Idiopathic dental conditions and the potential involvement of trigger points
|
|
|
- Cecil Webster
- 5 years ago
- Views:
Transcription
1 Idiopathic dental conditions and the potential involvement of trigger points Dr James Tang, CES, MBA, BDS, LDS RCS GDP, NASM Corrective Exercise Specialist, Level 3 Personal Trainer (REP registration no R ), Sports Nutritionist & Level 3 Sports Massage Therapist, with special interest in postural dysfunction and lower back problems Introduction Chronic myofascial pain is a condition that affects the fascia, the connective tissue that covers the muscles, hence the term myofascial. It is characterised by trigger points in the musculature and is the most common cause of musculoskeletal lower back and neck pain. Myofascial pain syndrome typically occurs after a muscle has been contracted repetitively or because of stressrelated muscle tension. In dentistry, trigger points in the masticatory and certain neck muscles can manifest as dental pain, temporomandibular joint (TMJ) dysfunction and sinus problems. These trigger point-induced conditions can be incredibly debilitating because their origins are difficult to identify. They can be responsible for chronic pain that seems to have no means of relief, which can ultimately result in depression. Here, the author will attempt to explore the interrelationships between myofascial pain and dentistry and give practical advice so that dentists can manage the intriguing symptoms of myofascial origin more effectively. So, what are trigger points? The term trigger point was coined by Dr Janet Travell in 1942 to describe painful nodules felt within tight bands of muscle. They are so ubiquitous that they can occur in any of the 700+ muscles in our bodies even babies have them. Unlike acupuncture points, trigger points are micro contraction knots within a muscle fibre that can be physically felt with the fingers. They should, however, not be confused with muscle spasms which affect the entire muscle, and they are not the same as tender points in patients with fibromyalgia who suffer from widespread diffuse musculoskeletal pain. 1
2 The effect of trigger points in the host muscles They are hyperirritable spots located within skeletal muscle and feel like nodules on palpation; when compressed, they cause a significant amount of pain. Essentially, part of the muscle fibre is contracted into a small thickened area and the rest of the fibre is stretched. The muscle fibres affected are not available for contraction as they are already contracted, making the host muscle weak. As a result, muscles containing trigger points are fatigued more easily and do not return to a relaxed state as quickly when muscle contraction ceases. The contracted tissues restrict blood and lymphatic circulation in their immediate vicinity, resulting in accumulation of metabolic by-products and deprivation of oxygen and nutrients. This crisis of energy produces sensitising substances that can cause pain, e.g. bradykinin, which is known to activate the muscle s nociceptors. Trigger points will not disappear without intervention; they accumulate over a lifetime and can exist indefinitely in a latent state. Although the actual pain may subside within a week or so, active trigger points simply turn latent and can be reactivated easily. Latent trigger points are the main cause of stiff joints and the restriction of a range of movements due to muscle tightness and weakness of the host muscle. They can also keep muscles out of balance, causing joints to click during function, and can potentially lead to osteoarthritis. Active trigger points usually refer pain locally and/or to distant areas of the body, and common patterns have been identified, but these referral patterns do not necessarily conform to the nerve pathways. As the majority of trigger points are not located where you feel symptoms, treating the painful area will not provide 2
3 relief. To complicate the situation further, they can also manifest in secondary muscles or as satellite trigger points in and around the vicinity of the primary site. Trigger points have been implicated in a range of conditions and they can often mimic the symptoms of others. They can cause diverse symptoms that are not normally associated with muscular problems. Many types of joint pain are mistakenly diagnosed as arthritis or tendonitis. Physiology of trigger points Muscle contraction begins with the two contractile proteins, myosin and actin, arranged in a series of compartments called sarcomeres that run the length of the myofibril. The actin is anchored to the end and the myosin sits within the middle of the sarcomere, pulling the actin from either end towards the middle to generate tension (sliding filament theory of muscle contraction). During muscular contraction, the myosin heads attach themselves to the actin filament and rotate, pulling on these filaments. Muscles with trigger points manifest in the region where sarcomeres and motor endplates become overactive. The actin and myosin myofilaments sitting within a taught band stop sliding over one another. The current hypothesis about the formation of trigger points involves the energy crisis component. When the nerve impulse arrives at the motor endplate, neurotransmitter acetylcholine is released causing calcium to be released from the sarcoplasmic reticulum (SR) and the muscle fibre involved to contract. Normally, when contraction of the muscle fibre ceases, the motor endplate stops releasing acetylcholine and the calcium pump in the SR recycle calcium back into the SR. Where there is an excessive motor endplate release of acetylcholine, surplus calcium can be released by the SR causing a maximal contracture of a segment of muscle, leading to maximal energy demand and impairment of local circulation. As a result of this deprivation of fuel and oxygen, the calcium pump is unable to return calcium back into the SR, and the muscle fibre continues to contract, creating trigger points. This vicious circle is self-perpetuating unless there is some form of intervention. Furthermore, the attachment sites of these tight muscle fibres can also become tender as they are stressed by the contraction in the centre of the fibre. 3
4 Why do we get trigger points? Active trigger points are often caused by an injury, prolonged poor posture or repetitive use. It is believed that trigger points are part of our protective mechanism. Any change in muscle biomechanics over time can manifest as areas of tight muscles, and because trigger points make the host muscles weak, they are a useful mechanism for rapidly switching off muscle power around an injury. This is essential if, for example, there is a fracture. Myofascial muscle pain is therefore a key part of our protective mechanism because pain is a valuable alarm bell that warns of a problem. 4
