Dual infections with different Legionella strains
|
|
|
- Arron Cameron
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE BACTERIOLOGY Dual infections with different Legionella strains G. Wewalka 1, D. Schmid 1, T. G. Harrison 2, S. A. Uldum 3 and C. L uck 4 on behalf of the European Society of Clinical Microbiology Infectious Diseases Study Group for Legionella Infections (ESGLI) 1) AGES, Institute for Medical Microbiology and Hygiene, Vienna, Austria, 2) Microbiology Service Division, HPA, London, UK, 3) Serum Statens Institute, Copenhagen, Denmark and 4) Institute of Medical Microbiology and Hygiene, Dresden, Germany Abstract In 2010 a case of a dual infection with Legionella pneumophila serogroup (sg) 1 and sg 3 was identified by culture of a blood sample collected from a female Austrian patient with septic pneumonia. Subsequently all 35 European National Legionella Reference Laboratories were interviewed regarding the frequency of dual infections in legionellosis. The Reference Laboratories in Denmark, the UK and Germany reported the detection of another 14 cases of dual infections with different Legionella strains between 2002 and Among the 15 cases, there were four cases with different Legionella species, six cases with different L. pneumophila serogroups, and five cases of dual infections with L. pneumophila sg 1 with different MAb-types. The median age of the 15 cases was 56 years and the male to female ratio 1:1.14. Six of the 15 patients were receiving immunosuppressive treatment following organ transplantation (n = 3) or for underlying haematological and solid malignancies (n = 3). Five of the 15 cases died within 30 days following diagnosis. Efforts to detect dual infections with different Legionella strains will improve our ability to correctly elucidate the causative sources of infection and enhance our understanding of the epidemiology of Legionella infections. Keywords: Case report, diagnosis, epidemiology, Legionnaires disease, multiple-strain infection Original Submission: 21 March 2013; Revised Submission: 3 June 2013; Accepted: 19 June 2013 Editor: G. Greub Article published online: 25 June 2013 Clin Microbiol Infect 2014; 20: O13 O / Corresponding author: G. Wewalka, Austrian National Reference Centre for Legionella Infections, Austrian Agency for Health and Food Safety, Institute for Medical Microbiology and Hygiene, W ahringer Straße 25a, 1096 Vienna, Austria E-mal: guenther.wewalka@ages.at Introduction Legionnaires disease (LD) is characterized by pneumonia caused by Legionella spp. These intracellular bacteria, which live in water and other moist environments, multiply in amoebae. According to a German study [1], almost 4% of all cases of community-acquired pneumonia are caused by Legionella spp. It is estimated that about cases of LD may occur in Germany every year but only about 500 cases are annually diagnosed and reported [2]. Apart from under-reporting, under-diagnosing of this disease also contributes to the underestimation of the true number of cases. From , 81.0 to 81.9% of the cases of LD reported in Europe to the European Working Group for Legionella Infection (EWGLI) and from 2009 on to the European Legionnaires Disease Surveillance Network (ELDSNet) were diagnosed by urinary antigen detection [3 5]. According to a review article from the Lancet, multiple-strain infections have been shown in more than 50 human pathogens [6]. The real frequency of multiple-strain infections might be underestimated in many cases because of technical limitations of detection. For LD it is not possible to identify cases of dual infections with different strains using only urinary antigen detection tests. Usually isolation of Legionella by culture is required to identify cases with more than one Legionella strain. A combination of culture and PCR/urinary antigen detection can reveal information on a dual infection with different Legionella species (e.g. case 15). Among the European cases notified in 2007 to 2010 only 8.8 to 10.3% were diagnosed by culture. In cases confirmed by culture only one single strain of Legionella is generally identified [3 5]. Clinical Microbiology and Infection ª2013 European Society of Clinical Microbiology and Infectious Diseases
2 O14 Clinical Microbiology and Infection, Volume 20 Number 1, January 2014 CMI We report on an Austrian case of an infection caused by two different Legionella strains. Recognition of this case raised the question of how common are infections with more than one Legionella strain. Methods The question of whether to ascertain information on further infections due to two (or more) different Legionella strains in Europe was put to the 35 European National Legionella Reference Laboratories, through the European Working Group for Legionella Infections (EWGLI), renamed as the ESCMID Study Group for Legionella Infections (ESGLI) in September These enquiries, to which all the Reference Laboratories responded, revealed 14 further cases. Information on such cases was provided by laboratories in Denmark (six cases), Germany (four cases) the UK (four cases). Data for the cases with dual Legionella infections on age, sex, underlying disease, categorized as severe (including status after organ transplantation and treatment for malignant disease) or moderate (including acute and chronic respiratory disease, chronic heart disease and status after surgical intervention), category of exposure (nosocomial, travel associated or community acquired), causative Legionella strains, source of infection and outcome were collected and analysed. The isolates of L. pneumophila sg 1 were serotyped by use of the monoclonal antibody panel (MAb-types) described by Helbig et al. [7]. All isolates were genotyped by sequence-based typing (SBT) of seven genes according to Gaia et al. [8] and Ratzow et al. [9]. Species of Legionella other than pneumophila were confirmed by mip gene sequencing [10] or MALDI-TOF (matrix-assisted-laser-desorption-deionization mass spectrometry) [11]. We also performed a review of the literature of the past 10 years focusing on dual infections with different Legionella strains in terms of multiple Legionella strain infection. Results Case series Case 1 from Austria, 2010: On 24 July a 70-year-old female was admitted to hospital C with signs and symptoms of pneumonia. The patient was diagnosed with Legionnaires disease (LD) by a positive Legionella urinary antigen test on 25 July. The patient died on 26 July. The underlying disease, a bronchial carcinoma, had been known since The patient received 11 cycles of intravenous cytostatic therapy, followed by oral administration, but had developed brain metastasis and also suffered from moderate stage chronic obstructive pulmonary disease. The onset of LD was on 22 July. On day 1 and day 2 prior to LD onset (20 21 July), the patient was in hospital B for a c-knife intervention; on day 2 to day 6 prior to onset (16 20 July), the patient stayed at home; and on day 6 to day 16 (6 16 July) the patient was in hospital A. In order to locate the source of infection, efforts were made to gain a post-mortem isolate. An autopsy was denied for religious reasons and bronchial secretion taken prior to the patient s death was not available. Blood cultures obtained pre-mortem on 25 July, which had given negative results by routine culture methods, were still available and sent to the Austrian National Reference Laboratory for Legionella Infections. Volumes of 0.1 and 0.5 ml from the bottles (Becton Dickinson, Heidelberg, Germany) were directly plated onto glycin-polymyxin B-vancomycin-cycloheximide (GVPC) agar and buffered charcoal yeast extract (BCYE) agar. Legionella pneumophila serogroup (sg) 1 and sg 3 were detected by latex agglutination of several single colonies followed by tests with monoclonal antibodies (MAb). Based on the colony counts of the plates resulting in 10 colony-forming units per ml blood culture fluid and considering a dilution of 1:4, a concentration of about 40 Legionella cells per ml blood was estimated. Water samples were taken from locations to which the patient had been exposed within the 10 days prior to disease onset and were examined for Legionella according to ISO Table 1 shows the water sampling and the results of the water investigation. Legionella was detected in low concentrations in the water system of hospital A, hospital B and the patient s home. MAb-typing and genotyping by SBT (Tables 1 and 3) proved that the patient acquired both the strain of L. pneumophila sg 1 and sg 3 from the water system of hospital A. Case 2 from Denmark, 2002: a 47-year-old male who had a kidney transplant, had onset of disease approximately 1 month TABLE 1. Results of environmental sampling related to the Austrian case of dual infection with different Legionella strains (case 1) Date of sampling Sites of sampling 29/07 Hospital A, patient room, faucet 29/07 Hospital A, patient room, shower 29/07 Hospital B, patient room, shower 04/08 Patient home, bathroom and kitchen CFU, colony forming units. Legionella strain isolated L. pneumophila sg 1, MAb-type Bellingham, ST 81 L. pneumophila sg 3, ST 93 Concentration 1 CFU/100 ml 7 CFU/100 ml L. pneumophila sg 1. 1 CFU/100 ml MAb-type OLDA, ST 442 L. pneumophila sg CFU/100 ml
