A Retrospective Study of High-Voltage, Pulsed Current as an Adjunctive Therapy in Limb Salvage for Chronic Diabetic Wounds of the Lower Extremity
|
|
|
- Lee Phillips
- 5 years ago
- Views:
Transcription
1 A Retrospective Study of High-Voltage, Pulsed Current as an Adjunctive Therapy in Limb Salvage for Chronic Diabetic Wounds of the Lower Extremity Jeremy J. Burdge, MD; Jodi F. Hartman, MS; and Michelle L. Wright, BS Abstract Complex diabetic ulcers of the lower extremity can be slow to heal and may lead to amputation. A retrospective study was conducted to evaluate the effect of a form of electrical stimulation using high-voltage, pulsed current (HVPC) as an adjunct to a multidisciplinary approach to limb salvage for chronic diabetic wounds of the lower extremity. Data from 30 patients with diabetes (17 men, 13 women, mean age 65.8 ± 12.6 years, mean HgbA1c level = 8.2 ± 1.5, with varying comorbidities) and 45 wounds were reviewed. Mean wound duration before referral and treatment was 25.0 weeks (range 4.0 to 60.0) and the mean wound surface area was 7.8 cm 2 (range 0.6 cm 2 to 62.0 cm 2 ). The majority (62.2%) of wounds were classified 1C, 2C, or 3D (University of Texas diabetic wound classifications). The mean number of treatments, administered two or three times a week, was 23.0 (range 6.0 to 65.0) and 35 wounds (77.8%) healed after a mean of 14.2 weeks (range 3.4 to 59.0). Of those, 31 remained healed at a mean follow-up of 39.8 weeks (range 11.1 to 84.3) and additional HVPC healed two of the four recurrences. These results suggest that HVPC is a useful addition to a multidisciplinary limb salvage management approach for complex lower extremity wounds. Further study is warranted to elucidate its role in this application. Key Words: chronic wounds, diabetic wounds, electrical stimulation, lower extremity wounds, wound healing Index: Ostomy Wound Management 2009;55(8):30 38 Potential Conflicts of Interest: none to disclose Complex diabetic wounds of the lower extremity can be slow to heal and have a significant impact on patient quality of life. 1,2 Approximately two thirds of patients with lower extremity ulcers exhibit a triad of neuropathy, foot deformity, and minor foot trauma. 3,4 Diabetic foot complications are the principal cause of nontraumatic lower extremity amputations. 5 Based on an average of 133,235 limb-loss hospital discharges per year, Goldman et al 6 estimate the direct annual cost of amputations in the US was $13 billion in Previous evidence 5 suggests that up to 85% of diabetic foot and leg amputations may be prevented with appropriate knowledge of risk factors and application of evidence-based multidisciplinary treatment. The effects of electrical stimulation on chronic wound healing have been studied since the mid-1960s. 7,8 Although the mechanism of action is not entirely understood, it has been theorized that the increased blood flow induced by electrical stimulation promotes microcirculation and healing in wounds. 6,8-10 Others have suggested that electrical stimulation increases the rate of wound healing by attracting and proliferating different cell types to the wound. 7,10 Electrical stimulation also has been shown to inhibit bacterial activity in vitro, which may further enhance wound healing. 11 A summary of the studies supporting these theories is beyond the scope of this paper; information has been detailed in several recent reviews and a meta-analysis. 7,8,12,13 Dr. Burdge is Medical Director, Plastic and Reconstructive Surgery, Grant Wound Care, Columbus, OH. Ms. Hartman is President and Ms. Wright is Clinical Research Manager, Orthopaedic Research and Reporting, Ltd., Gahanna, OH. Please address correspondence to: Jodi F. Hartman, MS, Orthopaedic Research and Reporting, Ltd., 585 Woodbay Drive, Gahanna, OH 43230; orthopaedicresearch@yahoo.com. 30 OSTOMY WOUND MANAGEMENT AUGUST
2 HIGH-VOLTAGE, PULSED CURRENT Gardner et al s 13 meta-analysis of 15 studies demonstrated that electrical stimulation therapy increased the rate of chronic wound healing 144% compared to control samples and concluded that electrical therapy is an effective adjunct for chronic wound healing. In 2002, the Centers for Medicare and Medicaid Services approved payment for electrical stimulation for the treatment of pressure ulcers and lower extremity wounds caused by venous and arterial insufficiency and diabetes that have not responded to at least 30 days of standard wound treatment. 8,14 A few prospective randomized studies and several retrospective studies documenting successful results with various forms of electrical stimulation in chronic lower extremity wounds have been published. 1,6,8-10,13,15-17 Many of the authors patients with diabetes and chronic foot wounds are referred for care in a final effort to achieve limb salvage and prevent major amputation; a previously unstudied form of high-voltage, pulsed current (HVPC) is used as an adjunct to a multidisciplinary approach to help achieve that goal. This form of HVPC uses higher voltage amplitude than previous methods and causes deep-layered, fused muscle contraction, which may facilitate muscle contraction and relaxation, thereby enhancing blood flow. Because this method of HVPC differs from traditional HVPC used in previously published studies focusing on chronic, lower extremity wounds, 1,6,9,10,16,17 a retrospective study was conducted to evaluate the effect of this treatment approach on healing for a consecutive series of patients with chronic, full-thickness, diabetic, lower extremity wounds. Methods and Procedures Standard management protocol. All patients included in this retrospective cohort were managed by a family physician or referring internist in conjunction with a multidisciplinary wound clinic at a level I trauma center. The multidisciplinary wound team included a plastic surgeon (senior author), vascular surgeon, infectious disease consultants, and podiatrists. As part of diabetic counseling, every effort was made to maintain glycemic control with a glycosylated hemoglobin (High) A1C level <7 and smokers were instructed about the necessity of nicotine cessation. Tissue perfusion was evaluated in all patients using noninvasive Doppler. Patients with ankle-brachial indices <0.7 or biphasic waveforms were seen by vascular surgery for angiography or