5 The relevance of trigger points in dentistry Head and neck symptoms caused by trigger points include, but are not limited to, toothache, hypersensitivity, malocclusion, TMJ dysfunction, trismus and sinus pain. Trigger points can cause diverse symptoms such as blurred vision, dizziness, vertigo, dry eyes and balance problems. They can also cause numb lips, painful tongue and drooping eyelid (Travell and Simons, 1999, ). Temporomandibular joint (TMJ) dysfunction The TMJ is a synovial joint between the articulation of the temporal bone of the cranium and the mandible. The symptoms of TMJ dysfunction can vary from mild occasional discomfort to frequent and extreme misery. Although trigger points are often involved in TMJ disorders, they are not always the primary cause because they can develop secondary to conditions such as TMJ synovitis and arthritis. Whatever the cause, the presence of trigger points can exacerbate the condition, worsen the prognosis and interfere with primary interventions. The various muscles that control jaw function have to work in synchrony for optimal masticatory performance. Trigger points in the masticatory muscles of the jaw and anterior neck, such as the sternocleidomastoid, are typically involved with the symptoms associated with TMJ disorders, including jaw clicking, dislocation, trismus and malocclusion (Travell and Simons, 1999, ). Furthermore, if the lateral pterygoid is tight or shortened by trigger points, this can easily lead to misalignment of the jaw, causing malocclusion and associated problems. Amazingly, trigger points that cause TMJ problems may also cause other diverse symptoms such as vertigo, vision disorders, tinnitus, itchiness deep in the ear, sinus issues, toothache and more! The involvement of trigger points in these muscles should not be ruled out if a patient is suffering from TMJ symptoms. Practical advice on the management of myofascial TMJ conditions Principles of management are based on an accurate diagnosis and should be non-invasive and reversible. The objective is to control pain, relax muscles and eradicate the causative trigger points. Although a combination of treatment is often required, it is possible to eradicate the symptoms simply by using 5
6 myofascial release techniques to remove the culprit trigger points in the involved muscle(s). A thorough clinical examination, history-taking and radiography should be used to exclude any pathology in the TMJ because structural changes are usually absent in myofascial pain. It may be necessary to refer your patients for behavioural or psychological assistance because there is often a strong correlation between TMJ problems and various types of emotional stress. Bruxism is common and many patients exhibit nocturnal teeth grinding. To avoid additional anxiety, it is important to reassure them that their condition is often self-limiting. General advice should also recommend the avoidance of repetitive jaw movement (constant chewing overtaxes the masticatory muscles) and prolonged jaw opening, as well as a soft diet. External application of heat can be recommended as this increases blood and lymphatic circulation to muscles that have been affected by trigger points. Although trigger points in masticatory muscles can result in malocclusion, poor occlusal balance can predispose to muscle imbalances and therefore rectification of the precipitating occlusal problems may help to prevent recurrence of problems. Soft splint therapy can be used to dampen the impact of jaw clenching and reduce muscle activity. Nevertheless, all these measures offer only symptomatic relief and will not eradicate the trigger points involved. Myofascial therapy is the only way to get rid of the trigger points. 6
7 Practical advice on the management of dental-related myofascial trigger points Trigger points in the pterygoid muscles These trigger points are a frequent cause of pain in the TMJ but unfortunately they are well hidden by the mandible, making it difficult to access for treatment. The medial pterygoid Anatomy this muscle originates from the medial surface of the lateral pterygoid plate of the sphenoid bone, the pyramidal process of the palatine bone and the maxillary tuberosity. It inserts to the medial surface of the ramus and the angle of the mandible. Action elevates and protrudes the lower jaw. Trigger points in the medial pterygoid restrict jaw opening and can cause pain in the TMJ. Pain can be referred to the hard palate and tongue, making swallowing painful. Treatment it is possible to massage the medial pterygoid extra-orally by pressing up with your thumb inside the inner edge towards the back of the mandible. The lateral pterygoid Anatomy the superior head originates from the lateral surface of the greater wing of the sphenoid and inserts to the capsule and articular disc of the TMJ. The inferior head originates from the lateral surface of the lateral pterygoid plate of the sphenoid and inserts to the neck of the mandible. Action protrudes the mandible, opens the mouth and moves the mandible from side to side. Trigger points in this muscle are the prime source of myofascial pain and TMJ dysfunction. Constant trigger point-generated tension here tends to pull the mandible forward, making the TMJ click and possibly even dislocating the joint. Trigger points can develop in this muscle as a result of repetitive biting, teeth grinding, prolonged jaw opening due to dental 7
8 work or breathing difficulties, emotional stress, thumb sucking, nail biting or occlusal malalignment. Pain can also be referred to the cheek and can mimic sinus pain (as with the masseter). Trigger points in the masseter and temporalis can predispose to satellite trigger points developing in the lateral pterygoid by making them work harder to open the mouth. Treatment massage the lateral pterygoid intra-orally with the index finger. The fingertip should seek the deep pocket posterior to the upper molars then push both inward and upward using tiny, short strokes. If trigger points are present, this can be excruciatingly painful. Sternocleidomastoid (SCM) trigger points Trigger points in this muscle can cause an incredible amount of pain (but it is all referred elsewhere and the muscles themselves rarely hurt) and a bewilderingly diverse set of symptoms, including headache, dry cough, sore throat, sinus pain, excessive eye tearing, visual disturbances and dizziness. Anatomy the SCM originates from the mastoid process with the sternal division runs diagonally downwards to attach to the sternum. The clavicular division attaches onto the medial aspect of the clavicle. Action unilateral contraction turns the head towards the opposite side whilst bilateral contraction flexes the neck and translates the head forward. Characteristics trigger points in the sternal division refer pain deep in the orbit, TMJ, back and top of the head. The clavicular division refers pain to the forehead, ear and ipsilateral molar teeth. It is unusual for trigger points on one side to refer pain to the contralateral side, but frontal headaches caused by clavicular trigger points can be cross-referred to the opposite side of the forehead. Trigger points in the SCM are frequently sponsored by trigger point activities in the upper trapezius typically induced by a forward head posture when these neck extensors have to remain constantly contracted to support the weight of the head. 8
9 Management trigger points in the sternocleidomastoid can be so tender to pressure that they can be mistaken for tender lymph nodes. To massage the sternocleidomastoid, grip the muscles between your fingers and knead firmly. Search for trigger points in each of the two branches, starting up behind the earlobe, all the way down to the clavicle. Please beware the carotid arteries and avoid massaging where you can feel a pulse, high up under the chin alongside the trachea. Masseter trigger points Anatomy the masseter is a powerful muscle of mastication consisting of a superficial and deep head, both originating from the zygomatic arch. The superficial part inserts on the masseter tuberosity at the outer surface of the mandibular angle whereas the deep part runs further dorsally to the outer surface of the ramus of the mandible. Characteristics those in the deep layer anterior to the ear can cause pain in the TMJ. Masseter trigger points can increase muscle tension so much that it can result in trismus. Trigger points in the superficial masseter in the middle of the muscle belly cause toothache that resembles dental abscess pain. Patients can usually pinpoint their toothache in their lower molars. Trigger points in the superficial masseter just below the zygomatic arch give patients a feeling of toothache that extends up into the roots, with sensitivity in their upper premolars and first upper molar. Pain is typically worse in the early morning or early evening. Like many of the trigger points in the TMJ musculatures, this one is activated by uneven and repetitive chewing or biting on hard objects (such as regular nail biting). These unpleasant symptoms can be avoided by giving up these habits. Misinterpretation of these symptoms can result in unnecessary and irreversible dental procedures, such as extraction. The secondary effect of masseter trigger points is that they may cause patients to neglect brushing due to hypersensitivity, leading to deterioration of their oral health. Trigger points in the masseter can also cause pain in the front of the face, under the eyes or over the eyebrows, symptoms often mistaken for sinusitis. 9
