Experimental Peri-implant Tissue Breakdown Around Different Dental Implant Surfaces: Clinical and Radiographic Evaluation in Dogs
|
|
|
- Maximilian Greene
- 5 years ago
- Views:
Transcription
1 Experimental Peri-implant Tissue Breakdown Around Different Dental Implant Surfaces: Clinical and Radiographic Evaluation in Dogs Marilia Compagnoni Martins, DDS, MS, PhD 1 /Ricardo Samih Georges Abi-Rached, DDS, MS, PhD 2 / Jamil Awad Shibli, DDS, MS, PhD 3 /Marcelo Werneck Barata Araujo, DDS, MS, PhD 3 / Elcio Marcantonio Jr, DDS, MS, PhD 2 Purpose: Tissue reactions to 4 different implant surfaces were evaluated in regard to the development and progression of ligature-induced peri-implantitis. Materials and Methods: In 6 male mongrel dogs, a total of 36 dental implants with different surfaces (9 titanium plasma-sprayed, 9 hydroxyapatitecoated, 9 acid-etched, and 9 commercially pure titanium) were placed 3 months after mandibular premolar extraction. After 3 months with optimal plaque control, abutment connection was performed. Forty-five days later, cotton ligatures were placed around the implants to induce peri-implantitis. At baseline and 20, 40, and 60 days after placement, the presence of plaque, peri-implant mucosal redness, bleeding on probing, probing depth, clinical attachment loss, mobility, vertical bone loss, and horizontal bone loss were assessed. Results: The results did not show significant differences among the surfaces for any parameter during the study (P >.05). All surfaces were equally susceptible to ligature-induced peri-implantitis over time (P <.001). Correlation analysis revealed a statistically significant relationship between width of keratinized tissue and vertical bone loss (r 2 = 0.81; P =.014) and between mobility and vertical bone loss (r 2 = 0.66; P =.04), both for the titanium plasma-sprayed surface. Discussion and Conclusions: The present data suggest that all surfaces were equally susceptible to experimental peri-implantitis after a 60-day period. INT J ORAL MAXILLOFAC IMPLANTS 2004;19: Key words: animal research, dental implants, digital radiography, implant surfaces, peri-implantitis, periodontal diseases Dental implant therapy has been associated with high success rates. 1,2 Nevertheless, dental implant failures have also been reported. 3,4 These failures can be classified on the basis of both chronologic (ie, early versus late) and etiologic aspects. Early implant failures have been attributed 1 Researcher, Department of Periodontology, Dental School at Araraquara, State University of São Paulo (UNESP), Araraquara, SP, Brazil. 2 Professor, Department of Periodontology, Dental School at Araraquara, State University of São Paulo (UNESP), Araraquara, SP, Brazil. 3 Assistant Professor, Dental Research Division, Department of Periodontology, Guarulhos University, Guarulhos, SP, Brazil. Correspondence to: Dr Elcio Marcantonio Jr, Departamento de Periodontia, Faculdade de Odontologia de Araraquara UNESP, R. Humaitá, 1680; Araraquara SP, Brasil. Fax: elciojr@foar.unesp.br to surgical trauma, poor bone quality and quantity, lack of primary stability, and bacterial contamination of the recipient site. 5 Late implant failures are commonly associated with the occurrence of periimplantitis. Peri-implantitis has been described as a destructive inflammatory process affecting the soft and hard tissues around osseointegrated implants, leading to the formation of a peri-implant pocket and loss of supporting bone. 6,7 The relationship between different dental implant surfaces and bacterial biofilm in periimplantitis development has not been completely evaluated. In addition, studies seeking to determine which surface (microstructure) or implant coating is more favorable for progression of peri-implantitis are scarce. Evaluations of peri-implantitis around uncoated, 8 10 titanium plasma-sprayed (TPS), and hydroxyapatite (HA) coated titanium dental implants have been reported The International Journal of Oral & Maxillofacial Implants 839
2 Tooth extraction Implant placement Abutment connection Ligature placement and clinical recordings Fig 1 Outline of the experiment. Thirty-six implants were placed in 6 dogs d Plaque control (chlorhexidine 0.12% daily) The aim of this study was to evaluate ligatureinduced peri-implantitis around implants with 4 different surfaces by means of clinical and radiographic evaluation in dogs. MATERIALS AND METHODS Implant Design The experimental design for this study has been previously described. 14 In brief, 36 dental implants with 4 different surfaces were used. Nine TPS implants (ITI Esthetic Plus; Straumann, Waldenburg, Switzerland); 9 HA-coated implants (Calcitek; Sulzer Medica, Carlsbad, CA), 9 implants with hybrid surfaces (machined titanium in the first 3 threads and acid-etched in other threads; Osseotite; 3i/Implant Innovations, Palm Beach Gardens, FL); and 9 commercially pure titanium (CPTi) implants (3i/Implant Innovations) were used. All implants had lengths of 10 mm and diameters of 3.75 mm (except the TPS implants, which had a diameter of 4.1 mm). Animals The Institute of Animal Care and Use Committee of the Dental School of Araraquara approved this protocol. Six adult male mongrel dogs were used. At the beginning of the study, the dogs were 2 years old, with an average weight of 18 kg. Surgery Extraction. Extractions were carried out under general anesthesia and sterile conditions using 0.05 mg/kg of subcutaneous preanesthesia sedation (atropine sulfate) and intravenous injection of chlorpromazine (0.2 ml/kg body weight) and a 4% thiopental sodium solution (0.5 ml/kg body weight). The surgical site was disinfected with 0.12% chlorhexidine. Subsequently, 2% lidocaine hydrochloride with epinephrine 1:100,000 was administered as local anesthesia, and all 4 mandibular premolars were extracted, creating an edentulous ridge. To avoid occlusal trauma interference, the maxillary premolars were also extracted. Both the mandibular quadrants and the alveoli were allowed to heal for a period of 3 months. Oral prophylaxis was performed for up to 2 weeks before tooth extraction. Plaque control during the healing period consisted of daily scrubbing with 0.12% chlorhexidine and scaling and root planing once a month until ligature placement (Fig 1). Dental Implant Placement. Under aseptic surgical conditions, all dental implants were placed using a full-thickness flap. Three implant sites per mandibular quadrant were prepared using original instruments for each dental implant system, according to the surgical techniques indicated by each implant manufacturer. A distance of approximately 10 mm between dental implant centers was maintained