Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care
|
|
|
- Beatrice Owens
- 5 years ago
- Views:
Transcription
1 Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care Authors affiliations: Bjarni E. Pjetursson, University of Iceland, Faculty of Odontology, Reykjavik, Iceland Christoph Helbling, Giovanni E. Salvi, Urs Brägger, University of Berne School of Dental Medicine, Berne, Switzerland Hans-Peter Weber, Tufts University School of Dental Medicine, Boston, USA Giedre Matuliene, Kurt Schmidlin, Private practice, Hamburg, Germany Marcel Zwahlen, Institute of Social and Preventive Medicine, University of Berne, Switzerland Niklaus P. Lang, The University of Hong Kong, Faculty of Dentistry, Hong Kong, China Corresponding author: Bjarni E. Pjetursson, DDS, Dr.med.dent., MAS (Perio) Department of Reconstructive Dentistry University of Iceland Vatnsmyrarvegur 16 IS-101 Reykjavik, Iceland Tel.: Fax: Key words: biological complications, bleeding on probing, dental implants, implant surfaces, long-term survival, maintenance care, marginal bone loss, peri-implantitis, periodontitis, residual pockets, risk factors, supportive periodontal therapy Abstract Objective: To assess the long-term survival of implants inserted in periodontally susceptible patients and to investigate the influence of residual pockets on the incidence of peri-implantitis and implant loss. Materials and methods: For 70 patients, comprehensive periodontal treatment was followed by installation of 165 Straumann Dental implants. Subsequently, 58 patients entered a University supportive periodontal therapy (SPT) program and 12 had SPT in a private practice. The follow-up time ranged from 3 to 23 years (mean 7.9 years). Bleeding on probing (BOP), clinical attachment level (CAL), and peri-implant probing depths (PPD) were evaluated at baseline (T0), completion of active treatment (T1), and at follow-up (T2). Peri-implant bone levels were assessed on radiographs at T2. Patients were categorized as having implants not affected by peri-implantitis (non-pip), or affected by peri-implantitis (PIP). Results: From 165 implants inserted, six implants were lost, translating into a cumulative survival rate of 95.8%. Solid screw implants yielded significantly higher survival rates than the hollow cylinder and hollow screw implants (99.1% vs. 89.7%). Implants lost due to peri-implant infection were included in the PIP groups. When peri-implantitis (PPD 5 mm, BOP+) was analyzed, 22.2% of the implants and 38.6% of patients had one or more implants affected by peri-implantitis. Using the peri-implantitis definition (PPD 6 mm, BOP+), the prevalence was reduced to 8.8% and 17.1%, respectively. Moreover, all these implants demonstrated significant ( 2 mm) bone loss at T2.At T1, the non-pip group had significantly (P = 0.011) fewer residual pockets ( 5 mm) per patient than the PIP group (1.9 vs. 4.1). At T2, the PIP group displayed an increased number of residual pockets compared to T1, whereas in the non-pip group, the number remained similar to T1. At T2, mean PPD, mean CAL and BOP were significantly higher in the PIP group compared with the non-pip group. The prevalence of peri-implantitis was lower in the group that was in a well organized SPT at the University. Conclusions: In periodontitis susceptible patients, residual pockets (PPD 5 mm) at the end of active periodontal therapy represent a significant risk for the development of peri-implantitis and implant loss. Moreover, patients in SPT developing re-infections are at greater risk for periimplantitis and implant loss than periodontally stable patients. Date: Accepted 06 March 2012 To cite this article: Pjetursson BE, Helbling C, Weber H-P, Matuliene G, Salvi GE, Brägger U, Schmidlin K, Zwahlen M, Lang NP. Periimplantitis susceptibility as it relates to periodontal therapy and supportive care. Clin. Oral Impl. Res. 23, 2012; doi: /j x The use of oral implants has become integral to comprehensive dental care. Today, the application of oral implants in replacing one or several missing teeth, in partially edentulous patients represents a frequent indication (Buser et al. 2008). The primary advantage of using oral implants in this indication lies in the fact that teeth may be replaced without the need of preparing adjacent teeth to anchor fixed dental prostheses (FDP), thereby preserving natural tooth structure (Preist 1999). Moreover, shortened dental arches John Wiley & Sons A/S
2 may, if indicated, be extended with implant supported short-span fixed dental prosthesis (Brägger et al. 1990). Although the long-term survival of oral implants in the partially edentulous oral cavity is well documented and high (Berglundh et al. 2002; Pjetursson et al. 2004; Holm-Pedersen et al. 2007; Jung et al. 2008), systemic and/or local conditions may affect long-term survival or success of such treatment. Oral implants will naturally be exposed to the individual ecological conditions present in the aqueous environment of the oral cavity and hence, bio-film formation on implant surfaces occurs predictably (Lang et al. 2000). As a matter of fact, sterile oral implants are colonized by microbes within half an hour following their placement into the oral cavity (Fürst et al. 2007), and this bacterial colonization appears to be predictive for the microbiota found in peri-implant sulci after 1 year (Salvi et al. 2008). Several studies have suggested that in partially edentulous patients, periodontal pathogens may be transmitted from periodontally compromised teeth to newly installed implants implying that periodontal niches may serve as reservoirs for bacterial colonization (Apse et al. 1989; Quirynen & Listgarten 1990; Leonhardt et al. 1992, 1993; Kohavi 1993; Koka et al. 1993; Mombelli et al. 1995; Lee et al. 1999). The importance of treating existing periodontitis prior to the placement of dental implants has often been emphasized (i.e. Mombelli et al. 1995; Heitz-Mayfield & Lang 2010). It has also been shown that periodontal conditions are correlated with the clinical condition diagnosed at implant sites (Brägger et al. 1997) indicating the possibility of spread of infection from periodontally incompletely treated sites to the peri-implant sulci (Mombelli et al. 1995). Aggregatibacter actinomycetemcommitans and Porphyromonas gingivalis were more frequently present in partially edentulous patients compared to totally edentulous patients (Mombelli et al. 1987; Kalykakis et al. 1994). Implant sites harboring A. actinomycetemcommitans, P. gingivalis or Prevotella intermedia demonstrated deeper peri-implant probing depths (PPD) along with clinical signs of inflammation (Kalykakis et al. 1994). Implant sites exposed to the oral environment for 3 4 years showed deeper probing depths than those with a shorter exposure. Periodontal pathogens identified in residual periodontal pockets at the time of implant installation were found adjacent to the newly installed implants 3 and 6 months later indicating the spread of pathogens (Mombelli et al. 1995). Some authors expressed little or no concern about installing implants in patients with a history of periodontitis (Nevins & Langer 1995; Nevins 2001), whereas others pointed to the fact that patients susceptible to periodontitis may be affected by peri-implant diseases more frequently than non-susceptible patients (Ellegaard et al. 1997; Karoussis et al. 2003, 2004). In that respect, in a longitudinal study of implants installed