peripheral vascular intervention as needed. All necrotic tissue was surgically excised to the level of healthy tissue. Wound cultures were obtained from all patients at the beginning of treatment and during treatment as dictated by change in wound status. Persons with bacterial colonization received oral or intravenous antibiotics in accordance with culture results and infectious disease consultation. Bioburden was minimized with appropriate topical antibacterials and weekly local wound debridement. Patients with osteomyelitis were treated with intravenous antibiotics as appropriate, excision of Ostomy Wound Management 2009;55(8):30 38 Key Points Despite diagnostic and treatment advances, managing lower extremity diabetic ulcers and preventing amputations remain considerable challenges. Although not completely understood, electrical stimulation has been documented to affect healing of chronic wounds, including diabetic foot ulcers. The results of this retrospective study involving 30 patients (45 wounds) suggest that prospective, controlled clinical studies to ascertain the efficacy of electrical stimulation using high-voltage, pulsed current as part of a multidisciplinary limb salvage program are warranted. necrotic bone, and topical antibacterials. Regular podiatric consultations to maintain appropriate offloading were obtained, and complete offloading with wheelchairs was encouraged for all patients with plantar ulcers. HVPC therapy was instituted after patients achieved glycemic and bacteriologic control as documented by negative wound cultures and following revascularization procedures if indicated. Treatment was provided two to three times per week for 16 weeks or until wound closure. Treatment three times per week was preferred but if travel was problematic a twice-weekly visit schedule was developed. All treatments were standardized they were performed in a procedure room where the temperature was controlled at 74 F using the HVPC system (MicroVas Vascular Therapy System, MicroVas Technologies, Inc., Tulsa, OK). The MicroVas treatment system is a patented technology patent number US 6,745,078, issued June 1, The MicroVas was pre-programmed at 45 minutes for each treatment. Four emitter pads are placed strategically over the wound and major muscle groups as fol- Table 1. University of Texas (UT) Wound Classification System 5,18 Grade 0 Completely epithelialized pre-or postulcerative lesions 1 Superficial wounds penetrating through the epidermis only or both the epidermis and dermis 2 Wounds penetrating into tendon or capsule, but not bone 3 Wounds penetrating to bone or into joint Stage A No infection or ischemia B Infection only present C Ischemia only present D Both infection and ischemia present AUGUST 2009 OSTOMY WOUND MANAGEMENT 31
3 Table 2: Wound distribution (N=30 patients) A C B UT Wound Grade N = 45 UT Grade 1 21 (46.7%) 1A 5 (11.1%) 1B 2 (4.4%) 1C 14 (31.1%) 1D 0 (0.0%) UT Grade 2 12 (26.7%) 2A 1 (2.2%) 2B 0 (0.0%) Figure 1: Photographs (A-C) demonstrating strategic emitter pad placement for HVPC. 2C 7 (15.6%) 2D 4 (8.9%) UT Grade 3 12 (26.7%) 3A 0 (0.0%) 3B 2 (4.4%) 3C 3 (6.7%) 3D 7 (15.6%) lows: rectangular (5 inch x 8 inch) pads on the anterior and posterior upper thigh; round (4-inch diameter) pads on the anterior compartment and posterior gastrocnemius muscle; smaller rectangular (3 inch x 5 inch) pads just above the ankle, overlying the path of the dorsalis pedis and the posterior tibial arteries; and square (3 inch x 3 inch) pads on the pedal arch on the top and bottom of each foot. Emitter pads were secured with enough pressure to ensure full contact between the pad and the lower extremity without compromising blood flow. In all instances, one emitter pad was placed directly over the wound, which first was covered with salinesoaked gauze. The opposing emitter pad was placed 180º from the wound (see Figure 1a-c). This form of HVPC creates a current that passes through the limb, in many cases creating muscular contraction, and produces a standardized biphasic, symmetric, square pulse wave, with a pulse width of 90- to 100 msec at Hz with a cycle width of 18 msec. The duration of the cycle was 1.5 seconds on and 1.5 seconds off. The voltage amplitude is variable to a maximum of 140 volts. The amplitude is individualized so each patient can maximize a fused tetanic contraction but remain below the noxious stimulation threshold. Relative contraindications to HVPC included cardiac pacemakers, malignant ulcers, pregnancy, partial-thickness wounds, or age less than 18 years. Study methods. After obtaining institutional review board approval, data from a consecutive series of patients with diabetes and chronic, full-thickness wounds of the lower extremity who were treated with HVPC as an adjunctive therapy to standard wound management during a period of 22 months (from October 2005 through August 2007) were reviewed. All patients had previously failed a multidisciplinary wound treatment plan. Data from all patients who returned for scheduled treatments were included. After reviewing a listing of all patients who received HVPC adjunctive therapy, 30 eligible patients (45 wounds) were identified. Variables. The senior author reviewed patient records to extract patient demographics, social history, comorbidities, previous lower extremity procedures, vascular interventions, High AlC blood levels, and wound variables. Wounds were classified according to initial presentation using the University of Texas (UT) Wound Classification System 5,18 (see Table 1). A digital planimeter is used to obtain pre-treatment surface area measurements from wound tracings routinely obtained during office examinations; the average of three measurements is recorded. In addition, the number of HVPC treatments performed, the incidence and time to wound healing, length of follow-up, and incidence of wound recurrence were extracted from the records. Healing was considered complete when full epithelialization was present across the wound or when the wound was closed by supplemental skin graft (see Figure 2a-e). Procedure-related complications and additional treatments also were documented. A spreadsheet using Microsoft Excel 2002 (Microsoft Corporation, Redmond, WA) was created for data entry. Statistical analysis. Descriptive statistics (mean, me- 32 OSTOMY WOUND MANAGEMENT AUGUST
