Post-operative impaired vocal cord. mobility related to cardiovascular surgery
|
|
|
- Alexander Henderson
- 6 years ago
- Views:
Transcription
1 Post-operative impaired vocal cord mobility related to cardiovascular surgery A study to the characteristics of cardiovascular surgery induced impairment of the vocal cords mobility Master Thesis Clinical Language Speech and Hearing Sciences Utrecht University, July 2011 Student: Eska Schuijling, Supervisor: Research institute : Prof. dr. P.H. Dejonckere Utrecht University, UMCU St. Antonius Hospital, Nieuwegein/Utrecht
2 ABSTRACT Background: injury to the recurrent laryngeal nerve during cardio-thoracic surgery is a well described phenomenon with an incidence of 1-2%, but is overlooked as a complication during admission. It may lead to an impaired mobility of the vocal cords and cause physical complaints like hoarseness, dyspnoea or aspiration and have a negative influence on the patient s quality of life. Aim: the present study investigates impaired vocal cord mobility as a complication after cardiovascular surgery among 23 patients in a large non-academic hospital in the Netherlands. The study aims at determining whether there are any significant relationships between otorhinolaryngology data of the vocal cord impairment, general risk-factors and surgical characteristics of cardiovascular surgery. Results: no significant relationships have been found. However, certain variables in the dataset did occur significantly more often than others. Conclusions: general risk-factors or characteristics of cardiovascular surgery were not found to be statistically related to uni-/ bilaterality, side and severity of mobility impairment, position of the impaired vocal cord, and spontaneous recovery in this study. However, analysis of the dataset shows that impaired vocal cord mobility after cardiovascular surgery occurs significantly more frequently unilaterally than bilaterally, and significantly more frequently in patients who underwent open thorax surgery than in those who underwent a minimal invasive surgical procedure. Further research is required to determine potential risk-factors for a post-operative impaired vocal cord mobility. Keywords: impaired vocal cord mobility, cardiovascular surgery, post-operative. 2
3 1. INTRODUCTION 1.1. Impaired vocal cord mobility and cardiac-thoracic surgery Impaired vocal cord mobility is a commonly known disorder in the field of speech and language therapy because of the hoarseness it causes. Trauma to the motor component of the vocal cords, known to be the recurrent laryngeal nerve, may be inflicted in many different ways. One of the possible causes for injury to the recurrent laryngeal nerve is cardiac-thoracic surgery. Unfortunately, vocal cord impairment after surgical intervention in the chest is often overlooked as a cause of post-operative respiratory insufficiency or hoarseness, and laryngeal examination is rarely clinically performed on post-operative patients (Hamdan, Moukarbel, Farhat, & Obeid, 2002; Shafei, El-Kholy, Azmy, Ebrahim, & Al-Ebrahim, 1996). Physical recovery is the primary goal after surgery, but vocal cord immobility can decrease a patient s quality of life (Tomoda et al., 2008). Literature on thyroid surgery points out dysphonia, hoarseness, dyspnea, ineffective cough, glottal obstruction and aspiration as a result of reduced vocal cord motion (Tomoda et al., 2008; Kundra et al., 2010). Cardiac-thoracic literature takes injury to the recurrent laryngeal nerve seriously in account during surgery, but nonetheless attributes the complication to non-surgical mechanisms like tracheal intubation. Dysphonia is thereby not addressed as a complication due to post-operative impaired mobility of the vocal cords (Dimarakis & Protopapus, 2004; Hamdan et al., 2002). The true incidence of impaired vocal cord mobility after cardiac-thoracic surgery is hard to establish. First, a routine post-operative laryngeal examinations is lacking in most institutes. Second, there often is uncertainty about the exact cause of the nerve trauma. Studies have reported an incidence between 1-2%, primarily on patients with open-heart surgery. In some cases the nature of the cardiac procedure remained undisclosed. Cardiac-thoracic surgery in general did not seem to damage the recurrent 3
4 laryngeal nerve irreversibly, except for a few cases. (Dimarakis & Protopapus 2004; Hamdan et al., 2002; Shafei et al., 1996) Anatomic and surgical aspects related to the recurrent laryngeal nerve The ipsilateral recurrent laryngeal nerve branches from the vagus nerve in the lower neck and lies in the tracheo-oesophageal groove. It innervates most of the larynx muscles, except the cricothyroid, and functions as the main motor for the vocal cords. The left recurrent branch passes under the arch of the aorta before ascending. The right recurrent branch loops around the right subclavian artery (Dimarakis & Protopapus, 2004; Nayler & Mackey, 2001). This non-symmetrical anatomy has surgical significance (Dimarakis & Protopapus, 2004). The left recurrent nerve is known to have a higher risk for injury because of its long intrathoracic segment compared to the much shorter right sided course (Hamdan et al., 2002). Although the vagus nerve is nearly always well identified and removed from the operative field during primary cardiac surgery, the recurrent laryngeal nerve remains at risk for trauma caused by e.g. self retained retractors in median sternotomy (Nayler & Mackey, 2001) Mechanisms of nerve injury during cardiac-thoracic surgery. Various mechanisms have been identified as a possible cause for post-operative vocal cord impairment. In the event of open heart surgery, longitudinal lateral strain may be put on both subclavian arteries trough chest retractors, which may forces an indirect injury to both recurrent nerves (Dimarakis & Protopapus, 2004). Other indirect strain trauma may be caused by the use of an inappropriately sized endotracheal tube cuff during intubation or an unnatural head and neck position during surgery. Direct trauma may be inflicted by traumatic endotracheal and/or nasogastric intubation and 4
5 direct manipulation and retraction of the heart during the procedure. Progress in prevention of nerve injury during surgery has been accomplished for hypothermic nerve trauma with the usage of saline slush in the last decade to cool the body temperature down during open heart surgery, instead of using ice in the pleural cavity. This with markedly less hypodermic nerve trauma as result (Hamdan et al., 2002) Present study Previous studies suggest that impaired vocal cord mobility after cardio-thoracic surgery is a commonly known post-operative complication, with various incidences between 1-2% (Dimarakis & Protopapus 2004; Hamdan et al., 2002; Shafei et al., 1996), generally is of a temporary nature (Hamdan et al., 2002; Shafei et al., 1996) and occurs more often on the left-, than on the right side (Dimarakis & Protopapus 2004; Hamdan et al., 2002). Nevertheless, there is little specific information in these studies about the surrounding, and perhaps explanatory factors. No differentiation has been made between factors like, amongst others, age, comorbidity, degree of the lesion or duration of surgery. Some factors have been named individually in particular previous studies, but they were never combined in order to find a possible relationship to impaired vocal cord mobility. Likewise, the duration of the vocal cord impairment has not been subject of any of the research discussed above. There seem to be commonly accepted factors related to post operative impaired vocal cord mobility that have not been researched in a broader context. Working on the speech and language therapy department of the participating hospital, impaired vocal cord mobility has always been a personal interest. Unfortunately there is little specific research which may serve as background information in therapy and council information towards affected patients. Especially in a large hospital (880 beds) that is specialized in cardiothoracic surgery and where impaired vocal cord immobility as a post operative 5