in patients previously affected by periodontitis, the presence of putative periodontal pathogens at peri-implant and periodontal sites did not appear to predict future attachment loss or implant failures (Sbordone et al. 1999). In contrast, a 10-year prospective cohort study involving 53 patients with 112 hollow screw implants (Straumann Dental Implant System, Straumann AG, Basel, Switzerland) revealed that implants inserted as replacement of periodontally involved teeth exhibited lower survival and significantly lower success rates at various threshold levels of bleeding on probing and probing depths, as well as a significantly greater number of biological complications than implants placed in patients without a history of periodontitis (Karoussis et al. 2003). In this study, hollow and perforated screw type implants with titanium-plasma-sprayed (TPS) surfaces (HS Implants, Straumann AG, Basel, Switzerland) were assessed. These implants may have exhibited a potentially greater risk for biological complications and subsequent failure due to their design and surface characteristics. Moreover, these designs are no longer available in the market today. A recent systematic review (Ong et al. 2008) concluded on the basis of nine studies that there was evidence that patients treated for periodontitis may experience more implant loss and biological complications than non-periodontitis patients. However, methodological issues limited the potential for drawing robust conclusions. The purpose of the present study was, therefore, to further assess the long-term survival and success of solid screw, hollow screw and hollow cylinder implants in a patient cohort with a history of periodontal disease and to investigate the influence of residual pockets at the end of active periodontal treatment on the incidence of periimplantitis and implant loss. Materials and methods During the period between the years 1978 and 2002, a total of 392 patients were treated according to the protocol of comprehensive periodontal therapy at the Department of Periodontology and Fixed Prosthodontics, University of Berne, Switzerland. Implant therapy was incorporated as part of comprehensive care in Following a comprehensive examination and treatment planning (T0), the treatment consisted of cause-related initial periodontal therapy including case presentation, oral hygiene instruction, and scaling and root planing under local anesthesia if necessary. After re-evaluation of the outcomes of initial therapy, periodontal surgery was performed if indicated (Pocket Probing Depths (PPD) 6 mm). Treatment outcomes after completion of periodontal therapy were assessed (T1). Eventually, prosthetic therapy using implant- or tooth-supported FDPs was performed. Subject cohort From the 392 treated patients, 199 could be recruited and re-examined during 2005 (T2). The remaining 193 patients were either deceased, had moved away from the area or were too frail to participate in the re-examination. For the patients to be included in this study at least two additional sets of periodontal and radiological examinations at baseline (before therapy, T0) and at the end of active periodontal therapy (T1) had to be available. Finally, 172 patients, 95 (55.2%) women and 77 (44.8%) men, between 14 and 69 years of age (Mean: 45 ± 11 years) at baseline (T0) were included in the analysis. The remaining 27 patients could not be analyzed owing to the lack of a complete documentation. Using the periodontal parameters of the baseline examination (T0), all patients were classified as having Level 1 or 2 periodontitis according to the definition of a periodontal case proposed at the 5th European Workshop on Periodontology (2005) (Tonetti & Claffey 2005). From the 172 patients selected, 70 patients had one or more dental implants (Straumann AG ; Basel, Switzerland) inserted during the comprehensive treatment. From the total of 177 implants inserted, 165 were inserted as part of the initial active therapy (corrective phase), and additional 12 implants were placed later during SPT. From the 165 implants originally placed detailed information was available for 161 implants. The majority or 105 implants were inserted in the maxilla and the remainder of 60 in the mandible. Regarding implant type, 115 were solid screws implants with a TPS or a sandblasted large grit and acid attacked surface 2012 John Wiley & Sons A/S 889 Clin. Oral Impl. Res. 23, 2012 /
3 and 50 were hollow screw and hollow cylinder implants with a TPS surface (Table 1). Thirty-five of the implants were placed in the anterior area, 74 in a premolar position and 52 in a molar position. The most frequently used implant length was 10 mm (74 implants), followed by 8 mm implants (58) and 12 mm implants (23). Only 6 of the 161 implants were short 6 mm implants (Table 1). Following the completion of treatment, 47 patients (67.1%) attended the supportive periodontal therapy (SPT) program at the University of Berne and twenty-three patients (32.9%) were referred back to the referring private practitioners for maintenance care. Clinical examinations At baseline (T0), before the initiation of the initial treatment, comprehensive periodontal and radiological examinations were performed. Probing pocket depth (PPD) and recession were measured at six sites per tooth to calculate the clinical attachment level (CAL). Bleeding on probing (BOP) was recorded at four sites per tooth, and fullmouth bleeding scores were obtained. Tooth mobility (Ramfjord 1967) as well as furcation involvement of multi-rooted teeth (Hamp et al. 1975) were assessed. A full-mouth periapical x-ray status was performed and radiographic bone loss was evaluated. The same periodontal and radiological examinations were performed at the end of active therapy (T1) and at re-evaluation (T2). At the re-evaluation (T2), the full-mouth radiographs were replaced by orthopantomograms (OPT). Definition of peri-implantitis Two definitions of peri-implant mucositis or peri-implantitis were utilized (Levels 1 & 2): In the first analysis, the Level 1 was defined as sites with PPD 5 mm and BOP positive (Mombelli & Lang 1994). In the second analysis, the threshold for Level 2 was set at PPD 6 mm and BOP positive (Mombelli & Lang 1994). On radiographs, peri-implantitis was defined as implants yielding radiographic marginal bone levels of 5 mm below the implant shoulder (IS). This equaled a marginal bone loss of 2 mm compared to what can be expected as a normal remodeling for a transmucosal implant with a 2.8 mm machined neck. Smoking and health status Using a questionnaire at the re-evaluation (T2), smoking habits at the time point T2, the health status at time point T2 and the frequency of recall visits during SPT were assessed. Radiographic examination Orthopantomograms (OPT) were obtained at the time of re-evaluation (T2). To perform the measurements, the OPTs were captured using a black and white video camera (Canon; Still Video Products Group, Tokyo, Japan) and viewed on a light box. The images were transferred to a computer and digitized with frame grabber hardware (Matrox Electronic Systems MVP/AT; Dorval, Quebec, Canada). Using image-processing software, digitized images were stored with a resolution of bit pixels (256 shades of gray). Stored images were then displayed on a monitor, and linear measurements were performed with the help of a cursor (Brägger 1996) by a calibrated examiner. The measurements were all repeated