The functional gastrointestinal disorders and the Rome II process
|
|
|
- Camron Greene
- 6 years ago
- Views:
Transcription
1 Gut 1999;45(Suppl II):II1 II5 II1 The functional gastrointestinal disorders and the Rome II process Man should strive to have his intestines relaxed all the days of his life. Moses Maimonides, AD A good set of bowels is worth more to a man than any quantity of brains. Josh Billings (Henry Wheeler Shaw), AD Toward a new understanding of the functional gastrointestinal disorders For centuries, physicians and historians have recognized that it is common for maladies to azict the intestinal tract, producing symptoms of pain, nausea, vomiting, bloating, diarrhea, constipation, diycult passage of food or feces, or any combination. 1 When these symptoms are experienced as severe, or when they impact on daily life, those azicted often attribute the symptoms to an illness and seek medical care. Traditionally, the physicians caring for these patients will search for inflammatory, infectious, neoplastic, and other structural abnormalities to make a specific diagnosis and over specific treatment. Yet as has been common in medical practice, 2 when no structural etiology is found, the patient is diagnosed as having functional symptoms and is treated symptomatically. Until recently, the limited scientific knowledge about the pathophysiology of these symptoms, and the need to diagnose by excluding organic disease, has led physicians to feel uncertain about the legitimacy of these symptoms as bona fide disorders. 3 Some have felt insecure in their ability to manage patients with these conditions, and might even avoid caring for patients with these complaints. But over the past two decades, two important processes have occurred to legitimize these conditions, and to increase attention toward the research and clinical care of patients with functional gastrointestinal disorders (FGID). The first has been a shift in conceptualizing these disorders from a disease-based, reductionistic model, where the evort is directed toward identifying a single underlying biological etiology, to a more integrated, biopsychosocial model of illness. 4 5 The latter model allows for symptoms to be understood as physiologically multidetermined (e.g., altered motility, enhanced visceral sensitivity, brain gut dysregulation) and as modifiable by sociocultural and psychosocial influences. The second change has been the remarkable growth in investigative techniques that support this newer conceptualization of brain gut interactions: improved motility assessment, the development of the barostat, imaging of the brain (positron emission tomography (PET), functional magnetic resonance imaging (fmri)), standardized psychological diagnostic instruments, and the molecular investigation of brain gut peptides. As a result, over the past two decades, there has been a 10-fold increment in Medline citations about irritable bowel syndrome (IBS), a much larger number of symposia and presentations at national and international meetings about the FGIDs, and increased evort by pharmaceutical companies to identify and test receptoractive agents to treat these disorders. These developments built support for an international evort to characterize and classify the FGIDs by investigators and clinicians, pharmaceutical regulatory organizations, pharmaceutical companies, and federal research agencies. The Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal Disorders (Rome Committees) began in the mid 1980s as a series of committees that developed consensus criteria for over 20 FGIDs and published them in several documents in Gastroenterology International. These documents were eventually updated and compiled into a book 6 as the Rome criteria. In this supplement, we present the second major evort of the Rome committees: the update of our growing knowledge of the FGIDs over the past five years. We include five articles that detail the FGIDs based on anatomic region, (esophageal, gastroduodenal, bowel, biliary, anorectal), and a separate article on pediatric FGIDs. We also present several articles summarizing current knowledge on the physiologic (motility/sensation), basic science (brain gut), and psychosocial aspects of the FGIDs, and provide recommendations for the design of treatment trials for these disorders. In addition, we include the revised (Rome II) diagnostic criteria for the FGIDs developed by consensus of experts and based on existing evidence. Finally, as we enter the new millennium, we offer recommendations for future studies that will help advance this growing field. In this introductory article, I will review the rationale and limitations of a symptom-based diagnostic (Rome II) classification system, discuss the process through which the criteria and consensus information were developed, and briefly summarize the pathophysiological knowledge that is evolving about the FGIDs. More detailed information is provided in the other articles written by the 10 committees. Rationale for symptom-based diagnostic criteria The Rome II classification system is based on the premise that for each disorder there are symptom clusters that breed true across clinical and population groups. While not completely true (see Qualifications, below), this presumption provides a framework for identification of patients for research, which can be modified as new scientific data emerge. The rationale for classifying the FGIDs into symptom-based subgroups has three bases. 7 SITE-SPECIFIC DIFFERENCES Patients with FGIDs report a wide variety of symptoms avecting diverent regions of the gastrointestinal tract. These symptoms have in common disturbances in sensory and/or motor gastrointestinal function, which may overlap across anatomic regions. However, epidemiological studies using factor analysis and other methods provide evidence for the existence of site-specific syndromes. 8 9 The clinical value of separating the functional gastrointestinal symptoms into discrete conditions (table 1) is that they can be reliably diagnosed and more specifically treated. The FGIDs are classified by anatomic region: esophageal (A), gastroduodenal (B), bowel (C) and functional abdominal pain (D), biliary (E), and anorectal (F). Within each anatomic category site, there can be several disorders, each with specific clinical features. For example, the functional bowel disorders (C), which include IBS (C1), functional abdominal bloating (C2), functional constipation (C3), and functional diarrhea (C4), are all functional bowel disorders attributed to the colon and rectum. Yet IBS, having pain associated with change in bowel habit, is distinct from functional diarrhea, which is characterized by loose stools
2 II2 Drossman Table 1 Functional gastrointestinal disorders A. Esophageal disorders A1. Globus A2. Rumination syndrome A3. Functional chest pain of presumed esophageal origin A4. Functional heartburn A5. Functional dysphagia A6. Unspecified functional esophageal disorder B. Gastroduodenal disorders B1. Functional dyspepsia B1a. Ulcer-like dyspepsia B1b. Dysmotility-like dyspepsia B1c. Unspecified (non-specific) dyspepsia B2. Aerophagia B3. Functional vomiting C. Bowel disorders C1. Irritable bowel syndrome C2. Functional abdominal bloating C3. Functional constipation C4. Functional diarrhea C5. Unspecified functional bowel disorder D. Functional abdominal pain D1. Functional abdominal pain syndrome D2. Unspecified functional abdominal pain E. Biliary disorders E1. Gall bladder dysfunction E2. Sphincter of Oddi dysfunction F. Anorectal disorders F1. Functional fecal incontinence F2. Functional anorectal pain F2a. Levator ani syndrome F2b. Proctalgia fugax F3. Pelvic floor dyssynergia G. Functional pediatric disorders G1. Vomiting G1a. Infant regurgitation G1b. Infant rumination syndrome G1c. Cyclic vomiting syndrome G2. Abdominal pain G2a. Functional dyspepsia G2b. Irritable bowel syndrome G2c. Functional abdominal pain G2d. Abdominal migraine G2e. Aerophagia G3. Functional diarrhea G4. Disorders of defecation G4a. Infant dyschezia G4b. Functional constipation G4c. Functional fecal retention G4d. Non-retentive fecal soiling and no pain. Presumably, each condition will have different diagnostic and treatment approaches. EPIDEMIOLOGICAL DATA Epidemiological studies show similar prevalences for these conditions across various studies and populations. The frequencies of bowel symptom patterns reported from England, France, and China are nearly identical (see Functional bowel disorders and Functional abdominal pain). In addition, a factor analysis study using two community samples 10 identified an irritable bowel factor, and these symptoms were very similar to those developed from a clinical population of patients with IBS using discriminant function analysis (Manning criteria). 11 NEED FOR DIAGNOSTIC STANDARDS OF CLINICAL CARE AND RESEARCH As, by definition, there are no physiological features of diagnostic value, and because it is symptoms that patients bring to physicians, the use of a symptom-based classification system is rational. Symptom-based criteria, used in psychiatry (e.g., DSM-IV) 12 and rheumatology 13 and most recently the Rome I criteria, 6 are becoming increasingly accepted within gastroenterology. Symptom-based criteria help guide the diagnostic and treatment approach, reduce the ordering of unneeded diagnostic tests, and help to standardize the selection of patients for clinical trials. QUALIFICATIONS FOR THE USE OF SYMPTOM-BASED CRITERIA Certain limitations and qualifications need to be considered. 