4 HIGH-VOLTAGE, PULSED CURRENT dian, standard deviation, frequency, and percentage) were used to describe demographic, diagnostic, treatment, and outcome data. Demographic and outcome variables were compared between the three UT grades. Kruskal-Wallis One Way Analysis of Variance on Ranks was performed to compare non-normally distributed, continuous variables. Chi-square analysis was used to compare categorical data. Additional analyses were conducted comparing demographic and outcome variables between full-thickness skin and subcutaneous tissue wounds and wounds with exposed tendon, muscle, or bone, neuropathic and non-neuropathic wounds, ischemic and nonischemic wounds, and infected and noninfected wounds. Student s t-test was used to compare normally distributed, continuous variables; Mann-Whitney Rank Sum Test was used to compare non-normally distributed, continuous data. Fisher Exact Test was used to compare categorical data. Spearman Rank Order Correlation was employed to ascertain a correlation between wound size and the number of treatments. Differences were considered to be statistically significant when the P value was <0.05 with a power of at least 0.8. Statistical analyses were performed using SigmaStat Software, version 2.0 (SPSS, Inc., Chicago, IL). Results Patient data. Of the 30 study participants, 17 (56.7%) were men and 13 (43.3%) were women, mean age of 65.8 years (SD = 12.6; median = 67.1; range 33.0 to 90.7 years). The mean High AlC blood level was 8.2 (SD = 1.5; median = 8.1; range 5.4 to 11.6). Diabetes was uncontrolled in eight (26.7%) patients. Other comorbidities included neuropathy (25, 83.3%), peripheral vascular disease (23, 76.7%), cardiac disease (11, 36.7%), infection (10, 33.3%), osteomyelitis (five, 16.7%), and morbid obesity (three, 10.0%). The majority (20, 66.7%) of patients did not have a history of smoking. Nine patients (30.0%) underwent previous amputations due to pre-existing vascular insufficiency or wound complications, five (16.7%) had normal peripheral vascular status, 11 (36.7%) had moderate peripheral vascular disease with biphasic waveforms, and 14 (46.7%) patients were documented as having severe peripheral vascular disease with monophasic waveforms and/or ischemic tissue loss. Ten (33.3%) patients underwent previous vascular interventions and two (6.7%) had unreconstructable peripheral vascular disease. Wound/treatment data. Wounds were located on the forefoot (22, 48.9%), heel (12, 26.7%), anterior/posterior tibia (seven, 15.6%), and ankle (four, 8.9%). Mean wound duration before treatment initiation was 25.0 weeks (SD = 15.6; median = 24.0; range 4.0 to 60.0 weeks). The study population was split nearly equally between full-thickness skin and subcutaneous tissue wounds (UT Grade 1) and wounds with exposed tendon, muscle, or bone (UT Grades 2 and 3) (see Table 2). The majority of wounds (35, 77.8%) were ischemic, 15 (33.3%) were clinically infected, and 11 (24.4%) were both ischemic and infected. The mean wound surface area before starting electrical stimulation treatment was 7.8 cm 2 (SD = 12.5; median = 2.4; range 0.6 to 62.0 cm 2 ). The mean number of HVPC treatments was 23.0 (SD = 10.8; median = 21.0; range 6.0 to 65.0 treatments). Skin grafts were used to close five (16.7%) wounds, all of which remained healed at a mean follow-up of 31.3 weeks. Thirty-five wounds (77.8%) healed in a mean time of 14.2 weeks (SD = 9.8; median = 12.6; range, 3.4 to 59.0 weeks). The patient with the largest wound measurement (62.0 cm 2 ) a 53.8-year-old man with a history of transmetatarsal amputation who had a neuropathic UT 1C plantar ulcer 16 weeks before treatment initiation required the highest number of treatments (65) and the longest time to heal (59.0 weeks). The patient initially underwent 35 HVPC treatments in a 5- to 6-month period, at which time his wound was 90% healed before he became noncompliant regarding finishing treatments. When he returned to the physician s office 3 months later, HVPC treatments resumed and the wound completely healed after 30 treatments over 5 months. Of the 45 wounds, 10 (22.2%) failed to heal (see Figure 3). One patient required a
5 A B C D E Figure 2: A pre-treatment photograph of the foot of a 61.9-year-old man with controlled diabetes, neuropathy, and infection who had a UT 1B forefoot plantar ulcer for approximately 9 months (A). Before beginning HVPC therapy, the patient was discouraged by the ineffectiveness of previous treatment and soaked the wound in extremely hot water containing Epsom salt. After suffering third-degree burns of the foot from the water temperature, the patient developed a UT 1B heel ulcer (B and C). After 25 HVPC treatments, both wounds healed at 8.9 and 12.6 weeks, respectively, and have not recurred at a most recent follow-up of 5 months (D and E). transmetatarsal amputation (one wound) and below-knee amputation was performed in four patients (five wounds). Of the four remaining wounds, one wound in one patient deteriorated and required further excision of necrotic tendon. Two patients (three wounds) were still undergoing treatment at the time of data collection. Only two of the 10 wounds that failed to heal deteriorated during the course of treatment. At a mean follow-up of 39.8 weeks (SD = 22.7; median = 36.5; range, 11.1 to 84.3 weeks) after complete healing, equivalent to a mean 56.4 weeks (SD = 23.4; median = 50.4; range 26.1 to 10.7 weeks) from treatment initiation, 31 (88.6%) of the 35 wounds remained healed. Of the four (11.4%) recurrences, additional HVPC was employed and subsequently healed two (5.7%) wounds, below-knee amputation was required in another, and treatment is continuing for the remaining wound. No complications related to the use of HVPC were reported. Statistical analysis. No statistically significant differences were noted between UT grades and patient demographic or wound outcome variables. Patient demographic, wound duration, wound size, and number of stimulation treatments also did not differ between healed and nonhealed wounds. In addition, no significant differences were noted in patient demographics, number of stimulation treatments, healing time, and wound failure rate between full-thickness skin and subcutaneous tissue wounds (UT Grade 1) and wounds with exposed tendon, muscle, or bone (UT Grades 2 and 3); between neuropathic and non-neuropathic wounds; between ischemic and nonischemic wounds; or between infected and noninfected wounds. No significant relationships were found among the following comparisons: 1) wound duration before treatment or wound size and number of stimulation treatments; 2) wound duration before treatment and healing time; and 3) wound size and number of stimulation treatments. Discussion Although not entirely understood, the theoretical effects of electrical stimulation on microcirculation, cell migration, cell 34 OSTOMY WOUND MANAGEMENT AUGUST 2009 proliferation, and bacterial inhibition suggest that this therapy has the potential to enhance the healing of chronic, diabetic wounds The method of HVPC employed in this study differs from those used in previously published studies focusing on chronic, lower extremity wounds. 