to avoid communication among the bone defects. The implants were randomly distributed among the dogs so that each dental implant surface was represented at least once in each animal (Table 1). The implants were placed at the bone level, and a cover screw was screwed onto the implants, including the TPS implant (this was made possible by a modification in placement technique indicated by the manufacturer, Straumann, for use with guided tissue regeneration, in which the implants are submerged) (Figs 2a and 2b). The flaps were sutured with single interrupted sutures to submerge all implants. Antibiotic therapy with potassium and sodium benzylpenicillum (24,000 IU/kg) was started and continued once a week for 2 weeks to avoid postsurgical infection, and paracetamol was given for pain control. The sutures were removed after 10 days. Experimental Peri-implantitis After a healing period of 3 months, healing abutments were connected, according to the indication of each dental implant system. After 45 days of periimplant soft tissue healing, cotton floss ligatures were placed in a submarginal position around the dental implants and sutured in the peri-implant mucosa to hold the ligatures in position (Figs 3a to 3d). The positions of the ligatures were checked twice a week; further ligatures were placed at 20- day intervals for a period of 60 days, or until the implants had a loss of about 40% of radiographic bone height, 14,15 to accelerate peri-implant bone loss (Figs 4a to 4c). 840 Volume 19, Number 6, 2004
3 Table 1 6 Dogs Random Distribution of 4 Dental Implant Surfaces in Right Left Animal PM2 PM3 PM4 PM2 PM3 PM4 1 CPTi AE TPS TPS HA AE 2 CPTi TPS HA HA AE CPTi 3 HA AE CPTi CPTi TPS HA 4 TPS HA AE AE CPTi TPS 5 HA AE CPTi CPTi TPS HA 6 TPS HA AE AE CPTi TPS TPS = titanium plasma-sprayed; HA = hydroxyapatite-coated; AE = acid-etched; CPTi = commercially pure titanium; PM2, PM3, PM4 = mandibular premolars. Fig 2a Clinical view of the implants placed at the bone level. Note the TPS implant (arrow). Fig 2b Diagram showing (A) the submerged and (B) nonsubmerged implants at level bone as well as the landmarks used to measure (1) VBL and (2) HBL. Clinical Evaluation Clinical parameters were recorded at baseline and at 20, 40, and 60 days after ligatures were placed. A single precalibrated examiner carried out the clinical exams. Presence of plaque, presence of periimplant mucosal redness, and bleeding on probing (BOP) within 30 seconds of probe retraction were recorded at distobuccal, midbuccal, mesiobuccal, mesiolingual, midlingual, and distolingual aspects of each implant. Probing depth (PD) and clinical attachment loss (CAL) were registered using a force-controlled calibrated periodontal probe (Florida Probe; Computerized Probe, Gainesville, FL) with a constant probing force of 0.20 N and a probe-tip diameter of 0.4 mm (Fig 5). PD and the distance between the gingival margin and a fixed point on the abutment surface were recorded. PD was then added to this distance to determine CAL. All measurements were performed at the same position with the aid of a dot marked in the abutment at baseline. The width of keratinized mucosa at baseline was measured to the nearest 0.5 mm at the midbuccal and midlingual aspects of each implant. Mobility Implant mobility was evaluated with the Periotest device (Siemens, Bensheim, Germany). The implants were tapped with the Periotest rod perpendicular to the longitudinal axis of the implants. The Periotest handpiece was held parallel to the floor at a distance of about 2.0 mm from the abutment surface. The spot chosen for tapping was on the buccal aspect of the abutment. This spot was marked, and the measurement was always performed at the same place. The same Periotest device was used during the entire experiment. The Periotest was calibrated before each measurement, and all measurements were performed by the same investigator. Periotest value (PTV) mean variations were assessed for each surface to avoid differences among the different implant surfaces used in this study. The International Journal of Oral & Maxillofacial Implants 841
4 Fig 3a Clinical view of experimental implants at baseline. Fig 3b Cotton floss ligature sutured in peri-implant mucosa (arrow). Fig 3c Clinical view of the same implants after a 60-day period of ligature-induced peri-implantitis. Fig 3d Detail of the peri-implant tissue breakdown (arrow) after ligature removal. Fig 4a Radiographic view at baseline of (left to right) a TPS implant, an HA-coated implant, and an acid-etched implant. Note the absence of radiolucency around all 3 experimental implants. Fig 4b Radiographic view after a 20-day period of ligature-induced peri-implantitis. Fig 4c Radiographic view of the implants after a 60-day period of ligature-induced peri-implantitis. 842 Volume 19, Number 6, 2004
5 Radiographic Analysis Standardized periapical radiographs were taken with a digital image system (Computed Dental Radiography; Schick Technologies, Long Island City, NY) to measure the relative peri-implant vertical bone loss (VBL) and horizontal bone loss (HBL). A film holder system was affixed in a silicone bite block made of polyvinylsiloxane putty impression material, which was also used to standardize the placement of the sensor in relationship to the implants and the x- ray source. Radiographs were obtained at baseline and 20, 40, and 60 days after ligature placement. A dental radiography machine equipped with a 35- cm-long cone was used to expose the periapical intraoral sensor. Exposure parameters were 70 kv (peak), 15 ma, and 0.25 second at a focus-to-sensor distance of 37 cm. The linear distance between a fixed point on the abutment and the first visible bone-to-implant contact (VBL) on the digital image was determined on the mesial and distal sides of each implant. The mesial and distal values were averaged to obtain a mean VBL for each implant. The distance between a fixed point on the implant shoulder and the crestal bone margins in the horizontal aspect on the digital image was measured to determine HBL. Two examiners made all radiographic measurements independently. If there was a discrepancy of 0.5 mm or less, the mean value of the 2 measurements was used. In situations with greater discrepancies, the images were analyzed again and discussed until consensus was reached. Statistical Analysis Data management and calculation were done using statistical software (SPSS version 10.1, Chicago, IL). Analysis of variance, using comparison of several proportions 16 (contingency table) was used to compare the distribution of percentage of plaque, redness, and BOP for each type of implant and for different