. Director, Institute of Pain Management Director, Florida Institute of Medical Research Jacksonville, FL HIPPOCRATIC OATH I I will prescribe
ABC of palliative care: Difficult pain problems
 BMJ 1997;315:867-869 (4 October) Clinical review ABC of palliative care: Difficult pain problems J Sykes, R Johnson, G W Hanks Roughly 80-90% of pain due to cancer can be relieved relatively simply with
BMJ 1997;315:867-869 (4 October) Clinical review ABC of palliative care: Difficult pain problems J Sykes, R Johnson, G W Hanks Roughly 80-90% of pain due to cancer can be relieved relatively simply with
Pain Management Clinic ISIC
 Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
Pain Management Clinic ISIC Let us rebuild a pain free life Pain is one of the commonest symptoms in patients attending OPDs of various hospitals and clinics. Chronic pain is any pain that has persisted
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES
 SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
SYMPATHETIC BLOCKS AND THEIR ROLE IN MANAGEMENT AND DIAGNOSIS OF CHRONIC PAIN SYNDROMES Overview Eugene Mitchell, MD Activity of the sympathetic efferents and their role in the pathology of chronic pain
2018 ASC FINAL Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 62263 62264 62268 62269 62270 62272 62273 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 62263 62264 62268 62269 62270 62272 62273 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE
 CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE By Eshaq AlShaqaq Clinical fellow Introduction Celiac Plexus
CELIAC PLEXUS NEUROLYSIS WITH REPEATED AMMONIUM SULPHATE INJECTION FOR THE TREATMENT OF CHRONIC NON- CANCER ABDOMINAL PAIN UNDER CT SCAN GUIDANCE By Eshaq AlShaqaq Clinical fellow Introduction Celiac Plexus
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE
 PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE The following CPT/HCPCS codes for pain management require prior authorization through evicore healthcare. In order to request
PAIN MANAGEMENT CODES PRIOR AUTHORIZATION REQUIRED THROUGH EVICORE HEALTHCARE The following CPT/HCPCS codes for pain management require prior authorization through evicore healthcare. In order to request
Sympathetic Nervous System
 Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
2019 ASC FINAL Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
2019 ASC Proposed Payment Rates
 20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
20526 20550 20551 20552 20553 20600 20605 20610 22510 22511 22513 22514 22869 27279 62263 62264 62268 62269 62270 Injection, therapeutic tendon sheath, ligament injection Tendon origin/insertion injection
Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management
 Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management Eric Roeland, MD GI Oncology Palliative Medicine Pancreatic Cancer Patient Tool Belt Chemotherapy Surgery Pain & Symptom
Optimizing Your Quality of Life During Cancer Treatment: Pain & Side Effect Management Eric Roeland, MD GI Oncology Palliative Medicine Pancreatic Cancer Patient Tool Belt Chemotherapy Surgery Pain & Symptom
ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT
 ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT Oscar A. de Leon-Casasola, MD Professor of Anesthesiology and Medicine Senior Vice-Chair Dept. of Anesthesiology, The Jacobs School of Medicine Chief, Pain
ALTERNATIVAS A LA ADMINISTRACION: OPIOIDES IT Oscar A. de Leon-Casasola, MD Professor of Anesthesiology and Medicine Senior Vice-Chair Dept. of Anesthesiology, The Jacobs School of Medicine Chief, Pain
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT
 Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
Discussion Points 10/17/16. Spine Pain is Ubiquitous. Interventional Pain Management
 Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Intercostal nerve blockade for cancer pain: effectiveness and selection of patients
 O R I G I N A L A R T I C L E Frank CS Wong TW Lee KK Yuen SH Lo WK Sze Stewart Y Tung Intercostal nerve blockade for cancer pain: effectiveness and selection of patients Objectives To review treatment
O R I G I N A L A R T I C L E Frank CS Wong TW Lee KK Yuen SH Lo WK Sze Stewart Y Tung Intercostal nerve blockade for cancer pain: effectiveness and selection of patients Objectives To review treatment
Autonomic Nervous System DR JAMILA EL MEDANY
 Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Tymaa Al-zaben & Amin Al-ajalouni
 Done by: Tymaa Al-zaben & Amin Al-ajalouni ** Hello SERTONIN! SLIDE 3 note:: the slide included within the sheet but make sure back to slide for pictures The Autonomic Nervous System Function : Regulate