3 CMI Wewalka et al. Dual infections with Legionella strains O15 after transplantation. L. pneumophila sg 3 and L. bozemanii were isolated from a tracheal aspirate. The case was categorized as probably community acquired, because the patient only stayed in the hospital for 2 days during the 10-day incubation period and no matching Legionella strains were found in the hospital water systems. No other source of infection was found. The patient recovered. Case 3 from Denmark, 2004: a 61-year-old female with no known underlying disease or risk factors. Two L. pneumophila sg 1 strains of different MAb and sequence types (ST) were isolated from a tracheal aspirate. The case was categorized as travel associated, with a travel history to Thailand 3 to 14 days prior to onset of symptoms. It was not possible to locate the source of infection. The patient recovered. Case 4 from Denmark, 2007: a 33-year-old female with leukaemia. L. pneumophila sg 3 and L. pneumophila sg 6 were isolated from a tracheal aspirate and a sputum sample. The case was categorized as nosocomial because the patient was hospitalized for 21 days before onset of symptoms, though no matching Legionella isolates were found in the hospital water systems. The patient recovered. Case 5 from Denmark, 2007: a 60-year-old female with chronic heart disease and status after heart operations with complications. Two different isolates of L. pneumophila were cultured from respiratory tract samples. One was identified as L. pneumophila sg 3 and the second isolate could not be placed in one of the formally described serogroups but belongs to L. pneumophila type H (according to J urgen Helbig, personal communication). Both isolates belonged to the same ST. The case was categorized as nosocomial because the patient was hospitalized in an intensive care unit for 3 months before onset of symptoms of LD. Legionella strains isolated from the hospital water system matched both human isolates. The patient recovered. Case 6 from Denmark, 2011: a 75-year-old male with chronic asthma, who was a heavy smoker until 4 years prior to onset of LD. He had a heart attack and underwent several pneumonia episodes before he was hospitalized. L. pneumophila sg 6 and L. bozemanii were isolated from a tracheal aspirate. The case was categorized as community acquired because he stayed at home for approximately 10 days before onset of the symptoms. Legionella spp. were isolated in low concentrations from water samples of his residence but these did not match the human isolates. The patient recovered. Case 7 from Denmark, 2012: a 61-year-old male with arteriosclerosis and a history of smoking and alcohol abuse. Two L. pneumophila sg 1 strains of different MAb types and ST were isolated from a sputum sample. The case was categorized as travel associated, with a history of travel to Turkey 0 to 7 days prior to onset of symptoms. The patient was part of a cluster of five Danish cases of LD associated with the same hotel. L. pneumophila sg 1 isolates with the same MAb type and ST were obtained from four of the cases. Legionella was not found in the hotel water system during follow-up investigations. The patient recovered. Case 8 from Germany, 2008: a 79-year-old female with dilatative cardiopathy with insufficiency of the mitral and tricuspid valves. Eleven days after cardiac surgery for reconstruction of both valves she developed pneumonia. L. pneumophila sg 1 was isolated from a sample of pericardial fluid. L. dumoffii, confirmed by mip gene sequencing and MALDI- TOF, was isolated from pericardial fluid as well as from pleural fluid. The case was categorized as hospital acquired. Despite intensive searches the Legionella strains could not be identified in the hospital water supply. The patient died from septic shock 18 days after hospitalization. Case 9 from Germany, 2009: a 47-year-old female who had received a heart transplant 1 year earlier. Two L. pneumophila sg 1 strains of different MAb types and ST were isolated from a broncho-alveolar lavage specimen. The case was categorized as nosocomial and one matching strain was found in the hospital water system. The patient died. Case 10 from Germany, 2010: a 61-year-old male who underwent surgical removal of a neurinoma and had no immunosuppressive therapy. He developed pneumonia postoperatively. Two L. pneumophila sg 1 strains of different MAb types and ST were isolated from respiratory tract samples. The case was categorized as nosocomial because the patient was hospitalized prior to onset of LD symptoms. Both strains were also found in the hospital s water supply. The patient died. Case 11 from Germany, 2011: a 26-year-old male with a haematological malignancy. The patient had a co-infection with influenza diagnosed by PCR from bronchial lavage material. Two L. pneumophila sg 1 strains of different MAb types and ST were isolated from respiratory tract samples. The case was categorized as community acquired. No attempts to isolate Legionella from the patient s private residence were performed. The patient recovered. Case 12 from the UK, 1997: a 51-year-old female, who had received a renal transplant 1 year earlier. She was admitted to hospital with a severe group A streptococcal infection of her leg after a trip to India. Fourteen days later, she developed pneumonia. L. pneumophila sg 11, SBT 2, 10, 14, 28, 2, 5, 0 (no result with neua and neuah primers) [12] and L. longbeachae sg 1 were isolated from broncho-alveolar lavage. Initially the case was considered to be travel associated, but because the patient developed pneumonia 14 days after admission to the hospital, the case was subsequently categorized as a nosocomial case. No environmental investigations were undertaken. The patient died.
4 O16 Clinical Microbiology and Infection, Volume 20 Number 1, January 2014 CMI Case 13 from the UK, 2004: a 53-year-old male was admitted to Hospital A with bone fractures after a brawl. The patient was discharged from Hospital A after an overnight stay but was admitted to Hospital B 4 days later. He developed pneumonia 5 days after admission to Hospital B. The case had a history of smoking and alcohol abuse but no other risk factors were noted. L. pneumophila sg 1 and L. pneumophila sg 6 were isolated from broncho-alveolar lavage. The case was categorized as nosocomial and both strains were recovered from the water system of Hospital A. The patient recovered. Case 14 from the UK, 2006: a 35-year-old male, who was found nearly drowned in a partly submerged vehicle in a ditch after a traffic accident and had hypothermia. He developed aspiration pneumonia. No risk factors were known. The patient died after 12 days in intensive care with multiple lung abscesses diagnosed at post-mortem examination. L. pneumophila sg 1 and L. pneumophila sg 6 were cultured from lung tissue sampled post-mortem. The case was categorized as community acquired but no samples were taken from the ditch that the car was found in. Case 15 from the UK, 2009: a 78-year-old female fell into a river while taking her dog for a walk. She was admitted to hospital in a confused state with hypothermia. She was discharged after 3 days but readmitted to the hospital with pneumonia after another 2 days. Legionella urinary antigen tests gave indeterminate results; L. bozemanii was grown from a broncho-alveolar lavage specimen gained after 10 days of antibiotic treatment. Additionally, L. pneumophila was detected by PCR. The case was categorized as probably nosocomial, but Legionella spp. were not recovered from the hospital water system and no samples were taken from the river the patient fell into. The patient recovered. Case data analysis Data for the 15 patients with infections due to multiple Legionella strains are summarized in Table 2 and characteristics of the Legionella strains are given in Table 3. The median age was 60 years (range, years); 10 of the 15 (67%) patients were older than 50 years. Eight of these patients (53.3 %) were female. Six of the 15 (40 %) patients had severe underlying conditions: status after renal transplantation (n = 2), status after heart transplantation (n = 1), haematological malignancy (one of them with an additional co-infection with influenza) (n = 2) and bronchial cancer with current cytostatic chemotherapy (n = 1). Nine patients (60 %) had only moderate co-morbidities or no risk factors were known. Among the TABLE 2. Data provided on cases with dual infections with different Legionella strains Case No. Country of residence Age Sex Underlying disease Outcome Category of exposure Environmental source identified 1 Austria 70 Female Severe Died Nosocomial Yes 2 Denmark 47 Male Severe Recovered Community No 3 Denmark 61 Female Not known Recovered Travel No 4 Denmark 33 Female Severe Recovered Nosocomial No 5 Denmark 60 Female Moderate Recovered Nosocomial Yes 6 Denmark 75 Male Moderate Recovered Community No 7 Denmark 61 Male Moderate Recovered Travel No 8 Germany 79 Female Moderate Died Nosocomial No 9 Germany 47 Female Severe Died Nosocomial Yes 10 Germany 61 Male Moderate Died Nosocomial Yes 11 Germany 26 Male Severe Recovered Community No 12 UK 51 Female Severe Died Nosocomial No 13 UK 53 Male Moderate Recovered Nosocomial Yes 14 UK 35 Male Moderate Died Community No 15 UK 78 Female Moderate Recovered Nosocomial No TABLE 3. Data provided on Legionella strains from patients with dual infections with different Legionella strains Case No. Site of isolates First isolate MAb type ST Second isolate MAb type ST 1 Blood culture L. pneumophila sg. 1 Bellingham 81 L. pneumophila sg. 3 n.a Respiratory sample L. pneumophila sg. 3 n.a. 371 L. bozemanii n.a. n.a. 3 Respiratory sample L. pneumophila sg. 1 Benidorm 42 L. pneumophila sg. 1 A/F Respiratory sample L. pneumophila sg. 3 n.a. 371 L. pneumophila sg. 6 n.a Respiratory sample L. pneumophila sg. 3 n.a. 337 L. pneumophila n.t. n.a Respiratory sample L. pneumophila sg. 6 n.a. 499 L. bozemanii n.a. n.a. 7 Respiratory sample L. pneumophila sg. 1 Benidorm 42 L. pneumophila sg. 1 Philadelphia 37 8 Pericardial and pleural fluid L. pneumophila sg. 1 Knoxville 1352 L. dumoffii n.a. n.a. 9 Respiratory sample L. pneumophila sg. 1 Benidorm 334 L. pneumophila sg. 1 Knoxville Respiratory sample L. pneumophila sg. 1 Benidorm 8 L. pneumophila sg. 1 OLDA 1 11 Respiratory sample L. pneumophila sg. 1 Knoxville 51 L. pneumophila sg. 1 Oxford 1 12 Respiratory sample L. pneumophila sg. 11 n.a. n.t. L. longbeachae sg. 1 n.a. n.a. 13 Respiratory sample L. pneumophila sg. 1 Oxford/OLDA 59 L. pneumophila sg. 6 n.a Post-mortem lung L. pneumophila sg. 1 Oxford/OLDA 54 L. pneumophila sg. 6 n.a Respiratory sample L. bozemanii n.a. n.a. L. pneumophila by PCR n.a. n.a. MAb, monoclonal antibody; ST, sequence type; n.t., not typeable; n.a., not applicable; A/F, Allentown/France.
