ORIGINAL ARTICLE. Transport Osteogenesis in the Maxillofacial Skeleton. Outcomes of a Versatile Reconstruction Method Following Tumor Ablation
|
|
|
- Conrad Stewart
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Transport Osteogenesis in the Maxillofacial Skeleton Outcomes of a Versatile Reconstruction Method Following Tumor Ablation Raúl González-García, MD; Luis Naval-Gías, MD, DMD, PhD Objectives: To report our clinical experience using bifocal distraction osteogenesis (BDO) with internal devices to treat patients having bony defects of the maxillofacial skeleton following tumor ablation and to focus on outcomes of dental implant placement in patients having maxillomandibular segmental defects. Design: Retrospective case series. Setting: Academic research. Patients: Patients were selected according to the following inclusion criteria: a bony defect in the maxillofacial skeleton, moderate soft-tissue defect, local or general conditions that preclude more aggressive surgery, and adequate patient compliance. Types of BDO included horizontal mandibular or maxillar alveolar, bilateral alveolar, vertical mandibular or maxillar, ramus and body, mandibular angle, symphysis, the 2-step procedure, temporalis muscle flap reconstruction, vascularized free fibular flap reconstruction, radial forearm free-flap reconstruction, and pectoralis muscle flap reconstruction. Main Outcome Measures: The latency period was 10 days, after which distraction was initiated at a rate of 0.5 mm/d. The distraction period continued until the transport disk reached the distal stump. The consolidation period ranged from 8 to 48 weeks. Seven patients required additional bone grafting to complete union with the residual bone. Results: Twenty-eight patients having bony defects of the maxillofacial skeleton underwent BDO. The mean (SD) bony defect length was 47.0 (20.1) mm. The mean (SD) distracted bone lengthening was 36.5 (20.0) mm, with a mean (SD) consolidation period of 16.4 (8.0) weeks. The bony defect involved the hemimandibular body in 12 patients, with greater involvement of the body and symphysis in 4 patients and of the bilateral mandibular body in 2 patients. Complications after BDO included the following: discomfort in 8 patients, complete intraoral exposure and infection in 3 patients, partial cutaneous exposure in 1 patient, premature consolidation in 1 patient, and temporomandibular joint ankylosis in 1 patient. Overall, BDO for reconstruction of bony defects was successful in 22 patients and failed in 6 patients. At the end of the follow-up period, 11 patients had undergone endosseous dental implant placement. Conclusions: Bifocal distraction osteogenesis potentially benefits patients with bony defects following tumor ablation at various locations in the maxillofacial skeleton. Sufficient bone is gained to allow dental implant placement, an important functional outcome. Arch Otolaryngol Head Neck Surg. 2010;136(3): Author Affiliations: Departments of Oral and Maxillofacial Head and Neck Surgery, University Hospital Infanta Cristina, Badajoz (Dr González-García), and University Hospital La Princesa, Madrid (Dr Naval-Gías), Spain. SINCE FIRST DESCRIBED BY McCarthy et al 1 in 1992, distraction osteogenesis (DO) of craniofacial bones has increasingly become a mainstay in bone regeneration. In patients having bony defects of the maxillofacial skeleton after tumor ablation, bifocal DO (BDO) allows regeneration of loosened bone following osteotomy and gradual separation of bony fragments. Distraction osteogenesis for reconstruction of segmental mandibular defects has been previously described. 2,3 The use of microvascular free flaps has been successful for reconstruction of large segmental mandibular defects. 4 A vascularized free-fibular flap (VFFF) aids in reconstructing bone and soft tissue in most adult patients undergoing mandible ablation in a single setting. However, the following 2 conditions preclude the use of mandibular BDO, despite the availability of a composite microvascular free flap: (1) patients with increased surgical risk who are unsuitable for prolonged surgical time or for more aggressive surgical procedures and (2) patients who require improved alveolar softtissue quality before endosseous dental implant placement. Bifocal DO allows reconstruction of segmental bony defects with an alveolar height that closely mimics the native mandible. It also provides attached gingiva that resemble the original. This is of utmost importance, as overlying soft tissue is often too thick following microvascular free-flap reconstruction, leading to unfavorable dental implant placement and maintenance because of the absence of attached gingiva. Most mandibular defects or other defects involving the maxillofacial skeleton require reconstruction of bone and sur- 243
2 Table 1. Patient Sex, Age, Primary and Secondary Diagnoses, and Local and Cervical Treatments Patient/Sex/ Age, y Primary Diagnosis Defect Location Local Treatment 1/F/70 SCC Palate Bone and soft-tissue resection, temporalis muscle Cervical Treatment Yes Oroantral fistula Secondary Diagnosis 2/F/36 Giant cell granuloma Mandible Bone and soft-tissue resection No... 3/F/50 SCC Maxilla Bone and soft-tissue resection Yes Oroantral fistula 4/M/33 Sarcoma Maxilla Bone and soft-tissue resection, VFFF Yes Oroantral fistula 5/F/62 SCC Base of tongue Soft-tissue resection, RFFF Yes Radionecrosis 6/M/53 SCC Floor of mouth Bone and soft-tissue resection, VFFF Yes VFFF lost 7/M/74 SCC Mandible Pectoralis muscle and bridging plate, BDO Yes... 8/M/76 Giant cell granuloma Maxilla 2 Alveolar BDO No Oroantral fistula 9/F/42 Ameloblastoma Mandible Bone and soft-tissue resection No... 10/F/60 Meningioma Skull Bone and soft-tissue resection No Soft-tissue or hard-tissue defects 11/M/17 Cleft palate Maxilla... No Soft-tissue or hard-tissue defects 12/M/67 SCC Floor of mouth Soft-tissue resection, VFFF twice Yes Second malignant neoplasm 13/F/78 SCC Floor of mouth Soft-tissue resection Yes Soft-tissue or hard-tissue defects 14/M/48 SCC Oropharynx (tonsil) Bone and soft-tissue resection Yes... 15/F/50 Leiomyosarcoma Mandible Bone and soft-tissue resection No Soft-tissue or hard-tissue defects, relapse 16/M/66 SCC Oropharynx (tonsil) Bone and soft-tissue resection, Yes Radionecrosis pectoralis flap 17/M/80 SCC Floor of mouth Bone and soft-tissue resection Yes Radionecrosis 18/M/69 Mucoepidermoid Retromolar trigone Bone resection, RFFF No... carcinoma 19/F/47 SCC Floor of mouth Bone and soft-tissue resection, VFFF Yes Second malignant neoplasm 20/F/53 Ameloblastoma Mandible Bone and soft-tissue resection, VFFF No... 21/F/48 SCC Hypopharynx RT, QT No Radionecrosis 22/M/49 SCC Mandible Bone resection, VFFF Yes Radionecrosis 23/M/14 Giant cell granuloma Mandible Bone resection, vertical alveolar BDO Yes Relapse 24/M/45 SCC Floor of mouth RT, QT No Radionecrosis 25/F/35 Periimplantitis Mandible... No... 26/M/32 Cleft palate Maxilla... No... 27/F/36 Odontogenic myxoma Mandible Bone resection, VFFF No VFFF lost 28/M/60 SCC Mandible... Yes Radionecrosis Abbreviations: BDO, bifocal distraction osteogenesis; ellipsis, not applicable; QT, chemotherapy; RFFF, radial forearm free flap; RT, radiation therapy; SCC, squamous cell carcinoma; VFFF, vascularized free-fibular flap. rounding soft tissue, for which BDO and VFFF reconstruction are effective. A previous study 3 focused on patients with adequate compliance and limited soft-tissue defects for inclusion in a distraction osteogenesis protocol. However, few investigators have reported patient inclusion criteria for various types of reconstruction; therefore, controversy exists about reconstruction of the mandible and other craniofacial bone defects. In the present study, we report our clinical experience