6 complication of cardiovascular surgery is not thought to be uncommon, can such research may be of great value for both practitioners and patients. The present study therefore makes a start with investigating impaired vocal cord mobility as a complication after cardiovascular surgery among patients in a large non-academic hospital in the Netherlands and determines whether there are any significant relationships between the otorhinolaryngological data of the vocal cord impairment, general risk-factors, and surgical characteristics. It is hypothesized that the otorhinolaryngological data will especially correlate with surgical characteristics of the cardiovascular operation and perhaps generally known risk-factors. 2. METHOD 2.1 Participants All adult patients that have been formally diagnosed in St. Antonius Hospital with impaired vocal cord mobility as a post-operative complication after cardiovascular surgery between January 2005 and May 2011, were included in the study. A total of 23 patients were found, consisting of 16 males and 7 females Material The present study uses existing medical records from adult patients with clinically identified vocal cord impairment after cardiovascular surgery between January 2005 and May Patients that visited the otorhinolaryngology department in this period were automatically screened by a internal and reliable electronic system used in the hospital, that selected them all by their reported diagnose code. The patients that had been endoscopically diagnosed with impaired mobility of the vocal cords as a postoperative complication after cardiovascular surgery were included. No further criteria have been formulated and/or used. A total of 23 otorhinolaryngology patients have 6
7 been analysed in the study. Subsequently, their cardiovascular surgical reports have been closely examined using the patients individual electronic personal health records Design for data collection Independent variables were formed prior of the data collection. Table 1 shows an overview of the factors that have been filtered from the electronic personal health records of every participant. All retrieved data has been treated anonymously. Three major groups were formed for general, otorhinolaryngological and surgical characteristics, consisting specific parameters which have been analysed on the study population. The general parameters were based on generally known personal risk factors for surgical complications such as increasing age and the presence of comorbidity as smoking, diabetes mellitus, chronic lung diseases (e.g. COPD) and obesity. The otorhinolaryngology parameters have been chosen to match with widely used terms and available data within the hospital s otorhinolaryngology (endoscopic) examination reports. The surgical parameters were selected by using general terms found in surgical reports and patient information resources. Main category General parameters Otorhinolaryngology parameters Subcategories Age Sex Presence of comorbidity Uni,- bilaterally impaired Side of impairment Gradation of impairment Position of impaired vocal cord(s) Recovery of vocal cord mobility Surgical parameters Type of surgery Operation procedure Duration of surgical procedure Table 1: overview of investigated parameters and variables in present study 7
8 Surgical Otorhinolaryngology General 2.4. Statistical analysis The present study hypothesizes that the research variables are interdependent and that there is a significant relationship between post-operative impaired mobility of the vocal cords and one or more of the considered parameters. The null hypothesis on the contrary holds that there is not enough evidence for any plausible relationship. The collected data was analysed within a 2x2 cross table, as showed in table 2. To compare two unpaired independent variables, the non-parametric Fisher s exact test has been performed two-sided in SPSS 17.0 for every combination of two variables between the general parameter and otorhinolaryngology parameter, and between the surgical parameter and the otorhinolaryngology parameter Variable Label of value 1 2 Age < 65 years 65 years Sex Male Female Presence of comorbidity Yes No Uni,- bilaterally impaired Unilateral Bilateral Side of impairment Left Right Gradation of impairment Partial paresis Full paralysis Position of impaired vocal cord(s) (Para)mediate Intermediary Recovery of vocal cord mobility Yes No Type of surgery Heart surgery Carotid surgery Operation procedure Minimal invasive Open thorax Duration of surgical procedure < 5 hours 5 hours Table 2: overview of independent variables and their label values used in 2x2 parametric analysis conducted in present study 8
9 Surgical General Additional analysis of the independent variables has been conducted by way of a second Fisher s exact test to analyze whether some value labels in the dataset occurred significantly more frequently than others. The null hypothesis implied that the frequency distribution of the variables is equal to a theoretical distribution of 1/1, so that every value label was 50% present within the variable itself. All variables were analysed because of indistinct indications in the literature about possible frequency distributions. 3. RESULTS The analysis of the data does not indicate any significant relationschip between postoperative impaired vocal cord mobility and the independent variables conducted in this study. All p-values measured by the Fisher s exact tests exceeded the level of alpha (0.05) as shown in table 3. The null hypotheses is therefore accepted, no plausible relationship could be proven. Otorhinolaryngology Uni,- bilateral Side Gradation Position Recovery Age Sex Presence of comorbidity Type of surgery Operation procedure Duration of surgery Table 3: p-values Fisher s exact test of every independent variable combination between the general-, and surgical parameters and the otorhinolaryngology parameters. 9