5 CMI Wewalka et al. Dual infections with Legionella strains O17 underlying diseases were status after heart surgery (n = 2) and nicotine and alcohol abuse (n = 2). Surface water aspiration was documented in two cases; it is unclear whether the water was the source of infection or water aspiration was a predisposing condition. Nine (60%) of the patients recovered and six (40%) died. Legionella spp. were recovered from respiratory tract samples in 12 cases (including four cases with broncho-alveolar lavage), and from lung tissue, pericardial fluid and blood culture bottles in one case each. Legionella isolates were recovered from all 15 patients: a total of 29 strains were cultured and, in one case, Legionella pneumophila was identified by use of PCR. A total of 14 isolates (48.3%) belonged to L. pneumophila sg 1. Of these isolates, nine (64.3) were MAb 3/1 positive (Philadelphia, Knoxville, Benidorm, Allentown/France) and five (35.7%) MAb 3/1 negative (Bellingham, Oxford/OLDA). A total of 11 other strains (37.9%) of L. pneumophila were determined, including sg 3 (n = 4), sg 6 (n = 4) and sg 11 (n = 1). One isolate of L. pneumophila was not typable with monoclonal antibodies against sg 1 15 and in one case serotyping was not possible because only a PCR-product was available. Five isolates (17.2%) belonged to Legionella other than pneumophila: L. bozemanii (n = 3), L. dumoffii (n = 1) and L. longbaechae sg 2 (n = 1). Nine cases (60%) were classified as nosocomial. Of these, five were proven nosocomial cases with corresponding environmental isolates. In four of these cases, both human strains were found in hospital water systems, and in one case, at least one patient strain matched with an environmental isolate. In the four other nosocomial or probably nosocomial cases, no matching environmental isolates were available. Four cases (26.7%) were community acquired and two cases (13.3%) were travel associated; also in these cases no environmental isolates were available. Discussion The review of the literature of the past 10 years on infections with different Legionella strains showed that these infections are rare. Franzin et al. [13] reported a fatal case of nosocomial co-infection of L. pneumophila sg 1 and L. bozemanii isolated from post-mortem lung tissue from Italy. Buchbinder et al. [14] described a dual infection of L. pneumophila with L. gormanii diagnosed by fluorescent in situ hybridization (FISH) and confirmed by polymerase chain reaction (PCR) in Germany. Recently, Matsui et al. [15] reported a case of a dual infection with L. rubrilucens and L. pneumophila (presumably sg 15) in Japan. L. rubrilucens was isolated from the patient s sputum and L. pneumophila was detected by PCR and urinary antigen test. L. rubrilucens and L. pneumophila sg 15 were also detected in water samples from hot springs to which the patient was exposed. Infections with different Legionella strains account for about 0.3% of all culture-proven cases diagnosed in Europe in 2002 to 2012 (17 cases including the two published ones out of about 5500 culture-proven cases). We compared the 15 cases of dual infections with different Legionella strains to all cases of LD registered in the European case database from 2007 to 2010 [3 5]. The proportion of females among cases of dual infections (53.3%) was significantly higher as compared with the total European cases (given around 27%). The case fatality in patients with dual infection was 40 %, compared with 6.6 to 10.8% annually among the European cases. The higher case fatality in patients with dual Legionella-strain infection may be ascribed to a higher frequency of severe co-morbidity in these patients as compared with patients with a single Legionella strain infection, as shown by St-Martin et al. [16]. Multiple-strain infections may more severely affect the host than a single Legionella strain infection due to mutualistic pathogen pathogen interactions such as provoking immunosuppression, which inhibit pathogen clearance and, therefore, increase the risk of fatal outcome [6]. Age did not differ significantly between the cases of dual infection and the European cases. Of the 2101 human Legionella isolates registered at the European database from 2007 to 2010, L. pneumophila sg 1 accounted for 87.39% (n = 1836). In cases of dual infection, L. pneumophila sg 1 was found in only 48.3% (14/29). L. pneumophila sg 2-14 or of unknown serogroups accounted for 11.04% (n = 232) of the isolates registered at the European database, compared with 37.9 %(11/29) of the isolates obtained from cases with dual Legionella strain infections. In cases with dual infections, five strains (17.2%) belonged to Legionella species other than pneumophila while in the European database only 38 (1.81%) isolates are Legionella species other than pneumophila. L. pneumophila sg 2 14 and Legionella species other than pneumophila are usually considered to be less virulent than L. pneumophila sg 1. Among the L. pneumophila sg 1 strains, seven out of 14 (50.0%) were MAb 3/1-negative strains, which are usually assessed as less virulent than MAb 3/1-positive strains. This frequency is much higher than that observed in culture-proven cases of LD infected by a single Legionella strain [17]. The 23 isolates of L. pneumophila, for which results of SBT were available, were compared with the sequence types (STs) of the cases registered at the EWGLI SBT database [18], comprising about 4000 human isolates up to November Only five of the isolates were common STs (ST 1, 37 and 42), which occur more than 100 times in the EWGLI SBT database; two isolates were uncommon STs (ST 59 and 93), which occur 20 to 50 times. The other 16 isolates belonged to rare STs,
6 O18 Clinical Microbiology and Infection, Volume 20 Number 1, January 2014 CMI which occur only one to nine times in the SBT database: ST 8, 187 and 334, 6 9 times; ST 81, 179, 337, 371 and 421, 2 5 times; ST 51, 54, 55, 499, 1002 and 1352, only once. Our findings support the hypothesis of Balmer and Tenner [6], who clamed that multiple infections are more likely with less virulent strains and are also more likely in immunocompromised hosts. Cases of dual infections with different Legionella strains are likely to be under-diagnosed due to the small number of culture-confirmed cases and insufficient typing. To reliably discover cases of dual Legionella strain infections it is necessary to select multiple colonies from culture plates for further characterization, reasonably at least five colonies in total, preferentially with different morphology. Cases of dual Legionella strain infections, which are not identified as such, could lead to false conclusions. For example, in case 7 two MAb-subgroups, Philadelphia and Benidorm, were identified. If only one strain was detected, the conclusion could have been that the infection was due to a L. pneumophila sg 1, subgroup Philadelphia, ST 37 strain, which would have excluded the case as part of the travel-associated cluster. Efforts to detect multiple Legionella strain infections will improve our ability to correctly elucidate the causative sources of infection and enhance our understanding of the epidemiology of Legionella infections. Acknowledgements We would like to thank Dr Jette M. Bangsborg, Herlev Hospital, Denmark, for providing isolates, Dr Tim Robotham, Falguni Naik, UK, Dr Gebhardt Fridemann, TU M unchen, and Dr Jette Jung, Max von Pettenkofer Institut M unchen, Germany, for providing patients data, and PD Dr Mag. Alexander Indra, Petra Hasenberger, AGES, Vienna, Austria, Kerstin L uck, Susann Menzel, TU Dresden, Germany, and Christina Wiid Svarrer, SSI Denmark, for performing typing of Legionella strains. Transparency Declaration This work was undertaken without funding support or study sponsors. The author received no compensation for the work, and has no relevant conflicts of interest. References 1. von Baum H, Ewig S, Marre R et al. Competence Network for Community Acquired Pneumonia Study Group. Community-acquired Legionella pneumonia: new insights from the German competence network for community acquired pneumonia. Clin Infect Dis 2008; 46: European Centre for Disease Prevention and Control (ECDC). Annual epidemiological report Reporting on 2009 surveillance data and 2010 epidemic intelligence data, Stockholm: ECDC, Available from: SUR_Annual_Epidemiological_Report_on_Communicable_Diseases_ in_europe.pdf [Accessed on 9 July 2013]. 3. Joseph CA, Rickets KD; on behalf of the European Working Group for Legionella Infections.Legionnaires disease in Europe Euro Surveill 2010; 15: pii= Available from: http// [Accessed on 9 July 2013]. 4. European Centre for Disease Prevention and Control (ECDC). Legionnaires disease in Europe, 2009, Stockholm: ECDC, Available from: _SR_Legionnaires%27%20disease_Europe_2009.pdf [Accessed on 9 July 2013]. 5. European Centre for Disease Prevention and Control (ECDC). Legionnaires disease in Europe, 2010, Stockholm ECDC; Available from: SUR-Legionnaires-disease-surveilance-2010.pdf [Accessed on 9 July 2013]. 6. Balmer O, Tanner M. Prevalence and implications of multiple-strain infections. Lancet Infect Dis 2011; 11: Helbig JH, Kurtz JB, Pastoris MC, Pelaz C, L uck PC. Antigenic lipopolysaccharide components of Legionella pneumophila recognized by monoclonal antibodies: possibilities and limitations for division of the species into serogroups. J Clin Microbiol 1997; 35: Gaia V, Fry NK, Afshar B, Lu PC, Etienne J, Peduzzi R et al. Consensus sequence-based scheme for epidemiological typing of clinical and environmental isolates of Legionella pneumophila. J Clin Microbiol 2005; 43: Ratzow S, Gaia V, Helbig JH, Fry NK, L uck PC. Addition of neua, the gene encoding N-acylneuraminate cytidylyl transferase, increases the dicriminatory ability of the consesus sequence-based scheme for typing Legionella pneumophila serogroup 1 strains. J Clin Microbiol 2007; 45: Ratcliff RM, Donnellan SC, Lanser JA, Manning PA, Heuzenroeder MW. Interspecies sequence differences in the Mip protein from the genus Legionella: implications for function and evolutionary relatedness. Mol Microbiol 1997 Sep; 25: Gaia V, Casati S, Tonolla M. Rapid identification of Legionella spp. by MALDI-TOF MS based protein mass fingerprinting. Syst Appl Microbiol 2011; 34: Farhat C, Mentasti M, Jacobs E, Fry NK, L uck C. The N-acylneuraminate cytidyltransferase gene, neua, is heterogenous in Legionella pneumophila strains but can be used as a marker for epidemiological typing in the consensus sequence-based typing scheme. J Clin Microbiol 2011 Dec; 49: doi: /jcm Epub 2011 Sep Franzin L, Cabodi D, Sinicco A, Di Petri G. Molecular typing of Legionella strains with pulsed-field gel electrophoresis and random primer-amplified polymorphic DNA in nosocomial Legionnaires disease. In: Marre R, Abu Kwaik Y, Bartlett C, Clanciott NP, Fields BC eds. Legionella, 2002, Washington, DC: ASM Press: Buchbinder S, Leitritz L, Trebesius K, Heesemann J, Banas B. Mixed lung infection by Legionella pneumophila and Legionella gormanii detected by fluorescent in situ hybridization. Infection 2004; 32: Matsui M, Fujii S-I, Shiroiwa R et al. Isolation of Legionella rubrilucens from a pneumonia patient co-infected with Legionella pneumophila. J Med Microbiol 2010; 59(Pt 10): St-Martin G, Uldum S, Mølbak K. Incidence and prognostic factors for Legionnaires Diease in Denmark Hindawi Publishing Corpo-
7 CMI Wewalka et al. Dual infections with Legionella strains O19 ration ISRN Epidemiology 2013; Article ID DOI: /2013/ Helbig JH, Bernander S, Castellani Pastoris M, Etienne J, Gaia V, Lauvers S et al. Pan-European study on culture-proven Legionnaires disease: distribution of Legionella pneumophila serogroups and monoclonal subgroups. Eur J Clin Microbiol Infect Dis 2002; 21: Metasti M, Fry NK. Euroean Working Group for Legionella Infections Sequence-Based Typing (SBT) protocol for epidemiological typing of Legionella pneumophila. Version 4.2. Oct 2009: 1-9. Available from: http// 20protocol%20for%20website%202008%20v4.2pdf [Accessed on 9 July 2013].