7 Other diseases may coexist that need to be excluded The high frequency of the FGIDs assures their coexistence with other (organic) diseases. In fact, IBS and inflammatory bowel disease (IBD) seem to have a greater than chance association, 14 and IBD may even predispose to IBS. 15 Similarly, Helicobacter pylori needs to be excluded and/or treated among patients with functional dyspepsia. So, it is necessary to exclude other diseases before a functional gastrointestinal designation can be applied. Symptoms may overlap with other functional gastrointestinal disorders Because diverent FGIDs may coexist, the criteria need to allow for hierarchical classification of the FGIDs. For example, if criteria for both IBS (C1) and functional dyspepsia (B1) are fulfilled, then both diagnoses co-exist. However, if criteria for IBS are fulfilled, but the patient also has upper gastrointestinal (dyspeptic-like) pain that is relieved by defecation, then only IBS exists. Also, an unspecified designation (e.g., unspecified functional bowel disorder) permits the inclusion of patients with functional gastrointestinal symptoms who do not meet more specific categories. Symptoms must be present for at least 12 weeks over the previous year To make a diagnosis of a FGID, symptoms should be present for at least 12 weeks out of the previous year. There are certain exceptions for example, chronic functional abdominal pain requires six months of symptoms, and certain pediatric and anorectal disorders require only several weeks of symptoms. The 12-week qualification is a change from the Rome I criteria, which only required that symptoms be present in the previous three months. The reasons for this change are that FGIDs are conditions that have a waxing and waning course, and (particularly for epidemiological surveys) symptoms might not have been present in the previous three months, but may have existed prior to that time. The 12 weeks need not be consecutive, and within each week, symptoms are only required for 1/7 days. In addition, we recognize the diyculty in translating the time requirement into a questionnaire. For some purposes, investigators may choose the last three months as the time requirement. This choice may be preferred for entry into clinical trials. Diagnostic categories do not include psychosocial criteria Although psychosocial disturbances can avect the onset, course and outcome of the FGIDs 16 (see Psychosocial aspects of functional gastrointestinal disorders), they are not required for diagnosis, as they do not occur in people with FGID who do not seek health care. Evidence is determined by clinical consensus and existing evidence The proposed diagnostic criteria are derived from the consensus of experts in the field (the committees and their consultants). Using the Rome I consensus criteria as a starting point, the committees had to justify all changes for the Rome II criteria based on existing scientific data, or on a rational recommendation agreed upon by the committee, the Coordinating Committee, and the reviewers. Also, these new criteria will be tested in future studies now underway, and this will form the basis for future modifications of the criteria. The process of developing diagnostic criteria The process for developing these criteria is a rigorous one. The consensus process was initiated by Professor Aldo
3 The functional gastrointestinal disorders and the Rome II process II3 Torsoli for the International Congress of Gastroenterology in Rome (Roma 88). Professor Torsoli charged the committees 19 to use a Delphi method 20 of decision-making, which fosters a team evort to produce consistency in opinion, or consensus (although not necessarily total agreement) for diycult questions not easily tackled. In 1995, the Rome II Coordinating Committee took on the responsibility of carrying these activities further using a rigorous four year, 10-step process: (1) The Coordinating Committee identified individuals with international research and clinical expertise to chair each of the 10 committees. Each Chair was charged to develop a manuscript for this supplement and an expanded manuscript for an upcoming book. (2) Each Chair, in consultation with the Coordinating Committee, identified a Co-Chair and recruited an international panel of up to five additional members having similar clinical and investigative skills to create the manuscripts. (3) Each committee member produced a document in response to specific assignments given by the Chair and Co-Chair. Usually the task was to synthesize the literature regarding the physiological, psychological, diagnostic, and treatment aspects of a particular functional disorder or scientific content area. (4) Each Chair incorporated all documents into a manuscript that was sent to the entire committee for review. (5) This process of modification and re-review by the committee was repeated two more times over a two year period. (6) Each committee met for three days in June 1998 to revise the document, using the Delphi method. 20 This face-to-face meeting led to consensus on the diagnostic criteria and scientific content. (7) Each Chair sent the revised document to at least six outside international experts and to scientists in the pharmaceutical industry for review and comment. (8) The committee Chairs responded to the reviewers comments either by modifying the manuscripts as requested, or providing a written response that addressed the reviewers concerns. (9) The revised manuscripts and the commentaries by the reviewers and authors were then sent to the Coordinating Committee who met in November 1998 and again in February 1999 to review these materials critically, and to submit critiques back to the authors. (10) Finally, when the document was completed, all members signed ov their approval before it was returned back to the Coordinating Committee for a final check on content and style prior to submission for publication. Observations on the functional gastrointestinal disorders In proposing the diagnostic groupings listed in table 1, we recognize that, despite diverences in location and symptom features, they share common features with regard to their motor and sensory physiology, central nervous system (CNS) relationships, and the approach to patient care. What follows are general observations and guidelines for these disorders. ABNORMAL MOTILITY It is well recognized that vomiting, diarrhea, acute abdominal pain, incontinence, and many other gastrointestinal symptoms are generated by disturbed gastrointestinal motility. Furthermore, in healthy subjects, strong emotion or environmental stress can lead to increased motility in the esophagus, stomach, small intestine, and colon. The FGIDs are characterized by having an even greater motility response to stressors (psychological or physiological) when compared with responses in normal subjects; candidate electrical activity markers have been proposed which may facilitate these responses. 21 However, these motor responses are only partially correlated with symptoms and are not suycient to explain reports of chronic or recurrent abdominal pain. VISCERAL HYPERSENSITIVITY The poor association of pain with gastrointestinal motility in many of the FGIDs (e.g., functional chest pain of presumed esophageal origin (A3), functional dyspepsia (B1), IBS (C1), functional abdominal pain (D)), is explained by more recent studies relating to abnormalities in visceral sensation. 22 These patients may have a lower pain threshold when tested with balloon distension of the bowel (visceral hyperalgesia), or they may have increased sensitivity even to normal intestinal function (e.g., allodynia), and there may be an increased or unusual area of somatic referral of visceral pain. It is not yet clear whether visceral hypersensitivity in the FGIDs relates to (a) altered receptor sensitivity at the viscus itself, (b) increased excitability of the spinal cord dorsal horn neurons, or (c) altered central modulation of sensation. 21 Another recent observation is that visceral hypersensitivity may be induced (stimulus hyperalgesia) in response to rectal or colonic distension in normal subjects 23 and to a greater degree in people with IBS. 24 So the pain of an FGID may relate to sensitization resulting from chronic motor hyperactivity (e.g., discrete clustered contractions), gastrointestinal infection (e.g., H pylori for functional dyspepsia and enteric infections for IBS (see later) or trauma/ injury to the viscera). INFLAMMATION Certain investigators have proposed that increased inflammation in the enteric mucosa or neural plexi may contribute to symptom development. 25 This may occur by peripheral sensitization (see earlier), and/or hypermotility activated by induction of mucosal inflammatory cytokines. 26 This hypothesis follows clinical observations that about one-third of patients with IBS report that their symptoms began after an acute enteric infection, and also, one-third of patients presenting with an acute enteric infection will go on to develop IBS-like symptoms. BRAIN GUT INTERACTIONS To bring these observations together, we emphasize a more integrative biopsychosocial understanding of these symptoms as being generated by a combination of intestinal motor, sensory, and CNS activity the brain gut axis. 29 Thus, extrinsic (vision, smell, etc.) or enteroceptive (emotion, thought) information have, by nature of their neural connections from higher centers, the capability to avect gastrointestinal sensation, motility, secretion, and inflammation. Conversely, viscerotopic evects (e.g., nociception) reciprocally avect central pain perception, mood, and behavior. For example, spontaneously induced contractions of the colon in rats lead to activation of the locus coeruleus in the pons, an area closely connected to pain and emotional centers in the brain. 30 Conversely, increased arousal or anxiety is associated with a decrease in the frequency of migrating motor complex activity of the small bowel. 31 Brain gut interactions may also influence postinfectious IBS. In a study of patients admitted for acute gastroenteritis, 23% developed IBS-like symptoms three months later. When comparing those who developed IBS symptoms with those who did not: (1) psychosocial diyculties (life stress