10 For analysis of the frequency distribution for individual variables, the boundaries for dismissal of equal distribution were determined by a second 2-sided Fisher s exact test. The considered thresholds were on the safe side to analyze the present distribution quite conservative, with less probability for a Type-I error (falsepositives): N=23 < 4 - > 19 Because of missing data in two of the variables, the thresholds for these variables were computed on a different sample size. For the variables position of impaired vocal cord(s) and recovery of mobility the thresholds respectively were: N=20 < 4 - > 16 N=18 < 3 - > 15 The conducted boundaries computed by the Fisher s exact test showed significant difference for the variables unilateral and bilateral impairment of the vocal cord mobility and the operation procedure, as shown in table 4. The values found fell under and above the stated thresholds and were therefore statistically unevenly distributed. No statistical significance was found within the group of general parameters. Unilateral impaired vocal cord mobility was significantly more frequently observed than a bilateral impairment within the group of the otorhinolaryngology parameters. Finally, within the group of surgical parameters open thorax surgery occurred significantly more than minimal invasive operations. For the remaining variables the null hypothesis has been accepted because the distribution fell within the estimated range of equal distribution. 10
11 Surgical Otorhinolaryngology General Variable N Label of value Frequency Age 23 < 65 years 65 years Sex 23 Male Female Comorbidity 23 Yes No Uni,- bilaterally impaired* 23 Unilateral Bilateral Side of impairment 23 Left Right Gradation of impairment 23 Partial pareses Full paralysis Position of impaired vocal cord(s) 20 (Para)mediate Intermediary 13 7 Recovery of mobility 18 Yes No Type of surgery 23 Heart surgery Carotid surgery Operation procedure* 23 Minimal invasive Open thorax Duration of surgical procedure 23 < 5 hours 5 hours Table 4: Frequency overview of every independent variable and their value labels. * = statistical significantly frequency distribution (under/above 50%) 4. DISCUSSION The hypothesis of this study, that there would be statistical relationships between otolaryngological data and the conducted parameters, was not confirmed by its results. No significant relationship between any of the general-, and/or surgical variables and the presence of impaired vocal cord mobility as a post-operative complication could be established. 11
12 The research design of the present study encountered some limitations. It was not possible to compute the actual incidence of impaired vocal cord mobility as a postoperative complication of cardiovascular surgery, due to the lack of parametric data from the full population of patients undergoing cardiovascular surgery in the hospital. The screening and analysis of the full surgical population could therefore not be accomplished practically within the period of time. The true incidence is thought to be a object for future research. Due to the relatively small dataset, this study lacked sensitivity and was only able to significantly detect coarse relationships. This limitation may well have influenced the statistical results and, in all, made the null hypothesis difficult to decline. The presence of light and refined relationships between the variables could not be derived from the present study population. The small size of the dataset may be attributed to the relatively short hospitalization time in the participating hospital, which is generally only 7 to 11 days before dismissal or transfer to another hospital 1. Some signs of vocal cord immobility, like hoarseness, are considered as regular and nonthreatening post-operative symptoms for a cardiologist, due to e.g. fatigue and a decreased physical condition. A considerable amount of these patients show a reduced diaphragm function in speaking because of common dyspnoea, which may understandably reduce the vocal quality during phonation. Therefore patients with clinical impairment to the vocal cord mobility as a post-operative complication are not always referred to an otorhinolaryngologist during admission itself. Another explanation may be found in the geographical distribution of patients undergoing cardiovascular surgery. From the 23 patients that were selected in this study, 61% were from the province of Utrecht. The remaining 39% came from a range of four 1 From the annual year report cardiac-thoracic surgery department of the St. Antonius hospital 2005 and
13 different provinces in the Netherlands, knowing to be Friesland (9%), Noord-Brabant (13%), Drenthe (4%) and Gelderland (13%). It may be assumed that patients with e.g. persisting dysphonia, and not living in the district of Utrecht, will rather consult an otolaryngologist close to their residence. Out of nine patients who did not come from the province of Utrecht, only one was already known by the examining otorhinolaryngologist in connection to a different medical complaint in the past. Three were referred to a different otorhinolaryngologist in a hospital closer to their hometown for a later check-up after their first (polyclinic) evaluation of the vocal cords in the participating hospital, so no further information about the recovery was registered in the participating hospital s system. The five remaining patients were examined during dismissal and afterwards dismissed to another hospital in their own region with expected spontaneous recovery of the impaired vocal cords. These patients are very likely to undergo further otorhinolaryngological examination and/or treatment in this other hospital, when spontaneous recovery of the vocal cords mobility fails. It is therefore very plausible that a substantial amount of the patients with impaired vocal cord mobility after cardiovascular surgery in the participating hospital will visit a (general) practitioner closer to their residence, in the event the reduced vocal function persists for a certain time after hospital dismissal or for a during admission recommended check-up in a later stage. Some patients are not registered at the otorhinolaryngologist department of the participating hospital with impaired vocal cord mobility and could therefore not be included in the present study trough the applied method of data collection. In the analysis itself the number of original formulated value labels was restricted in order to comply with the requirements for a multinomial Chi-square analysis with more than 20% of the cells having an expected cell count of less than 5. The amount of value labels within the different variables had therefore been cut down to fit a 2x2 13
14 crosstab, so a Fisher s exact test could be conducted on the data. This made the study less specific than was originally intended and prevented that possible risk factors for a post-operative impaired vocal cord mobility could be explored closer. On the other hand, a larger variety of value labels could make a possible relationship even more refined and, consequently, even harder to verify statistically, unless a more extensive dataset is used. Although generalization on the basis of the statistical analysis was not possible, there was there no reason to suspect any specific bias in the dataset that would distinguish the dataset from the full population of patients with a post-operative impaired vocal cord mobility after cardiovascular surgery. It is therefore assumed that the research population was representative. To conclude, there was no substantiated link found between possible risk factors for a impaired vocal cord mobility and the presence of this post-operative complication. This was against the expectation of the present study and the stated research hypothesis. 5. CONCLUSION This study primarily aimed on vocal cord immobility as a complication after cardiovascular surgery. Possible relations between a range of general, otorhinolaryngological, and surgical parameters were researched. It was hypothesized that there would be a relationship between post-operative impaired vocal cord mobility and one or more of the considered parameters. The statistical analysis nevertheless does not demonstrate any significant relationship. The otorhinolaryngological variables; uni-/bilaterality, side and severity of mobility impairment, position of impaired vocal cords, and spontaneous recovery were not found to be related to any characteristics of cardiovascular surgery or general risk- 14