Abstract. Introduction
 ORIGINAL ARTICLE MYCOLOGY The occurrence of Legionella species other than Legionella pneumophila in clinical and environmental samples in Denmark identified by mip gene sequencing and matrix-assisted laser
ORIGINAL ARTICLE MYCOLOGY The occurrence of Legionella species other than Legionella pneumophila in clinical and environmental samples in Denmark identified by mip gene sequencing and matrix-assisted laser
Commercial potting soils as an alternative infection source of Legionella pneumophila and other Legionella species in Switzerland
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2009.02742.x Commercial potting soils as an alternative infection source of Legionella pneumophila and other Legionella species in Switzerland S. Casati, A. Gioria-Martinoni
ORIGINAL ARTICLE 10.1111/j.1469-0691.2009.02742.x Commercial potting soils as an alternative infection source of Legionella pneumophila and other Legionella species in Switzerland S. Casati, A. Gioria-Martinoni
Molecular epidemiology of Legionnaires disease in Israel
 ORIGINAL ARTICLE EPIDEMIOLOGY Molecular epidemiology of Legionnaires disease in Israel J. Moran-Gilad 1,2, M. Mentasti 3, T. Lazarovitch 4, Z. Huberman 5, T. Stocki 3, C. Sadik 6, T. Shahar 6, E. Anis
ORIGINAL ARTICLE EPIDEMIOLOGY Molecular epidemiology of Legionnaires disease in Israel J. Moran-Gilad 1,2, M. Mentasti 3, T. Lazarovitch 4, Z. Huberman 5, T. Stocki 3, C. Sadik 6, T. Shahar 6, E. Anis
Current and Emerging Legionella Diagnostics
 Current and Emerging Legionella Diagnostics Nicole Wolter Centre for Respiratory Diseases and Meningitis (CRDM) National Institute for Communicable Diseases nicolew@nicd.ac.za 7 th FIDSSA Conference, Cape
Current and Emerging Legionella Diagnostics Nicole Wolter Centre for Respiratory Diseases and Meningitis (CRDM) National Institute for Communicable Diseases nicolew@nicd.ac.za 7 th FIDSSA Conference, Cape
LEGIONELLOSIS: A WALK-THROUGH TO IDENTIFICATION OF THE SOURCE OF INFECTION
 Cent Eur J Public Health 2017; 25 (3): 235 239 LEGIONELLOSIS: A WALK-THROUGH TO IDENTIFICATION OF THE SOURCE OF INFECTION Dimosthenis Chochlakis 1, 2, Vassilios Sandalakis 1, 2, Maria Keramarou 1, 2, Yannis
Cent Eur J Public Health 2017; 25 (3): 235 239 LEGIONELLOSIS: A WALK-THROUGH TO IDENTIFICATION OF THE SOURCE OF INFECTION Dimosthenis Chochlakis 1, 2, Vassilios Sandalakis 1, 2, Maria Keramarou 1, 2, Yannis
Epidemiology of Legionnaires Disease in Europe Birgitta de Jong on behalf of ELDSNet ESGLI conference 22 September 2016
 Epidemiology of Legionnaires Disease in Europe 2015 Birgitta de Jong on behalf of ELDSNet ESGLI conference 22 September 2016 ELDSNet annual data set Methods ECDC coordination Collection of disaggregate
Epidemiology of Legionnaires Disease in Europe 2015 Birgitta de Jong on behalf of ELDSNet ESGLI conference 22 September 2016 ELDSNet annual data set Methods ECDC coordination Collection of disaggregate
Evaluation of the Oxoid Xpect Legionella test kit for Detection of Legionella
 JCM Accepts, published online ahead of print on 6 May 2009 J. Clin. Microbiol. doi:10.1128/jcm.00397-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 6 May 2009 J. Clin. Microbiol. doi:10.1128/jcm.00397-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Community acquired pneumonia due to Legionella pneumophila in a tertiary care hospital
 101 Research article Community acquired pneumonia due to Legionella pneumophila in a tertiary care hospital Abstract BN Dissanayake 1,, DE Jayawardena 2, CG Senevirathna 1, TM Gamage 1 Sri Lankan Journal
101 Research article Community acquired pneumonia due to Legionella pneumophila in a tertiary care hospital Abstract BN Dissanayake 1,, DE Jayawardena 2, CG Senevirathna 1, TM Gamage 1 Sri Lankan Journal
Sequence-based typing of Legionella pneumophila serogroup 1 clinical isolates from Belgium between 2000 and 2010
 Research articles Sequence-based typing of Legionella pneumophila serogroup 1 clinical isolates from Belgium between 2000 and 2010 E Vekens (labomicro@uzbrussel.be) 1, O Soetens 1, R De Mendonça 2, F Echahidi
Research articles Sequence-based typing of Legionella pneumophila serogroup 1 clinical isolates from Belgium between 2000 and 2010 E Vekens (labomicro@uzbrussel.be) 1, O Soetens 1, R De Mendonça 2, F Echahidi
NE Regional AIHA Conference Legionella Analytical Developments. Dec 5, 2014
 NE Regional AIHA Conference Legionella Analytical Developments Dec 5, 2014 Diane Miskowski EMSL Analytical Inc. Cinnaminson, NJ 856-303-2528 dmiskowski@emsl.com EMSL Analytical, Inc.-Copyright 2011 1 Legionella
NE Regional AIHA Conference Legionella Analytical Developments Dec 5, 2014 Diane Miskowski EMSL Analytical Inc. Cinnaminson, NJ 856-303-2528 dmiskowski@emsl.com EMSL Analytical, Inc.-Copyright 2011 1 Legionella
Outbreak of travel-associated Legionnaires' disease Palmanova, Mallorca (Spain), September October Main conclusions and options for response
 RAPID RISK ASSESSMENT Outbreak of travel-associated Legionnaires' disease Palmanova, Mallorca (Spain), September October 2017 23 October 2017 Main conclusions and options for response An increase in Legionnaires
RAPID RISK ASSESSMENT Outbreak of travel-associated Legionnaires' disease Palmanova, Mallorca (Spain), September October 2017 23 October 2017 Main conclusions and options for response An increase in Legionnaires
Preventing Legionella Transmission An Environmental Health View
 Preventing Legionella Transmission An Environmental Health View April 25, 2013 Erin Reinsborough Environmental Health Specialist Mission Statement Together with the Halton community, the Health Department
Preventing Legionella Transmission An Environmental Health View April 25, 2013 Erin Reinsborough Environmental Health Specialist Mission Statement Together with the Halton community, the Health Department
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 25, 2018 0800 EDT NH-HAN 20180825 Cluster of Legionella pneumophila Pneumonia (Legionnaire
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 25, 2018 0800 EDT NH-HAN 20180825 Cluster of Legionella pneumophila Pneumonia (Legionnaire
Legionnaires Disease: Epidemiology and Outbreak Investigation
 Legionnaires Disease: Epidemiology and Outbreak Investigation Ellen Laine, JD, MPH Emerging Infections Unit Infectious Disease Epidemiology, Prevention and Control Division History of Legionnaires Disease
Legionnaires Disease: Epidemiology and Outbreak Investigation Ellen Laine, JD, MPH Emerging Infections Unit Infectious Disease Epidemiology, Prevention and Control Division History of Legionnaires Disease
Legionnaires disease in Europe
 Surveillance and outbreak reports Legionnaires disease in Europe 2007 2008 C A Joseph 1, K D Ricketts (katherine.ricketts@hpa.org.uk) 1, on behalf of the European Working Group for Legionella Infections
Surveillance and outbreak reports Legionnaires disease in Europe 2007 2008 C A Joseph 1, K D Ricketts (katherine.ricketts@hpa.org.uk) 1, on behalf of the European Working Group for Legionella Infections
Legionella spp. in UK composts a potential public health issue?