1,6,9,10,16,17 Traditional HVPC therapy involves placement of a few emitter pads on one side of the limb, which causes current penetration into the tissue by only a few centimeters. Typically, therapy is administered offsite using portable units and in many reported studies, the amplitude was set to evoke a sensory response, but was below the level of fused tetanic contraction. 6,9,10 The HVPC used in this study is administered in clinic and involves the use of multiple emitter pads placed on both sides of the limb. As a result, current penetrates to the major muscle groups. The voltage amplitude is increased until deep-layered, fused muscular contraction is achieved without noxious stimulation. This type of stimulation with a short pulse width of 90- to 100-msec, high-peak current, and a relatively long interpulse interval (55.19 Hz) allows a relatively comfortable stimulation while still effecting skeletal muscle contraction. 19 In addition, it is theorized that this level of stimulation may facilitate sympathetic smooth muscle contraction and relaxation; thereby, improving blood flow at the small arteriolar or venule level. 19 Because treatment is conducted at the clinic and not selfadministered, incorrect application is prevented and patient noncompliance greatly reduced. Conducting treatments in a clinic setting also ensures that the stimulation is conducted in a warm room, which has been shown in previous prospective clinical trials 20,21 to increase skin blood flow and wound healing. Finally, although optimal treatment frequency and duration remain the subject of investigation, HVPC was applied two to three times per week in the current study versus relying on self-administered daily treatment protocols 3 to 7 days per week as reported in previous studies. 1,6,9,10,17 Although less convenient than home use, administering HVPC in the clinic setting eliminates patient usage errors and reduces patient device use noncompliance, which was reported to be as high as 30%
6
7 Figure 3: Summary of additional procedures required for wounds that failed to heal using HVPC. Wide Excision of Tendon N=1 (3.3%) Additional Treatment N=2 (6.7%) Amputation N=5 (16.7%) in a previous randomized clinical trial. 17 The wounds comprising this study population were complex limb salvage cases most were ischemic and neuropathic ulcers and occurred in patients with a history of severe diabetes and previous amputation. Despite this complexity, 33 of the 45 wounds (73.3%) healed and no amputations were needed in 66.7% of patients. Furthermore, no infections occurred and routine surveillance cultures taken during the treatment period remained negative, which may suggest a possible bacterial inhibitory effect, as previously demonstrated. 22 The results from this study support the use of HVPC as an adjunctive therapy in the management of chronic, full-thickness, diabetic wounds of the lower extremity for which previous conservative management failed. Because no significant differences between wound types and outcome were observed, no conclusions based upon wound types and their responsiveness to HVPC could be made, which may be due to the study population size or be a reflection of the heterogeneity of ischemic wounds and their outcomes. 6 Although direct comparisons cannot be made, the results of this study correlate with previous studies examining HVPC in chronic diabetic wounds of the lower extremity that report complete healing. 9,10,17 In Peters et al s 17 randomized, double-blind, placebo-controlled pilot trial of HVPC as an adjunct in diabetic foot ulcers, 65% of wounds undergoing electrical stimulation healed at a mean time to healing of 6.8 weeks compared to a 35% healing rate for wounds receiving placebo at a mean time of 6.9 weeks. Although the proportion of healed ulcers is similar to the current findings, mean time to healing of 14.2 weeks in the current study is higher. However, patients in the Peters et al study received nightly HVPC treatments for 8 hours, 7 days per week, for 12 weeks or until healing was achieved, compared to the current study protocol of two to three times per week for 16 weeks or until healing was achieved. In a retrospective, observational case series 9 of six patients with inframalleolar ischemic diabetic wounds treated with HVPC, four (66.7%) wounds healed and two (33.3%) wounds resulted in amputation. Although the proportion of ulcers healed in the current study is similar, patients in the reported case series received more frequent (daily) treatments and wounds took an average of 7.25 months to heal, considerably longer than the current mean treatment duration of 14.2 weeks. Goldman et al s 10 retrospective, observational, controlled study demonstrated healing of nine out of 10 (90%) inframalleolar ischemic wounds after 1 year of HVPC. The mean duration of treatments for these healed wounds was 3.4 months and the protocol consisted of daily 1-hour treatments, 5 to 7 days per week, until healing. This population achieved a slightly higher incidence of healing with more frequent treatments within a comparable time period, but did include nondiabetic wounds, which may have influenced the overall healing incidence. Because no control group was involved, the positive results cannot be generalized to the total population of chronic diabetic lower extremity wounds or said to be the result of HVPC treatment only. However, results