4 II4 Drossman and hypochondriasis) predicted who would go on to develop IBS symptoms; (2) altered gut physiology (abnormal motility and visceral hypersensitivity) was present at three months in both groups (i.e., with or without symptoms); and (3) increased inflammatory cells were present only in the group with IBS symptoms. 28 So although the acute infection led to physiological disturbances in the gut (altered sensation and motility), it seems that the psychological distress contributed to the later experience of the symptoms. The stress may perpetuate IBS symptoms by CNS facilitation of inflammation, via disruption of the hypothalamic pituitary adrenal/ cytokine stress pathway. It is now possible to study the brain physiology of patients with FGIDs using PET, fmri, and related imaging modalities. 34 These studies may help us to understand the role of the CNS in modulating visceral pain and motility. They may also provide a marker for studying responses to psychological treatments or psychopharmacological agents, as has been shown in analogous studies of psychiatric disorders. It was recently reported that depressed patients with more active anterior cingulate gyrus activity on PET imaging were more likely to respond to antidepressants. 35 BRAIN GUT PEPTIDES A treatment approach consistent with the concept of brain gut dysfunction is likely to involve the neuropeptides and receptors present in the enteric and central nervous systems. Putative agents include primarily 5-hydroxytryptamine and its congeners, the enkephalins and opioid agonists, substance P, calcitonin gene related polypeptide, and cholecystokinin, among others. These neuropeptides have integrated activities on gastrointestinal function and human behavior depending upon their location. Ongoing phase II and III pharmacological treatment trials using agents active at these receptor sites are addressing the diverse, but interconnected symptoms of pain, bowel dysfunction, and psychosocial distress so commonly associated with the FGIDs. The information gained from these studies may increase our understanding of these conditions, as well as possibly provide more evective treatment for patients with these conditions. PSYCHOSOCIAL FACTORS Although psychosocial factors do not define these disorders, and are not required for diagnosis (see later), they are important modulators of the patient s experience and behavior, and ultimately, the clinical outcome. Research on the psychosocial aspects of patients with FGIDs yields three general observations: + Psychological stress exacerbates gastrointestinal symptoms. Psychological stress or one s emotional responses to stress can avect gastrointestinal function and produce symptoms in healthy subjects, but does so to a greater degree in patients with FGIDs Psychological disturbances modify the experience of illness and illness behaviors such as health care seeking. Although patients with FGIDs show greater psychological disturbance than otherwise healthy subjects and patients with medical disease (see Psychosocial aspects of functional gastrointestinal disorders), the data are drawn from patients seen at referral centers; among non-health care seekers, such disturbances are no diverent than in the general population So psychosocial factors modulate illness experience and behaviors such as health care seeking. This explains findings associated with psychosocial trauma (e.g., history of sexual or physical abuse) which is found to be more common in referral centers than in primary care, may lower pain FGID Conceptual model Early life Genetics Environment Psychosocial factors Life stress Psychologic state Coping Social support CNS ENS Physiology Motility Sensation FGID Symptoms Behavior Outcome Medications MD visits Daily function Quality of life Figure 1 A biopsychosocial conceptualization of the pathogenesis and clinical expression of the functional gastrointestinal disorders (FGID). CNS, central nervous system; ENS, enteric nervous system. threshold and symptom reporting, and is associated with a poorer clinical outcome An FGID may have psychosocial consequences. Any chronic illness has psychosocial consequences on one s general well-being, daily function status, one s sense of control over the symptoms, and the implications of the illness in terms of future functioning at work and at home. This is understood in terms of one s healthrelated quality of life (HRQOL). Several new HRQOL instruments have been developed to evaluate patients with FGIDs (see Psychosocial aspects of functional gastrointestinal disorders and Design of treatment trials for the functional gastrointestinal disorders). A biopsychosocial conceptualization As indicated by the findings summarized in the previous section, the links among psychosocial and physiological factors are essential for a full understanding of the mechanisms and varying presentations of the FGIDs. Figure 1 conceptualizes this biopsychosocial understanding of the relationship between psychosocial and physiological factors with functional gastrointestinal symptoms and the clinical outcome. Early in life, genetics and environmental influences (e.g., family attitudes toward bowel training or illness in general, major loss or abuse history, or exposure to an infection) may avect one s psychosocial development (susceptibility to life stress, psychological state, coping skills, development of social support) or the development of gut dysfunction (abnormal motility or visceral hypersensitivity). In addition, the presence and nature of a FGID is determined by the interaction of psychosocial factors and altered physiology via the brain gut axis. So, one individual azicted with a bowel disorder, but with no psychosocial disturbances and good coping skills and social support, may not experience the symptoms as distressing enough to seek medical care. Another, having co-existent psychosocial disturbance, high life stress, and poor social support, may experience the symptoms as severe and unmanageable, may see physicians frequently, and have a generally poor outcome. Based on the observations presented, it is no longer rational to try to discriminate whether physiological or psychologic factors produce pain or other bowel symptoms, dysmotility, or inflammation. Instead, the FGIDs seem to be understood in terms of dysregulation of brain gut function, and the task is to determine the degree to which each is operative and remediable. Concluding comments It is with great pleasure and anticipation that we introduce this supplement on the functional gastrointestinal disorders, containing information on over two dozen adult and
5 The functional gastrointestinal disorders and the Rome II process II5 pediatric FGIDs, as well as supplementary information on the basic, physiologic and psychosocial aspects of these conditions. We hope that the information will make a difference in increasing awareness and knowledge relating to the diagnosis and care of patients with FGIDs. This supplement, and the book to follow (Rome II: The Functional Gastrointestinal Disorders published by Degnon Associates, 2000), which will contain more detailed information, are the culmination of four years of evortbyover 60 internationally recognized investigators in the field. For further information, contact As new scientific data about these disorders accumulate, there will be a need to revise the diagnostic criteria and the information provided relating to the pathophysiology and treatment of these conditions. Therefore, we have set up a process for validation studies and other future activities of the Rome Committees that will permit ongoing review and modification of our current recommendations. On behalf of the coordinating committee, I would like to thank our sponsors and supporters. From the pharmaceutical industry, the following sponsors merit special commendation: Special sustaining sponsor: Janssen Pharmaceutica; Full sponsors: Astra-Zeneca, GlaxoWellcome, Novartis, Pfizer, Roberts Pharaceuticals, SmithKline Beecham, and Solvay Pharmaceuticals; and Partial sponsors: Procter and Gamble, Sanofi Winthrop, and TAP Holdings. In addition, the following professionals and organizations contributed generously of their time and expertise: the Food and Drug Administration (FDA); the Japan International Gastrointestinal Motility Society; the Functional Brain Gut Research Group; the International Foundation for Functional Gastrointestinal Disorders; the National Institute of Digestive Diseases and Kidney Disorders (NIDDK-NIH); Associazione per la NeUroGastroenterlogia e la Motilità Gastrointestinale (ANEMGI); and the over 53 authors on 10 committees who worked tirelessly to produce these documents. Finally, special thanks go to Ms Carlar Blackman for her creative intelligence and tireless evort to keep the numerous projects and activities underway; to George Degnon for his skills in coordinating our meetings and for his sound advice; Ms Emanuela Crescini for her coordination of the meeting in Rome; and Ms Lou Ann Brower for her technical assistance and genuine interest in producing the best in a final product. Chair, Coordinating Committee, Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal Disorders (Rome II) D A DROSSMAN Professor of Medicine and Psychiatry, Co-Director, UNC Center for Functional GI and Motility Disorders, Division of Digestive Diseases, 726 Burnett-Womack, CB#7080, University of North Carolina at Chapel Hill, Chapel Hill, NC , USA 1 Drossman DA. Psychosocial and psychophysiologic mechanisms in GI illness. In: Kirsner JB, ed. The growth of gastroenterologic knowledge in the 20th century. 