10 Practical advice on eradicating trigger points in the masseter: the trigger points are in the belly of the masseter just behind the roots of the teeth. Pressing on this knotted muscle can usually reproduce the symptoms in the teeth. Massage the masseter with two fingers, one inside and one outside, with your thumb inside the mouth, and knead the muscle between your thumb and fingers. Seek out each exquisitely tender knot, from the maxilla to the bottom of the mandible, and massage it as strongly as is bearable. Alternatively, apply firm but constant pressure on the trigger point until the pain subsides. Repeated treatment may be required for stubborn trigger points to completely release. Temporalis trigger points Anatomy the temporalis is a large, thin, fan-shaped masticatory muscle located in the side of the skull above and in front of the ear. It originates from the temporal and infratemporal crest, passing beneath the zygomatic arch and inserting into the coronoid process and the anterior ramus of the mandible. It elevates and retracts the mandible. Causes of temporalis trigger points masticatory muscles are easily overloaded, especially when we clench or grind our teeth (bruxism) which can activate trigger points in the muscle, or trigger points in the muscle can cause bruxism. In both cases, the temporalis becomes overworked and strained. Trigger points can result from prolonged jaw opening due to dental treatment: extensive dental work leads to trigger points in the temporalis muscle, adding to the facial pain and post-operative toothache, leading to the mistaken assumption that further dental work is required, which of course only worsens the problem. Other causes include chronic mouth breathing, excessive gum chewing, a cold draft of air on the side of the face and poor occlusion. Characteristics trigger points in the masseter and sternocleidomastoid sponsor satellite trigger points in the temporalis and can easily be reactivated shortly after attempts to subdue them. Furthermore, a hyperkyphotic posture, typically related to a forward head posture, can also lead to formation of trigger points in the temporalis. Unfortunately, muscles have this type of effect on one another. It is therefore important to track down and treat all the muscles that are interrelated by proximity or function. 10
11 Temporalis trigger points are associated with head pain. They refer pain to the ipsilateral head, sometimes to the front of the head over the eyebrow, and to the face and upper teeth. Sometimes, pain can be felt in the side of the face as a diffuse jaw pain extending all the way down to the neck region. Temporalis trigger points can also cause pain and hypersensitivity in the maxillary teeth. Diffuse pain in the upper teeth during mastication is likely to be coming from the temporalis. Trigger points in the front create sensitivity in the front teeth and those in the back create sensitivity in the back teeth. Temporalis trigger points are a feature of TMJ problems and chronic trigger points in the temporalis and masseter muscles can cause permanent structural damage to the synovial joint of the TMJ. Advice on treatment of temporalis trigger points find the trigger points at the front of the muscle first and build up gentle pressure. This often reproduces the deep pain that radiates to the teeth. Similar to the treatment of the masseter trigger points, maintain a firm and constant pressure until the pain alleviates. Then, massage the area gently and repeat with the next trigger point. To prevent these trigger points from recurring, advise your patients to eradicate causative factors such as gum chewing or chewing hard substances (e.g. finger nails). False sinus symptoms Trigger points in the jaw muscles can mimic the symptoms of sinusitis. When conventional sinus medication does not relieve a patient s sinus discomfort, it is pertinent to consider the involvement of trigger points as a differential diagnosis. Trigger points in the facial muscles, jaws and front of the neck can cause the production of excess mucus in the sinuses, nasal cavities and throat, which can lead to continuing sinus drainage, constant clearing of the throat, chronic cough, allergic rhinitis (runny nose), and persistent hay fever or cold symptoms. Naturally, all these widely varying symptoms can have causes other than myofascial trigger points. Nevertheless, any examination should consider the involvement of trigger points for abnormal and unexplained symptoms in the face, ears and jaws. Unfortunately, many dentists and patients are still illinformed about trigger points. 11
12 Management when trigger points are the cause of symptoms in the jaws, face, eyes, ears or teeth, significant relief can be obtained by applying myofascial release techniques. 12
13 Practical advice on the general principle of managing trigger points Combined with some simple lifestyle changes, myofascial release of trigger points can yield dramatic, immediate and sustainable results. The objectives of such therapies are: To identify the correct trigger point(s). To deactivate the point(s) using myofascial release. To prevent recurrence. Identify the correct trigger point(s) It is important to have good knowledge of the anatomy of the muscles to be treated because alleviating myofascial pain depends on locating the trigger points. The good news is that they always originate at the midpoint of a muscle s fibres where the motor nerve enters, transmitting the nerve impulse which initiates muscle contraction. The problem occurs when the fibres do not always run from one end of a muscle to the other. The orientation of the fibres in muscles varies, depending on their designated function. In a muscle made for speed, the fibres are parallel, running straight from end to end, and its trigger points are easily found halfway along. However, muscles that are made for power, like the masticatory muscles, have their fibres running diagonally at some angle to its length. Since trigger points may be found in the centre of each individual fibre, they may be situated anywhere along the muscle. That said, trigger points (active/latent) are relatively easy to locate because they are always very painful on palpation. Another problem with treating trigger points is that they typically refer pain to another site and working on the area where the pain is felt will not offer pain relief. Fortunately, the referral pattern is reproducible and well documented. The pattern of referral can be easily reproduced when the trigger point is pressed. To complicate the matter further, trigger points in the sternocleidomastoid and upper trapezius can sponsor satellite trigger points in the masticatory muscles and unless these primary trigger points are also dealt with, simply eradicating those in the satellite sites may not produce the desired long-lasting effects. It is therefore important to track down and treat all the muscles that are interrelated by proximity or function. Muscles do not operate in isolation this explains why 13