of providing good wound care for patients with neuropathic diabetic foot ulcers have been published. Specifically, Margolis et al 22 conducted a meta-analysis to determine the percentage of neuropathic diabetic foot ulcers that heal after receiving good wound care, defined as a standard care regimen consisting of debridement, wound care with either saline-moistened gauze or placebo gel and gauze, and explicit instructions to patients about avoiding weight-bearing ambulation. This protocol of care resulted in healing of approximately 31% of diabetic neuropathic ulcers (N = 450) after 20 weeks. The current study also was comprised primarily of neuropathic wounds but had a healing incidence twice as high as the benchmark provided in the Margolis et al 22 meta-analysis. The standard wound management protocol used in the current study meets the Margolis et al definition of good care, as it consisted of debridement, wound care with either saline-moistened gauze or placebo gel and gauze, and explicit instructions regarding avoiding weightbearing ambulation. 22 Thus, current results support the management of complex wounds via a multidisciplinary approach, which may include HVPC as an adjunct treatment. Based on these promising preliminary results, prospective, controlled randomized studies are warranted to elucidate the role of this form of HVPC in multimodal limb salvage and compare outcomes to control as well as other HVPC treatments. The wide range of HVPC protocols utilized in chronic diabetic lower extremity wound studies also illustrates the importance of additional studies examining optimal frequency and duration. Finally, standardized reporting of amplitude, frequency, and duration is needed to assist in comparing re- 36 OSTOMY WOUND MANAGEMENT AUGUST
8
9 sults between studies. Conclusion The encouraging results from this retrospective study suggest that this form of HVPC is a useful addition to a multidisciplinary limb salvage management approach for complex lower extremity diabetic wounds. Although this study is not without weaknesses (ie, retrospective design and lack of a control group), this study serves as a first step in assessing this particular treatment modality and was not designed to address rate of wound healing or tissue perfusion. Further study is warranted to better elucidate HVPC s role in this application. This overall multi-modal limb salvage approach will continue to be used by the senior author, who recommends its use to other clinicians. References 1. Houghton PE, Kincaid CB, Lovell M, et al. Effect of electrical stimulation on chronic leg ulcer size and appearance. Phys Ther. 2003;83(1): Phillips T, Stanton B, Provan A, Lew R. A study of the impact of leg ulcers on quality of life: financial, social, and psychologic implications. J Am Acad Dermatol. 1994;31(1): Boulton AJM, Kirsner RS, Vileikyte L. Neuropathic diabetic foot ulcers. New Engl J Med. 2004;351(1): Reiber GE, Vileikyte L, Boyko EJ, et al. Causal pathways for incident lowerextremity ulcers in patients with diabetes from two settings. Diabetes Care. 1999;22(1): Armstrong DG, Lavery LA, Harkless LB. Who is at risk for diabetic foot ulceration? Clin Podiatr Med Surg. 1998;15: Goldman R, Rosen M, Brewley B, Golden M. Electrotherapy promotes healing and microcirculation of infrapopliteal ischemic wounds: a prospective pilot study. Adv Skin Wound Care. 2004;17(6): Edsberg LE, Brogan MS, Jaynes CD, Fries K. Topical hyperbaric oxygen and electrical stimulation: exploring potential synergy. Ostomy Wound Manage. 2002;48(11): Kloth LC. Electrical stimulation for wound healing: a review of evidence from in vitro studies, animal experiments, and clinical trials. Lower Extremity Wounds. 2005;4(1): Goldman RJ, Brewley BI, Golden MA. Electrotherapy reoxygenates inframalleolar ischemic wounds on diabetic patients: a case series. Adv Skin Wound Care. 2002;15(3): Goldman R, Brewley B, Zhou L, Golden M. Electrotherapy reverses inframalleolar ischemia: a retrospective, observational study. Adv Skin Wound Care. 2003;16(2): Merriman HL, Hegyi CA, Albright-Overton CR, Carlos J Jr, Putnam RW, Mulcare JA. A comparison of four electrical stimulation types on Staphylococcus auerus growth in vitro. J Rehabil Res Dev. 2004;41(2): Cutting KF. Electric stimulation in the treatment of chronic wounds. Wounds. 2006;2(1): Gardner SE, Frantz RA, Schmidt FL. Effect of electrical stimulation on chronic wound healing: a meta-analysis. Wound Rep Reg. 1999;7: Centers for Medicare and Medicaid Services (CMS). Decision memo for electrostimulation for wounds (CAG-00068N). Medicare Coverage Database. Baltimore, MD: CMS; July 23, Available at: Accessed April 21, Baker LL, Chambers R, DeMuth SK, Villar F. Effects of electrical stimulation on wound healing in patients with diabetic ulcers. Diabetes Care. 1997;20(3): Lundeberg TCM, Eriksson SV, Malm M. Electrical nerve stimulation improves healing of diabetic ulcers. Ann Plast Surg. 1992;29(4): Peters EJ, Lavery LA, Armstrong DG, Fleischli JG. Electric stimulation as an adjunct to heal diabetic foot ulcers: a randomized clinical trial. Arch Phys Med Rehabil. 2001;82(6): Lavery LA, Armstrong DG, Harkless LB. Classification of diabetic foot ulcerations. J Foot Ankle Surg. 1996;35: Alon G. Principles of electrical stimulation. In: Nelson RM, Currier DP (eds). Clinical Electrotherapy, 2nd ed. Norwalk, CT: Appleton & Lange;1991: Lawson D, Petrofsky JS. A randomized control study on the effect of biphasic electrical stimulation in a warm room on skin blood flow and healing rates in chronic wounds of patients with and without diabetes. Med Sci Monit. 2007;13(6):CR258 CR Petrofsky J, Schwab E, Lo T, Cuneo M, Lawson D. The thermal effect on the blood flow response to electrical stimulation. Med Sci Monit. 2007;13(11):CR498 CR Margolis DJ, Kantor J, Berlin JA. Healing of diabetic neuropathic foot ulcers receiving standard treatment. A meta-analysis. Diabetes Care. 1999;22(5): OSTOMY WOUND MANAGEMENT AUGUST
HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
 Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
DIABETES AND THE AT-RISK LOWER LIMB:
 DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Arterial Studies And The Diabetic Foot Patient
 Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