 ORIGINAL ARTICLE EPIDEMIOLOGY Legionella spp. in UK composts a potential public health issue? S. L. Currie 1, T. K. Beattie 1, C. W. Knapp 1 and D. S. J. Lindsay 2 1) Department of Civil and Environmental
ORIGINAL ARTICLE EPIDEMIOLOGY Legionella spp. in UK composts a potential public health issue? S. L. Currie 1, T. K. Beattie 1, C. W. Knapp 1 and D. S. J. Lindsay 2 1) Department of Civil and Environmental
Legionellosis. Legionnaires Disease Pontiac fever Rare non pneumonic infections 10/04/2015. Nonmotile replicative phase inside amoebae
 Legionellosis Legionnaires Disease Pontiac fever Rare non pneumonic infections Planktonic flagellated virulent transmissive Nonmotile replicative phase inside amoebae 1 Biofilm in plumbing system 2 Clin
Legionellosis Legionnaires Disease Pontiac fever Rare non pneumonic infections Planktonic flagellated virulent transmissive Nonmotile replicative phase inside amoebae 1 Biofilm in plumbing system 2 Clin
Legionnaires disease, which is a severe form of. Colonization of Legionella Species in Hotel Water Systems in Turkey
 369 Colonization of Legionella Species in Hotel Water Systems in Turkey Haluk Erdogan, MD * and Hande Arslan, MD * Department of Infectious Diseases and Clinical Microbiology, Baskent University Alanya
369 Colonization of Legionella Species in Hotel Water Systems in Turkey Haluk Erdogan, MD * and Hande Arslan, MD * Department of Infectious Diseases and Clinical Microbiology, Baskent University Alanya
Evaluation of sensitivity of two serological tests for diagnosing pneumonia caused by Legionella
 J Clin Pathol 1987;40:77-82 Evaluation of sensitivity of two serological tests for diagnosing pneumonia caused by Legionella pneumophila serogroup 1 T G HARRSON,* E DOURNON,t A G TAYLOR* From the *Division
J Clin Pathol 1987;40:77-82 Evaluation of sensitivity of two serological tests for diagnosing pneumonia caused by Legionella pneumophila serogroup 1 T G HARRSON,* E DOURNON,t A G TAYLOR* From the *Division
Annual Epidemiological Report
 July 2018 Annual Epidemiological Report 1 Legionellosis in Ireland, 2017 Key Facts There were 25 cases of Legionnaires disease notified in Ireland in 2017 The rate per million population increased from
July 2018 Annual Epidemiological Report 1 Legionellosis in Ireland, 2017 Key Facts There were 25 cases of Legionnaires disease notified in Ireland in 2017 The rate per million population increased from
Development of ISO 11731:2017. Simon in t Veld Manager Microbiology Vitens Laboratorium Convenor ISO TC7/SC4/WG10 Legionella
 Development of ISO 11731:217 Simon in t Veld Manager Microbiology Vitens Laboratorium Convenor ISO TC7/SC4/WG1 Legionella Vitens Vitens Laboratory Content Standards ISO 11731:1998 ISO 11731-2:24 ISO 11731:217
Development of ISO 11731:217 Simon in t Veld Manager Microbiology Vitens Laboratorium Convenor ISO TC7/SC4/WG1 Legionella Vitens Vitens Laboratory Content Standards ISO 11731:1998 ISO 11731-2:24 ISO 11731:217
Research Article Survey of Legionella Species Found in Thai Soil
 Microbiology Volume 2012, Article ID 218791, 4 pages doi:10.1155/2012/218791 Research Article Survey of Legionella Species Found in Thai Soil Tatiana C. Travis, 1 Ellen W. Brown, 1 Leonard F. Peruski,
Microbiology Volume 2012, Article ID 218791, 4 pages doi:10.1155/2012/218791 Research Article Survey of Legionella Species Found in Thai Soil Tatiana C. Travis, 1 Ellen W. Brown, 1 Leonard F. Peruski,
Legionnella. You can t t see it but you can catch it. Dr Charmaine Gauci MD, MSc, PhD Head of Disease Surveillance Unit
 Legionnella You can t t see it but you can catch it Dr Charmaine Gauci MD, MSc, PhD Head of Disease Surveillance Unit Legionella infections First documented outbreak name from 221 cases of pneumonia occurred
Legionnella You can t t see it but you can catch it Dr Charmaine Gauci MD, MSc, PhD Head of Disease Surveillance Unit Legionella infections First documented outbreak name from 221 cases of pneumonia occurred
Guideline on the management of Legionella cases, incidents, outbreaks and clusters in the community Quick Reference Guide
 2 2014 Edition Guideline on the management of Legionella cases, incidents, outbreaks and clusters in the community Quick Reference Guide Health Protection Network Scottish Guidance November 2014 Initial
2 2014 Edition Guideline on the management of Legionella cases, incidents, outbreaks and clusters in the community Quick Reference Guide Health Protection Network Scottish Guidance November 2014 Initial
23/08/2015. What are we going to discuss here today? Legionella. Can dust and water harm you? Legionella Aspergillus
 Can dust and water harm you? Carol Robinson CNM3 Infection Prevention and Control SIVUH What are we going to discuss here today? Legionella Aspergillus Some bacteria not covered are Pseudomonas spp, Cryptosporidiosis,
Can dust and water harm you? Carol Robinson CNM3 Infection Prevention and Control SIVUH What are we going to discuss here today? Legionella Aspergillus Some bacteria not covered are Pseudomonas spp, Cryptosporidiosis,
Legionellosis Outbreak-Genesee County, June, 2014 March, Summary Analysis
 Legionellosis Outbreak-Genesee County, June, 2014 March, 2015 Summary Analysis Michigan Department of Health and Human Services Genesee County Health Department (This report was edited on January 15, 2016
Legionellosis Outbreak-Genesee County, June, 2014 March, 2015 Summary Analysis Michigan Department of Health and Human Services Genesee County Health Department (This report was edited on January 15, 2016
GUIDE TO INFECTION CONTROL IN THE HOSPITAL. Carbapenem-resistant Enterobacteriaceae
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER 47: Carbapenem-resistant Enterobacteriaceae Authors E-B Kruse, MD H. Wisplinghoff, MD Chapter Editor Michelle Doll, MD, MPH) Topic Outline Key Issue Known
2.3 Invasive Group A Streptococcal Disease
 2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
2.3 Invasive Group A Streptococcal Disease Summary Total number of cases, 2015 = 107 Crude incidence rate, 2015 = 2.3 per 100,000 population Notifications In 2015, 107 cases of invasive group A streptococcal
Methicillin-Resistant Staphylococcus aureus (MRSA) S urveillance Report 2008 Background Methods
 Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Methicillin-Resistant Staphylococcus aureus (MRSA) Surveillance Report 2008 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services
Sensitivity of three serum antibody tests in a large outbreak of Legionnaires disease in the Netherlands
 Journal of Medical Microbiology (2006), 55, 561 566 DOI 10.1099/jmm.0.46369-0 Sensitivity of three serum antibody tests in a large outbreak of Legionnaires disease in the Netherlands Ed P. F. Yzerman,
Journal of Medical Microbiology (2006), 55, 561 566 DOI 10.1099/jmm.0.46369-0 Sensitivity of three serum antibody tests in a large outbreak of Legionnaires disease in the Netherlands Ed P. F. Yzerman,
Legionella Antibodies in a Danish Hospital Staff with Known Occupational Exposure
 Environmental and Public Health Volume 2009, Article ID 812829, 6 pages doi:10.1155/2009/812829 Clinical Study Legionella Antibodies in a Danish Hospital Staff with Known Occupational Exposure M. Rudbeck,
Environmental and Public Health Volume 2009, Article ID 812829, 6 pages doi:10.1155/2009/812829 Clinical Study Legionella Antibodies in a Danish Hospital Staff with Known Occupational Exposure M. Rudbeck,
Microbiology of Atypical Pneumonia. Dr. Mohamed Medhat Ali
 Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
Microbiology of Atypical Pneumonia Dr. Mohamed Medhat Ali Pneumonia P n e u m o n i a i s a n infection of the lungs that can be caused by viruses, bacteria, and fungi. Atypical! Pneumonia Symptoms. X-ray
Identification of Mycoplasma spp. using MALDI-TOF Mass Spectrometry. Aric McDaniel
 Identification of Mycoplasma spp. using MALDI-TOF Mass Spectrometry Aric McDaniel Outline Background Information Introduction Methods Results Conclusion Next Steps Mycoplasma spp. Lack a cell wall Among
Identification of Mycoplasma spp. using MALDI-TOF Mass Spectrometry Aric McDaniel Outline Background Information Introduction Methods Results Conclusion Next Steps Mycoplasma spp. Lack a cell wall Among
MALDI-TOF MS: Translating Microbiology Laboratory Alphabet Soup to Optimize Antibiotic Therapy
 MALDI-TOF MS: Translating Microbiology Laboratory Alphabet Soup to Optimize Antibiotic Therapy September 8, 2017 Amy Carr, PharmD PGY-2 Infectious Diseases Pharmacy Resident Seton Healthcare Family amy.carr@ascension.org
MALDI-TOF MS: Translating Microbiology Laboratory Alphabet Soup to Optimize Antibiotic Therapy September 8, 2017 Amy Carr, PharmD PGY-2 Infectious Diseases Pharmacy Resident Seton Healthcare Family amy.carr@ascension.org
Legionellosis Water Management and Investigation Case Study
 Legionellosis Water Management and Investigation Case Study Michigan Department of Health and Human Services Bryce Spiker, MPH Legionellosis Epidemiologist Mike Wesenberg Environmental Health Specialist
Legionellosis Water Management and Investigation Case Study Michigan Department of Health and Human Services Bryce Spiker, MPH Legionellosis Epidemiologist Mike Wesenberg Environmental Health Specialist
ANSI/ASHRAE Standard Legionellosis: Risk Management for Building Water Systems
 ANSI/ASHRAE Standard 188-2015 Legionellosis: Risk Management for Building Water Systems Published June 26, 2015 Patricia T. Graef, P.E. Member SSPC-188 January, 2018 PURPOSE: Establish minimum legionellosis
ANSI/ASHRAE Standard 188-2015 Legionellosis: Risk Management for Building Water Systems Published June 26, 2015 Patricia T. Graef, P.E. Member SSPC-188 January, 2018 PURPOSE: Establish minimum legionellosis
Multi-clonal origin of macrolide-resistant Mycoplasma pneumoniae isolates. determined by multiple-locus variable-number tandem-repeat analysis
 JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Citation for published version (APA): IJzerman, E. P. F. (2009). Progress in diagnostics and prevention of Legionnaires' disease [S.n.