14 development of primary, central trigger points in one area of the body may lead to secondary or satellite trigger points distally. Using appropriate techniques to deactivate the point(s) Eradicating these trigger points completely usually requires multiple treatment sessions, depending on the muscle in question and the irritability of the trigger points involved up to five times a day for a week or so may be required. Persistence pays off. Clearly it is impractical for dentists to be always involved so it is advisable to instruct patients to carry out self-myofascial release so that they can mange their own trigger points in the comfort of their home. However, before attempting to treat patients, you should familiarise yourself with the effect of self-myofascial release. The best place to start is to run your fingers along your quadriceps you will almost certainly be able to feel numerous nodules that are painful to firm pressure. Applying a thin layer of cream or oil will help your finger to glide along the skin. You should use the thumb of one hand supported by the thumb of the other. Once you can feel the knot, press on it firmly (ischemic compression) until you can feel the pain (intensity 7/10; if you apply too much pressure and cause too much pain, your muscles will contract unnecessarily). Maintain the same pressure until the pain dissipates (this usually takes seconds). Unlike the trigger points in the masticatory muscles which can be easily manipulated with the fingers, finger pressure may not be adequate on the thick muscles of the legs and you may require tools such as foam rollers. Myofascial release with deep stroke massages can also be used. They work by breaking into the chemical and neurological feedback loop that maintains the micro muscular contraction. They also increase the circulation that has been restricted by the contracted tissue. Massage should be deep and in one direction only (do not attempt to rub the trigger points to and fro) and the pace should be slow because the aim is to deactivate overactive tissue and nothing should be done to make the tissue more excited. You may be tempted to discontinue working on the trigger point the moment it stops actively referring pain. However, if the trigger point still hurts when you press on it, you have only soothed it into a latent state which can be easily reactivated with the slightest overload, such as biting heavily or repetitive chewing. 14
15 The science behind this involves autogenic inhibition by activating the Golgi tendon organs located in the musculotendinous junctions. Skeletal muscle contains muscle spindles and the Golgi tendon organs, two neural receptors. Muscle spindles are sensitive to a change and rate of muscle being stretched. When stimulated, they will generate a stretch reflex that causes the muscle to contract. The Golgi tendon organs are stimulated by a change and rate of tension; this stimulation causes the muscle to relax. When a change in tension is sustained at an adequate intensity and duration, muscle spindle activity is inhibited causing a decrease in trigger point activity, allowing the muscle fibres to stretch, unknot and realign. Note, there are certain medical contraindications for trigger point therapy, such as, but not limited to, infectious skin conditions in the area involved, heart failure, or any other organ failure, and cancer. Prevention strategies Although aches and pains from trigger points are common, there can often be an underlying pathology. It is equally important to identify the causative factors of these trigger points as they rarely develop in isolation and may return if the underlying cause is not identified and addressed, whether it be a forward head posture, repetitive chewing actions, bruxism or faulty occlusion etc. If these are not rectified, symptoms can simply recur. Summary This article highlights the diversity of symptoms that can be caused by trigger points. As a consequence, it is possible to consider their involvement as a differential diagnosis for a patient s dental conditions. Presenting symptoms Bruxism Trismus TMJ dysfunction syndrome Sinus symptoms Likely location of trigger point(s) Temporalis Masseter Zygomaticus major Pterygoid muscles Masseter Sternocleidomastoid Lateral pterygoid 15
16 Toothache and hypersensitivity Clavicular branch of sternocleidomastoid Upper trapezius Masseter Temporalis Longus capitis (one of the neck flexors) 16
Muscles of mastication [part 1]
![Muscles of mastication [part 1] Muscles of mastication [part 1]](/thumbs/76/73586850.jpg) Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
Muscles of mastication [part 1] In this lecture well have the muscles of mastication, neuromuscular function, and its relationship to the occlusion morphology. The fourth determinant of occlusion is the
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS
 TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
The Role of Muscles in Movement
 The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
The Role of Muscles in Movement Muscles can t push, they can only pull as they contract, so most often body movements are the result of the activity of pairs or teams of muscles acting together or against
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Temporomandibular Joint. Dr Noman ullah wazir
 Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Temporomandibular Joint Dr Noman ullah wazir Type of Joint TMJ is a Synovial joint between : The condylar head of the mandible. The mandibular fossa of squamous part of temporal bone. The joint cavity
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014
 Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
Facial Accupressure Massage. Taha Haque, D.O. CAM Workshop
 Facial Accupressure Massage Taha Haque, D.O. CAM Workshop 1 10July2015 Benefits of facial accupressure Enhance local blood flow Firm and tone face and neck Mild to moderate symptomatic relief of headaches,
Facial Accupressure Massage Taha Haque, D.O. CAM Workshop 1 10July2015 Benefits of facial accupressure Enhance local blood flow Firm and tone face and neck Mild to moderate symptomatic relief of headaches,
Up Date on TMD WHAT IS TMD? Temporomandibular Disorders (TMD)*: Donald Nixdorf DDS, MS
 Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Up Date on TMD Donald Nixdorf DDS, MS Associate Professor Division of TMD and Orofacial Pain WHAT IS TMD? Temporomandibular Disorders (TMD)*: MUSCLE and JOINT DISORDERS * Temporomandibular Muscle and Joint
Oral cavity landmarks
 By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
By: Dr. Ahmed Rabah Oral cavity landmarks The knowledge of oral anatomy and physiology will help the operator and provides enough landmarks to act as positive guide during denture construction. This subject
TEMPORO-MANDIBULAR JOINT DISORDERS
 Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Disclaimer This movie is an educational resource only and should not be used to manage your dental health. All decisions about the management of TMJ Disorders must be made in conjunction with your Dental
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health
 T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
T M J D I S O R D E R S U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health CONTENTS 2 4 6 7 8 9 14 WHAT IS THE TEMPOROMANDIBULAR JOINT? WHAT ARE TMJ DISORDERS? WHAT CAUSES TMJ DISORDERS?
