Microbiota Around Root-Form Endosseous Implants: A Review of the Literature
|
|
|
- Moses Edwards
- 5 years ago
- Views:
Transcription
1 Microbiota Around Root-Form Endosseous Implants: A Review of the Literature Kees Heydenrijk, DDS, PhD 1 /Henny J. A. Meijer, DDS, PhD 2 /Wil A. van der Reijden, PhD 1 / Gerry M. Raghoebar, MD, DDS, PhD 2 /Arjan Vissink, MD, DDS, PhD 2 /Boudewijn Stegenga, DDS, PhD 2 Although high success rates for root-form endosseous implants have been reported, failures occasionally occur, and these implants must be removed. At least 10% of the failures have been suggested to be the result of peri-implantitis. There is some evidence that periodontal pathogens, mainly those belonging to the group of Gram-negative anaerobic rods, play a role in the etiology of peri-implantitis. This article provides an overview of the literature associated with common peri-implant microbiology and an assessment as to whether bacteria associated with periodontitis exert a possible risk for periimplant tissue breakdown. The peri-implant area is colonized by a large variety of oral microbial complexes. The microflora of the oral cavity prior to implant placement determines the composition of the microflora in the peri-implant area. Implants involved in peri-implantitis are colonized with large amounts of Gram-negative anaerobic bacteria, including Fusobacteria, spirochetes, Bacteroides forsythus, and black-pigmented bacteria such as Prevotella intermedia, Prevotella nigrescens, and Porphyromonas gingivalis. Also, Actinobacillus actinomycetemcomitans can be isolated from these lesions. Thus, the microflora of peri-implantitis lesions resembles that of adult or refractory periodontitis. However, the presence of periodontal pathogens does not always lead to a destructive process. Therefore, the etiologic role of specific microorganisms in implant failure related to infection is still not resolved. Controversy remains as to whether organisms recovered from the original microflora cause the failure (and if so to what extent) or merely result from the infection. Nevertheless, there is accumulating evidence that bacteria cause the disease, while the individual s genetic makeup and environmental influences determine the severity of the disease. (INT J ORAL MAXILLOFAC IMPLANTS 2002;17: ) Key words: dental implants, microbiology, peri-implantitis, periodontology Root-form endosseous implants are commonly used for the fixation of prosthetic restorations. Brånemark and coworkers 1 were the first to describe the anchorage of dental prostheses by osseointegrated dental implants. Over the years, 1 Assistant Professor, Department of Oral and Maxillofacial Surgery and Maxillofacial Prosthetics, University Hospital Groningen, The Netherlands. 2 Associate Professor, Department of Oral Biology, Section of Clinical Periodontal Microbiology, Academic Center for Dentistry Amsterdam, The Netherlands. Reprint requests: Dr Kees Heydenrijk, University Hospital Groningen, Department of Oral and Maxillofacial Surgery and Maxillofacial Prosthetics, P. O. Box 30001, 9700 RB Groningen, The Netherlands. Fax: k.heydenrijk@kchir.azg.nl many different implant systems have been introduced, and the indications for their application have gradually been extended. Although high success rates have consistently been reported for many implant systems, 2 failures leading to implant removal still occur. The overall failure rate for Brånemark System implants (Nobel Biocare, Göteborg, Sweden) is 7.7% over a 5-year period. 3 Failure rates in the edentulous maxilla and mandible are 10% and 3%, respectively, while in partially edentulous patients 4% of the implants are lost. 3 Comparable failure rates have been reported for other implant systems. 2 To achieve consensus on terminology, implant failure has been defined as the inadequacy of the host tissue to establish or to maintain osseointegration, 3 and peri-implantitis has been defined as the inflammatory process affecting the tissue around an The International Journal of Oral & Maxillofacial Implants 829
2 osseointegrated implant in function, resulting in loss of supporting bone. 4 Failing implants are characterized by loss of supporting bone and mobility. Patients experience spontaneous pain as well as pain on clenching, percussion, or palpation, and deep pockets may be present. Referring to the occurrence in time, early and late failures can be distinguished. In early failure, osseointegration has never been established, thus representing an interference with the healing process. Early failures occur prior to prosthetic rehabilitation. 3 Surgical trauma, insufficient quantity or quality of the bone surrounding the implant, premature loading of the implant, and bacterial infection have been implicated as causes for early implant failure. 5,6 In late failure, the established osseointegration is not maintained, implying processes involving loss of osseointegration. Late failures occur following prosthetic rehabilitation. 3 Late failures can be divided into 2 subgroups, with one including implants failing during the first year of loading ( soon late failures) and one including implants failing in subsequent years ( delayed late failures). Each makes up about 50% of the late failures. It seems reasonable to attribute most of the soon late failures to overloading in relation to poor bone quality and insufficient bone volume. The delayed late failures probably can be attributed to progressive changes of the loading conditions in relation to bone quality and volume and peri-implantitis. 6,7 There is evidence supporting the view that periodontal pathogens, mainly those belonging to the group of Gram-negative anaerobic rods, play an important role in developing peri-implantitis. In this article, this evidence is reviewed against the background of the current knowledge of the common peri-implant microbiology. This article provides a comprehensive review of studies published in the international peer-reviewed literature published in English concerning the subgingival microflora surrounding root-form endosseous oral implants in humans. Using MED- LINE (US National Library of Medicine), a literature search was performed on articles published between January 1980 through December Key words used in the search were: dental, implants, microorganisms, microbiota, microbiology, microflora, peri-implantitis, failure, periodontology, periodontitis, and genetic. Publications presented in abstract form and animal studies were ignored. All resulting papers were analyzed for their contents and included if appropriate. Because of major differences between study designs and/or methodologic shortcomings, it was not possible to execute a meta-analysis that includes a sufficient number of studies. MICROBIAL COLONIZATION OF THE MOUTH WITHOUT IMPLANTS It has been estimated that about 400 different microbial species are capable of colonizing the dentate oral cavity and that any individual may harbor over 150 different species. 3 Samples from the healthy gingival sulcus contain relatively few (10 3 to 10 6 ) cultivable organisms, predominantly consisting of Gram-positive cocci and rods, principally Actinomyces naeslundii (14%), Actinomyces gerencseriae (11%), Streptococcus oralis (14%), and Peptostreptococcus micros (5%) Gram-negative anaerobic rods account for 13% of the total cultivable organisms on average. Many of the suspected periodontal pathogens belong to this anaerobic group, indicating that colonization with putative periodontal pathogens in healthy subjects without signs of gingival inflammation is possible. 10 Subgingival bacterial counts range up to more than 108 in deep periodontal pockets. There is general agreement that periodontitis is an infectious disease associated with only a few of the bacterial species found in dental plaque. 13 With the development of periodontitis, there is a shift toward a subgingival flora containing a higher proportion of Gram-negative rods and decreased proportions of Gram-positive species. In an established periodontal lesion, low numbers of cocci and high numbers of motile rods and spirochetes are seen. Increased proportions of Porphyromonas gingivalis, Bacteroides forsythus, and species of Prevotella, Fusobacterium, Campylobacter, and Treponema have been detected. 11,12 P gingivalis was isolated in 79% of periodontitis patients. 14 However, it is still unknown whether the presence of the Gram-negative bacteria is secondary to altered nutritional and anaerobic conditions because of the inflammatory processes and pocket formation or is itself responsible for the periodontal destruction. 9 To become associated with destructive periodontitis, the microorganisms must comply with several criteria 8 : The species should be found more frequently and in higher proportions in cases of infection compared to non-diseased sites (association). Absence of the species should be accompanied by a parallel remission of disease (elimination). Production of antibodies or cellular immune response is directed specifically at that species (host response). 830 Volume 17, Number 6, 2002