15 factors. The null hypothesis that stated that there is no relationship was therefore accepted. Further analysis of the frequency distribution within the individual variables was performed to determine whether this distribution was significantly equal to the theoretical distribution of probability (50%). The results showed that impaired vocal cord mobility after cardiovascular surgery occured significantly more frequently unilaterally than bilaterally, and significantly more frequently in patients who underwent open thorax surgery compared than in those who underwent a minimal invasive surgical procedure. Further research is required to determine potential riskfactors for a post-operative impaired vocal cord mobility. 6. RECOMMENDATIONS Further research is necessary to determine whether any significant relationship exists between cardiovascular surgery and post-operative impaired vocal cord mobility. Future studies are recommended to be conducted on a larger number of patients for more specificity. A multinomial Chi-square can then be performed on different combinations of parameters and with a greater variety of variable labels. The use of surgical records of cardiovascular patients without this complication should be collected to investigate the true incidence. Consequently, regression analysis can clarify the understanding of impaired vocal cord mobility in the context of specific conditions and thereby possible risk-factors. This would have great value in preoperative patient information, patient therapy, and council information towards affected patients. 15
16 7. ACKNOWLEDGMENTS This study could not have been accomplished successfully without the collaboration of the St. Antonius Hospital in Nieuwegein and Utrecht. I express my gratitude for providing me with full access to the required medical files, the cooperation, help and advice I received from colleagues in various departments and for providing a enjoyable work environment in the past two years. I thank my supervisor prof. dr. P.H. Dejonckere for his guidance, feedback, advice and expertise during this study. Special thanks are directed to my co-workers on the department of speech therapy for pointing me in the right direction every now and then and for their interest and support in this project. Finally I thank my fellow students for carrying out their enthusiasm for our profession, Ben and André for their critical feedback and advise for improvement, and my family for their infinite trust in my capacities and unconditional patience and encouragement during this period. 8. REFERENCES Cronenwett J., & Johnston, W. (2010) Rutherford s vascular surgery, volume one (7 th edition). Philadelphia: W.B Saunders Company. Dimarakis, I. & Protopapus, A. (2004) Vocal cord palsy as a complication of adult cardiac surgery: surgical correlations and analysis. European Journal of Cardiothoracic surgery 26; Hamdan, A., Moukarbel, R., Farhat, F., Obeid, M. (2002) Vocal cord paralysis after open heart surgery. European Journal of Cardio-thoracic surgery 21; Kundra, P., Kumar, V., Srinivasan, K., Gopalakrishnan, S., Krishnappa, S. (2010) Laryngoscopic techniques to assess vocal cord mobility following thyroid surgery. ANZ journal of surgery 11;
17 Naylor, A. & Mackey, W. (2001) Carotid artery surgery. A problem based approach. London: W.B Saunders. Shafei, H., El-Kholy, A., Azmy, S., Ebrahim, M., Al-Ebrahim, K. (1997) Vocal cord dysfunction after cardiac surgery: an overlooked complication. European Journal of Cardio-thoracic surgery 11; Tomoda, C., Hirokawa, Y., Uruno, T., Takamura, Y., Ito, Y., Miya, A., Kobayashi, K., Matsuzuka, F., Kuma, K., Miyauchi, A. (2006) Sensitivity and specificity of intraoperative recurrent laryngeal nerve stimulation test for predicting vocal cord palsy after thyroid surgery. Word Journal of Surgery 30;
New technologies in Endocrine Surgery
 New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
New technologies in Endocrine Surgery 1. Nerve monitoring 2. New technologies in Endocrine Surgery Jessica E. Gosnell MD Post graduate course in General Surgery March 28, 2012 1 2 Recurrent laryngeal nerve
Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation
 Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation G. Kurland, MD Children s Hospital of Pittsburgh Geoffrey.kurland@chp.edu 11/2014 Objectives Discuss
Laryngotracheal/Pulmonary Problems and the Mechanically Ventilated Patient: Pediatric Lung Transplantation G. Kurland, MD Children s Hospital of Pittsburgh Geoffrey.kurland@chp.edu 11/2014 Objectives Discuss
Innervation of the cricothyroid muscle by the recurrent laryngeal nerve
 ORIGINAL ARTICLE Innervation of the cricothyroid muscle by the recurrent laryngeal nerve Hiroo Masuoka, MD, PhD,* Akira Miyauchi, MD, PhD, Tomonori Yabuta, MD, PhD, Mitsuhiro Fukushima, MD, PhD, Akihiro
ORIGINAL ARTICLE Innervation of the cricothyroid muscle by the recurrent laryngeal nerve Hiroo Masuoka, MD, PhD,* Akira Miyauchi, MD, PhD, Tomonori Yabuta, MD, PhD, Mitsuhiro Fukushima, MD, PhD, Akihiro
Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10
 GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules
 Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
Long-term Follow-up for Patients with Papillary Thyroid Carcinoma Treated as Benign Nodules YASUHIRO ITO, TAKUYA HIGASHIYAMA, YUUKI TAKAMURA, AKIHIRO MIYA, KAORU KOBAYASHI, FUMIO MATSUZUKA, KANJI KUMA
Hoarseness. Common referral Hoarseness reflects any abnormality of normal phonation
 Hoarseness Kevin Katzenmeyer, MD Faculty Advisor: Byron J Bailey, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 24, 2001 Hoarseness Common referral
Hoarseness Kevin Katzenmeyer, MD Faculty Advisor: Byron J Bailey, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 24, 2001 Hoarseness Common referral
Superior Laryngeal Nerve Injury: Diagnosis and Management. Presented by: Nyall London October 10, 2014
 Superior Laryngeal Nerve Injury: Diagnosis and Management Presented by: Nyall London October 10, 2014 1 Case Presentation 49 year old male s/p right side approach anterior cervical discectomy and fusion
Superior Laryngeal Nerve Injury: Diagnosis and Management Presented by: Nyall London October 10, 2014 1 Case Presentation 49 year old male s/p right side approach anterior cervical discectomy and fusion
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital.
 Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Introduction. Kana Yoshioka 1 Akira Miyauchi. Minoru Kihara 2 Akihiro Miya
 World J Surg (2016) 40:2948 2955 DOI 10.1007/s00268-016-3634-7 ORIGINAL SCIENTIFIC REPORT Surgical Methods and Experiences of Surgeons did not Significantly Affect the Recovery in Phonation Following Reconstruction
World J Surg (2016) 40:2948 2955 DOI 10.1007/s00268-016-3634-7 ORIGINAL SCIENTIFIC REPORT Surgical Methods and Experiences of Surgeons did not Significantly Affect the Recovery in Phonation Following Reconstruction
Specialist Referral Service Willows Information Sheets. Laryngeal paralysis
 Specialist Referral Service Willows Information Sheets Laryngeal paralysis Laryngeal paralysis tends to affect middle aged and older animals, especially large breed dogs such as Labrador Retrievers, Golden
Specialist Referral Service Willows Information Sheets Laryngeal paralysis Laryngeal paralysis tends to affect middle aged and older animals, especially large breed dogs such as Labrador Retrievers, Golden
Respiratory System. Clinical notes. Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz)
 Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Objectives. Purpose. Conference Calls 2 hrs. Process 9/7/2013. Clinical Practice Guideline: Improving Voice Outcomes after Thyroid Surgery
 Objectives Clinical Practice Guideline: Improving Voice Outcomes after Thyroid Surgery 37 th Annual Congress & Nursing Symposium Vancouver, BC September 29, 2013 Carolyn Waddington RN MS FNP-C CORLN Explain
Objectives Clinical Practice Guideline: Improving Voice Outcomes after Thyroid Surgery 37 th Annual Congress & Nursing Symposium Vancouver, BC September 29, 2013 Carolyn Waddington RN MS FNP-C CORLN Explain
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September ISSN
 International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September-2014 1196 Pneumomediastinum and subcutaneous emphysema secondary to blunt laryngeal traumafavourable outcome with
International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September-2014 1196 Pneumomediastinum and subcutaneous emphysema secondary to blunt laryngeal traumafavourable outcome with
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
Contents. Part A Clinical Evaluation of Laryngeal Disorders. 3 Videostroboscopy and Dynamic Voice Evaluation with Flexible Laryngoscopy...
 Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury
 J Neurosurg Spine 4:273 277, 2006 Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury CRAIG KILBURG, HUMBERT G. SULLIVAN, M.D., AND
J Neurosurg Spine 4:273 277, 2006 Effect of approach side during anterior cervical discectomy and fusion on the incidence of recurrent laryngeal nerve injury CRAIG KILBURG, HUMBERT G. SULLIVAN, M.D., AND
Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds
 Presented by: David F Smith, MD, PhD March 2, 2012 Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds 1
Presented by: David F Smith, MD, PhD March 2, 2012 Vocal Cord Paresis:Background and Case Reports The Greater Baltimore Medical Center, The Johns Hopkins Voice Center at GBMC Stroboscopy Grand Rounds 1
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
CASE STUDIES CONTENTS PART REINKE' S EDEMA, 3 VOCAL CORD DYSFUNCTION, 7. fiabit COUGH, 15 MUSCLE TENSION DYSPHONIA, 18 PUBERPHONIA, 33
 CONTENTS PART I CASE STUDIES REINKE' S EDEMA, 3 CASE STUDY 1-1: Postoperative Reinke's Edema, 4 VOCAL CORD DYSFUNCTION, 7 CASE STUDY 2-1: Vocal Cord Dysfunction, 8 CASE STUDY 2-2: Vocal Cord Dysfunction,
CONTENTS PART I CASE STUDIES REINKE' S EDEMA, 3 CASE STUDY 1-1: Postoperative Reinke's Edema, 4 VOCAL CORD DYSFUNCTION, 7 CASE STUDY 2-1: Vocal Cord Dysfunction, 8 CASE STUDY 2-2: Vocal Cord Dysfunction,
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
Survey on the Management of Syncope Patients performed by the ESC Council for Cardiology Practice
 Survey on the Management of Syncope Patients performed by the ESC Council for Cardiology Practice A survey on the use of ESC Guidelines on Syncope by Cardiologists Report from: Riccardo Asteggiano, Maxime
Survey on the Management of Syncope Patients performed by the ESC Council for Cardiology Practice A survey on the use of ESC Guidelines on Syncope by Cardiologists Report from: Riccardo Asteggiano, Maxime
Carcinogenesis and treatment of adenocarcinoma of the oesophagus and gastric cardia Hulscher, J.B.F.
 UvA-DARE (Digital Academic Repository) Carcinogenesis and treatment of adenocarcinoma of the oesophagus and gastric cardia Hulscher, J.B.F. Link to publication Citation for published version (APA): Hulscher,
UvA-DARE (Digital Academic Repository) Carcinogenesis and treatment of adenocarcinoma of the oesophagus and gastric cardia Hulscher, J.B.F. Link to publication Citation for published version (APA): Hulscher,
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Superior and Posterior Mediastinum. Assoc. Prof. Jenny Hayes
 Superior and Posterior Mediastinum Assoc. Prof. Jenny Hayes WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for the purposes of research or study.
Superior and Posterior Mediastinum Assoc. Prof. Jenny Hayes WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for the purposes of research or study.