Physiotherapy management of Temporomandibular Joint (TMJ) pain
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Physiotherapy management of Temporomandibular Joint (TMJ) pain Physiotherapy Department What is the TMJ? The jaw is also known
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Physiotherapy management of Temporomandibular Joint (TMJ) pain Physiotherapy Department What is the TMJ? The jaw is also known
The Scalp and Face Protocol. Julie Goodwin, BA, LMT
 The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
The Scalp and Face Protocol Julie Goodwin, BA, LMT The Scalp and Face Protocol Julie Goodwin, BA, LMT Julie Goodwin 2014 2 Agenda Pertinent Anatomy and Physiology Treatment Planning Strokes, Techniques
3. The Jaw and Related Structures
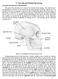 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
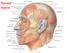 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Where is the Temporo-Mandibular Joint?
 TMJ Pain Open your jaw all the way and shut it. This simple movement would not be possible without the Temporo-Mandibular Joint (TMJ). It connects the temporal bone (the bone that forms the side of the
TMJ Pain Open your jaw all the way and shut it. This simple movement would not be possible without the Temporo-Mandibular Joint (TMJ). It connects the temporal bone (the bone that forms the side of the
Physiotherapy management of Temporomandibular Joint (TMJ) pain
 Physiotherapy management of Temporomandibular Joint (TMJ) pain Physiotherapy Department Patient information leaflet What is the TMJ? The jaw is also known as the TMJ or Temporomandibular Joint. It can
Physiotherapy management of Temporomandibular Joint (TMJ) pain Physiotherapy Department Patient information leaflet What is the TMJ? The jaw is also known as the TMJ or Temporomandibular Joint. It can
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Tempromandibular joint (TMJ) problems
 What is the tempromandibular joint (TMJ)? The tempromandibular joint (TMJ) is the jaw joint between the lower jaw (mandible) and the skull (in the temporal bone). There is one on each side of your face,
What is the tempromandibular joint (TMJ)? The tempromandibular joint (TMJ) is the jaw joint between the lower jaw (mandible) and the skull (in the temporal bone). There is one on each side of your face,
Temporomandibular Joint Disorders
 Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Temporomandibular Joint Disorders Introduction Temporomandibular joint disorders, or TMJ disorders, are a group of medical problems related to the jaw joint. TMJ disorders can cause headaches, ear pain,
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Diana Rose. Clinical Case Report Competition. West Coast College of Massage Therapy, Victoria. Second Place Winner. Winter 2009
 Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Winter 2009 Second Place Winner Diana Rose Reduction of temporomandibular
Massage Therapists Association of British Columbia Clinical Case Report Competition West Coast College of Massage Therapy, Victoria Winter 2009 Second Place Winner Diana Rose Reduction of temporomandibular
Taking Control of TMJ: Total Wellness Program
 Taking Control of TMJ: Total Wellness Program Slide 1 (Title page) There are millions of people who have jaw pain, headaches for no apparent reason, clicking, grating or difficulty opening and closing
Taking Control of TMJ: Total Wellness Program Slide 1 (Title page) There are millions of people who have jaw pain, headaches for no apparent reason, clicking, grating or difficulty opening and closing
This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors
 1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
1 This lab activity is aligned with Visible Body s Anatomy and Physiology app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES A. Watch the video 13.1 Muscular System Overview and observe
Photobiomodulation in Head and Neck Pain. Gerry Ross, DDS. Tottenham, Ontario Canada
 Photobiomodulation in Head and Neck Pain Gerry Ross, DDS Tottenham, Ontario Canada Disclosure: Dr. Ross provides education and training for Zolar Surgical Diode lasers, for which he receives a fee. No
Photobiomodulation in Head and Neck Pain Gerry Ross, DDS Tottenham, Ontario Canada Disclosure: Dr. Ross provides education and training for Zolar Surgical Diode lasers, for which he receives a fee. No
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION:
 ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
ChiroCredit.com Anatomy 226 INSTRUCTIONS/ASSIGNMENT FOR ANATOMICAL DISSECTION: Once you click on the link to open the dissection module, the first thing you need to do is to be sure you can see all the
OBJECTIVES. Unit 7:5 PROPERTIES OR CHARACTERISTICS OF MUSCLES. Introduction. 3 Kinds of Muscles. 3 Kinds of Muscles 4/17/2018 MUSCULAR SYSTEM
 OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
NEW PATIENT HOME CARE PACKET
 NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
Module 15: Stretching Fitness
 Module 15: Stretching Fitness In this module you will learn: The importance of warming up and stretching before exercising What happens to your muscles while stretching How to stretch without causing injury
Module 15: Stretching Fitness In this module you will learn: The importance of warming up and stretching before exercising What happens to your muscles while stretching How to stretch without causing injury
Manual Therapy Techniques
 Manual Therapy Techniques manual therapy: the use of hands-on techniques to evaluate, treat, and improve the status of neuromusculoskeletal conditions massage: the systematic and scientific manipulation
Manual Therapy Techniques manual therapy: the use of hands-on techniques to evaluate, treat, and improve the status of neuromusculoskeletal conditions massage: the systematic and scientific manipulation
TMJ Disorder & Sleep Conditions: The Effects on Your Body
 TMJ Disorder & Sleep Conditions: The Effects on Your Body TMJ Disorders: Temporomandibular Joint Disorders The mandible, or jaw, is the movable part of the head involving important functions of daily life,
TMJ Disorder & Sleep Conditions: The Effects on Your Body TMJ Disorders: Temporomandibular Joint Disorders The mandible, or jaw, is the movable part of the head involving important functions of daily life,
Essentials of Human Anatomy & Physiology. The Muscular System
 Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Essentials of Human Anatomy & Physiology The Muscular System The Muscular System Muscles are responsible for all types of body movement they contract or shorten and are the machine of the body Three basic
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
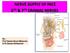 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
Dr. Sami Zaqout Faculty of Medicine IUG
 Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
INTRODUCTION. Okay, let's get started.