3 Potentially damaging metabolites are produced or properties possessed by a species (virulence factors). Periodontal disease progression conferred by the presence of a species at a given level is evaluated in a prospective study (risk assessment). On the basis of these criteria, several species have been related to the etiology of destructive periodontal diseases, of which Actinobacillus actinomycetemcomitans and P gingivalis have the strongest association. A actinomycetemcomitans is the most important microorganism in juvenile periodontitis, while P gingivalis is considered to be associated with adult periodontitis and refractory periodontitis. In low numbers, Prevotella intermedia and Prevotella nigrescens have been found in periodontally healthy subjects, but they may also be associated with the development of periodontitis. To affect periodontal tissues, these species probably must persist in the subgingival area at elevated levels over extended periods of time. Furthermore, B forsythus is found more frequently in periodontal patients, and its levels are related to probing depth and periodontal breakdown. 11,12,15 Other bacteria associated with periodontal destruction include Fusobacterium nucleatum, Campylobacter rectus, P micros, Treponema denticola, and Treponema vincentii. Like P intermedia, these species are probably opportunistic pathogens with relatively low pathogenic potential and have to colonize the subgingival area for longer periods of time at elevated levels to be able to affect the periodontium. Most of the above-mentioned periodontal pathogens are Gram-negative anaerobic rods. It is, therefore, not surprising that during the development of periodontitis, there is a shift toward a subgingival flora containing relatively more Gram-negative rods and fewer Gram-positive species. Following full-mouth tooth extraction, changes occur in the tissues and/or surfaces that are available for microorganism adherence. When patients with severe periodontitis become edentulous, A actinomycetemcomitans and P gingivalis are no longer detectable within a month after full-mouth tooth extraction, suggesting that their primary habitat is the dentition or the periodontal sulcus. 16 Furthermore, a marked reduction or even elimination of spirochetes, as well as a reduction in lactobacilli, yeasts, Streptococcus mutans, and Streptococcus sanguis occurs in edentulous adults with or without conventional removable dentures compared to dentate patients. 17 It seems that no significant periodontopathic flora capable of constituting a risk factor or reservoir for transmission, 16 eg, when implants will be placed, is left following full-mouth tooth extraction. MICROBIOTA AROUND STABLE IMPLANTS In edentulous patients, the subgingival area around implants consists mainly of Gram-positive facultative cocci and non-motile rods. On clinically stable implants, S sanguis and Streptococcus mitis are the most predominant organisms, while motile rods, spirochetes, fusiforms, and filaments are infrequently found. 18 A actinomycetemcomitans and P gingivalis are seldom detected, whereas P intermedia and P nigrescens are more common. The periimplant flora in edentulous patients is comparable to the flora colonizing oral soft tissues of denturewearing edentulous patients without implants and the subgingival flora of periodontally healthy dentate patients Furthermore, the peri-implant microbiota is established quite soon after implant placement, and significant subsequent shifts do not occur. 21,24 These data show that the microflora is stable in healthy patients, comprising a microbiota in which periodontal pathogens are present only at low or below detectable levels. In partially edentulous patients, the total number of peri-implant microorganisms is increased, and the proportion of motile rods, spirochetes, and cocci is increased when compared to edentulous patients Quirynen and coworkers 28 isolated the periodontal pathogens P intermedia/p nigrescens, A actinomycetemcomitans, and P gingivalis in 9 (26%), 1 (3%), and 1 (3%) of their sample of partially edentulous patients, respectively, and in none of the edentulous patients. More specifically, they observed that the proportion of spirochetes and motiles around the implants had increased at the expense of the proportion of cocci, if the flora of the remaining teeth harbored more than 20% spirochetes. The concept that the composition of the subgingival microflora around implants in partially edentulous patients is a resultant of the composition of the flora around the teeth has been confirmed in other studies Thus, the peri-implant microflora in partially edentulous patients seems to depend on the periodontal flora of the remaining dentition. As in edentulous patients, colonization of the implant sites with flora specific for that patient occurs soon after the implants are in contact with the oral environment, without major changes over time. 27,32,39 43 However, Kalykakis and associates 43 and Papaioannou and colleagues 27 have reported some time-dependent changes in the peri-implant flora. Papaioannou and colleagues 27 reported an increase in the proportion of motile rods and spirochetes at the expense of cocci around implants. Kalykakis and associates 43 reported an increase with time in the number of putative periodontal The International Journal of Oral & Maxillofacial Implants 831
4 Table 1 Studies Evaluating the Microbiota of the Peri-implant Area of Failing Implants Implants Study No. of Time of Publication design patients No. Type failure (mo) Results Mombelli et al 46 Retrospective 7 (E + PE) 8 ITI ND Failing implants harbored a flora similar to adult periodontitis with increased proportions of P intermedia, Fusocbacterium spp, and spirochetes. P gingivalis was not isolated Mombelli et al 21 Prospective 1 (E) 1 ITI 0 to 4* Chronologically, increased proportions of Actinomyces odontolitius followed by Fusobacterium spp and spirochetes were found around the failing implant Alcoforado et al 44 Retrospective 12 (E + PE) 18 5 different ND A great diversity in the microbial composition with oral as well as primarily non-oral organisms was isolated around the different failing implants Malmstrom et al 48 Retrospective 1 (PE) 4 Brånemark 0 to 2* C rectus, F nucleatum, and E corrodens were associated with implant failure in a patient with rapidly progressive periodontitis Quirynen et al 25 Retrospective 4 (E + PE) 4 Brånemark ND Implants failing due to overload demonstrated a flora similar to periodontal health, while implants failing due to infection were colonized by a periodontopathic flora Rosenberg et al 51 Prospective 5 (PE), 6 (E) 32 4 different 2 to 18 ** In implants failing with infection, many suspected periodontopathic organisms constituted high proportions of the cultivable microflora, while implants failing from suspected traumatic influences demonstrated a flora similar to periodontal health Rams et al 45 Retrospective 1 (PE) 1 Tri-Stage 10** High proportions of Fusobacterium spp and Peptostreptococcus prevotii were isolated in the failing implant Listgarten and Lai 47 Retrospective 41 (ND) 41 ND ND High incidence of B forsythus, spirochetes, Fusobacterium spp, P micros, and P gingivalis Van Winkelhoff et al 42 Prospective 1 (PE) 2 Brånemark 0 to 12** Implant loss was associated with high levels of P gingivalis E = edentulous; PE = partially edentulous; ND = not defined. *After implant placement; **After implant loading. Brånemark implants: Nobel Biocare, Göteborg, Sweden; ITI: Straumann Institut, Waldenburg, Switzerland; Tri-Stage: San Diego, CA. pathogens, such as P gingivalis, A actinomycetemcomitans, or P intermedia. Because of the retrospective nature of latter studies, the authors executed crosssectional statistics and only limited conclusions can be drawn. The true time effect can only be judged based on sufficiently large prospective longitudinal studies It is generally assumed that no significant changes in the oral microbiota occur in the long term and that present (potential) pathogens do not necessarily act in a peri-implant pathogenic manner. 39,40 It has been suggested that differences in the microbiota might occur as the result of various implant characteristics (ie, material, coating, roughness, shape). 3 However, studies by Alcoforado and coworkers, 44 Rams and associates, 45 Mombelli and coworkers, 30 and Lee and colleagues 35 could not relate the presence of particular microorganisms to a particular implant system. Thus, although only limited data are available comparing the microflora of different implant systems, the implant type and surface roughness do not seem to be of significance in the peri-implant microflora. MICROBIOTA AROUND FAILING IMPLANTS A wide variety of microorganisms can be cultivated from the peri-implant region of failing root-form endosseous implants in edentulous and partially edentulous patients. Implant failure cannot be related to a specific microorganism, but certain bacteria are present more frequently around failing implants (Table 1). 832 Volume 17, Number 6, 2002