usingbdowithinternaldevicestotreatpatientshavingbony defects of the maxillofacial skeleton following tumor ablation. We also evaluated the outcomes of endosseous dental implant placement as ideal restorative treatment. METHODS Patients treated from January 1, 2006, to December 31, 2008, were retrospectively evaluated and were selected according to the following inclusion criteria: (1) bony defect in the maxillofacial skeleton, (2) moderate soft-tissue defect, (3) local or general conditions that preclude more aggressive surgery, and (4) adequate patient compliance. Bone transport was used to reconstruct defects in all patients. The following clinical and treatment data were examined: sex, age, primary and secondary diagnoses, defect location and length, transport disk length, distracted bone lengthening, consolidation period, device location, number of devices, macroscopic quality of newly generated bone, radiation therapy before BDO, complications, success rate, follow-up period, bone grafting, and dental implant placement. Primarydiagnosesincludedsquamouscellcarcinoma, giantcell granuloma, odontogenic myxoma, ameloblastoma, sarcoma, leiomyosarcoma, mucoepidermoidcarcinoma, cleftpalate, periimplantitis, and meningioma (Table 1). Secondary diagnoses included VFFFreconstructionfailure, oroantralfistula, soft-tissueandhardtissue defects, radionecrosis, and recurrence of second malignant neoplasm. In all patients, computed tomography was performed beforesurgerytodeterminetheextentofthedefectandtheinvolvement of surrounding tissue. Panoramic radiographs were obtained monthly during the distraction and consolidation periods to evaluatetheprogressofbdoandtodeterminethevectorofthedistracted transport disk. Types of BDO included horizontal mandibular or maxillar alveolar, bilateral alveolar, vertical mandibular or maxillar, ramusandbody, mandibularangle, symphysis, the2-stepprocedure, temporalis muscle flap reconstruction, VFFF reconstruction, radial forearm free-flap reconstruction, and pectoralis muscle flap reconstruction. During the procedure, periosteum over the designed transport disk was preserved to ensure its vascularity. In 1 patient, periosteum or dura matter was preserved at the opposite side of the transported bone. An osteotomy was performed at a variable distance from the defect to create the transport disk. To create new bone in the gap, we used 2 types of unidirectional distraction devices (CranimaxillofacialDistractionSystem; SynthesInc, WestChester, Pennsylvania; and Modus MDO 1.5; Medartis AG, Basel, Switzer- 244
3 land). The movable part of the distraction device was fixed to the transport disk by 2 bicortical 10-mm to 14-mm screws. Two additional bicortical screws fixed the device to the residual bone. After verifying the mobility of the distractor, the device was returned to its original position with the distractor activator placed intraorally or percutaneously. Some challenging cases (eg, patient 4 in Table 1 with sarcoma of the maxilla and failure of VFFF reconstruction) required the use of a stereolithographic model before surgery to design adequate positioning of the BDO device (Figure 1). The distraction device allowed maximal distracted bone lengthening to 40 mm. For this reason, the following patients required 2 consecutive distraction devices at the same site: (1) patient 11 with an 80-mm calvarial defect, (2) patient 16 with an 80-mm mandibular angle defect, and (3) patient 19 with a 50-mm parasymphyseal defect. The following additional patients underwent reconstruction with 2 devices at 2 different sites: (1) patient 2 with a 70-mm left mandibular body and symphyseal defect; (2) patient 7 with an 80-mm mandibular body and symphyseal defect; (3) patient 9 with a 45-mm lateromaxillary defect; (4) patient 12 with a 20-mm premaxillary defect; (5) patient 18 with a 30-mm right mandibular body and a 40-mm left mandibular angle defect; and (6) patient 21 with right 25-mm and left 26-mm mandibular angle defects. The following patients required the use of 2 simultaneous distraction devices at the same site to achieve adequate bone outcome, followed by the use of 2 other distraction devices because of the presence of defects larger than 40 mm: (1) patient 5 with a 60-mm premaxillary defect, and (2) patient 23 with a 45-mm mandibular body defect. The latency period was 10 days, after which distraction was initiated at a rate of 0.5 mm/d. The distraction period continued until the transport disk reached the distal stump. The consolidation period ranged from 8 to 48 weeks. Seven patients required additional bone grafting to complete union with the residual bone as follows: (1) anteroiliac crest in patients 4, 5, and 18, (2) posteroiliac crest in patient 6 and patient 20, (3) mandibular ramus in patient 2, and (4) rib in patient 23. A VFFF was used in patient 13 because of complete failure of BDO. The rest of the patients underwent corticotomy in the distal stump of the transported bone and corticotomy in the residual bone. Both poles were fixed with titanium miniplates or bridging plates. Two patients (patient 14 and patient 16) underwent greenstick fracture at the proximal stump to achieve better curvature of the reconstructed mandible. Commercially available statistical software (SPSS 13.0; SPSS Inc, Chicago, Illinois) was used to analyze descriptive statistics for continuous and categorical variables. Institutional review board approval was obtained for the study. REPORT OF CASES CASE 1 A 36-year-old woman (patient 2) with giant cell granuloma of the left mandibular body and symphysis underwent bone and soft-tissue resection and subsequent reconstruction using 2 horizontal alveolar BDO devices (Figure 2). The defect length was 70 mm. Two 10-mm transport disks were designed, and 2 opposing BDO devices were placed for 60-mm distracted bone lengthening. The consolidation period was 12 weeks, and excellent new bone was observed. Bone graft from the mandibular ramus was used to achieve proper union between the distracted bone segments. Six endosseous dental implants were placed over the distracted bone. Figure 1. Bifocal distraction osteogenesis device in a stereolithographic model. CASE 2 A 66-year-old man (patient 16) with squamous cell carcinoma of the oropharynx underwent bone and softtissue resection and further reconstruction using a pectoralis major pedicled flap (Figure 3). Following radiation therapy, the patient experienced radionecrosis of the mandible, which required segmental mandibulectomy and further reconstruction by BDO of the mandibular body and symphysis for a defect length of 40 mm. After a 12-week consolidation period, greenstick fracture was performed at the distal stump, and union with the remaining bone was fixed using a 2.0-mm titanium miniplate. No complications were observed, and endosseous dental implants were placed in distracted bone. CASE 3 A 42-year-old woman (patient 9) with ameloblastoma of the right mandible underwent bone and soft-tissue reconstruction and subsequent reconstruction using horizontal alveolar BDO (Figure 3). A 30-mm defect was present. An 8-mm transport disk was designed to create a 25-mm bone segment. The consolidation period was 12 weeks, and excellent new bone was observed. No additional bone grafting was necessary. Subsequent restoration was achieved using 3 endosseous dental implants. RESULTS Twenty-eight patients having bony defects of the maxillofacial skeleton underwent BDO. Fifteen patients were male, and 13 patients were female, with a mean (SD) age of (17.46) years (age range, years). Primary diagnoses included the following: (1) squamous cell carcinoma in 15 patients; (2) giant cell granuloma in 3 patients; (3) ameloblastoma and cleft palate in 2 patients each; and (4) odontogenic myxoma, leiomyosarcoma, meningioma, mucoepidermoid carcinoma, sarcoma, and periimplantitis in 1 patient each. The primary defect location 245