Department of Pediatric Otolarygnology. ENT Specialty Programs
 Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Anatomy of the Airway
 Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Professional Development: proposals for assuring the continuing fitness to practise of osteopaths. draft Peer Discussion Review Guidelines
 5 Continuing Professional Development: proposals for assuring the continuing fitness to practise of osteopaths draft Peer Discussion Review Guidelines February January 2015 2 draft Peer Discussion Review
5 Continuing Professional Development: proposals for assuring the continuing fitness to practise of osteopaths draft Peer Discussion Review Guidelines February January 2015 2 draft Peer Discussion Review
Hoarseness. Evidence-based Key points for Approach
 Hoarseness Evidence-based Key points for Approach Sasan Dabiri, Assistant Professor Department of otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medial Sciences Definition:
Hoarseness Evidence-based Key points for Approach Sasan Dabiri, Assistant Professor Department of otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medial Sciences Definition:
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
School orientation and mobility specialists School psychologists School social workers Speech language pathologists
 2013-14 Pilot Report Senate Bill 10-191, passed in 2010, restructured the way all licensed personnel in schools are supported and evaluated in Colorado. The ultimate goal is ensuring college and career
2013-14 Pilot Report Senate Bill 10-191, passed in 2010, restructured the way all licensed personnel in schools are supported and evaluated in Colorado. The ultimate goal is ensuring college and career
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Anatomy II ANAT 302. Course Description
 Anatomy II ANAT 302 Course Description This course provides the students with lectures and comprehensive overview of the gross anatomy of the components of the respiratory, cardiovascular, digestive and
Anatomy II ANAT 302 Course Description This course provides the students with lectures and comprehensive overview of the gross anatomy of the components of the respiratory, cardiovascular, digestive and
Grossman, 1953), and there is little information so far concerning its function
 52 J. Physiol. (I957) I35, 52-57 A SURGICAL APPROACH TO THE SUPERIOR CERVICAL GANGLION AND RELATED STRIJCTURES IN THE SHEEP BY THE LATE A. B. APPLETON* AND G. M. H. WAITES From the Zoological Society of
52 J. Physiol. (I957) I35, 52-57 A SURGICAL APPROACH TO THE SUPERIOR CERVICAL GANGLION AND RELATED STRIJCTURES IN THE SHEEP BY THE LATE A. B. APPLETON* AND G. M. H. WAITES From the Zoological Society of
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
MSA. Sleep disorders MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR 1/26/2015. Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain
 MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain MSA Neurodegenerative disease Parkinsonism, cerebellar, dysautonomia Mean survival is less
MULTIPLE SYSTEM ATROPHY AND NOCTURNAL STRIDOR Alex Iranzo Neurology Service Hospital Clinic de Barcelona Spain MSA Neurodegenerative disease Parkinsonism, cerebellar, dysautonomia Mean survival is less
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Sternotomy in Thyroid Carcinoma: Experience of Loma Linda University Medical Center
 Sternotomy in Thyroid Carcinoma: Experience of Loma Linda University Medical Center Benjamin Bradford 1, Pedro A De Andrade Filho 1, Alfred Simental 1, Hannah Copeland 2, Allen Murga 2, Tracy Bailey 2,
Sternotomy in Thyroid Carcinoma: Experience of Loma Linda University Medical Center Benjamin Bradford 1, Pedro A De Andrade Filho 1, Alfred Simental 1, Hannah Copeland 2, Allen Murga 2, Tracy Bailey 2,
What do VFE s consist of?
 The Use of Vocal Function Exercises as a Treatment Modality in VF Paralysis UCSF VOICE CONFERENCE October 16-18, 2008 Wendy DeLeo LeBorgne, Ph.D. CCC-SLP Voice Pathologist & Singing Voice Specialist wleborgne@dhns.net
The Use of Vocal Function Exercises as a Treatment Modality in VF Paralysis UCSF VOICE CONFERENCE October 16-18, 2008 Wendy DeLeo LeBorgne, Ph.D. CCC-SLP Voice Pathologist & Singing Voice Specialist wleborgne@dhns.net
Autologous Fat Augmentation of the Vocal Folds
 Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Tokai J Exp Clin Med., Vol. 39, No. 3, pp. 146-150, 2014 Autologous Fat Augmentation of the Vocal Folds Shinya OKADA *1, Etsuyo TAMURA *2 and Masahiro IIDA *3 *1 Department of Otorhinolaryngology, Tokai
Validation of ultrasound as a diagnostic tool to assess vocal cord motion in an animal feasibility study
 Original Article Validation of ultrasound as a diagnostic tool to assess vocal cord motion in an animal feasibility study Karuna Dewan 1, Merry E. Sebelik 2, John D. Boughter 3, Courtney B. Shires 4 1
Original Article Validation of ultrasound as a diagnostic tool to assess vocal cord motion in an animal feasibility study Karuna Dewan 1, Merry E. Sebelik 2, John D. Boughter 3, Courtney B. Shires 4 1
Normal Voice. Evaluation of a Patient with Hoarseness. No disclosures. Hoarseness. Assessment. Assessment
 Evaluation of a Patient with Hoarseness No disclosures Mari Hagiwara, MD NYU Langone Medical Center ASHNR 2017 Hoarseness Symptom: any deviation from normal voice quality as perceived by self or others;
Evaluation of a Patient with Hoarseness No disclosures Mari Hagiwara, MD NYU Langone Medical Center ASHNR 2017 Hoarseness Symptom: any deviation from normal voice quality as perceived by self or others;
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
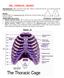 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Research Article Postthyroidectomy Throat Pain and Swallowing: Do Proton Pump Inhibitors Make a Difference?
 ISRN Otolaryngology Volume 2013, Article ID 135978, 4 pages http://dx.doi.org/10.1155/2013/135978 Research Article Postthyroidectomy Throat Pain and Swallowing: Do Proton Pump Inhibitors Make a Difference?
ISRN Otolaryngology Volume 2013, Article ID 135978, 4 pages http://dx.doi.org/10.1155/2013/135978 Research Article Postthyroidectomy Throat Pain and Swallowing: Do Proton Pump Inhibitors Make a Difference?