 INTRODUCTION This guide will help you determine if you have the hidden triggers to CHRONIC headaches. Find out if you have an underlying condition often overlooked when trying to eliminate headaches. Physicians
INTRODUCTION This guide will help you determine if you have the hidden triggers to CHRONIC headaches. Find out if you have an underlying condition often overlooked when trying to eliminate headaches. Physicians
What Your Dentist Should Know About FMS and CMP by Devin J. Starlanyl and Wesley Shankland, II
 What Your Dentist Should Know About FMS and CMP by Devin J. Starlanyl and Wesley Shankland, II This information may be freely copied and distributed only if unaltered, with complete original content including:
What Your Dentist Should Know About FMS and CMP by Devin J. Starlanyl and Wesley Shankland, II This information may be freely copied and distributed only if unaltered, with complete original content including:
ESSENTIALPRINCIPLES. Part II. Cervical Injuries
 ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
Functions of Muscle Tissue
 The Muscular System Functions of Muscle Tissue Movement Facilitation Thermogenesis Postural Support Regulation of Organ Volume Protects Internal Organs Pumps Blood (HEART) Characteristics of Muscle Tissue
The Muscular System Functions of Muscle Tissue Movement Facilitation Thermogenesis Postural Support Regulation of Organ Volume Protects Internal Organs Pumps Blood (HEART) Characteristics of Muscle Tissue
Skeletal Muscle. Smooth Muscle. Cardiac Muscle. I. 3 Types of Muscle Tissue. 1. Smooth 2. Cardiac 3. Skeletal
 I. 3 Types of Muscle Tissue 1. Smooth 2. Cardiac 3. Skeletal Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
I. 3 Types of Muscle Tissue 1. Smooth 2. Cardiac 3. Skeletal Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
LIPS TOGETHER AND TEETH APART
 John T. Mahoney, D.D.S. Family Dentistry 2117 Old Jeanerette Road New Iberia, LA 70563 Telephone 337-365-5865 Fax 337-365-6137 LIPS TOGETHER AND TEETH APART One of the most important steps in breaking
John T. Mahoney, D.D.S. Family Dentistry 2117 Old Jeanerette Road New Iberia, LA 70563 Telephone 337-365-5865 Fax 337-365-6137 LIPS TOGETHER AND TEETH APART One of the most important steps in breaking
Dental directorate Temporomandibular Disorders (TMD)
 Dental directorate Temporomandibular Disorders (TMD) Untitled-5 1 08/12/2015 17:18 This leaflet has been produced to provide you with information about Temporomandibular Disorders (TMD) and aims to answer
Dental directorate Temporomandibular Disorders (TMD) Untitled-5 1 08/12/2015 17:18 This leaflet has been produced to provide you with information about Temporomandibular Disorders (TMD) and aims to answer
Temporomandibular Joint
 6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
6 Temporomandibular Joint Most human bones are joined with one another. These connections of bones to each other are termed articulations or joints. Some joints are immovable as in the articulations of
LOCAL ANESTHESIA IN PEDIATRIC DENTISTRY
 Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of local anesthesia in pediatric dentistry must be made in conjunction
TruDenta Pain Relief Life Changing Dentistry
 Get Your Life Back! TruDenta Pain Relief Life Changing Dentistry Headache disorders impose a recognizable burden on sufferers including sometimessubstantial personal suffering, impaired quality of life
Get Your Life Back! TruDenta Pain Relief Life Changing Dentistry Headache disorders impose a recognizable burden on sufferers including sometimessubstantial personal suffering, impaired quality of life
Corrective Exercise For Temporomandibular Joint Imbalance
 Corrective Exercise For Temporomandibular Joint Imbalance Disclaimer: READ THIS FIRST! This information is not medical advice, and does not replace the diagnosis or treatment of a licensed physician. This
Corrective Exercise For Temporomandibular Joint Imbalance Disclaimer: READ THIS FIRST! This information is not medical advice, and does not replace the diagnosis or treatment of a licensed physician. This
Learn How to Manage Trigger Points
 Learn How to Manage Trigger Points What is a Trigger Point (TrP)? Ø A trigger point is a hyperirritable spot located in a taut band of skeletal muscle. They may form following a sudden trauma or may develop
Learn How to Manage Trigger Points What is a Trigger Point (TrP)? Ø A trigger point is a hyperirritable spot located in a taut band of skeletal muscle. They may form following a sudden trauma or may develop
Anatomy and physiology of Temporomandibular Joint
 Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Anatomy and physiology of Temporomandibular Joint Temporomandibular joint (TMJ): It is the articulation of the condyle of the mandible, and the inter-articular disc; with the mandibular fossa (glenoid
Myofascial Pain Massage Trigger point injection Heat, cold, acupuncture, relaxation training, and biofeedback Treatments. Pain medicines Exercise
 Myofascial Pain Myo is a Greek word for muscle. Fascia is the tough outer lining of a muscle that holds it in place. Myofascial pain is the term used to describe pain in the muscles and fascia. Myofascial
Myofascial Pain Myo is a Greek word for muscle. Fascia is the tough outer lining of a muscle that holds it in place. Myofascial pain is the term used to describe pain in the muscles and fascia. Myofascial
PH-04A: Clinical Photography Production Checklist With A Small Camera
 PH-04A: Clinical Photography Production Checklist With A Small Camera Operator Name Total 0-49, Passing 39 Your Score Patient Name Date of Series Instructions: Evaluate your Series of photographs first.
PH-04A: Clinical Photography Production Checklist With A Small Camera Operator Name Total 0-49, Passing 39 Your Score Patient Name Date of Series Instructions: Evaluate your Series of photographs first.
What s Causing Your Pain?