4 A B C D E Figure 2. Patient 2. A, Panoramic radiography showing a bony defect following resection of mandibular giant cell granuloma. B, Intraoperative view during insertion of a bifocal distraction osteogenesis (BDO) device. C, Panoramic radiography showing bone transport with 2 BDO devices. D, Panoramic radiography showing placement of 6 endosseous dental implants over distracted bone. E, Intraoperative view of placed dental implants. A B C Figure 3. Panoramic radiography of patient 16. A, Beginning of bifocal distraction osteogenesis. B, End of distraction phase. C, Union of distal stump by greenstick fracture and a titanium miniplate and insertion of endosseous dental implants in distracted bone. was the mandibular gingiva in 10 patients, floor of the mouth in 6 patients, maxilla in 5 patients, oropharynx in 2 patients, and skull, palate, retromolar trigone, base of tongue, and hypopharynx in 1 patient each. Local treatment of the primary defect consisted of the following: (1) bone and soft-tissue resection plus direct closure in 7 patients; (2) bone and soft-tissue resection plus VFFF reconstruction in 7 patients; (3) soft-tissue resection plus radial forearm free-flap reconstruction in 2 patients; (4) chemoradiotherapy in 2 patients; and (5) combinations of bone or soft-tissue resection plus pectoralis muscle flap, temporalis muscle flap, and bridging plates in the rest of the patients. Fifteen patients underwent modified type III radical neck dissection (Table 1). As adjuvant treatment following the first intervention, 12 patients underwent postoperative radiation therapy before BDO (mean [SD] ra- 246
5 Table 2. BDO Treatment, Defect Length and Location, Transport Disk Length, Distracted Bone Lengthening, Consolidation Period, Device Location and Number, and Macroscopic Quality of Newly Generated Bone Defect Length, mm Transport Disk Length, mm Distracted Bone Lengthening, mm Consolidation Period, wk Macroscopic Quality of Newly Generated Bone Patient BDO Treatment Defect Location Device Location No. of Devices 1 Horizontal alveolar... R mandible Palate 1 Twice Failure 2 Horizontal alveolar 70 L mandible BS L mandible BS 2 Excellent twice (alveolar) 3 Horizontal alveolar 25 Mandible R mandible 1 Excellent 4 Bilateral alveolar 60 R premaxilla 8 20, R and L mandible 2 Twice Good 2 steps twice 5 HBO 40 R mandible angle Symphysis, skin 1 Good 80 Mandible BS 15 17, Gonial angle 2 Good 6 Bilateral from mandible, HBO, bridging plate 7 Mandible 50 R mandible body Symphysis 1 Good 8 Maxilla twice 45 Premaxilla, 12 20, Lateromaxilla 2 Good lateromaxilla 9 Horizontal 30 R mandible body R mandible body 1 Excellent (alveolar) 10 Horizontal 2 steps 80 Calvarial parietofrontal , 12 Calvarial 1 Twice Excellent 11 Mandible twice 20 Premaxilla 8 15, 7 12 Maxilla 2 Good 12 Mandible 46 Hemimandible BS Gonial angle 1 Failure 13 RFFF 59 Hemimandible body Parasymphyseal 1 Good, but BDO not completed 14 VFFF for chin 37 Hemimandible body Body 1 Excellent project 15 VFFF second 80 Hemimandible body in each Gonial angle 1 Twice Excellent period 16 Ramus body, gonial 40 Hemimandible BS Parasymphyseal 1 Excellent 17 Mandible angle 80 R premolar region, R 29, L 7 R 30, L R mandible body, 2 Good twice L mandible A L mandible angle 18 Symphysis 2 steps 50 Hemimandible body Parasymphyseal 1 Twice Excellent 19 Temporalis flap 34 Hemimandible body Gonial angle 1 Good 20 Gonial twice R 25, L 26 Bilateral mandible R 15, L 16 R 35, L Gonial angle 2 Good body 21 RFFF 30 Hemimandible body Gonial angle 1 Good 22 2 Steps twice... R and L mandible 15 R 5, L Mandible body 2 Twice Moderate body 23 Vertical 20 Symphysis (alveolar) 5 20 Premature Symphysis 1 Excellent 24 Horizontal, HBO 40 R mandible body Symphysis 1 Poor 25 Vertical... Symphysis (alveolar) Symphysis 1... (alveolar) 26 Vertical twice 20 Premaxilla 5 R 40, L Lateromaxilla 1 Moderate 27 Horizontal... R mandible body R mandible body Horizontal 45 L mandible body L mandible body 1 Moderate Abbreviations: BDO, bifocal distraction osteogenesis; BS, body and symphysis; ellipsis, not applicable; HBO, hyperbaric oxygen therapy; L, left; RFFF, radial forearm free flap; R, right. diation therapy dosage, [3.93] J; range, J) (to convert joules to grays, multiply by 1.0). Secondary diagnoses included the following: (1) radionecrosis in 7 patients, (2) oroantral fistula and residual soft-tissue or hardtissue defects in 4 patients each, (3) relapse or second malignant neoplasm in 3 patients, and (4) loss of VFFF in 2 patients. Eight patients underwent primary BDO without a secondary diagnosis. The mean (SD) follow-up period was (19.86) months (range, 4-60 months). At the end of the follow-up period, 5 patients had died of their disease, 21 patients had no evidence of disease, and 2 patients were alive with disease. The mean (SD) bony defect length was 47.0 (20.1) mm (range, mm). The mean (SD) transport disk length was 13.7 (8.0) mm (range, 4-29 mm). The mean (SD) distracted bone lengthening was 36.5 (20.0) mm (range, mm), with a mean (SD) consolidation period of 16.4 (8.0) weeks (range, 8-48 weeks). The bony defect involved the hemimandibular body in 12 patients, with greater involvement of the body and symphysis in 4 patients and of the bilateral mandibular body in 2 patients. Two patients had mandibular symphyseal region involvement, and 1 patient had mandibular angle involvement. Three patients had premaxilla involvement, and 1 patient had premaxilla and lateromaxilla involvement. One patient had a parietofrontal calvarial defect (Table 2). Various BDO device locations were chosen relative to the bony defect. The most frequent transcu- 247
6 Table 3. Radiation Therapy Before BDO, Complications, Success, Patient Status, Bone Grafting and Donor Site, and Dental Implant Placement and Number Radiation Therapy Patient Before BDO Complications Success Follow-up Since Resection, mo Patient Evolution Bone Grafting Bone Grafting Donor Site Dental Implant Placement No. of Dental Implants 1 Yes Screws loosening No 36 NED No... No... 2 No Discomfort, vector problems Yes 48 NED Yes Ramus Yes 6 3 No Discomfort Yes 48 SCC recurrence No... No (scarce... bone) 4 Yes Discomfort, vector problems Yes 48 NED Yes Anteroiliac crest Yes 3 5 Yes No Yes 48 NED Yes Anteroiliac crest No... 6 Yes Lost dental implants, soft-tissue sequelae Yes 48 NED Yes Posteroiliac crest Yes 8 (Lost 5 dental implants) 7 No No Yes 6 NED No... Yes 5 8 No No Yes 12 NED No... Yes 5 9 No Discomfort Yes 36 NED No... Yes 3 10 No No Yes 60 NED No... No No Discomfort, vector problems Yes... NED No... No Yes, 64 J Complete intraoral exposure, No 15, Dead DOD No... No... infection 13 No Distant metastases, bad general status, BDO not completed No 4, Dead DOD No... No Yes, 60 J MIO decreased, temporomandibular joint ankylosis Yes 60 SCC recurrence No, greenstick fracture at proximal stump... Yes 5 Yes 60 NED No... Yes 6 15 No Pain at end of BDO period, slight asymmetry 16 Yes, 60 J No Yes 60 NED No, greenstick fracture at proximal stump... Yes 5 17 Yes, 62 J No Yes Dead NED No... No No No Yes 60 NED Yes Anteroiliac crest No Yes, 60 J Complete intraoral exposure, No Dead SCC recurrence, No... No... infection, submental abscess, fistulae DOD 20 No Pain at end of BDO period, Yes Resection elsewhere NED Yes Posteroiliac Yes 5 slight asymmetry 20 y previously crest 21 Yes, 70 J Partial cutaneous exposure, Yes 15 NED No... No... right hemimandibular body 22 Yes Discomfort, dyspnea Yes 36 NED Yes Rib No Premature consolidation No 24 NED No... No Yes Aesthetic complaint Yes 60 NED No... No No Complete intraoral exposure, No... NED No... No... infection 26 No Discomfort, vector