locations. PD, CALs, VBL, and HBL were compared by means of 2-tailed paired t tests. To determine the correlations between keratinized tissue and clinical and radiographic features as well as the correlations between PTVs and VBL and HBL, r 2 correlation was determined. All tests were stratified according to dog (unit of analysis), ie, n = 6. Level of significance was set at.05. RESULTS Clinical Parameters At baseline, following mechanical and chemical plaque control, the percentages of positive sites for Fig 5 Clinical view of the probe at the peri-implant pocket. plaque, peri-implant marginal redness, and BOP are presented in Table 2. There were no significant differences among the dental implant surfaces at baseline. After ligature placement and plaque accumulation, all indices increased significantly over time (P <.001). Some implants (2 CPTi, 1 HA, and 2 acid-etched) did not receive a ligature after 40 days of induced peri-implantitis because 40% of the peri-implant bone had already been lost. The mean PD ranged from 1.49 ± 0.55 mm for acid-etched surfaces to 1.97 ± 0.79 mm for HAcoated surfaces at baseline. After ligature placement, mean PDs increased over time, and statistically significant differences were observed in regard to baseline (P <.001) (Table 3). However, statistically significant differences were not observed among the implant surfaces. The TPS surface had the lowest mean PD over the 60-day period (3.02 ± 0.63) followed by the CPTi (3.58 ± 0.51 mm), HA (3.76 ± 0.56 mm), and acid-etched (3.83 ± 0.62 mm) surfaces. At baseline, CAL ranged from 7.47 ± 0.48 mm for HA surfaces to 8.24 ± 0.80 mm to CPTi surfaces at baseline (Table 4). After tissue breakdown, the CAL was associated with continuous increase. The mean CAL for the 60-day period ranged from 3.87 ± 1.69 mm for the TPS surface to 5.16 ± 1.53 mm for the CPTi surface. Statistically significant differences were not observed among the surfaces (P >.05); however, statistically significant differences were observed in regard to baseline (P <.05). Width of Keratinized Mucosa At baseline, the mean width of keratinized mucosa in the buccal and lingual aspects was 2.04 ± 0.84 mm for TPS implants, 1.91 ± 0.91 mm for HAcoated implants, 2.20 ± 0.71 mm for acid-etched The International Journal of Oral & Maxillofacial Implants 843
6 Table 2 Percentage of Positive Sites (Mean ± SD) for Each Clinical Parameter at Baseline Surface Parameter TPS HA AE CPTi P* Plaque ± ± ± Gingival redness ± ± ± BOP ± ± ± ± *No significant differences were found among implant surfaces. Table 3 PD (Mean ± SD) in mm at Baseline and 20, 40, and 60 Days After Ligature Placement Surface Baseline 20 d* 40 d* 60 d* Mean TPS 1.64 ± ± ± ± ± 0.63 HA 1.97 ± ± ± ± ± 0.56 AE 1.49 ± ± ± ± ± 0.62 CPTi 1.51 ± ± ± ± ± 0.51 *Values for all 4 surfaces differed significantly from baseline (P <.001). Mean PD for the 60-day period is shown. No significant differences were found among implant surfaces (P >.05). Table 4 CAL (Mean ± SD) in mm at Baseline and 20, 40, and 60 Days After Ligature Placement Mean Surface Baseline 20 d* 40 d* 60 d* over time TPS 7.60 ± ± ± ± ± 1.69 HA 7.47 ± ± ± ± ± 0.80 AE 8.08 ± ± ± ± ± 1.13 CPTi 8.24 ± ± ± ± ± 1.53 *Values for all 4 surfaces differed significantly from baseline (P =.002 for the TPS surface and P <.001 for all other surfaces). Mean CAL for the 60-day period is shown. No significant differences were found among implant surfaces (P >.05). Table 5 PTVs (Mean ± SD) at Baseline and 20, 40, and 60 Days After Ligature Placement Variation between Surface Baseline 20 d 40 d 60 d* baseline and 60 d TPS 2.17 ± ± ± ± ± HA 2.67 ± ± ± ± ± 3.01 AE 1.67 ± ± ± ± ± 2.00 CPTi 1.50 ± ± ± ± ± 3.54 *Values for all 4 surfaces differed significantly from baseline (P <.001 for the TPS surface, P =.017 for the HA-coated surface, P =.004 for the AE surface, and P =.045 for the CPTi surface). No significant differences were found among implant surfaces (P >.05). implants, and 1.95 ± 1.24 mm for CPTi implants. Statistical differences among implant surfaces were not found at baseline (P >.05). Mobility All dental implants remained immobile during the study. Mobility values were lower for the HA surface at baseline, but not significantly lower (P >.05). After ligature placement the PTV scores increased (Table 5). No significant differences were observed among implant surfaces. After ligature-induced peri-implantitis had developed, the TPS surface had the smallest difference between baseline and day 60 (1.67 ± 0.51), followed by the CPTi surface (3.83 ± 3.54), the acid-etched surface (4.00 ± 2.00), and the HA-coated surface (4.33 ± 3.01). No statistically significant differences were observed among the surfaces tested, although significant differences were observed in regard to the baseline measurements (P <.05). 844 Volume 19, Number 6, 2004
7 Table 6 VBL (Mean ± SD) in mm at Baseline and 20, 40, and 60 Days After Ligature Placement Baseline 20 d* 40 d* 60 d* Mean TPS 2.50 ± ± ± ± ± 0.97 HA 2.01 ± ± ± ± ± 0.47 AE 2.36 ± ± ± ± ± 0.57 CPTi 2.40 ± ± ± ± ± 0.61 *Values for all 4 surfaces differed significantly from baseline (P =.001 for all surfaces). Mean VBL for the 60-day period is shown. No significant differences were found among implant surfaces (P >.05). Table 7 HBL (Mean ± SD) in mm at Baseline and 20, 40, and 60 Days After Ligature Placement Baseline 20 d* 40 d* 60 d* Mean TPS 0.68 ± ± ± ± ± 0.50 HA 0.63 ± ± ± ± ± 0.35 AE 0.57 ± ± ± ± ± 1.29 CPTi 0.66 ± ± ± ± ± 0.50 *Values for all 4 surfaces differed significantly from baseline (P =.002 for the AE surface and P <.001 for all other surfaces). Mean HBL for the 60-day period is shown. No significant differences were found among implant surfaces (P >.05). Radiographic Parameters At baseline, no dental implant exhibited periimplant radiolucency. The means of relative VBL for all surfaces are presented in Table 6. Mean VBL was highest for implants with HA-coated surfaces (4.20 ± 0.47 mm) and lowest for implants with TPS surfaces (3.50 ± 0.97 mm), although no significant differences were observed among implant surfaces (P >.05). When the VBL was compared between baseline and 20, 40, and 60 days after ligature placement, statistically significant differences were observed (P <.001 for all surfaces). The mean HBLs are presented in Table 7. Mean HBL was highest for implants with acid-etched surfaces (3.27 ± 1.29 mm) and lowest for CPTi implants (2.65 ± 0.50 mm). However, no significant differences were observed among implant surfaces (P >.05). When HBL was compared between baseline and 20, 40, and 60 days after ligature placement, statistically significant differences were found (P =.002 for the AE surface and P <.001 for all other surfaces). Correlation Correlation analysis revealed a strong correlation between width of keratinized tissue and VBL for the TPS surface (r 2 = 0.81; P =.014) (Fig 6a). A significant correlation was also noted for PTV and VBL for the TPS surface (r 2 = 0.66; P =.04) (Fig 6b). DISCUSSION This study suggests that ligature-induced periimplantitis around different dental implant surfaces results in rapid peri-implant tissue breakdown in dogs. Significant attachment loss and bone loss were established within 60 days (P <.05). The implants seem to depend on a functioning tissue barrier provided by the peri-implant mucosa in close contact with the implant surface. 