 PRACTICE DENTISTRY PAIN-FREE What s Causing Your Pain? Musculoskeletal pain stems from numerous sources, including genetic predisposition, environment, previous injuries and age. While you have little
PRACTICE DENTISTRY PAIN-FREE What s Causing Your Pain? Musculoskeletal pain stems from numerous sources, including genetic predisposition, environment, previous injuries and age. While you have little
Lecture 07. Lymphatic's of Head & Neck. By: Dr Farooq Amanullah Khan PMC
 Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Types of Muscle: Skeletal- muscle involved in movement of the skeleton. Striated, has alternating bands of light and dark due to overlapping
 Types of Muscle: Skeletal- muscle involved in movement of the skeleton. Striated, has alternating bands of light and dark due to overlapping filaments within the muscle cell. Skeletal muscle can be consciously
Types of Muscle: Skeletal- muscle involved in movement of the skeleton. Striated, has alternating bands of light and dark due to overlapping filaments within the muscle cell. Skeletal muscle can be consciously
Roll, Roll, Roll Your Bod - Relieving Pain Through Foam Rolling
 Roll, Roll, Roll Your Bod - Relieving Pain Through Foam Rolling Pain is NOT a Lifestyle Series Self-Myofascial Release/Foam Roll Exercises Self-care Home Routine I often hear the question should I foam
Roll, Roll, Roll Your Bod - Relieving Pain Through Foam Rolling Pain is NOT a Lifestyle Series Self-Myofascial Release/Foam Roll Exercises Self-care Home Routine I often hear the question should I foam
Muscles Unit TEST and Final Exam Study Guide May 2017
 Muscles Unit TEST and Final Exam Study Guide May 2017 Part 1 of final exam is pictures, see bottom of the study guide Part 2 of the final exam is only going to cover muscles unit. If you do this study
Muscles Unit TEST and Final Exam Study Guide May 2017 Part 1 of final exam is pictures, see bottom of the study guide Part 2 of the final exam is only going to cover muscles unit. If you do this study
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Skeletal Muscle. Cardiac Muscle. Smooth Muscle. II. Muscular System. The Muscular System
 Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Chapter CHAPTER 8 8 The Muscular System College Prep NOTES Smooth Muscle Found in body organs,vessels, respiratory passages Not striated, tapered, single cell nucleus involuntary, peristaltic contractions
Microanatomy of Muscles. Anatomy & Physiology Class
 Microanatomy of Muscles Anatomy & Physiology Class Three Main Muscle Types Objectives: By the end of this presentation you will have the information to: 1. 2. 3. 4. 5. 6. Describe the 3 main types of muscles.
Microanatomy of Muscles Anatomy & Physiology Class Three Main Muscle Types Objectives: By the end of this presentation you will have the information to: 1. 2. 3. 4. 5. 6. Describe the 3 main types of muscles.
Key Points for Success:
 ANKLE & FOOT 1 2 All of the stretches described in this chapter are detailed to stretch the right side. Key Points for Success: Keep your movements slow and precise. Breathe in before you move and breathe
ANKLE & FOOT 1 2 All of the stretches described in this chapter are detailed to stretch the right side. Key Points for Success: Keep your movements slow and precise. Breathe in before you move and breathe
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Session 3-Part 2: Skeletal Muscle
 Session 3-Part 2: Skeletal Muscle Course: Introduction to Exercise Science-Level 2 (Exercise Physiology) Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI Copyright EFS Inc. All Rights Reserved. Skeletal
Session 3-Part 2: Skeletal Muscle Course: Introduction to Exercise Science-Level 2 (Exercise Physiology) Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI Copyright EFS Inc. All Rights Reserved. Skeletal
This Session by Simon Strauss
 This Session by Simon Strauss Myofascial Pain. Part A Myofascial Pain. Part B Pain Assessment Tools. Part C Definitions and Language of Pain Allodynia- 1. A lower than normal pain threshold. 2. A clinical
This Session by Simon Strauss Myofascial Pain. Part A Myofascial Pain. Part B Pain Assessment Tools. Part C Definitions and Language of Pain Allodynia- 1. A lower than normal pain threshold. 2. A clinical
DEEP TISSUE FOAM ROLLER MASSAGE GUIDE
 Recover, Recharge, & Renew your body and mind with RE by Empower. Soothe everyday aches & pains; reduce tension & stress; and improve your overall health. DEEP TISSUE FOAM ROLLER MASSAGE GUIDE Three phases
Recover, Recharge, & Renew your body and mind with RE by Empower. Soothe everyday aches & pains; reduce tension & stress; and improve your overall health. DEEP TISSUE FOAM ROLLER MASSAGE GUIDE Three phases
The Muscular System. - composed of mostly skeletal muscle tissue, nervous tissue, blood and connective tissue
 The Muscular System Every action the body takes utilizes a muscular activity. Some of the muscles of the body are under voluntary control (skeletal muscles), and by using these muscle, you are able to
The Muscular System Every action the body takes utilizes a muscular activity. Some of the muscles of the body are under voluntary control (skeletal muscles), and by using these muscle, you are able to
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK. Musculoskeletal Anatomy & Kinesiology II REVIEW
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology II REVIEW MSAK101-II Session 4 LEARNING OBJECTIVES: By the end of this session, the student will be
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology II REVIEW MSAK101-II Session 4 LEARNING OBJECTIVES: By the end of this session, the student will be
Muscular Tissue. Functions of Muscular Tissue. Types of Muscular Tissue. Skeletal Muscular Tissue. Properties of Muscular Tissue
 Muscular Tissue Functions of Muscular Tissue Muscle makes up a large percentage of the body s weight (40-50%) Their main functions are to: Create motion muscles work with nerves, bones, and joints to produce
Muscular Tissue Functions of Muscular Tissue Muscle makes up a large percentage of the body s weight (40-50%) Their main functions are to: Create motion muscles work with nerves, bones, and joints to produce
Prosthetic Management of TMJ Disorders
 Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Prosthetic Management of TMJ Disorders Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Mohd@DrMohdAlfarsi.com @DrMohdAlfarsi DrMohdAlfarsi 056 224 2227 Overview Overview
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
2/28/18. Muscular System. 1 Copyright 2016 by Elsevier Inc. All rights reserved. Introduction. Physiology. Anatomy. Muscle Fiber
 Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
2/28/18. Muscular System. Introduction. Anatomy. Chapter 20
 Muscular System Chapter 20 1 Introduction Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Muscular System Chapter 20 1 Introduction Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
TMJ UNDERSTANDING SYNDROME SPECIAL REPORT By Paul R. White, D.D.S. Special Report: Understanding TMJ Syndrome
 SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
SPECIAL REPORT Special Report: Understanding TMJ Syndrome UNDERSTANDING TMJ SYNDROME By Paul R. White, D.D.S. 804.715.1647 www.smilerichmond.com 804.715.1647 www.smilerichmond.com 1 UNDERSTANDING TMJ SYNDROME
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem-Solving: Back
 Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
CHAPTER 6 2/9/2016. Learning Objectives List the four traits that all muscle types have in common.