1st edn. Philadelphia: Lea and Febiger, 1993: Kroenke K, MangelsdorV AD. Common symptoms in ambulatory care: incidence, evaluation, therapy, and outcome. Am J Med 1989;86: Christensen J. Heraclides or the physician. Gastroenterol Int 1990;3: Engel GL. The need for a new medical model: a challenge for biomedicine. Science 1977;196: Drossman DA. Presidential address: gastrointestinal illness and biopsychosocial model. Psychosom Med 1998;60: Drossman DA, Richter JE, Talley NJ, et al (eds). The functional gastrointestinal disorders: diagnosis, pathophysiology and treatment. 1st edn. McLean, VA: Degnon Associates, Drossman DA. Do the Rome Criteria stand up? In: Goebell H, Holtmann G, Talley NJ, eds. Functional dyspepsia and irritable bowel syndrome: concepts and controversies (Falk Symposium 99). 1st edn. Dordrecht: Kluwer Academic Publishers, 1998: Whitehead WE. Functional bowel disorders: Are they independent diagnoses? In: Corazziari E, ed. Neurogastroenterology. 1st edn. Berlin: Walter de Gruyter, 1996: Whitehead WE, Gibbs NA, Li Z, et al. Is functional dyspepsia just a subset of the irritable bowel syndrome? Baillieres Clin Gastroenterol 1998;12: Whitehead WE, Crowell MD, Bosmajian L, et al. Existence of irritable bowel syndrome supported by factor analysis of symptoms in two community samples. Gastroenterology 1990;98: Manning AP, Thompson WG, Heaton KW, et al. Towards positive diagnosis of the irritable bowel. BMJ 1978;ii: American Psychiatric Association. Diagnostic and statistical manual of mental disorders DSM-IV. 4th edn. Washington, DC: American Psychiatric Association, Schumaker HR, Klippel JH, Robinson DR. Primer on the rheumatic diseases. 9th edn. Atlanta: Arthritis Foundation, Bayless TM. Inflammatory bowel disease and irritable bowel syndrome. Med Clin North Am 1990;49: Isgar B, Harman M, Kaye MD, et al. Symptoms of irritable bowel syndrome in ulcerative colitis in remission. Gut 1983;24: Drossman DA, Creed FH, Olden KW, et al. Psychosocial aspects of the functional gastrointestinal disorders. Gut 1999;45(suppl II):II Drossman DA, McKee DC, Sandler RS, et al. Psychosocial factors in the irritable bowel syndrome: a multivariate study of patients and nonpatients with irritable bowel syndrome. Gastroenterology 1988;95: Whitehead WE, Bosmajian L, Zonderman AB, et al. Symptoms of psychologic distress associated with irritable bowel syndrome: comparison of community and medical clinic samples. Gastroenterology 1988;95: Torsoli A, Corazziari E. The WTR s, the Delphic Oracle and the Roman Conclaves. Gastroenterol Int 1991;4: Milholland AV, Wheeler SG, Heieck JJ. Medical assessment by a delphi group opinion technic. N Engl J Med 1973;298: Drossman DA, Whitehead WE, Camilleri M. Irritable bowel syndrome: a technical review for practice guideline development. Gastroenterology 1997; 112: Mayer EA, Gebhart GF. Basic and clinical aspects of visceral hyperalgesia. Gastroenterology 1994;107: Ness TJ, Metcalf AM, Gebhart GF. A psychophysiological study in humans using phasic colonic distension as a noxious visceral stimulus. Pain 1990;43: Munakata J, NaliboV B, Harraf F, et al. Repetitive sigmoid stimulation induces rectal hyperalgesia in patients with irritable bowel syndrome. Gastroenterology 1997;112: Collins SM. Is the irritable gut an inflamed gut? Scand J Gastroenterol 1992; 27(suppl 192): Collins SM. The immunomodulation of enteric neuromuscular function: Implications for motility and inflammatory disorders. Gastroenterology 1996;111: McKendrick W, Read NW. Irritable bowel syndrome post salmonella infection. J Infect 1994;29: Gwee KA, Leong YL, Graham C, et al. The role of psychological and biological factors in post-infective gut dysfunction. Gut 1999;44: Mayer EA, Raybould HE. Role of visceral averent mechanisms in functional bowel disorders. Gastroenterology 1990;99: Svensson TH. Peripheral, autonomic regulation of locus coeruleus noradrenergic neurons in brain: putative implications for psychiatry and psychopharmacology. Psychopharmacology 1987;92: Valori RM, Kumar D, Wingate DL. EVects of diverent types of stress and or prokinetic drugs on the control of the fasting motor complex in humans. Gastroenterology 1986;90: Drossman DA. Mind over matter in the postinfective irritable bowel. Gut 1999;44: Drossman DA. Psychosocial factors in ulcerative colitis and Crohn s disease. In: Kirsner JB, ed. Inflammatory bowel disease. 5th edn. Philadelphia: WB Saunders, 1999 (in press). 34 Aziz Q, Thompson DG. Brain-gut axis in health and disease. Gastroenterology 1998;114: Mayberg HS, Brannan SK, Mahurin RK, et al. Cingulate function in depression: a potential predictor of treatment response. Neuroreport 1997;8: Whitehead WE, Crowell MD, Robinson JC, et al. EVects of stressful life events on bowel symptoms: subjects with irritable bowel syndrome compared to subjects without bowel dysfunction. Gut 1992;33: Drossman DA, Talley NJ, Olden KW, et al. Sexual and physical abuse and gastrointestinal illness: review and recommendations. Ann Intern Med 1995;123: For further information and updates on Rome II, visit our website at:
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514
 Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 History of Functional Disorders Douglas A. Drossman, MD Melissa Swantkowski THE PAST HISTORICAL PRECEDENTS Historians
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 History of Functional Disorders Douglas A. Drossman, MD Melissa Swantkowski THE PAST HISTORICAL PRECEDENTS Historians
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University
 CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
CHAPTER 11 Functional Gastrointestinal Disorders (FGID) Mr. Ashok Kumar Dept of Pharmacy Practice SRM College of Pharmacy SRM University 1 Definition of FGID Chronic and recurrent symptoms of the gastrointestinal
Rome III: an ongoing journey for better diagnosis and treatment of functional gastrointestinal disorders
 Mædica - a Journal of Clinical Medicine EDITORIALS Rome III: an ongoing journey for better diagnosis and treatment of functional gastrointestinal disorders Mircea DICULESCU, MD, Tudor ARBANAS, MD Gastroenterology
Mædica - a Journal of Clinical Medicine EDITORIALS Rome III: an ongoing journey for better diagnosis and treatment of functional gastrointestinal disorders Mircea DICULESCU, MD, Tudor ARBANAS, MD Gastroenterology
... SELECTED ABSTRACTS...
 ... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
... SELECTED ABSTRACTS... The following abstracts, from medical journals containing literature on irritable bowel syndrome, were selected for their relevance to this supplement. A Technical Review for
Throughout recorded history, and alongside structural
 GASTROENTEROLOGY 2006;130:1377 1390 INTRODUCTION The Functional Gastrointestinal Disorders and the Rome III Process DOUGLAS A. DROSSMAN, Guest Editor Division of Gastroenterology and Hepatology, UNC Center
GASTROENTEROLOGY 2006;130:1377 1390 INTRODUCTION The Functional Gastrointestinal Disorders and the Rome III Process DOUGLAS A. DROSSMAN, Guest Editor Division of Gastroenterology and Hepatology, UNC Center
190 Index Case studies, abdominal pain, 2 Crohn s disease, 2 3, cyclic vomiting syndrome (CVS), 2 fecal incontinence (FI), 2 medical c
 Index Abdominal pain, case study, 2 Achalasia, 75 Acupuncture 108 American Academy of Pediatrics, 49 Anxiety, 8 9, 98 Autism, GI disorders and, 25 27 BASC. See Behavior Assessment System for Children (BASC)
Index Abdominal pain, case study, 2 Achalasia, 75 Acupuncture 108 American Academy of Pediatrics, 49 Anxiety, 8 9, 98 Autism, GI disorders and, 25 27 BASC. See Behavior Assessment System for Children (BASC)
FUNCTIONAL DISORDERS ROME IV CRITERIA AND DIAGNOSTIC QUESTIONNAIRE DDW 2016,REVIEW. Presented by; Marjan Mokhtare Gastroenterologist, IUMS
 FUNCTIONAL DISORDERS ROME IV CRITERIA AND DIAGNOSTIC QUESTIONNAIRE DDW 2016,REVIEW Presented by; Marjan Mokhtare Gastroenterologist, IUMS Functional gastrointestinal disorders (FGIDs), the most common
FUNCTIONAL DISORDERS ROME IV CRITERIA AND DIAGNOSTIC QUESTIONNAIRE DDW 2016,REVIEW Presented by; Marjan Mokhtare Gastroenterologist, IUMS Functional gastrointestinal disorders (FGIDs), the most common
UKLIN1693a, date of preparation: March 2013.