5 Mombelli and associates 46 isolated an increased proportion of Gram-negative anaerobic rods in edentulous and partially edentulous patients, especially P intermedia, Fusobacteria, and spirochetes. Alcoforado and coworkers 44 observed high proportions of P micros, P intermedia, C rectus, and Fusobacterium species. Listgarten and Lai 47 isolated B forsythus (59%), spirochetes (54%), Fusobacterium (41%), P micros (39%), and P gingivalis (27%) around many of the failing implants in partially edentulous patients. Van Winkelhoff and colleagues 42 evaluated the microflora of periodontal pockets and the peri-implant sulcus in 20 partially edentulous patients on 4 occasions, ranging from implant placement up to 1 year after loading. Preoperatively, P gingivalis was isolated in 3 patients. In 1 of these patients, 2 implants were lost within 12 months after abutment connection because of the loss of osseointegration. In this prospective study, the authors suggested that P gingivalis might have played a role in this implant failure, although this observation is rather casuistic. The results of the aforementioned studies suggest similarities between the microbiota around failing implants and the microbiota associated with periodontitis. Because totally edentulous patients often lack potential periodontal pathogens, which are more common in dentate patients, it is of great interest to compare the microbiota around failing implants in edentulous and partially edentulous patients. Unfortunately, in only 1 study were the microbiota of a failing implant in an edentulous patient reported. 21 Other studies evaluating the microbiota of failing implants included edentulous as well as partially edentulous patients, but the authors did not describe their observations for each separate patient group. Therefore, the incidence or the pattern of failure in edentulous and partially edentulous patients cannot be compared. Also, the question as to whether peri-implantitis is more common in either partially edentulous or edentulous patients remains unanswered. The latter information might provide a clue in resolving the discussion as to whether the actual oral microbiota is the cause or the result of peri-implantitis. Malmstrom and coworkers 48 and Fardal and associates 49 concluded that implants placed in patients with a history of refractory (recurrent) periodontitis probably are at increased risk of failure, presumably because the chance to harbor potential periodontal pathogens is higher. The distressing results of these 2 case reports can easily lead to the hypothesis that implant placement is contraindicated in patients with (a history of) refractory periodontitis. However, this is not supported by larger studies in these periodontal patients, which report success rates exceeding 90%. 40,45,50 In a study by Leonhardt and colleagues, dentate periodontal patients were followed for 3 years after implant placement. Preoperatively, more than 30% of the patients were colonized with A actinomycetemcomitans or P gingivalis, and nearly all patients harbored P intermedia. Within 1 month after implant placement, these microorganisms were found around most implants, but at the 3-year evaluation, peri-implant marginal bone loss exceeding 0.5 mm was observed in only 1 patient. These results suggested that the presence of periodontal pathogens does not necessarily result in the development of peri-implantitis, but the presence of other co-factors is required as well. Thus, local or systemic circumstances are needed to give the supposed periodontopathic microorganism the opportunity to become really pathogenic and causative for infection. Quirynen and Listgarten 25 and Rosenberg and coworkers 51 observed significant differences in the peri-implant flora in patients with failures related to infection or associated with traumatic overloading. In patients with failing implants related to infection, many spirochetes and motile rods could be cultivated, while the peri-implant flora of implants failing caused by overloading resembled that of subjects with poor periodontal health. It seems realistic to conclude that it is possible to place implants with acceptable success rates in periodontal patients as long as the number of potential periodontal pathogens is kept at a low level 40 and other potential (co-)factors are within normal limits. EFFECT OF MUCOSAL CLINICAL VARIABLES AND PERI-IMPLANT BONE LEVEL ON THE MICROFLORA For teeth, clinical parameters such as Plaque Index, Bleeding Index, Gingival Index, and probing pocket depth are positively correlated with the presence of suspected periodontal pathogens. 52 It is of interest to note that comparable associations have been reported for dental implants in several studies. Positive correlations have been found between the Bleeding Index and the proportion of motile organisms 27 and also between probing pocket depth and the composition of microflora (Table 2). 24,26 28,34,35,53 57 In other studies, however, no such associations were established. 30,37,58 60 Although suspected periodontal pathogens were identified at implant sites in these studies, the clinical parameters were not indicative of deteriorating The International Journal of Oral & Maxillofacial Implants 833
6 Table 2 Studies Evaluating the Correlation Between Clinical Parameters and the Peri-implant Microflora Implants Study No. of Time of Publication design patients No. Type sampling Results Lekholm et al 54 Retrospective 20 (E + PE) 125 Brånemark 0.5 to 12 y Deeper pockets were correlated with increasing presence of spirochetes Sanz et al 53 Retrospective 13 (PE) 13 ESCI ND Pathogens associated with active periodontitis lesions were detected in higher frequencies and percentages in implants with pockets 4 mm, GI 2, or CFF 40 Mombelli and Prospective 18 (E) 36 ITI 2 to 3 y The relative proportion of Capnocytophaga Mericske-Stern 24 was related to PPD and bleeding Rams et al 45 Retrospective 9 (PE) 40 Tri-Stage 7 to 10 mo Increased PPD was related to decreased proportion of cocci and increased proportion of motiles. Pockets > 7 mm harbored more Fusobacterium spp and P prevotii (1 patient) Palmisano et al 55 Retrospective 25 (E + PE) 43 Integral > 1 y PPD was positively correlated with spirochetes and negatively correlated with cocci Dharmar et al 26 Retrospective 24 (E + PE) 64 Brånemark ND PPD was positively correlated with motile rods and negatively correlated with cocci Papaioannou et al 27 Retrospective 297 (E + PE) 561 Brånemark 1 to 120 PPD was positively correlated with spiromo chetes, fusiforms, and filaments and negatively correlated with cocci. BOP was positively correlated with motile rods Quirynen et al 28 Retrospective 159 (PE) 300 Brånemark 1 to 11 y Samples from peri-implant pockets 4 mm showed increased proportions of spirochetes and motiles Danser et al 57 Retrospective 20 (E) 91 Brånemark 1 to 12 y Subjects harboring P intermedia showed IMZ pockets 5 mm Tanner et al 56 Retrospective 12 (ND) 12 ND ND Implants with deeper probing depths or increased bone loss were frequently colonized by B forsythus, F nucleatum, and C rectus Keller et al 34 Retrospective 15 (PE) 60 ITI 0.5 to 5 y C rectus was found more frequently in pockets 4 mm. P gingivalis, Selenomonas spp, P melaninogenica, and A naeslundii were only isolated from pockets 4 mm E = edentulous; PE = partially edentulous; ND = not defined; GI = Gingival Index; CFF = crevicular fluid flow; PPD = probing pocket depth; BOP = bleeding on probing. Brånemark: Nobel Biocare, Göteborg, Sweden; ESCI: endosteal sapphire ceramic implant; ITI: Straumann Institut, Waldenburg, Switzerland; Tri-Stage: San Diego, CA; Integral: Calcitek, Carlsbad, CA; IMZ: Friedrichsfled, Mannheim, Germany. support or implant failure. This supports the hypothesis that co-factors are required for periodontopathic bacteria to become pathogenic. Probing pocket depth has been found to be the most important clinical parameter in relation to the peri-implant microbiota. 45 With increasing pocket depth, a significant decline in cocci and increase of other morphotypes (motiles and spirochetes), as well as for the total number of organisms, was observed. 45 Other clinical parameters seem to be less significant in relation to the peri-implant microbiota. Few studies have reported on the microbiota of implants with peri-implant bone defects (Table 3). 32,38,40,61 63 Again, these bone defects could not be related specifically to the presence of certain microorganisms, but certain microorganisms were detectable or present at higher levels in periimplant bone defects. Mengel and associates 32 did not find any correlation between the subgingival microflora and peri-implant marginal bone loss, while other authors reported some correlations. Frequently, P intermedia, P gingivalis, A actinomycetemcomitans, B forsythus, T denticola, P nigrescens, P micros, and F nucleatum were isolated in implants showing bone defects. 38,40,60 62 Again, co-factors seem to be required for periodontopathic bacteria to be associated with peri-implant bone loss. 834 Volume 17, Number 6, 2002