at two time intervals. The magnifying factor of the OPTs was estimated by measuring the known distance between implant treads. The following measurements were made: Marginal bone level the distance from the IS to the alveolar bone crest (AC), mesially and distally. Statistiscal analysis Data were entered in a computer data base and corrected for implausible entries. Stratified descriptive information on mean CAL and PPD as well as percentage of BOP for each patient, were calculated over all recorded sites. Comparisons between the two groups of patients were made by means of t-tests. For implant loss, the unit of analysis was the implant. Cumulative survival or cumulative incidence estimates and their 95% confidence intervals (CI) derived from Kaplan Meier calculations were provided (Kaplan & Meier 1958). The survival curves for implants using the log-rank test were compared. All analyses were conducted using Stata version 11 (Stata Corporation, College Station, Texas, USA). Results At the re-evaluation visit (T2), based on the entire patient cohort, 36.9% of the patients were non-smokers, 35.7% were former smokers, and 27.4% were current smokers. Of these, 28.3% of the smokers were light smokers (1 9 cig/day), 26.1% moderate (9 19 cig/day), and 45.6% were heavy smokers ( 20 cig/day). Survival and failure rates From a total of 165 dental implants inserted as part of the initial active therapy, six implants were lost during the follow-up period. Two implants were lost in the first year of function, one implant was lost in the second year and another implant in the third year of function. The fifth and the sixth implants were lost after 6 years of function. Hence, the cumulative survival rate after a mean follow-up time of 7.9 years was 95.8% (95% CI: %). Implant survival was also calculated according to implant types. From 115 solid screw implants, only one was lost, translating into a cumulative survival rate of 99.1% (95% CI: %) after a mean follow-up time of 6.4 years (Table 2). Five of 50 hollow screw or hollow cylinder implants were lost giving a cumulative survival rate of 89.7% (95% CI: %) after a mean follow-up time of 11.1 years (Table 2). The difference in implant loss between solid screw and hollow implants reached statistical significance (P = 0.008). Peri-implant soft tissue conditions At the re-evaluation (T2), the 70 patients included had a total of 171 implants. These implants consisted of the 159 implants surviving the entire observation period from the 165 implants originally placed during initial active therapy. In addition, 12 implants had been installed during the follow-up period (totaling 171 implants). For the evaluation of peri-implant soft tissue conditions, all 171 implants were included. At the time of re-evaluation (T2), 22.2% of the implants were affected by periimplantitis Level 1 (PPD 5 mm and BOP positive (Mombelli & Lang 1994)) or were lost due to peri-implantitis during the observation period. Moreover, on a patient level, 27 of the 70 patients (38.6%) had one or more implants affected by peri-implantitis or had lost implants due to peri-implantitis (Table 2). On the other hand, when the threshold for the definition of peri-implantitis Level 2 was set at PPD 6 mm and BOP positive (Mombelli & Lang 1994), the incidence of peri-im- Table 1. Distribution of implants installed according to design, location and length [Numbers and proportions (%)] Implant length 6 mm 6 (3.7%) 8 mm 58 (36%) 10 mm 74 (46%) 12 mm 23 (14.3%) Location Anterior 35 (21.7%) Premolar 74 (46.0%) Molar 52 (32.3%) Implant design Hollow screw 25 (15.2%) Solid screw 115 (69.6%) Hollow cylinders 25 (15.2%) 890 Clin. Oral Impl. Res. 23, 2012 / John Wiley & Sons A/S
4 Table 2. Cumulative survival rate for solid screw and hollow cylinder/screw implants Solid screw implants Hollow cylinder/screw implants Time (years) Number of implants Implants lost Survivor function 95% CI Number of implants Implants lost Survivor function % CI plantitis or implants lost due to peri-implantitis over a mean observation period of 8 years was reduced to 8.8% on an implant level and to 17.1% on a patient level. Radiographic examination Linear measurements to evaluate the marginal bone levels were performed on digitized images and could be made for 152 of the 171 implants. With the help of a cursor, the marginal bone level [the distance from IS to the first bone-to-implant contact (BIC)] was measured. Performing a frequency analysis, 78.3% of the implants showed stable bone levels between 0 and 3 mm (2.8 mm polished neck included) from the IS, 17.1% of the implants had marginal bone levels 0 1 mm below the expected marginal bone level for tissue level Straumann implants with a 2.8 mm machined neck, and 4.6% of the implants demonstrated significant ( 2 mm) bone loss. Periodontal conditions of peri-implantitis Level 1 group The patients were divided into two groups (Table 3). A group of 43 patients with implants not affected by peri-implantitis (non-pip) and a group of 27 patients with one or more implants lost or affected by peri-implantitis (PIP) Level 1 according to the definition of PPD 5 mm and BOP positive. At end of active treatment (T1), the non- PIP group had a mean PPD of 2.44 mm, a mean CAL of 3.65 mm and 16.1% of the sites with BOP compared with a PPD of 2.57 mm, a CAL of 3.64 mm and 20.4% BOP for the PIP Level 1 group. This difference in mean PPD, mean CAL and BOP did not reach statistical significance (P = 0.127, P = and P = 0.182). However, evaluating the number of residual pockets ( 5 mm), at the end of active treatment (T1), the non- PIP group had significantly (P = 0.022) fewer residual pockets per patient than did the PIP group Level 1, 1.9 residual pockets per patient (1.5% of sites) vs. 4.1 residual pockets per patient (3.1% of sites). At the re-evaluation (T2), the PIP group Level 1 had significantly higher mean PPD (P < ). Furthermore, the BOP in the residual dentition was significantly (P = 0.006) higher in the PIP group (25.9%) compared with the non-pip group (17.6%). For the non-pip group, the number of residual pockets was similar at follow-up time (T2) to that at end of active therapy (T1) (1.9 pockets or 1.5% of sites). On the other hand, in the PIP group Level 1, the number of residual pockets had increased significantly from T1 to T2 (6.4 pockets or 5.4% of sites). The difference in number of residual pockets at T2 between the non-pip and the PIP group was highly significant (P < ). Periodontal conditions of peri-implantitis Level 2 group For this analysis the patients were also divided into two groups (Table 3). The PIP Level 2 group consisted of 12 patients with one or more implants lost due to or affected by peri-implantitis according to the definition of PPD 6 mm and BOP positive and a group of 58 patients with no implants affected by peri-implantitis (non-pip). At end of active treatment (T1), the non- PIP group had a mean PPD of 2.48 mm, a mean CAL of 3.60 mm and 18.7% of the sites with BOP compared with a PPD of 2.52 mm, a CAL of 3.87 mm, and 13.7% BOP for the PIP Level 2 group. This difference in mean PPD, mean CAL and BOP did not reach statistical significance (P = 0.740, P = and P = 0.233). At the end of active treatment, the non-pip group had an average of 2.6 residual pockets ( 5 mm), compared with 3.4 residual pockets in the PIP group. This difference, however, did not reach statistical significance (P = 0.514). At the re-evaluation (T2), the PIP group Level 2 had significantly higher mean PPD (P = 0.001) and mean CAL (P = 0.023). The BOP in the residual dentition was higher in the PIP group (25.8%) compared with the Table 3. Clinical parameters at the end of active therapy (T1) and at the follow-up (T2) (average 7.9 years) for the patient groups with peri-implantitis (PIP) (Level 1: PPD 5 mm), the patient group with peri-implantitis (PIP)(Level 2: PPD 6 mm) and the healthy (non-peri-implantitis) patient groups (HP). BOP, Individual mean Bleeding on Probing percentage; PPD, Residual PPD after active therapy either 5 mm or 6 mm; Mean PPD, Mean probing depth of the dentition Peri-implantitis Level 1 (PPD 5 mm, BOP+) Peri-implantitis Level 2 (PPD 6 mm, BOP+) Non-peri-implantitis T1 T2 T1 T2 T1 T2 n = 27 n = 12 n = 43 n = 58 P-values BOP % 20.4% 25.9% 13.7% 25.8% 16.1% 18.7% 17.6% 19.7% P = 0.182, P = 0.233, PPD 5 mm 4.1 (3.1%) 6.4 (5.4%) 3.4 (2.5%) 8.2 (7.1%) 1.9 (1.5%) 2.6 (2.0%) 1.9 (1.5%) 2.7 (2.2%) P = 0.022, P = 0.583, Mean PPD (mm) P = 0.127, P = 0.740, Mean CAL (mm) P = 0.967, P = 0.344, John Wiley & Sons A/S 891 Clin. Oral Impl. Res. 23, 2012 /
5 non-pip group (19.7%). This difference did not reach statistical significance (P = 0.126). For the non-pip group, the number of residual pockets (2.7) was similar at follow-up time (T2) to that at end of active therapy (T1). On the other hand, in the PIP group Level 2, the number (6.2 pockets or 7.1% of sites) of residual pockets had increased significantly from T1 to T2. The difference in number and percent of residual pockets at T2 between the non-pip and the PIP group was highly significant (P = ). Supportive periodontal therapy (SPT) The prevalence of peri-implantitis was evaluated for the group of 47 patients that attended the SPT program at the University of Berne and by the group of twenty-three patients that were referred back to the referring private practitioners for maintenance care. In the former group that was included in a well-organized and regularly performed SPT at the University, 31.9% of the patients had one or more implants affected by peri-implantitis Level 1 or lost due to peri-implantitis compared with 52.2% of the patients that were referred back to the referring practitioners for SPT. When, analyzed for peri-implantitis Level 2 or implants lost due to periimplantitis, the prevalence was reduced to 14.9% for the University patients and 21.7% for the patients that had SPT in a private practice. For both peri-implantitis Levels 1 and 2, this difference did not reach statistical significance (P = and P = 0.475). When the same analysis was done on an implant level, 17.6% of the implants inserted in patients that had the SPT at the University and 30.2% of the implants inserted in patients that had the SPT in a private practice were affected by peri-implantitis Level 1 or had been lost due to peri-implantitis. Moreover, the incidence of implants affected by peri-implantitis Level 2 or lost due to peri-implantitis was 8.3% for the University patients and 9.5% for the patients that had the SPT in a private practice. This difference did not reach statistical significance for periimplantitis Level 1 (P = 0.057) and periimplantitis Level 2 (P = 0.791). Discussion This retrospective analysis of patients susceptible to and comprehensively treated for periodontitis and subsequently receiving implant therapy has demonstrated that those patients experiencing recurrent periodontitis yielded a significantly greater risk for the development of peri-implantitis than did the control group with a stable periodontal situation during maintenance. In this regard, the study is in agreement with results of previous reports of patient cohorts susceptible or not susceptible to periodontitis (Ellegaard et al.1997; Hardt et al. 2001; Karoussis et al. 2003). The prospective cohort previously presented (Karoussis et al.2003) encompassed 53 patients with 112 hollow screw implants. Among these were eight patients susceptible to periodontitis and 45 patients without a history of periodontitis with 21 and 91 implants, respectively. Although the survival rate after 10 years was 90.5% for the susceptible group, it was 96.5% for the non-susceptible group. This difference over 10 years in incidence of implant loss did not reach statistical significance owing to the fact that the difference was made up by only one implant out of a total loss of five. Over the years, implant systems, implant designs, and implant surfaces have not been considered a major factor regarding the longevity of implants inserted in patients susceptible to periodontitis (Matarasso et al. 2010). In the present retrospective analysis, two types of implants were utilized. Surprisingly, the survival rate of solid screw implants (99.1%) was significantly higher than the survival of hollow screw and hollow cylinder implants (89.7%). One of the explanations for this difference could be that the mean follow-up for the hollow implants was longer than that for the solid screw implants, 11.1 vs. 6.4 years, respectively. Nevertheless, the survival for the hollow TPS implants was already below 90% after 6 years. Another explanation could be that the implant surface and geometry also influenced the success of the implant treatment in periodontally susceptible patients. That would be in agreement with an experimental study in dogs (Albouy et al. 2008) that analyzed the tissue reaction to a ligature induced experimental peri-implantitis around commercially available dental implants. After 12 weeks of active breakdown, when 40 50% of the supporting bone was lost, the ligatures were removed and plaque was allowed to accumulate for additional 24 weeks. The authors concluded that the implant surface was a significant factor influencing the amount of tissue breakdown occurring during the experimentally ligature-induced peri-implantitis. In the present study, cohorts were defined on the basis of the prevalence of peri-implantitis. Two thresholds (Level 1 & 2) for this definition were applied choosing either 5 mm PPD (Level 1) or 6 mm PPD (Level 2) concomitant with a positive BOP score. In addition, the patients with implants lost as a result of infection (n = 6) were also included in the cohort affected by periimplantitis (PIP group). Consequently, the incidence over 8 years was 38.6% or 27 patients for peri-implantitis Level 1. If the peri-implantitis threshold of PPD 6mm (Level 2) was applied together with positive BOP scores and including the implant losses, the 8-year incidence was reduced to 17.1% of the patients. In comparison, a study of a patient cohort treated with another implant system than the one assessed in the present study, revealed a peri-implantitis prevalence of 28% of the patients with progressive bone loss after 5 20 years (mean: 9.1 years) (Fransson et al. 2005). On the implant level, however, 12.4% of the implants displayed progressive bone loss. In the present study, 8.8% of implants were lost due to bone loss or demonstrated significant ( 2 mm) bone loss. In another retrospective study over 9 14 years (Roos-Jansåker et al. 2006), the prevalence of peri-implantitis on the patient level was 16%, whereas 6.6% of the implants yielded peri-implantitis. In agreement with these studies, the results of the present analysis demonstrated that the prevalence on the patient level was substantially higher than that on the implant level irrespective of the threshold of probing depth