Arterial Studies And The Patient George L. Berdejo, BA, RVT, FSVU gberdejo@wphospital.org Disclosures I have nothing to disclose! Diabetes mellitus continues to grow in global prevalence and to consume
High Voltage Pulsed Current (HVPC) Mohammed Taher Ahmed Associate professor of PT Mobile phone :
 High Voltage Pulsed Current (HVPC) Mohammed Taher Ahmed Associate professor of PT E-Mail: momarar@ksu.edu.sa Mobile phone : 0542115404 Objective To review the core concepts and terminology used in high
High Voltage Pulsed Current (HVPC) Mohammed Taher Ahmed Associate professor of PT E-Mail: momarar@ksu.edu.sa Mobile phone : 0542115404 Objective To review the core concepts and terminology used in high
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Surgical Off-loading. Reiber et al Goals of Diabetic Foot Surgery 4/28/2012. The most common causal pathway to a diabetic foot ulceration
 Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Reiber et al. 1999 Surgical Off-loading The most common causal pathway to a diabetic foot ulceration Alex Reyzelman DPM Associate Professor California School of Podiatric Medicine at Samuel Merritt University
Oxygen is required for normal cellular
 Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks
 A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
Root Cause Analysis for nontraumatic
 Root Cause Analysis for nontraumatic amputations 2016 (Full Data) Date Richard Leigh and Stella Vig, Co-Chairs London SCN Footcare Network October 2015 Outline of London RCA 2016 London Hospitals invited
Root Cause Analysis for nontraumatic amputations 2016 (Full Data) Date Richard Leigh and Stella Vig, Co-Chairs London SCN Footcare Network October 2015 Outline of London RCA 2016 London Hospitals invited
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers
 A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Prediction of healing for post-operative diabetic foot wounds based on early wound area progression
 Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Hyperbarics in Diabetic Wound Care. Aurel Mihai, MD & Brian Kline, MD
 Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Transcutaenous Electrical Nerve Stimulation to Manage a Lower Extremity Wound Complicated by Peripheral Arterial Disease: A Case Report
 Feature Transcutaenous Electrical Nerve Stimulation to Manage a Lower Extremity Wound Complicated by Peripheral Arterial Disease: A Case Report Douglas D. Yarboro, DPT, MBA, CWS, ICLM; and Robert Smith,
Feature Transcutaenous Electrical Nerve Stimulation to Manage a Lower Extremity Wound Complicated by Peripheral Arterial Disease: A Case Report Douglas D. Yarboro, DPT, MBA, CWS, ICLM; and Robert Smith,
End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema. Original Policy Date
 MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 2.02.12 End Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
a,b and the annual cost of diabetic neuropathy is estimated to be $10.91 billion in the United States alone. 3
 eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE
 GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE Michael S. Conte MD Professor and Chief, Vascular and Endovascular Surgery Co-Director, Center for Limb Preservation Co-Director, Heart and Vascular
GLOBAL VASCULAR GUIDELINES: A NEW PATHWAY FOR LIMB SALVAGE Michael S. Conte MD Professor and Chief, Vascular and Endovascular Surgery Co-Director, Center for Limb Preservation Co-Director, Heart and Vascular
Risk factors for recurrent diabetic foot ulcers: Site matters. Received for publication 5 March 2007 and accepted in revised form
 Diabetes Care In Press, published online May 16, 2007 Risk factors for recurrent diabetic foot ulcers: Site matters Received for publication 5 March 2007 and accepted in revised form Edgar J.G. Peters
Diabetes Care In Press, published online May 16, 2007 Risk factors for recurrent diabetic foot ulcers: Site matters Received for publication 5 March 2007 and accepted in revised form Edgar J.G. Peters
The diabetic foot a focus on ischemia and infection
 The diabetic foot a focus on ischemia and infection Stephan Morbach, MD Department of Diabetes and Angiology Marienkrankenhaus ggmbh Soest, Germany s.morbach@mkh-soest.de Epidemiology of Diabetic Foot
The diabetic foot a focus on ischemia and infection Stephan Morbach, MD Department of Diabetes and Angiology Marienkrankenhaus ggmbh Soest, Germany s.morbach@mkh-soest.de Epidemiology of Diabetic Foot
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Fluorescent Angiography: Practical uses in the Clinical Setting
 Fluorescent Angiography: Practical uses in the Clinical Setting Charles Andersen MD, FACS, MAPWCA Chief Vascular/Endovascular/ Limb Preservation Surgery Service (Emeritus) Chief of Wound Care Service Madigan
Fluorescent Angiography: Practical uses in the Clinical Setting Charles Andersen MD, FACS, MAPWCA Chief Vascular/Endovascular/ Limb Preservation Surgery Service (Emeritus) Chief of Wound Care Service Madigan
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Lymphedema
 End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
End-Diastolic Pneumatic Compression Boot as a Treatment of Peripheral Vascular Disease or Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Topical Oxygen Wound Therapy (MEDICAID)
 Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care
 Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care Michael S. Conte MD Professor and Chief, Division of Vascular and Endovascular
Global Vascular Guideline on the Management of Chronic Limb Threatening Ischemia -a new foundation for evidence-based care Michael S. Conte MD Professor and Chief, Division of Vascular and Endovascular
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
A systematic approach to the failed plastic surgical reconstruction of the diabetic foot
 æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
æiefs PROCEEDINGS A systematic approach to the failed plastic surgical reconstruction of the diabetic foot Ioannis I. Ignatiadis, MD, PhD 1 *, Vassiliki A. Tsiampa, MD 2 and Apostolos E. Papalois, PhD
OF WOUNDS SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM. AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois
 1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
CLI Therapy- LINCed Multi disciplinary discussions on CLI