 1 This table shows the ICE model. Defining the patient s ideas, concerns, and expectations is an important part of the consultation that can lead to better outcomes. 2 Patients with IBS may have visceral
1 This table shows the ICE model. Defining the patient s ideas, concerns, and expectations is an important part of the consultation that can lead to better outcomes. 2 Patients with IBS may have visceral
Functional Dyspepsia. Norbert Welkovics Heine van der Walt
 Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Norbert Welkovics Heine van der Walt Characteristics: Central abdomen Pain or discomfort Not associated with bowel movements No structural or biochemical abnormalty Definition Part of Gastroduodenal disorders
Functional Heartburn and Dyspepsia
 Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Functional Heartburn and Dyspepsia Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina Objectives Understand the means of diagnosing functional heartburn
Psychosocial aspects of the functional gastrointestinal disorders
 Gut 1999;45(Suppl II):II25 II30 II25 Psychosocial aspects of the functional gastrointestinal disorders D A Drossman, F H Creed, K W Olden, J Svedlund, B B Toner, W E Whitehead Chair, Committee on Psychosocial
Gut 1999;45(Suppl II):II25 II30 II25 Psychosocial aspects of the functional gastrointestinal disorders D A Drossman, F H Creed, K W Olden, J Svedlund, B B Toner, W E Whitehead Chair, Committee on Psychosocial
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514
 Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Functional GI Disorders: What's in a name? Douglas A. Drossman, MD This article was originally published in the
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Functional GI Disorders: What's in a name? Douglas A. Drossman, MD This article was originally published in the
Irritable Bowel Syndrome
 Irritable Bowel Syndrome Functional gastrointestinal disorders Definition A variable combination of chronic or recurrent gastrointestinal symptoms (attributed to the pharynx, esophagus, stomach, biliary
Irritable Bowel Syndrome Functional gastrointestinal disorders Definition A variable combination of chronic or recurrent gastrointestinal symptoms (attributed to the pharynx, esophagus, stomach, biliary
Irritable bowel syndrome (IBS) is a ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome
 ... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
... PRESENTATION... Defining and Diagnosing Irritable Bowel Syndrome Based on a presentation by Marvin M. Schuster, MD Presentation Summary Approximately 20% of the general population has irritable bowel
SUPPLEMENTARY INFORMATION Associated with
 Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
Table1: Rome III and Rome IV diagnostic criteria for IBS, functional constipation and functional dyspepsia. Rome III diagnostic criteria 1,2 Rome IV diagnostic criteria 3,4 Diagnostic criteria for IBS
IBS - Definition. Chronic functional disorder of GI generally characterized by:
 IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
IBS - Definition Chronic functional disorder of GI generally characterized by: 3500 3000 No. of Publications 2500 2000 1500 1000 Irritable Bowel syndrome Irritable Bowel Syndrome 500 0 1968-1977 1978-1987
Weekly Prevalence of Symptoms USA vs. Colombia
 THE OVERLAP BETWEEN INFLAMMATORY BOWEL DISEASE AND FUNCTIONAL GASTROINTESTINAL DISORDERS: CHALLENGES AND TREATMENT IMPLICATIONS Miguel Saps, MD Professor of Pediatrics, Ohio State University Director of
THE OVERLAP BETWEEN INFLAMMATORY BOWEL DISEASE AND FUNCTIONAL GASTROINTESTINAL DISORDERS: CHALLENGES AND TREATMENT IMPLICATIONS Miguel Saps, MD Professor of Pediatrics, Ohio State University Director of
Functional bowel disorders and functional abdominal pain
 Gut 1999;45(Suppl II):II43 II47 II43 Chair, Committee on Functional Bowel Disorders and Functional Abdominal Pain, Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal
Gut 1999;45(Suppl II):II43 II47 II43 Chair, Committee on Functional Bowel Disorders and Functional Abdominal Pain, Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal
The Role of Food in the Functional Gastrointestinal Disorders
 The Role of Food in the Functional Gastrointestinal Disorders H. Vahedi, MD. Gastroentrologist Associate professor of medicine DDRI 92.4.27 vahedi@ams.ac.ir Disorder Sub-category A. Oesophageal disorders
The Role of Food in the Functional Gastrointestinal Disorders H. Vahedi, MD. Gastroentrologist Associate professor of medicine DDRI 92.4.27 vahedi@ams.ac.ir Disorder Sub-category A. Oesophageal disorders
Irritable Bowel Syndrome Now. George M. Logan, MD Friday, May 5, :35 4:05 PM
 Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
Irritable Bowel Syndrome Now George M. Logan, MD Friday, May 5, 2017 3:35 4:05 PM Dr. Logan indicated no potential conflict of interest to this presentation. He does not intend to discuss any unapproved/investigative
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions
 PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
PELVIC PAIN : Gastroenterological Conditions Departman Tarih Prof. A. Melih OZEL, MD Department of Gastroenterology Anadolu Medical Center Hospital Gebze Kocaeli - TURKEY Presentation plan 15 min. Introduction
Prevalence of irritable bowel syndrome according to different diagnostic criteria in a non-selected adult population
 https://helda.helsinki.fi Prevalence of irritable bowel syndrome according to different diagnostic criteria in a non-selected adult population Hillilä, M. T. 2004-08-01 Hillilä, M T & Färkkilä, MA 2004,
https://helda.helsinki.fi Prevalence of irritable bowel syndrome according to different diagnostic criteria in a non-selected adult population Hillilä, M. T. 2004-08-01 Hillilä, M T & Färkkilä, MA 2004,
Agreed by Gastroenterology Drafting Group May Adopted by CHMP for release for consultation 24 May Start of public consultation 8 June 2012
 1 2 3 24 May 2012 EMA/CHMP/172616/2012 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 7 Concept paper on the revision of the CHMP points to consider on the evaluation of medicinal products
1 2 3 24 May 2012 EMA/CHMP/172616/2012 Committee for Medicinal Products for Human Use (CHMP) 4 5 6 7 Concept paper on the revision of the CHMP points to consider on the evaluation of medicinal products
Functionele Maagdarmklachten als Stoornissen van Gut-Brain Interacties Leiden alle wegen naar Rome IV?
 Functionele Maagdarmklachten als Stoornissen van Gut-Brain Interacties Leiden alle wegen naar Rome IV? Lukas Van Oudenhove, MD, PhD Assistant Professor (KU Leuven Special Research Fund) Laboratory for
Functionele Maagdarmklachten als Stoornissen van Gut-Brain Interacties Leiden alle wegen naar Rome IV? Lukas Van Oudenhove, MD, PhD Assistant Professor (KU Leuven Special Research Fund) Laboratory for
David Leff, DO. April 13, Disclosure. I have the following financial relationships to disclosure:
 David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
David Leff, DO AOMA 94 th Annual Convention April 13, 2016 Disclosure I have the following financial relationships to disclosure: Speaker s Bureau: Allergan Labs, Takeda Pharmaceutical, Valeant Pharmaceutical
FUNCTIONAL DISORDERS TREATMENT ADVANCES. Dr. Adriana Lazarescu MD FRCPC Director GI Motility Lab, Edmonton Associate Professor University of Alberta
 FUNCTIONAL DISORDERS TREATMENT ADVANCES Dr. Adriana Lazarescu MD FRCPC Director GI Motility Lab, Edmonton Associate Professor University of Alberta Name: Dr. Adriana Lazarescu Conflict of Interest Disclosure
FUNCTIONAL DISORDERS TREATMENT ADVANCES Dr. Adriana Lazarescu MD FRCPC Director GI Motility Lab, Edmonton Associate Professor University of Alberta Name: Dr. Adriana Lazarescu Conflict of Interest Disclosure
A Guide to Gastrointestinal Motility Disorders
 A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord André Smout Jan Tack A Guide to Gastrointestinal Motility Disorders Albert J. Bredenoord Gastroenterology and Hepatology Academic Medical
Microbiome GI Disorders
 Microbiome GI Disorders Prof. Ram Dickman Neurogastroenterology Unit Rabin Medical Center Israel 1 Key Points Our gut microbiota Were to find them? Symbiosis or Why do we need them? Dysbiosis or when things
Microbiome GI Disorders Prof. Ram Dickman Neurogastroenterology Unit Rabin Medical Center Israel 1 Key Points Our gut microbiota Were to find them? Symbiosis or Why do we need them? Dysbiosis or when things
Prevalence of irritable bowel syndrome in Japan: Internet survey using Rome III criteria
 ORIGINAL RESEARCH Prevalence of irritable bowel syndrome in Japan: Internet survey using Rome III criteria Hiroto Miwa Division of Upper Gastroenterology, Department of Internal Medicine, Hyogo College
ORIGINAL RESEARCH Prevalence of irritable bowel syndrome in Japan: Internet survey using Rome III criteria Hiroto Miwa Division of Upper Gastroenterology, Department of Internal Medicine, Hyogo College
J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: /jnm Journal of Neurogastroenterology and Motility
 ㅋ JNM J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: 10.5056/jnm.2011.17.3.279 Journal of Neurogastroenterology and Motility Original Article Functional Gastrointestinal Disorders Diagnosed
ㅋ JNM J Neurogastroenterol Motil, Vol. 17 No. 3 July, 2011 DOI: 10.5056/jnm.2011.17.3.279 Journal of Neurogastroenterology and Motility Original Article Functional Gastrointestinal Disorders Diagnosed
Post-infectious gastrointestinal symptoms after acute Giardiasis. A 1-year follow-up in general practice
 Family Practice Advance Access published March 22, 2010 Family Practice 2010; 0:1 5 doi:10.1093/fampra/cmq005 Ó The Author 2010. Published by Oxford University Press. All rights reserved. For permissions,
Family Practice Advance Access published March 22, 2010 Family Practice 2010; 0:1 5 doi:10.1093/fampra/cmq005 Ó The Author 2010. Published by Oxford University Press. All rights reserved. For permissions,
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
June By: Reza Gholami
 ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
ACG/CAG guideline on Management of Dyspepsia June 2017 By: Reza Gholami DEFINITION OF DYSPEPSIA AND SCOPE OF THE GUIDELINE Dyspepsia was originally defined as any symptoms referable to the upper gastrointestinal
IBS: overview and assessment of pain outcomes and implications for inclusion criteria
 IBS: overview and assessment of pain outcomes and implications for inclusion criteria William D. Chey, MD Professor of Medicine University of Michigan What is the Irritable Bowel Syndrome Symptom based
IBS: overview and assessment of pain outcomes and implications for inclusion criteria William D. Chey, MD Professor of Medicine University of Michigan What is the Irritable Bowel Syndrome Symptom based
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
MANAGEMENT OF VISCERAL PAIN
 MANAGEMENT OF VISCERAL PAIN William D. Chey, MD, FACG Professor of Medicine University of Michigan 52 year old female with abdominal pain 5 year history of persistent right sided burning/sharp abdominal
MANAGEMENT OF VISCERAL PAIN William D. Chey, MD, FACG Professor of Medicine University of Michigan 52 year old female with abdominal pain 5 year history of persistent right sided burning/sharp abdominal
Biofeedback for Pelvic Floor Disorders and Incontinence
 The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
The UNC Center for Functional GI & Motility Disorders www.med.unc.edu/ibs Biofeedback for Pelvic Floor Disorders and Incontinence Olafur S. Palsson, Psy.D. Associate Professor of Medicine UNC Center for
Chronic Abdominal Pain. Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016
 Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
Chronic Abdominal Pain Dr. Robert B. Smith Tupelo Digestive Health Specialists August 26, 2016 Disclosures Speaker Bureau for Allergan Pharmaceuticals Abdominal Pain - Definitions Acute occurring for several
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
Alternating bowel pattern: what do people mean?