7 Table 3 Studies Evaluating the Correlation Between Marginal Bone Loss and the Peri-implant Microflora Implants Study No. of Time of Publication design patients No. Type sampling Results Leonhardt et al 40 Prospective 19 (PE) 63 Brånemark 0 to 36 mo At the 3-year evaluation, 3 implants in 1 patient showed bone loss > 0.5 mm. These implants were colonized with P intermedia Mengel et al 32 Prospective 5 (PE) 36 Brånemark 12 mo No correlation was found between the subgingival microflora and peri-implant marginal bone loss Augthun and Retrospective 12 (E) 18 IMZ 6 y All implants showed bone loss exceeding 5 Conrads 61 mm. Most implants were colonized by A actinomycetemcomitans and Prevotella spp Salcetti et al 62 Retrospective 29 (E + PE) 69 ND > 1 y Implants showing > 2 mm bone loss harbored more frequently F nucleatum, P micros, and P nigrescens Leonhardt et al 63 Retrospective 88 (E + PE) ND Brånemark 5 to 7 y Implants with bone loss 3 threads after the first year of loading were frequently colonized by P gingivalis, P intermedia, or A actinomycetemcomitans. Staphylococcus spp, enterics, and Candida spp were also found frequently Hultin et al 38 Retrospective 15 (PE) 55 Brånemark 10 y Five implants showed bone loss > 2 mm. These implants were colonized by A actinomycetemcomitans, P gingivalis, P intermedia, B forsythus, and T denticola E = edentulous; PE = partially edentulous; ND = not defined. The peri-implant tissues of dental implants are colonized by a large variety of oral microbial complexes. The microflora that is present in the oral cavity before implant placement determines the composition of the newly establishing microflora around implants. Implants with signs of deterioration (peri-implantitis) show a microbiota resembling that of adult or refractory periodontitis. These implants yield large amounts of Gram-negative anaerobic bacteria, with Fusobacteria, spirochetes, B forsythus, and black-pigmenting bacteria such as P intermedia and P nigrescens. P gingivalis and A actinomycetemcomitans are infrequently cultivated putative periodontal pathogens. It is controversial as to whether the recovered organisms are the cause of the failure or whether the actual microbiota is merely a result or a manifestation of changed intraoral circumstances. It has been shown that periodontal pathogens can be present in the subgingival area around implants for a long period of time without resulting in signs of destructive processes or implant failure. Moreover, when peri-implantitis is present around 1 of multiple implants in the same patient, the other implants (which are exposed to the same oral environment) do not necessarily show signs of deterioration. Therefore, the role of oral microbiota in implant failure is subject to discussion. 7 Local circumstances (ie, unsatisfactory oral hygiene, bone defects, deep pockets, overload) as well as systemic conditions (ie, diabetes, smoking, genetic factors) may be important contributing factors as well. This is in agreement with the current periodontal literature, in which it is increasingly emphasized that systemic factors play a role in the development of periodontitis The known periodontal pathogens are linked to periodontitis in different ways. A actinomycetemcomitans and P gingivalis seem to play a primary role in the development of periodontitis. 11,14,67 However, these microorganisms are found infrequently in peri-implantitis. Other periodontal pathogens play a secondary role in the development of periodontitis. They must be present in high numbers, or a co-factor is required for these pathogens to come to expression. 11 Therefore, the following hypothesis is postulated. Microorganisms have the potential to act as promoters or catalysts in implant failure, but they need a suitable oral environment to do so. In other words, favorable local circumstances or systemic conditions are required to allow microorganisms to become pathogenic. Since A actinomycetemcomitans and P gingivalis are infrequently found in periimplantitis patients and other periopathogens are thought to be less pathogenic, local circumstances The International Journal of Oral & Maxillofacial Implants 835
8 and systemic conditions are probably more important in implant failure than the presence of periopathogens only. This hypothesis is in agreement with the increasing evidence in periodontology supporting bacteria as the cause of the disease, but the individual s genetic makeup and environmental influences as determining the severity of the disease. 64,68 Peri-implantitis can be considered multifactorial as well and includes host-related factors. 64,65 Most likely, a complex interplay between the bacterial challenge and host factors determines whether a rapidly progressing peri-implantitis develops, leading to implant failure. Specific microorganisms may play a role in initiating this process but more likely are important in its maintenance or its progression. CONCLUSION Table 4 Summary of the Main Conclusions Derived from the Comprehensive Review of the Literature Conclusion In Table 4 the main conclusions derived from this comprehensive review of the literature are summarized, and references are provided that support these conclusions. Future research should concentrate on discovering relevant local and systemic conditions in the etiology of peri-implantitis. If these latter conditions are known, patients at risk can be defined and preoperative measures to increase implant survival can possibly be implemented. Probably this is a more rational approach than a microbial survey as such. Thus, a microbial survey can be reserved for patients who are potentially at risk, thus saving the costs and reducing the use of antibiotics in eradicating periopathogens. REFERENCES References The microflora of the oral cavity prior to implantation determines the composition of the flora in the peri-implant area The microflora around stable implants resembles that of the subgingival flora of healthy dentate patients The microflora of peri-implantitis lesions resembles that of 21, 25, 42, 44 46, 51 adult or refractory periodontitis Potential periodontal pathogens present in the oral cavity do not 39 41, 45, 50 necessarily act as peri-implant pathogens The etiology of peri-implantitis probably is multifactorial, 64, 65, 68 and genetic factors play an important role 1. Brånemark P-I, Zarb GA, Albrektsson T (eds). Tissue-Integrated Prostheses: Osseointegration in Clinical Dentistry. Chicago: Quintessence, Fiorellini JP, Martuscelli G, Weber HP. Longitudinal studies of implant systems. Periodontol ;17: Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. (I). Success criteria and epidemiology. Eur J Oral Sci 1998;106: Mombelli A, Lang NP. The diagnosis and treatment of periimplantitis. Periodontol ;17: Adell R, Lekholm U, Rockler B, Brånemark P-I. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 1981;10: Tonetti MS, Schmid J. Pathogenesis of implant failures. Periodontol ;4: Esposito M, Hirsch JM, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants (II). Etiopathogenesis. Eur J Oral Sci 1998;106: Socransky SS, Haffajee AD. Microbiology of periodontal disease. In: Lindhe J, Karring T, Lang NP (eds). Clinical Periodontology and Implant Dentistry, ed 3. Copenhagen: Munksgaard, 1997: Slots J. Microflora in the healthy gingival sulcus in man. Scand J Dent Res 1977;85: Tanner A, Maiden MF, Macuch PJ, Murray LL, Kent RL Jr. Microbiota of health, gingivitis, and initial periodontitis. J Clin Periodontol 1998;25: Haffajee AD, Cugini MA, Tanner A, et al. Subgingival microbiota in healthy, well-maintained elder and periodontitis subjects. J Clin Periodontol 1998,25: Ximenez-Fyvie LA, Haffajee AD, Socransky SS. Microbial composition of supra- and subgingival plaque in subjects with adult periodontitis. J Clin Periodontol ;27: Riviere GR, Smith KS, Tzagaroulaki E, et al. Periodontal status and detection frequency of bacteria at sites of periodontal health and gingivitis. J Periodontol 1996;67: Griffen AL, Becker MR, Lyons SR, Moeschberger ML, Leys KU. Prevalence of Porphyromonas gingivalis and periodontal health status. J Clin Microbiol 1998:36: Volume 17, Number 6, 2002