chosen for the definition of peri-implantitis. Although all patients of the present study were successfully treated for existing periodontitis and hence, were susceptible to periodontitis, they displayed various numbers of residual pockets defined as PPD 5mmat the termination of active therapy (T1). This, in turn, means that some patients were treated more successfully than others. Of the patients, later belonging to the PIP group, the mean PPD and BOP were similar to the values assessed for the non-pip group at the end of active treatment. At the time of re-assessment, approximately 8 years later, these values were significantly different. The mean BOP percentage at T2 was 25.9% for the PIP Level 1 group vs. 17.6% for the non-pip group. On the other hand, at the end of active treatment, the PIP Level 1 group averaged 4.1 residual pockets compared to 1.9 such pockets in the non-pip group. This points to the importance of clinical parameters of inflammation and residual periodontal niches as a reservoir for bacterial spread throughout the dentition including the newly 892 Clin. Oral Impl. Res. 23, 2012 / John Wiley & Sons A/S
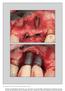
6 placed implants (Mombelli et al. 1995). The differences in residual pockets and BOP were important risk indicators at T2. Moreover, there was a significant contribution of the number of residual pockets at T1 to the prediction of future peri-implant infections. Thus, it appears reasonable to treat periodontitis to a level of absence of or minimal inflammation as well as to an absence of residual pockets following active therapy to reduce a possible influence of ecological niches on the integrity of implants and their stability. In the present study, 17.1% of the implants were affected by peri-implantitis Level 1 during the course of 8 years. Moreover, 4.2% of the implants were lost as a result of periimplant infection. Not considering the early losses (n = 2) during the first year, a loss of 3% within the subsequent 7 years represents a very low prevalence compared with systematic reviews on implant failures (Berglundh et al. 2002; Pjetursson et al. 2004). Furthermore, if the TPS hollow cylinder and hollow screw implants are excluded from the analysis, a survival rate of 99.1% for the solid screw implants must be considered very high, especially in a cohort consisting solely of periodontally susceptible patients. It is obvious that with 17.1% of the implants being affected by peri-implantitis revealed by this retrospective analysis, there is a substantial need for diagnosis and treatment of periimplant diseases. In this respect, the Level 2 definition with 6 mm PPD and BOP positive may serve as a standard for intervention. This assumption is substantiated by the fact that radiographic bone loss exceeding the remodeling process was recognized in 21.7% of implants. Since only 4.6% of the implants yielded substantial bone loss, it may be speculated that 1 in 20 implants requires advanced rescue measures to treat a peri-implantitis lesion over a period of 8 years (Fig.1). The implant longevity may significantly depend on the mode and frequency of SPT organized for patients susceptible to periodontitis rather than the implant systems applied (Matarasso et al. 2010). In this study comparing two implant systems in groups of patients with a history of periodontitis or Fig 1. Cumulative survival rate for solid screw and hollow cylinder/screw implants. periodontally healthy conditions, statistically significantly higher mean bone loss and numbers of sites with bone loss 3 mm were identified in patients with a history of periodontitis (Matarasso et al. 2010). Recently, 112 partially edentulous patients were assessed 10 years after implant installation with regard to adhesion to SPT (Roccuzzo et al. 2010). Patients were treated for moderate and severe periodontitis (periodontally compromised patients (PCP)) and compared to patients in periodontally healthy conditions (PHP). During the period of observation, 18 implants were removed because of biological complications. The implant survival rate was thus 96.6% for PHP, 92.8% for moderate PCP and 90% for severe PCP implants. A statistically significant difference was found between PHP and severe PCP. Lack of adhesion to SPT was correlated with a higher incidence of bone loss and implant loss. Hence, the authors concluded that patients with a history of periodontitis presented a lower implant survival rate and a statistically significantly higher number of sites with peri-implant bone loss. Moreover, the authors concluded that patients who did not completely adhere to the SPT, presented a higher implant failure rate. Hence, the value of the SPT in enhancing the long-term outcomes of implant therapy was documented, particularly in subjects affected by periodontitis (Roccuzzo et al. 2010). In the present study, differences in the prevalence of peri-implantitis were seen between the patients that had been incorporated into a well-organized SPT program at the University and those who had been referred for maintenance care to their referring private practitioners. However, these differences did not reach statistical significance, most likely owing to the fact that a relatively small number of implants were diagnosed as peri-implantitis Level 2. Yet, the present study also provides additional evidence that supports the importance of well-organized SPT for periodontally susceptible patients that have received dental implants. In conclusion, in periodontitis susceptible patients, residual pockets (PPD 5 mm) at the end of active periodontal therapy represent a significant risk for the development of periimplantitis and implant loss. Moreover, patients in SPT developing re-infections are at greater risk for peri-implantitis and implant loss than periodontally stable patients. Acknowledgements: This study has been supported by the Clinical Research Foundation (CRF) for The Promotion of Oral Health, Brienz, Switzerland. The co-operation of the Dental Assistants and the Dental Hygienists of the former Department of Periodontology & Fixed Prosthodontics of the University of Berne is highly appreciated. Conflict of interest: The authors declare no conflict of interest in relation with the products applied for or any other aspects of this study. References Albouy, J.P., Abrahamsson, I., Persson, L.G. & Berglundh, T. (2008) Spontaneous progression of peri-implantitis at different types of implants. An experimental study in dogs. I: clinical and radiographic observations. Clinical Oral Implants Research 19: Apse, P., Ellen, R.P., Overall, C.M. & Zarb, G.A. (1989) Microbiota and crevicular fluid collagenase activity in the osseointegrated dental implant sulcus: a comparison of sites in edentulous and partially edentulous patients. Journal of Periodontal Research 24: Berglundh, T., Persson, L. & Klinge, B. (2002) A systematic review of the incidence of biological and technical complications in implant dentistry reported in prospective longitudinal studies of at least 5 years. Journal of Clinical Periodontology 29(Suppl. 3): John Wiley & Sons A/S 893 Clin. Oral Impl. Res. 23, 2012 /