 University of Groningen Progress in diagnostics and prevention of Legionnaires' disease IJzerman, Eddy Peter Frans IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Progress in diagnostics and prevention of Legionnaires' disease IJzerman, Eddy Peter Frans IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
ARTICLE IN PRESS Systematic and Applied Microbiology xxx (2010) xxx xxx
 Systematic and Applied Microbiology xxx (2010) xxx xxx Contents lists available at ScienceDirect Systematic and Applied Microbiology journal homepage: www.elsevier.de/syapm Rapid identification of Legionella
Systematic and Applied Microbiology xxx (2010) xxx xxx Contents lists available at ScienceDirect Systematic and Applied Microbiology journal homepage: www.elsevier.de/syapm Rapid identification of Legionella
Cluster of Legionnaires disease cases caused by Legionella longbeachae serogroup 1, Scotland, August to September 2013
 Rapid communications Cluster of Legionnaires disease cases caused by, Scotland, August to September 2013 A Potts (alison.potts@nhs.net) 1, M Donaghy 1, M Marley 1, R Othieno 2, J Stevenson 2, J Hyland
Rapid communications Cluster of Legionnaires disease cases caused by, Scotland, August to September 2013 A Potts (alison.potts@nhs.net) 1, M Donaghy 1, M Marley 1, R Othieno 2, J Stevenson 2, J Hyland
Vol. 18 Weekly issue June 2013
 Europe s journal on infectious disease epidemiology, prevention and control Vol. 18 Weekly issue 23 6 June 213 Surveillance and outbreak reports Travel-associated Legionnaires disease in Europe, 21 2 by
Europe s journal on infectious disease epidemiology, prevention and control Vol. 18 Weekly issue 23 6 June 213 Surveillance and outbreak reports Travel-associated Legionnaires disease in Europe, 21 2 by
In vitro and Intracellular Activities of Peptide Deformylase. Inhibitor GSK against Legionella pneumophila Isolates
 AAC Accepts, published online ahead of print on 27 October 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.04006-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 In vitro
AAC Accepts, published online ahead of print on 27 October 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.04006-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 2 In vitro
NCCID RAPID REVIEW. 1. What are the case definitions and guidelines for surveillance and reporting purposes?
 NCCID RAPID REVIEW 1. What are the case definitions and guidelines for surveillance and reporting purposes? Middle East Respiratory Syndrome Coronavirus: Ten Questions and Answers for Canadian Public Health
NCCID RAPID REVIEW 1. What are the case definitions and guidelines for surveillance and reporting purposes? Middle East Respiratory Syndrome Coronavirus: Ten Questions and Answers for Canadian Public Health
Legionnaires Disease Q&A (General) (Source: OSHA) (4/29/10)
 Legionnaires Disease Q&A (General) (Source: OSHA) (4/29/10) Q. What is Legionnaires Disease? A. Legionnaires disease is a common name for one of the several illnesses caused by Legionella bacteria. Legionnaires
Legionnaires Disease Q&A (General) (Source: OSHA) (4/29/10) Q. What is Legionnaires Disease? A. Legionnaires disease is a common name for one of the several illnesses caused by Legionella bacteria. Legionnaires
Show me the evidence! Water can cause infection and illness if hospital water systems are not properly engineered and managed 6/29/2017
 Key Takeaways can May 5, 2017 HEALTHCARE PLUMBING SYSTEMS: PUBLIC HEALTH RISKS ASSOCIATED WITH LEGIONNAIRES DISEASE AND OTHER HEALTHCARE-ASSOCIATED INFECTIONS JOHN HANLIN AND IAN EISNER NALCO WATER A DIVISION
Key Takeaways can May 5, 2017 HEALTHCARE PLUMBING SYSTEMS: PUBLIC HEALTH RISKS ASSOCIATED WITH LEGIONNAIRES DISEASE AND OTHER HEALTHCARE-ASSOCIATED INFECTIONS JOHN HANLIN AND IAN EISNER NALCO WATER A DIVISION
Legionnaire s disease
 Legionnaire s disease Connecticut Environmental Health Association Meeting April 9, 2019 Paul Gacek MPH, CPH Legionellosis Surveillance Coordinator & Waterborne Disease Coordinator Epidemiology and Emerging
Legionnaire s disease Connecticut Environmental Health Association Meeting April 9, 2019 Paul Gacek MPH, CPH Legionellosis Surveillance Coordinator & Waterborne Disease Coordinator Epidemiology and Emerging
A Newborn withdomestically Acquired Legionnaires Disease Confirmed by Molecular Typing
 MAJOR ARTICLE A Newborn withdomestically Acquired Legionnaires Disease Confirmed by Molecular Typing Kirsi Skogberg, 1,4 J. Pekka Nuorti, 1 Harri Saxen, 5 Jaana Kusnetsov, 2 Silja Mentula, 3 Vineta Fellman,
MAJOR ARTICLE A Newborn withdomestically Acquired Legionnaires Disease Confirmed by Molecular Typing Kirsi Skogberg, 1,4 J. Pekka Nuorti, 1 Harri Saxen, 5 Jaana Kusnetsov, 2 Silja Mentula, 3 Vineta Fellman,
EPIDEMIOLOGY SURVEILLANCE REPORT Northeast Region. Namitha Reddy Regional Coordinator North/Central West Region
 EPIDEMIOLOGY SURVEILLANCE REPORT Northeast Region Namitha Reddy Regional Coordinator North/Central West Region 1 This report is for use by Public Health Officials only and not for public distribution.
EPIDEMIOLOGY SURVEILLANCE REPORT Northeast Region Namitha Reddy Regional Coordinator North/Central West Region 1 This report is for use by Public Health Officials only and not for public distribution.
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Main conclusions and options for response
 RAPID RISK ASSESSMENT Multi-country outbreak of Listeria monocytogenes PCR serogroup IVb, MLST ST6 6 December 2017 Main conclusions and options for response A multi-country outbreak of Listeria monocytogenes
RAPID RISK ASSESSMENT Multi-country outbreak of Listeria monocytogenes PCR serogroup IVb, MLST ST6 6 December 2017 Main conclusions and options for response A multi-country outbreak of Listeria monocytogenes
PCR Is Not Always the Answer
 PCR Is Not Always the Answer Nicholas M. Moore, PhD(c), MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted
PCR Is Not Always the Answer Nicholas M. Moore, PhD(c), MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted
Legionella. A detailed insight from our specialists. Overview Lifecycle How it manifests Strains and species Facts and statistics
 Legionella. A detailed insight from our specialists Overview Lifecycle How it manifests Strains and species Facts and statistics Laboratory process Sampling and analysis Illness and symptoms Interpreting
Legionella. A detailed insight from our specialists Overview Lifecycle How it manifests Strains and species Facts and statistics Laboratory process Sampling and analysis Illness and symptoms Interpreting
Whole genome mapping as a novel high-resolution typing tool for Legionella pneumophila
 JCM Accepted Manuscript Posted Online 22 July 2015 J. Clin. Microbiol. doi:10.1128/jcm.01369-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 3 Whole genome mapping as a novel
JCM Accepted Manuscript Posted Online 22 July 2015 J. Clin. Microbiol. doi:10.1128/jcm.01369-15 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 3 Whole genome mapping as a novel
Pseudomonas aeruginosa
 JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
SOP Objective To provide Healthcare Workers (HCWs) with details of the precautions necessary to minimise the risk of RSV cross-infection.