BILATERAL ABDUCTOR VOCAL CORD PALSY. Dr NITYA G Final year PG KIMS
 BILATERAL ABDUCTOR VOCAL CORD PALSY Dr NITYA G Final year PG KIMS INTRODUCTION Vocal cord paralysis is a sign of a disease It results from dysfunction of Recurrent laryngeal nerves on both sides Paralysis
BILATERAL ABDUCTOR VOCAL CORD PALSY Dr NITYA G Final year PG KIMS INTRODUCTION Vocal cord paralysis is a sign of a disease It results from dysfunction of Recurrent laryngeal nerves on both sides Paralysis
Disclosures. Primary Methods for Treating UVP. Key Factors Influencing Treatment Planning. Guiding principle with Treatment Planning 2/4/2018
 Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Chapter 1. Respiratory Anatomy and Physiology. 1. Describe the difference between anatomy and physiology in the space below:
 Contents Preface vii 1 Respiratory Anatomy and Physiology 1 2 Laryngeal Anatomy and Physiology 11 3 Vocal Health 27 4 Evaluation 33 5 Vocal Pathology 51 6 Neurologically Based Voice Disorders 67 7 Vocal
Contents Preface vii 1 Respiratory Anatomy and Physiology 1 2 Laryngeal Anatomy and Physiology 11 3 Vocal Health 27 4 Evaluation 33 5 Vocal Pathology 51 6 Neurologically Based Voice Disorders 67 7 Vocal
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Faculty of Clinical Forensic Medicine Committee 1/2018
 Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Causes of recurrent laryngeal nerve paralysis
 Auris Nasus Larynx 29 (2002) 41 45 www.elsevier.com/locate/anl Causes of recurrent laryngeal nerve paralysis Eiji Yumoto a, *, Ryosei Minoda a, Masamitsu Hyodo b, Takahiko Yamagata b a Department of Otolaryngology-Head
Auris Nasus Larynx 29 (2002) 41 45 www.elsevier.com/locate/anl Causes of recurrent laryngeal nerve paralysis Eiji Yumoto a, *, Ryosei Minoda a, Masamitsu Hyodo b, Takahiko Yamagata b a Department of Otolaryngology-Head
VOCAL CORD PALSY. Department of ENT, Head and Neck Surgery DR OSEGHALE DR AKPALABA
 VOCAL CORD PALSY Department of ENT, Head and Neck Surgery DR OSEGHALE DR AKPALABA Case Presentation M /70 years Pensioner Christain Bini Resides in Benin Had total thyroidectomy. Follicular Ca of thyroid
VOCAL CORD PALSY Department of ENT, Head and Neck Surgery DR OSEGHALE DR AKPALABA Case Presentation M /70 years Pensioner Christain Bini Resides in Benin Had total thyroidectomy. Follicular Ca of thyroid
Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler, MD, Roee Landsberg, MD, Dan M. Fliss, MD
 ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
ORIGINAL ARTICLE ELECTIVE PARATRACHEAL NECK DISSECTION FOR LATERAL METASTASES FROM PAPILLARY CARCINOMA OF THE THYROID: IS IT INDICATED? Avi Khafif, MD, Rami Ben-Yosef, MD, Avrum Abergel, MD, Ada Kesler,
P1: OTA/XYZ P2: ABC c01 BLBK231-Ginsberg December 23, :43 Printer Name: Yet to Come. Part 1. The Neurological Approach COPYRIGHTED MATERIAL
 Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
Free Data! Using Publicly- Available Data for Your Research Project
 Free Data! Using Publicly- Available Data for Your Research Project Tamara S. Ritsema MPH, MMSc, PA-C University of Nebraska Medical Center Physician Assistant Program Why Do Research? My dean / chair
Free Data! Using Publicly- Available Data for Your Research Project Tamara S. Ritsema MPH, MMSc, PA-C University of Nebraska Medical Center Physician Assistant Program Why Do Research? My dean / chair
FLEXIBLE FIBREOPTIC LARYNGOSCOPY VERSUS SIMPLE VOICE ASSESSMENT IN A ROUTINE CLINICAL SETTING TO PREDICT VOCAL CORD PARALYSIS AFTER THYROID SURGERY
 ISSN: 2250-0359 VOLUME 4 ISSUE 3 2014 FLEXIBLE FIBREOPTIC LARYNGOSCOPY VERSUS SIMPLE VOICE ASSESSMENT IN A ROUTINE CLINICAL SETTING TO PREDICT VOCAL CORD PARALYSIS AFTER THYROID SURGERY Sah BP, Bhandary
ISSN: 2250-0359 VOLUME 4 ISSUE 3 2014 FLEXIBLE FIBREOPTIC LARYNGOSCOPY VERSUS SIMPLE VOICE ASSESSMENT IN A ROUTINE CLINICAL SETTING TO PREDICT VOCAL CORD PARALYSIS AFTER THYROID SURGERY Sah BP, Bhandary
Page 126. Type of Publication: Original Research Paper. Corresponding Author: Dr. Rajesh V., Volume 3 Issue - 4, Page No
 ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
Intermittent intraoperative nerve monitoring in thyroid reoperations: Preliminary results of a randomized, single-surgeon study
 ORIGINAL ARTICLE Intermittent intraoperative nerve monitoring in thyroid reoperations: Preliminary results of a randomized, single-surgeon study Hu Hei, MD, 1 Bin Zhou, MD, 1 Jianwu Qin, MD, 1 Yongping
ORIGINAL ARTICLE Intermittent intraoperative nerve monitoring in thyroid reoperations: Preliminary results of a randomized, single-surgeon study Hu Hei, MD, 1 Bin Zhou, MD, 1 Jianwu Qin, MD, 1 Yongping
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Vocal Fold Motion Impairment. Surgical options 10/17/2008. Voice Changes after Treatment for Bilateral Vocal Fold Motion Impairment
 Voice Changes after Treatment for Bilateral Vocal Fold Motion Impairment Betty S. Tsai, MD Mark S. Courey, MD Sarah L. Schneider, MS, CCC-SLP Soha Al-Jurf, MS, CCC-SLP UCSF Department of Otolaryngology
Voice Changes after Treatment for Bilateral Vocal Fold Motion Impairment Betty S. Tsai, MD Mark S. Courey, MD Sarah L. Schneider, MS, CCC-SLP Soha Al-Jurf, MS, CCC-SLP UCSF Department of Otolaryngology
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics
 Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
Dr Kelly Jones Anesthesiologist at Northwest Orthopedics Decrease narcotic use in the immediate post operative period. Better Pain Control Less side effects then General Anesthesia Sedation Post operative
APHN. Shortness of breath. Ednin Hamzah CEO, Hospis Malaysia.
 APHN Shortness of breath Ednin Hamzah CEO, Hospis Malaysia ednin@hospismalaysia.org What is it? a subjective experience of difficult and uncomfortable breathing American Thoracic Society What do the patients
APHN Shortness of breath Ednin Hamzah CEO, Hospis Malaysia ednin@hospismalaysia.org What is it? a subjective experience of difficult and uncomfortable breathing American Thoracic Society What do the patients
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
Postoperative Phrenic Nerve Palsy
 Postoperative Phrenic Nerve Palsy in Patients with Open-Heart Surgery Omkar N. Markand, M.D., F.R.C.P.(C), S. S. Moorthy, M.D., Yousuf Mahomed, M.D., Robert D. King, M.D., and John W. Brown, M.D. ABSTRACT
Postoperative Phrenic Nerve Palsy in Patients with Open-Heart Surgery Omkar N. Markand, M.D., F.R.C.P.(C), S. S. Moorthy, M.D., Yousuf Mahomed, M.D., Robert D. King, M.D., and John W. Brown, M.D. ABSTRACT
Subspecialty Rotation: Otolaryngology
 Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Vocal Cord Medialization Medialization Laryngoplasty
 Vocal Cord Medialization Medialization Laryngoplasty Carolyn Waddington RN MSN FNP CORLN The Methodist Hospital Houston, TX SOHN, Boston, 2010 Objectives Describe the history of the first treatments for
Vocal Cord Medialization Medialization Laryngoplasty Carolyn Waddington RN MSN FNP CORLN The Methodist Hospital Houston, TX SOHN, Boston, 2010 Objectives Describe the history of the first treatments for
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
A Study of Incidence of External Hernias in N.W.F.P.