Done by: Tymaa Al-zaben & Amin Al-ajalouni ** Hello SERTONIN! SLIDE 3 note:: the slide included within the sheet but make sure back to slide for pictures The Autonomic Nervous System Function : Regulate
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain
 Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain Thesis Submitted for the partial fulfillment of MD Degree in anesthesiology and
Computed tomography versus fluoroscopy guidance in celiac plexus neurolysis for treatment of upper abdominal malignant pain Thesis Submitted for the partial fulfillment of MD Degree in anesthesiology and
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY
 GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
GUIDELINES ON PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
NERVOUS SYSTEM ANATOMY
 NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
Intrathecal Opioid Therapy for Management of Chronic Pain
 Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Nervous Systems: Diversity & Functional Organization
 Nervous Systems: Diversity & Functional Organization Diversity of Neural Signaling The diversity of neuron structure and function allows neurons to play many roles. 3 basic function of all neurons: Receive
Nervous Systems: Diversity & Functional Organization Diversity of Neural Signaling The diversity of neuron structure and function allows neurons to play many roles. 3 basic function of all neurons: Receive
ICD-9-CM Diagnosis Code options
 ICD-9-CM Diagnosis Code options Diagnosis codes are used by both physicians and facilities to document the indication for the procedure. Intrathecal drug delivery is directed at managing chronic, intractable
ICD-9-CM Diagnosis Code options Diagnosis codes are used by both physicians and facilities to document the indication for the procedure. Intrathecal drug delivery is directed at managing chronic, intractable
PAIN MANAGEMENT IN UROLOGY
 24 PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional experience
24 PAIN MANAGEMENT IN UROLOGY F. Francesca (chairman), P. Bader, D. Echtle, F. Giunta, J. Williams Eur Urol 2003; 44(4):383-389 Introduction Pain is defined as an unpleasant sensory and emotional experience
Dana Alrafaiah. - Amani Nofal. - Ahmad Alsalman. 1 P a g e
 - 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
- 2 - Dana Alrafaiah - Amani Nofal - Ahmad Alsalman 1 P a g e This lecture will discuss five topics as follows: 1- Arrangement of pelvic viscera. 2- Muscles of Pelvis. 3- Blood Supply of pelvis. 4- Nerve
Non-Pharmacological Management of Pain. Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies
 Non-Pharmacological Management of Pain Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies Practice Pharmacotherapy treats majority of pain(90%). Occasionally
Non-Pharmacological Management of Pain Anesthetic interventions Neurosurgical interventions Cognitive behavioral therapy Physical Therapies Practice Pharmacotherapy treats majority of pain(90%). Occasionally
The Role of the Neuromodulation in Management of Chronic Pain
 The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Role of the Neuromodulation in Management of Chronic Pain Adnan Al-Kaisy, MB ChB, FRCA, FFPMRCA, FIPP Clinical Lead of the Pain Management & Neuromodulation Centre Guy s & St Thomas Hospital, London,
The Nervous System: Autonomic Nervous System Pearson Education, Inc.
 17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
Indications for Kyphoplasty and Vertebroplasty
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Epidural Analgesia in Labor - Whats s New
 Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Epidural Analgesia in Labor - Whats s New Wichelewski Josef 821 Selective neural blockade has many clinical applications in medicine but nowhere has its use been so well accepted than in the field of Obstetrics.
Human Anatomy. Autonomic Nervous System
 Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
The Nervous System: Autonomic Nervous System
 17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Cancer Pain Management Pharmacological Treatment and Beyond. Marie Aouad-Maroun MD Professor Department of Anesthesiology
 Cancer Pain Management Pharmacological Treatment and Beyond Marie Aouad-Maroun MD Professor Department of Anesthesiology Palliative and End-of-Life Care Master Class October 18-19, 2013 Pain in cancer
Cancer Pain Management Pharmacological Treatment and Beyond Marie Aouad-Maroun MD Professor Department of Anesthesiology Palliative and End-of-Life Care Master Class October 18-19, 2013 Pain in cancer
Basic Standards for. Fellowship Training in. Acute and Chronic Pain Management. in Anesthesiology
 Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
ANATOMY & PHYSIOLOGY - CLUTCH CH THE AUTONOMIC NERVOUS SYSTEM.