problems Yes... NED No... No No No Yes 60 NED No... No Yes Discomfort Yes 60 NED No... No... Abbreviations: BDO, bifocal distraction osteogenesis; DOD, died of disease; ellipsis, not applicable; MIO, maximal interincisional opening; NED, no evidence of disease; SCC, squamous cell carcinoma. SI conversion factor: To convert joules to grays, multiply by 1.0. taneous locations for the device were the gonial region (6 patients) and the symphyseal-parasymphyseal region (8 patients). Other intraoral locations allowed more favorable manipulation of the device, including the lateromaxilla (5 patients) and the mandibular body (5 patients). Six patients required 2 BDO devices. The overall success rate of BDO in the series was 79% (22 of 28 patients). Bone formation failed to occur in 6 patients with complete intraoral exposure and infection, screw loosening, or poor general health. According to surgical findings after the distraction period, newly generated bone was macroscopically good or excellent in 20 patients and poor or moderate in 6 patients. Seven patients required additional bone grafting to complete union between the distal stump and the distracted bone. The rest of the patients underwent corticotomy in the distal stump of the distracted bone and corticotomy in the residual bone. Both poles were fixed with miniplates or bridging plates (Table 3). Complications after BDO included the following: (1) discomfort in 8 patients, (2) complete intraoral exposure and infection in 3 patients, (3) partial cutaneous ex- 248
7 posure in 1 patient, (4) premature consolidation in 1 patient, and (5) temporomandibular joint ankylosis in 1 patient. Overall, BDO for reconstruction of bony defects was successful in 22 patients and failed in 6 patients. At the end of the follow-up period, 46 endosseous dental implants (MG Osseous; Mozo-Grau SL, Valladolid, Spain) had been placed over distracted mandible or maxilla in 11 patients (Table 3). COMMENT Several studies 1-4 have focused on the possibility of reliable segmental mandibular reconstruction following tumor ablation. Because some patients undergo BDO as a secondary procedure, reconstructive goals in terms of function and aesthetics are of utmost importance. Adequate masticatory function is desirable. As previously noted by Costantino et al, 4 the diameter of newly generated bone is similar to that of the residual mandible and transport disk. Moreover, the inferior alveolar nerve and artery are recannulated in most cases. 5 These conditions favor placement of an ulterior endosseous dental implant, which may lead to better results in terms of function. In the present series, BDO was usually performed as a secondary procedure following severe complications or failure of the first treatment. Reconstruction using the VFFF was performed in defects involving the mandible (6 patients) and the maxilla (1 patient). Two patients with segmental mandibular defects experienced failure of the VFFF, while the patient with a defect of the maxilla developed an oroantral fistula. Mandibular osteoradionecrosis and development of a second malignant neoplasm occurred in the rest of the patients. Therefore, BDO was performed as secondary surgical treatment for these patients with recalcitrant disease. Consideration of BDO as a secondary choice in healthy patients avoids controversy about the use of BDO vs a vascularized freeosseous flap for maxillomandibular reconstruction. In patients who are not candidates for more aggressive surgery or prolonged surgical time because of poor general health, BDO is an appropriate primary surgical treatment. Poor peripheral vascularization of the lower part of the leg was bilaterally present in 2 of our patients with VFFF failure. In such patients, mandibular BDO is our preferred treatment option primarily and secondarily. Seven patients required additional bone grafting to fill the gap between the distracted bone and the distal stump. This is controversial, as the main criticism would be that the minimal benefit of BDO in ulterior bone grafting was necessary. In fact, the distraction device should apply compression forces at the docking sites to achieve fusion with the residual distal skeleton stump, although this is not always possible. We advocate BDO because the needed additional small bone graft is often much smaller than the one required if BDO is not used. Moreover, soft tissue is accordingly expanded. In our series, the mean defect length was 10 mm longer than the mean distracted bone lengthening. This was remedied by the use of additional bone grafting in selected patients. In most patients, bone grafting material was harvested from the anteroiliac or posteroiliac crest, which is a safe and easy donor site. In more than two-thirds of patients, bone grafting was unnecessary, and direct union between bone poles was achieved following corticotomy and plate fixation. Few studies have evaluated the role of adjuvant radiation therapy before BDO relative to distraction outcomes. A previous study 3 among 7 patients found 6 patients (85.7%) having successful DO following postoperative radiation therapy, in accord with the findings of other authors among smaller samples. 6,7 In the present series, 12 of 28 patients received adjuvant postoperative radiation therapy before BDO. Ten of 12 patients (83.3%) had successful BDO. Because more patients in our study received radiation therapy, this value is more accurate than previously published BDO success rates. However, outcomes among patients who received radiation therapy were poorer than those among patients who did not receive radiation therapy. For patients undergoing radiation therapy, the transport disk was designed to be as far as possible from the maximum dosage point in the radiation field, and the consolidation period was doubled. By using BDO in patients receiving radiation therapy, necrotic bone was eliminated, and soft tissue was expanded. We also eliminated associated fistulae and generated sufficient healthy bone to assure a bridging plate to improve facial symmetry and patient quality of life. All patients who underwent radiation therapy received high dosages of irradiation up to 70 J in accord with standard adjuvant treatment for head and neck cancer. Even with high irradiation dosages, at least 3 of 4 patients receiving radiation therapy will undergo successful BDO following maxillomandibular segmental resection. Thirty-six internal devices were used in the entire series, 8 of them consecutively. In 14 of 28 patients (50.0%), the activator of the device was located transcutaneously. The external activator of these semiburied devices allowed easier access for activation. Previously, decreased infection and dehiscence with this type of access was observed because an intraoral approach is avoided. 3 However, 10 of 28 patients (35.7%) with defects of the lateromaxilla or mandibular body required intraoral devices. Because the mean defect length was 47.0 mm for the entire series, 8 of 28 patients (28.6%) required 2 BDO devices placed simultaneously or in consecutive steps. The distractor used in this study achieves maximal distracted bone lengthening of 40 mm. Although other distraction devices allow longer distractions such as 50 mm, 8 the shorter BDO devices used in the present series allowed better control of the distraction vector. In fact, the direction traversed by the transport disk after initial osteotomy may cause inferior results, as it tends to move parallel to the proximal segment of the residual bone, and greenstick fracture osteotomy following distractor removal may be necessary to reproduce the curvature of the mandible or maxilla in some patients. Slight changes in the distraction vector following the first distraction step may be useful to replicate adequate maxillomandibular curvature and remedy this complication. Consequently, we prefer shorter devices over more complicated systems such as the use of a traction wire plus a bridging reconstruction plate and bracket with miniplates for fixing the transport disk. 9 Overall, BDO success with adequate bone formation was observed in 22 of 28 patients in our series. Good or 249