9 15. Haffajee AD, Socransky SS. Microbial etiological agents of destructive periodontal diseases. Periodontol ; 5: Danser MM, van Winkelhoff AJ, de Graaff J, Loos BG, van der Velden U. Short-term effect of full-mouth extraction on periodontal pathogens colonizing the oral mucous membranes. J Clin Periodontol 1994;21: Socransky SS, Manganiello SD. The oral microbiota of man from birth to senility. J Periodontol 1971;42: Mombelli A, Lang NP. Microbial aspects of implant dentistry. Periodontol ;4: Gusberti FA, Gada TG, Lang NP, Geering AH. Cultivable microflora of plaque from full denture bases and adjacent palatal mucosa. J Biol Buccale 1985;13: Nakou M, Mikx FHM, Oosterwaal PJM, Krijsen JCWM. Early microbial colonization of permucosal implants in edentulous patients. J Dent Res 1987;66: Mombelli A, Buser D, Lang NP. Colonization of osseointegrated titanium implants in edentulous patients. Early results. Oral Microbiol Immunol 1988;3: Sordyl CM, Simons AM, Molinari JA. The microbial flora associated with stable endosseous implants. J Oral Implantol 1995;21: Danser MM, van Winkelhoff AJ, de Graaff J, van der Velden U. Putative periodontal pathogens colonizing oral mucous membranes in denture-wearing subjects with a past history of periodontitis. J Clin Periodontol 1995;22: Mombelli A, Mericske-Stern R. Microbiological features of stable osseointegrated implants used as abutments for overdentures. Clin Oral Implants Res 1990;1: Quirynen M, Listgarten MA. Distribution of bacterial morphotypes around natural teeth and titanium implants ad modum Branemark. Clin Oral Implants Res 1990;1: Dharmar S, Yoshida K, Adachi Y, Kishi M, Okuda K, Sekine H. Subgingival microbial flora associated with Brånemark implants. Int J Oral Maxillofac Implants 1994;9: Papaioannou W, Quirynen M, Nys M, van Steenberghe D. The effect of periodontal parameters on the subgingival microbiota around implants. Clin Oral Implants Res 1995;6: Quirynen M, Papaioannou W, van Steenberghe D. Intraoral transmission and the colonization of oral hard surfaces. J Periodontol 1996;67: Kohavi D, Greenberg R, Raviv E, Sela NL. Subgingival and supragingival microbial flora around healthy osseointegrated implants in partially edentulous patients. Int J Oral Maxillofac Implants 1994;9: Mombelli A, Marxer M, Gaberthuel T, Grunder U, Lang NP. The microbiota of osseointegrated implants in patients with a history of periodontal disease. J Clin Periodontol 1995;22: Papaioannou W, Quirynen M, van Steenberghe D. The influence of periodontitis on the subgingival flora around implants in partially edentulous patients. Clin Oral Implants Res 1996;7: Mengel R, Stelzel M, Hasse C, Flores-de-Jacoby L. Osseointegrated implants in patients treated for generalized severe adult periodontitis. An interim report. J Periodontol 1996;67: Kalykakis GK, Mojon PH, Nisengard R, Spiekermann H, Zafiropoulos G-G. Clinical and microbial findings on osseointegrated implants: Comparisons between partially dentate and edentulous subjects. Eur J Prosthodont Restorative Dent 1998;6: Keller W, Brägger U, Mombelli A. Peri-implant microflora of implants with cemented and screw retained suprastructures. Clin Oral Implants Res 1998;9: Lee KH, Maiden MF, Tanner AC, Weber HP. Microbiota of successfully osseointegrated dental implants. J Periodontol 1991;70: Lee KH, Tanner AC, Maiden MF, Weber HP. Pre- and post-implantation microbiota of the tongue, teeth, and newly placed implants. J Clin Periodontol 1999;26; Sbordone L, Barone A, Ciaglia RN, Ramaglia L, Iacono VJ. Longitudinal study of dental implants in a periodontally compromised population. J Periodontol 1999;70: Hultin M, Gustafsson A, Klinge B. Long-term evaluation of osseointegrated dental implants in the treatment of partly edentulous patients. J Clin Periodontol 2000;27: Koka S, Razzoog ME, Bloem TJ, Syed S. Microbial colonization of dental implants in partially edentulous subjects. J Prosthet Dent 1993;70: Leonhardt A, Adolfsson B, Lekholm U, Wikstrom M, Dahlen G. A longitudinal microbiological study on osseointegrated titanium implants in partially edentulous patients. Clin Oral Implants Res 1993;4: Pontoriero R, Tonelli MP, Carnevale G, Mombelli A, Nyman SR, Lang NP. Experimentally induced peri-implant mucositis. A clinical study in humans. Clin Oral Implants Res 1994;5: Van Winkelhoff AJ, Goene R, Benschop C, Folmer T. Early colonization of dental implants by putative periodontal pathogens in partially edentulous patients. Clin Oral Implants Res 2000;11: Kalykakis G, Zafiropoulos G-G, Murat Y, Spiekermann H, Nisengard RJ. Clinical and microbiological status of osseointegrated implants. J Periodontol 1994;65: Alcoforado GA, Rams TE, Feik D, Slots J. Microbial aspects of failing osseointegrated dental implants in humans. J Parodontol 1990;10: Rams TE, Roberts TW, Feik D, Molzan AK, Slots J. Clinical and microbiological findings on newly inserted hydroxyapatite-coated and pure titanium human dental implants. Clin Oral Implants Res 1991;2: Mombelli A, van Oosten M, Schurch E, Lang NP. The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiol Immunol 1987; 2: Listgarten MA, Lai CH. Comparative microbiological characteristics of failing implants and periodontally diseased teeth. J Periodontol 1999;70: Malmstrom HS, Fritz ME, Timmis DP, Van Dyke T. Osseointegrated implant treatment of a patient with rapidly progressive periodontitis. A case report. J Periodontol 1990;61: Fardal O, Johannessen AC, Olsen I. Severe, rapid progressing peri-implantitis. J Clin Periodontol 1999;26: Nevins M, Langer B. The successful use of osseointegrated implants for the treatment of the recalcitrant periodontal patient. J Periodontol 1995;66: Rosenberg ES, Torosian JP, Slots J. Microbial differences in 2 clinically distinct types of failures of osseointegrated implants. Clin Oral Implants Res 1991;2: Savitt ED, Socransky SS. Distribution of certain subgingival microbial species in selected periodontal conditions. J Periodontal Res 1984;19: The International Journal of Oral & Maxillofacial Implants 837
10 53. Sanz M, Newman MG, Nachnani S, Holt R, Stewart R, Flemmig T. Characterization of the subgingival microbial flora around endosteal sapphire dental implants in partially edentulous patients. Int J Oral Maxillofac Implants 1990;5: Lekholm U, Adell R, Lindhe J, et al. Marginal tissue reactions at osseointegrated titanium fixtures (II). A cross-sectional retrospective study. Int J Oral Maxillofac Surg 1986; 15: Palmisano DA, Mayo JA, Block MS, Lancaster DM. Subgingival bacteria associated with hydroxylapatite-coated dental implants: Morphotypes and trypsin-like enzyme activity. Int J Oral Maxillofac Implants 1991;6: Tanner A, Maiden MF, Lee K, Shulman LB, Weber HP. Dental implant infections. Clin Infect Dis 1997;25(suppl 2):S213 S Danser MM, van Winkelhoff AJ, van der Velden U. Periodontal bacteria colonizing oral mucous membranes in edentulous patients wearing dental implants. J Periodontol 1997;68: Lekholm U, Ericsson I, Adell R, Slots J. The condition of the soft tissues at tooth and fixture abutments supporting fixed bridges. A microbiological and histological study. J Clin Periodontol 1986;13: Adell R, Lekholm U, Rockler B, et al. Marginal tissue reactions at osseointegrated titanium fixtures (I). A 3-year longitudinal prospective study. Int J Oral Maxillofac Surg 1986; 15: Apse P, Ellen RP, Overall CM, Zarb GA. Microbiota and crevicular fluid collagenase activity in the osseointegrated dental implant sulcus: A comparison of sites in edentulous and partially edentulous patients. J Periodontal Res 1989; 24: Augthun M, Conrads G. Microbial findings of deep periimplant bone defects. Int J Oral Maxillofac Implants 1997; 12: Salcetti JM, Moriarty JD, Cooper LF, et al. The clinical, microbial, and host response characteristics of the failing implant. Int J Oral Maxillofac Implants 1997;12: Leonhardt A, Renvert S, Dahlen G. Microbial findings at failing implants. Clin Oral Implants Res 1999;10: Wilson TG. Not all patients are the same: Systemic risk factors for adult periodontitis. Gen Dent 1999;47: Wilson GW, Nunn M. The relationship between the interleukin-1 periodontal genotype and implant loss. Initial data. J Periodontol 1999;70: Kronstrom M, Svensson B, Erickson E, Houston L, Braham P, Persson GR. Humoral immunity host factors in subjects with failing or successful titanium dental implants. J Clin Periodontol 2000;27: Timmerman MF, van der Weijden GA, Abbas F, et al. Untreated periodontal disease in Indonesian adolescents. Subgingival microbiota in relation to experienced progression of periodontitis. J Clin Periodontol 2001;28: McGuire MK, Nunn ME. Prognosis versus actual outcome IV. The effectiveness of clinical parameters and IL-1 genotype in accurately predicting prognoses and tooth survival. J Periodontol 1999;70: Volume 17, Number 6, 2002
Detection of predominant subgingival periopathogens around submerged and non submerged hydroxy apatite implants
 [Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
[Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Materials and Methods: Literature review and Authors opinion.