 !! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
!! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1)
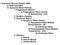 I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
[ANATOMY #12] April 28, 2013
![[ANATOMY #12] April 28, 2013 [ANATOMY #12] April 28, 2013](/thumbs/86/93473883.jpg) Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Sympathetic chain : Sympathetic chain is each of the pair of ganglionated longitudinal cords of the sympathetic nervous system; extend from level of atlas (base of skull) till coccyx. It is paravertebral
Spinal nerves. Aygul Shafigullina. Department of Morphology and General Pathology
 Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
ISPUB.COM. Lumbar Sympathectomy by Laser Technique. S Kantha, B Kantha METHODS AND MATERIALS
 ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
ISPUB.COM The Internet Journal of Minimally Invasive Spinal Technology Volume 1 Number 2 Lumbar Sympathectomy by Laser Technique S Kantha, B Kantha Citation S Kantha, B Kantha. Lumbar Sympathectomy by
Managing Bone Pain in Metastatic Disease. Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018
 Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
Managing Bone Pain in Metastatic Disease Rachel Schacht PA-C Medical Oncology and Hematology Associates Presented on 11/2/2018 None Disclosures Managing Bone Pain in Metastatic Disease This lecture will
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Group of students. - Rawan almujabili د. محمد المحتسب - 1 P a g e
 - 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
- 14 - Group of students - Rawan almujabili د. محمد المحتسب - 1 P a g e Nerves of the posterior abdominal wall The spinal cord gives off spinal nerves between the vertebrae. In the abdomen, through the
Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems
 Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans
Cigna Medical Coverage Policies Musculoskeletal Implantable Intrathecal Drug Delivery Systems Effective January 1, 2016 Instructions for use The following coverage policy applies to health benefit plans
Perioperative Pain Management
 Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
Perioperative Pain Management Overview and Update As defined by the Anesthesiologist's Task Force on Acute Pain Management are from the practice guidelines from the American Society of Anesthesiologists
01/07/2018 MANAGEMENT OF RECTAL TENESMUS PRESENTATION OUTLINE
 MANAGEMENT OF RECTAL TENESMUS Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE Definition A Clinical Case Epidemiology Pathophysiology
MANAGEMENT OF RECTAL TENESMUS Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE Definition A Clinical Case Epidemiology Pathophysiology
Chapter 15: The Autonomic Nervous System. Copyright 2009, John Wiley & Sons, Inc.
 Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
2012 CPT Changes Affecting Radiology REVISIONS
 2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
2012 CPT Changes Affecting Radiology REVISIONS 22520 Percutaneous vertebroplasty (bone biopsy included when performed), 1 vertebral body, unilateral or bilateral injection; thoracic 22521 lumbar 22522
2013 FINAL - Physician Payment Rates
 ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
ASC/Hospital) Injection, therapeutic (eg, local anesthetic; corticosteroid), 20526 carpal tunnel $74.88 $56.50 $76.55 $56.48 2.2% 0.0% tendon sheath, ligament injection 20550 $57.18 $40.85 $58.52 $41.17
Spinal Analgesia (Neuraxial analgesia in humans)
 Spinal Analgesia (Neuraxial analgesia in humans) Paul Farquhar-Smith The Royal Marsden NHS Foundation Trust And other humanoid species Neuraxial analgesia Cancer pain ADDITIONAL ANALGESIC MEASURES FINAL
Spinal Analgesia (Neuraxial analgesia in humans) Paul Farquhar-Smith The Royal Marsden NHS Foundation Trust And other humanoid species Neuraxial analgesia Cancer pain ADDITIONAL ANALGESIC MEASURES FINAL
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives
 UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives Overview Further Interventional Pain training over 4 weeks
UBC Pain Medicine Residency Program: CanMEDS Goals and Objectives of the 4 week UBC Interventional Pain Management Elective: Goals & Objectives Overview Further Interventional Pain training over 4 weeks
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
2019 PROPOSED - Physician Payment Rates rates compared to 2018 rates
 Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $78.96 $59.58 $79.56 $59.76 $79.30 $59.84-0.3% 0.1% tendon sheath, ligament injection 20550 $53.83 $40.55 $54.36 $40.68
Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $78.96 $59.58 $79.56 $59.76 $79.30 $59.84-0.3% 0.1% tendon sheath, ligament injection 20550 $53.83 $40.55 $54.36 $40.68
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
UTERINE FIBROID EMBOLIZATION
 INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
INTERVENTIONAL RADIOLOGY PROTOCOLS UTERINE FIBROID EMBOLIZATION Interventional Radiology Tower Health Medical Group offers the option to treat uterine fibroids with fibroid embolization (UFE), an alternative
Types of blocks. Clinical considerations 8/11/2009. Let s Discuss Sympathetic Blocks. Stellate Celiac plexis Lumbar sympathetic Hypogastric
 Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Let s Discuss Sympathetic Blocks Janette Elliott, RN-BC, MSN, AOCN ASPMN 19 th Annual Conference September 2009 Types of blocks Stellate Celiac plexis Lumbar sympathetic Hypogastric Clinical considerations
Nerves on the Posterior Abdominal Wall
 Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoasmuscle from the anterior ramiof the upper
IMPLANTABLE INTRATHECAL DRUG DELIVERY SYSTEMS
 evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
evicore healthcare. Clinical Decision Support Tool Diagnostic Strategies This tool addresses common symptoms and symptom complexes. Imaging requests for patients with atypical symptoms or clinical presentations
2017 FINAL - Physician Payment Rates rates compared to 2016 rates
 Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $79.18 $59.47 $79.06 $59.74 $78.96 $59.58-0.3% 0.2% tendon sheath, ligament injection 20550 $60.19 $42.99 $54.02 $40.78
Injection, therapeutic (eg, local anesthetic; corticosteroid), carpal tunnel 20526 $79.18 $59.47 $79.06 $59.74 $78.96 $59.58-0.3% 0.2% tendon sheath, ligament injection 20550 $60.19 $42.99 $54.02 $40.78
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Autonomic Nervous System. Ms. DS Pillay Room 2P24
 Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Classification of the nervous system. Prof. Dr. Nikolai Lazarov 2
 1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
1 1. Formation and general organization 2. Spinal ganglia 3. Zonal and segmental innervation 4. Dorsal rami of the spinal nerves 5. Ventral rami of the spinal nerves 6. Cervical plexus Classification of
Biology 218 Human Anatomy
 Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Anesthesia Processing Guidelines
 Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
Anesthesia Processing Guidelines Policy Number: 10.01.511 Last Review: 5/2014 Origination: 10/1988 Next Review: 5/2015 Policy The following guidelines are utilized in processing anesthesia claims: 1) Anesthesia
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Chapter 16. APR Enhanced Lecture Slides
 Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
ANATOMY OF SPINAL CORD. Khaleel Alyahya, PhD, MEd King Saud University School of
 ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
ANATOMY OF SPINAL CORD Khaleel Alyahya, PhD, MEd King Saud University School of Medicine @khaleelya OBJECTIVES At the end of the lecture, students should be able to: Describe the external anatomy of the
Neuroplasty or Epidural Adhesiolysis / Neurolysis
 Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
Epidural injections are a very common treatment for neck, back and extremity pain. Back problems have become one of the most common medical conditions in our society today. Approximately 80 percent of
Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief
 Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief Okan Akhan 1 Mustafa N. Ozmen Nuri Basgun Devrim Akinci Oguzhan Oguz Mert Koroglu Musturay Karcaaltincaba
Long-Term Results of Celiac Ganglia Block: Correlation of Grade of Tumoral Invasion and Pain Relief Okan Akhan 1 Mustafa N. Ozmen Nuri Basgun Devrim Akinci Oguzhan Oguz Mert Koroglu Musturay Karcaaltincaba
Gross Anatomy of Lower Spinal Cord
 Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
Chapter 13 Spinal Cord, Spinal Nerves and Somatic Reflexes Spinal cord Spinal nerves Somatic reflexes Gross Anatomy of Lower Spinal Cord Meninges of Vertebra & Spinal Cord Spina Bifida Congenital defect
8/28/18. Anesthetic considerations for patients with implanted devices for treating chronic pain and more. Objectives:
 Anesthetic considerations for patients with implanted devices for treating chronic pain and more Alaa Abd-Elsayed, MD, MPH Medical Director, UW Pain Services Medical Director, Pain Clinic Section Head,
Anesthetic considerations for patients with implanted devices for treating chronic pain and more Alaa Abd-Elsayed, MD, MPH Medical Director, UW Pain Services Medical Director, Pain Clinic Section Head,
ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA
 1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
1 ANATOMY OF PELVICAYCEAL SYSTEM -DR. RAHUL BEVARA 2 KIDNEY:ANATOMY OVERVIEW Kidneys are retroperitoneal, in posterior abdominal region, extending from T12 L3 Bean-shaped Right kidney is lower than left
Labor Epidural: Local Anesthetics and Beyond
 Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
IN PRESS. Case Report. A Challenging Case of Ganglion Impar Block in a Patient with. Kevin Wong, DO and Brian R. Monroe, MD
 Case Report Interventional Pain Management Reports Volume 1, Number 1, pp71-77 2017, American Society of Interventional Pain Physicians A Challenging Case of Ganglion Impar Block in a Patient with Coccygeal
Case Report Interventional Pain Management Reports Volume 1, Number 1, pp71-77 2017, American Society of Interventional Pain Physicians A Challenging Case of Ganglion Impar Block in a Patient with Coccygeal
Dr. Guy Buchanan MBBS, FANZCA, FFPMANZCA Specialist Pain Medicine Physician & Anaesthetist Associate - Victoria Pain Specialists
 anagement of Patients with Implante Dr. Guy Buchanan MBBS, FANZCA, FFPMANZCA Specialist Pain Medicine Physician & Anaesthetist Associate - Victoria Pain Specialists overview brief introduction to the
anagement of Patients with Implante Dr. Guy Buchanan MBBS, FANZCA, FFPMANZCA Specialist Pain Medicine Physician & Anaesthetist Associate - Victoria Pain Specialists overview brief introduction to the
Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain
 966 Journal of Pain and Symptom Management Vol. 22 No. 5 November 2001 Original Article Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain Jan H. Vranken, MD,
966 Journal of Pain and Symptom Management Vol. 22 No. 5 November 2001 Original Article Increasing the Efficacy of a Celiac Plexus Block in Patients with Severe Pancreatic Cancer Pain Jan H. Vranken, MD,
Paraspinal Blocks a new paradigm in truncal analgesia
 Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
Paraspinal Blocks a new paradigm in truncal analgesia Ki Jinn Chin, MBBS (Hons), MMed, FRCPC Associate Professor Toronto Western Hospital University of Toronto Online Resources https://youtu.be/lockhd
C ODING PAIN C LINICS. After attending this presentation, attendee will be able to: Coding Check List
 Home Town Health Take the Pain out of Coding Pain Clinics J E NAN C U S TER C P C, C C S, C D I P AH IMA A PPROVED IC D - 1 0 - C M/PC S T RAINER AND A MBASSADOR D IRECTOR OF C ODING H EALTHCARE C ODING
Home Town Health Take the Pain out of Coding Pain Clinics J E NAN C U S TER C P C, C C S, C D I P AH IMA A PPROVED IC D - 1 0 - C M/PC S T RAINER AND A MBASSADOR D IRECTOR OF C ODING H EALTHCARE C ODING
Reimbursement Guidelines for Pain Management Procedures 1
 GE Healthcare Reimbursement Guidelines for Pain Management Procedures 1 April 2015 www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for pain management procedures
GE Healthcare Reimbursement Guidelines for Pain Management Procedures 1 April 2015 www.gehealthcare.com/reimbursement This overview addresses coding, coverage, and payment for pain management procedures
Systems Neuroscience November 21, 2017 The autonomic nervous system
 Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
Vertebral Augmentation for Compression Fractures. Scott Magnuson, MD Pain Management of North Idaho, PLLC
 Vertebral Augmentation for Compression Fractures Scott Magnuson, MD Pain Management of North Idaho, PLLC OVCFs are most common type of fragility fracture 20-25% Caucasian women and men over 50 yrs have
Vertebral Augmentation for Compression Fractures Scott Magnuson, MD Pain Management of North Idaho, PLLC OVCFs are most common type of fragility fracture 20-25% Caucasian women and men over 50 yrs have
Role and safety of epidural analgesia
 Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
Anaesthesia for Liver Resection Surgery The Association of Anaesthetists Seminars 21 Portland Place, London Thursday 15 th December 2005 Role and safety of epidural analgesia Lennart Christiansson MD,