17 When plaque accumulation occurs, this barrier collapses, resulting in an inflammatory infiltrate, which leads to 2 distinct events: peri-implant mucositis, a lesion confined to the superficial soft tissues, and periimplantitis, which involves the deeper soft tissues as well as the peri-implant bone. 14,18,19 At baseline all parameters confirmed the healthy status of all implants, with no differences among the dental implant surfaces (Table 2). At this time plaque control was suspended and the ligatures were placed. During the following observation period the presence of plaque, redness, and BOP increased significantly for all dental implant surfaces (P <.001). Based on the available literature, it seems meaningful to use several clinical parameters to evaluate the health of dental implants The percentage of BOP was relatively high at baseline, but it was not associated with plaque and mucosal status. In periodontal disease the BOP parameter is not a useful predictor of disease activity, 25,26 although the absence of BOP is useful as a clinical indicator of The International Journal of Oral & Maxillofacial Implants 845
8 VBL (mm) VBL (mm) Keratinized tissue (mm) PTV Fig 6a Relationship between width of keratinized mucosa and VBL for TPS surface (r 2 = 0.81; P =.014). Fig 6b Relationship between PTVs and VBL for TPS surface. (r 2 = 0.66; P =.04). periodontal stability. 27 Peri-implant probing could provoke bleeding unrelated to the amount of inflammation in peri-implant soft tissues. These findings were in agreement with published animal 28,29 and human studies. 30,31 In addition, the higher BOP scores suggested that the junctional epithelium around implants might be more fragile than that found around teeth. 32,33 All implant surfaces presented an increase of PD and CAL after a short time period (20 days) (Tables 2 to 4). These increases were similar to results achieved by Lang and coworkers, 9 Schou and associates, 10 and Nociti and colleagues. 34 Increase of PD contributed to initial CAL, while other studies have shown gingival recession to be responsible for continued attachment loss. 9,11 13 The importance of the PD around dental implants has not received much attention. Several authors have evaluated relationship between PD and microbiologic and immunologic factors and have shown a positive association between deeper peri-implant pockets and the detection of periodontal pathogens. However, the clinical impact of probing measurements around dental implants is not clear. Some authors 10,29 have examined probe penetration around teeth and implants and concluded that probes penetrate deeper in peri-implant tissue. Recently, Schou and colleagues 28 evaluated probing measurements around implants and teeth in monkeys. The authors compared the PD in monkeys with healthy tissue, gingivitis/mucositis, and periodontitis/peri-implantitis. They observed that marginal inflammation was associated with deeper probe penetration around dental implants in comparison to teeth. The authors also suggested that differences between peri-implant and periodontal PD might be explained by the different marginal connective tissue fiber configurations. 9 The data obtained from the present study showed PD increase as well as CAL over time; however, the study design (clinical evaluation) did not allow direct conclusions about the influence of connective tissue fiber configuration on soft peri-implant tissue. Mobility is regarded as an important indicator of implant success or failure. 1,32 Mobility was highest for CPTi surfaces and lowest for TPS surfaces, although no statistically significant differences were observed among implant surfaces. Differences between mechanisms of osseointegration of the implant surface and bone, different macrostructures among the implant surfaces, and difference available surface areas (ie, different microstructures) may somewhat explain the different PTVs observed. In addition, the greater diameter of the TPS implants used (4.1 mm for TPS implants versus 3.75 mm for other implants) may somewhat explain and validate these data. However, all implant surfaces presented statistically significant differences from the baseline PTV after 60 days of experimental peri-implant tissue breakdown. These results are in agreement with Tillmanns and associates 11 and Ericsson and coworkers. 37 All 36 implants placed achieved successful tissue integration at baseline, demonstrating ankylotic stability without clinical signs of early failure. Crestal bone changes were observed around all implant surfaces at 60 days, although there were no statistically significant differences among implant surfaces. VBL was initially lowest for the HA-coated surface, but at the end of the experimental peri-implantitis period, the HA-coated surface presented the highest mean 846 Volume 19, Number 6, 2004
9 VBL, followed by the CPTi, acid-etched, and TPS surfaces. In a previous study, 14 VBL was measured by means of periapical intraoral radiography. The results obtained from that study and the present investigation showed that both radiographic techniques (conventional and digital) were able to assess the progression of bone loss after experimental periimplantitis. In contrast, the HBL average was higher for the acid-etched surface and lower for the CPTi surface. It can be speculated that different mechanisms are instrumental in VBL and HBL. 38 The parallel collagen fiber orientation observed around dental implants could influence this bone resorption mechanism. 28 Implant surface characteristics can influence bone response during the healing period. The sandblasted acid-etched surface has better osteoconductive properties compared to the TPS surface. 