 Haffajee AD, Bogren A, Hasturk H et al. Subgingival microbiota of chronic periodontitis subjects from different geographic locations. J Clin Periodontol 2004; 31:996-1002. Purpose: To compare the subgingival
Haffajee AD, Bogren A, Hasturk H et al. Subgingival microbiota of chronic periodontitis subjects from different geographic locations. J Clin Periodontol 2004; 31:996-1002. Purpose: To compare the subgingival
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Dynamics of initial subgingival colonization of pristine peri-implant pockets
 Marc Quirynen Roel Vogels Wouter Peeters Daniel van Steenberghe Ignace Naert Anne Haffajee Dynamics of initial subgingival colonization of pristine peri-implant pockets Authors affiliations: Marc Quirynen,
Marc Quirynen Roel Vogels Wouter Peeters Daniel van Steenberghe Ignace Naert Anne Haffajee Dynamics of initial subgingival colonization of pristine peri-implant pockets Authors affiliations: Marc Quirynen,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis
 157 Journal of Oral Science, Vol. 46, No. 3, 157-161, 2004 Original Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis Mohammad Hossein Salari and Zainab Kadkhoda Department
157 Journal of Oral Science, Vol. 46, No. 3, 157-161, 2004 Original Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis Mohammad Hossein Salari and Zainab Kadkhoda Department
Periodontal Microbiology (Dental Plaque)
 Periodontal Microbiology (Dental Plaque) Dental plaque Dental plaque is soft deposits that form the biofilm adhering to the tooth surface of other hard surface in the oral cavity, including removable and
Periodontal Microbiology (Dental Plaque) Dental plaque Dental plaque is soft deposits that form the biofilm adhering to the tooth surface of other hard surface in the oral cavity, including removable and
University of Groningen
 University of Groningen Microbiota around teeth and dental implants in ly healthy, partially edentulous patients Meijndert, Leo; van der Reijden, Wil A.; Raghoebar, Gerry; Meijer, Hendrikus; Vissink, Arjan
University of Groningen Microbiota around teeth and dental implants in ly healthy, partially edentulous patients Meijndert, Leo; van der Reijden, Wil A.; Raghoebar, Gerry; Meijer, Hendrikus; Vissink, Arjan
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars
 J Oral Maxillofac Surg 60:1234-1240, 2002 Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars Raymond P. White, Jr, DDS, PhD,* Phoebus N. Madianos,
J Oral Maxillofac Surg 60:1234-1240, 2002 Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars Raymond P. White, Jr, DDS, PhD,* Phoebus N. Madianos,
actinomycetemcornitans and
 Periodontology 2000, Vol. 20, 1999, 341-362 Printed in Denmark. All rights reserved Copyright 8 Munksgaard 1999 PERIODONTOLOGY 2000 ISSN 0906-6713 Ecological considerations in the treatment of Actinobacillus
Periodontology 2000, Vol. 20, 1999, 341-362 Printed in Denmark. All rights reserved Copyright 8 Munksgaard 1999 PERIODONTOLOGY 2000 ISSN 0906-6713 Ecological considerations in the treatment of Actinobacillus
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care
 Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Journal of Dentistry, Tehran University of Medical Sciences
 Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
FACULTY OF HEALTH SCIENCES INSTITUTE OF CLINICAL DENTISTRY
 Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose?
 Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose? Arndt Güntsch & Bernd W. Sigusch Parodontologie Nachrichten 1/2010 Literaturverzeichnis (1) Berglundh T, Lindhe J, Marinello
Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose? Arndt Güntsch & Bernd W. Sigusch Parodontologie Nachrichten 1/2010 Literaturverzeichnis (1) Berglundh T, Lindhe J, Marinello
Polyspecies biofilm formation involved in overdenture peri-implantitis
 Romanian Biotechnological Letters Vol., No. x, Copyright 2016 University of Bucharest Printed in Romania. All rights reserved ORIGINAL PAPER Polyspecies biofilm formation involved in overdenture peri-implantitis
Romanian Biotechnological Letters Vol., No. x, Copyright 2016 University of Bucharest Printed in Romania. All rights reserved ORIGINAL PAPER Polyspecies biofilm formation involved in overdenture peri-implantitis
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Hoeksema, A. (2016). Oral health in frail elderly [Groningen]: Rijksuniversiteit Groningen](/thumbs/87/96311633.jpg) University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Oral health in frail elderly Hoeksema, Albert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
Outcome of dental implants in patients with a history of periodontitis
 Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Transmission of periodontopathic ba Title natural teeth to implants. Okuda, K; Sato, T; Ishihara, K
 Transmission of periodontopathic ba Title natural teeth to implants. Author(s) Aoki, M; Takanashi, K; Matsukubo, T Alternative Okuda, K; Sato, T; Ishihara, K Clinical implant dentistry and rela Journal
Transmission of periodontopathic ba Title natural teeth to implants. Author(s) Aoki, M; Takanashi, K; Matsukubo, T Alternative Okuda, K; Sato, T; Ishihara, K Clinical implant dentistry and rela Journal
Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report
 Journal of Periodontology & Implant Dentistry Case Report Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report Ponnudurai Samuel Ganna Prakash * Ramalingm
Journal of Periodontology & Implant Dentistry Case Report Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report Ponnudurai Samuel Ganna Prakash * Ramalingm
Microbial biofilms are
 Managing the complexity of a dynamic biofilm John G. Thomas, MS, PhD; Lindsay A. Nakaishi, BS Microbial biofilms are common in nature. Virtually any fluid environment in which microorganisms are subject
Managing the complexity of a dynamic biofilm John G. Thomas, MS, PhD; Lindsay A. Nakaishi, BS Microbial biofilms are common in nature. Virtually any fluid environment in which microorganisms are subject
- BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis
 Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Attachment of Oral Gram-negative Anaerobic Rods to a Smooth Titanium Surface: An Electron Microscopy Study
 Attachment of Oral Gram-negative Anaerobic Rods to a Smooth Titanium Surface: An Electron Microscopy Study Heidi Kuula, DDS 1 /Eija Könönen, DDS, PhD 2 /Kari Lounatmaa, PhD 3 /Yrjö T. Konttinen, MD, PhD
Attachment of Oral Gram-negative Anaerobic Rods to a Smooth Titanium Surface: An Electron Microscopy Study Heidi Kuula, DDS 1 /Eija Könönen, DDS, PhD 2 /Kari Lounatmaa, PhD 3 /Yrjö T. Konttinen, MD, PhD
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Microbiota and Oral Disease Prof. Dennis Cvitkovitch
 1 Professor Dennis Cvitkovitch Faculty of Dentistry Dental Research Institute University of Toronto The human microbiome We are a composite species: eukaryotic, bacterial, archeal Every human harbors over
1 Professor Dennis Cvitkovitch Faculty of Dentistry Dental Research Institute University of Toronto The human microbiome We are a composite species: eukaryotic, bacterial, archeal Every human harbors over
In recent decades, the clinical replacement of natural
 Effect of Intracrevicular Restoration Margins on Peri-implant Health: Clinical, Biochemical, and Microbiologic Findings Around Esthetic Implants up to 9 Years Catherine Giannopoulou, Dr Med Dent 1 /Jean-Pierre
Effect of Intracrevicular Restoration Margins on Peri-implant Health: Clinical, Biochemical, and Microbiologic Findings Around Esthetic Implants up to 9 Years Catherine Giannopoulou, Dr Med Dent 1 /Jean-Pierre
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Oral bacterial interactions in periodontal health and disease
 Vol. 6(5), pp. 51-57, August 2014 DOI: 10.5897/JDOH2014.0127 Article Number: 84910BB46956 ISSN 2006-9871 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/jdoh
Vol. 6(5), pp. 51-57, August 2014 DOI: 10.5897/JDOH2014.0127 Article Number: 84910BB46956 ISSN 2006-9871 Copyright 2014 Author(s) retain the copyright of this article http://www.academicjournals.org/jdoh
Interrelationship between Periodontitis and Peri-Implantitis: Myth or Reality?
 REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
Journal of Periodontology & Implant Dentistry. Research Article
 Journal of Periodontology & Implant Dentistry Research Article Assessment of Aggregatibacter actinomycetemcomitans and Prevotella intermedia Counts around Healthy Implants, Diseased Implants and Sound
Journal of Periodontology & Implant Dentistry Research Article Assessment of Aggregatibacter actinomycetemcomitans and Prevotella intermedia Counts around Healthy Implants, Diseased Implants and Sound
Periodontal Microbiology. Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University
 Periodontal Microbiology Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University 2016 Topics introduction, historical perspective pathogens of destructive periodontal diseases microbial
Periodontal Microbiology Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University 2016 Topics introduction, historical perspective pathogens of destructive periodontal diseases microbial
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up
 Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Subgingival microbiota of chronic periodontitis subjects from different geographic locations
 J Clin Periodontol 2004; 31: 996 1002 doi: 10.1111/j.1600-051X.2004.00597.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Subgingival microbiota of chronic periodontitis
J Clin Periodontol 2004; 31: 996 1002 doi: 10.1111/j.1600-051X.2004.00597.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Subgingival microbiota of chronic periodontitis
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions
 Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Evaluation of Subgingival Microflora in Diabetic and Nondiabetic Patients
 JCDP 10.5005/jp-journals-10024-1113 ORIGINAL RESEARCH Evaluation of Subgingival Microflora in Diabetic and Nondiabetic Patients Evaluation of Subgingival Microflora in Diabetic and Nondiabetic Patients
JCDP 10.5005/jp-journals-10024-1113 ORIGINAL RESEARCH Evaluation of Subgingival Microflora in Diabetic and Nondiabetic Patients Evaluation of Subgingival Microflora in Diabetic and Nondiabetic Patients
Volume 2 Issue
 Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
 J Clin Periodontol 2007; 34: 805 815 doi: 10.1111/j.1600-051X.2007.01106.x Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
J Clin Periodontol 2007; 34: 805 815 doi: 10.1111/j.1600-051X.2007.01106.x Impact of supportive periodontal therapy and implant surface roughness on implant outcome in patients with a history of periodontitis
Received 18 June 2004; returned 6 August 2004; revised 1 December 2004; accepted 8 December 2004
 Journal of Antimicrobial Chemotherapy (2005) 55, 347 351 doi:10.1093/jac/dki013 Advance Access publication 4 February 2005 Concentrations and in vivo antibacterial activity of spiramycin and metronidazole
Journal of Antimicrobial Chemotherapy (2005) 55, 347 351 doi:10.1093/jac/dki013 Advance Access publication 4 February 2005 Concentrations and in vivo antibacterial activity of spiramycin and metronidazole
Many of the problems reported by conventional
 Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
Maxillary Overdentures Retained by Splinted and Unsplinted Implants: A Retrospective Study Timo O. Närhi, DDS, PhD 1 /Miluska Hevinga, DDS 2 / Ralph A. C. A. Voorsmit, DDS, PhD 3 /Warner Kalk, DDS, PhD
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review
 The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
The Effects of Anti-infective Preventive Measures on the Occurrence of Biologic Implant Complications and Implant Loss: A Systematic Review Giovanni E. Salvi, DMD, Prof Dr Med Dent 1 /Nicola U. Zitzmann,
INTRODUCTION TO DENTAL IMPLANTOLOGY HISTORY OF DENTAL IMPLANTS EUGENIA PROKOPETS, DDS LSU PERIODONTICS
 INTRODUCTION TO DENTAL IMPLANTOLOGY HISTORY OF DENTAL IMPLANTS EUGENIA PROKOPETS, DDS LSU PERIODONTICS Thank you Dr. Simmons BEFORE THE COMMON ERA 16TH AND 17TH CENTURIES Archeological records from China
INTRODUCTION TO DENTAL IMPLANTOLOGY HISTORY OF DENTAL IMPLANTS EUGENIA PROKOPETS, DDS LSU PERIODONTICS Thank you Dr. Simmons BEFORE THE COMMON ERA 16TH AND 17TH CENTURIES Archeological records from China
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS
 THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
Research Centre of Stomatology, Department of Stomatology, Faculty of Medicine, Masaryk University, Brno 2. Received after revision April 2008
 SCRIPTA MEDICA (BRNO) 81 (2): 85 96, June 2008 Occurrence of periodontal pathogens in patients treated with fixed orthodontic appliances Černochová P. 1, Augustin P. 1, Fassmann A. 1, Izakovičová-Hollá
SCRIPTA MEDICA (BRNO) 81 (2): 85 96, June 2008 Occurrence of periodontal pathogens in patients treated with fixed orthodontic appliances Černochová P. 1, Augustin P. 1, Fassmann A. 1, Izakovičová-Hollá
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study
 A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
A Multicenter Report on 1,022 Consecutively Placed ITI Implants: A 7-Year Longitudinal Study Daniel Brocard, DCD, DSO 1 /Pierre Barthet, DCD, DSO 2 /Eric Baysse, DCD 1 / Jean François Duffort, DCD, DSO
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
University of Groningen
 University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
University of Groningen A Technique for Standardized Evaluation of Soft and Hard Peri-Implant Tissues in Partially Edentulous Patients Meijndert, Leo; Meijer, Hendrikus; Raghoebar, Gerry; Vissink, Arjan
Aggressive and chronic periodontitis
 J Periodontol February 2005 Prevalence of Periodontopathic Bacteria in Aggressive Periodontitis Patients in a Chilean Population Marta Gajardo,* Nora Silva,* Leyla Gómez,* Rubén León, Beatriz Parra, Adolfo
J Periodontol February 2005 Prevalence of Periodontopathic Bacteria in Aggressive Periodontitis Patients in a Chilean Population Marta Gajardo,* Nora Silva,* Leyla Gómez,* Rubén León, Beatriz Parra, Adolfo
Pathogens in Relation to Periodontal Status
 J Dent Res 74(11): 1789-1793, November, 1995 Salivary Levels of Suspected Periodontal Pathogens in Relation to Periodontal Status and Treatment B. von Troil-Lindenl*, H. Torkko2, S. Alaluusua3, H. Jousimies-Somer4,
J Dent Res 74(11): 1789-1793, November, 1995 Salivary Levels of Suspected Periodontal Pathogens in Relation to Periodontal Status and Treatment B. von Troil-Lindenl*, H. Torkko2, S. Alaluusua3, H. Jousimies-Somer4,
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
The Microbial Etiology and Pathogenesis of Peri-Implantitis
 The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
The evaluation of long-term treatment results for
 Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
Long-Term Results After Placement of Dental Implants: Longitudinal Study of 1,964 Implants over 16 Years Nicole Noack, MD*/Jürgen Willer, DMD**/Jürgen Hoffmann, MD, DMD*** In a retrospective study, Kaplan-Meier
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
FACTORS AFFECTING PERI-IMPLANT TISSUE REACTIONS
 Department of Periodontology, Institute of Odontology, Karolinska Institutet, Stockholm, Sweden FACTORS AFFECTING PERI-IMPLANT TISSUE REACTIONS by Margareta Hultin Stockholm 2001 OPPONENT: Professor Jan
Department of Periodontology, Institute of Odontology, Karolinska Institutet, Stockholm, Sweden FACTORS AFFECTING PERI-IMPLANT TISSUE REACTIONS by Margareta Hultin Stockholm 2001 OPPONENT: Professor Jan
Microbial Composition in Peri-implant Health and Disease