 CLI Therapy- LINCed Multi disciplinary discussions on CLI Critical limb ischemia and managing the infected wound Michiel Schreve North West Clinics Alkmaar, The Netherlands Disclosure Speaker name: Michiel
CLI Therapy- LINCed Multi disciplinary discussions on CLI Critical limb ischemia and managing the infected wound Michiel Schreve North West Clinics Alkmaar, The Netherlands Disclosure Speaker name: Michiel
Role of free tissue transfer in management of chronic venous ulcer
 Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Original Article Role of free tissue transfer in management of chronic venous ulcer K. Murali Mohan Reddy, D. Mukunda Reddy Department of Plastic Surgery, Nizams Institute of Medical Sciences, India. Address
Principles of Electrical Currents. HuP 272
 Principles of Electrical Currents HuP 272 Electricity is an element of PT modalities most frightening and least understood. Understanding the basis principles will later aid you in establishing treatment
Principles of Electrical Currents HuP 272 Electricity is an element of PT modalities most frightening and least understood. Understanding the basis principles will later aid you in establishing treatment
Perfusion Assessment in Chronic Wounds
 Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Perfusion Assessment in Chronic Wounds American Society of Podiatric Surgeons Surgical Conference September 22, 2018 Michael Maier, DPM, FACCWS Cardiovascular Medicine Cleveland Clinic Disclosures Speaker,
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds
 Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/30/2012 Radiology Quiz of the Week # 79 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/30/2012 Radiology Quiz of the Week # 79 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Novitas Medicare Policy Primer
 Novitas Medicare Policy Primer Medicare Jurisdiction (JL and JH) AR, CO, LA, MS, NM, OK, TX, DC, DE, MD, NJ, & PA Counties of Arlington and Fairfax in Virginia and the city of Alexandria in Virginia Application
Novitas Medicare Policy Primer Medicare Jurisdiction (JL and JH) AR, CO, LA, MS, NM, OK, TX, DC, DE, MD, NJ, & PA Counties of Arlington and Fairfax in Virginia and the city of Alexandria in Virginia Application
Negative Pressure Wound Therapy (NPWT)
 Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES
 ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
ASSESSING THE VASCULAR STATUS OF THE FEET FOR PATIENTS WITH DIABETES Caroline McIntosh is Senior Lecturer in Podiatry, University of Huddersfield, Yorkshire A reduced blood supply to the lower limb, due
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Disclosures. Outpatient NPWT Options Free up Hospital Beds, but Do They Work? Objectives. Clinically Effective: Does it Work?
 4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD
 Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
USWR 23: Outcome Measure: Non Invasive Arterial Assessment of patients with lower extremity wounds or ulcers for determination of healing potential
 USWR 23: Outcome Measure: Non Invasive Arterial Assessment of patients with lower extremity wounds or ulcers for determination of healing potential MEASURE STEWARD: The US Wound Registry [Note: This measure
USWR 23: Outcome Measure: Non Invasive Arterial Assessment of patients with lower extremity wounds or ulcers for determination of healing potential MEASURE STEWARD: The US Wound Registry [Note: This measure
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Clasificación WIFI: Finalmente hablaremos el mismo idioma! WIfI: Wound, Ischemia, foot Infection The SVS Threatened Limb Classification
 Clasificación WIFI: Finalmente hablaremos el mismo idioma! WIfI: Wound, Ischemia, foot Infection The SVS Threatened Limb Classification Joseph L. Mills, Sr., M.D. Professor of Surgery, Chief, Vascular
Clasificación WIFI: Finalmente hablaremos el mismo idioma! WIfI: Wound, Ischemia, foot Infection The SVS Threatened Limb Classification Joseph L. Mills, Sr., M.D. Professor of Surgery, Chief, Vascular
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
DIABETIC ULCERS V PRESSURE ULCERS SO, WHAT DO YOU CALL IT?
 DIABETIC ULCERS V PRESSURE ULCERS SO, WHAT DO YOU CALL IT? Arthur Stone, DPM Mary Sieggreen, MSN,CNS,NP,CVN Faculty Disclosure Dr. Stone has listed an affiliation with: Advisory Board Member..FXI, Inc.
DIABETIC ULCERS V PRESSURE ULCERS SO, WHAT DO YOU CALL IT? Arthur Stone, DPM Mary Sieggreen, MSN,CNS,NP,CVN Faculty Disclosure Dr. Stone has listed an affiliation with: Advisory Board Member..FXI, Inc.
CASE 1: TYPE-II DIABETIC FOOT ULCER
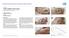 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Hyperbaric Oxygen Utilization in Wound Care
 Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
DO NOT DUPLICATE. E-Stimulation: Every action in the body, from the. An Effective Modality to Facilitate Wound Healing
 E-Stimulation: An Effective Modality to Facilitate Wound Healing Pamela Scarborough, PT, DPT, MS, CDE, CWS, CEEAA; and Luther C. Kloth PT, MS, FAPTA, CWS, FACCWS Every action in the body, from the cellular
E-Stimulation: An Effective Modality to Facilitate Wound Healing Pamela Scarborough, PT, DPT, MS, CDE, CWS, CEEAA; and Luther C. Kloth PT, MS, FAPTA, CWS, FACCWS Every action in the body, from the cellular
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology
 A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
Setting The setting was a hospital. The economic study was carried out in the USA.
 A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Negative Pressure Therapy for Complex Wounds in Patients with Sickle-Cell Disease: A Case Study
 Negative Pressure Therapy for Complex Wounds in Patients with Sickle-Cell Disease: A Case Study Andre Oliveira Paggiaro, MD; Viviane Fernandes de Carvalho, PhD, ETN; Guilherme Henrique Hencklain Fonseca,
Negative Pressure Therapy for Complex Wounds in Patients with Sickle-Cell Disease: A Case Study Andre Oliveira Paggiaro, MD; Viviane Fernandes de Carvalho, PhD, ETN; Guilherme Henrique Hencklain Fonseca,
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
I have no financial interests to disclose in regards to this lecture.
 Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Acknowledgements. No tengo conflictos de interés que revelar. I have no conflicts of interest to disclose. Michael S. Conte. David G.