39 When the 4 different dental implant surfaces were compared, no clinically statistical difference could be found. However, when the results for each dental implant surface were compared with baseline recordings, statistical differences were found for all clinical and radiographic parameters in this investigation. These findings suggest, in the short term (60 days), that the analyzed dental implant surfaces are similarly susceptible to and respond similarly to ligature-induced peri-implantitis. The finding concerning which implant surface is more susceptible to peri-implant infection is still controversial. Studies have shown that TPS and HA surfaces are most affected by peri-implant disease. 5,17,40,41 In the present investigation, contrasts were found with regard to bone loss. The TPS surface presented the lowest means for VBL while the CPTi surface presented a lower range for HBL. The HA-coated surface exhibited both the highest VBL over time and the greatest HBL. Some authors have suggested that the HA-coated surface may be reabsorbed and consequently may lose osseointegration in the presence of periodontal pathogens. 41,42 However, the present data must be analyzed with caution because of the short period utilized for periimplant tissue breakdown, the small sample size, the mechanical production of peri-implantitis, and the use of an animal model. Further studies evaluating these surfaces for longer periods are needed. ACKNOWLEDGMENTS This study was supported by grants from FAPESP (Fundação de Amparo a Pesquisa do Estado de São Paulo, Brazil) nos 98/ , 98/ , and 1999/ The authors wish to thank Drs Carlos Nassar, Patricia Nassar, Rodrigo Rego, Solange Alonso Vergani, and Susana d Avila for assistance in surgical and clinical procedures. The authors also thank 3i/Implant Innovations of Brazil for supplying some of the implants used in this project. REFERENCES 1. van Steenberghe D, Quirynen M, Naert I. Survival and success rates with oral endosseous implants. In: Lang NP, Karring T, Lindhe J (eds). Proccedings of the 3rd European Worshop on Periodontology. Berlin: Quintessenz, 1999: Adell R, Lekholm U, Rockler B, et al. Marginal tissue reactions at osseointregrated titanium fixtures. (I). A 3-year longitudinal prospective study. Int J Oral Maxillofac Surg 1986;15: Quirynen M, De Soete M, van Steenberghe D. Infectious risks for oral implants: A review of the literature. Clin Oral Implants Res 2002;12: Salcetti JM, Moriarty JD, Cooper LF, et al. The clinical, microbial, and host response characteristics of the failing implant. Int J Oral Maxillofac Implants 1997;12: Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci 1998;106: Mombelli A. Prevention and therapy of peri-implant infections. In: Lang NP, Karring T, Lindhe J (ed). Proceedings of the 3rd European Worshop on Periodontology. Berlin: Quintessenz, 1999: Mombelli A, Lang NP. The diagnosis and treatment of periimplantitis. Periodontol ;17: Lindhe J, Berglundh T, Ericsson I, Liljenberg B, Marinello C. Experimental breakdown of peri-implant and periodontal tissues. A study in the beagle dog. Clin Oral Implants Res 1992;3: Lang NP, Bragger U, Walther D, Beamer B, Kornman KS. Ligature-induced peri-implant infection in cynomolgus monkeys. I. Clinical and radiographic findings. Clin Oral Implants Res 1993;4:2 11 [erratum 1993;4:11]. 10. Schou S, Holmstrup P, Stoltze K, Hjorting-Hansen E, Kornman K. Ligature-induced marginal inflamation around osseointegrated implants and ankylosed teeth. Clin Oral Implants Res 1993;4: Tillmanns HWS, Hermann JS, Cagna DR, Burgess AV, Meffert RM. Evaluation of three different dental implants in ligature-induced peri-implantitis in the beagle dog. Part I. Clinical evaluation. Int J Oral Maxillofac Implants 1997;12: Tillmanns HWS, Hermann JS, Tiffee JC, Burgess AV, Meffert RM. Evaluation of three different dental implants in ligature-induced peri-implantitis in the beagle dog. Part II. Histology and microbiology. Int J Oral Maxillofac Implants 1998;13: Hanisch O, Cortella CA, Boskovic MM, James RA, Slots J, Wikesjö UME. Experimental peri-implant tissue breakdown around hydroxyapatite-coated implants. J Periodontol 1997; 68: Shibli JA, Martins MC, Lotufo RFM, Marcantonio E Jr. Microbiologic and radiographic analysis of ligature-induced peri-implantitis with different dental implant surfaces. Int J Oral Maxillofac Implants 2003;18: The International Journal of Oral & Maxillofacial Implants 847
10 15. Wetzel AC, Vlassis J, Caffesse RG, Hämmerle CH, Lang NP. Attempts to obtain re-osseointegration following experimental peri-implantitis in dogs. Clin Oral Implants Res 1999;10: Armitage P, Berry G, Matthews JNS. Statistical Methods in Medical Research, ed 4. Great Britain: Blackwell Science, 2002: Abrahamsson I, Berglundh T, Lindhe J. Soft tissue response to plaque formation at different implant systems. A comparative study in the dog. Clin Oral Implants Res 1998;9:73 79 [erratum 1998;9:281]. 18. Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci 1998;106: Tonetti MS. Risk factors for osseodisintegration. Periodontol ;17: Rutar A, Lang NP, Buser D, Burgin W, Mombelli A. Retrospective assessment of clinical and microbiological factors affecting periimplant tissue conditions. Clin Oral Implants Res 2001;12: Leonhardt A, Adolfsson B, Lekholm U, Wikstrom M, Dahlen G. A longitudinal microbiological study on osseointegrated titanium implants in partially edentulous patients. Clin Oral Implants Res 1993;4: Becker W, Becker BE, Newman MG, Nyman S. Clinical and microbiologic findings that may contribute to dental implant failure. Int J Oral Maxillofac Implants 1990;5: George K, Zafiropoulos GG, Murat Y, Hubertus S, Nisengard RJ. Clinical and microbiological status of osseointegrated implants. J Periodontol 1994;65: Salvi GE, Lang NP. Changing paradigms in implant dentistry. Crit Rev Oral Biol Med 2001;12: Badersten A, Nilveus R, Egelberg J. Effect of nonsurgical periodontal therapy. VII. Bleeding, suppuration and probing depth in sites with probing attachment loss. J Clin Periodontol 1985;12: Lang NP, Joss A, Orsanic T, Gusberti FA, Siegrist BE. Bleeding on probing. A predictor for the progression of periodontal disease? J Clin Periodontol 1986;13: Lang NP, Adler R, Joss A, Nyman S. Absence of bleeding on probing. An indicator of periodontal stability. J Clin Periodontol 1990;17: Schou S, Holmstrup P, Stolze K, Hjorting-Hansen E, Fiehn NE, Skovgaard LT. Probing around implants and teeth with healthy or inflamed peri-implant mucosa/gingiva. A histologic comparison in cynomolgus monkeys (Macaca fascicularis). Clin Oral Implants Res 2002;13: Ericsson I, Lindhe J. Probing depth at implants and teeth. An experimental study in the dog. J Clin Periodontol 1993; 20: Lekholm U, Adell R, Lindhe J, et al. Marginal tissue reactions at osseointegrated titanium fixtures. (II) A cross-sectional retrospective study. Int J Oral Maxillofac Surg 1986; 15: Leonhardt A, Grondahl K, Bergstrom C, Lekholm