 Page 1 of 11 SOP Objective To provide Healthcare Workers (HCWs) with details of the precautions necessary to minimise the risk of RSV cross-infection. This SOP applies to all staff employed by NHS Greater
Page 1 of 11 SOP Objective To provide Healthcare Workers (HCWs) with details of the precautions necessary to minimise the risk of RSV cross-infection. This SOP applies to all staff employed by NHS Greater
Herpes virus reactivation in the ICU. M. Ieven BVIKM
 Herpes virus reactivation in the ICU M. Ieven BVIKM 07.04.2011 Introduction: Viruses identified in critically ill ICU patients Viral diseases have recently been the subject of numerous investigations in
Herpes virus reactivation in the ICU M. Ieven BVIKM 07.04.2011 Introduction: Viruses identified in critically ill ICU patients Viral diseases have recently been the subject of numerous investigations in
Pneumococcal pneumonia
 Pneumococcal pneumonia Wei Shen Lim Consultant Respiratory Physician & Honorary Professor of Medicine Nottingham University Hospitals NHS Trust University of Nottingham Declarations of interest Unrestricted
Pneumococcal pneumonia Wei Shen Lim Consultant Respiratory Physician & Honorary Professor of Medicine Nottingham University Hospitals NHS Trust University of Nottingham Declarations of interest Unrestricted
Presence and persistence of viable, clinically relevant Legionella pneumophila bacteria in
 AEM Accepted Manuscript Posted Online 17 June 2016 Appl. Environ. Microbiol. doi:10.1128/aem.00595-16 Copyright 2016 van Heijnsbergen et al. This is an open-access article distributed under the terms of
AEM Accepted Manuscript Posted Online 17 June 2016 Appl. Environ. Microbiol. doi:10.1128/aem.00595-16 Copyright 2016 van Heijnsbergen et al. This is an open-access article distributed under the terms of
point-of-care test (POCT) Definition: an analytical or diagnostic test undertaken in a setting distinct from a normal hospital or non-hospital
 point-of-care test (POCT) Definition: an analytical or diagnostic test undertaken in a setting distinct from a normal hospital or non-hospital laboratory performed by a health care professional or non-medical
point-of-care test (POCT) Definition: an analytical or diagnostic test undertaken in a setting distinct from a normal hospital or non-hospital laboratory performed by a health care professional or non-medical
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Fact Sheet: Legionellosis March 2017
 Fact Sheet Fact Sheet: Legionellosis March 2017 Brought to you by the APSP Recreational Water Quality Committee (RWQC) I. INTRODUCTION Legionellosis is an infection caused by the bacterium Legionella.
Fact Sheet Fact Sheet: Legionellosis March 2017 Brought to you by the APSP Recreational Water Quality Committee (RWQC) I. INTRODUCTION Legionellosis is an infection caused by the bacterium Legionella.
NOSOCOMIAL LEGIONELLA SEPTICEMIA IN PATIENT WITH SYSTEMIC LUPUS ERYTHEMATOSUS: A CASE REPORT AND LITERATURE REVIEW
 NOSOCOMIAL LEGIONELLA SEPTICEMIA IN PATIENT WITH SYSTEMIC LUPUS ERYTHEMATOSUS: A CASE REPORT AND LITERATURE REVIEW Theerawat Naksanguan and Pakpoom Phoompoung Division of Infectious Diseases and Tropical
NOSOCOMIAL LEGIONELLA SEPTICEMIA IN PATIENT WITH SYSTEMIC LUPUS ERYTHEMATOSUS: A CASE REPORT AND LITERATURE REVIEW Theerawat Naksanguan and Pakpoom Phoompoung Division of Infectious Diseases and Tropical
Complex clinical and microbiological effects on Legionnaires disease outcone; A retrospective cohort study
 Levcovich et al. BMC Infectious Diseases (2016) 16:75 DOI 10.1186/s12879-016-1374-9 RESEARCH ARTICLE Complex clinical and microbiological effects on Legionnaires disease outcone; A retrospective cohort
Levcovich et al. BMC Infectious Diseases (2016) 16:75 DOI 10.1186/s12879-016-1374-9 RESEARCH ARTICLE Complex clinical and microbiological effects on Legionnaires disease outcone; A retrospective cohort
Legionella pneumophila SG1 Kit for the CellStream
 Legionella pneumophila SG1 Kit for the CellStream Ultrafast Detection Including Viability Assessment Speed Separation, concentration and purification of Legionella in 1-2 hours Specificity High specificity
Legionella pneumophila SG1 Kit for the CellStream Ultrafast Detection Including Viability Assessment Speed Separation, concentration and purification of Legionella in 1-2 hours Specificity High specificity
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Healthcare-associated infections acquired in intensive care units
 SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
Örebro University Hospital
 Örebro University Hospital Department of Laboratory Medicine Susanne Jacobsson Date: 2015-02-18 Page 1 (8) Neisseria meningitidis 2014 Annual report concerning serogroup, genosubtype and antibiotic susceptibility
Örebro University Hospital Department of Laboratory Medicine Susanne Jacobsson Date: 2015-02-18 Page 1 (8) Neisseria meningitidis 2014 Annual report concerning serogroup, genosubtype and antibiotic susceptibility
ESCMID Online Lecture Library. by author
 Microbiological evaluation: how to report the results Alvaro Pascual MD, PhD Infectious Diseases and Clinical Microbiology Unit. University Hospital Virgen Macarena University of Sevilla BSI management
Microbiological evaluation: how to report the results Alvaro Pascual MD, PhD Infectious Diseases and Clinical Microbiology Unit. University Hospital Virgen Macarena University of Sevilla BSI management
Key Findings. Mortality Rates
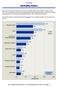 Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Mortality Rates Statewide in-hospital mortality rates showed a statistically significant decrease from to in nine of the 15 conditions reported. The largest decrease was in, where the mortality rate decreased
Received 3 August 2005/Returned for modification 13 September 2005/Accepted 13 January 2006
 CLINICAL AND VACCINE IMMUNOLOGY, Mar. 2006, p. 361 364 Vol. 13, No. 3 1556-6811/06/$08.00 0 doi:10.1128/cvi.13.3.361 364.2006 Copyright 2006, American Society for Microbiology. All Rights Reserved. Evaluation
CLINICAL AND VACCINE IMMUNOLOGY, Mar. 2006, p. 361 364 Vol. 13, No. 3 1556-6811/06/$08.00 0 doi:10.1128/cvi.13.3.361 364.2006 Copyright 2006, American Society for Microbiology. All Rights Reserved. Evaluation
ARDS with septic shock due to Legionella longbeachae pneumonia in a patient with polymyalgia rheumatica
 CASE REPORT Heart, Lung and Vessels. 2014; 6(2): 114-118 114 ARDS with septic shock due to Legionella longbeachae pneumonia in a patient with polymyalgia rheumatica T. Reynaldos Canton Migotto 1, S. Györik
CASE REPORT Heart, Lung and Vessels. 2014; 6(2): 114-118 114 ARDS with septic shock due to Legionella longbeachae pneumonia in a patient with polymyalgia rheumatica T. Reynaldos Canton Migotto 1, S. Györik
Liver cirrhosis as a predisposing condition for Legionnaires disease: a report of four laboratoryconfirmed
 Journal of Medical Microbiology (2012), 61, 1023 1028 DOI 10.1099/jmm.0.040170-0 Case Report Correspondence Zhujun Shao shaozhujun@icdc.cn Liver cirrhosis as a predisposing condition for Legionnaires disease:
Journal of Medical Microbiology (2012), 61, 1023 1028 DOI 10.1099/jmm.0.040170-0 Case Report Correspondence Zhujun Shao shaozhujun@icdc.cn Liver cirrhosis as a predisposing condition for Legionnaires disease:
PCR Is Not Always the Answer
 PCR Is Not Always the Answer Nicholas M. Moore, PhD, MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted research:
PCR Is Not Always the Answer Nicholas M. Moore, PhD, MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted research:
Pneumococcal Vaccine in Children: current situation
 Pneumococcal Vaccine in Children: current situation LAU Yu Lung Chair Professor of Paediatrics Doris Zimmern Professor in Community Child Health LKS Faculty of Medicine, The University of Hong Kong Chairman
Pneumococcal Vaccine in Children: current situation LAU Yu Lung Chair Professor of Paediatrics Doris Zimmern Professor in Community Child Health LKS Faculty of Medicine, The University of Hong Kong Chairman
IMPACT #: Local Inventory #: form 04. Age at admission: d. mo yr. Postal code:
 - Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
- Date of birth: birth: Date of admission: year month day year month day Age at admission: d mo yr Postal code: Ethnic code: Hospital: Gender: 1 = male 2 = female 1 = Impact 2 = Other local, specify: Code
Health Board Logo. Post SARS Outbreak Surveillance. Report of possible or probable cases (Form version 1) February 11 th 2004
 Post SARS Outbreak Surveillance Report of possible or probable cases (Form version 1) February 11 th 2004 This form is to be used for persons who fit the surveillance case definition of possible or probable
Post SARS Outbreak Surveillance Report of possible or probable cases (Form version 1) February 11 th 2004 This form is to be used for persons who fit the surveillance case definition of possible or probable
Chain of Infection Agent Mode of transmission Contact (direct, indirect, droplet spread) Airborne Common-vehicle spread Host
 Goals Microbiology of Healthcare-associated Infections William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University
Goals Microbiology of Healthcare-associated Infections William A. Rutala, Ph.D., M.P.H. Director, Statewide Program for Infection Control and Epidemiology and Research Professor of Medicine, University
Haemophilus influenzae, Invasive Disease rev Jan 2018
 Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
Investigating Legionella: PCR Screening and Whole-Genome Sequencing
 Investigating Legionella: PCR Screening and Whole-Genome Sequencing June 13, 2017 Kimberlee Musser, PhD Chief, Bacterial Diseases Wadsworth Center 1976 Philadelphia Legionnaires' disease outbreak 2 July
Investigating Legionella: PCR Screening and Whole-Genome Sequencing June 13, 2017 Kimberlee Musser, PhD Chief, Bacterial Diseases Wadsworth Center 1976 Philadelphia Legionnaires' disease outbreak 2 July
Legionella pneumophila SG1 Kit for the CellStream
 Legionella pneumophila SG1 Kit for the CellStream Ultrafast Detection Including Viability Assessment Speed Separation, concentration and purification of Legionella pneumophila in 1-2 hours Specificity
Legionella pneumophila SG1 Kit for the CellStream Ultrafast Detection Including Viability Assessment Speed Separation, concentration and purification of Legionella pneumophila in 1-2 hours Specificity
Sunkaru Touray 1,2, Michael C Newstein 1,2, Justin K Lui 1,2, Maureen Harris 2 and Kim Knox 2
 554673SMO0010.1177/2050312114554673SAGE Open MedicineTouray et al. research-article2014 Original Article SAGE Open Medicine Legionella pneumophila cases in a community hospital: A 12-month retrospective
554673SMO0010.1177/2050312114554673SAGE Open MedicineTouray et al. research-article2014 Original Article SAGE Open Medicine Legionella pneumophila cases in a community hospital: A 12-month retrospective
Trends in Legionnaires Disease, : Declining Mortality and New Patterns of Diagnosis
 MAJOR ARTICLE Trends in Legionnaires Disease, 1980 1998: Declining Mortality and New Patterns of Diagnosis Andrea L. Benin, a Robert F. Benson, and Richard E. Besser Respiratory Diseases Branch, Division
MAJOR ARTICLE Trends in Legionnaires Disease, 1980 1998: Declining Mortality and New Patterns of Diagnosis Andrea L. Benin, a Robert F. Benson, and Richard E. Besser Respiratory Diseases Branch, Division
Unit II Problem 2 Microbiology Lab: Pneumonia
 Unit II Problem 2 Microbiology Lab: Pneumonia - What are the steps needed to obtain a proper sputum specimen? You need the following: A wide-mouth labeled container. Gloves. Water. Mouth wash + tissues.