 No tengo conflictos de interés que revelar I have no conflicts of interest to disclose. Critical Limb Ischemia : The Need for a New System to Define Disease Burden and Stratify Amputation Risk and Need
No tengo conflictos de interés que revelar I have no conflicts of interest to disclose. Critical Limb Ischemia : The Need for a New System to Define Disease Burden and Stratify Amputation Risk and Need
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): 3/1/2012 Most Recent Review Date (Revised): 9/6/2018 Effective Date: 11/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Original Issue Date (Created): 3/1/2012 Most Recent Review Date (Revised): 9/6/2018 Effective Date: 11/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
STPH Clinic for Wound Care and Hyperbaric Medicine
 STPH Clinic for Wound Care and Hyperbaric Medicine Ochsner/St. Tammany Partnership John Kessels, MD Medical Director St. Tammany Wound Center Chantal Lorio, DPM Associate Medical Director Ochsner Wound
STPH Clinic for Wound Care and Hyperbaric Medicine Ochsner/St. Tammany Partnership John Kessels, MD Medical Director St. Tammany Wound Center Chantal Lorio, DPM Associate Medical Director Ochsner Wound
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound
 Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound Craig M. Walker, MD, FACC, FACP Chairman, New Cardiovascular Horizons Clinical Professor of Medicine Tulane
Peripheral Artery Disease Interventions Utilizing the Angiosomal Approach to the Complex Wound Craig M. Walker, MD, FACC, FACP Chairman, New Cardiovascular Horizons Clinical Professor of Medicine Tulane
Diabetes Foot and Skin Care. Diabetes and the feet. Foot problems: Major cause of morbidity and mortality
 Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
Session # 11 Diabetes Foot and Skin Care Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE Diabetes and the feet Diabetes affects circulation and immunity. Over time, the sensory nerves in the
A Comparison of Two Diabetic Foot Ulcer Classification Systems. The Wagner and the University of Texas wound classification systems
 Pathophysiology/Complications O R I G I N A L A R T I C L E A Comparison of Two Diabetic Foot Ulcer Classification Systems The Wagner and the University of Texas wound classification systems SAMSON O.
Pathophysiology/Complications O R I G I N A L A R T I C L E A Comparison of Two Diabetic Foot Ulcer Classification Systems The Wagner and the University of Texas wound classification systems SAMSON O.
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Hyperbaric Oxygen Therapy (HBO)
 MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
MP9055 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes-as shown below None Prevea360 Health Plan Medical Policy: 1.0 Hyperbaric Oxygen therapy (HBO)
The Diabetic Foot. Michael Anthony, DPM. 422 million diabetic million % adult population 90% Type II
 The Diabetic Foot Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center Prevalence of Diabetes 422 million diabetic 2016 382 million
The Diabetic Foot Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center Prevalence of Diabetes 422 million diabetic 2016 382 million
The Diabetic Foot. Prevalence of Diabetes United States. Prevalence of Diabetes
 The Diabetic Foot Prevalence of Diabetes Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center 422 million diabetic 2016 382 million
The Diabetic Foot Prevalence of Diabetes Michael Anthony, DPM Assistant Professor - Clinical Department of Orthopaedics The Ohio State University Wexner Medical Center 422 million diabetic 2016 382 million
Case 1. July 14, th week wound gel 3 cm x 2.5 cm = 7.5 cm². May 25, st wound gel on 290 days PI treatment 4 cm x 2.4 cm = 9.
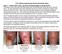 2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
Diabetic Foot Ulcer. A Complete Solution. Therapy Approach with Adapted Products
 Diabetic Foot Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Diabetic Foot Ulcers This booklet focuses on the recommended treatment of diabetic foot ulcers. Diabetes
Diabetic Foot Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Diabetic Foot Ulcers This booklet focuses on the recommended treatment of diabetic foot ulcers. Diabetes
Taking Charge of Chronic Wounds An Introduction to Electrical Stimulation and Wound Healing. Table of Contents
 Table of Contents Introduction....2 Instructions & Objectives 2 Introduction to Electrical Stimulation. 3 Applications Lab.... 11 Case Studies..14 Supplemental Information...24 Post-Test.25 Seminar Evaluation..27
Table of Contents Introduction....2 Instructions & Objectives 2 Introduction to Electrical Stimulation. 3 Applications Lab.... 11 Case Studies..14 Supplemental Information...24 Post-Test.25 Seminar Evaluation..27
JMSCR Vol 05 Issue 03 Page March 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.188 Comparison of Vacuum Assisted Closure
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.188 Comparison of Vacuum Assisted Closure
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Quality ID #437: Rate of Surgical Conversion from Lower Extremity Endovascular Revascularization Procedure National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #437: Rate of Surgical Conversion from Lower Extremity Endovascular Revascularization Procedure National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
National Clinical Conference 2018 Baltimore, MD
 National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
National Clinical Conference 2018 Baltimore, MD No relevant financial relationships to disclose Wound Care Referral The patient has been maximized from a vascular standpoint. She has no other options.
FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in
 11 Evaluation and Management of Peripheral Arterial Disease Joseph L. Mills, Sr., MD FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in the United States, foot problems ulceration, infection, and
11 Evaluation and Management of Peripheral Arterial Disease Joseph L. Mills, Sr., MD FOR THE 18 MILLION INDIVIDUALS with diabetes mellitus in the United States, foot problems ulceration, infection, and
Resection Arthroplasty for Limb Salvage of the Unreconstructable Charcot Foot & Ankle
 Resection Arthroplasty for Limb Salvage of the Unreconstructable Charcot Foot & Ankle Michael Greaser MD and James Brodsky MD Baylor University Medical Center Dallas, TX Resection Arthroplasty for Limb
Resection Arthroplasty for Limb Salvage of the Unreconstructable Charcot Foot & Ankle Michael Greaser MD and James Brodsky MD Baylor University Medical Center Dallas, TX Resection Arthroplasty for Limb