8 excellent bone quality was macroscopically observed in 20 of 28 patients (71.4%). These results seem acceptable for a procedure that is a secondary reconstruction option in many patients in whom VFFF reconstruction has failed. To achieve better functional outcome, 11 of 28 patients (39.3%) underwent endosseous dental implant placement. A total of 46 dental implants were placed, with an overall dental implant success rate of 89.1% (41 of 46 dental implants). All failed dental implants were observed in 1 patient with previous VFFF loss, softtissue sequelae, and intraoral exposure of distracted bone. Bifocal DO allows reconstruction of the defect with an alveolar height that closely mimics the native mandible, with the advantage of a near-original attached gingiva. In contrast, the overlying soft tissue of microvascular free flaps is often thick, and dental implant placement is less favorable because of the absence of attached gingiva. Complications were common. The most frequent complaint was discomfort by 8 patients. This was not secondary to pain during distraction, which was present in only 2 patients at the end of the distraction period. Discomfort was reported by 5 patients with an intraoral activator placed in the maxilla and by 3 patients with the activator placed in the mandibular body. This represents interference with the normal surrounding soft tissue such as the cheeks or lips. Discomfort was absent when the activator was placed externally, but this was socially more disturbing. The primary cause of poor final results was complete intraoral exposure and infection, which were observed in 3 patients with complete failure of the distraction procedure. The overall success rate of BDO was 79% (22 of 28 patients), and surgeons must expect a potential 20% failure rate despite rigorous patient selection and adequate BDO protocol. In summary, BDO is of potential benefit for patients with bony defects following tumor ablation at various locations in the maxillofacial skeleton. It is useful for treating patients who are unsuitable for more aggressive surgery or prolonged surgical time because of poor general health or for patients in whom primary treatment using a vascularized free-osseous flap has failed. Bifocal DO is a reliable tool to gain sufficient bone to allow dental implant placement, an important functional outcome. Submitted for Publication: March 23, 2009; final revision received September 14, 2009; accepted September 29, Correspondence: Raúl González-García, MD, Calle Los Yébenes 35, 8C, 28047, Madrid, Spain (raulmaxilo@gmail.com). Author Contributions: Dr González-García had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: González-García. Acquisition of data: Naval-Gías. Analysis and interpretation of data: González-García. Drafting of the manuscript: González-García. Critical revision of the manuscript for important intellectual content: Naval-Gías. Statistical analysis: González-García. Study supervision: Naval-Gías. Financial Disclosure: None reported. REFERENCES 1. McCarthy JG, Schreiber J, Karp N, Thorne CH, Grayson BH. Lengthening the human mandible by gradual distraction. Plast Reconstr Surg. 1992;89(1): Block MS, Otten J, McLaurin D, Zoldos J. Bifocal distraction osteogenesis for mandibular defect healing: case reports. J Oral Maxillofac Surg. 1996;54(11): González-Garcia R, Rubio-Bueno P, Naval-Gías L, et al. Internal distraction osteogenesis in mandibular reconstruction: clinical experience in 10 cases. Plast Reconstr Surg. 2008;121(2): Costantino PD, Shybut G, Friedman CD, et al. Segmental mandibular regeneration by distraction osteogenesis: an experimental study. Arch Otolaryngol Head Neck Surg. 1990;116(5): Karaharju-Suvanto T, Karaharju EO, Ranta R. Mandibular distraction: an experimental study in sheep. J Craniomaxillofac Surg. 1990;18(6): Sawaki Y, Hagino H, Yamamoto H, Ueda M. Trifocal distraction osteogenesis for segmental mandibular defect: a technical innovation. J Craniomaxillofac Surg. 1997; 25(6): Herford AS. Use of plate-guided distraction device for transport distraction osteogenesis of the mandible. J Oral Maxillofac Surg. 2004;62(4): Muraki Y, Tominaga K, Yoshioka I, et al. Mandibular reconstruction with bone transport in a patient with osteogenesis imperfecta. Int J Oral Maxillofac Surg. 2008; 37(9): Hibi H, Ueda M. New internal transport distraction device for reconstructing segmental defects of the mandible. Br J Oral Maxillofac Surg. 2006;44(5):
Intraoral mandibular distraction osteogenesis in facial asymmetry patients with unilateral temporomandibular joint bony ankylosis
 Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Int. J. Oral Maxillofac. Surg. 2002; 31: 544 548 doi:10.1054/ijom.2002.0297, available online at http://www.idealibrary.com on Intraoral mandibular distraction osteogenesis in facial asymmetry patients
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Cover Page The handle http://hdl.handle.net/1887/31632 holds various files of this Leiden University dissertation. Author: Mensink, Gertjan Title: Bilateral sagittal split osteotomy by the splitter-separator
Bifocal distraction osteogenesis as a surgical bed for dental implants in complete maxillo-mandibular defects
 Stomatological Dis Sci 2017;1:62-8 DOI: 10.20517/2573-0002.2016.18 Original Article Stomatological Disease and Science www.sdsjournal.com Open Access Bifocal distraction osteogenesis as a surgical bed
Stomatological Dis Sci 2017;1:62-8 DOI: 10.20517/2573-0002.2016.18 Original Article Stomatological Disease and Science www.sdsjournal.com Open Access Bifocal distraction osteogenesis as a surgical bed
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis CASE REPORT
 Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Reconstruction of the mandible after ablative
 Scientific Foundations Experimental Mandibular Regeneration by Distraction Osteogenesis with Submerged Devices: Preliminary Results of A Canine Model Pilar Rubio-Bueno, MD, PhD* Fidel Sanromán, MD, DVM,
Scientific Foundations Experimental Mandibular Regeneration by Distraction Osteogenesis with Submerged Devices: Preliminary Results of A Canine Model Pilar Rubio-Bueno, MD, PhD* Fidel Sanromán, MD, DVM,
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Treatment of Mandibular Asymmetry by Distraction Osteogenesis and Orthodontics: A Report of Four Cases
 Case Report Treatment of Mandibular Asymmetry by Distraction Osteogenesis and Orthodontics: A Report of Four Cases Azita Tehranchi, DMD a ; Hossein Behnia, DMD b Abstract: Distraction osteogenesis devices
Case Report Treatment of Mandibular Asymmetry by Distraction Osteogenesis and Orthodontics: A Report of Four Cases Azita Tehranchi, DMD a ; Hossein Behnia, DMD b Abstract: Distraction osteogenesis devices
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
GENERAL DISCUSSION & SUMMARY
 GENERAL 9 DISCUSSION & SUMMARY 139 140 Chapter 9 The aim of this thesis was to investigate problems, obstacles, and complications arising from treatment using mandibular DO. Further specification for various
GENERAL 9 DISCUSSION & SUMMARY 139 140 Chapter 9 The aim of this thesis was to investigate problems, obstacles, and complications arising from treatment using mandibular DO. Further specification for various
DISTRACTION PRODUCT OVERVIEW. For a wide variety of facial applications
 DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