U. Longterm follow-up osseointegrated titanium implants using clinical, radiographic and microbiological parameters. Clin Oral Implants Res 2002;13: Nishimura K, Itoh T, Takaki K, Hosokawa R, Naito T, Yokota M. Periodontal parameters of osseointegrated dental implants. A 4-year controlled follow-up study. Clin Oral Implants Res 1997;8: Gould T, Brunette DM, Westburg L. The attachment mechanism of epithelial cells to titanium in vitro. J Periodontal Res 1981;16: Nociti FH Jr, Toledo RC, Machado MAN, Stefani CM, Line SRP, Goncalves RB. Clinical and microbiological evaluation of ligature-induced peri-implantitis and periodontitis in dogs. Clin Oral Implants Res 2001;12: Apse P, Ellen RP, Overall CM, Zarb GA. Microbiota and crevicular fluid collagenase activity in the ossointegrated dental implant sulcus: A comparison of sites in edentulous and partially edentulous patients. J Periodontal Res 1989; 24: Shibli JA. Etiology, Progression and Treatment of Periimplant Diseases [thesis]. Araraquara, SP, Brazil: Dental School of Araraquara, Ericsson I, Randow K, Glantz PO, Lindhe J, Nilner K. Clinical and radiographical features of submerged and nonsubmerged titanium implants. Clin Oral Implants Res 1994;5: Tarnow DP, Cho SC, Wallace SS. The effect of interimplant distance on the height of inter-implant bone crest. J Periodontol 2000;71: Buser D, Schenk RK, Steinemann S, Fiorellini JP, Fox CH, Stich H. Influence of surface characteristics on bone integration of titanium implants. A histomorphometric study in miniature pigs. J Biomed Mater Res 1991;25: Wheeler SL. Eight-year clinical retrospective study of titanium plasma-sprayed and hydroxyapatite-coated cylinder implants. Int J Oral Maxillofac Implants 1996;11: Mukherjee DP, Dorairaj NR, Mills DK, Graham D, Krauser JT. Fatigue properties of hydroxyapatite-coated dental implants after exposure to a periodontal pathogen. J Biomed Mater Res 2000;53: Shibli JA, Martins MC, Nociti FH Jr, Garcia VG, Marcantonio E Jr. Treatment of ligature-induced peri-implantitis by lethal photosensitization and guided bone regeneration: A preliminary histologic study in dogs. J Periodontol 2003;74: Volume 19, Number 6, 2004
Over the past few decades, an improved
 RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
RESEARCH SANDBLASTED/ACID-ETCHED VS SMOOTH- SURFACE IMPLANTS: IMPLANT MOBILITY AND CLINICAL REACTION TO EXPERIMENTALLY INDUCED PERI-IMPLANTITIS IN BEAGLE DOGS Rodrigo Tadashi Martines, DDS; Wilson Roberto
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Interest in and studies on osseointegration
 CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
The effect of peri-implant bone exposure on soft tissue healing and bone loss in two adjacent implants
 Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Research Article J Periodontal Implant Sci 2012;42:20-24 http://dx.doi.org/10.5051/jpis.2012.42.1.20 on soft tissue healing and bone loss in two adjacent implants Seung-Yun Shin 1, Seung-Boem Kye 1, Jongrak
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
The use of dental implants to restore. Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs RESEARCH
 RESEARCH Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs Marwa Madi, MDS 1 * Osama Zakaria, MDS, PhD 2 Shohei Kasugai, DDS, PhD 2 In this study, hydroxyapatite
RESEARCH Coated vs Uncoated Implants: Bone Defect Configurations After Progressive Peri-implantitis in Dogs Marwa Madi, MDS 1 * Osama Zakaria, MDS, PhD 2 Shohei Kasugai, DDS, PhD 2 In this study, hydroxyapatite
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The 2B-3D rule for implant planning, placement and restoration
 IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
IJOI 27 INTERDISCIPLINARY TREATMENT The 2B-3D rule for implant planning, placement and restoration 1. What is biologic width? Is there a golden rule for implant planning, placement and restoration as the
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
The peri-implant mucosa has
 Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
Influence of Early Cover Screw Exposure on Crestal Bone Loss Around Implants: Intraindividual Comparison of Bone Level at Exposed and Non-Exposed Implants Tae-Hyung Kim,* Dong-Won Lee,* Chong-Kwan Kim,
SPECIAL SUPPLEMENT. Inside this issue: 2014 No. 3. Peri-implant disease Implant surface: An evolution Summaries of select scientific publications
 www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
www.jird.com SPECIAL SUPPLEMENT Inside this issue: Peri-implant disease Implant surface: An evolution Summaries of select scientific publications Official Publication of The Institute for Implant and Reconstructive
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
The International Journal of Periodontics & Restorative Dentistry
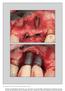 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial
 Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Interproximal Papilla Levels Following Early Versus Delayed Placement of Single-Tooth Implants: A Controlled Clinical Trial Lars Schropp, DDS, PhD /Flemming Isidor, DDS, PhD, Dr Odont /Lambros Kostopoulos,
Tae-Hyung Kim. The Graduate School. Yonsei University. Department of Dental Science
 Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
Influence of early cover screw exposure on the crestal bone loss around implants: comparison between exposed and non-exposed implants in identical subjects Tae-Hyung Kim The Graduate School Yonsei University
CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES
 Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Braz J Periodontol - September 2014 - volume 24 - issue 03 CEMENT-RETAINED PROSTHESES INCREASE RISK OF PERI-IMPLANTITIS WHEN COMPARED TO SCREW- RETAINED PROSTHESES Rachel de Queiroz Ferreira Rodrigues
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs
 Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Biologic Width and Crestal Bone Remodeling with Sintered Porous-Surfaced Dental Implants: A Study in Dogs Douglas Deporter, DDS, PhD 1 /Arwa Al-Sayyed, DDS, MSc 2 /Robert M. Pilliar, BSc, PhD 1 /Nancy
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets
 Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
INTRODUCTION. long-term results in the restoration of both totally and partially
 CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
CLINICAL RESTORATION OF THE SOFT-TISSUE MARGIN IN SINGLE-TOOTH IMPLANT IN THE ANTERIOR MAXILLA Jamil Awad Shibli, DDS, MS, PhD Susana d Avila, DDS, MS KEY WORDS Dental implants Subepithelial connective
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The clinical use of endosseous implants has
 A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