 Learning Objectives List the four traits that all muscle types have in common. CHAPTER 6 The Muscular System Demonstrate and explain the use of antagonistic muscle pairs. Describe the attachment of muscle
Learning Objectives List the four traits that all muscle types have in common. CHAPTER 6 The Muscular System Demonstrate and explain the use of antagonistic muscle pairs. Describe the attachment of muscle
Temporomandibular Joint Treatment
 Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
Temporomandibular Joint Treatment Preamble As stated in the AAMT Position Statement, the Code of Ethics and Standards of Practice governing massage therapy apply to treating the Temporomandibular Joint
Anatomy & Physiology B. Chapter 6: Muscles
 Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
Anatomy & Physiology B Chapter 6: Muscles Warm-up What are the three types of muscle tissue? Where are each located? Which are voluntary and which are involuntary? Which are striated which are unstriated?
7/10/18. Introduction. Muscular System. Anatomy. Physiology. Skeletal Muscle Anatomy. Muscle Fiber
 Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
10/4/18. Muscular System. 1 Copyright 2016 by Elsevier Inc. All rights reserved. Introduction. Anatomy. Physiology. Skeletal Muscle Anatomy
 Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction Muscular System Chapter 20 Shortening or lengthening of a muscle results from changes in relative positions of one small part of a muscle cell to another To understand contraction, we will
Introduction to Occlusion and Mechanics of Mandibular Movement
 Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
Introduction to Occlusion and Mechanics of Mandibular Movement Dr. Pauline Hayes Garrett Department of Endodontics, Prosthodontics, and Operative Dentistry University of Maryland, Baltimore Assigned reading
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Principle of Occlusion
 Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Principle of Occlusion Mohammed Alfarsi BDS, MDSc(Pros), PhD www.drmohdalfarsi.com com.+*()ا&%$ر"!. www Overview Principle of Occlusion Overview Principle of Occlusion Point centric Long centric Freedom
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Pain Differential Diagnosis - Enrico Dellacà M.D Ph.D. Abductor pollicis brevis muscle Myofascial Pain Syndrome
 Overview Abductor pollicis brevis muscle Myofascial Pain Syndrome Definition Pain Differential Diagnosis - Enrico Dellacà M.D Ph.D. The Myofascial pain syndrome (MPS) is a syndrome characterized by chronic
Overview Abductor pollicis brevis muscle Myofascial Pain Syndrome Definition Pain Differential Diagnosis - Enrico Dellacà M.D Ph.D. The Myofascial pain syndrome (MPS) is a syndrome characterized by chronic
CLASS SET Unit 4: The Muscular System STUDY GUIDE
 NPHS Anatomy & Physiology Questions to answer: 1) List three functions of the muscular system. 1) movement 2) thermogenesis (generates heat) 3) posture & body/joint support CLASS SET Unit 4: The Muscular
NPHS Anatomy & Physiology Questions to answer: 1) List three functions of the muscular system. 1) movement 2) thermogenesis (generates heat) 3) posture & body/joint support CLASS SET Unit 4: The Muscular
Emad F. Abdallah, DMD, MS Member, American Association of Orthodontists Diplomate, American Board of Orofacial Pain
 Patient s Date: Age: Sex: Date of Birth: Home Occupation: Chief Complaint: Duration of the problem: Problem most severe: Morning Afternoon Evening Sleeping Eating No pattern SYMPTOMS Left Right Face Pain
Patient s Date: Age: Sex: Date of Birth: Home Occupation: Chief Complaint: Duration of the problem: Problem most severe: Morning Afternoon Evening Sleeping Eating No pattern SYMPTOMS Left Right Face Pain
Initial Doctor Questionnaire
 Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Initial Doctor Questionnaire DO NOT enter the patient in this study: if your patient does not have a TMD pain diagnosis if your patient does not need treatment at this time if you are not going to treat
Case Presentation #1 for the American Board of Craniofacial Pain July 2013
 Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Case Presentation #1 for the American Board of Craniofacial Pain July 2013 Case I Summary Presentation Pain in right temporomandibular joint with opening of mouth( 7 out of 10 ). Acute right non-reducing
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Chapter 9 - Muscle and Muscle Tissue
 Chapter 9 - Muscle and Muscle Tissue I. Overview of muscle tissue A. Three muscle types in the body: B. Special characteristics 1. Excitability: able to receive and respond to a stimulus 2. Contractility:
Chapter 9 - Muscle and Muscle Tissue I. Overview of muscle tissue A. Three muscle types in the body: B. Special characteristics 1. Excitability: able to receive and respond to a stimulus 2. Contractility:
33.2. Muscular System. Humans have three types of muscle.
 33.2 Muscular System VOCABULARY muscular system muscle fiber skeletal muscle tendon smooth muscle cardiac muscle myofibril sarcomere 10A, 10C, 11A Key Concept Muscles are tissues that can contract, enabling
33.2 Muscular System VOCABULARY muscular system muscle fiber skeletal muscle tendon smooth muscle cardiac muscle myofibril sarcomere 10A, 10C, 11A Key Concept Muscles are tissues that can contract, enabling
Human Anatomy and Physiology - Problem Drill 09: The Muscular System
 Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
Human Anatomy and Physiology - Problem Drill 09: The Muscular System Question No. 1 of 10 The muscular system of the human body fulfills many different roles. Which of the following statements about the