7 Brägger, U. (1996) Radiographic diagnosis of periodontal disease progression. Current Opinions in Periodontology 3: Brägger, U., Bürgin, W., Hämmerle, C.H.F. & Lang, N.P. (1997) Associations between clinical parameters assessed around implants and teeth. Clinical Oral Implants Research 8: Brägger, U., Hämmerle, C.H.F. & Weber, H.P. (1990) Fixed reconstructions in partially edentulous patients using two part ITI implants (Bonefit ) as abutments. Clinical Oral Implants Research 1: Buser, D., Chen, S.T., Weber, H.P. & Belser, U.C. (2008) Early implant placement following singletooth extraction in the esthetic zone: biologic rationale and surgical procedures. International Journal of Periodontics & Restorative Dentistry 28: Ellegaard, B., Baelum, B. & Karring, T. (1997) Implant in periodontally compromised patients. Clinical Oral Implant Research 8: Fransson, C., Lekholm, U., Jemt, T. & Berglundh, T. (2005) Prevalence of subjects with progressive bone loss at implants. Clinical Oral Implants Research 16: Fürst, M.M., Salvi, G.E., Lang, N.P. & Persson, G. R. (2007) Bacterial colonization immediately after installation on oral titanium implants. Clinical Oral Implants Research 18: Hamp, S-E., Nyman, S. & Lindhe, J. (1975) Periodontal treatment of multirooted teeth. Results after 5 years. Journal of Clinical Periodontology 2: Hardt, C.R.R., Gröndahl, K., Lekholm, U. & Wennström, J.L. (2001) Outcome of implant therapy in relation to experienced loss of periodontal bone support. Clinical Oral Implants Research 13: Heitz-Mayfield, L.J. & Lang, N.P. (2010) Comparative biology of chronic and aggressive periodontitis vs. peri-implantitis. Periodontology 2000: Holm-Pedersen, P., Lang, N.P. & Müller, F. (2007) What are the longevities of teeth and oral implants? Clinical Oral Implants Research 18 (Suppl. 3): Jung, R.E., Pjetursson, B.E., Glauser, R., Zembic, A., Zwahlen, M. & Lang, N.P. (2008) A systematic review of the 5-year survival and complication rates of implant-supported single crowns. Clinical Oral Implants Research 19: Kalykakis, G., Zafiropoulos, G.G., Murat, Y., Spiekermann, H. & Nisengard, R.J. (1994) Clinical and microbiological status of osseointegrated implants. Journal of Periodontology 65: Kaplan, E.L. & Meier, P. (1958) Nonparametric estimation from incomplete observations. Journal of the American Statistical Association 53: Karoussis, I.K., Müller, S., Salvi, G.E., Heitz-Mayfield, L.J.A., Brägger, U. & Lang, N.P. (2004) Association between periopdontal and peri-implant conditions: a 10- year prospective study. Clinical Oral Implants Research 15: 1 7. Karoussis, I.K., Salvi, G.E., Heitz-Mayfield, L.J.A., Brägger, U., Hämmerle, C.H.F. & Lang, N.P. (2003) Long-term implant prognosos in patients with and without a history of chronic periodontitis: a 10-year prospective cohort study of the ITI Dental Implant System. Clinical Oral Implants Research 14: Kohavi, D. (1993) Complications in the tissue integrated prostheses components: clinical and mechanical evaluation. Journal of Oral Rehabilitation 20: Koka, S., Razzoog, M.E., Bloem, T.J. & Syed, S.A. (1993) Microbial colonization of dental implants in partially edentulous subjects. Journal of Prosthetic Dentistry 70: Lang, N.P., Wilson, T.G. & Corbet, E.F. (2000) Biological complications with dental implants: their prevention, diagnosis and treatment. Clinical Oral Implants Research 11(Suppl. 1): Lee, K.H., Maiden, M.F.J., Tanner, A.C.R. & Weber, H.P. (1999) Microbiota of successful osseointegrated dental implants. Journal of Periodontology 70: Leonhardt, A., Adolfsson, B., Lekholm, U., Wikström, M. & Dahlén, G. (1993) A longitudinal microbiological study on osseointegrated titanium implants in partially edentulous patients. Clinical Oral Implants Research 4: Leonhardt, A., Berglundh, T., Ericsson, I. & Dahlén, G. (1992) Putative periodontal pathogens on titanium implants and teeth in experimental gingivitis and periodontitis in beagle dogs. Clinical Oral Implants Research 3: Matarasso, S., Rasperini, G., Iorio Siciliano, V., Salvi, G.E., Lang, N.P. & Aglietta, M. (2010) A 10- year retrospective analysis of radiographic bonelevel changes of implants supporting single-unit crowns in periodontally compromised vs. periodontally healthy patients. Clinical Oral Implants Research 21: Mombelli, A. & Lang, N.P. (1994) Clinical parameters for the evaluation of dental implants. Periodontology : Mombelli, A., Marxer, M., Gaberthüel, T., Grunder, U. & Lang, N.P. (1995) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiology and Immunology 2: Mombelli, A., van Oosten, M.A., Schürch, E. Jr & Lang, N.P. (1987) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiology and Immunology 2: Nevins, M. (2001) Will implants survive well in patients with a history of inflammatory periodontal disease? Journal of Periodontology 72: Nevins, M. & Langer, B. (1995) The successful use of osseointegrated implants for the treatment of the recalcitrant periodontal patient. Journal of Periodontology 66: Ong, C.T., Ivanovski, S., Needleman, I.G., Retzepi, M., Moles, D.R., Tonetti, M.S. & Donos, N. (2008) Systematic review of implant outcomes in treated periodontitis subjects. Journal of Clinical Periodontology 35: Pjetursson, B.E., Tan, K., Lang, N.P., Brägger, U., Egger, M. & Zwahlen, M. (2004) A systematic review of the survival and complication rates of fixed partial dentures (FPDs) after an observation period of at least 5 years. Clinical Oral Implants Research 15: Preist, G. (1999) Single tooth implants and their role in preserving remaining teeth: a 10-year survival study. International Journal of Oral & Maxillofacial Implants 14: Quirynen, M. & Listgarten, M.A. (1990) Distribution of bacterial morphotypes around natural teeth and titanium implants ad modum Brånemark. Clinical Oral Implants Research 1: Ramfjord, S.P. (1967) The periodontal disease index (PDI). Journal of Periodontology 38(Suppl.): Roccuzzo, M., DeAngelis, N., Bonino, L. & Aglietta, M. (2010) Ten-year results of a three-arm prospective cohort study on implants in periodontally compromised patients. Part 1: implant loss and radiographic bone loss. Clinical Oral Implants Research 21: Roos-Jansåker, A.M., Lindahl, C., Renvert, H. & Renvert, S. (2006) Nine- to fourteen-year followup of implant treatment. Part II: presence of periimplant lesions. Journal of Clinical Periodontology 33: Salvi, G.E., Fürst, M.M., Lang, N.P. & Persson, G. R. (2008) One-year bacterial colonization patterns of Staphylococcus aureus and other bacteria at implants and adjacent teeth. Clinical Oral Implants Research 19: Sbordone, L., Barone, A., Ciaglia, R.N., Ramaglina, L. & Iacono, V.J. (1999) Longitudinal study of dental implants in a periodontally compromised population. Journal of Periodontology 70: Tonetti, M.S. & Claffey, N. (2005) Advances in the progression of periodontitis and proposal of definitions of a periodontitis case and disease progression for use in risk factor research. Group C consensus report of the 5th European workshop in periodontology. Journal of Clinical Periodontology 32(Suppl. 6): Clin. Oral Impl. Res. 23, 2012 / John Wiley & Sons A/S
Outcome of dental implants in patients with a history of periodontitis
 Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta
 Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Factors influencing ridge alterations following immediate implant placement into extraction sockets
 Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Jorge Ferrus Denis Cecchinato E. Bjarni Pjetursson Niklaus P. Lang Mariano Sanz Jan Lindhe Factors influencing ridge alterations following immediate implant placement into extraction sockets Authors affiliations:
Interrelationship between Periodontitis and Peri-Implantitis: Myth or Reality?
 REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up
 Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years
 REVIEW S155 Lars Hjalmarsson, Maryam Gheisarifar, Torsten Jemt A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years Key words 10-year
REVIEW S155 Lars Hjalmarsson, Maryam Gheisarifar, Torsten Jemt A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years Key words 10-year
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
A systematic review of the 5-year survival and complication rates of implant-supported single crowns
 Ronald E. Jung Bjarni E. Pjetursson Roland Glauser Anja Zembic Marcel Zwahlen Niklaus P. Lang A systematic review of the 5-year survival and complication rates of implant-supported single crowns Authors
Ronald E. Jung Bjarni E. Pjetursson Roland Glauser Anja Zembic Marcel Zwahlen Niklaus P. Lang A systematic review of the 5-year survival and complication rates of implant-supported single crowns Authors
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
Proposed score for occlusal-supporting ability
 Open Journal of Stomatology, 2013, 3, 230-234 http://dx.doi.org/10.4236/ojst.2013.33040 Published Online June 2013 (http://www.scirp.org/journal/ojst/) OJST Proposed score for occlusal-supporting ability
Open Journal of Stomatology, 2013, 3, 230-234 http://dx.doi.org/10.4236/ojst.2013.33040 Published Online June 2013 (http://www.scirp.org/journal/ojst/) OJST Proposed score for occlusal-supporting ability
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
More than a beautiful smile. A new quality of life with dental implants.
 More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
More than a beautiful smile. A new quality of life with dental implants. Why tooth loss matters Think of tooth loss and the first thing that comes to mind may be an unattractive appearance. It s true that
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets
 Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
Luca Cordaro Ferruccio Torsello Mario Roccuzzo Clinical outcome of submerged vs. non-submerged implants placed in fresh extraction sockets Author s affiliations: Luca Cordaro, Ferruccio Torsello, Eastman
Complex Rehabilitation of Advanced Periodontitis Subject with a Staged Approach; Implant Supported Fixed Detachable Prosthesis
 International Journal of Dental Sciences and Research, 2016, Vol. 4, No. 1, 5-9 Available online at http://pubs.sciepub.com/ijdsr/4/1/2 Science and Education Publishing DOI:10.12691/ijdsr-4-1-2 Complex
International Journal of Dental Sciences and Research, 2016, Vol. 4, No. 1, 5-9 Available online at http://pubs.sciepub.com/ijdsr/4/1/2 Science and Education Publishing DOI:10.12691/ijdsr-4-1-2 Complex
Creating emergence profiles in immediate implant dentistry
 Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
Creating emergence profiles in immediate implant dentistry AUTHORS Dr. Daniel Capitán Maraver Dr. Manuel Fuentes Ortiz Visiting lecturers in the Master s Degree in Clinical Practice in Implantology and
01/05/2014. Background. Minimally invasive tooth extraction. Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry
 Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Background Remodelling of alveolar bone following extraction Minimally invasive tooth extraction Thomas Dietrich Professor of Oral Surgery University of Birmingham, School of Dentistry 2 weeks 4 weeks
Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
 J Clin Periodontol 2007; 34: 805 815 doi: 10.1111/j.1600-051X.2007.01106.x Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
J Clin Periodontol 2007; 34: 805 815 doi: 10.1111/j.1600-051X.2007.01106.x Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
 Wittneben JG, Kern M: Imitation der Rot-Weiß-Ästhetik im Frontzahnbereich Literatur: 1 Buser D, Sennerby L, De Bryn H: Modern implant dentistry based on osseointegration: 50 years of progress, current
Wittneben JG, Kern M: Imitation der Rot-Weiß-Ästhetik im Frontzahnbereich Literatur: 1 Buser D, Sennerby L, De Bryn H: Modern implant dentistry based on osseointegration: 50 years of progress, current
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
Over the last decades, the use
 LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
GuidedService. The ultimate guide for precise implantations
 GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
GuidedService The ultimate guide for precise implantations ABGuidedService The ultimate guide for precise implantations At A.B. Dental we've brought implantology into the future with a 3D digitally planned
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Why implants need even better care than natural teeth.
 Why implants need even better care than natural teeth. ± How to increase the lifespan of your implant. BETTER ORAL HEALTH FOR ALL Expert advisory board Hugo Roberto Lewgoy, DDS, MSc, PhD., Department of
Why implants need even better care than natural teeth. ± How to increase the lifespan of your implant. BETTER ORAL HEALTH FOR ALL Expert advisory board Hugo Roberto Lewgoy, DDS, MSc, PhD., Department of
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant placement
 Guy Huynh-Ba Bjarni E. Pjetursson Mariano Sanz Denis Cecchinato Jorge Ferrus Jan Lindhe Niklaus P. Lang Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant
Guy Huynh-Ba Bjarni E. Pjetursson Mariano Sanz Denis Cecchinato Jorge Ferrus Jan Lindhe Niklaus P. Lang Analysis of the socket bone wall dimensions in the upper maxilla in relation to immediate implant
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident
 Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Case Report 13 2011 Oral Rehabilitation with CAMLOG implants after loss of dentition due to an accident Dr Hitoshi Minagawa Tokyo, Japan Prosthetics Dr Hitoshi Minagawa successfully completed his studies
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
Microbiota Around Root-Form Endosseous Implants: A Review of the Literature
 Microbiota Around Root-Form Endosseous Implants: A Review of the Literature Kees Heydenrijk, DDS, PhD 1 /Henny J. A. Meijer, DDS, PhD 2 /Wil A. van der Reijden, PhD 1 / Gerry M. Raghoebar, MD, DDS, PhD
Microbiota Around Root-Form Endosseous Implants: A Review of the Literature Kees Heydenrijk, DDS, PhD 1 /Henny J. A. Meijer, DDS, PhD 2 /Wil A. van der Reijden, PhD 1 / Gerry M. Raghoebar, MD, DDS, PhD
Implants- immediate restoration of postextraction edentation both esthetically and functionally
 Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Implants- immediate restoration of postextraction edentation both esthetically and functionally Otilia Stana (Gag), LileIoana Elena, Freiman Paul, Mugur Popescu, Elisei Gabriela, Sebesan Voicu, Vincze
Detection of predominant subgingival periopathogens around submerged and non submerged hydroxy apatite implants
 [Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
[Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
The International Journal of Periodontics & Restorative Dentistry
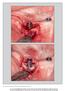 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
photodynamic therapy, surface decontamination
 Dorothee Schär Christoph A. Ramseier Sigrun Eick Nicole B. Arweiler Anton Sculean Giovanni E. Salvi Anti-infective therapy of peri-implantitis with adjunctive local drug delivery or photodynamic therapy:
Dorothee Schär Christoph A. Ramseier Sigrun Eick Nicole B. Arweiler Anton Sculean Giovanni E. Salvi Anti-infective therapy of peri-implantitis with adjunctive local drug delivery or photodynamic therapy:
ASSESSMENT OF THE PROGNOSIS OF PRESERVATION OR EXTRACTION OF PERIODONTOPATHIC TEETH FOR IMPLANT DECISIONS
 Parodontology ASSESSMENT OF THE PROGNOSIS OF PRESERVATION OR EXTRACTION OF PERIODONTOPATHIC TEETH FOR IMPLANT DECISIONS Atamna Hussein Magde 1, Mâr]u Silvia 2 1. PhD Student, Gr.T.Popa U.M.Ph Iasi, Romania,
Parodontology ASSESSMENT OF THE PROGNOSIS OF PRESERVATION OR EXTRACTION OF PERIODONTOPATHIC TEETH FOR IMPLANT DECISIONS Atamna Hussein Magde 1, Mâr]u Silvia 2 1. PhD Student, Gr.T.Popa U.M.Ph Iasi, Romania,
The restoration of partially and completely
 CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
CLINICAL MANAGEMENT OF DENTAL IMPLANT FRACTURES. ACASE HISTORY Firas A. M. AL Quran, PhD, MSc Med; Bashar A. Rashan, MS; Ziad N. AL-Dwairi, PhD The widespread use of endosseous osseointegrated implants
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
An Introduction to Dental Implants
 An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
An Introduction to Dental Implants Aims: This article provides an introduction to dental implants, outlining the categories of dental implants, the phases involved in implant dentistry and assessing a
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients
 Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
Nima Bazrafshan Ivan Darby Retrospective success and survival rates of dental implants placed with simultaneous bone augmentation in partially edentulous patients Authors affiliations: Nima Bazrafshan,
Clinical Research by the UofT Prosthodontics Graduate Residents of Importance for the Practicing Dentist
 Toronto Academy of Dentistry Winter Clinic. Nov 4, 2011 Clinical Research by the UofT Prosthodontics Graduate Residents of Importance for the Practicing Dentist ASBJORN JOKSTAD, DDS, PhD Prosthodontics,
Toronto Academy of Dentistry Winter Clinic. Nov 4, 2011 Clinical Research by the UofT Prosthodontics Graduate Residents of Importance for the Practicing Dentist ASBJORN JOKSTAD, DDS, PhD Prosthodontics,
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature
 The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
Improvement of Systemic Symptoms after Dental Implant Removal
 Open Journal of Stomatology, 2016, 6, 37-46 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2016.62005 Improvement of Systemic Symptoms after
Open Journal of Stomatology, 2016, 6, 37-46 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojst http://dx.doi.org/10.4236/ojst.2016.62005 Improvement of Systemic Symptoms after
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
Conclusions: I-I FPDs had statistically significant fewer biological complications compared to with the I-T FPDs. I-T FPDs had statistically more
 Bragger U, Karoussis, J, Persson R, et al. Technical and biological complications/failures with single crowns and fixed partial dentures on implants: a 10-year prospective cohort study. Clin. Oral Impl.
Bragger U, Karoussis, J, Persson R, et al. Technical and biological complications/failures with single crowns and fixed partial dentures on implants: a 10-year prospective cohort study. Clin. Oral Impl.
ITI. Treatment Guide. Editors: D. Wismeijer, D. Buser, U. Belser. Not for Publication
 ITI Editors: D. Wismeijer, D. Buser, U. Belser Treatment Guide Authors: D. Morton, J. Ganeles Volume 2 Loading Protocols in Implant Dentistry Partially Dentate Patients Publishing Co, Ltd Berlin, Chicago,
ITI Editors: D. Wismeijer, D. Buser, U. Belser Treatment Guide Authors: D. Morton, J. Ganeles Volume 2 Loading Protocols in Implant Dentistry Partially Dentate Patients Publishing Co, Ltd Berlin, Chicago,
Arbeit unter der Leitung von Dr. med. Dr. med. dent. D. Schneider
 Universität Zürich Zentrum für Zahn-, Mund- und Kieferheilkunde Vorsteher: Prof. Dr. med. dent. C. Hämmerle Klinik für Kronen- und Brückenprothetik, Teilprothetik und Zahnärztliche Materialkunde Direktor:
Universität Zürich Zentrum für Zahn-, Mund- und Kieferheilkunde Vorsteher: Prof. Dr. med. dent. C. Hämmerle Klinik für Kronen- und Brückenprothetik, Teilprothetik und Zahnärztliche Materialkunde Direktor:
Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
 Case Reports in Dentistry Volume 2015, Article ID 217895, 10 pages http://dx.doi.org/10.1155/2015/217895 Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
Case Reports in Dentistry Volume 2015, Article ID 217895, 10 pages http://dx.doi.org/10.1155/2015/217895 Case Report Immediate, Early, and Conventional Implant Placement in a Patient with History of Periodontitis
Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function
 Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
Jung-Joo Kim n Dong-Won Lee n Chong-Kwan Kim Kwang-Ho Park Ik-Sang Moon Effect of conical configuration of fixture on the maintenance of marginal bone level: preliminary results at 1 year of function Authors
Introduction. Clinical Periodontal Examination 11/1/16
 Is Radiologic Assessment of Alveolar Crest Height Useful to Monitor Periodontal Disease Activity? Based on DCNA chapter: Hattan A.M. Zaki, Kenneth R. Hoffmann, Ernest Hausmann, Frank A. Scannapieco Periodontitis,
Is Radiologic Assessment of Alveolar Crest Height Useful to Monitor Periodontal Disease Activity? Based on DCNA chapter: Hattan A.M. Zaki, Kenneth R. Hoffmann, Ernest Hausmann, Frank A. Scannapieco Periodontitis,
Peri-implantitis. Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
 Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results
 Rafael Juan Blanes Jean Pierre Bernard Zulema Maria Blanes Urs Christoph Belser A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results Authors
Rafael Juan Blanes Jean Pierre Bernard Zulema Maria Blanes Urs Christoph Belser A 10-year prospective study of ITI dental implants placed in the posterior region I: Clinical and radiographic results Authors
The Endodontic / Implant Controversy
 The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
The Endodontic / Implant Controversy Innovations in Endodontics Series Robert Handysides DDS Associate Professor and Chair Department of Endodontics Loma Linda University School of Dentistry Endodontic
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
The International Journal of Periodontics & Restorative Dentistry
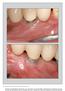 The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
2017 WORLD WORKSHOP. Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March DOI: /jcpe.12957
 Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
In recent decades, the clinical replacement of natural
 Effect of Intracrevicular Restoration Margins on Peri-implant Health: Clinical, Biochemical, and Microbiologic Findings Around Esthetic Implants up to 9 Years Catherine Giannopoulou, Dr Med Dent 1 /Jean-Pierre
Effect of Intracrevicular Restoration Margins on Peri-implant Health: Clinical, Biochemical, and Microbiologic Findings Around Esthetic Implants up to 9 Years Catherine Giannopoulou, Dr Med Dent 1 /Jean-Pierre