A Prospective Multicenter Clinical Trial of 3i Machined-Surface Implants: Results After 6 Years of Follow-up Dietmar Weng, DDS, Dr Med Dent 1 /Zhimon Jacobson, DDS 2 /Dennis Tarnow, DDS 3 / Markus B. Hürzeler,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
BOUCHLARIOTOU, Ioana, et al. Abstract
 Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Article Long-term stability of osseointegrated implants in bone regenerated with a collagen membrane in combination with a deproteinized bovine bone graft: 5- year follow-up of 20 implants BOUCHLARIOTOU,
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients
 Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
Amount of bone loss after maxillary dental implant loading in smoker and non-smoker patients Taha Y. Hamad, B.D.S., H.D.D., M.Sc. (1) Background: Excessive crestal bone loss after dental implant occurs
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Since the introduction of osseointegrated dental implants
 CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
CLINICAL Papilla Formation in Response to Computer-Assisted Implant Surgery and Immediate Restoration Paul A. Schnitman, DDS, MSD 1 * Chie Hayashi, DDS, PhD, MMSc 2 This retrospective analysis was undertaken
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Failures in Endosseous Dental Implants A Literature review
 Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
Eswaran Arumugam et al/ International Journal of Biomedical Research 2015; 6(10): 756-762. 756 International Journal of Biomedical Research ISSN: 0976-9633 (Online); 2455-0566 (Print) Journal DOI: 10.7439/ijbr
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Peri-implant pathology has been described as
 Microleakage at the Abutment-Implant Interface of Osseointegrated Implants: A Comparative Study Martin Gross, BDS, LDS, MSc*/Itzhak Abramovich, DMD**/Ervin I. Weiss, DMD*** Microleakage can occur at the
Microleakage at the Abutment-Implant Interface of Osseointegrated Implants: A Comparative Study Martin Gross, BDS, LDS, MSc*/Itzhak Abramovich, DMD**/Ervin I. Weiss, DMD*** Microleakage can occur at the
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
Initially, implant dentistry was focused on
 CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
CASE LETTER Correction of Esthetic Complications of a Malpositioned Implant: A Case Letter Sergio Alexandre Gehrke, PhD INTRODUCTION Initially, implant dentistry was focused on successful osseointegration
A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report of two cases
 Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Case Report J Periodontal Implant Sci 2010;40:194-200 doi: 10.5051/jpis.2010.40.4.194 A simple approach to preserve keratinized mucosa around implants using a pre-fabricated implantretained stent: a report
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
The International Journal of Periodontics & Restorative Dentistry
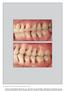 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Classifications for Gingival Recession: A Mini Review
 Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Galore International Journal of Health Sciences and Research Vol.3; Issue: 1; Jan.-March 2018 Website: www.gijhsr.com Review Article P-ISSN: 2456-9321 Classifications for Gingival Recession: A Mini Review
Effects of Immediate Loading with Threaded Hydroxyapatite-Coated Root-Form Implants on Single Premolar Replacements: A Preliminary Report
 Effects of Immediate Loading with Threaded Hydroxyapatite-Coated Root-Form Implants on Single Premolar Replacements: A Preliminary Report Periklis Proussaefs, DDS, MS 1 /Joseph Kan, DDS, MS 2 /Jaime Lozada,
Effects of Immediate Loading with Threaded Hydroxyapatite-Coated Root-Form Implants on Single Premolar Replacements: A Preliminary Report Periklis Proussaefs, DDS, MS 1 /Joseph Kan, DDS, MS 2 /Jaime Lozada,
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
An osseointegrated oral implant is characterized
 Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Mobility Assessment with the Periotest System in Relation to Histologic Findings of Oral Implants Flemming Isidor, DDS, PhD, Dr Odont* The relationship between mobility assessment with the Periotest system
Advanced Probing Techniques
 Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Module 21 Advanced Probing Techniques MODULE OVERVIEW The clinical periodontal assessment is one of the most important functions performed by dental hygienists. This module begins with a review of the
Soft tissue responses to differential shapes of the implant abutment
 대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
대한치주과학회지 : Vol. 36, No. 1, 2006 Soft tissue responses to differential shapes of the implant abutment Soo-Yong Ahn 1, Chong-Hyun Han 2, Seong-Joo Heo 3, Tae-Il Kim 1, Yang-Jo Seol 1, Yong-Moo Lee 1, Young
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report
 Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Successful Bone Formation at Immediate Transmucosal Implants: A Clinical Report Christoph H.F. Hämmerle, PD Dr med dent*/urs Brägger, Prof Dr med dent*/ Bruno Schmid, Dr med dent**/niklaus P. Lang, Prof
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Working together as a team, the periodontist
 The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
The Team Approach to Esthetic Immediate Implant Placement Bobby L. Butler, DDS; and Greggory Kinzer, DDS Working together as a team, the periodontist and restorative dentist can provide an increased level
Lethal photosensitization and guided bone regeneration in treatment of peri-implantitis: an experimental study in dogs
 Jamil Awad Shibli Marilia Compagnoni Martins Fernando Salimon Ribeiro Valdir Gouveia Garcia FranciscoHumbertoNocitiJr Elcio Marcantonio Jr Lethal photosensitization and guided bone regeneration in treatment
Jamil Awad Shibli Marilia Compagnoni Martins Fernando Salimon Ribeiro Valdir Gouveia Garcia FranciscoHumbertoNocitiJr Elcio Marcantonio Jr Lethal photosensitization and guided bone regeneration in treatment
Clinical and morphological aspects of the implant/soft tissue interface
 Clinical and morphological aspects of the implant/soft tissue interface Rodrigo F. Neiva, DDS, a Kathleen G. Neiva, DDS, b Tae-Ju Oh, DDS, MS, a and Hom-Lay Wang, DDS, MSD a a Department of Periodontics/Prevention/Geriatrics,
Clinical and morphological aspects of the implant/soft tissue interface Rodrigo F. Neiva, DDS, a Kathleen G. Neiva, DDS, b Tae-Ju Oh, DDS, MS, a and Hom-Lay Wang, DDS, MSD a a Department of Periodontics/Prevention/Geriatrics,
Department of Oral Surgery, Heinrich Heine University, D Düsseldorf, Germany.