DISTRACTION PRODUCT OVERVIEW For a wide variety of facial applications DISTRACTION PRODUCT OVERVIEW. STRONG, MODULAR, VERSATILE CRANIOFACIAL DISTRACTION External Midface Distractor Distraction of the maxilla,
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS. FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy
 MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
MORPHOFUNCTIONAL APPROACH TO TREAT TMJ ANKYLOSIS RESECTION OF TMJ ANKYLOSIS FACIAL ASYMMETRY CORRECTION Prof. Dr. Dr. Srinivas Gosla Reddy MBBS MDS FDSRCS (Edin) FDSRCS (Eng) PhD Dr. Dr. Rajgopal Reddy
Surgery in Head and neck cancers.principles. Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer
 Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
Surgery in Head and neck cancers.principles Dr Diptendra K Sarkar MS,DNB,FRCS Consultant surgeon,ipgmer Email:diptendrasarkar@yahoo.co.in HNC : common inclusives Challenges Anatomical preservation R0 Surgical
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Case Reports Pediatric Mandibular Distraction Osteogenesis: The Present and the Future
 Case Reports Pediatric Mandibular Distraction Osteogenesis: The Present and the Future Samuel T. Rhee, MD, and Steven R. Buchman, MD Ann Arbor, Michigan Pediatric mandibular distraction osteogenesis (MDO)
Case Reports Pediatric Mandibular Distraction Osteogenesis: The Present and the Future Samuel T. Rhee, MD, and Steven R. Buchman, MD Ann Arbor, Michigan Pediatric mandibular distraction osteogenesis (MDO)
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
LOGIC SURGICAL TECHNIQUE GUIDE. In d i c at i o n s. Co n t r a i n d i c at i o n s. Mandibular Distraction System
 TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
TM SURGICAL TECHNIQUE GUIDE In d i c at i o n s The OSTEOMED Mandibular Distractor system is indicated for use as a mandibular bone lengthener for patients diagnosed with conditions where treatment includes
In Scandinavia, malignant tumors in the maxillofacial
 Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Oral Implant Rehabilitation in Irradiated Patients Without Adjunctive Hyperbaric Oxygen Gunilla Andersson, DDS, PhD*/Lars Andreasson, MD, PhD**/Göran Bjelkengren, MD*** In 15 patients treated for malignant
Facelift approach for mandibular resection and reconstruction
 ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
ORIGINAL ARTICLE Facelift approach for mandibular resection and reconstruction Bernardo Bianchi, MD, Andrea Ferri, MD, * Silvano Ferrari, MD, Chiara Copelli, MD, Enrico Sesenna, MD Maxillo-Facial Surgery
2018 Dental Code Set For dates of service from 1/1/ /31/2018
 D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
D0120 PERIODIC ORAL EVALUATION - ESTABLISHED PATIENT D0140 LIMITED ORAL EVALUATION - PROBLEM FOCUSED D0150 COMPREHENSIVE ORAL EVALUATION - NEW OR ESTABLISHED PATIENT D0160 DETAILED AND EXTENSIVE ORAL EVALUATION
2018 Dental Code Set
 D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
D0120 D0140 D0150 D0160 D0180 D0210 D0220 D0230 D0240 D0250 D0251 D0270 D0272 D0273 D0274 D0277 D0290 D0310 D0330 D0340 D0350 D0393 D0470 D0502 PERIODIC ORAL EVALUATION ESTABLISHED PATIENT LIMITED ORAL
Reconstruction with fibular osteocutaneous free flap in patients with mandibular osteoradionecrosis
 Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Kim et al. Maxillofacial Plastic and Reconstructive Surgery (2015) 37:7 DOI 10.1186/s40902-015-0007-3 RESEARCH ARTICLE Open Access Reconstruction with fibular osteocutaneous free flap in patients with
Article in press. Distraction Osteogenesis: Role and Clinical Application in the Maxillofacial Region. Case Report
 Case Report Distraction Osteogenesis: Role and Clinical Application in the Maxillofacial Region Thongchai Nuntanaranont 1, Wipapan Ritthagol 2 and Butsakorn Akarawatcharangura 1 1 Department of Oral and
Case Report Distraction Osteogenesis: Role and Clinical Application in the Maxillofacial Region Thongchai Nuntanaranont 1, Wipapan Ritthagol 2 and Butsakorn Akarawatcharangura 1 1 Department of Oral and
Mandibular Reconstruction Using ProPlan CMF: AReview
 THIEME Review Article e35 Mandibular Reconstruction Using ProPlan CMF: AReview Ryo Sasaki, DDS, PhD 1,2 Michael Rasse, MD, DDS, PhD 1 1 Department of Craniomaxillofacial and Oral Surgery, Medical University
THIEME Review Article e35 Mandibular Reconstruction Using ProPlan CMF: AReview Ryo Sasaki, DDS, PhD 1,2 Michael Rasse, MD, DDS, PhD 1 1 Department of Craniomaxillofacial and Oral Surgery, Medical University
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
King's College Hospital Dental School, London, S.E. 5.
 OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
OSTECTOMY AT THE MANDIBULAR SYMPHYSIS J. H. SOWRAY, B.D.S., F.D.S.R.C.S. (Eng.), L.R.C.P., M.R.C.S. and R. HASKELL, M.B., B.S., F.D.S.R.C.S. (Eng.). King's College Hospital Dental School, London, S.E.
Reconstruction of large oroantral defects using a pedicled buccal fat pad
 Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
Yang et al. Maxillofacial Plastic and Reconstructive Surgery (2018) 40:7 https://doi.org/10.1186/s40902-018-0144-6 Maxillofacial Plastic and Reconstructive Surgery CASE REPORT Open Access Reconstruction
Learning Objectives. Head and Neck Cancer: Post-Treatment Changes. Neck Dissection Classification * Radical neck dissection. Radical Neck Dissection
 Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
New innovations in craniomaxillofacial fixation: the 2.0 lock system
 LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
LECTURE New innovations in craniomaxillofacial fixation: the 2.0 lock system Brian Alpert, Rolf Gutwald1 and Rainer Schmelzeisen1 Departments of Oral & Maxillofacial Surgery and Surgical & Hospital Dentistry,
RECONSTRUCTION OF SEGmental
 ORIGINAL ARTICLE Combining Use of Resin Models With External Fixation in Mandibular Reconstruction Emre Vural, MD; James C. Yuen, MD Objective: To obtain accurate occlusion in mandibular reconstruction
ORIGINAL ARTICLE Combining Use of Resin Models With External Fixation in Mandibular Reconstruction Emre Vural, MD; James C. Yuen, MD Objective: To obtain accurate occlusion in mandibular reconstruction
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area.
 Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Mandible External Fixator II. Provides treatment for fractures of the maxillofacial area. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
ORIGINAL ARTICLE. most commonly result. involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial
 ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
Patient information booklet Orthognathic Surgery
 Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
Patient information booklet Orthognathic Surgery 2 Table of contents This patient information booklet contains all the answers to your questions regarding orthognathic surgery. + + + + + + What is Orthognathic
The resident will be assigned to be on call with the Oral and Maxillofacial service. Call will be set according to PARO guidelines.
 Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
Goals and Objectives for the Otolaryngology-Head & Neck Resident on the Oral and Maxillofacial Surgery (OMFS) Rotation St. Catharines General Hospital (1 four-week rotational block) During the second year
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Research report for MSc Dent. University of Witwatersrand. Faculty of health science. Dr J Beukes. Student number: h
 Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Research report for MSc Dent University of Witwatersrand Faculty of health science Dr J Beukes Student number: 9507510h Supervisor: Prof JP Reyneke October 2011 1 1. Title 2. Aim 3. Introduction 4. Objectives
Case Report. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System.
 Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Case Report Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System and MatrixORTHOGNATHIC Plating System. Orthognathic Correction of Class II Open Bite. Using the Piezoelectric System
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
CHAPTER 8 SECTION 1.4 ORAL SURGERY TRICARE/CHAMPUS POLICY MANUAL M DEC 1998 SPECIAL BENEFIT INFORMATION
 TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
TRICARE/CHAMPUS POLICY MANUAL 6010.47-M DEC 1998 SPECIAL BENEFIT INFORMATION CHAPTER 8 SECTION 1.4 Issue Date: October 8, 1986 Authority: 32 CFR 199.4(e)(10) I. DESCRIPTION There are certain oral surgical
Mandibular Distraction Micro Zurich II Distractors
 MANDIBULAR DISTRACTION Mandibular Distraction Micro Zurich II Distractors Early intraoral distraction therapy for babies and infants aged up to one year requires distractors with an especially small profile
MANDIBULAR DISTRACTION Mandibular Distraction Micro Zurich II Distractors Early intraoral distraction therapy for babies and infants aged up to one year requires distractors with an especially small profile
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
(loco-regional disease)
 (loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
(loco-regional disease) (oral cavity) (circumvillae papillae) (subsite) A (upper & lower lips) B (buccal membrane) C (mouth floor) D (upper & lower gingiva) E (hard palate) F (tongue -- anterior 2/3 rds
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Osteoradionecrosis of Jaw in Head and Neck Cancer Patient Treated with Free Iliac Bone and Umbilical Fat Pad Graft
 Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
Maxillofac Plast Reconstr Surg 2014;36(2):62-66 http://dx.doi.org/10.14402/jkamprs.2014.36.2.62 ISSN 2288-8101(Print) ISSN 2288-8586(Online) Case Report Osteoradionecrosis of Jaw in Head and Neck Cancer
ORIGINAL ARTICLE. The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited. decades, the range of reconstructive
 ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization
 Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
Assessment of Relapse Following Intraoral Vertical Ramus Osteotomy Mandibular Setback and Short-term Immobilization Koroush Taheri Talesh, DDS, a Mohammad Hosein Kalantar Motamedi, DDS, b Mahdi Sazavar,
CT findings of osteoradionecrosis of the mandible
 CT findings of osteoradionecrosis of the mandible Poster No.: C-2569 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Abreu e Silva, M. J. Magalhães, N. Costa, S. Ramos Alves, M. V. P. P. Gouvea;
CT findings of osteoradionecrosis of the mandible Poster No.: C-2569 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Abreu e Silva, M. J. Magalhães, N. Costa, S. Ramos Alves, M. V. P. P. Gouvea;
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Circumferential skin defect - Ilizarov technique in plastic surgery
 Brief Communication Circumferential skin defect - Ilizarov technique in plastic surgery Vrisha Madhuri, Shankar R. Kurpad, Manasseh Nithyananth, Thilak S Jepegnanam, V. T. K. Titus, Prema Dhanraj Department
Brief Communication Circumferential skin defect - Ilizarov technique in plastic surgery Vrisha Madhuri, Shankar R. Kurpad, Manasseh Nithyananth, Thilak S Jepegnanam, V. T. K. Titus, Prema Dhanraj Department
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps
 World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
World Articles of Ear, Nose and Throat ---------------------Page 1 Reconstruction for Oral Neoplasms in Indian Setup: Redebating the Utility of Radial Artery Free Flaps Authors: Ranjan G Aiyer*, Rahul
Cancer of the Oral Cavity
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology Cancer of the Oral Cavity Ashok Shaha Principals of Management of Oral Cancer A)
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases
 Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Placement of implants in the mandible reconstructed with free vascularized fibula flap: comparison of 2 cases Mehmet Kürkcü, DDS, MSc, PhD, a Mehmet Emre Benlidayı, DDS, b Cem Kurtoğlu, DDS, PhD, c and
Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor
 Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
Plastic Surgery International Volume 2011, Article ID 421245, 5 pages doi:10.1155/2011/421245 Clinical Study Open Reduction of Subcondylar Fractures Using a New Retractor Akira Sugamata, 1 Naoki Yoshizawa,
The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases
 CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
CASE REPORT http://dx.doi.org/10.5125/jkaoms..40.2.91 pissn 2234-7550 eissn 2234-5930 The treatment of malocclusion after open reduction of maxillofacial fracture: a report of three cases Sung-Suk Lee,
SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
Intraoral mandibular distraction osteogenesis: special attention to treatment planning
 Journal of Cranio-Maxillofacial Surgery (2001) 29, 254 262 # 2001 European Association for Cranio-Maxillofacial Surgery doi:10.1054/jcms.2001.0235, available online at http://www.idealibrary.com on Intraoral
Journal of Cranio-Maxillofacial Surgery (2001) 29, 254 262 # 2001 European Association for Cranio-Maxillofacial Surgery doi:10.1054/jcms.2001.0235, available online at http://www.idealibrary.com on Intraoral
Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy
 1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
1 Variations in the anatomical dimensions of the mandibular ramus and the presence of third molars: its effect on the sagittal split ramus osteotomy J. Beukes 1,, J. P. Reyneke 1,2,3,4, P. J. Becker 5,6
Case Study. Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor.
 Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Case Study Micrognathia Secondary to Pierre Robin Sequence. Treated with distraction osteogenesis using an internal mandible distractor. Micrognathia Secondary to Pierre Robin Sequence Patient profile
Correction of Dentofacial Deformities (Orthognathic Surgery)
 Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
Correction of Dentofacial Deformities (Orthognathic Surgery) BDS, MSc, German board of Oral and Maxillofacial Surgery ( Berlin-Germany), Doctoral degree by LBMS Definition Orthognathic surgery is a combination
THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY
 Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Simultaneous gap arthroplasty and intraoral distraction and secondary contouring surgery for unilateral temporomandibular joint ankylosis
 Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Sharma et al. Maxillofacial Plastic and Reconstructive Surgery (2016) 38:12 DOI 10.1186/s40902-016-0058-0 CASE REPORT Open Access Simultaneous gap arthroplasty and intraoral distraction and secondary contouring
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Survival impact of cervical metastasis in squamous cell carcinoma of hard palate
 Vol. 116 No. 1 July 2013 Survival impact of cervical metastasis in squamous cell carcinoma of hard palate Quan Li, MD, a Di Wu, MD, b,c Wei-Wei Liu, MD, PhD, b,c Hao Li, MD, PhD, b,c Wei-Guo Liao, MD,
Vol. 116 No. 1 July 2013 Survival impact of cervical metastasis in squamous cell carcinoma of hard palate Quan Li, MD, a Di Wu, MD, b,c Wei-Wei Liu, MD, PhD, b,c Hao Li, MD, PhD, b,c Wei-Guo Liao, MD,
Long-term success for osteointegrated
 CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
CASE REPORT Symphyseal Bone Cylinders Tapping With the Dental Implant Into Insufficiency Bone Situated Esthetic Area at One-Stage Surgery: A Case Report and the Description of the New Technique Umut Tekin,
Spontaneous Regeneration of the Mandible after Hemimandibulectomy:
 Case Report Spontaneous Regeneration of the Mandible after Hemimandibulectomy: Report of a Case A. Khodayari 1, A. Khojasteh 2, MT. Kiani 3, A. Nayebi 4, L. Mehrdad 5, M. Vahdatinia 6 1 DMD, MS. Associate
Case Report Spontaneous Regeneration of the Mandible after Hemimandibulectomy: Report of a Case A. Khodayari 1, A. Khojasteh 2, MT. Kiani 3, A. Nayebi 4, L. Mehrdad 5, M. Vahdatinia 6 1 DMD, MS. Associate
Buccal Corticotomy for Closure of Oroantral Openings: Case Report
 Turk J Med Sci 34 (2004) 409-414 TÜB TAK SHORT REPORT Buccal Corticotomy for Closure of Oroantral Openings: Case Report Bedrettin Cem fiener, Hasan GAR P, Faysal U URLU, Kamil GÖKER Department of Oral
Turk J Med Sci 34 (2004) 409-414 TÜB TAK SHORT REPORT Buccal Corticotomy for Closure of Oroantral Openings: Case Report Bedrettin Cem fiener, Hasan GAR P, Faysal U URLU, Kamil GÖKER Department of Oral
Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document.
 ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
ORTHOGNATHIC SURGERY Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Case Scenario. 7/13/12 Anterior floor of mouth biopsy: Infiltrating squamous cell carcinoma, not completely excised.
 Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
Case Scenario 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of alcohol.
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION
 COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
COMPARISON OF MINIPLATES AND RECONSTRUCTION PLATES IN MANDIBULAR RECONSTRUCTION Richard J. Shaw, FRCS, 1 A. N. Kanatas, MFDS, 2 Derek Lowe, C Stat, MSc, 1 James S. Brown, FRCS, MD, 1 Simon N. Rogers, FRCS,
ORIGINAL ARTICLE. Condylar Prostheses in Head and Neck Cancer Reconstruction
 Condylar Prostheses in Head and Neck Cancer Reconstruction Alpen Patel, MD; Robert Maisel, MD ORIGINAL ARTICLE Objective: To discuss the use of condylar prostheses after mandibular resection for tumor.
Condylar Prostheses in Head and Neck Cancer Reconstruction Alpen Patel, MD; Robert Maisel, MD ORIGINAL ARTICLE Objective: To discuss the use of condylar prostheses after mandibular resection for tumor.
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.
 This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
This Presentation Is Trademarked by Lawrence H. Zager, D.D.S.! The next presentation is from the private collection of patient s treated in my practice with the use of implants and other prosthetic devices
Large Dentigerous Cyst
 Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Volume 16.2.1 Feb 2016 This Lecture Series qualifies for 0.5 Informal CPD Learning Hours Large Dentigerous Cyst By Dr Hassem Geha A 55 year-old male presented with a painless swelling in the right mandible.
Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle
 Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Acta Orthop. Belg., 2009, 75, 611-615 ORIGINAL STUDY Treatment of non-union of forearm bones with a free vascularised cortico - periosteal flap from the medial femoral condyle Luc DE SMET From the University
Osteotomy of the Premaxilla
 182 J. max.-fac. Surg. 8 (1980) 182-186 Osteotomy of the Premaxilla John BROUNS, Peter EGYEDI Department of Maxillo-Facial Surgery (Head: Prof. P. Egyedi, M.D., D.M.D.) State University of Utrecht, The
182 J. max.-fac. Surg. 8 (1980) 182-186 Osteotomy of the Premaxilla John BROUNS, Peter EGYEDI Department of Maxillo-Facial Surgery (Head: Prof. P. Egyedi, M.D., D.M.D.) State University of Utrecht, The
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
University of Groningen. Dental implants in maxillofacial prosthodontics Korfage, Anke
 University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
University of Groningen Dental implants in maxillofacial prosthodontics Korfage, Anke DOI: 10.1016/j.bjoms.2014.05.013 10.1016/j.ijom.2013.04.003 10.1002/hed.24053 IMPORTANT NOTE: You are advised to consult
Case Scenario 1. 7/13/12 Anterior floor of mouth biopsy: Infiltrating squamous cell carcinoma, not completely excised.
 Case Scenario 1 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of
Case Scenario 1 7/5/12 History A 51 year old white female presents with a sore area on the floor of her mouth. She claims the area has been sore for several months. She is a current smoker and user of
Combined tongue flap and V Y advancement flap for lower lip defects
 British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
British Journal of Plastic Surgery (2005) 58, 258 262 CASE REPORTS Combined tongue flap and V Y advancement flap for lower lip defects Kenji Yano*, Ko Hosokawa, Tateki Kubo Department of Plastic and Reconstructive
Oral and Maxillofacial Surgery Privileges REAPPOINTMENT Effective from July 1, 2015 to June 30, 2016
 Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the Health Authority or Hospital, effective: 11/Dec/2014.
Initial privileges (initial appointment) Renewal of privileges (reappointment) All new applicants must meet the following requirements as approved by the Health Authority or Hospital, effective: 11/Dec/2014.
Interesting Case Series. Virtual Surgical Planning in Orthognathic Surgery
 Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
Interesting Case Series Virtual Surgical Planning in Orthognathic Surgery Suraj Jaisinghani, MS, a Nicholas S. Adams, MD, b,c Robert J. Mann, MD, b,c,d John W. Polley, MD, b,c,d, and John A. Girotto, MD,
IN 1996, BLACKWELL et al1 reported. The Bridging Lateral Mandibular Reconstruction Plate Revisited ORIGINAL ARTICLE
 The Bridging Lateral Mandibular Reconstruction Plate Revisited Keith E. Blackwell, MD; Victor Lacombe, MD ORIGINAL ARTICLE Background: Lateral oromandibular reconstruction using a soft tissue free flap
The Bridging Lateral Mandibular Reconstruction Plate Revisited Keith E. Blackwell, MD; Victor Lacombe, MD ORIGINAL ARTICLE Background: Lateral oromandibular reconstruction using a soft tissue free flap
Case Report. Eduardo Yugo Suzuki a ; Masayo Watanabe b ; Boonsiva Buranastidporn c ; Yoshiyuki Baba d ; Kimie Ohyama e ; Masatoshi Ishii f
 Case Report Simultaneous Maxillary Distraction Osteogenesis Using a Twin-Track Distraction Device Combined with Alveolar Bone Grafting in Cleft Patients: Preliminary Report of a Technique Eduardo Yugo
Case Report Simultaneous Maxillary Distraction Osteogenesis Using a Twin-Track Distraction Device Combined with Alveolar Bone Grafting in Cleft Patients: Preliminary Report of a Technique Eduardo Yugo
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation.
 LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
LCP Medial Distal Tibia Plate, without Tab. The Low Profile Anatomic Fixation System with Angular Stability and Optimal Screw Orientation. Technique Guide LCP Small Fragment System Table of Contents Introduction
Maxillary Reconstruction with the Free Fibula Flap
 Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
International J. of Healthcare and Biomedical Research, Volume: 03, Issue: 01, October 2014, Pages
 Original article: Distraction osteogenesis following gap arthroplasty to correct facial asymmetry - a defined protocol in treatment of patients with temporomandibular joint ankylosis. 1Dr. Babu S. Parmar,
Original article: Distraction osteogenesis following gap arthroplasty to correct facial asymmetry - a defined protocol in treatment of patients with temporomandibular joint ankylosis. 1Dr. Babu S. Parmar,
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework
 Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Case report: Replacement of failing 2 stage implants by basal implants and conventional bridgework Authors Dr. Aleksandar Lazarov Solunska Str. 3 BG-1000 Sofia Bulgaria Email: alex.lazarov@yahoo.co.uk
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
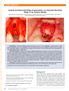 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