 Abstract A Study of Incidence of External Hernias in N.W.F.P. Pages with reference to book, From 119 To 121 Mukkaram Khan ( Surgical 'B' Unit, Lady Reading Hospital, Peshawar. ) Tariq S. Mufti ( Assistant
Abstract A Study of Incidence of External Hernias in N.W.F.P. Pages with reference to book, From 119 To 121 Mukkaram Khan ( Surgical 'B' Unit, Lady Reading Hospital, Peshawar. ) Tariq S. Mufti ( Assistant
Chronic Obstructive Pulmonary Disease (COPD) Measures Document
 Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Emedica SRA Revision Service Guidance for authors
 Emedica SRA Revision Service Guidance for authors Thank you for your interest in writing questions for the Emedica online revision service. This guide will clarify the type / format of question we are
Emedica SRA Revision Service Guidance for authors Thank you for your interest in writing questions for the Emedica online revision service. This guide will clarify the type / format of question we are
Ear Nose and Throat ENT 316. Bachelor of Medicine and Surgery; MB, BCh. Fourth. (department council approval)
 1* Ear Nose and Throat ENT 316 Basic Information Program Title Bachelor of Medicine and Surgery; MB, BCh Department Offering the Course Ear Nose and Throat Academic Year / Level Fourth Date of Specification
1* Ear Nose and Throat ENT 316 Basic Information Program Title Bachelor of Medicine and Surgery; MB, BCh Department Offering the Course Ear Nose and Throat Academic Year / Level Fourth Date of Specification
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Patient Information Leaflet P2
 Patient Information Leaflet P2 POTENTIAL CONSEQUENCES OF PARATHYROID SURGERY Parathyroid surgery is generally a safe procedure. The vast majority of patients undergoing an operation on the parathyroid
Patient Information Leaflet P2 POTENTIAL CONSEQUENCES OF PARATHYROID SURGERY Parathyroid surgery is generally a safe procedure. The vast majority of patients undergoing an operation on the parathyroid
Introducing the Fastrach-LMA. Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council
 Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Anatomy Sheet #5. In the previous lecture, we finished discussion about the larynx; now we continue with trachea, lungs and pleura.
 Anatomy Sheet #5 In the previous lecture, we finished discussion about the larynx; now we continue with trachea, lungs and pleura. Trachea and lungs The knowledge about the pleura and lungs is very important
Anatomy Sheet #5 In the previous lecture, we finished discussion about the larynx; now we continue with trachea, lungs and pleura. Trachea and lungs The knowledge about the pleura and lungs is very important
National COPD Audit Programme
 National COPD Audit Programme COPD: Who cares when it matters most? National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Outcomes from the clinical audit of COPD exacerbations admitted
National COPD Audit Programme COPD: Who cares when it matters most? National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Outcomes from the clinical audit of COPD exacerbations admitted
Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries
 REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
REVIEW ARTICLE J Korean Thyroid Assoc Vol. 4, No. 2, November 2011 Surgical Treatment for Papillary Thyroid Carcinoma in Japan: Differences from Other Countries Yasuhiro Ito, MD and Akira Miyauchi, MD
Carcinoma of the larynx L 4. Carcinoma of the larynx is the most common head & neck cancer, this has a high cure rate which may reach 90%.
 L 4 Carcinoma of the larynx Carcinoma of the larynx is the most common head & neck cancer, this has a high cure rate which may reach 90%. Incidence: It is more common in males than females in ratio 5:1.
L 4 Carcinoma of the larynx Carcinoma of the larynx is the most common head & neck cancer, this has a high cure rate which may reach 90%. Incidence: It is more common in males than females in ratio 5:1.
HOARSENESS. Prevention and types of treatment
 HOARSENESS Prevention and types of treatment What is hoarseness? What are the causes of hoarseness? How is hoarseness evaluated? When do I need to seek specialized medical evaluation? What are the treatments
HOARSENESS Prevention and types of treatment What is hoarseness? What are the causes of hoarseness? How is hoarseness evaluated? When do I need to seek specialized medical evaluation? What are the treatments
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):10-11, 1998.
 Citation Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):1-11, 18. Full Text As experts in airway management, anesthesiologists are at risk for liability
Citation Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):1-11, 18. Full Text As experts in airway management, anesthesiologists are at risk for liability
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Laser Cordectomy. Glottic Carcinoma
 Laser Cordectomy in Glottic Carcinoma Department of Otolaryngology gy Head & Neck Surgery Alexandria University Historical Review Endolaryngeal extirpation of vocal cord cancers is a controversial o issue
Laser Cordectomy in Glottic Carcinoma Department of Otolaryngology gy Head & Neck Surgery Alexandria University Historical Review Endolaryngeal extirpation of vocal cord cancers is a controversial o issue
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Clinical Trials of Active Surveillance of Papillary Microcarcinoma of the Thyroid
 World J Surg (2016) 40:516 522 DOI 10.1007/s00268-015-3392-y ORIGINAL SCIENTIFIC REPORT Clinical Trials of Active Surveillance of Papillary Microcarcinoma of the Thyroid Akira Miyauchi 1,2 Published online:
World J Surg (2016) 40:516 522 DOI 10.1007/s00268-015-3392-y ORIGINAL SCIENTIFIC REPORT Clinical Trials of Active Surveillance of Papillary Microcarcinoma of the Thyroid Akira Miyauchi 1,2 Published online:
Council on Education of the Deaf. Office of Program Accreditation. CED Program Review Evaluation Rubric
 Council on Education of the Deaf Office of Accreditation CED Review Evaluation Rubric Evaluation Rubric Cover Sheet Institution State Date submitted Name of Preparer Email Evaluation Review Team Member
Council on Education of the Deaf Office of Accreditation CED Review Evaluation Rubric Evaluation Rubric Cover Sheet Institution State Date submitted Name of Preparer Email Evaluation Review Team Member