 Lasers Surg Med. 2007 Jun;39(5):428-40 Immunohistochemical characterization of periodontal wound healing following nonsurgical treatment with fluorescence controlled Er:YAG laser radiation in dogs. Schwarz
Lasers Surg Med. 2007 Jun;39(5):428-40 Immunohistochemical characterization of periodontal wound healing following nonsurgical treatment with fluorescence controlled Er:YAG laser radiation in dogs. Schwarz
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
In the early years of modern implantology, the Brånemark
 Influence of Two Different Machined-Collar Heights on Crestal Bone Loss Mariano Herrero-Climent, MD, DDS, MSc, PhD 1 /Manuel María Romero Ruiz, MD, DDS, MSc 2 / Carmen María Díaz-Castro, DDS, MSc 3 /Pedro
Influence of Two Different Machined-Collar Heights on Crestal Bone Loss Mariano Herrero-Climent, MD, DDS, MSc, PhD 1 /Manuel María Romero Ruiz, MD, DDS, MSc 2 / Carmen María Díaz-Castro, DDS, MSc 3 /Pedro
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
INTRODUCTION MATERIAL AND METHODS
 Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
Original Research Loss of Interdental Crestal Bone Comparison Following Immediate and Delayed Loading after Delayed Placement of Dental Implants in Mandible - A Clinical Study Potharaju Santhi Priya 1,
More than pure esthetics. The natural and strong solution.
 More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
More than pure esthetics. The natural and strong solution. Expand your patient pool with an innovative solution. With the Straumann PURE Ceramic Implant, clinicians have an additional option to convince
Core build-up using post systems
 Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Core build-up using post systems Dr. Gergely Pataky Department of Conservative Dentistry What to speak about today General considerations Classification of post systems Dowel-core or fibre post? Biologic
Hyun-Jae Cho, Kun-Soo Jang, Ki-Hyun Jeong, Jae-Yun Jeon, Kyung-Gyun Hwang, Chang-Joo Park
 Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Vol. 33 No. 1, March 2014 Peri-implant gingival tissue changes following immediate placement of maxillary anterior single implant with a collagen-coated xenograft: A 1-year follow-up result Hyun-Jae Cho,
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study
 Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
Buccal Bone Resorption Around Posterior Implants After Surgery: A 1-Year Prospective Study Toshio Takuma, DDS 1,2 /Keiji Oishi, DDS, PhD 3 /Tomofusa Manabe, DT 2 / Satoshi Yoneda, DDS, PhD 4 /Toshihiko
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery
 A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
A 1-year prospective clinical study of soft tissue conditions and marginal bone changes around dental implants after flapless implant surgery Seung-Mi Jeong, DDS, PhD, a Byung-Ho Choi, DDS, PhD, b Jihun
New dental implant designs
 RESEARCH Mineralized Tissue Formation Associated With 2 Different Dental Implant Designs: Histomorphometric Analyses Performed in Dogs Sergio Olate, DDS, MS, PhD 1,2 * Henrique Duque de Miranda Chaves
RESEARCH Mineralized Tissue Formation Associated With 2 Different Dental Implant Designs: Histomorphometric Analyses Performed in Dogs Sergio Olate, DDS, MS, PhD 1,2 * Henrique Duque de Miranda Chaves
Vertical and/or horizontal alveolar
 CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
CLINICAL Vascularized Connective Tissue Flap for Bone Graft Coverage Alan S. Herford, DDS, MD 1 * Todd C. Cooper, DDS 1 Carlo Maiorana, DDS, MD 2 Marco Cicciù, DDS, PhD 2 Alveolar defects are characterized
Effect of varying horizontal mismatched implants on crestal bone level and peri-implant soft tissue: An in vivo study
 2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
2018; 4(2): 141-148 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(2): 141-148 2018 IJADS www.oraljournal.com Received: 05-02-2018 Accepted: 09-03-2018 Dr. Renu Gupta Head of Department, Department
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Review. The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang*
 The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
The Causes of Early Implant Bone Loss: Myth or Science? Tae-Ju Oh,* Joongkyo Yoon,* Carl E. Misch, and Hom-Lay Wang* The success of dental implants is highly dependent on integration between the implant
The dentogingival junction to the
 Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Volume 79 Number 10 RedefiningtheBiologicWidthinSevere, Generalized, Chronic Periodontitis: Implications for Therapy M. John Novak,* Huda M. Albather, and John M. Close Background: Previous studies demonstrated
Lethal photosensitization in microbiological treatment of ligature-induced peri-implantitis: a preliminary study in dogs
 17 Journal of Oral Science, Vol. 45, No. 1, 17-23, 2003 Original Lethal photosensitization in microbiological treatment of ligature-induced peri-implantitis: a preliminary study in dogs Jamil Awad Shibli,
17 Journal of Oral Science, Vol. 45, No. 1, 17-23, 2003 Original Lethal photosensitization in microbiological treatment of ligature-induced peri-implantitis: a preliminary study in dogs Jamil Awad Shibli,
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Improved osseiointegration techniques have led to
 Experimentally Induced Peri-implantitis: A Review of Different Treatment Methods Described in the Literature Monika Baron, MD 1 /Robert Haas, DMD, MD 2 / Orhun Dörtbudak, DMD, MD 3 /Georg Watzek, DMD,
Experimentally Induced Peri-implantitis: A Review of Different Treatment Methods Described in the Literature Monika Baron, MD 1 /Robert Haas, DMD, MD 2 / Orhun Dörtbudak, DMD, MD 3 /Georg Watzek, DMD,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Surgical reconstruction of lost papilla around implant with a modified technique: A case report
 Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
Journal of Periodontology & Implant Dentistry Case Report Surgical reconstruction of lost papilla around implant with a modified technique: A case report Mahdi Faraji* Andre Van Zyl University of Pretoria,
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
Replacement of missing teeth by means of
 Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
Peri-Implant Bone Level Around Implants with Platform-Switched Abutments Stefan Fickl, Dr Med Dent 1 /Otto Zuhr, Dr Med Dent 2 /Jamal M. Stein, Dr Med Dent 3 / Markus B. Hürzeler, Prof Dr Med Dent 2,4
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Antimicrobial Treatment of Peri-implant Diseases
 Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