 Alimentary Pharmacology & Therapeutics Alternating bowel pattern: what do people mean? R. S. CHOUNG*, G. R. LOCKE III*, A. R. ZINSMEISTER, L.J.MELTONIIIà &N.J.TALLEY* *Dyspepsia Center and Division of
Alimentary Pharmacology & Therapeutics Alternating bowel pattern: what do people mean? R. S. CHOUNG*, G. R. LOCKE III*, A. R. ZINSMEISTER, L.J.MELTONIIIà &N.J.TALLEY* *Dyspepsia Center and Division of
2017 NEEDS ASSESSMENT SURVEY
 2017 NEEDS ASSESSMENT SURVEY Quick Overview: Educational Topic Findings The online 2017 Needs Assessment survey was programmed through SurveyMonkey and a personalized request to complete the questionnaire
2017 NEEDS ASSESSMENT SURVEY Quick Overview: Educational Topic Findings The online 2017 Needs Assessment survey was programmed through SurveyMonkey and a personalized request to complete the questionnaire
Outline. Definition (s) Epidemiology Pathophysiology Management With an emphasis on recent developments
 Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Chronic Dyspepsia Eamonn M M Quigley MD FRCP FACP MACG FRCPI Lynda K and David M Underwood Center for Digestive Disorders Houston Methodist Hospital Houston, Texas Outline Definition (s) Epidemiology Pathophysiology
Why does my stomach hurt? Exploring irritable bowel syndrome
 Why does my stomach hurt? Exploring irritable bowel syndrome By Flavio M. Habal, MD, PhD, FRCPC Case In this article: 1. What is IBS? A 45-year-old female is referred to your office with recurrent 2. How
Why does my stomach hurt? Exploring irritable bowel syndrome By Flavio M. Habal, MD, PhD, FRCPC Case In this article: 1. What is IBS? A 45-year-old female is referred to your office with recurrent 2. How
Functional disorders of the anus and rectum
 Gut 1999;45(Suppl II):II55 II59 II55 Functional disorders of the anus and rectum Chair, Committee on Functional Anorectal Disorders, Multinational Working Teams to Develop Diagnostic Criteria for Functional
Gut 1999;45(Suppl II):II55 II59 II55 Functional disorders of the anus and rectum Chair, Committee on Functional Anorectal Disorders, Multinational Working Teams to Develop Diagnostic Criteria for Functional
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Irritable Bowel Syndrome and Mood Disorders Pedro Ramos, University of Louisville, Louisville, KY
 Paper P06-2009 Irritable Bowel Syndrome and Mood Disorders Pedro Ramos, University of Louisville, Louisville, KY ABSTRACT This case study describes the use of SAS technology in streamlining cross-sectional
Paper P06-2009 Irritable Bowel Syndrome and Mood Disorders Pedro Ramos, University of Louisville, Louisville, KY ABSTRACT This case study describes the use of SAS technology in streamlining cross-sectional
Medical Policy. MP Ingestible ph and Pressure Capsule
 Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
Medical Policy BCBSA Ref. Policy: 2.01.81 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 2.01.20 Esophageal ph Monitoring 6.01.33 Wireless Capsule Endoscopy as a
FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE
 FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE ETHELLE JEANETTE BENNETT BA (HONS) A thesis submitted in fulfilment of the requirements
FUNCTIONAL GASTROINTESTINAL DISORDERS: RELATIONS BETWEEN PSYCHOSOCIAL FACTORS, SYMPTOMS AND SENSORIMOTOR DISTURBANCE ETHELLE JEANETTE BENNETT BA (HONS) A thesis submitted in fulfilment of the requirements
IBS and Functional GI Disorders (FGIDs)
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/ibs-and-functional-gi-disorders-fgids/7424/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/gi-insights/ibs-and-functional-gi-disorders-fgids/7424/
Common Gastrointestinal Problems in the Elderly
 Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Common Gastrointestinal Problems in the Elderly Brian Viviano, D.O. Objectives Understand the pathophysiology, clinical manifestations, diagnosis and management of GI diseases of the elderly. Differentiate
Gastrointestinal Society 2016 SURVEY RESULTS
 Gastrointestinal Society 2016 SURVEY RESULTS Irritable Bowel Syndrome (IBS) The GI (Gastrointestinal) Society represents Canadians living with gastrointestinal diseases and disorders including those who
Gastrointestinal Society 2016 SURVEY RESULTS Irritable Bowel Syndrome (IBS) The GI (Gastrointestinal) Society represents Canadians living with gastrointestinal diseases and disorders including those who
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 6 April 2011
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 6 April 2011 METEOXANE, capsules B/60 (CIP code: 306 693-3) Applicant: IPRAD Simethicone Hydrated phloroglucinol ATC
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 6 April 2011 METEOXANE, capsules B/60 (CIP code: 306 693-3) Applicant: IPRAD Simethicone Hydrated phloroglucinol ATC
PATIENTS WITH IBS. ESSIC 2008 Annual Meeting Rome. Irritable bowel syndrome and/in BPS/IC Enrico Corazziari 1 IRRITABLE BOWEL SYNDROME AND/IN BPS/IC
 IRRITABLE BOWEL SYNDROME AND/IN BPS/IC Enrico Corazziari A Dynamic MRI B Enrico Corazziari Gastroenterologia A Dipartimento di Scienze Cliniche Università degli Studi di Roma Sapienza enrico.corazziari@uniroma1.it
IRRITABLE BOWEL SYNDROME AND/IN BPS/IC Enrico Corazziari A Dynamic MRI B Enrico Corazziari Gastroenterologia A Dipartimento di Scienze Cliniche Università degli Studi di Roma Sapienza enrico.corazziari@uniroma1.it
Guideline for a Starters in Reviewing. a Journal for the J Neurogastroenterol Motil
 Guideline for a Starters in Reviewing a Journal for the J Neurogastroenterol Motil Review process of J Neurogastroenterol Motil Authors Submit a manuscript to JNM homepage. Manuscript editor Check a manuscript
Guideline for a Starters in Reviewing a Journal for the J Neurogastroenterol Motil Review process of J Neurogastroenterol Motil Authors Submit a manuscript to JNM homepage. Manuscript editor Check a manuscript
Entrustable Professional Activity
 Entrustable Professional Activity 1. Title: Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Description of Activity Pediatric
Entrustable Professional Activity 1. Title: Care for infants, children, and adolescents with common outpatient GI, liver/biliary, pancreatic and nutritional issues 2. Description of Activity Pediatric
WOMEN WITH IRRITABLE BOWEL SYNDROME ACCORDING TO ROME II CRITERIA IN JORDAN
 Original Article WOMEN WITH IRRITABLE BOWEL SYNDROME ACCORDING TO ROME II CRITERIA IN JORDAN Kassab Harfoushi 1 ABSTRACT Objectives: To characterize the possible risk factors, clinical features and outcome
Original Article WOMEN WITH IRRITABLE BOWEL SYNDROME ACCORDING TO ROME II CRITERIA IN JORDAN Kassab Harfoushi 1 ABSTRACT Objectives: To characterize the possible risk factors, clinical features and outcome
The role of psychosocial factors in irritable bowel syndrome
 Baillière s Clinical Gastroenterology Vol. 13, No. 3, pp 437 452, 1999 6 BAILLIÈRE S BEST PRACTICE & RESEARCH The role of psychosocial factors in irritable bowel syndrome Bradley N. Gaynes* MD, MPH Assistant
Baillière s Clinical Gastroenterology Vol. 13, No. 3, pp 437 452, 1999 6 BAILLIÈRE S BEST PRACTICE & RESEARCH The role of psychosocial factors in irritable bowel syndrome Bradley N. Gaynes* MD, MPH Assistant
ACG Clinical Guideline: Management of Benign Anorectal Disorders
 ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
ACG Clinical Guideline: Management of Benign Anorectal Disorders Arnold Wald, MD, MACG 1, Adil E. Bharucha, MBBS, MD 2, Bard C. Cosman, MD, MPH, FASCRS 3 and William E. Whitehead, PhD, MACG 4 1 Division
Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders.
 Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders. SmartPill benefits your practice: Convenient performed right in your office Test standardization Provides direct
Our evidence. Your expertise. SmartPill : The data you need to evaluate motility disorders. SmartPill benefits your practice: Convenient performed right in your office Test standardization Provides direct
Presenter. Irritable Bowel Syndrome. Objectives. Introduction. Rome Criteria. Irritable Bowel Syndrome 2/28/2018
 Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Presenter Irritable Bowel Syndrome Current evidence for diagnosis & management Julie Daniels DNP, CNM Assistant Professor Course Coordinator of Primary Care of Women Faculty at Frontier Nursing University
Epidemiology and Impact of IBS
 Epidemiology and Impact of IBS Speaker: Nicholas Talley Mayo Clinic Jacksonville, FL Epidemiology and Impact of IBS What is the worldwide prevalence of IBS? What is the natural history of IBS? What is
Epidemiology and Impact of IBS Speaker: Nicholas Talley Mayo Clinic Jacksonville, FL Epidemiology and Impact of IBS What is the worldwide prevalence of IBS? What is the natural history of IBS? What is
There are clues to help to decide if the bellyache is a medical problem:
 Bellyaches in Children Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New Orleans, Louisiana By: Paul Hyman,
Bellyaches in Children Pediatric and Adolescent Gastrointestinal Motility & Pain Program Department of Pediatrics, Louisiana State University Health Sciences Center, New Orleans, Louisiana By: Paul Hyman,
A Prospective Assessment of Bowel Habit in Irritable Bowel Syndrome in Women: Defining an Alternator
 GASTROENTEROLOGY 2005;128:580 589 A Prospective Assessment of Bowel Habit in Irritable Bowel Syndrome in Women: Defining an Alternator DOUGLAS A. DROSSMAN,* CAROLYN B. MORRIS,* YUMING HU,* BRENDA B. TONER,
GASTROENTEROLOGY 2005;128:580 589 A Prospective Assessment of Bowel Habit in Irritable Bowel Syndrome in Women: Defining an Alternator DOUGLAS A. DROSSMAN,* CAROLYN B. MORRIS,* YUMING HU,* BRENDA B. TONER,
IBS is associated with an increased incidence of psychological
 Does Depression Influence Symptom Severity in Irritable Bowel Syndrome? Case Study of a Patient With Irritable Bowel Syndrome and Bipolar Disorder CATHERINE CRANE, BA, MARYANNE MARTIN, MA, DPHIL, DEREK
Does Depression Influence Symptom Severity in Irritable Bowel Syndrome? Case Study of a Patient With Irritable Bowel Syndrome and Bipolar Disorder CATHERINE CRANE, BA, MARYANNE MARTIN, MA, DPHIL, DEREK
Digestion: Small and Large Intestines Pathology
 Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
fever a persistent unexplained change in bowel habit in somebody over 50 years of age a family history of bowel or ovarian cancer.
 If you have had these symptoms for some time, if they come and go but never completely go away, then go and see your doctor. In practice, IBS is a diagnosis of exclusion. There is no test or marker that
If you have had these symptoms for some time, if they come and go but never completely go away, then go and see your doctor. In practice, IBS is a diagnosis of exclusion. There is no test or marker that
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders What are functional GI disorders?
 The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD and Kellie Bunn, PA-C What are functional GI
The Use of Antidepressants in the Treatment of Irritable Bowel Syndrome and Other Functional GI Disorders Christine B. Dalton, PA-C Douglas A. Drossman, MD and Kellie Bunn, PA-C What are functional GI
Functional Dyspepsia
 Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
Functional Dyspepsia American College of Gastroenterology Boston Massachusetts, June 2015 Brian E. Lacy, PhD, MD, FACG Professor of Medicine Geisel School of Medicine at Dartmouth Chief, Section of Gastroenterology
WHAT EVERYONE SHOULD KNOW ABOUT GASTROINTESTINAL DISORDERS IN WOMEN. By Robyn G. Karlstadt, M.D., FACG
 WHAT EVERYONE SHOULD KNOW ABOUT GASTROINTESTINAL DISORDERS IN WOMEN By Robyn G. Karlstadt, M.D., FACG Originally published in October 2002. Updated by Dr. Robyn G. Karlstadt, M.D., MACG in April 2007.
WHAT EVERYONE SHOULD KNOW ABOUT GASTROINTESTINAL DISORDERS IN WOMEN By Robyn G. Karlstadt, M.D., FACG Originally published in October 2002. Updated by Dr. Robyn G. Karlstadt, M.D., MACG in April 2007.
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
IBS. Patient INFO. A Guide to Irritable Bowel Syndrome
 Patient INFO IBS A Guide to Irritable Bowel Syndrome The information provided by the AGA Institute is not medical advice and should not be considered a replacement for seeing a medical professional. About
Patient INFO IBS A Guide to Irritable Bowel Syndrome The information provided by the AGA Institute is not medical advice and should not be considered a replacement for seeing a medical professional. About
A Case of Nutcracker Esophagus Associated with Chest Pain and Antidepressant Treatment
 2001 ; 7 : 227-232 1 *, * * * * * * * = Abstract = A Case of Nutcracker Esophagus Associated with Chest Pain and Antidepressant Treatment Suck Chei Choi, M.D.*, Sang Yeol Lee, M.D., Ji Hun Choi, M.D.*,
2001 ; 7 : 227-232 1 *, * * * * * * * = Abstract = A Case of Nutcracker Esophagus Associated with Chest Pain and Antidepressant Treatment Suck Chei Choi, M.D.*, Sang Yeol Lee, M.D., Ji Hun Choi, M.D.*,
Diagnosing and Managing IBS in IBD Patients. September 2012
 Diagnosing and Managing IBS in IBD Patients September 2012 Professor David S Sanders Consultant Gastroenterologist Royal Hallamshire Hospital & University of Sheffield Patient Comes to see you with GI
Diagnosing and Managing IBS in IBD Patients September 2012 Professor David S Sanders Consultant Gastroenterologist Royal Hallamshire Hospital & University of Sheffield Patient Comes to see you with GI
Non-Ulcer Dyspepsia: what is it? What can we do with these patients? Overview. Dyspepsia Definition. Functional Dyspepsia. Dyspepsia the Basics
 Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
Non-Ulcer : what is it? What can we do with these patients? Temporal Changes and Geographic Variations in Developing Peptic Ulcer Disease Gastric Cancer 1900 Eamonn M M Quigley MD FACG Alimentary Pharmabiotic
Diagnosis and Treatment of Irritable Bowel Syndrome
 Special Issue Diagnosis and Treatment of Irritable Bowel Syndrome Myung Gyu Choi, M.D. Department of Internal Medicine The Catholic University of Korea, College of Medicine Kangnam St. Mary's Hospital
Special Issue Diagnosis and Treatment of Irritable Bowel Syndrome Myung Gyu Choi, M.D. Department of Internal Medicine The Catholic University of Korea, College of Medicine Kangnam St. Mary's Hospital
F A M N O P R S ! D !
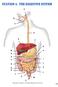 A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
A B C D E F A M N O P Q G H I J R S T U V 595 W http://www.encognitive.com/images/digestive-system-2.jpg K L M A N B C O P D E F G D Q R H S I J K http://apbrwww5.apsu.edu/thompsonj/anatomy%20&%20physiology/2020/2020%20exam%20reviews/exam%203/colon%20diagram.jpgd
Diagnostic value of the Manning criteria in irritable bowel syndrome
 Gut, 1990, 31, 77-81 Diagnostic value of the Manning criteria in irritable bowel syndrome 77 N J Talley, S F Phillips, L J Melton, C Mulvihill, C Wiltgen, A R Zinsmeister Gastroenterology Unit, Mayo Clinic
Gut, 1990, 31, 77-81 Diagnostic value of the Manning criteria in irritable bowel syndrome 77 N J Talley, S F Phillips, L J Melton, C Mulvihill, C Wiltgen, A R Zinsmeister Gastroenterology Unit, Mayo Clinic
The role of psychological and biological factors in postinfective gut dysfunction
 400 Gut 1999;44:400 406 Gastrointestinal Motility Unit, University of SheYeld, Northern General Hospital, SheYeld S5 7AU, UK K-A Gwee Y-L Leong N W Read Department of Infectious Diseases, Royal Hallamshire
400 Gut 1999;44:400 406 Gastrointestinal Motility Unit, University of SheYeld, Northern General Hospital, SheYeld S5 7AU, UK K-A Gwee Y-L Leong N W Read Department of Infectious Diseases, Royal Hallamshire
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary
 Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
Xifaxan, Lotronex and Viberzi Prior Authorization and Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1,2 Lotronex (alosetron) a Indication For women with severe diarrheapredominant irritable
SERUM CYTOKINES ARE ELEVATED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME (IBS) BUT LARGELY UNRELATED TO SYMPTOM CHARACTERISTICS
 SERUM CYTOKINES ARE ELEVATED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME (IBS) BUT LARGELY UNRELATED TO SYMPTOM CHARACTERISTICS SEAN M. P. BENNET 1, OLAFUR PALSSON 2., WILLIAM E WHITEHEAD 2., DAVID A BARROW
SERUM CYTOKINES ARE ELEVATED IN PATIENTS WITH IRRITABLE BOWEL SYNDROME (IBS) BUT LARGELY UNRELATED TO SYMPTOM CHARACTERISTICS SEAN M. P. BENNET 1, OLAFUR PALSSON 2., WILLIAM E WHITEHEAD 2., DAVID A BARROW
Is one of the most common chronic disorders. causing patients to seek medical treatment.
 ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ILOs After this lecture you should be able to : Define IBS Identify causes and risk factors of IBS Determine the appropriate therapeutic options for IBS Is one of the most common chronic disorders causing
ALMIRALL AND IRONWOOD ANNOUNCE POSITIVE RESULTS FROM A PHASE 3 TRIAL WITH LINACLOTIDE IN PATIENTS WITH IRRITABLE BOWEL SYNDROME WITH CONSTIPATION
 FOR IMMEDIATE RELEASE Ironwood Contact: Almirall Contact: Susan Brady Ketchum Pleon Corporate Communications Amanda Sefton 617.621.8304 +44 (0) 207.611.3653 sbrady@ironwoodpharma.com amanda.sefton@ketchumpleon.com
FOR IMMEDIATE RELEASE Ironwood Contact: Almirall Contact: Susan Brady Ketchum Pleon Corporate Communications Amanda Sefton 617.621.8304 +44 (0) 207.611.3653 sbrady@ironwoodpharma.com amanda.sefton@ketchumpleon.com
Perceptual responses in patients with inflammatory and functional bowel disease
 Gut 2;47:497 55 497 Perceptual responses in patients with inflammatory and functional bowel disease L Chang, J Munakata, E A Mayer, M J Schmulson, T D Johnson, C N Bernstein, L Saba, B NaliboV, P A Anton,
Gut 2;47:497 55 497 Perceptual responses in patients with inflammatory and functional bowel disease L Chang, J Munakata, E A Mayer, M J Schmulson, T D Johnson, C N Bernstein, L Saba, B NaliboV, P A Anton,
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 4 October, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm15016 Original Article Validity
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 21 No. 4 October, 2015 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm15016 Original Article Validity
Visceral Pain-Related Anxiety: Role of Glucocorticoids
 Visceral Pain-Related Anxiety: Role of Glucocorticoids Brent Myers, Ph.D. Department of Psychiatry University of Cincinnati Center for Neuroscience University of Oklahoma Health Sciences Center Irritable
Visceral Pain-Related Anxiety: Role of Glucocorticoids Brent Myers, Ph.D. Department of Psychiatry University of Cincinnati Center for Neuroscience University of Oklahoma Health Sciences Center Irritable
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function
 Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Viscous Fluid Retention: A New Method for Evaluating Anorectal Function Michael Srensen, M.D., Tine Tetzschner, M.D., le 0. Rasmussen, M.D., John Christiansen, M.D. From the Department of Surgery D, Glostrup
Irritable Bowel Syndrome and Chronic Constipation. Treatment of IBS. Susan Lucak, M.D. Columbia University Medical Center
 Ti tl e s l i d e - p a rt 1 Irritable Bowel Syndrome and Chronic Constipation Susan Lucak, M.D. Columbia University Medical Center Treatment of IBS Abdominal pain / discomfort Antispasmodics Antidepressants
Ti tl e s l i d e - p a rt 1 Irritable Bowel Syndrome and Chronic Constipation Susan Lucak, M.D. Columbia University Medical Center Treatment of IBS Abdominal pain / discomfort Antispasmodics Antidepressants
IRRITABLE BOWEL SYNDROME Dr E Lalor, MB ChB, FRCPC 2016 (but written before Rome IV see Gastroenterology, May 2016).
 IRRITABLE BOWEL SYNDROME Dr E Lalor, MB ChB, FRCPC 2016 (but written before Rome IV see Gastroenterology, May 2016). Irritable bowel syndrome (IBS) is one of the functional GI (gastro-intestinal) disorders,
IRRITABLE BOWEL SYNDROME Dr E Lalor, MB ChB, FRCPC 2016 (but written before Rome IV see Gastroenterology, May 2016). Irritable bowel syndrome (IBS) is one of the functional GI (gastro-intestinal) disorders,
IBS The Physiologist s Perspective
 IBS The Physiologist s Perspective Dr Anthony R. Hobson PhD Consultant Clinical Scientist, London The Functional Gut Clinic Reclaiming the F word The f-word functional has become a by-word for failure
IBS The Physiologist s Perspective Dr Anthony R. Hobson PhD Consultant Clinical Scientist, London The Functional Gut Clinic Reclaiming the F word The f-word functional has become a by-word for failure
Functional esophageal disorders
 Gut 1999;45(Suppl II):II31 II36 II31 Chair, Committee on Functional Esophageal Disorders, Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal Disorders (Rome II),
Gut 1999;45(Suppl II):II31 II36 II31 Chair, Committee on Functional Esophageal Disorders, Multinational Working Teams to Develop Diagnostic Criteria for Functional Gastrointestinal Disorders (Rome II),
Psycho-pharmacologic Therapy. Objectives
 Psycho-pharmacologic Therapy for Functional Bowel Disorders John J. Hutchings, M.D. Assistant Professor of Medicine and Psychiatry Louisiana i State t University it School of Medicine i Department of Medicine
Psycho-pharmacologic Therapy for Functional Bowel Disorders John J. Hutchings, M.D. Assistant Professor of Medicine and Psychiatry Louisiana i State t University it School of Medicine i Department of Medicine
Prof. Dr. Mufti Munsurar Rahman Dept. of Medicine Enam Medical College Hospital
 Prof. Dr. Mufti Munsurar Rahman Dept. of Medicine Enam Medical College Hospital Functional constipation : prevalence and life style factors in a district of Bangladesh Perveen I, Rahman MM, Saha M, Parvin
Prof. Dr. Mufti Munsurar Rahman Dept. of Medicine Enam Medical College Hospital Functional constipation : prevalence and life style factors in a district of Bangladesh Perveen I, Rahman MM, Saha M, Parvin
The Importance of Hypochondriasis in Dyspeptic Patients
 American Journal of Psychology and Behavioral Sciences 2018; 5(1): 1-9 http://www.openscienceonline.com/journal/ajpbs ISSN: 2381-5957 (Print); ISSN: 2381-5965 (Online) The Importance of Hypochondriasis
American Journal of Psychology and Behavioral Sciences 2018; 5(1): 1-9 http://www.openscienceonline.com/journal/ajpbs ISSN: 2381-5957 (Print); ISSN: 2381-5965 (Online) The Importance of Hypochondriasis
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D.
 Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Gastrointestinal Motility 2: Intestinal and Colonic Motility Jack Grider, Ph.D. OBJECTIVES: 1. Contrast the types of motility in the small intestine. 2. Describe the neural circuits that mediate peristalsis.
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514
 Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily
Drossman Gastroenterology 55 Vilcom Center Drive Boyd Hall, Suite 110 Chapel Hill, NC 27514 Normal Gastrointestinal Motility and Function "Motility" is an unfamiliar word to many people; it is used primarily
Irritable bowel syndrome (IBS) is characterized by recurrent
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:321 328 Symptom Severity but Not Psychopathology Predicts Visceral Hypersensitivity in Irritable Bowel Syndrome PATRICK P. J. VAN DER VEEK,* YANDA R. VAN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:321 328 Symptom Severity but Not Psychopathology Predicts Visceral Hypersensitivity in Irritable Bowel Syndrome PATRICK P. J. VAN DER VEEK,* YANDA R. VAN
Validated questionnaire on diagnosis and symptom severity for functional constipation in the Chinese population
 Aliment Pharmacol Ther 2005; 22: 483 488. doi: 10.1111/j.1365-2036.2005.02621.x Validated questionnaire on diagnosis and symptom severity for functional constipation in the Chinese population A. O. O.
Aliment Pharmacol Ther 2005; 22: 483 488. doi: 10.1111/j.1365-2036.2005.02621.x Validated questionnaire on diagnosis and symptom severity for functional constipation in the Chinese population A. O. O.