Unit II Problem 2 Microbiology Lab: Pneumonia - What are the steps needed to obtain a proper sputum specimen? You need the following: A wide-mouth labeled container. Gloves. Water. Mouth wash + tissues.
European Legionnaires Disease Surveillance Network (ELDSNet) TECHNICAL DOCUMENT
 European Legionnaires Disease Surveillance Network (ELDSNet) Operating procedures for the surveillance of travel-associated Legionnaires disease in the EU/EEA 2017 www.ecdc.europa.eu ECDC TECHNICAL DOCUMENT
European Legionnaires Disease Surveillance Network (ELDSNet) Operating procedures for the surveillance of travel-associated Legionnaires disease in the EU/EEA 2017 www.ecdc.europa.eu ECDC TECHNICAL DOCUMENT
6-8 November EICC, Edinburgh. Registration now open Abstract submission deadline: June 24th
 6-8 November EICC, Edinburgh Registration now open Abstract submission deadline: June 24th An outbreak of prosthetic valve endocarditis Dr Tim Boswell Consultant Medical Microbiologist Nottingham Case
6-8 November EICC, Edinburgh Registration now open Abstract submission deadline: June 24th An outbreak of prosthetic valve endocarditis Dr Tim Boswell Consultant Medical Microbiologist Nottingham Case
Infectious Disease Case Studies: What s Lurking Out There?
 Infectious Disease Case Studies: What s Lurking Out There? ASCLS-WI State Convention April 14, 2016 Case Study #2 Tim Monson, MS Microbiologist Supervisor Wisconsin State Lab of Hygiene timothy.monson@slh.wisc.edu
Infectious Disease Case Studies: What s Lurking Out There? ASCLS-WI State Convention April 14, 2016 Case Study #2 Tim Monson, MS Microbiologist Supervisor Wisconsin State Lab of Hygiene timothy.monson@slh.wisc.edu
Page 126. Type of Publication: Original Research Paper. Corresponding Author: Dr. Rajesh V., Volume 3 Issue - 4, Page No
 ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
ISSN- O: 2458-868X, ISSN P: 2458 8687 Index Copernicus Value: 49. 23 PubMed - National Library of Medicine - ID: 101731606 SJIF Impact Factor: 4.956 International Journal of Medical Science and Innovative
BC MHOs, PHNLs, ICPs, ERDOCs, IDSPEC, MEDMICRO, AMBULANCE, BCCDC Internal Groups, National Surveillance Network Partners
 To: Subject: Purpose: Action required: Recommendations: BC MHOs, PHNLs, ICPs, ERDOCs, IDSPEC, MEDMICRO, AMBULANCE, BCCDC Internal Groups, National Surveillance Network Partners November 1, 2013 Emerging
To: Subject: Purpose: Action required: Recommendations: BC MHOs, PHNLs, ICPs, ERDOCs, IDSPEC, MEDMICRO, AMBULANCE, BCCDC Internal Groups, National Surveillance Network Partners November 1, 2013 Emerging
Infections with mimivirus in patients with chronic obstructive pulmonary disease
 Respiratory Medicine (2012) 106, 1690e1694 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Infections with mimivirus in patients with chronic obstructive pulmonary
Respiratory Medicine (2012) 106, 1690e1694 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Infections with mimivirus in patients with chronic obstructive pulmonary
Influenza-Associated Pediatric Deaths Case Report Form
 STATE USE ONLY DO NOT SEND INFORMATION IN THIS SECTION TO CDC Form approved OMB No. 0920-0007 Last Name: First Name: County: Address: City: State, Zip: Patient Demographics 1. State: 2. County: 3. State
STATE USE ONLY DO NOT SEND INFORMATION IN THIS SECTION TO CDC Form approved OMB No. 0920-0007 Last Name: First Name: County: Address: City: State, Zip: Patient Demographics 1. State: 2. County: 3. State
Investigation of a Neisseria meningitidis Serogroup A Case in the Meningitis Belt. January 2017
 January 2017 Investigation of a Neisseria meningitidis Serogroup A Case in the Meningitis Belt Introduction Since the progressive introduction of meningococcal serogroup A conjugate vaccine (MACV) in the
January 2017 Investigation of a Neisseria meningitidis Serogroup A Case in the Meningitis Belt Introduction Since the progressive introduction of meningococcal serogroup A conjugate vaccine (MACV) in the
IMMUVIEW L. PNEUMOPHILA AND L. LONGBEACHAE URINARY ANTIGEN TEST. SSI Diagnostica
 IMMUVIEW L. PNEUMOPHILA AND L. LONGBEACHAE URINARY ANTIGEN TEST SSI Diagnostica 2 IMMUVIEW L. PNEUMOPHILA AND L. LONGBEACHAE URINARY ANTIGEN TEST For in vitro diagnostic use Intended use The ImmuView and
IMMUVIEW L. PNEUMOPHILA AND L. LONGBEACHAE URINARY ANTIGEN TEST SSI Diagnostica 2 IMMUVIEW L. PNEUMOPHILA AND L. LONGBEACHAE URINARY ANTIGEN TEST For in vitro diagnostic use Intended use The ImmuView and
Table Of Content. European surveillance of travel associated legionnaires' disease... 2 Summary... 3 Coordinator, Leader contact and partners...
 Table Of Content European surveillance of travel associated legionnaires' disease... 2 Summary... 3 Coordinator, Leader contact and partners... 5 Statens Serum Institute... 5 National Environmental Health
Table Of Content European surveillance of travel associated legionnaires' disease... 2 Summary... 3 Coordinator, Leader contact and partners... 5 Statens Serum Institute... 5 National Environmental Health
PROCEDURE FOR DEALING WITH MENINGITIS AND MENINGOCOCCAL DISEASE
 PROCEDURE FOR DEALING WITH MENINGITIS AND MENINGOCOCCAL DISEASE 1 INTRODUCTION 1.1 Purpose of Procedure To ensure that the University has clear guidelines on preventing or managing cases of meningitis
PROCEDURE FOR DEALING WITH MENINGITIS AND MENINGOCOCCAL DISEASE 1 INTRODUCTION 1.1 Purpose of Procedure To ensure that the University has clear guidelines on preventing or managing cases of meningitis
Surveillance of Influenza in Northern Ireland
 Surveillance of Influenza in Northern Ireland 2016 2017 Contents Summary... 1 Introduction... 3 Enhanced influenza surveillance systems... 3 In-hours Sentinel GP Practice surveillance... 3 GP Out-of-Hours
Surveillance of Influenza in Northern Ireland 2016 2017 Contents Summary... 1 Introduction... 3 Enhanced influenza surveillance systems... 3 In-hours Sentinel GP Practice surveillance... 3 GP Out-of-Hours
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
What is Legionnaires' disease?
 Understanding Legionnaires disease: A Fact Sheet For Workers Organization(s): New York Committee for Occupational Safety and Health Other languages: Spanish Summary Statement: This NYCOSH fact sheet is
Understanding Legionnaires disease: A Fact Sheet For Workers Organization(s): New York Committee for Occupational Safety and Health Other languages: Spanish Summary Statement: This NYCOSH fact sheet is