 Microbial Composition in Peri-implant Health and Disease Authors Malak Hamzé Saad Fadhel Tutor Py Palmqvist ABSTRACT Although the infectious initiation of peri-implantitis is commonly accepted, differences
Microbial Composition in Peri-implant Health and Disease Authors Malak Hamzé Saad Fadhel Tutor Py Palmqvist ABSTRACT Although the infectious initiation of peri-implantitis is commonly accepted, differences
The International Journal of Periodontics & Restorative Dentistry
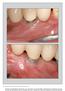 The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
JSS Medical and Dental College and Hospital, JSS University, Mysore, India *Author for Correspondence
 CLINICAL, MICROBIOLOGICAL AND MOLECULAR STUDY OF PORPHYROMONAS GINGIVALIS IN PATIENTS WITH CHRONIC PERIODONTITIS *Mayuri Vajawat 1, Vijay Kumar 2, K.G. Rajeshwari 3 and P.C. Deepika 4 1&4 Department of
CLINICAL, MICROBIOLOGICAL AND MOLECULAR STUDY OF PORPHYROMONAS GINGIVALIS IN PATIENTS WITH CHRONIC PERIODONTITIS *Mayuri Vajawat 1, Vijay Kumar 2, K.G. Rajeshwari 3 and P.C. Deepika 4 1&4 Department of
Periodontopathic Bacteria: A Microbiological View
 ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 873-877 http://www.ijcmas.com Review Article Periodontopathic Bacteria: A Microbiological View Bhadoria Kiran 1 *, Jana A.M 2 and Shrivastav Archana 1 1 Department
ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 873-877 http://www.ijcmas.com Review Article Periodontopathic Bacteria: A Microbiological View Bhadoria Kiran 1 *, Jana A.M 2 and Shrivastav Archana 1 1 Department
Subgingival microbiota of periodontally untreated Mexican subjects with generalized aggressive periodontitis
 J Clin Periodontol 2006; 33: 869 877 doi: 10.1111/j.1600-051X.2006.01006.x Subgingival microbiota of periodontally untreated Mexican subjects with generalized aggressive periodontitis Laurie Ann Ximenez-Fyvie,
J Clin Periodontol 2006; 33: 869 877 doi: 10.1111/j.1600-051X.2006.01006.x Subgingival microbiota of periodontally untreated Mexican subjects with generalized aggressive periodontitis Laurie Ann Ximenez-Fyvie,
An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments
 An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments Reiner Mengel, Dr med dent, DDS*/Christian-Eiben Buns, Dr med dent, DDS*/ Claudia Mengel, Dr med dent, DDS*/ Lavin Flores-de-Jacoby,
An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments Reiner Mengel, Dr med dent, DDS*/Christian-Eiben Buns, Dr med dent, DDS*/ Claudia Mengel, Dr med dent, DDS*/ Lavin Flores-de-Jacoby,
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Over the last decades, the use
 LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
LITERATURE REVIEW Splinting Osseointegrated Implants and Natural Teeth in Partially Edentulous Patients: A Systematic Review of the Literature Anastasios Mamalis, DDS, MBA, MSc, PhD 1 Kleopatra Markopoulou,
Current Health Sciences Journal Vol. 36, No. 3, 2010
 Update Periimplantitis. Aetiology, diagnosis, treatment. A review from the literature F. BOBIA (1), R. V. POP (2) (1) Department of Removable Dental Prosthesis, Faculty of Dentistry, UMF Craiova; (2) Privat
Update Periimplantitis. Aetiology, diagnosis, treatment. A review from the literature F. BOBIA (1), R. V. POP (2) (1) Department of Removable Dental Prosthesis, Faculty of Dentistry, UMF Craiova; (2) Privat
Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study
 G. Charalampakis Å. Leonhardt P. Rabe G. Dahlén Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study Authors affiliations: G. Charalampakis, G. Dahlén,
G. Charalampakis Å. Leonhardt P. Rabe G. Dahlén Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study Authors affiliations: G. Charalampakis, G. Dahlén,
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
JOMI on CD-ROM, 1990 Mar ( ): The Applicability of Osseointegrated Oral Imp
 The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
The Applicability of Osseointegrated Oral Implants in the Rehabilitation of Partial Edentulism: A Prospective Multicenter Study on 558 Fixtures Daniel van Steenberghe, MD, PhD/Ulf Lekholm, DDS, PhD/Charles
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Biomedical engineering of dental implant infections
 J. Acad. Indus. Res. Vol. 1(5) October 2012 227 REVIEW ARTICLE ISSN: 2278-5213 Biomedical engineering of dental implant infections A.C. Mongra Dept. of Biomedical Engineering, Adesh Institute of Engineering
J. Acad. Indus. Res. Vol. 1(5) October 2012 227 REVIEW ARTICLE ISSN: 2278-5213 Biomedical engineering of dental implant infections A.C. Mongra Dept. of Biomedical Engineering, Adesh Institute of Engineering
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation
 The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps
 CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
CLINICAL AND RESEARCH REPORTS Developing Keratinized Mucosa Around Nonsubmerged Dental Implants. Part I: The Use of Vascularized Flaps Jay R. Beagle Despite the continued debate regarding the need for
University of Groningen. Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees
 University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
University of Groningen Two-stage dental implants inserted in a one-stage procedure Heijdenrijk, Kees IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
The International Journal of Periodontics & Restorative Dentistry 827 Thirty-Two Year Success of Dental Implants in Periodontally Compromised Dentition Thomas J. Balshi, DDS, PhD, FACP 1 Glenn J. Wolfinger,
Clinical and morphological aspects of the implant/soft tissue interface
 Clinical and morphological aspects of the implant/soft tissue interface Rodrigo F. Neiva, DDS, a Kathleen G. Neiva, DDS, b Tae-Ju Oh, DDS, MS, a and Hom-Lay Wang, DDS, MSD a a Department of Periodontics/Prevention/Geriatrics,
Clinical and morphological aspects of the implant/soft tissue interface Rodrigo F. Neiva, DDS, a Kathleen G. Neiva, DDS, b Tae-Ju Oh, DDS, MS, a and Hom-Lay Wang, DDS, MSD a a Department of Periodontics/Prevention/Geriatrics,
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
The International Journal of Periodontics & Restorative Dentistry 3 Influence of the 3-D Bone-to-Implant Relationship on Esthetics Ueli Grunder, DMD* Stefano Gracis, DMD** Matteo Capelli, DMD** There are
A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY
 A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY INTRODUCTION Marginal periodontium is the seat of acute and chronic diseases that pose a particular problem in general
A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY INTRODUCTION Marginal periodontium is the seat of acute and chronic diseases that pose a particular problem in general
Short-term evaluation of dental implants in a diabetic population: an in vivo study
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.3.134 Short-term evaluation of dental implants in a diabetic population: an in vivo study Athiban Inbarajan*, MDS, Padmanabhan Thallam Veeravalli,
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.3.134 Short-term evaluation of dental implants in a diabetic population: an in vivo study Athiban Inbarajan*, MDS, Padmanabhan Thallam Veeravalli,
Overview of Periodontics for the General Practicioner
 Overview of Periodontics for the General Practicioner Nashville Area Dental Continuing Education August 27, 2008 Phillip D. Woods, DDS, MPH Commander, USPHS BOP National Periodontal Consultant Diplomate,
Overview of Periodontics for the General Practicioner Nashville Area Dental Continuing Education August 27, 2008 Phillip D. Woods, DDS, MPH Commander, USPHS BOP National Periodontal Consultant Diplomate,
